RESP1193 Cardio A&P Chapter 17, Functional Antomy of the Cardiovascular System
1/102
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
103 Terms
Mediastinum behind the sternum
location of the heart
Apex
lower tip of the heart
Base
the top end of the heart where the great vessels are located
Point of maximal Impact (PMI)
this is created by the repeated impact of the heartbeat on the inner chest wall.
Apical Beat
another term for PMI
The 5th intercostal space
Where is PMI typically felt
Shift the heart to the left
How will a right lung pneumothorax affect the heart?
Pericardium
Loose fitting membranous sac which covers the heart
fibrous pericardium
Tough, superficial most portion of pericardium
Parietal Pericardium
Lines the inner surface of the fibrous pericardium
Visceral pericardium (epicardium)
innermost layer of pericardium directly adhered to the hearts surface
epicardium (visceral pericardium), myocardium, endocardium
Name the 3 components of the heart wall from most superficial to most deep.
cardiac muscle
what is myocardium?
right atrium
heart chamber that receives deoxygenated blood from the vena cava and coronary sinus
Tricuspid Valve
Blood flows from the right atria to the right ventricle via this structure
The pulmonary artery
The right ventricle pumps deoxygenated blood into...
Semilunar Valves
Valves that are closed during ventricular diastole
atrioventricular valves (AV)
valves that are open during ventricular diastole
atrioventricular valves
valves that are closed during ventricular systole
Semilunar Valves (SV)
valves that are open during ventricular systole
left atrium
heart chamber that receives oxygenated blood from the 4 pulmonary veins
bicuspid (mitral) valve
blood flows from the left atrium to the left ventricle thru this structure
Pulmonary artery, Aorta
where are the semi-lunar vales located?
atrioventricular valves
structure that prevents backflow of blood into the atria during ventricular systole
interatrial septum
structure that separates the two atria, preventing the mixture of oxygenated and deoxygenated blood
semilunar valves
structure that prevents backflow of blood into the ventricles during atrial systole.
interventricular septum
structure that separates the right and left ventricles preventing the mixture of oxygenated and deoxygenated blood.
papillary muscles
cone shaped pillars which attach to the chordae tendinae
Chordae Tendinae
strong connective tissue strings that attach to the AV valves allowing them to open and close
Fibrous annuli
tough set of connected rings that form a semi-rigid framework to which the heart valves and and cardiac muscle are attached
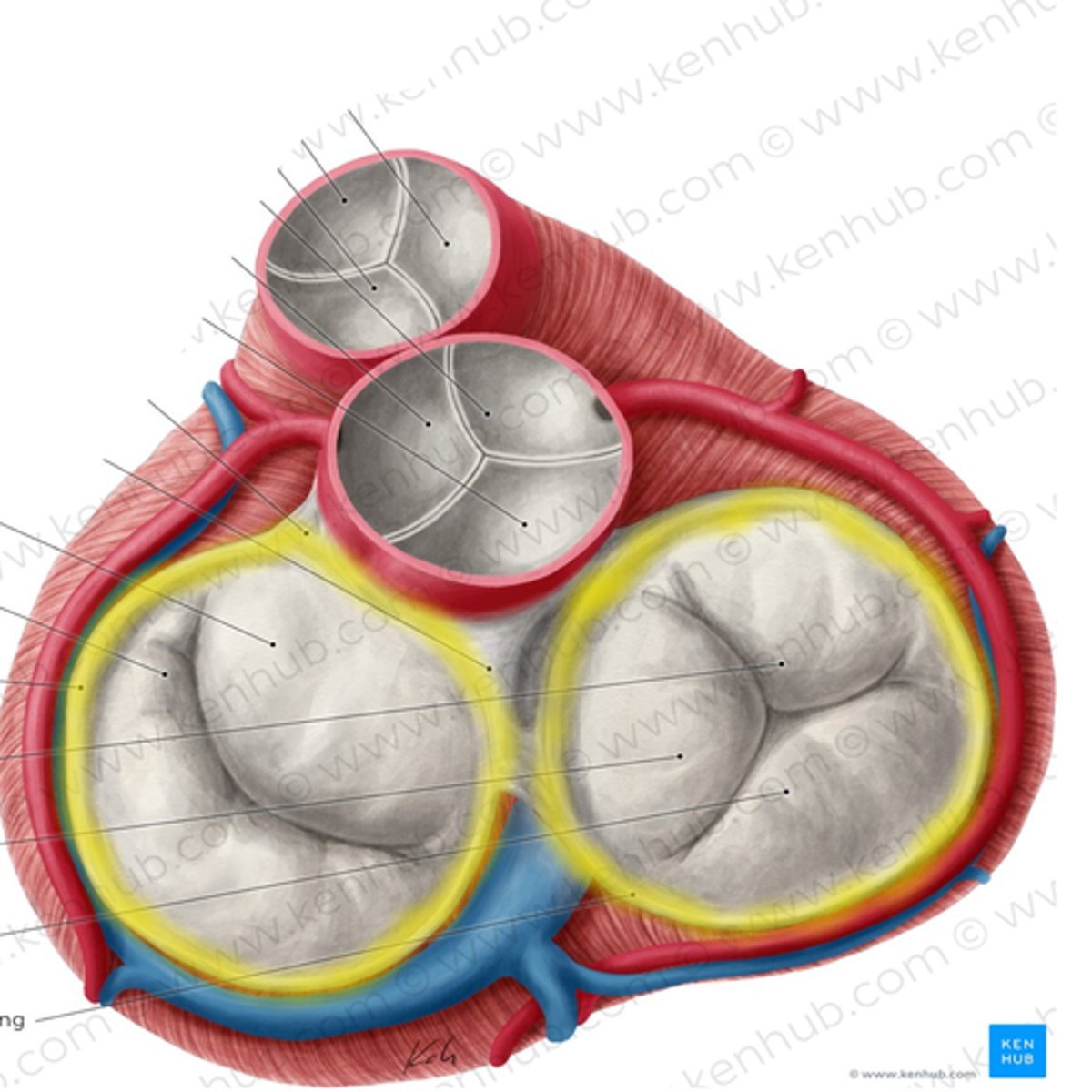
Apex, Base
blood stroke volume is squeezed from _________ to __________
the right and left coronary arteries
Where does the myocardium itself receive it's blood supply from?
right coronary artery
which coronary artery is the dominant blood supplier in the coronary circulation
FALSE: there is a lack of collateral circulation between the coronary arteries; if one becomes blocked, there are few detours the blood flow can take.
True or False: There is an abundance of collateral circulation between the coronary arteries.
Ischemia, Angina Pectoris
potential consequences of occluded coronary blood flow
ischemia (tissue hypoxia)
decreased oxygen supply to the heart
angina pectoris
central chest pain caused by occluded coronary blood flow
myocardial infarction
heart muscle tissue death caused by tissue hypoxia
True
True or False: Coronary veins flow parallel to coronary arteries
Coronary sinus (right atrium)
where does 75% of the coronary venous drainage empty
All four; contributing to normal anatomical shunt
which heart chamber(s) do Thesbian (coronary) veins empty into?
70%
how much oxygen does the myocardium extract from it's arterial blood?
Exercise increases myocardial oxygen requirements, thus increasing coronary blood flow
how does exercise affect myocardial oxygen needs?
myocardial oxygen needs
what factor governs coronary blood flow?
ventricular diastole
coronary blood flow only occurs during which phase of heartbeat?
4-5%
coronary blood is what percent of total cardiac output?
TRUE: this momentarily stops coronary blood flow during ventricular systole.
True or False: During systole, the ventricles compress the coronary blood vessels.
shortens diastolic time
effect of extreme tachycardia on diastolic time
1. decreased coronary blood flow
2. decreased end diastolic volume
3. Decreased ejected stroke volume
name 3 effects of a shortened diastolic time
Stroke volume (SV)
the volume of blood ejected by a ventricle with each heartbeat
Cardiac Output (CO)
measurement of the amount of blood ejected per minute from either ventricle of the heart
to conduct electrical impulses to stimulate rhythmic, synchronized myocardial contractions.
Purpose of the cardiac conduction system
SA node
AV node
Bundle of His
Right/Left Bundle Branches
Purkinje Fibers
List the order of impulse conduction in the cardiac conduction system
sinoatrial (SA) node
"Pacemaker" that initiates electrical impulses of the heart
Bundle of His (AV bundle)
this structure is the only connection of action potential between the atria and ventricles
Right/Left Bundle branches
this structure conducts the electrical impulse to the right/left ventricles via the interventricular septum
Purkinje fibers
subdivision of bundle branches throughout the right and left ventricular myocardium
Beta 1 receptors
Sympathetic receptors that increase heart rate and contractility are?
decrease heart rate and contractility
Effect of parasympathetic fibers on SA and AV nodes
myocyte
muscle fiber cell bounded by the sarcolemma
Sarcolemma
muscle cell membrane
T tubules
deep dipping of sarcolemma into the cells interior allowing electrical impulses to travel deep inside the muscle cell
sarcoplasmic reticulum
intracellular network of tubules throughout the muscle fiber that store calcium
Calcium is released from the sarcoplasmic reticulum
what happens when electrical impulses within the t-tubule stimulate adjacent sarcoplasmic reticulum
Cardiac Cycle (one heart beat)
A complete heartbeat consisting of contraction (systole) and relaxation (diastole) of both atria and both ventricles
ventricular filling
Preload is defined by
preload is 80% passive and 20% active (atrial kick)
what percent of ventricular filling (preload) is active, and passive?
isovolumetric contraction
brief period during ventricular emptying when all valves are closed before blood is ejected from the ventricles
afterload
the amount of resistance to ejection of blood from the ventricle
End Diastolic Volume (EDV)
volume of blood in each ventricle at end of ventricular diastole (PRELOAD)
Ejection fraction
the filled ventricles normally eject about 60% EDV. This is known as...
CO= HR x SV
cardiac output formula
decreased stroke volume
an increased afterload would have what effect on stroke volume?
dichrotic notch
"shock wave" from forceful closure of semilunar valves on the arterial pressure waveform
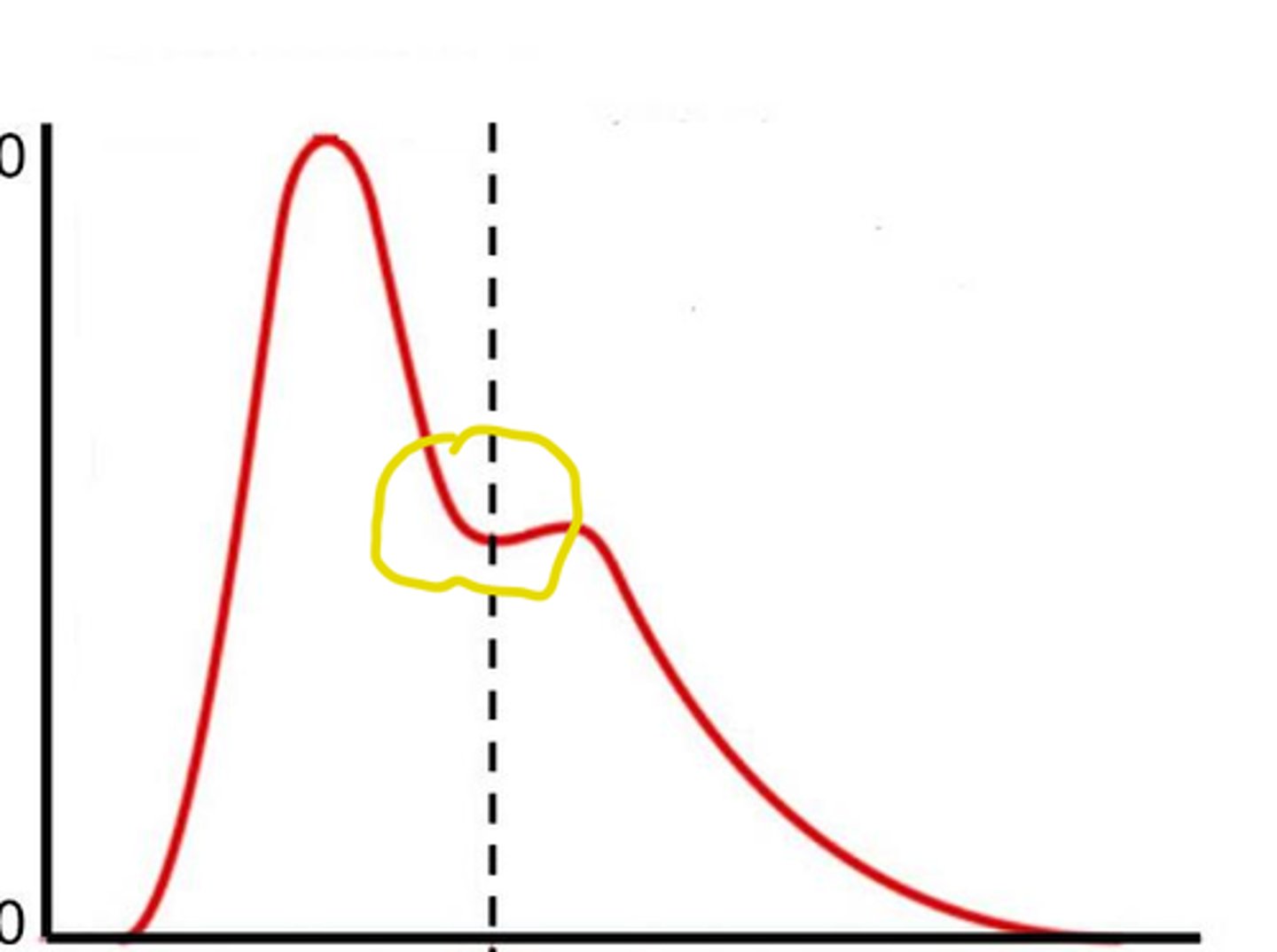
Frank-Starling Mechanism
venous blood return to the right atrium determines overall cardiac output. what is this concept?
increased blood flow
increased ventricular filling
increased muscle fiber distension
increased force of contraction
Explain the mechanics of the Frank-Starling Mechanism
Drugs, Exercise, Anxiety
name 3 sympathetic stimuli that regulate pumping activity
Respiratory vagal stimulation
name a parasympathetic regulator of pumping activity
increased cardiac output
effect of increased heart rate on cardiac output
the hearts pumping action; elastic recoil of the arteries
what are the 2 forces responsible for perfusion pressure?
systemic arterioles
these structures can form precapillary sphincters that can constrict or dilate
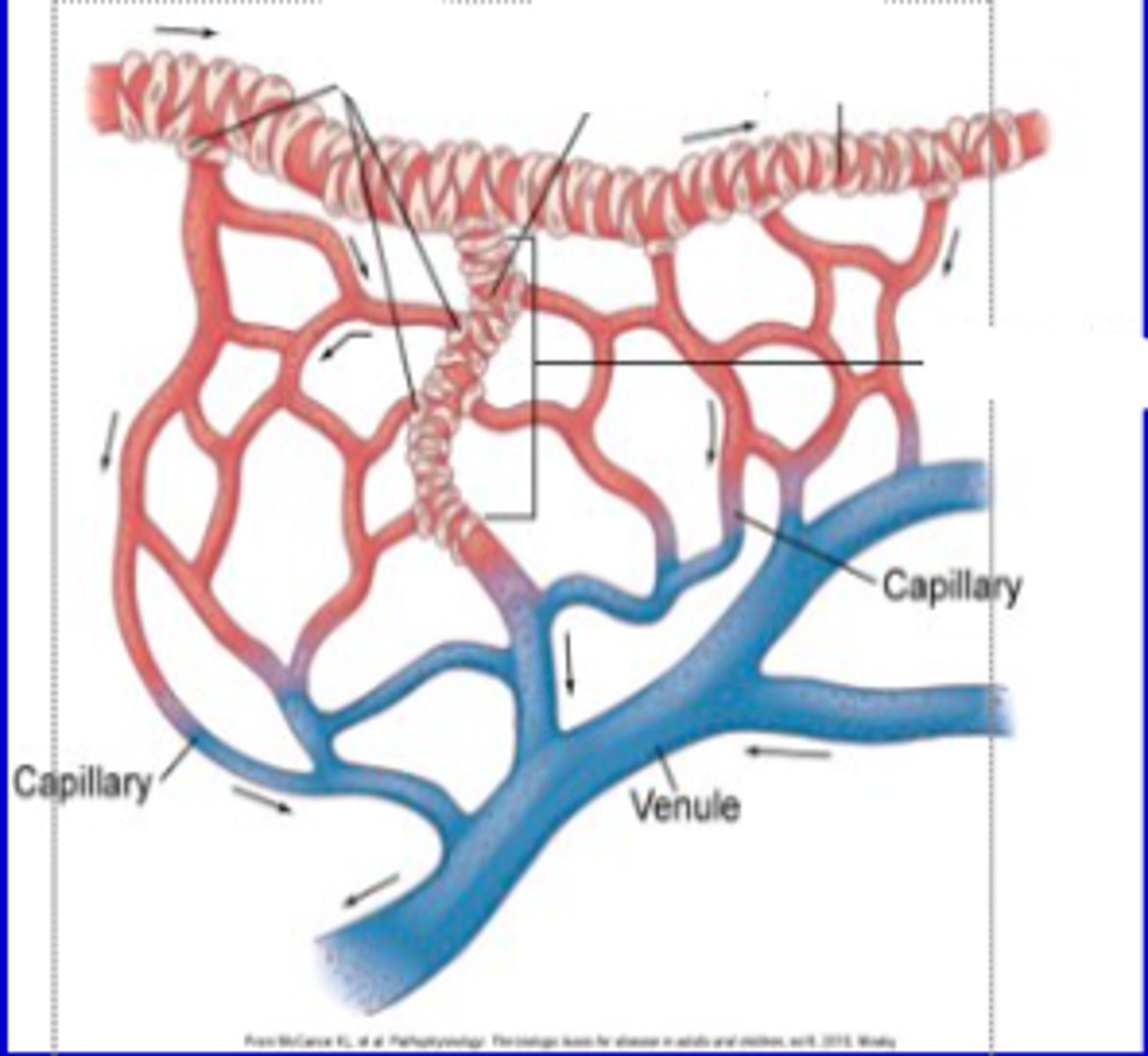
constrict
at rest, precapillary sphincters will ___________
the arteries will dilate to increase perfusion in order to meet increased tissue oxygen needs.
what happens to arteries in hypoxia, where PaCO2 is increased and pH is decreased (acidosis)
vasoconstriction
contrary to systemic arteries, hypoxia in the pulmonary artery will cause ___________
veins; contain 64% of blood volume
vessels that contain the greatest proportion of blood volume at a given time due to high distensibility
skeletal muscle milking
sympathetic venous constriction
cardiac pumping action
subatmospheric intrathoracic pressure during breathing
name 4 factors that augment (increase) venous return
high, low
in arteries, blood flows from ________ to
__________ pressure areas
P(systolic) - P(diastolic)
pulse pressure formula
{P(syst) + 2(Pdiast)]/3
Mean Arterial Pressure Formula
FALSE: Heart is in diastole 2/3 of the time; Systole is only 1/3 of the time.
True or False: Heart remains in systole longer than diastole
Lowest, Highest
Systolic pressure in the vena cava reads the ________; Sytolic pressure in the aorta reads the ___________.
increase vascular resistance
how will a decrease in the area of a vascular bed affect vascular resistance?
capillaries
what vessel does gas exchange occur in?
-Stroke Volume
-Arterial Compliance (elasticity/recoil force)
-Arterial Resistance (vessel diameter)
name the 3 factors that determine Mean Arterial Pressure
P(syst) > 135-140mmHg; P(diast) > 90mmHg
what are the systolic and diastolic pressures that characterize hypertension?
-increased workload to heart >>> heart failure
-Cerebral Vascular Accident (CVA)
-Renal Hemmorrhages
name 3 detrimental effects of hypertension
because blood from all systemic veins flows into the right atrium; thus anything that affects RAP affects all venous pressures in the body.
why is right atrial pressure (RAP) known as "central venous pressure (CVA)?"
-the hearts ability to pump blood out
-rate of blood return to the vena cava
name the 2 factors of that the determine RAP (Right Atrial Pressure)
JVD (jugular vein distention)
Hepatomegaly (enlarged liver)
Pedal (peripheral) edema
a RAP greater than 6 mmHg can cause
0-6 mmHg; RAP/CVP
what is the ventricular pressure value for RVEDP; what is used to measure it?