Reproduction I (Males)
1/25
Earn XP
Description and Tags
CC, SEQ Animal Reproduction | CC Components of Male reproduction | SEQ sperm production | SEQ, HD Male endocrinology
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
26 Terms
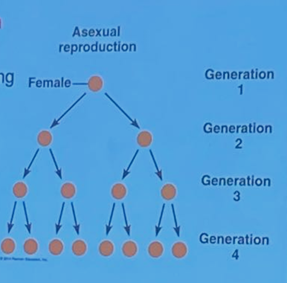
What is Asexual Reproduction?
A single parent leads to 2+ offspring.
Offspring are identical clones w/ no gamete fusion or meiosis.
Advantage: Rapid offspring, don’t need to find a mate, but have a change to get wiped out by sickness or predator.
List the types of Asexual reproduction
Budding (Asymmetrical split in an organisms)
Fission (Daughters organisms split into two equal sizes)
Fragmentation & regeneration (Starfish)
Parthenogenesis (Both sexual & asexual Ants)
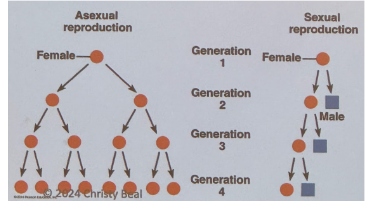
What is Sexual Reproduction?
Reproduction involving production and fusion of gametes leading to genetic diversity.
Sperm + Egg = zygote (2n)
Disadvantage: “Reproductive cost” - Only ½ of population can actually reproduce
List the structures to the male reproductive system.
Testes
Epididymis
Scrotum
Penis
Accessory Glands ( Seminal vesicles, Prostate Gland, Bulbourethral Glands )
What is the pathway for sperm? “SEVEn UP”
“SEVEn UP”
Testes (seminiferous tubules) → epididymis → vas deferens → ejaculatory duct → urethra → penis → release from body
Describe the Testes structure & function of the male reproductive.
Male Gonads (reproductive organs)
Seminiferous tubules: This is the site of spermatogenesis, it is a long hollow tube with a small diameter.
Leydig cells: They produce testosterones & other male sex hormones and are scattered between seminiferous tubules
Describe the Epididymis structure & function of the male reproductive.
A coiled tube connected to the testes that stores, transports, and matures (Gaining motility & fertilizing ability) sperm.
Describe the Scrotum structure & function of the male reproductive.
A skin covered sac, that surrounds the testes & epididymis.
It is external which helps to keep the sperm cooler than body temp.
Describe the Penis structure & function of the male reproductive.
Function:
Delivers sperm into the female reproductive tract.
Urethra: Runs through the penis, allowing urine and sperm to exit the body.
Structure:
Erectile Tissue: Three parallel columns that fill with blood during sexual stimulation.
Nitric Oxide (NO) Release: Increases blood flow, leading to erection, causing hydrostatic skeleton
Glans: Tip of the penis, many sensory nerves.
Prepuce (Foreskin): Covers and protects the glans.
List all the Accessory Glands in the male reproductive system
Seminal Vesicles
Prostate Gland
Bulbourethral Gland
Describe the Seminal Vesicles structure & function. (Accessory Gland)
Produce and secrete fluid into the vas deferens to mix with sperm.
Fluid is rich in:
Fructose: Provides energy for sperm after ejaculation.
Prostaglandins: Stimulate uterine contractions to help sperm movement.
Describe the Prostate Gland structure & function. (Accessory Gland)
Secretes fluid into the urethra to mix with sperm and seminal fluid.
Fluid contains:
Citrate: A nutrient for sperm.
Anticoagulant enzymes: Help keep semen in a liquid state for sperm mobility.
Describe the Bulbourethral Gland structure & function. (Accessory Gland)
1st gland to secrete into the urethra during arousal. Two small glands located on either side of the urethra.
Produces bulbourethral fluid (mucus) that:
Neutralizes acidic urine in the urethra.
What is semen?
It is a mixture of sperm and fluids gained from accessory glands as it moves through the conducting tubes.
Sequence the sperm path
Epididymis – Sperm is stored and matures here.
Vas Deferens – Sperm ducts (one from each epididymis) extend from the scrotum to the pelvic cavity.
Ejaculatory Duct – Passes through the prostate gland and joins the urethra.
Urethra – Carries both urine and semen through the penis for excretion or ejaculation.
What is spermatogenesis?
It is the production of mature sperm cells that occurs continuously.
What is the first process in spermatogenesis? (Embryonic)
Embryonic stage: Primordial germ cells divide and differentiate.
They develop into spermatogonia (stem cells), which later undergo further division to produce sperm.
What is the second process in spermatogenesis? (Testes)
Spermatogonial stem cells → Mitosis → Spermatogonia (2n)
Spermatogonia (undifferentiated cells) → Located in the walls of seminiferous tubules, are maintained via mitotic divisions.
Some spermatogonia → Differentiate into Primary Spermatocytes for further stages.
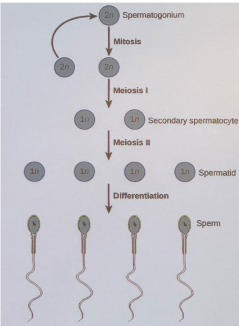
What is the third process in spermatogenesis? (Spermatocytes)
A Primary Spermatocyte (2n) divvies via meiosis at puberty's
Meiosis 1 → produces secondary spermatocytes (n)
Meiosis 2 → produce spermatids (n)
spermatids differentiate into mature sperm cells (n) capable of fertilization (7 weeks to produce mature)
At puberty, the process of spermatogenesis is triggered, leading to the following key changes:
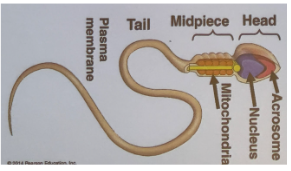
What is the structure of a sperm cell?
Mature Sperm - takes about 7 weeks to produce
Only nucleus enters egg
Head
DNA in nucleus
Acrosome - contains enzymes to penetrate the egg
Midpiece - mitochondria (ATP)
Tail - flagellum
What are Androgens?
They are the principle sex hormones in males, testosterone being the most important.
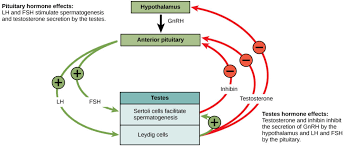
Sequence the Signaling Pathway for Spermatogenesis
Hypothalamus secretes GnRH (Gonadotropin-Releasing Hormone).
Anterior Pituitary (AP) releases two gonadotropins:
Luteinizing Hormone (LH)
Follicle Stimulating Hormone (FSH)
LH stimulates Leydig cells in the testes to produce testosterone.
FSH stimulates Sertoli cells in the seminiferous tubules to support spermatogenesis and aid in the maturation of sperm cells.
What role does Luteinizing Hormone (LH) in spermatogenesis?
LH targets the Leydig cells in the testes to produce testosterone
High levels of testosterone are needed for spermatogenesis.
What role does Follicle Stimulating Hormone (FSH) in spermatogenesis?
FSH stimulates Sertoli cells in the seminiferous tubules to secrete androgen binding protein (ABP)
ABP binds to testosterone, helping maintain high levels of testosterone in the testes, essential for spermatogenesis.
Inhibin, a peptide hormone secreted by Sertoli cells, inhibits the secretion of FSH to regulate spermatogenesis
What role does Testosterone in spermatogenesis?
Stimulates puberty and sexual maturation.
Growth spurt during puberty.
Development of primary male sex characteristics (reproductive organs).
Development of secondary sex characteristics: body hair, deep voice, muscle growth.
What type of feed back regulation is used in Male Endocrinology?
The male endocrine system primarily uses negative feedback regulation to maintain hormonal balance:
Testosterone: High levels of testosterone inhibit the release of GnRH from the hypothalamus and LH from the AP
Inhibin: Secreted by Sertoli cells in the testes, inhibin inhibits the release of FSH (Follicle Stimulating Hormone) from the anterior pituitary.