5. ophthalmic pharmacology
1/18
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
19 Terms
what parts of the eye can be targeted with topical treatment?
ocular surface to posterior lens capsule
corneal disease, anterior uveittis (intraocular inflammation)
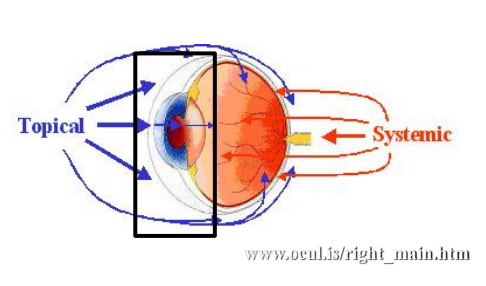
what parts of the eye can be targeted with systemic treatment?
lids, orbit, posterior segment, perforated globe
blepharitis (lid infection/inflammation), posterior uveitis, rupture
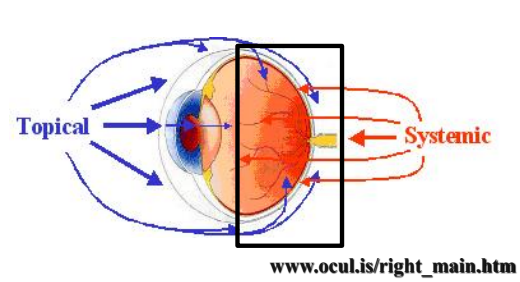
ocular barriers to drugs (4)
tear film (topical)
dilutes
blinking — distributes tear film, removes drugs
corneal epithelium — tight junctions (topical)
diffuse through cells (lipophilic); small molecules between cells
stroma (topical)
high water content (hydrophilic)
drugs which penetrate the cornea must be lipophilic and hydrophilic
blood:eye barrier
tight junctions in blood vessels of uvea, retinal pigmented epithelium, retinal blood vessels
keeps media clear
types of topical drugs
solutions — most common
shortest duration
water-soluble; drugs completely dissolved in solvent
suspensions — most steroids
particles of active ingredient + saturated aqueous vehicle → must be shaken prior to use
ointments — most are mineral oil/petrolatum
longest duration
drug mixed into melted vehicle, then cooled
greasy; blur vision
how are topical broad spectrum antibiotics used to treat corneal lesions?
prophylactic treatment of non-infected superficial epithelial loss
more frequent application if infected
how do most antiviral drugs inhibit viruses?
most are nucleoside analogues
substitute for nucleotides in DNA synthesis → interfere with DNA polymerase & replication
most don’t kill virus
which oral antiviral drug is safe to use in cats?
famciclovir
(others → bone marrow & kidney toxicity)
which anti-fungal class is most effective against equine isolates?
azoles
what type of drugs is most commonly used to treat KCS (dry eye)? what are their effects?
calcineurin inhibitors
decrease T lymphocyte activation
direct lacrimogenic effect — increase tear production
primary vs. secondary glaucoma
primary: problem only with drainage
secondary: drainage problem caused by something else (inflammation, lens out of position, etc)
how do prostaglandin derivatives help with glaucoma? how are they used?
increase aqueous outflow, may decrease production
only useful in dogs; only for primary glaucoma
side effects: uveitis; may add topical steroid
how do carbonic anhydrase inhibitors help with glaucoma?
decrease aqueous production
use in both primary & secondary glaucoma
how do topical beta blockers help with glaucoma? what are potential adverse effects
decrease aqueous production
may increase outflow (miosis)
primary or secondary glaucoma; prophylaxis
some may worsen asthma (cats); bradycardia; decreased tear production
topical corticosteroids are typically used to treat what? when are they contraindicated?
typically used to treat anterior uveitis (inflammation of front part of eye)
corneal penetration is essential
contraindicated if corneal ulcer present
which topical corticosteroids have the best corneal penetration?
acetates (susp.) > alcohols (susp.) >> phosphates (solution)
prednisolone acetate
dexamethasone alcohol
topical NSAIDs are used to treat what? what are potential drawbacks?
used for uveitis
good corneal penetration, some intraocular penetration
may potential bacterial infection, corneal melting (don’t use if corneal ulcer present)
caution: hyphema
ocular effects of atropine
parasympatholytic; long acting (hrs — days)
paralyzes ciliary body
pain relief — ciliary body spasm in uveitis
stabilizes blood:aqueous barrier
effects & uses of proparacaine HCl 0.5% / tetracaine (equine)
topical anesthetic — not analgesic
facilitates taking samples, measuring intraocular pressure
epitheliotoxic, drying, delays wound healing
cannot use for pain relief
effects & uses of tropicamide 1%
parasympatholytic (paralyzes pupillary sphincter muscle) — dilator
similar to atropine but shorter acting (~1-2 hr)
used for retinal exams