BSCI202: Blood Vessels, Blood Flow, and Blood Pressure
1/159
Earn XP
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
160 Terms
What is the pathway of distribution of blood vessels?
Arteries → Arterioles → capillaries → venules → veins
What structure is the only one that comes into intimate contact with tissue cells and serve cellular needs?
Capillaries
How long do the blood vessels stretch?
60000 miles
What are the three vessel tunics?
Tunica Intima, Tunica Media, Tunica Externa
Innermost layer with simple squamous endothelium and its underlying connective tissue
Tunica Intima
Middle layer of smooth muscle (thickest in arteries)
Tunica Media
What happens in the Tunica Media?
Vasoconstriction and Vasodilation
When vasoconstriction and vasodilation happens, what is innervated for this to happen?
Sympathetic Nervous System
What is the shrinking of lumen called?
Vasoconstriction
What is the enlarging of lumen called?
Vasodilation
Outer layer of connective tissue for support, with nerve fibers and small vessels (thickest in veins)
Tunica Externa
What are series of small vessels bringing blood to large vessel walls called?
Vasa vasorum
Where does vasa vasorum happen in?
Tunica Externa
What is this vessel?
Structure of wall: Three layers (endothelium, smooth muscle, fibrous connective tissue)
Thickness of wall: Thick
Relative diameter of lumen: Narrow
Direction of blood flow: Away from the heart
Valve: Absent
Oxygen transported: Carries oxygenated blood (except pulmonary artery)
Relative blood pressure: High (=Resistant vessels)
Valves: NO
Artery
What is this vessel?
Structure of wall: Single (endothelium)
Thickness of wall: Very thin (single cell)
Relative diameter of lumen: Very narrow (about size of single erythrocyte)
Direction of blood flow: From arteries to vein (Diffusion)
Valve: Absent
Oxygen transported: Arteriole carries oxygenated blood, venule carries deoxygenated blood
Relative blood pressure: Gradually decreases from the arteriole end to the venule end
Valves: NO
Capillary
What is this vessel?
Structure of wall: Three layers (endothelium, smooth muscle, fibrous connective tissue)
Thickness of wall: Thin
Relative diameter of lumen: Wide
Direction of blood flow: Towards the hearts
Valve: Present
Oxygen transported: Carries deoxygenated blood (except pulmonary vein)
Relative blood pressure: Lowest (=Capacitance vessels)
Valves: YES
Vein
Out of all of the vessels, what is the most abundant?
Systemic veins and venules
What moves away from the heart and their number increases as their diameter decreases?
Arteries
What are the three basic types of arteries?
Elastic (conducting) arteries, Muscular (distributing) arteries, and Arterioles
What arteries are 2.5cm to 1cm and recoil to maintain blood pressure?
Elastic (conducting) arteries
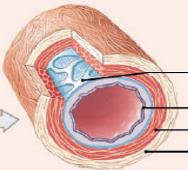
What arteries are 1cm to 0.3mm, control blood flow, and supply groups of organs, organs, and parts of organs?
Muscular (distributing) arteries
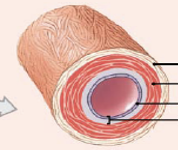
What are almost microscopic and important in regulating blood flow into capillaries and controlling blood pressure?
Arterioles
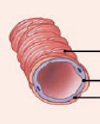
As an artery’s diameter decreases, what happens with elastic fibers and smooth muscle?
decrease in the amount of elastic fibers
increase in the amount of smooth muscle
What are the three types of veins?
Large sized, Medium sized, and Venules
What is the organization of veins?
Same 3 organization as arterial system (Tunica Intima, Tunica, media, and Tunica adventitia)
What is the veins also known as?
Capacitance vessels or Blood reservoir
What vessel has much lower blood pressure and thinner walls than arteries?
Veins
To return blood to the heart, veins have special adaptations which include:
Large-diameter lumens (less resistance to flow) and valves (preventing backflow of blood)
What are specialized, flattened veins with extremely thin walls (ie. coronary sinus of the heart)
Venous sinuses
What are the three types of capallaries?
Continuous, Fenestrated, and Sinusoid
Endothelial cells that form a continuous tube except for intercellular clefts (found in brain, lungs, skeletal and smooth muscle)
Continuous capillaries
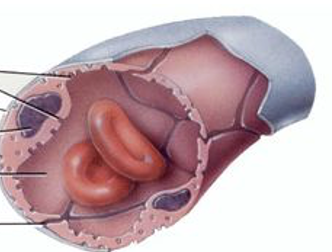
The plasma membrane has fenestrations or pores (Found in kidneys, villi of small intestine, choroid plexus in brain, endocrine glands)
Fenestrated capillaries
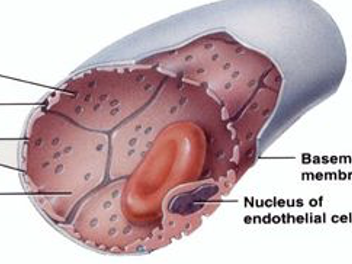
Wider, more winding. Large fenestrations and an incomplete basement membrane. Protein & RBCs can pass (Found in red bone marrow, liver, spleen, anterior pituitary)
Sinusoid capillaries
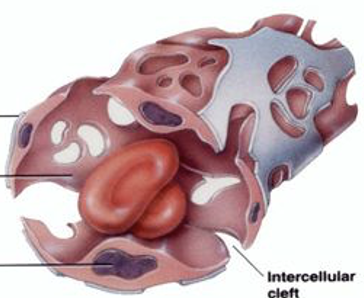
Network of capillaries in tissues
Capillary Beds
What is this an anatomy of a capillary bed?
Terminal arteriole, metarteriole, capillaries, throughfare channel, postcapillary venule
Flow of blood from arteriole to venule through the capillary bed where oxygen and nutrients cross to cells and where carbon dioxide and metabolic waste products cross into blood.
Microcirculation
The cuffs of smooth muscle at the base of true capillaries where its function is to regulate blood flow into the true capillaries. If they are open, exchange happens in tissue cells. If they are closed, blood bypasses the exchange vessels. What is this structure?
Precapillary sphincters
What is a pathway that allows blood to flow directly from the arteriole to the venule, bypassing the true capillaries when precapillary sphincters are closed?
Shunt
When does Capillary exchange occur?
Precapillary sphincters open
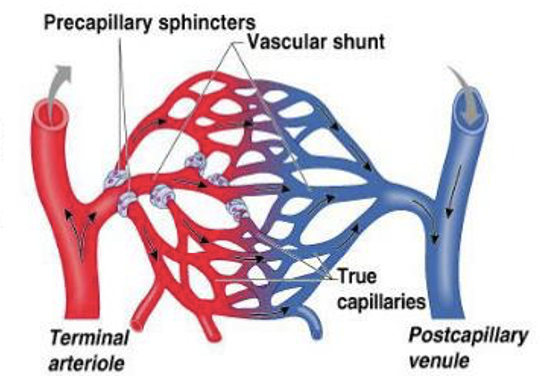
When no capillary exchange occurs as blood shunted through the metarteriole-thoroughfare channel (vascular shunt), what happened?
Precapillary sphincters closed
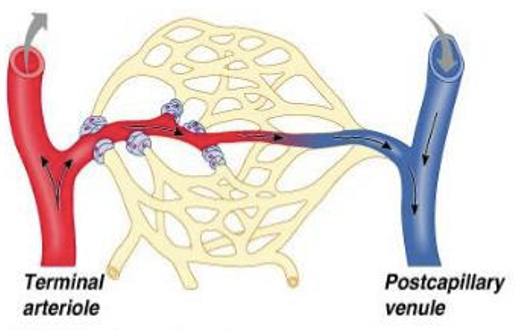
What does the contraction of ventricles generate? The pressure also falls progressively with distance from left ventricle and huge factor includes total volume of blood.
Blood pressure
Highest pressure attained in arteries during systole
systolic blood pressure
Lowest arterial pressure during this diastole
Diastolic blood pressure
When the left ventricle ejects blood into the aorta, what happens to aortic pressure?
Aortic pressure rises
As the left ventricle is relaxing and refilling, what happens to aortic pressure?
Aortic pressure falls
The maximal aortic pressure following rejection (when heart contracts)
systolic pressure
The lowest pressure in the aorta, which occurs just before the ventricle ejects blood into the aorta (when heart relaxes)
diastolic pressure
What is the normal rate of Systolic/Diastolic BP?
120/80
What is the high rate of Systolic/Diastolic BP?
140/90
The resistance to pump blood in the small arterial branches that carry blood to tissues.
Peripheral resistance (TPR)
The volume of blood pumped by heart within a specified time.
Cardiac output
What is the blood pressure formula (abbreviated terms)?
BP=TPR*CO
Blood pressure relies on three factors, what are they?
Blood volume, Peripheral resistance/Diameter of arterioles, Cardiac output
What affects blood volume (with examples)?
Fluid loss (dehydration), Fluid retention (Aldosterone, ADH)
What affects peripheral resistance?
Sympathetic nervous system activity (vasodilation, vasoconstriction), Renin/angiotensin II, and increase in blood viscosity
What affects cardiac output?
Stroke volume (preload, contractility, afterload), Heart rate (sympathetic nervous system, parasympathetic nervous system, and epinephrine)
What is the major cardiovascular variable being regulated in the systemic circulation? It also drives blood flow through all organs (except lungs) and maintenance is required for ensuring adequate blood flow.
Mean arterial pressure (MAP)
The average volume of blood in the systemic arteries (mean arterial blood volume, MABV) is determined by what?
CO and TPR
What is the equation for Mean Arterial pressure (MAP)?
(Pulse pressure/3) + Diastolic pressure
OR
(systolic pressure + 2x diastolic pressure)/3
What is the equation for pulse pressure?
Systolic pressure - diastolic pressure
Cardiac cycle lasts 0.8s and during a cardiac cycle the heart spends 0.3s in systole; 0.5s in diastole. Thus, in calculating the MAP, DBP is doubled (X2) If BP is 120/80, what is the MAP?
93.3 mmHg
If a patient with hypertension undergoes lifestyle changes in hopes of reducing his/her blood pressure, how can you assess the change?
The patient’s blood pressure before lifestyle changes was 180/120 and the blood pressure after lifestyle changes was 170/140, did the lifestyle changes work?
Measuring BP(MAP) before lifestyle change and after lifestyle change (140mmHg → 150mmHg); I have concluded that lifestyle changes did not work, in fact, the blood pressure increased.
If a patient with hypertension undergoes lifestyle changes in hopes of reducing his/her blood pressure, how can you assess the change?
The patient’s blood pressure before lifestyle changes was 145/100 and the blood pressure after lifestyle changes was 150/90, did the lifestyle changes work?
Measuring BP (MAP) before lifestyle change and after lifestyle change (115mmHg → 110mmHg); I have concluded that yes, the lifestyle changes worked (but not significantly).
An increase in cardiac output leads to what? What happens to the total peripheral resistance?
Increase in mean arterial pressure; TPR remains the same
An constant cardiac output leads to what? What happens to the total peripheral resistance?
Increase in mean arterial pressure; TPR increases
Used to calculate the resistance to blood flow in the cardiovascular system
Poiseuille’s Law
How is blood flow affected in vasodilation?
Diameter is doubled → flow increases 16 times
How is blood flow affected in vasoconstriction?
Diameter is halved → flow decreases 1/16 of original flow
How is blood flow affected in Obesity?
Increase in adipose tissue results in lengthening of blood vessel → increase in resistance → decrease in blood flow
How is blood flow affected in Polycythemia?
Increased blood viscosity → decrease blood flow
How is blood flow affected in Dehydration?
Increased viscosity → decrease in blood flow
What is opposition to blood flow due to friction between blood and walls of blood vessels called?
Vascular resistance
What does vascular resistance depends on?
size of lumen, blood viscosity, total blood vessel length
For each 2.2lbs of fat, there is an additional ________ of blood vessels.
400 miles
What hormone promotes Na+ and water retention in the kidneys?
Aldosterone
How does Aldosterone affect BP and blood flow?
increases blood volume and pressure
What is the pathway from aldosterone increasing blood volume to increasing blood pressure (vascular resistance, end diastolic volume, Preload, stroke volume, cardiac output)?
increase blood volume → increase vascular resistance → increase end diastolic volume → increase preload → increase stroke volume → increase cardiac output → increase blood pressure
What is atrial natriuretic factor?
increase of urinary sodium excretion
What is the effect of atrial natriuretic factor?
generalized vasodilation
How does atrial natriuretic factor affect blood pressure?
Decrease in CO → decrease in BP
This hormone helps with water retention and vasopressin
ADH
What effect comes from ADH?
vasoconstriction
How does ADH affect blood pressure (BV, vascular resistance, end diastolic volume, Preload, stroke volume, cardiac output, total peripheral resistance)?
increase BV → Increase VR → Increase EDV → increase SV → Increase CO → Increase TPR → Increase BP
How does the hormones epinephrine and norepinephrine affect blood pressure and blood flow?
fight or flight response → vasoconstriction and vasodilation
Epinephrine and norepinephrine affects most blood vessels which bind to what? Leading to what?
a-adrenergic receptors, leading to vasoconstriction
Epinephrine and norepinephrine affects skeletal and cardiac muscle blood vessels which bind to what? Leading to what?
B-adrenergic receptors, leading to vasodilation
How does vasoconstriction affect the blood pressure (and TPR)?
increase in TPR → Increase in BP
What triggers the renin-angiotensin-aldosterone (RAA) system?
Hyponatremia (low blood sodium) → decreased blood volume → decreased venous return (VR) → decreased end-diastolic volume (EDV) → decreased preload → decreased stroke volume (SV) → decreased cardiac output (CO) → decreased blood pressure (BP), sensed by juxtaglomerular cells in the kidneys.
What enzyme do juxtaglomerular cells release in response to low BP, and what does it do?
They release renin, which catalyzes the conversion of angiotensinogen → angiotensin I (ANG I)
How is angiotensin II (ANG II) formed?
Angiotensin-converting enzyme (ACE) converts angiotensin I (ANG I) → angiotensin II (ANG II)
What are the two main biological actions of angiotensin II (ANG II)?
1. Potent vasoconstrictor → increases total peripheral resistance (TPR) → increases BP.
2. Stimulates release of aldosterone from adrenal glands.
What does aldosterone do in the kidneys?
Stimulates Na⁺ reabsorption, followed by Cl⁻ reabsorption (to maintain electrical neutrality). NaCl reabsorption is followed by obligatory water reabsorption to maintain blood osmolality
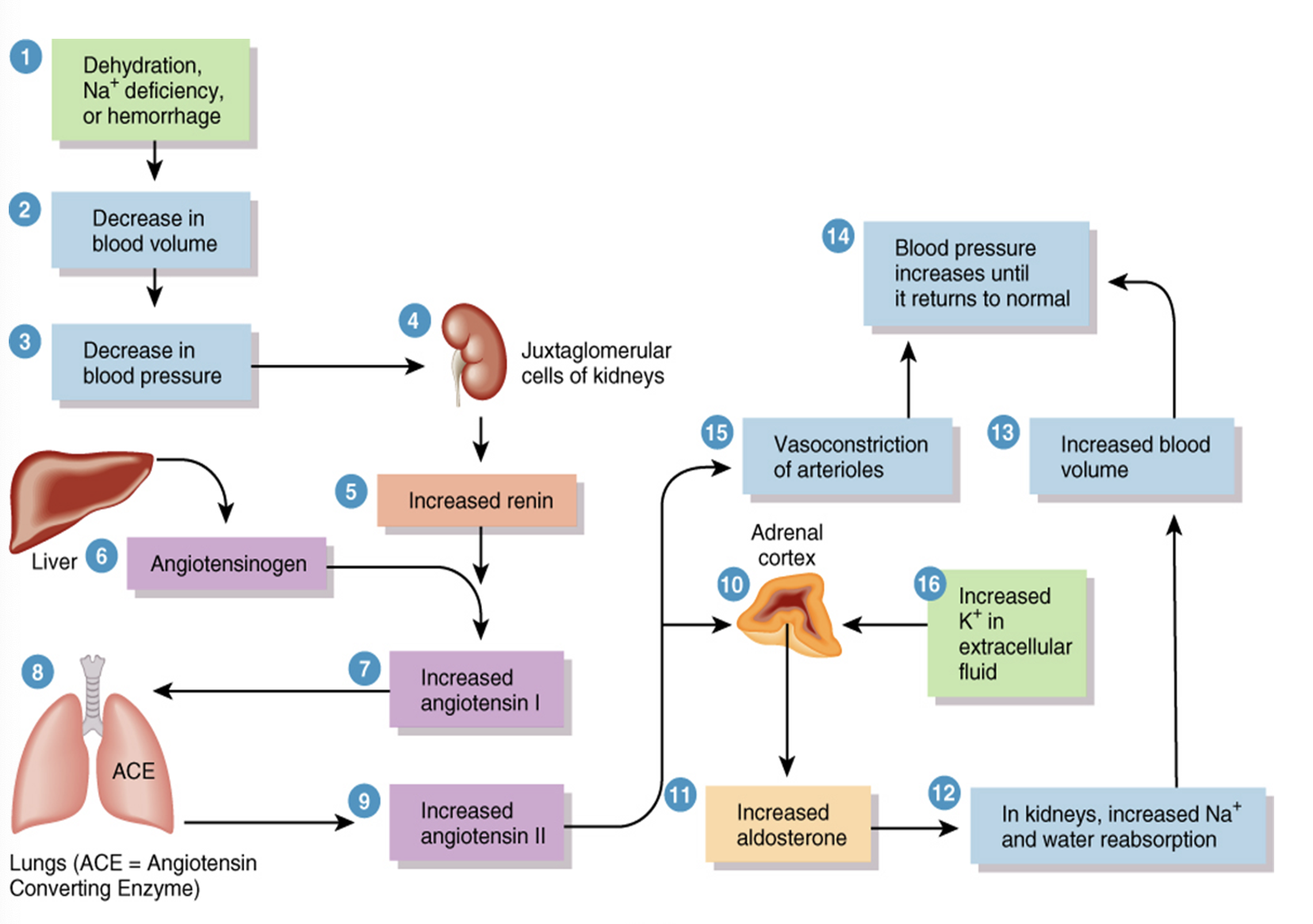
This image represents what?
Renin-Angiotensin-Aldosterone Pathway
How does the RAA system increase blood pressure?
Increase Blood volume → Increase VR → Increase EDV → Increase preload → Increase SV → Increase CO → Increase BP
What can excess angiotensin II and excess aldosterone lead to?
Hypertension
What is the name to the rapid response to the change in pressure (stretch) for the control of blood pressure
Baroreceptor Reflex
What structures is the baroreceptor reflex located in?
Carotid sinus and aortic arch
Increased MAP _________ firing of baroreceptors which _________ sympathetic tone. _________ the parasympathetic tone.
increases; decreases; increases
Decreased MAP _________ firing of baroreceptors which _________ sympathetic tone. _________ the parasympathetic tone.
decreases; increases; decreases
What happens to baroreceptor firing when blood pressure increases?
Baroreceptors increase firing (increase action potential frequency) to the cardiovascular center in the medulla oblongata