Postural Control In Standing
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
Force of gravity
fundamental force of attraction between any two objects that have mass or energy
Center of gravity (COG) or center of mass (COM)
point where the weight is evenly distributed on all sides, so you have good balance
at your sacral tube(?)
will change with height
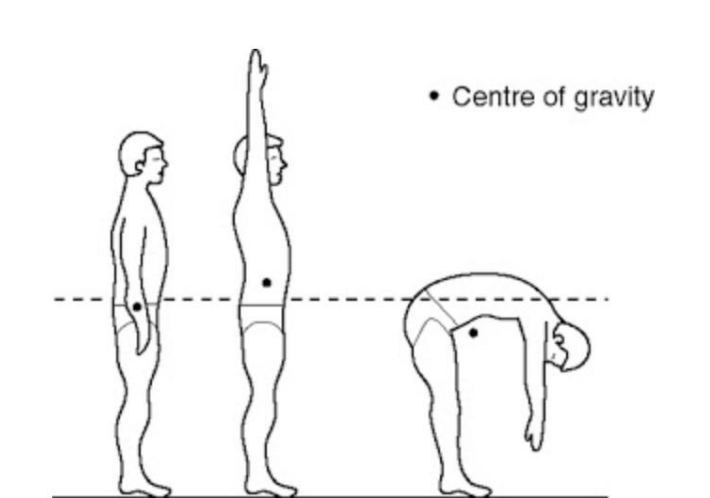
Line of Gravity
an imaginary, vertical line that extends down from an object's center of gravity to the supporting surface; it represents the direction and line of action of the force of gravity acting on an object
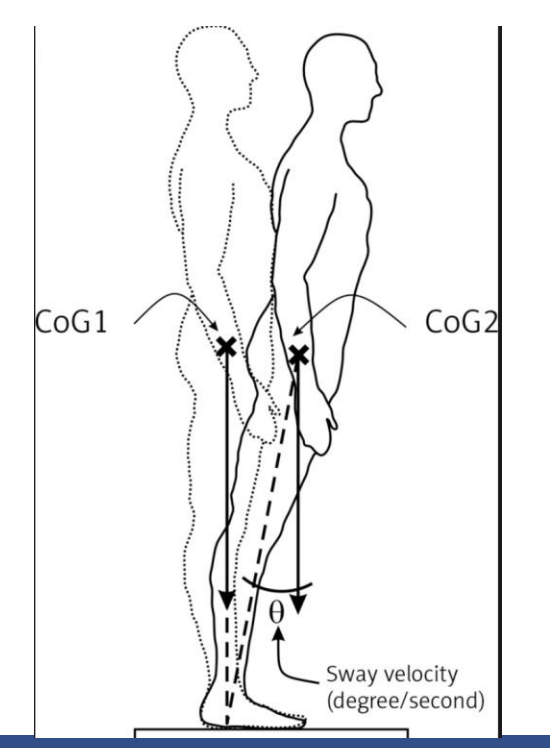
Balance
the ability to control your center of gravity over your base of support
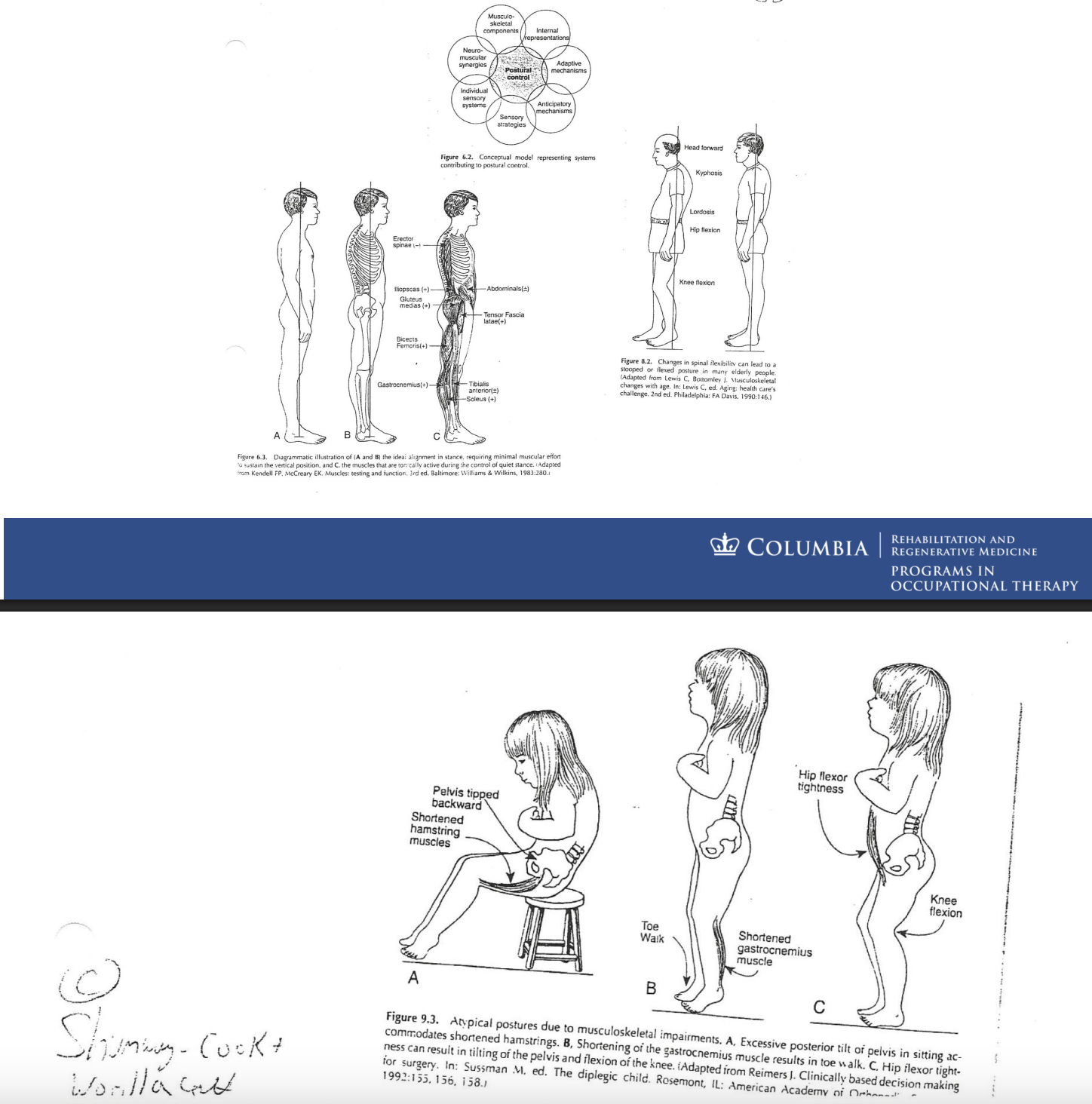
Posture
maintained position of alignment in any position of task
Limits of Stability
actual vs perceived
actual
actual balance is better than what the person perceives
person thinks their balance is not great, but it’s actually better
e.g., person does not have confidence in balance and won’t attempt their daily activities
less safety concerns because the person is not taking chances
perceived
the opposite of ^; actual balance is worse than what the person perceives
person thinks their balance is really good, but it’s actually worse
e.g., person keeps trying to get up and walk when they are not ready
more safety concerns because the person is more impulsive; they need grounding and safety education
Postural set
postural readiness (when doing something)
e.g., when presenting infront of a class, a person will have 2 feet planted shoulder width apart, with head and trunk up (prevents them from falling over)
CNS Integration of Information
Cerebellum
integrating info for postural control + any adjustments
plays a role in balance
Basal Ganglion
plays a role in balance
disorder —> e.g., Parkinson’s
== rigidity, bradykinesia, tremors
Brainstem
integrates vestibular info and initiates compensatory eye movements
plays a role in balance
Sensory organization that supports upright function
Vision
used to track and navigate through the environment
vertical, horizontal, rotational
peripheral
can be tricked (by illusions)
Proprioception/somatosensory
e.g., if you have peripheral neuropathy in your feet, you cannot feel where you are walking; this affects feedback to our proprioception and subsequently balance
Vestibular
helps to determine head position
you have semicircular canals (functional when shaking or nodding your head)
you have otoliths for linear movement
stabilizes gaze
probably used the least out of everything here
Sensory Strategy
Postural Control in Standing
Diagnosis
e.g., stroke, TBI, MS, Guillain-Barré
Goals of postural control in standing
Postural reactions
Restore equilibrium (i.e., getting your balance back)
Synergistic movements (i.e., movements don’t occur in isolation; e.g., hips and ankles will probably move at the same time when regaining balance)
Automaticity (i.e., restoring balance without being aware of doing it- subconsciously)
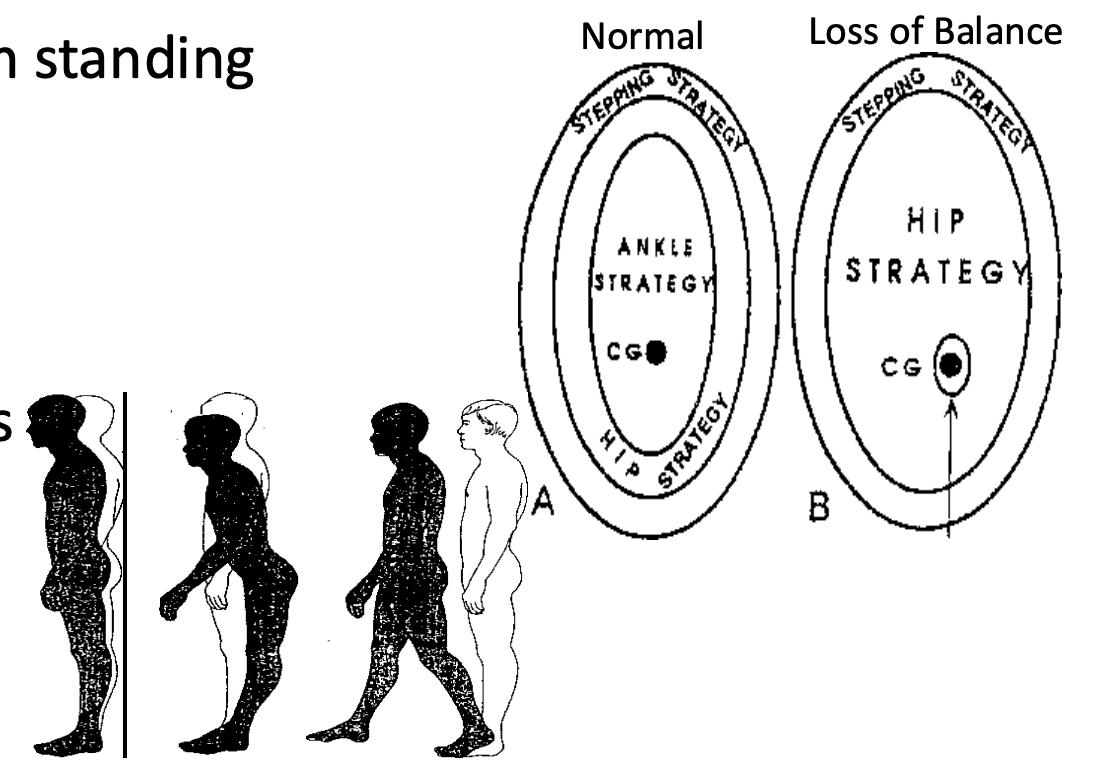
Types of postural reactions
Ankle
a little sway to keep balance, with toes/heels pointing forward/back
Hip
coming forwards/backwards (flex/extend) and side-to-side
Stepping
increasing the base of support by widening
e.g., taking a step when the subway gets you off balance
Evaluation
Observation
look for physical signs
e.g., are they standing shoulder-width apart? is their head in midline? is one shoulder higher than the other? is one hip higher than the other?
look for balance issues
e.g., using their environment to help them (e.g., wall walking), overuse of arms (e.g., holding onto things), getting external support (e.g., leaning against items), too wide a base of support, stiffening or guarding (b/c they are nervous of falling), taking small steps (b/c they are scared to take bigger strides)
Subjective Interview
Premorbid health hx
Prior level of function
e.g., goal will not be to stand if the patient originally presented in a wheelchair
Perspective of current functioning
Neurologic
e.g., stroke locations and lesion locations could mean different things for balance
Non-Neurologic
e.g., ROM and strength of LE, any orthopedic conditions, any cardiac conditions (which could affect standing and endurance)
Component Evaluation
Physical Status
Coordination
static and dynamic
sitting and standing
Gait
Vertigo & Dizziness
e.g., peripheral vertigo if it’s in the inner ear (BPPV)
small particles get dislodged from their normal location in the inner ear and enter the semicircular canals, causing an abnormal sensation of spinning; there are positions you can put your head into to move these particles back into their proper place
Balance
BOS (base of support)
small, large?
Limits of stability
real vs. perceived
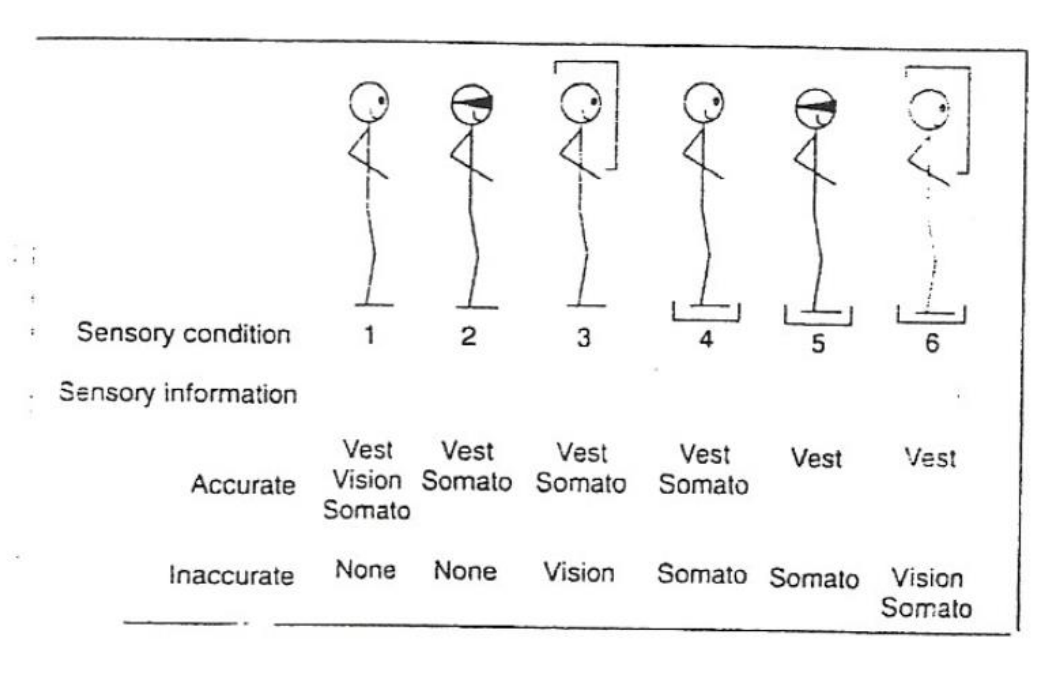
Clinical Test of Sensory Interaction and Balance
see what their balance is like when…
when standing upright on a flat surface
when standing upright on a flat surface w/ eyes closed
getting rid of their vision
if they’re having problems with this, it’s likely that they are over-relying on their vision
when standing upright on a flat surface w/ a dome over a person’s head
not getting rid of their vision, but their vision is not accurate
if they’re having problems with this, it’s likely that they are over-relying on their vision
when standing upright on an unbalanced surface
when standing upright on an unbalanced surface w/ eyes closed
when standing upright on an unbalanced surface w/ a dome over a person’s head
Balance grading
Functional Measure (standardized)
Berg Balance Scale (BBS)
vestibular disorders, stroke, SC, pulmonary disorders, PD, Osteoarthritis, older adults, limb loss/amputation, brain injury
14 items, 0-4 Likert scale, 15-20 minutes, no formal training needed
Higher scores mean better performance
Older adults: <45 greater risk of falls
Timed Up and Go (TUG)
vestibular disorders, stroke, spinal cord, PD, older adults, Osteoarthritis, AD, progressive dementia, brain injury
1 item with use of assistive device if needed (sit in chair, stand up, walk 3 meters, turn, walk back, and sit down); < 3 min, no formal training
Older adults: >12 seconds is a risk of falls
Functional Reach Test (FRT)
vestibular disorders, stroke, SC, PD, older Adults
Patient stands next to the wall, but not touching, with the arm closer to the wall, with the shoulder 90 degrees, with the fist (with a yard stick parallel to the floor), measure from the 3rd metacarpal, and say “reach as far as you can forward without taking a step”, then record the location of the 3rd metacarpal
5 trials- 2 practice then average last 3.
Older adult in community dwellings: <7 inches (unable to leave neighborhood without help, limited mobility skills, most restricted in ADLS)
Tinetti Performance Oriented Mobility Assessment (POMA) or TMT (Tinetti mobility)
Balance and gait sections
stroke, older adults, ALS
TASK ANALYSIS!; make note of…
Simple to complex
e.g., adding bilateral coordination and crossing midline
Combination & weighting of physical and cognitive skills
e.g., trying activities that require more cognition (IADLs > ADLs)
Environmental factors
e.g., what surfaces will they be walking on at home (e.g., carpet, hardwood, rug, etc.)?, how much light is there in the home?, what kinds of environmental obstacles are there?
generally, should also try to replicate the home as best as possible
Fatigue
e.g., having trouble maintaining their balance, shakiness, having trouble breathing, leaning/holding onto things for support
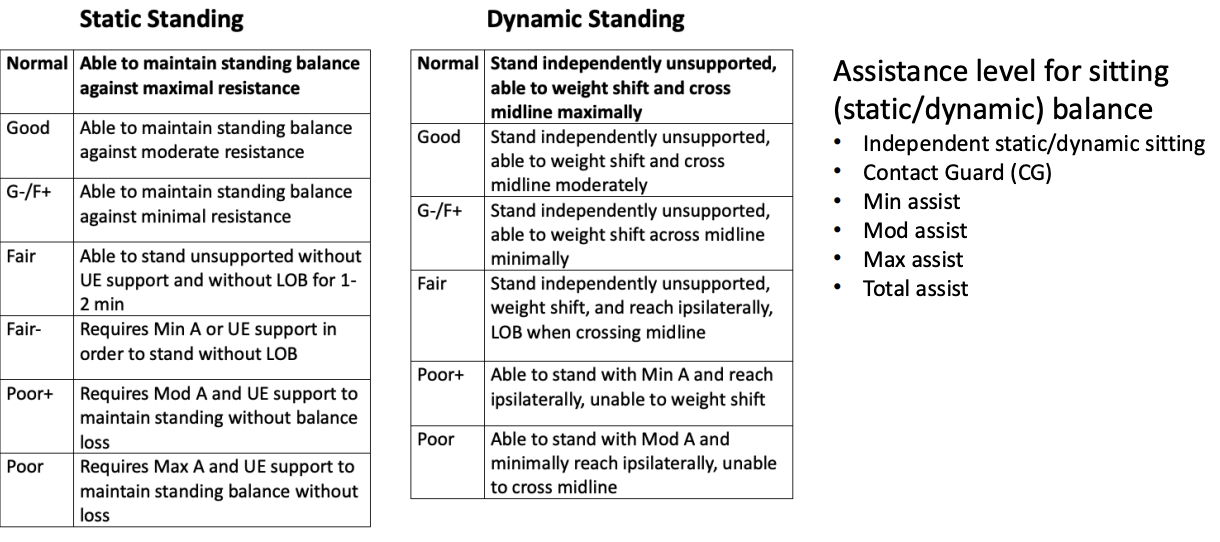
Balance Grading Review
Assistance level for sitting (static/dynamic) balance
Independent static/dynamic sitting
Contact Guard (CG)
touching for reassurance and support
Min assist
Mod assist
Max assist
Total assist

Berg Balance Scale (BBS)
performance-based test that assesses a person's static and dynamic balance through 14 tasks
each task is scored on a scale from 0 (unable to perform) to 4 (normal performance), with a total possible score of 56
scores below 45 may indicate a higher risk of falling in older adults, while a score of 45 or above suggests good balance

Timed Up and Go (TUG)
quick assessment of an individual's balance and functional mobility, commonly used for older adults and those with neurological conditions
to perform the test, a person stands up from a chair, walks three meters, turns around, walks back to the chair, and sits down
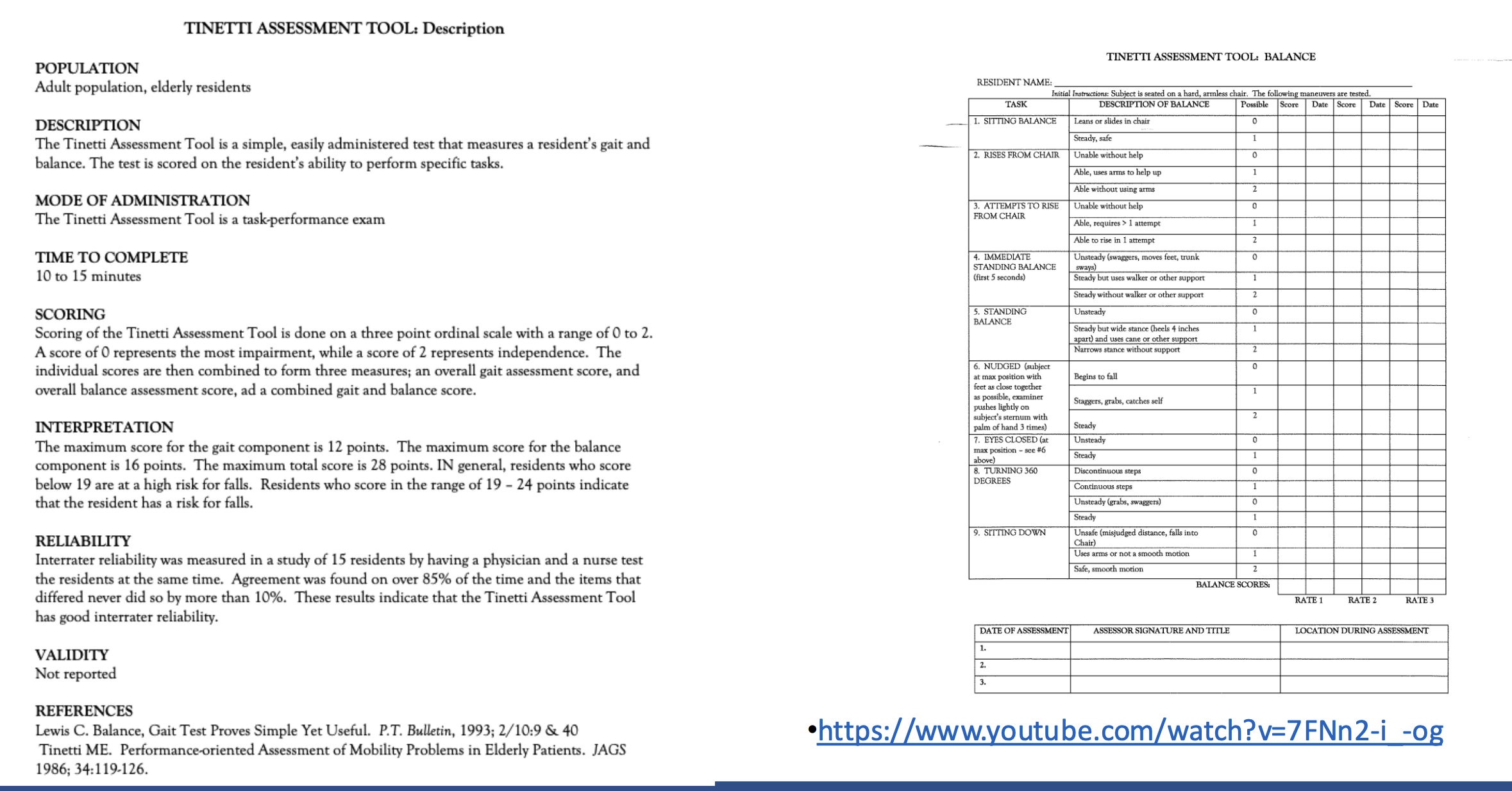

Tinetti Performance Oriented Mobility Assessment (POMA) or TMT (Tinetti mobility)
What the test assesses
Balance: Evaluates the ability to maintain balance in various situations, such as sitting, standing, and turning
Gait: Measures a person's walking pattern, including step length, foot clearance, and step symmetry
How it's scored
Each item is scored on a three-point scale, from 0 (highest impairment) to 2 (independence)
The total score combines the balance and gait scores
The maximum possible score is 28, with a maximum of 16 for the balance section and 12 for the gait section
Task Analysis