HS2711 - W4 Physical Health & Aging
1/122
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
123 Terms
What is the difference between life span and life expectancy?
life span = # of years a member of a species can live at birth at that time/a specfic age at that time
life expectancy = # of years an avg member of a population can expect to live at birth, MAX #
interventions should be?
targeted
feasible
accessible
why is disability important to gerontology?
systematic study (bio-psycho-socio-cultural aspects) of aging
assume old ppl disabled in life → overestimate
what coping methods do you use as you age?
personal → compensation, tech, assistive device
society → adjust enviro, change policy, PH prevetion
what are life course models?
hard to analyze & quantify → stat analysis complex & X easy collect all people
exposure happen thru out life but X affect same rate late
morbidity
anything other than healthy
physical, social, mental
what are the 3 aspects of health
physical
social
psychological
what is biological aging? what are it’s factors?
Progressive decline in physical functions
happen but vary w rate in people & hint in epidemiology who do it right
Intrinsic
Extrinsic
intrinsic aging
type of factor that leads to biological aging
normal biological wear & tear
variations in speed BUT universal
extrinsic aging
type of factor that leads to biological aging
environment based
vary w lifestyle and contextual factors
linear INC in health issues & want to DEC this
what is the relationship with the rates of chronic diseases, disability, and cognitive decline with age?
linear INC
exception = asthma
gene environment interaction
bio & enviro interact thru out life to influence healthy outcomes
older people = INC opp for interactions
bio & envrio work together or against to stay healthy/be ill
suppress enviro if X helpful
biology X = destiny
demo X = distiny , can change/modify
What percentage of seniors aged 65+ in private households report good to excellent health?
78.8% of women and 78.6% of men = good, very good, or excellent health
X sex diff & most say healthy
What percentage of people aged 85+ report good to excellent health?
69% of women and 67.9% of men report good, very good, or excellent health
discrepancy w perception VS reality in aging for older adults
even tho INC chance get chronic condition
Successful Aging WHO Model
holistic interactions of health, participation and security
Even if someone is physically healthy and socially active, unsafe or inaccessible environments can undermine successful aging
Health – physical and mental well‑being, chronic disease management, mobility, resilience.
Participation – social engagement, meaningful roles, community involvement.
Security – safe environments, financial stability, accessible resources.
How do frail homebound older adults perceive their health?
50% still rate their health as good, very good, or excellent.
How does education impact self-reported health in seniors?
Higher education levels predict an increase in seniors reporting very good or excellent health.
Why will more senior women report good health in the future?
Because more women in older generations have attended university as it became more socially accepted.
How has the shift to an older population in Canada affected disease patterns?
There has been a decrease in acute illnesses (e.g., diphtheria, typhoid, measles) and an increase in chronic illnesses.
What percentage of deaths worldwide are now due to chronic illness?
71% of all deaths worldwide are from chronic diseases.
What is the epidemiological transition?
shift from infectious diseases (mainly acute childhood illness e.g., measles, chickenpox) → chronic degenerative diseases as main causes of death
occur during econ dvlp → most of pop get reliable access to basic materials needed for life
RESULT → live longer, chronic degenerative diseases X kill people quickly
What is chronic illness?
A condition lasting six months or more that has been diagnosed by a health professional.
How much of the age group 65-79 reported multiple chronic diseases?
80%+ = 1+ chronic illness
50% = 2-3 chronic conditions
16% ≥4 chronic disease
7% = 7+ chronic disease
INC condition X auto = disability/poor quality of life
How does the number of chronic illnesses change with age?
The number of chronic conditions per person increases with age, increasing healthcare needs.
Does the number of contracted chronic diseases lead to compounding quality of life outcomes?
X necessarily = functional disabilities, isolation, low quality of life, dissatisfaction with life, and perceiving to be unhealthy
Depends on medical care, education, environment (physical and social)
Why do older women have more chronic illnesses and use more healthcare services?
Possible reasons include biological differences, longer life expectancy, and male denial of health issues.
What is health deficit accumulation?
The gradual buildup of medical conditions, disabilities, and chronic illnesses over time.
How does health deficit accumulation progress with age?
The number of health deficits doubles every 15.4 years, meaning it quadruples from ages 50 to 80.
What are three reasons for higher COVID-19 death rates among seniors?
Declining immune cells with age, chronic low-grade inflammation, and medications that suppress the immune system.
How do chronic illnesses impact COVID-19 risk?
Chronic conditions weaken immunity and increase the risk of severe COVID-19 infection and death.
How does chronic illness lead to disability?
Chronic illnesses can cause functional disability, limiting a person's ability to perform normal daily activities.
What is functional disability?
A limitation in performing normal daily activities due to illness or injury.
How does disability prevalence change with age and gender?
Disability increases with age, and women have higher rates of disability than men.
What factors does the ICF model include?
Social conditions and personal factors affecting disability and recovery.
Who is at greater risk of nutritional problems, men or women?
Women, especially those who live alone, have a greater risk of poor nutrition.
How does activity limitation change with age for women?
1 in 5 women in their 60s reports a daily activity limitation, increasing to 1 in 3 for women in their 80s.
How common is obesity in older women?
Women aged 65+ have the highest rates of being overweight, with 25% being obese.
what is a strong positive association with obesity?
watching TV
Which gender is more affected by osteoporosis?
Women are much more likely to have osteoporosis than men, and the risk increases with age.
How does hypertension (high blood pressure) affect older women?
Blood pressure increases with age, and women 65+ suffer twice the rate of hypertension as women 50-64.
Who has higher rates of diabetes, older men or women?
Older men have higher rates of diabetes, but Indigenous women are disproportionately affected.
How do cancer rates differ between men and women?
Men have higher rates of bladder and prostate cancer, while breast cancer is the most common cancer among women.
Which group reports the lowest stress levels?
Seniors report the lowest stress levels, but older women report more stress than older men.
What contributes to higher stress in older women?
Chronic illness and caregiving responsibilities.
How does disability prevalence change with age?
The percentage of people with disabilities increases with age, and women show higher rates at every age.
what is the standard measure of disability?
common:
Activities of Daily Living (ADLs)
Instrumental Activities of Daily Living (IADLS)
if lsoe 1 of IADLs, X function in society
physical:
Short physical performance battery (SPPB)
Nagi scale
Late-Life Disability Instrument (LLDI)
What are activities of daily living (ADLs)?
Basic self-care tasks such as bathing, dressing, eating, walking, and using the toilet.
What are instrumental activities of daily living (IADLs)?
More complex tasks such as cooking, shopping, managing finances, and housekeeping.
What is more common, activity limitations or disabilities?
Activity limitations are more common than diagnosed disabilities.
Who is more likely to pay for help with daily activities, men or women?
Women are more likely to pay for assistance, and this increases with age.
Why do more older women report unmet care needs?
More women live alone as widows, while older men are more likely to have a spouse for support.
What are the five leading causes of disability in older adults?
Foot problems, arthritis, cognitive impairment, heart problems, and vision loss.
Which combination of conditions leads to the most functional limitations?
Foot problems, arthritis, and heart problems together cause the greatest activity restrictions.
What proportion of older people report no limitations in ADLs?
Two-thirds of older adults report no limitations in their daily activities.
Is disability always permanent in older adults?
No, some older adults recover or regain their independence.
What impact does an increase in disabled seniors have on healthcare?
It increases costs and requires new policies to support aging populations.
Do most older adults with chronic conditions develop disabilities?
No, many older adults have chronic conditions but do not develop functional disabilities or require daily assistance.
what are individual ways to respond to disability?
environmental adjustment
modify built enviro to support indpt
cheap but poor job
technology
internet-danger of misleading health information
assistive devices
should be sensitive to physical, mental, and emotional needs → people don't want to stand out/show their disability
How does social support affect younger arthritis patients?
Those with social support are more likely to replace lost activities with new ones, improving their quality of life.
Who is more likely to report chronic pain, older men or women?
Older women report more chronic pain than older men, and this increases with age.
How does pain affect mental health in older adults?
Higher pain intensity is linked to lower chances of reporting "flourishing" mental health.
What coping methods do older adults use for physical decline?
Maintaining a positive attitude, adjusting daily routines, and seeking help from others.
How does a strong social support network affect seniors?
It improves well-being, life satisfaction, and overall health.
What are the ways older adults cope individually?
(1) compensation strategies
(2) improvements in technology
(3) changes in lifestyle
overall adjust expectations of activity
what are ways older adults can cope societally?
Policy changes
environmental adjustments
public health prevention → policies that support preventive healthcare, home care, and community-based services
Smoking secession
Moderate drinking
Healthy diet
Exercise
Reducing ‘sitting’ time
Supportive social network
What are sense thresholds, and how do they change with age?
Sense thresholds are the points at which a person can perceive a stimulus
start increasing as early as age 30
by age 60, most notice changes in their senses
How can environmental changes help older adults cope with physical decline?
Changes such as moving to a one-story house, installing grab bars, or improving lighting can make daily life easier and safer.
How can changes in social interactions help older adults cope with decline?
The way others speak to or treat an older person can affect their confidence and ability to function independently.
assistive devices
technologies that help compensate for physical or sensory decline
How does the use of assistive devices change with age?
The use of assistive devices increases with age, with a higher proportion of older women using mobility aids.
What is Telehomecare, and how does it benefit older adults?
Telehomecare allows healthcare services to be delivered remotely, enabling older adults to receive medical care while staying in their own homes.
How has internet use changed among older adults?
Internet use has increased among people 65+ across all age groups, helping them communicate, save time, and access information.
How do men and women differ in their online health searches?
Women tend to search for information about specific diseases and medications, while men look for details on healthcare systems and delivery.
What percentage of older adults with a disability use an assistive device?
81% of people aged 65+ with a disability use some form of aid or assistive device.
What factors influence whether seniors use assistive devices?
(1) Awareness of the device, (2) understanding of its usefulness, and (3) affordability and accessibility.
What is hypokinesia?
Hypokinesia refers to physical problems caused by a lack of movement.
How does physical activity change with age?
Each older age group shows an increase in physical inactivity.
Does moderate exercise provide the same benefits as vigorous exercise?
Yes, studies show moderate exercise offers similar health benefits as vigorous exercise.
Why is weight training important for older adults?
It helps maintain strength, mobility, and independence.
How does exercise affect the aging brain?
Exercise improves brain plasticity, adaptability, and resilience, helping protect against cognitive decline.
At every age, do men or women engage in more weekly physical activity?
Men engage in more physical activity than women at every age.
Why do seniors report lower stress levels than younger adults?
Retirement and a more relaxed lifestyle contribute to lower stress levels in older adults.
Why is stress reduction still important for seniors?
Even though stress levels are lower in seniors, managing stress remains important for overall health and well-being.
What is compression of morbidity?
postpone age of onset disease/severe chronic illness only near the end of life → shorten period of morbidity only right before death
same prevalence BUT morbidity compress right before death
onset of morbidity at 85-95 instead of 65-95
what is expansion of morbidity?
INC life expectancy w extended years of illness/disability
crude death rate
absolute number of people who died
ISSUE → CAD older & die more & need age standardization + adjust for outcomes related to aging
EX → cancer INC prevalent in older people
what evidence of compression of morbidity exists in Canada?
none bc X clear trend from 1994-2010 at national level
have HP & morbidity X 60, starts later BUT # CD still same
only sick short period & later on
disability free years INC
some in NL + PEI
What is disability-free life expectancy?
The number of years a person can expect to live without a disability
often free bc compression of morbidity
What is dependence-free life expectancy?
The number of years a person can live without needing assistance for daily tasks.
What is health-adjusted life expectancy (HALE)?
The number of years a person can expect to live in good health.
What is rectangularization (or squaring) of the survival curve?
The trend of more people surviving into old age, creating a more squared survival curve → show demo result of INC compression of morbidity
if compression happen, curve rectangulize bc ppl X die & healthy
when hit 85, die suddenly
BUT X clear trend
RESULT → INC p(survive from birth to eldery)
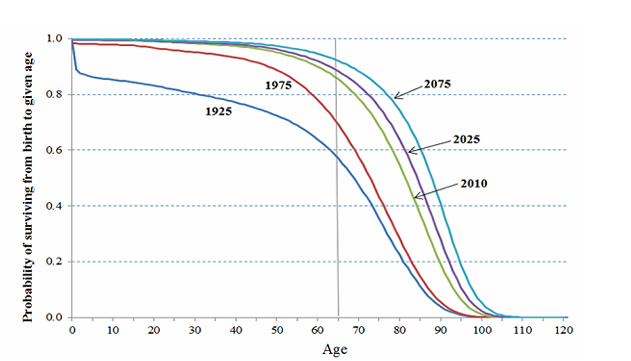
What were Fries' three predictions about a longer life?
(1) More people would reach the maximum lifespan
(2) chronic illnesses would be reduced
(3) severe chronic illness would occur only near the end of life
How does income affect mortality rates?
Lower-income groups have higher mortality rates.
How does income impact longevity?
Higher-income individuals are more likely to reach age 75.
How does socioeconomic status (SES) impact health?
Lower SES leads to worse health outcomes and greater healthcare needs.
How does education affect health in old age?
Higher education leads to better health, lower disability rates, and healthier lifestyle choices.
life course theories?
links w 'adult and older health' + physical/social exposures during → gestation, childhood, adolescence, earlier in adult life, or across generations
ex: violence
Lifetime physical violence associated with mobility decline through depression and reduced activity pathways
what models are part of the life course theory?
critical period model
accumulation of risk model
chain of risk model
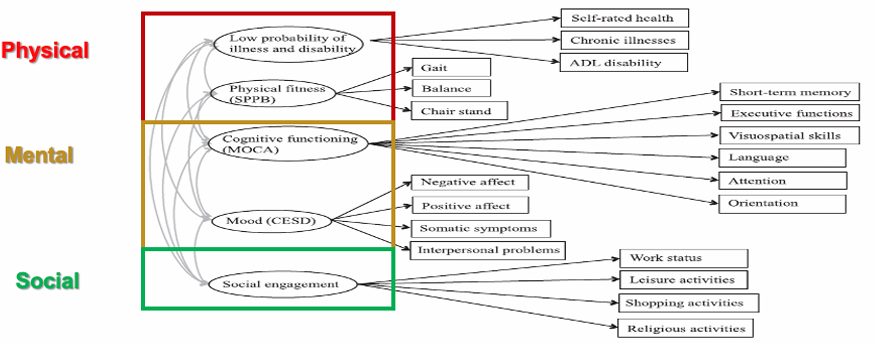
what is the successful aging comprehensive model?
diff factors & test what relevant beyond WHO model
look at specfic factors w focus cognitive
squares = measred & grouped for sucessful aging
physical
low probability of illness and disability
physical fitness (SPPB)
mental (INC impt than physical)
cognitive functioning (MOCA)
Mood (CESD)
social
social engagement
what is the critical period model?
Exposure during a specific period of life has lasting or lifelong effects
Vulnerable ages → fetal, adolescence, early old age (65-75), older adult X as vulnerable
SES impacts health outcomes @ stages
ex: Dutch Hunger Winter
Fetal origin of old age diseases bc malnutrition = INC chronic disease later in life
ex: Negative effect of retirement on the cognitive function of old men