Unit 2. Endocrine System (Chapter 16)
1/114
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
115 Terms
Endocrine system
The body system that interacts with the nervous system to coordinate and integrate cellular activity using hormones transported in blood.
Endocrinology
The study of hormones and endocrine organs.
Nervous system vs. Endocrine system (Response speed)
Nervous system initiates responses rapidly, while the endocrine system initiates them slowly.
Nervous system vs. Endocrine system (Duration)
Nervous system has short-duration responses, while the endocrine system has long-duration responses.
Nervous system vs. Endocrine system (Signal type)
Nervous system acts via action potentials and neurotransmitters; endocrine system acts via hormones in blood.
Nervous system vs. Endocrine system (Location)
Nervous system acts at specific locations determined by axons; endocrine system acts at diffuse locations where blood reaches.
Nervous system vs. Endocrine system (Distance)
Neurotransmitters act over very short distances; hormones act over long distances.
Nervous system vs. Endocrine system (Signal coding)
Nervous system uses frequency of action potentials; endocrine system uses hormone concentration.
Major processes of endocrine system
Reproduction, growth and development, maintenance of electrolyte/water/nutrient balance, regulation of metabolism, and mobilization of body defenses.
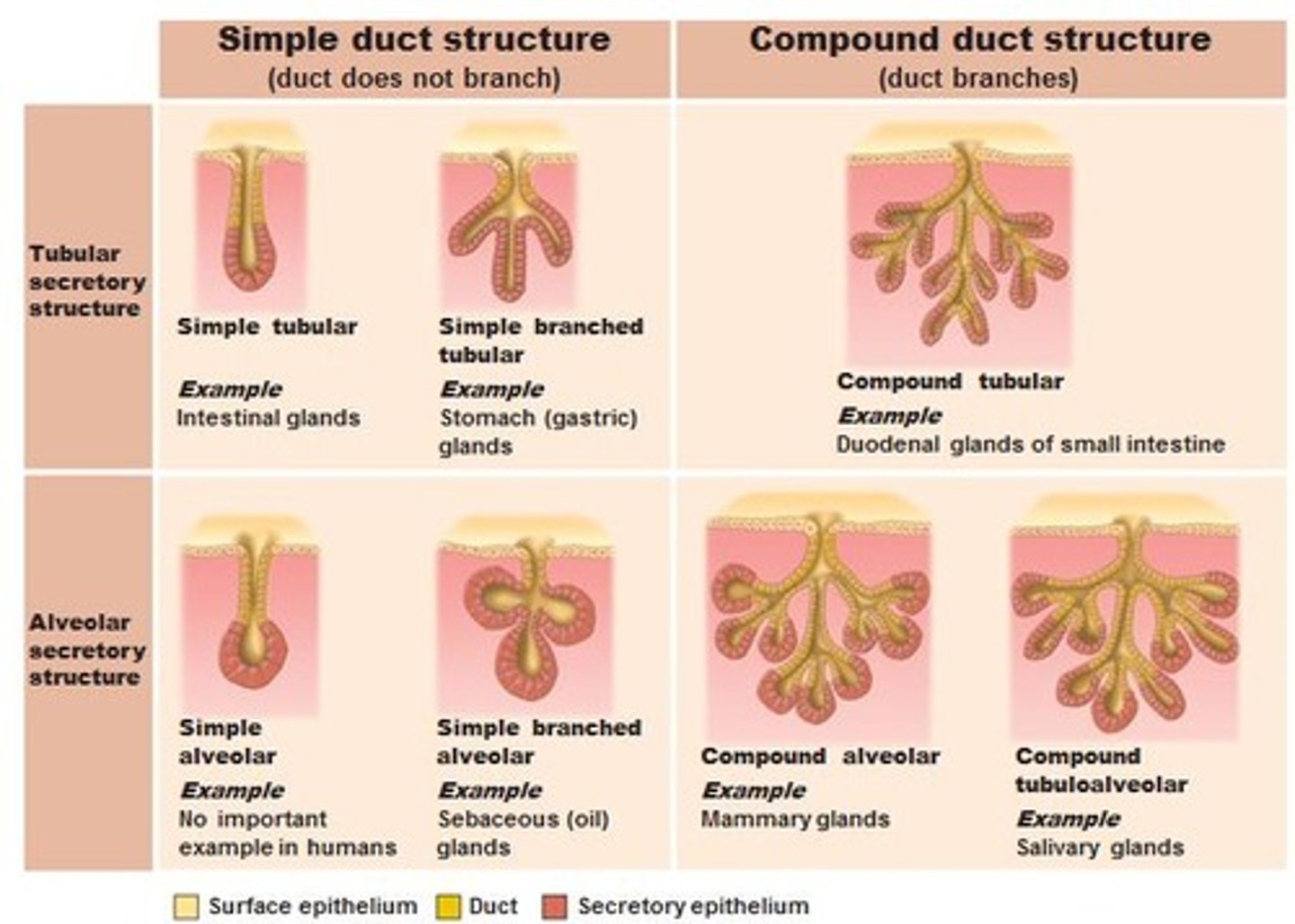
Exocrine glands
Glands that produce nonhormonal substances (sweat, saliva) and have ducts to carry secretions to a membrane surface.
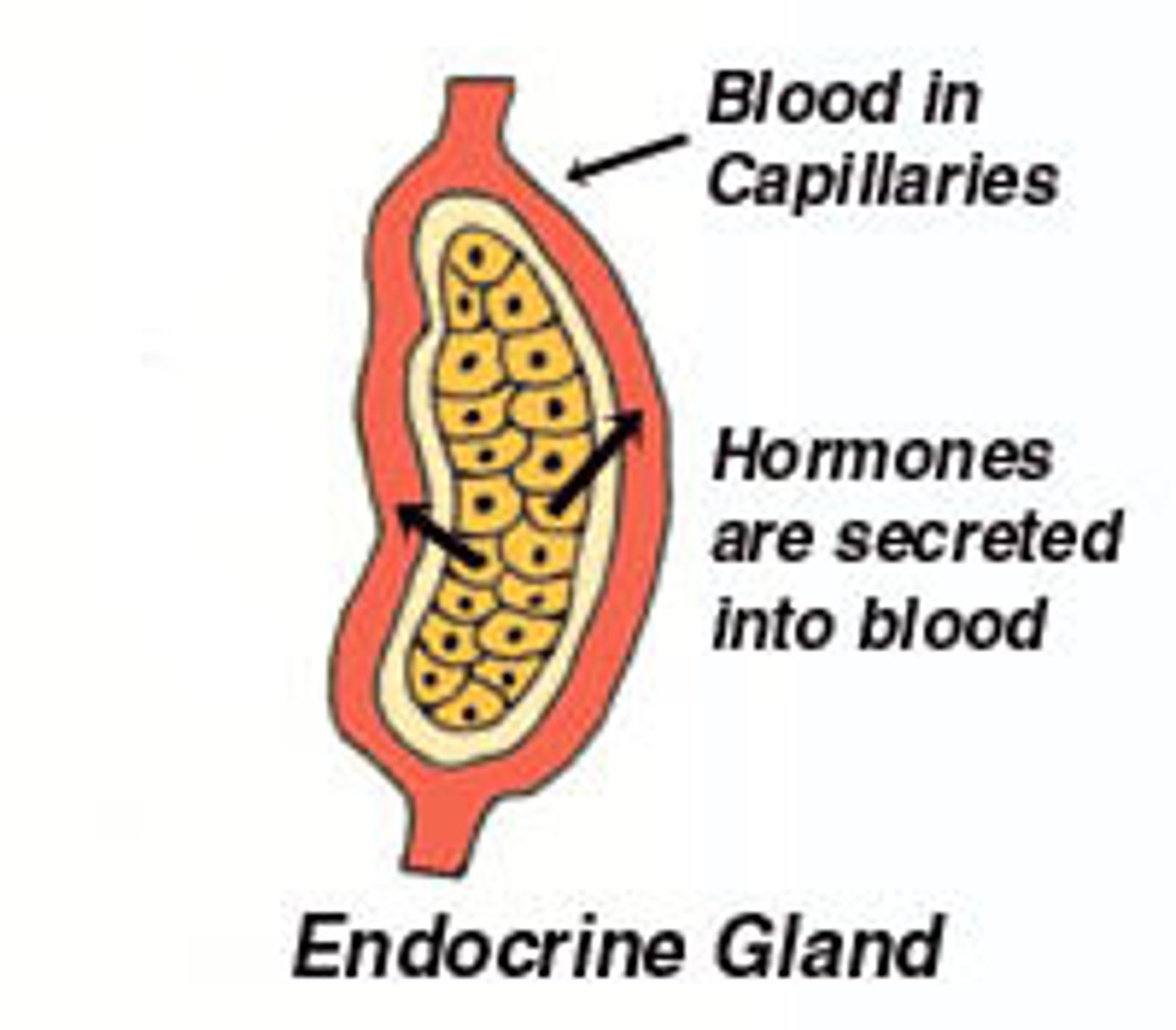
Endocrine glands
Ductless glands that produce hormones secreted directly into surrounding extracellular fluid.
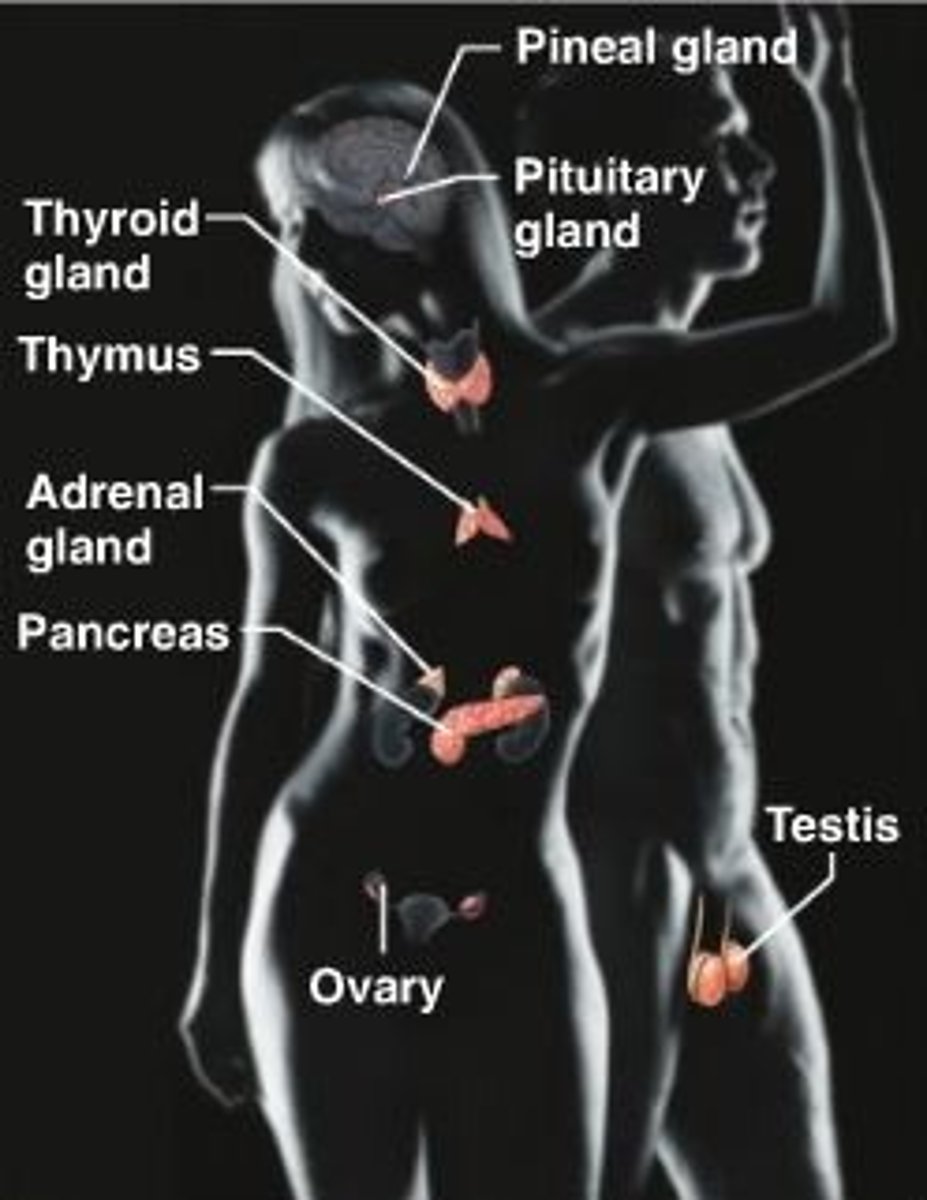
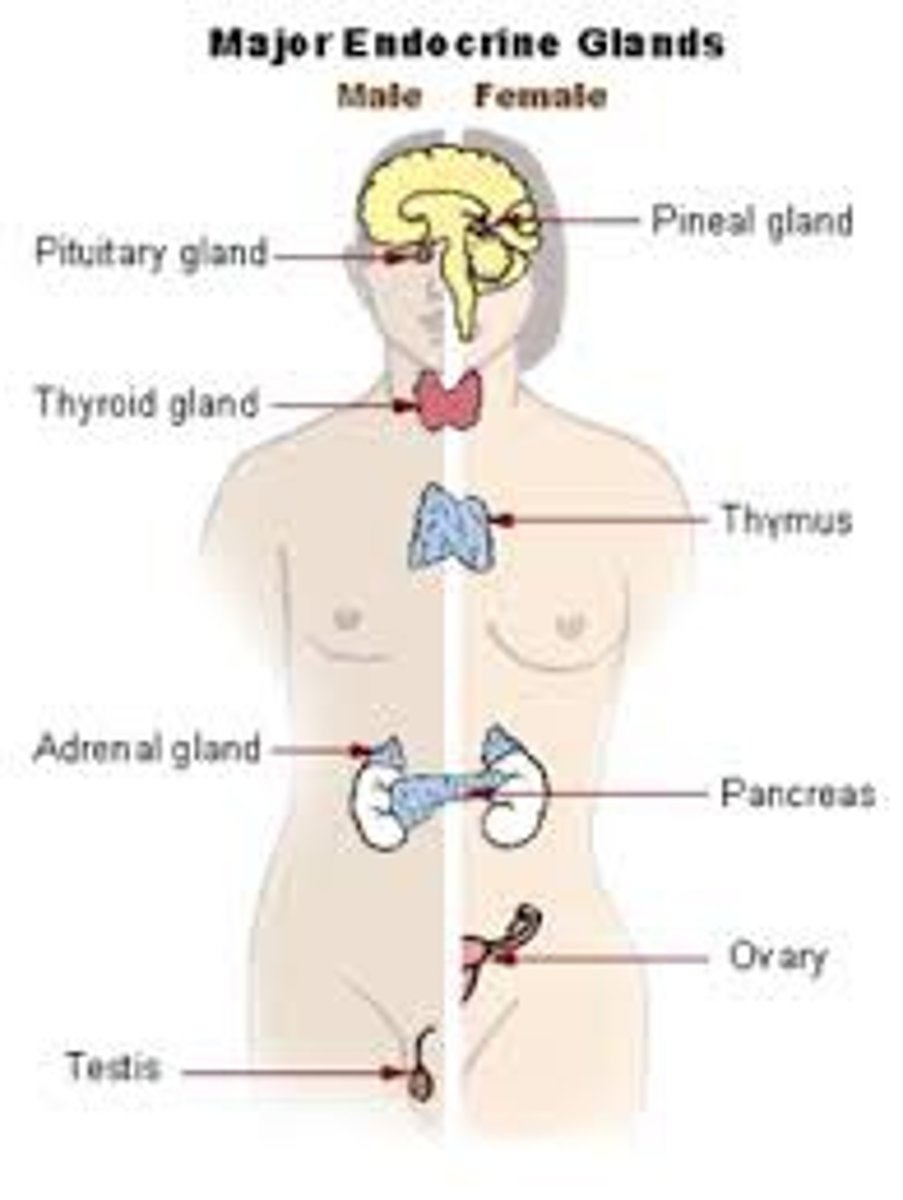
Primary endocrine glands
Pituitary, thyroid, parathyroid, adrenal, and pineal glands.
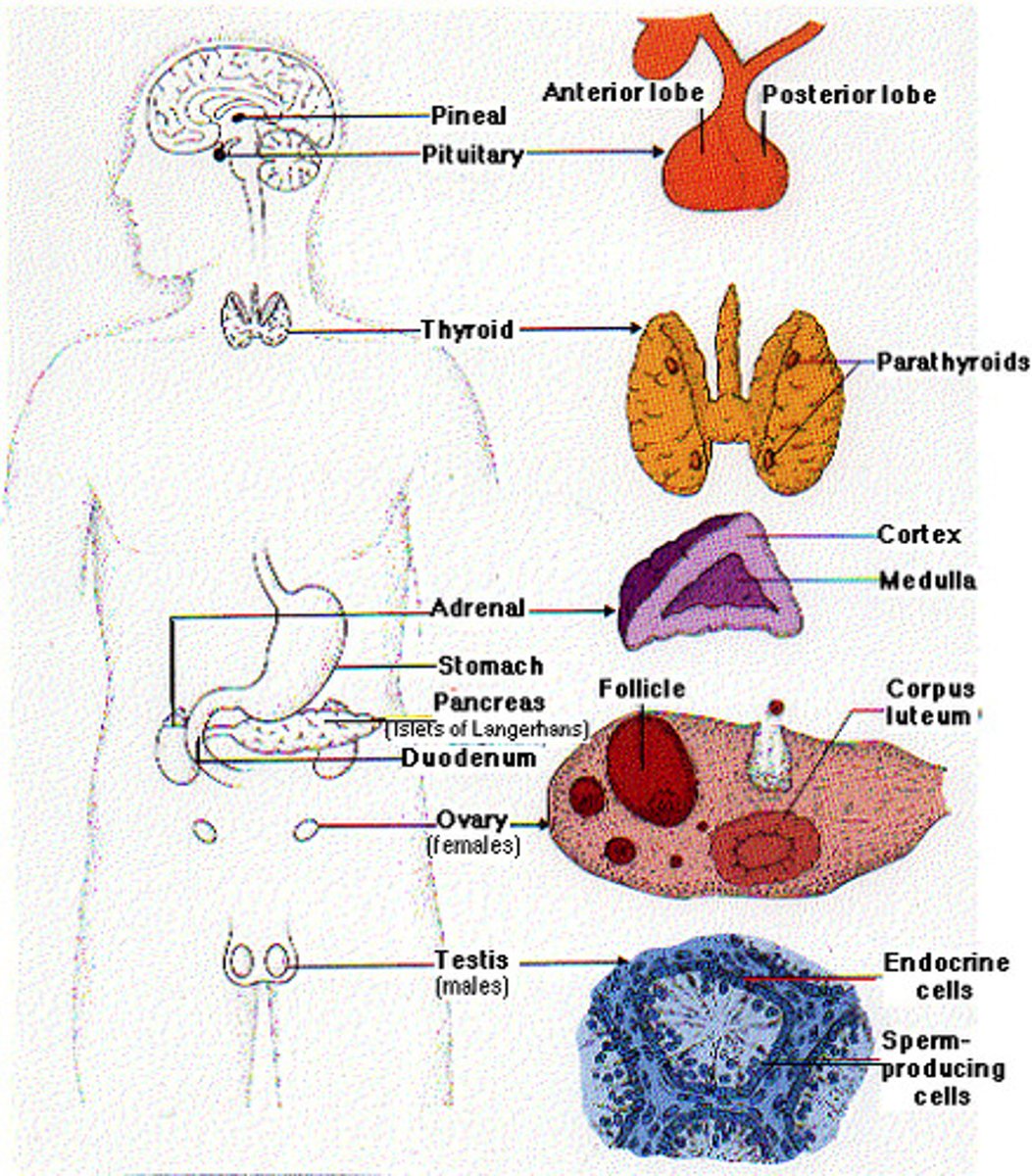
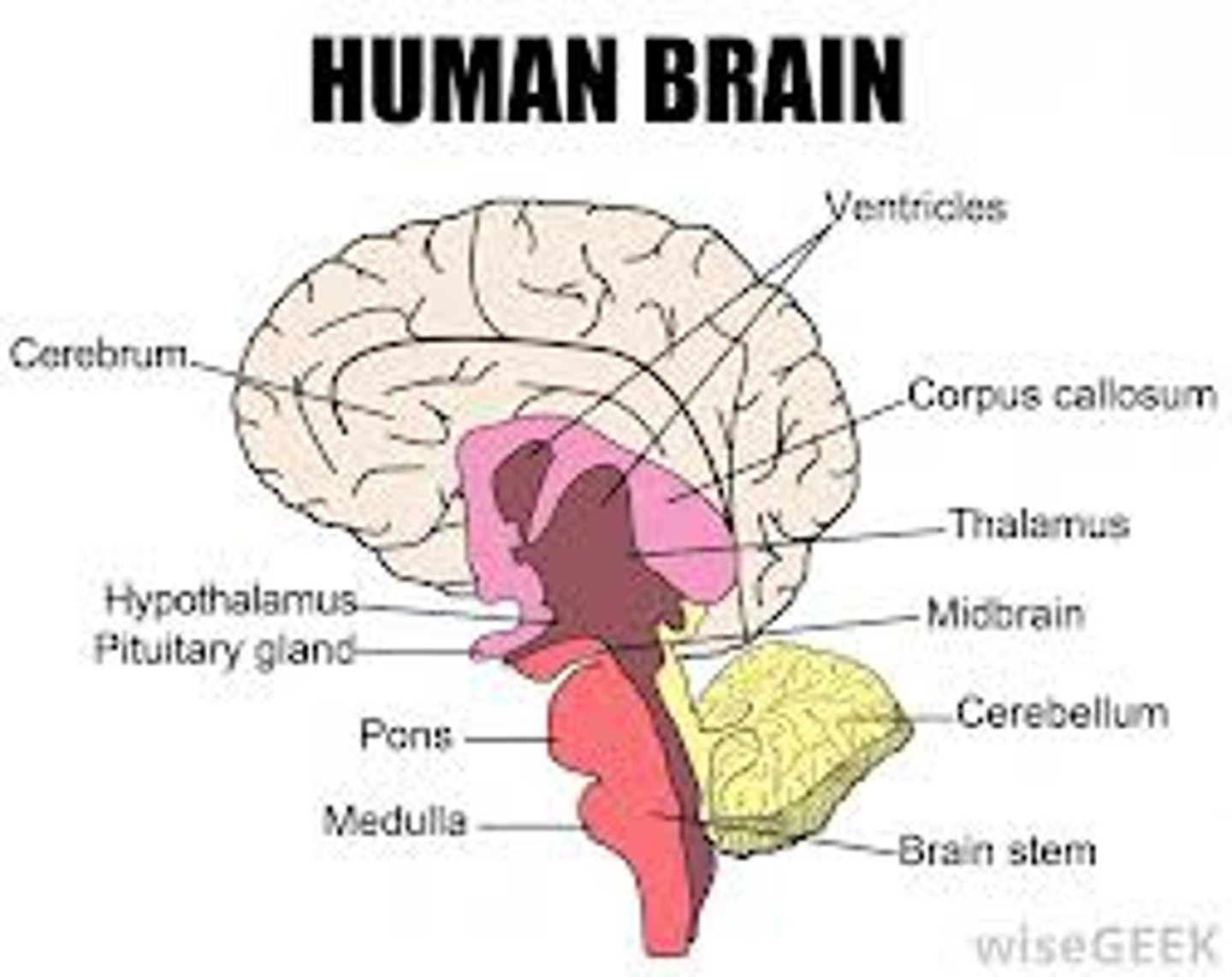
Hypothalamus
A neuroendocrine organ that connects the nervous and endocrine systems.
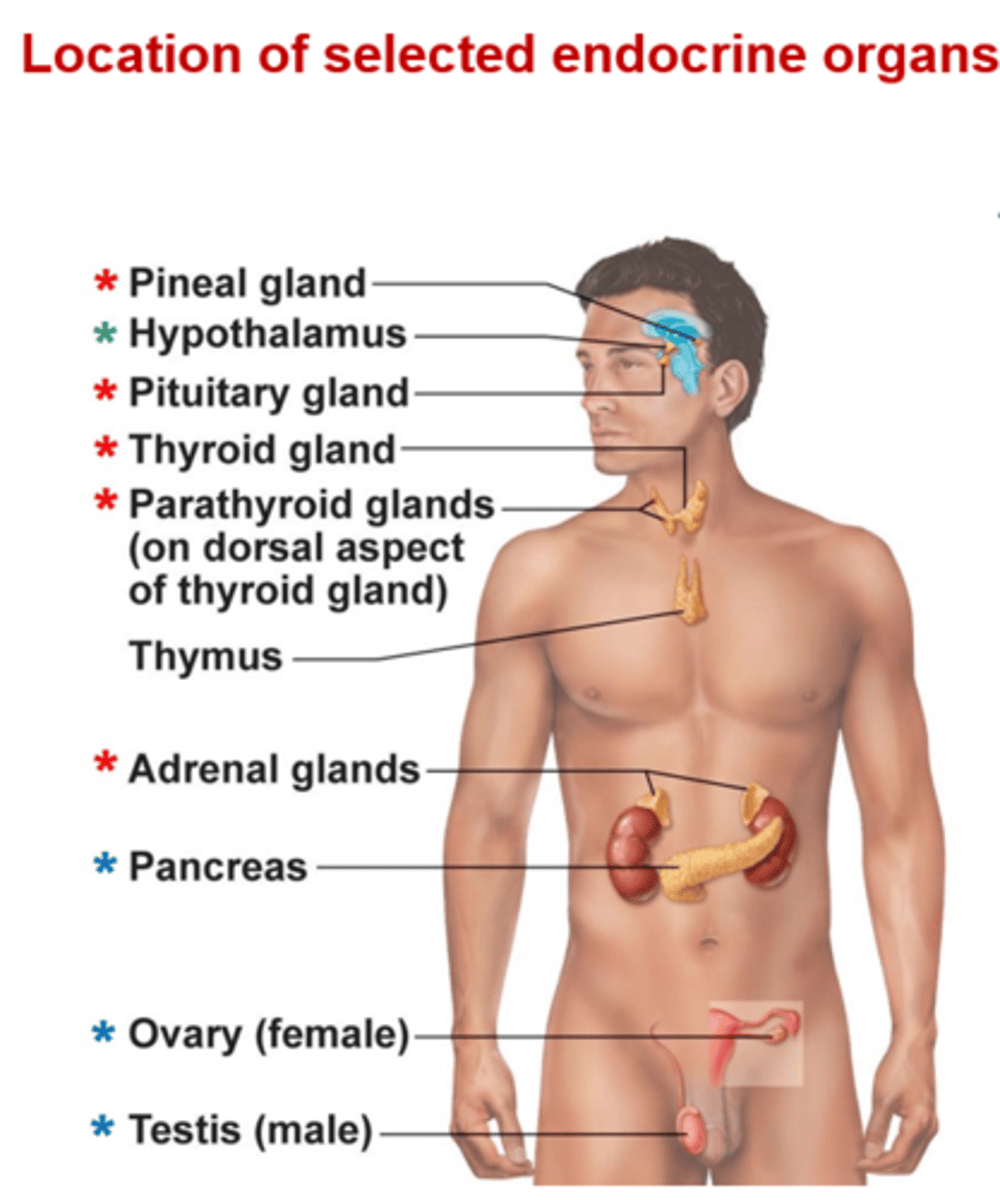
Organs with endocrine tissue
Pancreas, gonads, placenta, stomach, intestine, heart, kidneys, skin, thymus, bone, and adipose tissue.
Hormones
Long-distance chemical signals that travel in blood to reach target cells.
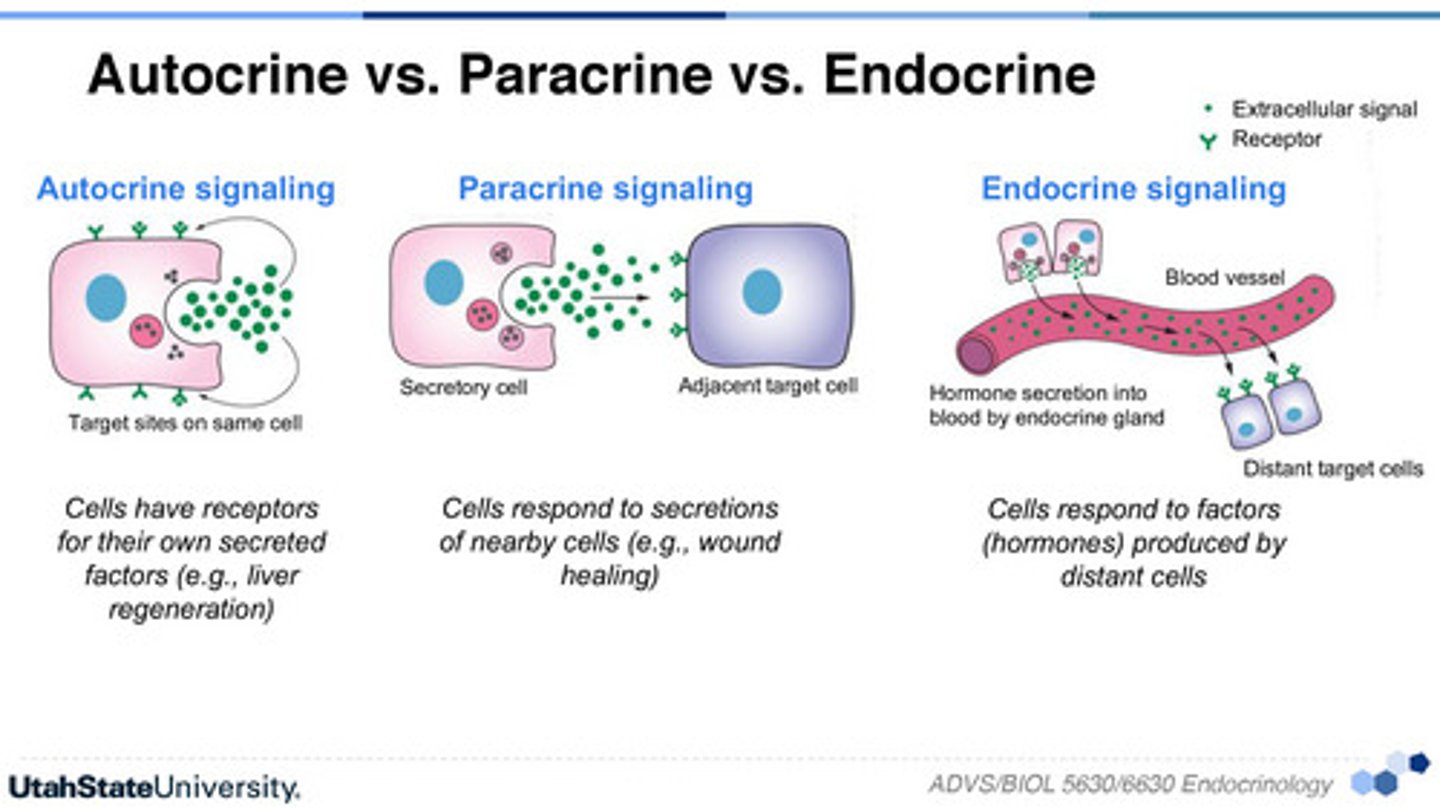
Autocrines
Local chemical messengers that exert effects on the same cells that secrete them.
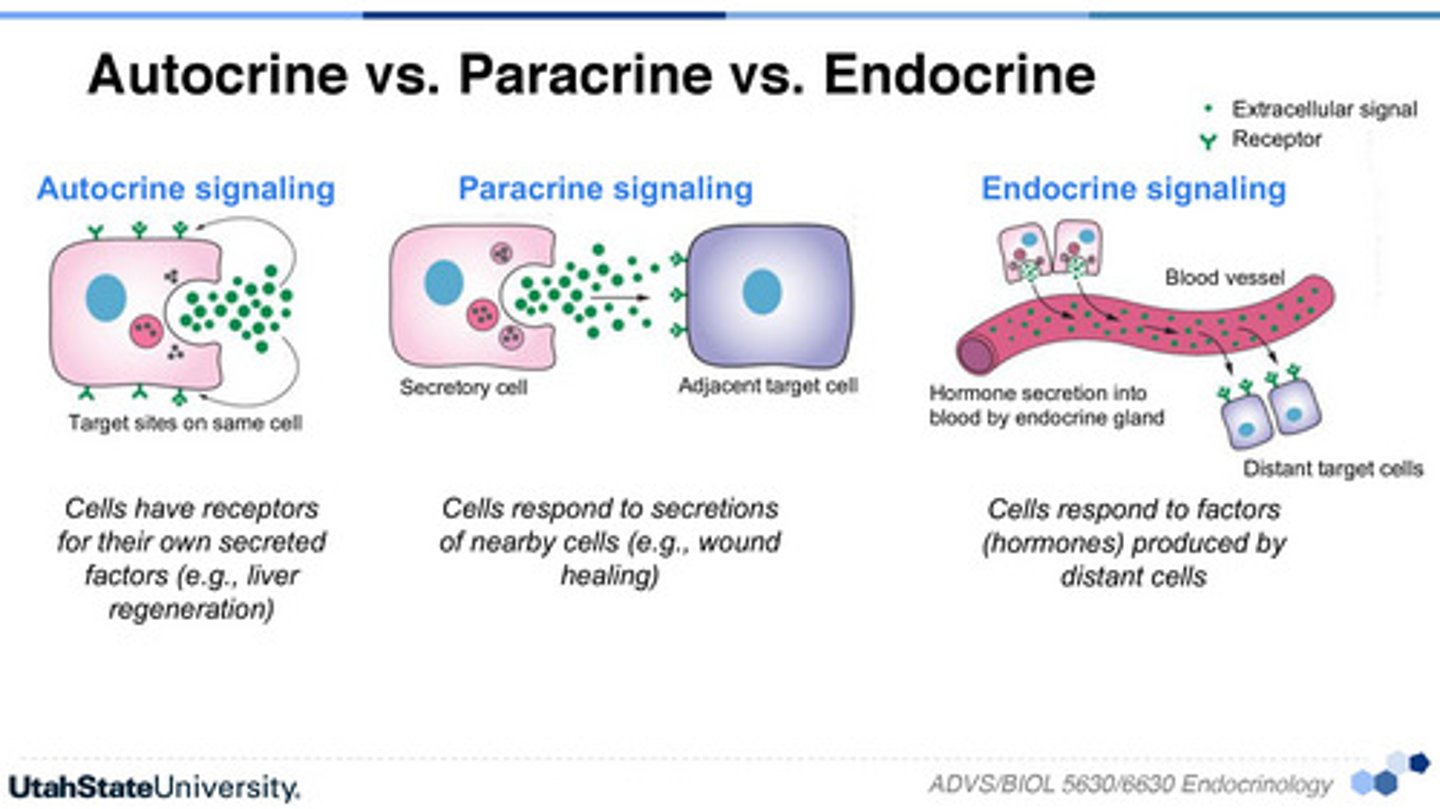
Paracrines
Local chemical messengers that affect neighboring cells.
Amino acid-based hormones
Water-soluble hormones (except thyroxine) that include derivatives, peptides, and proteins; they cannot cross the plasma membrane.
Steroid hormones
Lipid-soluble hormones synthesized from cholesterol that can cross the plasma membrane; includes gonadal and adrenocortical hormones.
Target cells
Tissue cells that possess specific receptors for a particular hormone.
Hormone-induced target cell changes
Altered membrane permeability/potential, protein synthesis, enzyme activation/deactivation, secretory activity, and mitosis stimulation.
Water-soluble hormone mechanism
Act on plasma membrane receptors and are usually coupled via G proteins to second messengers like cyclic AMP.
Lipid-soluble hormone mechanism
Diffuse across the plasma membrane to act on intracellular receptors that directly activate genes and trigger protein synthesis.
Negative feedback mechanism
A stimulus triggers hormone secretion; rising hormone levels then inhibit further release to keep levels within a narrow range.
Humoral stimuli
Changing blood levels of ions and nutrients directly stimulate hormone release (e.g., low calcium stimulating PTH).
Neural stimuli
Nerve fibers stimulate hormone release (e.g., sympathetic fibers stimulating the adrenal medulla).
Hormonal stimuli
Hormones stimulate other endocrine organs to release their hormones
(e.g., hypothalamic hormones regulating the anterior pituitary).
Nervous system modulation
The nervous system can override normal endocrine controls, such as raising blood glucose during severe stress.
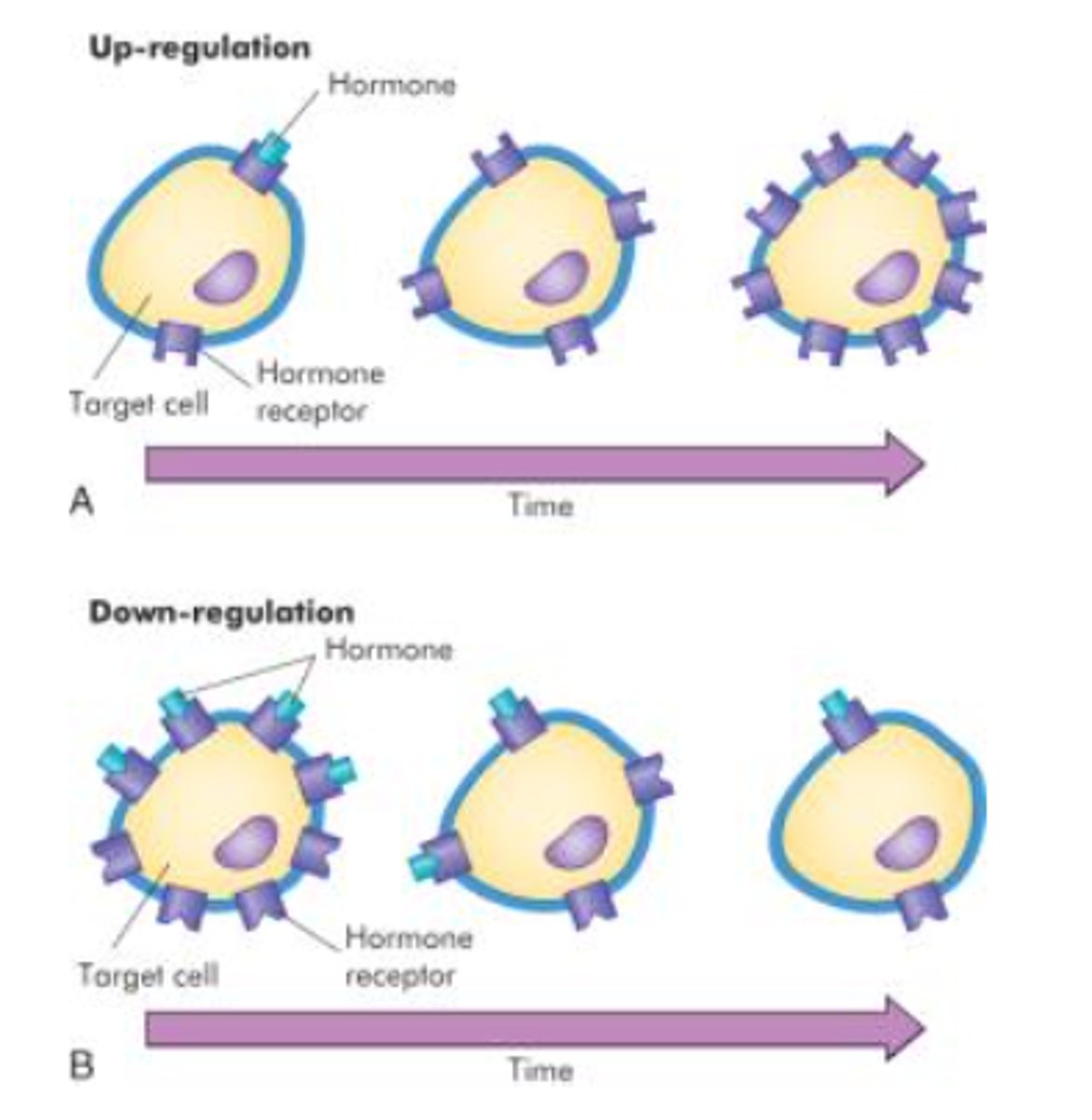
Up-regulation
Target cells add more receptors in response to persistently low hormone levels to increase sensitivity.
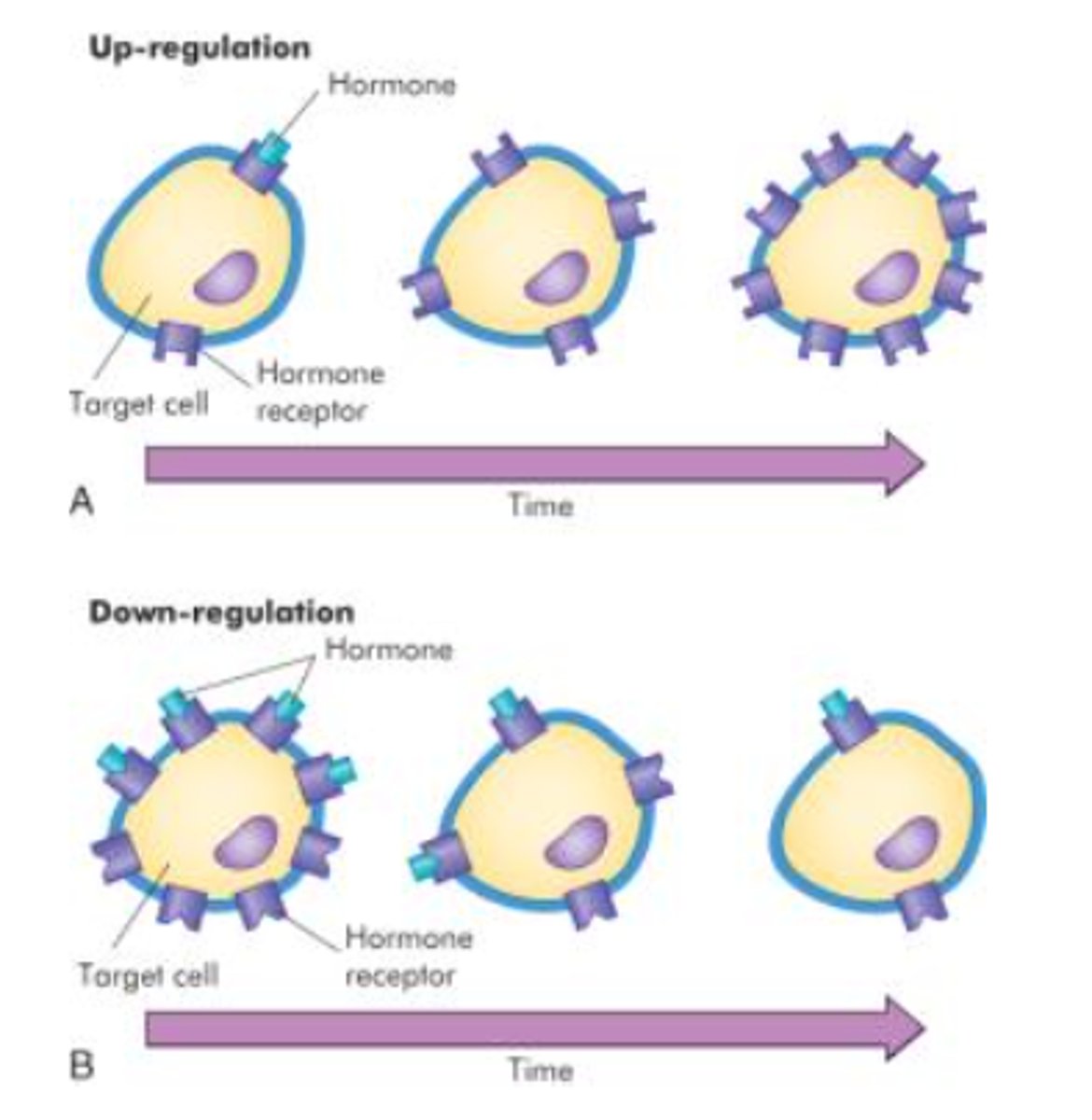
Down-regulation
Target cells remove receptors in response to persistently high hormone levels to prevent overstimulation.
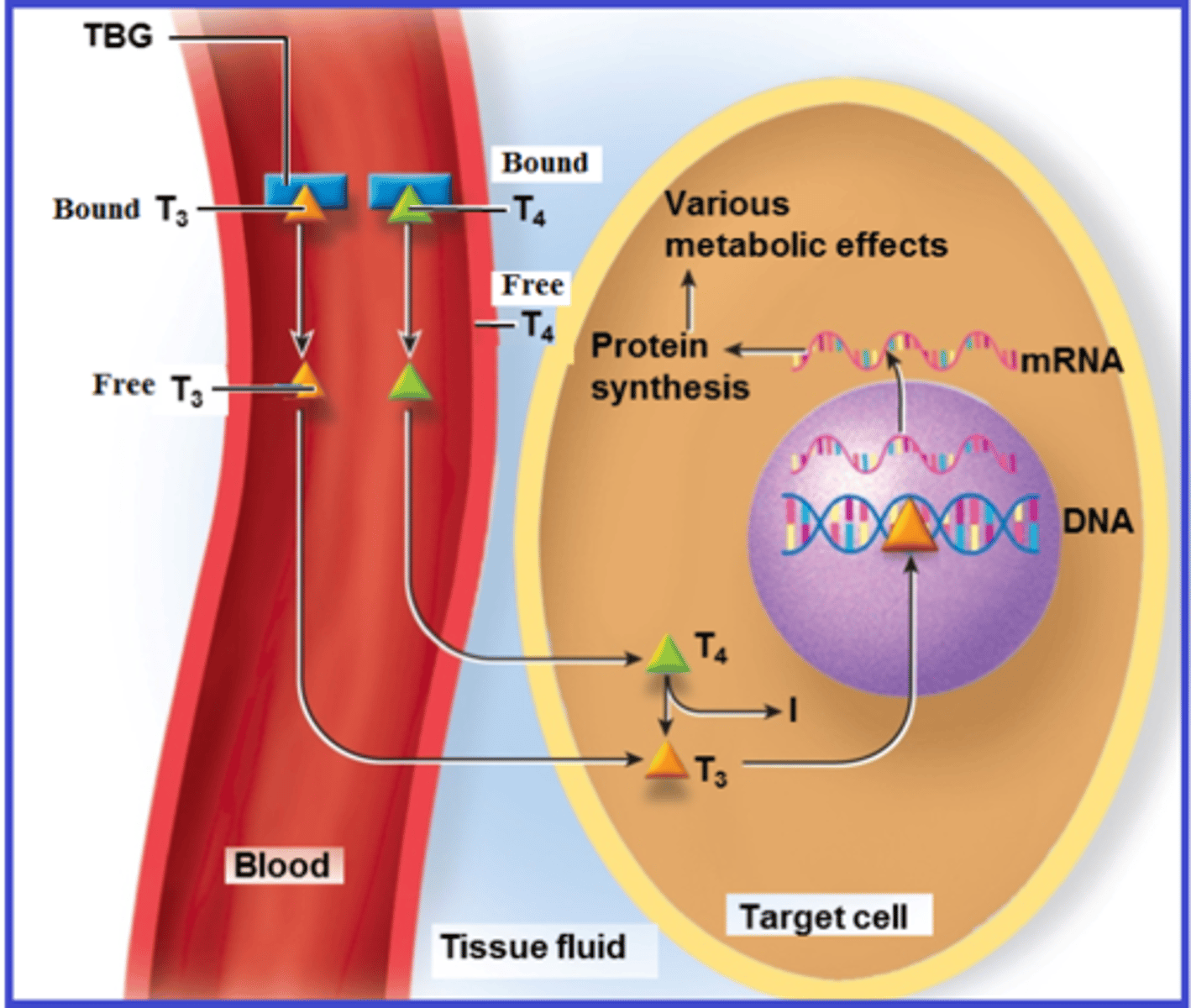
Hormone transport
Steroids and thyroid hormone travel bound to plasma proteins; most others circulate freely.
Half-life
The time required for a hormone's blood level to decrease by half.
Permissiveness
One hormone cannot exert its full effects without another hormone being present (e.g., reproductive hormones needing thyroid hormone).
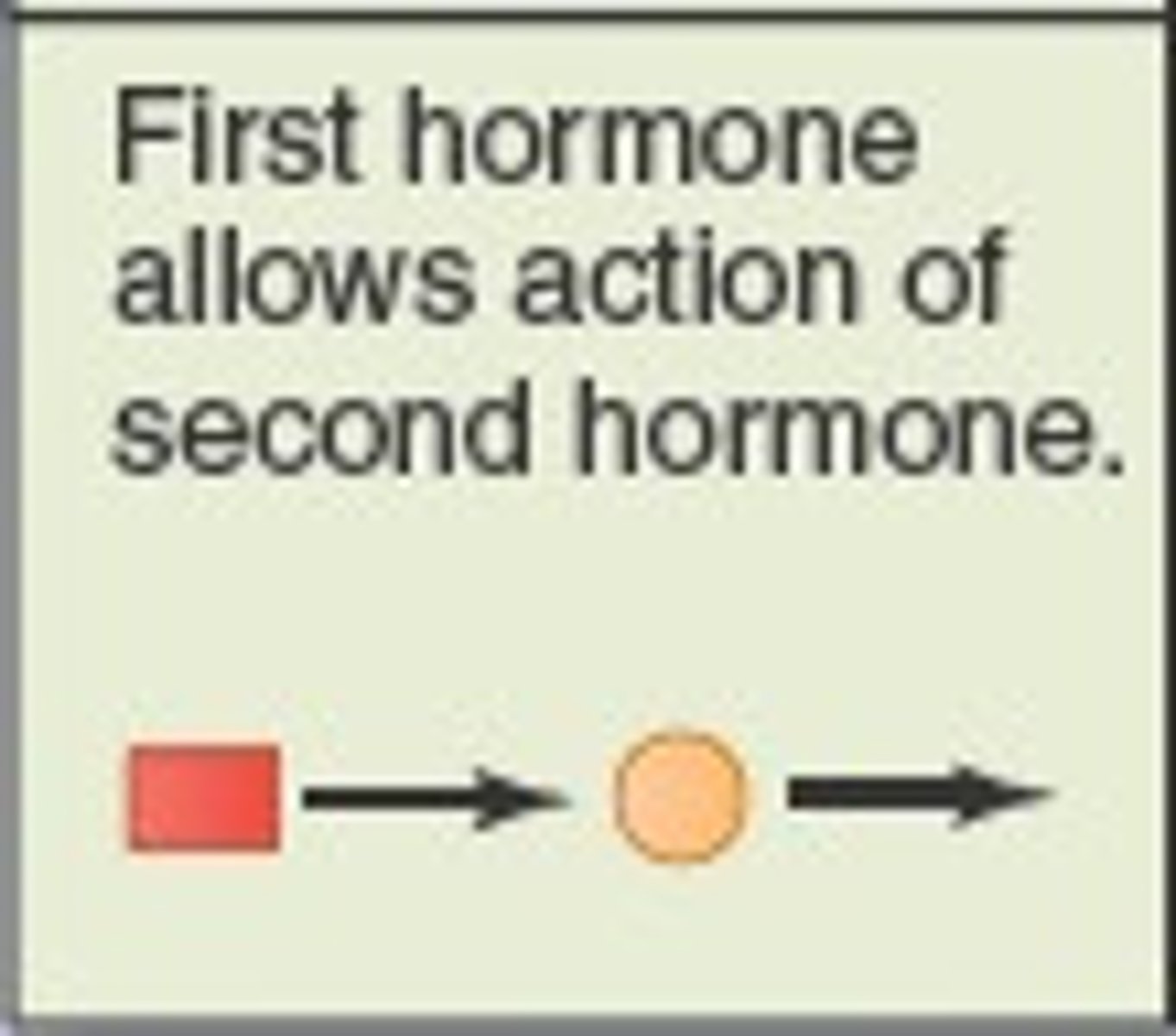
Synergism
More than one hormone produces the same effects, and their combined effects are amplified (e.g., glucagon and epinephrine).
Antagonism
One or more hormones oppose the action of another hormone (e.g., insulin and glucagon).
Posterior pituitary (neurohypophysis)
Composed of neural tissue; stores and secretes oxytocin and ADH produced by the hypothalamus.
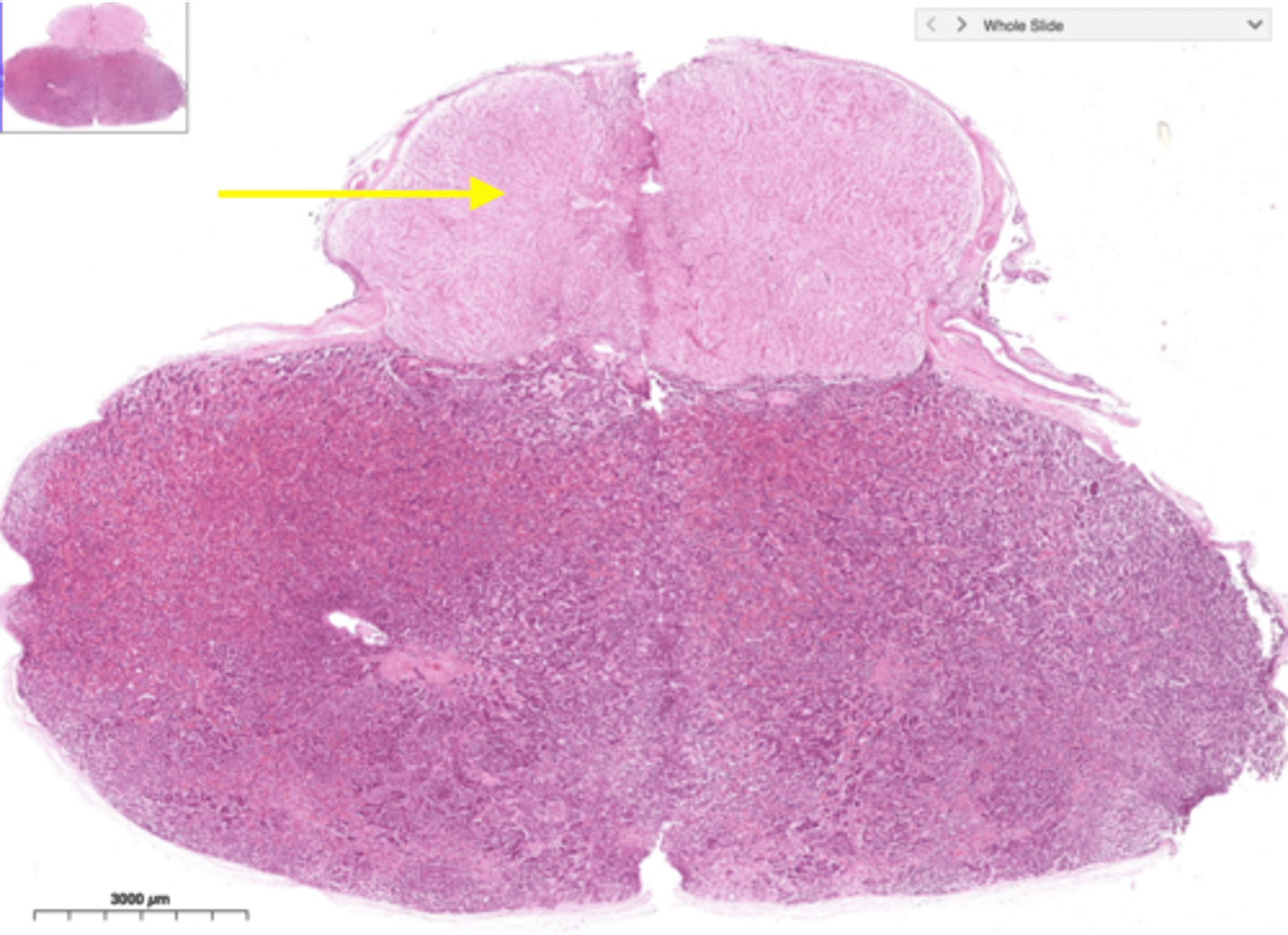
Anterior pituitary (adenohypophysis)
Glandular tissue that manufactures and secretes GH, TSH, ACTH, FSH, LH, and PRL.
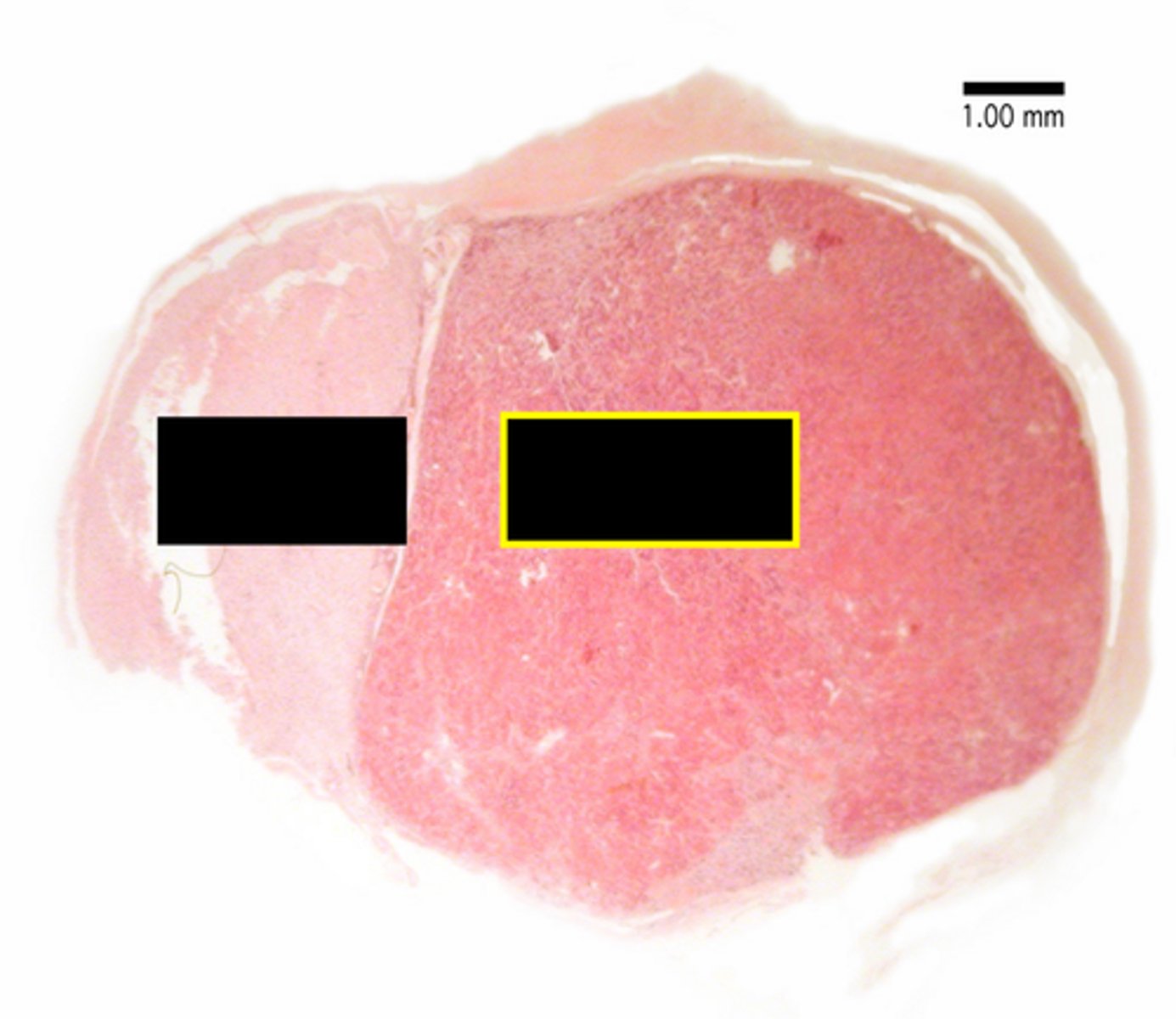
Hypophyseal portal system
The vascular connection between the hypothalamus and anterior pituitary used to transport releasing and inhibiting hormones.
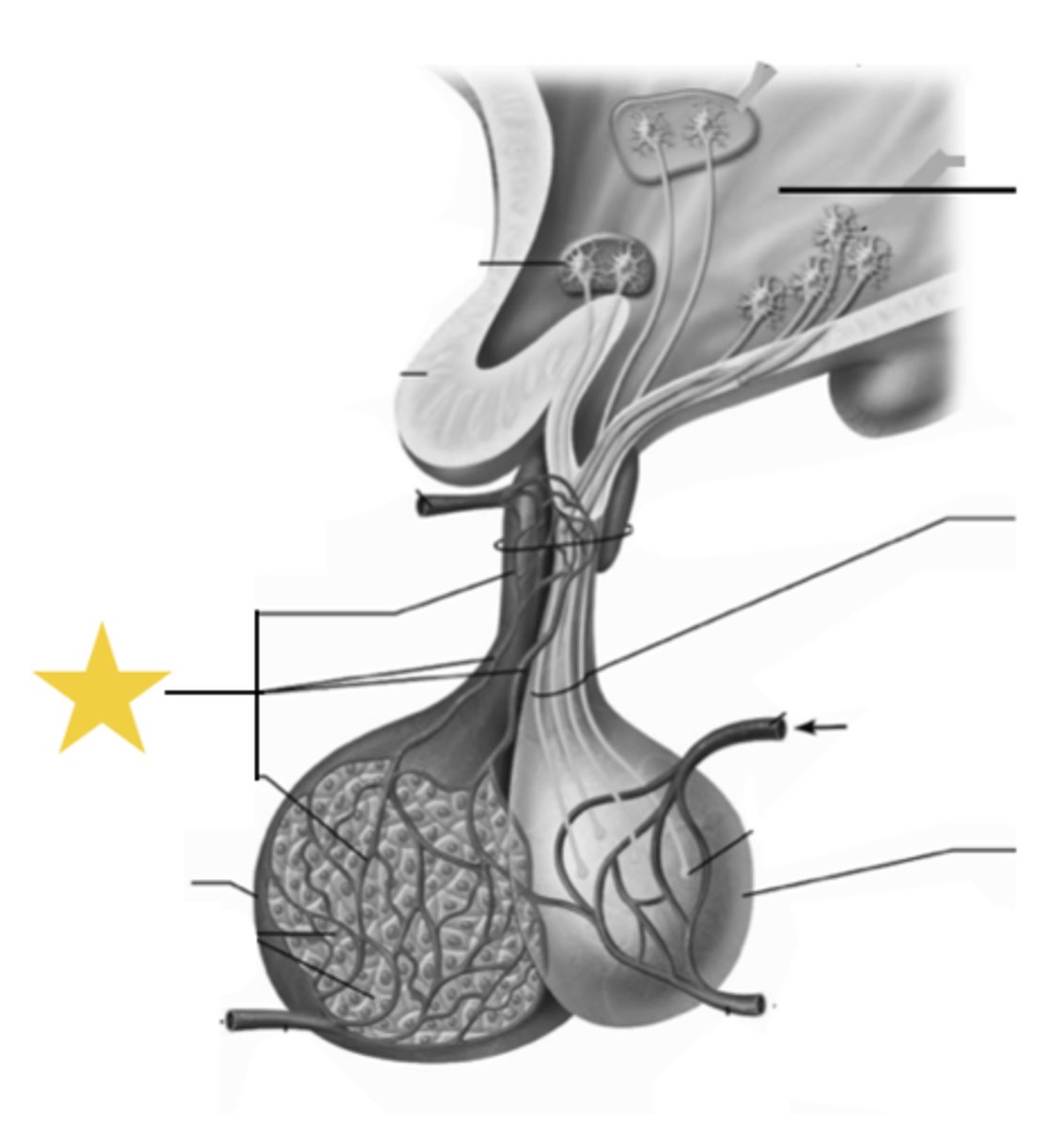
Oxytocin
Peptide that stimulates uterine contractions during labor and triggers milk ejection during breastfeeding; acts via positive feedback.
Antidiuretic hormone (ADH/Vasopressin)
Peptide that signals kidneys to reabsorb water to reduce blood osmolarity; inhibited by alcohol.
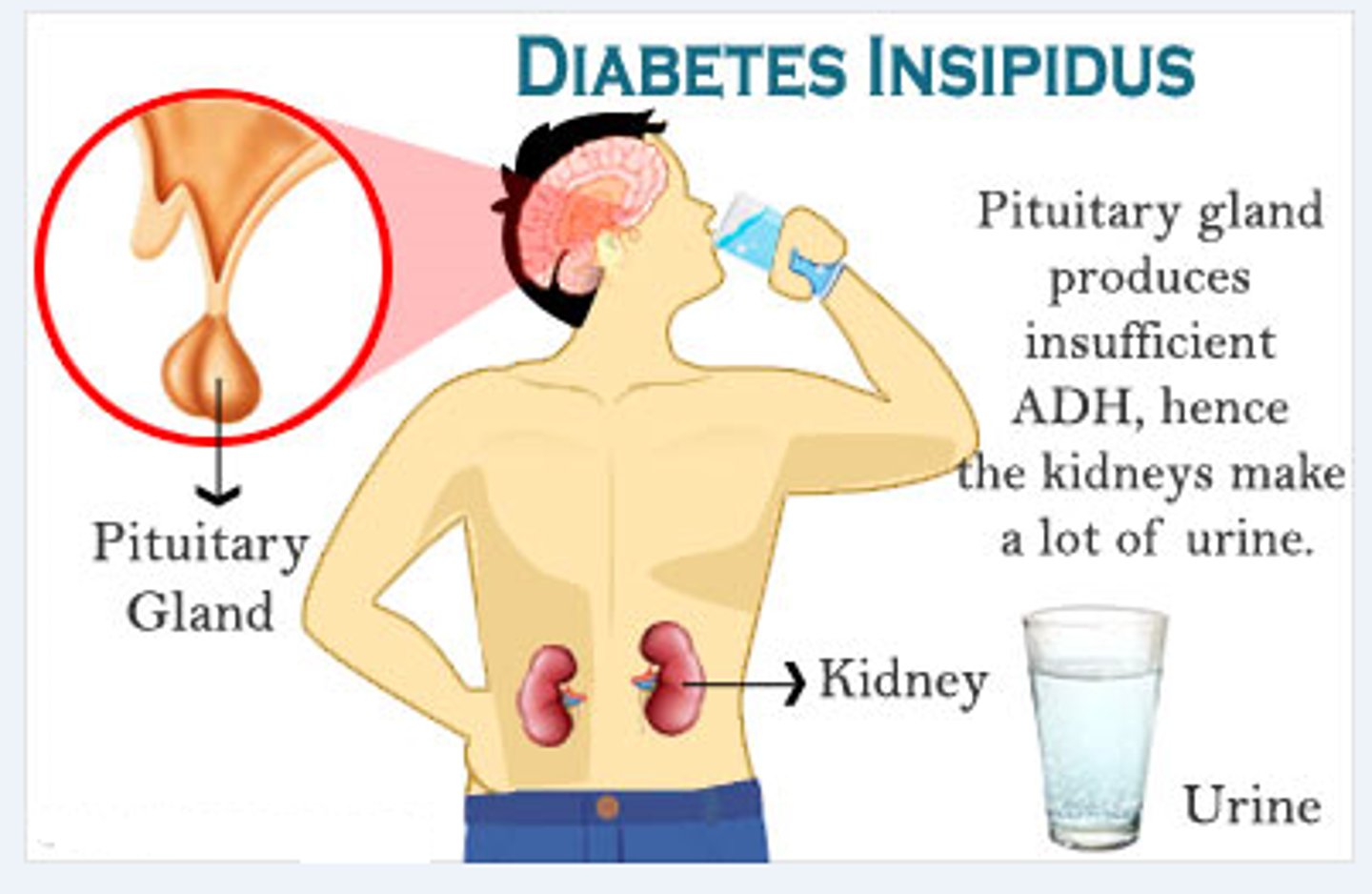
Diabetes insipidus
Condition caused by ADH deficiency, leading to intense thirst and huge urine output.
Growth Hormone (GH)
Anabolic hormone that stimulates somatic growth and mobilizes fats; regulated by GHRH and GHIH.
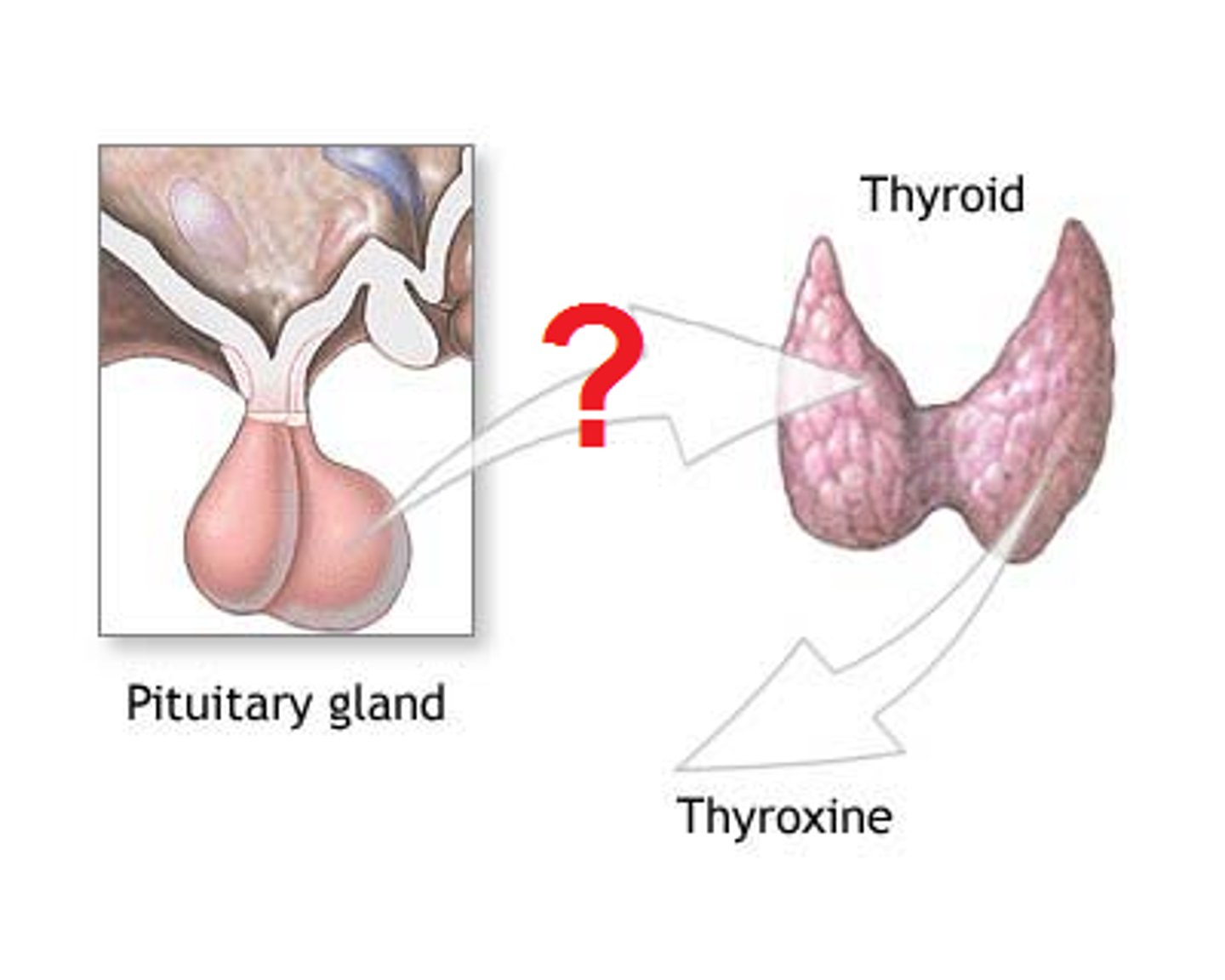
Thyroid-stimulating hormone (TSH)
Stimulates the thyroid gland to release thyroid hormones; triggered by hypothalamic TRH.
Adrenocorticotropic hormone (ACTH)
Stimulates the adrenal cortex to release glucocorticoids to help resist stress; triggered by hypothalamic CRH.
Follicle-stimulating hormone (FSH)
Stimulates production of gametes (eggs or sperm).
Luteinizing hormone (LH)
Triggers ovulation and ovarian hormone production in females; promotes testosterone production in males.
Prolactin (PRL)
Protein hormone that promotes lactation; inhibited by dopamine (PIH).
Thyroid hormone (TH)
Includes T4 (thyroxine) and T3 (triiodothyronine); lipid-soluble amine that increases metabolic rate and heat production.
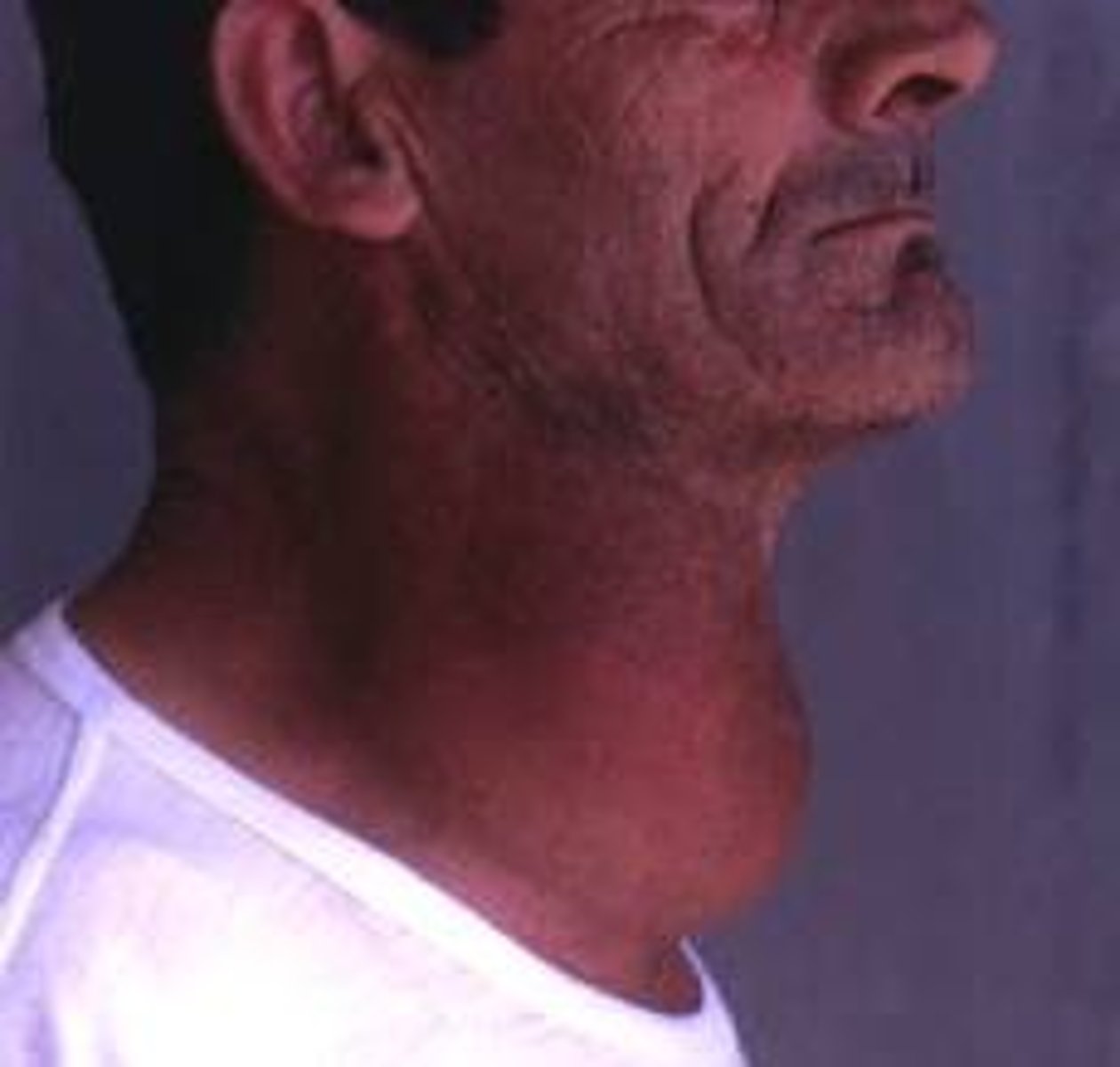
Goiter
Enlargement of the thyroid gland often caused by a lack of iodine.
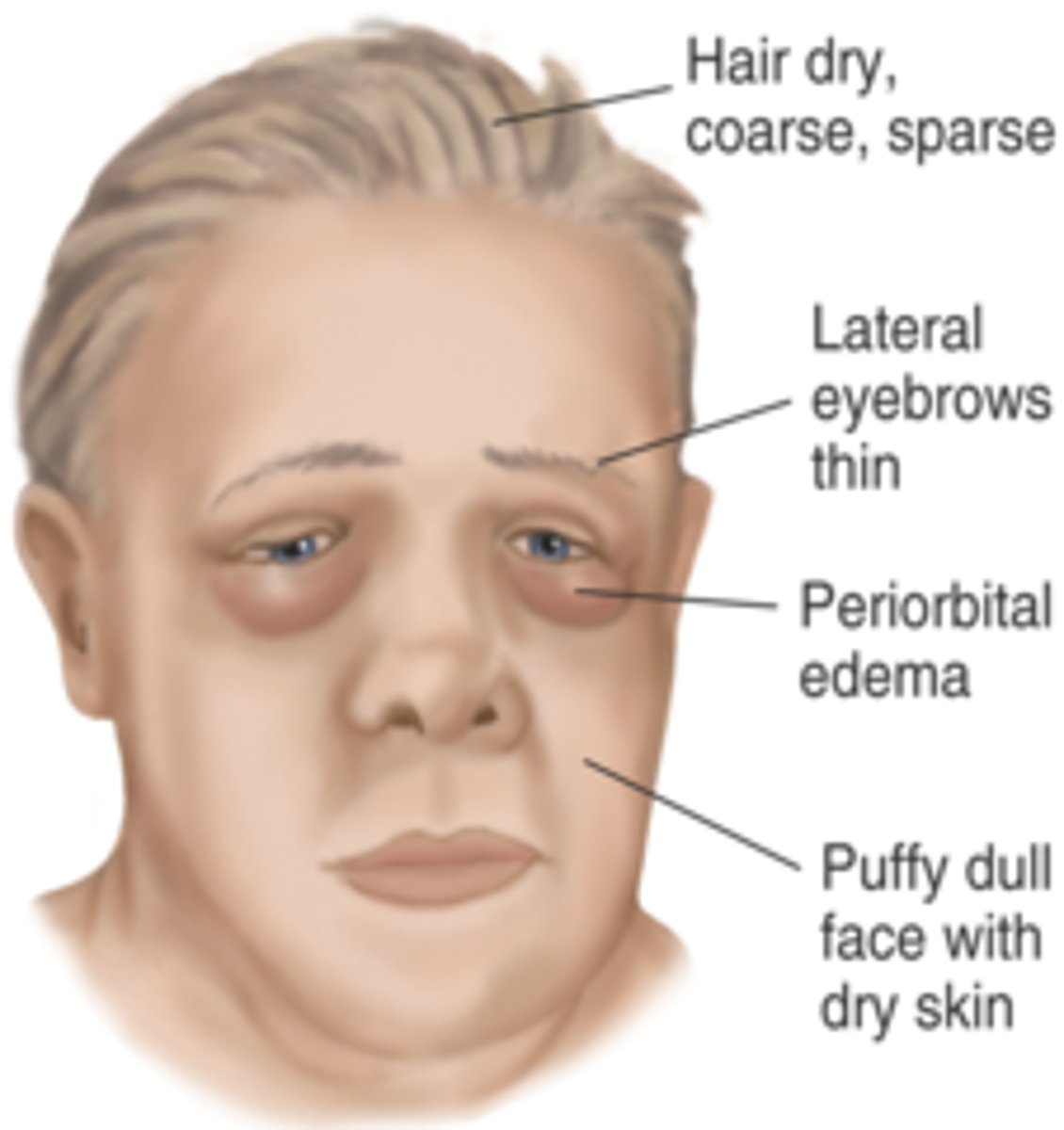
Myxedema
Full-blown hypothyroid syndrome in adults characterized by low metabolic rate, chilled feeling, and mental sluggishness.
Graves' disease
Autoimmune hyperthyroidism where antibodies mimic TSH, leading to elevated metabolism, sweating, and rapid heart rate.
Calcitonin
Hormone produced by parafollicular cells that inhibits osteoclast activity and stimulates calcium uptake into bone at high doses.
Parathyroid hormone (PTH)
The most important hormone for calcium homeostasis; stimulates osteoclasts and enhances calcium reabsorption by kidneys.
Adrenal cortex
Outer glandular region producing mineralocorticoids, glucocorticoids, and gonadocorticoids.
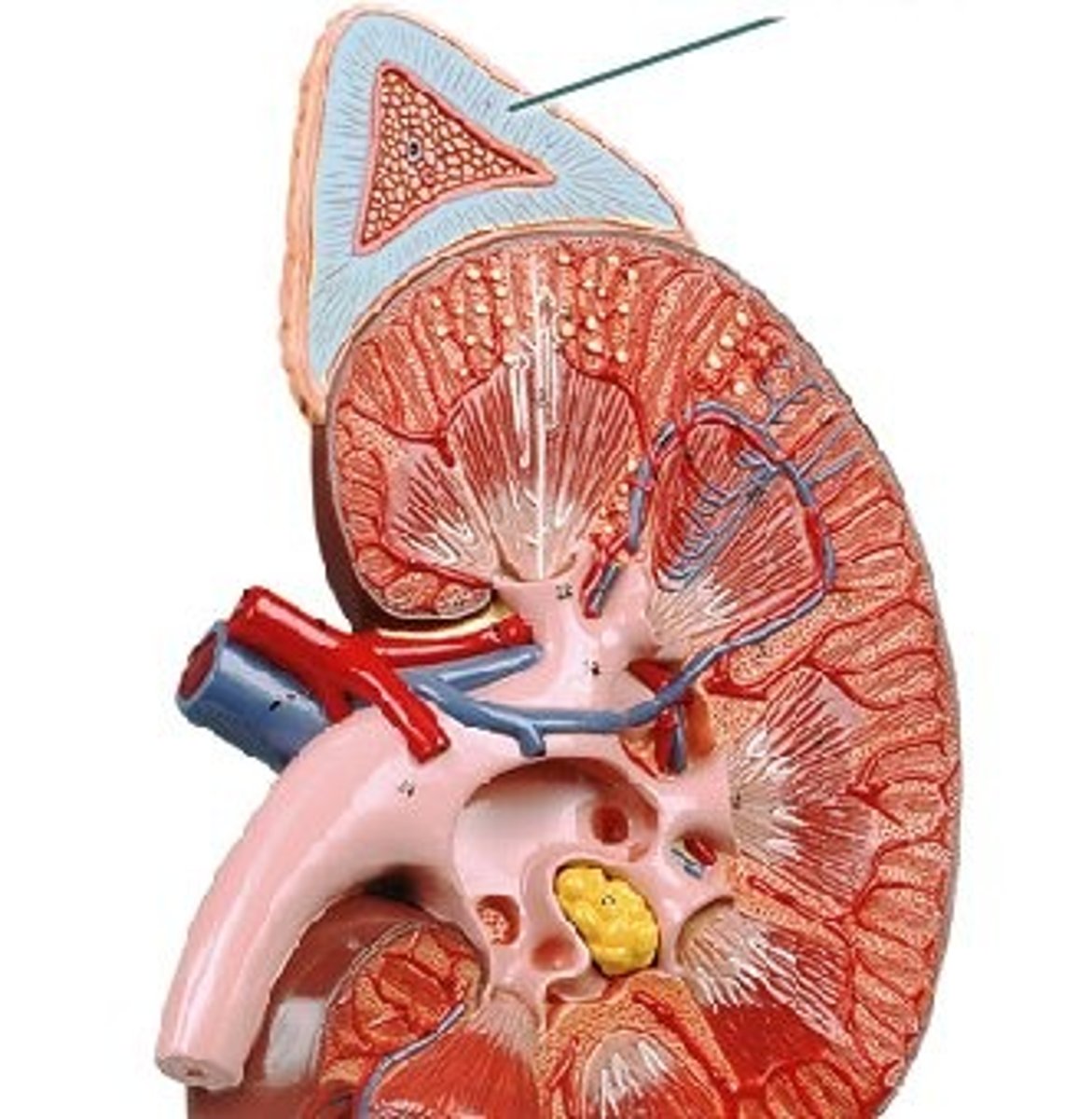
Adrenal medulla
Inner nervous tissue region secreting epinephrine and norepinephrine during "fight-or-flight".
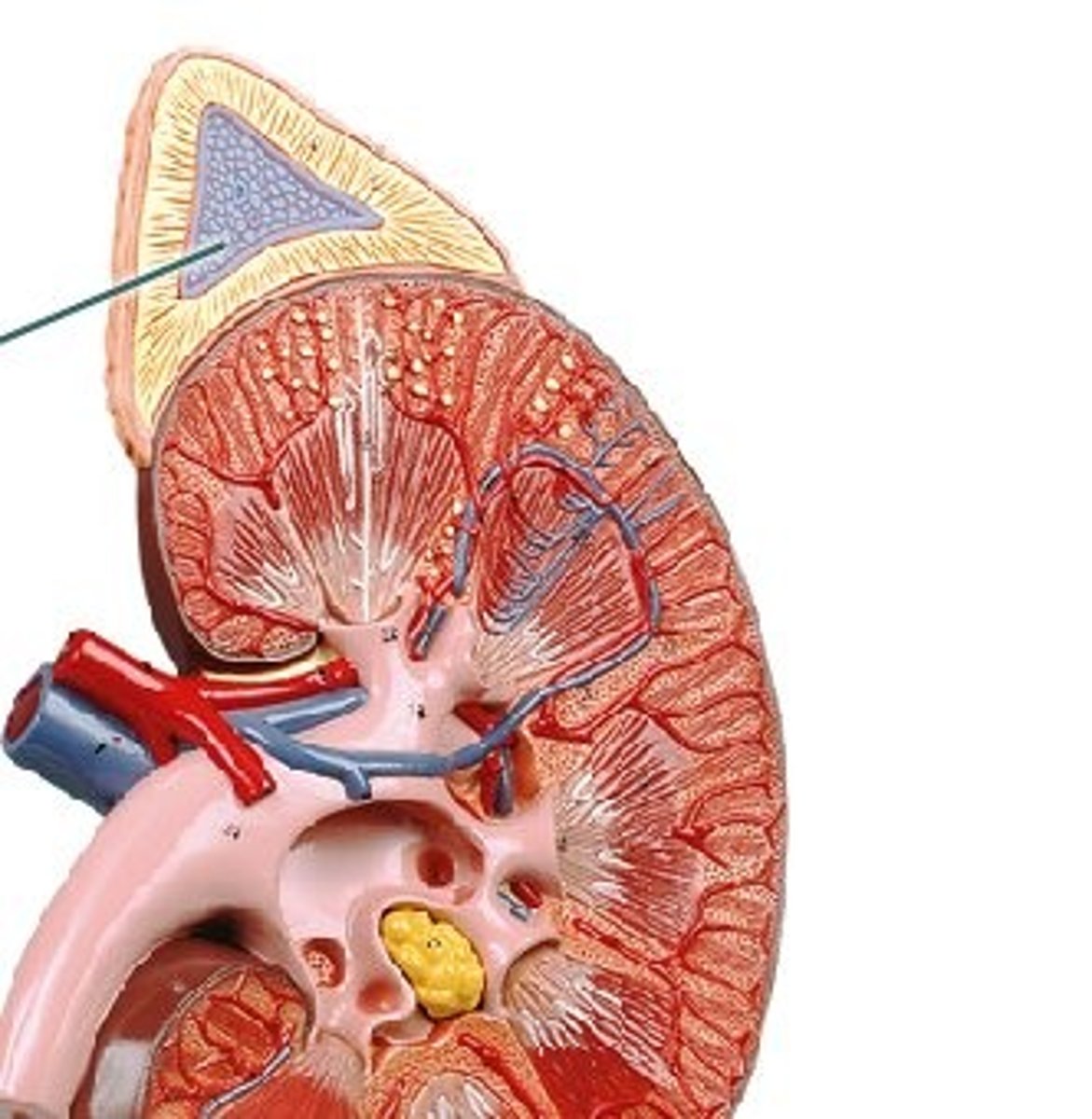
Aldosterone
Primary mineralocorticoid that stimulates sodium reabsorption and potassium excretion by the kidneys to regulate blood pressure.
Renin-angiotensin-aldosterone system
Mechanism where low blood pressure triggers renin release, leading to aldosterone secretion and blood pressure increase.
Atrial natriuretic peptide (ANP)
Hormone secreted by the heart that blocks renin and aldosterone to decrease blood pressure.
Cortisol
Primary glucocorticoid that increases blood glucose (gluconeogenesis) and helps the body resist stressors.
Cushing's syndrome
Condition caused by glucocorticoid excess, leading to "moon face," "buffalo hump," and high blood glucose.
Addison's disease
Hyposecretory disorder of the adrenal cortex involving deficits in both glucocorticoids and mineralocorticoids.
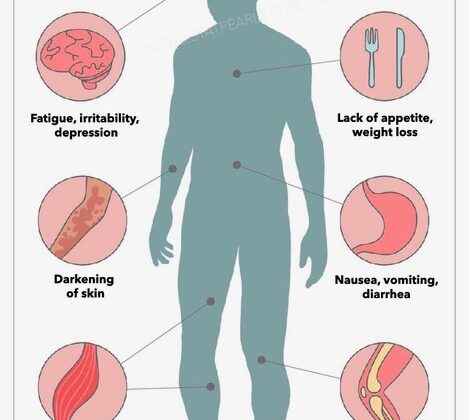
Androgens
Weak male sex hormones (like DHEA) from the adrenal cortex; contribute to female libido and secondary sex characteristics.
Epinephrine and Norepinephrine
Catecholamines that increase heart rate, metabolic rate, and blood pressure during short-term stress.
Melatonin
Hormone from the pineal gland that regulates the sleep-wake cycle and acts as an antioxidant.
Glucagon
Hyperglycemic hormone from pancreatic alpha cells that raises blood glucose by stimulating glycogenolysis and gluconeogenesis.
Insulin
Hypoglycemic hormone from pancreatic beta cells that lowers blood glucose by enhancing membrane transport into cells.
Diabetes mellitus (DM)
Disease resulting from insulin hyposecretion (Type 1) or hypoactivity (Type 2).
Three cardinal signs of DM
Polyuria (huge urine output),
polydipsia (excessive thirst),
polyphagia (excessive hunger).

Ketosis
Accumulation of ketone bodies in the blood due to excessive fat metabolism, which can lead to life-threatening ketoacidosis.
Estrogen and Progesterone
Steroid hormones from ovaries responsible for female reproductive organ maturation and the menstrual cycle.
Testosterone
Primary male androgen responsible for reproductive organ maturation, sperm production, and sex drive.
Leptin
Hormone produced by adipose tissue that suppresses appetite and increases energy expenditure.
Erythropoietin (EPO)
Glycoprotein from the kidneys that stimulates red blood cell production in response to hypoxia.
Osteocalcin
Peptide from bone that increases insulin production and sensitivity.
Cholecalciferol
Vitamin D3 precursor produced by the skin; activated by kidneys to help absorb dietary calcium.
Thymulin, thymopoietins, thymosins
Peptides from the thymus involved in T lymphocyte development and immune responses.
Signal strength coding
The nervous system codes signal strength by the frequency of action potentials, while the endocrine system codes it by the concentration of hormone.
Autocrines and paracrines classification
These are considered local chemical messengers and are typically not classified as part of the endocrine system because they do not travel long distances in the blood.
Eicosanoids
A possible third class of hormones, though most scientists classify them as paracrines or autocrines due to their highly localized effects.
Factors for target cell activation
Activation depends on
-blood levels of the hormone
-the relative number of receptors on the target cell
-and the affinity (binding strength) between the hormone and receptor.
Hormone inactivation and removal
Hormones are removed from the blood by degrading enzymes in target tissues, or more commonly by the liver or kidneys.
Hypothalamic-hypophyseal tract
A bundle of axons that connects the hypothalamus to the posterior pituitary, arising from the paraventricular and supraoptic nuclei.
Paraventricular nuclei
Hypothalamic nuclei that primarily produce the hormone oxytocin.
Supraoptic nuclei
Hypothalamic nuclei that primarily produce antidiuretic hormone (ADH).
Vasopressin
An alternative name for antidiuretic hormone (ADH) because it causes vasoconstriction at high concentrations.
SIADH (Syndrome of Inappropriate ADH Secretion)
A condition of ADH hypersecretion characterized by fluid retention, headache, and disorientation.
Tropic hormones (tropins)
Hormones that regulate the secretory activity of other endocrine glands
(TSH, ACTH, FSH, and LH)
GH direct metabolic actions
Increases blood glucose (anti-insulin effect) and mobilizes fats for use as fuel (lipolysis).
GH indirect growth actions
Mediated by insulin-like growth factors (IGFs), which stimulate the uptake of nutrients for DNA/protein synthesis and bone matrix deposition.
Gigantism
Hypersecretion of growth hormone in children with active growth plates.
Acromegaly
Hypersecretion of growth hormone in adults, leading to the thickening of bones in the hands, feet, and face.

Pituitary dwarfism
Hyposecretion of growth hormone in children, resulting in slow long bone growth.

Pro-opiomelanocortin (POMC)
The large precursor molecule that is split to produce adrenocorticotropic hormone (ACTH).
Gonadotropin functions in females
FSH stimulates follicle maturation and estrogen production; LH triggers ovulation and the formation of the corpus luteum.
Gonadotropin functions in males
FSH stimulates sperm production; LH promotes the production of testosterone.
PIH (Prolactin-Inhibiting Hormone)
A hypothalamic hormone that regulates prolactin secretion, which is actually the neurotransmitter dopamine.
Thyroid follicles
Hollow, colloid-filled spheres formed by follicular cells that produce the glycoprotein thyroglobulin.
Colloid
The amber-colored, sticky fluid in thyroid follicles that contains thyroglobulin with attached iodine atoms.
T4 (Thyroxine)
The major hormone secreted by thyroid follicles, consisting of two tyrosine molecules with four bound iodine atoms.
T3 (Triiodothyronine)
Formed at target tissues by converting T4; it is 10 times more active and consists of two tyrosines with three iodine atoms.