Chapter 17 Microbiology : Vaccines, Diagnostics, and Immune Disorders
1/24
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
25 Terms
Active immunization
injecting antigen, which stimulates the immune system and elicits a response. Because of this, antigen-specific antibodies and T cells are made. This category includes vaccines.
Passive immunization
protective antibodies are administered, supplies the immune system with fully synthesized antibodies. This naturally occurs during breastfeeding (IgA). This is the injection or transfer of immunoglobulin. Antitoxins.
- It should not harm the person being vaccinated.
- It should stimulate B cell and T cell responses.
- It should result in long-term memory.
- It should not require many boosters.
- It should protect against the natural pathogen.
What are the requirements of an effective vaccine?
- killed whole cells or inactivated viruses are used. Antigenicity remains. Examples: cholera and rabies.
- live, attenuated (weakened) bacteria or viruses are used. Mutated for growth in host only and mimic infection to generate stronger immunity. Examples: MMR.
- purified components (antigenic subunits) of an infectious agent (acellular or toxoid).
- DNA or RNA vaccines (not commercially available).
What are the four basic types of vaccines?
Herd Immunity
occurs when a large portion of the population is immunized against a threat. Only possible for diseases that are contagious and transmitted between humans. ~3/4 of a population must be immunized to reduce disease through this type of immunity. This type of immunity also varies with each pathogen.
- allergic reactions (which are very rare).
- causes autism or diabetes (false).
- they could be not safe (also false).
What are the major oppositions to vaccines?
specificity
measures how selective an antibody is toward an antigen
Sensitivity
reflects how many antigen or antibody molecules must be present for a test to turn positive.
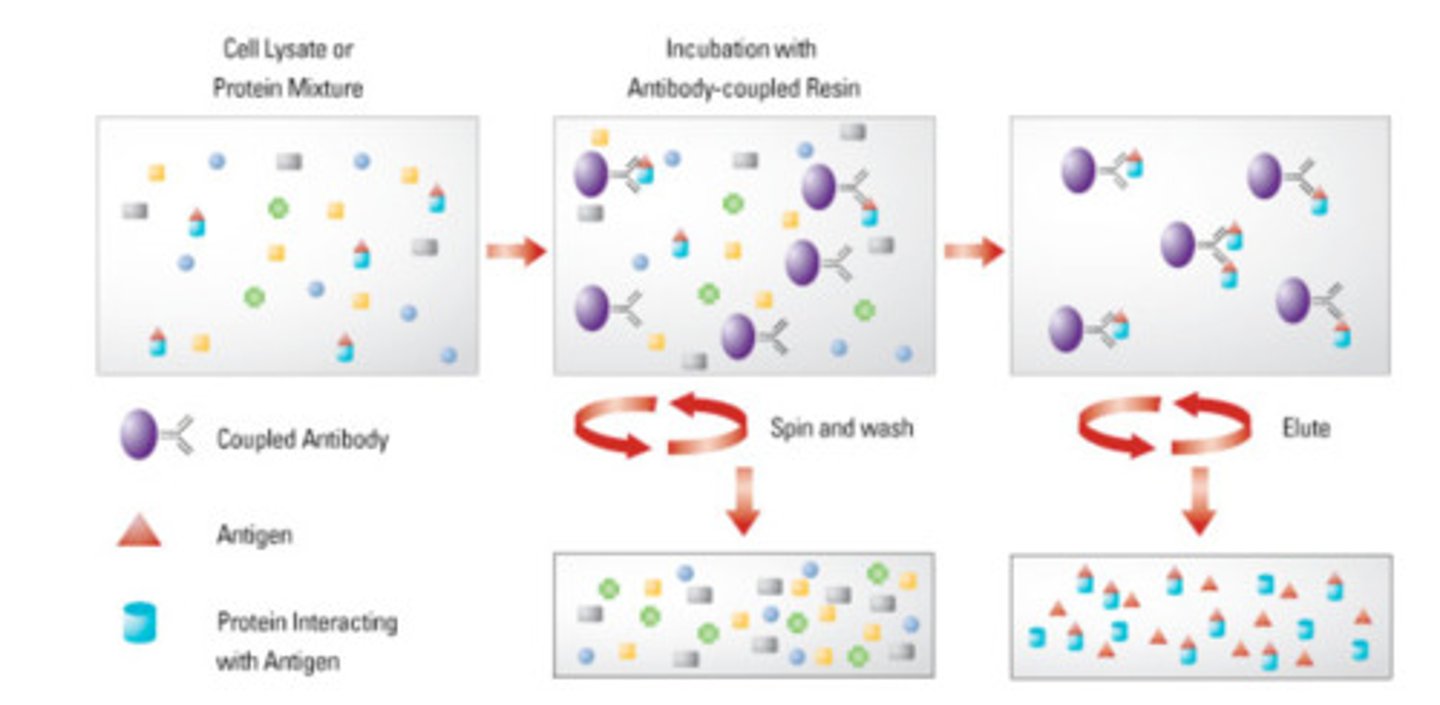
immunoprecipitation
ratio of antigen and antibody dependence. Equivalence: antigenic sites equals antigen-binding sites.
agglutination
like precipitation, is based on antibody-antigen cross-linking. measures insoluble antigen on whole cell and identification of bacterial pathogens. also used in blood typing; two drops of blood are mixed with A antibody and B antibody. Antibody-antigen interaction = Clumping (positive, which indicates your blood type).
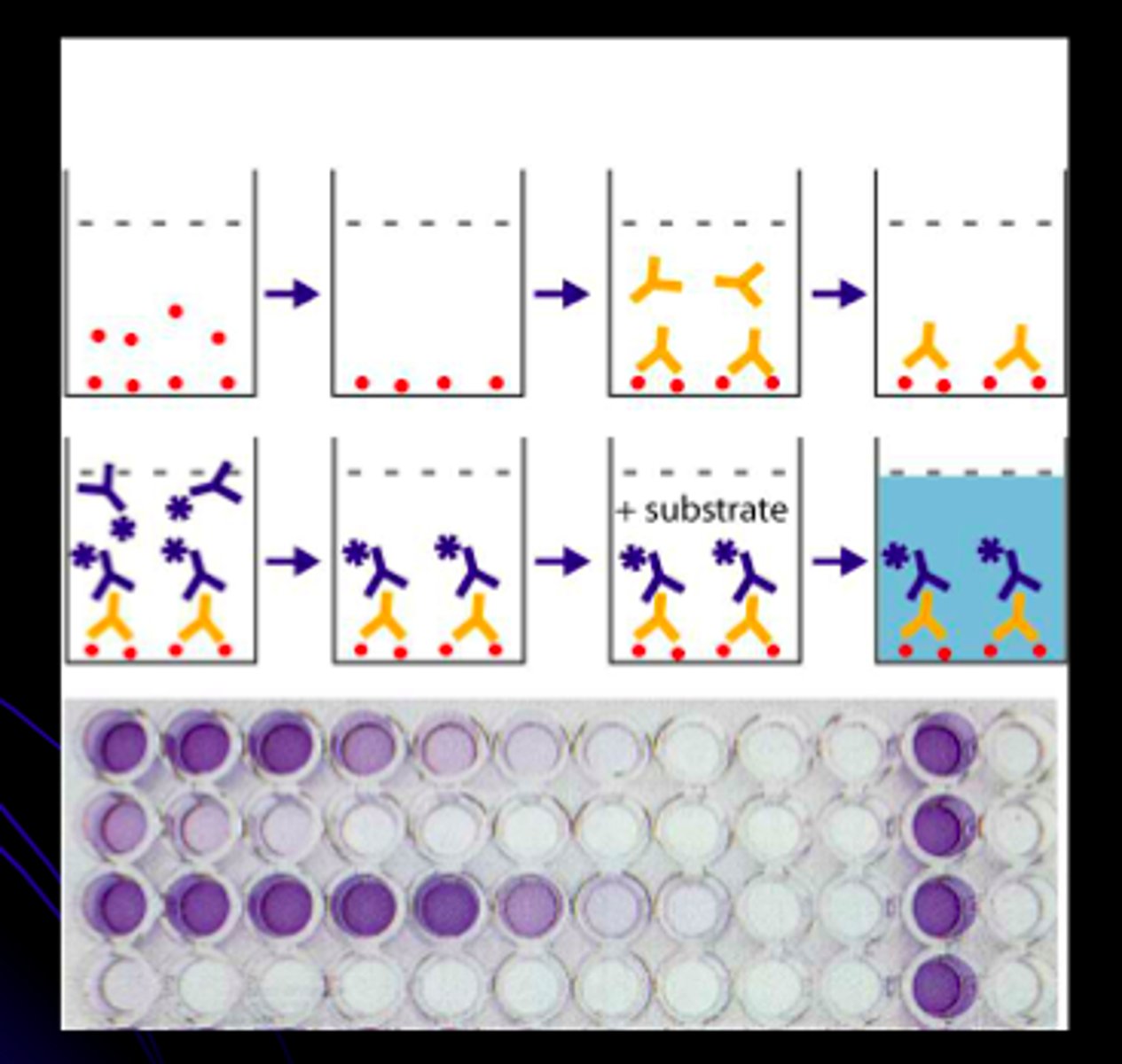
Enzyme-Linked Antibody
converts colorless substrate to a colorful product. used for identification of antibody or antigen.
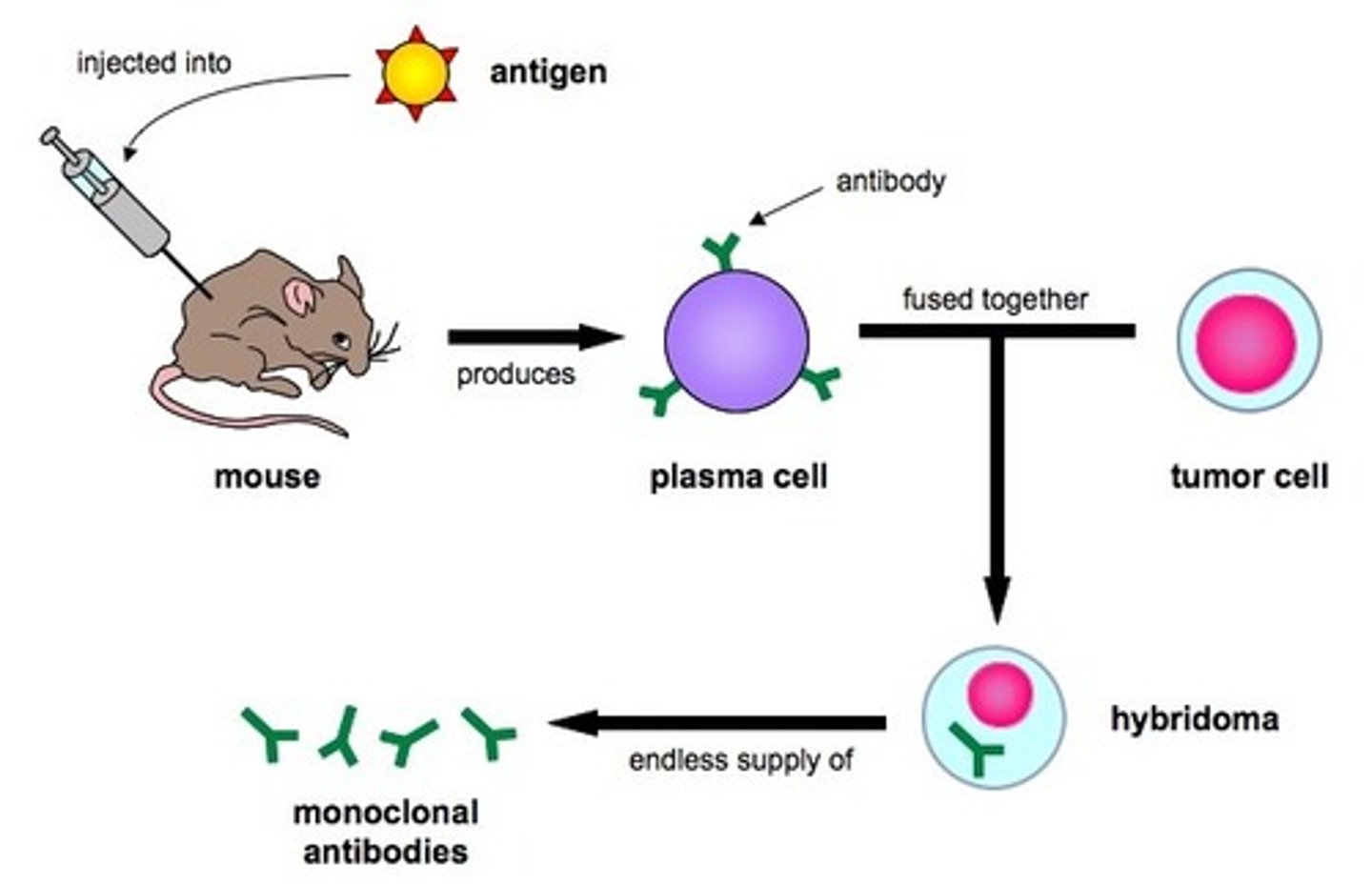
Monoclonal antibodies
epitope-specific antibodies; produced by a single antibody-producing B cell clone.
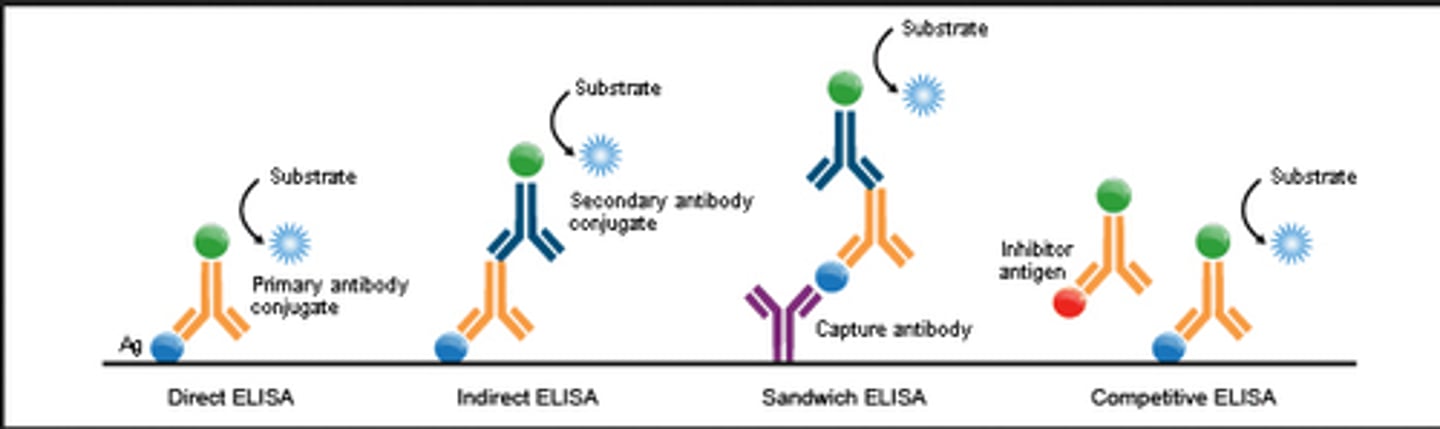
Enzyme-Linked Immunosorbent Assay (ELISA)
three types: direct, indirect, sandwich. Looking for color change to detect antigen.
titer
The measurement used to express the antibody or antigen concentration in a solution is called a
Polyclonal antibody
Antiserum that contains all antibody isotypes with specificities directed against many different epitopes of an antigen.
type I hypersensitivity
symptoms can be mild or severe, but the reaction to the allergen is swift.
anaphylaxis
(type I hypersensitivity) Can be immediate and severe and is known as _______________.
Rhinitis, watery itchy eyes, and sneezing
(type I hypersensitivity) Can be mild and localized and typically causes
Swelling (edema), low blood pressure, cardiovascular collapse, breathing difficulties, suffocation
(type I hypersensitivity) Can cause a systemic response which can cause
Sensitization in Type I Hypersensitivity
• Initial exposure
• Allergen elicits IgE production
• IgE binds mast cells
• Second exposure = mast cell degranulation
- Histamine, leukotriene, and prostaglandin release
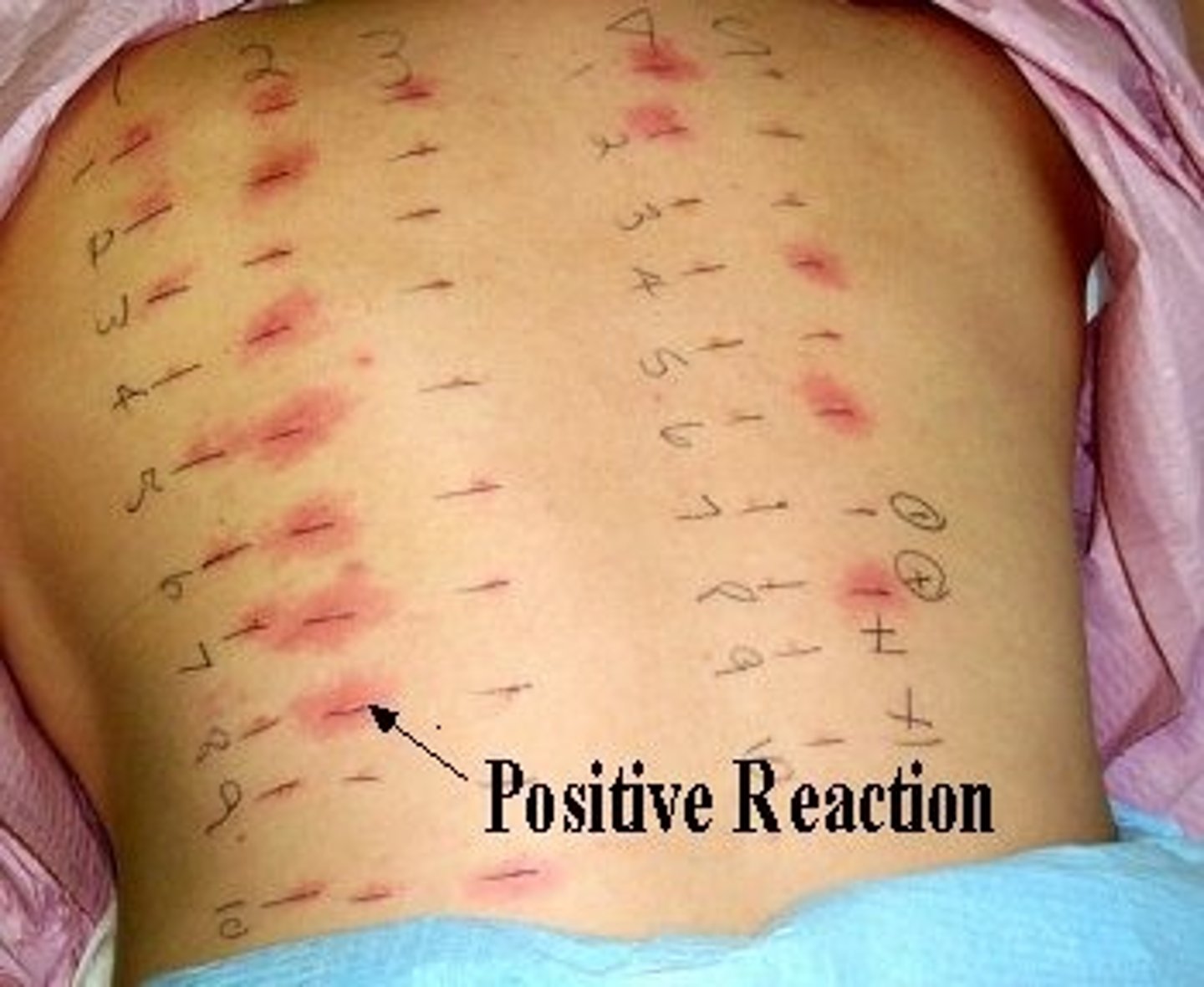
skin test
Allergens are delivered locally to the skin to determine if there is an inflammatory reaction.
Type II hypersensitivity
occurs when antibody binds to antigen on a cell surface.
AB positive, O negative
The universal recipient of blood type is _______. The universal donor of blood type is ________.
Incompatibility occurs - Specific antibodies in serum bind to antigen on foreign red blood cells (RBCs). Eventually, cell lysis will occur.
A patient with blood type A cannot receive blood type B because.....
Rh incompatibility disease
Another type II hypersensitivity.
• Rh antigens are chemical groups on RBCs.
• A mother who is Rh-negative can react to a fetus that inherited the Rh+ gene from the father.