Biol 204 exam 3 lecture 1
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
82 Terms
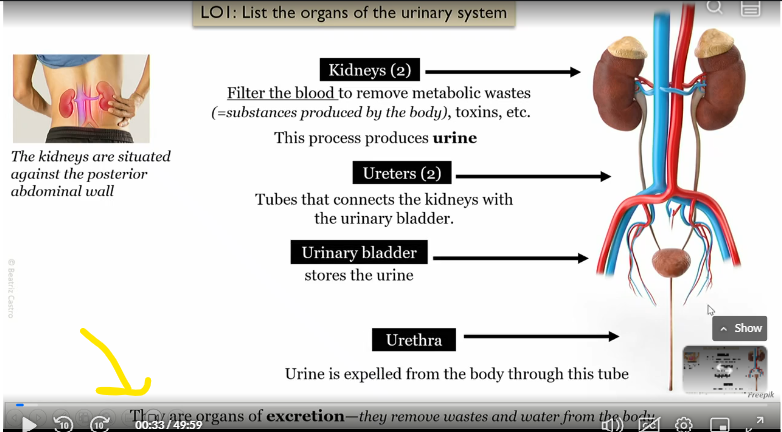
kidneys
filter the blood to remove metabolic wastes, toxins etc
This process produces urine
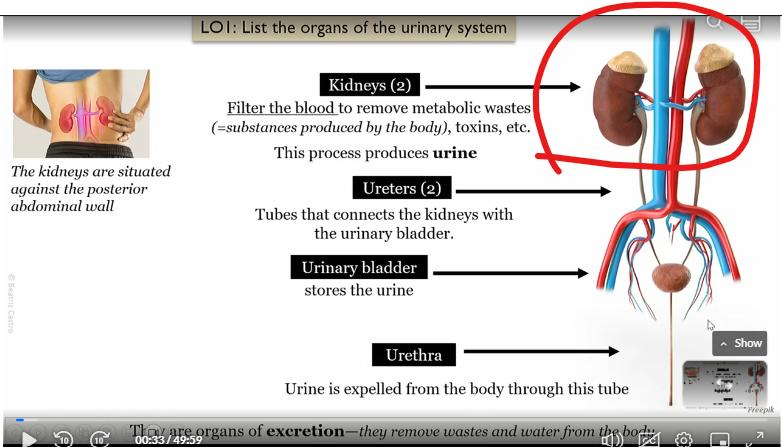
Uterer
Tubes that connect kidneys to bladder
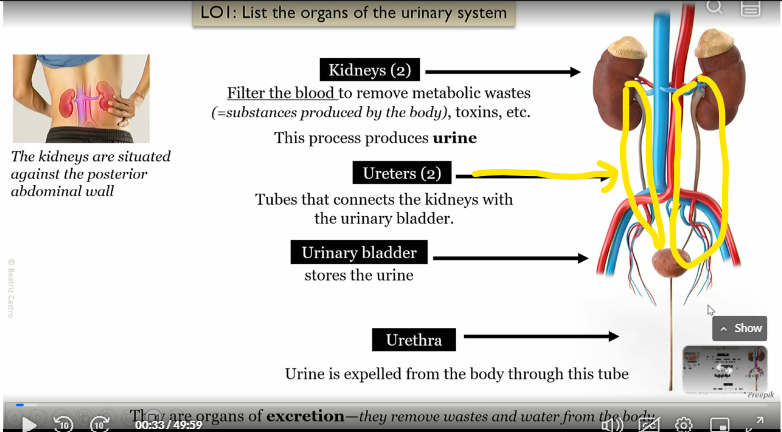
urinary bladder
connected to the kidneys via the uterer, stores the urine
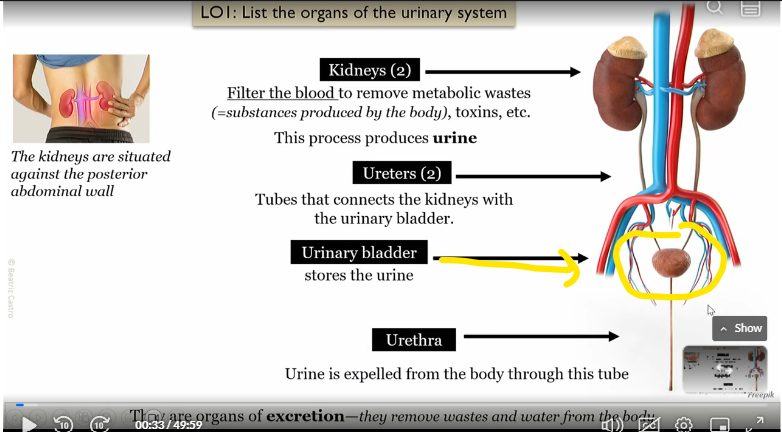
urethera
connected to urinary bladder, urine is expelled from the body to the tube
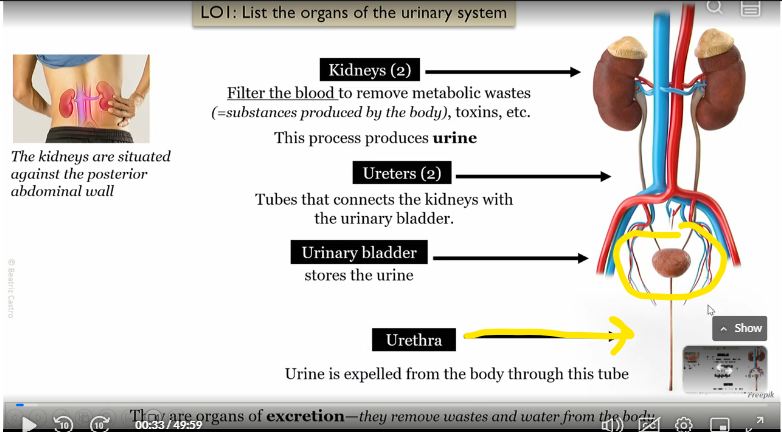
what type of organs are the kidney, uterer, bladder, and urethera?
organs of excretion, which remove wastes and water from the body
Where are the kidneys situated?
Against the posterior abdominal wall
What does the kidney excrete
urea, creatine, and uric acid
c urea c uri (nitrogenous waste)
and ingested toxins
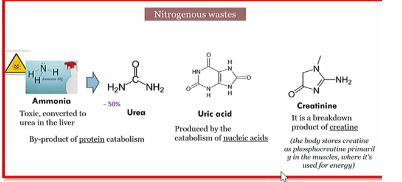
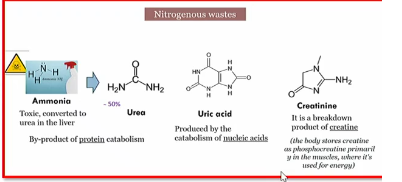
Nitrogenous waste
urea, creatine, and uric acid
c urea c uri (Korea Curry)
excreted by kidney
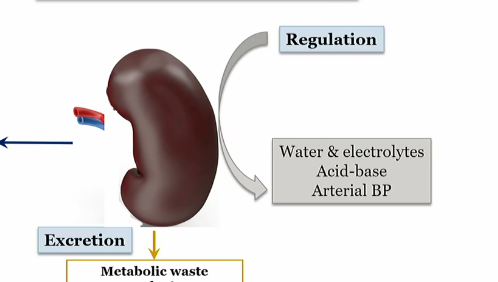
what does the kidney Regulate
Water and electrolytes
Acid base
arterial BP
WAR (waghhh)
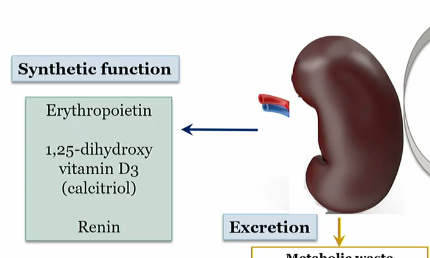
What does the kidney produce in its syntheic function
erythopoietin
1-25 dihydroxy vitamin D3 (calcitriol)
renin
4-evr
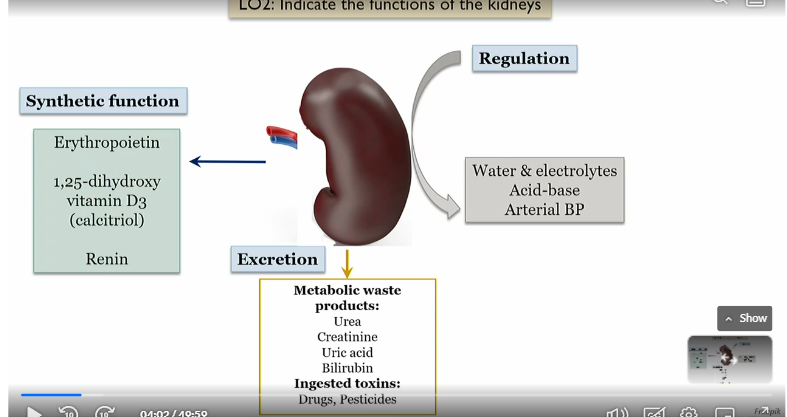
Functions of the kidneys
Regulation, excretion, synthetic function
Where are nephrons
within the renal pyramids in the medulla and in the cortex depending on type
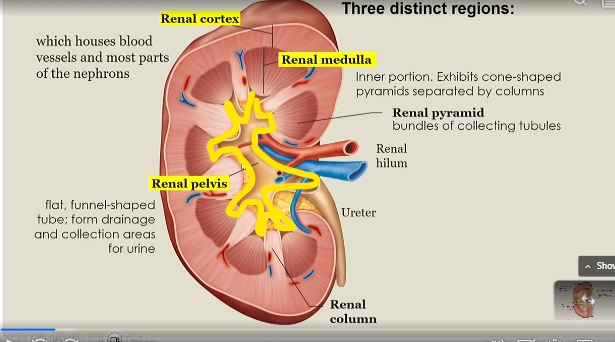
renal cortex
houses blood vessels and most parts of the nephrons
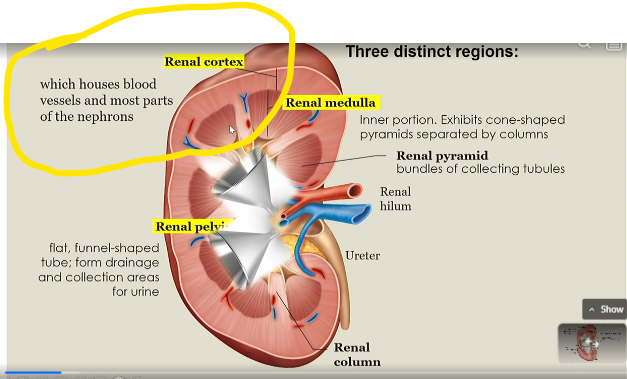
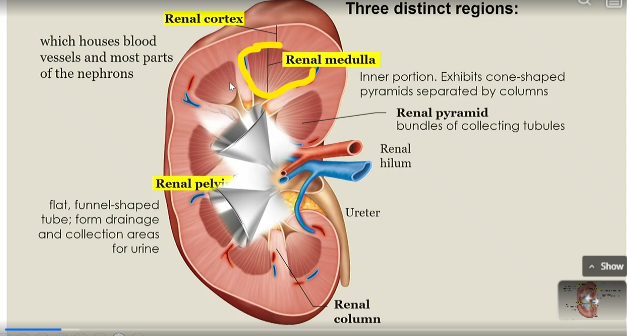
renal medulla
inner portion of kidney that exhibits cone shaped pyramids seperated by columns
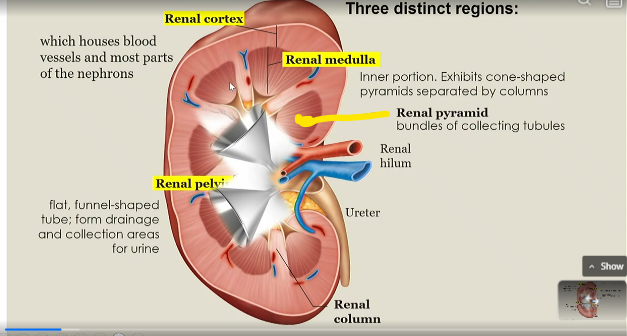
renal pyramid
bundles of collecting tubules
Renal column
seperates renal medullas
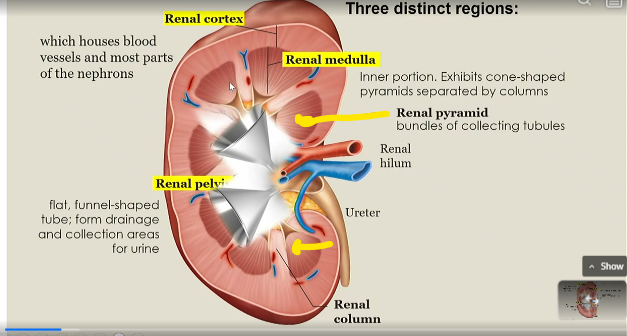
Renal pelvis
flat, funnel shaped tube that forms drainage and collection areas for urine
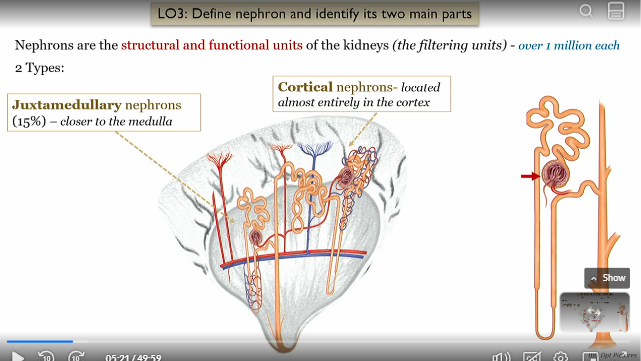
What are nephrons
the structural and functional units of the kidneys (filtering units)
can be juxtamedullary or cortical
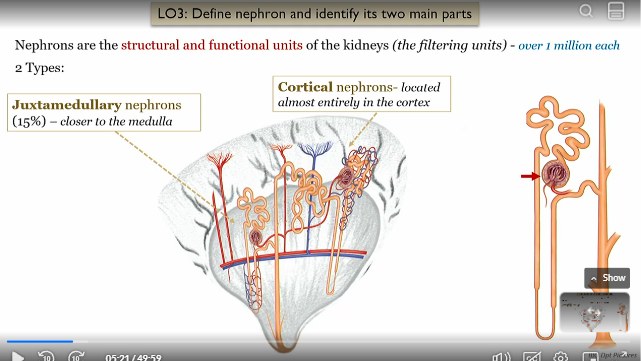
How much nephrons are there
1 million per kidney
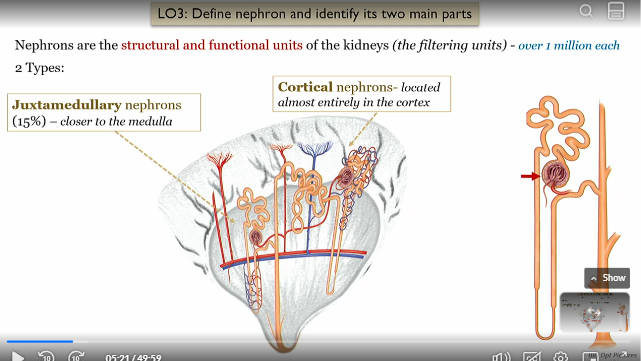
Cortical nephrons location
located almost entirely in the renal cortex
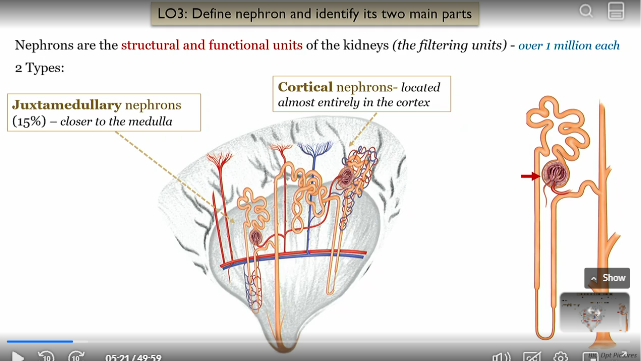
Juxtamedullary nephrons location
15% located closer to the renal medulla
Nephron anatomy
Renal corpuscle (filters the blood)
renal tubule (converts the filtrate to urine)
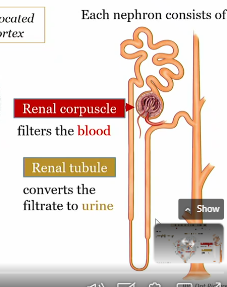
renal corpuscle purpose
part of nephron that filters the blood
renal tubule purpose
part of nephron that converts filtrate from the renal corpuscle into urine
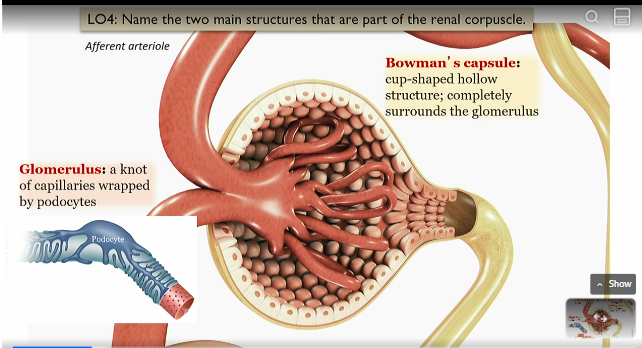
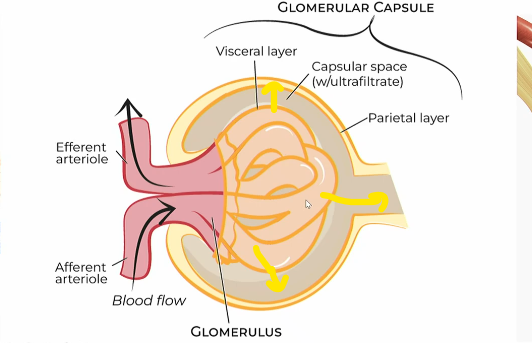
Bowman’s capsule
cup shaped hollow structure that surrounds the glommerulus
outer part of the renal corpuscle
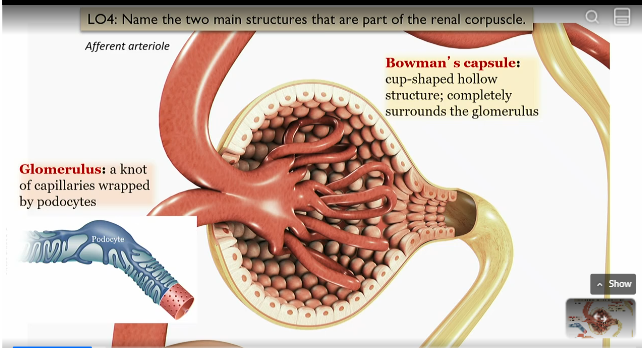
Glommerulus
part of renal corpuscle surrounded by bowmans capsule
knot of capillaries wrapped by podocytes
Layers of bowman’s capsule
parietal layer
capsular space with ultrafiltrate
visceral layer
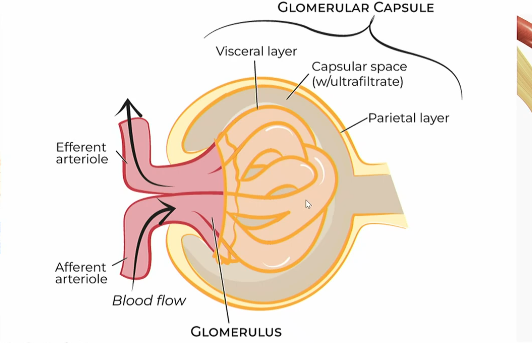
visceral layer of bowmans capsule
the podocytes that wrap around the glomerulus capillaries
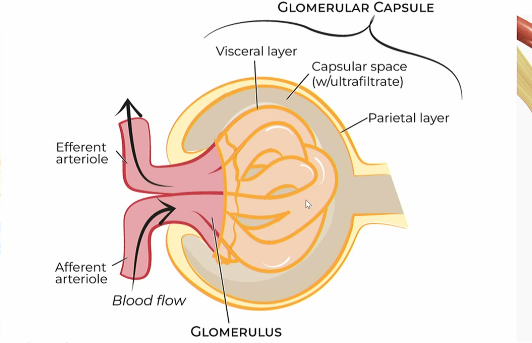
Flow of blood filtration in bowman’s capsule
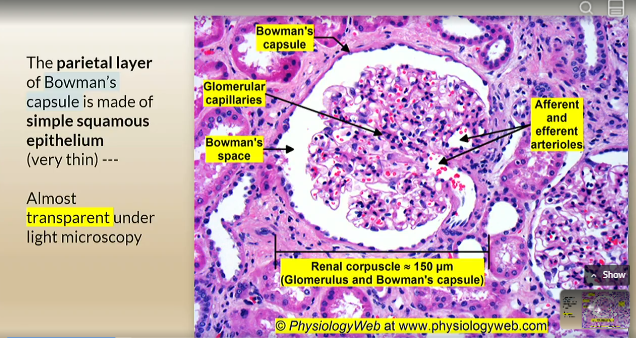
what is the parietal layer of bown’s capsule made of
simple squamous epithelium
Glomerrular filtration
process of which water and some solutes in the blood plasma pass from the capillaries of the glomerulus into the capsular space of the nephron
Afferent atriole
Brings blood to the glommerulus capillaries in the renal corpuscle
efferent atriole
carries away blood from the glommerulus capillaries in the renal corpuscle
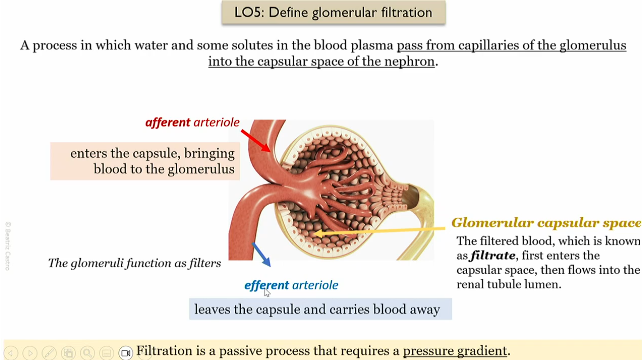
Glommerular filtration process
afferent atriole brings in blood to the glommerulus in the renal capsule
Filtered blood enters the capsular space, which then enters the renal lumen of the nephron
The efferent atriole takes the blood away from the glomeerulus
Passive process that requires a pressure gradient to work
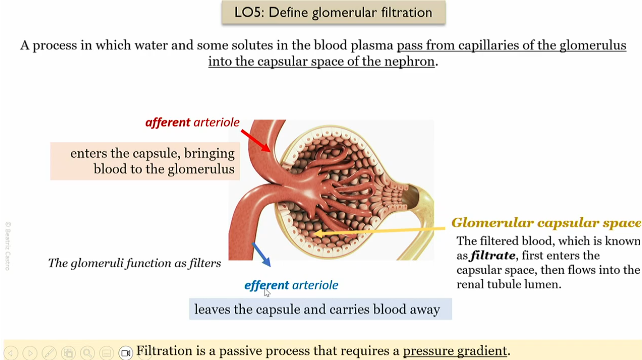

false, glomerulus blood flow gees
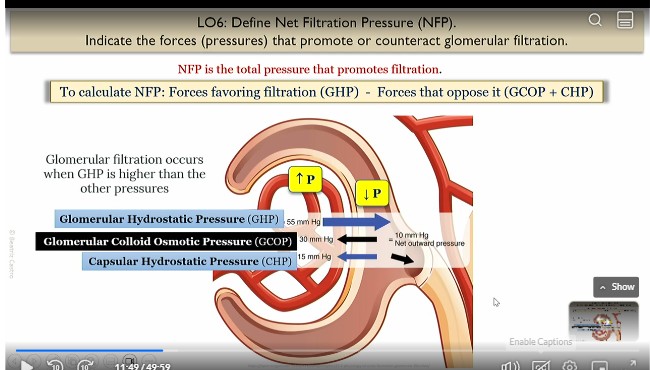
Net filtration pressure
total pressure that promotes filtration
NFP = favors that favor filtration (GHP) - forces that oppose it (GCOP + CHP)
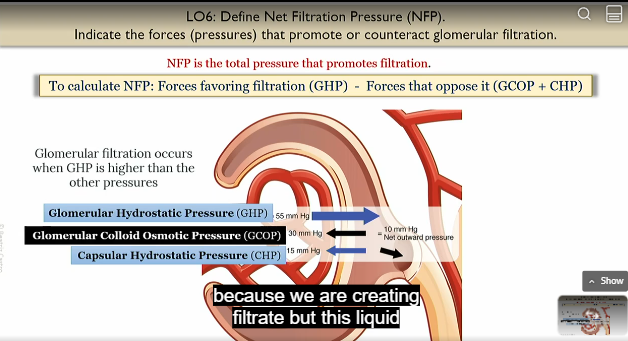
GHP
Glomerullar hydrostatic pressure
pressure in glomerulus wanting to come out
favors filtration
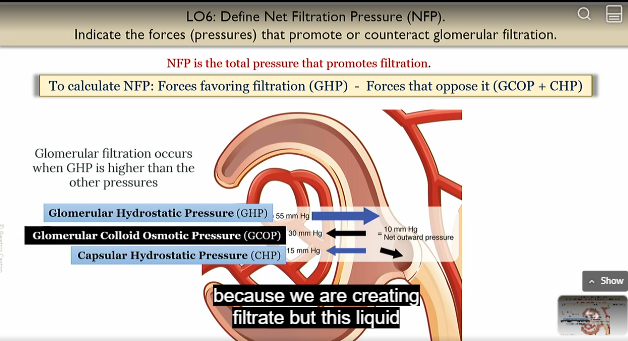
GCOP
glommerular collloid osmotic pressure
due to proteins like albumins bringing in water
unfavorable to filtration
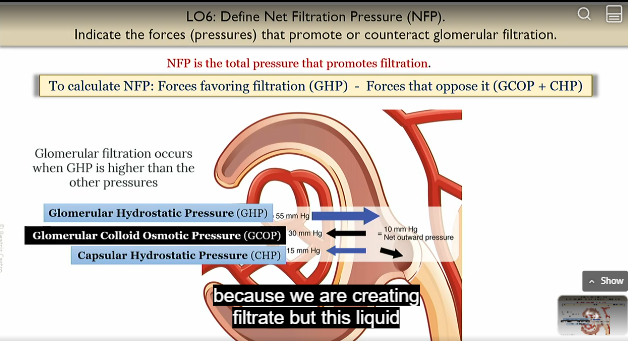
CHP
capsular hysrostatic pressure
due to capsular space of bowman’s capsule accumulating with liquid and opposing flow
unfavorable to filtration
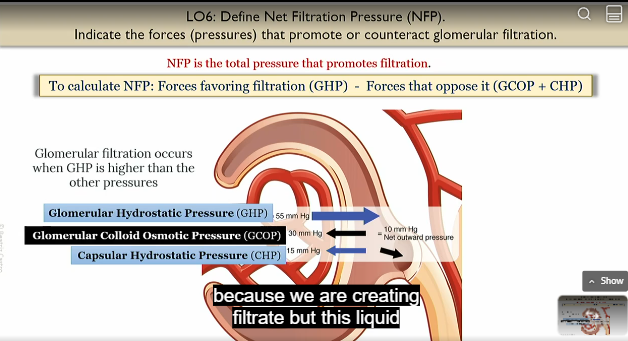
In order for filtration to happen, what do the pressures in the renal corpuscle need to be?
Glomerulus needs to be higher
Bowmans capsule capuslar space needs to be lower
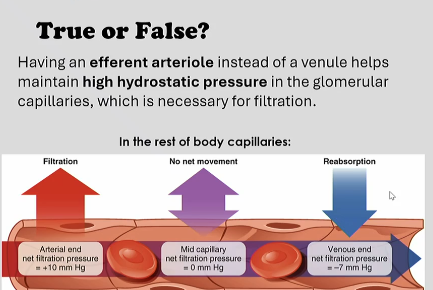
true, venules have lower pressure
Why is it that the glommerulus uses two atrioles betwen as opposed to the ususal flow of one atriole to capilaries to venule?
Arterioles can constrict and dialate
For example, if you constrict the efferent atriole (moves blood away)
Pressure in the glomerulus goes up, and filtration goes up
For example, if you dialate the efferent atriole (moves blood away)
Pressure in the glomerulus goes down, and filtration goes down
The venules just hold the blood, lots of pressure, lots of room

Basement membrane of the glomerulus
middle layer
consists of proteoglycan gel, prevents filtration of large proteins
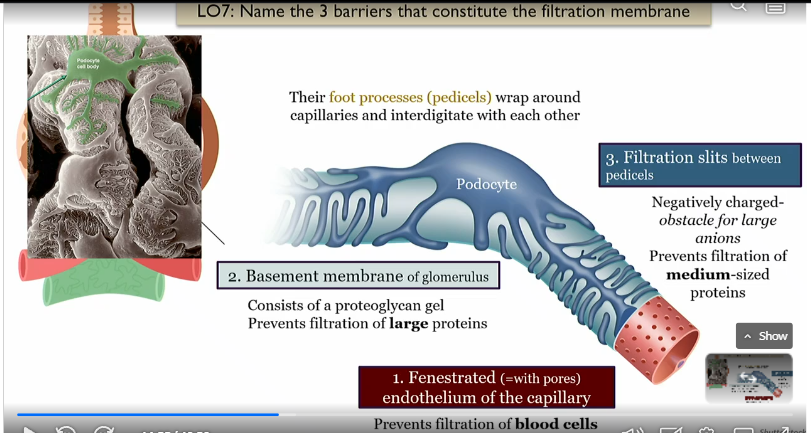
Fenestrated endothelium of the capillary
prevents filtration of blood cells, innrmost layer of glommerulus
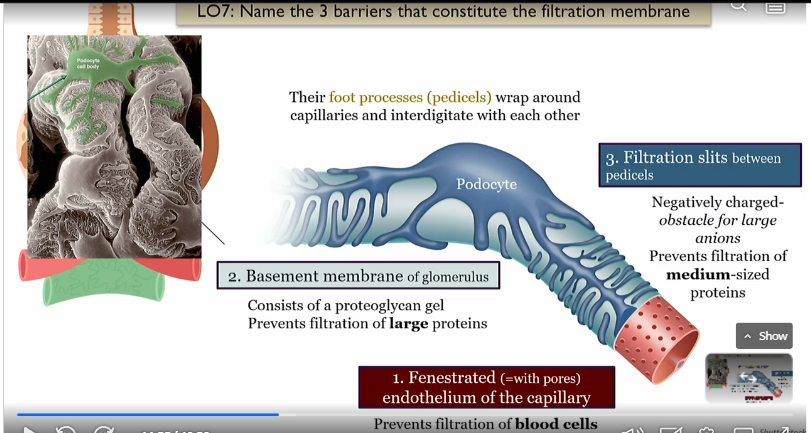
Filtration slits between pedicels
outermost barrier to filtration which is a negativley charged obstacle for large Anions, and prevents filtration of medium sized proteins
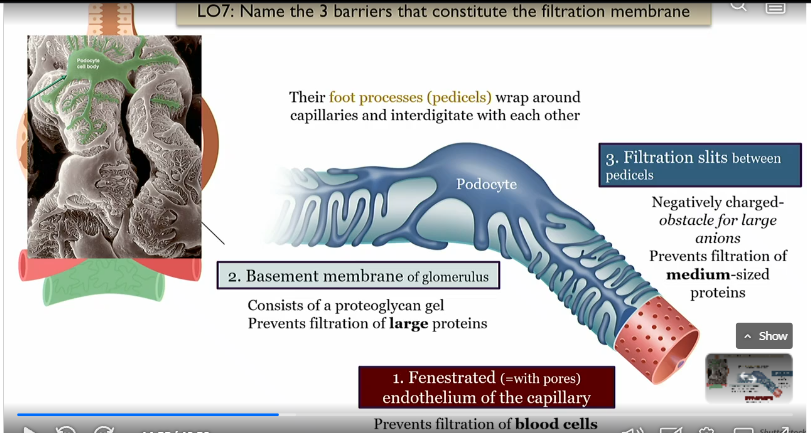
Barriers to filtration in glommerulus
fenestrated endothelium in the capillary
basement membrane
filtration slits between pedicels
prevents blood cells 2. prevents large proteins 3. prevents anions and proteins due to negative charge
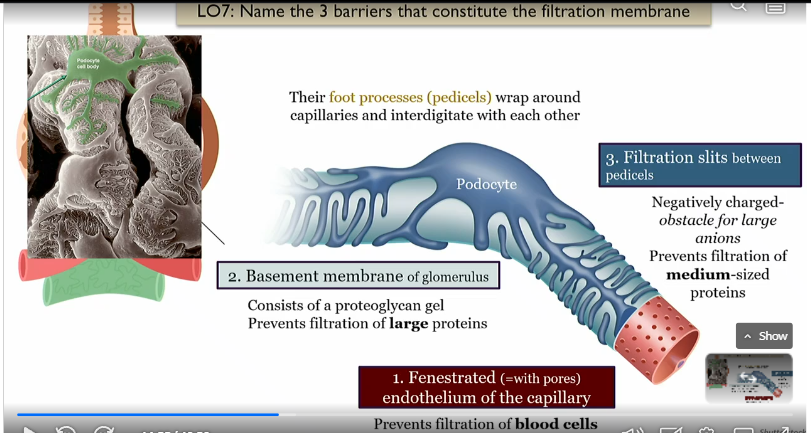
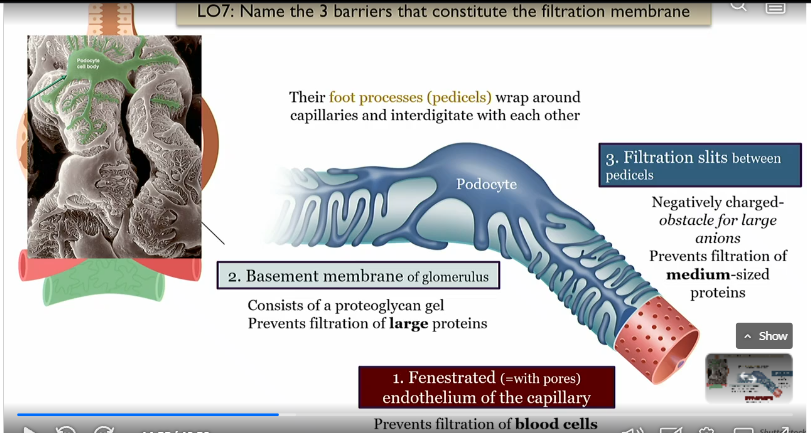
Pedicels
foot processes of podocytes that wrap around capillaries and interdigitate with each other
Filtration slit
narrow gap between two pediciels that is covered by a thin structure called the slit diaphragm, made of proteins
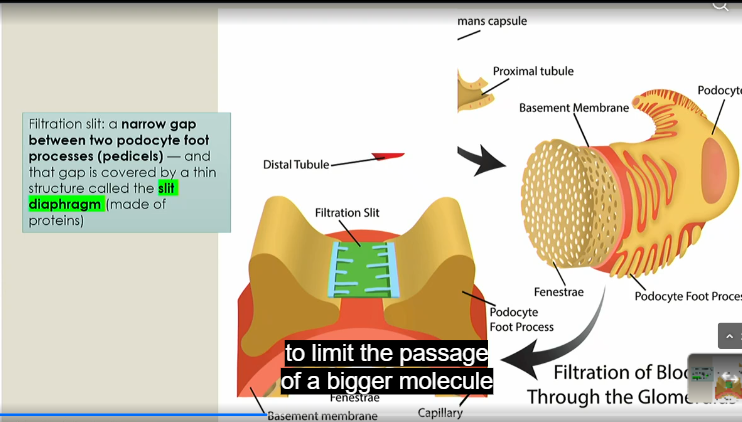
What can pass the filtration membrane in the glommerulus?
less than 3 nm, smaller than protiens
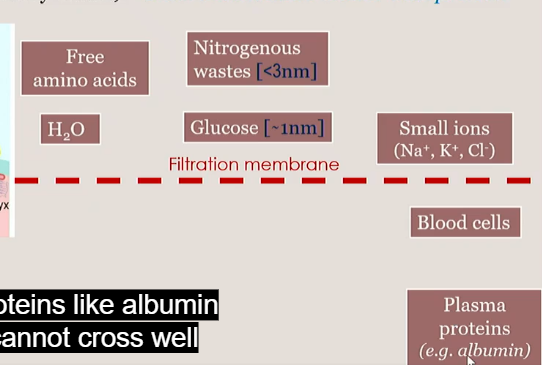
Glommerular filtration rate
ampunt of filtrate created by renal corpuscle per minute

Male glommerullar filtration rate
125 mL/min (180 L/day)
Female glommerullar filtration rate
105 mL/min (150 L/day)
What is a Glomerullar filtration rate of less than 60 indicative of
kindey disease or failure

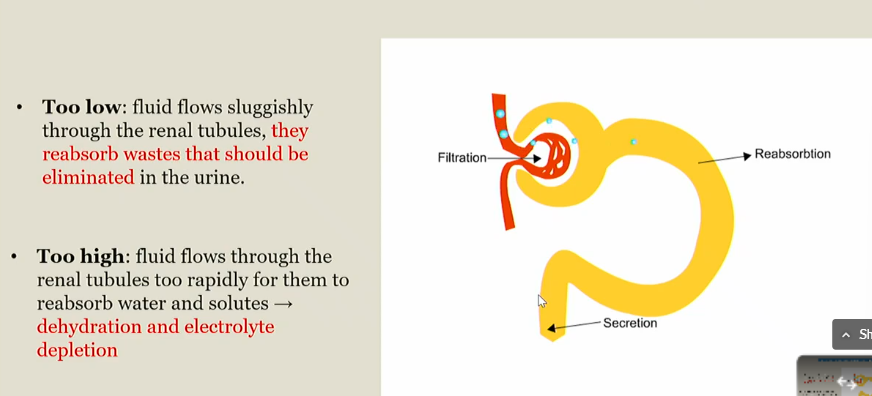
Too low Glomerullar filtration rate
Fluid flows sluggishly through the renal tubules, and they reabsorb wastes that should be eliminated in the urine
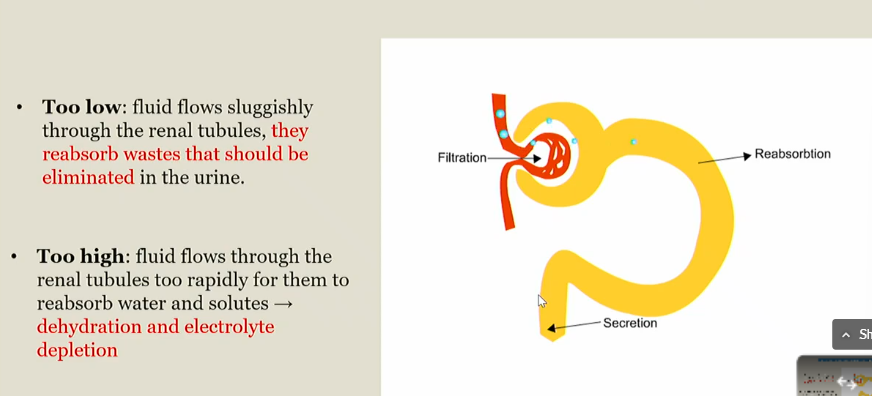
too high Glomerullar filtration rate
Fluid flow fast through the renal tubules, and they cant reabsorb water and solutes
Leads to dehydration and electrolyte depletion
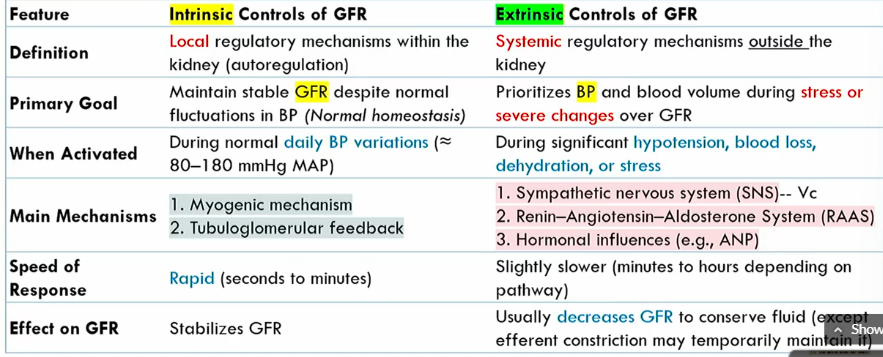
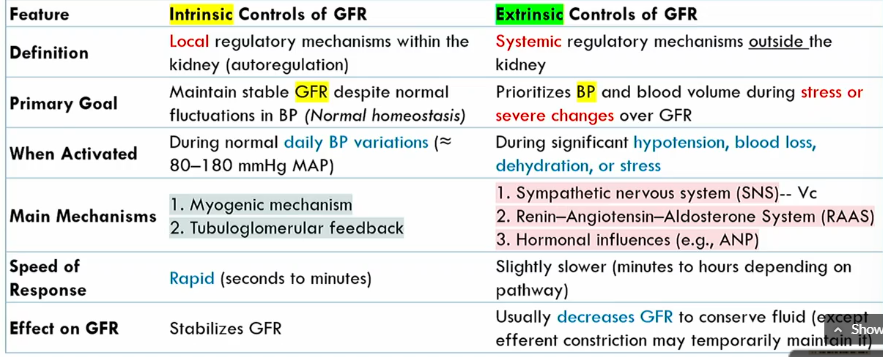
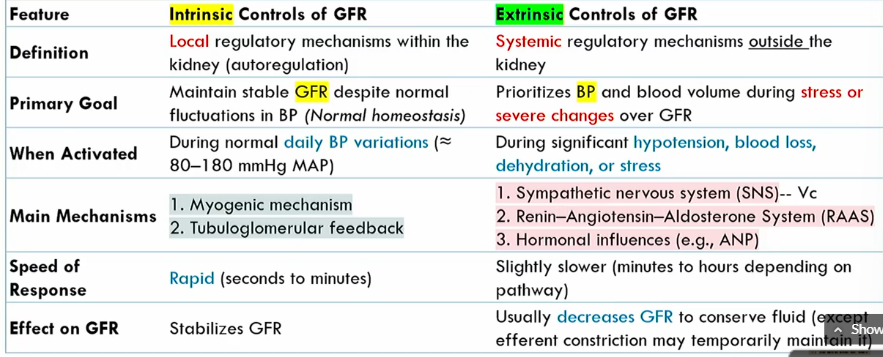
Intrinsic controls of GFR meaning
local regulatory mechanisms within the kidney (autoregulation)
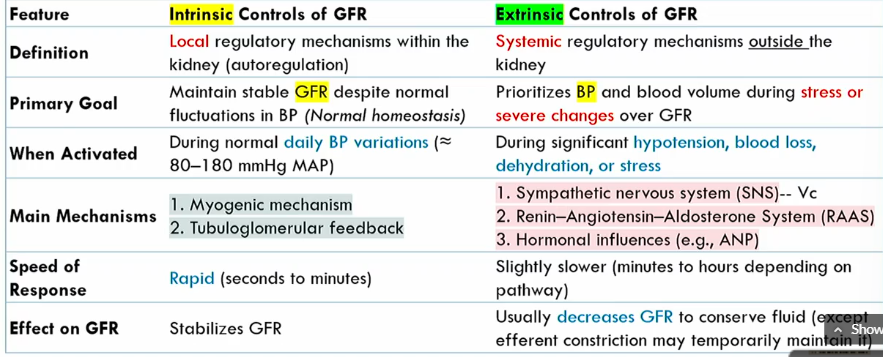
Intrinsic controls of GFR primary goals
maintains stable GFR despite noromal fluctuations in BP (normal homeostasis)
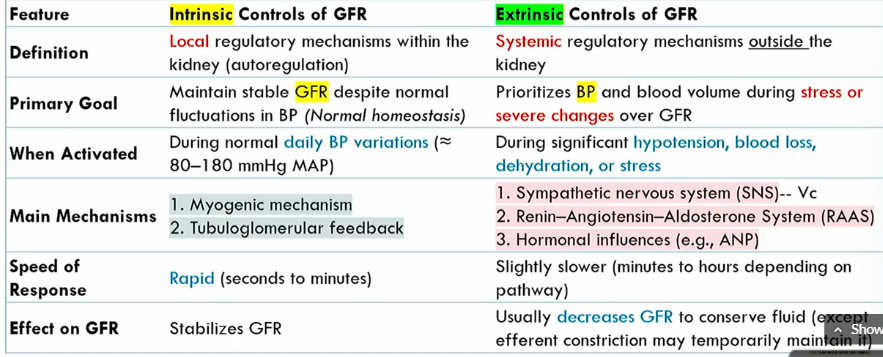
when are the Intrinsic controls of GFR activated
During normal blood pressure fluctuations, around 80-1280 mmHg MAP
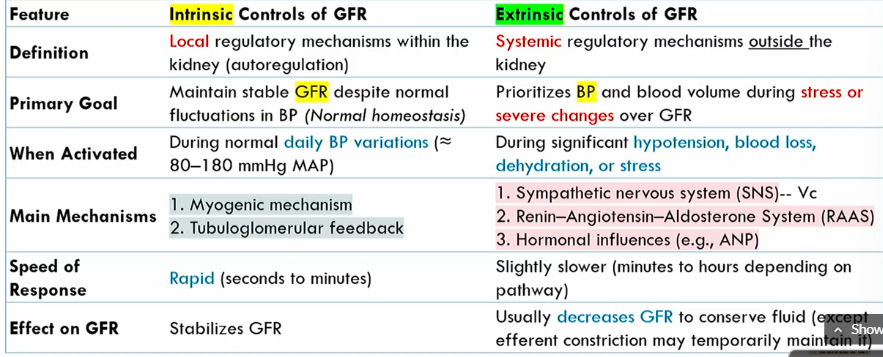
mechanisms of Intrinsic controls of GFR
Myogenic mechanism
tubuloglomerular feedback
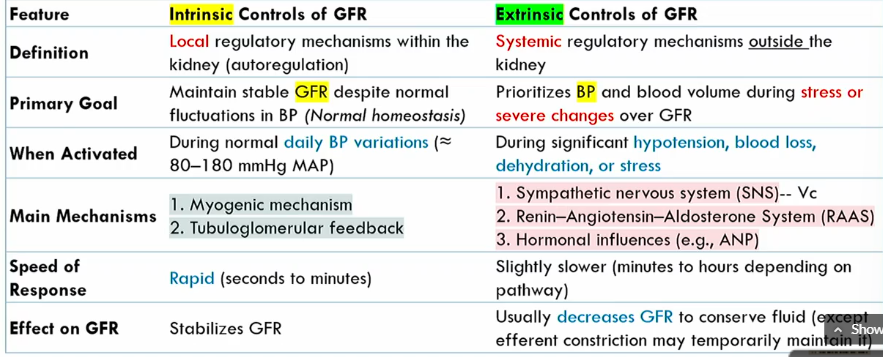
speed of Intrinsic controls of GFR
rapid
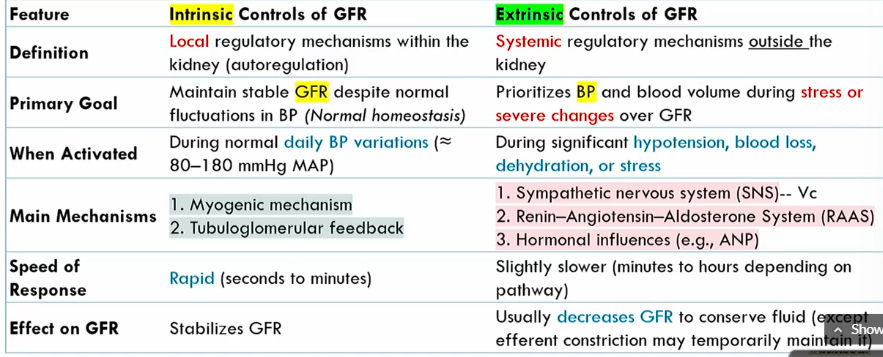
intrinsic conrols of GFR effect on GFR
stabilizes it
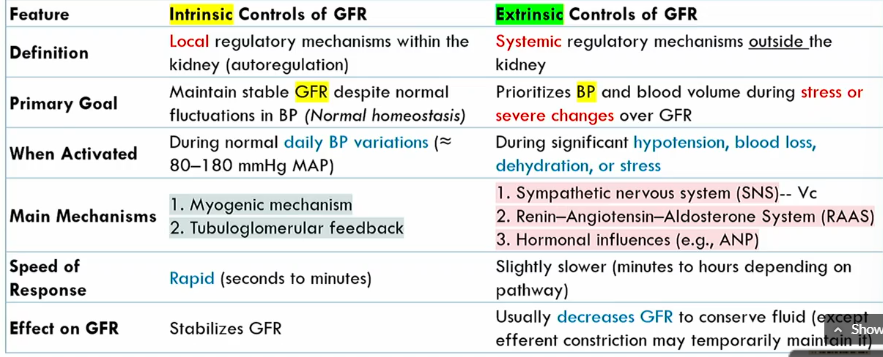
Extrinsic controls of GFR definition
systemic regulatory mechanisms outside the kidney
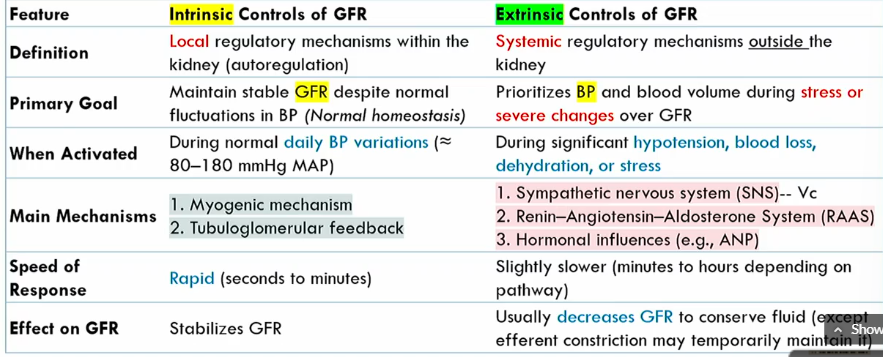
Extrinsic controls of GFR goal
prioritizes blood volume volume during stress or severe changes over GFR
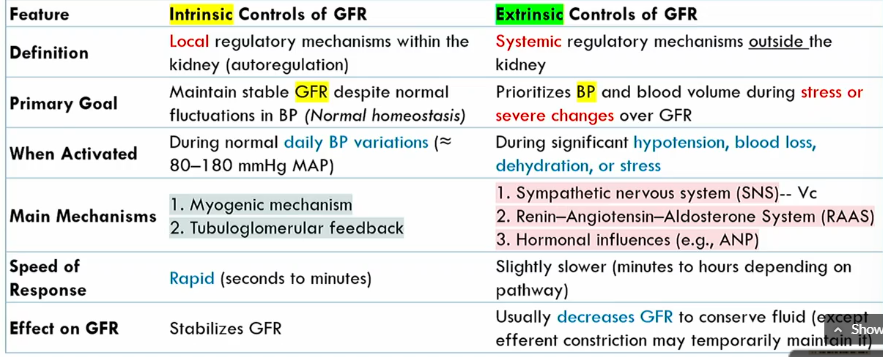
when are the Extrinsic controls of GFR activated
during significant hypotension, blood loss, dehydration, or stress
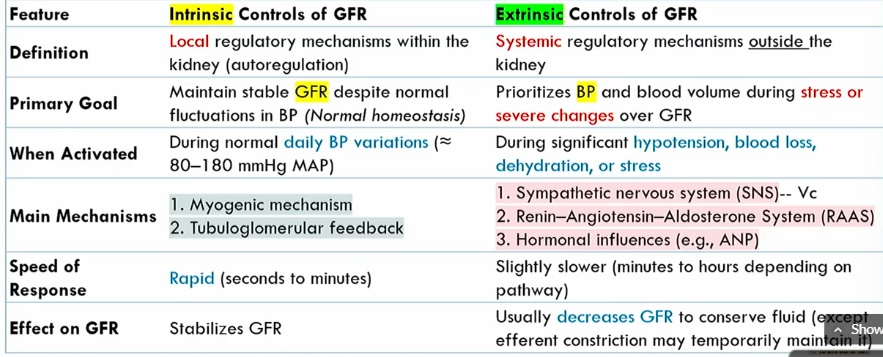
what are the main mechanisms of Extrinsic controls of GFR
SNS
renin-agiotensin-aldoseterone system
hormonal influences
speed of Extrinsic controls of GFR
slightly slower than intrinsic controls of GFR (minutes to hours)
effect of Extrinsic controls of GFR
Decreases GFR to conserve fluid (expect for efferent atriole constriction)
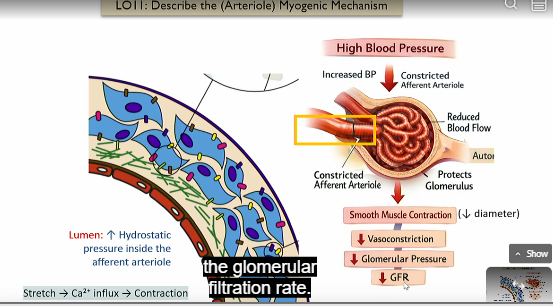
High blood pressure arteriole myogenic mechanism
Intrinsic control of GFR
High blood pressure leads to increased hydrostatic pressure inside the afferent atriole leads to a stretch
stretch leads to an influx in ca2+
ca2+ leads to contraction
diameter then decreases in afferent atriole
this leads to vasoconstriction
Leads to lower glomerular pressure
less net flow from glomerulus to capsule space of bowman’s capsule
lower GFR
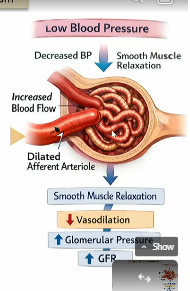
low blood pressure arteriole myogenic mechanism
low blood pressure leads to decreased hydrostatic pressure inside the afferent atriole
smooth muscle relaxes
leads to decreased vasodilation in the afferent atriole
leads to higher flow
Leads to higher glomerular pressure
more net flow from glomerulus to capsule space of bowman’s capsule
higherGFR
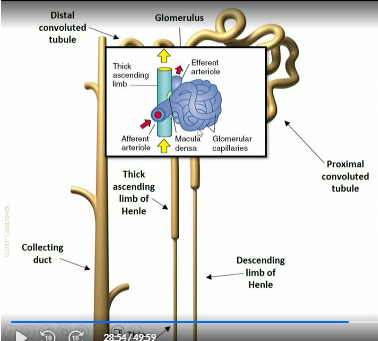
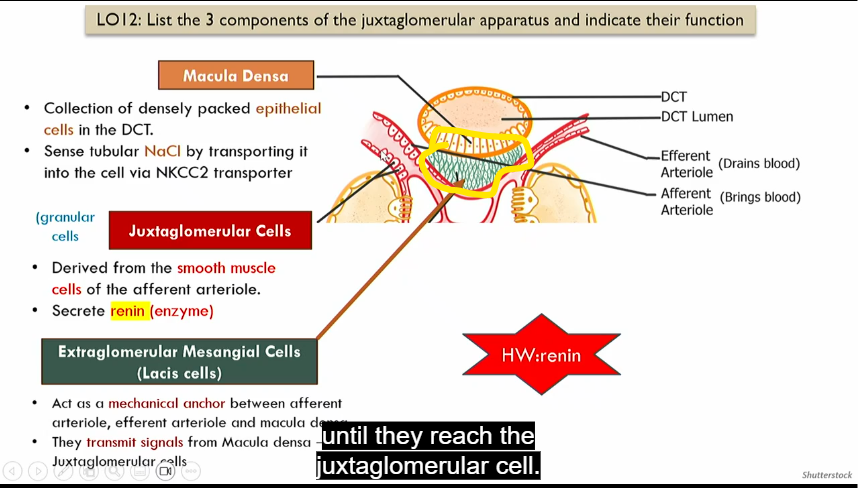
Location of juxtaglomerular apparatus
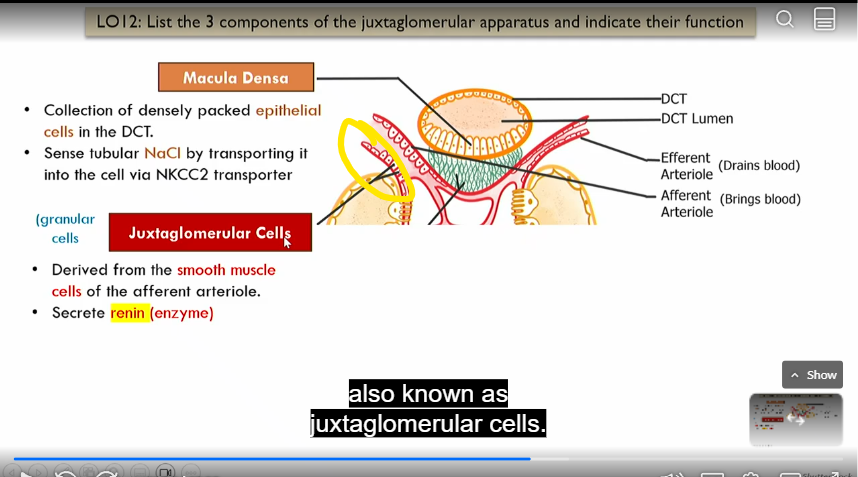
Macula densa
Intrinsic control of GFR, part of juxtaglomerular apparatus
collection of densely packed epithelial cells in distal convoluted tube that sense nacl by absorbing it via NKCC2 transporter
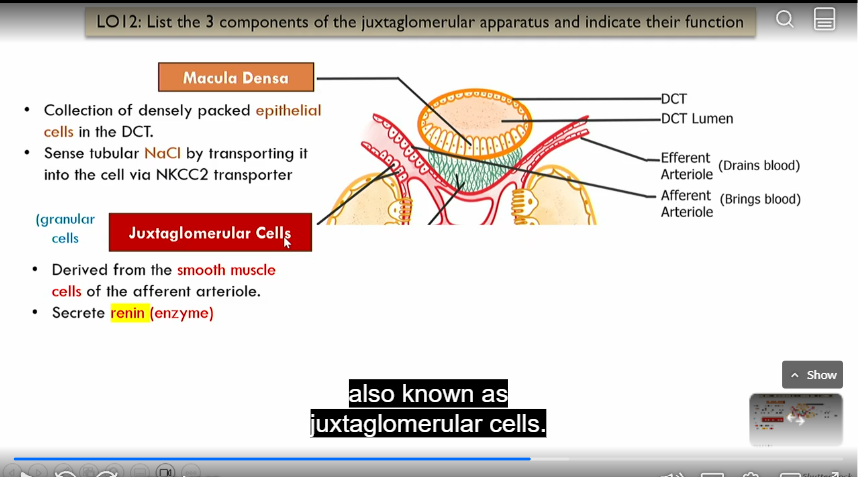
juxtaglomerrular cells
Intrinsic control of GFR, part of juxtaglomerular apparatus
in afferent atriole
derived form smooth muscle cells of efferent atriole, secrete renin (enzyme)
extraglomerular mesangial cells
act as a mechanical anchor between afferent atriole, efferent atriole and macula densa
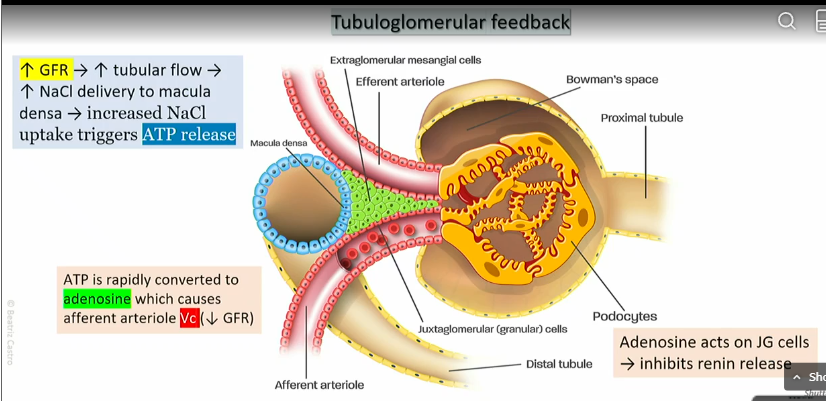
Tuberomerular feedback - high nacl
High GFR leads to high tubular flow
high amounts of Nacl delivered to the macula densa
increased NaCl uptake triggers ATP release
ATP is rapidly converted into adenosine which causes the efferent atriole to vasoconstrict
GFR decreases
Adenosine acts on JG cells, which inhibit renin release
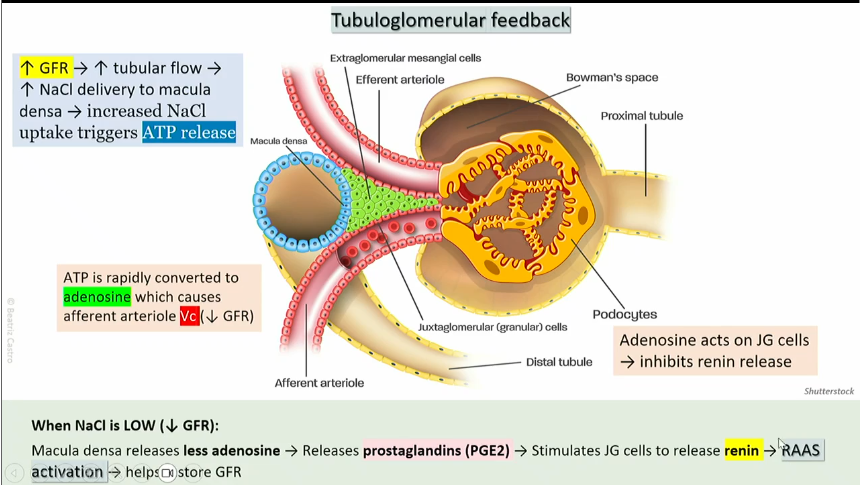
Tuberomerular feedback - LOW
NaCl
low GFR leads to low tubular flow
low amounts of Nacl delivered to the macula densa
decreased NaCl uptake triggers less ATP release, which is then turned into adenosine
less adenosine release leads to prostoglandin release
prostoglandin acts on JG cells, which activates RAAS
RAAS helps restore GFR
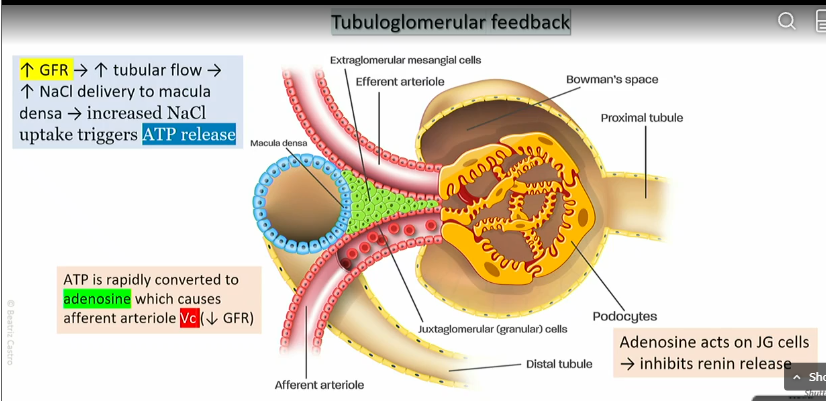
Granular cells
part of afferent atriole in juxtaglomerrular apparatus
Renin aldosterone system
The liver constantly produces angiotensinogen, an innactive precursor circulating in blood
Blood pressure falls, Juxtoglomerular cells release renin
in the bloodstream, renin converts angiotensinogen into angiotensinogen I
in the lungs and vascular endothelium ACE (angiotensin convertin enzyme) converts angiotensin I into angiotensin II (active form of angiotensin I)
angiotensin II makes adrenal gland release aldosterone , which stimulates the reabsorbtion of sodium and water
angiotensin II also acts on the smooth muscle to constrict blood vessels (the kidney prefers the efferent atriole)
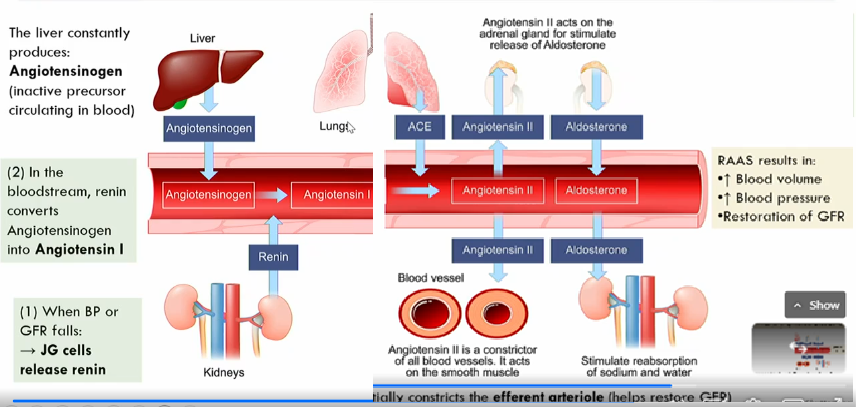
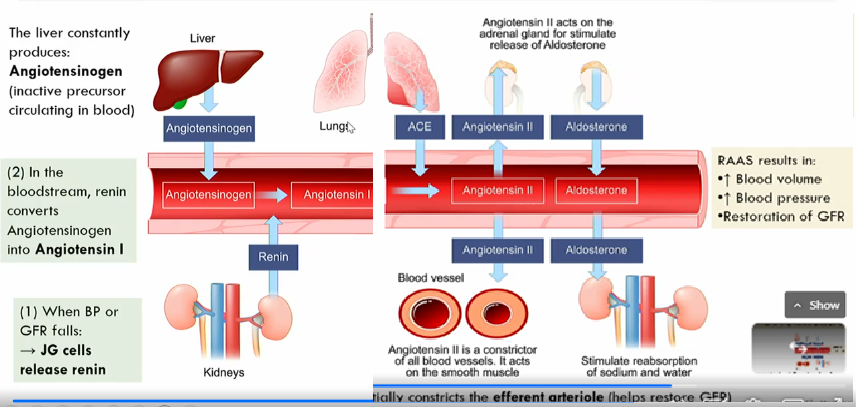
What does angiotensin II do?
active form of angiotensin I
angiotensin II makes adrenal gland release aldosterone , which stimulates the reabsorbtion of sodium and water
angiotensin II also acts on the smooth muscle to constrict blood vessels
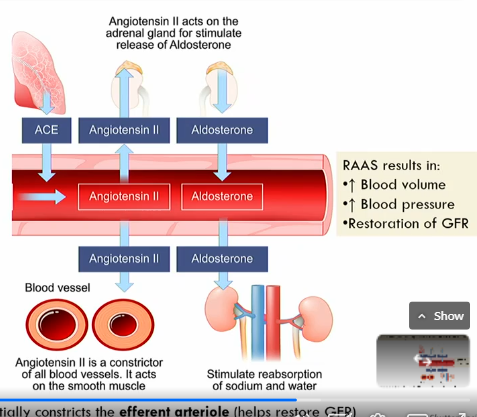
What does RAAS result in?
Increased blood volume
increased blood pressure
restoration of GFR
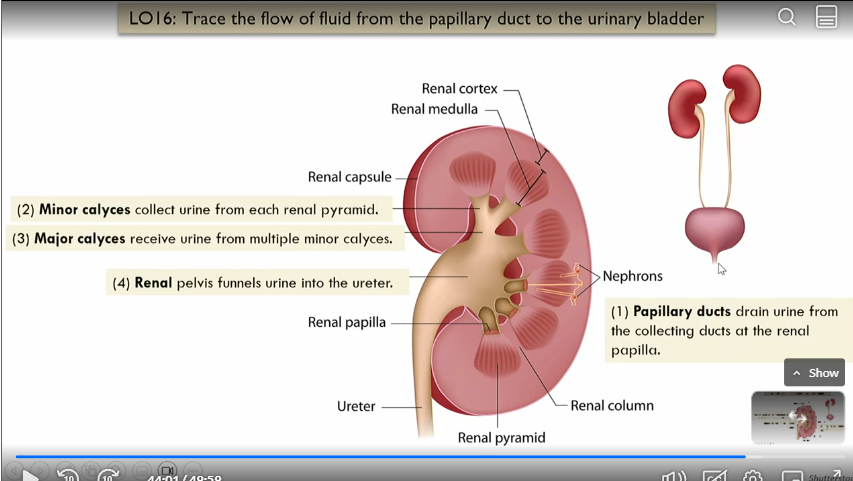
Flow of glomerular filtrate
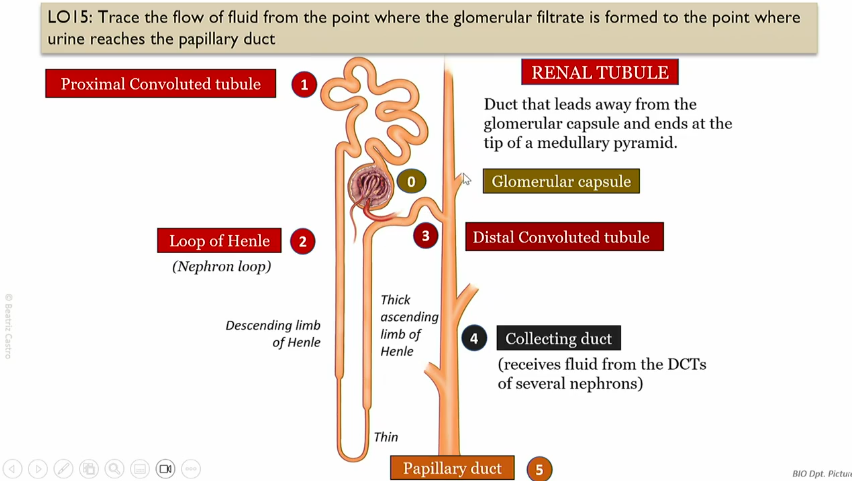
What does the collecting duct do?
recieves fluid form DCTs of several nephrons
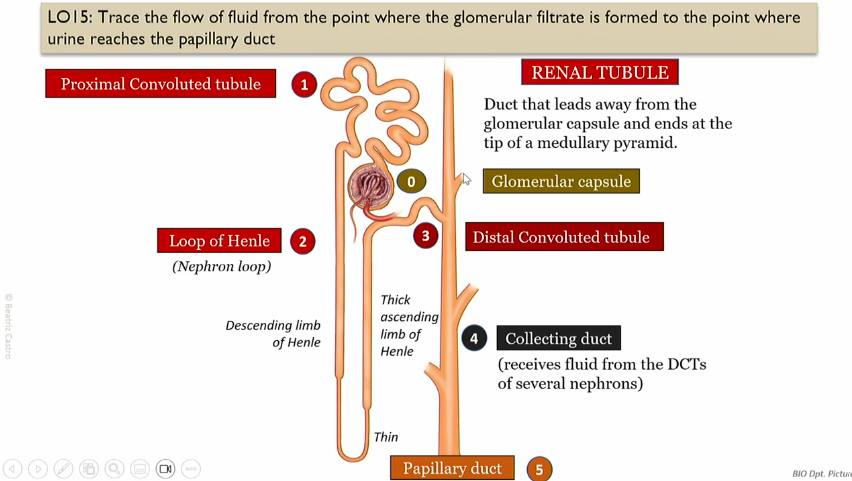
Flow of fluid from papillary duct to the urinary bladder