Johnes disease
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
What is the causative agent of Johnes disease?
Mycobacterium avium subspecies Paratuberculosis
What type of bacteria is Mycobacterium paratuberculosis?
obligate intracellular pathogen
Slow growing, fastidious acid fast bacillus
member of Mycobacterium avium
once infected —> infected for life
How long can Mycobacterium paratuberculosis live in the environment?
12 months in water
2 years in soil (low pH increases survival
What are the different types of MAP?
Bovine or Type II (or C for Cattle) strains
Sheep or Type I (S) strains
How does Johnes disease present pathologically?
MAP in macrophages
Granulomata in distal ileum & LN
infect macrophages & Lymph
Cattle – diffuse thickening of distal ileum and colon
Lymph node involvement
Thick, corrugated intestine
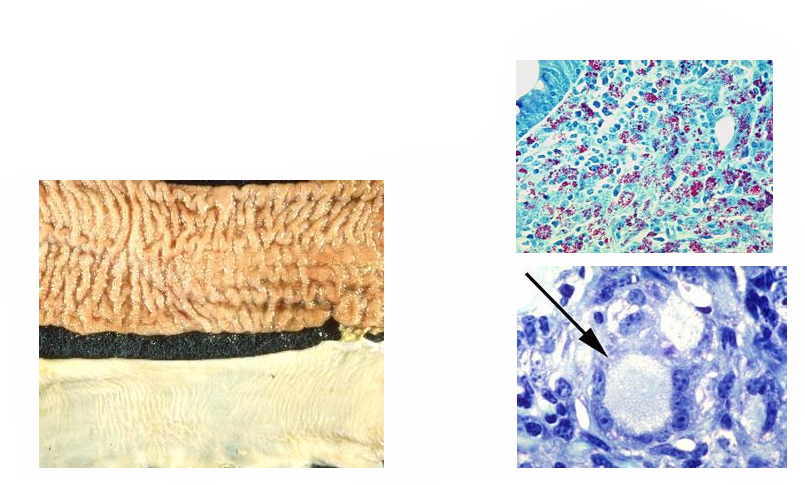
What is the presentation of Johnes disease in clinical disease?
older animals: >3yrs
often seen after calving (stress)
profuse diarrhoea (+/- bubbles) —> protein losing enteropathy
weight loss
bottle jaw
BAR + DUDE

Why is this concerning?
pooled milk so may infect many calves
ok setup if milk replacer being used
high risk of transmission if waste milk
What is the link of crohne's disease with johnes?
mycobacterium avium ss. paratuberculosis has been found in some cronhes biopsies
means crohne's may have many types some of which related to MAP
What is the effect of johnes disease on cattle + production?
reduced milk yield
increased risk of mastitis/ SCC/ digestive disease/ resp. disease
Impaired mucosal barrier function
malabsorption (& consequently diarrhoea)
protein losing enteropathy (& consequently muscle wastage, hypoproteinaemia, oedema)

What is the difference between a clinical and sub-clinical case?
clinical is
actively shedding
ELISA +ve
lost immune control
List susceptible members of a herd to Johnes
most to least likely
new born calf
young heifer
old cows and heifers
before birth (in utero- dam is clinical)
What are the Johnes infection routes in young cows?
faeco-oral transmission
in utero (transplacental)
dirty environment
dam faeces
teat or environment
colostrum- dam or pooled
What affects the likelihood of johnes infection?
Dam shedding status
How does the immune system respond to Johnes disease infection?
infection as calf
MAP in macrophages
cell mediated immunity protective
halts disease progression
no shedding
if cell mediated immunity fails —> disease progresses
antibody response
suppresses CMI
Shedding occurs
infectious
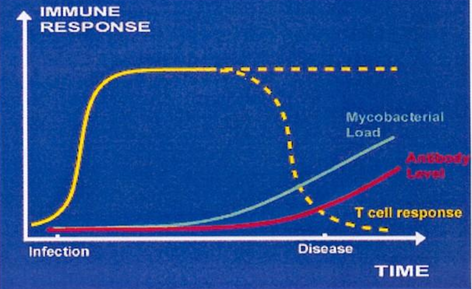
What are the different types of shedders?
Infectious
low
high
super
infected but not shedding
How can Johnes disease be diagnosed?
faecal culture +/- PCR (can also perform on blood + milk)
detects shedders (> threshold)
ELISA (serology)
detects antibodies
probably a shedder
Actiphage
releases DNA of MAP for PCR
gamma interferon
detects cell mediated immunity
PCR
Stained faecal smears
Tissue biopsy
Postmortem examination
What are the pros and cons of:
culture
PCR
ELISA?
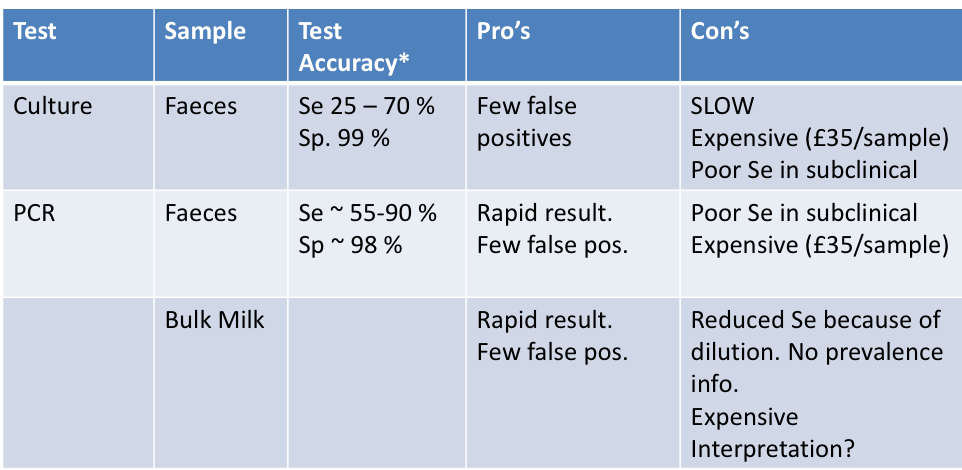
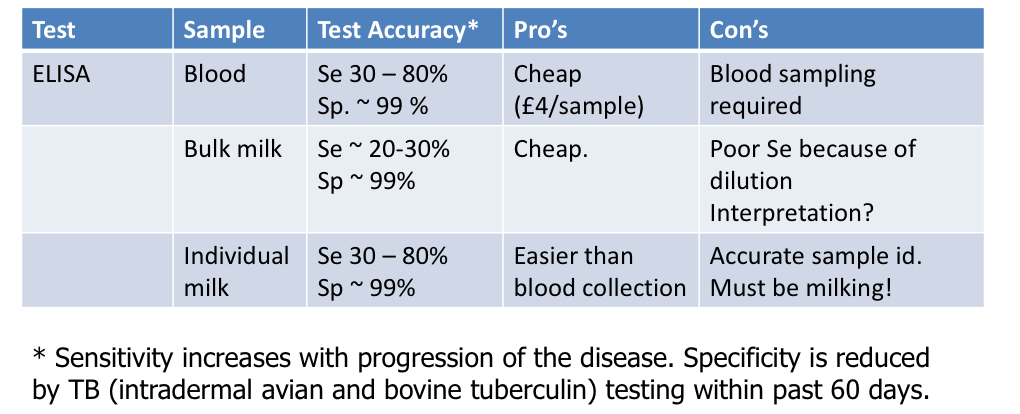
What are the good standard diagnostic tool for Johnes disease?
Faecal culture
detects shedders
affected by intermittent shedding
lower sensitivity to PM biopsies
PCR
use pooled samples
higher sensitivity than culture for shedders
Outline sampling for Johnes detection
milk/ blood antibodies
to detect infection in herd
select cows most likely to be +
thin,
mastitis
lame
poor yield
older
can sample over period
How does ELISA work for Johnes Dx?
detects antibodies
animal clinical
sensitivity dependent on
age distribution of herd
stage of disease
sample: different cut-off values with milk or blood
What is the most sensitive testing programme for Johnes?
repeated whole herd screens
What is phage testing?
uses an antiphage (virus that targets bacteria) to lyse the MAP bacteria and increase the sensitivity of the PCR test
try to increase sensitivity
Does a negative ELISA confirm the cow is free fromthe disease?
could be in cell mediated stage of disease + antibodies not yet being produced
What is a super shedder?
> 1 million cfu/g faeces
(colony forming units per gram)
List types of antibody testing strategies
quarterly milk testing
allows creation of risk groups
single test- pre dry off
segregate + animals away from low risk cattle
double test- pre-dry off and pre- breeding
allows additional info for breeding decisions to be made
What is the most common route of transmission?
INGESTION > transplacental
Outline control of Johne's disease
reduce transmission to young stock
reduce risk factors
cull animals likely to be shedding
possible faecal PCR testing of young stock
improve husbandry
How can risk factors of Johne's be reduced?
avoid faeces
calving area: snatch calving at birth
cleaning calving/ calf pens
separate young stock from adults
only dam's colostrum
no pooled colostrum or waste milk feeding
What is the effect of colostrum use on Johne's transmission?
frozen colostrum
from heifers
from test -ve cows
Do not feed pooled colostrum or waste milk
do not use on-farm pasteurised milk or milk replacer
potential contamination
What are some other transmission risk factors of Johne's?
slurry / manure spread whilst grazing
water courses esp. stagnant water
contamination of feeds
other hosts
sheep, deer, rabbits
How can the risk of purchasing animals into the herd be reduced?
from low risk herds
no Hx
test negative on last 3 tests
CHeCS level 1
ELISA test result history of whole herd (or individual)
faecal culture indicidual
What breeds of beef sucklers is Johne's a problem?
Welsh blacks
Limousin
How can farm management be improved for Johne's control in beef sucklers?
outdoor calving
or move outside immediately after calving
cull daughters
clip and clean teats prior to calving
CHeCS level 1 clean bull
What is the affect of MAP and bTB on each others testing/ diagnosis?
MAP may give false –ve to TB test
reacts +ve to avian ppd (“bigger top lump”)
TB test compares avian ppd and bovine ppd reactions
i.e. reduces TB test sensitivity
TB test will give “false +ve” to MAP ELISA test
ensure 60-day time lag between TB test & ELI