Exam content
1/100
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
101 Terms
what regulates the reproductive system
the complex hypothalamus-pituitary-gonad axis,. it also includes the targets of steroid hormones secreted by the gonads (as well as egg and sperm by LH and FSH)
environmental factors and reproduction
chemical, visual, photic, thermal, and tactile stimuli operate through effects on neural and endocrine factors frequently determine the timing of reproduction
which two hormones control reproduciton
Luteinizing hormone and follicle stimulating hormone
tonic center
located in the hypothalamus of both males and females, maintains a relatively constant pattern on pulsatile release of GnRH and produces static circulating levels of both LH and FSH
surge center
found only in female brains, and is responsible for the midcycle LH surge observed in mature females in response to elevated estrogen (ovulation)
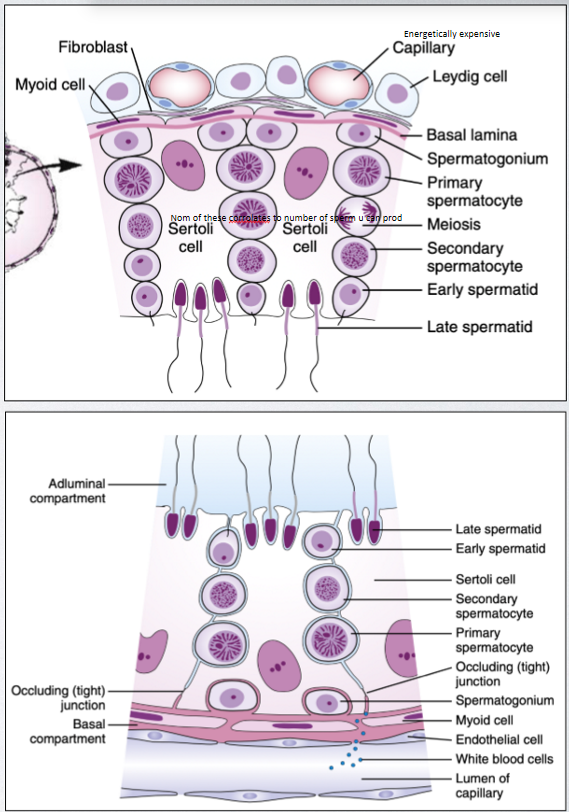
LH and FSH table
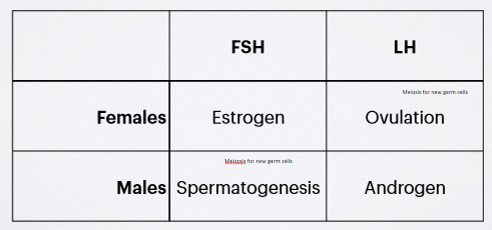
production of estrogens in the female is accomplished by the ovary under stimulation by FSH, and LH and responsible for ovulation; in the male, spermatogenesis in stimulated by FSH, and LH is responsible for stimulating androgen synthesis by the testes. these are just the main effects, there are many more
gonadal steroids
secreted as a result of the action of GTHs on special cells in the ovaries and testes, control differentiation and maintenance of many sexual characters (such as uterus and mammary glands of the F and muscle development and beard growth in human M)
history of gonadal action discovery
recognized hundreds of years ago by the chinese, who used gonadal and placental preparations routinely to treat conditions ranging from impotence in males to the inability of a female to bear sons. They had a level of understanding before science did, that gonadal tissue could release things to treat pathologies
feedback of reproductive system simple
the hypothalamic centers regulating GnRH release are sensitive to circulating steroids that generally produce -ve feedback on GnRH release, the exception to the pattern being the +ve effect by estrogens on release of GnRH from the surge center and subsequent stimulation of LH release from the pituitary
spermatogenesis
controlled by GTHs and a number of paracrine factors, including testosterone, initiated indirectly by FSH through mitotic proliferation of spermatogonia and formation of primary spermatocytes. this increases mitosis in sertoli cells, which are directly proportional to sperm abundance
why is FSH initiation in spermatogenesis indirect
bc FSH acts on receptors in sertoli cells, which release paractine factors
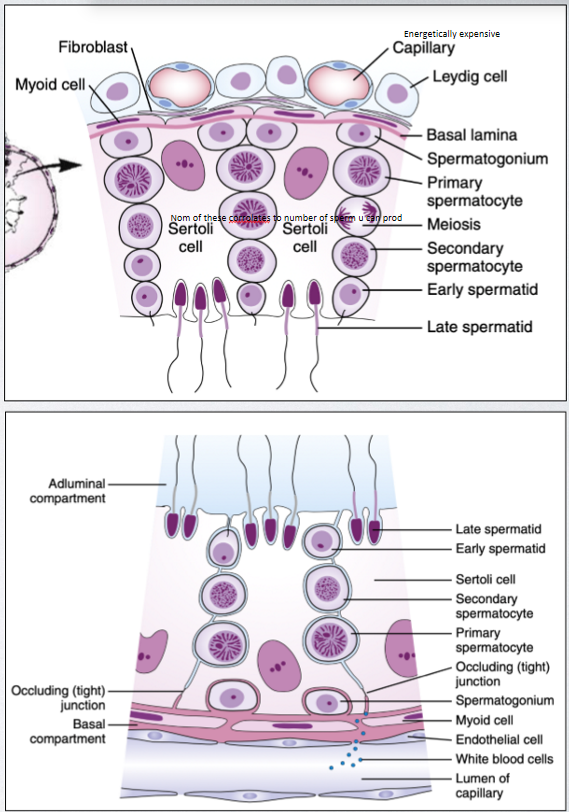
testosterone regulation of testicular functions
testosterone (T) is the major circulating androgen in mammals, although other androgens such as androstenedione or 5α-dihydrotestosterone (DHT) may circulate in significant amounts. T has several important paracrine effects on spermatogenesis and T conc within the testis are generally orders of mag greater than circ testosterone levels
androgen regulation of testicular functions
androgens activate a multitude of genes, one of which produces a gonadotropin-regulated testicular helicase (GRTH/DDTX25) in leydig cells and germ cells. GRTH is transported into the nucleus, where is binds to nuclear RNAs as a component of messenger ribonucleoprotein complexes to promote meiosis
estrogen regulation of testicular function
estrogen receptors are present on germ cells that also possess aromatase activity. the local metabolism of DHT to an androgen metabolite 5α-androstane-3β,17β(3β-diol) has been reported in brain, prostate, and testes. 3β-diol binds and activates ERs which presumably facilitate spermatogenesis, though mechanism is unresolved (aromatase knockout male mice that cannot convert T to estrogens exhibit disruption of spermatogenesis, supporting a local role for ER-binding regulators)
endocrine regulation of testicular functions
androgen actions are probably indirect, as T receptors appear to be absent or occur in very low number on germ cells. essentially, in the early germ cells that will be spermatogonia to produce sperm, these cells are already building up transcripts they need to promotes spermatogenesis. This makes them all ready so that when time, they can produce what they need to. they bind to messenger RNP complex, take prepackaged transcriptions and protect from degradation
eutherian M and F
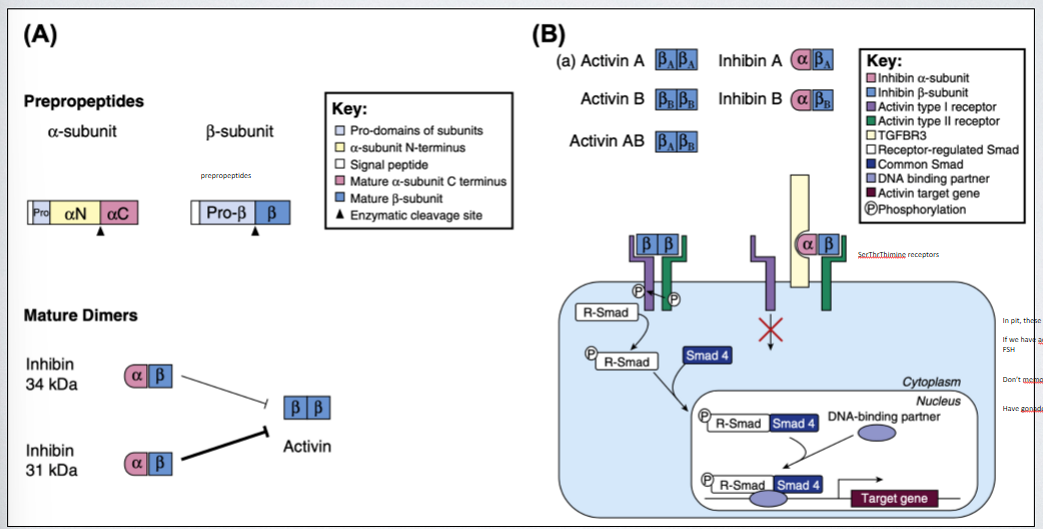
when releasing GnRH in hypothalamus to stimulate LH and FSH in pituitary, especially during surge in F mostly bc we get hugh upregulation of LH and way less FSH bc of -ve feedback response that blocks it owns release through this inhibition pathway. inhibin production in gonadotropes early in surge center, they bind preferentially to type 2 receptors. in pituitary, these release LH and FSH, if we have activin binding to R we see increase in second messenger signaling that promotes release of FSH (dont memorise 2nd messenger pathway). have gonadotropes synthesize and release FSH
ovarian cycle
ovary undergoes cyclical development in response to gonad tissue hormones (GTHs), sometimes seasonally, in humans monthly.
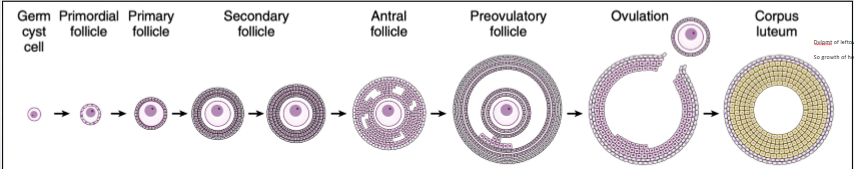
follicular phase
during proestrus, the growth of one of more follicles occurs in the ovaries. start w single germ cyst cell and build tissue of multiple cells around it. preovulatory follicle most advanced, as we build it, it has specific morphology
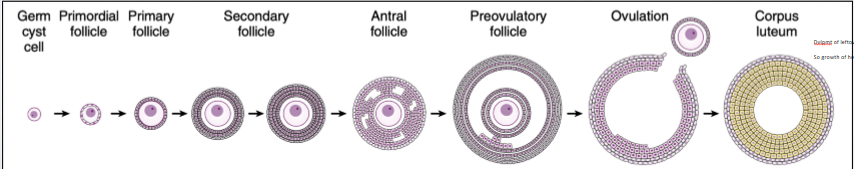
luteal phase
following ovulation, which ends the follicular phase, the remains of a ruptured follicle are transformed into a corpus luteum, thus ovulation also marks the onset of the luteal phase of the ovarian cycle
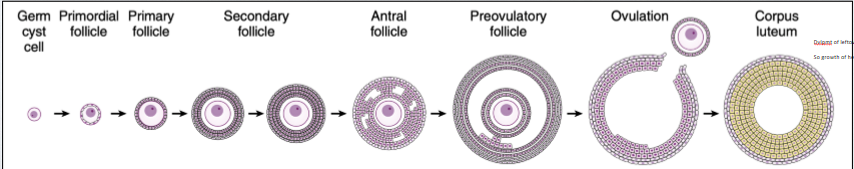
tonic hypothalamic center
releases small quantities of GnRH into the portal circulation and relatively low but rather constant circulating levels of FSH and LH and maintained. under the influence of LH and FSH as well as a variety of paracrine factors, growing ovarian follicle synthesize and release estrogen, predominantly estradiol (17β-estradiol) into the general circulation. so not just releasing germ cells but also becoming endocrine gland, it prod its own estrogen paracrine signalling and also bloodstream to get to surge for +ve feedback so big surge so large estrogen levels as follicular phase. LH stim the thecal cells to prod androgens (principally andostenedione) that are aromatized by the granulosa cells to form estradiol; conversion of androgens to estradiol by the granulosa cells is stim by FSH (FSH also causes the GCs to prod inhibins which feed back on the pit to selectively inhibit FSH). inhibin also inhibits p450aro activity locally in granulosa cells, whereas the related peptide activin increases p450aro activity