Topic 3B- More Exchange and Transport Systems
1/59
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
60 Terms
Why is food broken down into smaller molecules during digestion?
Some biological molecules are too large to fit across cell membranes meaning they can’t be absorbed from the gut to the blood
During digestion, these large molecules are broken down by hydrolysis into smaller molecules which can move across cell membranes
This makes the absorption and transport of these substances easier around the body
How is starch broken down in the body?
Salivary glands and the pancreas secrete amylase which breaks down starch into maltose by hydrolysis of the glycosidic bond between glucose monomers
Membrane-bound disaccharides attached to the cell membrane of epithelial cells lining the ileum called maltase breaks down maltase which is a disaccharide of glucose into glucose monomers by hydrolysis of the glycosidic bond
The molecule has now been broken down enough to be able to be absorbed by epithelial cells
How are lipids broken down?
Lipase breaks down lipids into monoglycerides and fatty acids by hydrolysis of ester bonds
It is made in the pancreas and works in the small intestine
How are lipids absorbed into cell?
Hydrolysed by lipase to form fatty acids and monoglycerides
Bile salts emulsify lipids and cause them to form multiple small, insoluble droplets
This provides a larger surface area than just one large droplet
Micelles containing bile salts, fatty acids and monoglycerides carry these substances to the epithelial lining of the ileum
Fatty acids/ monoglycerides absorbed by diffusion
Triglycerides reformed in cells/chylomircrons made by packaging of triglycerides in golgi apparatus form
Vesicles move to the membrane for exocytosis
What do exopeptidases do?
The break peptide bonds on the outsides of a polypeptide chain (terminal amino acids)
What do endopeptidases do?
Break peptide bonds in the middle of a polypeptide chain
What do dipeptidases do?
Break peptide bonds between dipeptides to give the monomers, amino acids
By what process are amnio acids and monosaccharides absorbed across cell membranes?
Co-transport
What is the structure of haemoglobin?
Quaternary structure protein made up of four polypeptide chains
Each chain has a haem group which contains an iron ion and gives haemoglobin it’s red colour
Each chain as one haem group
How does oxygen bind to haemoglobin?
Haemoglobin has a high affinity for oxygen as each molecule can carry up to four oxygen molecules
In the lungs, oxygen binds to the Fe2+ ion in the haem group, forming an Fe3+ ion
This makes a molecule called oxyhaemoglobin
This is a reversible reaction- oxygen can dissociated from oxyhaemoglobin, turning the molecule back into haemoglobin
What is partial pressure of oxygen (pO2) and carbon dioxide (pCO2)?
A measure of oxygen and carbon dioxide concentration
How is haemoglobin’s affinity for oxygen loading affected by it’s partial pressure?
The affinity increases with partial pressure
At high partial pressures, oxygen loads onto haemoglobin
At low partial pressures, oxygen unloads from oxyhaemoglobin
How is the exchange of oxygen to and from haemoglobin affected by partial pressure?
Oxygen enters the blood at the alveoli where partial pressure is high, so oxygen loads onto haemoglobin to form oxyhaemoglobin
When cells respire, they use up oxygen which lowers the partial pressure
Red blood cells deliver oxygen to these respiring tissues, where it unloads the oxygen
Haemoglobin then returns alveoli to pick up more oxygen
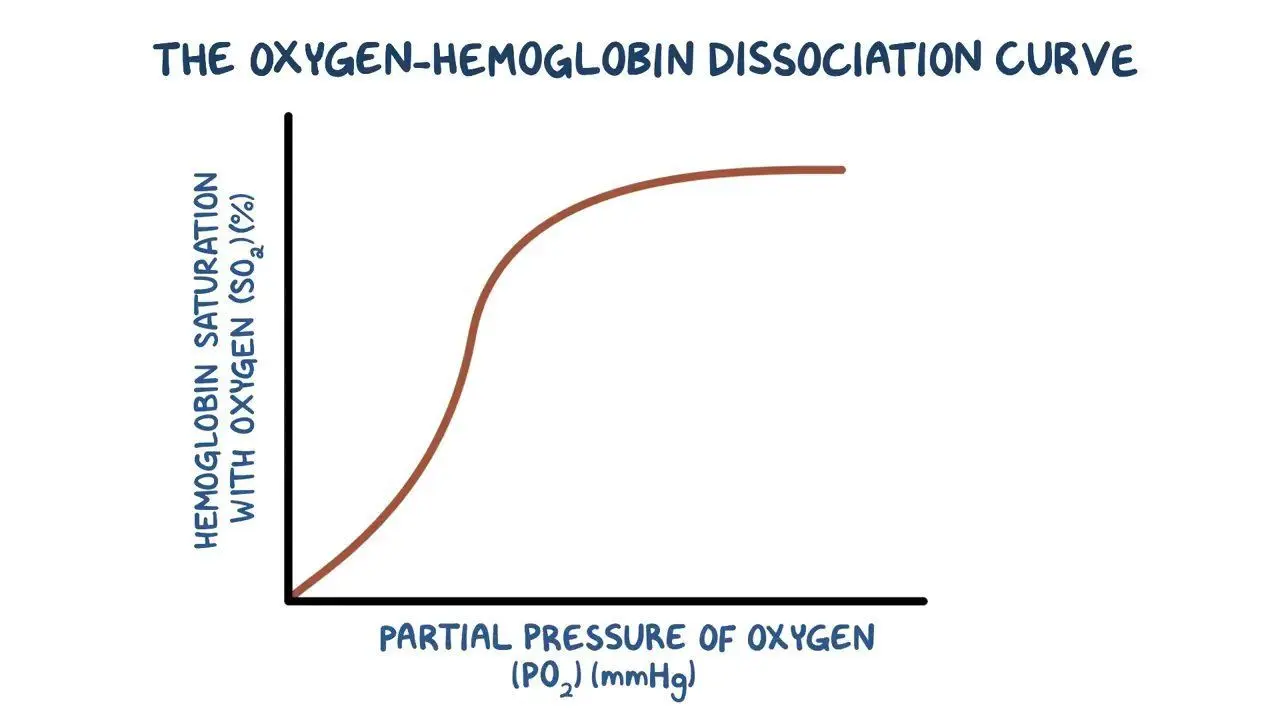
What does a oxygen-haemoglobin dissociation curve show?
It shows how saturated haemoglobin is with oxygen at any given partial pressure
It is S shaped (sigmoid curve)
Where partial pressure is high, haemoglobin has a high affinity for oxygen and vice versa
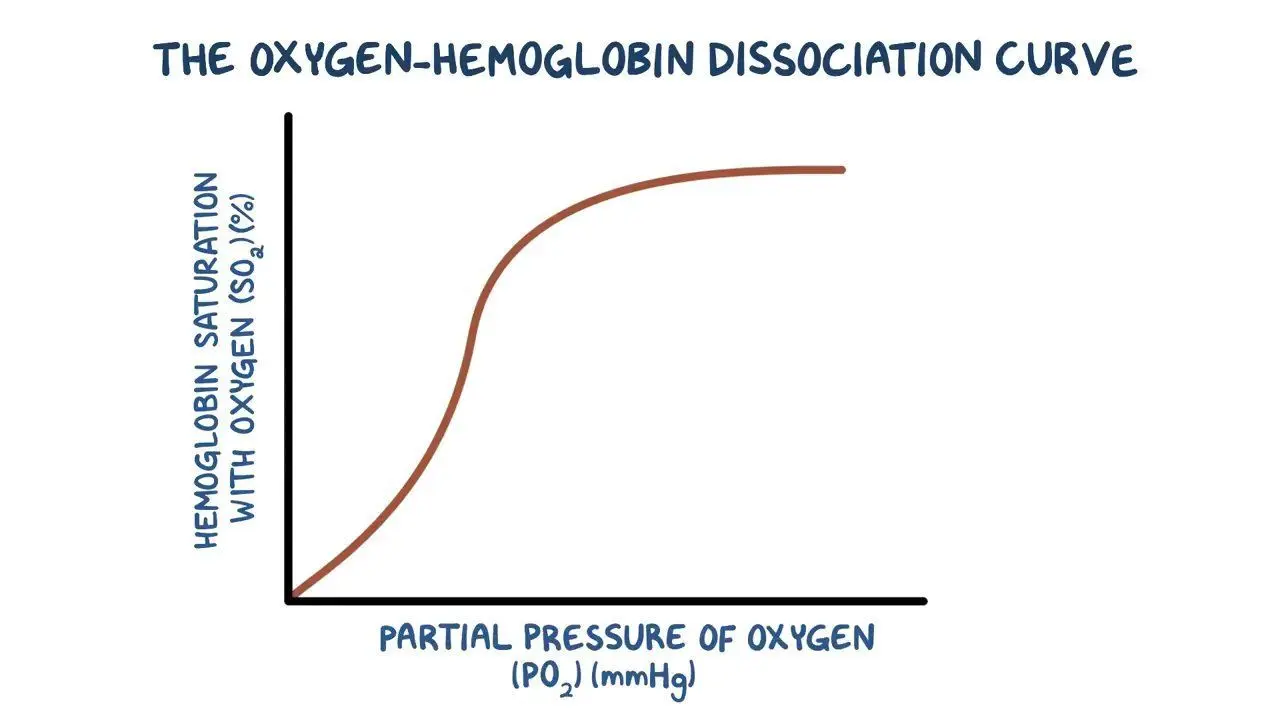
Explain the shape of the oxygen-haemoglobin dissociation curve
When no oxygen is bound to haemoglobin, it is difficult for oxygen to load onto it due to it’s shape which is why the graph is shallow at the start, showing that at low partial pressures, there is a low affinity for the binding of oxygen
When the first oxygen molecule binds, haemoglobin changes shape to make it easier for subsequent oxygen to binds, which is why in the middle of the graph, there is a large increase in %saturation with a small increase of partial pressure as the affinity for oxygen of haemoglobin increases
It once again gets shallow at the top because as 3 oxygen molecules load onto haemoglobin, there are less binding sites available for the last oxygen molecule, decreasing the likelihood that the last oxygen will bind to the last site
How does carbon dioxide concentration affect the shape of oxygen-haemoglobin dissociation curve?
Haemoglobin has a lower affinity for oxygen at any given partial pressure
When cells respire, they increase the partial pressure of carbon dioxide
This increases the rate of oxygen unloading as there is a low partial pressure of oxygen at these respiring cells due to oxygen being used up so the dissociation curve shifts right
The saturation of blood with oxygen is lower for a given partial pressure of oxygen meaning that more oxygen is released
As well as this, dissolved carbon dioxide (carbonic acid) is acidic and can cause the tertiary structure of haemoglobin to change, lowering haemoglobin’s affinity for oxygen, so it is more readily unloaded into respiring tissues
This is called the Bohr shift
What does a shift to the left or right mean in the oxygen-haemoglobin dissociation curve mean?
Left- Higher affinity for oxygen at any given partial pressure
This normally occurs in a low oxygen environment
Organisms that have a low respiratory demand and are living in environment with plentiful oxygen
Right- Low affinity at any given partial pressure
High respiratory demand
Active
High surface SA:V ratio
What blood vessels supplies the heart with oxygen?
The right and left coronary arteries
What are arterioles and venules ?
Arterioles- Very small blood vessels that carry oxygenated blood from an artery to tissues
Venules- Very small blood vessels that return deoxygenated blood from tissues to veins that go to the heart
What blood vessels carry blood into the heart and where are they found?
Vena Cava- Found attached to the right atrium of the heart
Hepatic vein- Connected to liver
Renal vein- Connected to kidney
Pulmonary vein- Delivers oxygenated blood to the heart from the lungs
What blood vessels carry blood away from the heart and where are they found?
Pulmonary artery- Attached to the right ventricle of the heart and carries deoxygenated blood away from heart to lungs
Aorta- carries blood away from heart to other parts of the body
Hepatic artery- Connected to liver
Renal artery- Connected to kidneys
What is the basic structure of all blood vessels?
A tough outer layer that resists pressure changes
A muscle layer that can contract to control the flow of blood
Elastic layer than can stretch and recoil to maintain high blood pressure
A smooth inner endothelium to reduce friction
Lumen through which blood flows
What is the structure of arteries and how are they adapted for their function?
All arteries carry oxygenated blood from the heart to the rest of the body except for the pulmonary artery
Muscle layer allows for the control of blood flow - thicker than in veins
Elastic tissue allows the arteries to stretch and recoil as the heart beats, maintaining high pressure while maintaining shape
The endothelium (inner lining) is folded, allowing for the artery to stretch which aids in maintaining high pressure and is smooth to reduce friction
Protein coat - prevents artery wall splitting
The lumen is the hole where blood flows through
What is the structure of arterioles?
Arteries divide into these smaller vessels called arterioles which form a network throughout the body
The muscle layer is relatively thicker than in arteries- contracting of these muscles allows for the control of blood flow to areas of demand
Arterioles carry blood under lower pressure from arteries to capillaries and therefore have relatively thinner elastic layers
What is the structure of veins and what is their function?
All veins carry deoxygenated blood from the body to the heart except for the pulmonary vein which carries oxygenated blood from the lungs to the heart
Veins take blood back to the heart under low pressure and so have wider lumen and little elastic or muscle tissue
There are valves to prevent the backflow of blood
Blood flow is helped by the contraction of surrounding body muscles
What is the structure of capillaries and how are they adapted for their function?
Substances like glucose and oxygen are exchanged between cells and capillaries
They are always found near to cells in exchange tissues
There are a large number of capillaries to increase SA for exchange (highly branched)
The capillary wall only consists of the endothelium making the walls thin, decreasing diffusion distance
What are networks of capillaries in tissue called?
Capillary beds
What is tissue fluid?
Fluid that surrounds cells in tissues
It is made up from small molecules that leave the blood plasma
Red blood cells and proteins are not present as they are too large to be pushed out of the capillary walls
What happens in pressure filtration with tissue fluid?
There is a higher hydrostatic pressure caused by contraction of the left ventricle at the start of the capillary bed in the arteriole end than in tissue fluid
This difference in hydrostatic pressure forces fluid out of the capillaries into the spaces around cells forming tissue fluid
This consists of glucose, water, oxygen and amino acids
Due to fluid loss and the increasing concentration of plasma proteins that are too large to leave the capillary, the water potential at the venule end decreases to be lower than that of the tissue fluid
Some water re-enters the capillary at the venule end by osmosis
Excess tissue fluid is drained into the lymphatic system
Lymph returns to blood
What is the structure of the heart?
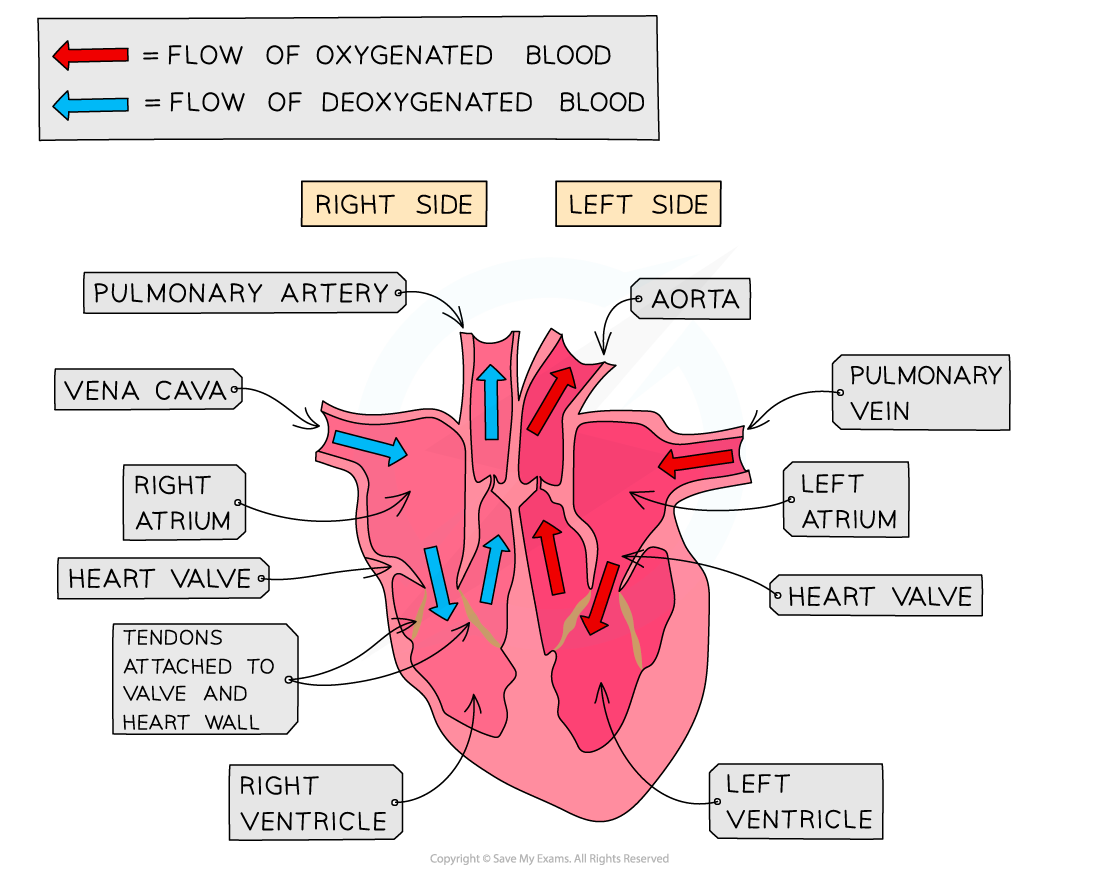
How does blood flow through the heart?
When blood enters the heart, the ventricles are relaxed while the atria contract
This decreases the volume of the atria, increasing the pressure
The pressure behind the atrioventricular valve in the atria is greater than in the ventricle so blood is forced into the ventricle
The ventricles now contract while the atria relax
This decreases the volume of the ventricles, in turn increasing the pressure
Because the pressure in front of the atrioventricular valve is now greater than behind it in the atria, the valve closes to prevent the backflow of blood
An increase in pressure behind the semi-lunar valves means that they will open and allow blood to flow into the aorta/pulmonary artery so blood in forces into these vessels
When the pressure in the pulmonary artery/aorta is higher than in the ventricles, the semi-lunar valves shut as the pressure is front of the valves is now grater than behind it
This prevents the backflow of blood into the ventricles
When blood returns to the heart, the pressure in the vena cava/pulmonary vein increases as the pressure is higher in these vessels than in the atria, causing the atria to fill again
This in turn increases pressure in the atria
As ventricles continue to relax, the pressure in them drops to below the pressure of the atria so the AV valves open allowing blood to flow passively (without contraction) into the ventricles
The atria contract and the process starts again
How does atheroma formation happen?
The endothelium of arteries is normally smooth and unbroken
If damage occurs to the endothelium, white blood cells and lipids from the blood clump together under the lining to form fatty streaks
Over time, white blood cells, lipids and connective tissue build up to form a fibrous plaque called an atheroma
What are the effects of atheroma formation?
The plaque partially blocks the lumen of the artery and restricts blood flow, causing blood pressure to increase
CHD is a cardiovascular disease that occurs when many atheroma have formed, restricting blood flow to heart muscle which can lead to myocardial infarction
What are aneurysms and how are they formed?
Balloon-like swelling of the artery
Atheroma plaques damage and weaken arteries and narrow them, increasing blood pressure
When blood travels through a weakened artery at high pressure, it can push the inner layers of the artery through the outer elastic layer to form a balloon like swelling
This aneurysm may burst, causing a haemorrhage
What is thrombosis on how does it occur?
The formation of a blood clot
Atheroma plaque can rupture the endothelium
This damages the artery wall and leaves a rough surface
Platelets and fibrin accumulate at the site of damage and form a blood clot (thrombus)
This thrombus can cause a complete blockage of the artery or it can become dislodged and block a blood vessel elsewhere in the body
Debris from the rupture can cause another blood clot to form further down the artery
How does myocardial infarction occur and what are the effects
Heart muscle is supplied with blood by the coronary arteries
This blood contains oxygen for the respiration of heart muscle cells
If the coronary artery becomes completely blocked, an area of heart muscle has it’s oxygen supply cut off
This causes myocardial infarction (a heart attack)
Symptoms include pain in the chest and upper body, shortness of breath, sweating
If large areas of the heart are affected, heart failure can occur which is often fatal
What are the common risk factors for cardiovascular disease?
High cholesterol
Cigarette smoking
High blood pressure
Genetic predisposition/Age
How does high cholesterol and diet increase risk of cardiovascular disease?
High cholesterol increases the risk of cardiovascular disease
Cholesterol is one of the main components of fatty deposits that form atheromas which can increase blood pressure and form blood clots than can cause blockages
A diet high in saturated fat increases cholesterol levels
A diet high in salt increases blood pressure
How does cigarette smoking increase the risk of cardiovascular disease?
Nicotine and carbon monoxide increase risk
Nicotine increases blood pressure
Carbon monoxide binds to haemoglobin and reduces the amount of oxygen transported in the blood
Carbon monoxide does not unbind easily
Decreases the amount of antioxidants in the blood which are important for protecting cells from damage
Fewer antioxidants means cell damage in coronary artery walls is more likely, leading to atheroma formation
How does high blood pressure increase the risk of cardiovascular disease?
Increases the risk of damage to artery walls which in turn increases the risk of atheroma formation causing a further increase in blood pressure
Atheromas can cause blood clots to form which can block blood flow, leading to myocardial infarction
Anything that increases blood pressure like being overweight, not exercising, excessive alcohol consumption can increase the risk of cardiovascular disease
How can genetic predisposition and age increase the risk of cardiovascular disease?
Some comorbidities like some form of diabetes cause increase risk
Older age can lead to cardiovascular disease as over time fatty deposits build up
What are the two mass transport systems in plants?
Xylem- transports water and mineral ions up the plant from the roots to the leaves
Phloem- Transports organic substances like sugars up and down the plant
What are xylem vessels?
Long tube-like structures formed from dead cells joined end to end
There are no end walls on these cells, making an uninterrupted tube that allows water to pass up the middle easily
What is transpiration?
Water evaporates from moist cell walls and accumulates in gaps between cells in the leaf
When the stomata open, water moves out of the leaf down it’s concentration gradient
What is the cohesion tension theory of transpiration?
Water evaporates from leaves
This creates tension/suction which pulls more water into the leaf
This is because as water evaporates, water potential decreases, so more water moves to leaf cells by osmosis
Water molecules are cohesive because of hydrogen bonding between molecules meaning they stick together so when some are pulled into the leaf, others follow
This allows a continuous column of water to flow within the plant, allowing it to move upwards
Water enters the stem through the roots
What four factors affect transpiration rate and how?
Light- The stomata open at high light intensity to allow carbon dioxide in for photosynthesis, meaning that water can evaporate out of the stomata, at night they close to conserve water
Temperature- Water molecules at higher temperatures have more KE and therefore evaporate faster and this increases the diffusion gradient between the leaf and the outside, increasing the rate of diffusion out of the leaf
Humidity- Lower humidity means that transpiration rate will be faster as the concentration gradient between the inside and outside of the leaf is increased, increasing transpiration
Wind- Wind can blow away water molecules from the stomata, maintaining a steep concentration gradient, which increases the rate of transpiration
What is a potometer?
Apparatus used to measure the rate of transpiration in plants
Why is a potometer an indirect measurement of water loss in plants?
Because it actually measures water uptake
Water uptake is assumed to be directly related to water loss
How do you set up a potometer?
Cut a plant shoot underwater to prevent air from entering the xylem
You can cut at a slant to increase the surface area available for water uptake
Assemble the potometer in water and insert the shoot in the water
Remove the apparatus from the water but keep the end of the capillary tube submerged in a beaker of water
Make sure the apparatus is airtight
Dry the leaves and allow for the shoot to acclimate, then shut the tap
Remove the end of the capillary tube from the water until one bubble forms, then submerge it again
How can a potometer be used to measure the rate of transpiration?
Record the starting position of the air bubble
Start a stopwatch and record the distance moved by the bubble per unit time
The rate of air bubble movement is an estimation of transpiration rate
Remember to only change one variable at a time
How is phloem tissue adapted for transporting solutes?
Sieve tube elements are living cells that form the tube for transporting solutes
These tubes have no nucleus and few organelles so there are companion cells for each sieve tube element
Companion cells have lots of mitochondria to carry out respiration, providing the energy needed for the active transport of solutes
What is translocation?
The movement of solutes like sucrose and amino acids to where they are needed in a plant
It is an energy-requiring process
It moves solutes from ‘source’ to ‘sink’
Source is where the solute is produced, sink is where they are used up or stored
What is the mass flow hypothesis for translocation?
In the source/leaf, sugars are actively transported into the phloem by companion cells
This lowers the water potential of sieve tube elements and water enters into them by osmosis
This increase in hydrostatic pressure causes mass movement towards the sink/root as solutes are pushed down their pressure gradient
Solutes are then unloaded from the phloem by active transport into the sink
Sugars are then used in respiration or converted in the sink for storage
How is a concentration and pressure gradient maintained from source to sink by enzymes?
At the sink end, enzymes maintain these concentration gradients
They do this by removing solutes from the phloem by active transport, using them in metabolic processes, converting solutes in the sink to something else or breaking them down
This increases water potential in the phloem, so water leaves the sieve tubes by osmosis
This ensures there is always a lower concentration of solutes at the sink that at the source and the movement of water lowers the pressure in the sieve tubes, forming a pressure gradient
How do ringing experiments support the mass flow hypothesis?
If a ring of bark that includes the phloem but not the xylem is removed from a woody stem, a bulge forms above the ring
The fluid from the bulge has a higher concentration of sugars than fluids from below the ring- evidence of the downward flow of sugars
How do aphids support the mass flow hypothesis?
Aphids pierce the phloem of plants and leave mouthparts behind, allowing sap to flow out
The sap flows out quicker near the leaves than further down the stem, supporting the idea of a pressure gradient
How do metabolic inhibitors support the mass flow hypothesis?
An inhibitor which prevents ATP production is put into the phloem, then translocation stops
Evidence that active transport is involved
How can we use radioactive tracers to support the mass flow hypothesis?
Supply a plant with an organic substance like carbon dioxide that has a radioactive label like 14C
This can be supplied to one leaf by being pumped into a container only containing that one leaf
Radioactive carbon is then incorporated into organic substances produced by the leaf which would be moved around the plant by translocation
These movements can be tracked by autoradiography
The plant is killed by freezing it in liquid nitrogen and then the plant is placed on photographic film- radioactive substance is present wherever the film turns black
The results demonstrate the translocation of substances from source to sink over time- autoradiographs of plants killed at different times can be used to show the overall movement of solutes from leaves towards the roots
What are some objections to the mass flow hypothesis?
Sugars travel to many different sinks, not just to the one with the highest water potential as the model suggests
Sieve plates would create a barrier to mass flow, a lot of pressure would be needed for solutes to get through at a reasonable rate
How do electrical impulses control the heartbeat?
SAN (sinoatrial node) generates electrical impulses → atria contract.
Impulse reaches AVN (atrioventricular node) → short delay by non-conductive tissue so ventricles fill.
Impulse travels down Bundle of His through the septum.
Impulse spreads through Purkyne fibres in ventricle walls.
Ventricles contract from base upwards → blood pumped into arteries.