Behavioral Med OSCE
1/35
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
36 Terms
if your patient has this history, what diagnosis are you thinking?
- persistent low mood for the past 6-7 months
- they no longer enjoy painting or hiking like they use to
- sleep a lot, but still feel tired during the day
- they feel like they are a "burden" to their family
major depressive disorder
if you are suspecting MDD (major depressive disorder) as your patient's diagnosis, what are some things you will want to ask about/discuss?
PHQ-9 → in the past 2 weeks, 5 or more of the following:
1) Feeling down, depressed, or hopeless?
2) Little interest or pleasure in doing things (anhedonia)?
3) Trouble falling or staying asleep, or sleeping too much?
4) Feeling tired or having little energy?
5) Poor appetite or overeating?
6) Feeling bad about yourself?
7) Trouble concentrating on things?
8) Moving/speaking so slowly that others have noticed? Or being so fidgety/restless?
9) Thoughts that you would be better off dead or of hurting yourself in some way?
**ask about manic or hypomanic episodes (to rule out bipolar)**
treatment for MDD?
SPEAK (Schedule, Pleasurable activities, Exercise, Assertiveness by letting others know opinions/wants/needs, Kind thoughts about oneself)
CBT (cognitive behavioral therapy)
SSRI (Sertraline (Zoloft) 50mg daily, Escitalopram (Lexapro) 10 mg daily)
f/u in 6 weeks
if your patient has this history, what diagnosis are you thinking?
Hx of depressive episodes
2 months ago they had a week of extreme energy and made grandiose business plans
has spent a lot of money on some recent impulsive purchases
now, they are feeling very depressed and are struggling to get out of bed
bipolar disorder
if you are suspecting bipolar disorder as your patient's diagnosis, what are some things you will want to ask about/discuss?
ask if they have had a period where they felt unusually confident, barely needed sleep, or were extremely productive?
ask about thoughts of self-harm or suicide
treatment for bipolar disorder?
CBT (identify and challenge cognitive distortions)
mood stabilizers (lithium 300 mg BID to start, target is 600 mg BID) (clozapine (antipsychotic) 12.5 mg QHS to start, target is 200 mg daily)
f/u in 2 weeks
if your patient has this history, what diagnosis are you thinking?
- has been feeling very worried over the past 7 months
- has difficulty sleeping at night due to racing thoughts
- has had no panic attacks or depressive episodes
generalized anxiety disorder (GAD)
if you are suspecting generalized anxiety disorder (GAD) as your patient's diagnosis, what are some things you will want to ask about/discuss?
GAD-7 *not at all = 0, several days = 1, more than 1/2 = 2, nearly every day = 3*
1) feeling nervous, anxious, on edge
2) not being to stop/control worrying
3) worrying too much about different things
4) trouble relaxing
5) being so restless, hard to sit still
6) easily annoyed/irritable
7) afraid something awful might happen
5-9 is mild, 10-14 is moderate, 15-21 is severe
treatment for generalized anxiety disorder?
Explain the diagnosis
lifestyle changes (sleep, exercise, minimize caffeine and alcohol)
couseling - CBT
SSRI: paroxetine 10mg QD or escitalopram 5 mg QD
f/u in 6 weeks
if your patient has this history, what diagnosis are you thinking?
has been having episodes of heart racing, chest tightness, dizziness, SOB
they are now avoiding crowded places to avoid another attack
panic disorder
if you are suspecting panic disorder as your patient's diagnosis, what are some things you will want to ask about/discuss?
ask if they have ever had a sudden attack of intense fear with their heart racing or trouble breathing
ask what they think might have triggered it
treatment for panic disorder?
address triggers
CBT
SSRI (paroxetine 10mg QD)
f/u in 6 weeks
if your patient has this history, what diagnosis are you thinking?
- they think that the government is spying on them through the phone
- they hear voices whispering threats
- have disorganized speech and difficulty following conversations
- social isolation over the past year
schizophrenia
if you are suspecting schizophrenia as your patient's diagnosis, what are some things you will want to ask about/discuss?
ask if they hear voices, see things others don't, lack of motivation
2 of the 5 need to occur for greater than or equal to 6 months
Positive: hallucinations, delusions, disorganized thinking (flight of ideas)
Negative: reduced emotional expression, poverty of speech, anhedonia, lack of motivation, lack of desire to form social relationships
treatment for schizophrenia?
CBT
first-gen antipsychotic (haloperidol 0.5mg BID) - meds are only helpful for positive sx
f/u in 2 weeks
A patient with newly diagnosed schizophrenia is set to be prescribed medications and they ask what side effects they should be aware of
Extrapyramidal side effects (EPS) - haloperidol
dystonia (involuntary muscle contraction)
parkinsonism (cogwheel rigidity)
tardive dyskinesia
CV
QT prolongation (monitor with EKG) - can lead to arrhythmias
Sedation
Anticholingeric
constipation
urinary retention
dry mouth
cog impairement
Metabolic syndrome
weight gain
if your patient has this history, what diagnosis are you thinking?
- smoking for the past 20+ years
- they have previously tried quitting but had strong cravings and irritability
tobacco use disorder
if you are suspecting tobacco use disorder as your patient's diagnosis, what are some things you will want to ask about/discuss?
ask if they have tried quitting before to assess their willingness to quit
ask why they are worried about quitting or why they smoke
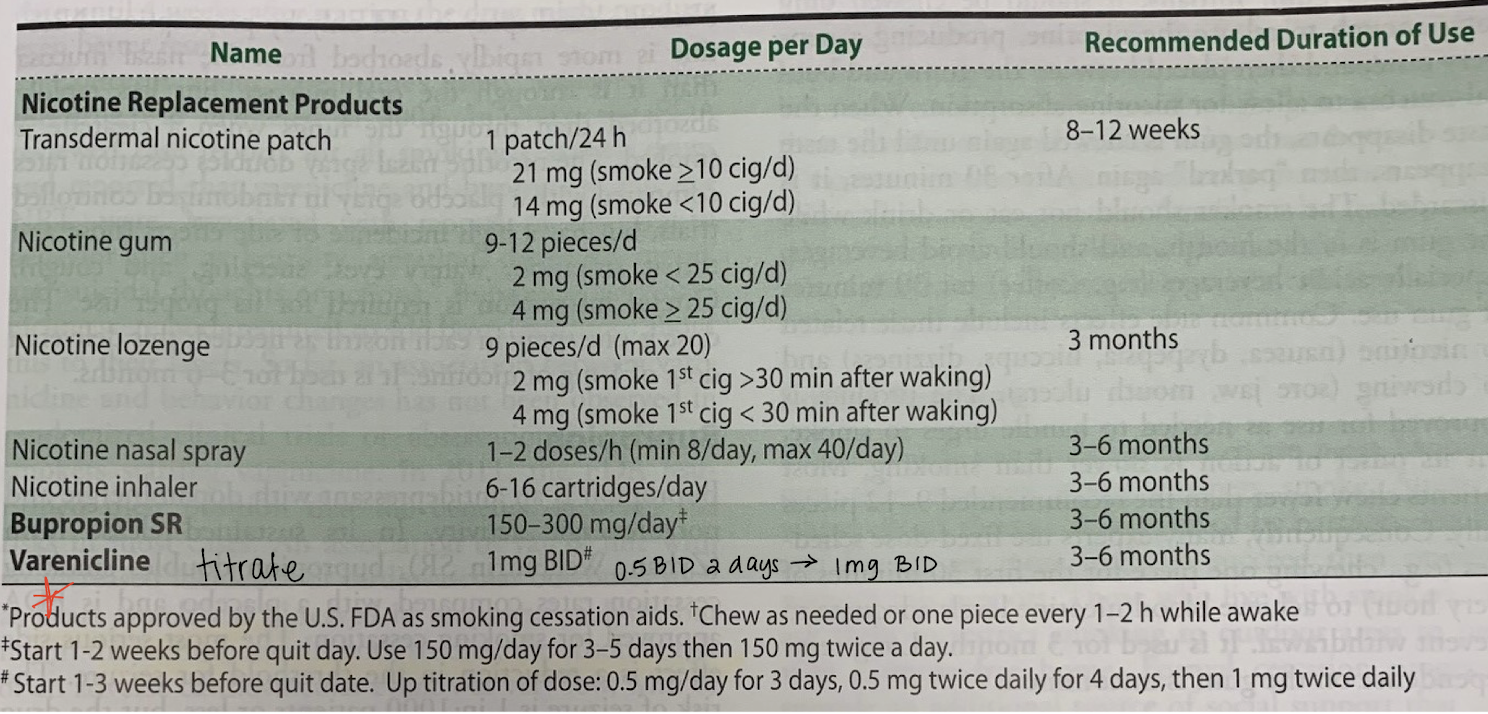
treatment for tobacco use disorder?
smoking cessation program and counseling
transdermal nicotine patch (1 patch/24 hr) + nicotine gum (1 piece PRN, 9-12/day)
and/or
2 weeks before quitting:
Chantix (varenicline 1mg BID; needs titrated up) or Wellbutrin (buproprion SR 150mg QD x 3 days, then 150mg BID; do not use in hx of seizure)
f/u in 2 weeks
*key is to provide a nicotine replacement x 2 (patch + other NR) or NR + behavioral smoking cessation support
if your patient has this history, what diagnosis are you thinking?
- drinks wine daily to "take the edge off"
- multiple DUI arrests in the past year
- they have tried cutting back but felt shaky and irritable
alcohol use disorder
if you are suspecting alcohol use disorder as your patient's diagnosis, what are some things you will want to ask about/discuss?
"ASK," "ASSESS"
CAGE questions:
felt you need to Cut back on drinking?
have people Annoyed you by criticizing your drinking?
ever felt Guilty about your drinking?
Eye-opener
(1 = needs more thorough assessment, 2 = high likelihood)
what test can you use for further assessment of AUD?
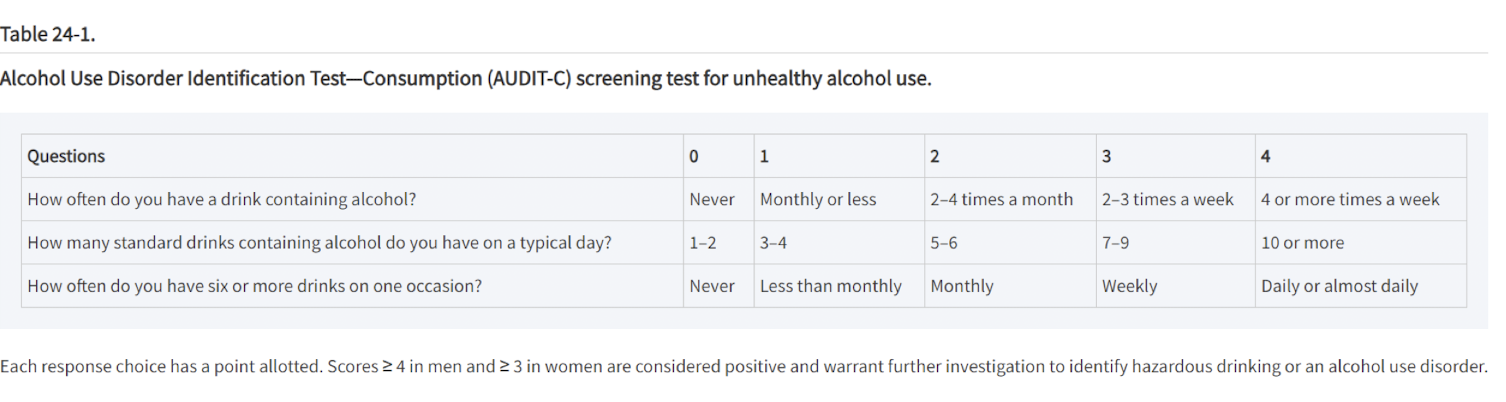
AUDIT (Alcohol Use Disorders Identification Test)
how often do you have a drink containing alcohol?
how many standard drinks containing alcohol do you have on a typical day?
how often do you have 6 or more drinks on one occasion?
What are the physical exam and lab findings for alcohol abuse?
PE:
palmar erythema
gynecomastia
facial rash
Labs:
MCV
increased AST, ALT, GGT
ETOH level increased
conduct urine drug test
treatment for alcohol use disorder?
"ADVISE," "ASSIST"
counseling, AA
Outpt:
(mild) withdrawal: 25-50mg chlordiazepoxide (Librium) PRN Q4-6 hours initially, then taper + biopsychosocial approach
naltrexone (50mg QD). - outpatient tx maintenance
Inpt:
benzodiazepine to depress CNS
hydration
electrolyte correction
thiamine, folic acid, mulitvitamin
f/u in 2 weeks
if your patient has this history, what diagnosis are you thinking?
- has chronic back pain for which they were initially prescribed oxycodone
- they are now buying pills from friends
- experiences sweating, nausea, body aches when they don't take them
opioid use disorder
diagnosis (stages) for opiate withdrawal?
0 - craving, anxiety
1 - sweating, yawning, lacrimation, rhinorrhea
2 - above sxs, mydriasis, tremor, anorexia, myalgias, cold/hot flases
3/4 - above sxs, elevated HR, BP, temp, RR
severe - N/V/D, orgasm
treatment for opioid use disorder?
counseling, narcotics anonymous
Suboxone (buprenorphine/naloxone 8mg/2mg SL films QD #14)
or
naltrexone (25mg QD) (for maintenance only)
send home with naloxone, counsel on use
if your patient has this history, what diagnosis are you thinking?
- prescribed Xanax years ago for anxiety
- they now take higher doses to get the same effect
- they feel jittery or anxious without them
benzodiazepine dependence
treatment for benzodiazepine dependence?
taper off the benzos
treat underlying condition (anxiety/sleep)
if your patient has this history, what diagnosis are you thinking?
- taking Adderall without a prescription for focus
- stays awake for long hours, talks fast
- has lost weight and feels anxious
amphetamine dependence
treatment for amphetamine dependence?
individual or group therapy and/or intensive outpatient therapy
if your patient has this history, what diagnosis are you thinking?
- bruises on arms and face at different stages of healing
- partner controls her the patients finances
- flinches when asked about home life
intimate partner violence (IPV)
if you are suspecting intimate partner violence as your patient's diagnosis, what are some things you will want to ask about/discuss?
HITS: have you ever been...
Hit
Insulted
Threatened
Screamed at
SAFE:
what stress do you experience in relationship? do you feel safe?
are there situations you are afraid or abused?
are friends/family aware?
do you have an emergency plan? (would you like to talk to a counselor, social worker, or me about one?)
treatment for IPV?
refer to counseling, provide resources
assess safety
discuss emergency safety planning
document (photos, encounter location(s), disposition)
what 4 things do you need to have in your plan?
diagnostics, therapeutics, patient education, follow-up
how do you calculate pack years?
packs smoked per day X years smoked
Indicates How much total damage/exposure the lungs (and body) have had - moving foward what screenings are needed and how often (lung cancer)