Pharm exam 3
1/85
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
86 Terms
What is tuberculosis (TB)?
Slow growing lung disease, although it can spread to kidneys, spine and brain; spread through airborne droplets and can be latent or active
What is the acronym for remembering TB meds?
RIPE
What is a broad-spectrum antimycobacterial?
Rifampin
How does rifampin work?
Bactericidal as a result of inhibition of protein synthesis; kills slower-growing organisms
When is rifampin given?
In combination with at least one other antitubercular drug to help prevent antibiotic resistance
What are some complications of rifampin?
Discoloration of body fluids (orange-reddish staining); hepatotoxicity; mild GI discomfort; pseudomembranous colitis
What are some contraindications/precautions to consider when a patient is on rifampin?
Use cautiously in patients who have liver dysfunction; nonhormonal form of birth control should be used
What interacts with rifampin?
Rifampin accelerates metabolism of warfarin, oral contraceptives, protease inhibitors, and NNRTIs for HIV; concurent use with isoniazid and pyrazinamide increases risk of hepatotoxicity
What are med examples of antimycobacterial?
Prototype is isoniazid; exemplars are pyrazinamide and ethambutol
If a patient has latent TB, what meds would they take and for how long?
Can either take just isoniazid for 9 months daily OR isoniazid with rifapentine once weekly for 3 months
If a patient has active TB, what meds would they take?
Several antimycobacterial drugs, usually a four drug regimen, to decrease resistance
What are some complications of isoniazid, pyrazinamide, and ethambutol?
Peripheral neuropathy, hepatotoxicity, and (if they have gout) increased uric acid formation
What are some other complications pyrazinamide and ethambutal?
Pyrazinamide causes photosensitivity and greatly increases risk for sunburn; ethambutol can cause optic neuritis with high doses, which can lead to blindness
What are contraindications/precautions for isoniazid, pyrazinamide and ethambutol?
Contraindicated in liver disease
What interacts with isoniazid, pyrazinamide and ethambutol?
Isoniazid inhibits metabolism of phenytoin; concurrent use of tyramine, alcohol, rifampin, and pyrazinamide can increase risk for hepatotoxicity
Nursing administration for antimycobacterial drugs
Usually given PO, but if IM, warm to room temperature and inject deeply into large muscle; for active, DOT needs to be done; consider second form of birth control, take isoniazid 1hr before or 2hrs after meals with a full glass of water and complete full course of meds; monitor kidney and liver function before and during treatment and avoid alcohol
How do you know that antimycobacterial were effective?
Improvement of tuberculosis manifestations (clear breath sounds, no night sweats, increased appetite, no afternoon rises of temp) and three negative sputum cultures for tuberculosis (usually takes 3-6 months to achieve)
How do most antivirals work?
Altering viral reproduction; only effective during viral replication and ineffective when virus is dormant
What antiviral is used to treat the herpes simplex and varicella?
Acyclovir
What is the MoA of acyclovir?
Prevents the reproduction of viral DNA and interrupts cell replication
What are some complications of acyclovir?
Phlebitis and inflammation at the site of infusion, nephrotoxicity, nausea, HA, and diarrhea
Nursing administration for acyclovir
Administer IV slowly over 1+ hours; healed herpetic lesions should continue to use condoms
What antiviral treats influenza?
Oseltamivir
What is the MoA of oseltamivir?
Decreases the release of the virus from infected cells
What are some complications of oseltamivir?
N/V/D, self-injury and delirium
Nursing administration for oseltamivir
Should be taken within 48 hours of flu symptoms, not a substitute for influenza vaccines
What is highly active antiretroviral therapy (AART)?
A regimen that combines multiple antiretroviral medications; reduces viral replication to undetectable levels
What is a med example of a antiretroviral that inhibits fusion/entry?
Enfuvirtide (SQ)
What is the MoA of enfuvirtide?
Blocks HIV from attaching to and entering CD4 T cell
What are some complications of enfuvirtide?
Localized reaction at injection site; bacterial pneumonia; fever, chills, rash and hypotension
Nursing administration for enfuvirtide
Rotate injection sites and take exactly as prescribed
What is a med example of an antiretroviral that is a CCR5 antagonist?
Maraviroc
What is the MoA of maraviroc?
Prevents HIV from entering lymphocytes by binding to CCR5 on cell membranes
What are some complications of maraviroc?
Cough and upper respiratory tract infections; dizziness, orthostatic hypotension; hepatotoxicity; pseudomembranous colitis (severe colon inflammation often caused bacteria overgrowth after antibiotic use)
Nursing administration for maraviroc
Monitor LFTs, BP, and CBC; take at regular intervals
What is a med example of a antiretroviral nucleoside reverse transcriptase inhibitor (NRTIs)?
Zidovudine (oral and IV)
What is the MoA of zidovudine?
Inhibits DNA synthesis, which inhibits viral replication (first-line antiretroviral)
What are some complications of zidovudine?
Suppressed bone marrow, lactic acidosis, N/V/D, hepatomegaly, and fatty liver
Nursing administration for zidovudine
Baseline CBC and platelets, monitor regularly; take exactly as prescribed
What is a med example of an antiretroviral non-nucleoside reverse transcriptase inhibitor (NNRTIs)?
Efavirenz (oral)
What is the MoA of efavirenz?
Binds to reverse transcriptase to stop growth of DNA by stopping replication (often used in combination to prevent resistance)
What are some complications of efavirenz?
N/V/D, dizziness, drowsiness, rash (Stevens-Johnsons syndrome), flu-like S/S, HA, and fatigue
Nursing administration for efavirenz
Monitor for rash; take as prescribed; use barrier form of contraception
What is a med example of an antiretroviral protease inhibitor?
Ritonavir
What is the MoA of ritonavir?
Inhibits enzymes needed for HIV replication
What are some complications of ritonavir?
Bone loss, DM or hyperglycemia, hypersensitivity, N/V, elevated lipid levels, and altered fat distribution
Nursing administration for ritonavir
Take with food to increase absorption; use barrier form of contraception
What is a med example of an antiretroviral integrase strand transfer inhibitor (INSTI)?
Raltegravir
What is the MoA of raltegravir?
Inhibits enzyme (integrase) required for viral replication
What are some complications of raltegravir?
HA, insomnia, rash, liver injury, renal failure, and suicidal ideation
Nursing administration of raltegravir
Monitor baseline LFTs + CBC; take exactly as prescribed
What is biktarvy?
INSTI/NRTI/NRTI combination antiretroviral drug; most patients tolerate
What are some complications of biktarvy?
Rare; liver toxicity, renal impairment and lactic acidosis; if pt has both HIV and Hep B, risk of liver failure
Nursing administration for biktarvy
Take drug every day at the same time
What is PrEP?
Pre exposure prophylaxis, taken by HIV-negative people; reduces risk of HIV transmission; tenofovir 300mg + emtricitabine 200mg (idk if we need to know this)
What are some complications of PrEP?
Renal toxicity and reduced bone mineral density; regular HIV testing and renal monitoring needed
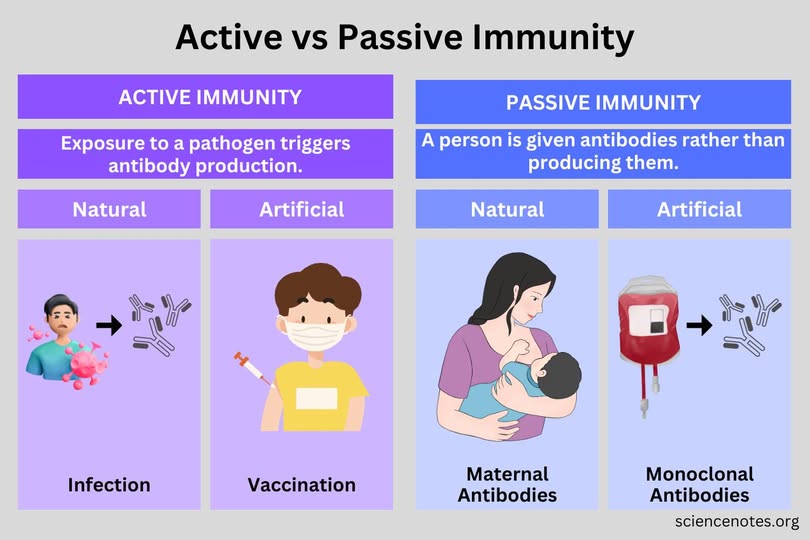
What is active immunity?
When immune system produces antibodies in response to antigens; can be both artificial and natural
What is passive immunity?
Temporary; when antibodies are created by another human/animal and then transferred to the patient; can be artificial or natural
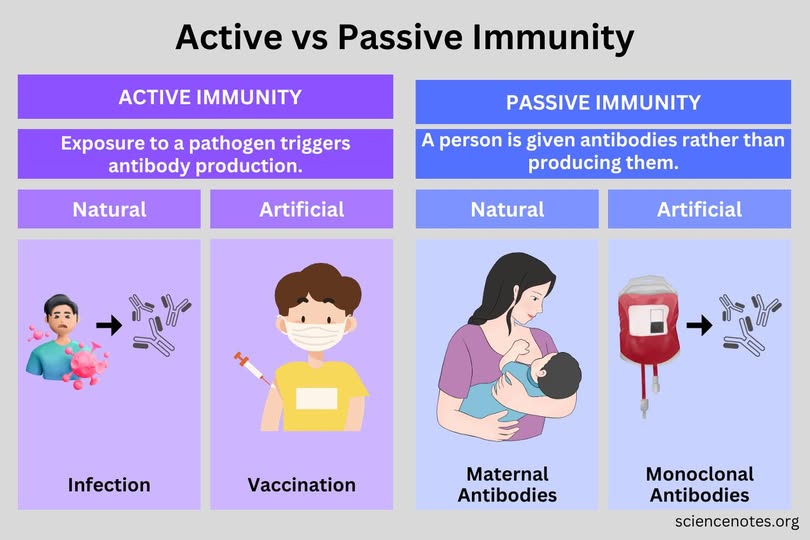
helpful imagery
I don’t know how in depth we need to know this but this is useful!
What are some complications of immunizations?
Anaphylactic reaction (no more doses of that vaccine after reaction); no live virus vaccines to immunocompromised patients; patients with common cold or other minor illnesses can still receive vaccines
Nursing administration of vaccines to infants and children
Obtain informed consent from legal guardian; IM, for infants and young children, in vastus lateralis or VG muscle; IM, for older children and adults, in deltoid; strategies to minimize discomfort; avoid aspirin; have emergency drugs and equipment on standby; document date, route, site of immunization, type, manufacturer, lot number and expiration date and evidence of informed consent
How often should everyone get the flu vaccine?
Annually, beginner at 6 months of age
What are some contraindications of live, attenuated vaccines?
Immunocompromised patients, pregnant patients, and patients who previously had a severe allergic reaciton
What are some common examples of live attenuated vaccines?
MMR: doses at 12-15 months and 4-6 years
Varicella: doses at 12-15 months and 4-6 years
Rotavirus
What are some diseases that vaccines can protect against?
HPV, herpes zoster, pneumococcal disease, MMR, varicella, diphtheria, tetanus, pertussis, hepatitis B, and polio
What are peptic ulcers?
Ulcers that occur in the stomach, duodenum or esophagus
What causes peptic ulcer disease (PUD)?
Helicobacter pylori infection, NSAIDs, and severe stress
What are the S/S of PUD?
Bleeding, perforation, and obstruction
What is GERD?
Chronic reflux of gastric contents into the esophagus
What are the S/S of GERD and what are the complications?
S/S: heartburn, regurgitation, and dysphagia
Complications: esophagitis, and Barrett’s esophagus
What are the goals of therapy for PUD?
Assess what happened to gastric mucosal defenses (antagonist factors like H. pylori or smoking, NSAID use, or issues with mucus and bicarbonate); use antibiotics to eliminate H. pylori, and generally promote health of GI tract
What are some antibiotics that might be used for PUD?
Amoxicillin, bismuth, clarithromycin, tetracycline, and metronidazole
What are some med examples of H2 receptor blockers?
Prototype is cimetidine; exemplars are famotidine and nizatidine
What is the MoA of cimetidine?
Blocks H2 receptors leading to decreased gastric acid production
What is cimetidine used for?
Prevent or treat gastric/duodenal ulcers, GERD, and heartburn; used in conjunction with antibiotics to treat ulcers
What are some complications with cimetidine?
Blocked androgen receptors (decreased libido, gynecomastia, and impotence); lethargy, hallucinations, confusion, and restlessness; constipation, diarrhea, and nausea
What are some interactions that cimetidine has?
Can increase levels of warfarin, phenytoin, theophylline, and lidocaine; concurrent use of antacids can decrease absorption; smoking can decrease effectiveness
Nursing administration for cimetidine
Avoid smoking, and see provider if manifestations persist
What should the patient know when taking cimetidine?
Notify provider for any indication of GI bleed, avoid alcohol and foods that increase GI irritation, limit use of ASA or NSAIDs, and increase fiber and fluid intake
What are some med examples of proton pump inhibitors (PPIs)?
Prototype is omeprazole; everything ends in -prazole
What is the MoA of omeprazole?
Irreversibly inhibits enzyme that produces gastric acid (reduces gastric acid secretion)
What is omeprazole used for?
Short-term therapy of gastric and duodenal ulcers and GERD; prevention of stress ulcers for at-risk patients
What are some complications of omeprazole?
Pneumonia, osteoporosis and fractures, rebound acid hypersecretion, hypomagnesemia, and C-diff; if breastfeeding, only use if benefits outweigh risks
What are some interactions that omeprazole has?
Increases levels of digoxin, diazepam, antifungals, and phenytoin when used concurrently
Nursing administration for omeprazole
Active ulcers should be treated for 4-6 weeks, notify provider for indication of GI bleed, and take once a day prior to eating in the morning