N307 Chapter 13: Abnormal Skin Findings & Photos
1/60
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
61 Terms
Primary Skin Lesions
hese are the immediate results of a specific causative factor; primary lesions develop on previously unaltered skin.
Macule, Patch, Papule, Plaque, Nodule, Tumor, Wheal, Urticaria, Vesicle, Bulla, Cyst, Pustule
Macule
Solely a color change, flat and circumscribed, < 1 cm. Examples: freckles, flat nevi, hypopigmentation, petechiae, measles, scarlet fever.
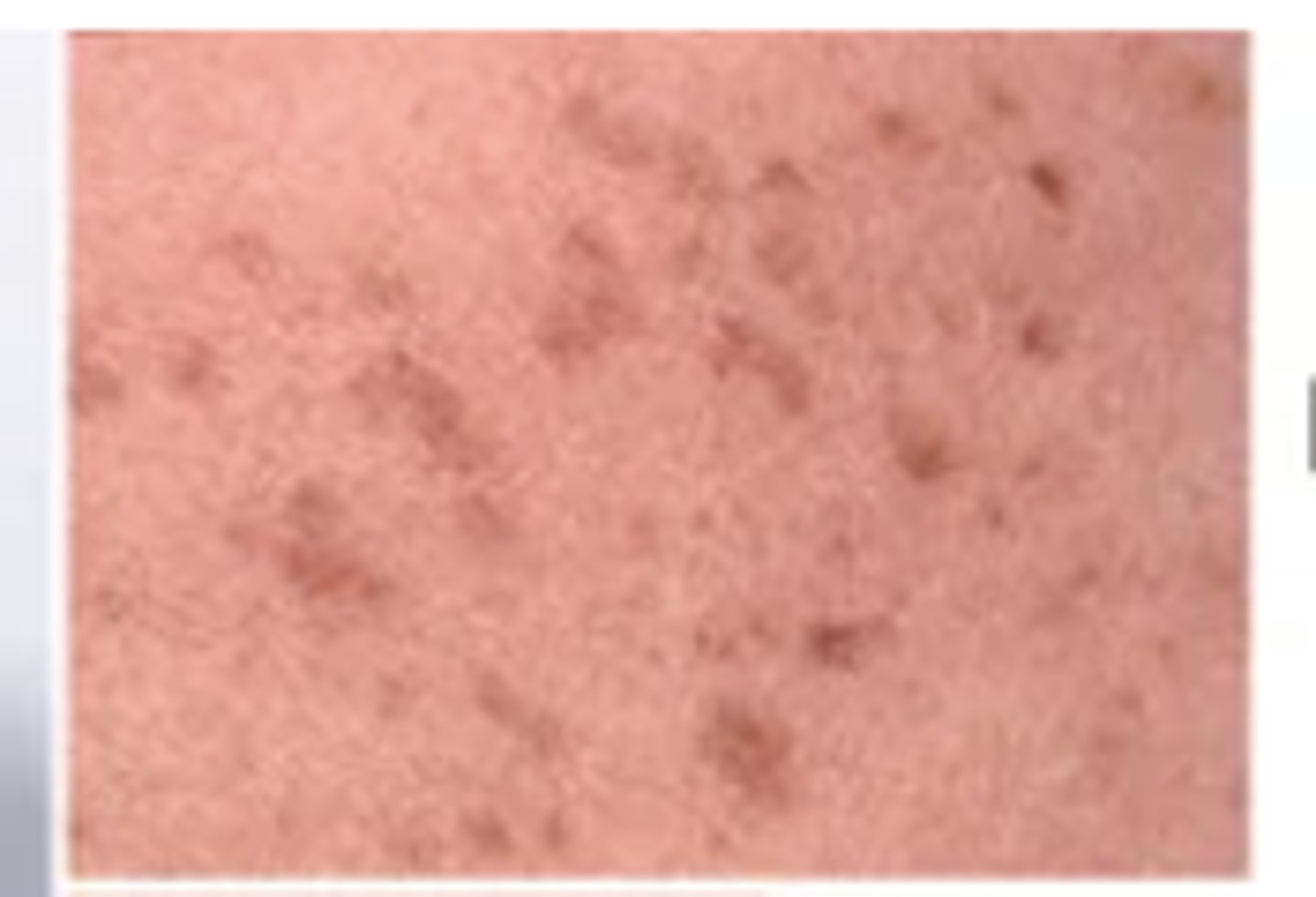
Patch
flat, macule that is >1cm (Mongolian spot, café au lait)

Papule
elevated, solid lesion <1cm, lesion you can feel (mole, wart)
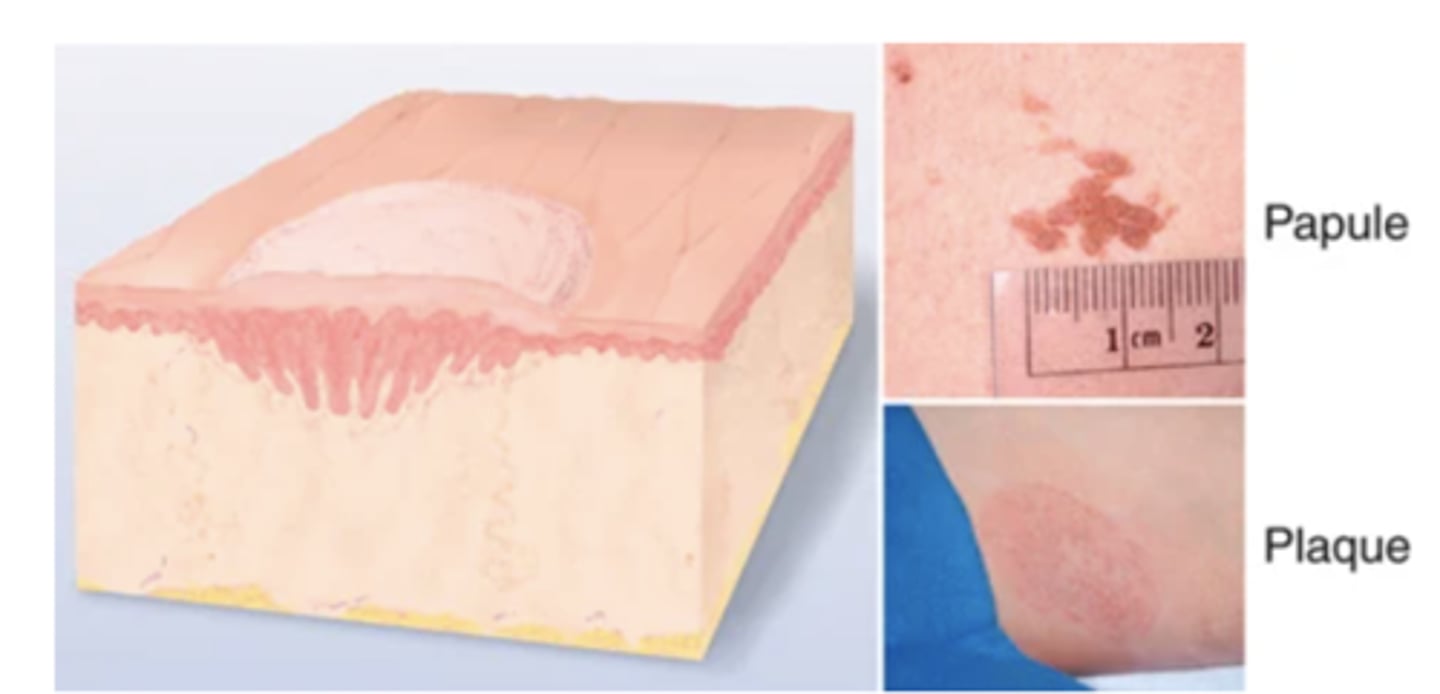
Plaque
papule >1cm in width - surface elevation wider than 1 cm(psoriasis)
Papules coalesce to form surface elevation wider than 1 cm. A plateaulike, disk-shaped lesion. Examples: psoriasis, lichen planus.
Tumor
Larger than a few centimeters in diameter, firm or soft, deeper into dermis; may be benign or malignant, although "tumor" implies "cancer" to most people. Examples: lipoma, hemangioma.
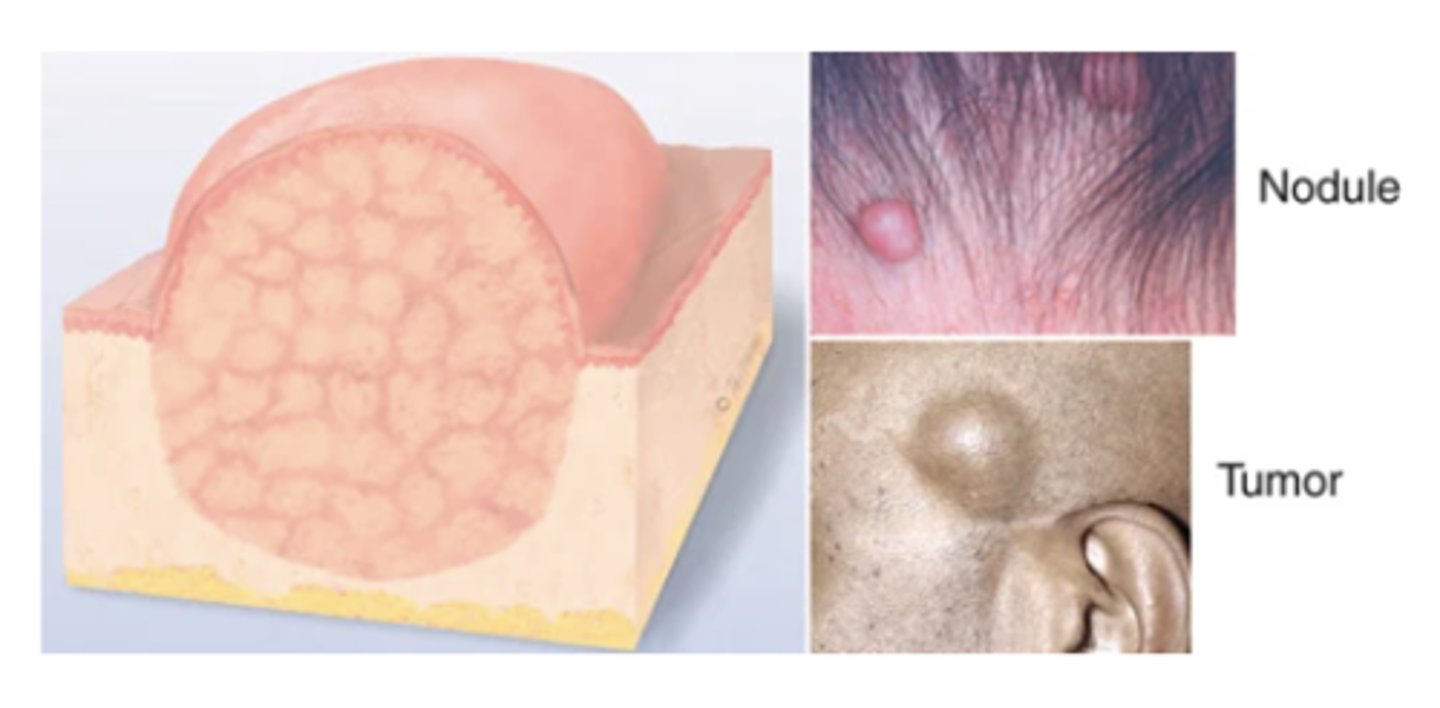
Nodule
Solid, elevated, hard or soft, larger than 1 cm. May extend deeper into dermis than papule. Examples: xanthoma, fibroma, intradermal nevi.
Wheal
Superficial, raised, transient, and erythematous; slightly irregular shape from edema (fluid held diffusely in the tissues). Examples: mosquito bite, allergic reaction, dermographism.
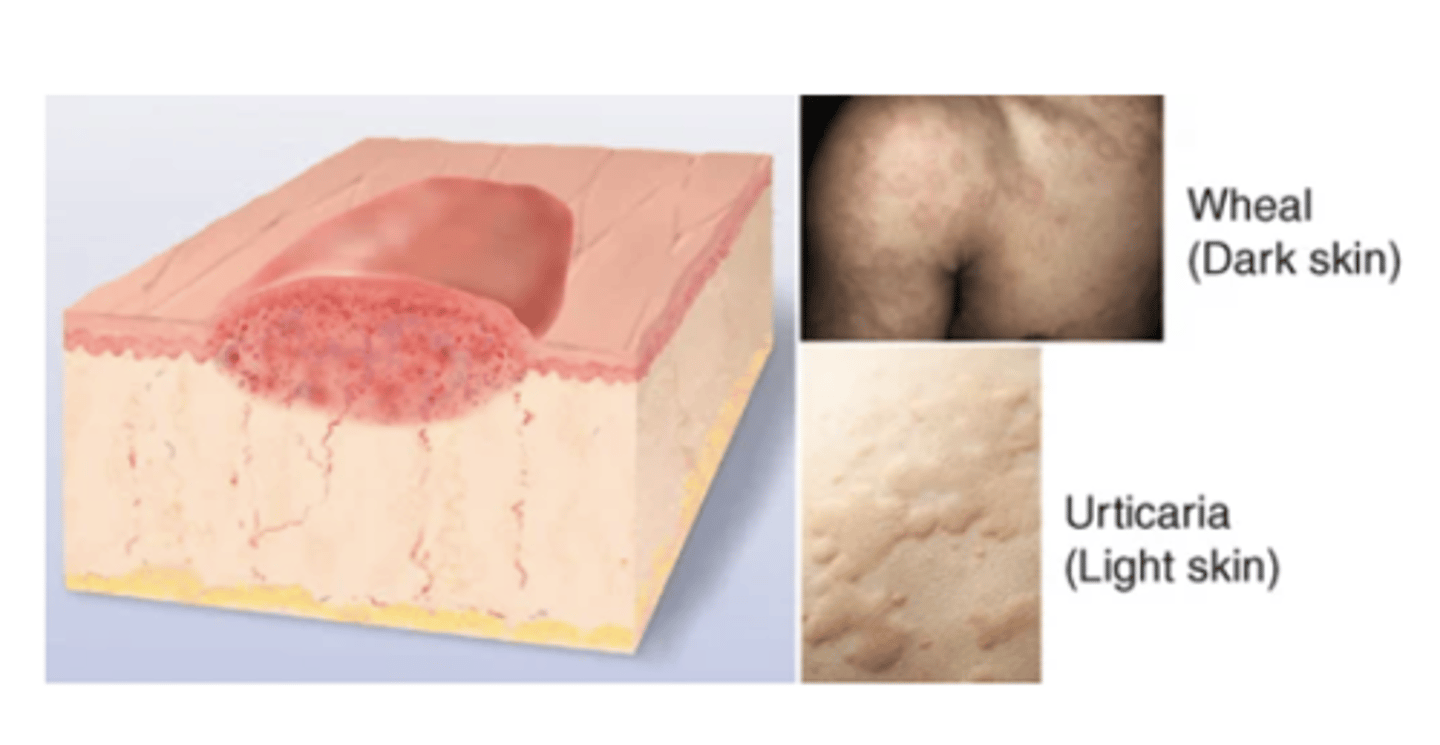
Urticaria (Hives)
Wheals coalesce to form extensive reaction, intensely pruritic.
Vesicle- Elevated cavity containing free fluid, up to 1 cm; a "blister." Clear serum flows if wall is ruptured. Examples: herpes simplex, early varicella (chickenpox), herpes zoster (shingles), contact dermatitis.
Bulla- Larger than 1 cm diameter; usually single chambered (unilocular); superficial in epidermis; thin-walled and ruptures easily. Examples: friction blister, pemphigus, burns, contact dermatitis.
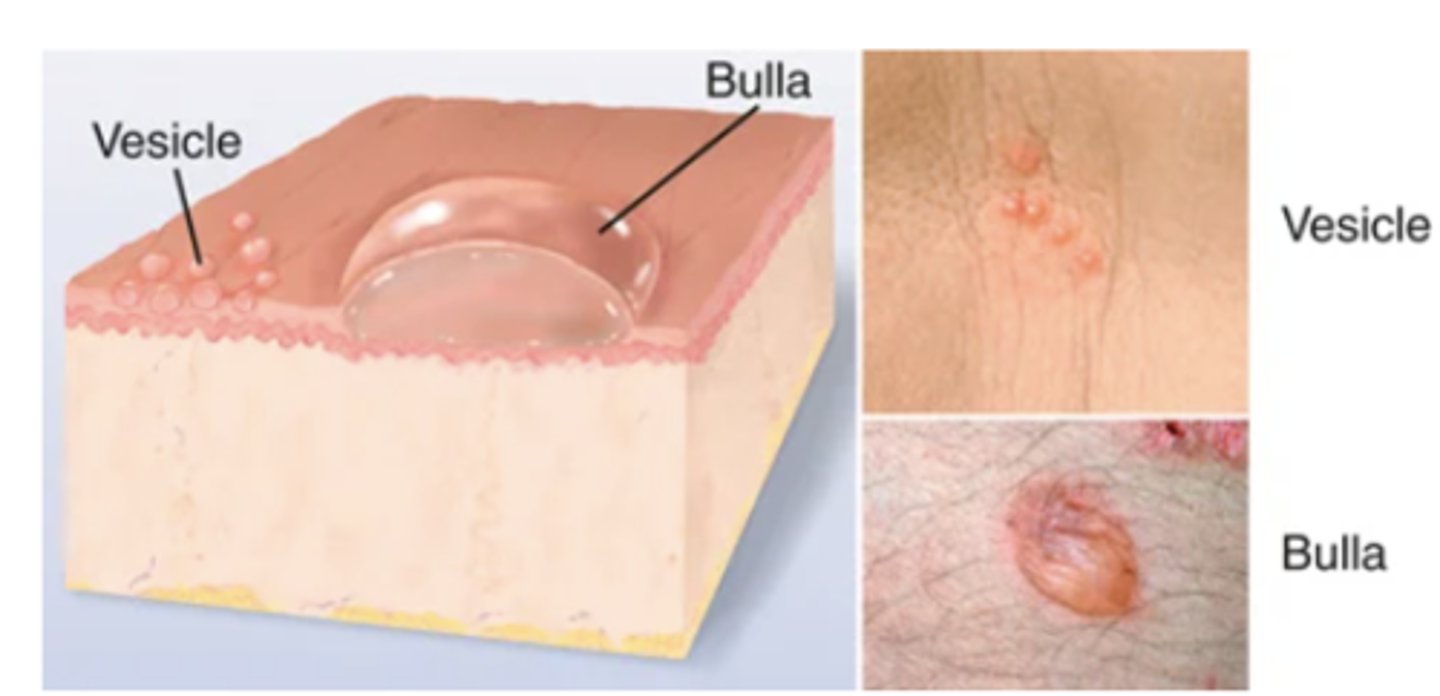
cyst
Encapsulated fluid filled cavity
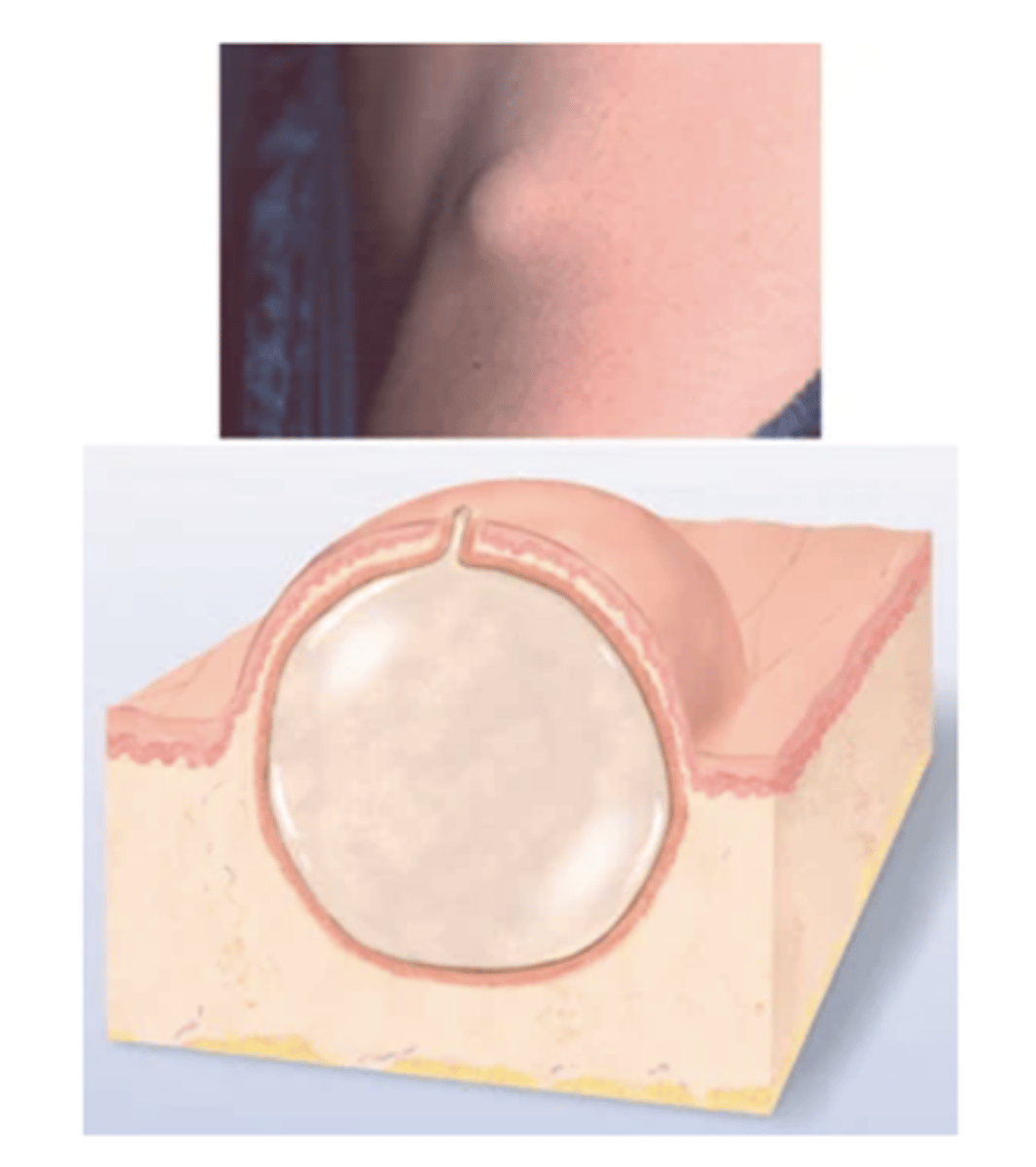
Pustule
Turbid fluid (pus) in the cavity. Circumscribed and elevated. Examples: impetigo, acne.
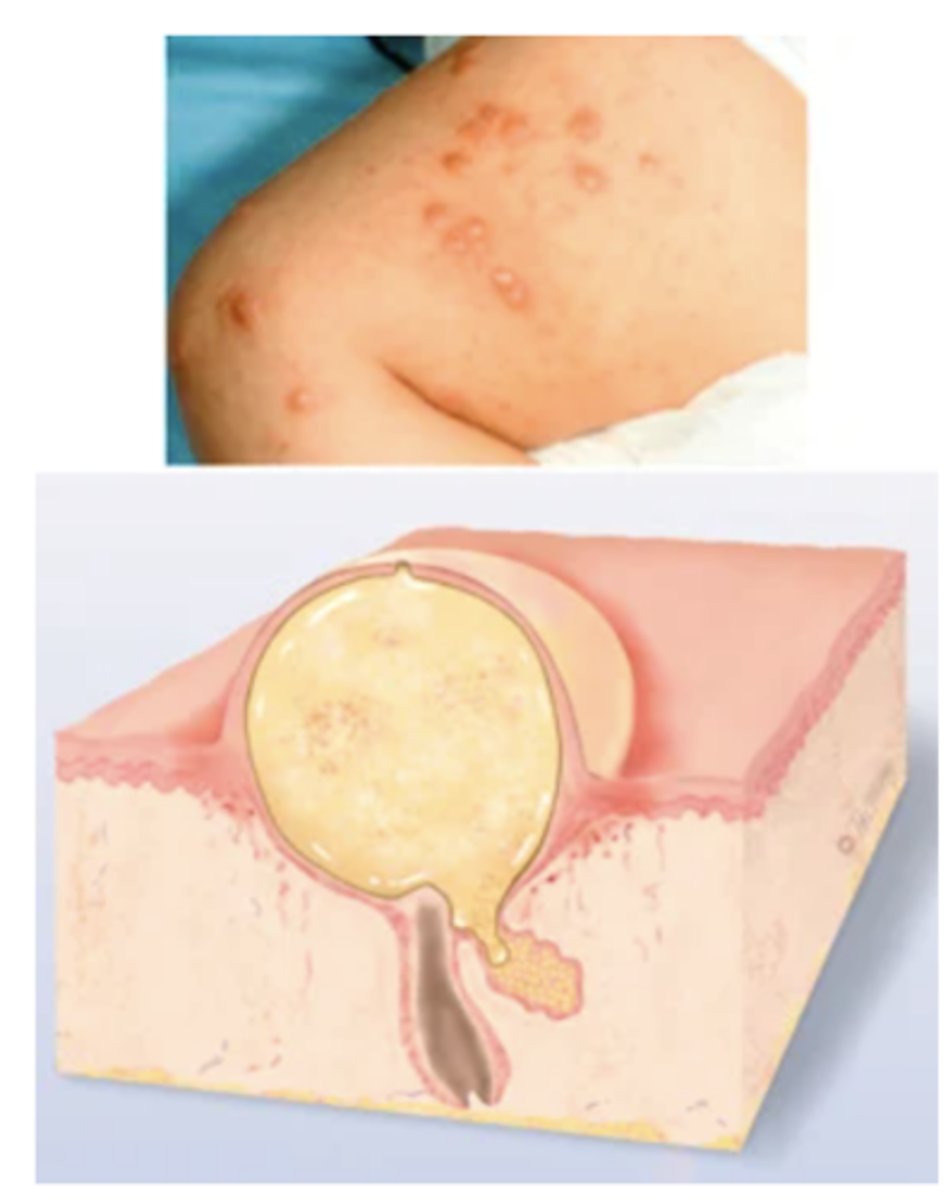
Secondary Lesions
These result from a change in a primary lesion from the passage of time; an evolutionary change.
Crust, Scale, Fissure, Erosion, Ulcer, Excoriation, Scar, Atrophic Scar, Lichenification, Keloid Note: Combinations of primary and secondary lesions may coexist in the same person. Such combined designations may be termed papulosquamous, maculopapular, vesiculopustular, or papulovesicular.
Crust
The thickened, dried-out exudate left when vesicles/pustules burst or dry up. Color can be red-brown, honey, or yellow, depending on fluid ingredients (blood, serum, pus). Examples: impetigo (dry, honey-colored), weeping eczematous dermatitis, scab after abrasion.
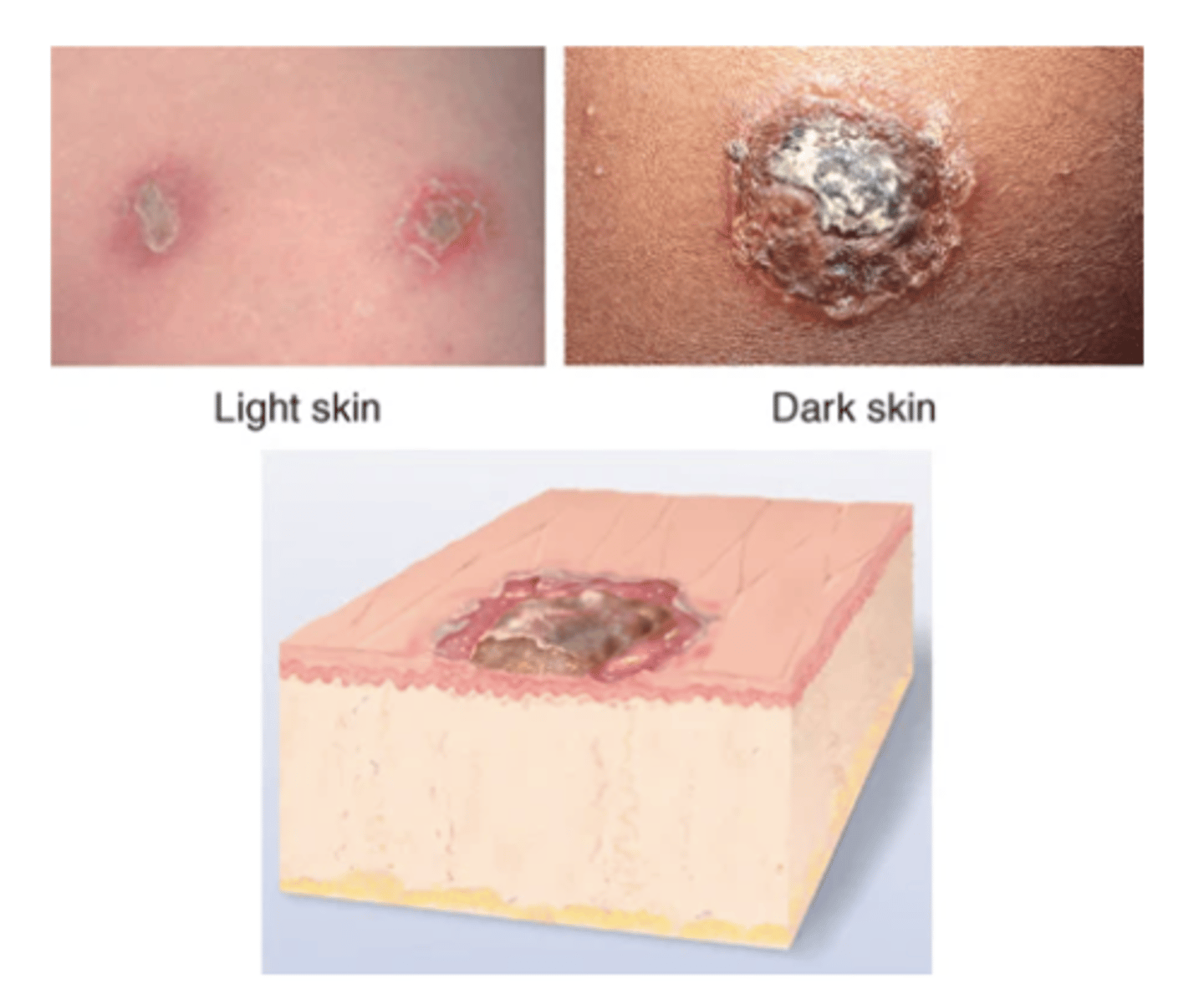
Scale
Compact, desiccated flakes of skin, dry or greasy, silvery or white, from shedding of dead excess keratin cells. Examples: after scarlet fever or drug reaction (laminated sheets), psoriasis (silver, micalike), seborrheic dermatitis (yellow, greasy), eczema, ichthyosis (large, adherent, laminated), dry skin.
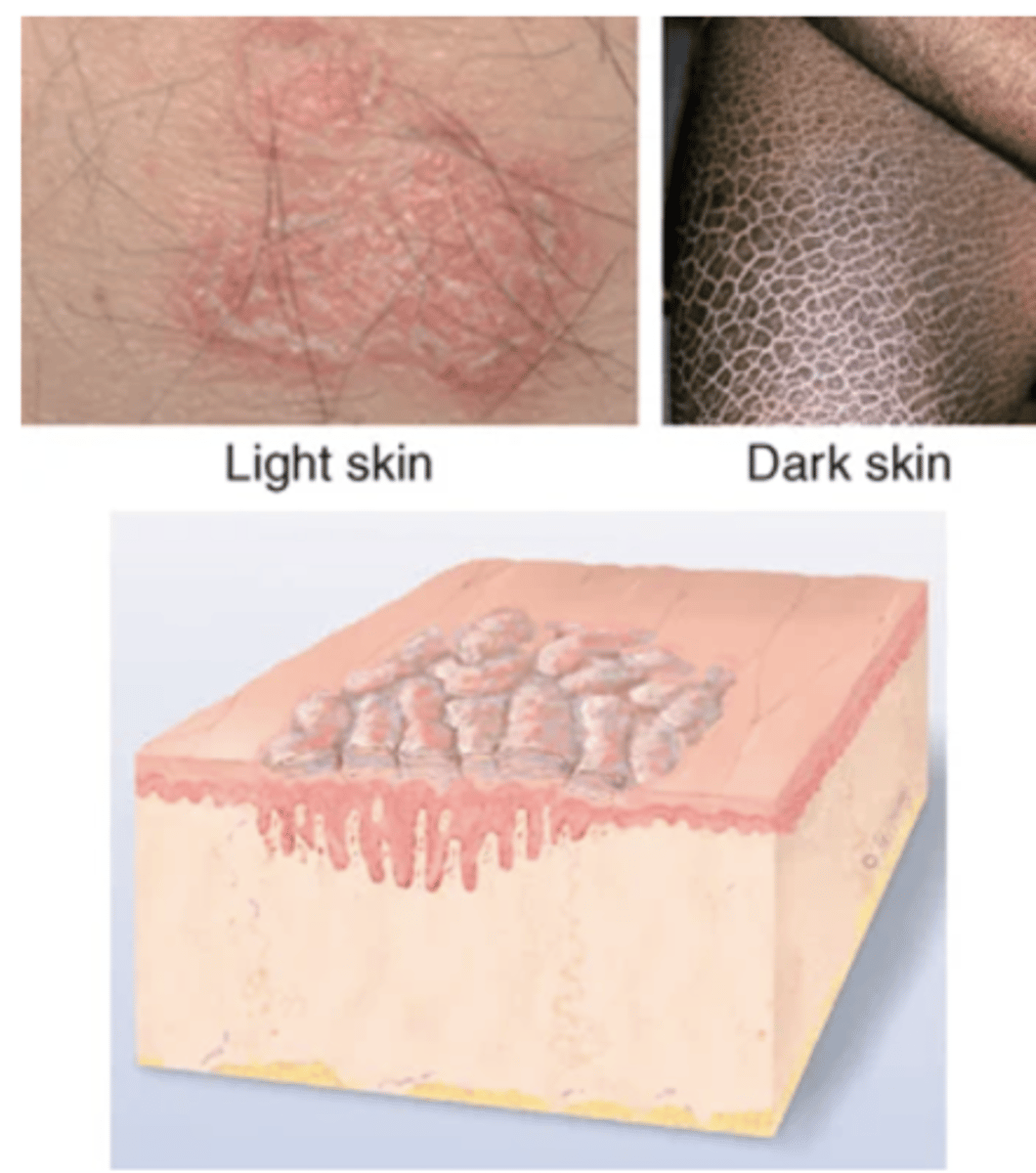
Fissure
Break in Continuity of Surface
Linear crack with abrupt edges; extends into dermis; dry or moist. Examples: cheilosis—at corners of mouth caused by excess moisture; athlete's foot.
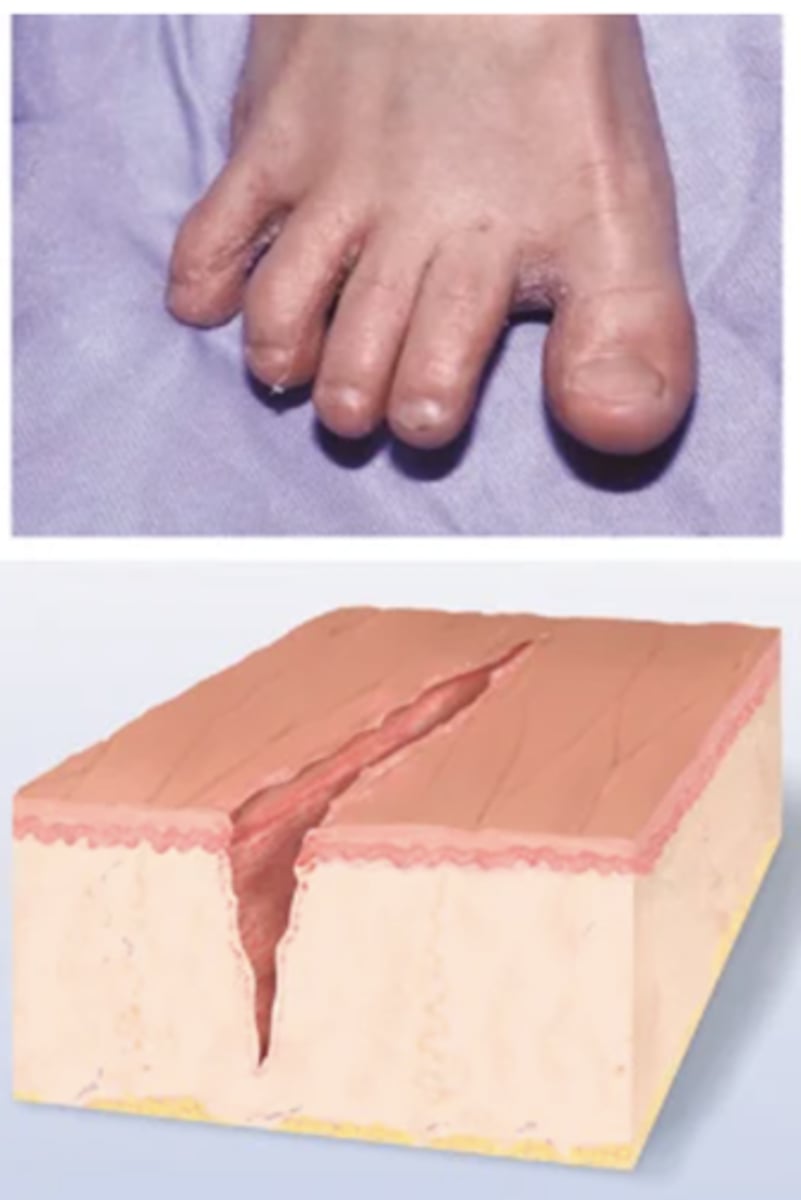
Erosion
Break in Continuity of Surface
Break in Continuity of Surface
Scooped-out but shallow depression. Superficial; epidermis lost; moist but no bleeding; heals without scar because erosion does not extend into dermis.
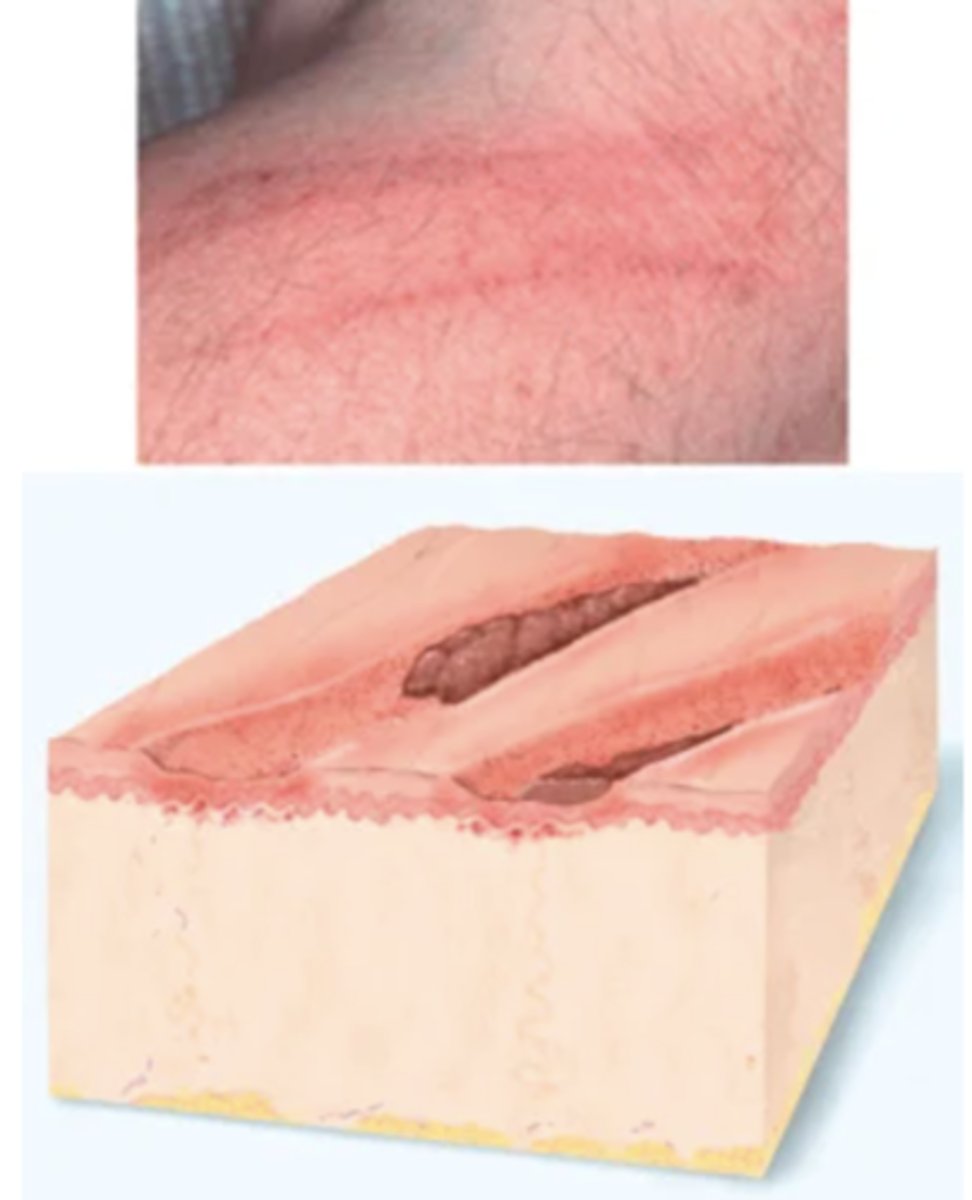
Ulcer
Deeper depression extending into dermis, irregular shape; may bleed; leaves scar when heals. Examples: stasis ulcer, pressure injury, chancre.
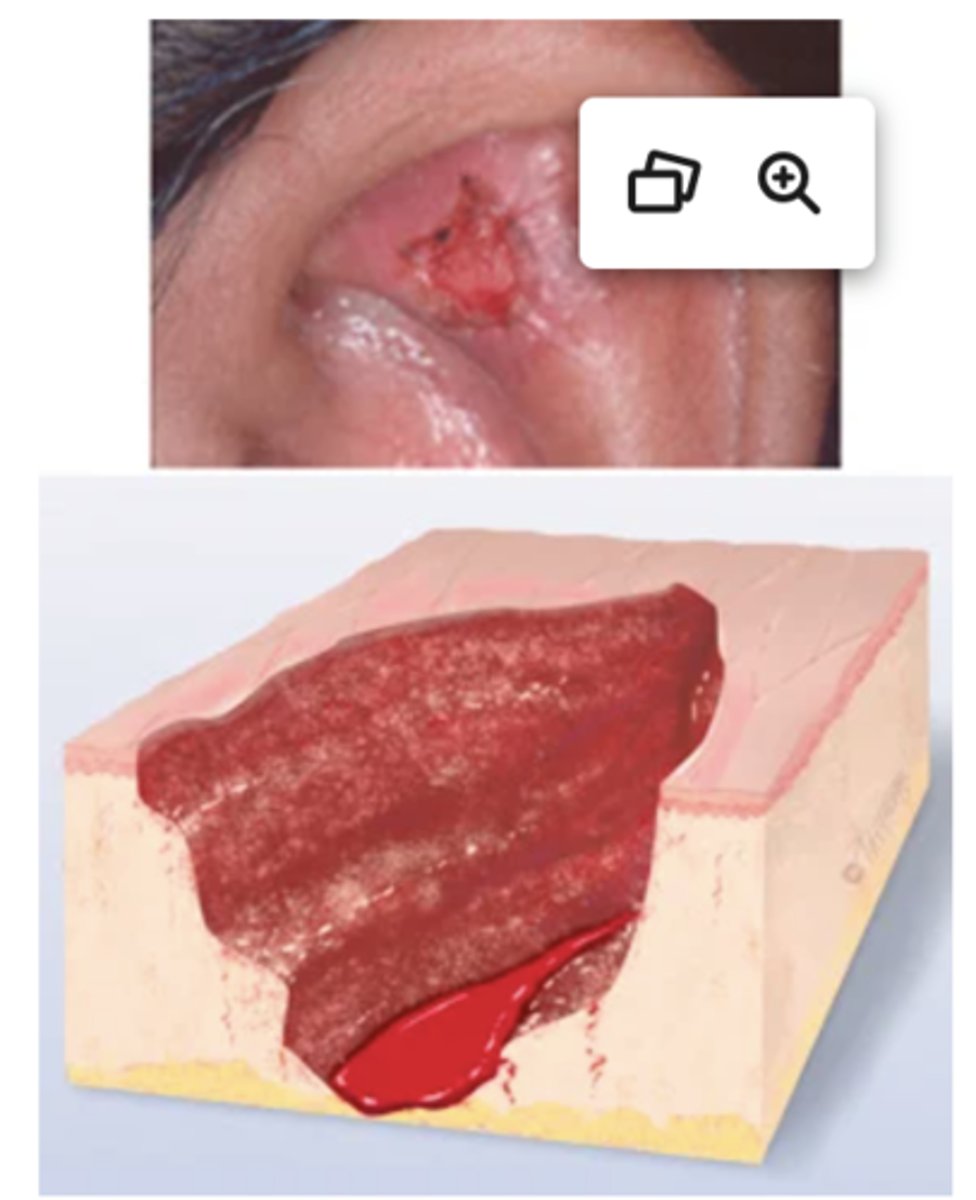
Excoriation
Self-inflicted abrasion; superficial; sometimes crusted; scratches from intense itching. Examples: insect bites, scabies, dermatitis, varicella.
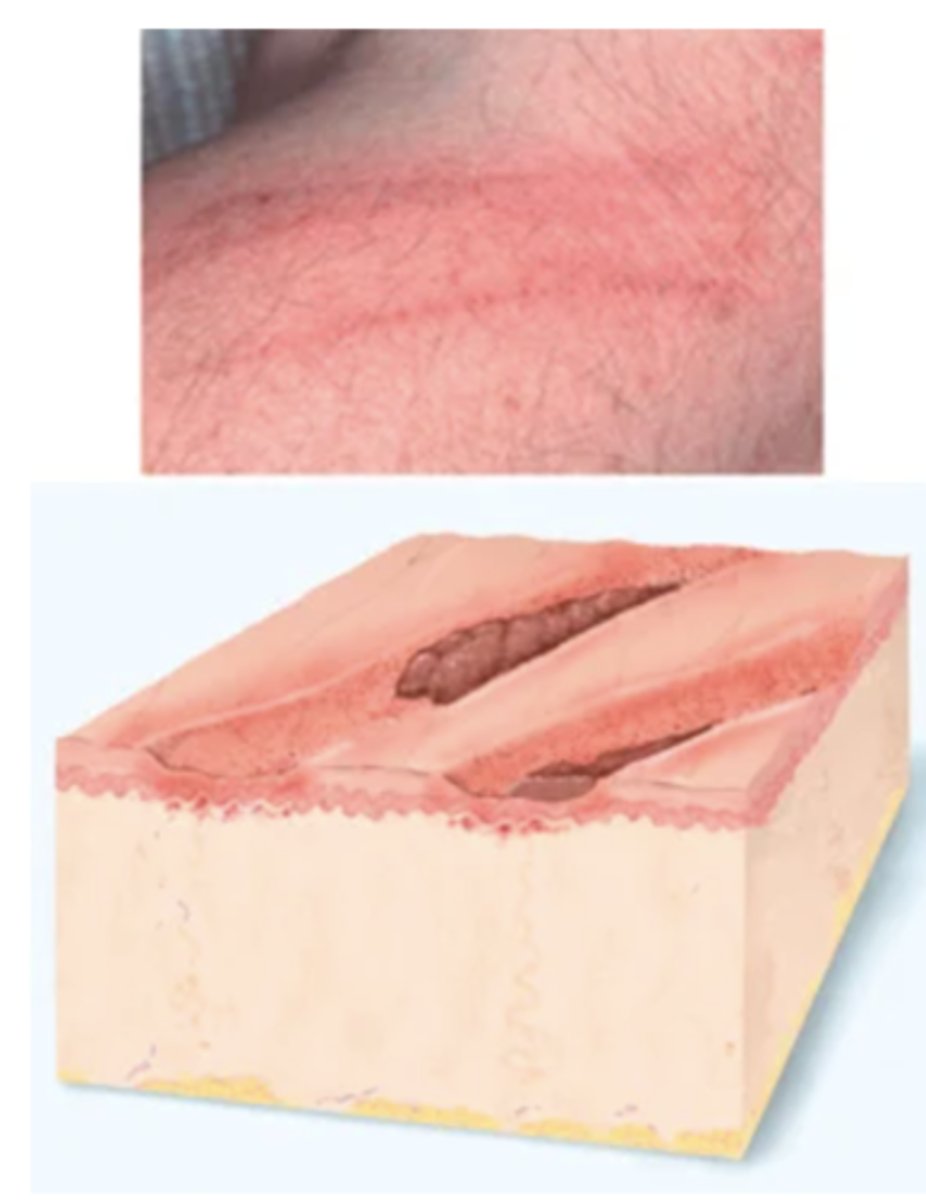
Atrophic Scar
The resulting skin level is depressed with loss of tissue; a thinning of the epidermis. Example: striae.
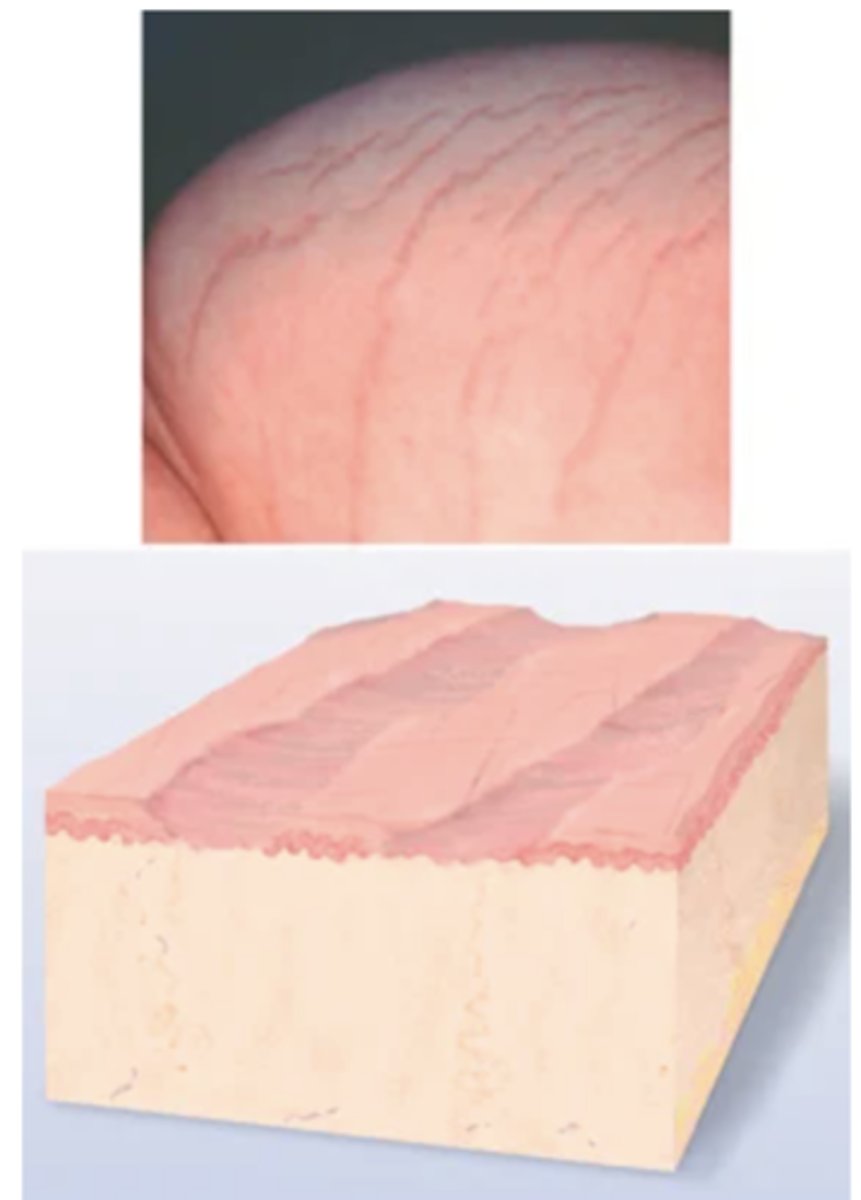
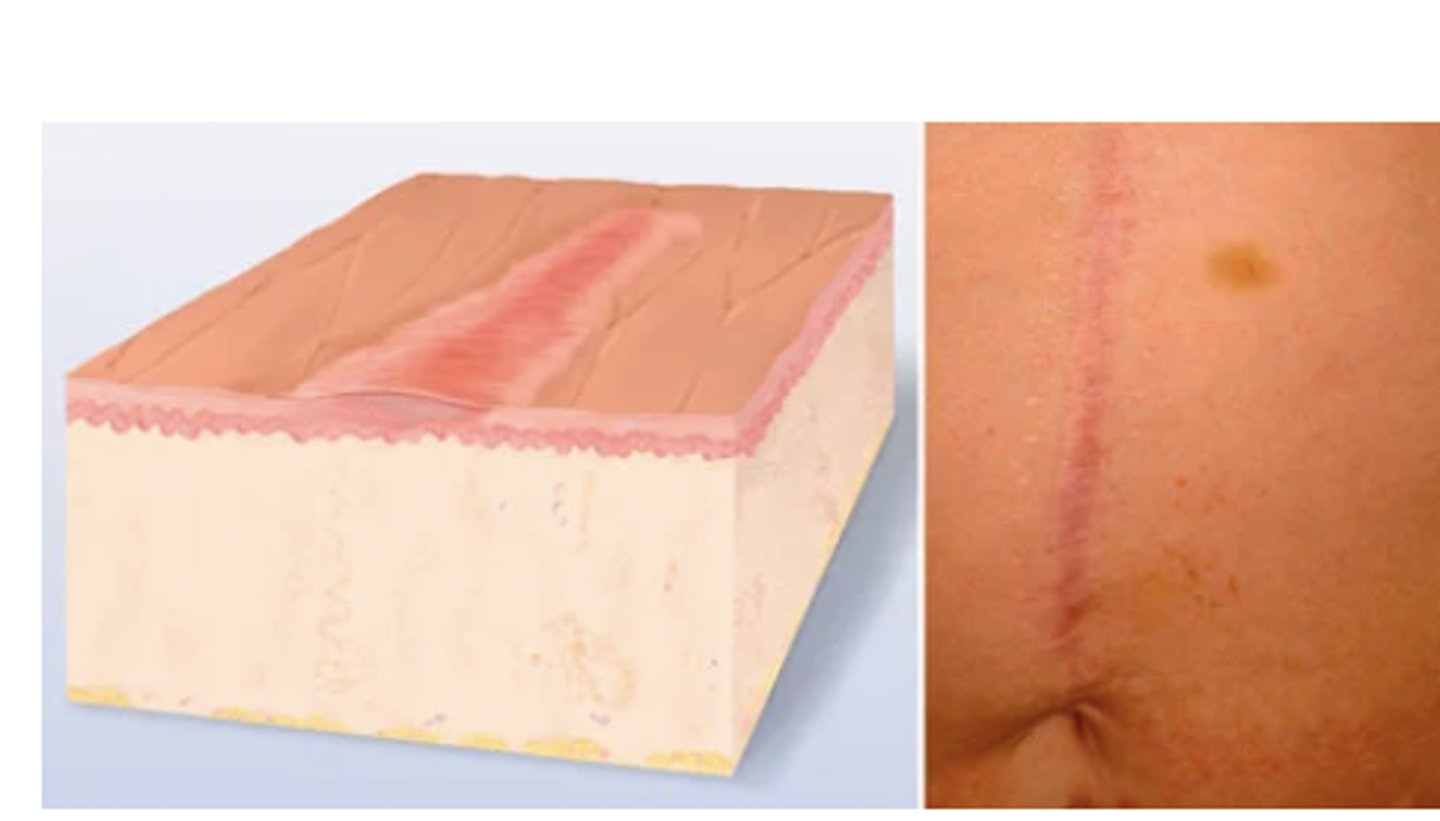
Scar
After a skin lesion is repaired, normal tissue is lost and replaced with connective tissue (collagen). This is a permanent fibrotic change. Examples: healed area of surgery or injury, acne.
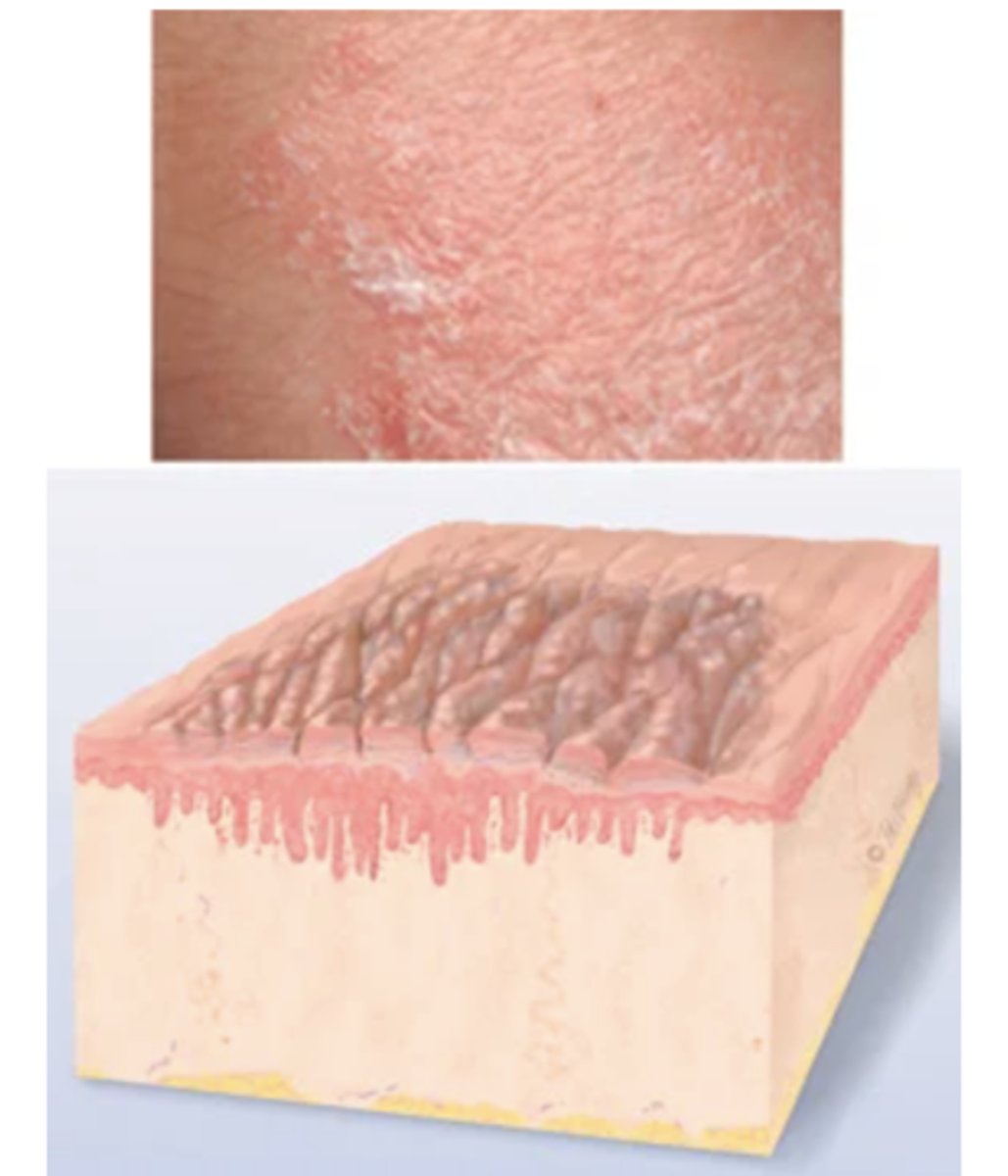
Lichenification
Prolonged, intense scratching eventually thickens skin and produces tightly packed sets of papules; looks like surface of moss (or lichen).
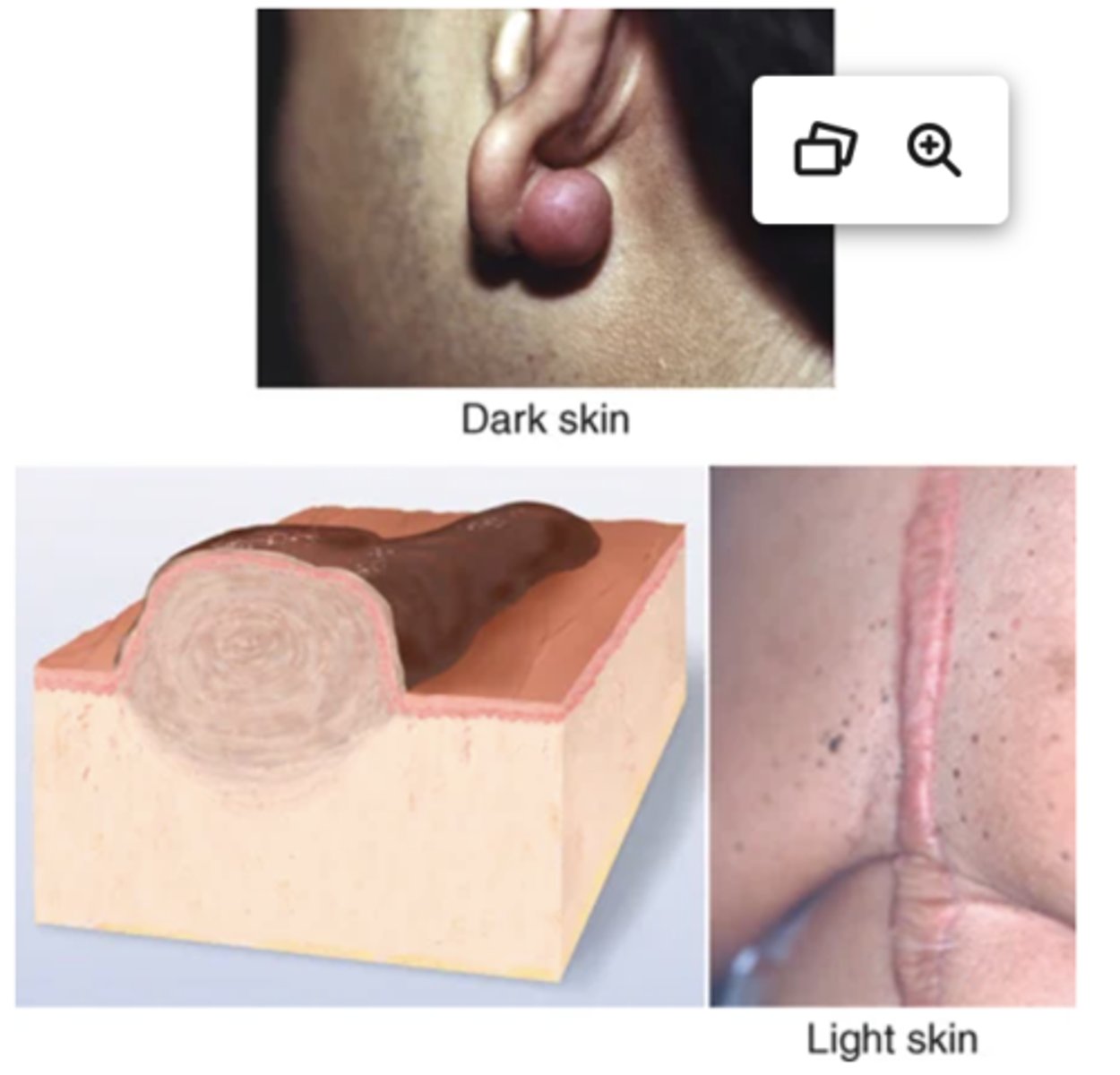
Keloid
A benign excess of scar tissue beyond sites of original injury: surgery, acne, ear piercing, tattoos, infections, burns.16 Looks smooth, rubbery, shiny, and "clawlike"; feels smooth and firm. Found in ear lobes, back of neck, scalp, chest, and back; may occur months to years after initial trauma. Most common ages are 10-30 years; higher incidence in Black, Latino, and Asian people.
Vascular Lesions
Purpura, Petechiae, Contusion, Ecchymosis, Hemangioma
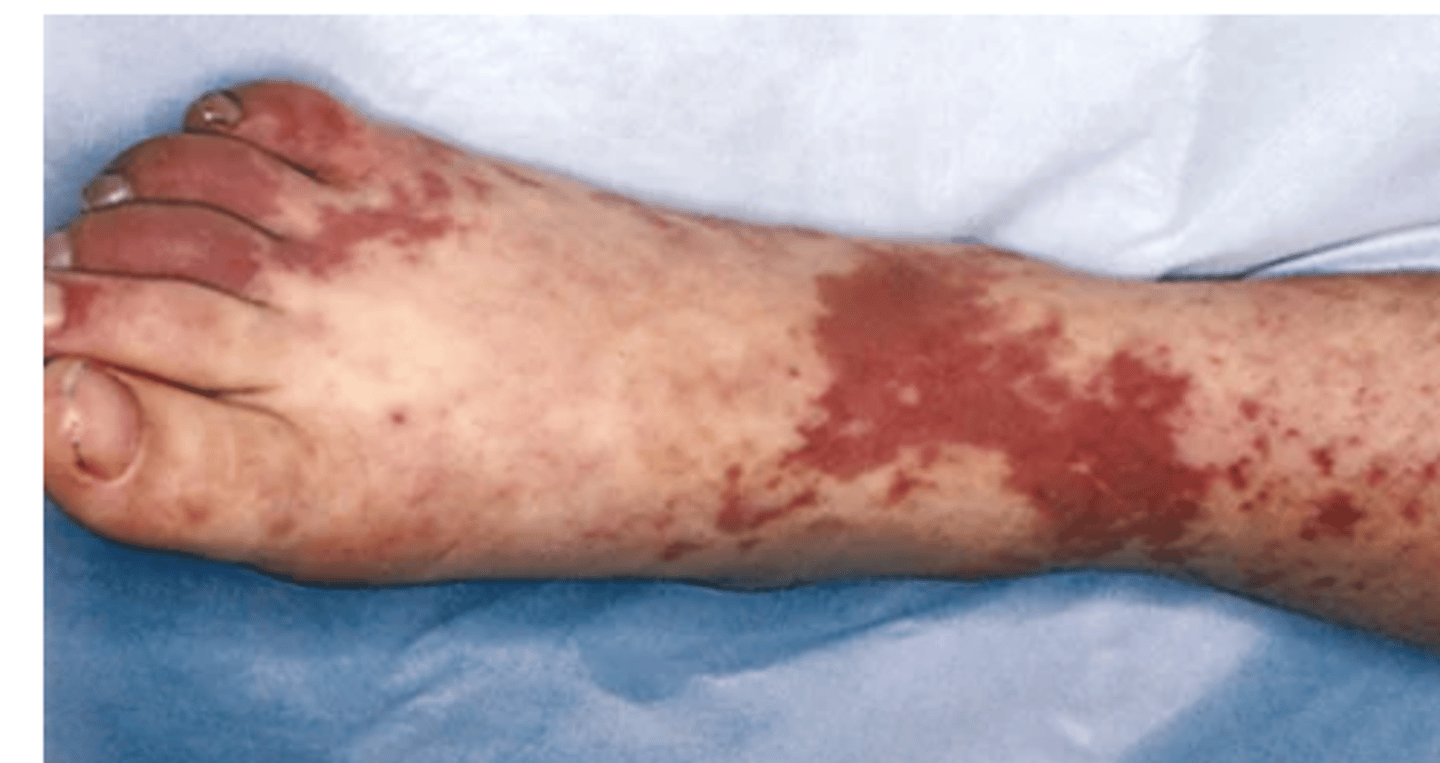
Purpura
Confluent and extensive patch of petechiae and ecchymoses; >3 mm, flat, red to purple, macular hemorrhage. Seen in generalized disorders such as thrombocytopenia, coagulation disorders, and scurvy. Also occurs in old age as blood leaks from capillaries in response to minor trauma and diffuses through dermis.
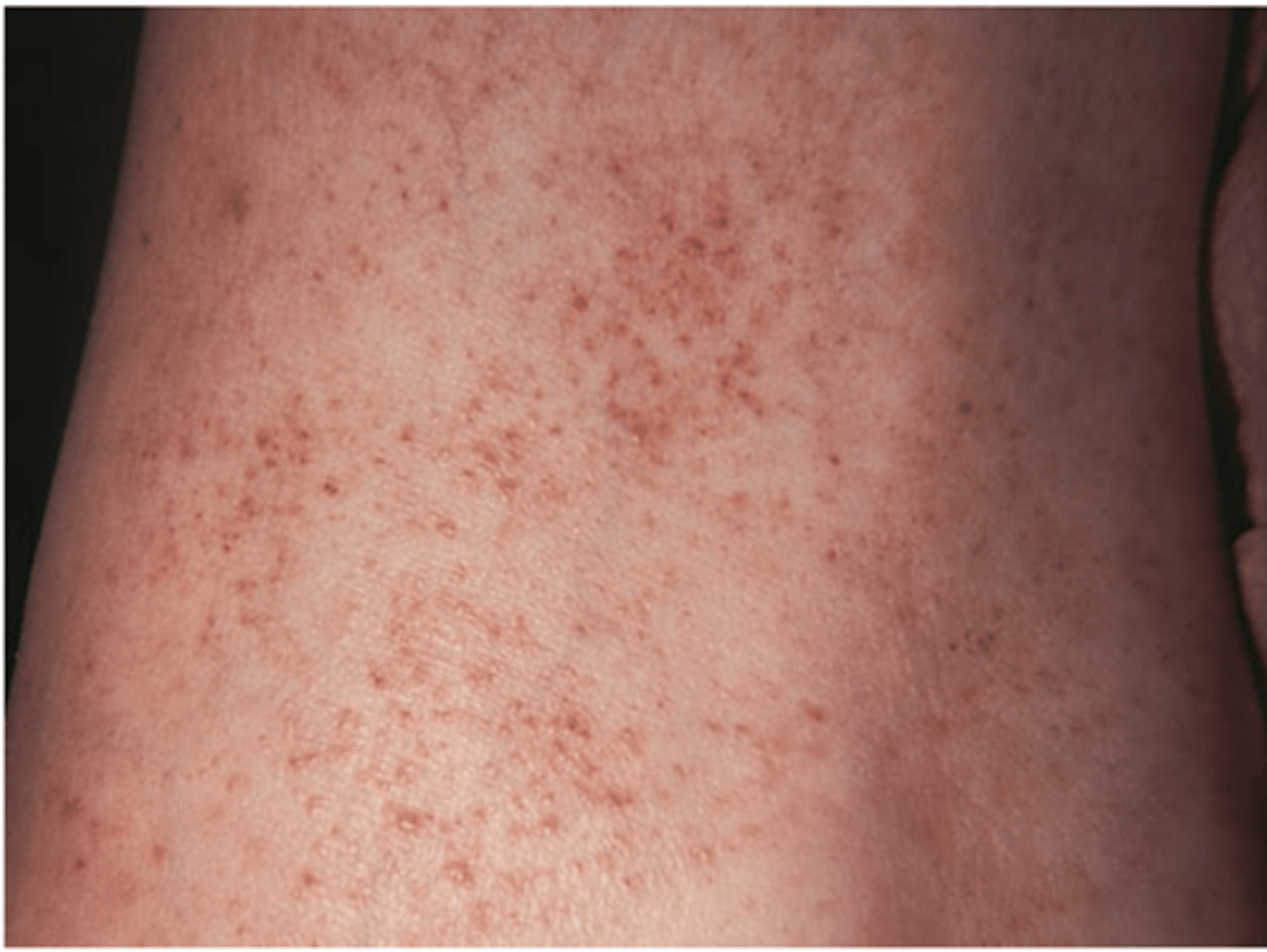
Petechiae
1-3 mm tiny, pinpoint, round hemorrhages, tiny flat blood spots ranging in color-red, purple, or brown (abnormal clotting, sepsis) Caused by bleeding from superficial capillaries; will not blanch
In dark-skinned people petechiae are best visualized in the areas of lighter melanization (e.g., the abdomen, buttocks, and volar surface of the forearm), but when the skin is very dark, petechiae cannot be seen.
Most of the diseases that cause bleeding and microembolism formation, such as thrombocytopenia, subacute bacterial endocarditis, and other septicemias, are characterized by petechiae in the mucous membranes and on the skin. Thus you should inspect for petechiae in the mouth, particularly the buccal mucosa, and in the conjunctivae.
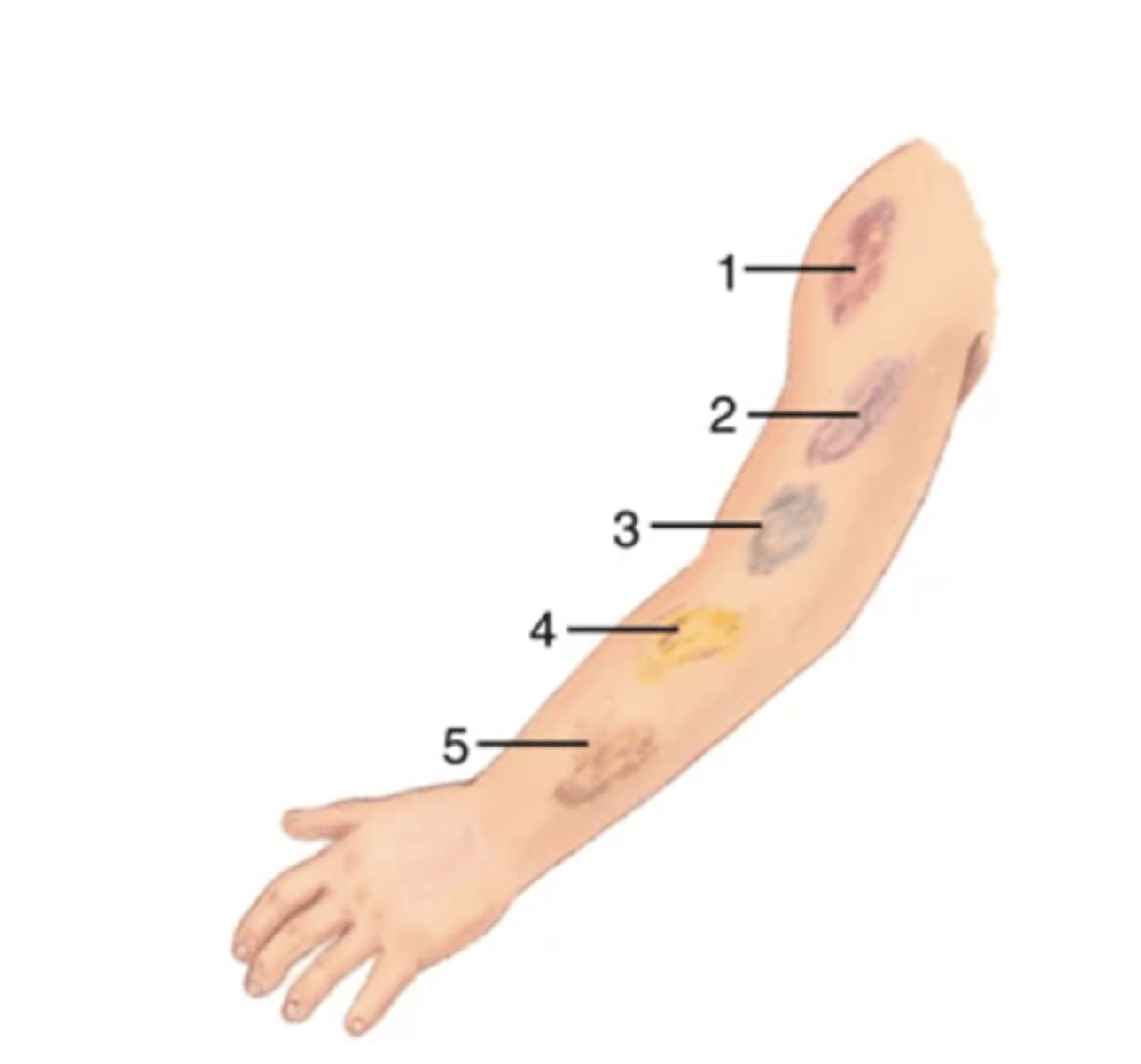
Contusion (Bruise)
A mechanical injury (e.g., a blow) results in hemorrhage into tissues. Skin is intact. Color in a light-skinned person is usually (1) red-blue or purple immediately after or within 24 hours of trauma and generally progresses to (2) blue to purple, (3) blue-green, (4) yellow, and (5) brown to disappearing. A recent bruise in a dark-skinned person is deep, dark purple. Note that it is not possible to date the age of a bruise from its color. Pressure on a bruise will not cause it to blanch. A bruise usually occurs from trauma but can also result from bleeding disorders and liver dysfunction.
NOTE: A bruise is different from petechiae, ecchymosis, and purpura because these 3 are not caused by blunt force trauma.
Ecchymosis
A purplish patch resulting from extravasation of blood into the skin, >3 mm in diameter.
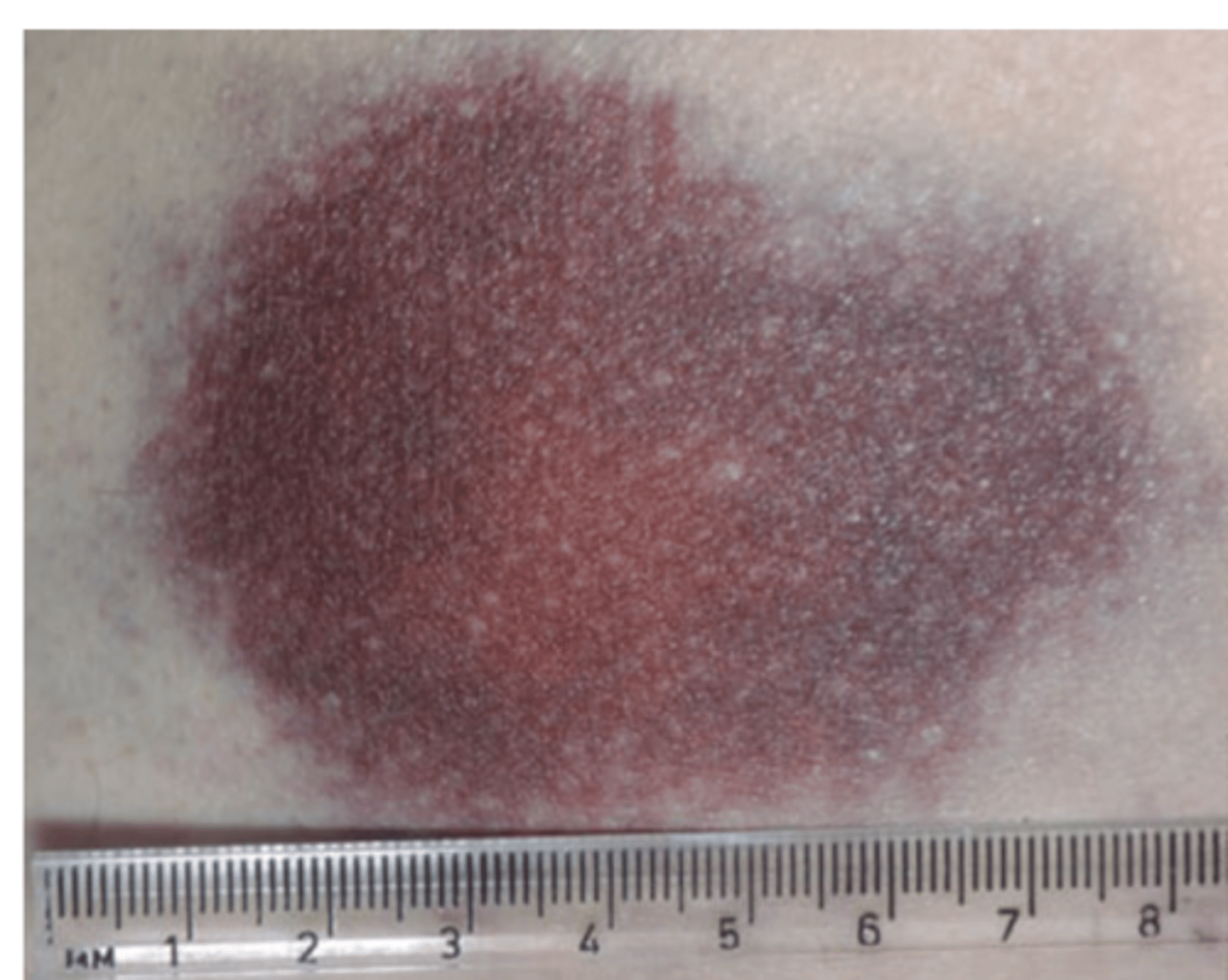
Hemangiomas
Caused by a benign proliferation of blood vessels in the dermis.
Malignant Skin Lesions
The link between ultraviolet (UV) radiation and skin cancer is well known; the UV radiation in sunlight and indoor tanning beds promotes all three forms of skin cancer shown below. More than half a person's lifetime sun damage occurs before adulthood.
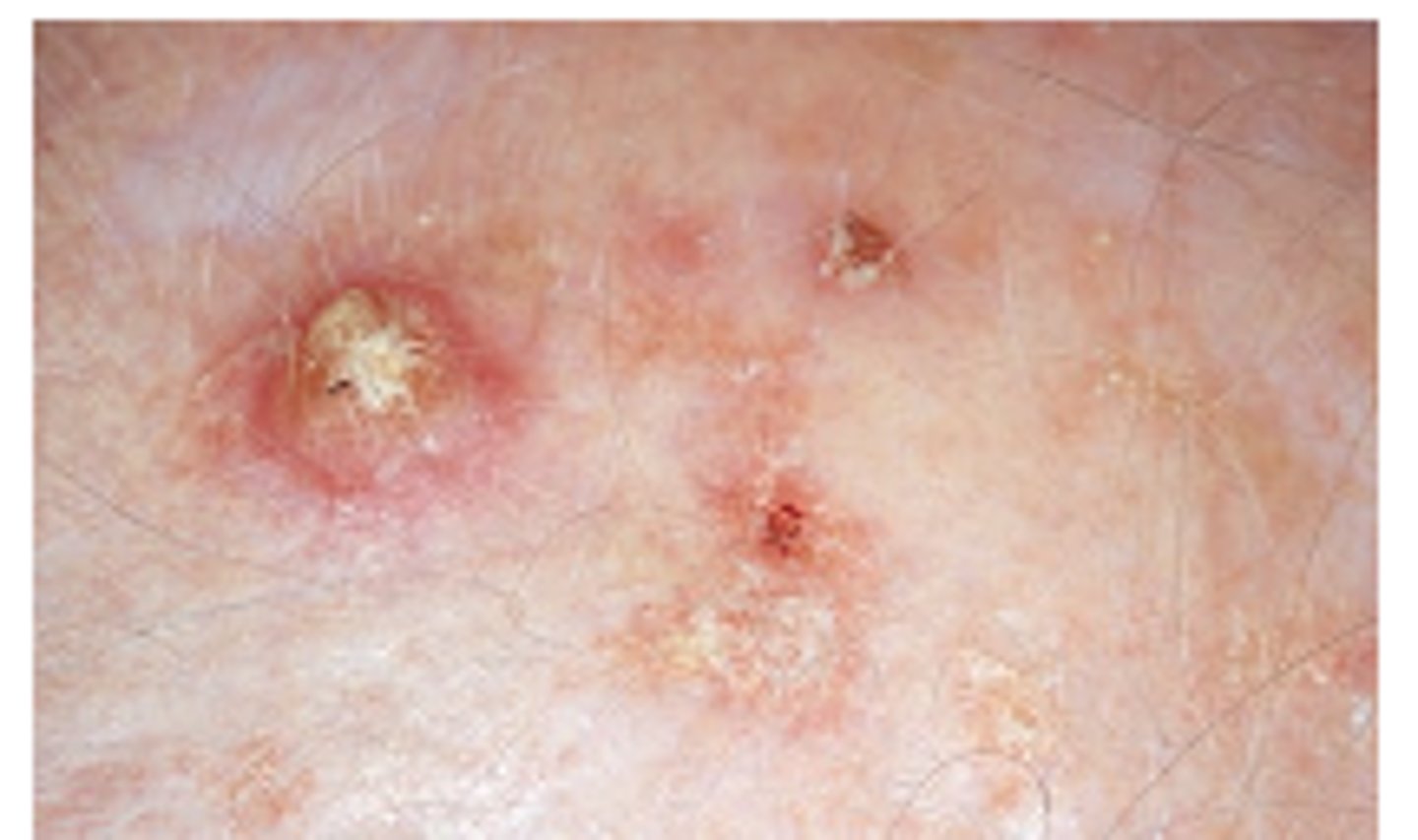
Basal Cell Carcinoma
small pink or red papule with pearlytranslucent top and broken blood vessel at center thendevelops rounded, pearly boarders with central red ulcer orlarge open pore with central yellowing- slow growing
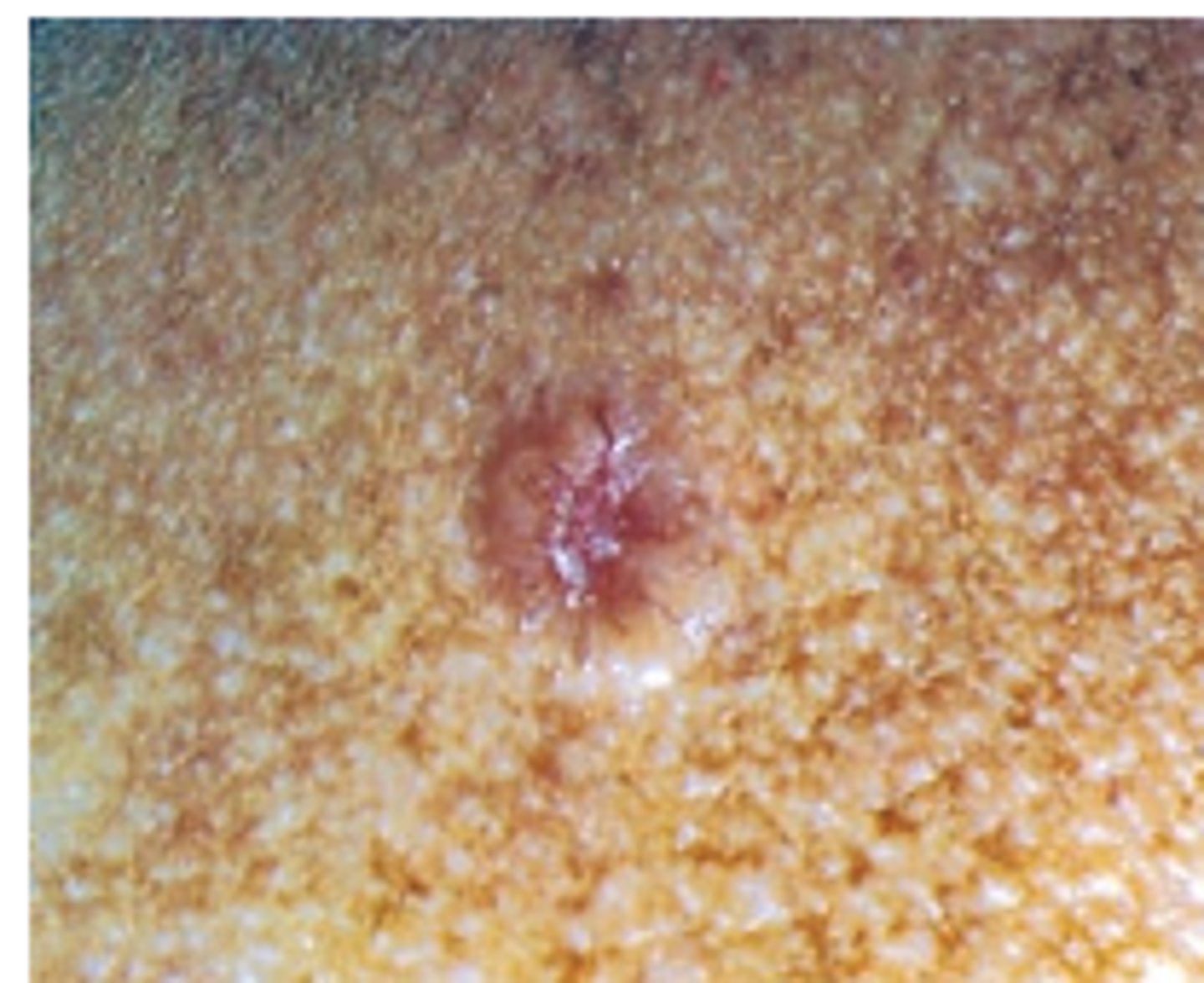
Squamous Cell Carcinoma
arises from actinic keratoses ordenovo. Erythematous scaly patch with sharp margins, 1 cmor more, develops central ulcer and surrounding erythema-fast growing
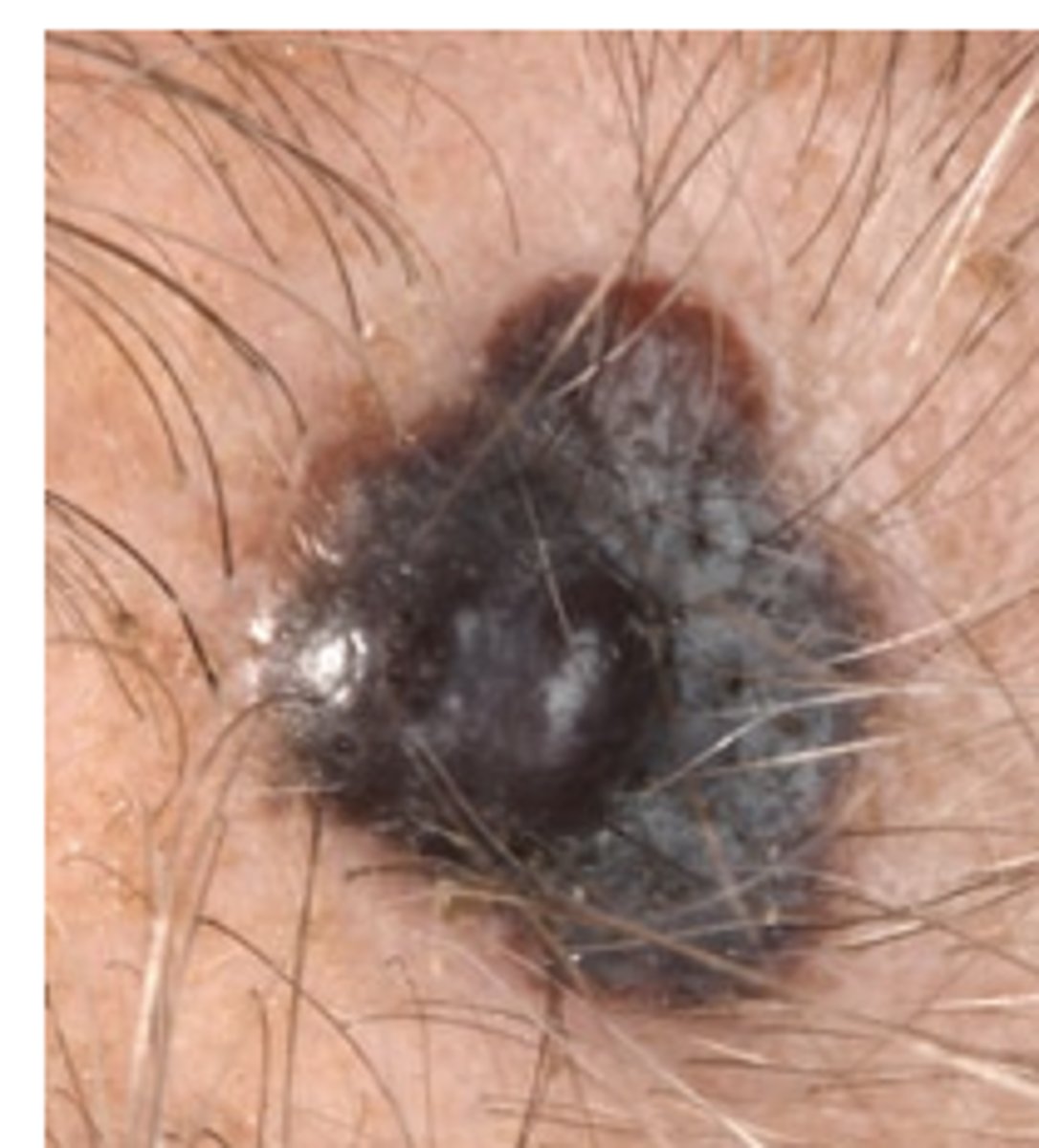
malignant melanoma-
Brown, tan, black, pink-read, purple ormixed pigmentation. Irregular boarders, scaling, flaking ,oozingMalignant Skin Lesions
The malignant transformation of melanocytes is most often cutaneous. About 80% of cutaneous melanomas arise in sun/ artificial UV-exposed regions with some risk of genetic mutations in predisposed persons.5 Usually brown; can be tan, black, pink-red, purple, or mixed pigmentation. Often irregular or notched borders. May have scaling, flaking, oozing texture. The most common type is superficial spreading melanoma (on left); it begins as a brown to black macule with irregular borders and color variation. Nodular melanoma (on right) is the next most common, with quickly growing blue, black, pink, or red nodules, possibly with ulceration or bleeding. These occur at any body site, most often the trunk, head, and neck.
Wounds
Abrasion- scrapes away superficial layers of skin caused by friction as body scrapes across a rough surface
Incision-cause by a clean, sharp-edged object scalpel, knife, razor, glass shard it has clean edges such as a surgical incision
Laceration- irregular tear-like wounds caused by blunt trauma and has jagged edges
Puncture- sharp pointed object entering skin, something passes through or is impaled
Avulsion- characterized by a flap Wounds
Wounds Assess:
1. approximation of edges
2. color,
3. edema,
4. drainage
5. exudate
6. odor
7. Pain
Classic Signs of Wound Infection
-Increased pain around the wound bed-Redness or warmth
-Fever /chills or other flu-like symptoms-Pus draining from the wound bed
-Increasing odor from the wound
-Increased firmness of skin or swelling around the wound bed
Pressure Injuries (PI) - Pressure Ulcer,Decubitus Ulcer- Deep depression extending into dermis,irregular shape; may bleed leaves scar whenheals i.e. pressure injury, stasis ulcer,chancre
PIs appear on the skin over a bony prominence when circulation is impaired, e.g., when confined to bed or immobilized. Immobilization impedes delivery of blood carrying oxygen and nutrients to the skin, and it impedes venous drainage carrying metabolic wastes away from the skin. This results in ischemia and cell death. Common sites for PIs are on the back (heel, ischium, sacrum, elbow, scapula, vertebra) or the side (ankle, knee, hip, rib, shoulder).
Stages
Stage I: Non-blanchable erythema
Stage II: Partial-thickness skin loss
Stage III: Full-thickness skin loss
Stage IV: Full-thickness skin/tissue lossPressure
Stage Unstageable
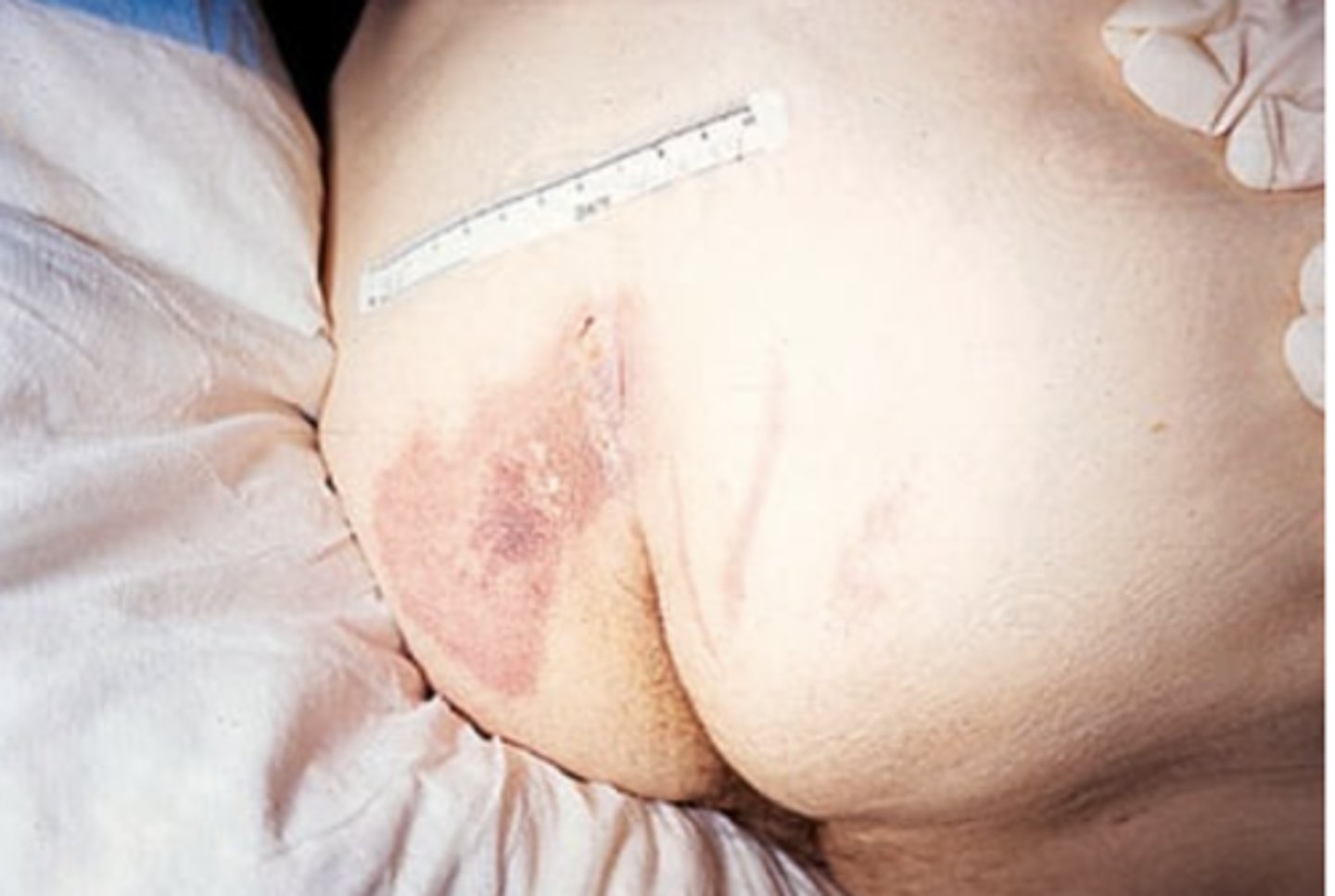
Stage I: Non-blanchable erythema
Intact skin is red but unbroken. Localized redness in lightly pigmented skin does not blanch (turn light with fingertip pressure). Dark skin appears darker but does not blanch. May have changes in sensation, temperature, or firmness.
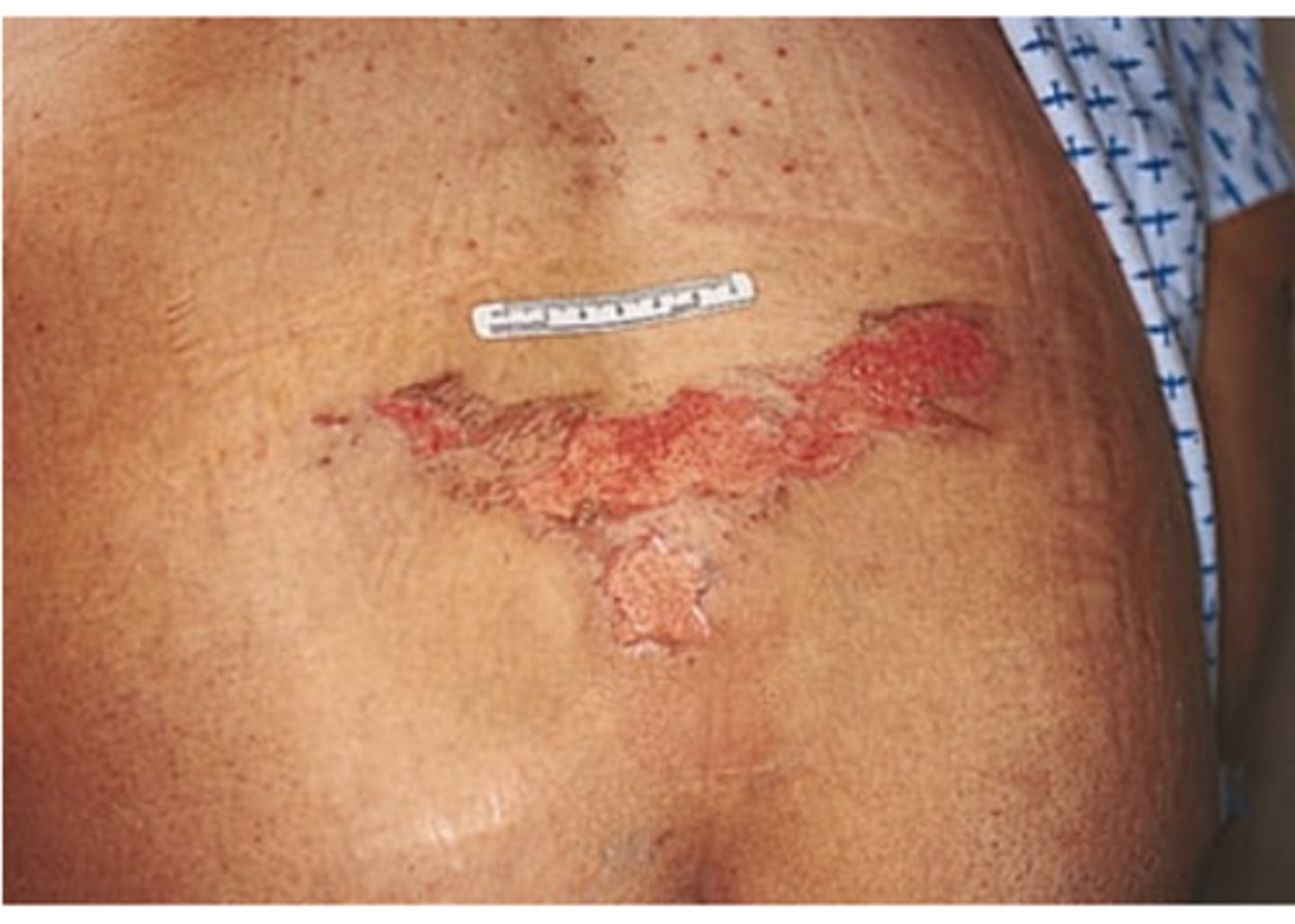
Stage 2—Partial-Thickness Skin Loss
Loss of epidermis and exposed dermis. Superficial ulcer looks shallow like an abrasion or open blister with a red-pink wound bed. No visible fat or deeper tissue.
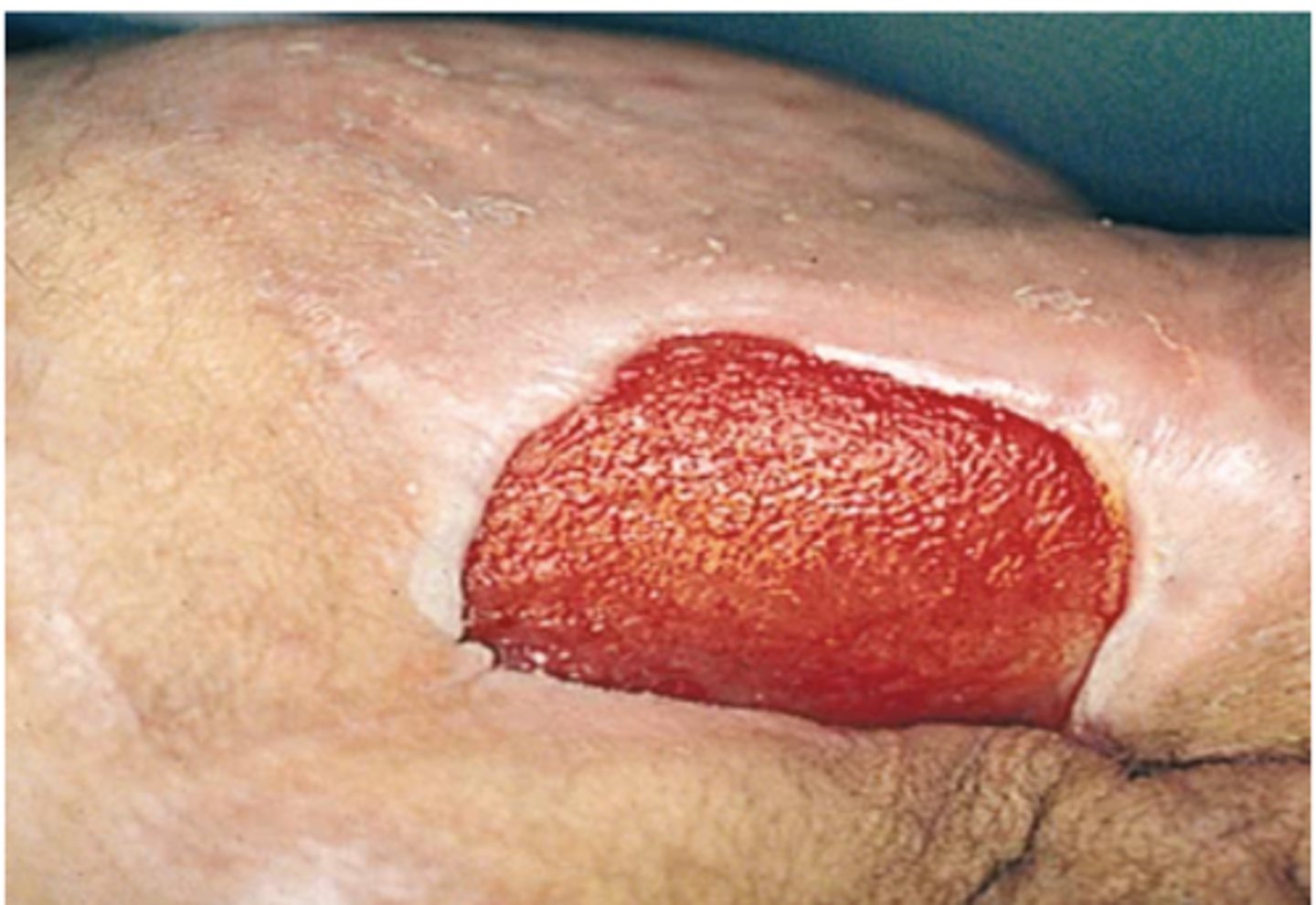
Stage 3—Full-Thickness Skin Loss
PI extends into subcutaneous tissue and resembles a crater. See subcutaneous fat, granulation tissue, and rolled edges, but not muscle, bone, or tendon.
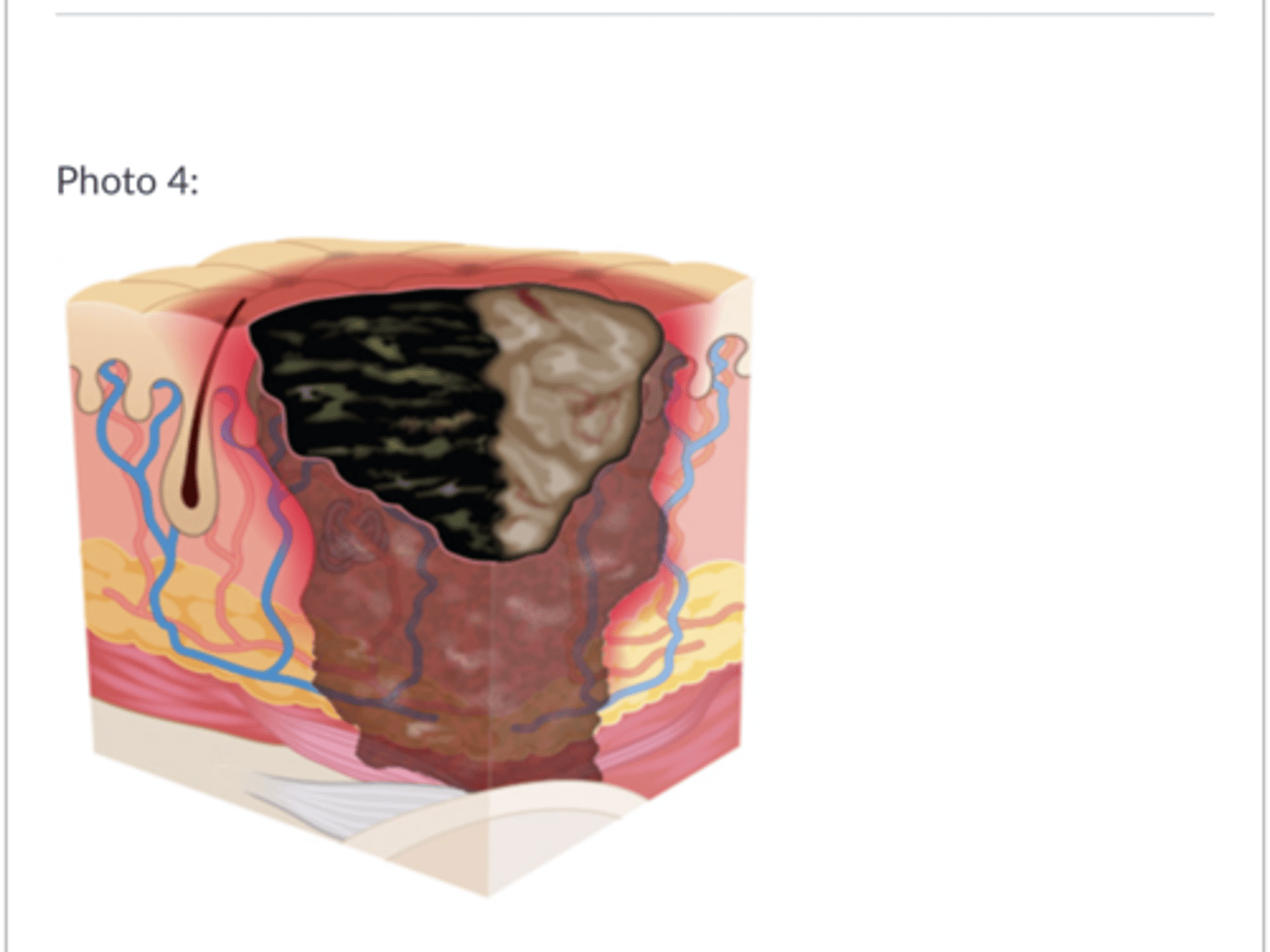
Stage 4—Full-Thickness Skin/Tissue Loss
PI involves all skin layers and extends into supporting tissue. Exposes muscle, tendon, or bone, and may show slough (stringy matter attached to wound bed) or eschar (black or brown necrotic tissue), rolled edges, and tunneling.
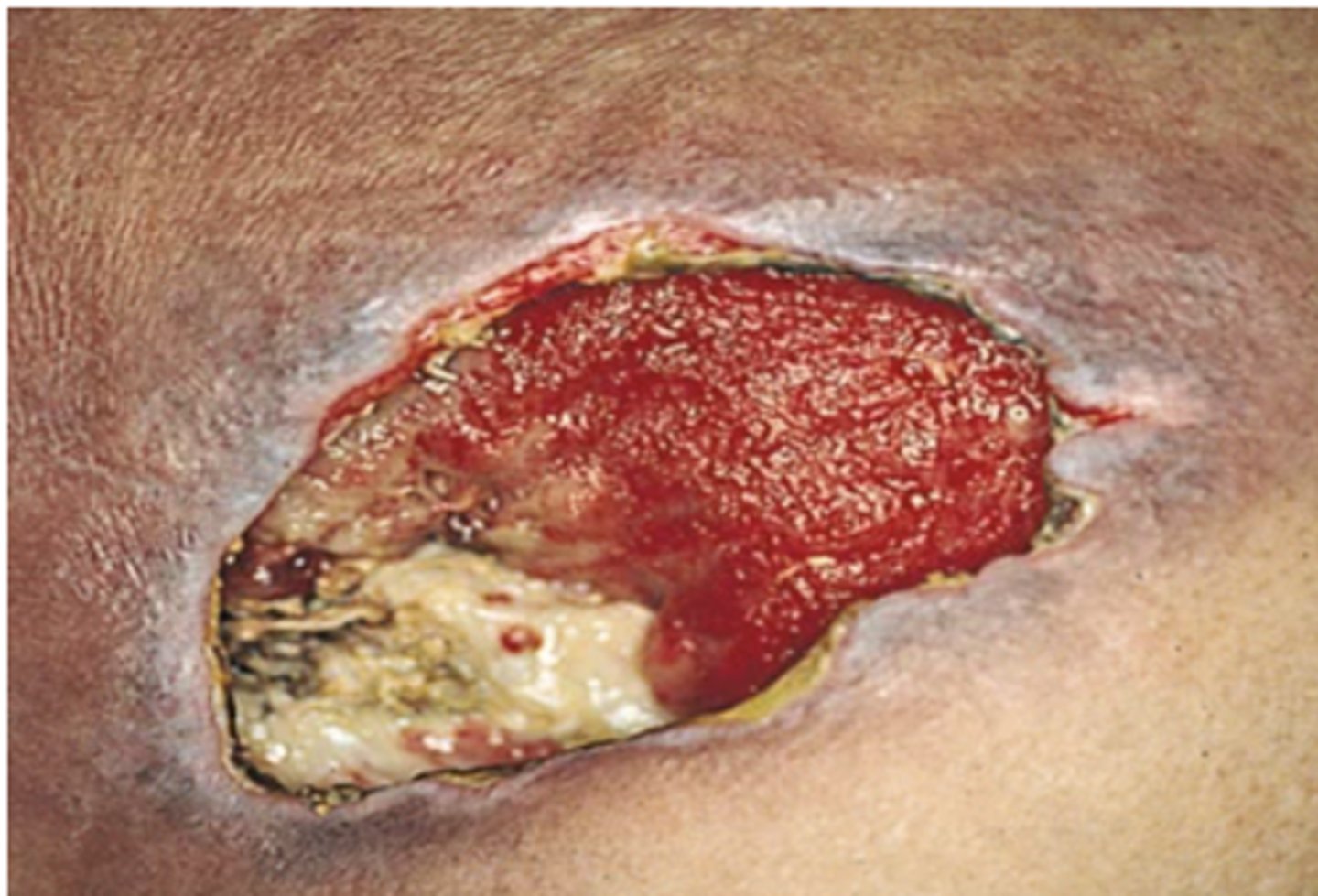
Non Cancerous Findings
- seborrheic keratosis
- Actinic keratosis
- Senile lentigines (lentigo)
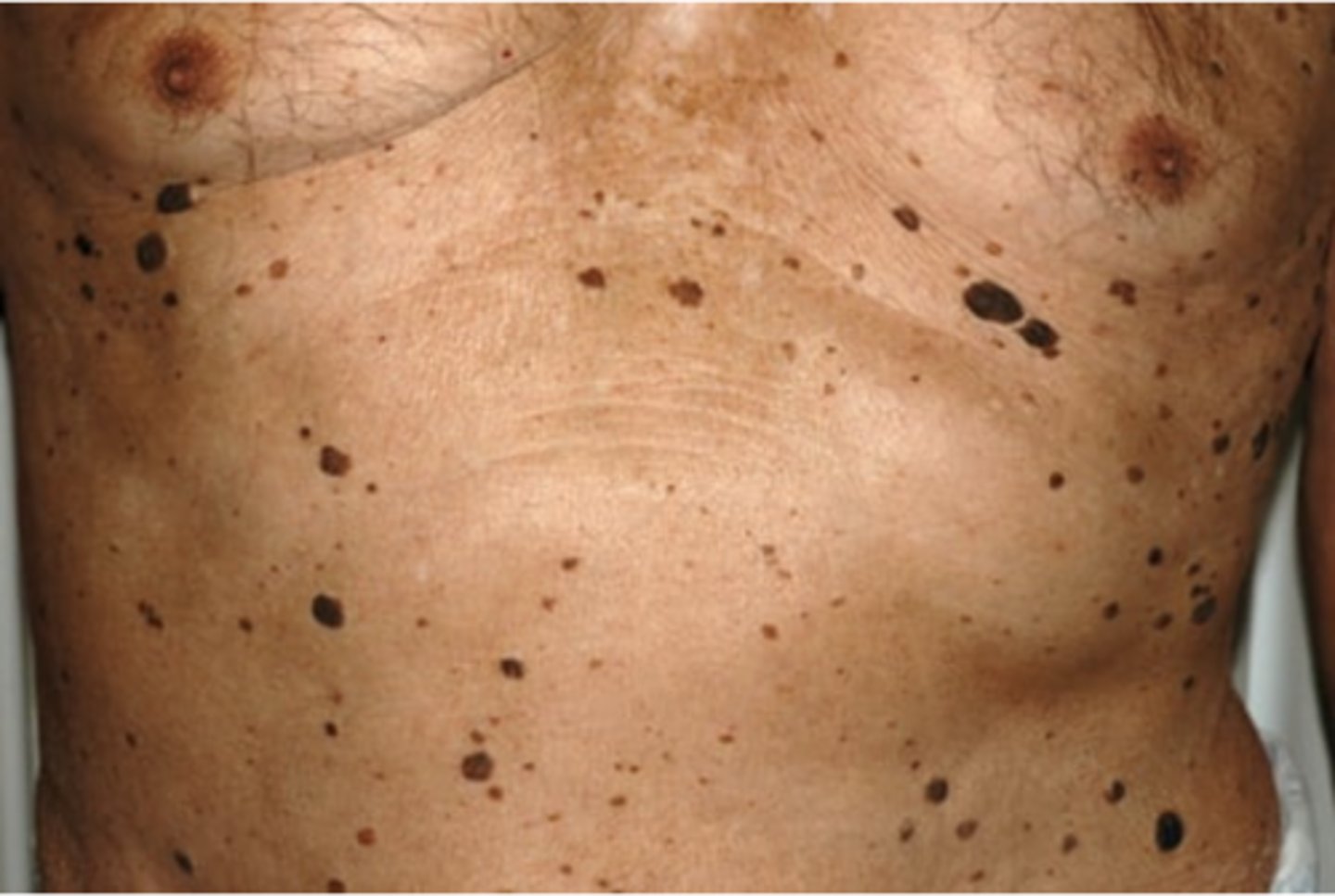
seborrheic keratosis
dark, greasy and "stuck on" Developmostly on trunk, hands and face on both unexposed and sunexposed areas. Do not become cancerous
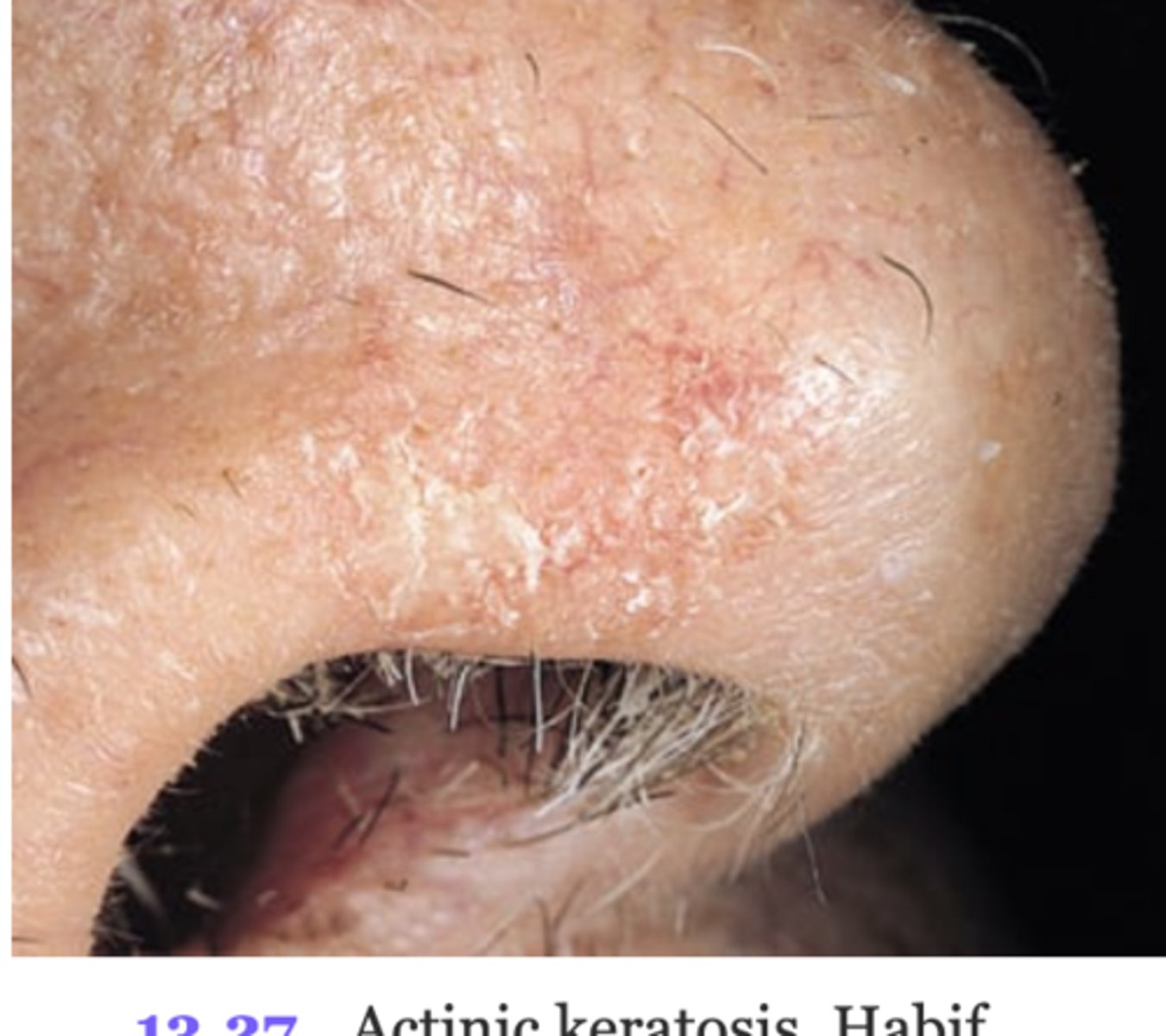
Actinic keratosis
red-tan scaly plaques, raised roughened.May have silvery white scale adherent to plaque. Occurs onsun-exposed surfaces and are directly related to sunexposure. Premalignant and may develop into squamouscell carcinoma.
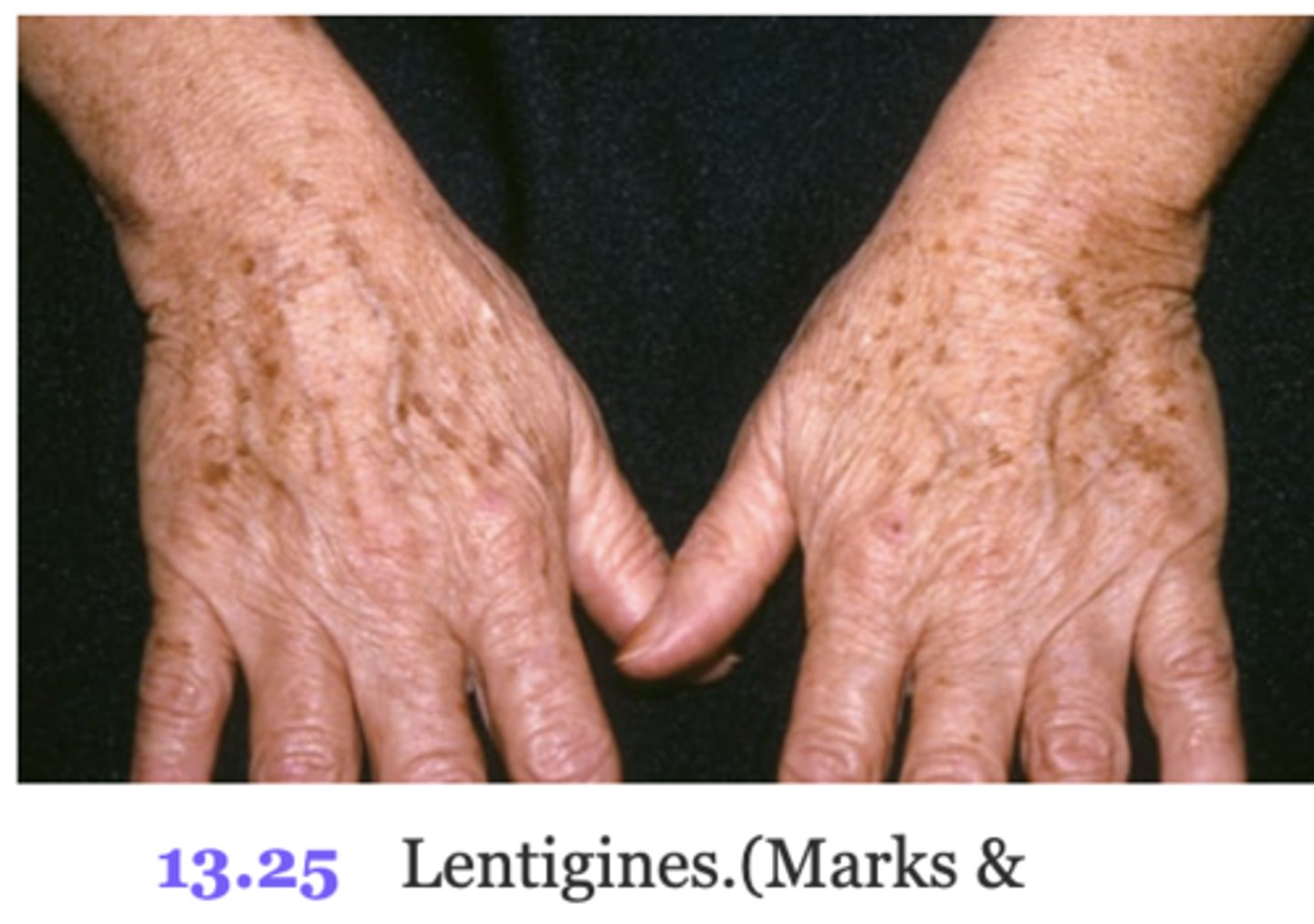
Senile lentigines (lentigo)
common variation of hyperpigmentation, liver spots, flat brown macules, extensive sun exposure and are not malignant and do not require trmt.
Chronic Arterial Ischemia
(Limb Skin Changes) Subjective and Objective Findings:

Chronic Venous Insufficiency
(Limb Skin Changes) Subjective and Objective Findings:

Chronic Venous Insufficiency
Ulcers associated w/ CVI
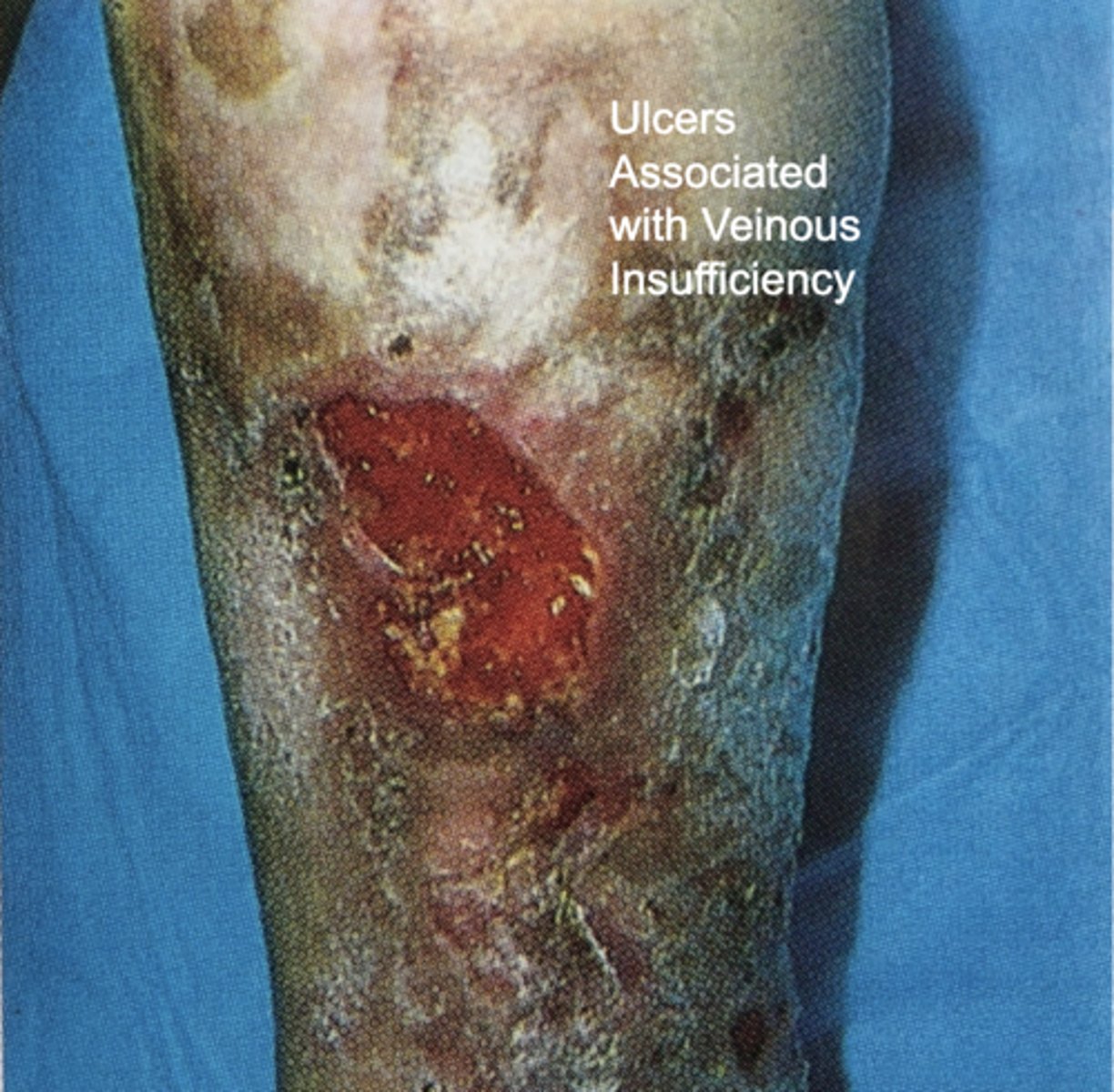
Shapes and Configurations of Lesions (select all)
Confluent
Discrete
Grouped
Linear
Zosteriform
ALL
Confluent
Lesions run together
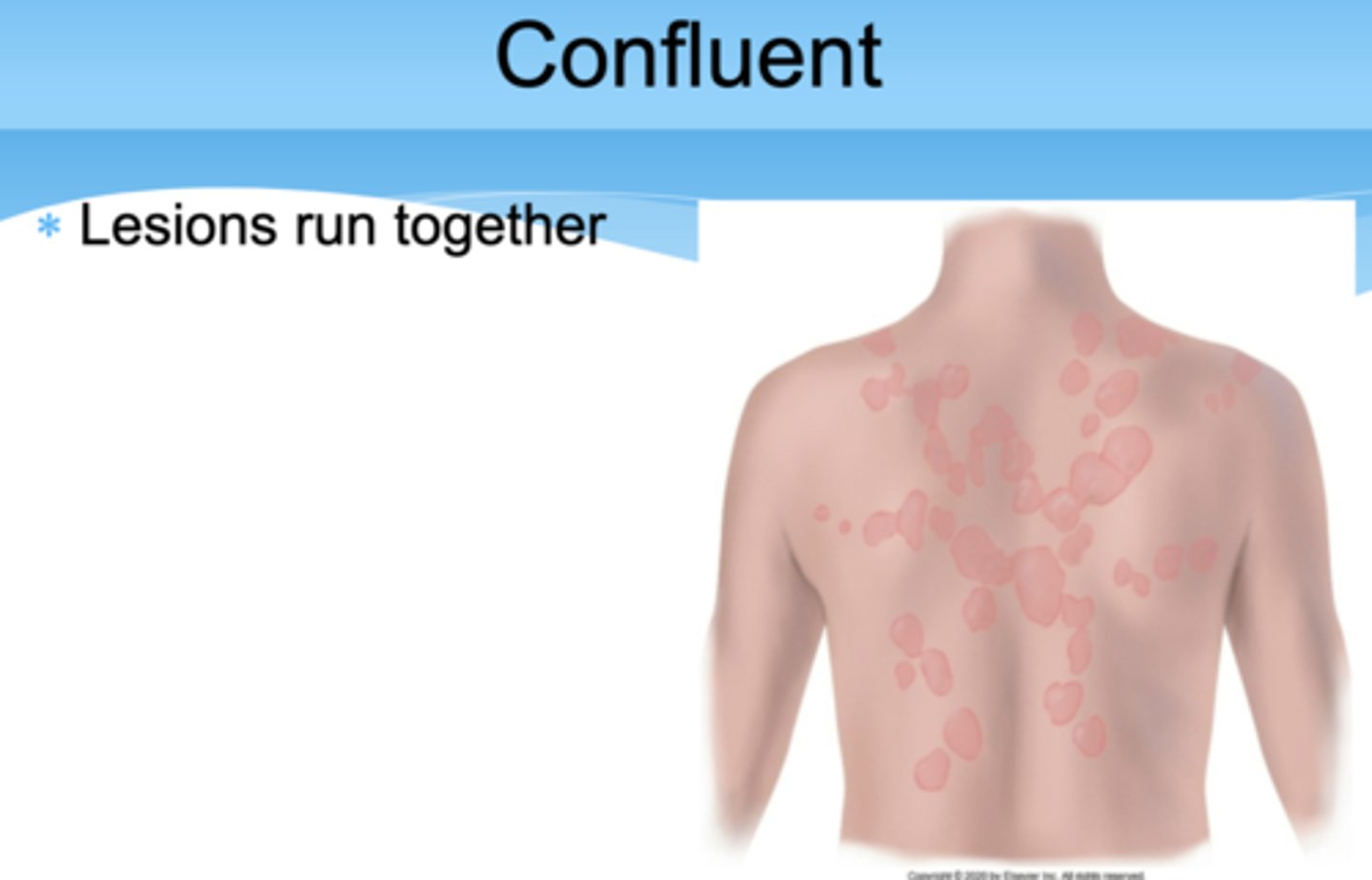
Discrete
Distinct and separate
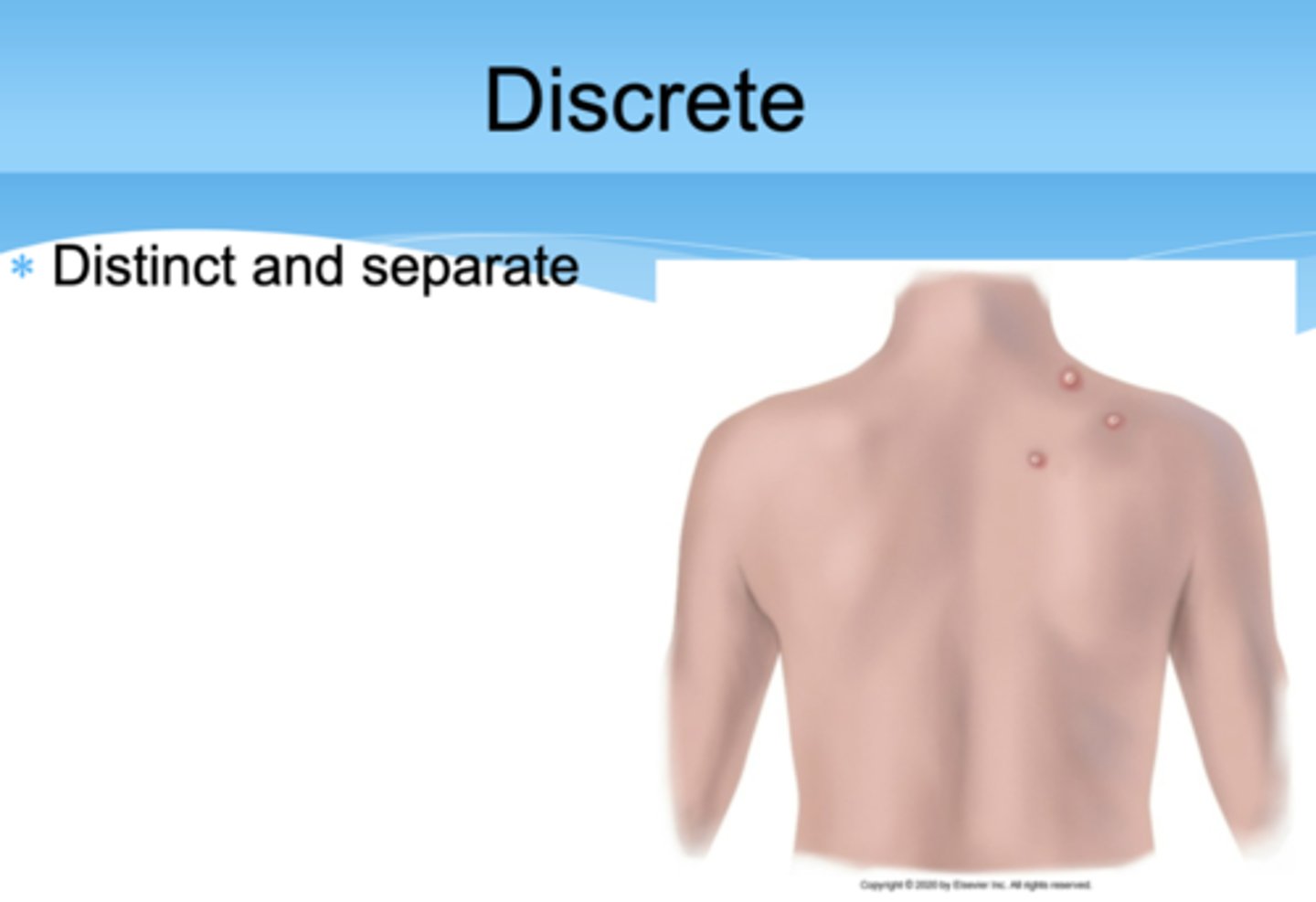
Grouped
Cluster of lesions
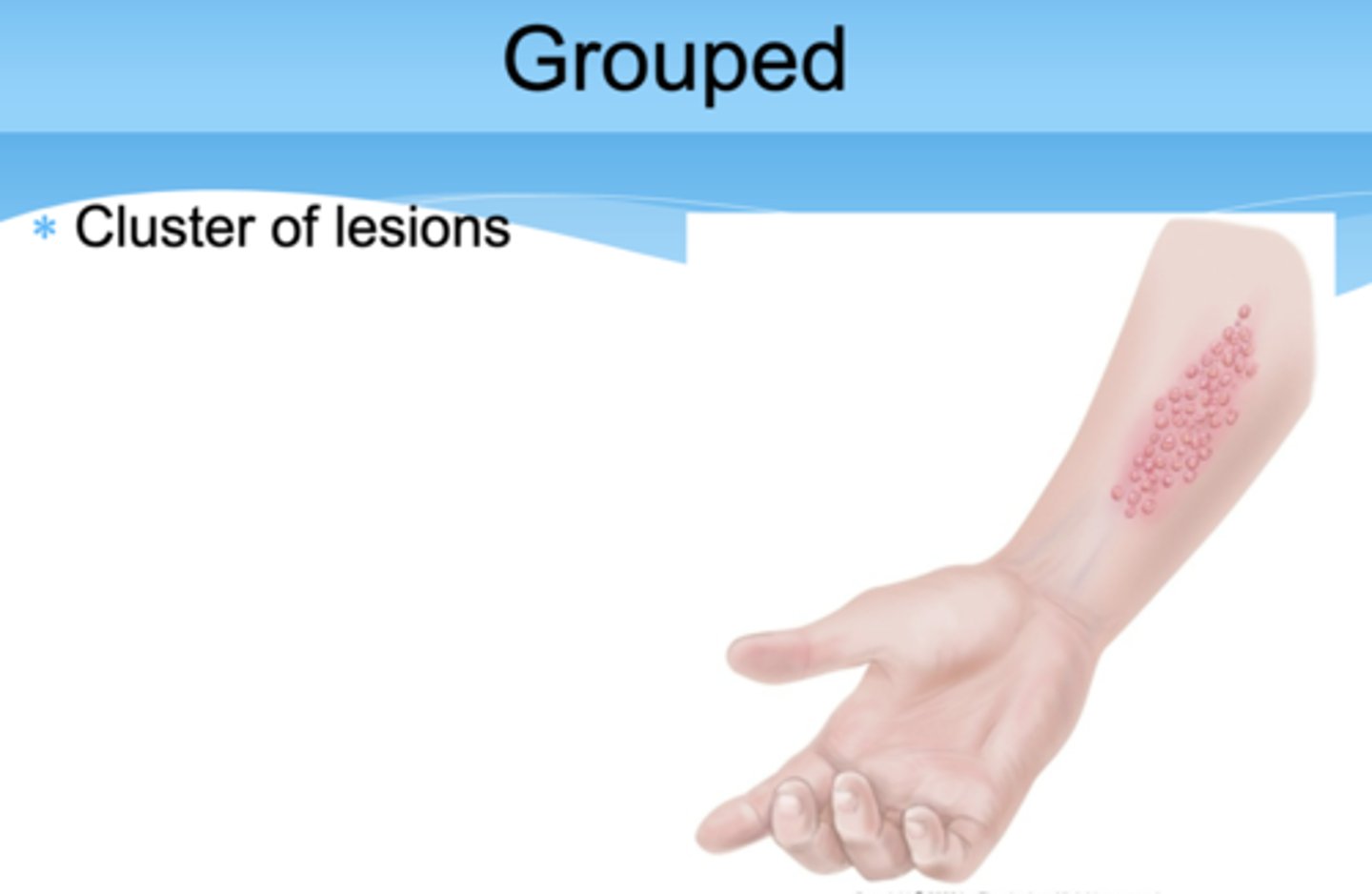
Linear
Scratch, streak, line, or stripe
Zosteriform
Linear arrangement following a unilateral nerve route
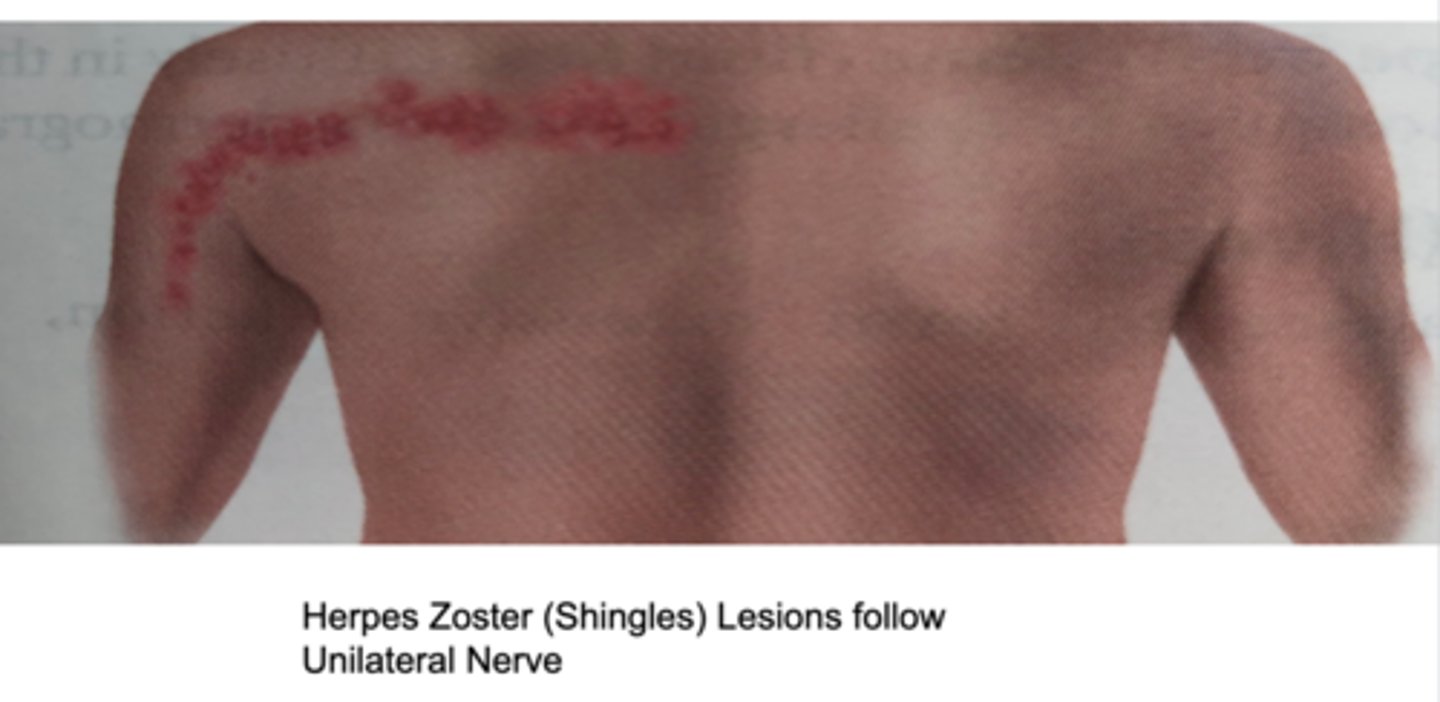
abnormal skin findings
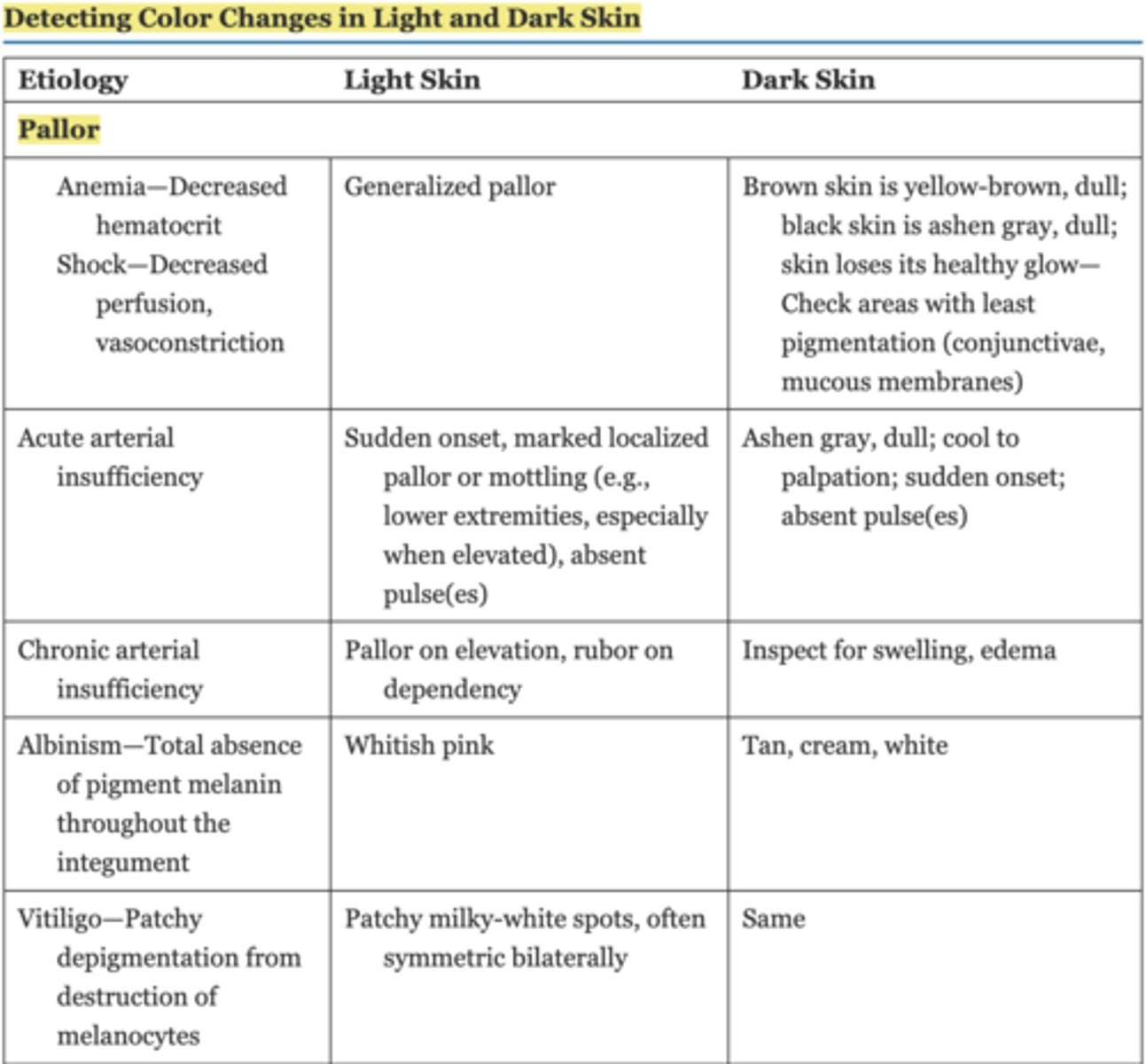
*Table 13.2 Detecting Color Changes in Light andDark Skin (extremely important) Chapter 13 pg. 226-228
Cyanosis- Increased amount of unoxygenated hemoglobin
Central—Chronic heart and lung disease cause arterial desaturation
Peripheral—Exposure to cold, anxiety
(light skin) -dusky blue color to skin or mucous membranes as a result of increased amount of nonoxygenated hemoglobin
(Dark skin) Dark but dull, lifeless; only severe cyanosis is apparent in skin—Check conjunctivae, oral mucosa, nail beds. Note brown-colored mucosa in figure below, normally it is pink.
erythema
Hyperemia—Increased blood in engorged arterioles (e.g., inflammation, fever, alcohol intake, blushing)
(light skin) intense redness/bright pink of the skin due to excessblood in dilated superficial capillaries, as in fever orinflammation
(dark skin) Purplish tinge but difficult to see; palpate for increased warmth with inflammation, taut skin, and hardening of deep tissues
Polycythemia—Increased red blood cells, capillary stasis
(light skin) Increased red blood cells, capillary stasis Ruddy blue in face, oral mucosa, conjunctiva, hands, and feet
(dark skin) Well concealed by pigment; check for redness in lips
Carbon monoxide poisoning
(Light skin) bright cherry red in face and upper torso
(dark skin) Cherry-red color in nail beds, lips, and oral mucosa
Jaundice- Increased serum bilirubin from liver inflammation or hemolytic disease such as after severe burns, some infections
(light skin) yellow color to skin, palate, and sclera due to excess bilirubin in the blood
(dark skin) Check sclera for yellow all the way up to iris; do not mistake normal yellowish fatty deposits in the scleral periphery for jaundice; jaundice best noted in junction of hard and soft palate, also palms
Carotenemia- Increased deposit of carotene from high intake of carrots, yellow squash, even in baby food
Carotenemia-yellow pigmentation of the skin (palms, soles and nasolabial folds secondary to excretion by sebaceous glands in sweat) associated with increased blood carotene (Vitamin A) levels (carrots, squash,pumpkin, breast milk)Abnormal Skin Findings
(dark skin) Yellow-orange tinge in palms and soles
Function of Skin
Skin is waterproof, protective, andadaptive
Protection from environment
Prevents penetration
Perception
Temperature regulation
Identification
Communication
Wound repair
Absorption and excretion
Production of vitamin D