A&P 2: Respiration
1/185
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
186 Terms
Structures of the upper respiratory tract
nose, pharynx
Structures of the lower respiratory tract
larynx, trachea, bronchi, lungs
What structures does the path of air pass through?
1. nasal cavity
2. pharynx
3. larynx
4. trachea
5. primary bronchi
6. secondary bronchi
7. tertiary bronchi
8. bronchioles
9. alveoli
Pharynx (+ location, function)
- hollow tube that starts posterior to internal nares and runs to opening of larynx in neck
function: passageway for air and food and houses tonsils
Function and types of tonsils
function: houses lymphocytes and traps bacteria entering through nose/mouth
types: pharyngeal (adenoids), palatine, lingual, tubal
Location and function of nasopharynx
location: behind internal nares
function: contains pharyngeal tonsils (adenoids) and the opening of auditory tubes and acts as an airway
Location and function of oropharynx
location: behind mouth
function: respiratory and digestive functions and houses the palatine and lingual tonsils
Which tonsils are removed during a tonsilectomy?
Palatine tonsils
Location and function of laryngopharynx
location: inferiorly and opens into larynx and esophagus
function: respiratory and digestive functions
What are the 3 regions of the pharynx?
1. Nasopharynx
2. Oropharynx
3. Laryngopharynx
What two cartilages are used as a landmark for making cricothyrotomy?
Thyroid cartilage and cricoid cartilage
What is the purpose of a cricothyrotomy?
Emergency airway
Ventricular folds
false vocal cords external to the true vocal cords surrounding the glottic opening
What structures form the rima glottidis?
The true vocal cords or vocal folds
Epiglottis (+ location, function)
- flap of elastic cartilage covered with mucous membrane
location: attached to roof of tongue
function:
breathing- held anteriorly
swallowing- pulled backward to close off the glottic opening and divert food away from trachea and into esophagus
What type of cells is the respiratory tract made of?
Ciliated pseudostratified columnar epithelium
How does the cilia of the respiratory tract move in the upper vs. lower respiratory tracts?
Upper: cilia move mucous and trapped particles down toward pharynx
Lower: cilia move mucous and trapped particles up toward larynx
Trachea (+ length, location)
- semi-rigid pipe made of semi-circular cartilaginous rings
location: anterior to esophagus extending into mediastinum where it divides into left/right primary bronchi
length: 12 cm long
Carina (+ function)
- internal ridge located at the junction of the two main stem bronchi
function: sensitive trigger for coughing reflex
Location and function of trachealis muscle
location: posterior trachea directly adjacent to the esophagus
function: contract the trachea to increase airflow velocity and enhance the expulsion of mucous and foreign particles during coughing
What structural changes occur as bronchi branch into bronchioles?
- mucous membrane changes then disappears
- cartilaginous rings become more sparse and eventually disappear
- as cartilage decreases, smooth muscle increases
Effect of sympathetic stimulation on smooth muscle of bronchi/bronchioles
airway dilation
Effect of parasympathetic stimulation on smooth muscle of bronchi/bronchioles
airway constriction
Alveoli (+ function, how many cells thick, type of epithelium)
- cup-shaped outpouchings for gas exchange
function: gas exchange
- one cell thick
-simple squamous epithelium
Function of alveolar ducts
connect terminal bronchioles to alveolar sacs
Alveolar sacs
clusters of alveoli
How is the right lung divided?
into 3 lobes (superior, middle, and inferior) by the oblique and horizontal fissure
How is the left lung divided?
into 2 lobes (superior and inferior) by the oblique fissure
Apex of lungs
superior and extends slightly above the clavicles
Base of lungs
flat bottom sitting on diaphragm
Cardiac notch
the indention for the heart in the left lung (makes the left lung 10% smaller than right)
What are the thoracic muscles for inhalation?
1. sternocleidomastoid
2. scalenes
3. external intercostals
4. diaphragm
What are the thoracic muscles for exhalation?
1. internal intercostals
2. external oblique
3. internal oblique
4. tranversus abdominis
5. rectus abdominis
6. diaphragm
Functions of the nose
provides airway for respiration
moistens/warms entering air
filters/cleans air
resonating chamber for speech
houses olfactory receptors
What is the external nose composed of?
the nasal bone and several cartilages
Types of mucosas in the nasal cavity
olfactory and respiratory mucosa
Location and type of epithelium of olfactory mucosa
located in the superior region of the nasal cavity and contains olfactory epithelium
Location of respiratory mucosa
location:
lines most of the nasal cavity
nasopharynx
larynx (except vocal cords)
trachea
bronchial tree (down to bronchioles)
Location and function of nasal conchae
protrude medially from the lateral walls of the nasal cavity
their shape increases mucosal area exposed to air and enhances turbulent flow
during inhalation they filter, heat, and moisten air and then reclaim most of the heat/moisture during exhalation
What bones are the paranasal sinuses located in?
frontal, sphenoid, ethmoid, maxillary
paranasal sinuses and functions
spaces in the skull that connect the nasal cavity
lighten the skull
secrete mucus
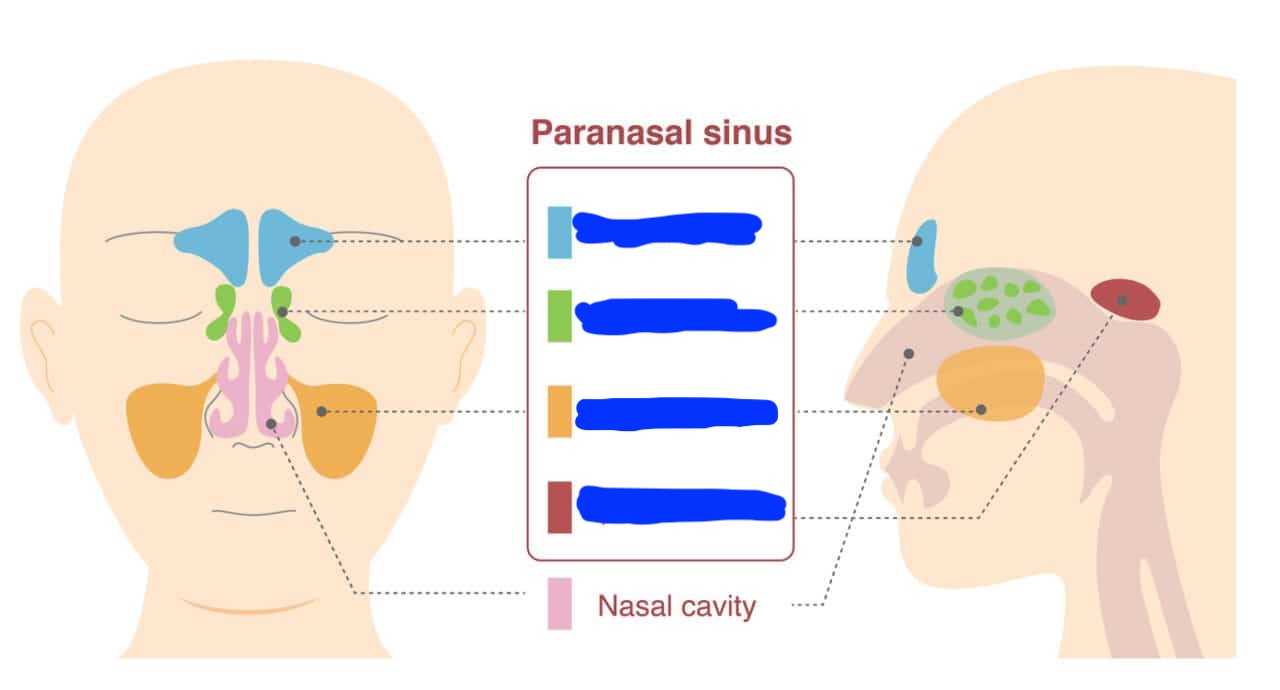
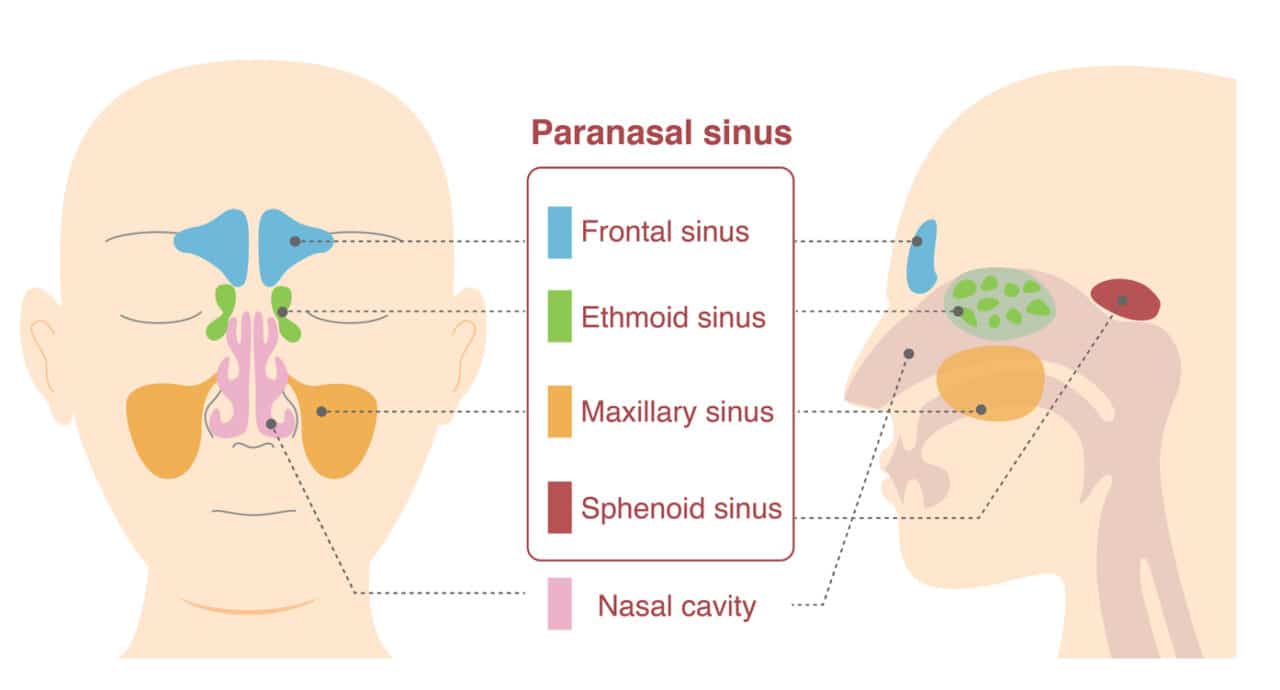
Label each paranasal sinus
frontal sinus - on forehead
ethmoid sinus - on sides of bridge of nose
maxillary sinus - on cheeks beside nose
sphenoid sinus - behind eyes
What happens during swallowing that prevents food from going into the nasopharynx?
The uvula and soft pallete move superiorly to block nasopharynx during swallowing
What covers the opening of the auditory tubes in the nasopharynx?
tubal tonsils
Isthmus of Fauces
archway between oropharynx and oral cavity
What type of epithelium is in the laryngopharynx?
stratified squamous epithelium
If swallowing, which has right of way, air or food?
food has right of way so airflow temporarily stops
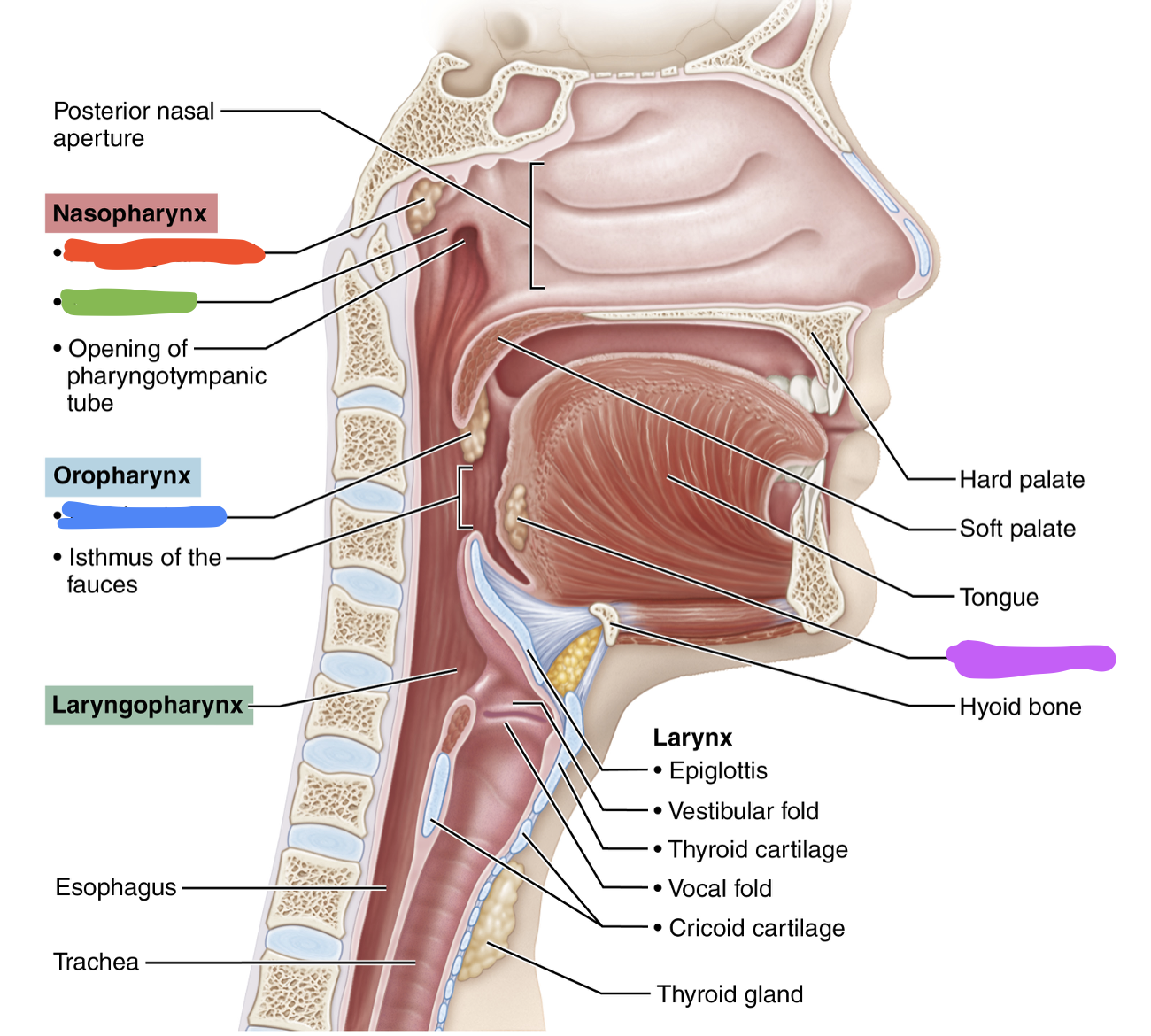
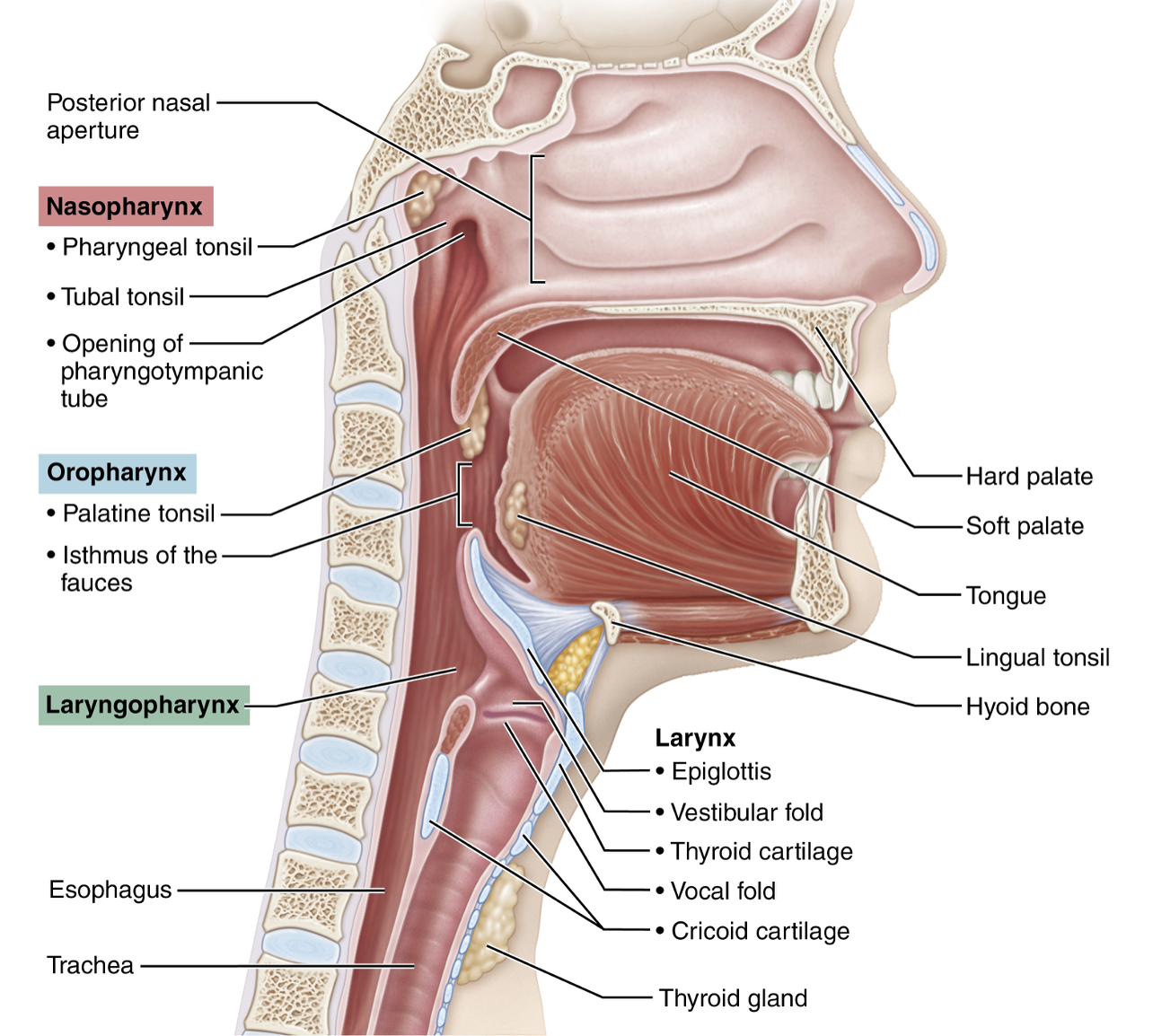
Label each blank
Red - pharyngeal tonsil
Green - tubal tonsil
Blue - palatine tonsil
Purple - lingual tonsil
Respiratory zone + structures
sites for gas exchange
respiratory bronchioles
alveolar ducts
alveoli
Conducting zone + functions
all other airways from nose to bronchioles
transport air to/from sites of gas exchange
cleanse, warm, and humidify incoming air
What vertebrae does the larynx span from?
C3 to C6
Functions of the larynx
provides open airway, routes air/food into proper channels, and voice production
What are the structures of hyaline cartilage and elastic cartilage in the larynx?
Hyaline:
thyroid cartilage
cricoid cartilage
arytenoid cartilage
cuneiform cartilage
corniculate cartilage
Elastic:
epiglottis
Laryngeal prominence
“adam’s apple” anterior midline ridge on the thyroid cartilage
What are the 3 pairs of small cartilages in the larynx?
arytenoid cartilage
cuneiform cartilage
corniculate cartilage
Epiglottis + function
elastic cartilage covered in taste bud containing mucosa
covers laryngeal inlet during swallowing as larynx is pulled superiorly
Vocal folds (synonym, function, formed by…)
also called “true vocal cords”
mucosal folds that vibrate to produce sound as air passes through during expiration
formed by vocal ligaments
Vocal ligaments (location + function)
lie deep to mucosa and attach thyroid cartilage to arytenoid cartilage and form true vocal cords
Vestibular folds
also called “false vocal cords”
no sound production but helps close glottis during swallowing
Speech
intermittent release of expired air during opening/closing of glottis
How is pitch determined?
by length and tension of vocal folds (tenser folds vibrate faster to produce higher pitch)
How is loudness determined?
depends on force of airflow vibrating folds
What structure muscles shape speech into language?
pharynx, tongue, soft palate, and lips
Laryngitis, causes, and consequences
inflammation of vocal cords
caused by viral infections, overuse of voice, dry air, tumors of vocal cords, inhalation of irritating chemicals
can result in hoarseness and in severe cases, speaking limited to a whisper
3 layers of the trachea wall from inside to outside
mucosa
submucosa
adventitia
Mucosa layer of the trachea wall
respiratory epithelium
Submucosa layer of the trachea wall
CT with seromucous glands supported by 16-20 cartilage rings to prevent airway collapse
How does smoking affect breathing?
Smoking inhibits and destroys cilia, which causes coughing because it is the only way to prevent mucus accumulation
Does cilia return several weeks after quitting smoking?
Yes
Heimlich maneuver
procedure where air in a victim’s lungs is used to expel an obstructing piece of food
How many generations of branching do airways undergo?
23
Hilum
place on lung where primary bronchi enter
Why are secondary bronchi also called “lobar bronchi”?
Because each lobe of the lungs gets one secondary bronchi
What are the differences structurally between bronchi and bronchioles?
bronchi have cartilage rings and bronchioles have smooth muscle
bronchioles have cuboidal epithelium while bronchi have respiratory epithelium
How thick is the respiratory membrane and what is it composed of?
about 0.5 um thick and made of the alveolar wall, capillary wall, and a shared basement membrane
Types of cells in the alveolar wall
type I alveolar cells
type II alveolar cells
mobile alveolar macrophages
Type I alveolar cells
simple squamous epithelium
Type II alveolar cells (+ function)
scattered cuboidal cells that secrete surfactant and antimicrobial proteins along inner surface
Function of alveolar macrophages
keep inner surface clean and consume bacteria and debris
Function of alveolar pores
connect adjacent alveoli, equalize air pressure throughout lungs, and provide alternate routes in case of airway blockages
Atmospheric air is…
21% oxygen, 0.04% CO2, and 78% nitrogen
type of epithelium of respiratory mucosa
contains respiratory epithelium with goblet cells resting on a basement membrane with seromucos glands.
What is the function of surfactant and what secretes it?
function: reduces attraction/cohesiveness between water molecules to prevent alveolar collapse and reduce work of lung inflation
secreted by type II alveolar cells
lobule (+ shape, separated by…)
smallest subdivision of lung visible to the naked eye
hexagonal in shape
separated by CT
What does the connective tissue that connects lobules look like in smokers?
Blackened with carbon
Lung tissue composition
alveoli within a stroma
Stroma
“bed” of mostly elastic connective tissue which reduces work of breathing
What are the two divisions of lung circulation?
Pulmonary and bronchial
Function of pulmonary arteries
carry systemic venous blood from heart to lungs for oxygenation
branch and lead into pulmonary capillary networks that surround alveoli
Which division of lung circulation is low/high pressure and low/high volume?
Pulmonary: low pressure, high volume
Bronchial: high pressure, low volume
Function of pulmonary veins
carry oxygenated blood from alveoli back to heart (left atria)
Where are enzymes that act on blood housed?
Capillary epithelium of pulmonary capillary networks
Bronchial arteries (function, place of origin, and place of insertion)
provide oxygenated blood to lung tissue (except alveoli)
arise from aorta
enter lungs at hilum
What are the three parts of innervating the lungs?
parasympathetic fibers
sympathetic fibers
visceral sensory fibers
What causes bronchoconstriction?
parasympathetic stimulation
What causes bronchodilation?
sympathetic stimulation
Where do parasympathetic and sympathetic fibers enter into the lungs and then go?
The pulmonary plexus on lung root and run along bronchial tree and blood vessels
Pleurae
double-layered serous membrane that divides thoracic cavity into two pleural compartments and mediastinum
Parietal pleurae
lines inner surface of thoracic wall, superior face of diaphragm, and lateral walls of mediastinum
Visceral pleurae
lines external surface of lungs and dips into fissures