L25- gut microbiome and ageing
1/41
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
42 Terms
microbiome definition
the genome of all the microorganisms (bacteria, archea, viruses and fungi), symbiotic and pathogenic, living in and on all vertebrates.
where in the body has the greatest density of bacteria
the gut has highest density on the planet
healthy human gut can house at least 1000 different species of bacteria, the majority belonging to Bacteroidetes and Firmicutes
Gut microbiome is genetically more complex than the human genome- and more dynamic; 316 million different genes
what are the benefits of the gut microbiome
protection against pathogens
synthesis of vitamins
immune system development
promotion of intestinal angiogenesis
promotion of fat storage
SCFA production by fermentation of dietary fibre
modulation of central nervous system
what are some conditions linked to dysbiosis
Obesity: Firmicutes prevalent, lower diversity. Probiotics (Lactobacillus, Bifidobacterium lactis) may help regulate
Type 2 diabetes
Irritable bowel syndrome (IBS)
Cardiovascular diseases caused by proinflammatory metabolites
may also correlate to ageing
what SCFAs
short chain fatty acids
(acetate, propionate, butyrate) are products of anaerobic fermentation of dietary fiber and resistant starch, and to a lesser extent of proteins.
what are the 3 roles of SCFAs (8)
provide energy substrate for colonocytes and hepatocytes
contribute to intestinal barrier integrity by upregulating the expression of tight junction proteins and mucus production
Immuno-effects: protect against inflammation (by inducing regulatory T-cell differentiation and IL secretion). Butyrate turns macrophages into super-killers
reduce the risk of colorectal cancer
increase insulin secretion by beta-pancreatic cells
effects on DNA homeostasis in the nuclei of gut and brain cells, by inhibiting a histone deacetylase (HDAC)
Regulate skeletal muscle metabolism and function
Modulate the central nervous system (CNS)
what us the brain gut connection
vagus nerve carries signals between brain, heart and gut
CNS affects the gut motility, secretion, blood flow, nociception and immune function, which in turn affect the microbiome
Gut has peristaltic movement to push forward, initiated by vagus nerve
What are the main pathways of the gut–brain axis?
Neural: vagus nerve
Hormonal: GLP-1, PYY
Immune: interleukins
Metabolic: SCFAs (acetate, propionate, butyrate)
Key idea:
Gut microbiota communicate with the brain via multiple systems
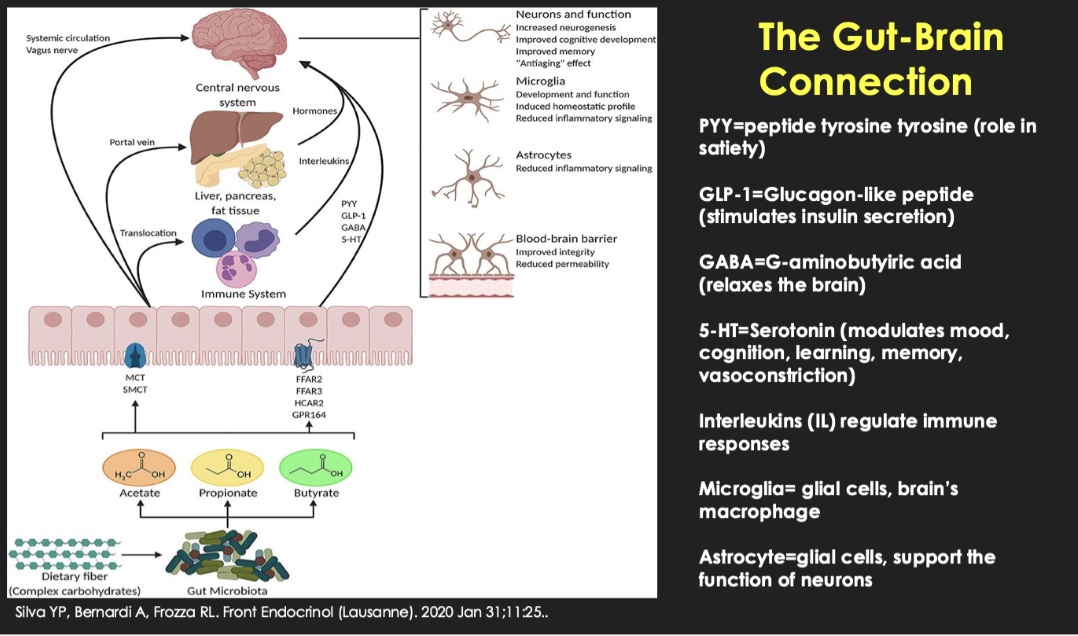
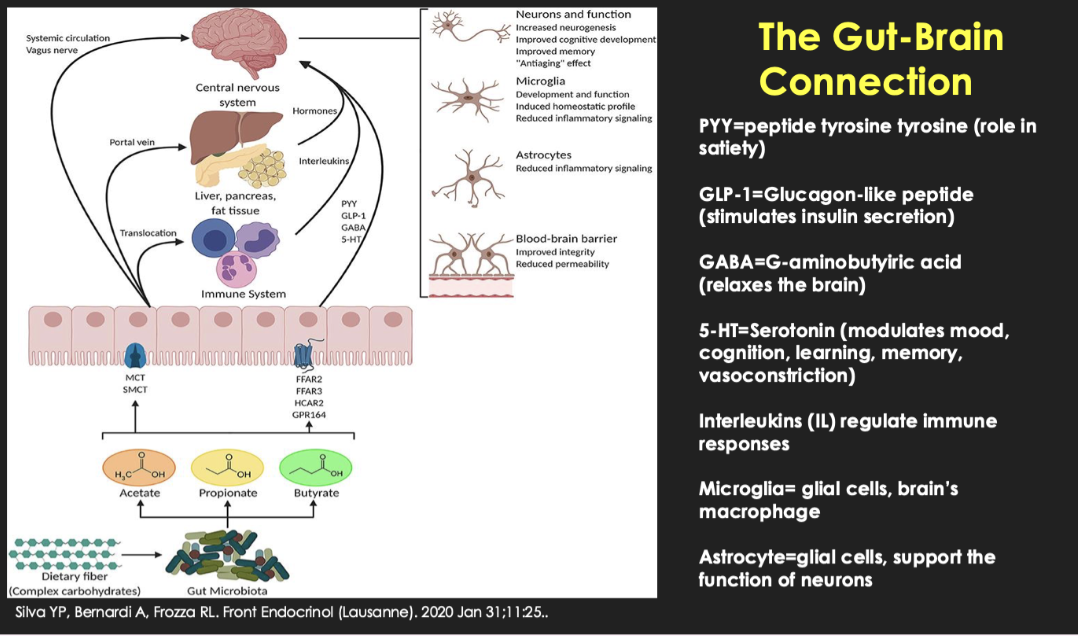
How does the gut–brain axis affect brain function?
Key signals:
GLP-1 → insulin
PYY → satiety
Serotonin → mood/cognition
GABA → inhibitory
Effects on brain:
Neurons, microglia, astrocytes, BBB
Inflammation & cognition
Key idea:
Gut health influences brain health; insulin spikes/metabolic dysfunction can be harmful
what is the possible relationship between SCFA/CNS and autism
propionate has negative effects in mice (abnormal, repetitive behaviour, decreased social interaction)
butyrate has beneficial ones (restores social interaction)
dysbiosis (altered gut microbiome) in autistic children may increase toxic metabolite production (phenols, indols-derivates, p-cresols) and cytokine-mediated inflammation
what is the possible relationship between SCFA/CNS and depression
butyrate has beneficial effects (restores social interaction)
what is the possible relationship between SCFA/CNS and alzheimer’s disease
butyrate has beneficial effect by disrupting the interaction between amyloid-beta peptides
what is the possible relationship between SCFA/CNS and parkinson disease
butyrate prevents aggregation of alpha-synuclein (unfolded protein that accumulates in clumps called Lewy bodies)
how can the gut brain connection be studies
Mice under germ free (GF, lack microbiome) vs specific pathogen free (SPF) housing conditions
Young (6-10 weeks) vs old (96-104 weeks)
Gene expressions (RNA sequencing) → Age-dependent “transcriptomic signature”- strongest
changes in genes involved in cytoskeleton, immune function and mitochondrial function
Old SPF vs GF differences in microglia: upregulation of ROS-promoting genes and ROS-response
genes. ROS levels and mitochondrial function-ATP production
Metabolomics: examine metabolites in serum, brain and faeces.
Gut permeability, Fecal matter transfer from old/young mice into germ free mice
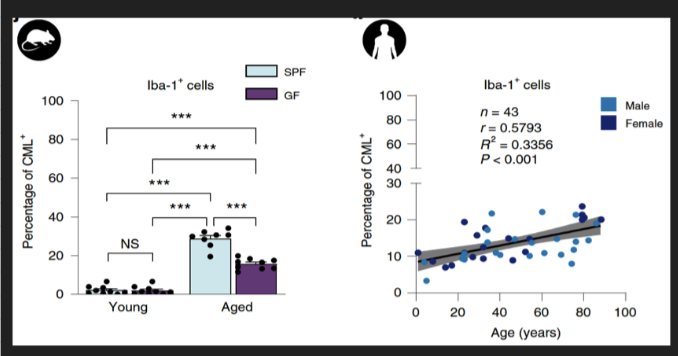
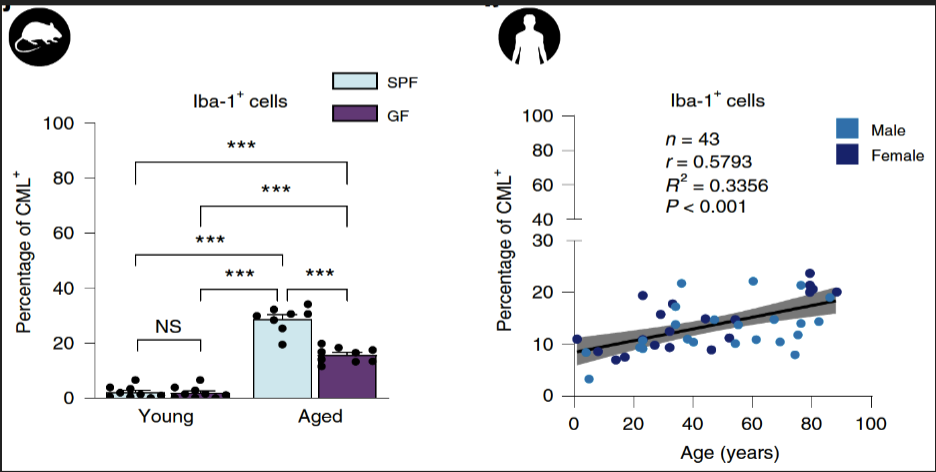
what is CML
N(6)-carboxymethyllysine metabolite is generated through oxidation and glycation of proteins. Elevated in certain diseases (AD) and ageing.
what microglia
a type of neuroglia (glial cell) located throughout the brain and spinal cord (10-15% of cells). The resident macrophage cells, the first and main form of active immune defence in the CNS;
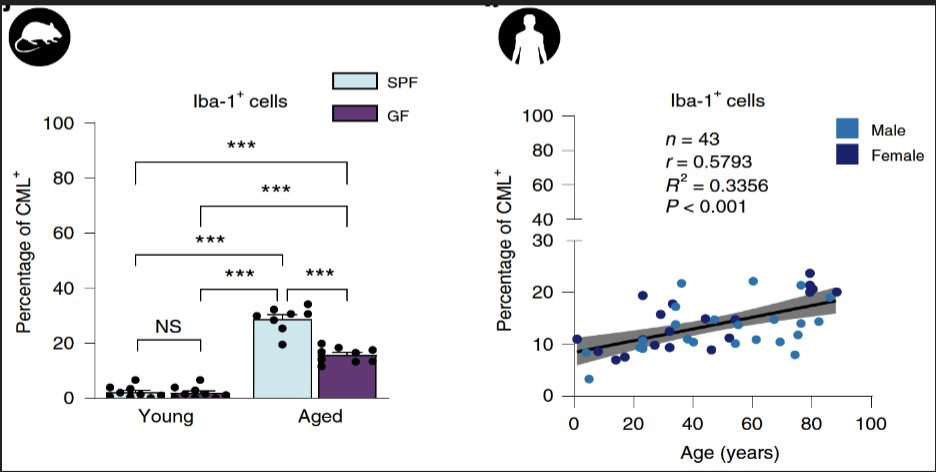
how does CML leakage affect microglia in old mice
Critical involvement of CML in oxidative stress and Mitochondrial disfunction of microglia of old mice
Egress of CML from the gut (rather than oral CML) is Required for the harmful impact
The gut microbiome changes with age and plays a key role in leakage from the aged gut
Important role in microglia aging and presumably CNS aging
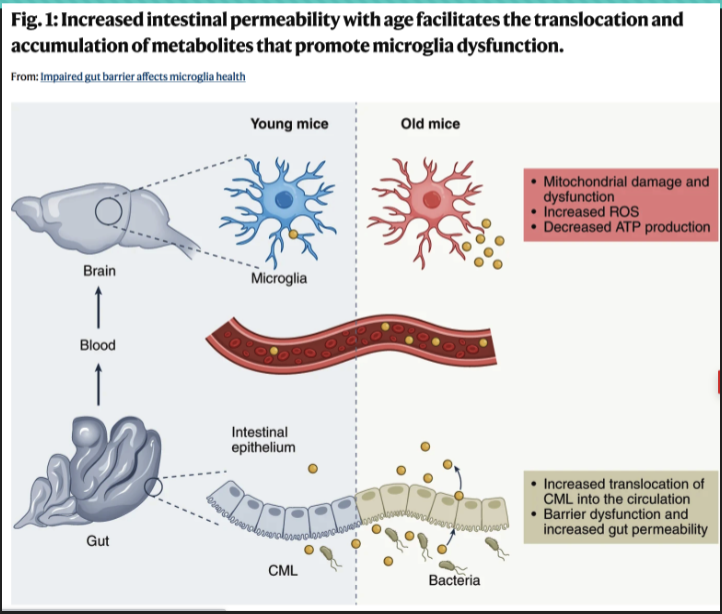
what are the 2 types of starch
rapidly digested starch
resistant starch
prebiotics
what is rapidly digested starch
(especially amyloidose, the branched starch) are reduced to glucose in the small intestine
what is resistant starch
(starch molecules, especially amylose, form crystalline regions that are resistant to digestion by our own enzymes). Similarly to dietary fibre, it is one of the best sources of SCFAs.
what are raw legumes, why are they good
a source of resistant starch
(beans, pulses, lentils) are very high in amylose (up to 40% of the total starch, or 30% of the dry weight). Boiling legumes reduces the resistant starch (RS) to only 4- 5% of their DW. Cooling o/n may increase the RS slightly.
what are the 2 types of fibre
soluble fibre
insoluble fibre
prebiotics
what is soluble fibre
gelatinous texture (jama)
has demulcent properties that protect the stomach (gastritic, heartburn)
helps treat constipation and reduce cholesterol
what is insoluble fibre
dry texture (wheat bran)
it satisfies the appetite and has a laxative effect (obesity)
reduces cholesterol
contained in whole grains, nuts and seeds
what are some features of irritable bowel syndrome (IBS)
10% of elderly are affected
strong genetic component
begins in young adults
symptoms (abdominal pain and cramps, bloating, diarrhea or constipation
what are some features of inflammatory bowel disease (IBD)
Crohn’s disease, Ulcerative colitis):
Helicobacter hepaticus
early and late onset (10-15% diagn. at >60 years of age, especially for colitis)
elderly more at risk of complications, including venous trombosis
describe infection with Clostridium difficile
anaerob, lives in soil
5% people are carrier
risk factors: hospital stay, oral antibiotics, compromised immune system, age > 65 years
what are some features gastrointestinal cancer
Helicobacter pilori
-1:100 risk over lifetime
-age >65 years
what are some features colorectal cancer
-1: 24 risk over lifetime
- age >70 years
how does the intestinal epithelium act as a firewall
The intestinal epithelium forms a protective barrier maintaining gut homeostasis
Interacts with microbiota, metabolites, and immune responses (inflammation)
With ageing:
Altered microbiota + ↑ inflammation
Reduced stem cell function → poorer repair
Increased cellular senescence
→ Overall: barrier integrity declines (“leaky gut”) → systemic inflammation and disease risk
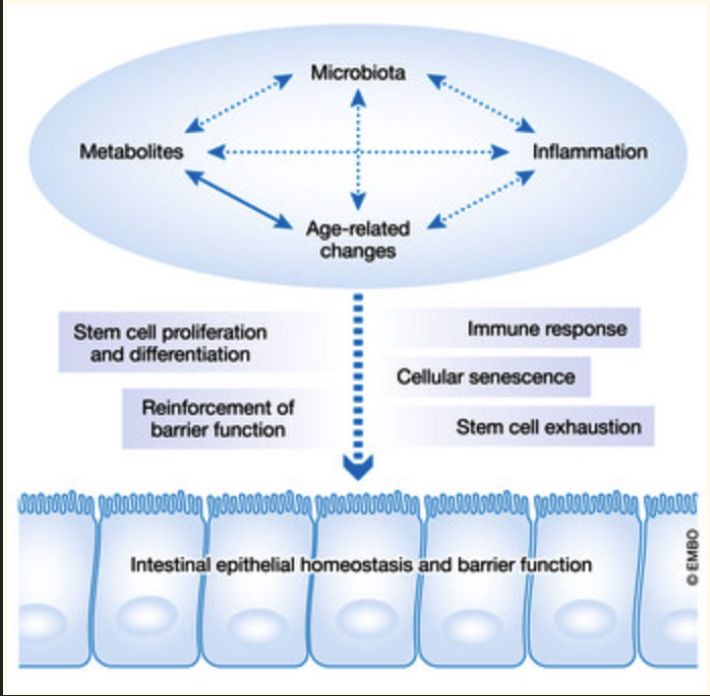
Increased permeability of the ageing gut — what changes occur?
Normal: tight epithelial barrier prevents leakage from lumen
Ageing:
Disrupted tight junctions
Epithelial cell damage/loss (enterocytes)
Impaired stem cell regeneration
Result:
Bacteria/toxins leak across barrier (“leaky gut”)
Local + systemic inflammation increases
→ Contributes to ageing-related diseases and overall decline
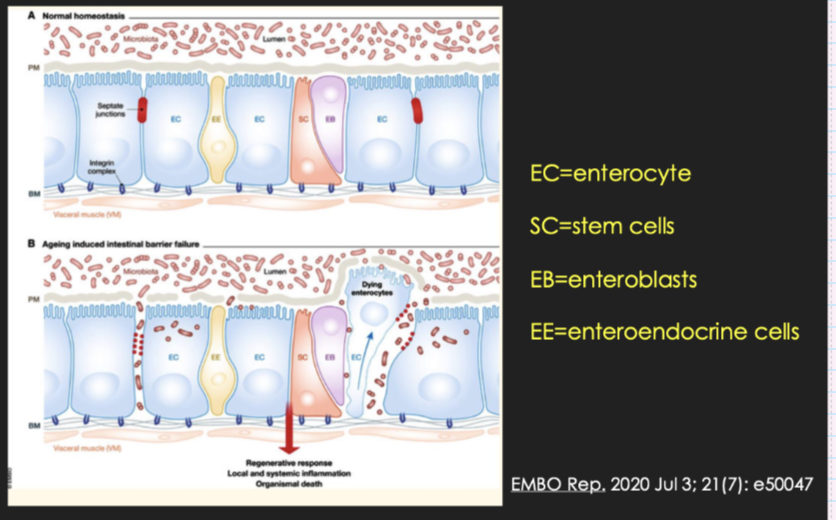
what aerobes are found in the gut
Bacteroides, Firmicutes, Prevotella, Ruminococcus
prevent the overgrowth of harmful bacteria by competing for nutrients and attachment sites to the mucus membranes of the gut
what anaerobes are found in the gut
Peptostreptococcus, Bifidobacterium, Lactobacillus, and Clostridium
prevent the overgrowth of harmful bacteria by competing for nutrients and attachment sites to the mucus membranes of the gut
how does the composition of the gut change throughout ageing
Young adults in the same geographical area have relatively similar gut microbiomes
From the mid age, their microbiome appear to progressively change, acquiring an “unique” signature in old age.
The more their microbiome have changed, the healthier the individual appeared in old age
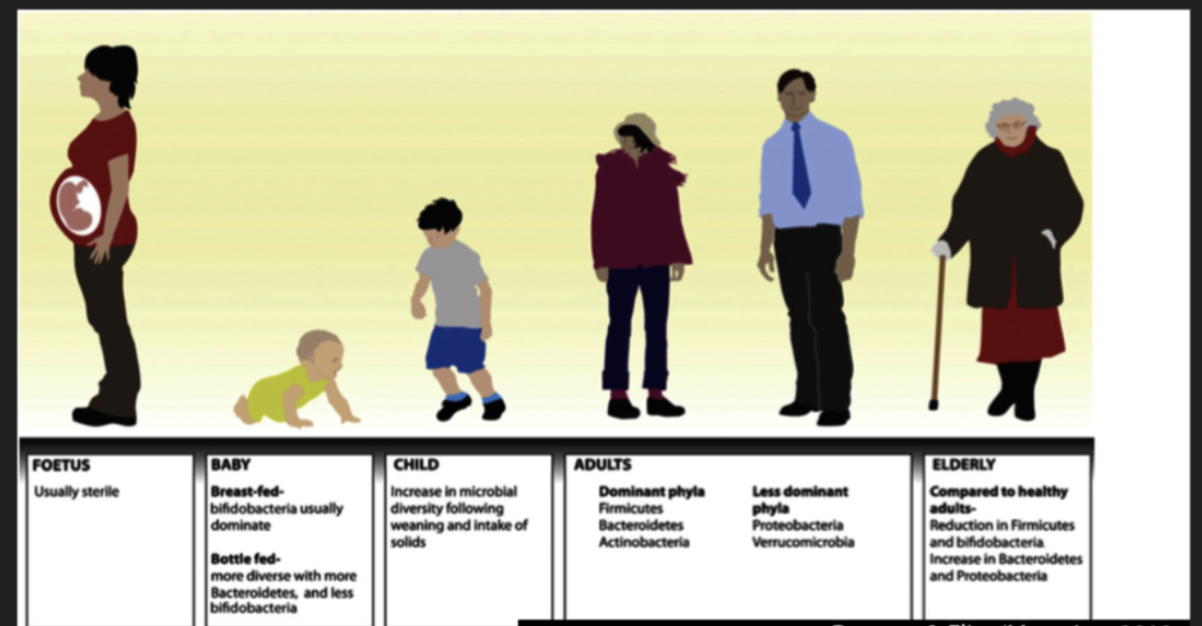
how does the microbiome of older people in poorer health produce
The microbiome of elderly people in poorer health (more medication, higher cholesterol and triglycerides, lower levels of vitamin D, less active, could not walk too fast) appeared to have changed less from the mid age, and was associated with significantly decreased survival in the course of a 4-year follow-up!
How do age-related changes in diet and microbiota affect the gut barrier?
In ageing: ↓ dietary fibre, ↑ processed food
When fibre is low: Bacteroides switch to feeding on the mucus layer
Mucus layer = protective barrier lining the gut
Result: thinning of mucus → weakened barrier
What are the downstream consequences of a weakened gut barrier in ageing?
Reduced barrier → microbes trigger immune response
Persistent activation → chronic inflammation
Chronic inflammation contributes to:
Heart disease
Diabetes
Cancer
Osteoarthritis
→ Key idea: Microbes that were beneficial earlier can become harmful in old age
Phenol metabolites in ageing — what do they indicate?
Phenols (e.g. p-cresol, phenylacetylglutamine) = gut bacterial products (from phenylalanine/tyrosine)
Associated with increased frailty in elderly (long-term care residents)
BUT phenylacetylglutamine also ↑ in centenarians & long-lived mice
→ Role is complex/context-dependent
Indole metabolites in ageing — effects?
Indoles (from tryptophan metabolism) associated with:
Improved physical function in older adults
Reduced in obese individuals
Experimental evidence:
↓ liver inflammation
Protect against colitis
→ Generally protective/beneficial metabolites
How can gut inflammation in the elderly be alleviated?
Diet changes: ↑ fibre, probiotics, complex carbs, polyphenols
Fecal microbiota transplant (FMT): beneficial effects
Oral SCFAs and other metabolites
Immune modulation:
Anti-TNF
Anti-IL-23
Regulatory T-cell therapies
Risks/limitations of microbiome-based therapies (e.g. FMT)?
May expand antibiotic resistance genes via horizontal transfer
Growth of beneficial microbes may produce metabolites that support pathobionts
→ Interventions must be carefully controlled
whera are phenols and indoles from
Phenols = gut bacterial products of phenylalanine & tyrosine
Indoles = gut bacterial products of tryptophan (measured in plasma
→ Key idea: Different amino acid-derived metabolites have distinct (context-dependent) effects on ageing and inflammation