Female Genitalia: Hx/PE/Health Maintenance
1/65
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
66 Terms
ROS female GU
menstrual regularity/frequency/duration/volume of periods; last period; bleeding between menses; dysmenorrhea; menopause/post-menopausalbleeding; vaginal discharge/pruritis; vulvar lesions/pruritis/pain; dyspareunia; bleeding after intercourse
red flags female GU
sudden incontinence, post-menopausal bleeding
sudden incontinence is concerning for
cauda equina syndrome
post-menopausal bleeding is concerning for
endometrial cancer
menarche
onset of menses
dysmenorrhea
painful menstruation
premenstrual syndrome
cluster of emotional, behavioral, and physical symptoms occurring 5 days before menses for three consecutive cycles
amenorrhea
absence of menstruation
abnormal uterine bleeding
bleeding between menses; infrequent, excessive, prolonged, or postmenopausal bleeding
menopause
absence of menses for 12 consecutive months bt ages 48 and 55
postmenopausal bleeding
bleeding occurring 6 mo or more after cessation of menses
primary amenorrhea
Absence of ever initiating periods
causes of primary amenorrhea
Congenital defects, genetic disorders, acquired CNS lesions
secondary amenorrhea
cessation of periods after they have been established
Causes of secondary amenorrhea
pregnancy, lactation, menopause, low body weight, malnutrion, anorexia nervosa, stress, chronic illness, hypothalmic-pituitary-ovarian dysfunction
primary dysmenorrhea
painful menstruation that begins at puberty and has no clear cause
causes of primary dysmenorrhea
excess prostaglandin production during the luteal phase when estrogen and progesterone levels decline
Secondary dysmenorrhea
painful menstruation that begins during adult life, usually as a consequence of a pelvic disorder
causes of Secondary dysmenorrhea
endometriosis, adenomyosis, pelvic inflammatory disease, endometrial polyps
criteria for premenstrual syndrome
SS in the 5 days prior to menses for at least 3 consecutive cycles, cessation of SS within 4 days after onset of menses, and interference with daily activities
polymenorrhea
less than 21-day intervals between menses
oligomenorrhea
infrequent bleeding
menorrhagia
excessive menstrual bleeding, bright red with clots
metrorrhagia
bleeding between periods or intermenstrual bleeding
menometrorrhagia
excessive uterine bleeding at both the usual time of menstrual periods and at other irregular intervals
postcoital bleeding
bleeding after intercourse which suggests cervical polyps, cancer, or atrophic vaginitis in older women
Postmenopausal bleeding
bleeding occurring 6 months or more after cessation of menses
MCC of acute pelvic pain
pelvic inflammatory disease
How should the pt be positioned for a pelvic exam?
Drape the patient, place her heels in the foot holders, and assist her into the lithotomy position with thighs flexed, abducted, and externally rotated. Ensure her buttocks extend slightly beyond the table edge and support her head with a pillow.
graves speculum description
wider, larger, curved
indications for a graves speculum
parous women with vaginal prolapse
pederson speculum description
narrower, flatter blades
indication for pederson speculum
small introitus such as a virgin or elderly women
most comfortable speculum for a sexually active woman
medium pederson
during a papsmear, cells collected from the ectocervix are
squamous epithelium
during a papsmear, cells collected from the endocervix are
columnar epithelium
cervical broom
Press, turn, scrape in full circle
cervical scrape
Press, turn, scrape in full circle
endocervical brush
Press, turn, scrape in half circle
tanner stage 1
Preadolescent—no pubic hair except for the fine body hair (vellus hair) similar to that on the abdomen
tanner stage 2
Sparse growth of long, slightly pigmented, downy hair, straight or only slightly curled, chiefly along the labia
tanner stage 3
Darker, coarser, curlier hair, spreading sparsely over the pubic symphysis
Tanner stage 4
Coarse and curly hair as in adults; area covered greater than in stage 3 but not as great as in the adult and not yet including the thighs
tanner stage 5
Hair adult in quantity and quality, spreads on the medial surfaces of the thighs but not up over the abdomen
cystocele
a bulge of the upper two-thirds of the anterior vaginal wall with the bladder
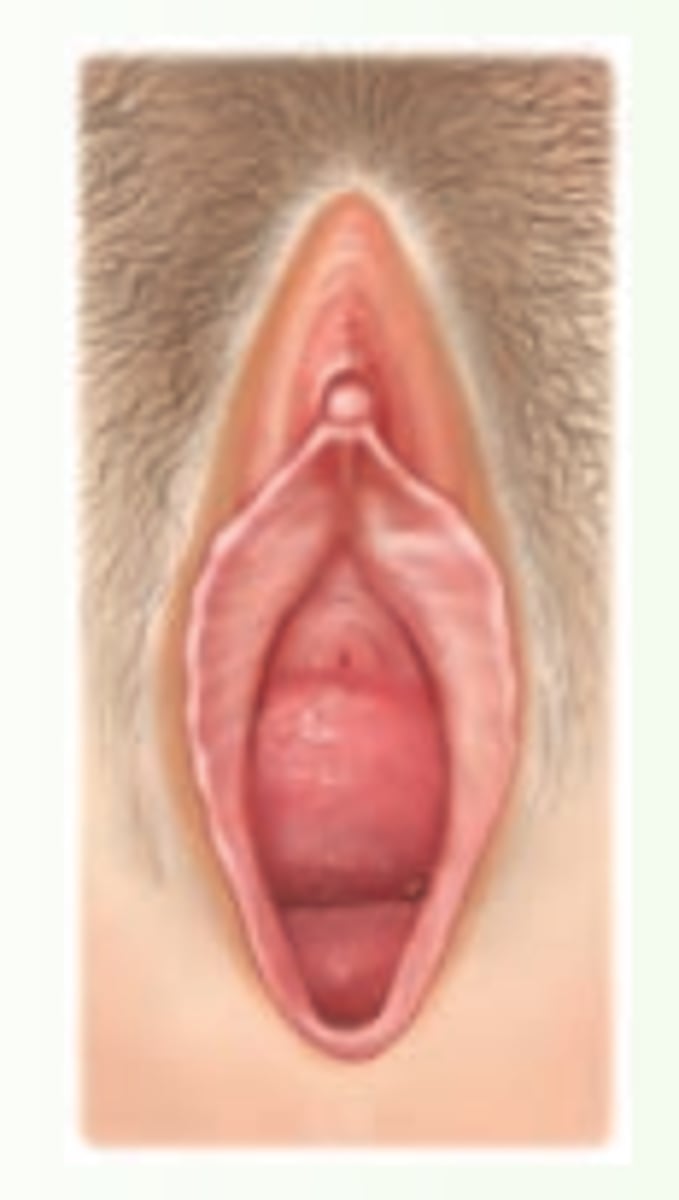
urethral caruncle
small red benign tumor visible at the posterior urethral meatus
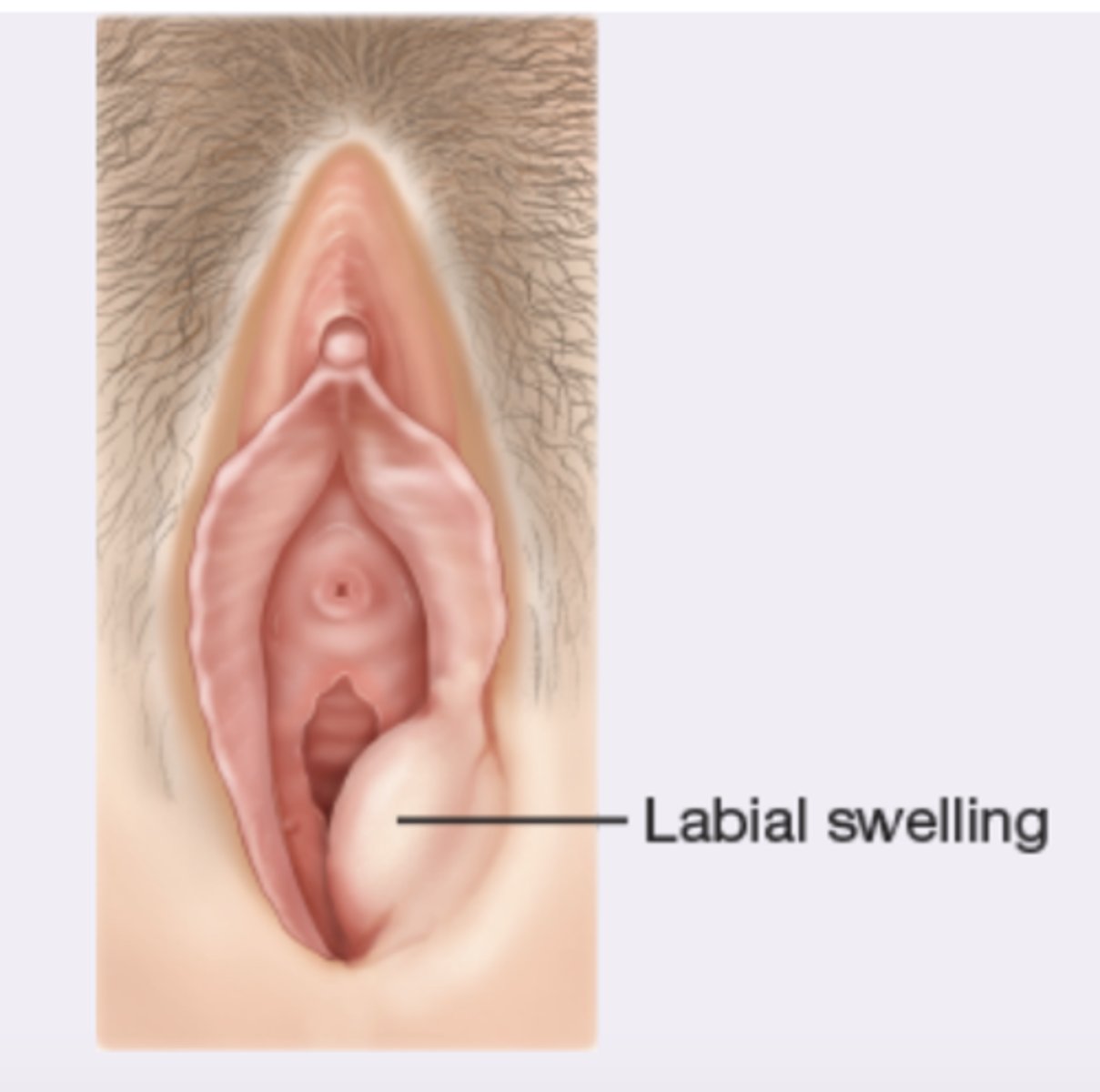
bartholin gland infection
Acute-tense, hot, tender abscess, pus or erythema from or near duct; chronic-nontender cyst large or small
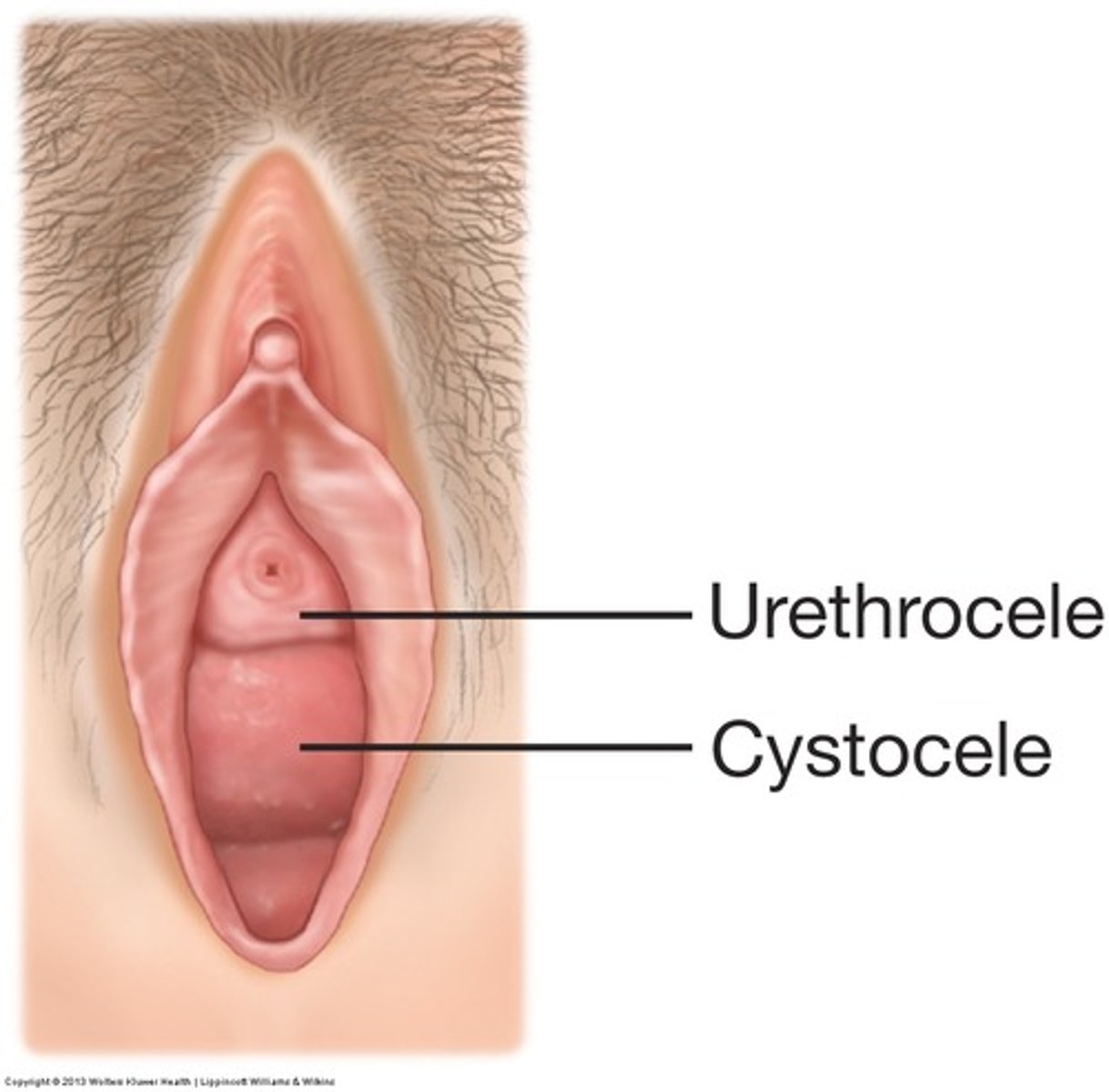
cystourethrocele
bulging of the anterior vaginal wall, bladder, and urethra
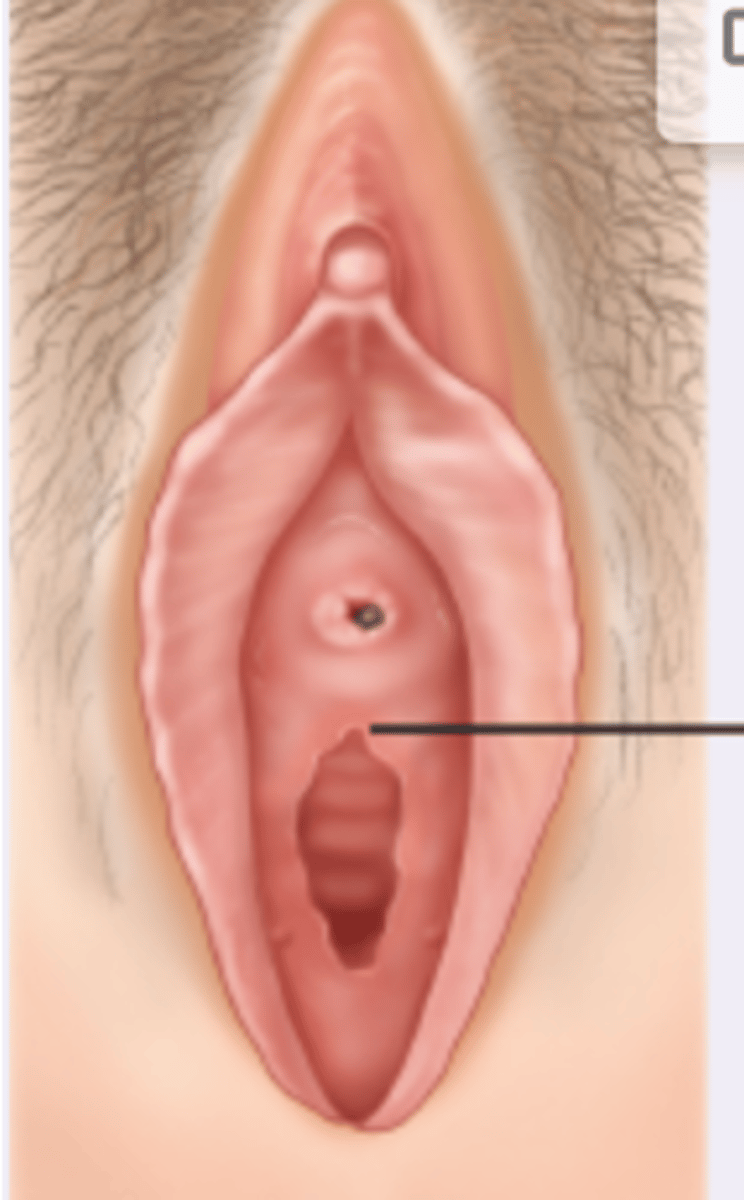
prolapse of the urethral mucosa
swollen red ring around the urethral meatus
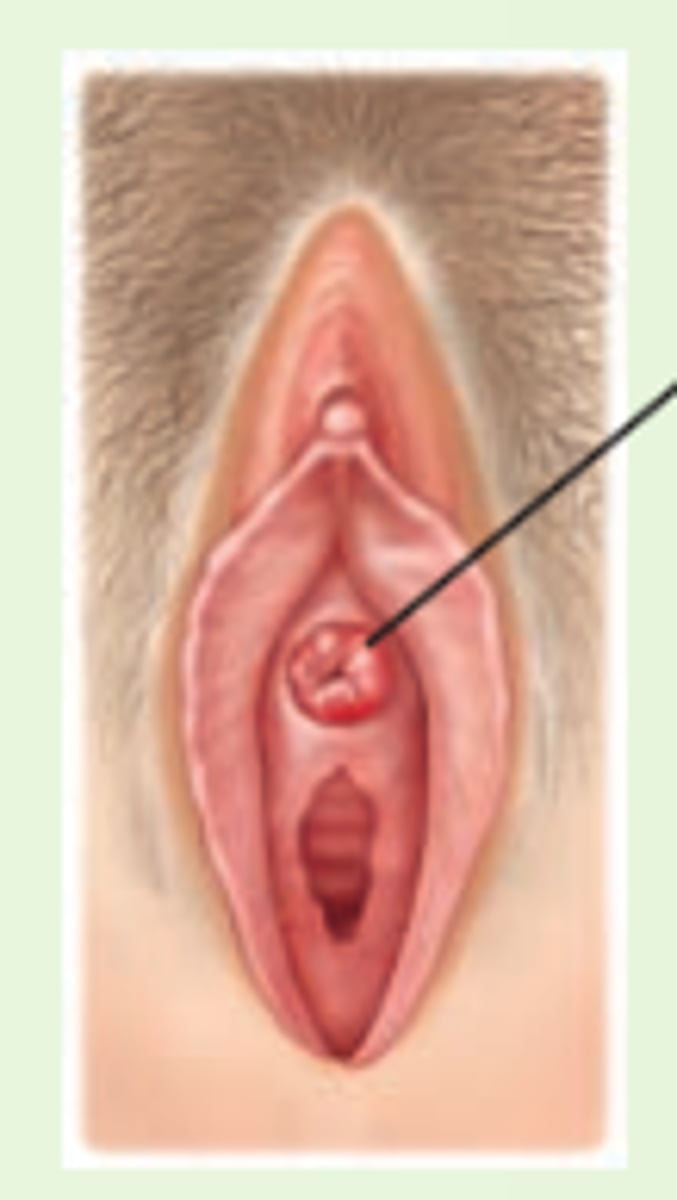
rectocele
herniation of the rectum into the posterior wall of the vagina
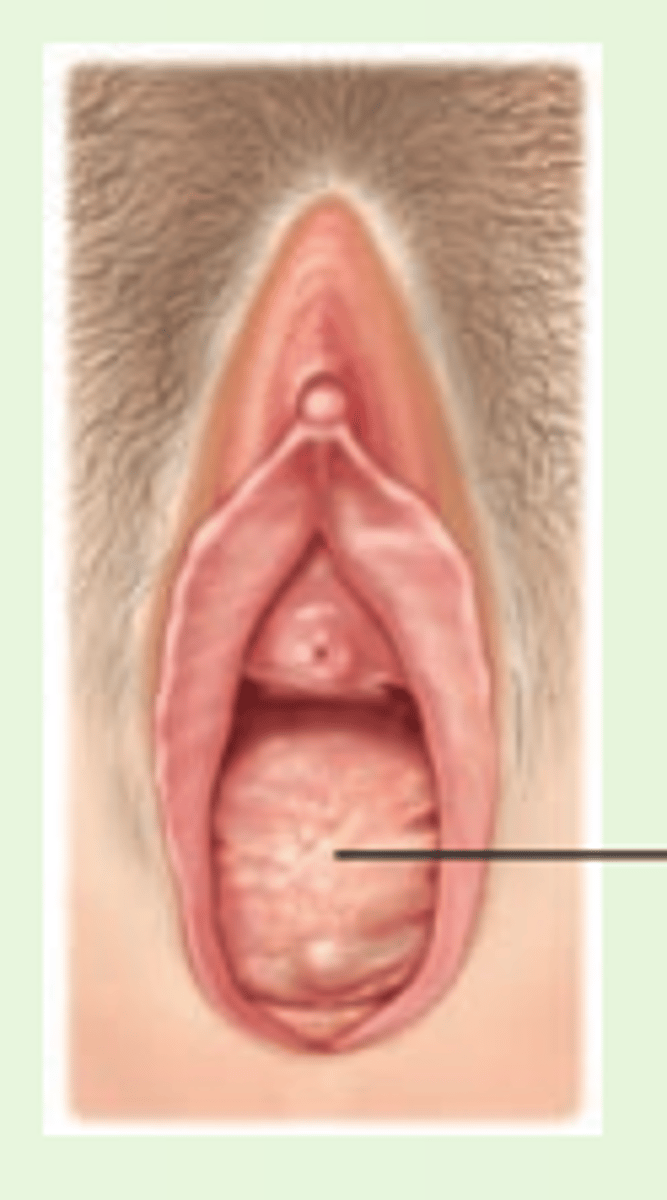
retention cysts
translucent nodules on cervical surface, no pathologic significance, occur via metaplasia and blocking secretions of columnar epithelium
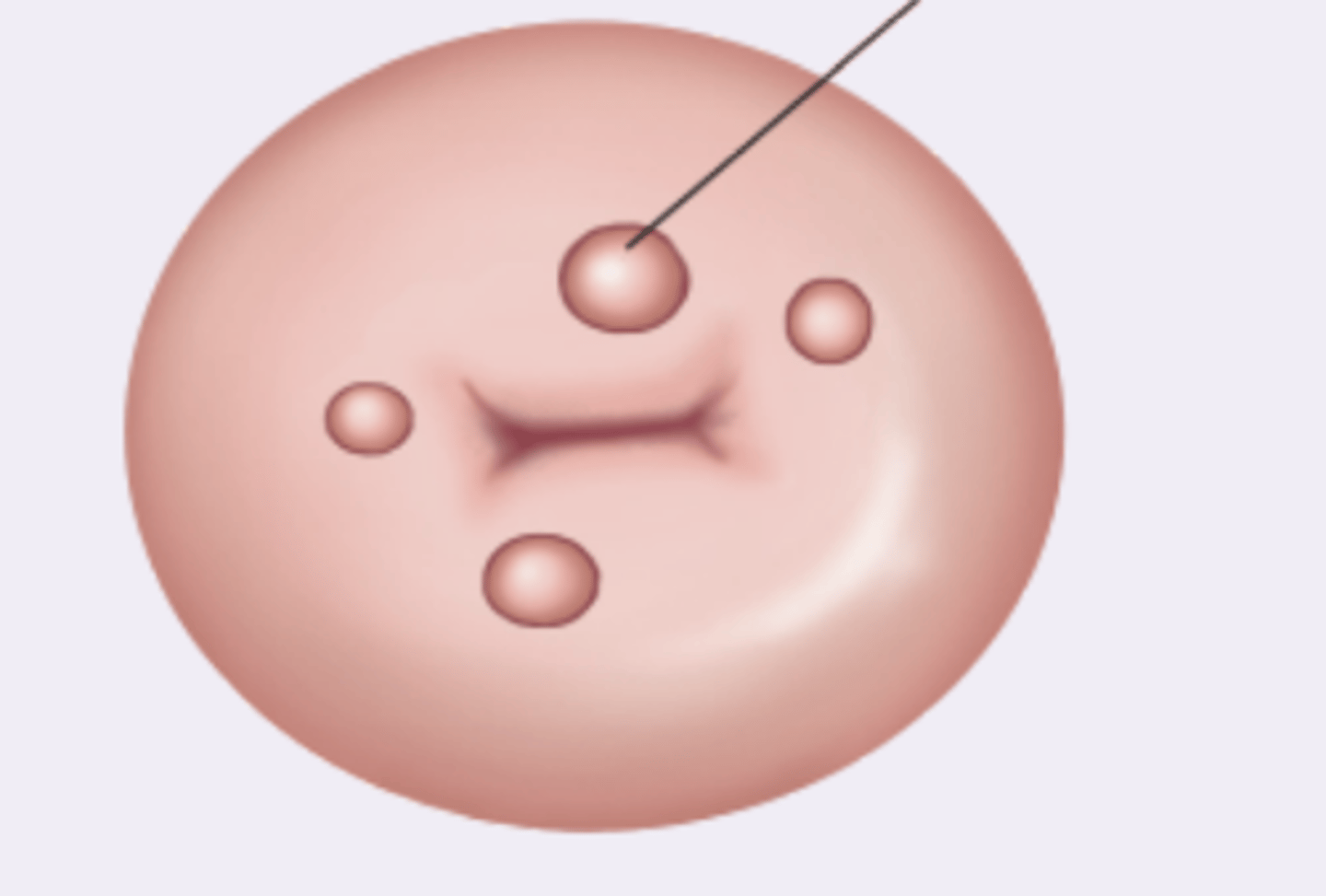
cervical polyp
arises from the endocervical canal, bright red, soft, fragile; benign but may bleed
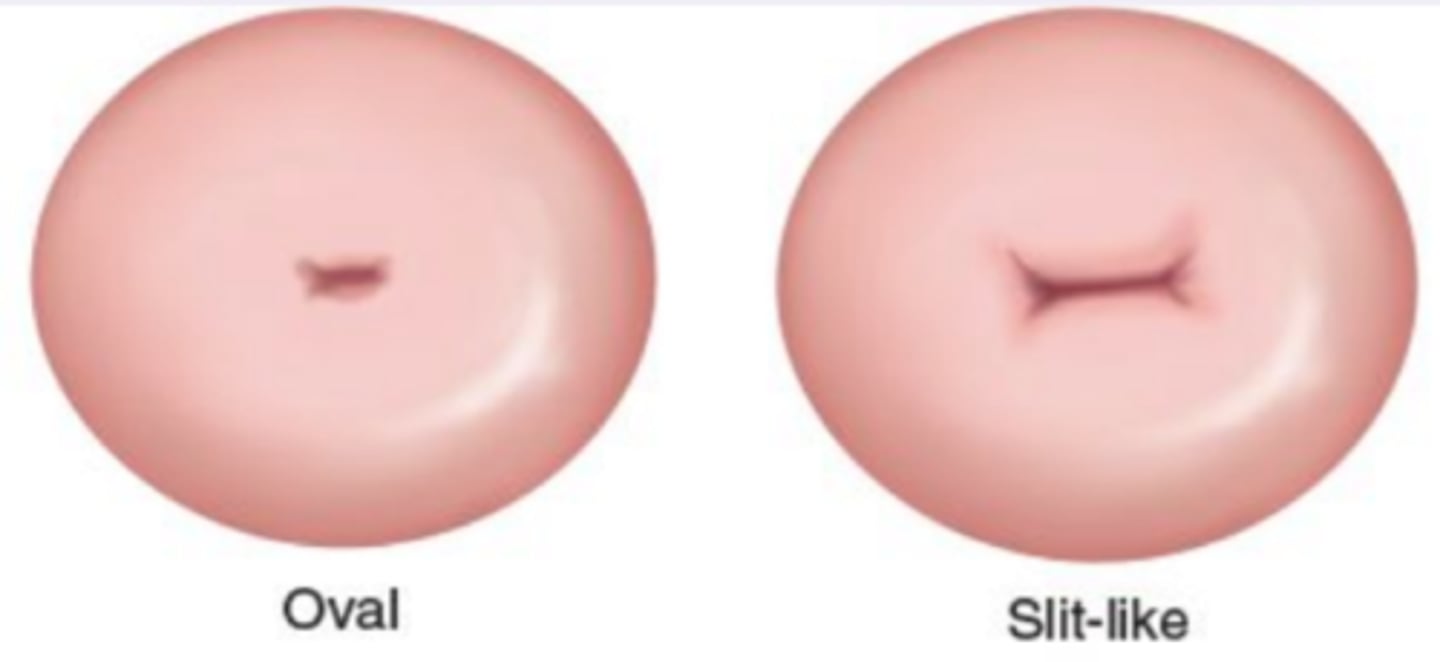
normal shape of cervical os
oval and slit-like
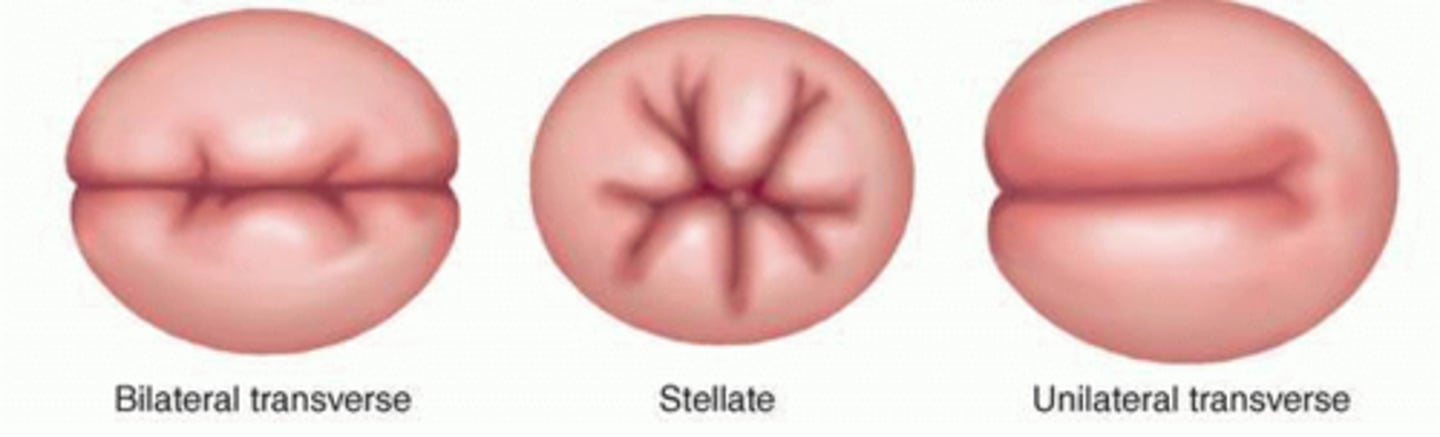
types of cervical lacerations from delivery
bilateral transverse, stellate, unilateral transverse
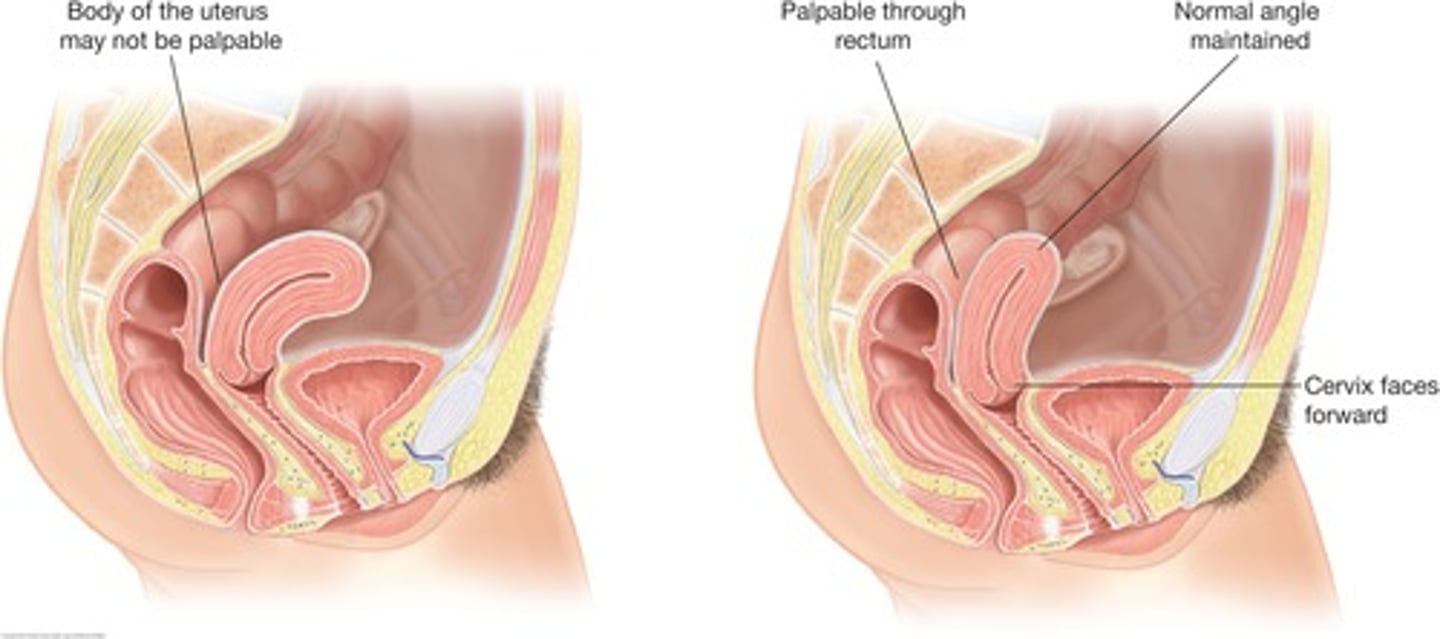
normal positions of the uterus
retroversion and retroflexion
retroversion of the uterus
tilting backward of the entire uterus
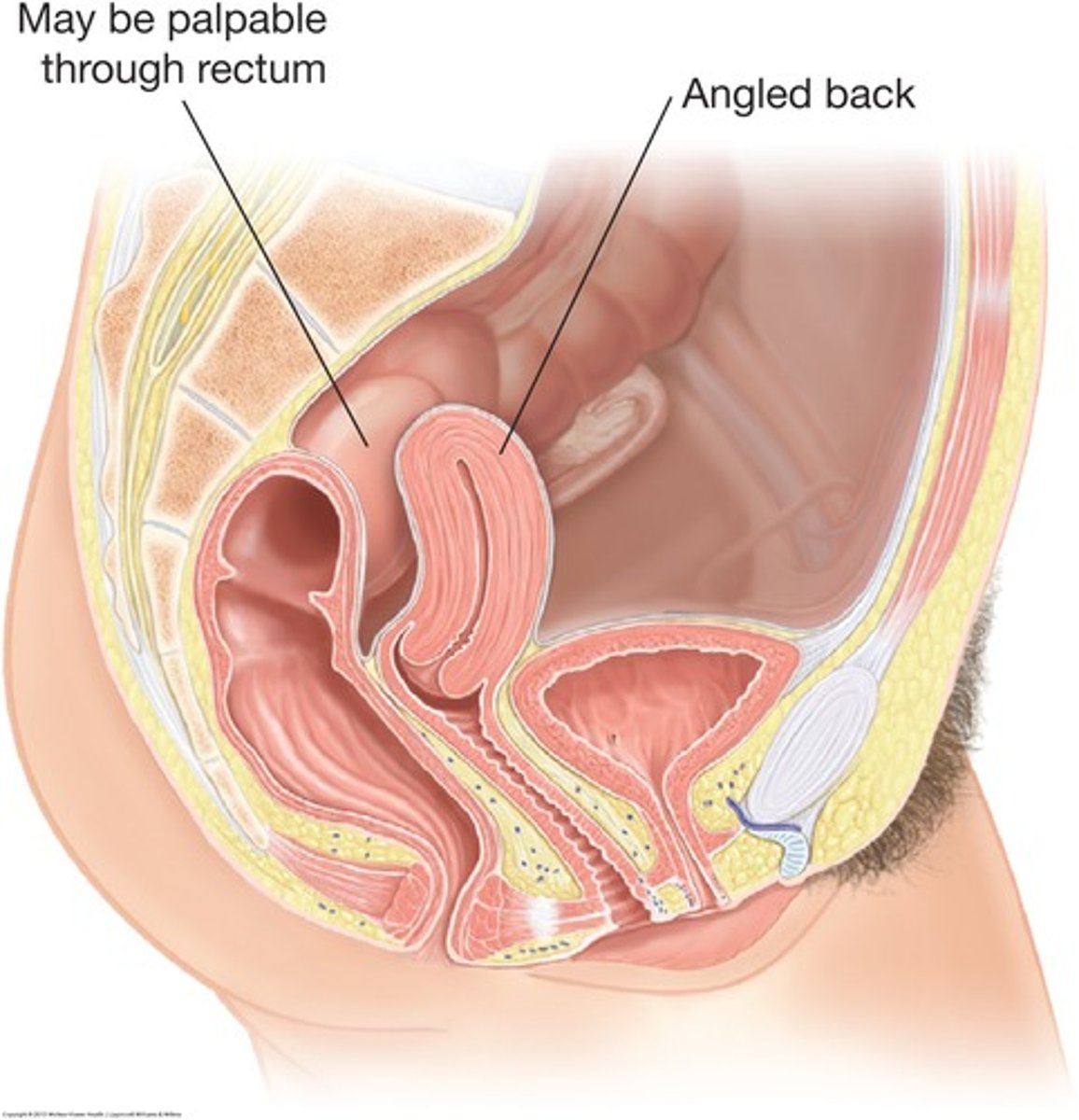
retroflexion of the uterus
backward angulation of the body of the uterus in relation to the cervix
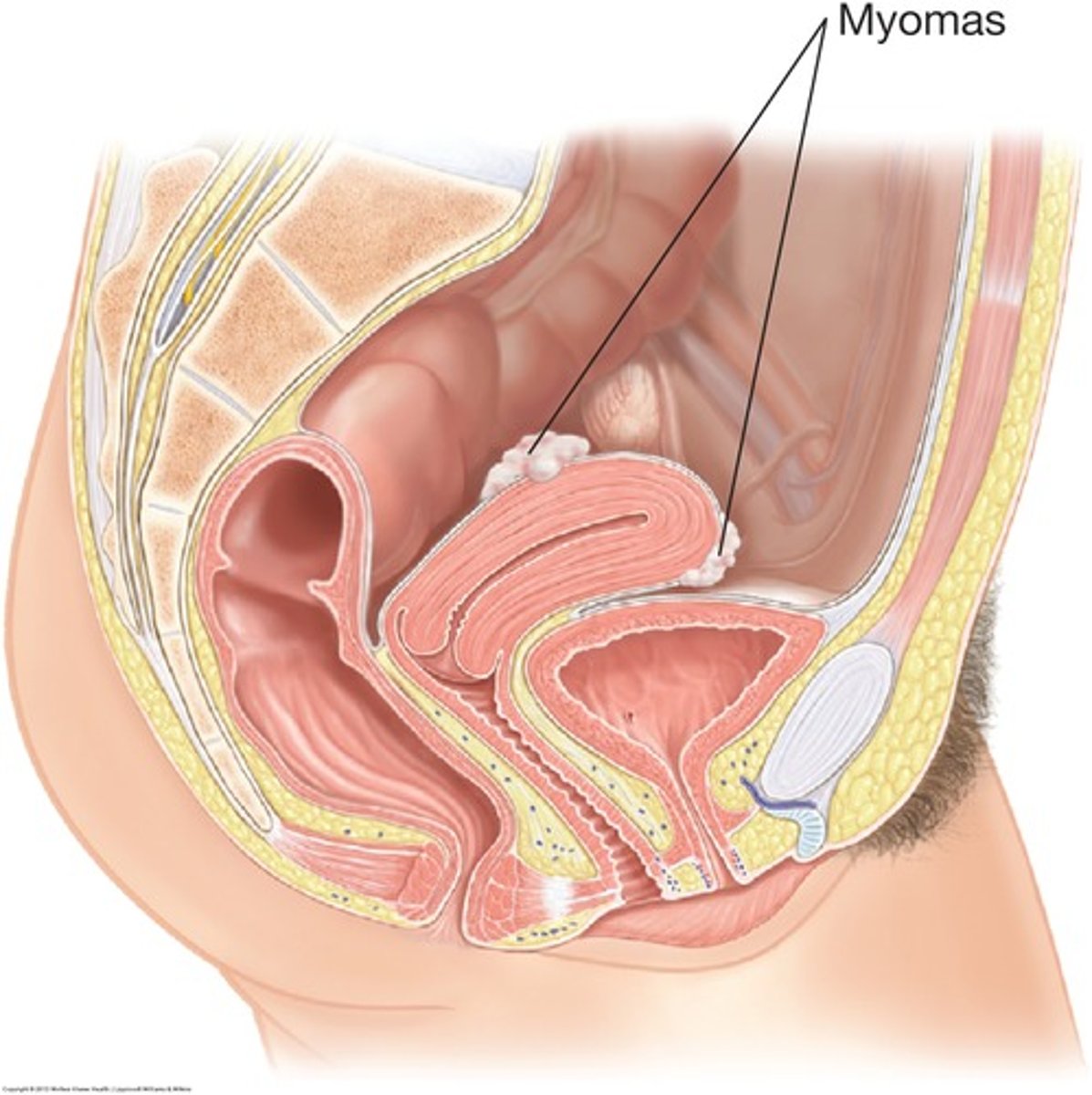
myomas of the uterus (fibroids)
common benign uterine tumors, firm irregular nodules that are continuous with the uterine surface
prolapse of the uterus
results from weakness of the supporting structures of the pelvic floor; associated with a cystocele and rectocele
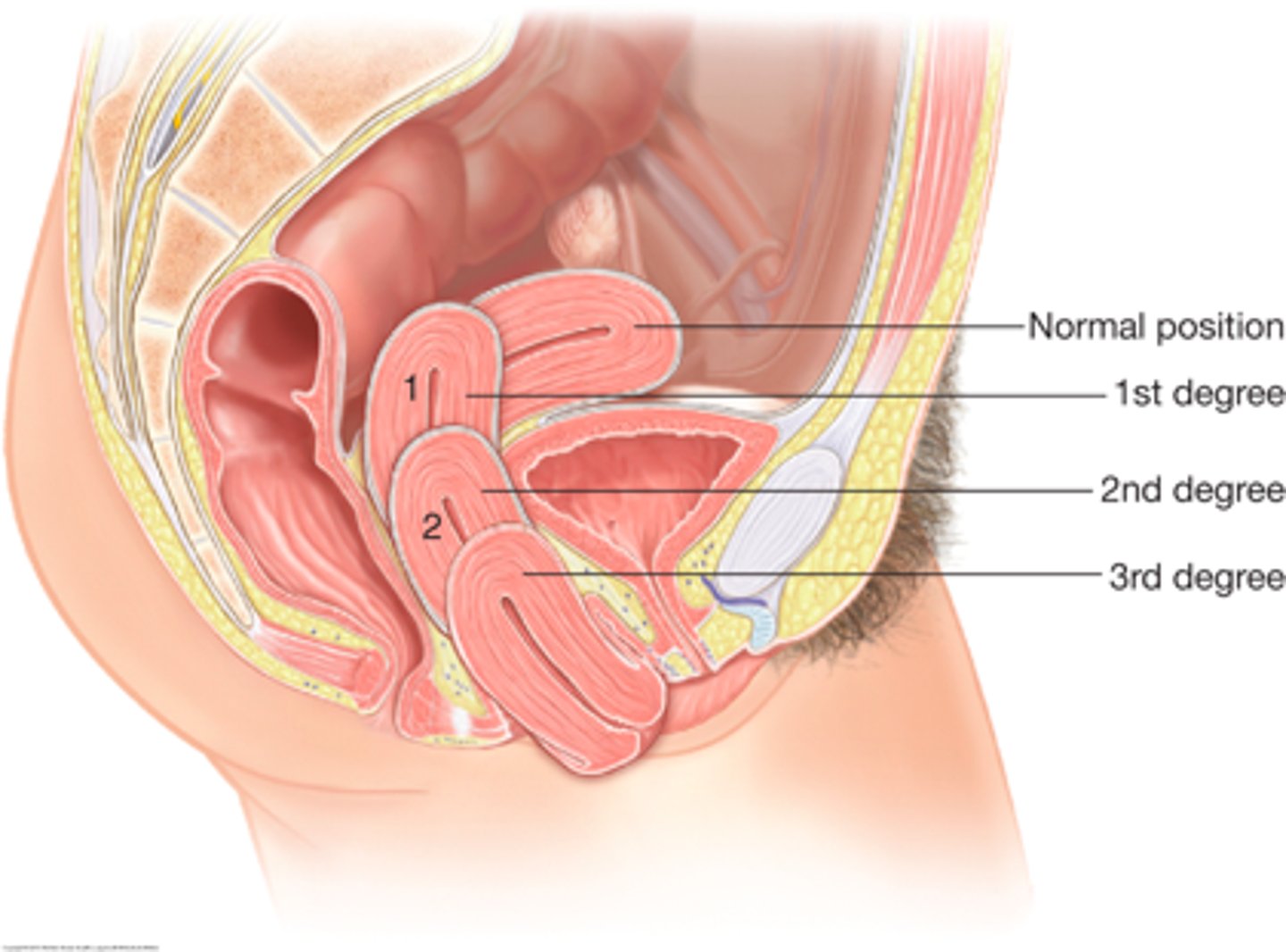
first degree prolapse
cervix is still well within the vagina
second degree prolapse
at the introitus
third degree prolapse
cervix and vagina are outside the introitus
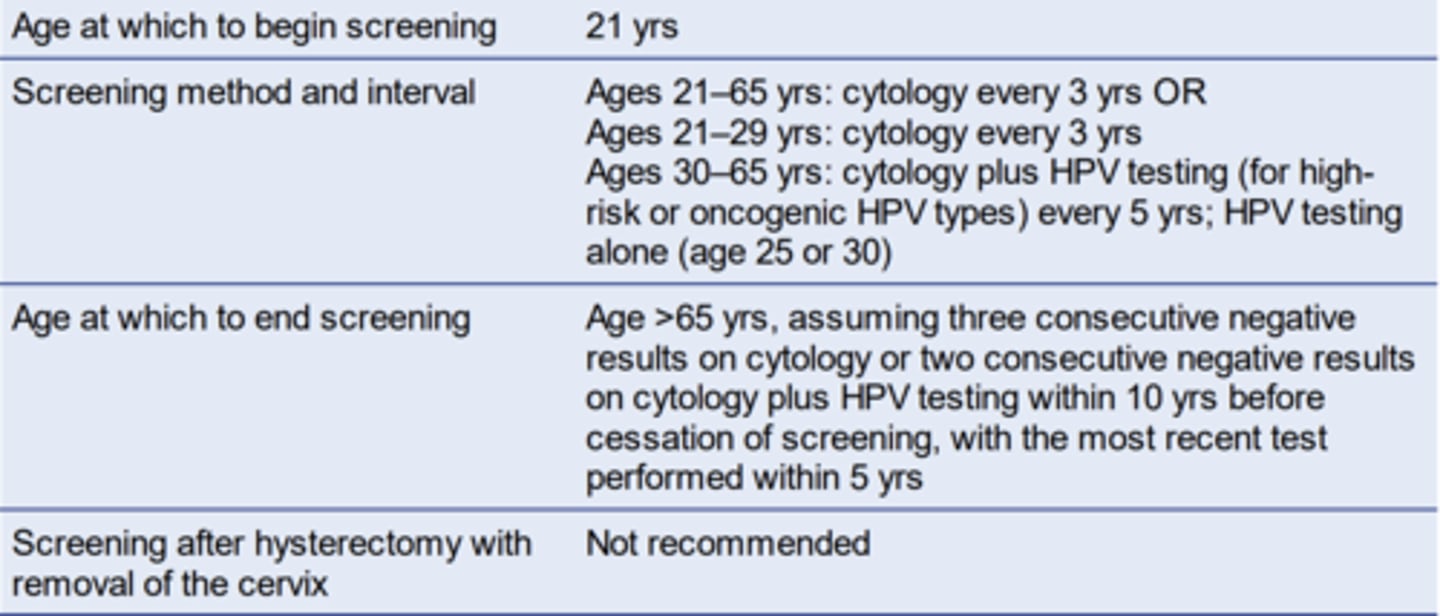
current cervical cancer screening guidelines for average risk women
start at 21, end at >65 yo
current USPSTF guidelines regarding menopause and hormone replacement therapy
Recommends against the use of either estrogen alone for women who have had a hysterectomy or combined use of estrogen and progesterone; did not address using HRT to treat menopausal symptoms
current USPSTF guidelines regarding screening for ovarian cancer
Not recommended for asymptomatic, average risk patients; screen women with BRCA mutation with transvaginal US, pelvic exams, serum cancer antigen 125 testing
What reduces ovarian cancer in women with a BRCA mutation?
chemoprevention or prophylactic surgery