VSAC450 - Orthopedics
1/237
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
238 Terms
What is osteomyelitis? What are its etiologies?
inflammation of bone and bone marrow
caused by bacteria or fungi
How did bacteria enter the bone? (4)
1. traumatic contamination from outside --> in
2. traumatic contamination from inside --> out
3. during surgery
4. extension of soft tissue infection
Can osteomyelitis have a hematogenous origin? Where would the bacteria be deposited in such situation?
yes
deposit at ends of bones due slower blood flow at loops
What are common sources of bacteria in the blood stream (4)?
1. nasty teeth
2. cystitis
3. pyoderma
4. umbilical infection
Who commonly gets osteomyelitis? At which part of the bone?
young animals
metaphysis
What are the most common bacteria in canine bone infections (2)? Anaerobe or aerobic bacteria?
Staphylococcus
Streptococcus
Anaerobe
In what situations would result in one and Multiple bacterial infection?
one: hematogeouns
many: trauma/soft tissue extension
What factors favour the conversion of contamination to persistent infection? (4)
Immunosuppression
Fracture instability
Shit blood supply to the bone
Presence of foreign bodies or dead bones
How do biofilm affect osteomyelitis infection?
bacteria clings to hardware --> biofilm protects bacteria from phagocytosis/antibodies/antibiotics + more numerous
How can bacteria develop a biofilm?
Sequestrum: dead, avascular, piece of bone
foreign object
What are common fungi that cause osteomyelitis? (4)
blastomycosis, coccidioidomycosis, histoplasmosis, cryptococcocosis
How do fungi infect the bone? What other organs are typically infected?
hematogenous route
lungs and eyes, enlarged LN
What part of the bone is affected by fungal osteomyelitis? Can they infect ajacent joints?
metaphyses + epiphyses
yes
What are the clinical signs of osteomyelitis? What are the acute vs chronic differences?
lameness, systemic illness + fever ( fungi ONLY)
acute: swelling, redness discharge
chronic: draining tracts
What are draining tracts characteristics associated with osteomyelitis (4)?
small wounds that come and go
can have multiple
often distal to inf
can be associated with sequestrum
What are the radiographic findings for an osteomyelitis infection?
ragged, proliferative bone with areas of lysis
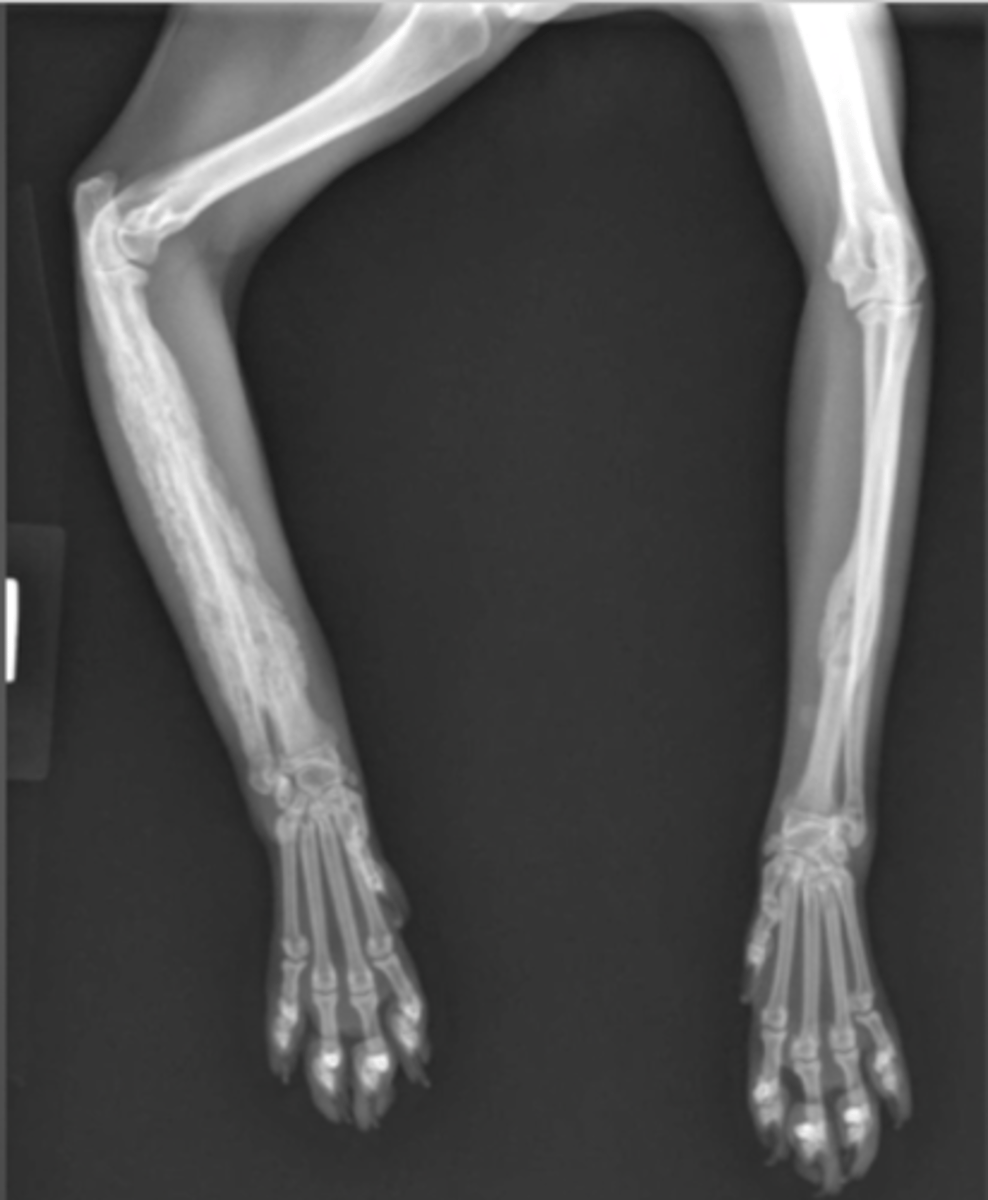
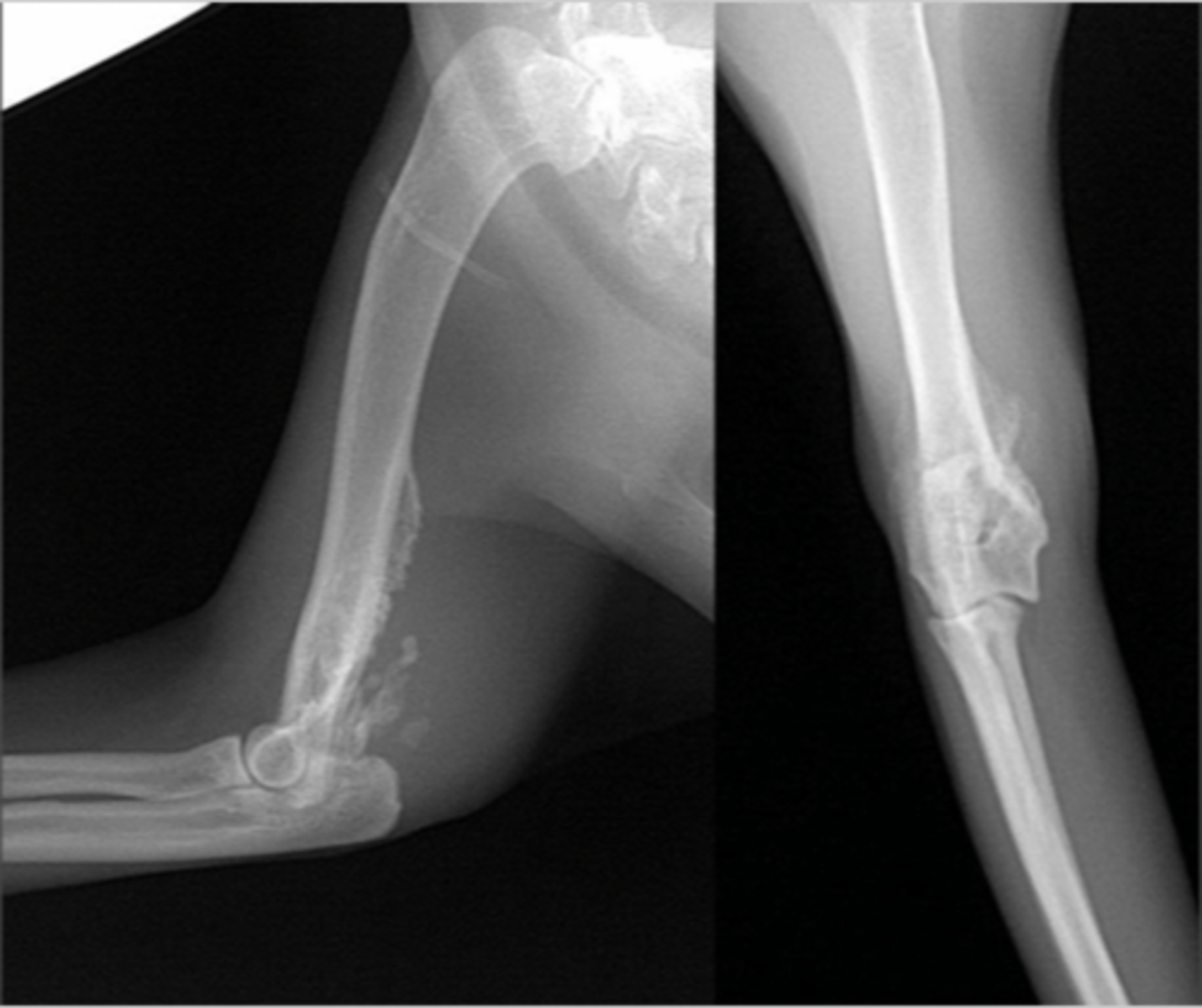
How would you describe this lesion?
lysis and bone proliferation of the distal metaphysis-diaphysis of the humorous
What are the clinical pathological findings of osteomyelitis?
elevated C-reative protein
biopsy
culture (not draining track)
histopathology
How is acute BACTERIAL osteomyelitis treated?
hematogenous: sys antibiotics for 3w minimum
What conditions are necessary to heal from a chronic BACTERIAL osteomyelitis?
can heal with adequate blood supply + stable
How can chronic BACTERIAL osteomyelitis be treated? (5)
remove sequestra
stabilize fracture
remove or replace inf hardware
regional perfusion with antibiotcs
4-6w on systemic antibiotics
How is fungal osteomyelitis treated?
systemic long-teerm antifungal therapy
amputation or debridement
relapses common
What is the common signalment of panosteitis (eosinophilic panosteitis)?
unknown cause, during first 2 years in large breed dogs (young german shepard)
What is the pathogenesis of panosteitis?
high pressure in medullary canal --> excessive bone remodeling --> necrosis of fat of medullary canal --> replaced with fibrous tissue --> woven bone forms + pain
What are the clinical signs of panosteitis? (5)
varying degrees of lameness + shifting
lethargic
febrile
usually eosinophilic
painful when palpate at diaphyses
What lesions are seen on radiograph for a dog with panosteitis?
early: normal
patchy, mottled, sclerotic densities in medullary canal
late: periosteal proliferation
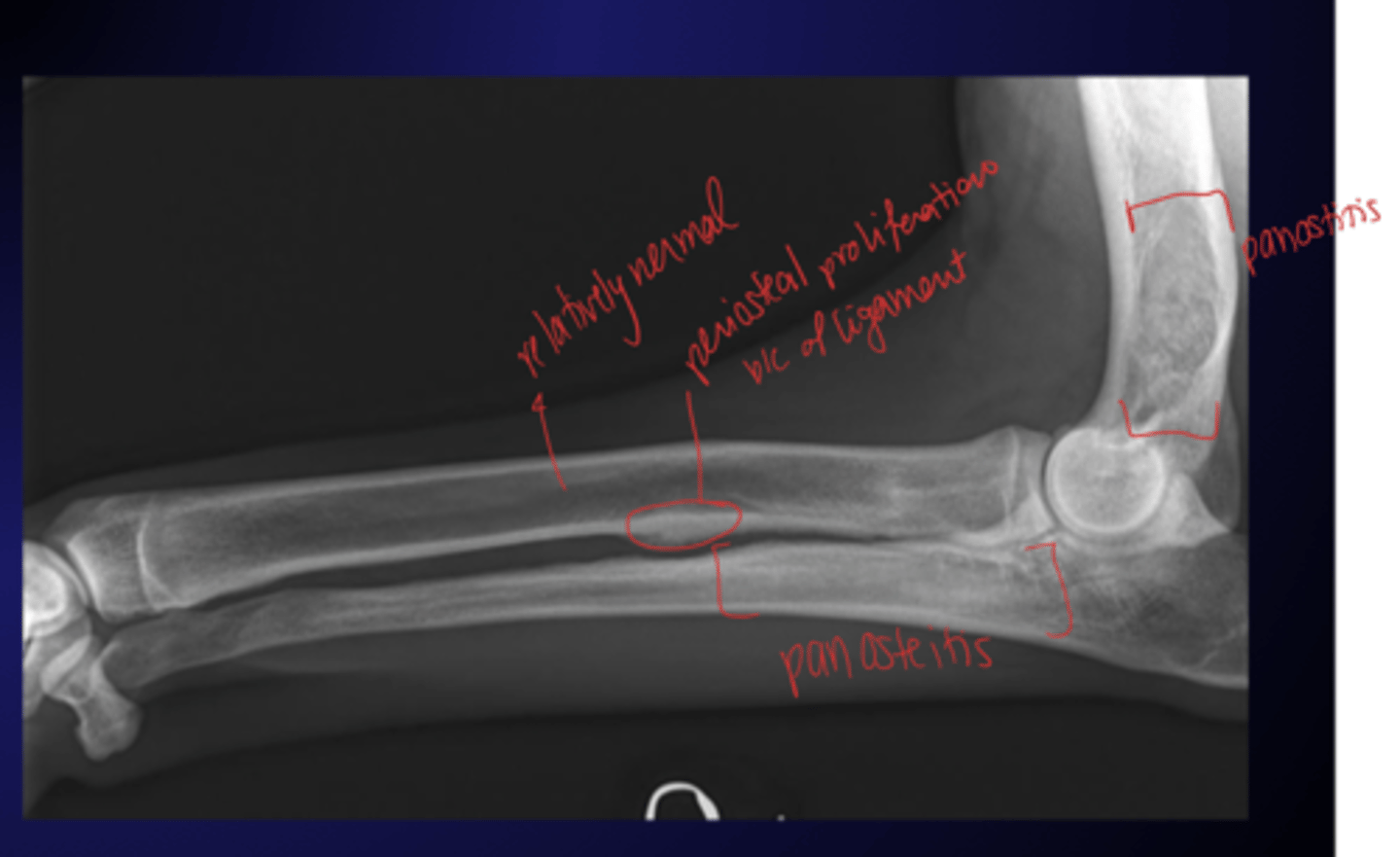
How is panosteitis diagnosed?
rule out other possible cause of lameness
How is panosteitis treated?
self-limiting
can give analgesics
What is the common signalment for a dog with Hypertrophic osteodystrophy (HOD)?
2-6m large breed dog
What are the common clinical signs for Hypertrophic osteodystrophy (HOD)? How long do symptoms last?
symmetrical lameness/swelling at fore/hindlimbs
fever
anorexia
lethargy
7-10 days
What is the pathogenesis for HOD?
immune cells attack metaphysis adjacent to physis --> necrosis, hemorrhage, inflammation, resorbed bone --> physis remodels + widens --> subperiosteal hemorrhage --> periosteal proliferation/flaring of metaphyses
What are the radiographic findings for HOD?
enlargement of metaphyses at radius, ulna and tibia
"double" physis
periosteal proliferation can be there
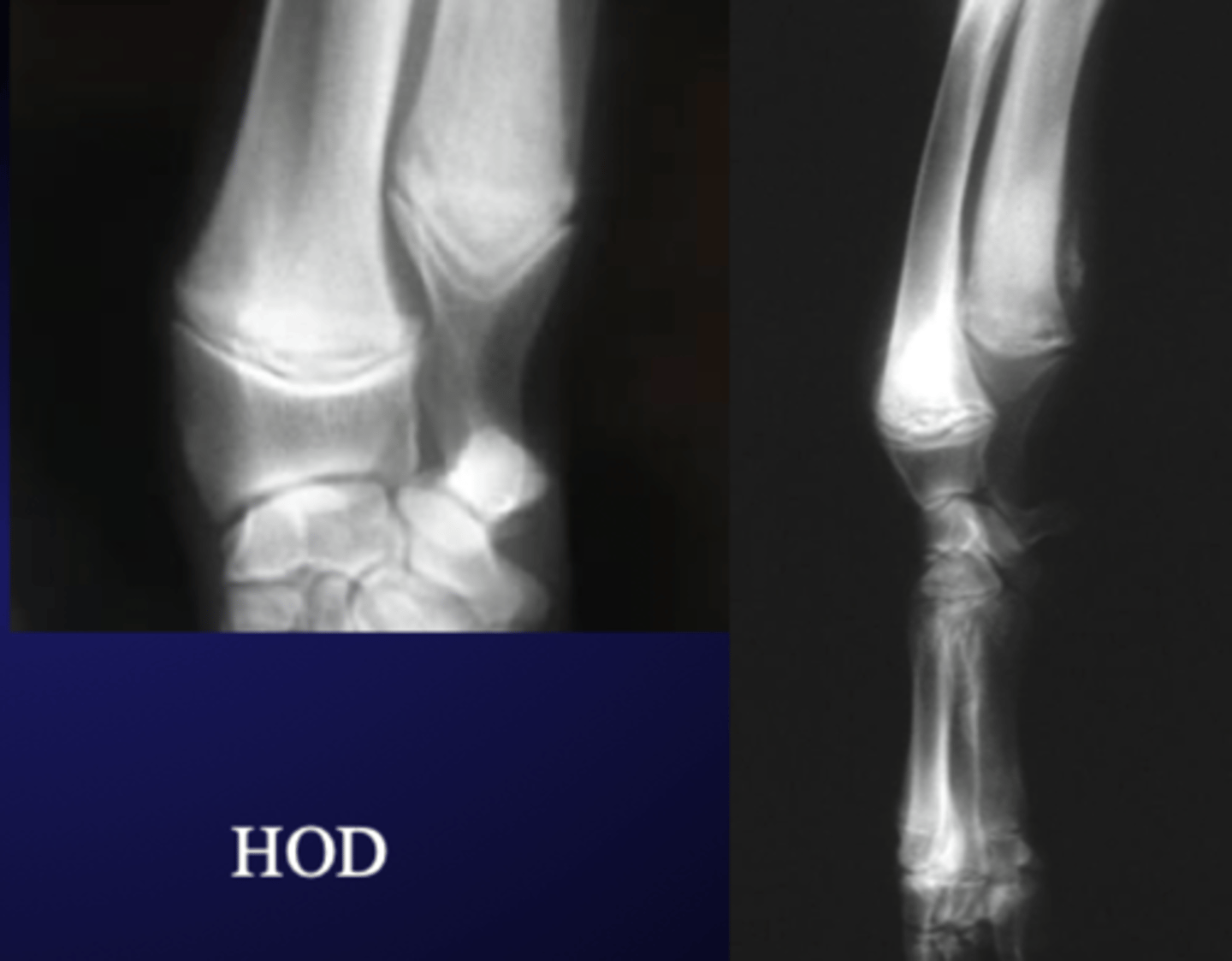
What is the most common etiology for HOD?
immune-mediated disease
bac inf
How is HOD treated? (6)
usually self-limiting
possible limb-deformities
supportive care
analgesics
antibiotic therapy
corticosteroids
What is the signalment of craniomandibular osteopathy?
3-8m west highland white and scottish terriers
How is craniomandibular osteopathy characterized?
proliferation of woven bone in mandibles
painful + difficult to open mouth
What are common radiographic findings for craniomandibular osteopathy?
proliferation of woven bone of mandible and skull
usually bilaterally symmetrical
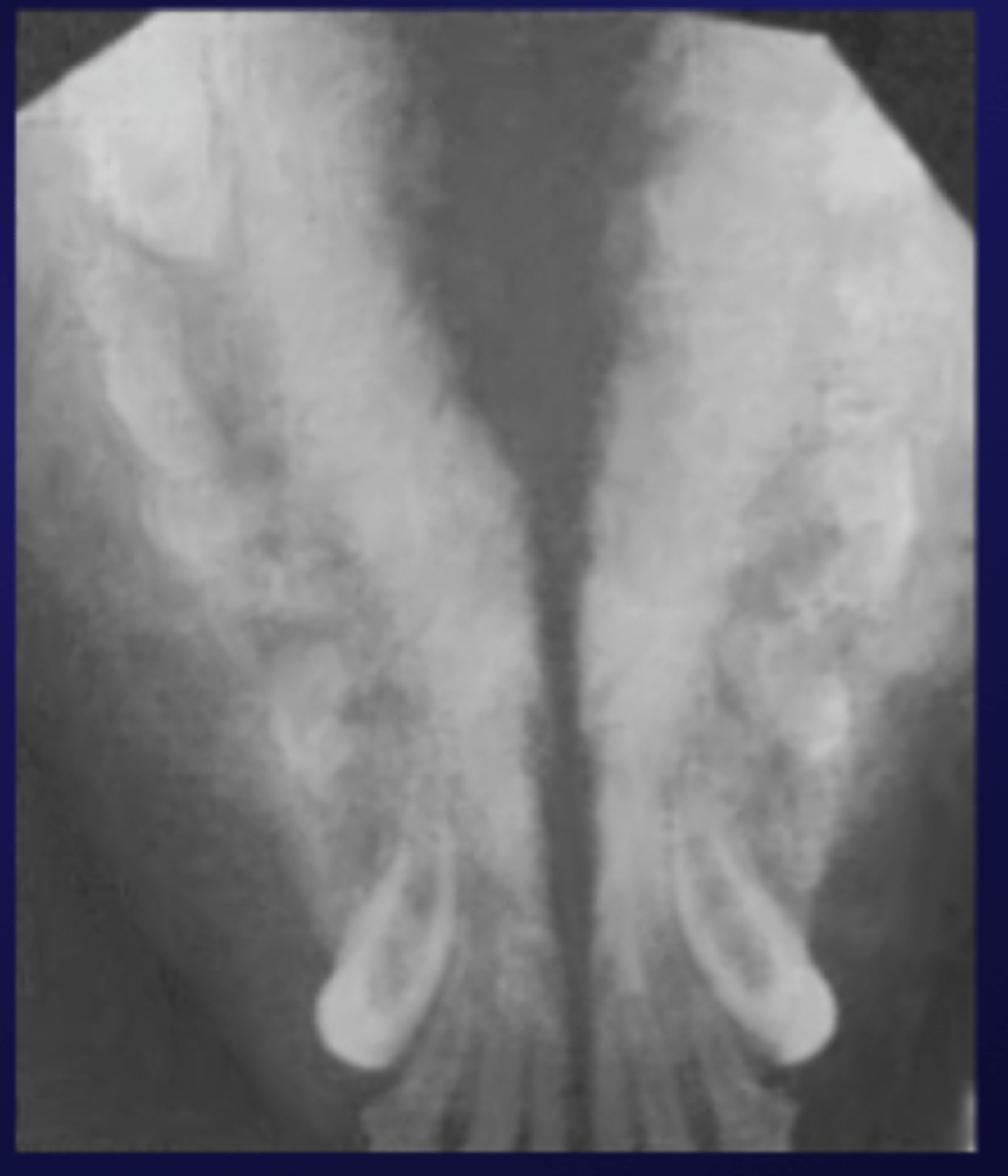
How is craniomandibular osteopathy diagnosed?
radiograph, CT, biopsy to rule out other diseases
How is craniomandibular osteopathy treated?
supportive care, analgesics, wait it out until proliferation recedes
What are characteristics for Hypertrophic Osteopathy (HO)?
symmetrical periosteal proliferation over bones in distal extremeties
associated with thoracic or abdo masses
What are common physical findings for Hypertrophic Osteopathy (HO)?
ok joints
stiff gait in all limbs thicker + painful metacarpi, metatarsi, antebrachium and crus
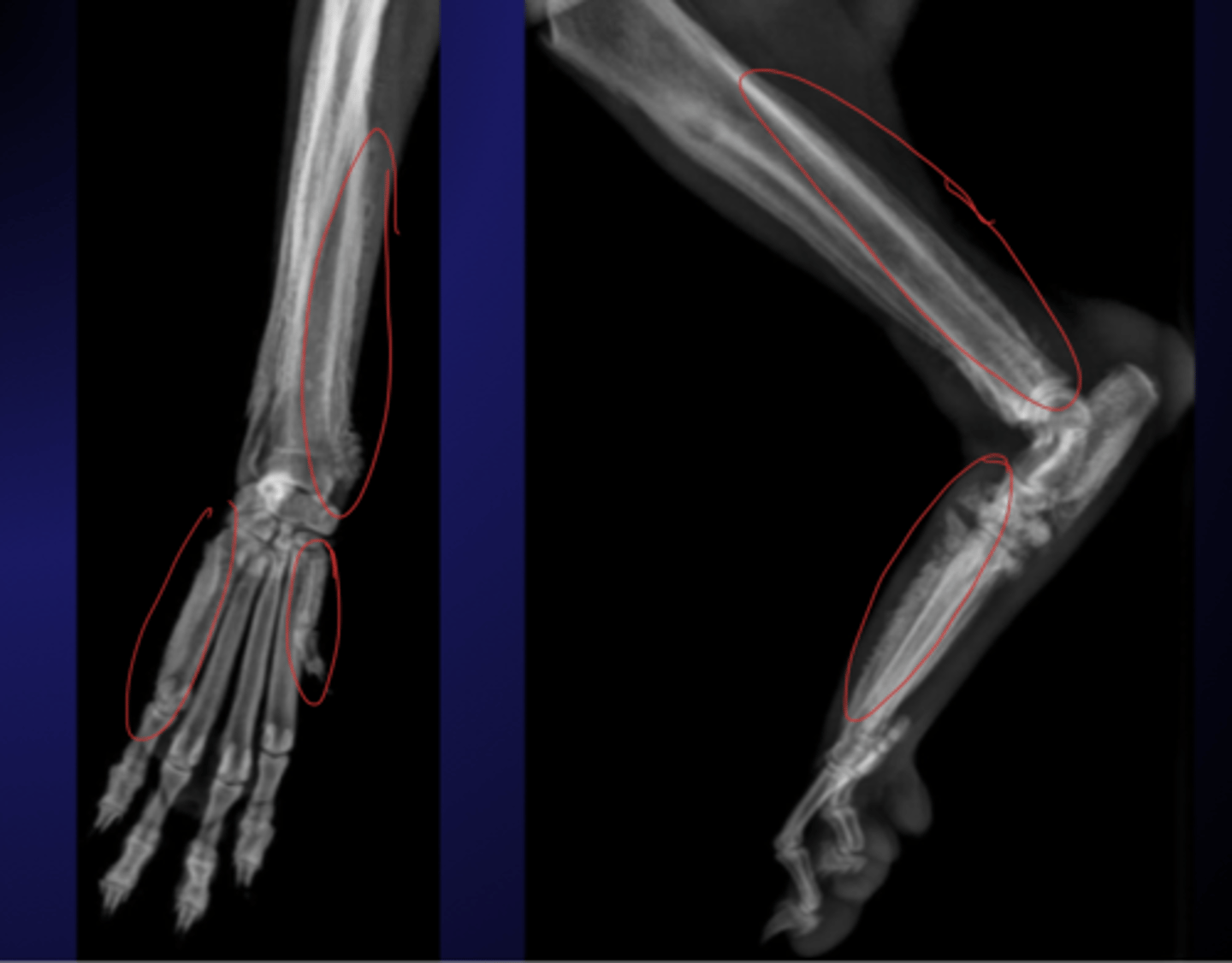
What is the pathophysiology for Hypertrophic Osteopathy (HO)?
mass stimulate autonomic nerves --> vasodilation + increased subperiosteal blood supply --> new bone formation + lifting of periosteum = pain
tumor makes growth factors to continue new vessel and new bone formation
What kind of masses cause HO?
neoplastic (90%), abcess, spirocerca lupi inf
How is HO treated?
analgesics
vagotomy
lesions recede if primary mass is removed
What causes osteopenic and fragility disorders?
Ca/P imbalance due to hyperparathyroidism
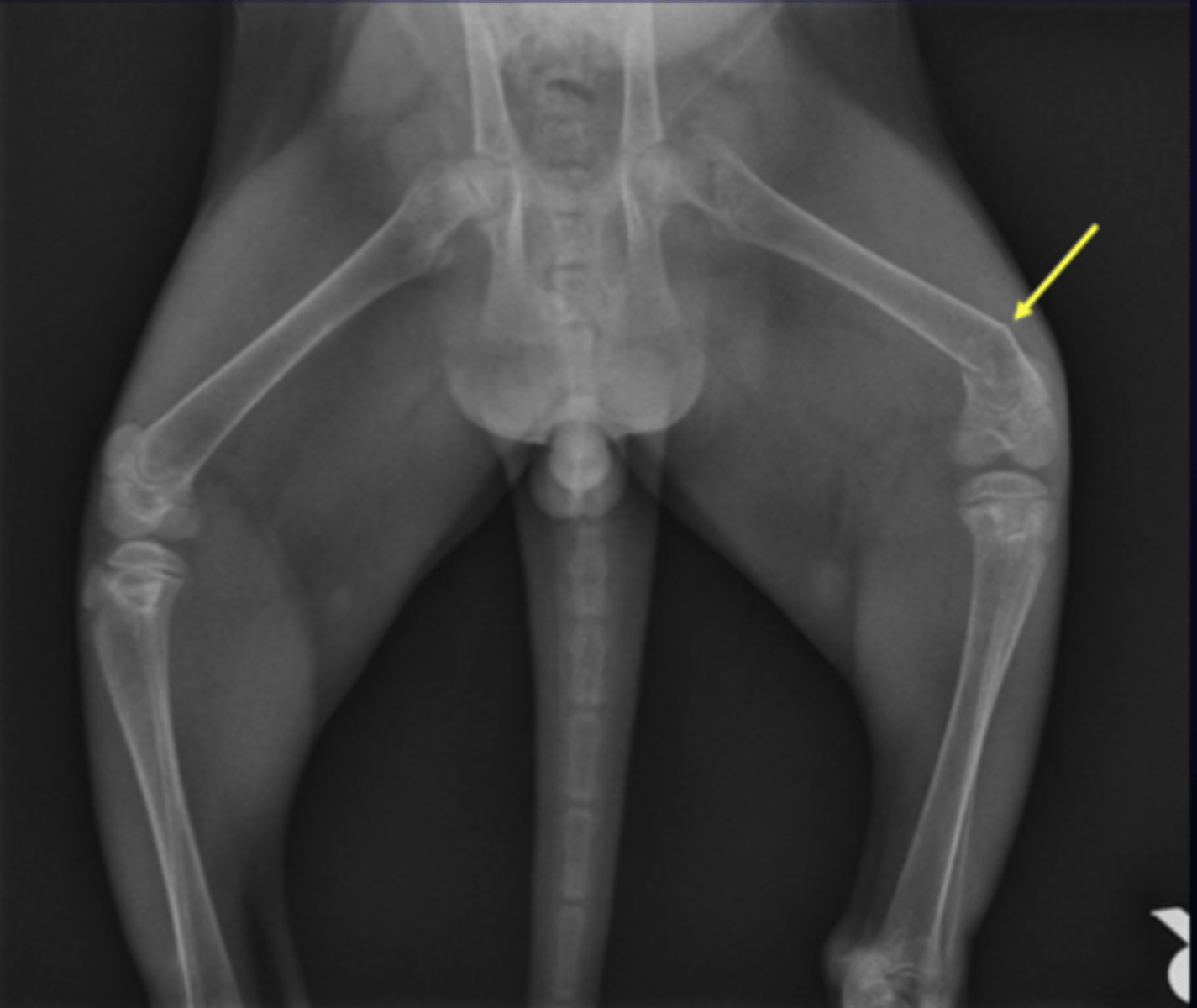
How can primary hyperparathyroidism cause osteopenia (2)?
parathyroid tumour
parathyroid hyperplasia
How can secondary hyperparathyroidism cause osteopenia (2)?
nutritional (low Ca:P ratio)
renal failure
What is the pathogenesis for nutritional secondary hyperparathyroidism?
diet is low in Ca or improper Ca:P ratio --> extra PTH seecreted --> move Ca out of bones into blood --> osteopenic bones --> folding fractures
What are other nutritional problems affecting bones?
Vit A or D deficiency or oversupplementation --> skeletal problems
restricted protein diets in growing animals
What are differential diagnoses for folding fractures (osteopenia)?
vit-D dependent rickets type 2
osteogenesis imperfecta
How is nutritional secondary hyperparathyroidism treated?
correct diet + no internal fixation
What are the characteristics for Diffuse Idiopathic Hyperostosis (DISH)?
flowing bone bridging the vertebral column over 3 continuous disks
stiffness
What are the kinds of Primary Bone Tumours? (5)
osteosarcoma (90%)
chondrosarcoma
fibrosarcoma
hemangiosarcoma
multilobular osteochondrosarcoma (MLO)
What is the common signalment for osteosarcoma (+ chondrosarcoma)?
middle aged (5-9y) giant breed dog
very agressive form seen in 2y olds
What is the common site for osteosarcoma (+ chondrosarcoma)?
metaphyses/epiphyses
doesn't cross joints
distal radius, proximal humerus, both ends of tibia/femur
What are the common radiographic findings for osteosarcoma?
mix of lysis = new bone formation
can get pathologic fractures
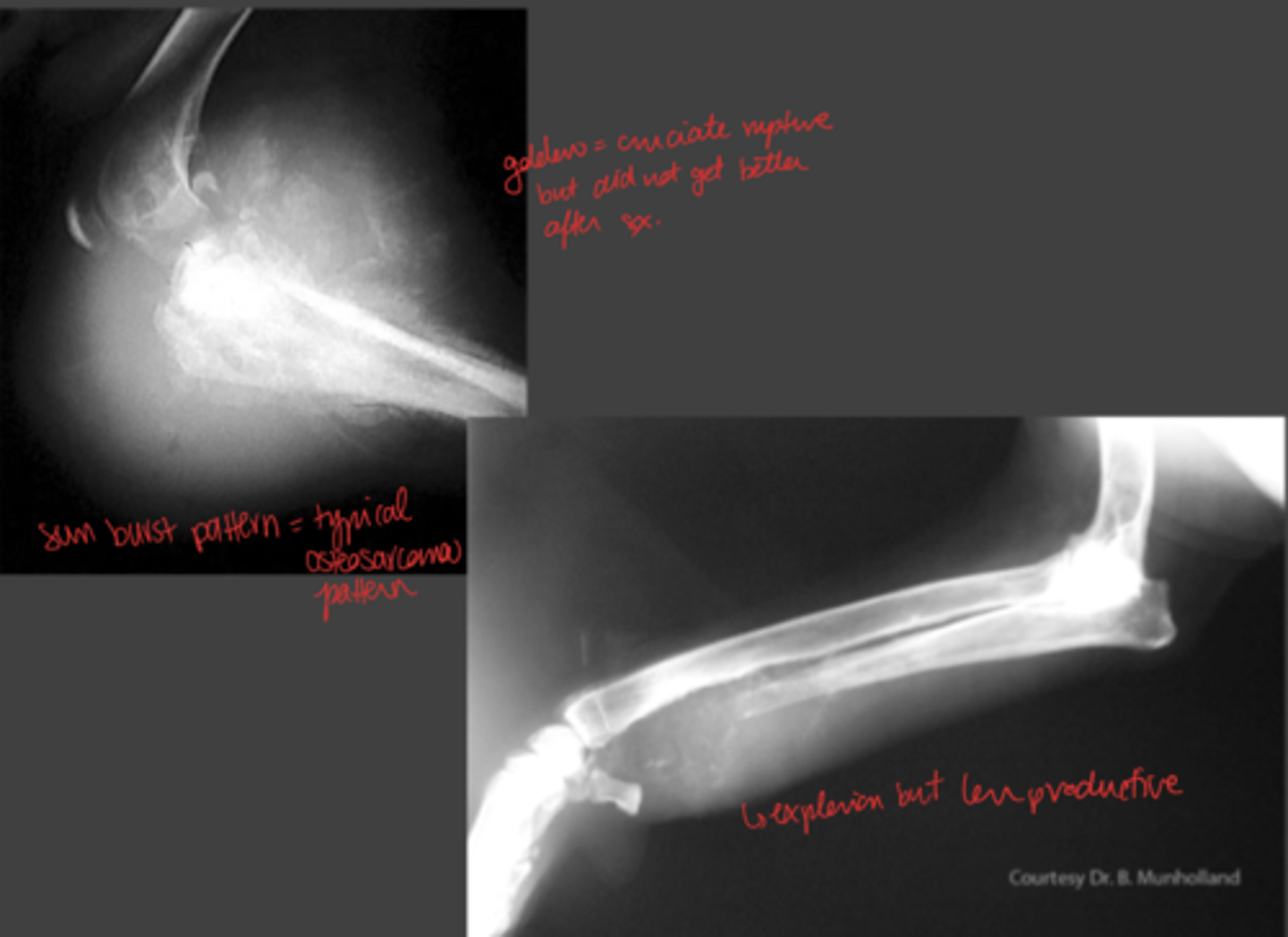
What is the early radiographic finding for osteosarcoma?
irregular trabecular pattern or lysis
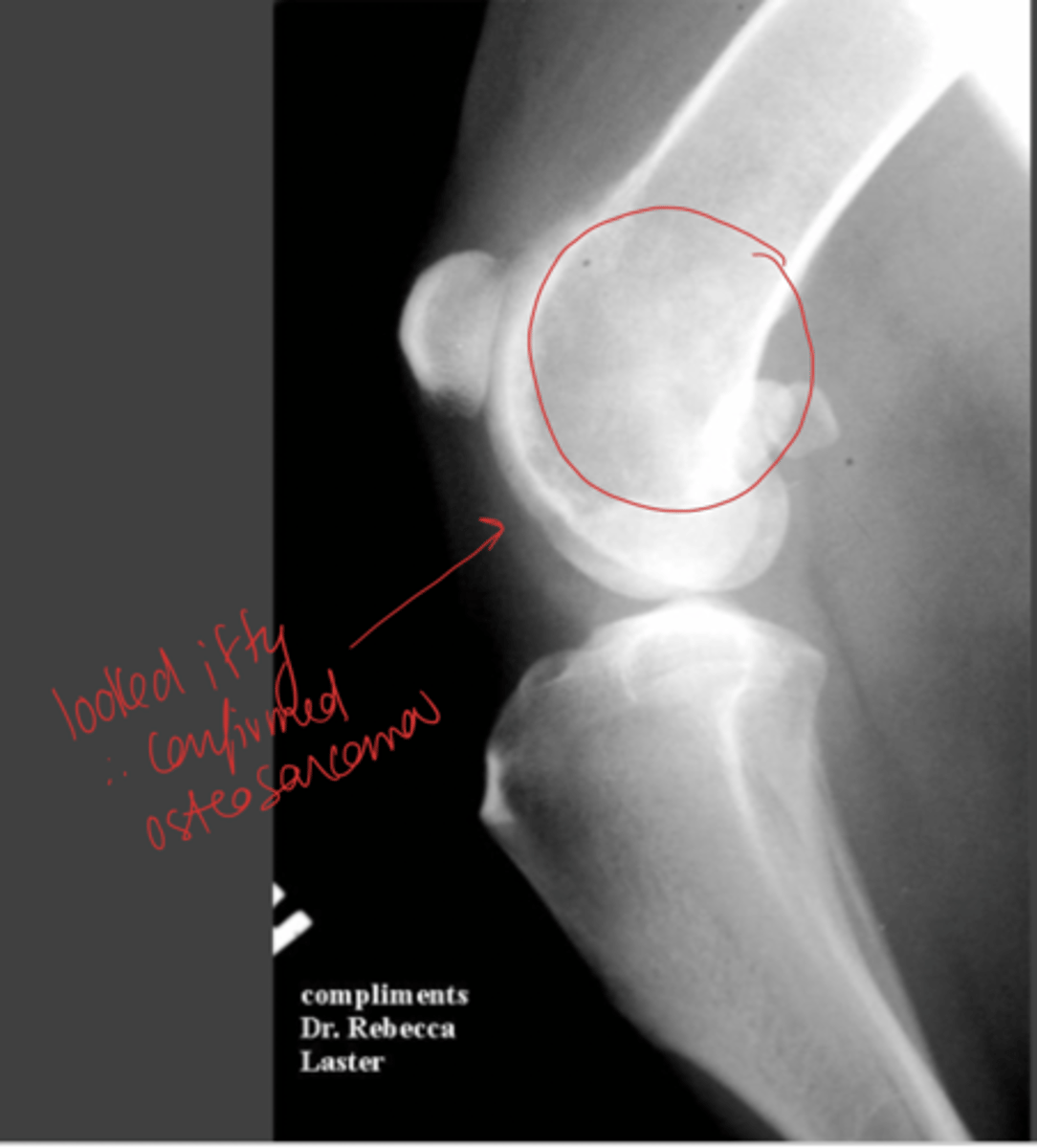
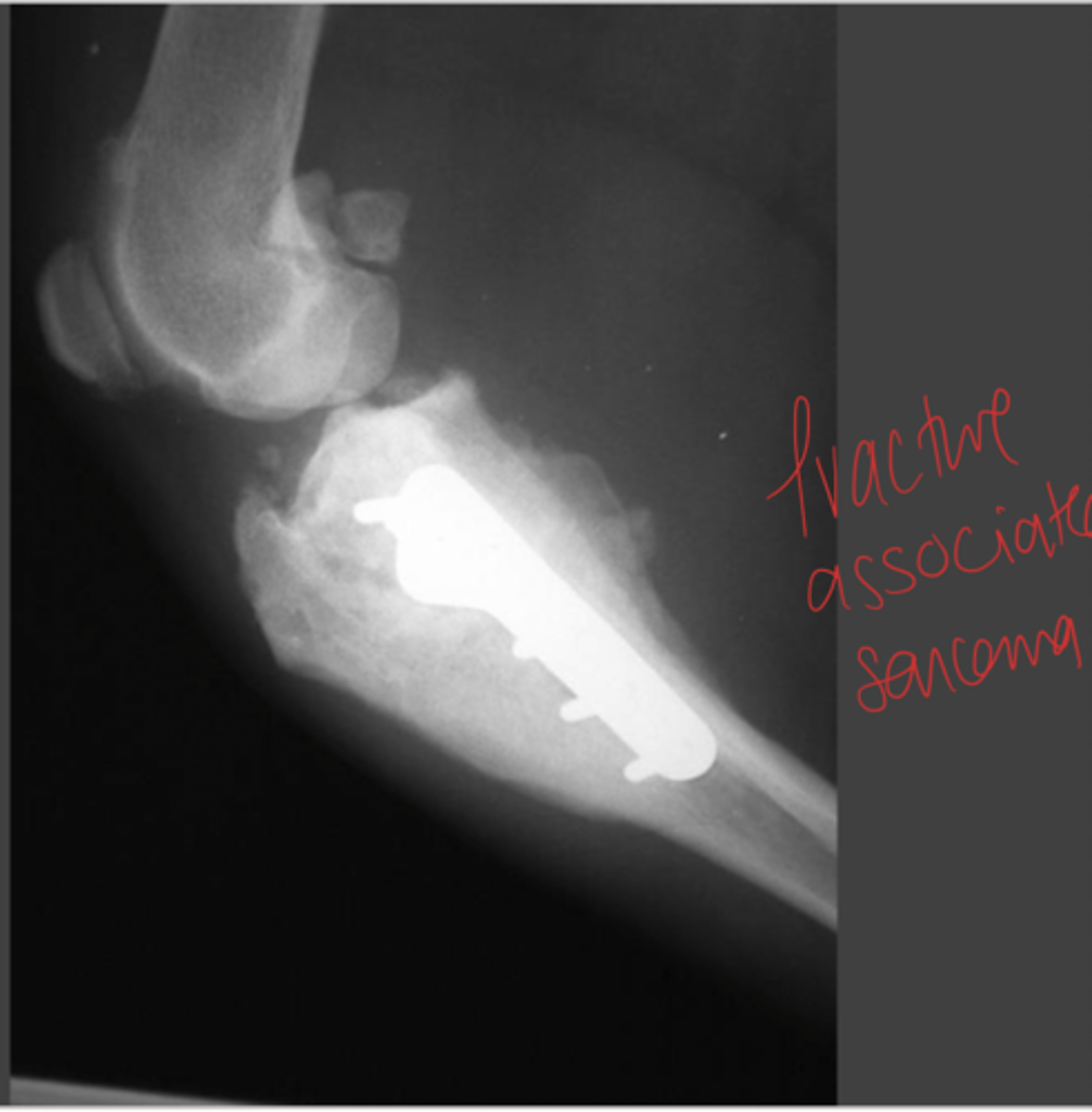
Where do fracture-associated sarcomas form? Why?
site of previous fracture
complication (inf or delayed union) or metal corrosion
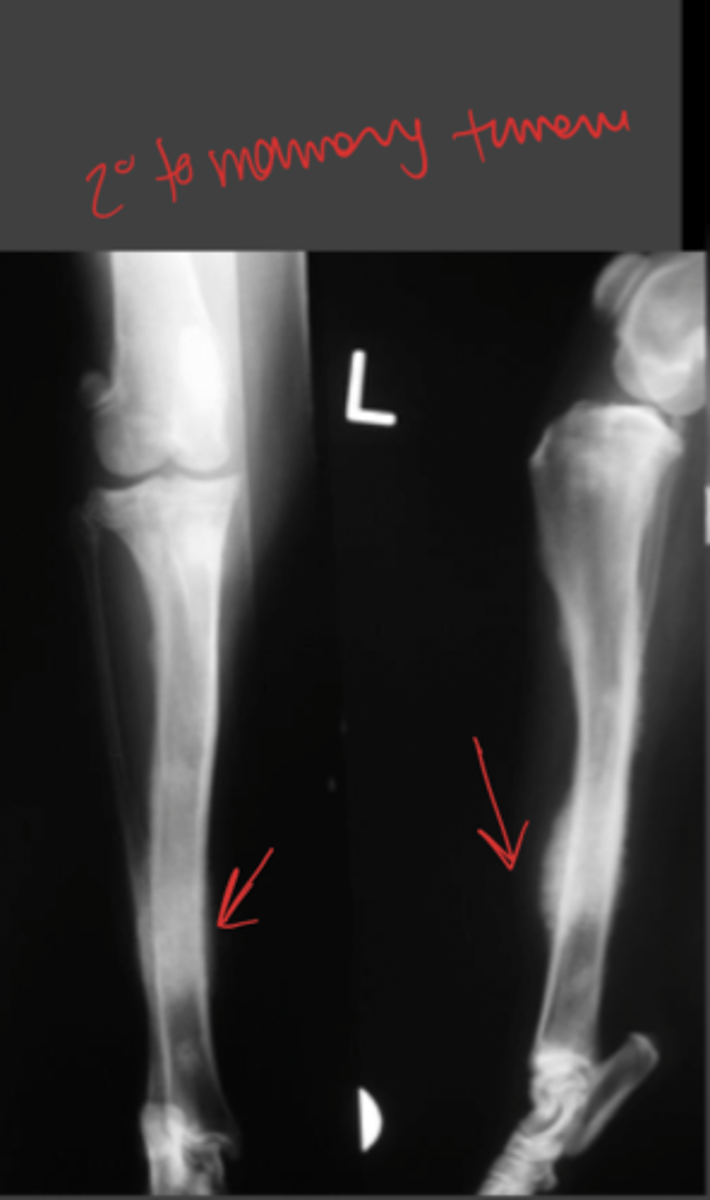
What are the most common tissue types that cause secondary tumours in bones? (7)
prostatic
mammary
transitional cell carcinoma
sarcoma
multiple myeloma
lymphoma
Where are common bone lesions found in bones with secondary tumours?
can be anywhere
most common = diaphysis
How are bone neoplasias diagnosed?
x ray (include chest if primary)
definitive: cytology or bone biopsy + histo
What is the biological behaviour of osteosarcoma (OSA)?
OSA has already metastasized (LUNGS) by the time it gets diagnosed
What are the risk factors for developing OSA? (3)
genetics: abnormal p53 gene
previous fracture/infection
spayed or neutered during first year of life
What is the prognosis in dogs with OSA?
no tx or remove primary tumour: 5m
chemo: 10-11m
How is cat OSA different from dog OSA?
cat = slower to metastasize therefore good candidate for amputation when diagnosed (curative)
How is OSA treated?
amputation
limb-sparing procedure
chemo (cisplatin or doxorubicin)
immunotherapy
How is OSA treated PALLIATIVELY?
remove primary tumour
palliative radiation
pain management
biphosphonate therapy
Describe the characteristics of each grade of Chondrosarcomas. (1 +3)
1. least aggressive + cured by removing primary tumour
3. like OSA except less chemoresponsive
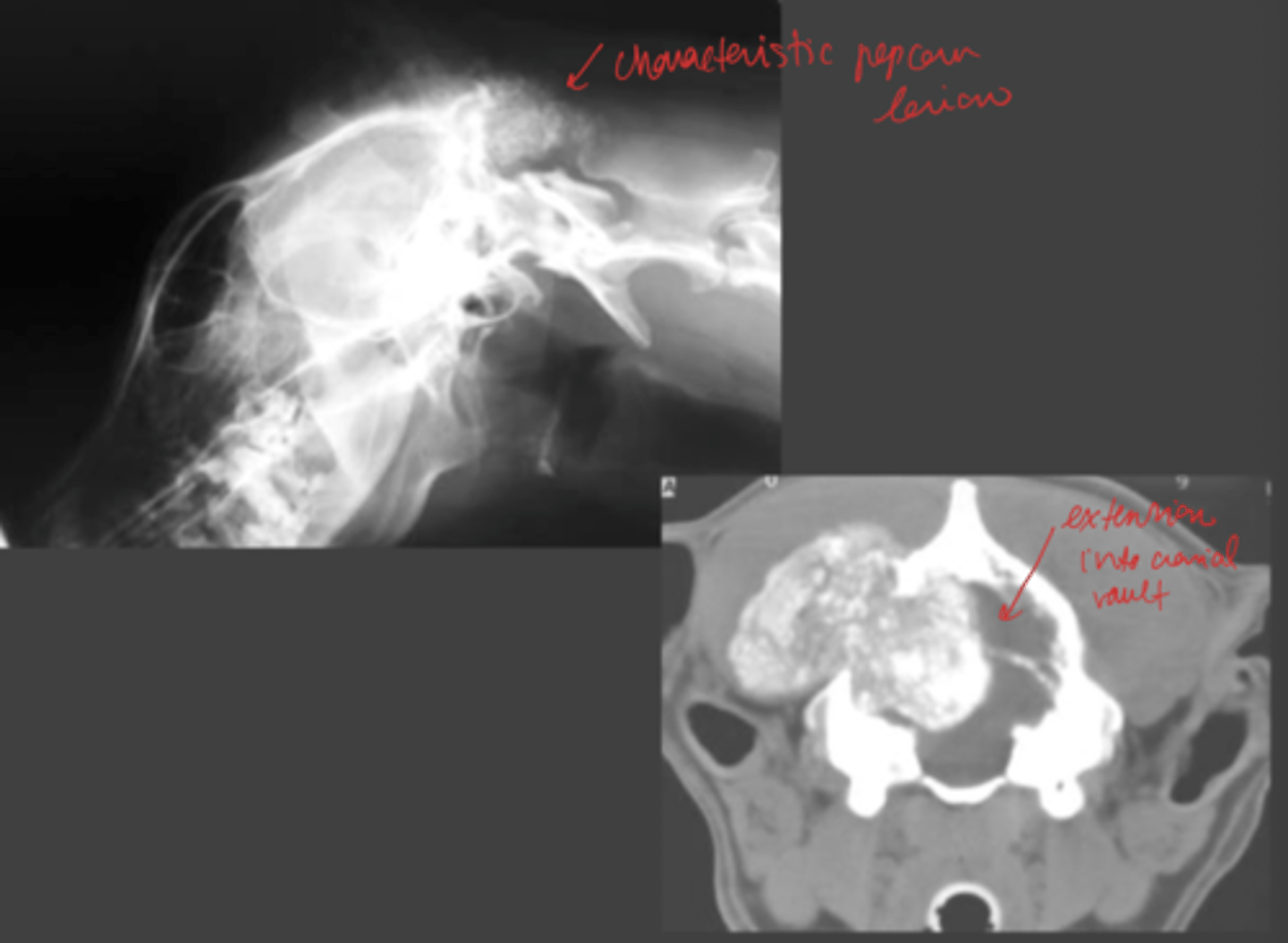
What are the characteristics for Multilobular Osteochondrosarcoma?
axial skeleton (skull)
osteoproductive
50% chance LT survival with removal + chemo
What is the biological behaviour and prognosis for secondary bone tumours?
death + painful + specific to primary cell tumor type
How are secondary bone tumours treated? What about in bone?
address primary tumour + metastases
palliative ration, drugs, sx removal for bone
What are the characteristics of synovial sarcoma?
primary or secondary tumor
CROSSES JOINTS
3 grades (3 is worst)
How are synovial sarcomas treated?
amputation
What are the indications for amputation? (9)
1. severe nerve damage
2. severe blood supply damage
3. severe muscle or bone loss
4. necrotizing fasciitis
5. neoplasia
6. chronic, debilitating muscle contractures
7. atrophic non-unions
8. sever osteoarthritis in a limb
9. chronic osteomyelitis + nonresponsive to tx
What are NOT indications for amputation? (7)
1. puppy + kitten fracture
2. fractures you can fix
3. fractures of tibia, ulna, radius, metacarpals, metatarsals
4. degloving injuries
5. hip/shoulder injury
6. cruciate ligament ruptures
7. acute nerve injuries
Where is a forelimb amputation done?
forequarter disarticulation with the scapula
Where are hindlimb amputations done? (3)
1. hemopelvectomy (remove part of pelvis)
2. hindquarter disarticulation at the hip
3. proximal third femur amputation
How is an amputation performed for prosthetic use?
1. done through a joint
2. leave lots of soft tissue to be comfy
3. best = at or below carpus/tarsus
What are the components of an osseointegrated prosthese?
part of prosthesis is implated into bone + external foot
What are types of distal amputations with pad transfer? What is it's purpose?
types: carpal pad transposition + free footpad transfer
purpose: make limb functional when amputated at or distal to carpo(tarso)metacarpal(tarso) junction
What are the characteristics of digital amputations?
any/all digits can be removed
all 3 phalanges can be removed
How is osteochoncrosis defined?
disruption of endochondral ossification (cartilage to bone) when articular cartilage/epiphysis are developing
What causes osteochoncrosis?
microtrauma to vessels --> affects blood supply --> necrosis of subchondral bone
What are the histo characteristics of osteochoncrosis?
cartilage = tick + abnormal, defect in subchondral done
How are microtrauma to vessels occur in osteochondrosis? What are possible consequences?
everyday minor trauma --> microfissures
fissures spread to surface --> make flap
consequence: osteochondritis dissecans (OCD)
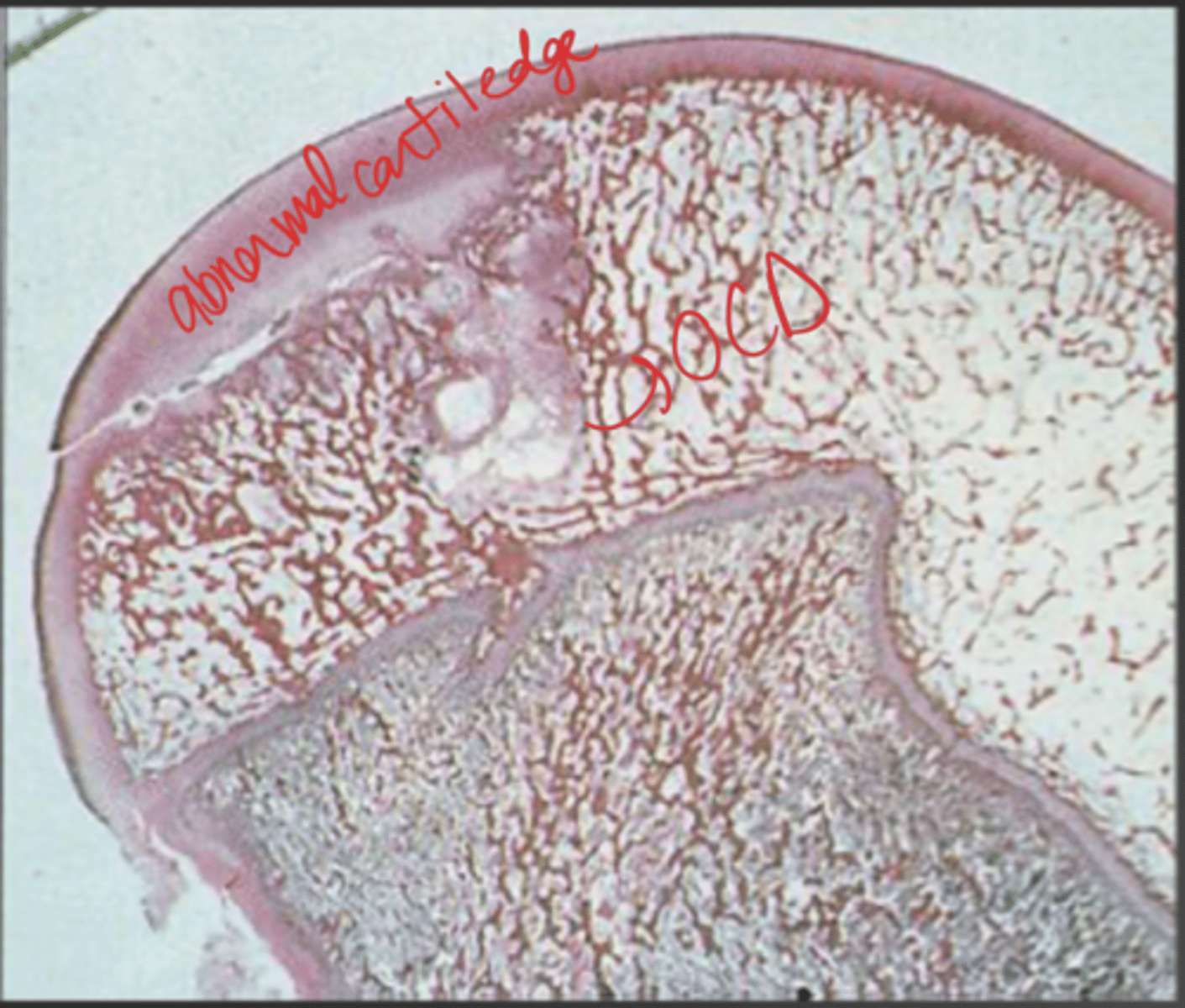
What are possible etiologies for osteochondrosis/OCD?
genetic
nutritional
traumatic
ischemis
What are characteristics of OCD?
large/giant breed dogs
onset at 4-12m
c/s: lameness and joint swelling
What are the most common sites for OCD?
caudal humeral head, medial humeral condyle, medial trochlear ridge of talus, lateral femoral condyle, distal ulnar metaphysis
How is OCD diagnosed?
PE (joint swelling), xray (lucent area in subchondral bone), CT = best
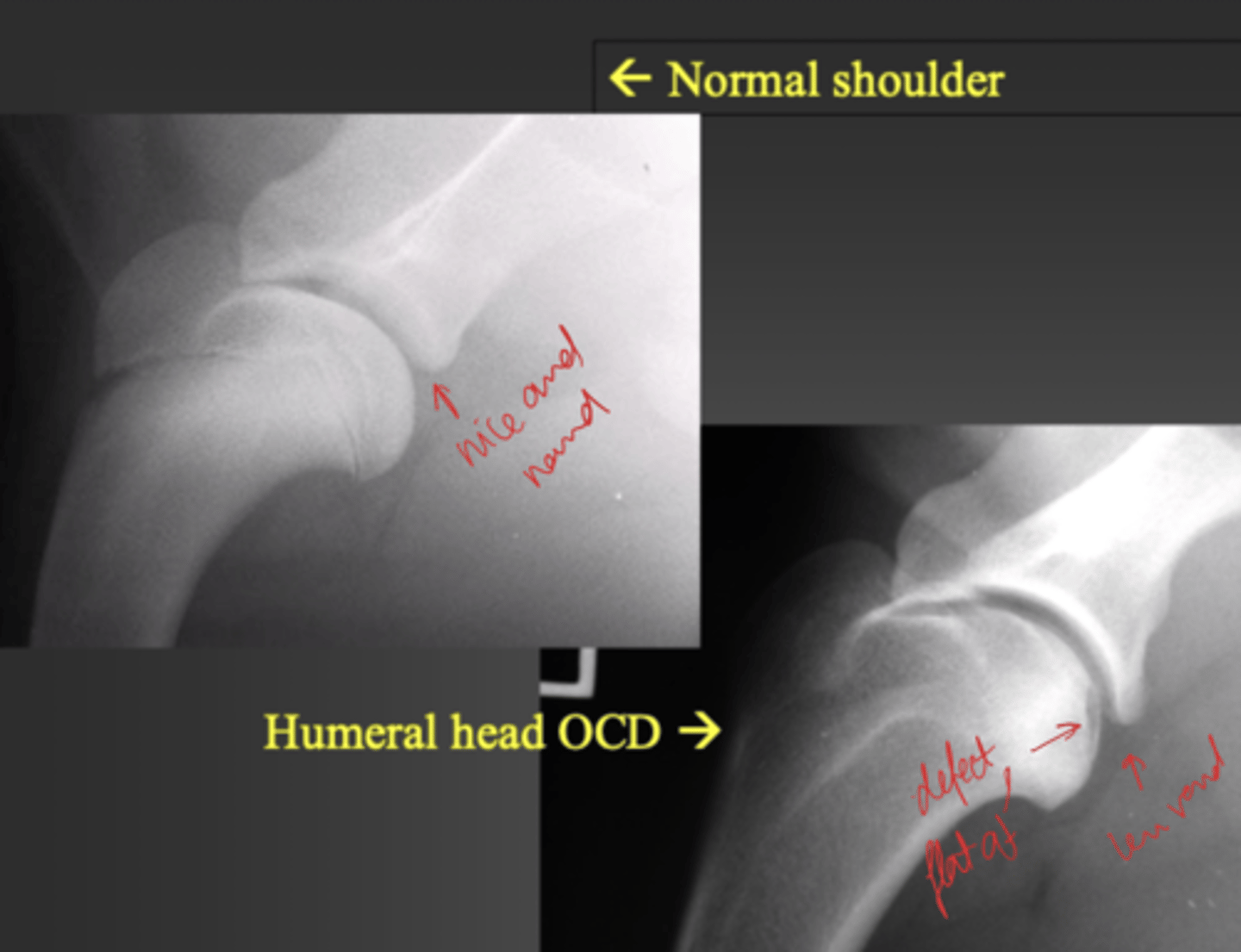
True or False: OCD is frequently bilateral.
TRUE
How is OCD treated? (7)
1. medical therapy (exercise, NSAIDs, chondroprotective agents)
2. arthrotomy/arthroscopy: remove flap + debride
3. osteochondral transplantation
4. implant resurfacing
5. chondrocyte implant
6. stem cells
7. arthrodesis (chronically affected/arthritic joints)
What is the definition of osteoarthritis (OA) or degenerative joint disease (DJD)?
slow degeneration of articular cartilage
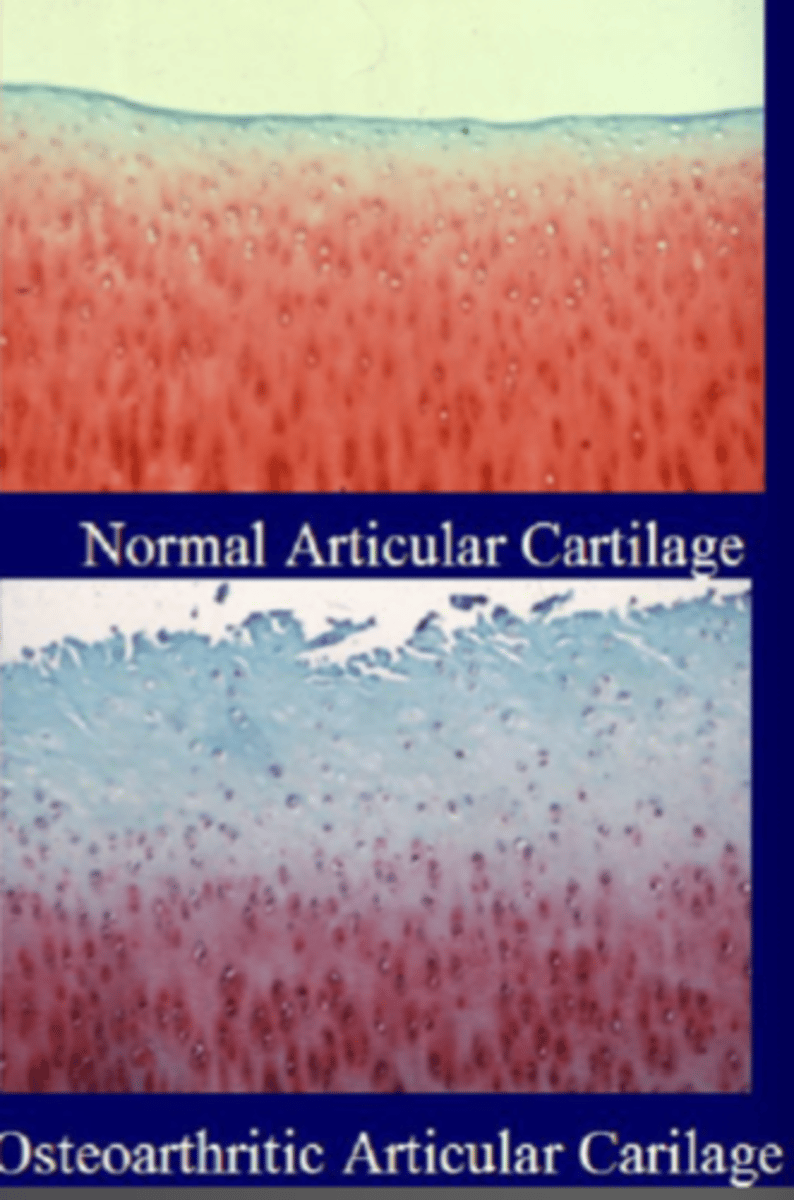
How does OA/DJD occur?
articular cartiledge loses its normal matrix --> fibrillated chondrocytes --> fissured --> subchondral bone exposed
How does OA/DJD look radiographically?
thickened joint capsule
osteophytes at joint capsule attachment
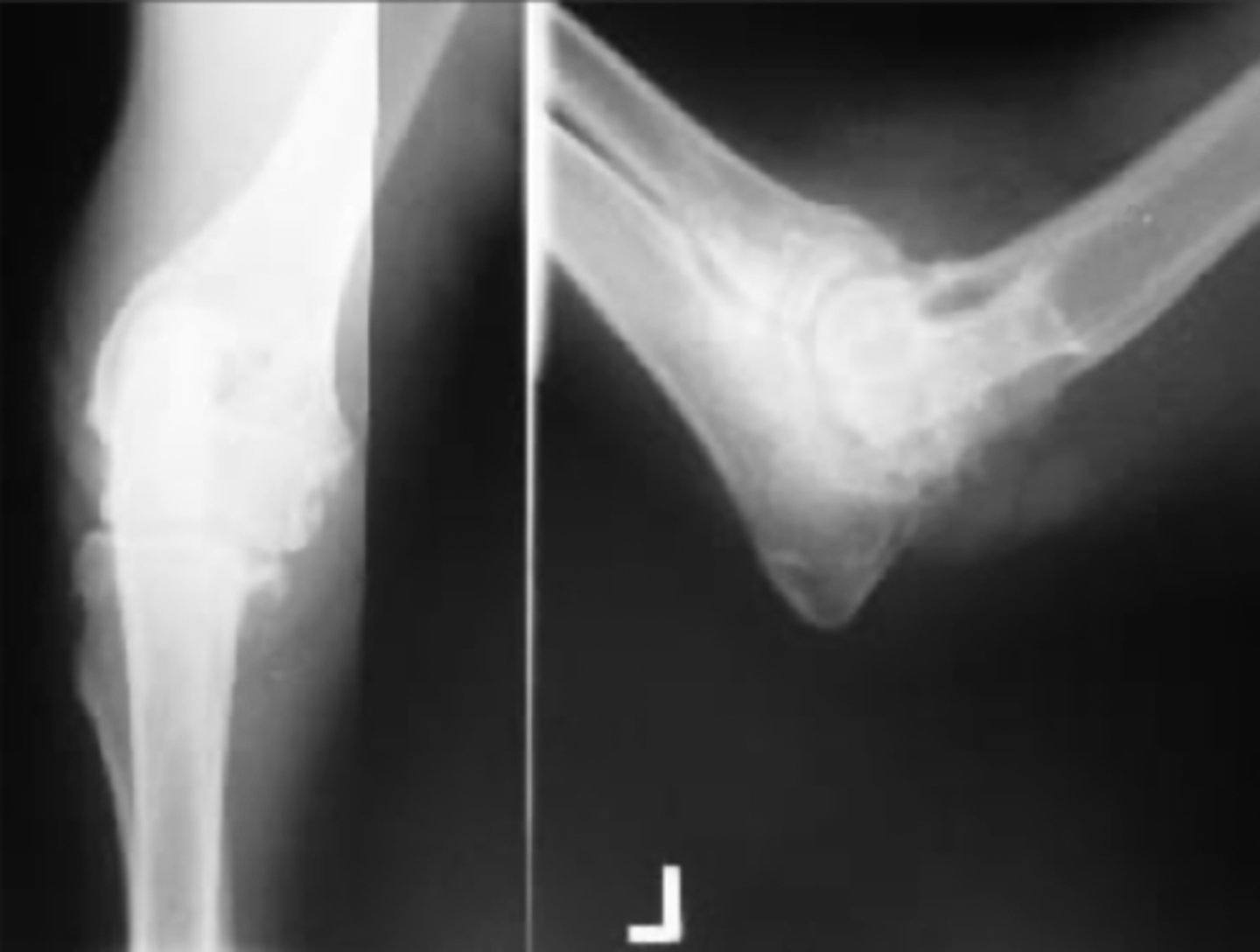
What causes OA? (4)
1. articular fractures
2. joint incongruity
3. joint instability
septic and immune-mediated arthritis
4. toxic insults
How is OA treated in dogs?
result of another joint problem --> treat underlying cause
What are clinical signs of OA in a DOG? (4)
1. sometimes none
2. decreased joint range of motion
3. stiffness in morning
4. lameness after exercise
What are clinical signs of OA in a CAT? (5)
1. weight loss, A-
2. U+/feces outside litterbox
3. attitude change
4. poor grooming
5. reluctance to jump
What are strategies for treating OA? (7)
1. weight loss (decrease load on joint)
2. corrective osteotomy (shift load to normal part of joint)
3. molecular/gene therapy
4. modify cartilage metabolism (DMOAs) --> omega-3
5. decrease pain/inflammation --> NSAIDs, nerve growth factor inhibitors, corticosteroids, stem cells, platlet-rich plasma
6. rehab
7. remove (excision arthroplasty), replace, fuse joint (arthrodesis)
What are differences between pediatric vs adult patient? (4)
1. growth plates
2. thickker cartilage + periosteum
3. higher collagen compared to mineral
4. ligaments stronger than bone