physics test 2
1/56
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
57 Terms
detectors in digital imaging - advantage
its post processing abilities
once you take the image you are able to edit and change it - contrast and brightness editing
film digitiser
acquire image on a film and use the CCD camera or a scanner for convert that into a digital format
better because if you keep film for a long time it can be spoiled
computed radiography
initially, there is a storage phosphor imaging plate
when it is exposed to xrays it will excite the electrons and they will move up in energy shells
then to read that image you expose the plate to a laser which will emmit visible light
direct radiography using CCD
phosphor imaging plate where xray is converted into light
using lenses, the light will be foccussed onto a CCD camera making a digital image
direct radiography using CCD camera - disadvantages
can cause more scatter = decreased spatial resolution
DR flat pannel - indirect
use a TFT array
use a cesium iodide phosphor where xray is converted into light
then will be converted into electrons using the photodiode and the TFT reads that charge at each point
DR flat pannel - indirect
not the best spatial resolution
DR flat pannel - direct
xray is converted into charge using a photoconductor
no intermediate step which reduces any spatial resolution issues
when pixel size is more
there is a less number of pixels
spatial resolution decreases
higher number of pixels advantage
better reslution and better quality
each pixel corresponds to
a certain pixel detector element
other than pixel size, what can spatial resolution depend on
detector performance
focal spot size
scatter
the pixel is an integer whose value is proportional to what
its brightness
how can pixels be displayed
showing different shades of gray
higher number of bits/pixels advantage
better contrast resolution
gives more information to be analysed
dead pixels correction
in every detector system certain detector elements will not work
if you expose the detectors for too long you can damage them
what do the dead pixels cause?
artefacts
how to artefacts appear on the image
appear as a dark (or white) spot on the image
how do we correct the artefacts
the gray scale in adjacent pixels is averaged
that value replaces the value of the dead pixel
dark noise correction (dark feild correction)
electronic noise is associated with each detector element in the absence of xrays
noise coming from the detector elements
this results in finite gray scale even without any exposure
how do we correct dark noise/field
a large number of dark images are acquired and averaged over
this dark image is subtracted from the raw image produced by the detector array
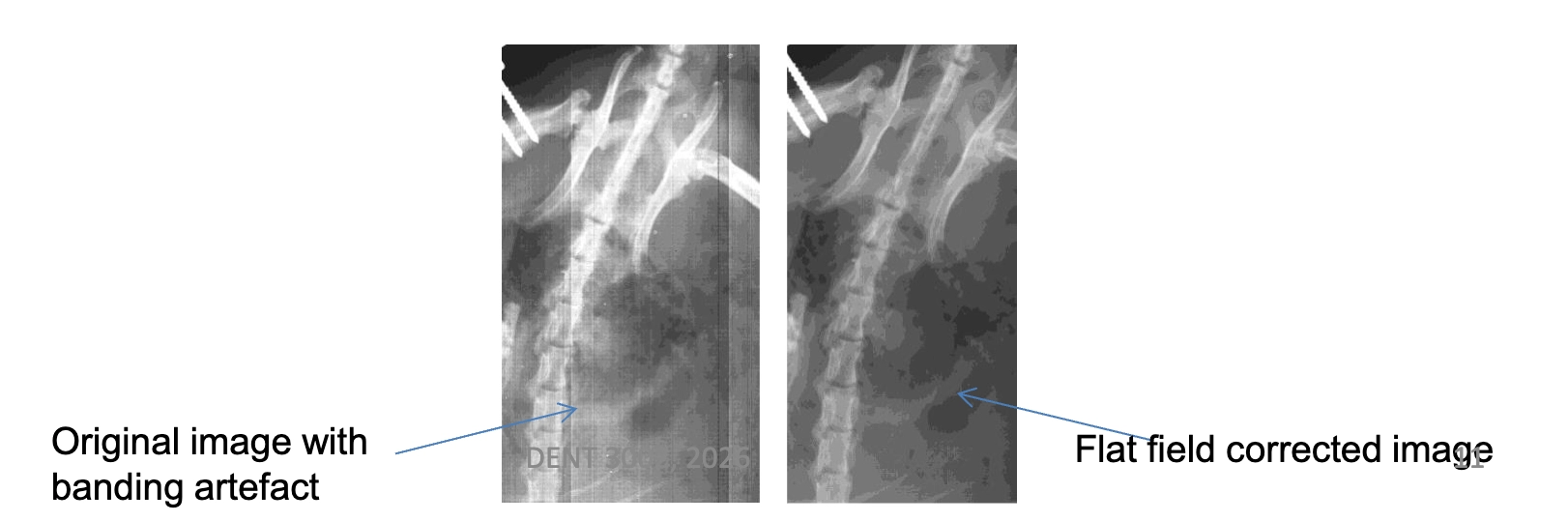
flat field cause
there are subtle differences between the sensitivity of each of the elements
also, the gain associated with with amplifiers connected to individual elements varies between detectors
all receptors react slightly differently to eachother
how do we correct flat field artefacts
a flat field (uniform field) is corrected and averaged
this information is used to compensate for the different gains and sensitivity for each of the detector images
after flat field correction, a uniform signal will create a uniform output
these corrections are applied automatically by the detector system before the image is displayed
why is gray scale chosen with window width and level
ability to encompass all pixel values
window level
the midpoint of the pixels being displayed
why is window level important
we have to choose a certain range of the pixel values to be displayed
what does windowing and levelling improve in images
imrpoves contrast
Windowing allows us to focus on a specific range of pixel values, making a small difference in that range easier to see
changing window level changes the pixel range to be displayed
also, changes the brightness of the image (darker or brighter)
if we want to enhance the contrast difference in the brighter portion, we may select a window from 150 to 255 - what number of pixels will be displayed as dark?
all of the pixels with values under 150
if we want to enhance the contrast difference in the darker portion, we may select a window from 0-100
the pixel values from 101-255 will be displayed as white
what does a smaller window width mean
much higher contrast
how to choose window level
Low WL (-600) = 600 lung
Medium WL (40) - soft tissue
High WL (300-600) - bone
Lung visualisation (lung window)
the lung contains very low densities (air) and higher densities such as vessels and airway walls
wide range of attenuation values
a large window width is therefore required to visualise all structures
Mediastinal (soft tissue)
mediastinum contains lots of soft tissue structures (heart, etc)
all structures have similar attenuation
a smaller window width is therefore needed to increase the contrast on that image
linear LUT
poor contrast
default modality LUT
a small range of pixel values are chosen to display
value of interest LUT
encompasses the full range of values and displays the output according to the displays capabilities
inverted LUT
inverts image contrast
high contrast LUT
very narrow window is selected
convolution
manipulation of digital images often involves a mathematical operation known as convolution
an image is convolved with a kernel (also known as a filter mask)
blurred (smooth image)
reduces quantum noise in low dose imaging, improving visibility of large anatomical structures
often applied before edge detection of image segmentation to remove noise and avoid false edges (pre-processing step)
edge enhanced image
enhances edges of structures, helping to visualise bone margins, fractures, or vessel boundaries better
useful in interventional imaging to improve visibility of catheters, guidewires, or stents
harmonised image
to imrpove visibility of both fine structure and soft tissue contrast
why is contrast media needed in radiography
if two organs have similar densities and average atomic numbers it is not possible to distinguish them on a radiograph
contrast resolution atomic number
they have a high atomic number so that blood vessels can be attenuated less and will show up brighter on a radiograph
alters the atomic number of the structure to be radiographed
digital subtraction angiography
mainly used to visualise vessels in a boney or soft tissue envinroment
a digital radiographic image of the patients anaotmy is acquired - mask image (pre contrast image)
process of DSA
after the mask image is taken a radio opaque contrast agent is injected
a series of images are taken during and after the agent has been injected
the mask image is subtracted from the image with the contrast agent
what does the subtracted image do
provides details of anatomy - where background anatomy is subtracted out
enhances the contrast and improve blood vessel visibility
disadvantage in DSA
due to the exponential attenuation of radiation into the matter, if two images are directly subtracted from one another, the final images will contain artefacts
how do we counteract artefact in DSA
the raw image data are logarhythmically processed by computing the natural logarhythm of the transmitted intensities before subtraction
road mapping
a software and video enhanced variant of the last frame hold feature
useful for placement of catheters and wires in complex and small vasculature
a DSA sequence is performed and the frame with maximum vessel opacification is identified
this frame becomes the road map mask
what do we do with the road map mask
it is subtracted from subsequent live fluoroscopy images
this produces real time subtracted fluoroscopic images layed on a static image of blood vessels
why is road mapping advantageous
provides a good idea about the path of the vessels and facillitates maneouvering through the vasculature
dual energy subtraction - dual energy chest radiography advantage
reduces anatomical noise
exploites the difference in atomic numbers of bone and soft tissue
requirement of dial energy subtraction
requires two images - one at low energy and high energy
Two xray exposures at different kVp (two- pulse)
Or done simultaneously using a sandwich detector (low dos
dual energy subtraction technique after image is taken
two imaged are weighted to logarhythmic subtraction
Mathematically, ln(Ihigh) - R ln(Ilow); where R is a constant used to change the weighting
by adjusting R, the soft tissue points or bones can be viewed clearly
we subtract the low energy one from the high energy one
photoelectric absorption
the attenuation curves have energy dependance as well as Z dependance
Photoelectric absorption a Z3
The higher the atomic number, the higher the photoelectric absorption
Photoelectric absorption a 1/E3
PE absorption reduces with energy
how are we able to do dual energy subtraction
because of the different energy dependecy in different tissue types, the aqcuisition of two radiographic images at two different energy levels, enables either the bone component or the soft tissue component to be removed by prost processing