Session 10: Personalised Medicine I
1/43
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
44 Terms
Personalised medicine
uses information about each individual's genetic material to tailor therapy with best response and highest safety margin to ensure better patient care
Benefits of personalised medicine
- Earlier diagnosis
- Risk assessment
- Optimal treatment
- Improves healthcare
- Lowers costs
The P's of personalised medicine & brief description
1) Prediction & prevention of disease
Identification of high-risk people before onset of symptoms to better inform lifestyle changes and reduce burden of disease/costs. Preventative measures can be taken
2) Precise diagnoses
When paired with improved imaging technology, better knowlege of an individual's abnormality can inform better diagnoses which informs earlier and better treatment.
3) More participatory role for patients
Increased public awareness is the most powerful driver for personalised medicine
4) Prevent adverse side effects
Variants in the genetic code can be used to predict potential adverse drug reactions = significantly reduces burden on NHS and improves patient experience
An example of a disease in which preventative treatment exists for potential cardiovascular events in the future
Familial hypercholesterolemia (FH)
- An inexpensive medication can be given to people as preventative measure for cardiovascular events
Example of a new/improved imaging technique that (when paired with personalised medicine) can provide a more precise diagnosis
Multiparametric MRI
- PROSTATE CANCER = classification of tumours volume/size/dynamic of growth/typical markers for malignancy and invasion of other organs
Spectroscopy
- Used to differentiate between lesions and inflammation on a molecular level
Example of a drug used to treat HIV in which patients must now take genomic test prior to using the drug (prevent allergic reaction)
Abacavir
- First-line treatment for HIV that 1/17 people have fatal adverse reaction
- Patients have specific genomic test before taking this drug which identifies those who could be allergic
- Reduced pressure on NHS
Why is cost-effective healthcare (personalised medicine) important?
State three reasons
1) Reduced trial-and-error dosing of medicines
2) Reduced hospitalisations due to adverse drug reactions
3) Reduced late diagnoses

100,000 Genome Project sequenced DNA from ___ people
85,000 people
Genetic variants are classified on a five-point scale.
What are these classifications?
1) Pathogenic variant
2) Likely pathogenic variant
3) Variant of uncertain significance (VUS)
4) Likely benign variant
5) Benign variant
Cancer is a ___ disease (>200 types)
heterogeneous
Biomarker
Biological molecule found in blood, body fluids, or tissues that indicates a normal or abnormal process or condition/disease e.g., cancer
Give examples of bodily fluids in which biomarkers can be found
- Circulation = whole blood, serum, plasma
- Excretions/secretions = stool, urine, sputum, nipple discharge
- Tissue-derived = biopsy
Genetic biomarkers can be ___ or somatic
Inherited
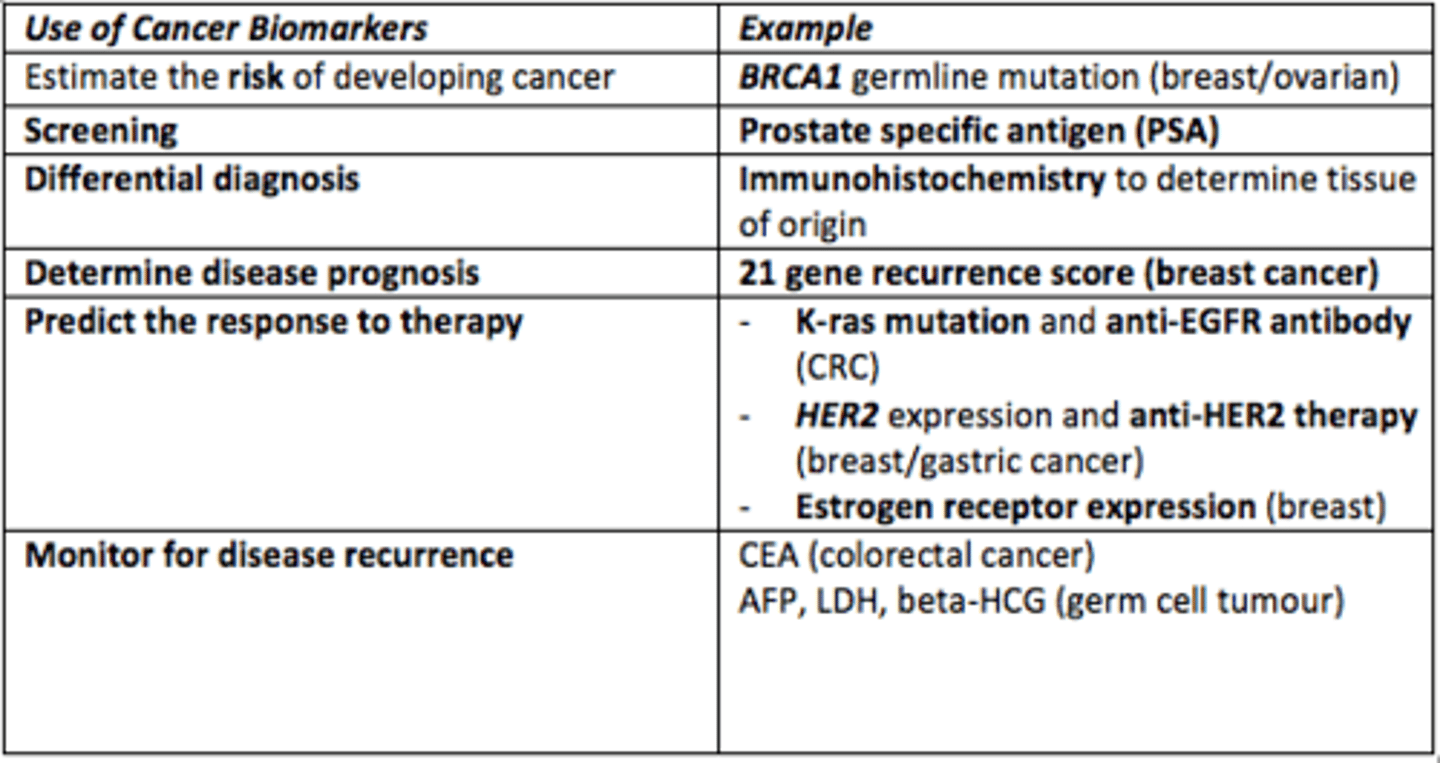
Give an example of a cancer biomarker which is used to estimate the risk of developing a specific type of cancer
BRCA1 germline mutation for breast/ovarian cancer
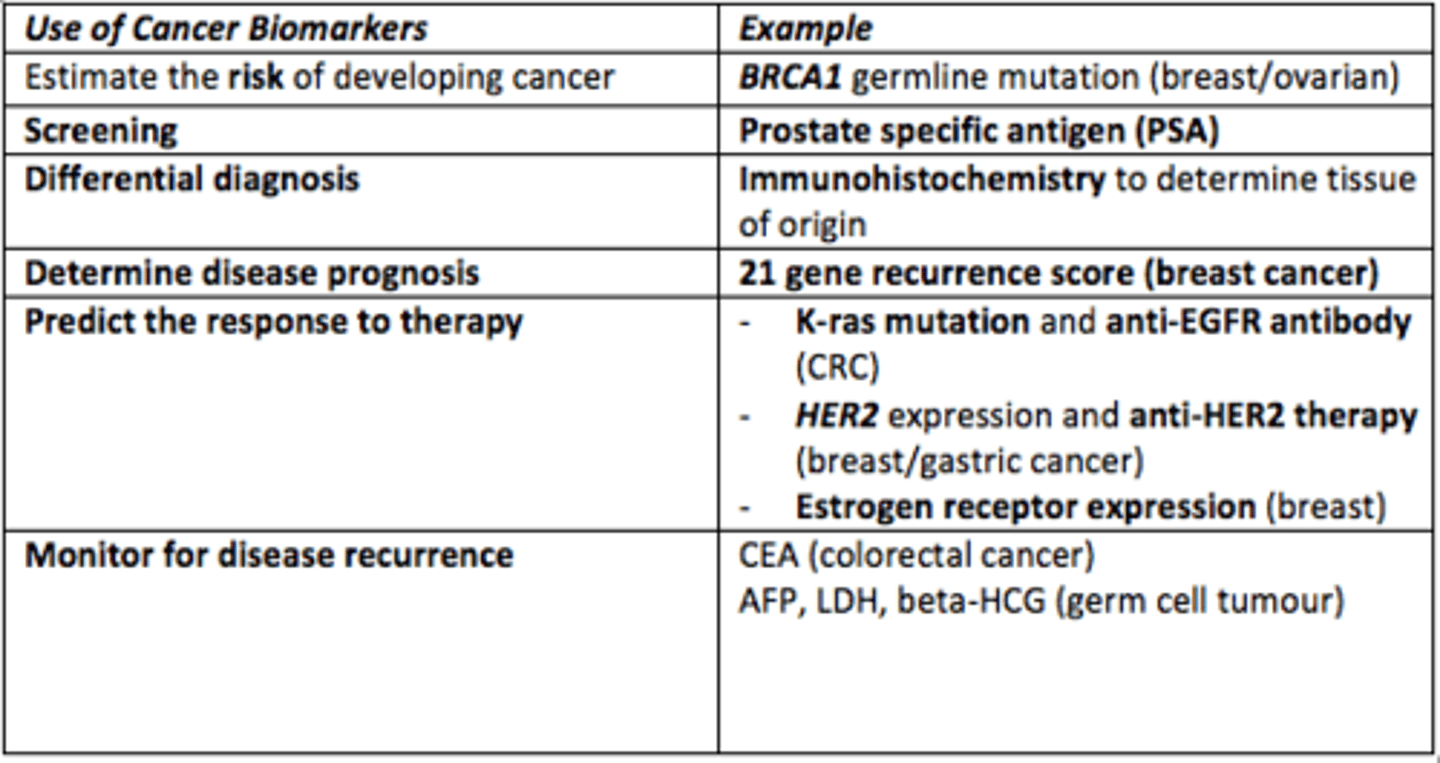
Give example of a cancer biomarker used for screening for prostate cancer
Prostate Specific Antigen (PSA)
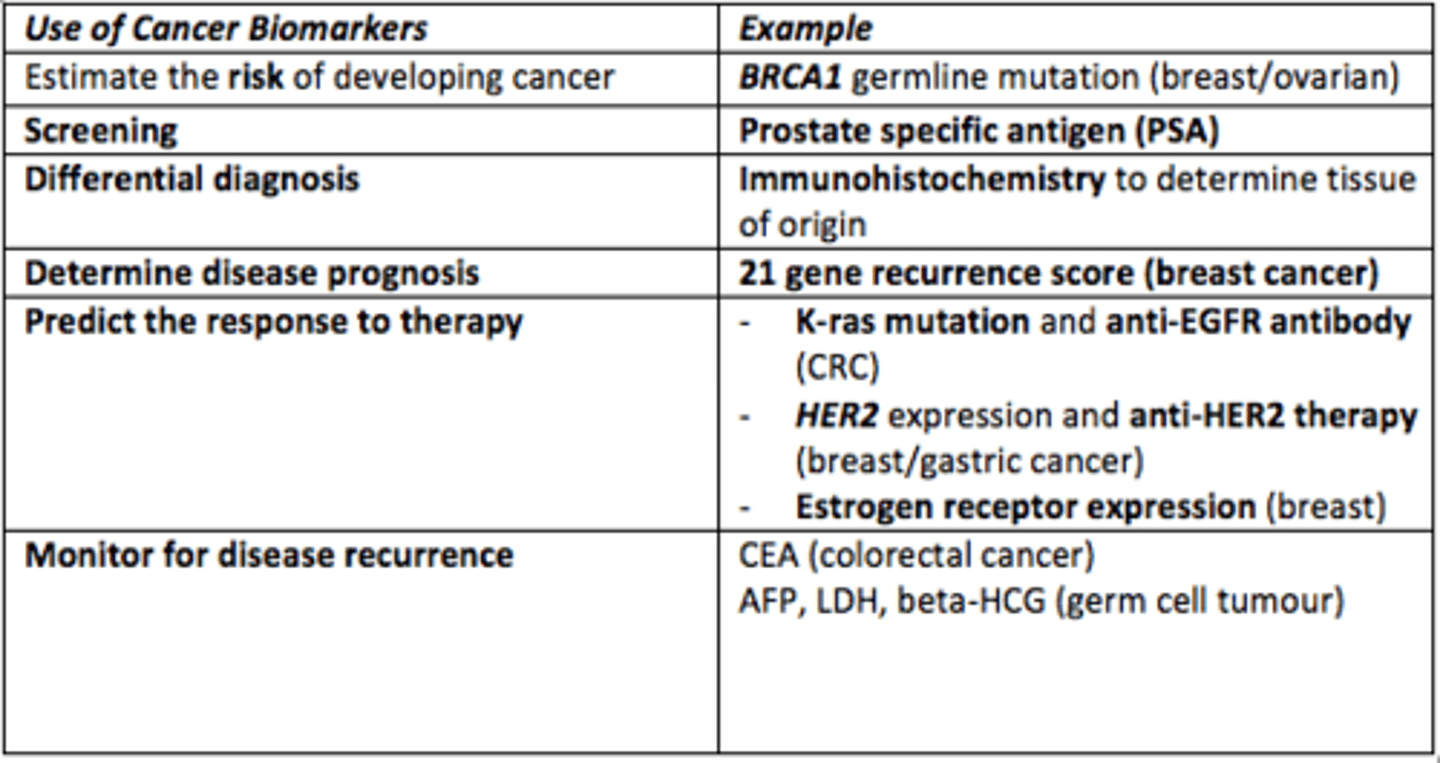
Give example of a technique used for differential diagnosis of cancer
Immunohistochemistry to identify the tissue of origin
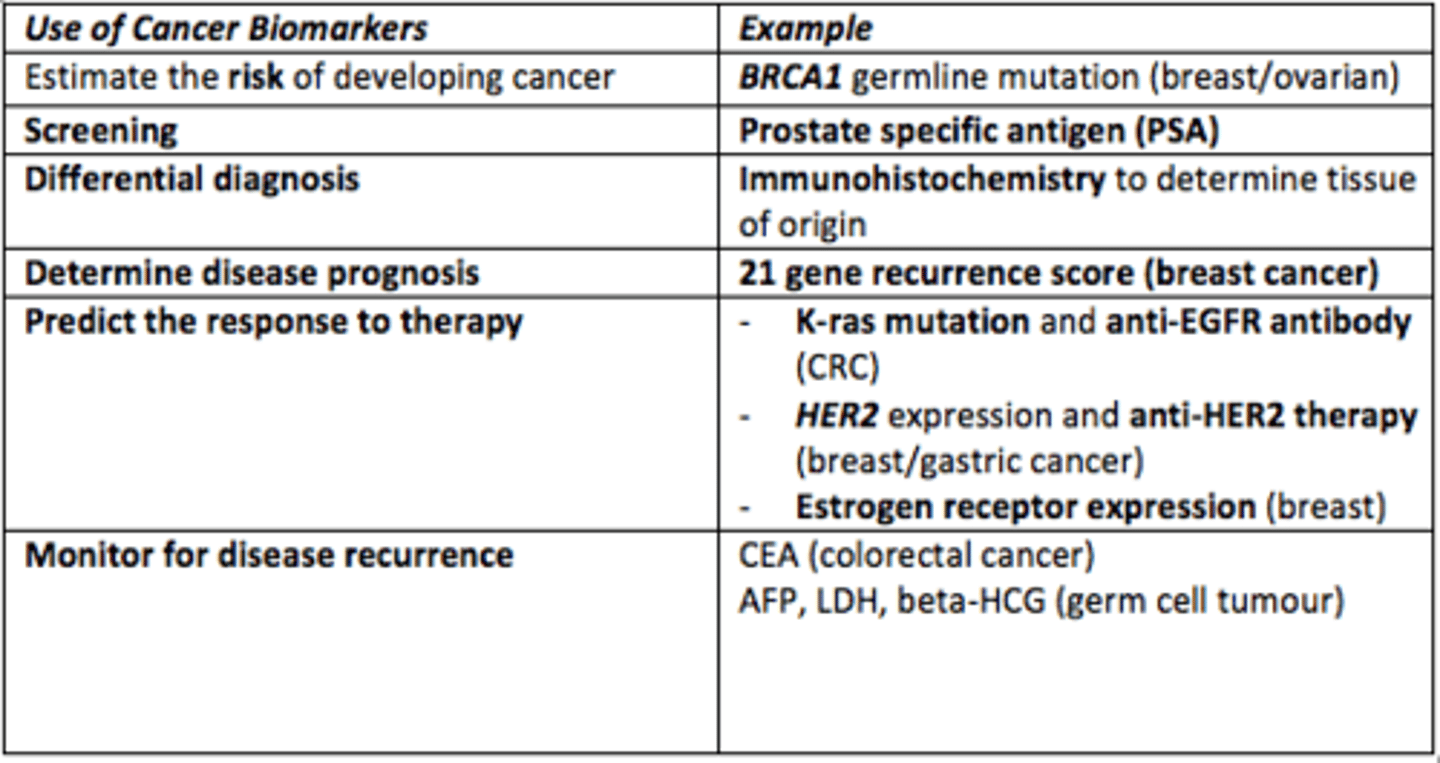
Give an example of a cancer biomarker which is used to predict response to cancer therapy/treatment
- K-ras mutation and anti-EGFR antibody = colorectal cancer
- HER2 expression and anti-HER2 therapy = breast & gastric cancer
- ER (estrogen receptor) expression = breast cancer
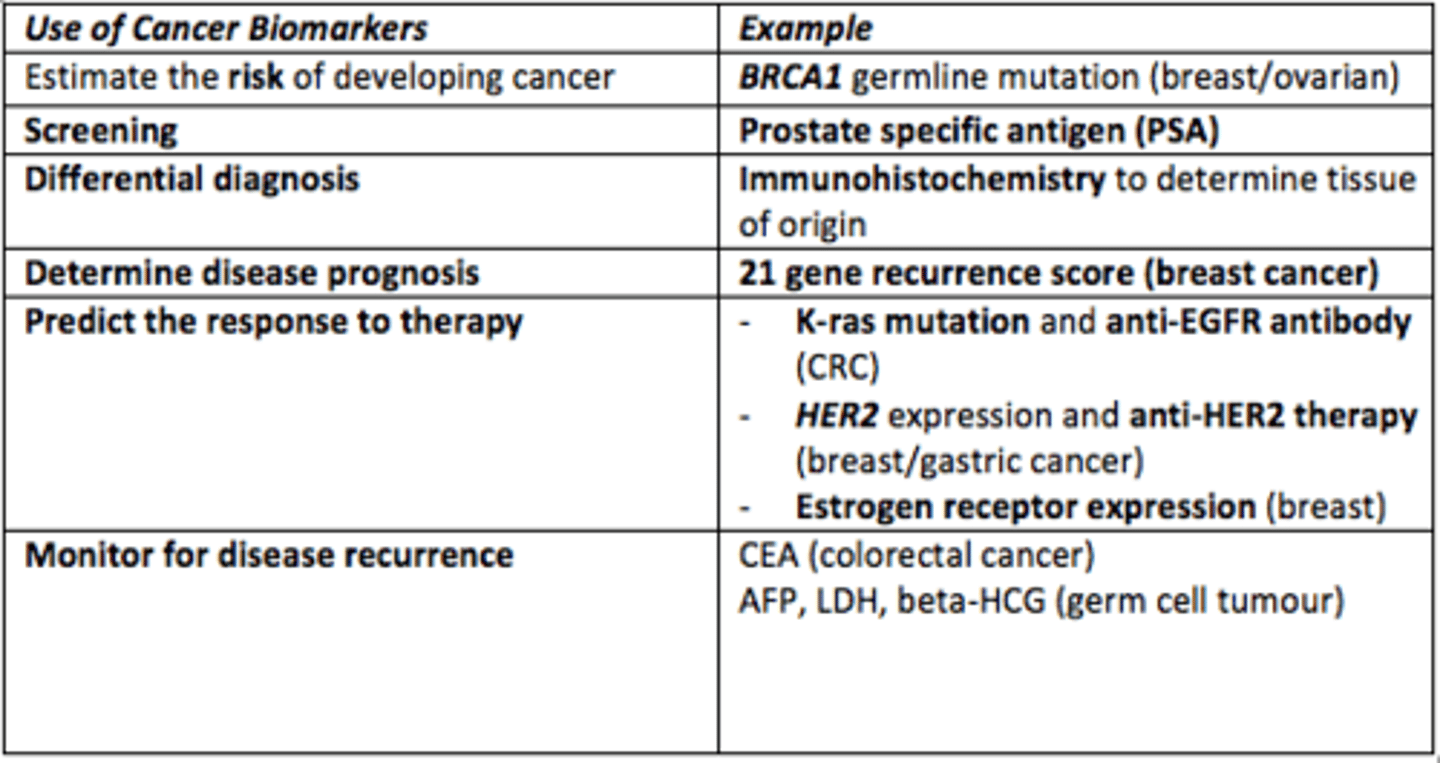
Give an example of a cancer biomarker which monitors for disease recurrence in colorectal cancer
Carcinoembryonic antigen (CEA) test for colorectal cancer
Five main intrinsic/molecular subtypes of breast cancer
1) Luminal A (best prognosis)
2) Normal-like
3) Luminal-B
4) HER2-enriched
5) Triple negative (worst prognosis)
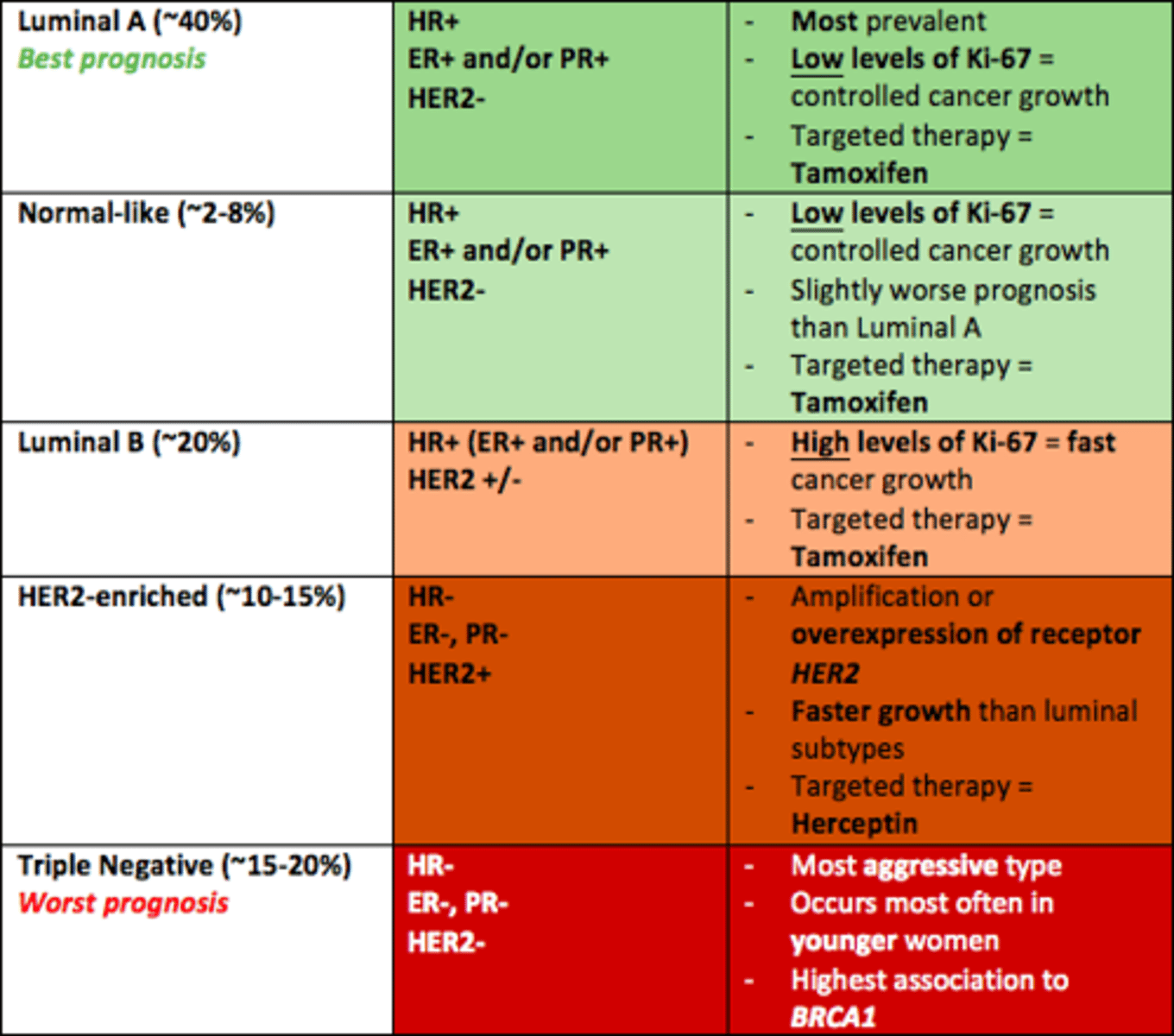
What is the breast cancer subtype with the best prognosis
Luminal A
HR+
ER+ and/or PR+
HER-
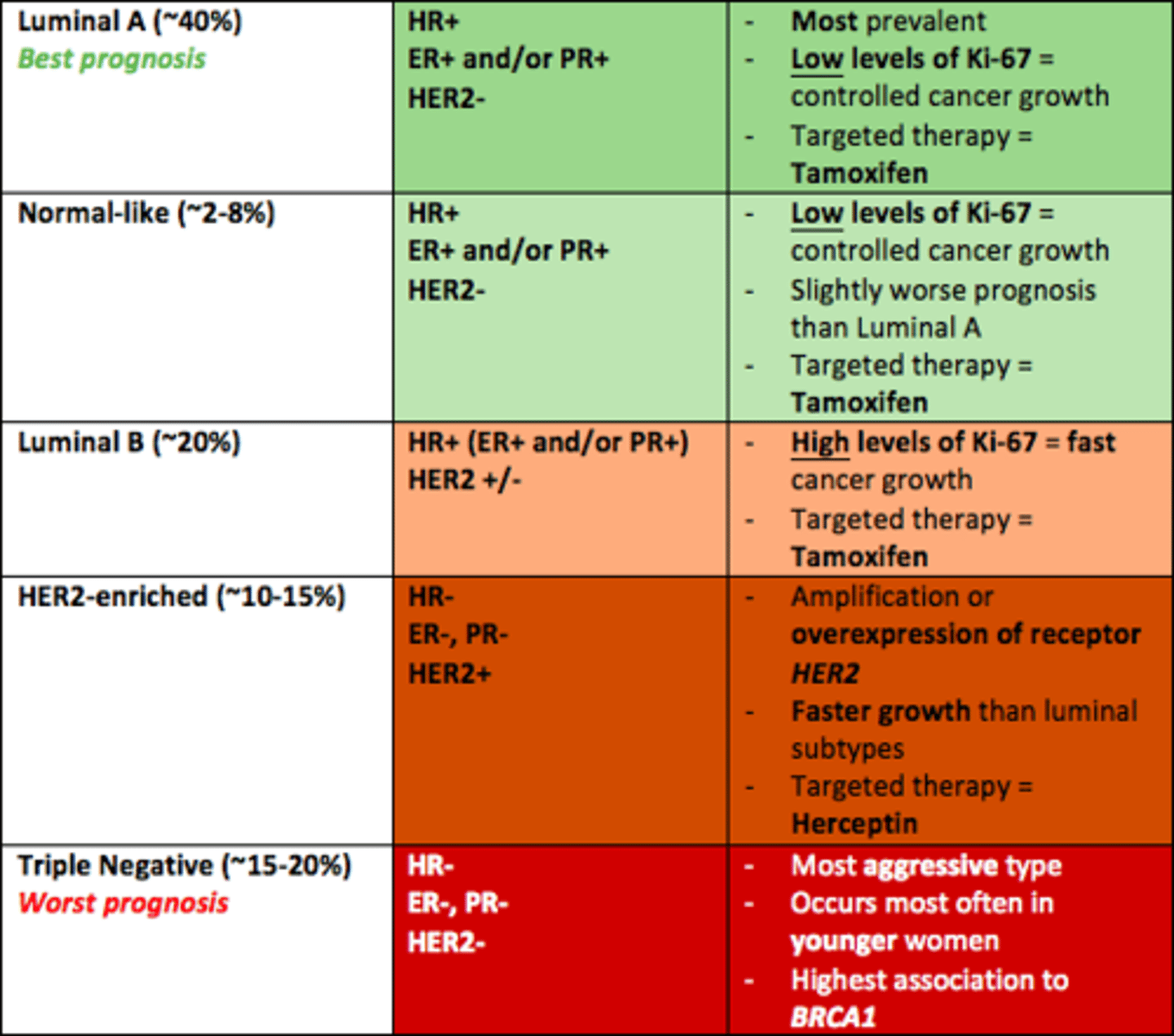
What is the breast cancer subtype with the worst prognosis
Triple Negative
HR-
ER-
PR-
HER2-
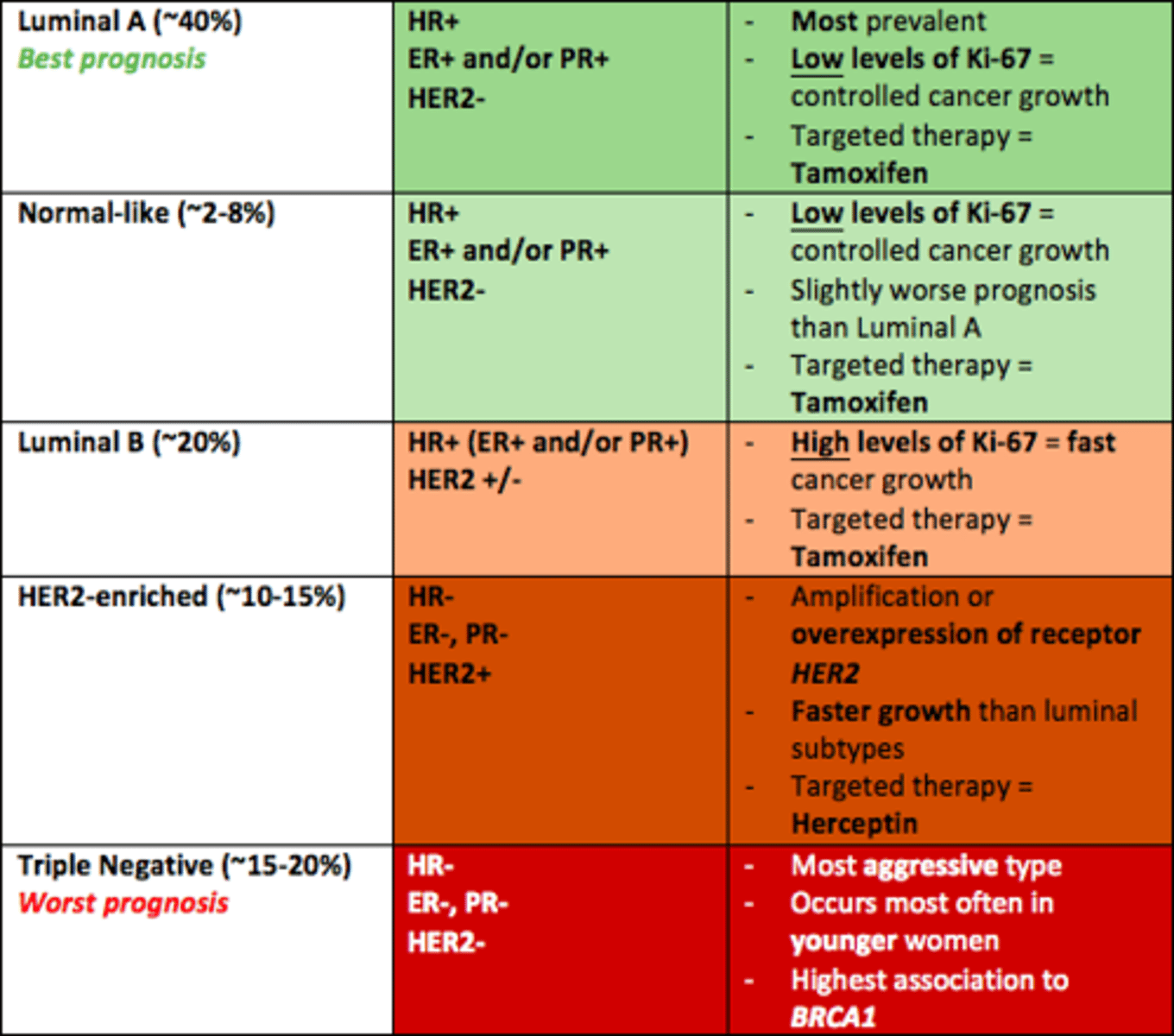
Which breast cancer subtypes respond to Tamoxifen
1) Luminal A
2) Normal-like
3) Luminal B
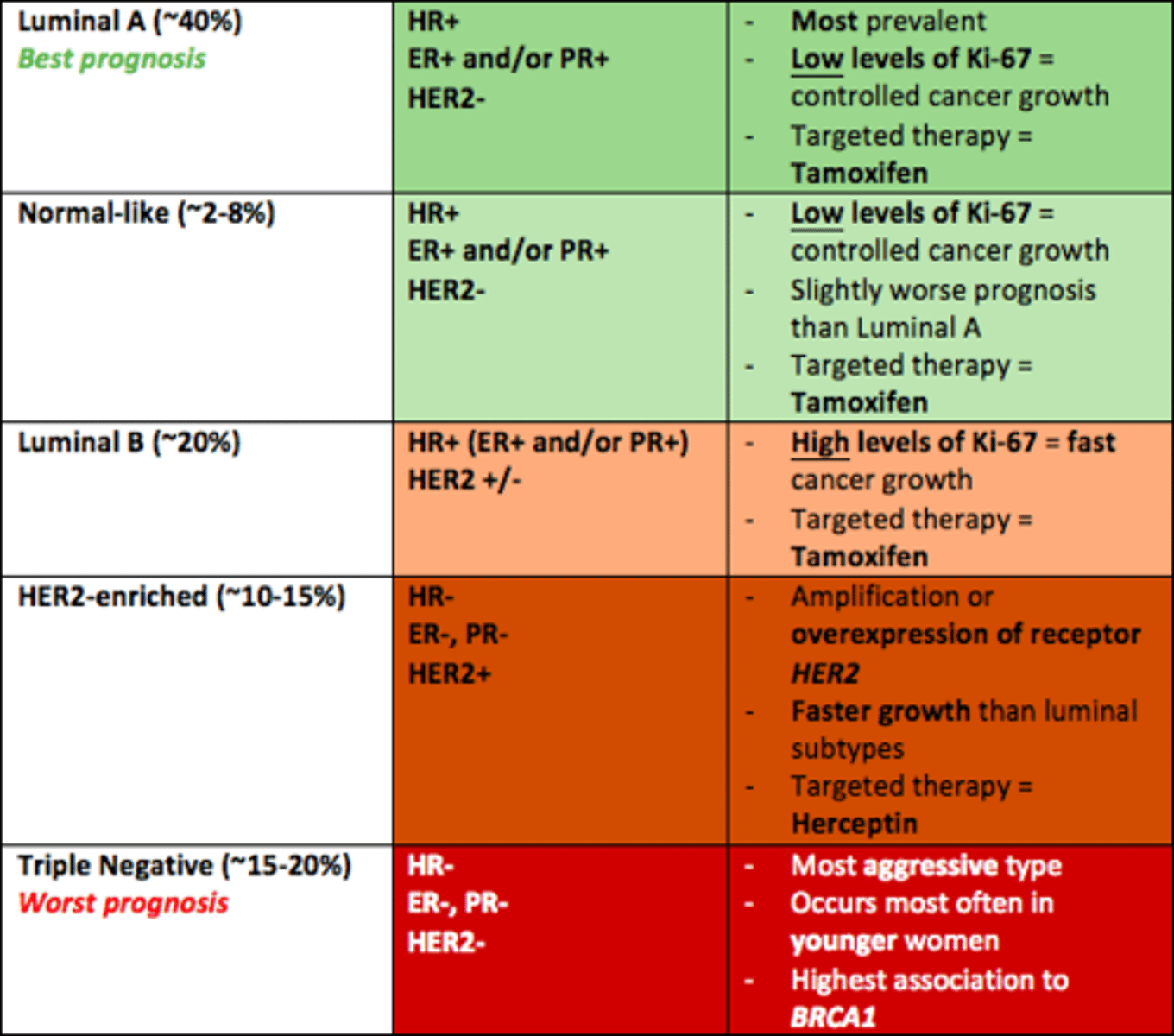
Which breast cancer subtype responds to Herceptin
HER2-enriched
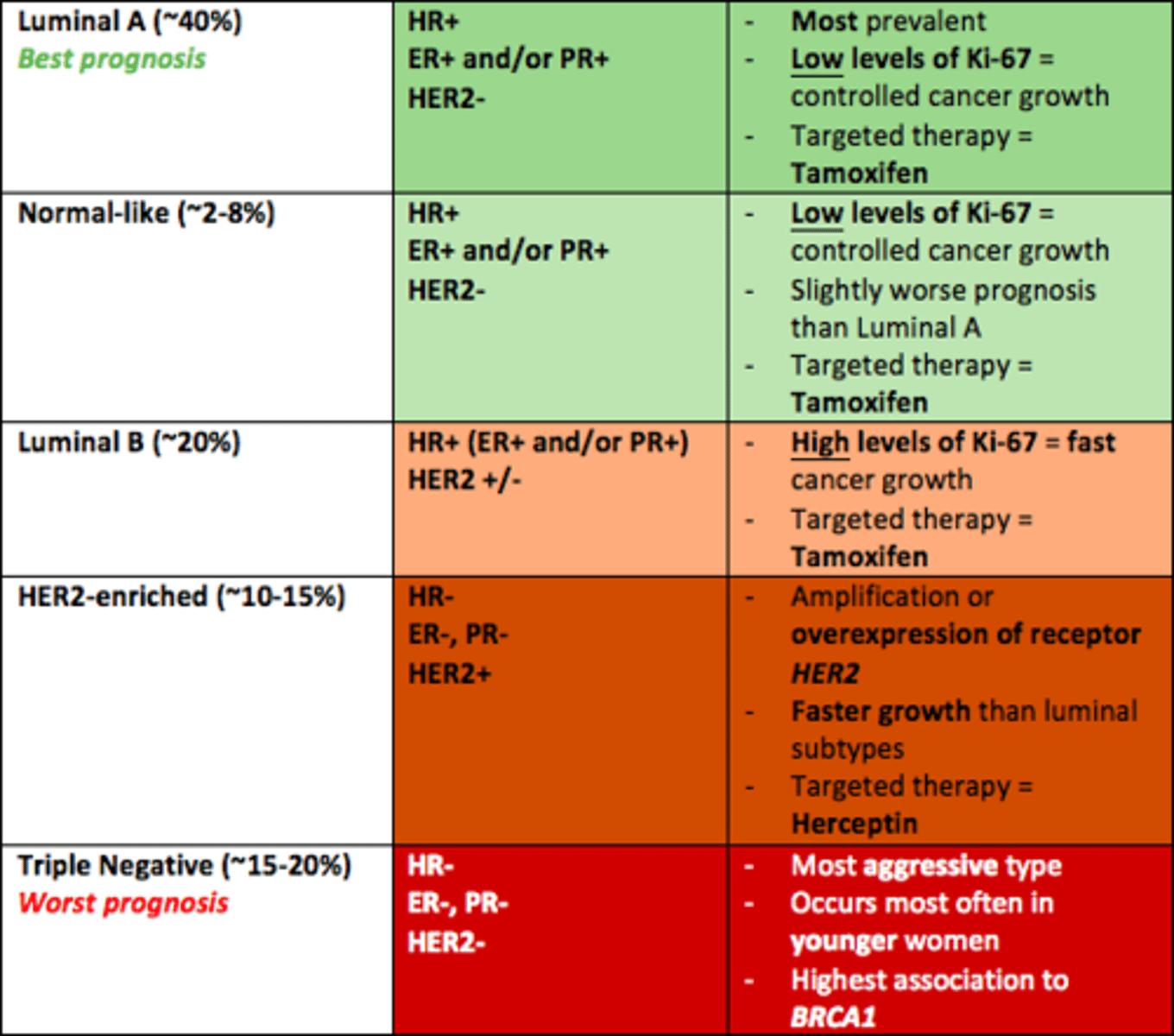
Which breast cancer subtype has the highest association to BRCA1
Triple Negative
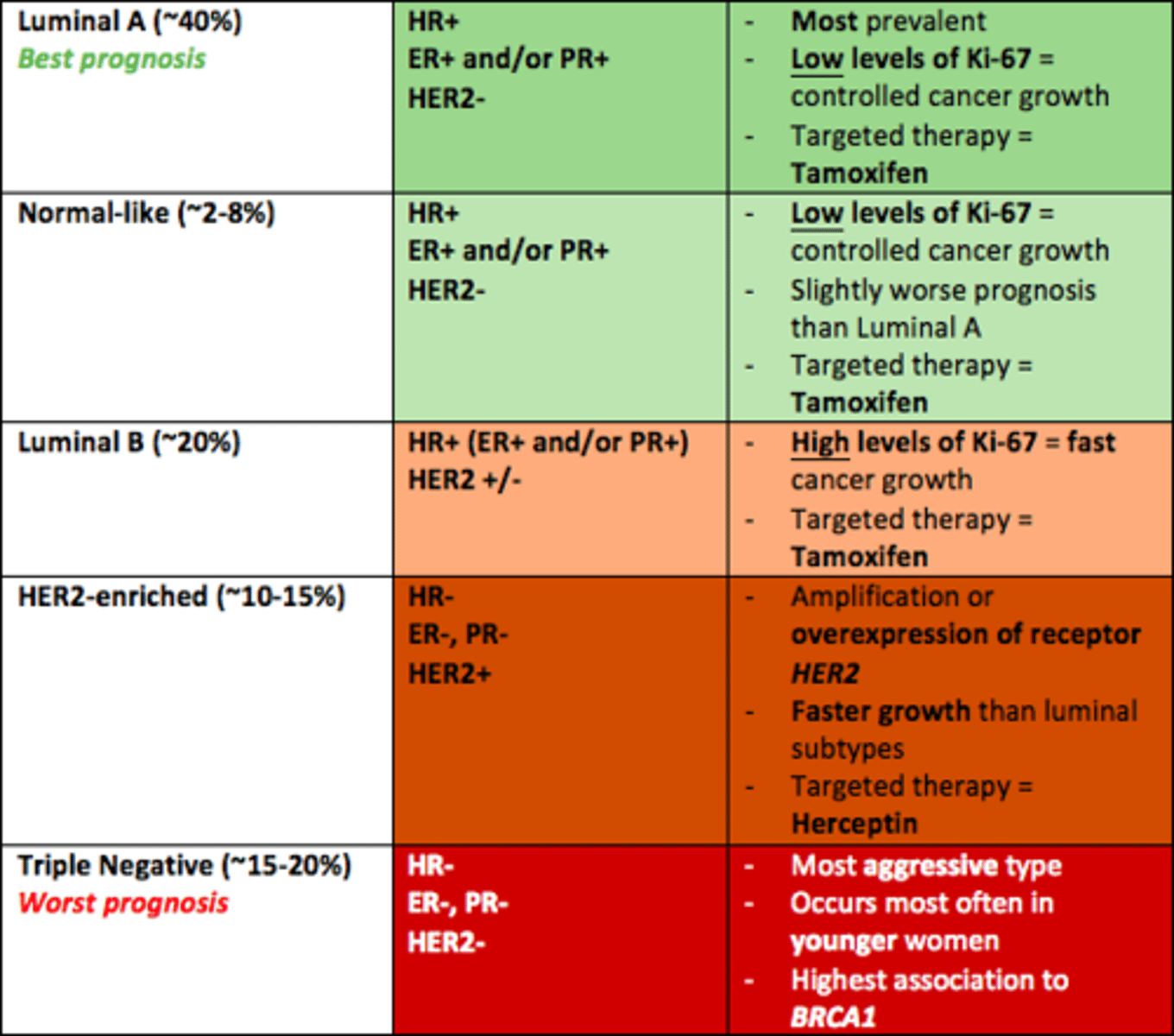
What is the standard approach for reducing risk of recurrence in women with estrogen receptor positive (ER+) early-stage breast cancer
Tamoxifen
How does Tamoxifen work in women with ER+ breast cancer
Tamoxifen → Edoxifen
Edoxifen (primary active metabolite) blocks estrogen receptors (ER)
What is the enzyme that metabolises Tamoxifen into primary active metabolite of Edoxifen?
CYP-2D6
Tamoxifen is used to treat ___ positive early-stage breast-cancer
ER positive
Herceptin (trastuzumab) - what is it
Anti-HER2 monoclonal antibody used to treat women with HER2+ breast cancer
What is the Oncotype DX test?
Used to help determine the need for chemotherapy for women with stage I or II hormone receptor-positive cancer. Looks at 21 genes within the tumor to determine the likelihood of...
- Cancer recurrence
- Cancer response to treatment
The two functions of the Oncotype DX prognostic and predictive test for breast cancer
1) How likely breast cancer will reoccur
2) Predicts response to treatment (chemo/radiation)
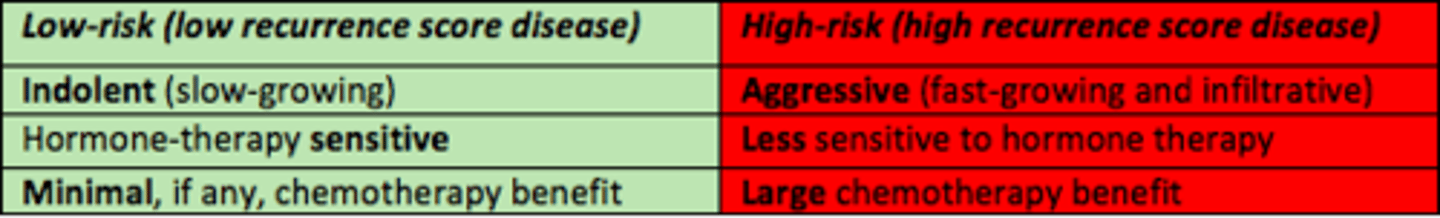
Low-risk score of the Oncotype DX test means...
- Indolent (slow-growing)
- Hormone-therapy sensitive
- Minimal chemotherapy benefit
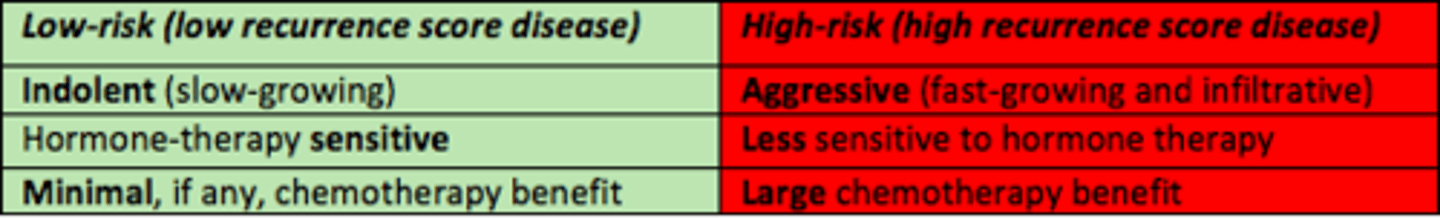
High-risk score of Oncotype DX test means...
- Aggressive (fast-growing)
- Less sensitive to hormone therapy
- Large chemotherapy benefit
What are some breast cancer prevention steps?
1) Lifestyle modifications
2) Early intervention with elective surgery (mastectomy)
3) Chemoprevention
4) Increased mammography frequency
What are some current barriers to personalised medicine?
1) Costs of tests/treatment
2) Guidelines = NICE (UK), FDA (USA)
3) Current knowledge and understanding
4) Massive amount of data to integrate (genomics, transcriptomics etc)
What is drug repurposing?
Identifying new therapeutic uses for old or already-existing drugs
Drug repurposing relies on two scientific bases
What are they?
1) The discovery (through human genome) that some diseases share common biological targets
2) The concept of pleiotropic drugs
Pleiotropic
A gene that influences many traits, rather than just one
Give three examples of drug repurposing
1) Aspirin
- Initially used as analgesic
- Repurposed as antiplatelet aggregation drug (prevent cardiovascular events)
2) Thalidomide
- Initially used for morning sickness - banned for teratogenicity
- Repurposed for leprosy (inhibition of TNF-a)
- Repurposed again as first-line drug for multiple myeloma
3) Sildenafil
- Initially used as anti-hypertensive drug (angina)
- Repurposed for vasodilation for erections (viagra)
- Second repurposing = treatment of idiopathic form of pulmonary arterial hypertension
Give an example of a drug that was repurposed before it even reached the market
Sildenafil

Direct-to-Consumer (DTC) Genetic Testing
Genetic testing that is offered directly to individuals. There is typically no input, recommendation, or follow-up by a genetics professional
e.g., 23-and-Me
23-and-Me (Direct-to-Consumer Genetic Testing) screens for ___ variants that predispose individuals to certain conditions
23-and-Me (Direct-to-Consumer Genetic Testing) screens for allelic variants that predispose individuals to certain conditions
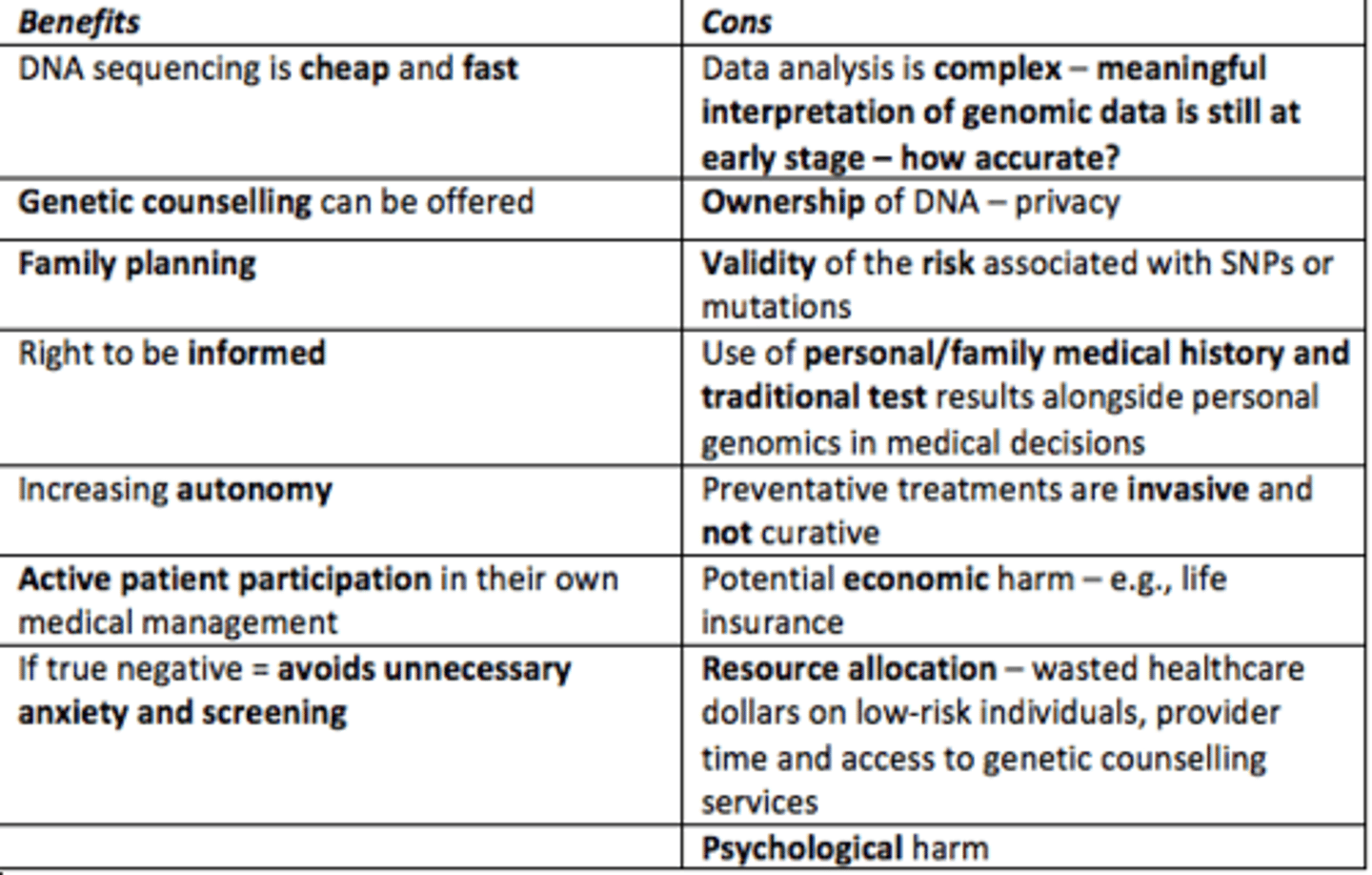
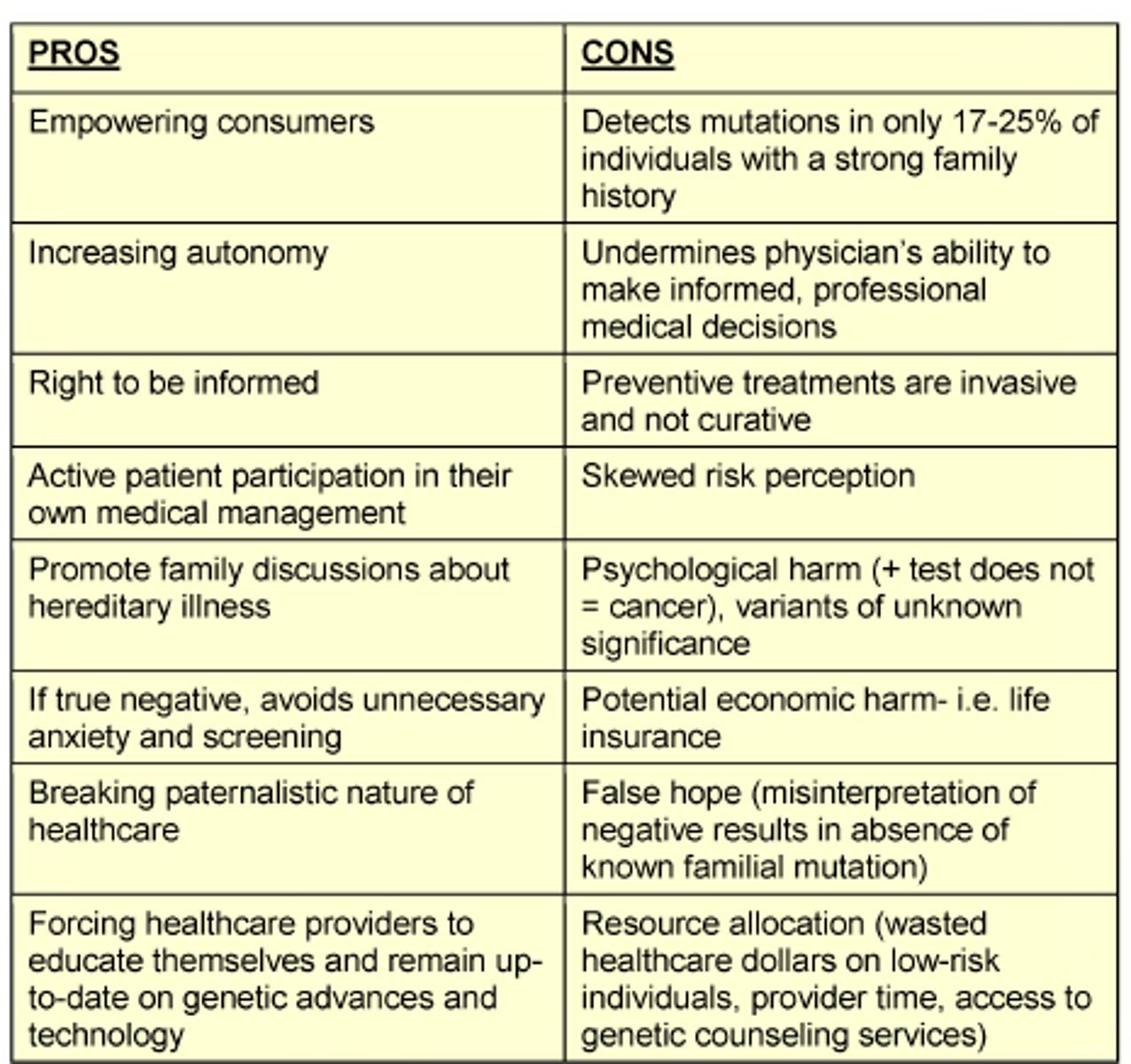
Some benefits of Direct-to-Consumer (DTC) genetic testing
- Family planning
- Cheap and fast
- Increases autonomy
- Right to be informed (breaking paternalistic approach to healthcare)
- Active patient participation in their own medical management
- If true negative = avoids unnecessary anxiety and screening
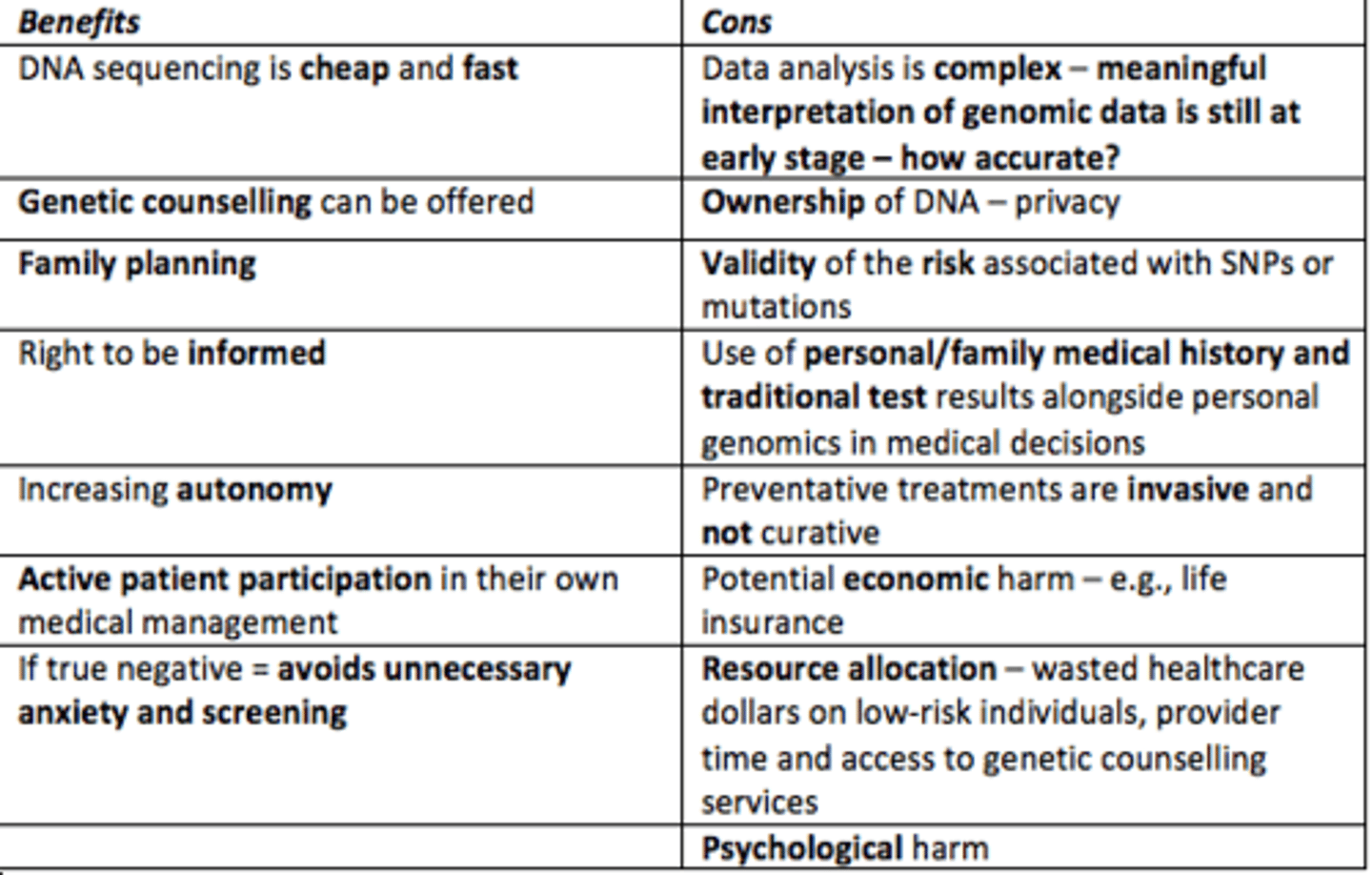
Some cons to Direct-to-Consumer (DTC) genetic testing
- May not be entirely accurate results
- Ownership of DNA (privacy)
- Validity of risk
- Preventative treatments are invasive/not curative
- Potential economic harm e.g., life insurance
- Resource allocation = wasted healthcare money on low-risk individuals, provider time & access to genetic counselling services
- Psychological harm