Biology 2108 Exam Three (Part Two)
1/104
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
105 Terms
What is the nervous system and what is its core purpose
It is the body’s electrical communication network, and detects what’s happening inside and outside the body, processes that information, and coordinates a response.
Three core functions of the nervous system
Sensory Input: Detecting stimuli from inside or outside the body
Integration: Processing that information in the CNS
Motor Output: Generating a response
CNS v. PNS
CNS: brain and spinal cord
the integration center: receives signals, processes them, and decides what to do.
protected by done and cerebrospinal fluid
PNS: all nervous tissue outside of the CNS
Carries signals to and from the CNS
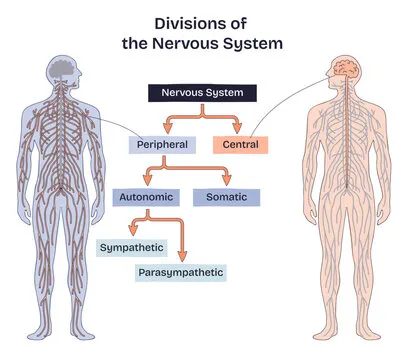
What are the two divisions of the PNS motor system
Somatic Nervous System: controls voluntary skeletal muscle movement
Consciously controlled
Automatic Nervous System: controls involuntary functions (heart rate, breathing, etc.)
splits into sympathetic (fight or flight) and parasympathetic (rest and digest)
Axon Hillock
The junction between the cell body and the axon
This is where the decision to fire is made. If the signal reaches the threshold here, an action potential and triggered.
The most electrically excitable part of the neuron
Myelin Sheath
The fatty insulating layer wrapped around the axon via glial cells.
It speeds up signal conduction by forcing the signal to jump between gaps called Nodes of Ranvier (called Saltatory Conduction), rather than traveling continuously.
Nodes of Ranvier
Gaps in the myelin sheath where the axon is exposed.
The action potential regenerates at each node and jumps from node to node, much faster than continuous conduction.
Dendrites
Branched extensions that receive incoming signals from other neurons or sensory receptors.
Signal travels towards the cell body
More dendrites means more inputs the neuron can recieve
Axon terminals
Branched endings of the axon that contains synaptic vessels filled with neurotransmitters
When an electrical signal arrives, they trigger neurotransmitter release into the synapse to communicate with the next cell
Three types of Neurons
Sensory Neurons (afferent): carries signals from receptors TO the CNS
Interneurons: entirely within the CNS and performs integration (thought, memory processing)
Motor Neurons (efferent): carries signals FROM the CNS TO muscles and glands
Afferent V. Efferent
Afferent: Arrives at the CNS
Efferent: Exits the CNS
Neuroglia: Astrocytes
Forms the blood-brain barrier: controls what enters the brain via the blood
Regulates the chemical environment around neurons, recycle neurotransmitters, and provides structural support
The most abundant glial cell in the brain
Neuroglia
Support cells of the Nervous System
Neuroglia: Oligodendrocytes
Produces the myelin sheath in the CNS
One can myelinate segments of multiple axons simultaneously
Destroyed by Multiple Sclerosis
Neuroglia: Schwann Cells
Produces myelin in the PNS
each Schwann cells myelinates only one segment of one axon, and these cells enable peripheral nerve regeneration.
Neuroglia: Microglia
The immune cells of the CNS
they patrol for damage and infection, engulf debris and pathogens.
The brain’s built in defense system
Neuron At Rest
When a neuron is in this state, it is maintaining a state of readiness, like a compressed spring.
actively maintaining a charge difference across its membrane using ion pumps and leak channels, storing potential energy ready to be released when triggered.
Membrane Potential
The electrical voltage difference across the cell membrane.
It exists because ions are distributed unequally on each side of the membrane
Inside of neuron is approximately -70 mV and is maintained by ion channels and the Na/K pump
The Two Forces that Drive Ion movement across the Membrane
Concentration gradient: Ions move from high to low concentration (like diffusion)
Electrical Gradient: opposite charges attract, and like charges repel.
These two are called the Electrochemical Gradient
Most Important Ion at Rest in a Neuron
Potassium (K)
Higher concentration inside the cell, and membrane is relatively permeable to K at rest.
K drifts out, making the neuron more negative.
Na Importance at Rest
At rest, Sodium wants to enter, and is pushed by both the concentration gradient (high outside) and electrical gradient (negative inside attracts positive Na), but the voltage-gates Na channels are closed at rest, so it mostly cannot get inside.
Large Anions inside the cell At Rest
Large negatively charged proteins and organic molecules trapped inside the cell — they cannot cross the membrane. Their negative charge contributes significantly to the negative interior of the resting neuron.
Ion channels vs Ion pumps
Channels: protein pores that allow ions to pass DOWN into the electrochemical gradient
passive transport
Pumps: moves ions AGAINST their electrochemical gradient
Active transport
Three types of Ion Channels
Leak Channels: always open; K leak channels establish the Resting Membrane Potential
Voltage-Gates Channels: open/close based on voltage; located mainly on the axon and critical for action potential
Ligand-gated Channels: open when a neurotransmitter binds; located mainly on dendrites and cell body
Na/K Pump
For every 1 ATP consumed,
3 Na are pushed OUT of the cell
2 K are pushed INTO the cell
this restores ion concentrations after signaling and maintains resting potential for the long term. It runs constantly.
Equilibrium Potential
The specific membrane voltage at which the electrical force and concentration force for one ion exactly cancel each other out — no net movement of that ion occurs.
K⁺ equilibrium ≈ −90 mV
Na⁺ equilibrium ≈ +60 mV
Why is RMP -70 mV?
While the membrane is more permeable to K at rest, the small Na leak through open channels nudges the RMP slightly less negative from -90 until -70 mV
Action Potential
A rapid, dramatic reversal and restoration of the membrane potential that travels down the axon like a wave. It is the neuron's signal — the electrical impulse that carries information from one end of the neuron to the other. Triggered at threshold, it runs to completion automatically.
Threshold
Critical membrane voltage (-55mV) at which an action potential is triggered
enough voltage gated Na channels open that Na rushes in, making the inside more positive, opening more channels.
this is a self amplifying positive feedback loop that cannot be stopped once it has begun
All or None Principle
An action potential happens either completely or not at all.
aa either full spike to (+40 mV) or none
A stronger stimulus doesn’t create a bigger spike, just a higher frequency of firing, which is how the nervous system makes a stimulus more intense.
Depolarization
During this, voltage gated Na channels are open, which allows it to rush INTO the cell. The membrane potential rises rapidly from -70 mV to +40 mV.
This is the rising phase of the action potential strike
Repolarization
Voltage gates Na channels close, and Voltage gated K channels open. K rushes OUT of the cell. Membrane potential returns toward -70 mV
This is the falling phase of the spike
Hyper-polarization
K channels are slow to close, meaning excess K leaves, lowering the membrane to dip to approximately -80 mV.
The Na/K pump restores this, and membrane returns to rest.
Refractory Period
The period after an action potential when the neuron cannot fire again immediately.
Absolute refractory period — Na⁺ channels are inactivated; firing is physically impossible.
Relative refractory period — during after-hyperpolarization; firing requires a stronger-than-normal stimulus.
This ensures action potentials travel in one direction only.
When does Na enter the cell?
Depolarization.
Na⁺ enters because both forces point inward simultaneously — the concentration gradient (high Na⁺ outside, low inside) AND the electrical gradient (negative inside attracts positive Na⁺). Voltage-gated Na⁺ channels open at threshold, allowing this flood.
When does K leave the cell?
Repolarization.
K⁺ flows out because: its concentration gradient points outward (more K⁺ inside), AND because the inside is now positive (+40 mV), the electrical gradient also pushes K⁺ outward. Voltage-gated K⁺ channels open during this phase.
Why can’t electrical signals jump directly from neuron to neuron?
Neurons don’t physically touch.
The synaptic cleft sits between them, so when it is time to cross, the electrical signal is converted into a chemical signal and crosses the gap itself, where it is turned back into an electrical signal.
Synaptic Cleft
The space between the pre- and postsynaptic neuron.
Approx. 20-40 nanometers wide
Neurotransmitters
Chemical messenger molecules released from the presynaptic axon terminal into the synaptic cleft
they bind to specific receptor proteins on the postsynaptic neuron and change its membrane potential
GABA, Dopamine, Serotonin
Role of Calcium in Synaptic Transmission
The trigger linking electrical arrival to chemical release.
When the action potential arrives at the axon terminal, it opens voltage-gated Ca²⁺ channels. Ca²⁺ floods in, triggering synaptic vesicles to fuse with the membrane (exocytosis) and release neurotransmitters.
Sequence of Events in a Chemical Synapse
Action potential arrives at axon terminal
Voltage-gated Ca channels open
Ca floods in
Synaptic vesicles fuse with membrane (Exocytosis)
Neurotransmitters are released into synaptic cleft
Neurotransmitters diffuse across cleft
They bind to the post synaptic receptors
Ligand-gated ion channels open
Ion flow changes post-synaptic potential
Neurotransmitter cleared!
Excitatory V. Inhibitory Synapse
Excitatory (EPSP): open channels allowing Na in. Membrane depolarizes (less negative), moving closer to the threshold
Makes firing more likely
Main excitatory neurotransmitter: Glutamate
Inhibitory (IPSP): open channels allowing Cl- in or K out. Membrane hyperpolarizes (more negative), moving further from the threshold
Makes firing less likely
Main inhibitory neurotransmitter: GABA
Summation
A neuron integrates all incoming EPSP and IPSP simeoultanerously. If excitatory dominates, the neuron fires, if inhibitory dominates, it doesn’t.
this is how the nervous system makes decisions.
How is a neurotransmitter cleared from the synaptic cleft?
Three mechanisms:
Enzymatic breakdown: enzymes in the cleft degrade the neurotransmitter
Reuptake: the presynaptic terminal reabsorbs the neurotransmitter for reuse
Diffusion: It drifts away from the cleft.
Why are inhibitory synapses necessary?
Without inhibition, neural circuits would spiral into uncontrolled, excessive firing — similar to a seizure.
What is the fundamental three step model of nervous system function?
Sensory input (afferent) → Integration (CNS) → Motor Output (efferent)
Transduction
Conversion of a stimulus into an electrical signal via a sensory receptor.
ex: photoreceptors converting light into electrical signals.
Sensation
The raw awareness of a stimulus
This is what happens when a transduced signal reaches the CNS and is registered.
It is the basic detection of the signal before any interpretation
Perception
The interpretation and conscious experience of a sensation, giving it meaning based on context, memory, and attention. Happens in the cerebral cortex
Sensation V. Perception
Sensation = detection. The raw signal arriving at the CNS.
Perception = interpretation. The brain giving that signal meaning.
Phantom Limb Pain
The brain perceives pain from a limb that no longer exists — because the neural circuits representing that limb are still active.
represents that perception is a construction of the brain, not a perfect recording of reality.
Reflex
A response that bypasses the brain. In a spinal reflex, the signal goes sensory receptor → spinal cord → motor neuron → muscle — without reaching the brain.
The response happens before you are consciously aware of the stimulus.
Effectors
The organs that carry out a response: muscles and glands
Muscle responses: skeletal (movement), smooth (gut, blood vessels), cardiac (heart rate)
Gland responses: secretion of hormones, enzymes, sweat, saliva
Organization of the Human Nervous System
Sexual Reproduction V. Asexual Reproduction
Asexual reproduction — one parent produces genetically identical offspring (clones). No gametes needed. Fast and energy-efficient.
Sexual reproduction — two parents contribute gametes (egg + sperm) that fuse to form a genetically unique offspring. Requires meiosis and fertilization.
Forms of Asexual Reproduction
Budding — a new organism grows out of the parent's body
hydra, yeast
Fragmentation — body breaks into pieces, each regeneratessea stars
Fission — parent splits into two equal offspringsea anemones
Parthenogenesis — egg develops without fertilizationKomodo dragons, bees, sharks
Vegetative propagation — plants producing runners or bulbs.
Parthenogenesis
form of asexual reproduction in which an unfertilized egg develops into a new individual
no sperm needed
offspring are often haploid or diploid depending on species
Advantages of Asexual Reproduction
Fast: no need to find a mate; one individual can populate the environment rapidly
Energy Efficient: no resources spent on finding mates or producing gametes
All offspring can reproduce: no males needed
Works well in stable environments: if the parent is well adapted, clones will be too
Disadvantages of Asexual Reproduction
No genetic diversity — all offspring are clones. A single disease or environmental change can wipe out the entire population.
No adaptation — cannot evolve quickly in response to new threats.
Accumulation of harmful mutations — bad mutations passed to all offspring with no way to shuffle them out.
Advantages of Sexual Reproduction
Genetic diversity — offspring are genetically unique, increasing variation in the population.
Adaptability — diverse populations can evolve faster in changing environments.
Harmful mutations can be masked — a good allele from one parent can compensate for a bad one from the other.
Shuffles alleles through crossing over and independent assortment.
Disadvantages of Sexual Reproduction
Costly — finding and attracting mates requires time, energy, and resources.
Only half the population reproduces directly — males don't bear offspring, reducing reproductive efficiency.
Risk of disease transmission — close physical contact spreads STIs.
Slower — reproduction is more complex and time-consuming than asexual.
External V. Internal Fertilization
External fertilization — egg and sperm are released into the environment (usually water) and fuse outside the body.
Requires water
produces many eggs to compensate for low survival rates.
Ex: most fish and amphibians
Internal fertilization — sperm deposited inside the female's reproductive tract; fertilization occurs inside the body.
Better protection
fewer offspring needed
reptiles, birds, mammals.
R-strategies V. K-strategies
r-strategists — produce many small offspring, little parental care, short lifespan, boom-and-bust populations.
Thrive in unstable environments.
insects, mice, dandelions.
K-strategists — produce few large offspring, heavy parental investment, long lifespan, stable populations near carrying capacity (K).
Thrive in stable environments
elephants, humans, whales.
Monogamy v. Polygamy
Monogamy: one male with one female forms a long lasting pairing
Polygamy: one individual mates with multiple partners
polygyny - one male with multiple women
polyandry - one female with multiple men
Sexual Selection
Individuals with certain traits are more successful at attracting mates, even if those traits reduce survival.
drives the evolution of elaborate features, like peacock tails
Intersexual V. Intrasexual Selection
Intrasexual selection — competition between members of the same sex (usually males) for access to mates.
elk fighting with antlers, elephant seals competing for harems.
Intersexual selection — one sex (usually females) chooses among potential mates based on traits that signal genetic quality or resource availability.
female peacocks choosing males with the most elaborate tails.
Sex V. Gender V. Gender Identity
Sex — biological characteristics (chromosomes, hormones, anatomy) typically categorized as male or female. A biological concept.
Gender — social and cultural roles, behaviors, and expectations associated with being a man, woman, or another identity. A social construct.
Gender identity — a person's internal, personal sense of their own gender. May or may not align with sex assigned at birth.
Gametes
Haploid sex cells that fuse during fertilization to form a new organism.
Sperm : made in testes of a man
Eggs: made in ovaries of a woman
Spermatogenesis
The process of producing mature sperm from stem cells.
occurs continuously after puberty in seminiferous tubules.
each primary spermatophyte → 4 equal, functional sperm via meiosis.
takes approximately 64-74 days
Millions produced daily
Oogenesis
begins before birth, arrested at meiosis 1 until puberty
each primary oocyte → 1 functional egg + 2-3 polar bodies (which degrade)
Only 400 eggs released in a lifetime
Why does oogenesis only produce 1 egg?
Cell division is unequal, so one cell gets almost all of the cytoplasm, while the others become polar bodies that degrade.
Conserves resources, giving the egg maximum cytoplasm and nutrients for early embryo development.
Hormones Regulating the Reproductive System
The hypothalamus-pituitary-gonad axis:
GnRH (hypothalamus) → stimulates pituitary to release.
FSH (follicle-stimulating hormone) → stimulates gamete production.
LH (luteinizing hormone) → triggers ovulation (females) or testosterone production (males).
Gonadal hormones (testosterone, estrogen, progesterone) feed back to regulate the axis.
How does cannabis affect male and female reproduction
Male: THC reduces testosterone production, decreases sperm count, impairs sperm mobility and morphology, and reduces libido
may impair hypothalamus-pituitary axis signaling
Female: Disrupts the hormonal cycle, affects ovulation timing, and alters GnRH signaling.
associated with irregular menstrual cycles and potential effects on fetal development if used during pregnancy
Why are testes held outside the body in the scrotum?
Sperm production requires a body temperature about 2-3 degrees Celsius lower than the core body temp. (37 C)
scrotum is that exact temp (34-35 C)
cremaster muscle can also raise or lower testes to regulate temperature.
Semen
The fluid ejaculated from the penis.
Seminal vesicle fluid
In the semen.
has fructose (energy for sperm), prostaglandins, alkaline fluid
Prostate gland fluid
in the semen.
contains enzyes, citric acid, zinc.
helps liquify semen after ejaculation
Bulbourethral Gland Fluid
In the semen.
Mucus that lubricates and neutralizes acid in the urethra before ejaculation
Path of Sperm from Production to Ejaculation
Seminiferous tubules
Epididymis (maturation and storage)
Vas deferens (muscular tube carrying sperm up)
Ejaculatory duct
Urethra
Exits through Penis
Remembered through the Mnemonic: SEVEN UP
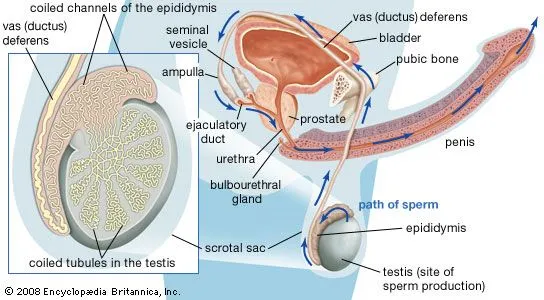
Epididymis
A coiled tube sitting on the back of each testis where sperm mature and are stored.
they spend 2-3 weeks in here gaining mobility and the ability to fertilize an egg.
Urethra
Serves both the reproductive and urinary systems.
carries both urine and semen, but never at the same time.
Seminiferous Tubules
Highly coiled tubes inside the testes where spermatogenesis occurs. They are lined with two key cell types:
Spermatogonia, Sertoli cells
If uncoiled, the tubules from one testis would be about 250 meters long.
Sertoli Cells (Sustentacular Cells)
Nurse cells lining the seminiferous tubules that support and nourish developing sperm.
forms the blood-testis barrier and protects developing sperm from the immune system
Responds to FSH
Secretes inhibin (feeds back to reduce FSH)
Leydig cells
Interstitial cells located between the seminiferous tubules that produce testosterone in response to LH from the pituitary.
Hormones that regulate Spermatogenesis
GnRH (hypothalamus) → pituitary releases:
FSH → acts on Sertoli cells → stimulates sperm production and inhibin secretion.
LH → acts on Leydig cells → stimulates testosterone production.
Testosterone → feeds back negatively to hypothalamus and pituitary to reduce GnRH and LH.
Inhibin → feeds back to reduce FSH specifically.
Male sexual response
Erection: parasympathetic nervous system causes vasodilation of penile arteries, and blood fills up corpus cavernosum and corpus spongiosum.
compresses veins to maintain engorgement
Ejaculation: sympathetic nervous system triggers peristaltic contractions of epididymis, vas deferens, and accessory glands. bulbocavernosus muscle expels semen.
Female Reproductive System differences from Male
Female reproductive and urinary systems are completely seperate from one another, and have distinct openings, unlike the male reproductive and urinary systems
female reproductive system is also largely internal with ovaries, fallopian tubes, uterus, and cervix all within the pelvic cavity.
Ovaries
Serves two functions:
Gametogenesis: produces eggs (oocytes) through oogeneiss
Hormone production: secretes estrogen and progesterone, which regulate the menstrual cycle, maintain pregnancy, and develop secondary sex characteristics
Fallopian Tubes
Captures the egg after ovulation and transport it towards the uterus using cilia and peristaltic contractions.
fertilization normally occurs here, not in the uterus.
the journey to the uterus normally takes 3-4 days
Uterus
Muscular, pear shaped organ that…
receives and implants the fertilized egg
nourished the developing embryo/fetus via endometrium and placenta
expels the fetus during labor via powerful myometrium contractions
Sheds its lining if no fertilization occurs (menstruation)
Ovarian Follicle
A structure in the ovary consisting of an immature egg (oocyte) surrounded by follicle cells, which develop in stages:
Primordial follicle → primary → secondary → Graafian (mature) follicle → ovulation (egg released) → corpus luteum (what remains after ovulation).
Females are born with 1 or 2 million follicles, but only 400 will ever ovulate
Phases of the Ovarian Cycle
Follicular phase (days 1–13) — FSH stimulates follicle development; growing follicles secrete estrogen; one dominant follicle selected.
Ovulation (day 14) — LH surge triggers release of the mature egg from the Graafian follicle.
Luteal phase (days 15–28) — ruptured follicle becomes the corpus luteum; secretes progesterone and estrogen to maintain endometrium.
Phases of the Uterine (Menstrual) Cycle
Menstrual phase (days 1–5) — endometrial lining sheds; estrogen and progesterone are low.
Proliferative phase (days 6–13) — rising estrogen causes endometrium to thicken and rebuild; corresponds with follicular phase.
Secretory phase (days 15–28) — progesterone from corpus luteum causes endometrium to become secretory and vascular, preparing for implantation; corresponds with luteal phase.
How are the Ovarian and Uterine cycles interconnected?
They run in parallel and drive each other through hormones:
Follicle development (ovarian) → estrogen rise → uterus proliferates (uterine).
Ovulation → corpus luteum forms → progesterone rise → uterus becomes secretory.
If no fertilization → corpus luteum degenerates → progesterone and estrogen fall → endometrium sheds (menstruation) → FSH rises → new follicle develops. The cycle repeats.
Specific effects of FSH and LH on the ovarian cycle
FSH (follicle-stimulating hormone):
• Stimulates follicle growth and maturation
• Stimulates estrogen production by follicle cells
LH (luteinizing hormone):
• The LH surge (day 13–14) triggers ovulation — rupture of the mature follicle
• Stimulates formation of the corpus luteum after ovulation
• Stimulates corpus luteum to produce progesterone
Effects of Estrogen and Progesterone on the Uterus
Estrogen (rising during follicular phase):
• Causes the uterus to proliferate and thicken
• Rebuilds the functional layer shed during menstruation
Progesterone (dominant during luteal phase):
• Makes the uterus secretory and vascular — glands develop, blood supply increases
• Prepares the uterus for implantation of a fertilized egg
Negative feedback in Female Hormonal Cycle
Negative feedback (most of the cycle):
Rising estrogen and progesterone suppress GnRH, FSH, and LH — prevents multiple ovulations and controls cycle length.
Positive Feedback in Female Hormonal Cycle
Positive feedback (just before ovulation):
High estrogen (from the dominant follicle) stimulates the pituitary to release a massive LH surge — the one moment in the cycle where a rising hormone causes more of itself.
This LH surge triggers ovulation.
Corpus Luteum
The ruptured follicle that remains after ovulation, transformed into an endocrine structure
secretes progesterone and estrogen to maintain the uterus during luteal phase.
Uterus if egg is NOT fertilized
Without fertilization, no embryo produces hCG, so the corpus luteum degenerates
progesterone and estrogen levels drop sharply
functional layer of the endometrium loses its blood supply, breaks down, and is shed as menstruation