anatomy of urinary system
1/35
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
36 Terms
urinary system functions
Filtration of blood plasma to remove waste and produce urine
Filtration of blood plasma to detoxify (clear hormones and drugs)
Regulation of blood pressure and blood volume
Regulation of ion levels (Na+, K+, Ca++, PO4-)
Regulation of pH (H+ and bicarbonate)
organs of the urinary system
2 kidneys (main workers)
2 ureters
bladder
urethra
kidneys
retroperitoneal organs that are located posterior to abdominal cavity (behind peritoneum)
right kidney slightly lower than left due to liver
layers of connective tissue of kidneys (superficial to deep)
renal fascia
perirenal fat capsule (perinephric fat)
fibrous capsule
pararenal fat capsule
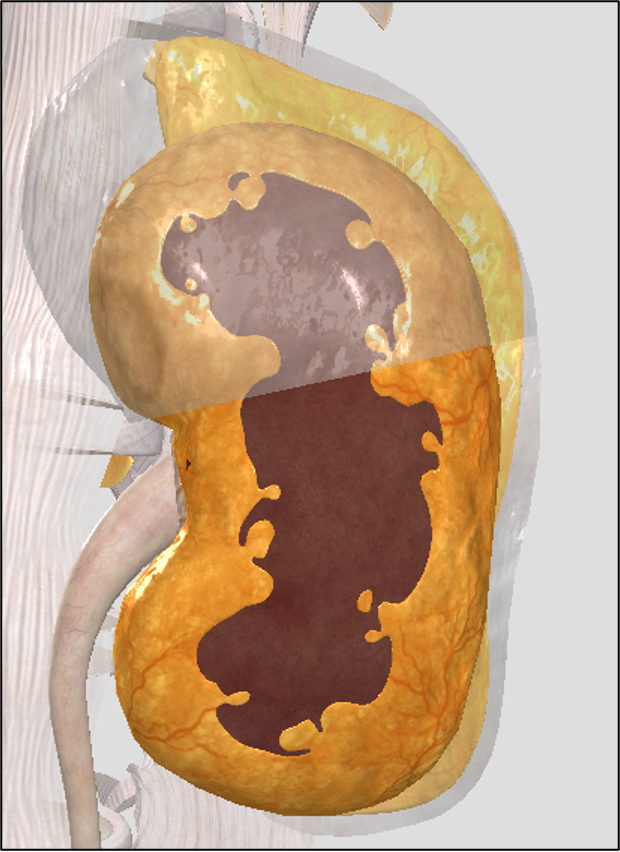
renal fascia
Dense irregular fibrous connective tissue
Attaches kidney to abdominal wall
Deep to the peritoneum
Surrounded by fat on two sides…
clear covering
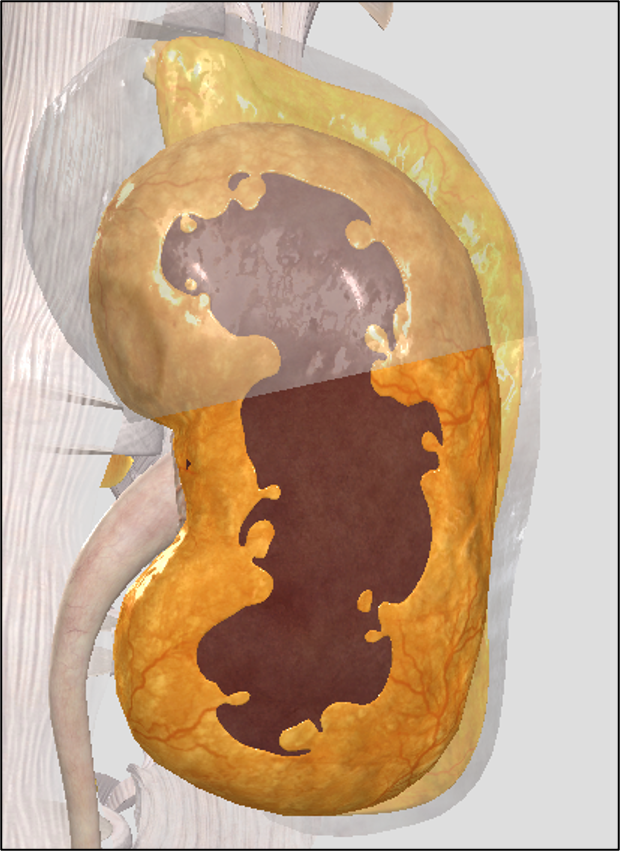
perirenal fat capsule (perinephric fat)
A brown adipose tissue cushion that holds kidney in place
yellow covering
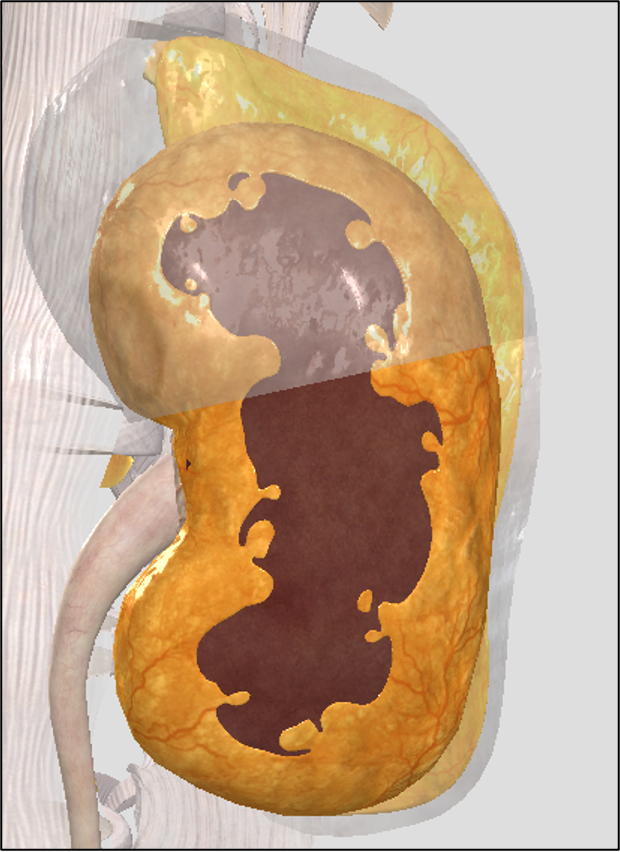
fibrous capsule
Dense irregular CT
Collagen and elastic fibers that wrap and protect the kidney
Collagen fibers extend to the renal fascia to anchor kidneys in place
inside brown layer
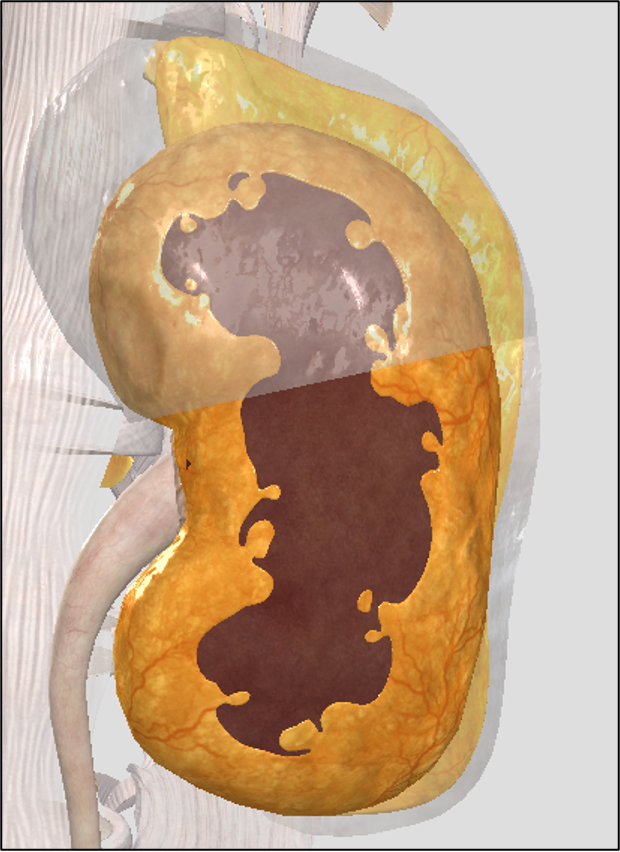
pararenal fat capsule (body)
A white adipose tissue on the posterior side of the kidney
region of kidneys
renal cortex
renal medulla
renal pelvis
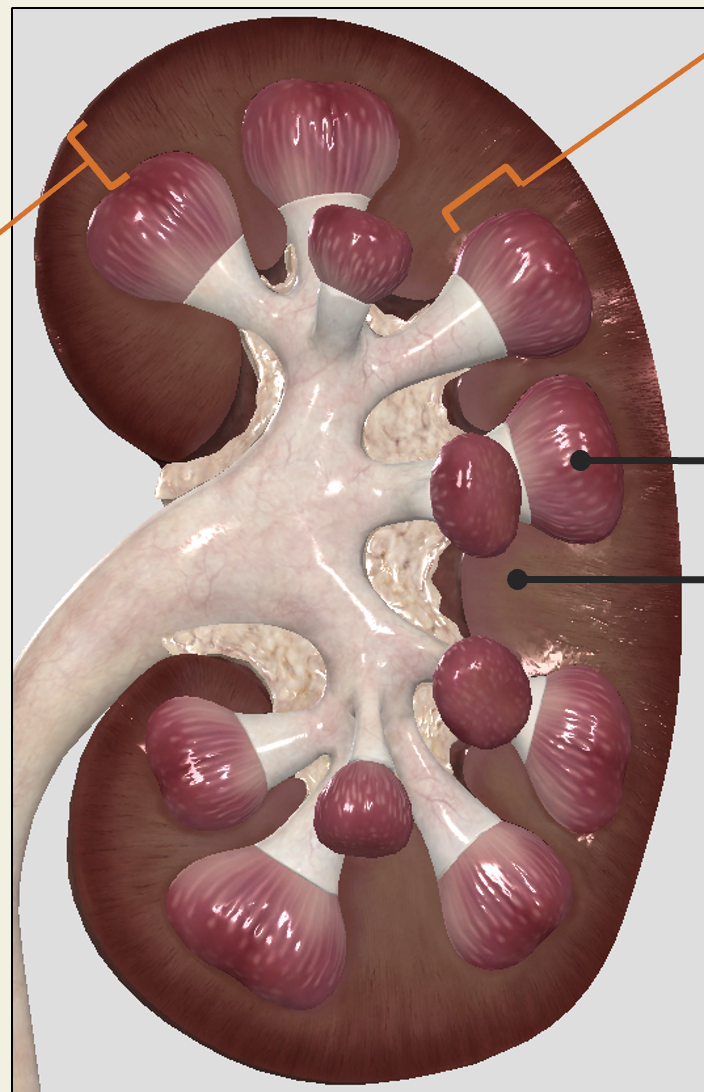
renal cortex
Outer layer of parenchyma (“functional tissue”)
Appears granular due renal corpuscles of nephrons
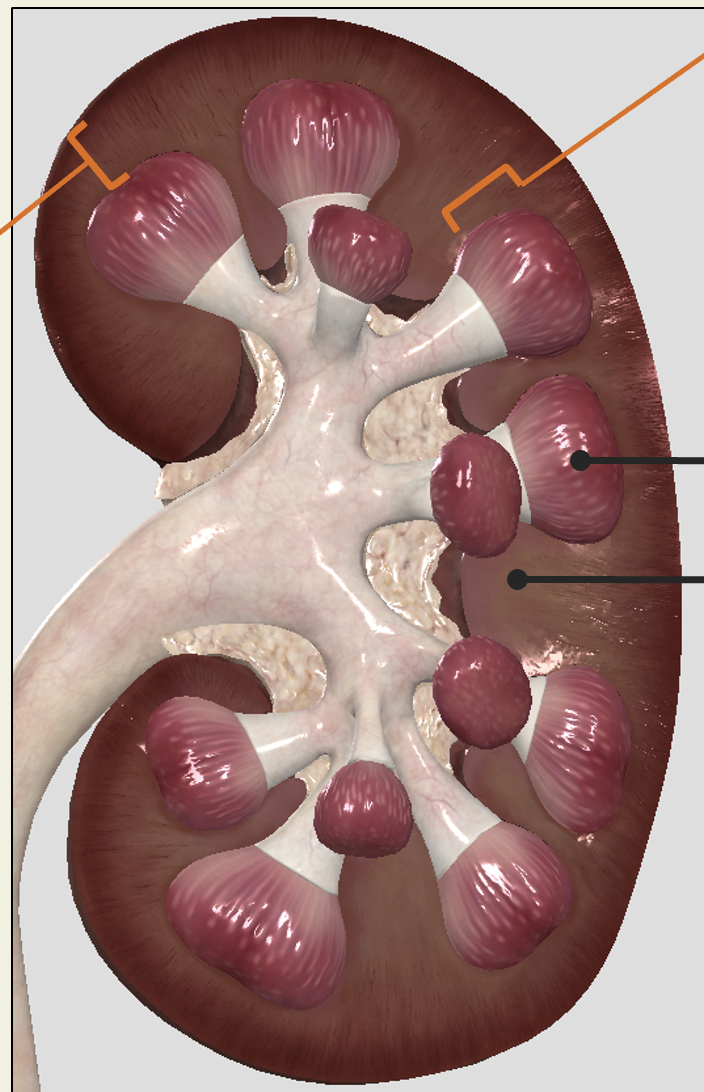
renal medulla
Inner layer of parenchyma facing sinus
Divided into renal pyramids by columns from cortex (renal columns are part of medulla)
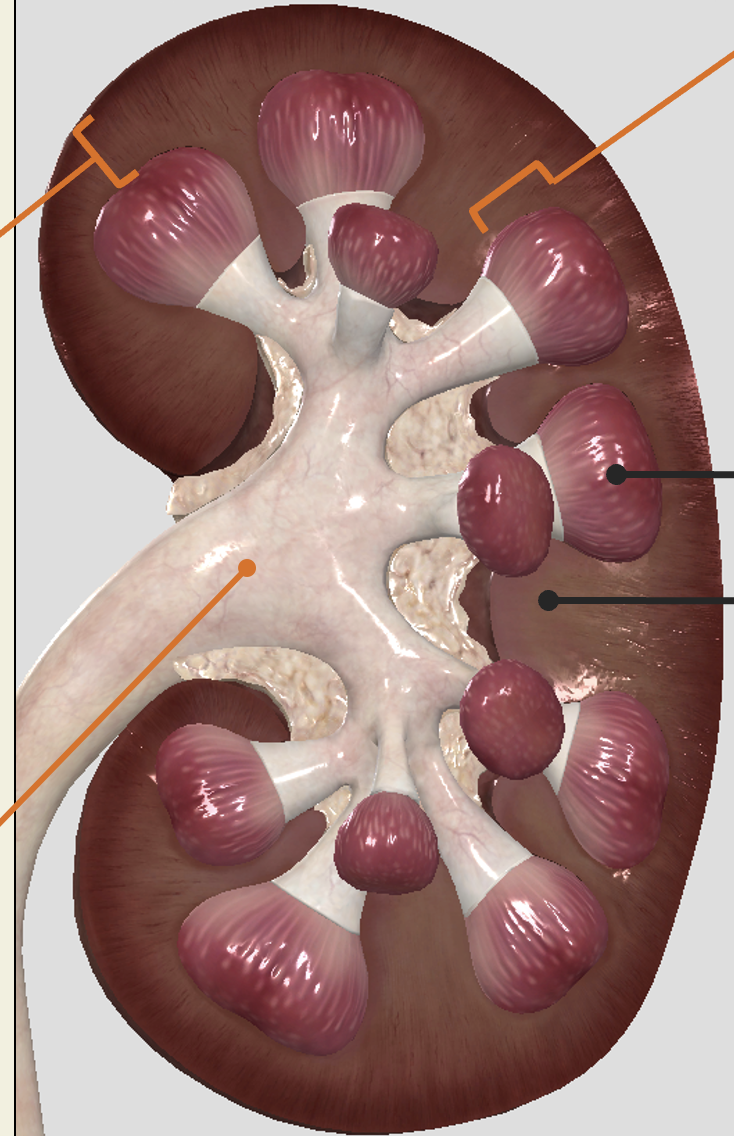
renal pelvis
Tube-like structure leaving kidney into ureter
Drains fluid from major calyces
Major calyces drain from minor calyces
Minor calyces receive fluid from renal papilla of medulla
Urine drained by peristaltic contraction of smooth muscle
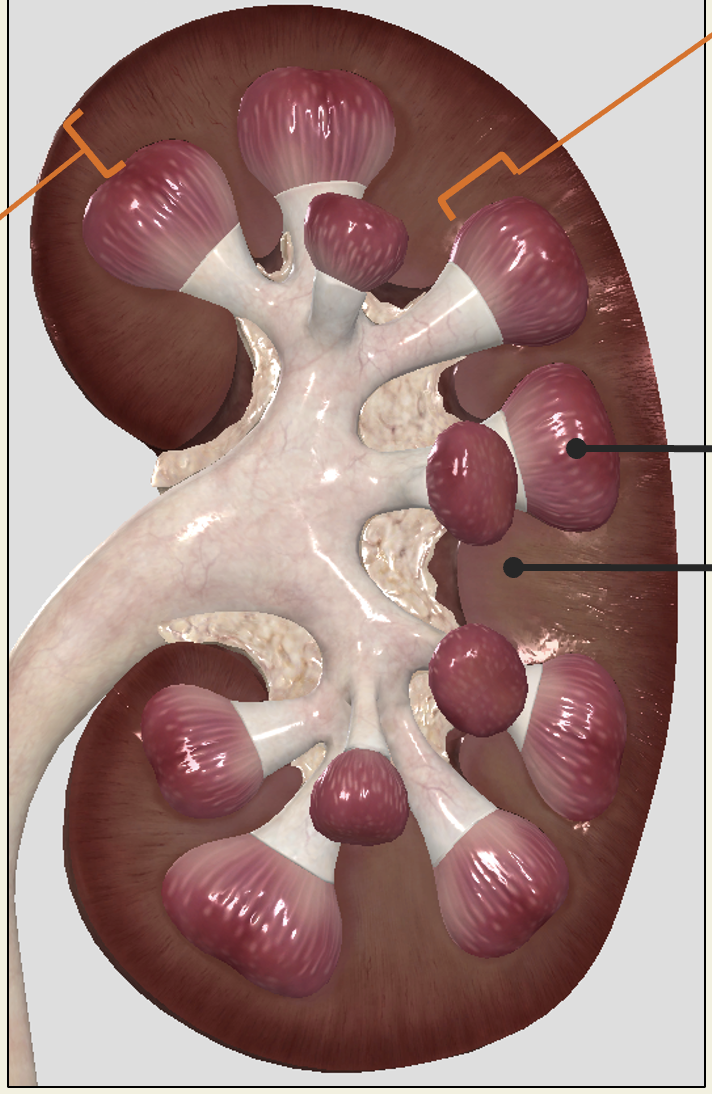
renal pyramid
in renal medulla
broad base, and a pointed end called the renal papilla (attached to calyx)
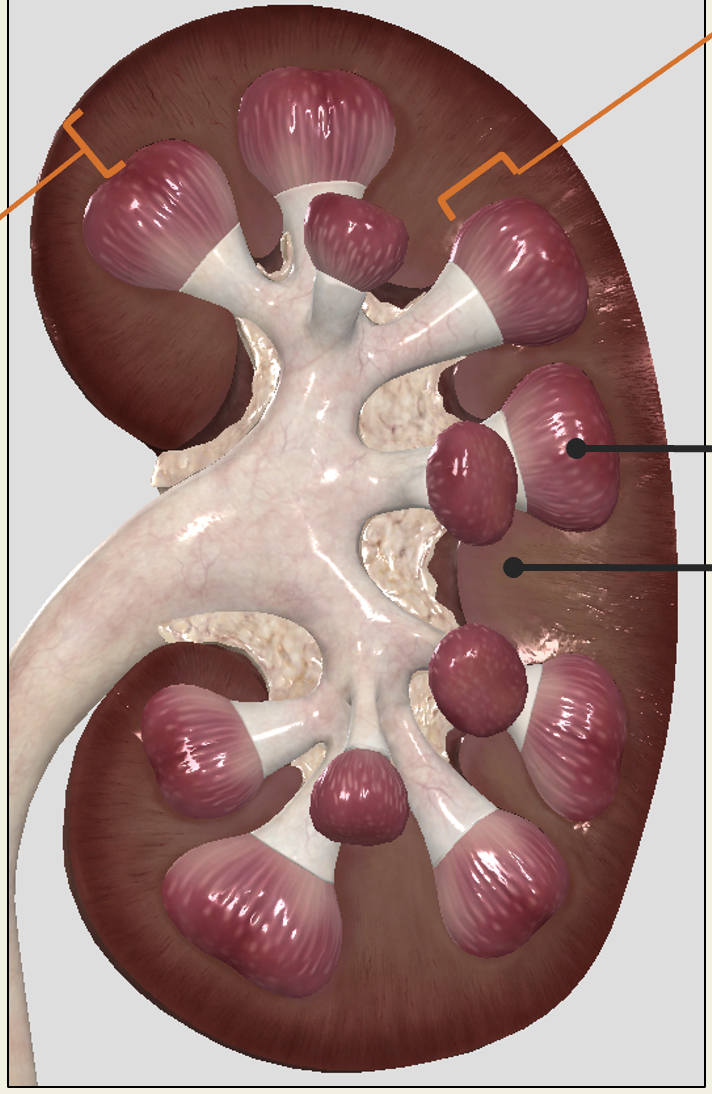
renal columns
in renal medulla
Stripped appearance comes from parallel arrangement of collecting tubules and capillaries
renal sinus
region that contains minor + major calyx and renal pelvis
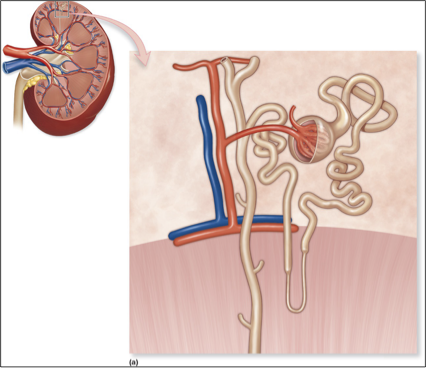
nephrons
functional unit of the kidney, the structure that actually produces urine in the process of removing waste and excess substances from the blood
cortical nephron
Close to surface; short loops; 85% of nephrons
juxtamedullary nephron
long loops extending into renal pyramids; primarily concerned with salt balance/levels
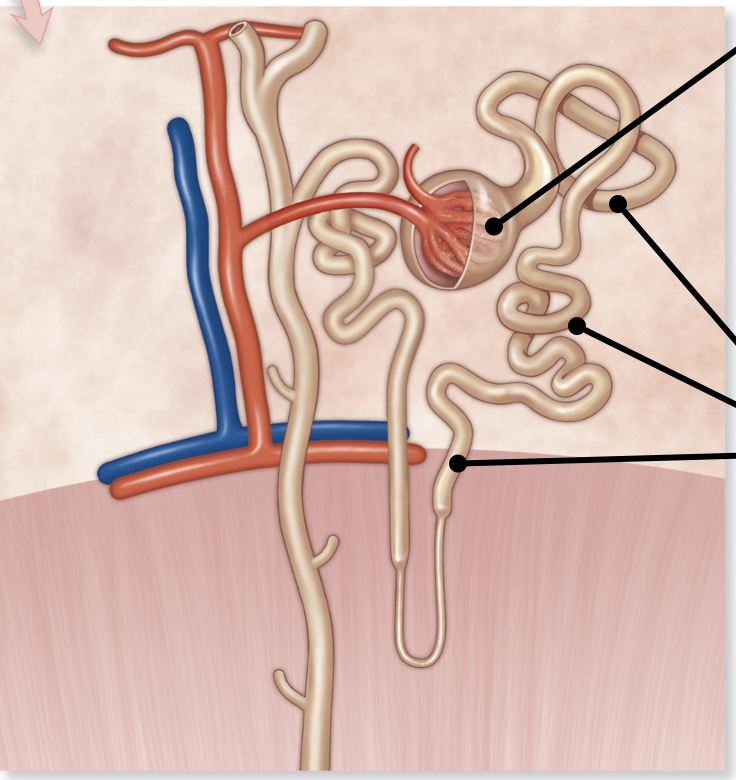
renal corpuscle
enlarged region where filtration occurs
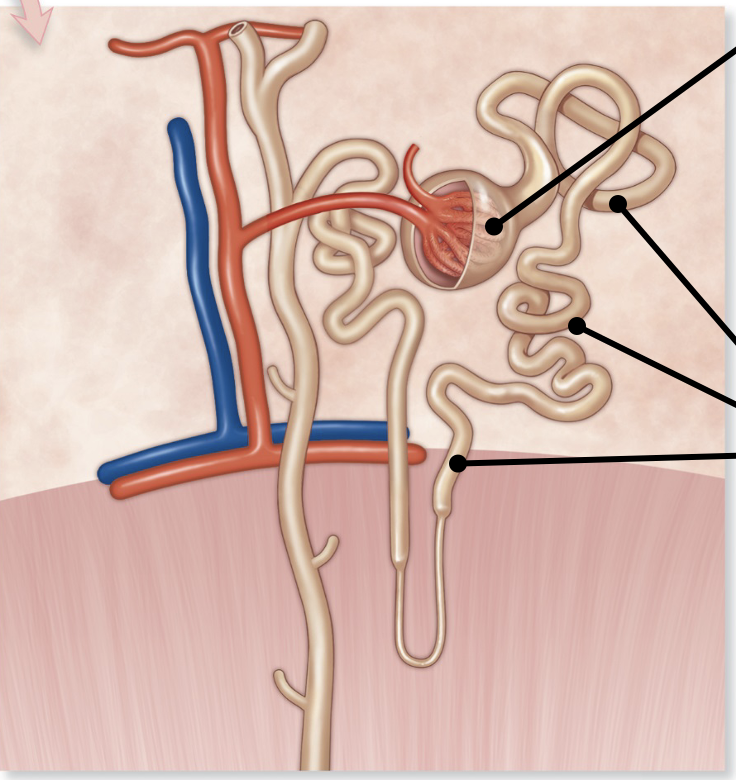
renal tubule
Tube like portion of nephron
PCT, nephron loop, DCT
Sites of secretion and absorption
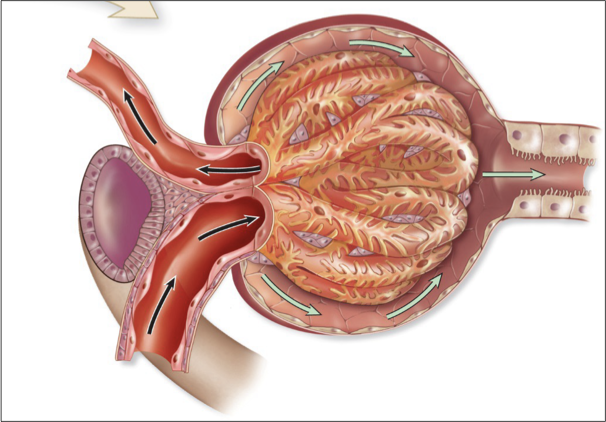
glomerular capillary bed
supplied by an afferent arteriole and drained by an efferent arteriole
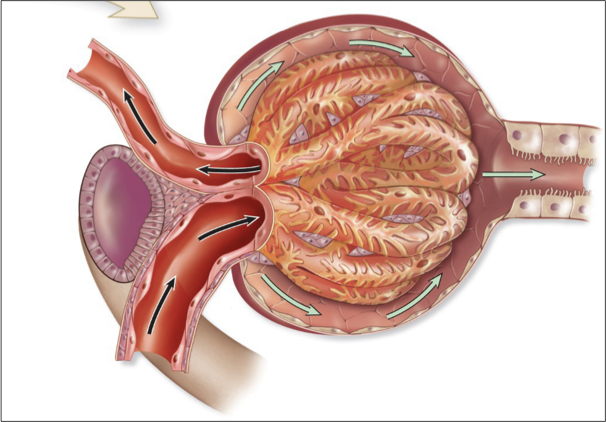
parietal layer
surrounds capsule
Simple squamous epithelium for structure, not diffusion!
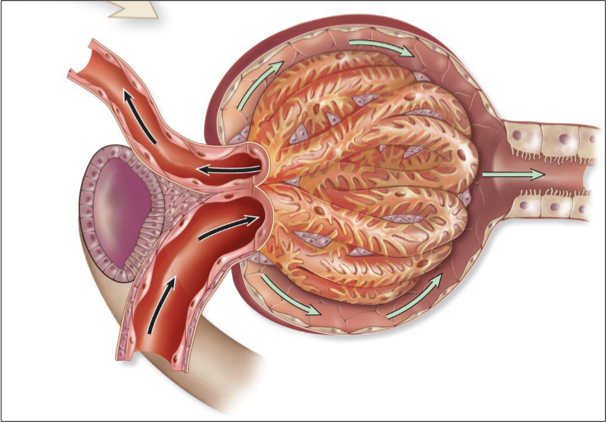
glomerulus
High pressure blood capillaries (central capillaries in corpuscle) where filtration occurs
A ‘dump’ of contents out of the capillary
only bed with two arteriole ends
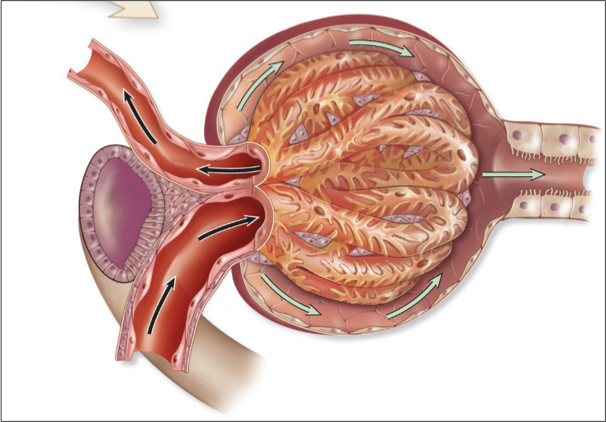
visceral layer
surrounds capillaries
Podocytes that wrap around capillaries and interdigitate
Form filtration slits for passage of solutes
renal tubule
reabsorbs and secretes various molecules
Na+ handling
K+ handling
Nutrient handling
Water handling
single layer of epithelial cells on basement membrane
nephron loop (loop of Henle)
distal convoluted tubule
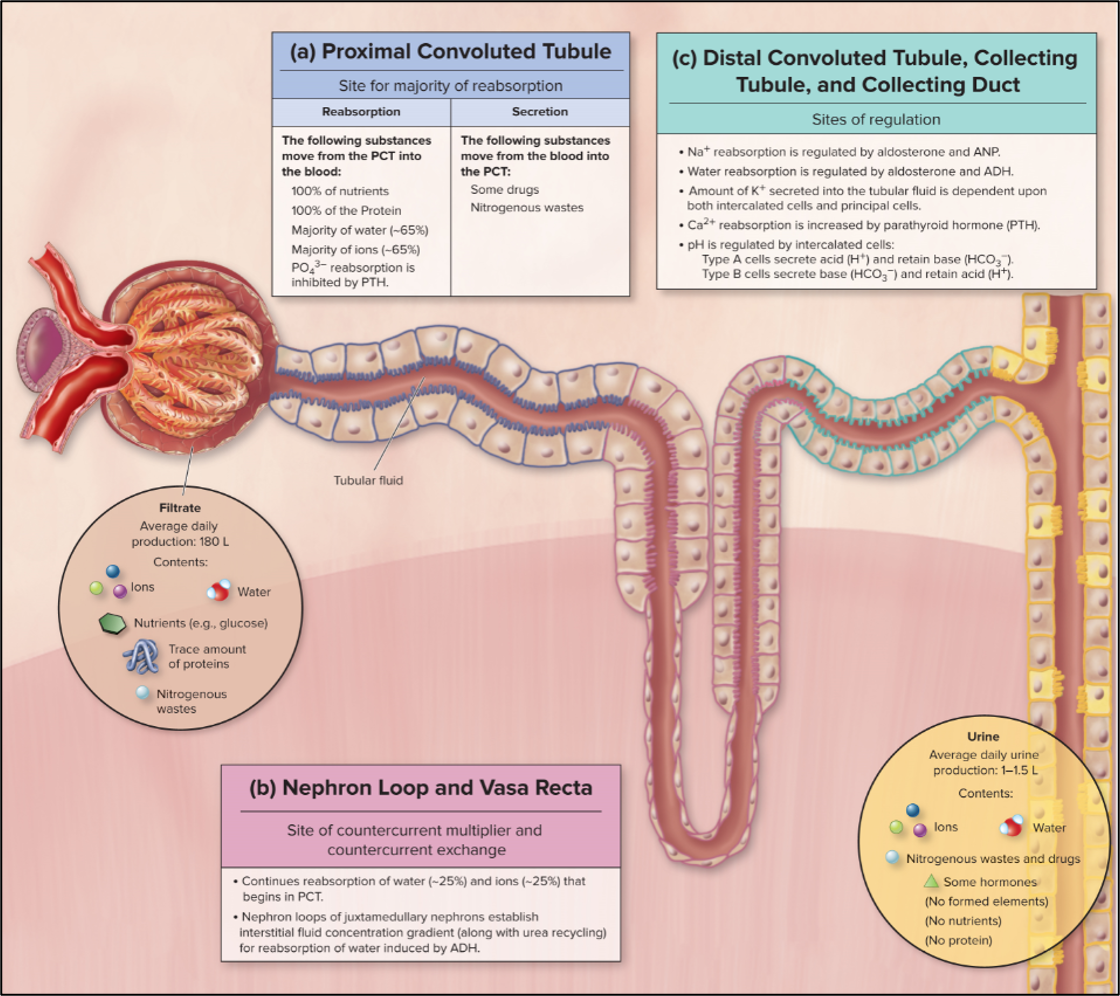
nephron loops
proximal straight tubule- thick descending portion of nephron loop
Thin descending portion of nephron loop
Thin ascending portion of nephron loop
Distal straight tubule- thick ascending portion of nephron loop
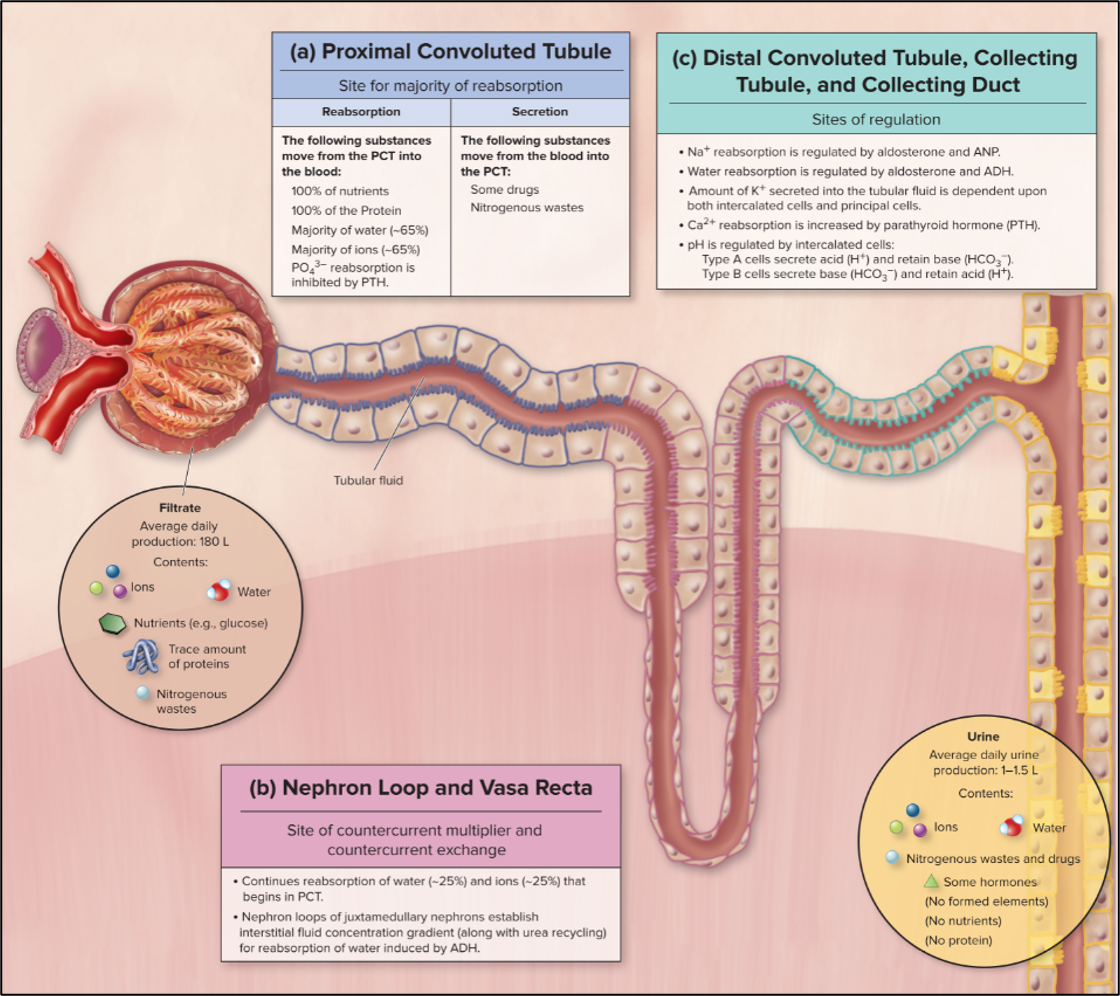
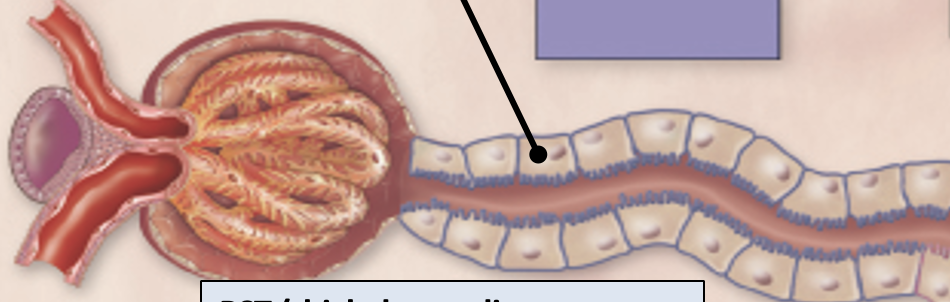
PCT (proximal convoluted tube)
simple cuboidal epithelium with LOTS of microvilli. Lots of mitochondria
primary resorptive function: Na+, glucose, amino acids, phosphates, and water
hormonal influence: angiotensin 2
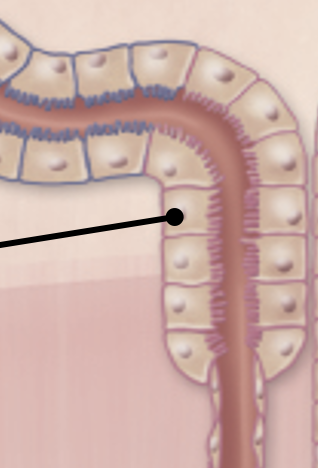
PST (thick descending segment)
similar to PCT except microvilli fewer and not packed as tightly
primary resorptive function: water reabsorption
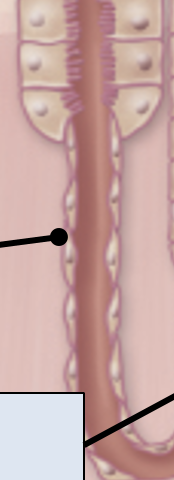
Thin descending segment
simple squamous epithelial cells (water reabsorption specialists)
primary resorptive function: Water reabsorption; some Na+ reabsorption
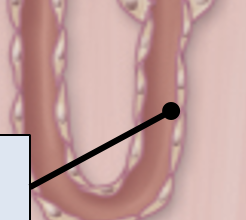
Thin ascending segment
simple squamous epithelial cells (ion reabsorption specialists)
primary resorptive function: Na+, K+reabsorption

DST (thick ascending limb)
simple cuboidal epithelium with few to no microvilli
primary resorptive function: Na+, K+ reabsorption
hormonal influence: ADH
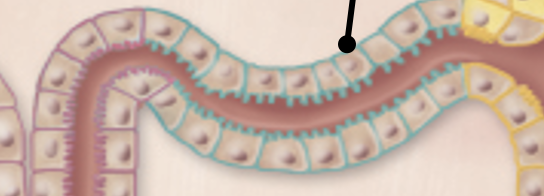
DCT (distal convoluted tube)
simple cuboidal epithelium with few to no microvilli
primary resorptive function: Na+ reabsorption, K+ secretion
hormonal influence: ADH, aldosterone
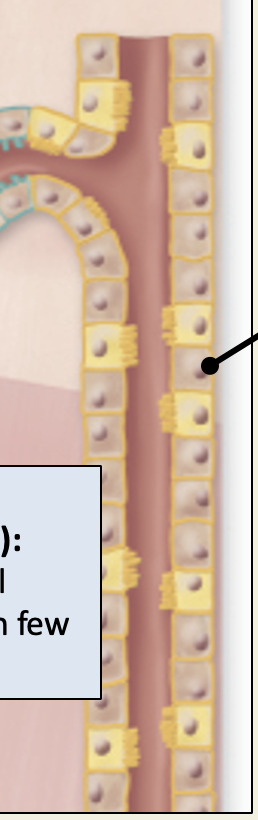
collecting duct
Simple cuboidal to columnar epithelium; distinct cell borders
primary resorptive function: Na+, K+, H+, water reabsorption, K+ secretion
hormonal influence: ADH, aldosterone
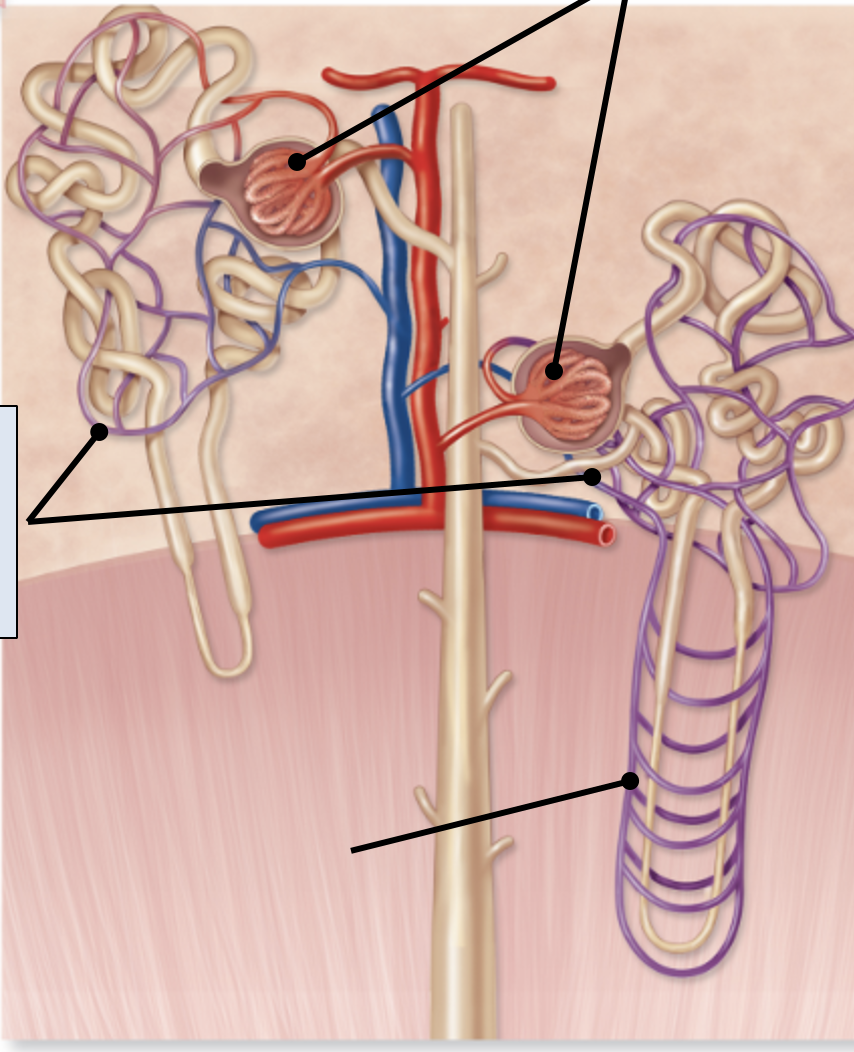
capillary beds in kidneys
peritubular capillaries
vasa recta
glomerulus
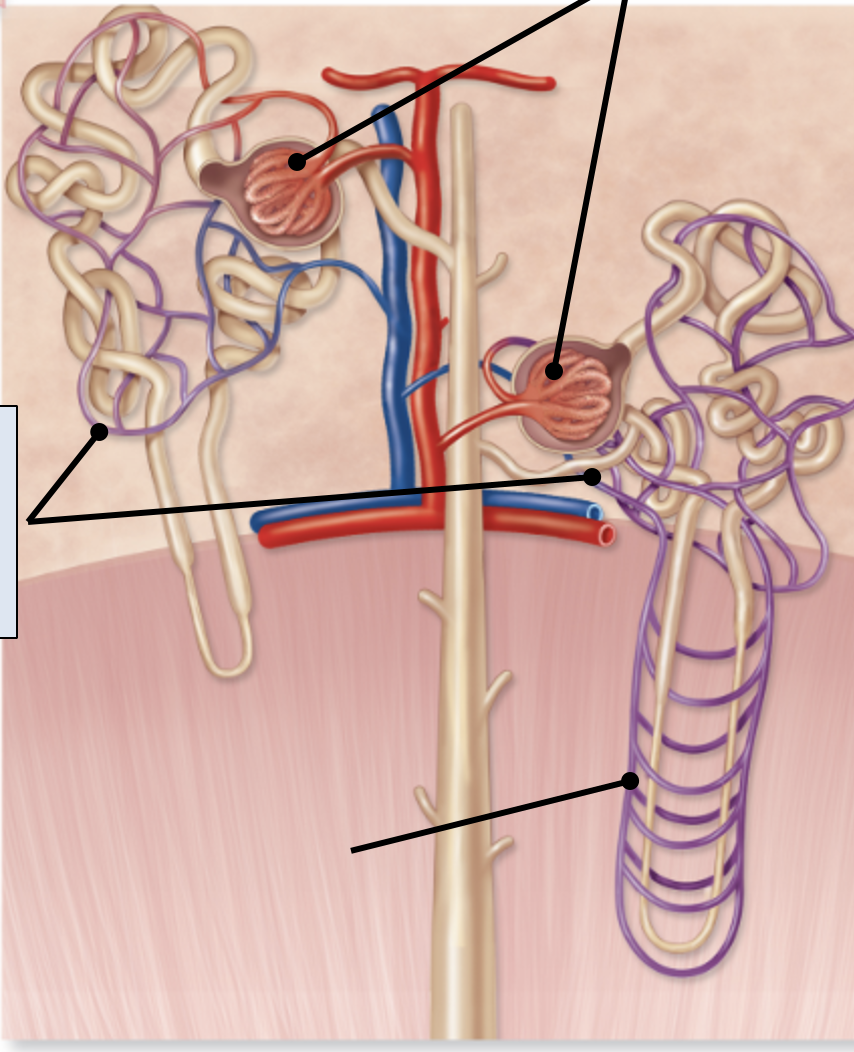
peritubular capillaries
Surround tubules and reabsorbs water and solutes from tubules
Transport these substances back to venous system
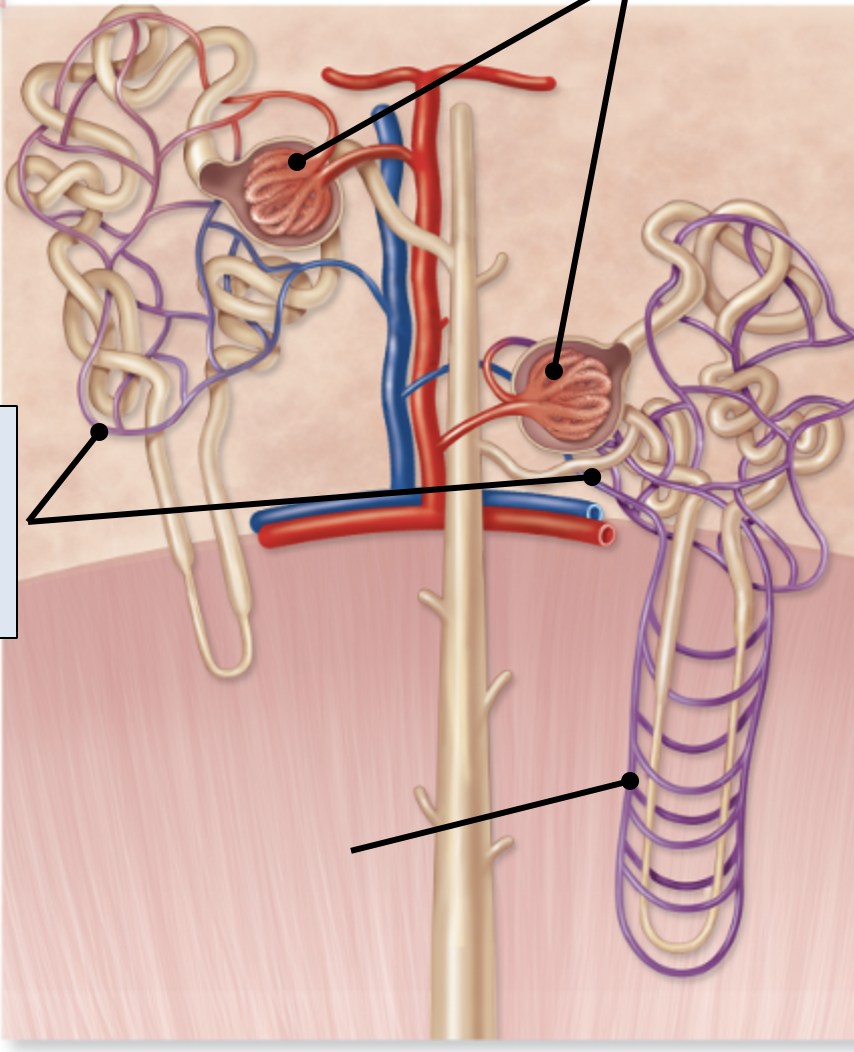
vasa recta
Specialized capillary bed of juxtamedullary nephrons
These are peritubular capillaries except these vessels are more “straight”
Supplies renal medulla with blood (1-2% of total blood)
Important in establishing and maintain salt concentration in medulla