Heart Anatomy (External and Internal)
1/73
Earn XP
Description and Tags
mrs. garcia said the nervous system was the hardest but ts is definitely the hardest unit like why tf is the heart so GODDAMN COMPLICATED GRRRRRR
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
74 Terms
Heart Location and Other Facts
the heart is a hollow muscular organ about the size of a closed fist located between the lungs
the apex (tip) of the heart is pointed towards the left hip
contracts about 72 times per year
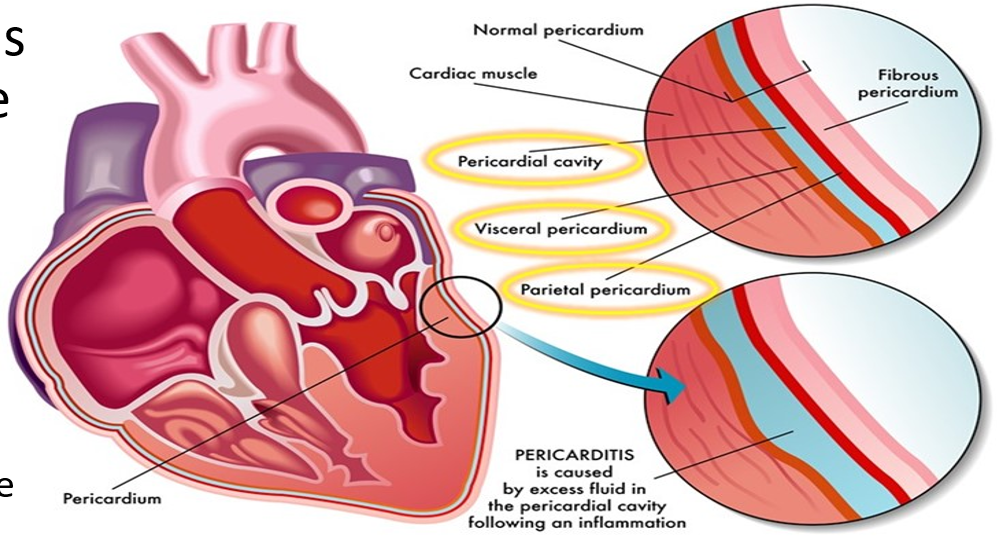
Pericardium
a protective layer of tissue protecting the heart
Layers of Pericardium (Superficial to Deep)
Fibrous Pericardium - provides protection and anchors the heart in place
Serous Pericardium - provides lubricating fluid which collects in the pericardial cavity to reduce friction of the heart against other tissues
Parietal Pericardium (superficial to the pericardial cavity)
Visceral Pericardium (deep to the pericardial cavity)
2 Cardiovascular Circuits
Pulmonary Circuit (oxygenating blood)
Systemic Circuit (distributing to body tissues)
Pulmonary Circuit
carries blood from the heart to the lungs and back
picks up O2 and released CO2
Major Blood Vessels involved in this Circuit:
pulmonary trunk (splits into right and left pulmonary arteries)
pulmonary veins
Systemic Circuit
carries blood from the heart to the body tissues and back
drops of O2 and picks up CO2
Major Blood Vessels involved in the Circuit:
Venae Cavae (superior and inferior)
Aorta
Chambers of the Heart
4 chambers:
2 atria (right and left atriums) (receive blood) (on top)
2 ventricles (right and left ventricles) (pump blood out) (on bottom)
Left Side of the Heart: receives oxygenated blood from the pulmonary veins
Right Side of the Heart: receives de-oxygenated blood from the body tissues
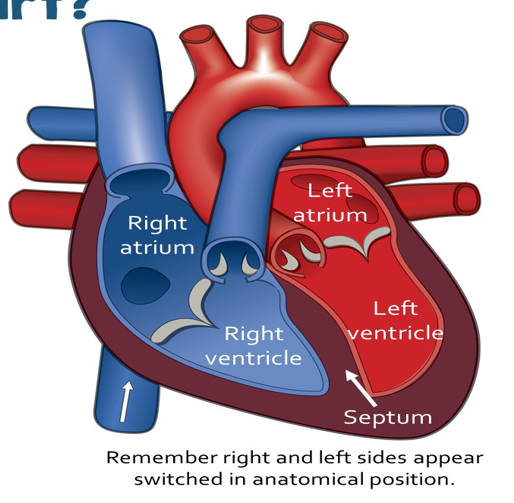
Septum
The barrier in the middle to prevent the oxygenated and de-oxygenated blood from mixing.
Superior Vena Cava
returns blood to heart from the upper body (blue)
Inferior Vena Cavae
returns blood to heart from lower body (blue)
Right Atrium
receives de-oxygenated blood from body tissues
covered by auricle (the blobby tissue you actually see)
Left Atrium
receives oxygenated blood from the lungs
covered by auricle (the blobby tissues you actually see)
Pulmonary Veins
brings oxygenated blood from lungs
although it transports oxygenated blood (making it show up as red on a heart diagram), it is classified as a vein as it is bringing blood to the heart which is what veins do
Pulmonary Arteries
carries de-oxygenated blood to the lungs to pick up oxygen
although it transports deoxygenated blood (making it show up as blue on a heart diagram), it is classified as an artery because it is moving blood away from the heart
Coronary Blood Vessels
provide oxygen to the heart itself
veins (blue), arteries (red)
Right Ventricle
receives de-oxygenated blood from the right atrium
Left Ventricle
receives oxygenated blood from the left atrium
Aorta
takes oxygenated blood to the body tissues
Apex
tip of the heart (pointed to the left hip)
Valves
flaps of tissue that prevent blood from flowing backwards
like a set of swinging doors
the opening and closing of these things are what make the heartbeat sound
Atrioventricular Valves
between atria and ventricles
tricuspid and bicuspid/mitral valves
Tricuspid Valve
valve that have 3 flaps of tissue
can be found in between right atrium and right ventricle
Bicuspid Valves
valve that have 2 flaps of tissue
can be found in between left atrium and left ventricle
Semilunar Valves
prevents backwards flow into the heart
pulmonary valve: between left ventricle and pulmonary vein
aortic valve: between right ventricle and aorta
Systole
contraction of heart chambers (atrim and ventricle)
Diastole
relaxation of heart chambers (atrium and ventricle)
The Cardiac Cycle
changes in pressure in heart chambers opens and closes valves, which create the cycle
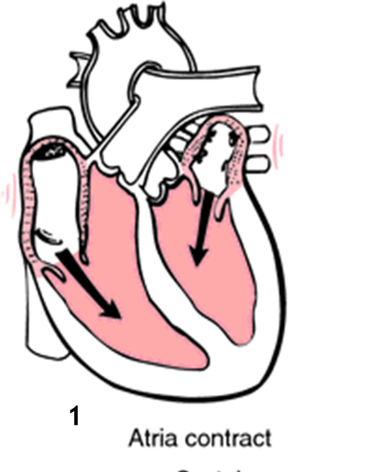
Atrial Systole
Movement of Blood: into the ventricles
Ventricles are relaxed, Atria are contracted
AVs are open, SLs are closed
Atrial Diastole/Ventricle Systole
Movement of Blood: from ventricles into the pulmonary vein/aorta
Atria are relaxed, Ventricles are contracted
AVs are closed, SLs are open
Isovolumentric Contraction
this is the step between atrial systole and ventricular systole
this is when the ventricles contract to increase pressure to open the semilunar valves, but they do this in a way that dosent affect blood volume (so not actually squeezing anything out)
Cardiac Conduction System
the heart is autorhythmic, meaning that it contracts by itself without external nervous system stimulation
the heart contains specialized cells that generate and distribute cardiac cell impulses
SA Node (Sino-Atrial Node)
Pacemaker of the heart (since it starts the cardiac impulses)
located in the right atrium (ONLY THE RIGHT ATRIUM) near the superior vena cava
it initiates rhythmic contractions and contracts the atria
(the impulse travels to the left atrium through interatrial pathways called Bachmann’s bundles and contracts the left atrium at the same time as the right atrium)
AV Node (Atrio-Ventricular Node)
located in the superior part of the septum
controls timing of contraction between atria and ventricles
delays signal
(delaying the signal is important because this delay allows the ventricles to be filled up with blood (after the atria contract) before they contract and send the blood to their respective locations)
AV Bundle
connects the atria to the ventricles
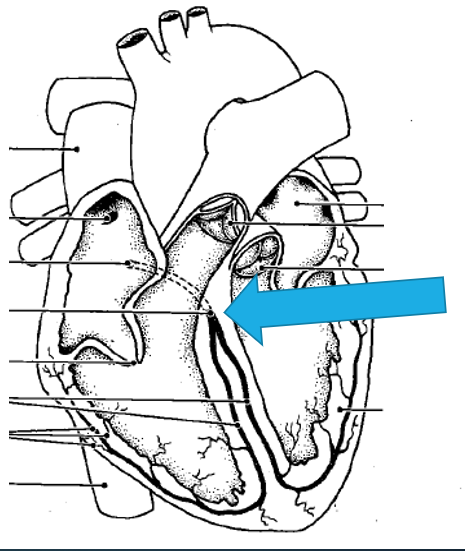
Bundle Branches
travel through the septum to the left and right sides of the heart
basically when the AV bundle splits, it splits into the right and left bundle branches
Purkinje Fibers
branched network that stimulates the myocardium to contract the ventricles
EKG
a measurement of electrical activity and impulses created by the heart
EKG or ECG
electrodes are placed on the chest and each impulse is translated into a wave pattern
What do the EKG Lines mean?
flat lines: no electrical activity
upward spikes: depolarization
downward spikes: repolarization
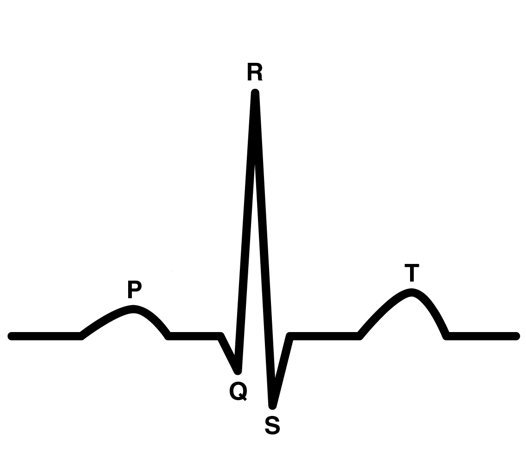
P Wave in EKG
depolarization of the atria (which causes the atria to contract)
Gap Between P Wave and Q Spike
This is the delay in electrical signal caused by the AV Node
QRS Wave/Complex
caused by the depolarization of ventricles and repolarization of atria
this wave is much bigger than the P wave because the ventricles are bigger than the atria
Gap Between QRS Complex and T Wave
the completion of ventricle depolarization
T Wave
this is caused by the repolarization of ventricles (resting of ventricles)
Video Review!!
review the video notes in my onenote page about the cardiac cycle
Types of Blood Vessels
arteries, veins, capillaries
Branching out of the Blood Vessels
Arteries are huge and carry blood away from the heart to the body
the arteries pass the blood onto smaller arterioles
the arterioles pass the blood to even smaller capillaries
in the tiny capillaries, the walls of the capillaries are so thin that gases (O2 and CO2) in the blood can be exchanged with tissues in these capillaries
after dropping off O2 and picking up CO2, the capillaries collect blood into larger venules
the venules collect into larger veins which return the blood to the heart
Structural Differences between Arteries and Veins (and Capillaries i guess….)
Capillaries only have 1 layer of cells surrounding them, allowing for easy exchange of gases
Arteries and Veins are both bigger than capillaries and both have 3 layers: (superficial to deep)
Tunica Externa (or Tunica Adventitia): fibrous connective tissue to protect and support the blood vessel
Tunica Media: thicker layer of muscle
Arteries have much thicker layers of tunica media than veins, letting them retain their circle shape much better than veins
Tunica Intima: slippery, thin layer
Arteries are more flexible than veins because they receive blood from the heart at high pressures
Veins have thinner walls and receive blood from tissues in low pressures
3 Ways Veins Maintain Blood Flow under Low Pressues
Muscular Pumping: as muscles contract, blood is squeezed through the veins
Respiratory Pumping: the expansion of the chest during inhalation causes blood in the veins to move
Valves: larger veins have valves inside to prevent backflow of blood
Capillary Structure
Capillaries contain of two portions:
Shunt: a shortcut from the artery to the vein (the highlighted portion)
True Capillaries: all the tiny portions that exchange gases with the tissues
Between the arterioles and the shunt are sphincters which can restrict the flow of blood to the tissues when blood is needed elsewhere (like if you are in fight or flight mode)
Pulse
expansion of the heart wall
Pulse = rate of contraction of the left ventricle
Normal Rate: 60-100 bpm
Pulse Measurement
Commonly at radial (near wrist), brachial (near elbow), or carotid (near neck) arteries
use index and middle finger for pulse not thumb (bc you can feel your thumb’s pulse and it might mess up the count)
Normal Systolic and Diastolic Values
Systolic: max 120
Diastolic: max 80
Hypertension
above 140/90
tension can cause tears in the blood vessels which will accumulate cells that can block blood flow in the heart (coronary) or brain (stroke).
symptoms: (although sometimes not visible) headache, dizziness, shortness of breath, feeling of pulsations in the head or neck
caused by: high sodium intake, arteriosclerosis, atherosclerosis, obesity, renal problems
results in: damage to arterial walls (aneurysm) , damage to coronary arteries, left ventricular hypertrophy, heart failure, stroke
Medications for Hypertension
Angiotensin - Converting Enzyme Inhibitors/Blockers: angiotensin-2 is a hormone that narrows blood vessels. this treatment inhibits this hormone, which lets blood vessels not be constricted, reducing blood pressure
Calcium Channel Blockers: this keeps calcium from coming into the muscle cells of your heart, allowing blood vessels to relax, lowering your BP
Diuretics: increases urine output, lowers blood volume
Hypotension
Less that 90/60
Symptoms: lightheadedness, dizzyness, fainting (syncope), angina (pressure/pain in heart), shock
Caused by: change my body position, decreased blood volume, medications
Results in: low blood volume to the organs, brain/heart/kidney damage
Blood Pressure and Arterioles
BP dramatically decreases in the arterioles
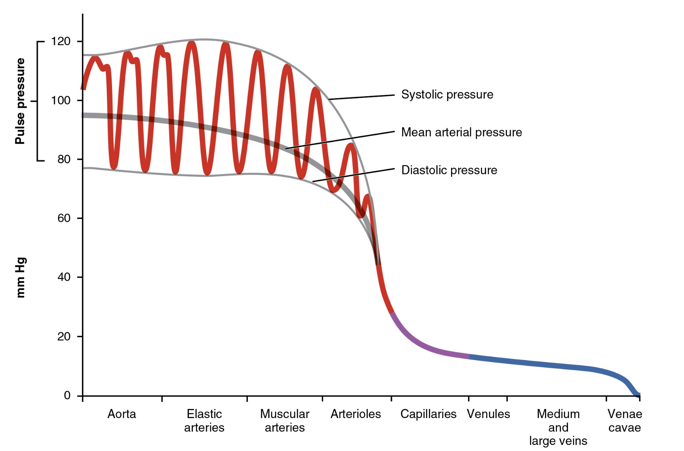
Perfusion
french verb perfuser: pour over or through
passage of blood through circulatory system to an organ or tissue
measured at the rate which blood is delivered to tissue
Factors that Affect Blood Pressure
blood volume
cardiac output
peripheral resistance
Blood Volume Factor
greater blood volume → more fluid to press on the walls of the arteries → resulting in greater pressure
sweating/blood loss/dehydration: temporarily reduces blood volume/pressure
high sodium/salt diet: increases water retention → increases blood volume therefore increase in BP
Stroke Volume
volume of blood ejected from each ventricular contraction
average SV for a male: 70mL
Cardiac Output
volume of blood ejected per minute
Cardiac Output: SV x BPM = mL/BPM
Sympathetic and Parasympathetic NS
Sympathetic - increases HR, cardiac output, and SV
Parasympathetic - decreases HR, cardiac output, and SV
Sympathetic NS and Systolic BP
SNS controls proprioceptors (stretch/tension) in joints or muscles send signals which cause an inc in HR
causes an increase in systolic BP ONLY, not diastolic
also causes vasodilation of blood vessels in the muscles and the skin to increase blood flow
Cardiac Hypertrophy
increase in heart muscle and enlargement of the muscle fibers
benefits of exercise: increases SV and allows the heart to pump more slowly
Trained Athletes: 60% greater ventricular mass than normal people
Hypertrophic Cardiomyopathy
enlargement of the muscle fibers → ventricle walls thicken → blocks blood flow out of the ventricle
can be inherited, develop (due to high BP), or caused by a disease (thyroid, diabetes)
Peripheral Resistance
blood vessel diameter
blood viscosity
vessel elasticity
Blood Vessel Diameter
larger diameter = less pressure
vasoconstriction vs vasodilation
regulated by sympathetic nerve fibers
Blood Viscosity
thickness of the blood
the greater the viscosity, the more difficult to get the blood moving
greater pressure needed to pump same amount of viscous blood
Arteriosclerosis
“hardening of the arteries”
decreases elasticity of the arteries
Atherosclerosis
lipid (plaque) deposits on the artery walls producing blockages
Stages of Diastole
atrial contraction - ventricles fill with blood
AV valves close - making the first heartbeat sound “lub”
Stages of Systole
Isovolumetric Contraction - ventricles are contracting with all the valves closed
Ejection Phase - pressure in the ventricles builds up until the semilunar valves open and blood is released into the blood vessels. blood is also refilling the atria during this phase.
Semilunar valves close - making the second heartbeat sound “dub”
isovolumetric relaxation - ventricles relax with all valves closed
Stroke Volume Changes
Exercise: additional blood return from muscles brings in more volume to the ventricles
Rapid Blood Loss: decreases blood returning to the heart
Heart Rate Changes
Stress: sympathetic and parasympathetic NS causes rate to increase or decrease
Hormones: epinephrine and thyroxine increase HR
ions: electrolyte imbalances affect the ability for the heart to contract
physical factors: age, body temperature, and overall health