Histology Lecture #20: The Lymphatic System
1/144
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
145 Terms
What are the two main structural components of lymphoid tissue?
Stroma and parenchyma
What forms the stroma of lymphoid tissue?
A network of reticular fibers and fibroblastic reticular cells.
What does the parenchyma of lymphoid tissue consist of? (3)
Lymphocytes
various antigen-presenting cells (APCs)
plasma cells
Where is diffuse lymphoid tissue found?
Within areas of loose connective tissue (CT).
Does diffuse lymphoid tissue have a capsule?
No, it does not have a capsule.
What surrounds lymphoid organs?***
A capsule of connective tissue.
Where are lymphoid nodules (or follicles) found?
In tissues and organs.
What are lymphoid nodules made of?***
Aggregates of B cells.
Which cells do B cells interact with in lymphoid nodules?
Follicular dendritic cells
What is the origin of follicular dendritic cells?
Mesenchymal origin.
Do follicular dendritic cells have MHC class II molecules?
No, they do not have MHC class II molecules.
How do follicular dendritic cells help activate B cells?
By using antigen-antibody complexes on their surface that bind to receptors for complement proteins and Ig Fc regions.
What happens when B cells are activated?
They aggregate and form the nodules.
What is a primary lymphoid nodule?
A small aggregate of activated B cells.
What type of cell density is seen in a primary lymphoid nodule?
Uniform cell density.
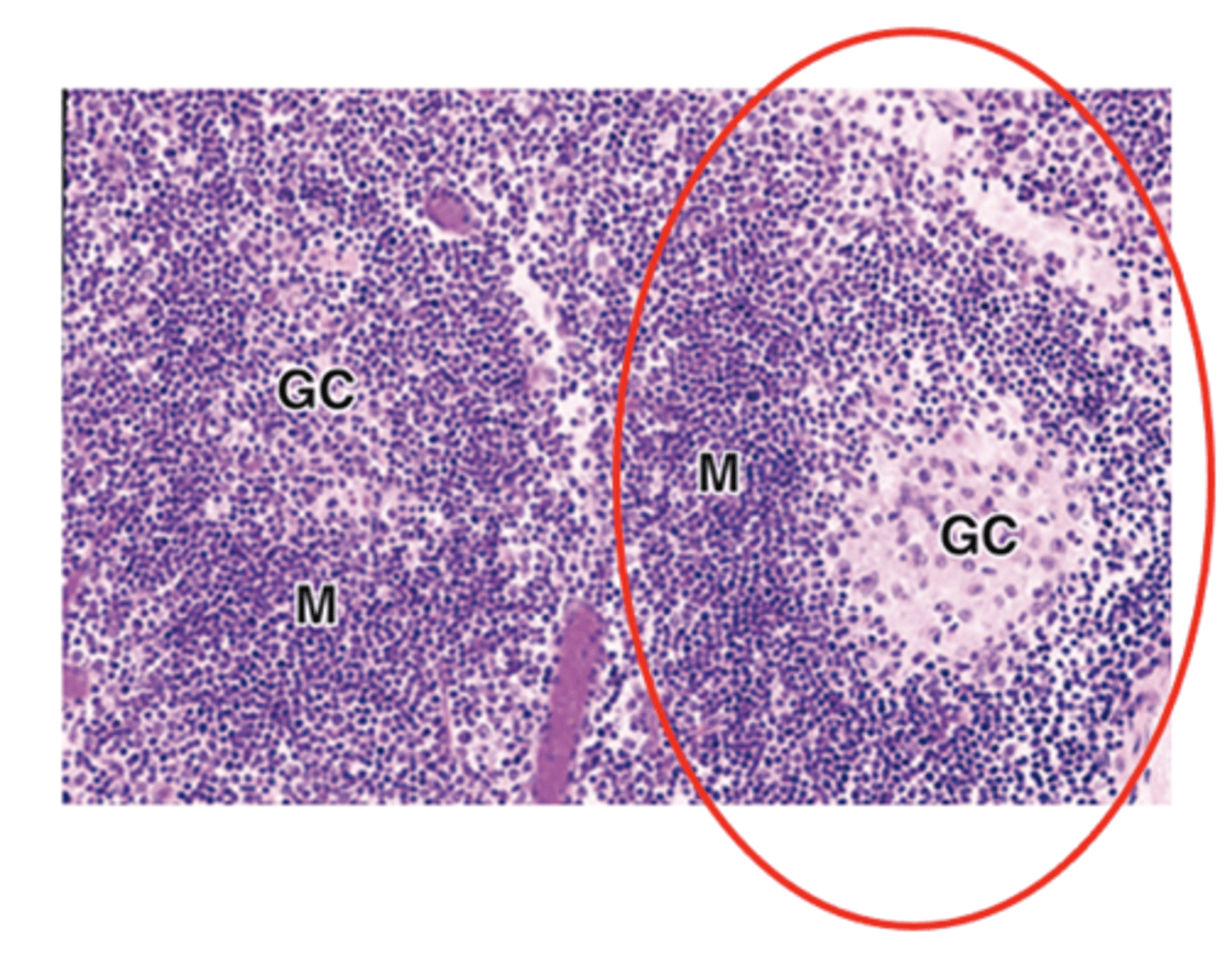
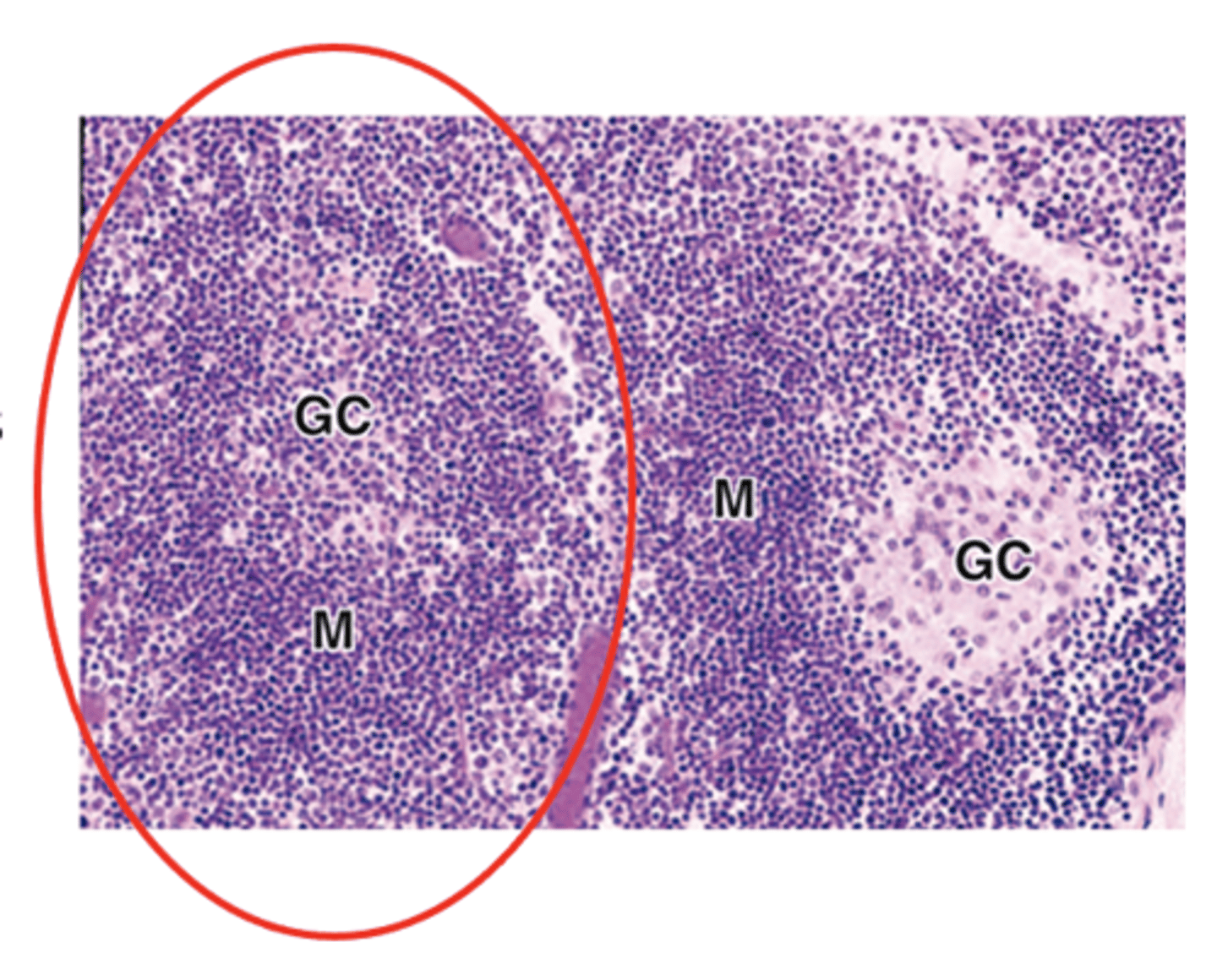
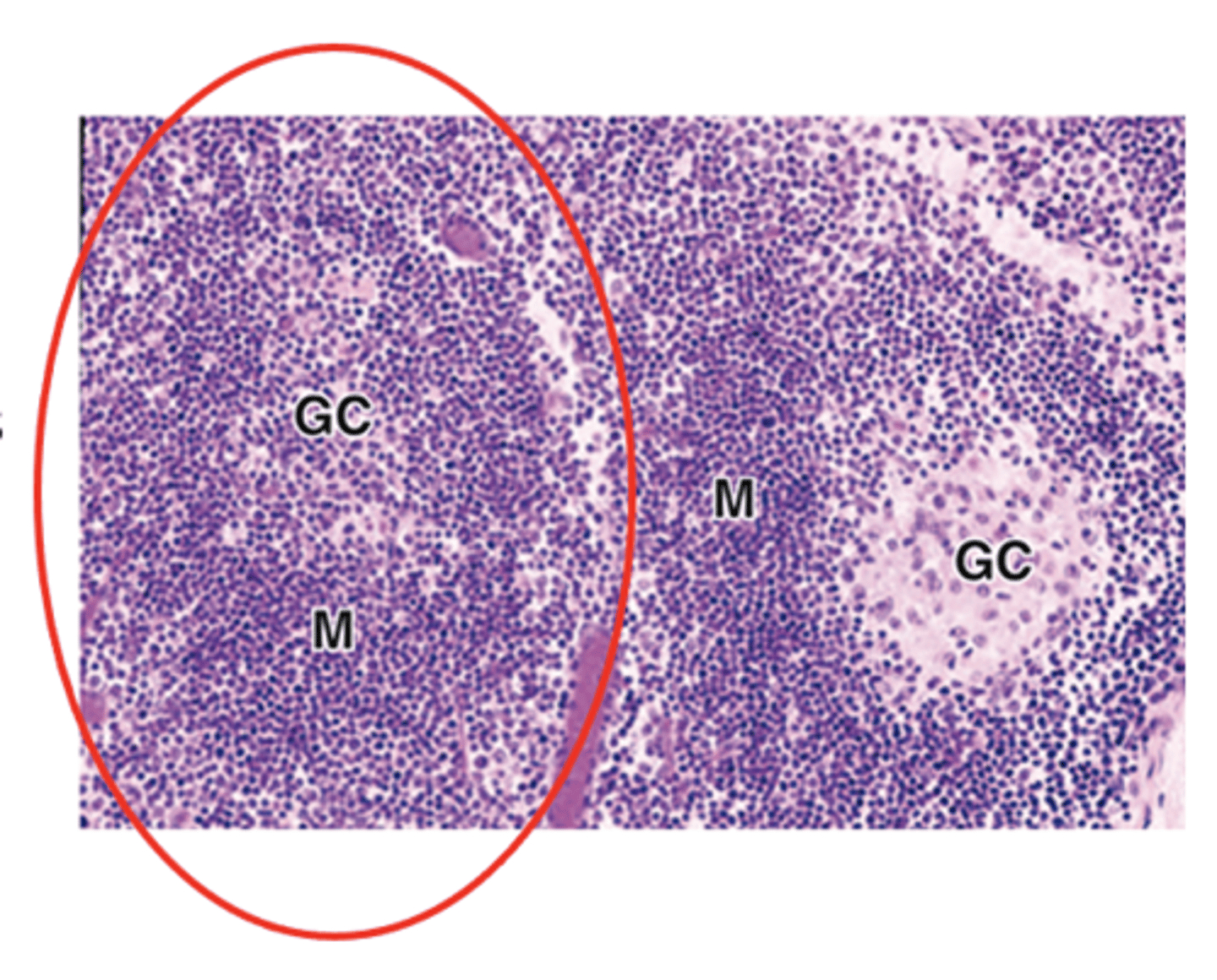
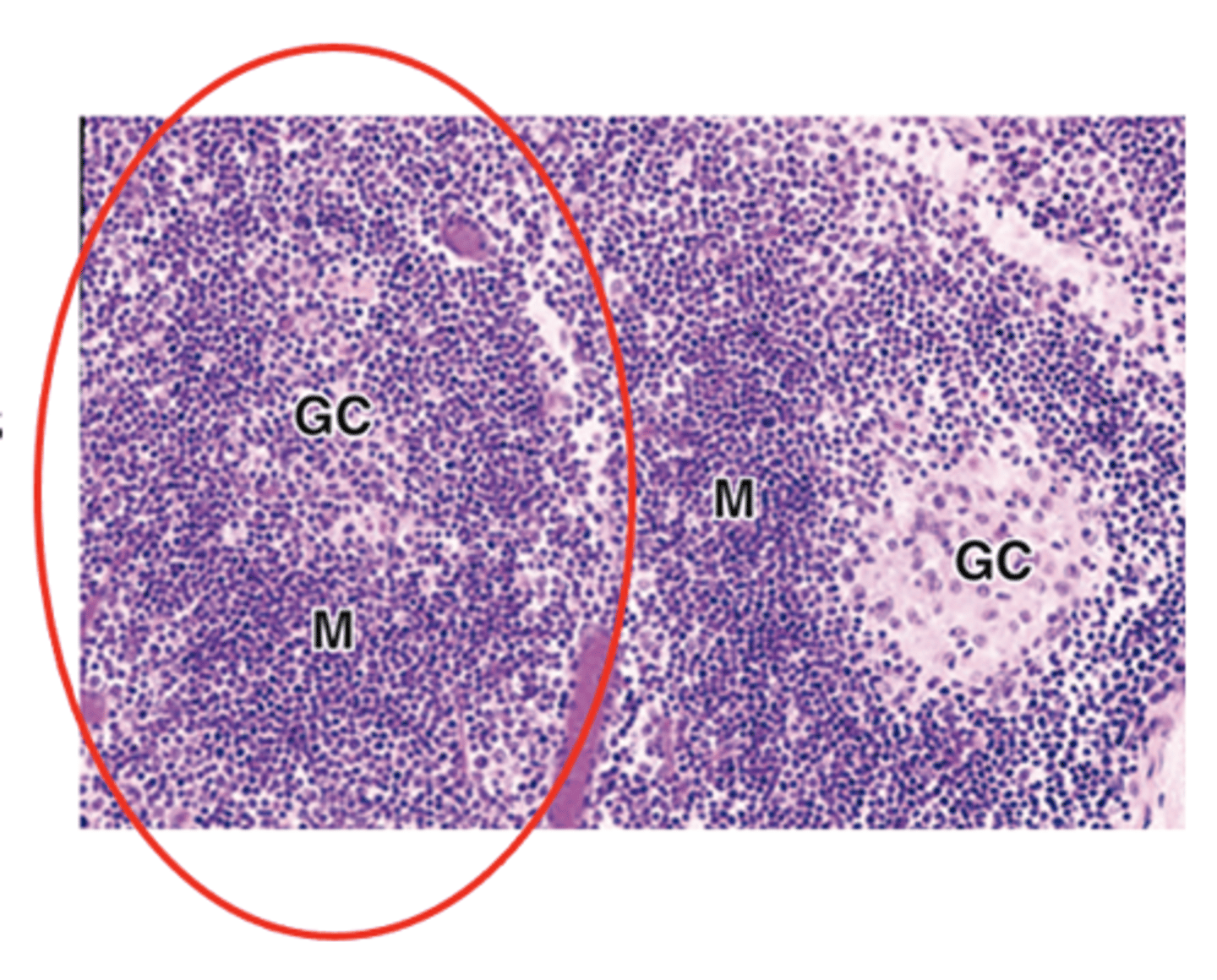
What is the defining feature of secondary lymphoid nodules?
The presence of a germinal center
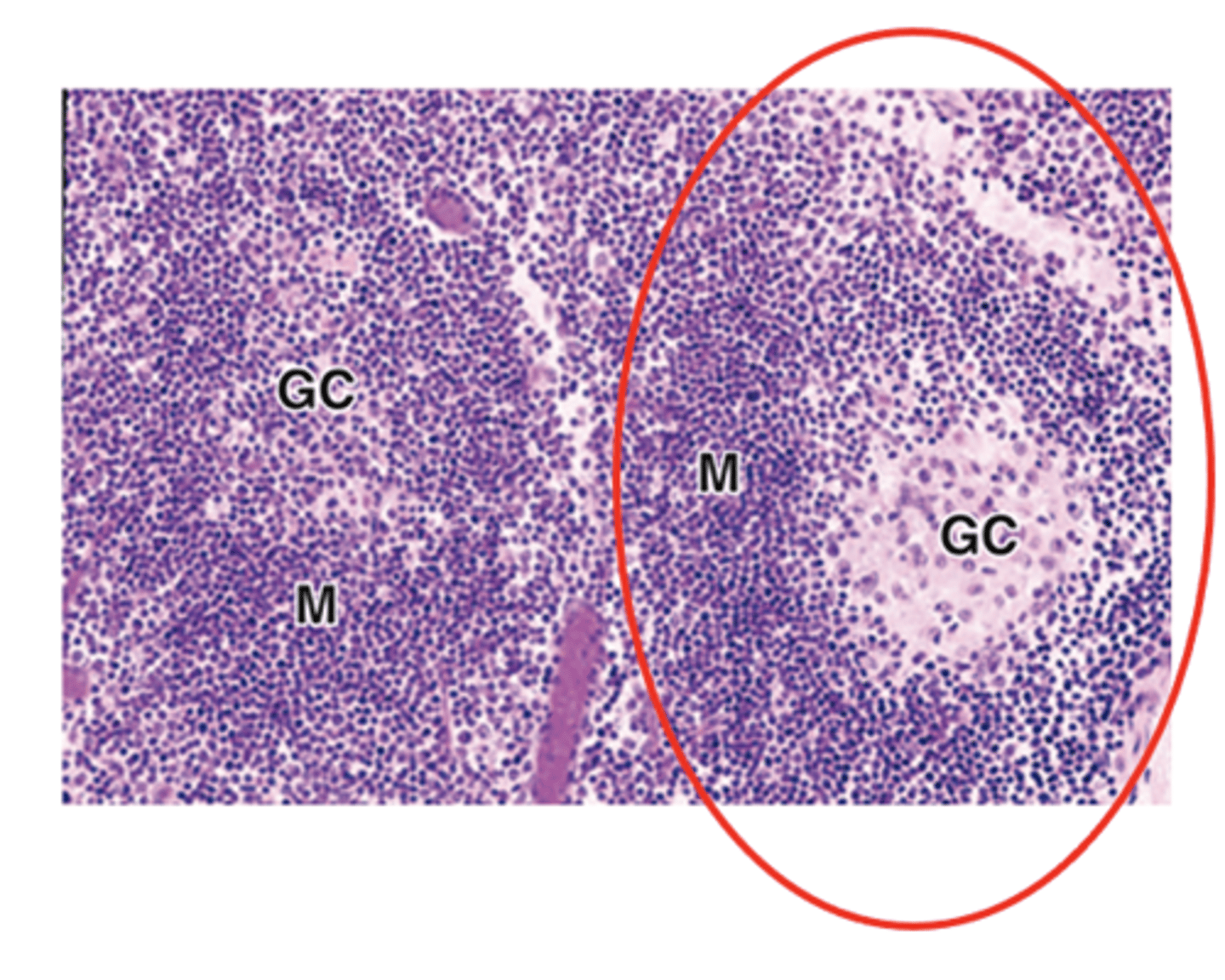
What type of cells are found in the germinal center of secondary lymphoid nodules?
Large lymphoblasts called centroblasts.
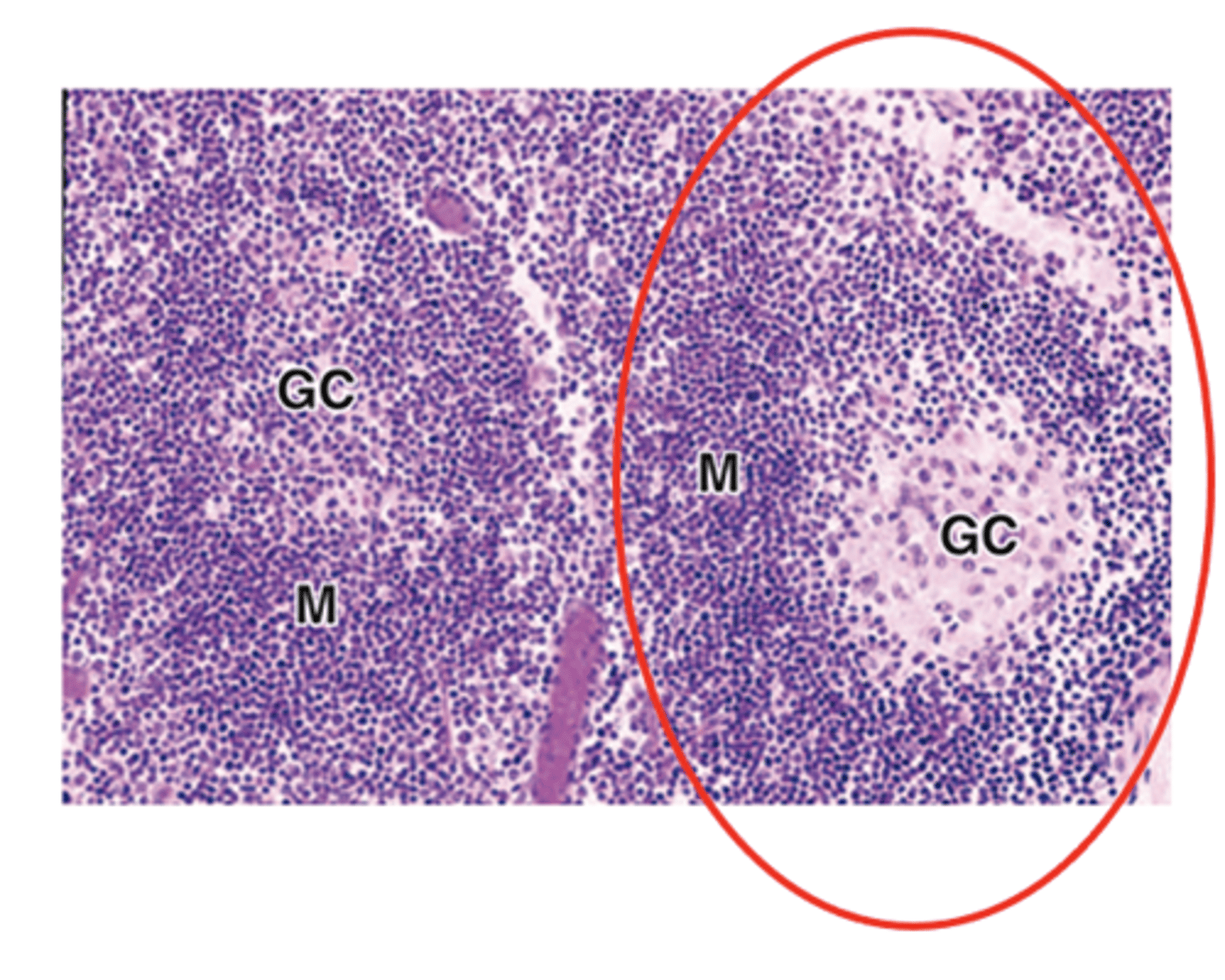
What important processes occur in the germinal center of secondary lymphoid nodules?
• Immunoglobulin gene recombination
• Rapid proliferation
• Quality control
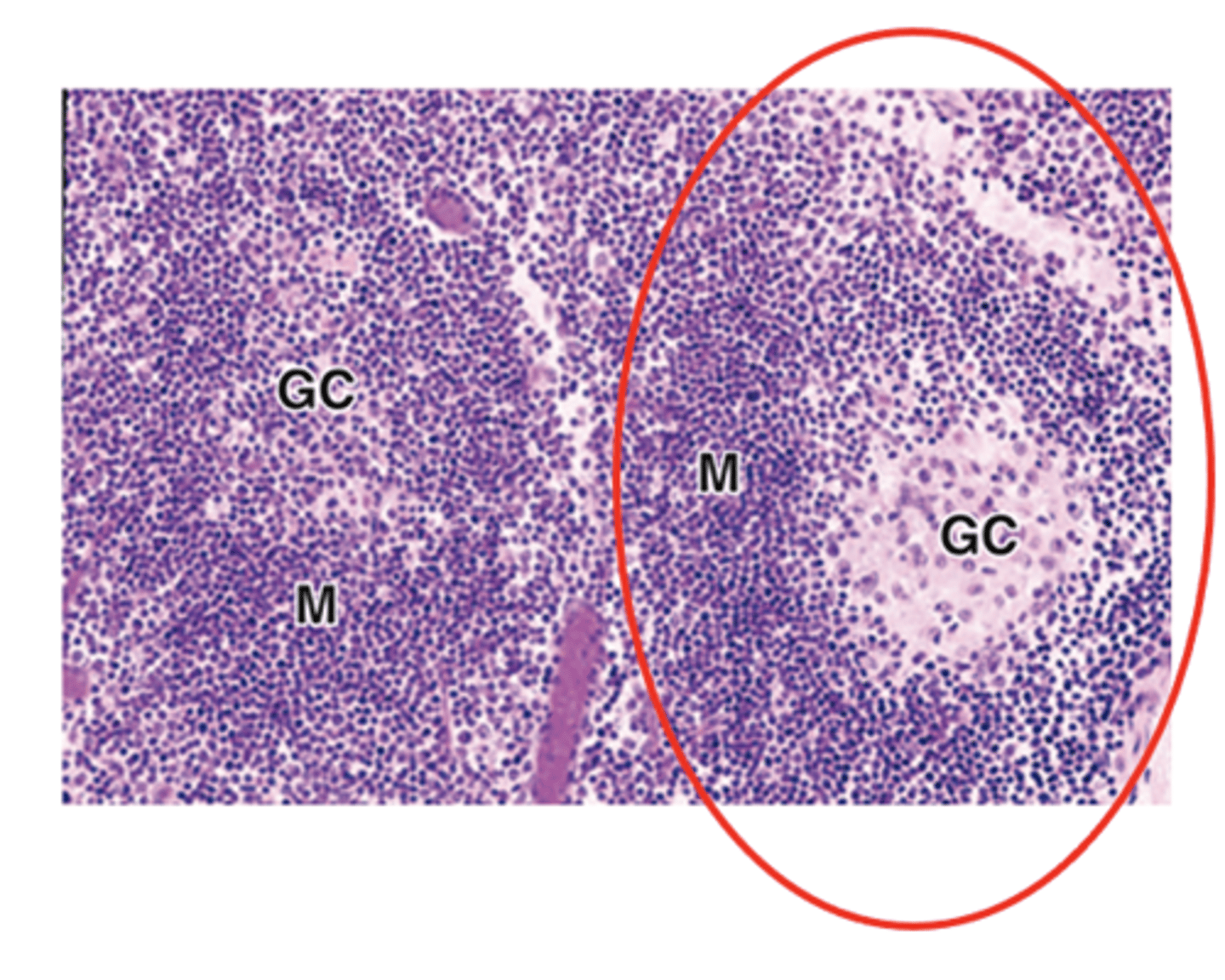
What are the staining characteristics and type of cells in the peripheral mantle of secondary lymphoid nodules?
Basophilic
Naive, non-proliferating B cells
What happens to activated proliferating B cells during the progression of secondary nodules?
They differentiate into plasma cells and memory B cells.
What happens to the mantle and germinal center cells after a few weeks?
They disperse
The structure of the secondary nodule is lost
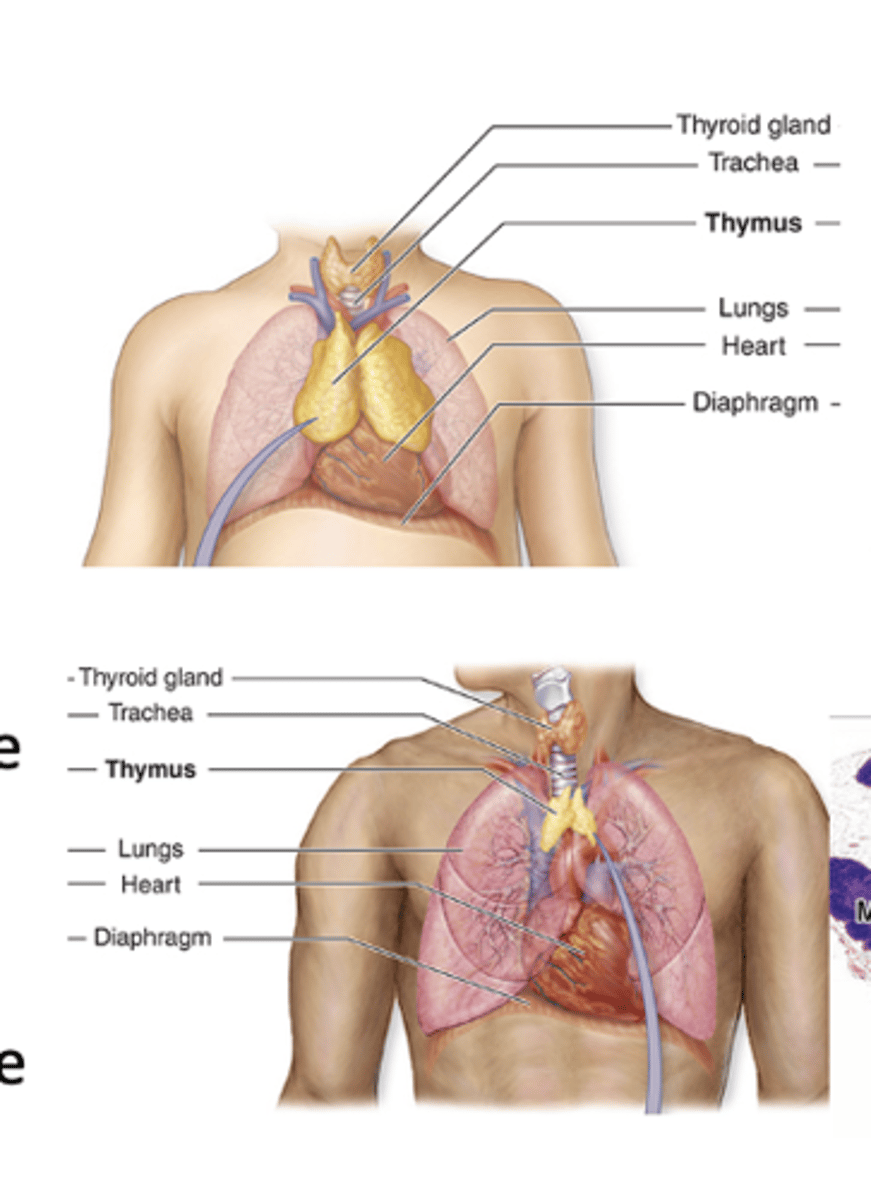
Where is the thymus located?
It is a bilobed organ located in the mediastinum.
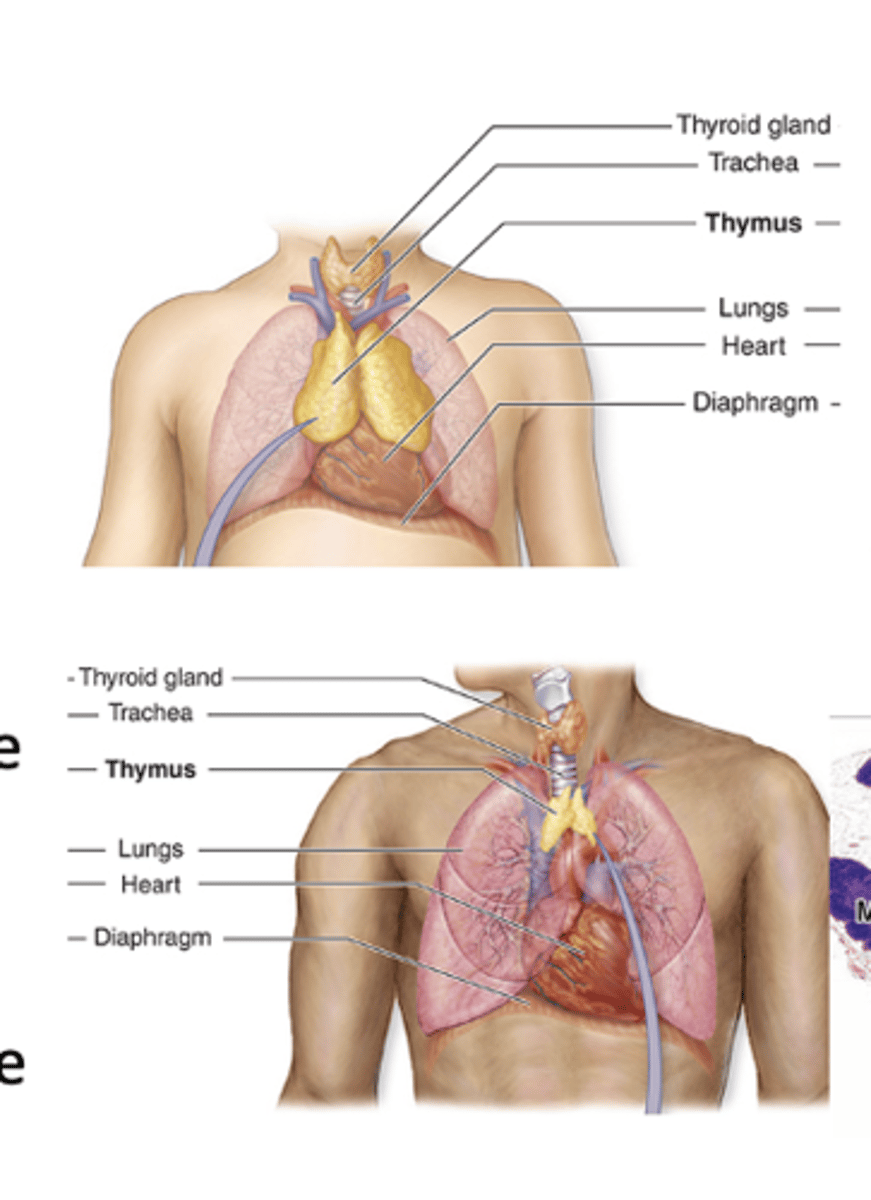
What is the main function of the thymus?
It is responsible for the maturation of T cells.
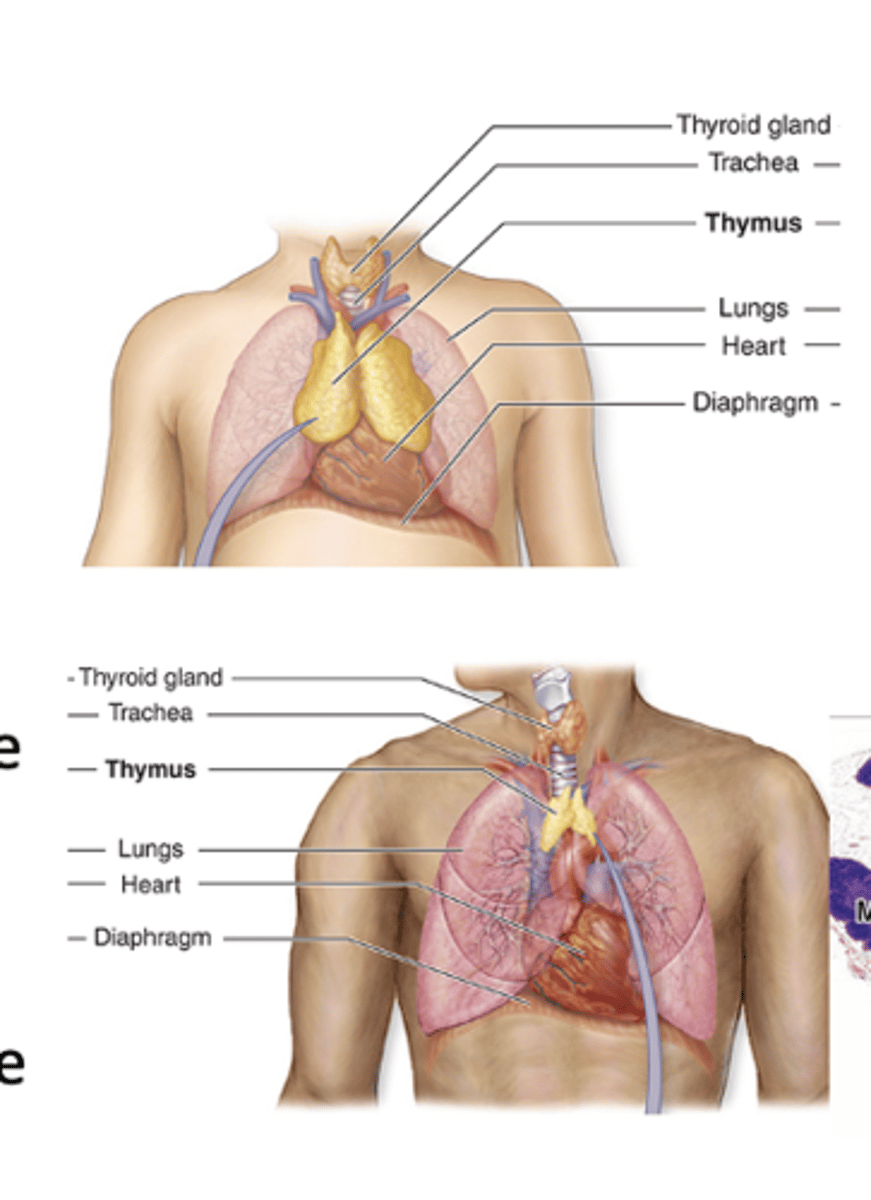
What important immune process occurs in the thymus to prevent autoimmunity?
Induction of central tolerance
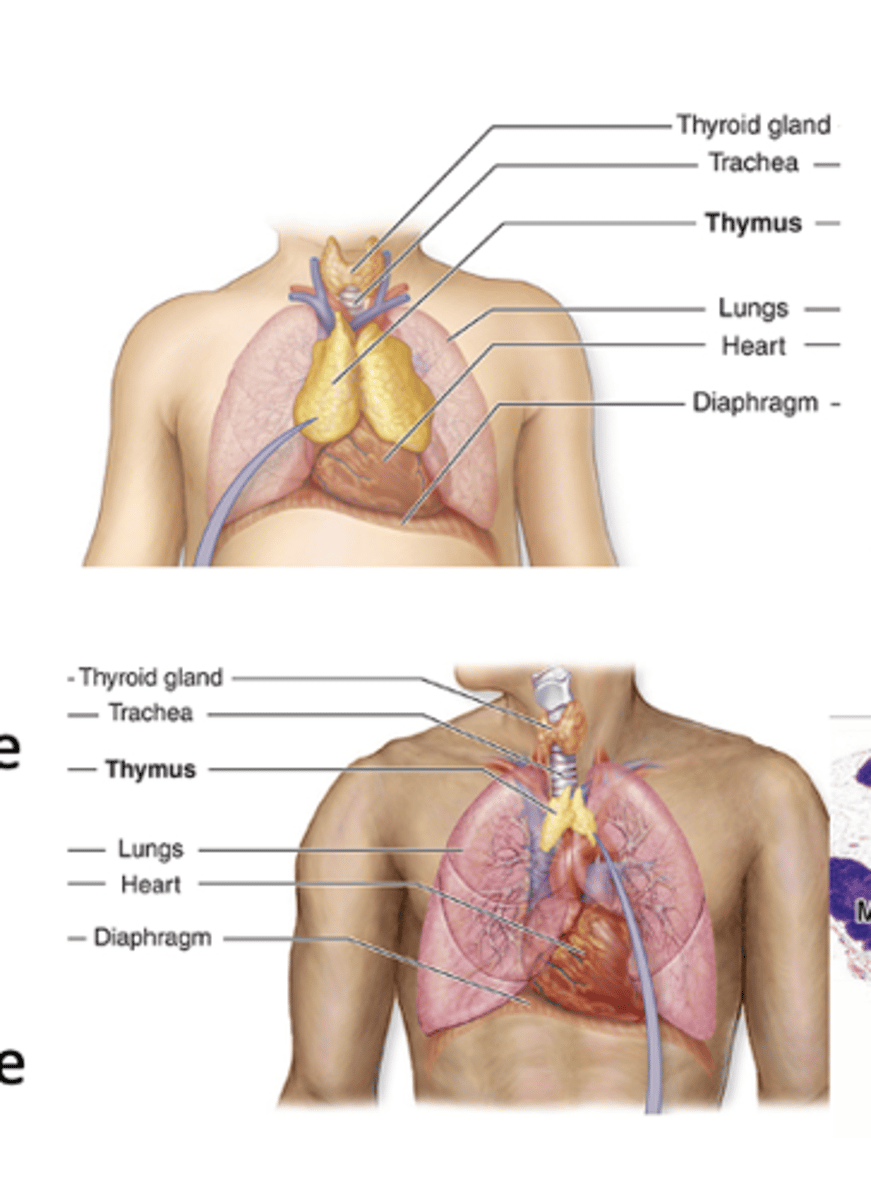
The thymus develops from which embryonic structure?
The endoderm of the third pair of pharyngeal arches.
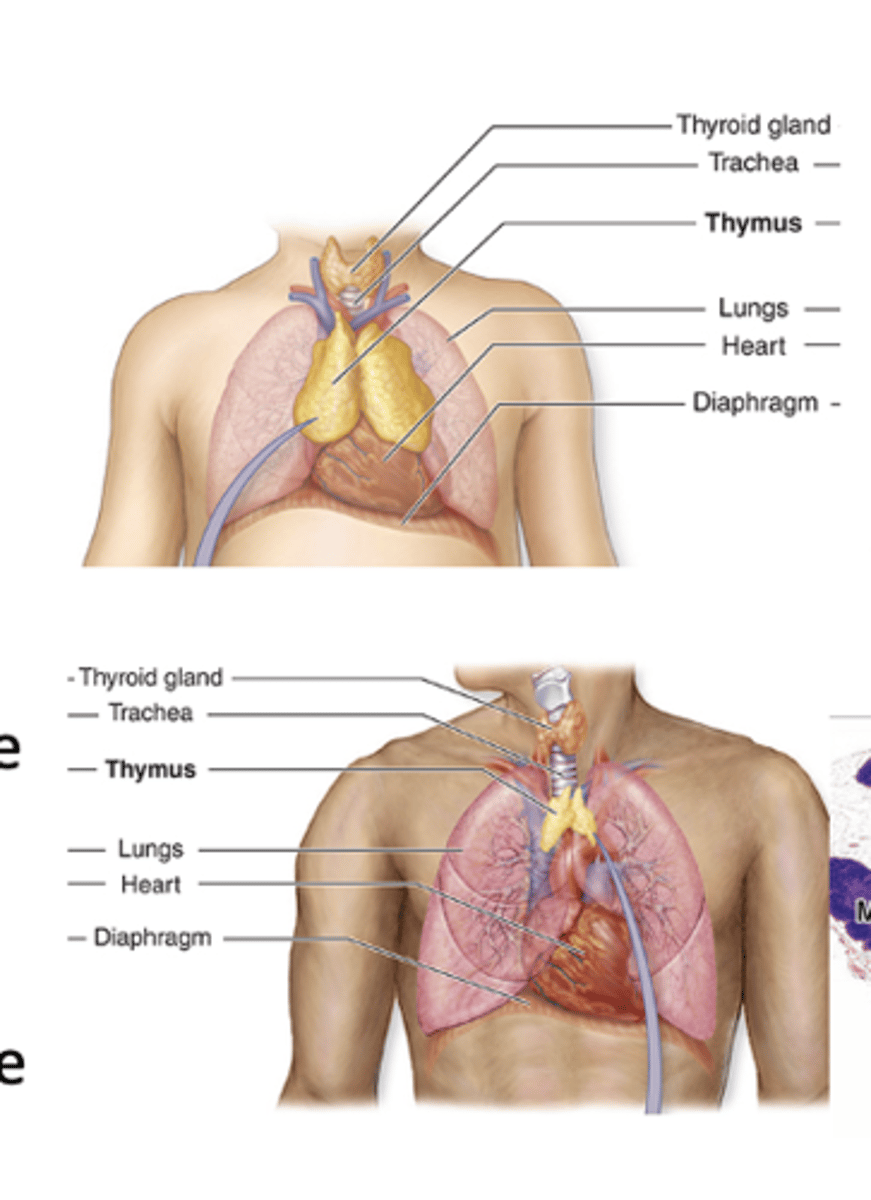
Which cells invade the thymus during development?
Lymphoblasts from the bone marrow.
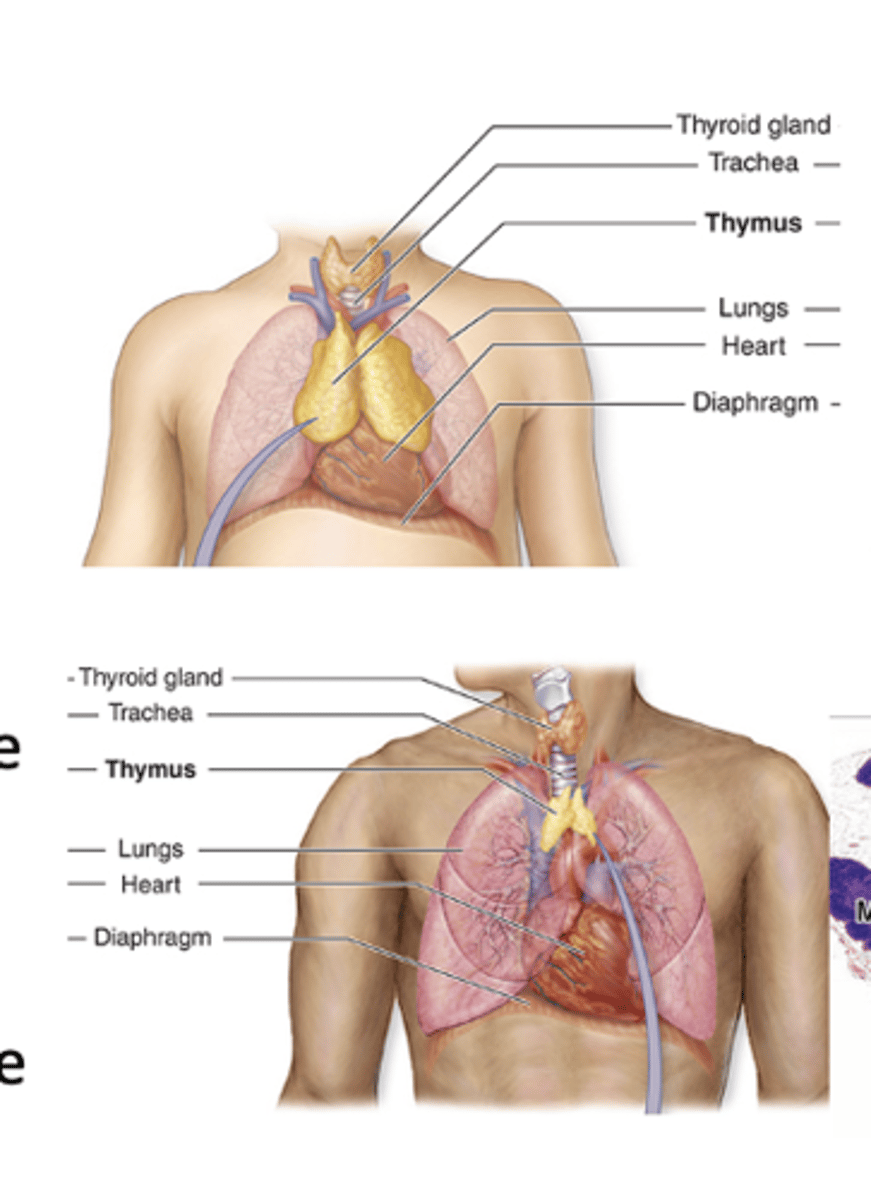
When is the thymus fully functional?
At birth and during puberty.
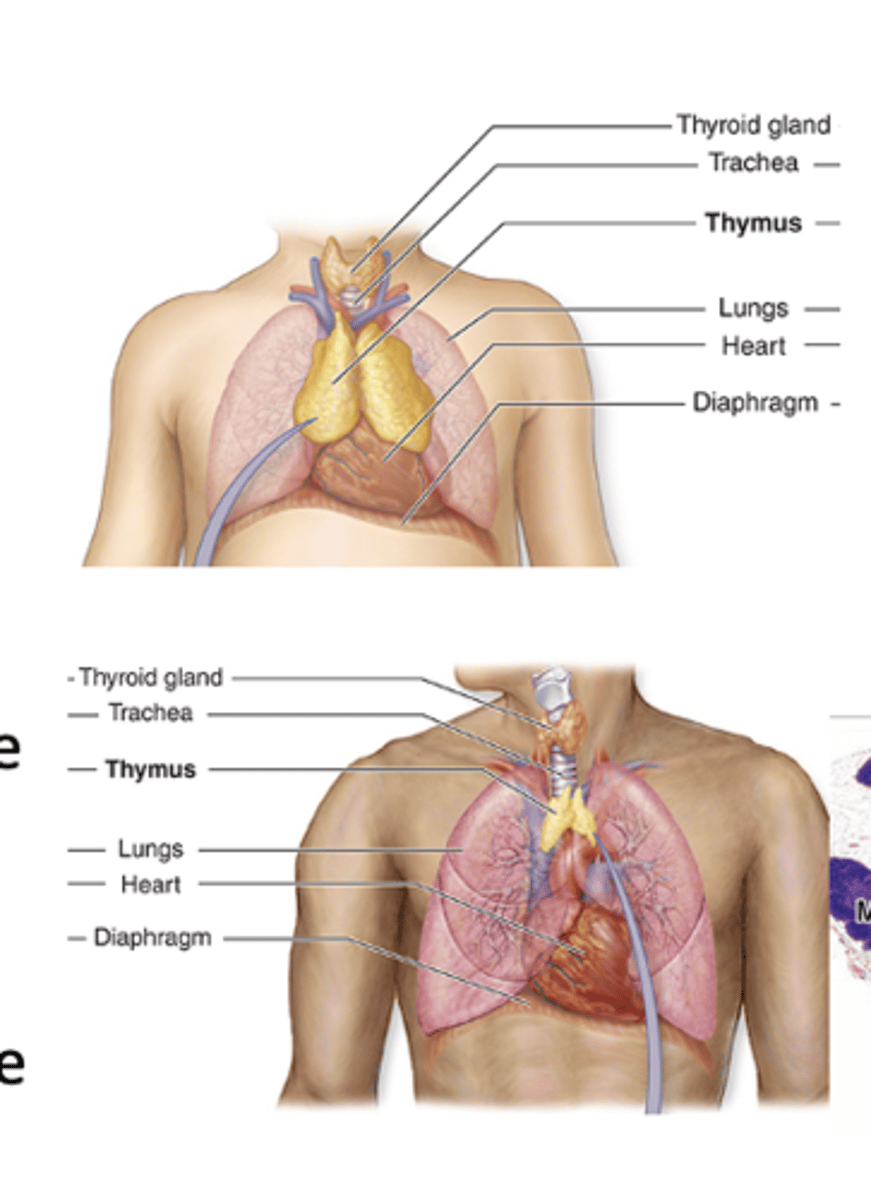
What happens to thymic cellularity and T cell output during involution?
Both are considerably reduced.
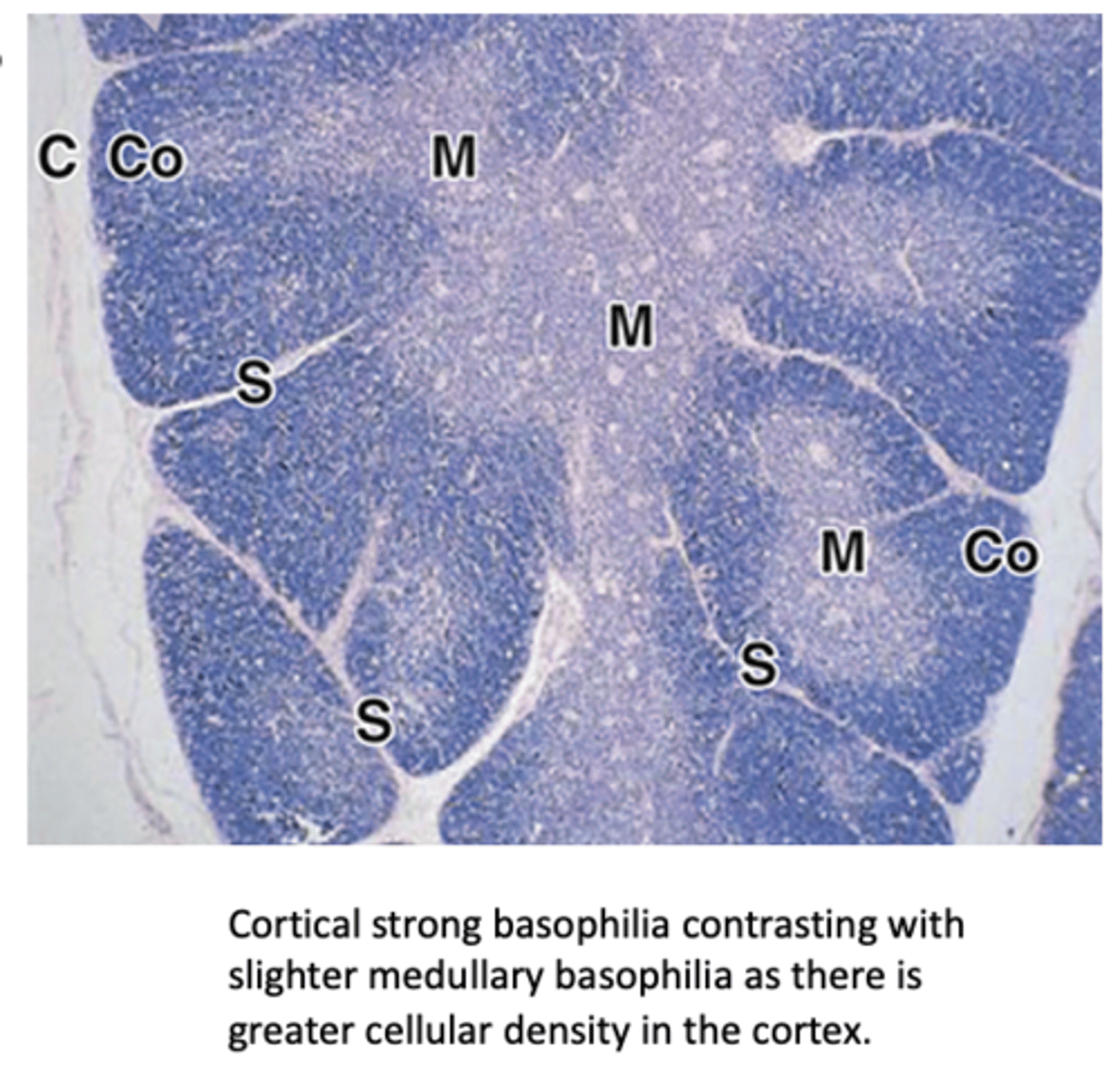
What surrounds the thymus histologically?
A vascularized capsule of connective tissue (CT).
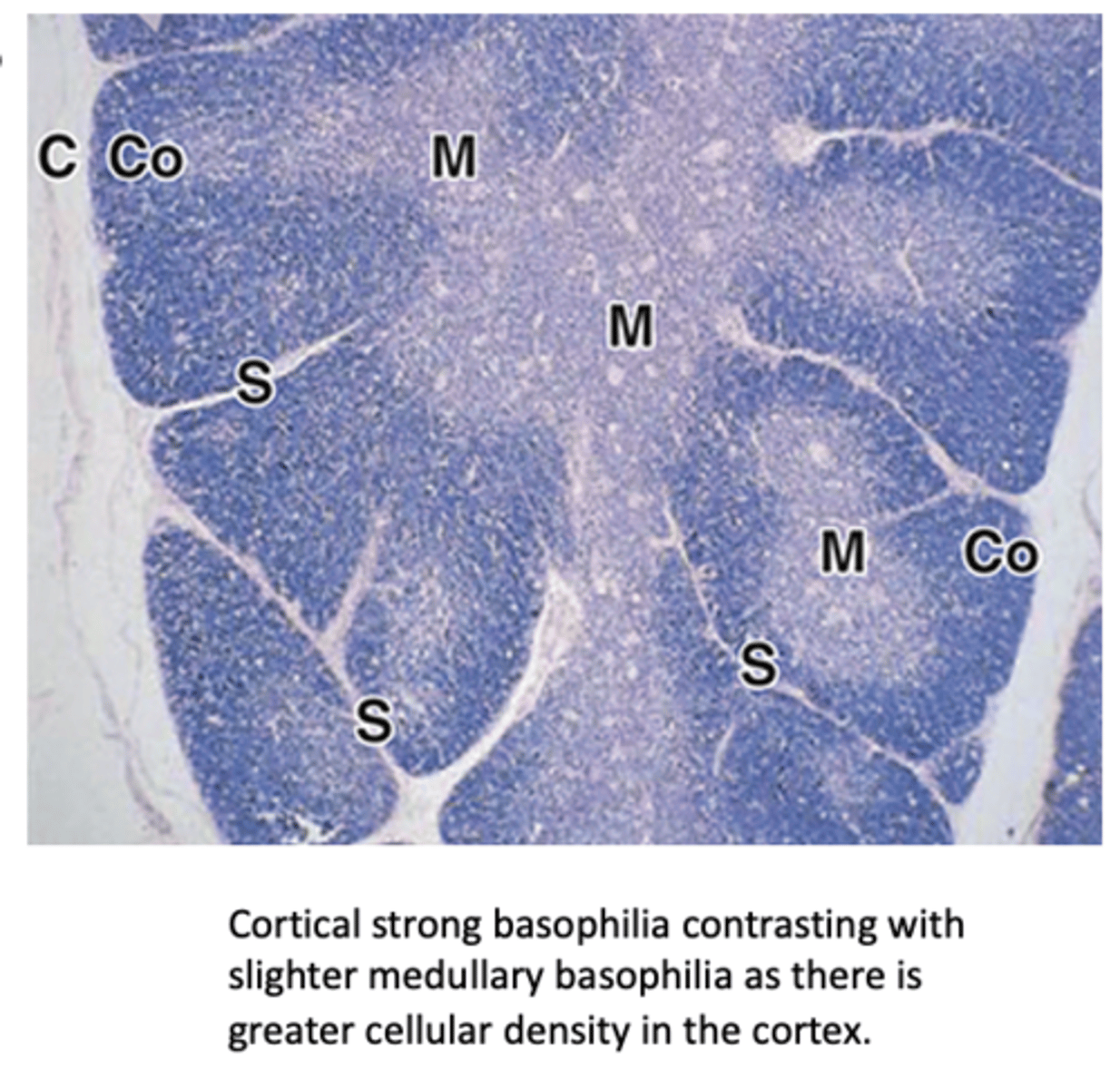
What divides the thymic parenchyma into incomplete lobules?
Septa that extend from the capsule.
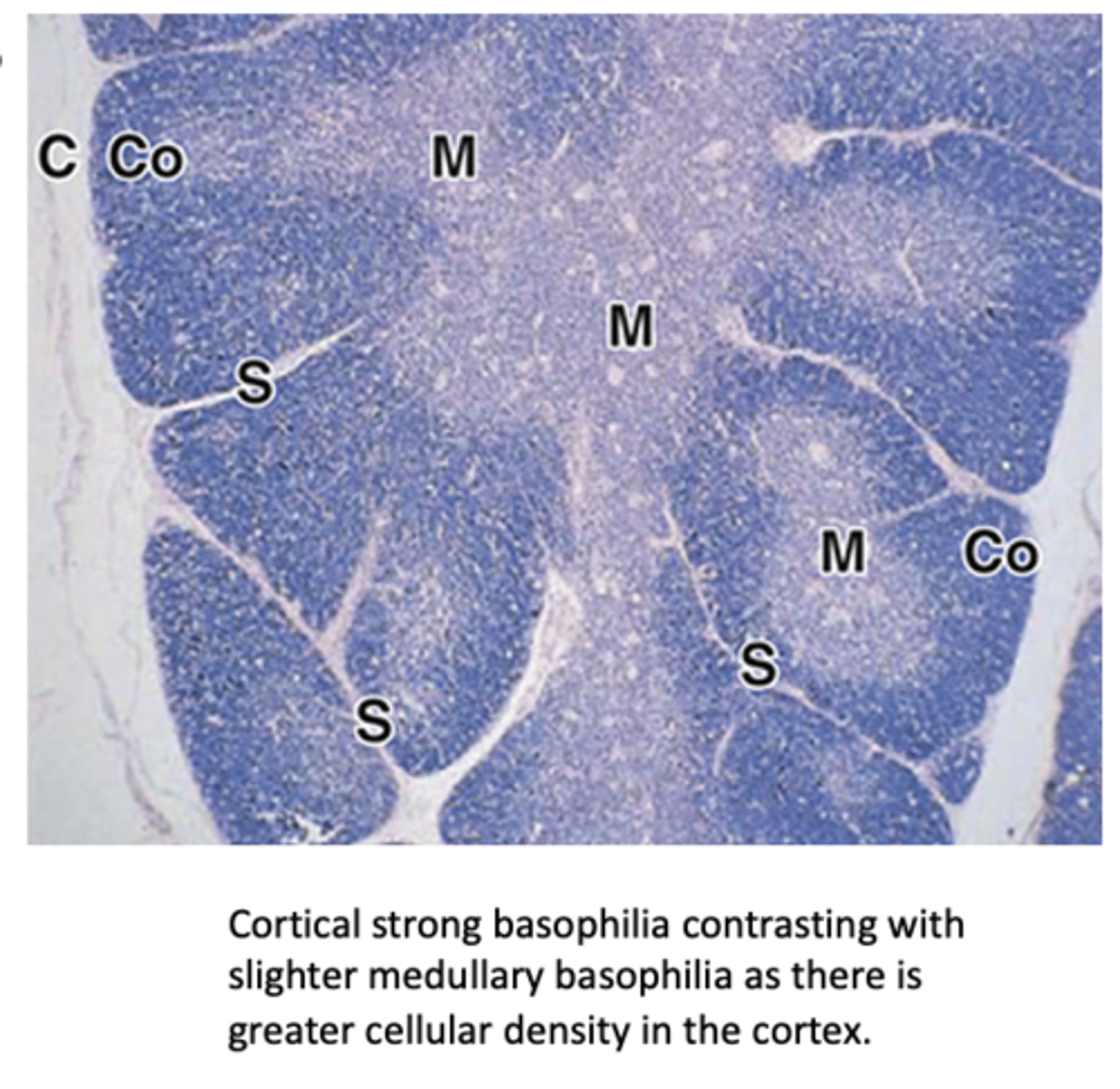
What are the two main regions of each thymic lobule?
The cortex and the medulla.
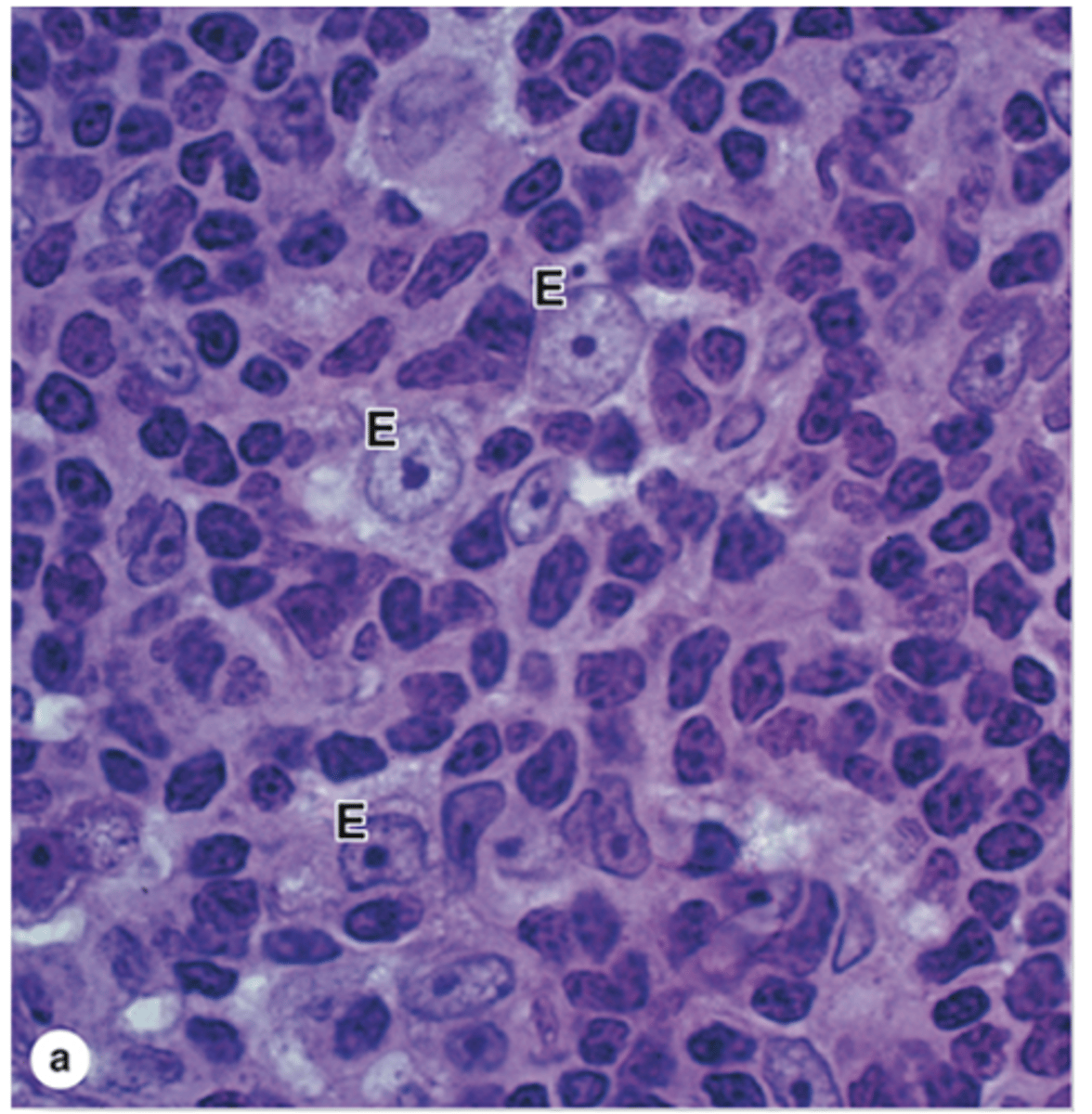
What are the major cells found in the thymic cortex? (3)
1. T lymphoblasts (thymocytes)
2. Macrophages
3. Thymic epithelial cells***
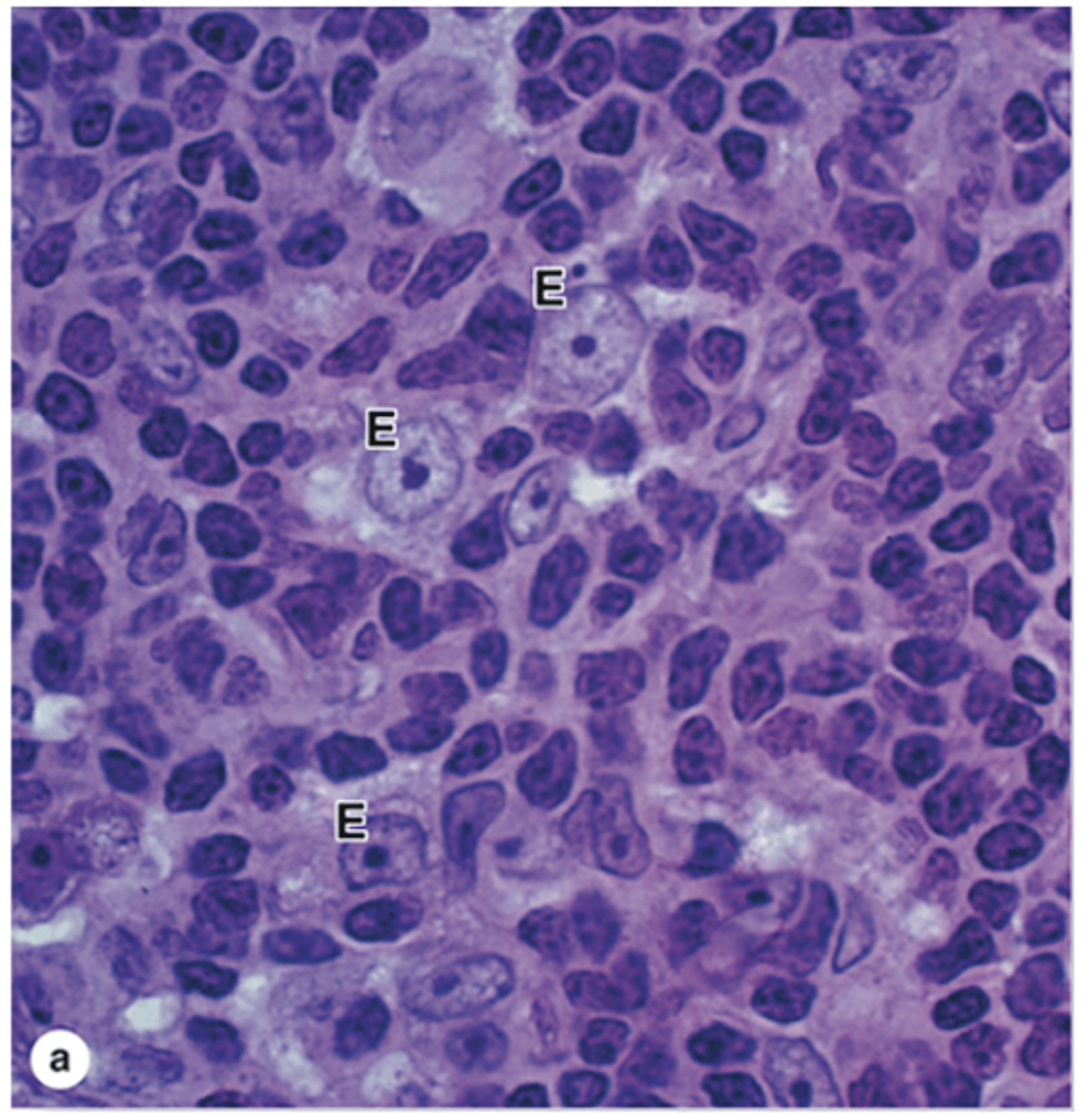
Which type of cell is very abundant in the thymic cortex?
T lymphoblasts or thymocytes.
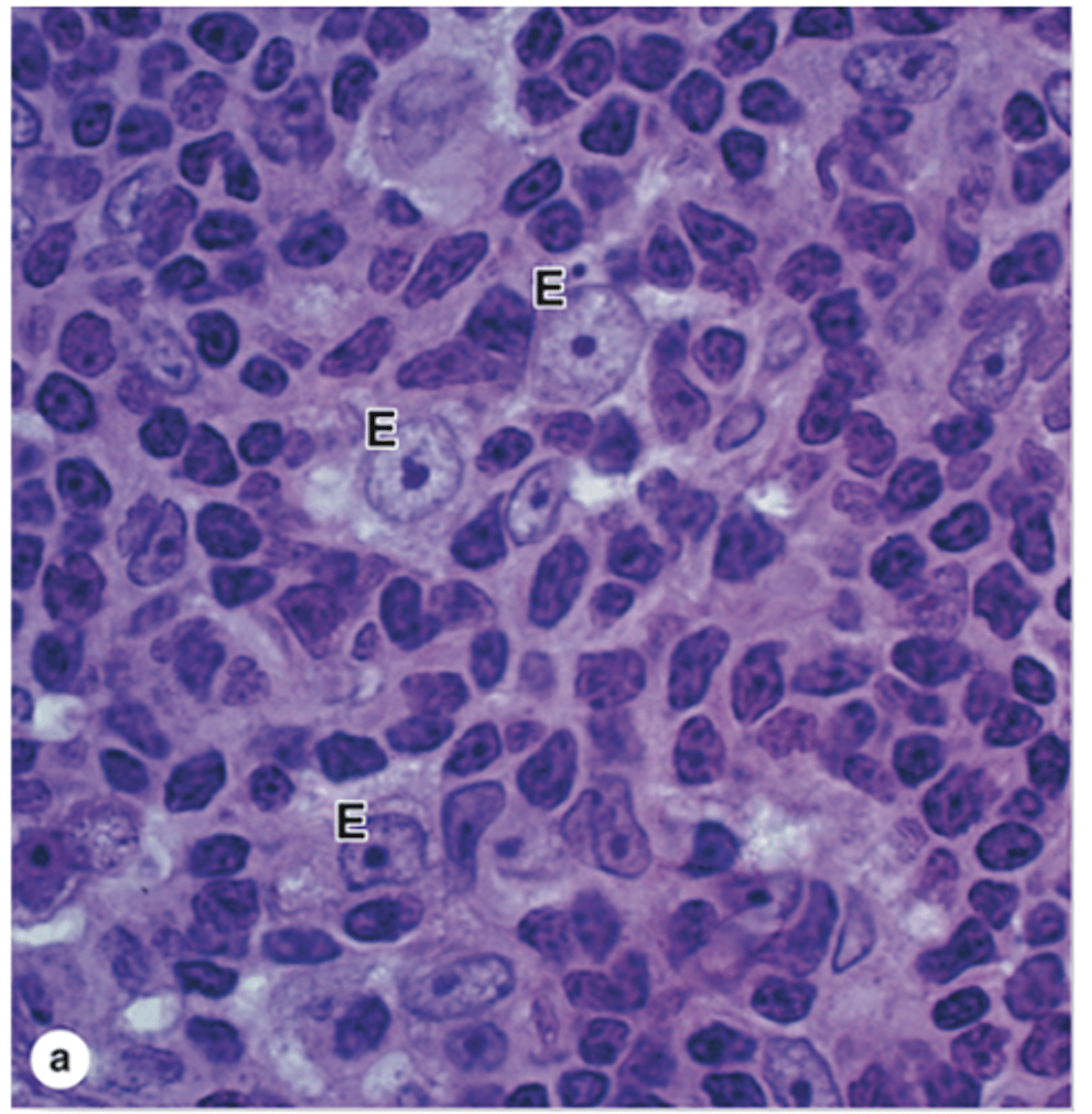
What features do thymic epithelial cells have?
both epithelial and reticular features
- There are three types!
What are the three types of thymic epithelial cells in the cortex?
1. Squamous TECs (type I epithelioreticular cells)
2. Stellate TECs (type II epithelioreticular cells)
3. Type III epithelioreticular cells
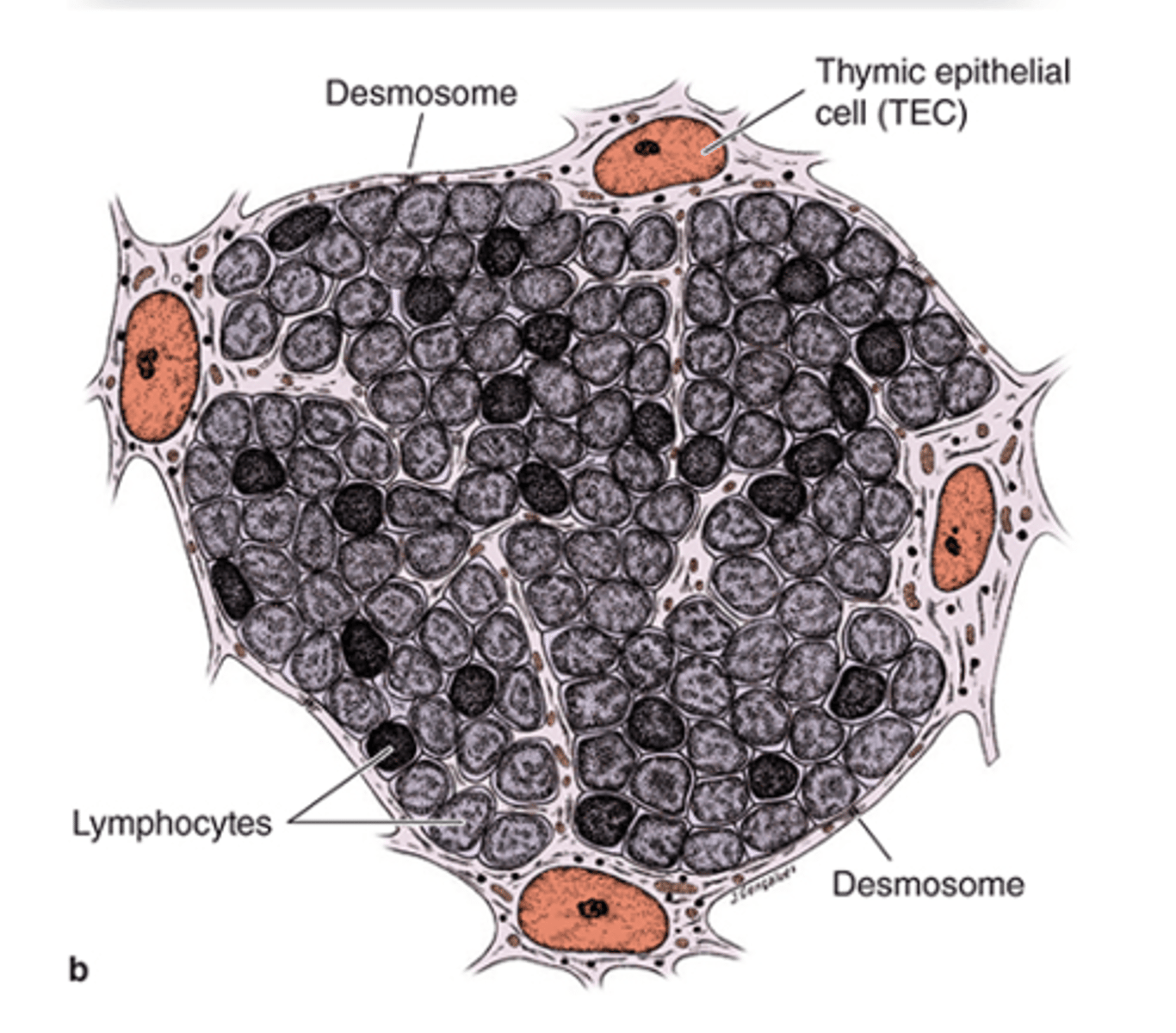
How are Squamous TECs (type I epithelioreticular cells) connected to each other?
They are joined by desmosomes and occluding junctions.
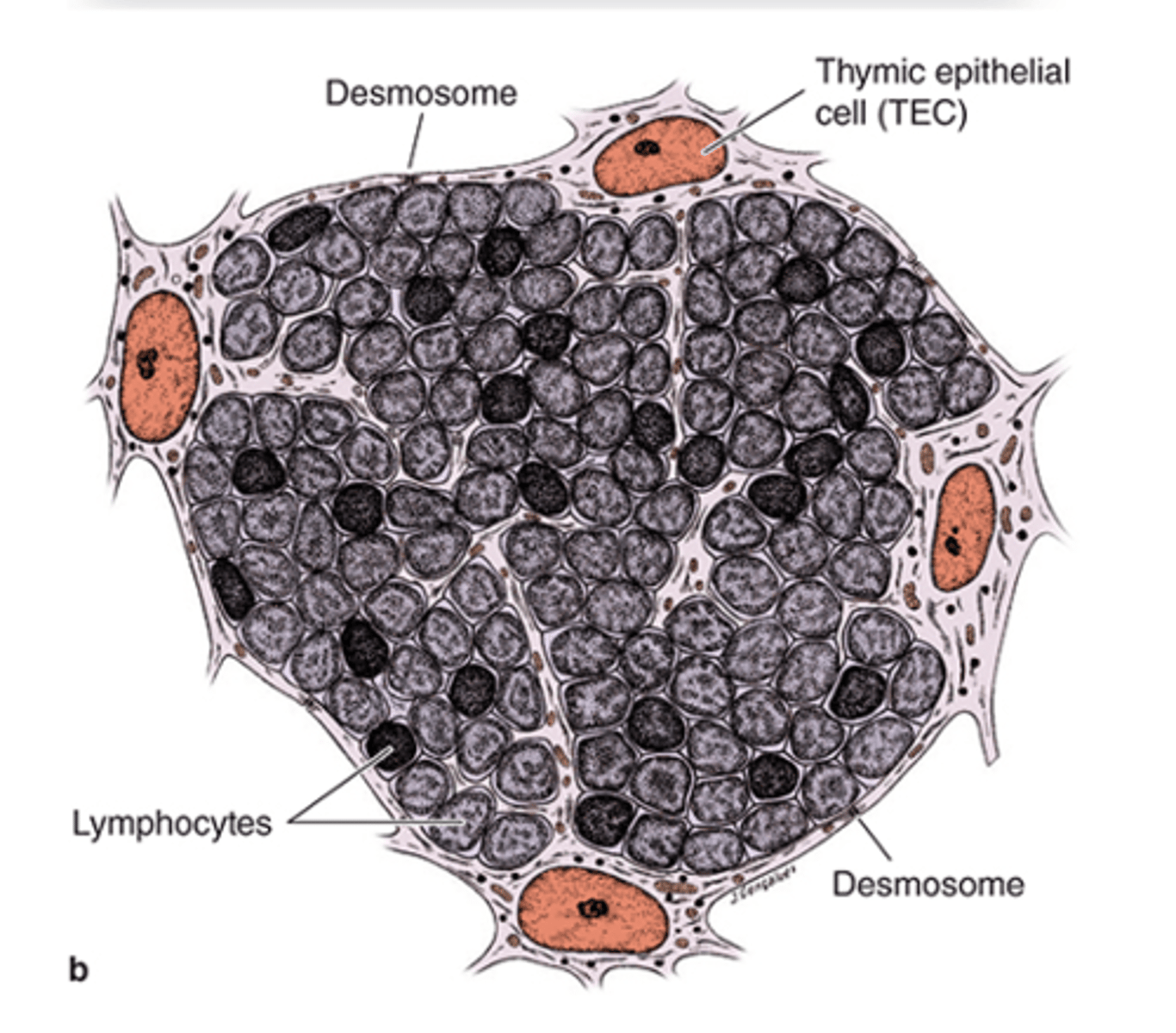
Where are Squamous TECs (type I epithelioreticular cells located in the thymus?
They line the connective tissue (CT) of the capsule and septa and surround blood vessels.
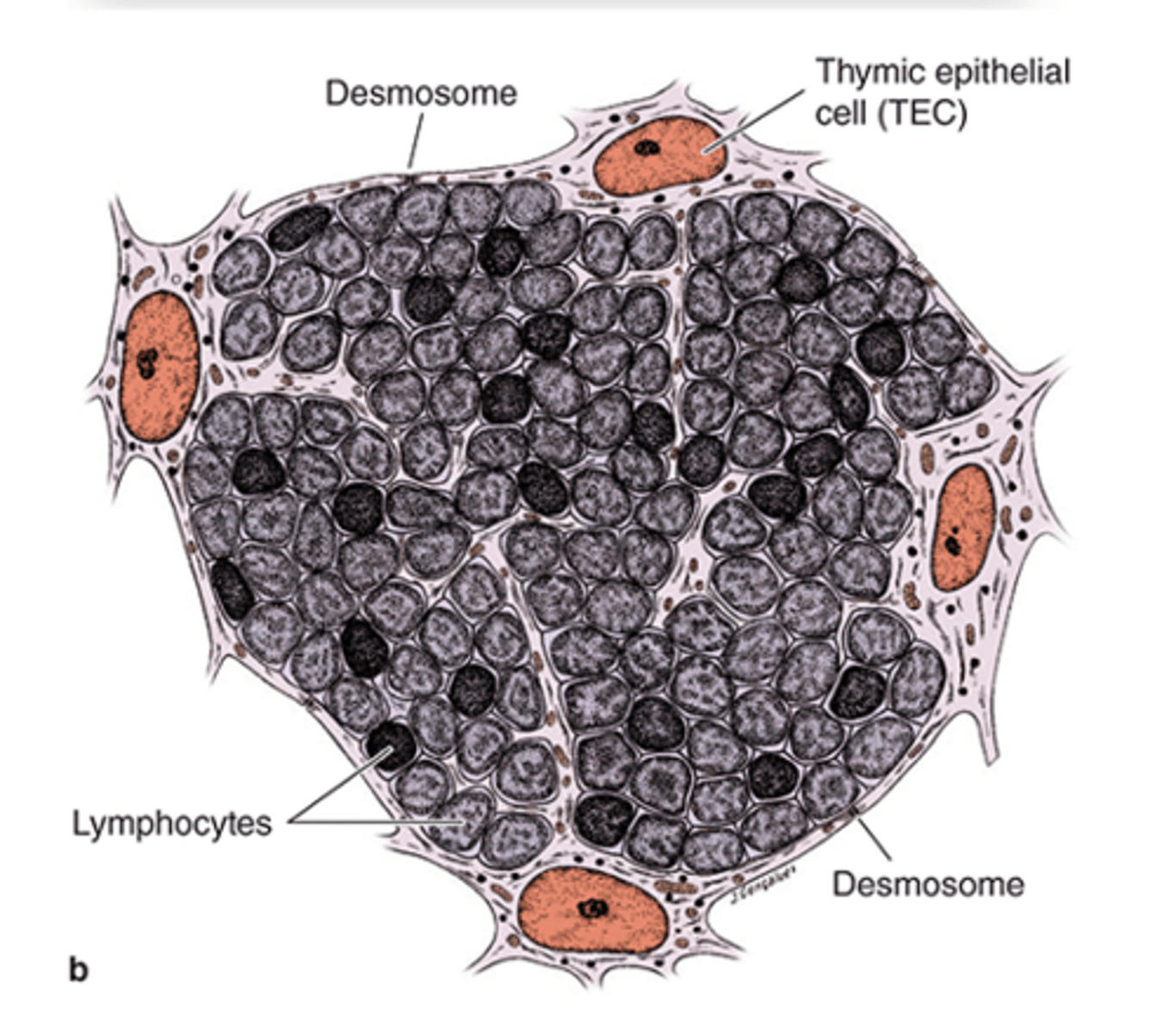
What important structure do Squamous TECs (type I epithelioreticular cells) help form?****
The blood-thymus barrier
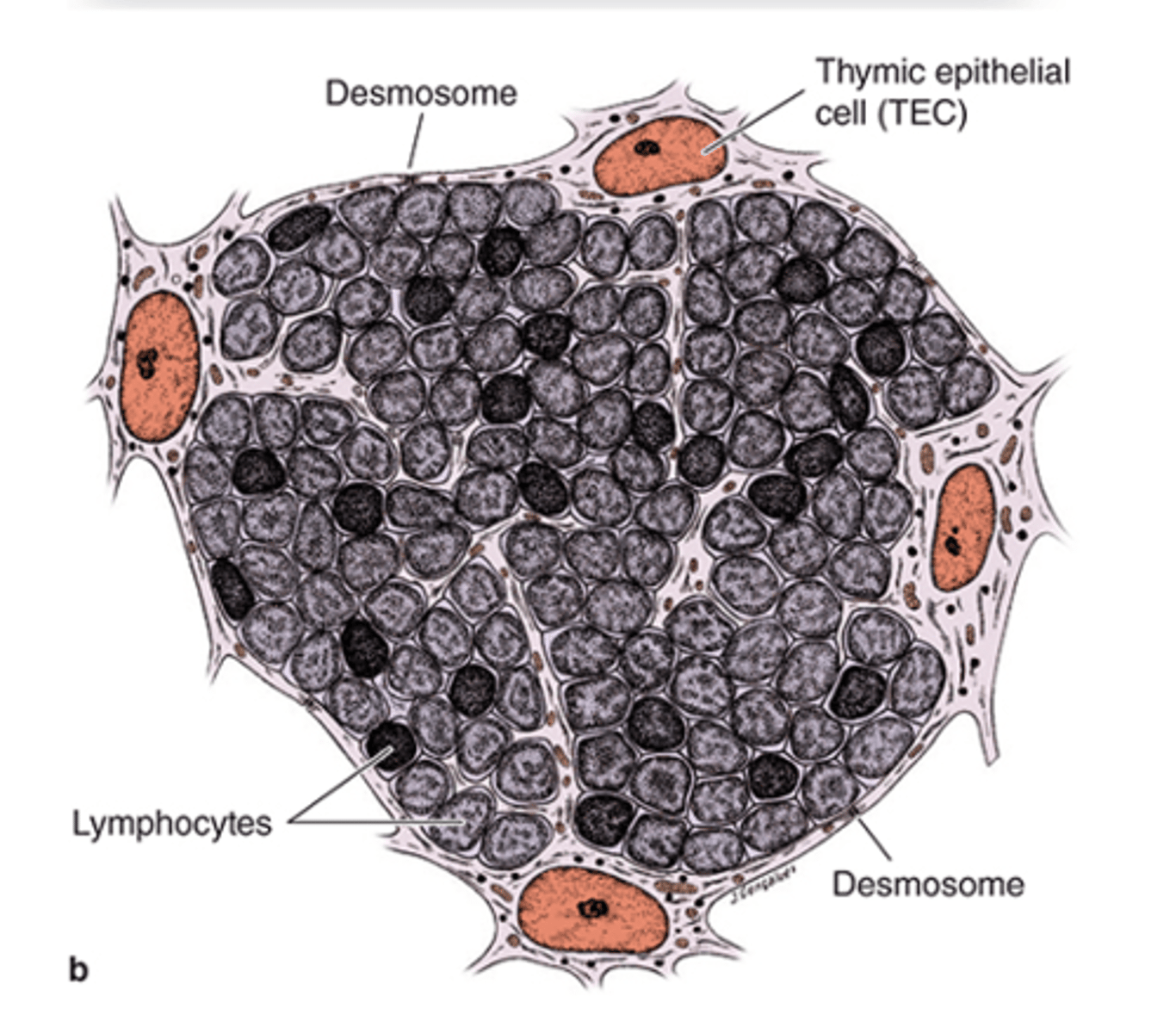
Which other cells work with squamous TECs to form the blood-thymus barrier?
Pericytes and vascular endothelial cells.
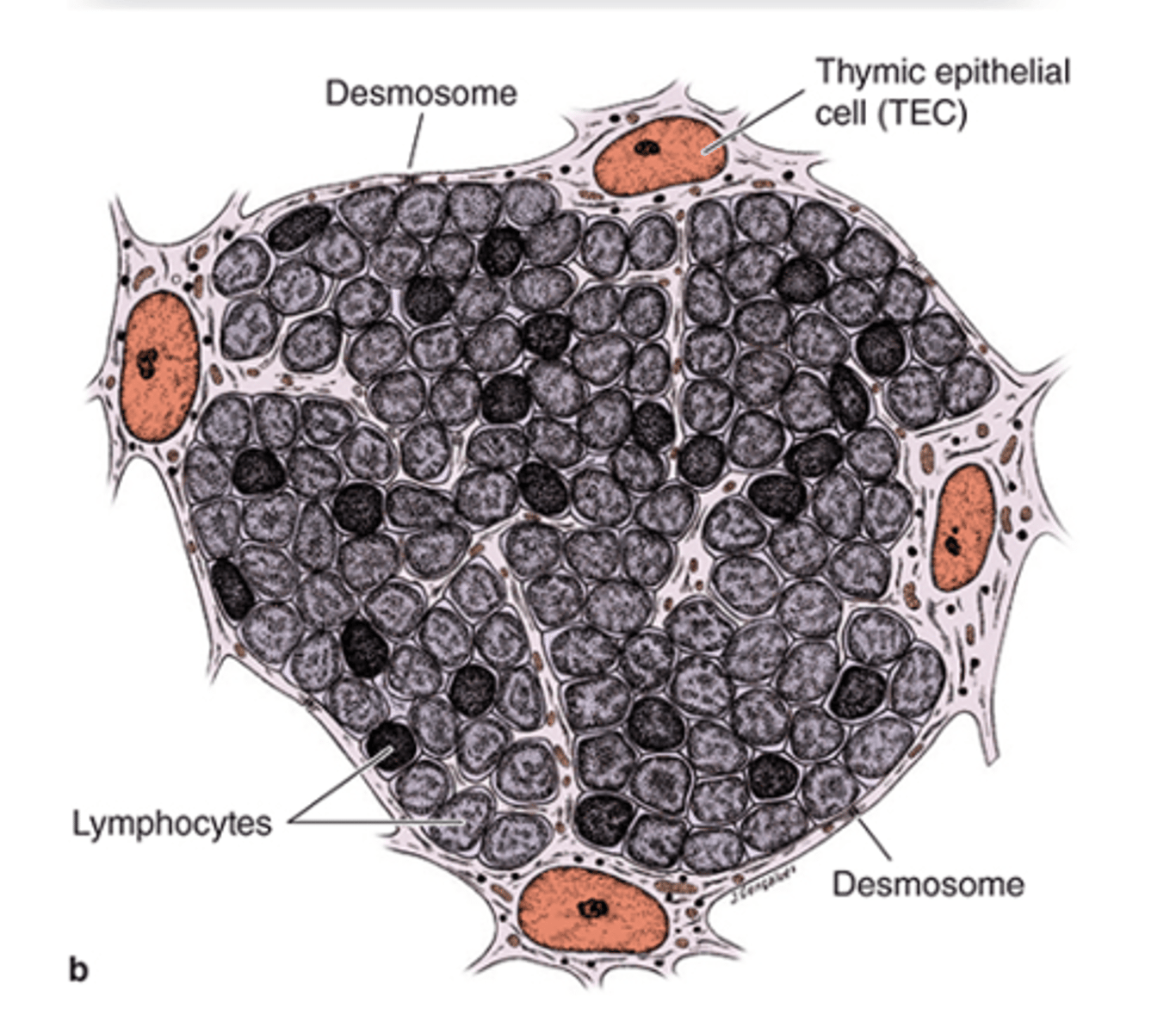
What is the function of the blood-thymus barrier?***
It prevents exposure of thymocytes to circulating antigens.
What do the processes of Stellate TECs (type II epithelioreticular cells) contain?
Keratin tonofilaments
How are Stellate TECs (type II epithelioreticular cells) connected to one another?
They are joined by desmosomes.
What structure do Stellate TECs (type II epithelioreticular cells) form to support macrophages and developing lymphocytes?
A cytoreticulum (since the thymus lacks reticular fibers).
What antigen-presenting molecules do Stellate TECs (type II epithelioreticular cells) express?
MHC class I and MHC class II molecules.
What do Stellate TECs secrete to aid immune cell maturation?
Cytokines (promote T cell development)
Where are Type III epithelioreticular cells located in the thymus?
At the boundary between the cortex and medulla.
What barrier do Type III epithelioreticular cells help form?
The functional corticomedullary barrier.
What type of junctions are found between the sheet-like cytoplasmic extensions of Type III epithelioreticular cells?
Occluding junctions (tight junctions)
Which antigen-presenting molecules do Type III epithelioreticular cells express?
MHC class I and MHC class II
What is the main function of cortical macrophages in the thymus?
Phagocytosis of apoptotic T cells.
What cellular feature is characteristic of cortical macrophages?
The presence of large lysosomes.
Which stain highlights cortical macrophages well?
PAS (Periodic acid-Schiff) stain.
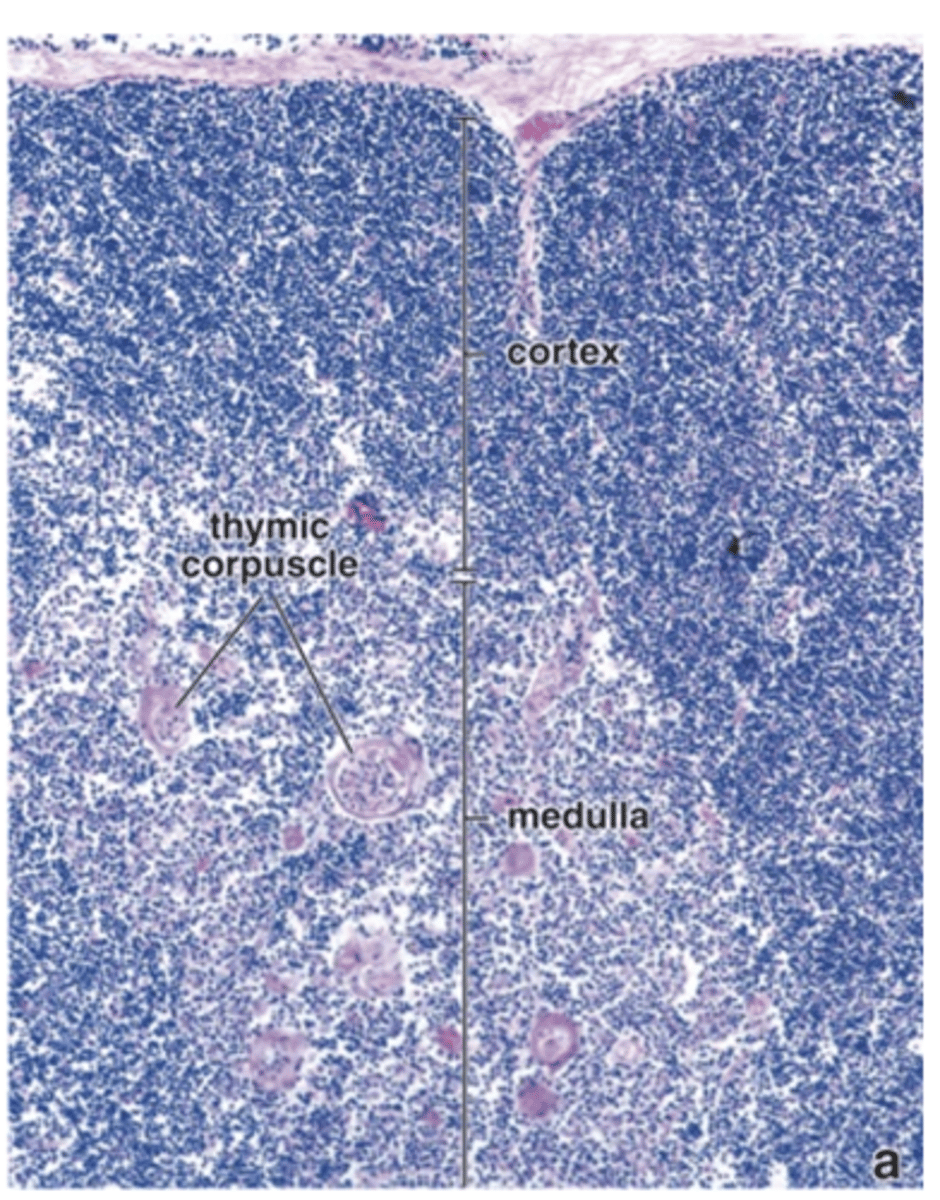
How does the thymic medulla appear compared to the cortex in staining?
It stains lighter than the cortex.
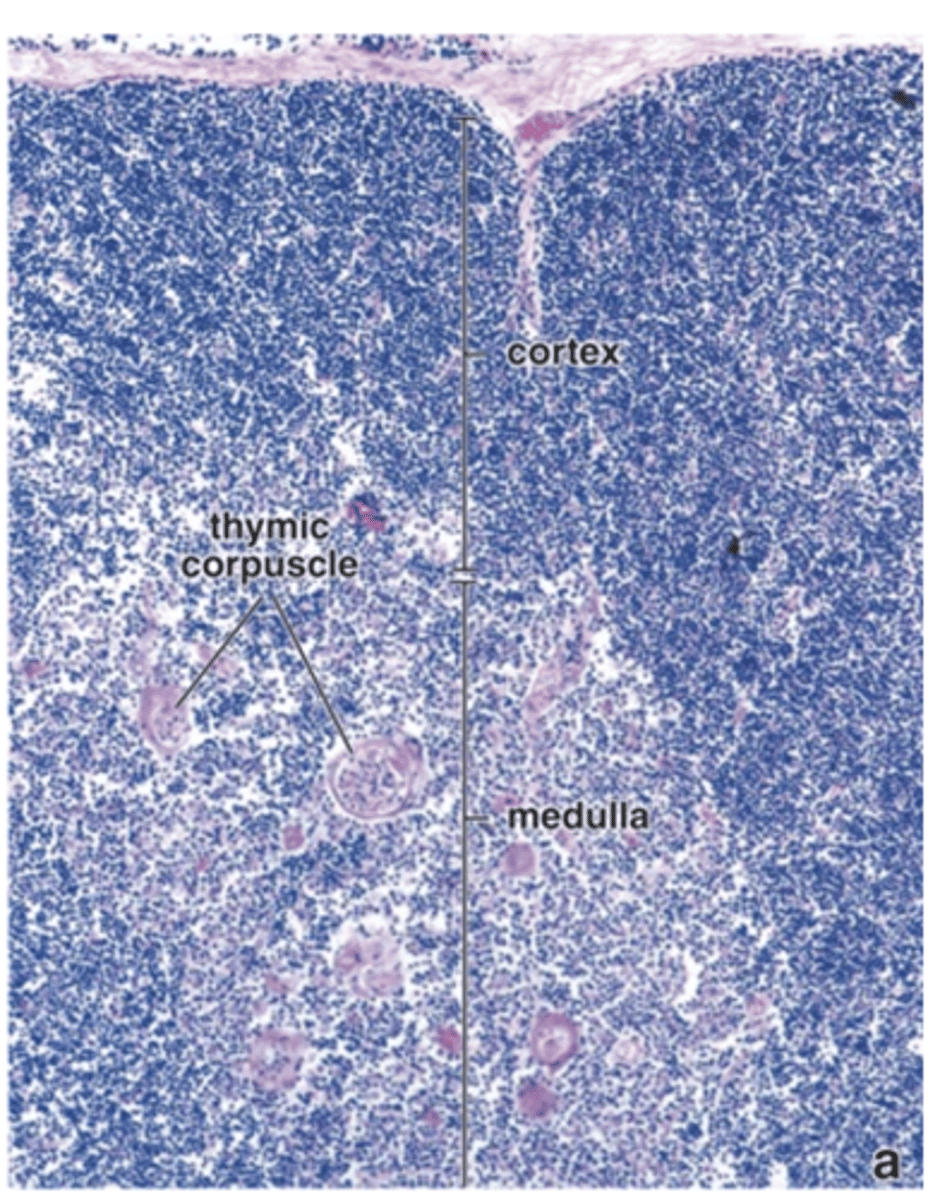
How do the lymphocytes in the thymic medulla differ from those in the cortex?
They are fewer in number but larger and more mature.
What are the three types of medullary thymic epithelial cells (TECs) present in the thymic medulla?
1. Type IV epithelioreticular cells
2. Type V epithelioreticular cells
3. Type VI epithelioreticular cells
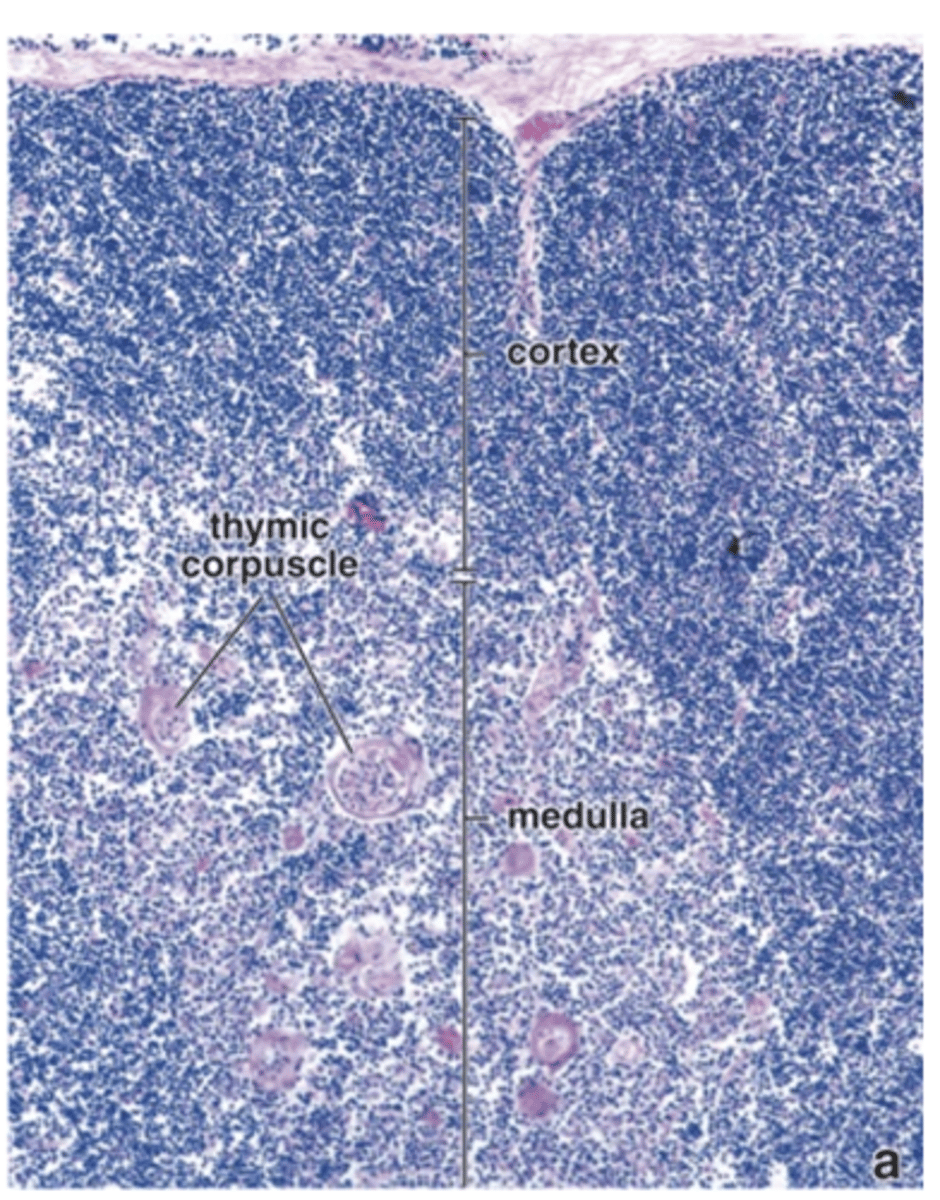
What distinctive structures are found in the thymic medulla?
Hassall’s corpuscles.
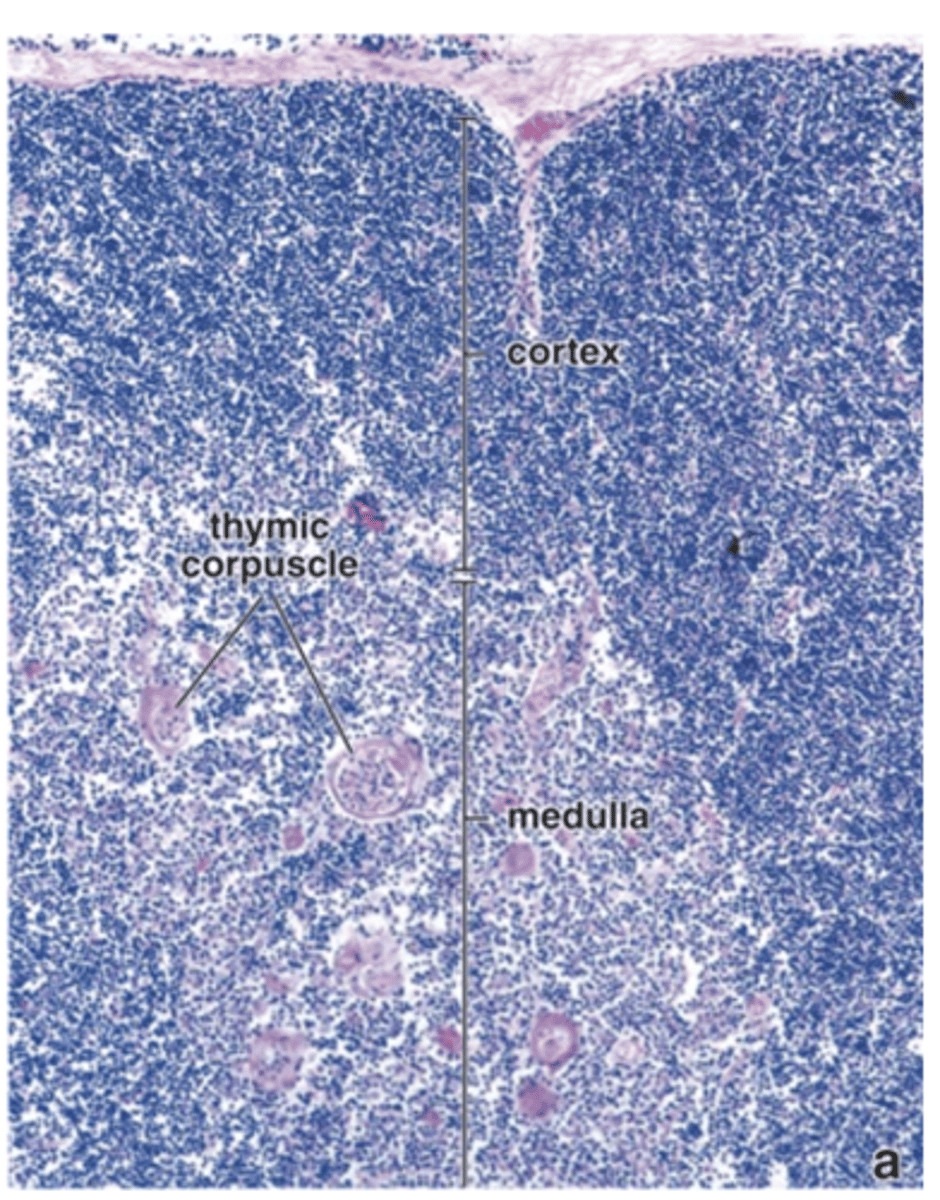
What are Hassall’s corpuscles made of?
Isolated masses of concentrically arranged type VI TECs.
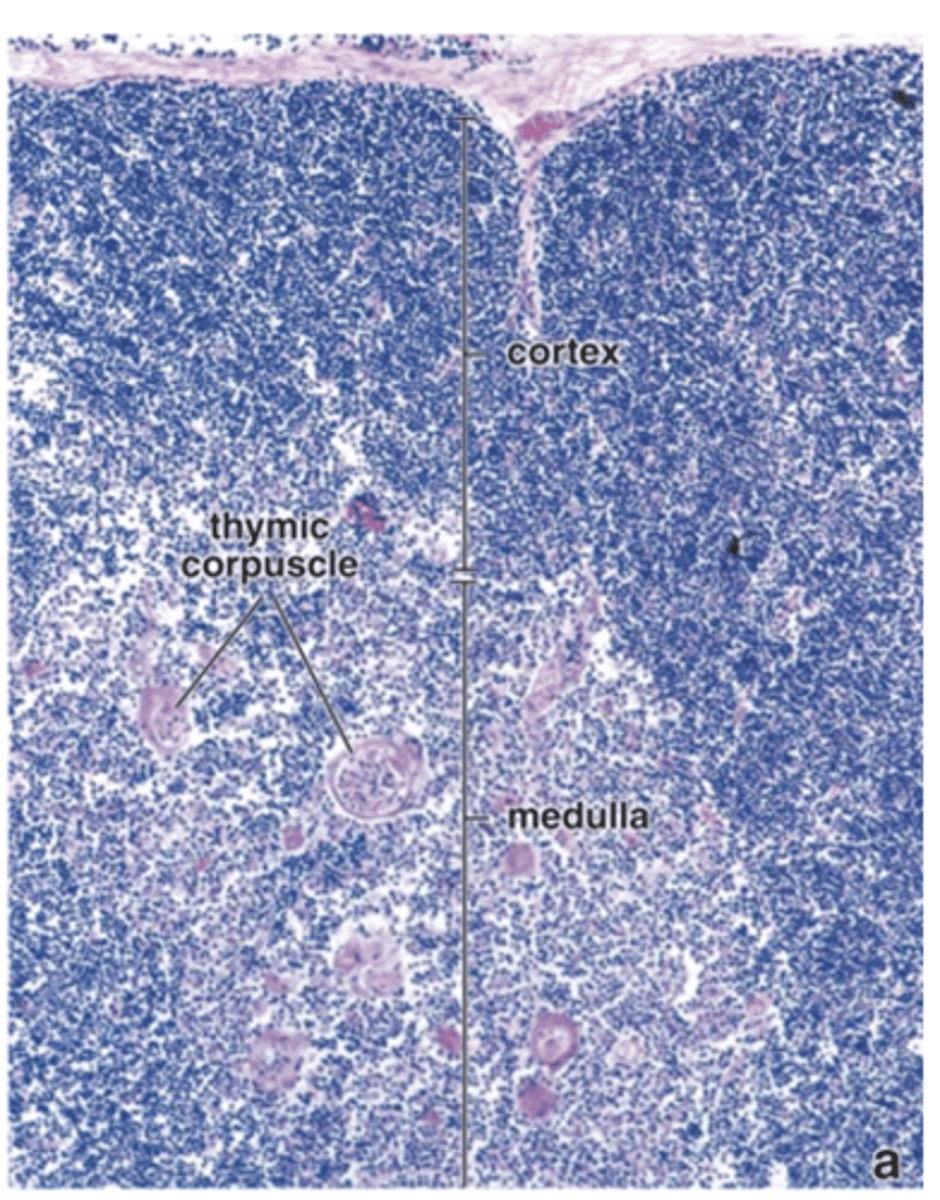
Where are Hassall’s corpuscles uniquely found?
In the thymic medulla.
Where are Type IV epithelioreticular cells located in the thymus medulla?
They form a second layer between the medulla and the cortex.
Which cortical cells are Type IV epithelioreticular cells closely associated with?
Type III (cortical) thymic epithelial cells.
What barrier do Type IV and Type III epithelioreticular cells work together to form?
The corticomedullary barrier.
What types of cells do Type IV epithelioreticular cells form occluding junctions with?
Adjacent Type IV cells and Type III cells.
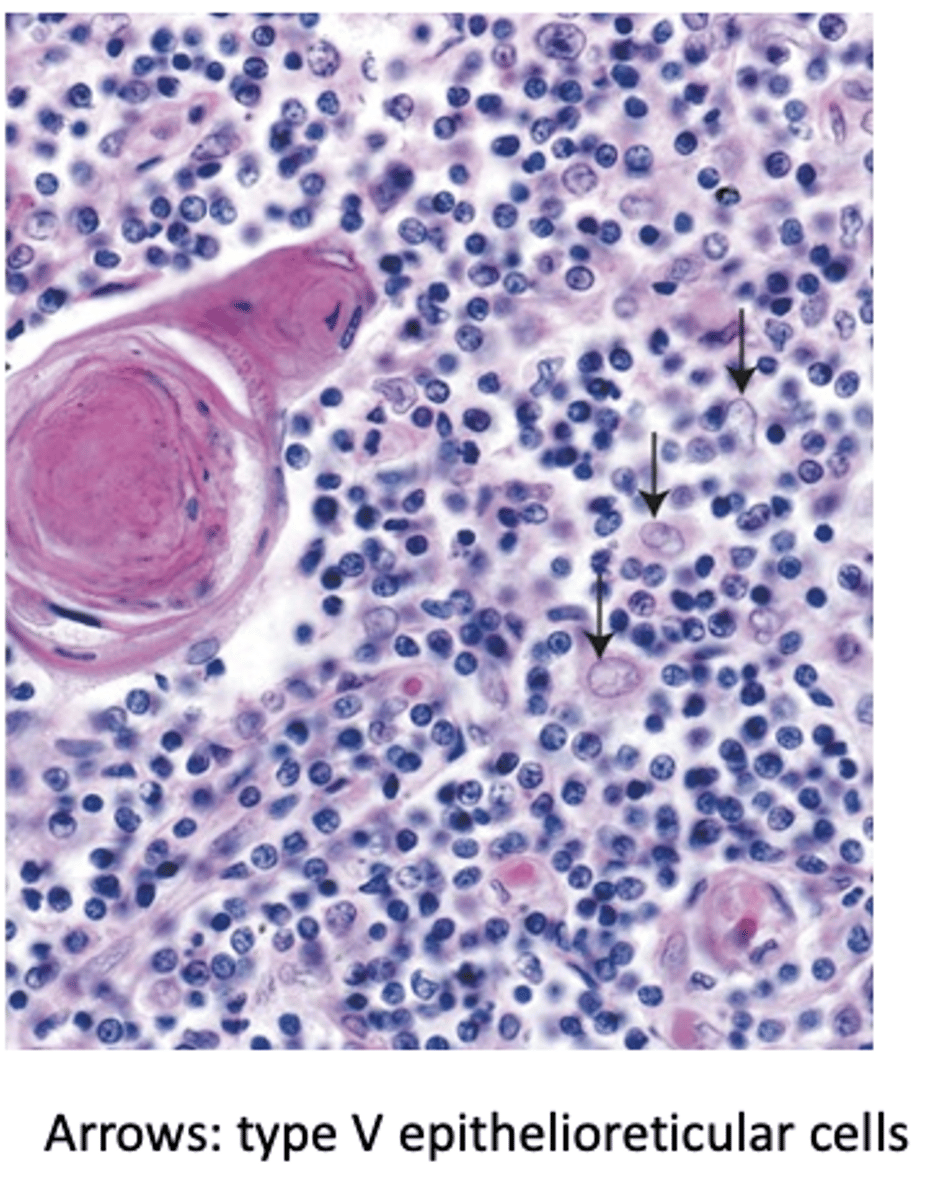
Where are Type V epithelioreticular cells located in the thymus?
Throughout the medulla.
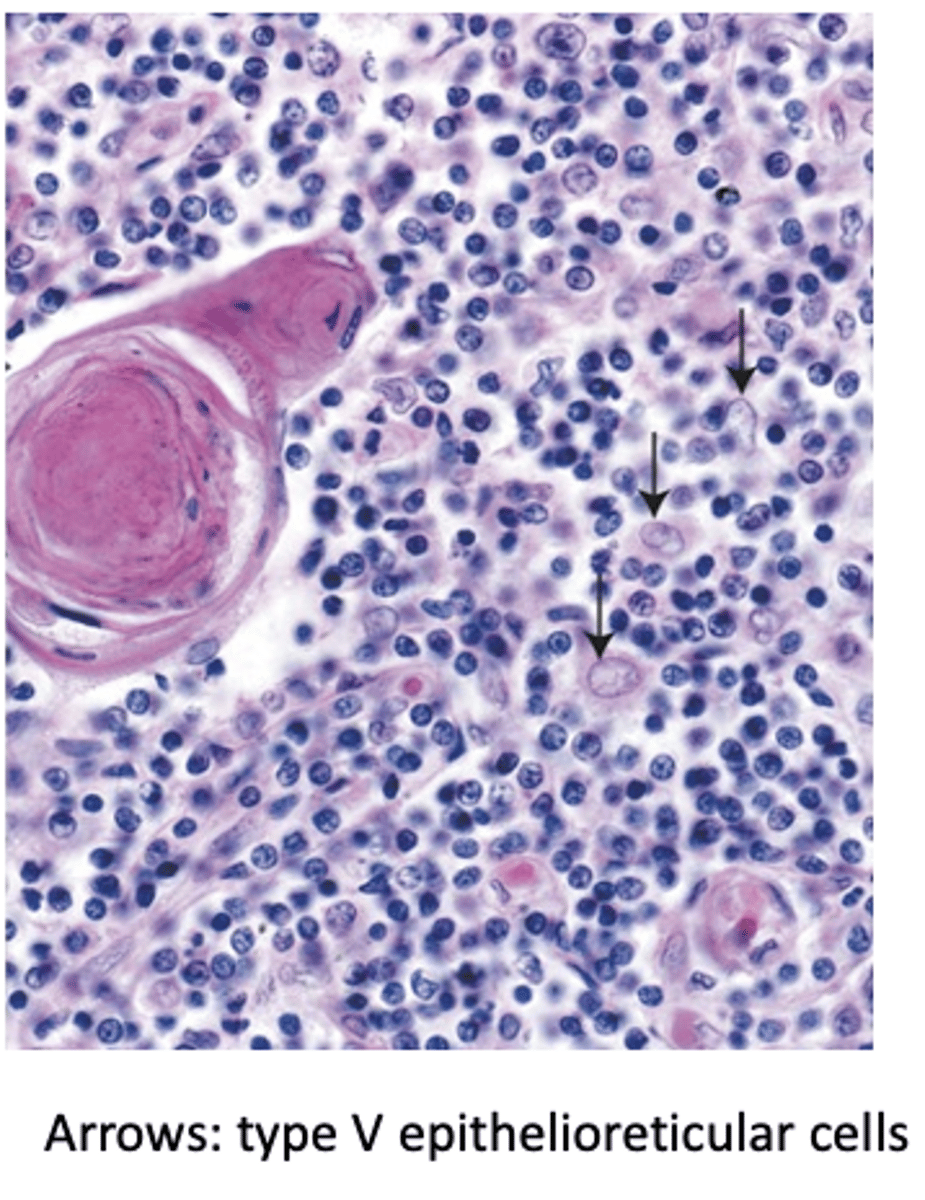
How are the processes of Type V epithelioreticular cells connected?
By desmosomes
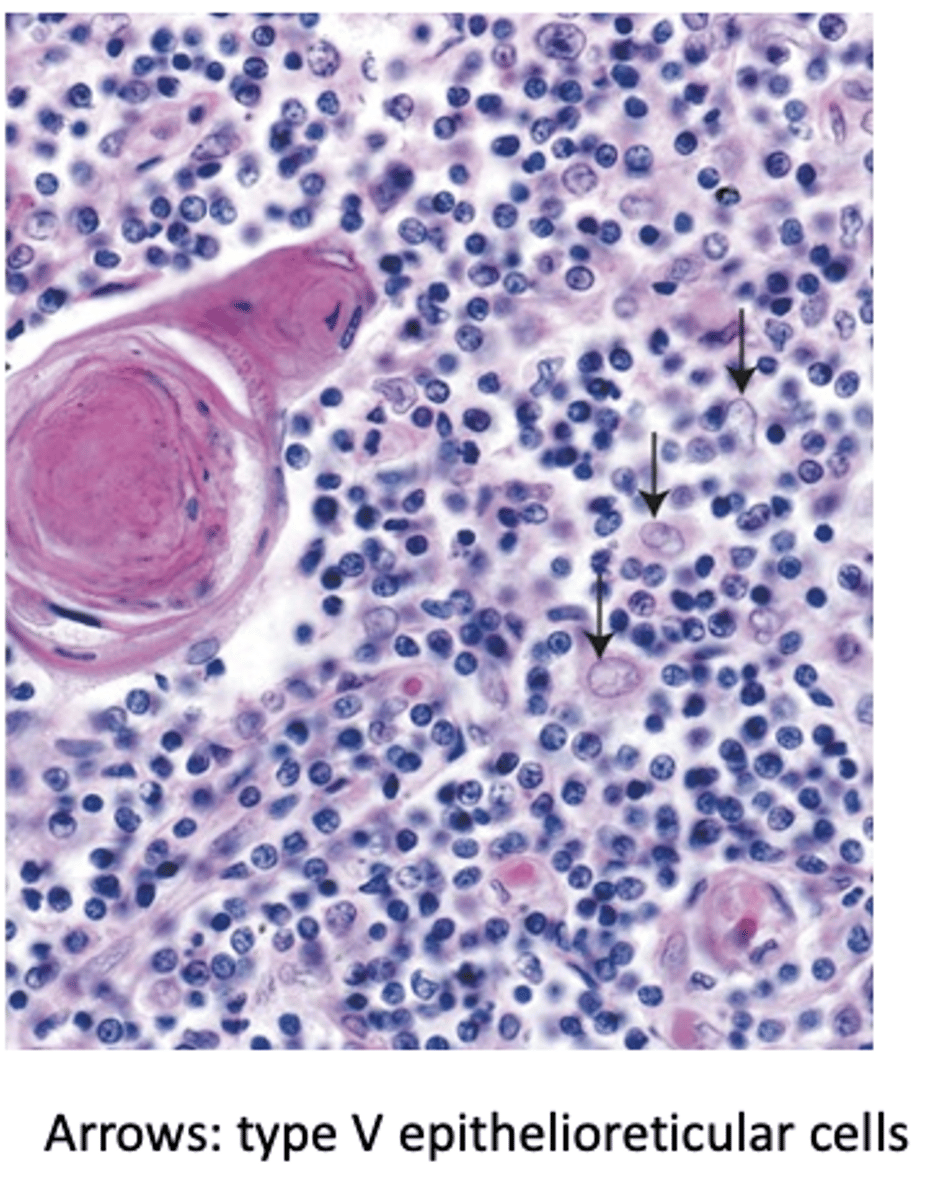
What structure do Type V epithelioreticular cells form?
A cytoreticulum.
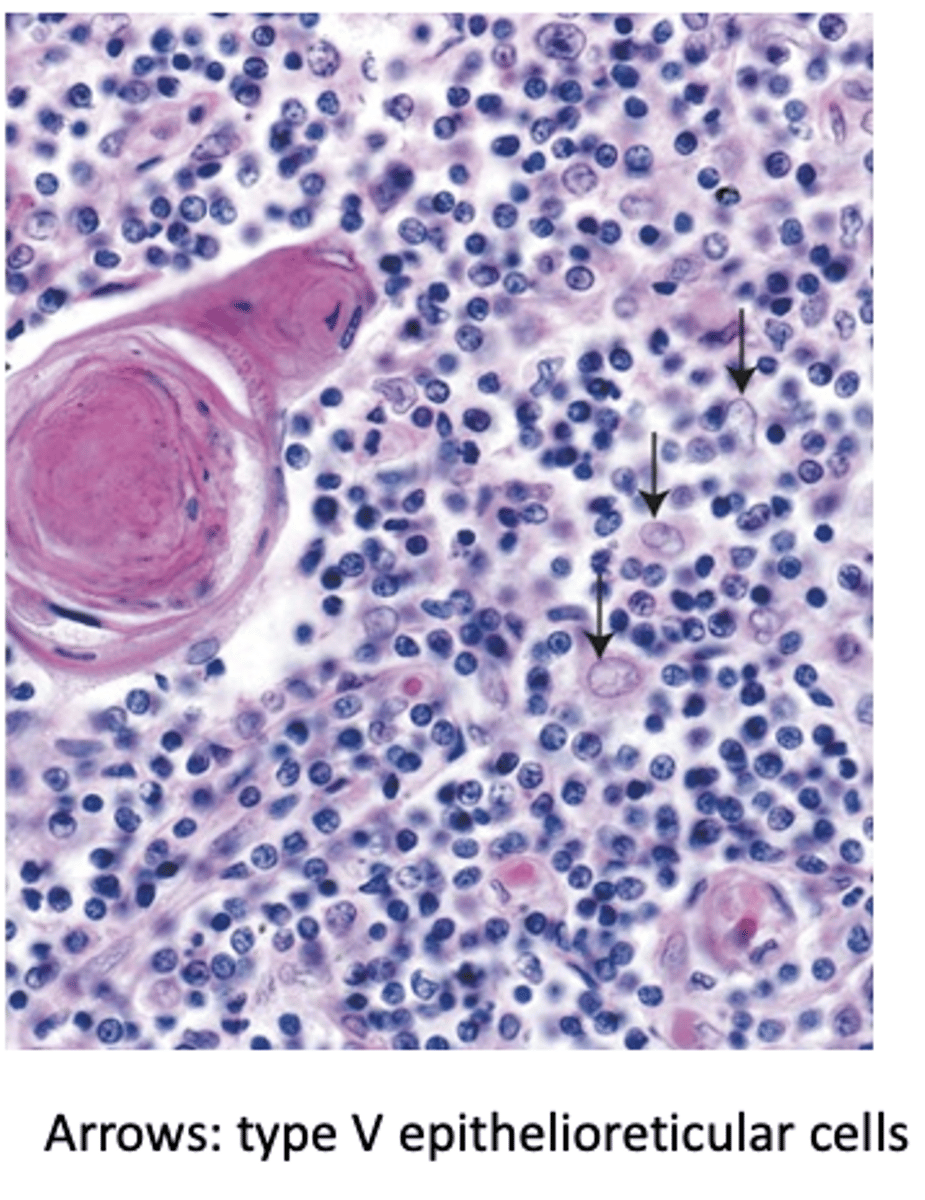
Which cells are supported by the cytoreticulum formed by Type V TECs? (3)
T lymphocytes, dendritic cells, and macrophages.
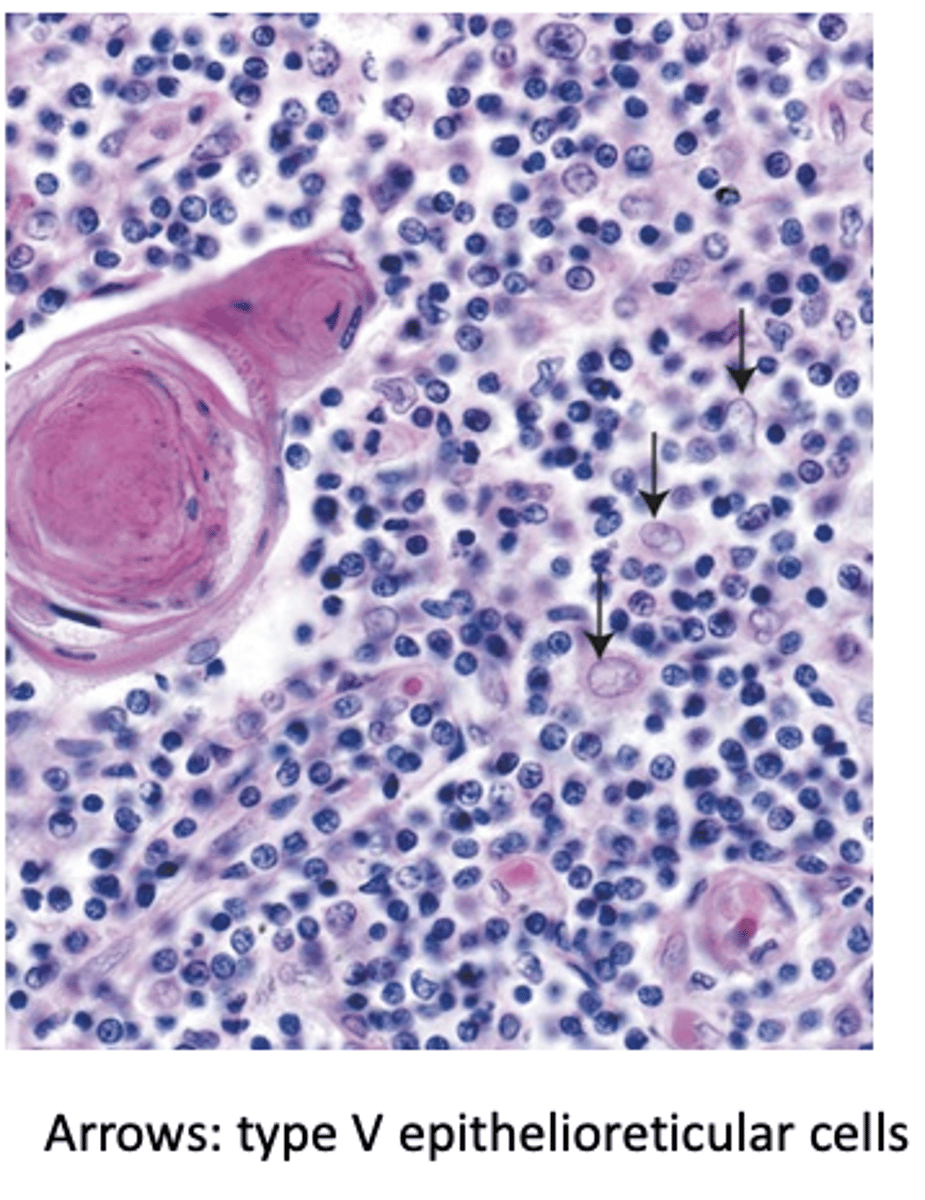
What unique function do Type V epithelioreticular cells perform beyond the thymus?
They express specialized proteins that affect other organs
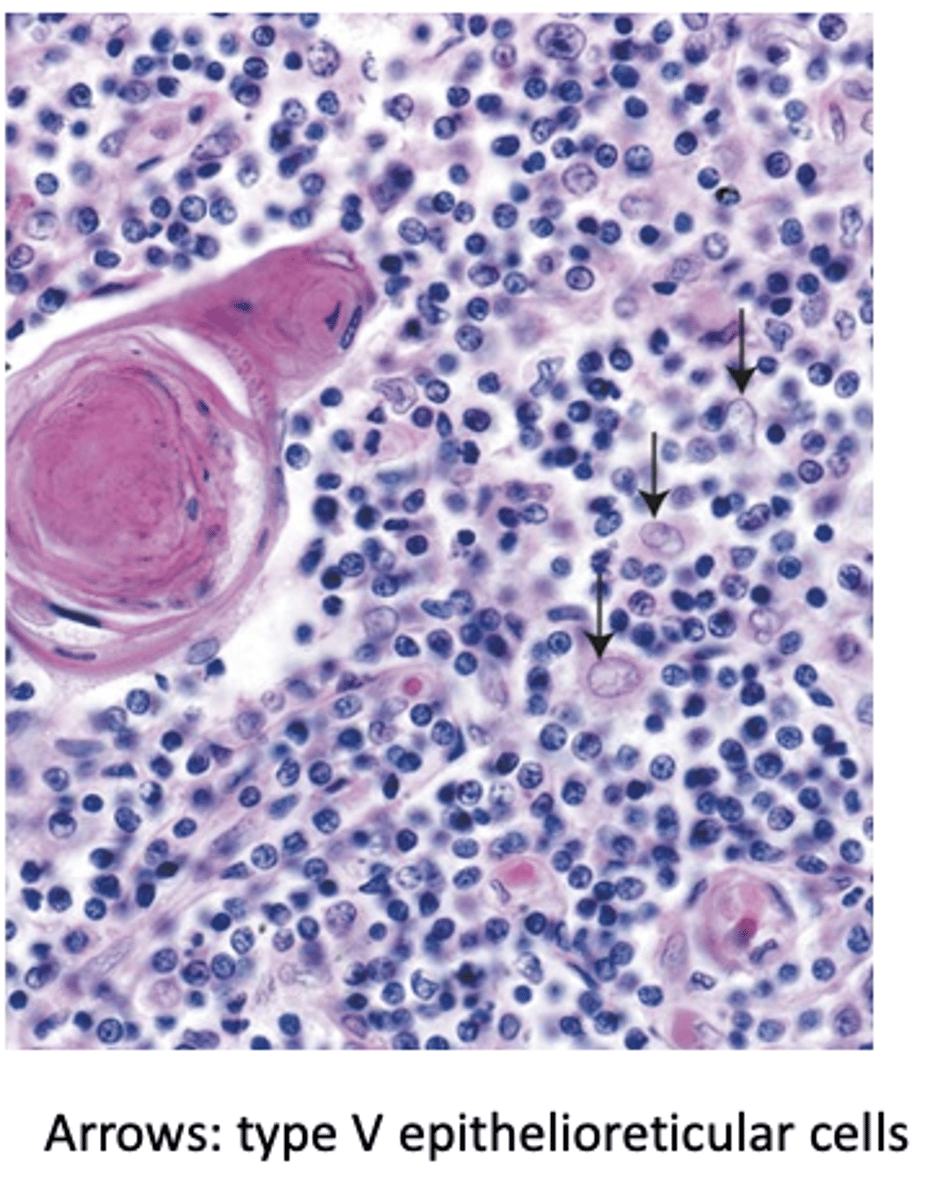
What is the role of Type V epithelioreticular cells in thymic organization?
They compartmentalize groups of lymphocytes.
What structures do Type VI epithelioreticular cells form?
Hassall’s corpuscles
How are Type VI epithelioreticular cells connected to each other?
They are densely packed and joined by desmosomes.
What types of cytoplasmic inclusions are found in Type VI epithelioreticular cells?
Keratohyaline granules, bundles of intermediate filaments, and lipid droplets.
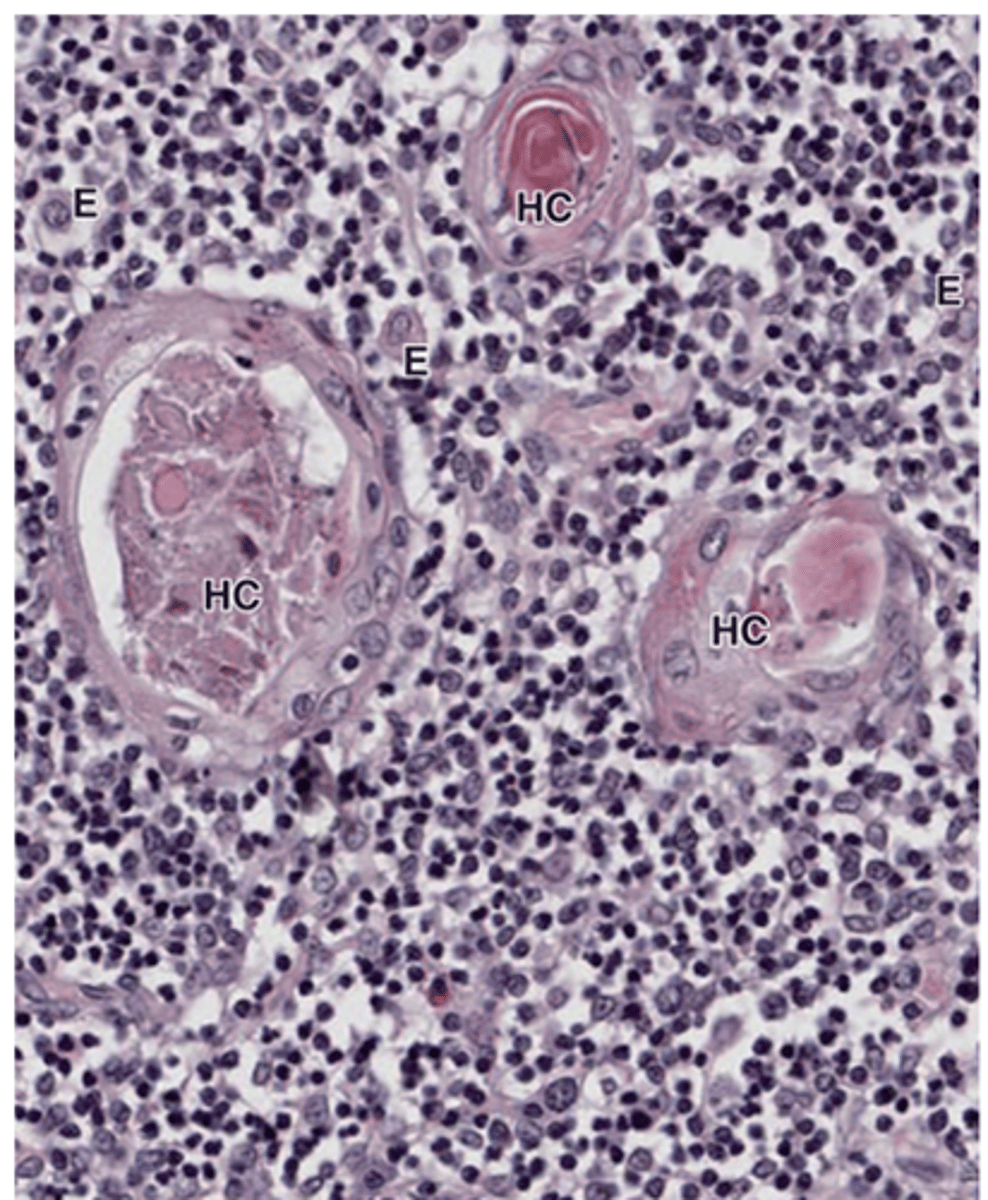
What process occurs at the center of Hassall’s corpuscles?
Central keratinization.
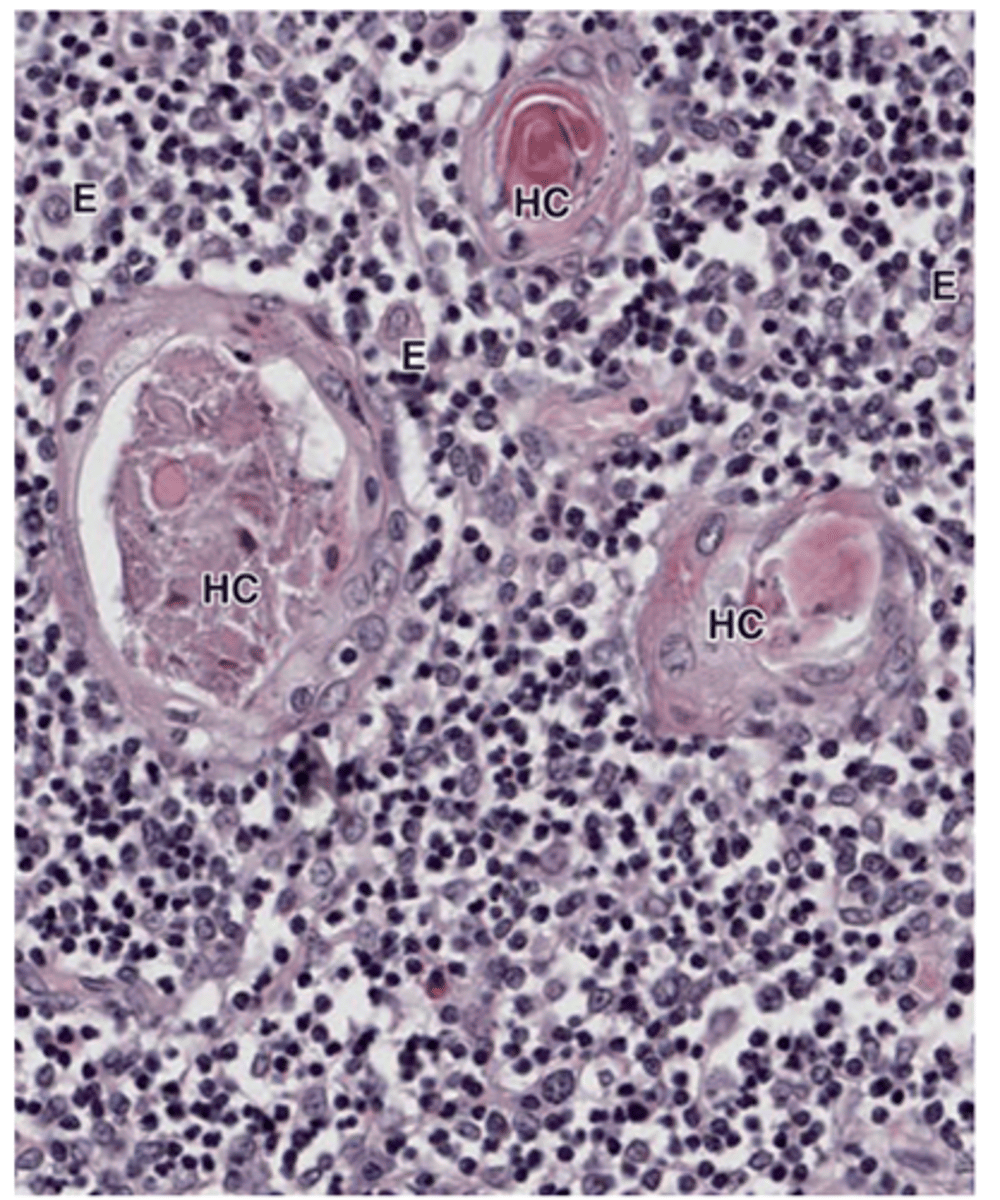
What are the functions of Hassall’s corpuscles?
•Thought to produce interleukins
- Thymic differentiation
- Education of T lymphocytes
- Control of local dendritic cells
- Stimulation of development of regulatory T cells for peripheral tolerance
What is the purpose of positive selection of pre-T cells in the thymic cortex?
It allows survival only of T cells with functional TCRs that can recognize MHC class I and class II molecules.
Where are positive selection of pre-T cells found?
Thymic cortex
What happens when Positive selection of pre-T cells binds to MHC molecule? What happens if it doesn't?
Positive selection of pre-T cell:
- Binds to MHC molecule = Survive and advance to medulla
- DOES NOT bind MHC Molecule = Dies by apoptosis
What is the purpose of negative selection of pre-T cells in the thymic medulla?
It allows survival only of T cells that do not tightly bind self-antigens presented on dendritic cells in the medulla.
What happens when the Negative selection of pre-T cells occurs if they recognize the self-antigen and then they do not?
Recognizes the self antigen: Die by apoptosis
Does NOT recognize the self antigen: Survive and complete maturation
What does MALT stand for and what is it?
MALT stands for Mucosa Associated Lymphoid Tissue, a secondary lymphatic structure in the connective tissue of mucosae.
What types of immune cells are found in MALT connective tissue? (3)
•CT of mucosae with large collection of
1. Lymphocytes (also in the epithelium – intraepithelial lymphocytes)
2. Plasma cells (secrete IgA)
3. APCs
What are examples of lymphoid nodules in MALT?
tonsils, Peyer’s patches, and nodules in the appendix.
Approximately what percentage of the body’s immune cells are in MALT?
About 70% of the body's immune cells are found in MALT.
Which type of lymphocytes are most abundant in MALT?
Most lymphocytes in MALT are B cells, and CD4+ T helper cells are the most abundant T helper cells.
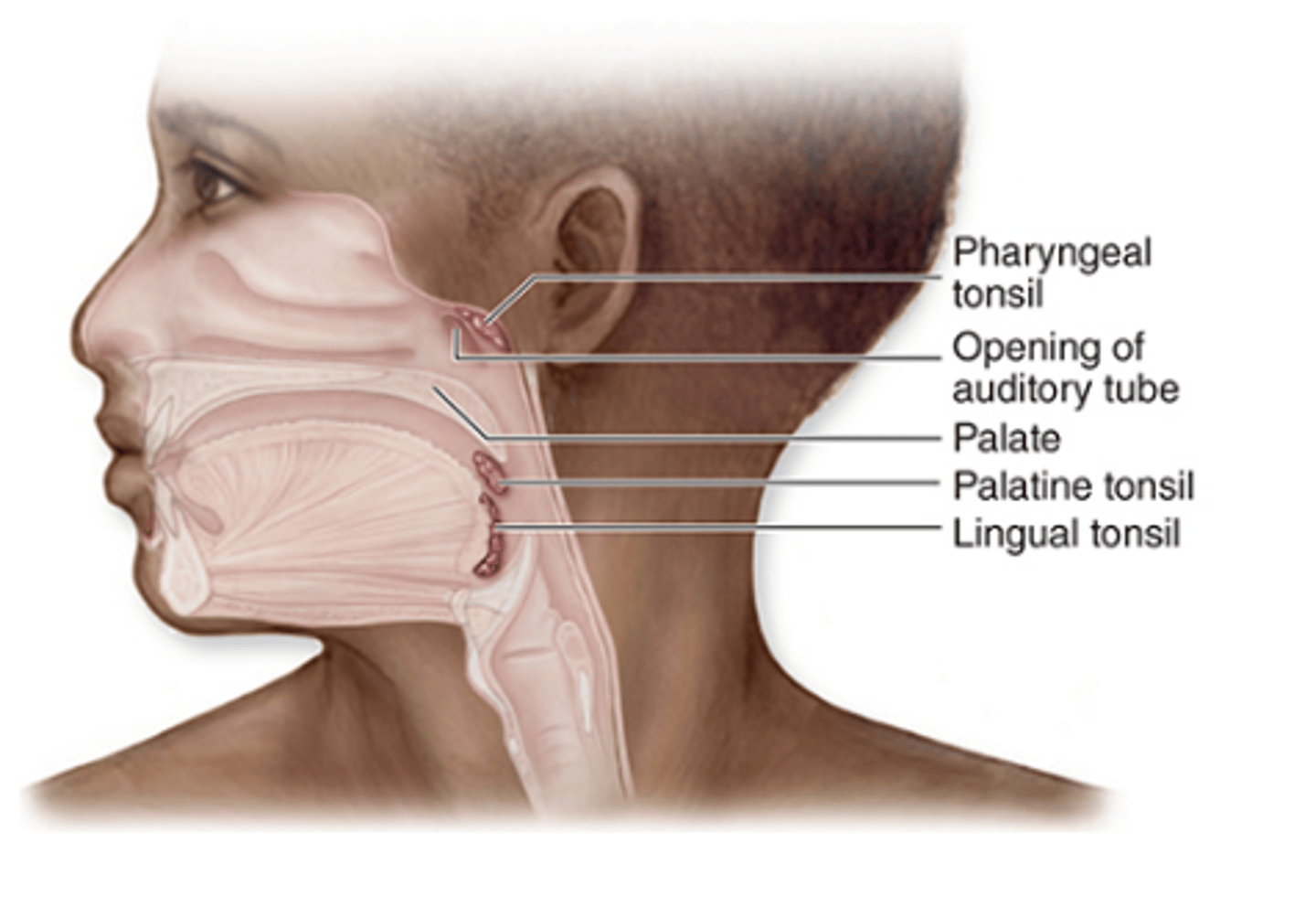
What is nodular MALT in the tonsils?
Nodular MALT in the tonsils consists of irregular masses of lymphoid tissue located in the mucosa of the posterior oral cavity and nasopharynx, closely associated with the epithelial surface.
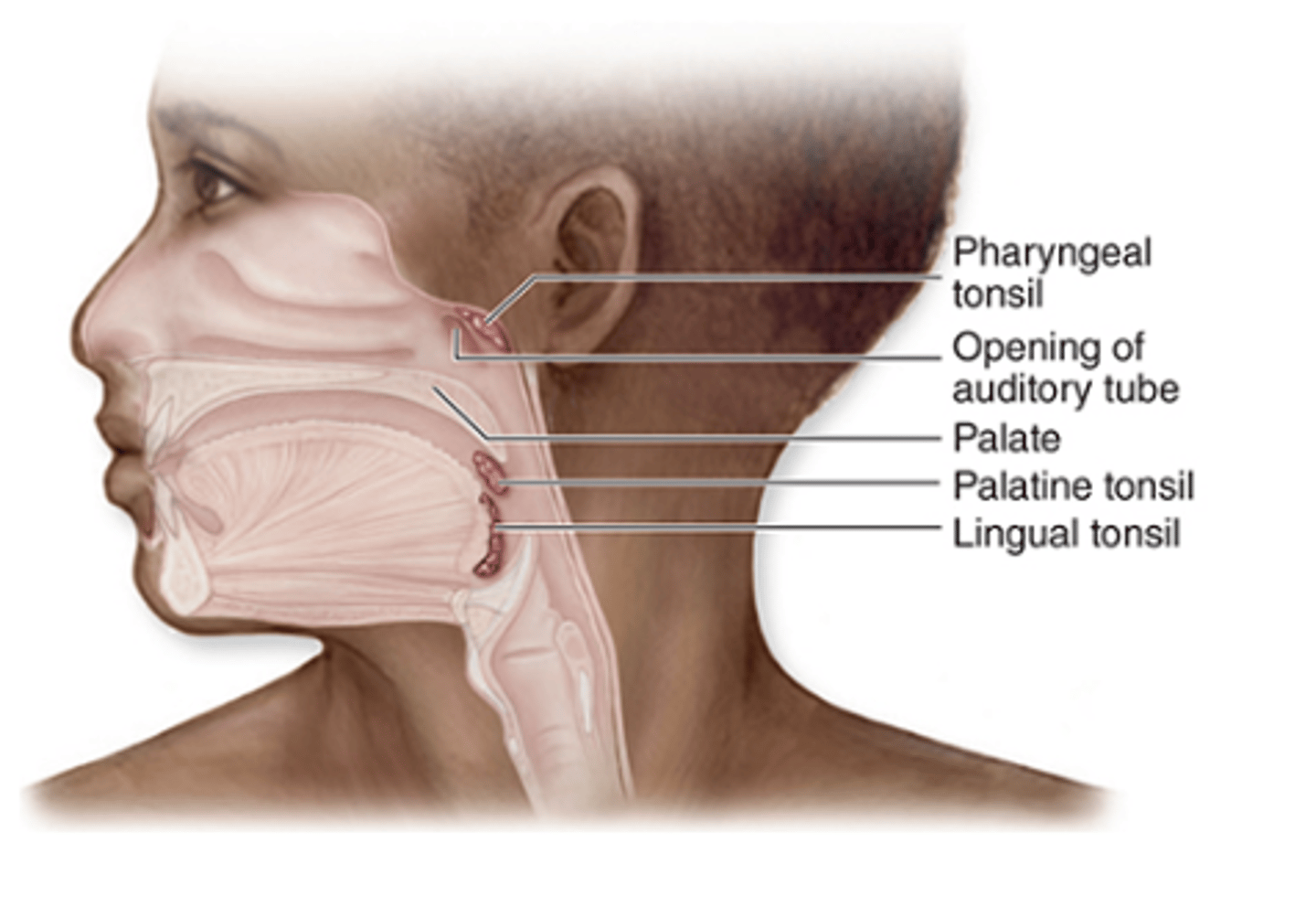
Where is the lymphoid tissue of tonsils located relative to the epithelium?
The lymphoid tissue in tonsils is closely associated with the epithelial surface.
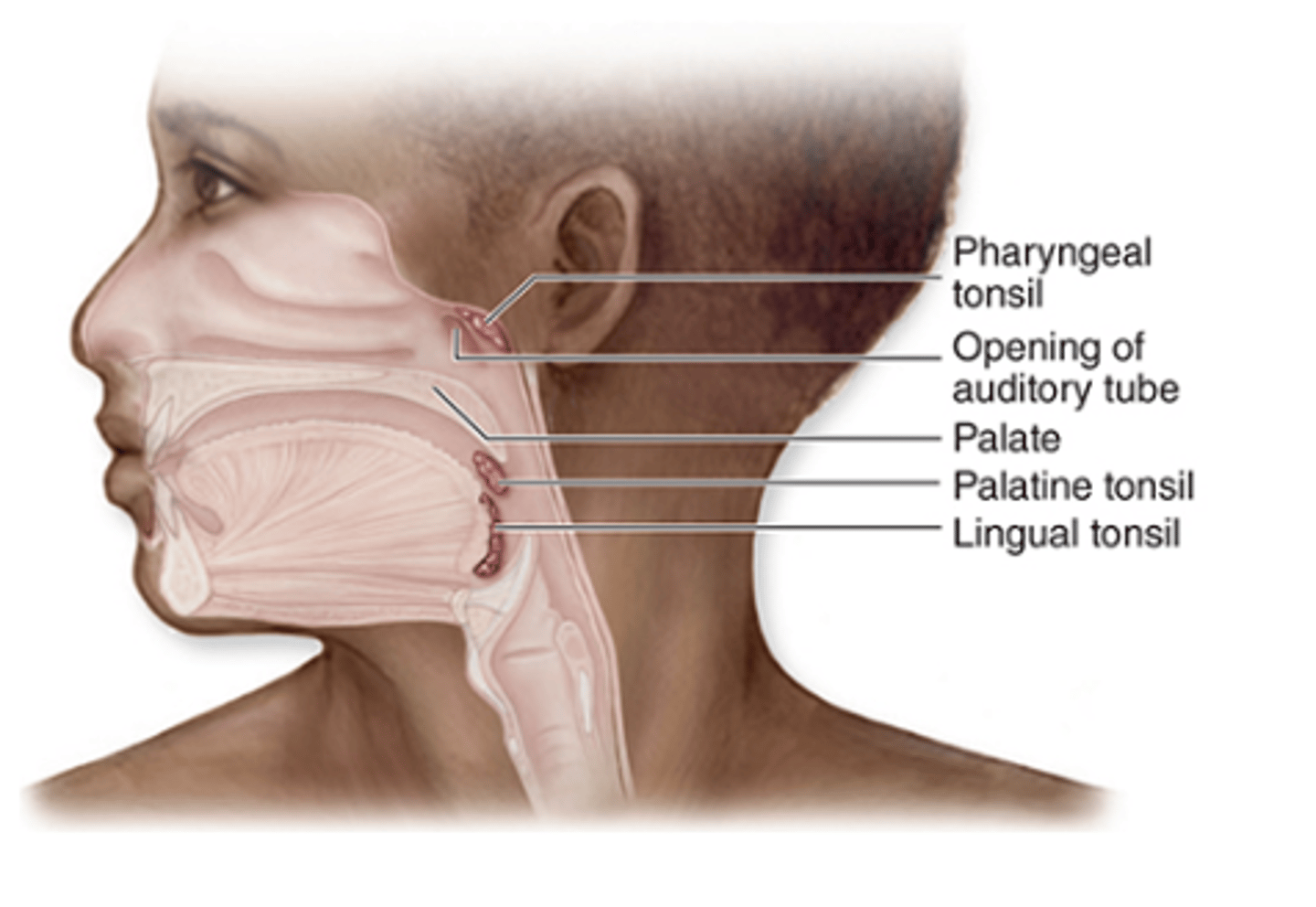
What are the three major types of tonsils?
1. Palatine tonsils (paired)
2. Lingual tonsils (paired)
3. Pharyngeal tonsil (single)
What type of epithelium covers the palatine tonsils?
Stratified squamous epithelium
What are tonsillar crypts and how many do palatine tonsils have?
Tonsillar crypts are deep invaginations of the epithelium; palatine tonsils have 10–20 crypts.
What immune cells are found in the cryptal epithelium of palatine tonsils?
Extensive amounts of lymphocytes and other leukocytes.
Describe the lymphoid tissue structure in palatine tonsils.
- Diffuse lymphocytes
- Abundant secondary lymphoid nodules around the crypts
How do lingual tonsils compare to palatine tonsils?
Lingual tonsils are similar to palatine tonsils but lack distinct capsules.
What type of epithelium covers the pharyngeal tonsil?
Respiratory epithelium
Describe the capsule and invaginations of the pharyngeal tonsil.
It has a thin underlying capsule and invaginations but lacks true crypts.
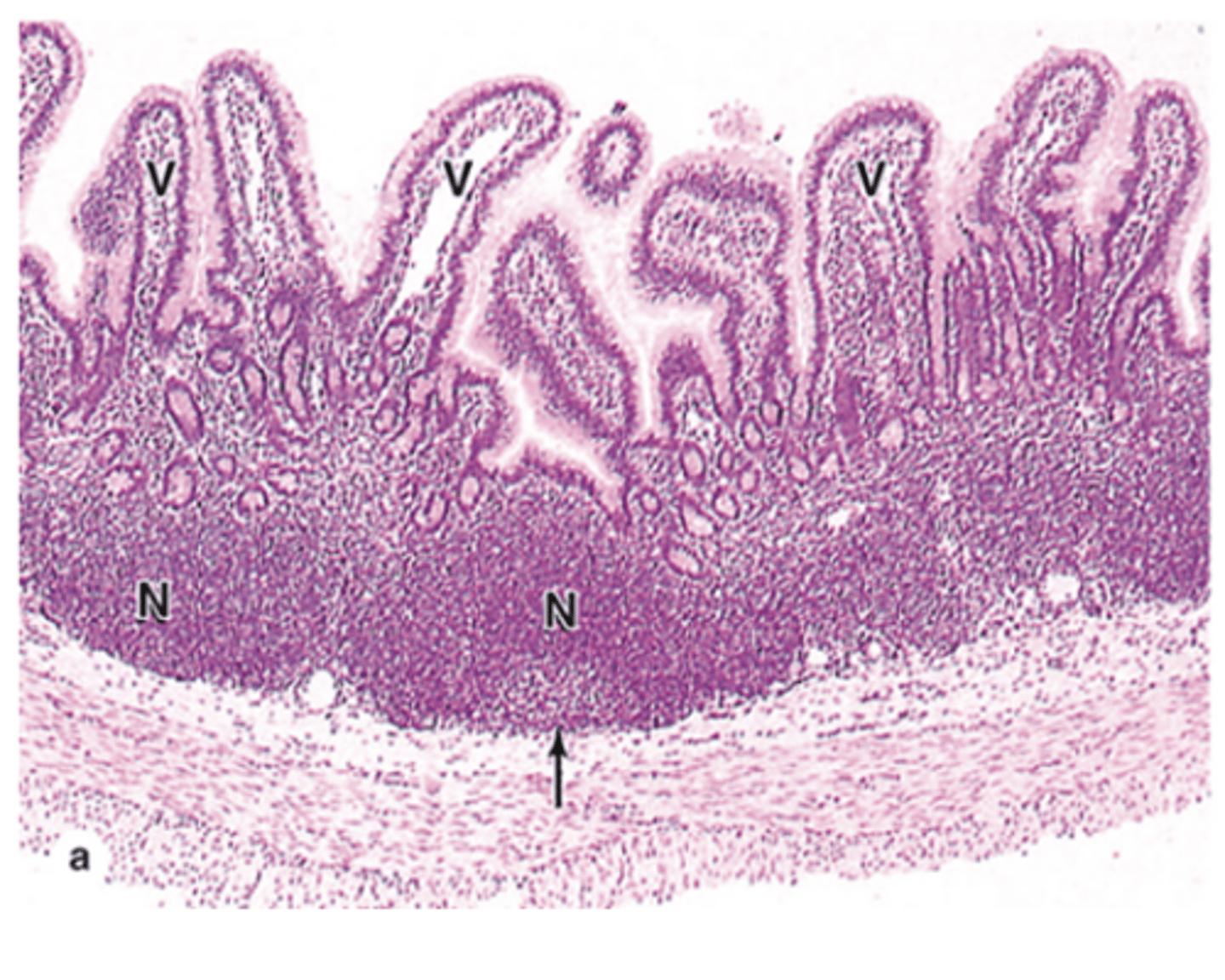
Where are Peyer’s patches located?
in the mucosa and submucosa of the ileum.
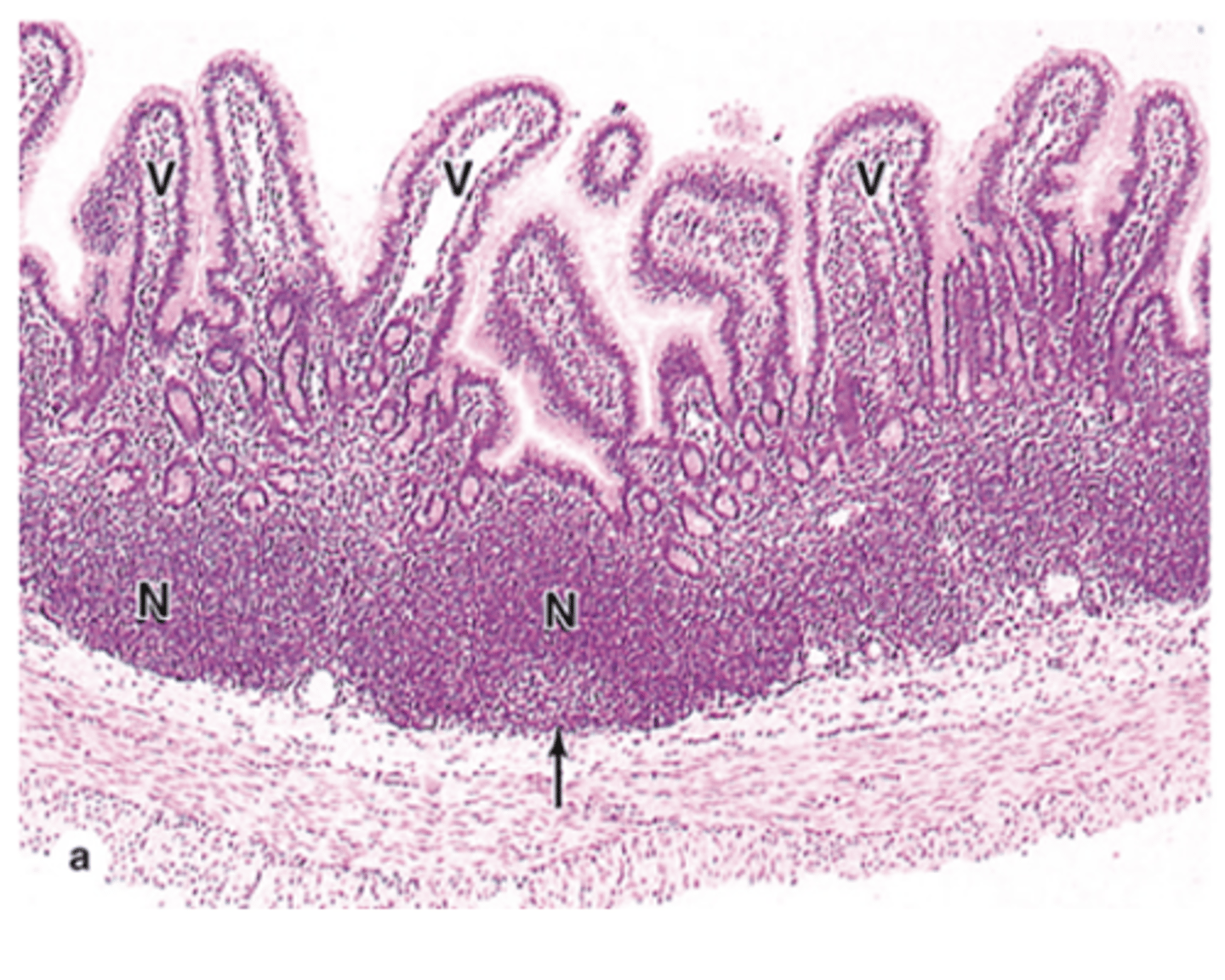
How many nodules do Peyer’s patches typically contain?
They contain about a dozen nodules.
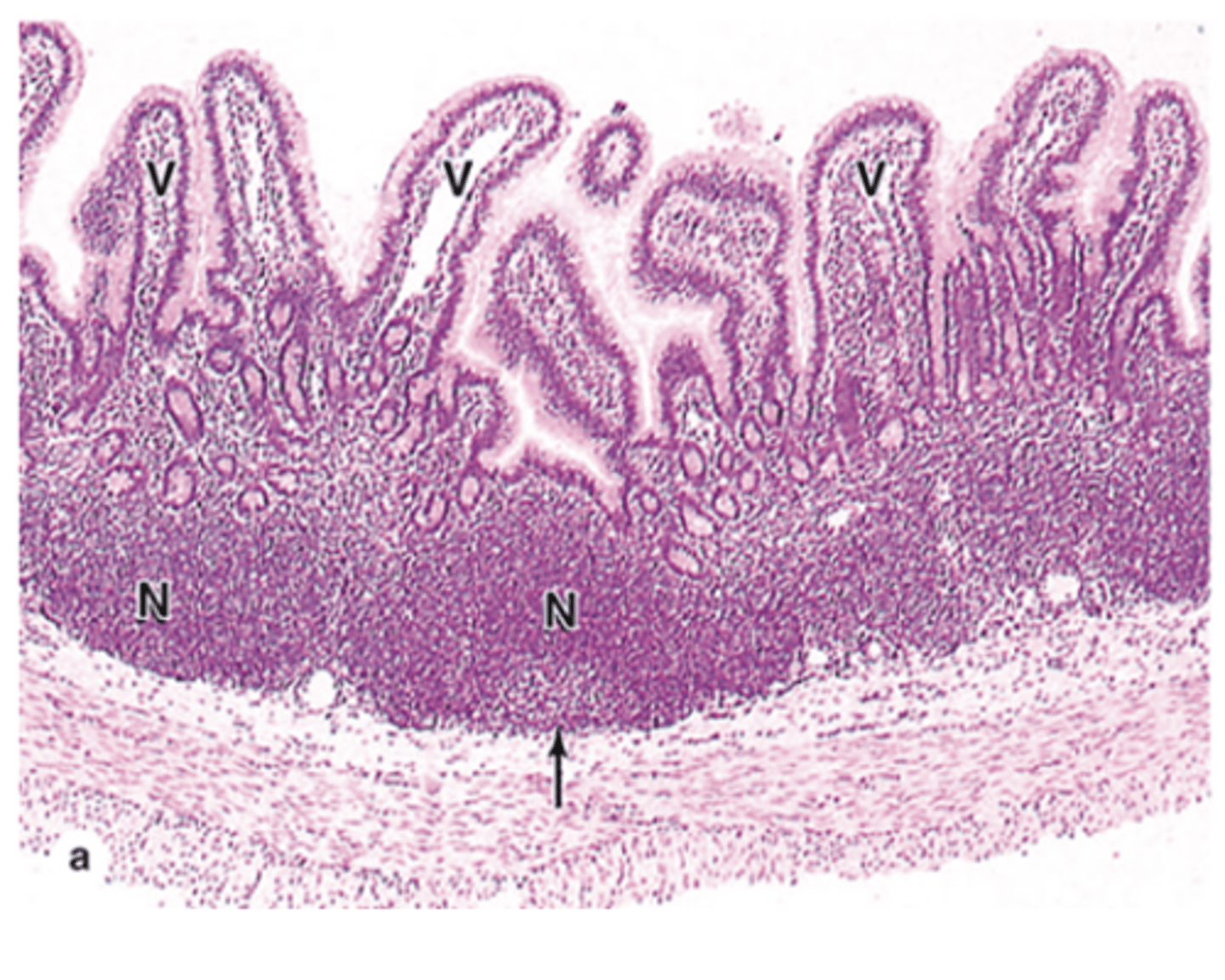
Do Peyer’s patches have a connective tissue capsule?
No, they lack a connective tissue capsule.
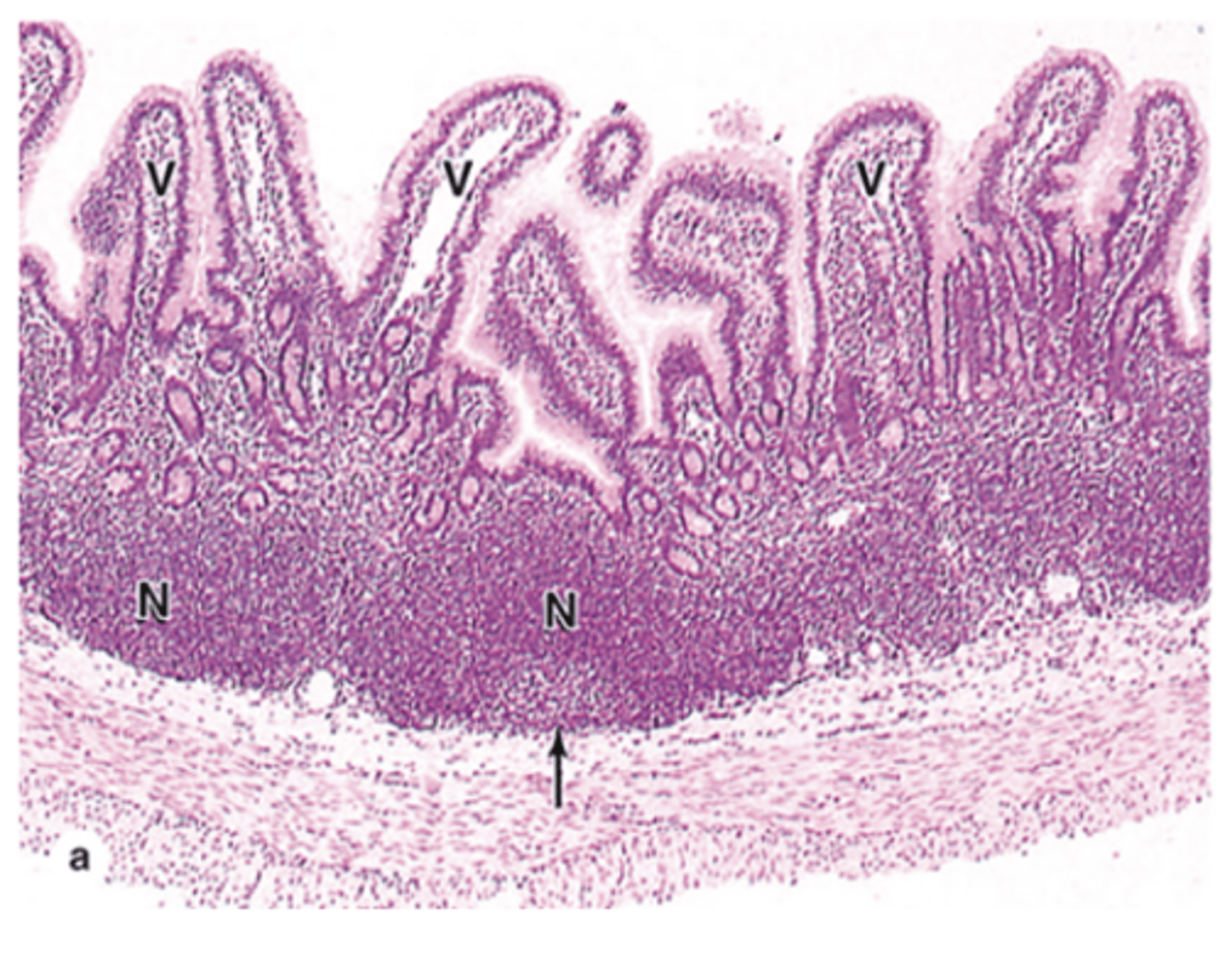
What type of epithelium covers Peyer’s patches?
Simple columnar epithelium, which is the lining of the gut.
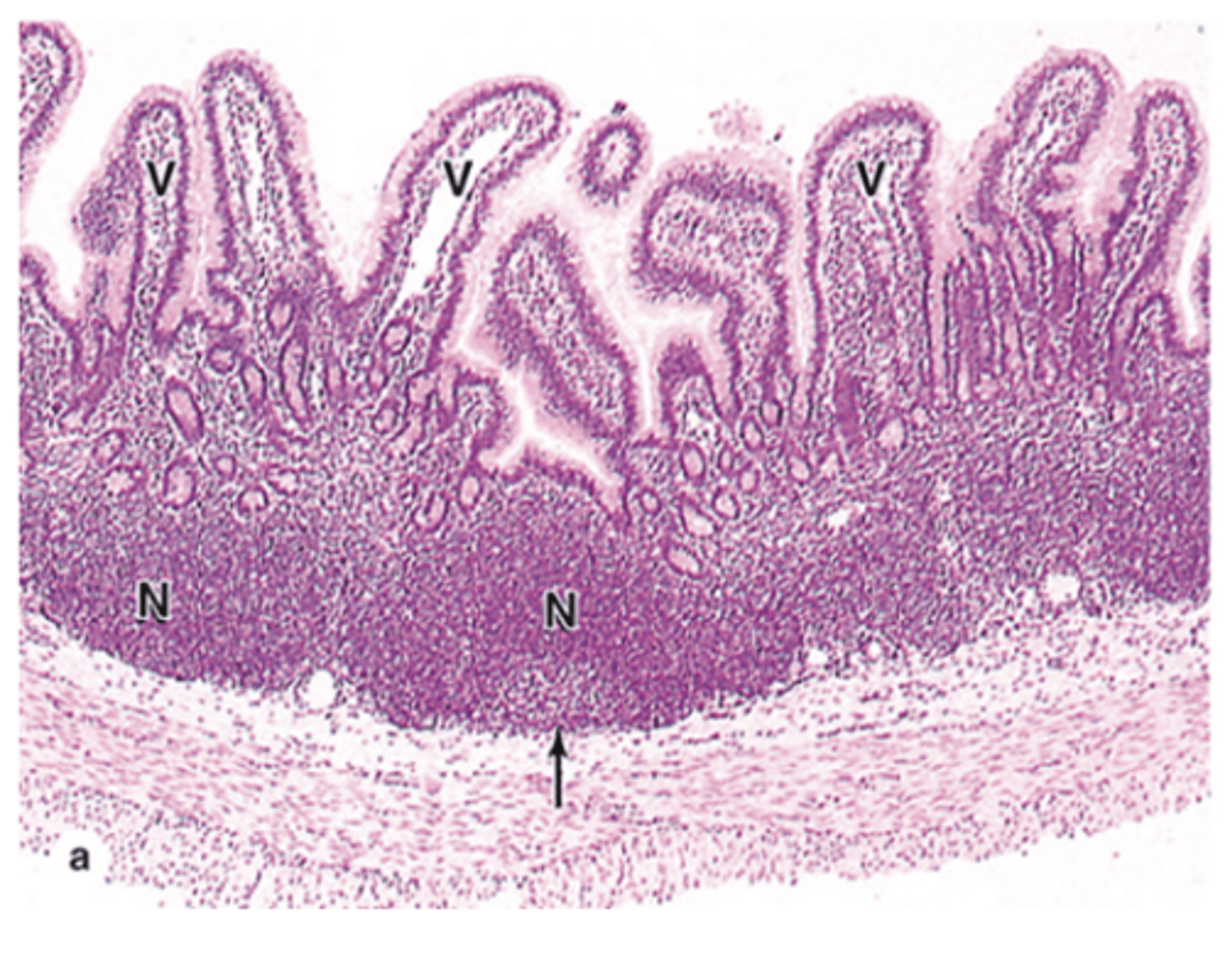
Besides columnar cells, what special epithelial cells are found in Peyer’s patches?
M cells (microfold cells).
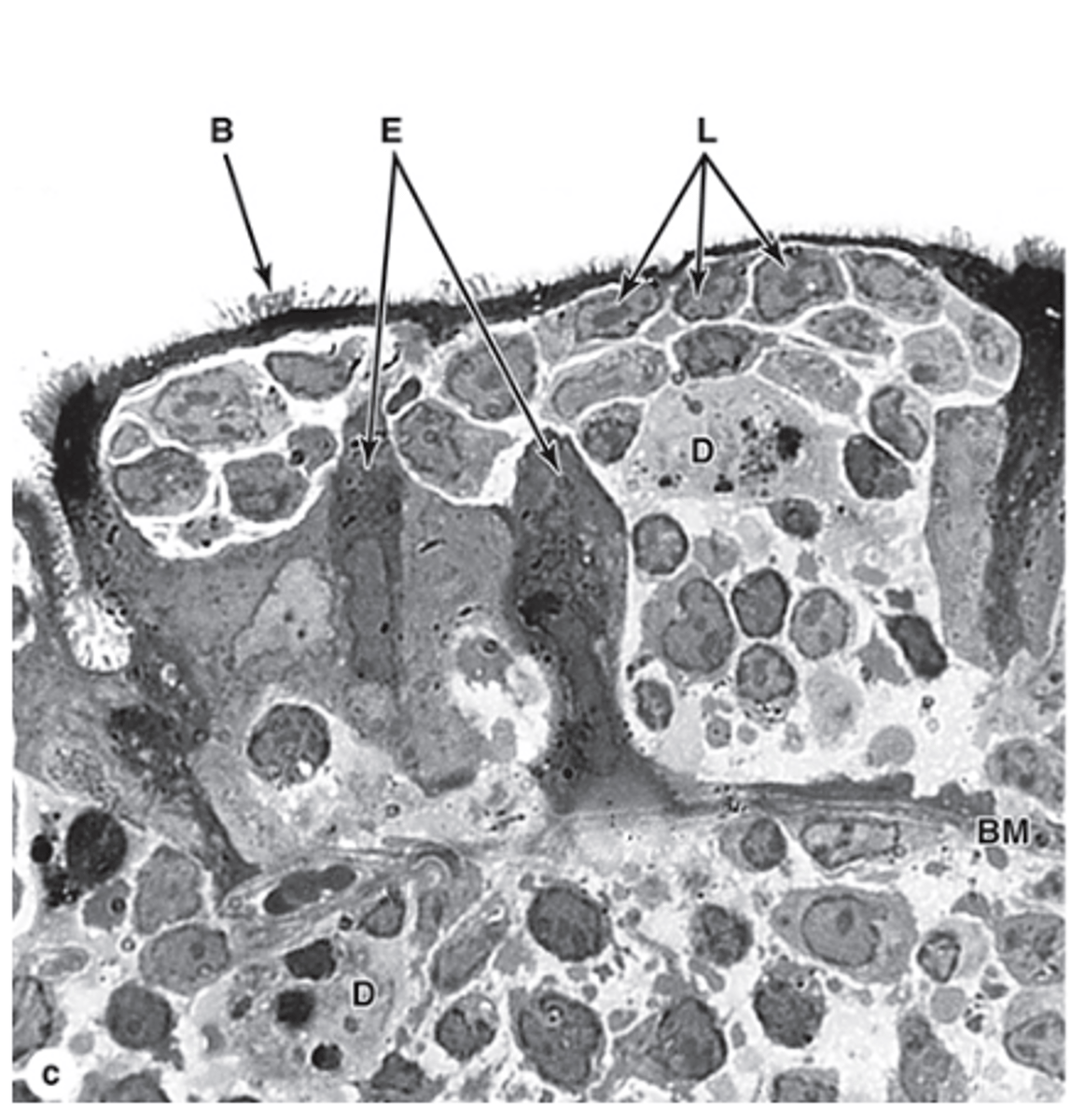
What are M cells in Peyer’s patches?
M cells are special epithelial cells in Peyer’s patches with apical microfolds instead of a brush border.
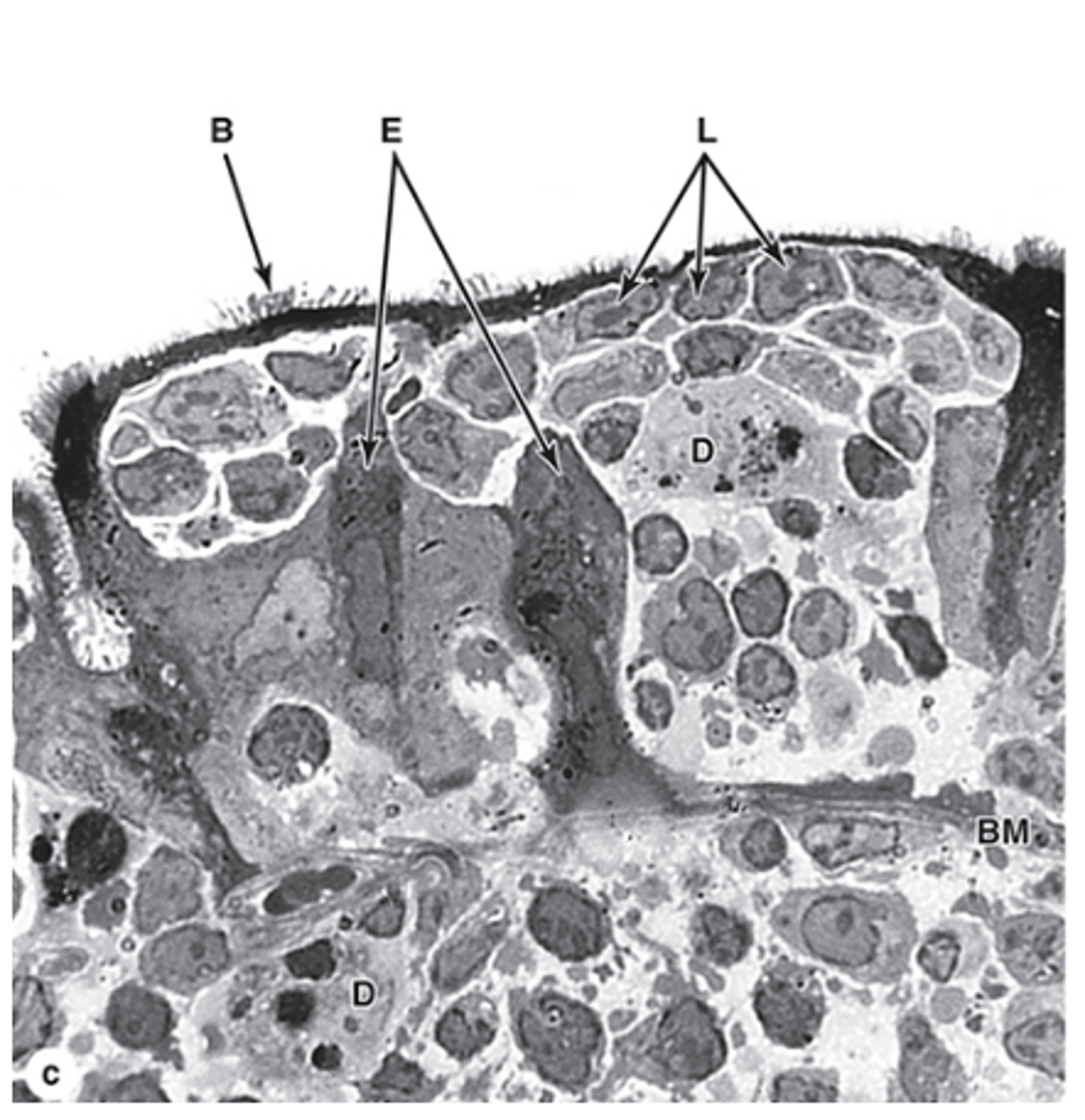
What is the main function of M cells?
They sample antigens on the luminal surface of the ileum and transfer them to lymphocytes and dendritic cells.