Shock & Sepsis: Causes, Management, and Nursing Interventions
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
28 Terms
What is shock?
A syndrome of inadequate tissue perfusion.
What are the major types of shock?
Hypovolemic, Cardiogenic, Neurogenic, Septic, Anaphylactic, and Obstructive.
What causes hypovolemic shock?
Hemorrhage, severe dehydration, or fluid shifts.
What is the primary issue in cardiogenic shock?
Loss of pumping ability of the heart.
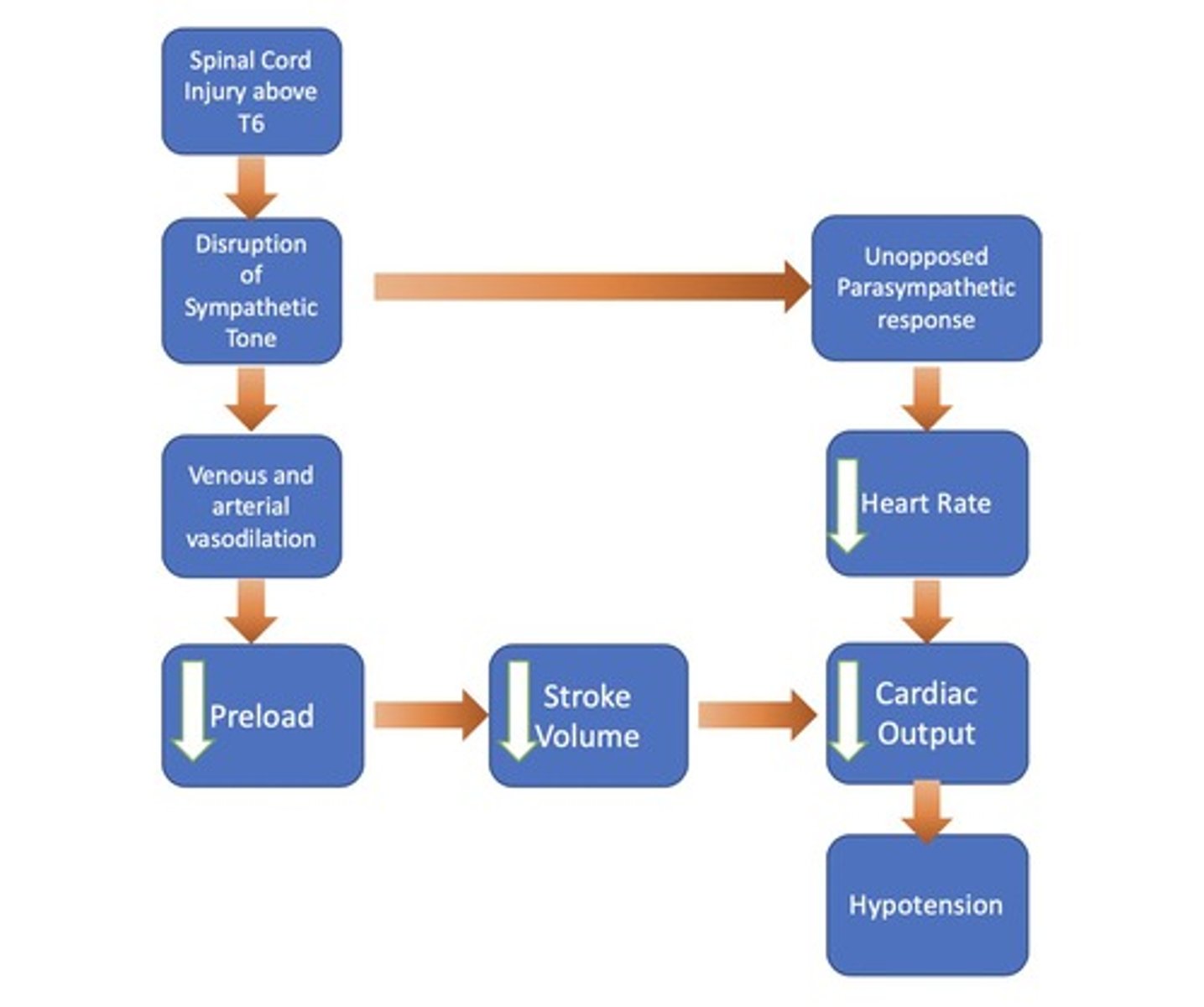
What triggers neurogenic shock?
Spinal cord injury above T-6.
What is septic shock?
Sepsis resulting in hypotension despite adequate volume resuscitation.
What is the significance of Mean Arterial Pressure (MAP)?
Normal MAP is 70 to 100 mm Hg; must be > 60 mmHg to maintain perfusion.
What are the signs of diminished perfusion?
Changes in vital signs, CNS status, skin condition, cardiovascular, genitourinary, and gastrointestinal systems.
What compensatory mechanisms are activated in response to loss of cardiac output?
Activation of the sympathetic nervous system (SNS), renin-angiotensin-aldosterone system (RAAS), and antidiuretic hormone (ADH).
What are the consequences of inadequate perfusion?
Shift to anaerobic metabolism, release of lactic acid, metabolic acidosis, and cellular dysfunction.
What is the management for hypovolemic shock?
Control bleeding or fluid loss, maintain oxygenation, insert large bore IVs, replace volume, and monitor perfusion.
What diagnostic tests are used for cardiogenic shock?
Cardiac enzymes, EKG, chest X-ray, echocardiogram, BNP, CBC, and CMP.
What is the primary goal in managing neurogenic shock?
To maintain perfusion of the spinal cord.
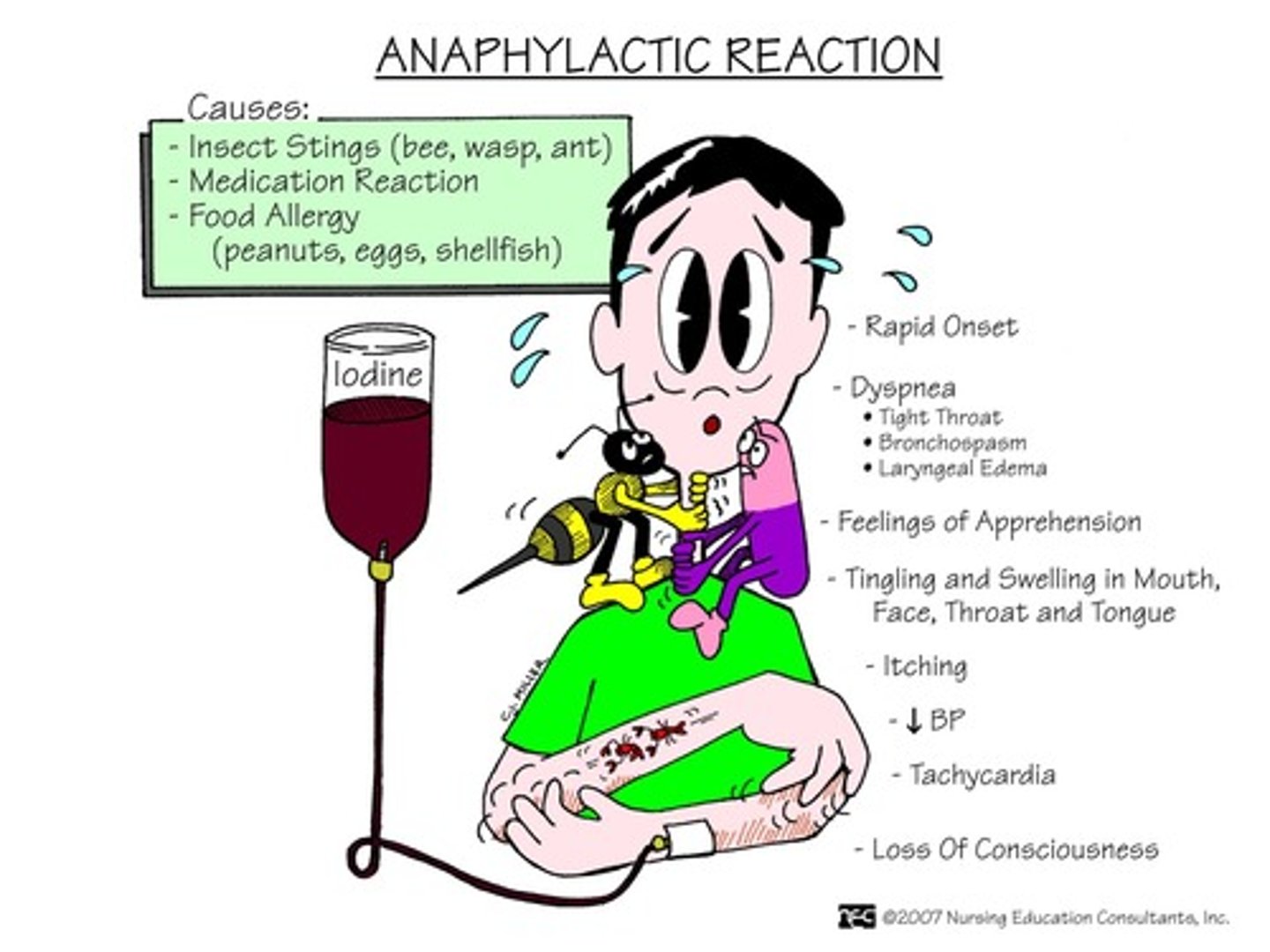
What is the pathophysiology of anaphylactic shock?
IgE mediated immune reaction leading to mast cell degranulation, resulting in bronchospasm and hypotension.
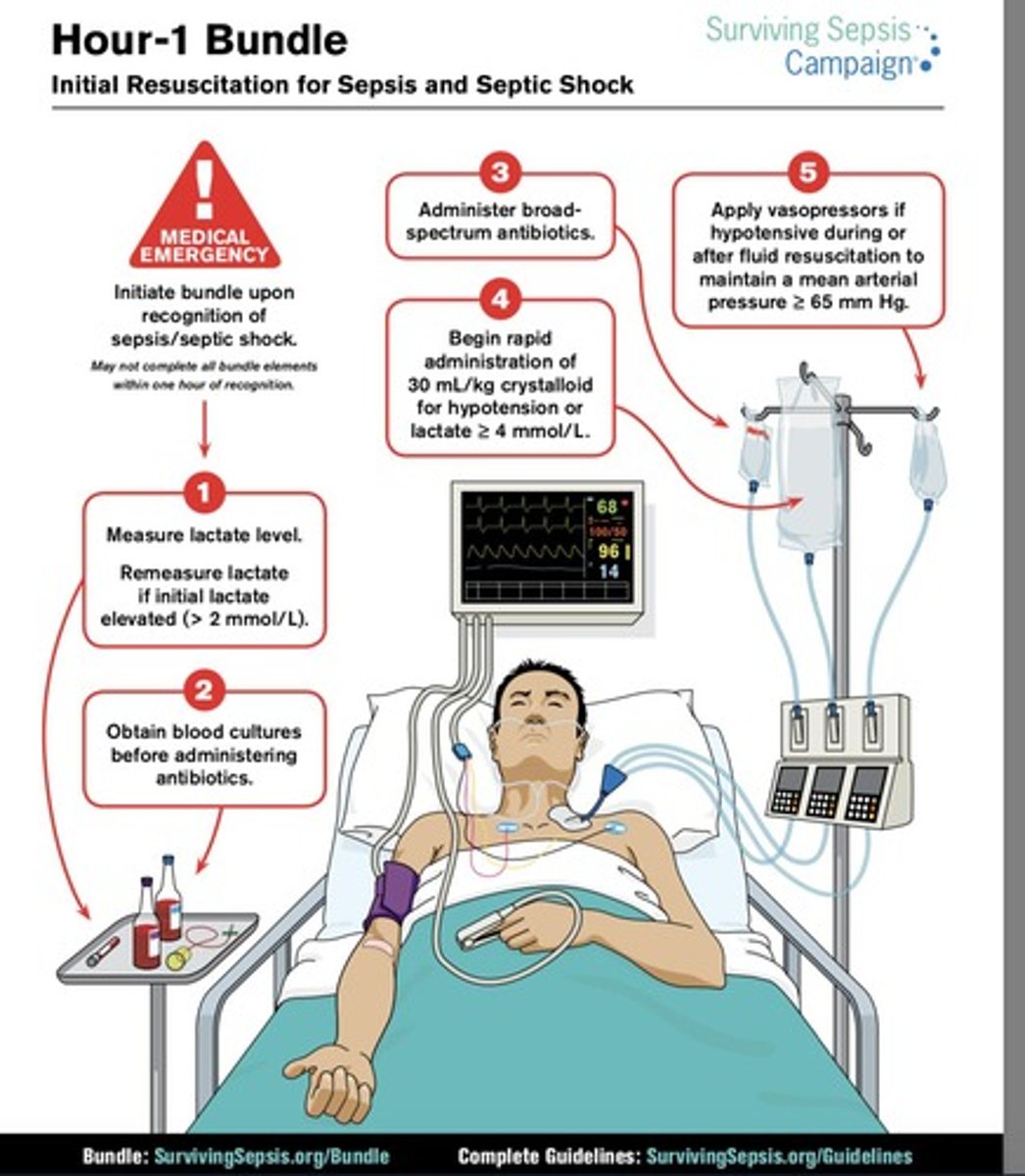
What are the key interventions in the Surviving Sepsis Campaign?
Administer high flow O2, start IV fluid resuscitation, draw blood cultures, and initiate IV antibiotics within 1 hour.
What are the criteria for Systemic Inflammatory Response Syndrome (SIRS)?
Presence of known or suspected infection and at least 2 of the following: fever or hypothermia, tachycardia, tachypnea, or abnormal WBC count.
What indicates septic shock?
Hypotension (MAP < 60 mm Hg) despite fluid resuscitation.
What are the complications associated with shock or sepsis?
ARDS, renal failure, GI bleeds, DIC, and multiple organ dysfunction syndrome (MODS).
What nursing interventions are important in shock management?
Ongoing assessment, titration of fluids and vasopressors, respiratory support, and preventing complications of immobility.
What is the first step in managing anaphylactic shock?
Remove the offending substance and establish airway.
What should be monitored to evaluate response to treatment in shock?
MAP, urine output, and lactate levels.
What is the expected urine output in effective management of shock?
Urine output should be greater than 30 mL/hour.
What is the role of epinephrine in anaphylactic shock management?
It counteracts severe allergic reactions by causing vasoconstriction and bronchodilation.
What is the relationship between sepsis and organ dysfunction?
Severe sepsis is sepsis complicated by organ dysfunction.
What is the importance of early recognition in sepsis?
Early recognition is key to improving survival rates.
What vital signs indicate hypovolemic shock?
Low blood pressure and increased heart rate.
What is the significance of serum lactate levels in sepsis?
Elevated lactate levels indicate tissue hypoperfusion and can guide treatment.
What should be done if a patient presents with suspected sepsis?
Initiate IV fluids, obtain blood cultures, and start broad-spectrum antibiotics.