Endometriosis + PCOS
1/96
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
97 Terms
What is endometriosis?
Endometriosis is a chronic condition characterized by the growth of hormone-responsive endometrial tissue outside the uterine cavity
Where are ectopic endometriotic implants found?
Typically, found on the peritoneal surface, within the ovary or invading the rectovaginal septum
Can be found in other regions
What is the overall prevalence of endometriosis?
among reproductive-age people is around 10% (190 million)
What is endometriosis often followed up with?
Accompanied by pelvic pain or infertility in up to 90 million persons worldwide
What are the social symptoms associated with endometriosis?
Work absenteeism, social isolation, and high costs of therapy
What is the stats of having endometriosis?
one in ten
What is endometriosis network canada dedicated to?
to providing education, awareness, hope, and support services for individuals with #Endometriosis
What is the experience of pain and cramps for those with endometriosis?
Those with endometriosis typically describe menstrual pain that is far worse than usual
Tend to report that the pain increases over time
Is the severity of pain a reliable indicator?
▸The severity of the pain isn't necessarily a reliable indicator of the extent of the condition
▸Some people with mild endometriosis have intense pain, while others with advanced endometriosis may have little pain or even no pain at all
What are common sign and symptoms of endometriosis:
▸Painful periods (dysmenorrhea). Pelvic pain and cramping may begin before a period and extend several days. There can be lower back and abdominal pain.
▸Pain with intercourse. Pain during or after sex is common with endometriosis.
▸Pain with bowel movements or urination. Most likely to experience these symptoms during a period.
▸Excessive bleeding. Occasional heavy periods (menorrhagia) or bleeding between periods (menometrorrhagia).
▸Infertility. Endometriosis is first diagnosed in some people who are seeking treatment for infertility.
▸Other symptoms. The experience of fatigue, diarrhea, constipation, bloating or nausea, especially during menstrual periods.
What are some other symptoms prominent during mensuration?
The experience of fatigue, diarrhea, constipation, bloating or nausea, especially during menstrual periods.
What is the relationship between fertility and endometriosis?
Endometriosis is first diagnosed in some people who are seeking treatment for infertility.
What is the Excessive bleeding?
Occasional heavy periods (menorrhagia) or bleeding between periods (menometrorrhagia).
What is menorrhagia
Occasional heavy periods
What is menometrorrhagia
bleeding between periods
What is Pain with bowel movements or urination?
Most likely to experience these symptoms during a period.
What are Painful periods (dysmenorrhea)?
Pelvic pain and cramping may begin before a period and extend several days. There can be lower back and abdominal pain.
What are Pain with intercourse?
Pain during or after sex is common with endometriosis.
What is dysmenorrhea?
Painful periods
Where are the most common sites of endometrosis?
▸ The ovaries
▸ The fallopian tubes
▸ Ligaments that support the uterus (uterosacral ligaments)
▸ The posterior cul-de-sac, i.e., the space between the uterus and rectum
▸ The outer surface of the uterus
▸ The lining of the pelvic cavity
Where else can you find endometrial tissue?
▸ The intestines
▸ The rectum
▸ The bladder
▸ The vagina
▸ The cervix
▸ The vulva
What is the current gold standard for diagnosis?
Direct visualization of endometriotic implants is the current gold standard for diagnosis
Where are superficial lesions found?
lesions are found on the peritoneal or ovarian surfaces.
How do superficial lesions appear?
appear dark blue or brown =hemosiderin content
non-pigmented lesions= usually white in colour and may show vesicular or fibrotic appearances.
What is Haemosidren?
When red blood cells break down and start to release iron
What is a vesicle?
Small fluid-filled sac in the body
What is a fibrotic?
The formation of an abnormal amount of fibrous tissue
What is a laparoscopy?
A small telescope (laparoscope) is inserted into the abdomen to look directly at the internal tissue.
Laparoscopies are always carried out under general anesthetic.
What can you do alongside a laparoscopy
Various procedures can be performed in order to destroy or remove the endometriosis, endometriotic cysts and release scar tissue (adhesions).
What were physicians taught that endometrial implants were?
▸ Physicians were taught that endometriosis implants were blue-black “powder burns” or “mulberry lesions”.
▸ In recent years, several stages of implant development have been appreciated, each with a corresponding appearance.
What is the variety of early lesions of implants appear as?
Can appear as papular excrescences (solid mass) or vesicles, and can range in colour from clear to bright red.
What are lesions in phase with eutopic endometrium?
About one third of lesions are in phase with the eutopic endometrium and have a tendency to spontaneously grow and regress.
This characteristic suggests a fluctuating proliferation in association with hormone production during the menstrual cycle.
What are endometriomas?
-Cysts that form in the ovaries when the same kind of tissue that grows in the uterus (endometrium).
-These cysts fill with blood as they grow.
-The blood turns into a dark brown fluid, so endometriomas are sometimes called “chocolate cysts.”
-Endometriomas can cause pain and discomfort, as well as scarring and damage to the ovaries.
Generally what is classification of stages based on?
Is based on the location, amount, depth, and size of the endometrial implants.
What does each stage mean?
Stage I is minimal
Stage II is mild
Stage III is moderate
Stage IV is severe.
What is the aspects of criteria to determine endometrial implants severity?
[1] Extent of the spread of the implants
[2] Involvement of pelvic structures in the disease
[3] Extent of pelvic adhesions
[4] Blockage of the fallopian tubes
What are the 3 theories on how endometriosis began?
Retrograde or Reflux menstruation
Coelomic Metaplasia
Lymph & vascular metastasis
What is the Retrograde or Reflux menstruation theory?
▸ Endometriosis derives from the reflux of endometrial fragments regurgitated through the fallopian tubes during menstruation with subsequent implantation on the peritoneum and the ovary.
What is the steps of retrograde menstruation?
Endometrial cells in menstrual fluid reach the peritoneal cavity
Once adhesion invasion occurs, activation and infiltration of inflammatory and immune flow
After cell growth, angiogenesis and antiapoptosis occurs
Leads to secretion of prostaglandins, estradiol
Finally causing fibrosis scarring pain
What is a summary of steps that occur during retrograde menstruation?
Proposed establishment of peritoneal endometriotic implants via retrograde menstruation, attachment, proliferation, migration, neovascularization, inflammation, and fibrosis.
How was prostaglandin initially discovered?
Two gynecologists discovered that human semen contains a substance that causes contraction of the human uterus
discovered that the active substance in semen was fat soluble
Why was prostaglandin given that name?
Named prostaglandin because it was thought to be secreted by the prostate gland into semen
The seminal vesicles are the major source of prostaglandins
Where are prostaglandins produced?
Are produced in every tissue of the body
Where are prostaglandins made and why?
Are made at sites of tissue damage or infection, where they cause inflammation, pain and fever as part of the healing process
What is coelomic metaplasia?
- a committed cell type (e.g., mesothelium) trans-differentiates into an alternative cell type (e.g., endometrial epithelium).
reprogramming of mesenchymal stem cells may be involved
What are other clinical examples of metaplasia?
-Barrett’s esophagus, where bile acids transform stratified squamous esophageal cells into mucin-containing goblet cells
-And in the lung, where columnar tracheobronchial epithelium can be induced by cigarette smoking to undergo squamous differentiation
What is the lymph & vascular metastasis theory/
▸The metastasis theory hypothesizes that menstrual tissue travels from the endometrial cavity to lymph nodes and from there through lymphatic channels and veins to distant sites.
Where did the lymph and vascular metastasis theory begin from?
Endometriosis has also been identified in sites distant from the pelvis, including abdominal lymph nodes, lungs, pleura, spinal cord, and even in the nose.
What reagents are responsible for the pain during endometriosis?
▸Endometriotic implants secrete estradiol (E2) as well as prostaglandin E2 (PGE2 ), agents that attract
-macrophages,
-neurotrophic peptides,
-enzymes for tissue remodelling,
-and tissue inhibitors,
and proangiogenic substances.
Why can endomteriosis be so painful?
They are infiltrated by sensory, sympathetic, and parasympathetic nerves and elicit an inflammatory response
Peritoneal endometriosis can also release what?
aromatase which means
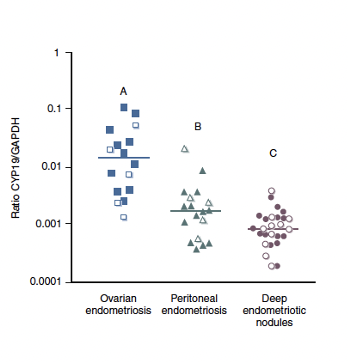
can release estrogen as seen in this
What does Nonsteroidal anti-inflammatory drug help with?
Dysmenorrhea
What does oral contraceptives help with?
Dysmenorrhea
What does aromatase inhibitors help with and what can be a problem?
Helps as a Third line: Dysmenorrhea, chronic pelvic pain
Can Cause: Hypoestrogenism (because aromastse is not active)
What does GnRH agonist help with and what can be a problem?
Helps as a third line: Dysmenorrhea, chronic pelvic pain
Can Cause: Hypoestrogenism because more GnRH creates a negative feedback loop
Why is estrogen related to pain here
it can cause proliferation of implanted tissue which cna cause pain
What is March?
March is endometriosis and PCOS
What is PCOS?
A variable disorder that is marked especially by amenorrhea, hirsutism, obesity, infertility, and ovarian enlargement and is usually initiated by an elevated level of luteinizing hormone, androgen, or estrogen which results in an abnormal cycle of gonadotropin release by the pituitary gland
What is PCOS also referred to as?
Called also polycystic ovary disease, polycystic ovary syndrome, Stein-Leventhal syndrome
Where can dysmenorrhea pain be felt?
iThe pain is typically cramping in nature and may be felt in the lower abdomen, back, or thighs.
What does it mean if dysmenorrhea is primary?
Meaning that there is no underlying medical condition causing the pain
What does it mean if dysmenorrhea is secondary?
which means that it is caused by a medical condition, such as endometriosis or uterine fibroids.
What are options for dysmenorrhea treatment?
May include over-the-counter pain medications, hormonal birth control, or other prescription medications.
What if a functional cyst?
The most common type of ovarian cyst is called a functional cyst.
These cysts are described as "functional" because they often develop during the menstrual cycle
What are follicular cysts?
These usually go away on their own in 1 to 3 months.
These form when an egg doesn't release as expected, so the follicle keeps growing.
What are corpus luteum cyst?
These also usually go away on their own.
These form after the follicle ruptures at ovulation.
The follicle reseals and fluid starts to buildup within it.
They can enlarge and cause pain, bleed, or twist the ovary.
What are the two types of functional cyst?
Follicular
Corpus Luteum cysts
What are 2 other forms of cysts then functional??
can also be related to endometriosis
formed from the outer surface of the ovary (cystadenomas)
formed with non-ovarian tissue (dermoid cysts)
Is PCOS a common endocrine disorder?
PCOS is the most common endocrine disorder in reproductive aged people
With a prevalence between 5% and 15%, depending on the diagnostic criteria applied
What is the relationship between familial occurrence and PCOS ?
It has been well documented that PCOS tends to aggregate within families
In a study of 115 sisters of 80 probands, PCOS was demonstrated in 22% of reproductive-aged siblings whereas hyperandrogenemia was found in an additional 24%.
What genome-wide association?
Studies are a relatively new way for scientists to identify genes involved in human disease
What does genome-wide association tell us?
For small variations, called single nucleotide polymorphisms or SNPs, that occur more frequently in people with a particular disease than in people without the disease
Each study can look at hundreds or thousands of SNPs at the same time
What is the use of SNPS study?
▸Each study can look at hundreds or thousands of SNPs at the same time
▸Researchers use data from this type of study to pinpoint genes that may contribute to a person’s risk of developing a certain disease
What is the the basic characteristics of PCOS?
A familial heterogeneous disorder of reproductive-aged people characterized by hyperandrogenism, ovulatory dysfunction, and polycystic ovary morphology
Do we know the molecular basis for PCOS?
Despite intensive efforts by many investigators, the molecular basis of PCOS remains unclear
What is PCOS is a complex trait modulated by what genetic factors?
Intrauterine and environmental exposures
Insulin resistance
Pancreatic β cell function
Steroidogenesis
Steroid hormone metabolism
What are the criteria for PCOS?
Oligomenorrhea: Infrequent periods
Hyperandrogenism
Polycystic ovaries on Ultrasound
What is a cyst?
The definition of a cyst is a fluid-filled sac
Cysts can occur anywhere in the body
Why do we people develop cyst?
Individuals can develop "cysts" due to eggs not being released over time
The follicles keep growing and form multiple "cysts"
Explain the difference between normal ovary and PCOS?
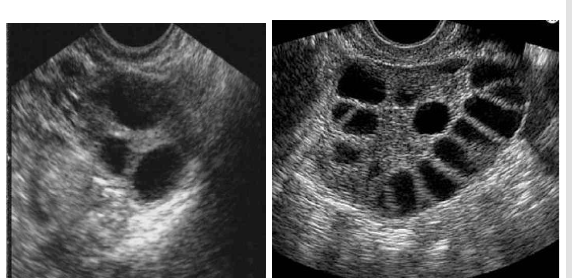
What are the gross characteristics of the polycystic ovaries?
Bilateral enlarged ovaries with a smooth and thickened capsule
On cut section, multiple follicular cysts surrounded by abundant ovarian stroma are found throughout the cortex of the ovary
What are the microscopic characteristics of PCOS?
Subcapsular antral follicles arrested at mid-stage of development
Hyperplasia of theca cell layer
What is the description of how theca and granulosa cells appear in pcos
PCOS follicle has thickened theca cell layer with disrupted and degenerative granulosa cells
Greater width in theca cells, less of a width in granulosa cell layers.
What is hirsutism?
Excessive hair growth
The degree of which is variable from mild to severe
What is the most distinct and visible clinical feature of PCOS?
The most distinctive and visible clinical feature of PCOS is hirsutism
What is the pathophysiology of hirsutism?
In PCOS, the amount of hirsutism has been correlated to serum androgen concentrations
Free Testosterone increased when Sex Hormone Binding Globulin decreases
How can pre-existing conditions affect hirsutism?
Coexisting conditions that alter the bioactivity of androgens, such as hypothyroidism and obesity may also give rise to excessive hair growt
What is menstruation dysfunction?
Menstrual dysfunction is primarily characterized by irregular, infrequent, or absent menstrual bleeding
In approximately 20% of people, there is complete absence of menses, whereas 5% to 10% of cases demonstrate regular ovulatory function
When can the onset of chronic anovulation emerges?
In some, the onset of chronic anovulation emerges beyond adolescence, but this is unusual
Does recognition of normal ovulation in PCOS?
Is significant in that a history of regular menstrual cycles does not exclude the diagnosis
What change in ovulation may occur in women with PCOS later in reproductive life?
It has been reported that in late reproductive life, PCOS women begin to experience regular ovulation [for unknown reasons]
What are some characteristics aging PCOS women with regular menstrual cycles appear to have?
[1] smaller follicle cohort,
[2] higher serum FSH levels and,
[3] lower androgen levels compared to age-matched PCOS with persistent anovulation
What is the ovarian morphology?
Classically, those with PCOS have enlarged ovaries with numerous peripheral small antral follicles and increased central stroma
Normal follicular growth appears to occur up to the mid-antral stage, after which maturation ceases
What happens to the granulosa reaches the mid-antral stage?
The granulosa cell layer becomes progressively degenerative and the entire structure may have the appearance of a thin-walled cyst
What happens to the theca reaches the mid-antral stage?
Layer that surrounds the follicle becomes substantially hyperplastic and thickened compared to that of normal follicles and is responsible for increased androgen production
What do histomorphometric studies show?
Revealed a twofold to threefold increase in the numbers of primary, secondary, and tertiary follicles compared to those of the normal ovary
What do histomorphometric studies show in ?
Ovaries are endowed with a greater number of follicles
Whether the rate of programmed cell death is decelerated compared to the normal ovary has not been systematically studied