Digestive system
1/108
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
109 Terms
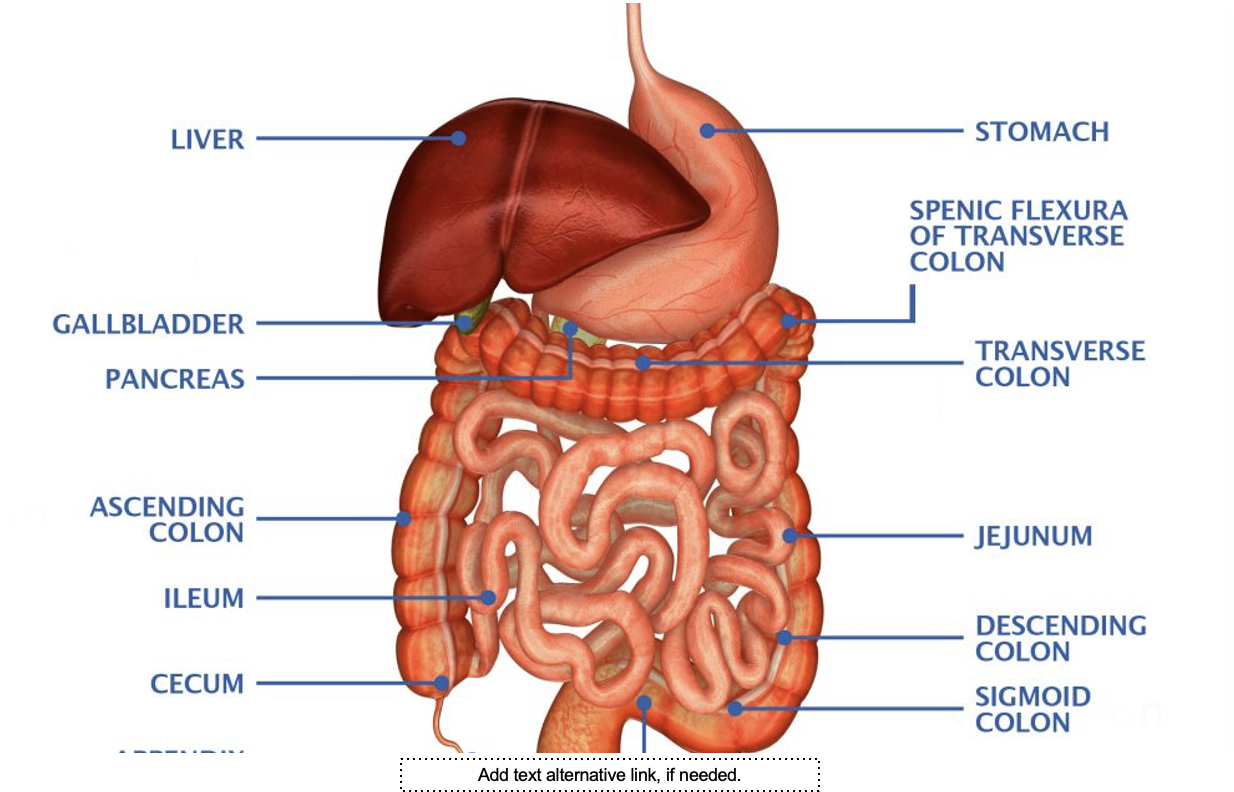
What is this system
Digestive system
The organs of the digestive System fall
into two main groups
the alimentary canal (gastrointestinal or GI tract) and the accessory digestive organs.
The accessory Organs of Digestion
Teeth, tongue, gallbladder, digestive glands (salivary
glands), liver, and pancreas
The accessory digestive glands produce a variety of
secretions that help break down foodstuffs.
Ingestion
Taking in food into the digestive tract
Propulsion
moves from through the alimentary canal,
includes swallowing (voluntary action), and peristalsis(
involuntary action)-constriction
Mechanical breakdown
increases the surface area of ingested food, physically preparing it for chemical digestion by enzymes. Includes segmentation-rhythmic constrictions of the small intestine. Mixes food with digestive juices and
make absorption more efficient
Digestion
a series of catabolic reactions in which enzymes
break down complex food molecules into smaller molecules.
Absorption
passage of digestive end products, vitamins,
minerals, and water, from the GI tract into blood or lymph.
Defecation
elimination of indigestible substances from the
body via the anus in the form of feces.
Most digestive organs reside in the
abdominopelvic cavity
All ventral body cavities contain
slippery serous membrane.
The peritoneum of the abdominopelvic cavity is the most
extensive of the membranes.
Visceral peritoneum
covers the external surfaces of most
digestive organs and is continuous with the parietal
peritoneum which lines the body walls.
Peritoneal cavity
found between the visceral and parietal
peritoneum
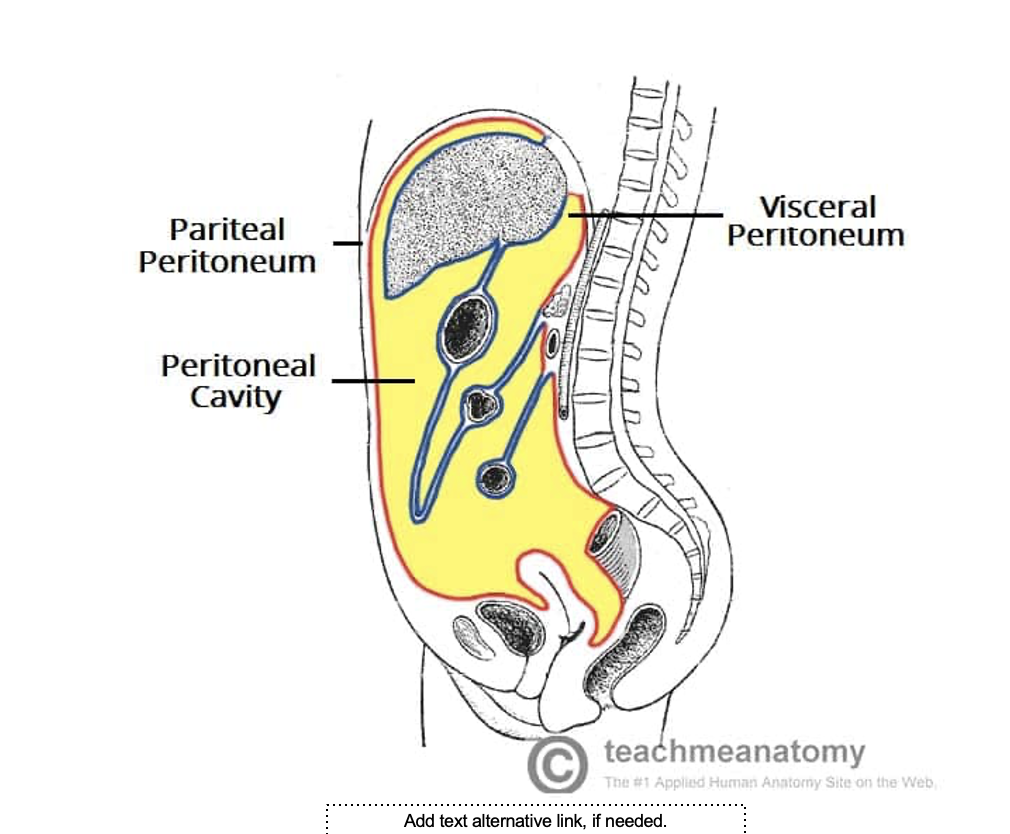
what is this image
cavities of the body
Mesentery
A double layer of peritoneum-a sheet of two serious
membranes fused back-to-back that extends to the
digestive organs from the body wall.
• Provide routes for blood vessels, lymphatics, and nerves
to reach the digestive viscera.
• Hold organs in place and store fat
• It is dorsal in most places and attaches to the posterior
abdominal wall. There are also ventral mesenteries.
• Not all alimentary canal organs are suspended by
mesenteries.
Retroperitoneal Organs
Organs which lose their mesentery during
development and come to lie posterior to the
peritoneum,
• Some regions of the small intestines, most of
the pancreas and duodenum.
Intraperitoneal or peritoneal organs
Keep their mesentery and remain in the
peritoneal cavity.
Clinical
Connection
Peritonitis
• Inflammation of the
peritoneum
• Can result from a piercing
abdominal wound,
perforating ulcers, poor
sterile technique during
abdominal surgery.
The walls of the alimentary canal have the same
four basic layers or tunics
Mucosa
• Submucosa
• Muscularis externa
• Serosa
Mucosa (mucous membrane)
innermost layer, secretes mucus,
digestive enzymes, and hormones, absorbs the end products of
digestion into the blood, protect against infectious disease.
Submucosa
external to the mucosa, contains a rich supply of blood
and lymphatic vessels, lymphoid follicles, and nerve fibers, it is
abundant in elastic fibers
Muscularis Externa
surrounds the submucosa, responsible for
segmentation and peristalsis, contains sphincters that act as valves to
control food passage from one organ to next and prevents backflow
Serosa
the outermost layer is the visceral peritoneum
Blood Supply
Splanchnic circulation-
arteries that branch from
the abdominal aorta to
serve the digestive
organs and the hepatic
portal circulation.
The Enteric Nervous System
Is the nerve supply to the alimentary canal.
• Contains enteric neurons that regulate
digestive activity.
• Submucosal nerve plexus occupies the
submucosa
• Myenteric nerve plexus(larger) lies
between the circular and longitudinal
muscle layers of muscularis externa.
Functional
Anatomy of the
Digestive System
Ingestion occurs
only in the mouth
Mouth (oral
cavity/buccal
cavity)
Lips and Cheeks
Keep food between the teeth when we chew
• Orbicularis Oris-forms the fleshy lips
• Buccinators-form the cheeks
• Oral vestibule
• Labial frenulum
• Palate-hard and soft palates
• Palatine raphe
• Tongue-skeletal muscles, grips the food, mixes the food
with saliva to form bolus, lingual frenulum, contains
papillae: filiform papillae, fungiform papillae, vallate
papillae, and foliate papillae
Ankyloglossia
Salivary Glands
Secrete saliva
• Cleanses the mouth
• Dissolves food chemicals so they can be tasted
• Moistens food and helps compact it into a bolus
• Contains the enzyme-amylase-begins the
digestion of starchy foods,
• Parotid gland-anterior to the ear between the
masseter muscle and the skin, contains the
parotid duct
Submandibular
gland-lies between
the media aspect of
the mandibular body.
Sublingual gland-lies
anterior to the
submandibular gland
Salivary glands are
composed ot two
types of secretory
cells
Serous cells-produce a watery secretion
containing enzymes, ions, and tiny bit of mucin.
• Mucous cell-produces mucus-stringy, viscous
solution
Composition of Saliva
Water-97 to 99%
• Acidic-6.75 to 7.00
• Electrolytes (Na, K, Cl, PO4, HCO3)
• Contains amylase and lingual lipase
• Contains mucin, lysozyme, IgA
• Urea and uric acid
Function
of Saliva
Protects against microorganisms
• Contains IgA antibodies
• Lysozyme
• Defensins
Control of
Salivation
Parasympathetic division of the
autonomic nervous system-
Chemoreceptors
mechanoreceptorsSalivatory nuclei.
• Dehydration
Clinical Connection
Anything that inhibits the production of saliva promotes
tooth decay.
• Decomposition of food particles accumulates and
bacteria flourish. Halitosis
Mumps
Common in children
• Inflammation of the parotid glands caused by the mumps virus.
THE TEETH
Found in sockets in the gum-covered margins of the
mandible and maxilla.
• By age 21, there are two sets of teeth, primary and
permanent dentitions.
• Primary dentitions-deciduous teeth
• Frist set at about 6 months
• About 24 months, all twenty milk teeth should have emerged.
• Fall out between 6 and 12 years old.
• Wisdom teeth (third molars) emerge between ages 17 and 25
Classification of the Teeth
Shape and function
• incisors-cutting, holding, or nipping off
• Canines-tearing and piercing
• Premolars and molars-grinding and crushing
• Dental Formula
• 2I, 1C, 2M(upper jaw)/2I, 1C, 2M(lower jaw) x2 = 20 teeth
• 2I, 1C, 2PM, 3M (upper jaw)/2I, 1C, 2PM, 3M (lower jaw) x2 =32
teeth.
Structure of the Tooth
Crown and the root
• Enamel covers the crown-exposed part of the tooth
above the gingiva (gum), is the hardest substance in the
body.
• The root-the portion embedded in the jawbone
• The neck connects the crown and the root
• Cement-covers the outer surface of the root and
attaches the root to the thin periodontal ligament.
Dentin
bonelike material, underlies the enamel cap and
forms the bulk of a tooth. Surrounds a central pulp cavity-
contains, blood vessels and nerve fibers.
Pulp
supplies nutrients to the tooth tissues and provides
tooth sensation
Root canal
where the pulp cavity extends into the root.
• Apical foramen-found at the end of the root canal.
Deglutition
(swallowing) involves four cranial nerves.
The epiglottis closes off the glottis so that the bolus moves
to the esophagus.
Peristalsis
moves the bolus through the esophagus.
Anatomy of the Stomach
The stomach has three layers of smooth muscle in its
walls, each oriented in a different direction.
The lining of the stomach has rugae for more surface area
to accommodate gastric pits that lead to gastric glands.
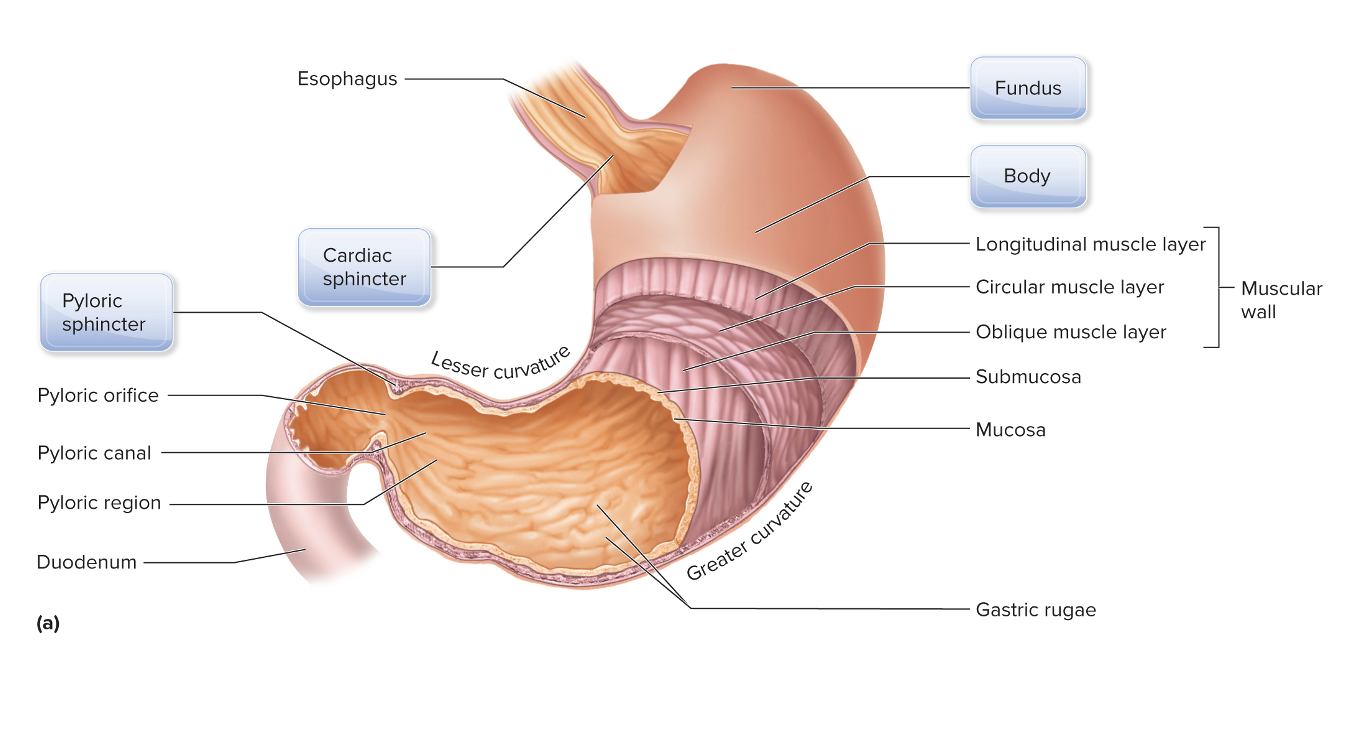
What organ is this?
Stomach
Gastric pits and gastric glands are composed of five
types of cells:
Mucous cells produce alkaline mucus.
• Endocrine cells produce gastrin.
• Parietal cells produce hydrochloric acid and intrinsic factor.
• Chief cells produce pepsinogen and gastric lipase.
• Regenerative cells are stem cells to replace all other cells.
Physiology of Digestion in the Stomach
During swallowing, the medulla oblongata sends signals to
the stomach, telling it to relax.
• The cardiac sphincter opens to allow the bolus to enter.
• Stretching of the stomach walls starts peristaltic
contractions.
• The pyloric sphincter remains closed until the pH of the
stomach contents reaches 2.
Physiology of Digestion in the Stomach
Hydrochloric acid changes pepsinogen to pepsin so that
proteins are partially digested.
• Hydrochloric acid activates lingual lipase, which partially
digests lipids along with gastric lipase.
• Intrinsic factor binds to vitamin B12 so that it can be
absorbed later.
• Once gastric secretions are mixed with the bolus, it is
called chyme
Negative feedback: moving food to small intestine
pH of chyme falls, stomach pH approaches 2
• Endocrine cells stop producing acids
• Causes pyloric sphincter to open and chyme to leave the
stomach into the duodenum
Anatomy of Digestive Accessory Structures
Liver
The liver’s four lobes are arranged in hepatic lobules.
• Hepatocytes produce bile that contains bile acids and
lecithin, both of which aid in the chemical digestion by
emulsifying lipids.
• Bile is released into hepatic ductules leading to the hepatic
duct
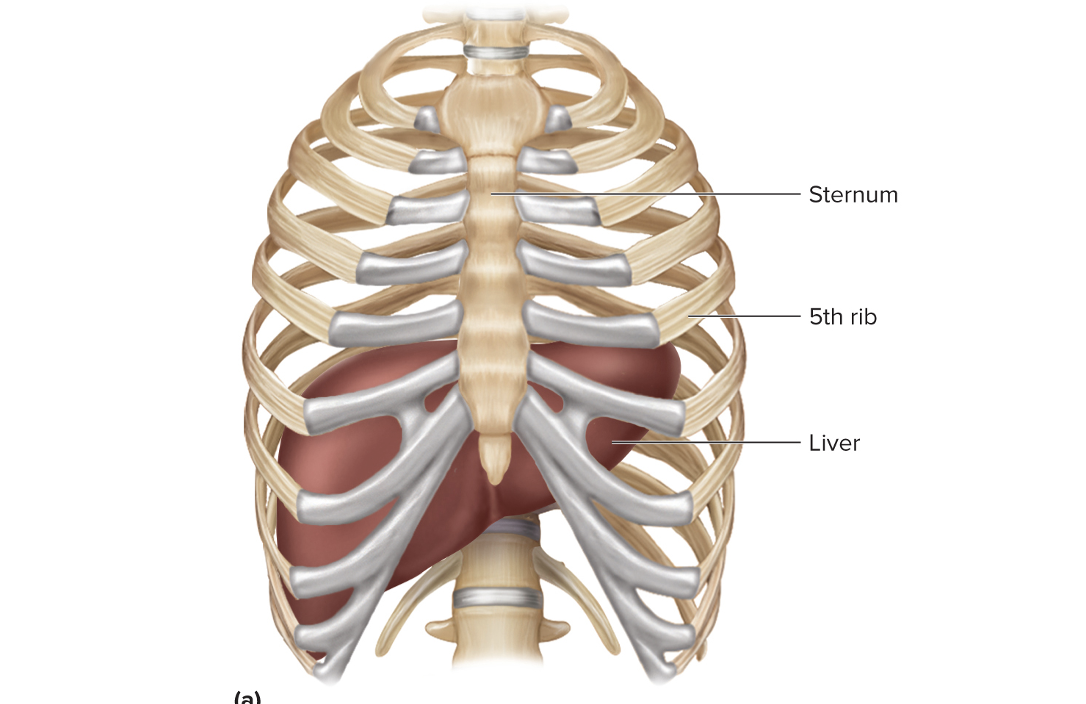
Which organ does this image show?
Liver
The common bile duct is a
tube common to the hepatic
duct, the cystic duct, and the pancreatic duct.
The hepatopancreatic sphincter
controls the opening of
the common bile duct to the duodenum
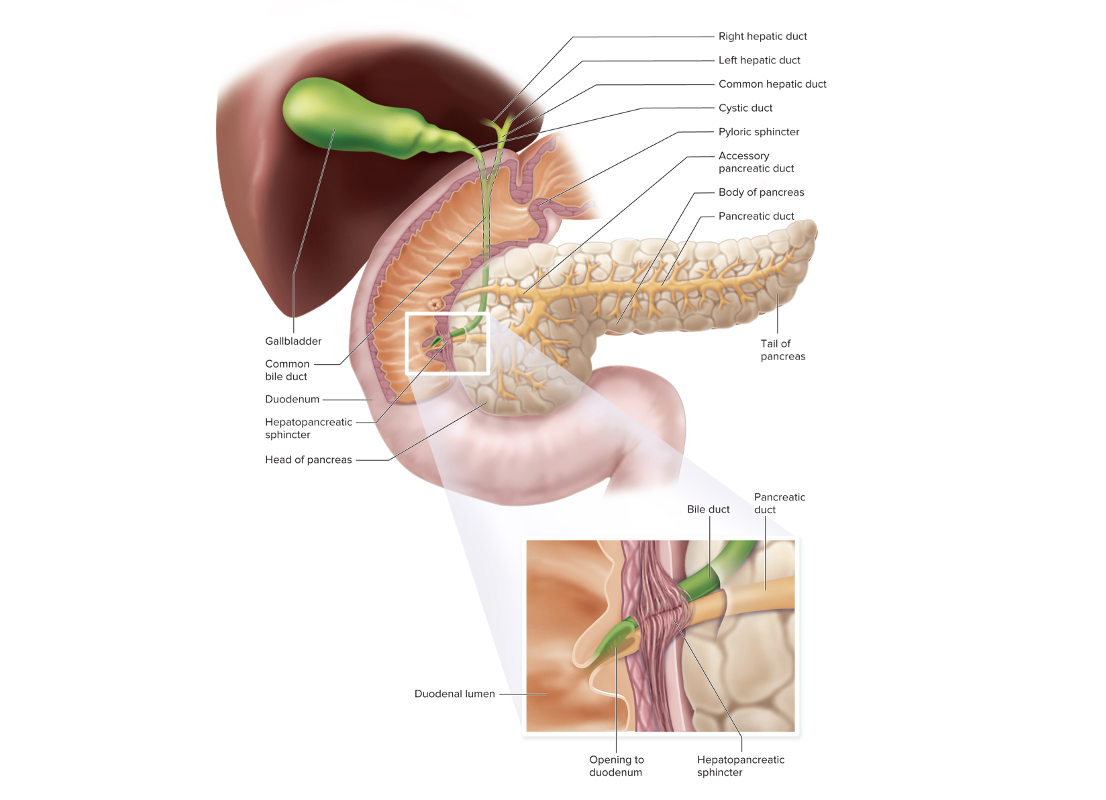
Gallbladder, Pancreas, and Bile Ducts
Gallbladder, Pancreas, and Bile Ducts
The gallbladder collects
the overflow of bile from the
common bile duct and concentrates it.
The pancreas
secretes bicarbonate ions and enzymes for
carbohydrate, lipid, and protein digestion.
Anatomy of the Small Intestine
The small intestine is composed of the duodenum, the
jejunum, and the ileum.
• All parts of the small intestine have smooth muscle in their
walls and are lined by villi.
• Endocrine cells of the duodenum secrete secretin and
cholecystokinin.
the ileocecal valve controls
the movement of materials
from the small intestine to the colon.
Physiology of Digestion in the Small Intestine
Secretin is released from endocrine cells of the duodenum
in response to the acidic chyme.
• Secretin tells the pancreas to release bicarbonate ions to
neutralize the chyme in the duodenum.
Physiology of Digestion in the Small Intestine
Cholecystokinin is secreted by endocrine cells in the
duodenum in response to the presence of lipids.
• Cholecystokinin targets the gallbladder (telling it to release
bile) and the hepatopancreatic duct (telling it to relax).
Physiology of Digestion in the Small Intestine
The release of bicarbonate ions from the pancreas carries
the digestive enzymes through the pancreatic duct to the
duodenum, where all further chemical digestion is
completed
Segmentation
ensures that all the contents of the small
intestine come in contact with villi for absorption
Peristalsis
further moves the contents through the
jejunum and ileum to the ileocecal valve.
Absorption of Nutrients in the Small Intestine
Monosaccharides and amino acids are absorbed through
the epithelium of the villi into capillaries by facilitated
diffusion.
• Fatty acids and glycerides are absorbed across the
epithelial membranes of the villi by diffusion, coated with
proteins, and exocytosed to lacteals.
Anatomy of the Large Intestine
The colon is composed of the cecum, the ascending
colon, the transverse colon, the descending colon, the
sigmoid colon, and the rectum.
The anus contains two sphincter muscles: the smooth
muscle internal anal sphincter, controlled by the
autonomic nervous system, and the skeletal muscle
external anal sphincter, controlled by the somatic
nervous system
Physiology of Digestion in the Large Intestine
The large intestine absorbs water, compacts materials to
form feces, and then stores the feces until they are
removed through defecation.
• Bacteria living in the large intestine produce vitamin K and
flatus
Stretching of the stomach and duodenum causes a
mass movement of fecal material from the transverse colon to
the rectum.
Stretch receptors in the rectal walls initiate the defecation
reflex.
• Defecation happens voluntarily when the external anal
sphincter is relaxed.
Types of Absorbed Nutrients
Proteins, carbohydrates, lipids, vitamins, and minerals are
absorbed in the small intestine.
Circulation of Absorbed Nutrients
The hepatic portal vein drains nutrient-rich blood from the
capillaries in the villi and carries it to the capillary beds in
the liver.
• The fatty acids and glycerides absorbed into lacteals in the
villi join the bloodstream at the subclavian veins and
eventually reach the liver through the hepatic artery
Control of Digestion
The autonomic nervous system controls digestion.
• Parasympathetic fibers of the vagus nerve stimulate
digestion.
• Sympathetic neurons from the celiac ganglion suppress
digestion in part by diverting blood to skeletal muscles and
the heart.
Functions of the Digestive System
The functions of the digestive system include ingestion,
digestion, absorption, and defecation.
Effects of Aging on the Digestive System
Tooth enamel thins, and the gingiva recede.
• The lining of the stomach atrophies.
• The liver may metabolize drugs differently.
• Movement of material through the large intestine slows
with age.
A barium swallow/upper GI series is an
X-ray test used
to evaluate the upper GI tract, which includes the
esophagus, stomach, and small intestine
A colonoscopy
is a procedure in which a lighted
colonoscope is used to visualize the colon.
Computerized tomography (CT)
s an imaging technique
to visualize internal structures
A fecal occult blood test
is a noninvasive procedure that
detects blood in stool
Hepatic screening
is a collection of several tests used to
determine whether the liver is functioning properly
Laparoscopy
is a procedure in which a lighted
laparoscope is used to visualize, collect biopsies from or
perform surgical procedures in the abdomen or pelvic
region
Magnetic resonance imaging (MRI)
is a imaging technique to visualize soft tissue internal structures.
Proctoscopy
is a procedure in which a lighted endoscope is used to visualize the rectum.
Sigmoidoscopy
is a procedure in which a lighted endoscope is used to visualize the lower colon and rectum
A stool culture
is procedure that involves collecting a
stool sample and performing various tests to detect the
presence of disease-causing pathogens
An ultrasound
is an imaging technique in which sound waves are used to visualize internal structures.
Leukoplakia
White patches that occur on the surface of the tongue,
inside the mouth, or on the inside surfaces of the cheek
• Usually from contact with rough surfaces like dentures,
tobacco products, or teeth with rough surfaces
Gastroenteritis
Inflammation of the gastrointestinal tract caused by a
bacterial, viral, or parasitic infection.
Diverticular Disease
Small pouches (diverticula) in the lining of the large
intestine as it ages
• A person with multiple diverticula has a condition known
as diverticulosis.
Abdominal Hernias
Protrusions of the contents in the abdomen through a weak
portion in the abdominal wall
• Inguinal hernias—protrusions into the groin
• Umbilical hernias—through the umbilicus where the
umbilical cord was once attached
• Incisional hernias—protrusions through an incision from
past abdominal surgery
Irritable Bowel Syndrome
Abdominal pain and discomfort, a change in the frequency
of bowel movements, and a change in the consistency of
stool
Crohn’s Disease
Autoimmune inflammatory bowel disease that causes
chronic inflammation along the gastrointestinal tract
• Usually associated with the intestines
Peptic Ulcers
Erosions of the Lining of the Digestive Tract
• Esophageal ulcers—may happen in the lower esophagus if there is
reflux of gastric juices through the cardiac sphincter
• Gastric ulcers—in the stomach, usually from bacteria
• Duodenal ulcers—the most common; caused when the chyme
entering the duodenum is not sufficiently neutralized
Intussusception
When a portion of the intestines folds back into itself,
similar to a telescope, resulting in obstruction of the
intestines and possible ischemia
Cirrhosis
Formation of scar tissue in the liver
• Scar tissue will eventually block blood flow to parts of the
liver and interfere with the liver’s ability to function
properly.
• Two main causes of cirrhosis are excessive alcohol
consumption and chronic hepatitis infection.
Hepatitis
Inflammation of the Liver
Hepatitis A
virus causes acute liver disease
Hepatitis B
transmitted by contact with infected blood or
other bodily fluids, sexual contact, mother to newborn,
shared needles
Hepatitis C
more likely causes a chronic infection;
spreads by contact with infected blood and by sharing
contaminated needles
Hepatitis D
rare in U.S., very serious
Hepatitis E
Outbreaks are usually associated with
contaminated water supplies.