Module 5 - SHS310
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
82 Terms
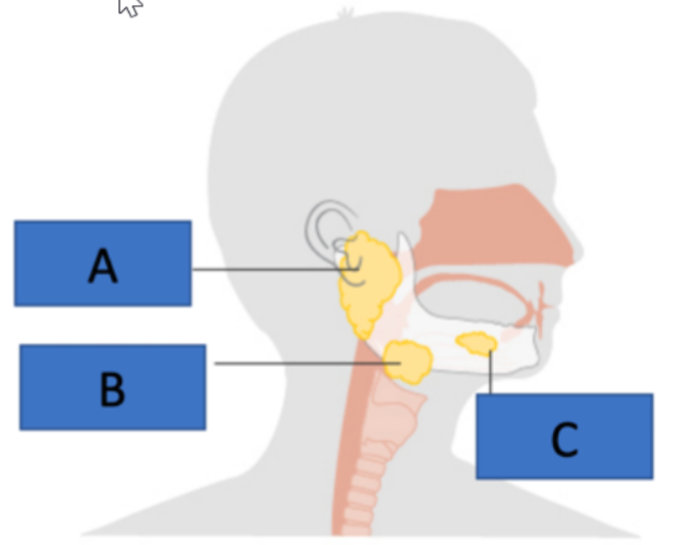
Identify all components indicated by the letters
A - parotid salivary gland
B - submandibular salivary gland
C - sublingual salivary gland
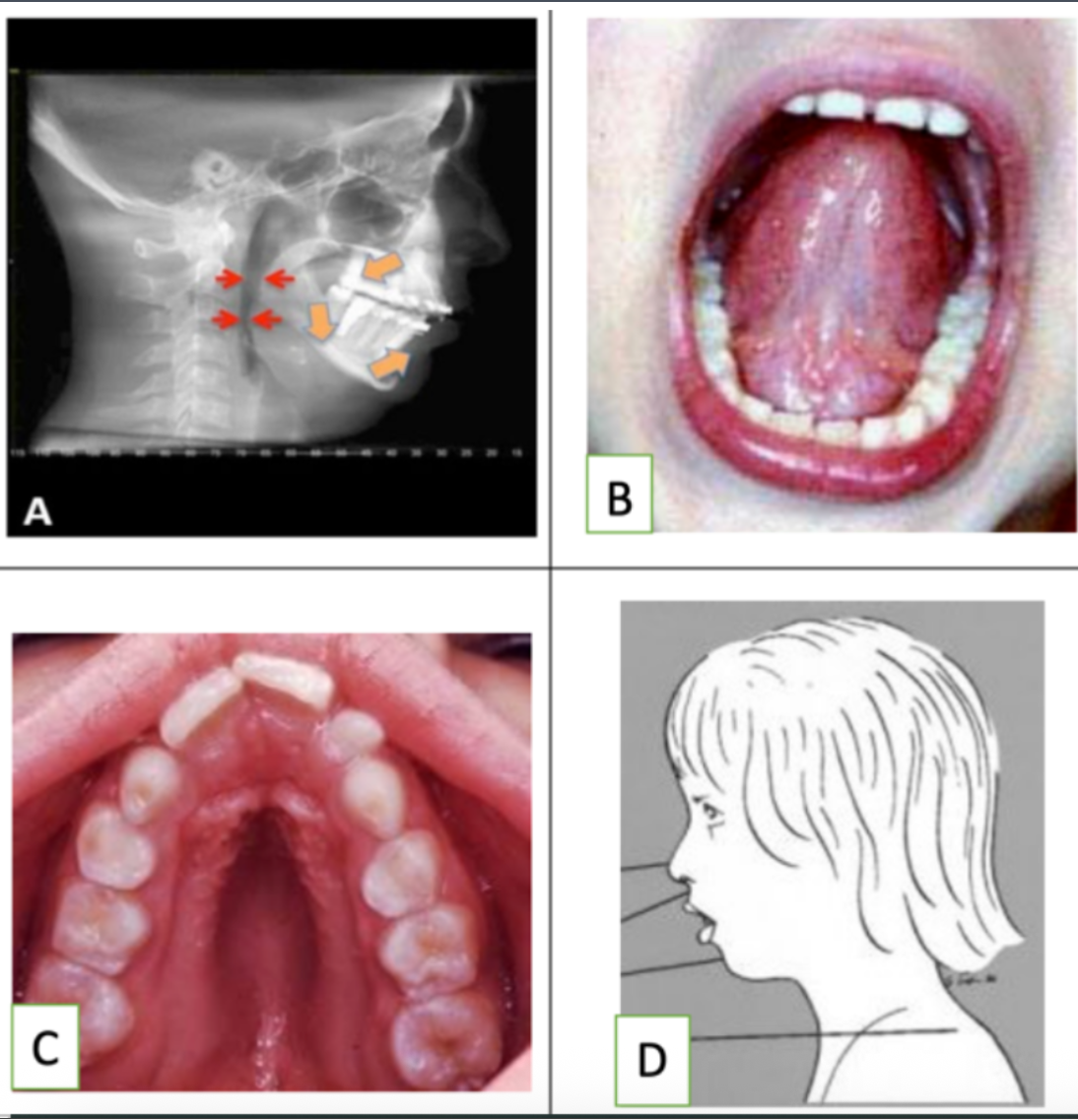
Looking at the pictures: which of the pictures show no evidence of orofacial myofunctional disorder?
B
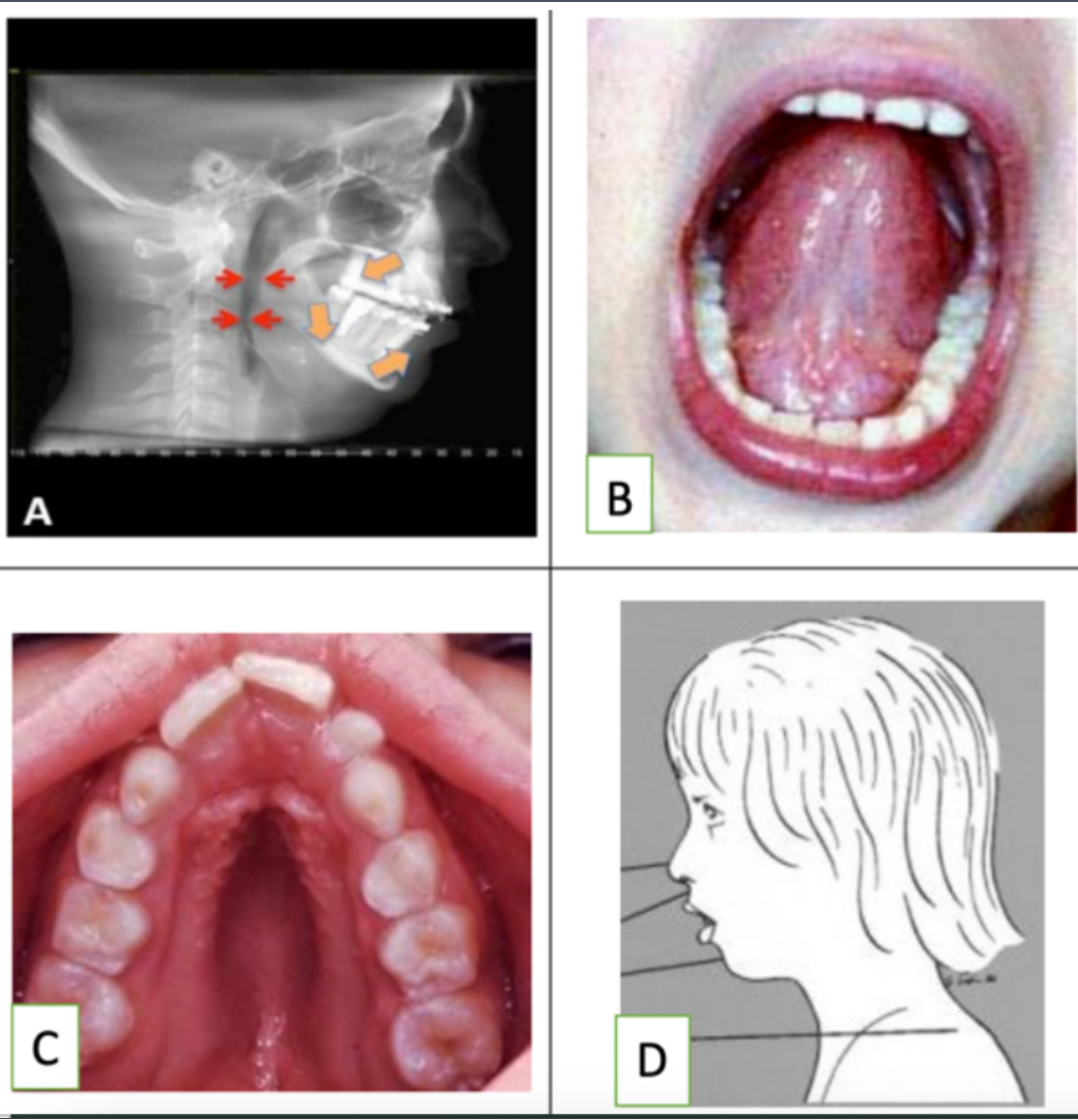
Looking at the pictures, Which of the pictures is a direct result of low tongue position in the mouth?
C
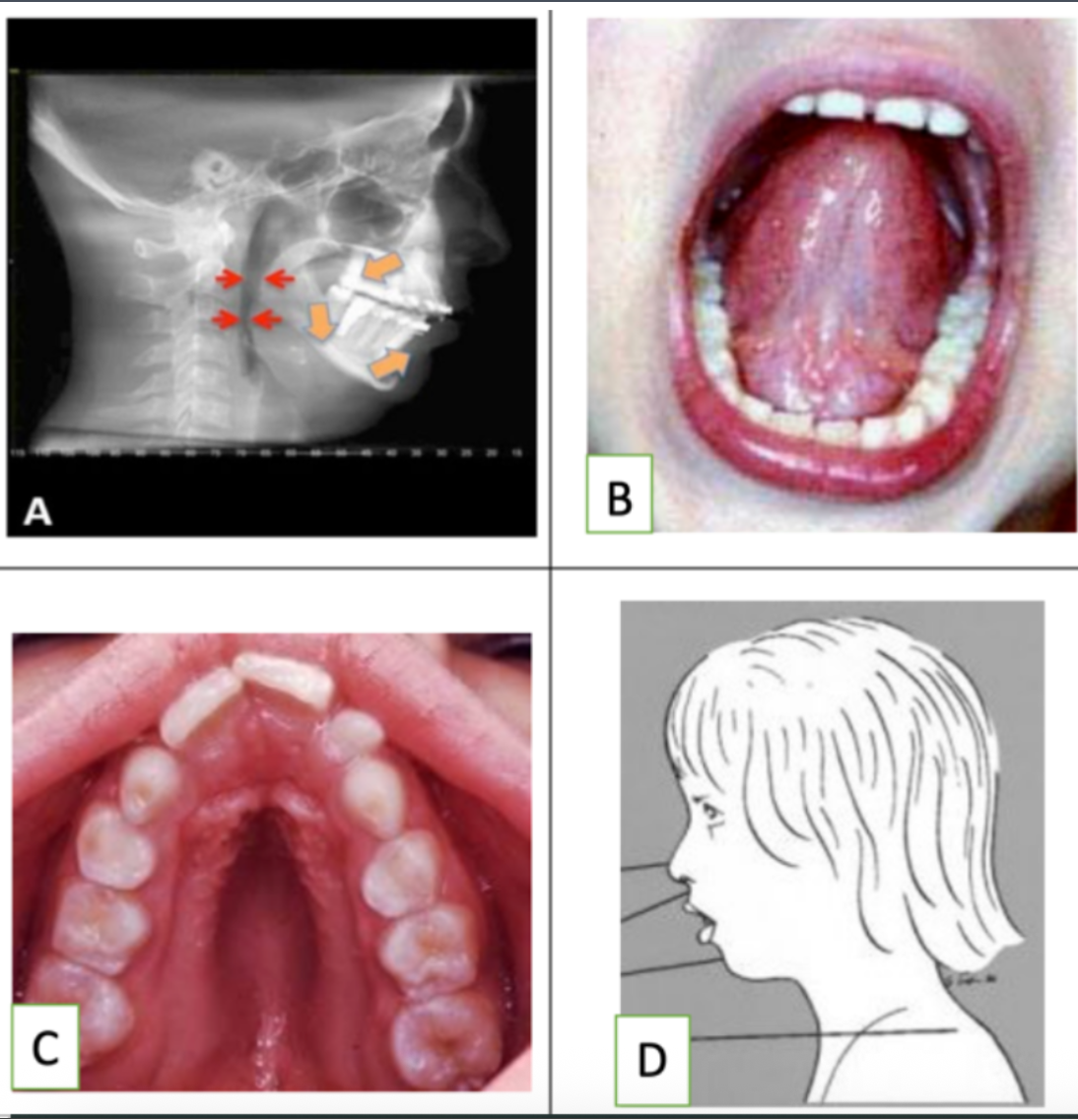
Looking at the pictures, Which of the pictures represents an individual who would be at risk for sleep apnea?
A, C, and D
What is the location and function of the parotid salivary glands?
Location - front of each ear, extending toward the cheek area
Function - produce watery saliva and provide lubrication during swallowing
What saliva is produced in the parotid gland?
Serous (watery) saliva
What is the location and function of the submandibular salivary gland?
Location - Beneath the mandible (lower jaw)
Function - Moisten the oral cavity and support bolus formation during the oral preparatory phase
What saliva is produced in the submandibular gland?
Mucoid (viscous) saliva
What is the location and function of the sublingual salivary gland?
Location - under the tongue
Function - assist in bolus cohesion and maintain oral moisture
What saliva is produced in the sublingual gland?
Mucoid (viscous) saliva
There are additional small salivary glands, where are they found and their function?
Found in the lips cheek, tongue, and palate
provide constant moisture within the oral cavity
What role does serous saliva have?
Lubricates bolus during swallowing
Helps move the bolus efficiently through the pharynx
Important for the pharyngeal phase
What role does the mucoid saliva have?
Helps form and hold the bolus together
Maintains moisture in the oral cavity
Important for the oral preparatory phase
Why is saliva important for swallowing?
Keeps the oral cavity moist
Reduces tooth decay
Begins digestion
Helps create a cohesive bolus
Provides lubrication for smooth transport through the pharynx and esophagus
What is the duration of oral preparatory phase?
~ 1 to 3 seconds
Is oral preparatory voluntary or involuntary?
Voluntary
What are the key structural positions and movement in the oral preparatory phase?
Lips seal to keep food inside mouth.
Tongue is “dished” to form a bowl for liquids.
Jaw performs mastication for solids.
Velum is down, allowing breathing while chewing.
Submandibular and sublingual glands produce mucoid saliva to form bolus.
Is the airway protection or bolus propulsion in the oral preparatory phase?
No airway closure yet. focus is bolus preparation, not propulsion
What are the pressures in the oral preparatory phase?
Oral cavity pressure is neutral; no propulsion yet
What is happening to the UES and LES in the oral preparatory phase?
UES is closed and LES is not involved yet
What is the duration of the oral transport phase?
~0.5 seconds
Is oral transport phase voluntary or involuntary?
Voluntary, but transitions into involuntary reflex triggers
What are the key structural positions and movements in oral transport phase?
Tongue tip elevates.
Tongue performs peristaltic-like movement to move bolus posteriorly.
Contact with velum and faucial pillars triggers the swallow reflex → velum elevates.
Velopharyngeal closure begins at the end of this phase.
Is the airway protection or bolus propulsion in the oral transport phase?
Airway is still limited in protection and propulsion of bolus to pharynx
What are the pressures in oral transport phase?
Oral cavity pressure becomes slightly positive to push bolus backward
What is the UES and LES doing in the oral transport phase?
UES remains closed until reflexively opened in the next phase
What is the durations of the pharyngeal phase?
~0.5 secs
Is the pharyngeal phase voluntary or involuntary?
Involuntary, controlled by the central pattern generator
What are the key structural positions and movements in the pharyngeal phase?
Airway Protection Events:
Velopharyngeal closure (velum rises).
Hyo-laryngeal elevation (hyolaryngeal complex pulled up and forward).
True vocal fold adduction.
Epiglottic inversion.
Bolus Propulsion Events:
Pharyngeal walls contract peristaltically.
Pressure generated behind the bolus.
Parotid glands produce serous saliva for lubrication.
Is the pharyngeal phase in the airway protection or bolus propulsion?
Both occur at the same time
What are the pressures of the pharyngeal phase?
High pressure generated behind bolus by pharyngeal constrictors
Low pressure created below bolus by UES relaxation
What is the UES and LES doing pharyngeal phase?
UES relaxes and opens, while LES is not involved yet
What is the duration of the esophageal phase?
8 to 20 seconds
Is the esophageal phase voluntary or involuntary?
involuntary
What are the key structural positions and movements to the esophageal phase?
UES closes after bolus passes.
Esophagus uses peristalsis to move bolus downward.
LES dilates to allow entry into stomach.
Is the airway protection or bolus propulsion during the esophageal phase?
Airway protection complete (all structures return to breathing configuration).
Primary action: propulsion via esophageal peristalsis.
What are the pressures in the esophageal phase?
Low pressure in front of bolus; peristaltic high pressure behind bolus
LES maintains high resting pressure to prevent reflux
What does the UES and LES do in the esophageal phase?
UES: relaxes then closes.
LES: opens to allow bolus into stomach; prevents gastric reflux.
What variables influence swallowing?
Bolus characteristics: consistency, volume, taste, temperature
Swallow mode: single vs sequential
Environment: mealtime eating vs clinical swallow test
Cued vs uncued swallow
What are some unique characteristics of infant swallowing
Rooting and sucking reflexes dominate feeding behavior.
Infants can breathe while swallowing because:
Velum locks into space between tongue and epiglottis
This configuration temporarily seals airway
Different anatomy:
Larger velum
More horizontal orientation
Elevated, anteriorly positioned hyoid
Elevated larynx
Infants perform 3–4 suck pumps → then swallow.
Which phases of swallowing are voluntary?
Oral preparatory phase and oral transport phase (cortically controlled).
Which phases of swallowing are involuntary?
Pharyngeal phase and esophageal phase
What is the function of the Central Pattern Generator (CPG)?
Generates pre-programmed, sequential motor commands for the involuntary phases of swallowing.
Where is the Central Pattern Generator located?
In the medulla
What is the main function of the Nucleus Tractus Solitarius (NTS)?
Acts as the sensory nucleus for swallowing—receives sensory input from CN V, VII, IX, and X.
What kinds of sensory information go to the NTS?
Taste, general sensation from the face, tongue, palate, pharynx, and larynx.
What is the main role of the Nucleus Ambiguus (NA)?
Provides motor output for swallowing—sends motor commands to muscles of the palate, pharynx, larynx, esophagus, lips, jaw, and tongue.
Which nucleus triggers the motor sequence of the swallow?
Nucleus Ambiguus (NA), based on CPG commands.
Which nucleus integrates sensory input to initiate the swallow reflex?
Nucleus Tractus Solitarius (NTS)
Which cranial nerves send sensory input to the NTS?
CN V, VII, IX, and X
Which cranial nerves receive motor output from the NA for swallowing?
CN V, VII, IX, X, and XII
What happens once the swallow is triggered?
The CPG automatically coordinates and completes the pharyngeal and esophageal phases.
What is the definition of dysphagia?
Difficulty in swallowing secondary to paralysis or paresis, typically affecting the pharyngeal phase.
Which phase of swallowing is most affected in dysphagia?
The pharyngeal phase
What are “tethered oral tissues”?
Another term for restricted frenum or tongue tie—a condition where the lingual frenulum is too tight or short.
How do tethered oral tissues affect swallowing?
They prevent the tongue tip from lifting to the alveolar ridge, disrupting the normal peristaltic tongue movement needed for the oral transport phase.
What swallowing problems can tethered oral tissues cause in infants?
Difficulty breastfeeding because the baby cannot extend the tongue properly.
How does a restricted frenum affect bolus movement?
The tongue stays low and forward, leading to anterior tongue carriage and inefficient oral transport.
What is the Modified Barium Swallow (MBS)?
An evaluation conducted by an SLP to assess the pharyngeal phase of swallowing using X-ray imaging.
What is FEES (Fiberoptic Endoscopic Evaluation of Swallowing)?
A swallow evaluation performed by an SLP working with a physician, where a small camera is inserted through the nose to visualize pharyngeal structures during swallowing.
Which provider gives the medical diagnosis during FEES?
The physician (M.D.); the SLP describes the swallowing function.
What is a Barium Swallow (Esophagram)?
An evaluation performed by a gastroenterologist to assess the esophageal phase of swallowing.
Which swallow evaluation is used to examine the esophageal phase?
The barium swallow
Which evaluations are conducted by an SLP?
Modified Barium Swallow (MBS)
FEES (in collaboration with a physician)
What is an Orofacial Myofunctional Disorder (OMD)?
A disorder of muscle function of the face and mouth, primarily involving abnormal tongue placement and difficulty in the oral preparatory and oral transport phases of swallowing.
What are other names for OMD?
Tongue thrust, immature swallow, reverse swallow, anterior tongue carriage.
What oral phases of swallowing are affected in OMD?
Oral preparatory and oral transport phases.
What are the main categories of causes of OMD?
Oral habits
Restricted frenum (tongue tie)
Adaptation to restricted airway
How do oral habits cause OMD?
Objects in the mouth (pacifiers, thumbs, sippy cups) prevent oral closure and push the tongue forward.
How does a restricted frenum cause OMD?
Prevents the tongue tip from raising to the alveolar ridge, leading to anterior tongue carriage and disrupted tongue peristalsis.
How does airway obstruction cause OMD?
The tongue moves forward to enlarge the airway, resulting in low, anterior tongue posture and open-mouth breathing.
How is OMD connected to mouth breathing?
Low or forward tongue posture opens the mouth, leading to habitual mouth breathing and altered facial development.
How is OMD connected to posture?
Mouth breathers often adopt a forward head posture to open the airway.
How does OMD influence facial growth?
Low tongue posture removes the tongue’s “retainer” effect, causing:
High, narrow palate
Decreased nasal cavity volume
Elongated lower face
Receded chin
Short upper lip
How is OMD related to sleep apnea?
Without proper tongue anchoring, the tongue can fall backward during sleep, contributing to sleep-disordered breathing or obstructive sleep apnea.
How does OMD affect speech?
Causes dentalized or interdental /s, z/ due to anterior tongue carriage; same structures needed for proper swallowing.
What are common characteristics of OMD?
Forward tongue position
Tongue thrust during swallowing
Open-mouth posture
Difficulty creating lip seal
High, narrow palate
Scalloped tongue
Thumb/pacifier habits
Restricted frenum
How do these characteristics impact function?
Tongue thrust: inefficient swallow, orthodontic issues
Open-mouth posture: mouth breathing, facial changes
Low tongue posture: altered palate and nasal cavity
Restricted frenum: impaired breastfeeding, disordered swallow
Scalloped tongue: chronic pressure against teeth
Habits: reinforce improper oral posture
What visual signs help identify OMD in photos?
Open-mouth rest posture
Visible tongue during /s/ and /z/
Narrow or V-shaped palate
Receded chin
Elongated lower face
Pursed lips when swallowing
Scalloped tongue edges
Anterior tongue resting position
What does OMD therapy (OMT) aim to accomplish?
Retrain muscle patterns
Establish proper swallow pattern
Correct tongue resting posture
Improve nasal breathing
Reduce oral habits
Support orthodontic treatment
Improve speech affected by tongue placement
Improve airway stability (related to sleep apnea)
Which professionals treat OMD?
SLPs trained in OMD
Certified Orofacial Myologists (COM)
Orofacial Myofunctional Therapists
Dentists/Orthodontists
Oral hygienists (RDH)
Nutritionists (in some cases)
Can all SLPs treat OMD?
No—ASHA requires additional training to treat OMD.