Week 2 - Alterations to Blood Flow Pt. 1
1/66
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
67 Terms
Define blood pressure
The amount of force exerted onto arterial walls by the blood as its being pumped around the body
Differentiate between systolic and diastolic pressre
Systolic - pressure exerted onto the arteries as the heart is contracting
Diastolic - pressure exerted onto arteries as the heart is contracting
State the formula of blood pressure
BP = Cardiac output x peripheral resistance
Define peripheral resistance
The force opposing blood flow within the arteries
Define hypertension
Consistent increase in systemic arterial blood pressure
Explain the advice a GP would give to someone will prehypertension or hypertension stage 1
Lifestyles changes such as diet and exercise
Explain the advice a GP would give to someone with hypertension stage 2
Lifestyles changes as well as medication
Explain the advice a GP would give to someone with hypertension crisis
They require immediate medical attention (possibly emergency)
List the 2 types of hypertension and state how common they are
Primary Hypertension - 95%
Secondary Hypertension - 5%
Explain the cause of primary hypertension
There is no specific cause, instead a combination of factors including genetic, environmental and lifestyle factors
List the risk factors of primary hypertension
Aging
Obesity
Anxiety and stress
Increased sodium intake
Increased alcohol consumption
Being male
Explain the cause of secondary hypertension
Specific causes including kidney diseases, endocrine diseases such as hyper/hypothyroidism as well as drugs
State the 4 processes within the body that contribute to hypertension
Reduced renal sodium excretion
Overactive RAAS
Overactive sympathetic nervous system
Endothelium dysfunction
Explain how reduced renal sodium excretion can contribute to hypertension
Reduced sodium in urine results in sodium and water retention in the blood. Increasing blood volume and therefore BP.
Explain how the 3 ways an overactive RAAS system can contribute to hypertension
Angiotensin ll increased vasoconstriction, increasing peripheral resistance and therefore BP
Angiotensin ll stimulates aldosterone production, increasing sodium and therefore water retention. This increases blood volume and therefore BP
Angiotensin ll activates sympathetic nervous system activity, increasing HR, vasoconstriction and therefore BP
List 2 causes for endothelium dysfunction
Inflammation
Insulin resistance
Explain how hypertension can lead to serious complications
High blood pressure can damage endothelial cells
Endothelium can no longer undergo normal functions eg, vasodilation/constriction, prevent blood clotting and play a role in inflammation
Consequences are location-dependent
List some of the complications that arise from hypertension
Myocardial infarction
Stroke
Renal failure
Vision loss
Sexual dysfunction
Fractures
Name some of the symptoms of hypertension in later stages
Headaches
Chest pain
SOB
Cardiac arrhythmias
Blurred vision
Differentiate between arteriosclerosis and atherosclerosis
Arteriosclerosis is an overarching term for arterial disorders that result in decreased blood flow due to degeneration.
Atherosclerosis is a form of arteriosclerosis in which lipid accumulation in the arteries leads to plaque formation and hypertension
Explain where the plaque forms in atherosclerosis
In the tunica intima, the innermost layer that is directly in contact with the blood.
State what 2 main diseases arise from atherosclerosis
Coronary heart disease
Cerebrovascular disease
Explain how a plaque is formed within the artery
Endothelium damages
LDL enters the tunica intima through damaged endothelium
LDL oxidises and inflammatory response is activated, triggering monocytes and T cells adhere to endothelium
Monocytes differentiate into macrophages as they enter the tunica intima
Macrophages phagocytose LDL, forming foam cells
Foam cells release cytokines that amplify immune response and attract more macrophages
Foam cells accumulate to form a fatty streak
Smooth muscle proliferates which migrates to cover the fatty streak, creating plaque
State the alternative name for plaque
Atheroma
Name and explain the 2 components of an atheroma
Fibrous cap - top portion made of smooth muscle cells, extracellular matrix and collagen
Necrotic core - progression of fatty streak containing debris, dead cells, foam cells and lipids.
Name and explain the 2 types of plaques
Stable plaque - contain a thick fibrous cap and result in predictable decreased blood flow
Unstable plaque - contain a thin fibrous cap that typically ruptures, resulting in the formation of a thrombus and can cause more serious consequences
Name the 4 outcomes of atherosclerosis
Aneurysm and rupture of blood vessel
Stenosis
Thrombus occlusion
Atheroembolism
Explain an aneurysm
The dilation of a vessel wall or cardiac chamber in which changes to collagen and elastin cause weakening. The vessel/chamber can no longer efficiently propel blood throughout the systemic circulation and are prone to rupture.
State the part of the body most susceptible to aneurysms and explain why
The aorta due to the constant stress to propel blood to the rest of the body
Define a thrombus
A blood clot that forms within a vessel
Explain why a thrombus forms
Inflammatory response activates coagulation
Stasis of blood flow
Explain the difference between a thrombus and an embolus
Thrombus is a blood clot that lodges and occludes a blood vessel
Embolus is a blockage that breaks off and travels to and lodges at a distal site
Define a thromboembolism
An embolus that forms by breaking off from a thrombus, travelling and lodging at a distal site
Explain DVT
Deep vein thrombosis occurs when a thrombus forms within a vein (typically the femoral vein) that is likely to cause a pulmonary embolism.
State what will occur if there is atherosclerosis to the internal carotid artery
Ischemia to the brain and a stroke
State what will occur if there is atherosclerosis to the anterior descending coronary artery
Ischemia to the myocardium and myocardial infarction
State what will occur if there is atherosclerosis to the renal artery
Ischemia to the kidneys and renal failure
Define acute coronary syndromes
Any condition that occurs due to a severe reduction in blood flow to the myocardium
List 2 examples of acute coronary syndromes
Unstable angina
Myocardial infarction
Define angina pectoris
Intermittent chest pain as a result of periodic myocardial ischemia
Name the 3 types of angina
Stable
Prinzmetal/variant
Unstable
List symptoms of angina
Chets pain
Dyspnea (SOB)
Pain radiating to the neck, jaw, shoulder and arm
Define stable angina
Predictable chest pain caused by the onset of stress
Explain how atherosclerosis can lead to stable angina
Those who have atherosclerosis with stable plaques will experience stable angina.
Explain why those will stable plaques have stable angina
This is because at rest, blood flow is normal and energy demands can be met. However during periods of stress such as exercise, energy demands increase and the narrowing of arteries due to stable plaque prevents the body from increasing blood flow in order to meet these demands.
Explain how symptoms of stable angina can be relieved
Symptoms are relieved by rest, ceasing stressful activities and certain medications.
Define prinzmetal/variant angina
Rare chest pain caused by coronary artery vasospasms.
Define unstable angina
Unpredictable chest pain caused by sudden myocardial ischemia
Explain how atherosclerosis leads to unstable angina
Those who have atherosclerosis with unstable plaques will rupture and form a thrombus. This thrombus occludes a blood vessel in which there is transient myocardial ischemia for 10-20 mins and blood flow returns before necrosis.
Explain how the symptoms of unstable and stable angina differ
Symptoms are the same however for unstable angina these symptoms occur at rest and are more severe and frequent.
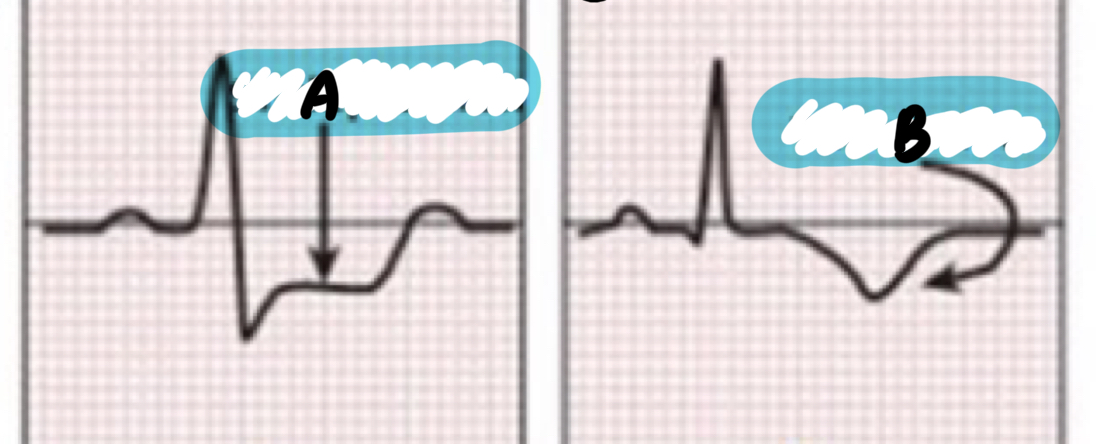
List these features of an ECG that occur for patients with unstable angina during an episode
A - ST depression
B - T wave inversion
Define a myocardial infarction
Necrosis of the myocardium due to the lack of blood flow through the coronary arteries for a sustained period of time.
Name the 2 types of myocardial infarctions
Subendocardial infarction
Transmural
Differentiate between subendocardial and transmural infarctions
Subendocardial occurs when there is damage only to the endocardium due to thrombus breaking off and travelling elsewhere before further damage occurs
Whereas transmural occurs when there is damage to all layers of the cardiac wall due to a permanently lodges thrombus
Explain the different terms used when analysing an ECG for infarctions
STEMI - ST elevation caused by a transmural infarction
NSTEMI - no ST elevation caused by a subendocardial infarction
Explain how atherosclerosis can lead to a myocardial infarction
Those who have an atherosclerosis with unstable plaques that rupture and form a thrombus. This thrombus occludes a vessel that causes sustained myocardial ischemia, leading to a myocardial infarction.
State the percentage of unstable angina cases that progress to myocardial infarction
20%
Differentiate between transient and sustained ischemia
Transient ischemia is periodic and cell damage is reversible whereas sustained ischemia is for extended time periods in which cell damage is irreversible.
Explain how transient ischemia/partially ischemic cells can lead to reduced impulse conduction and contractile function
Reduce blood flow and oxygen results in anaerobic respiration
This causes accumulation of lactate that reduces pH
Also causes reduction in ATP production
These changes reduces pumping of ions and the integrity of cell membranes
This decreases impulse conduction and contractions
Explain how transient ischemia/partially ischemic cells can lead to the activation of the SNS and RAAS
Use of anaerobic respiration reduces ATP production
This triggers SNS and RAAS to increase vasoconstriction and BP in attempt to increase cardiac output for aerobic respiration
Explain how sustained ischemia/totally ischemic cells leads to cell death
Lack of blood flow means no oxygen reaching cells
After 20 mins cells lose integrity of cell membrane
Cell death
Explain how myocardial infarction can be diagnosed from blood tests
Certain intracellular enzymes are released into the blood after myocardial cell death.
List the 3 phases of cell repair after a myocardial infarction
Inflammatory
Proliferative
Maturation/remodelling
Explain the inflammatory phase of myocardial repair including time-span
24 hours after, immune cells such as macrophages and neutrophils migrate to remove debris and dead cells.
Explain the proliferative phase of myocardial repair including time-span
10-14 days after, angiogenesis occurs and fibroblasts form scar tissue.
Explain the maturation/remodelling phase of myocardial repair including time-span
Myocyte hypertrophy occurs to compensate for inefficient function of scar tissue.
Explain how symptoms of myocardial infarction differ for men and women
The traditional symptoms including intense chest pain, dyspnea and nausea are not as common forr women who may experience dizziness, weakness and trouble sleeping.