part 2: 744 Clinical Management of Postural Control Slides
1/43
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
44 Terms
examination: impairment level


#1: may hypothesize that impaired anticipatory aspects of postural control may be a contributing factor and choose a test or measure that specifically examines anticipatory aspects of postural control in standing (e.g., stool touch or lean over and pick up a slipper from the floor)
#2: suggests a hypothesis related to sensory components of balance control, specifically difficulty in maintaining balance when visual cues are removed and standing on a reduced slippery surface.
#3: This action typically involves several dynamic head movements with respect to a relatively stable standing position. These functional situations can then be tested specifically, for example, by observing whether the patient increases sway or requires assistance to prevent a fall
evaluation: interpreting results of the examination

movement system diagnoses for balance
Don’t have to memorize but you should be able to easily use this language – you should be able to come up with one of the three categories
If they cant hold SSPC. Why? 4 things in it


#1: may hypothesize that impaired anticipatory aspects of postural control may be a contributing factor and choose a test or measure that specifically examines anticipatory aspects of postural control in standing (e.g., stool touch or lean over and pick up a slipper from the floor)
#2: suggests a hypothesis related to sensory components of balance control, specifically difficulty in maintaining balance when visual cues are removed and standing on a reduced slippery surface.
#3: This action typically involves several dynamic head movements with respect to a relatively stable standing position. These functional situations can then be tested specifically, for example, by observing whether the patient increases sway or requires assistance to prevent a fall
intervention

intervention: task-oriented balance rehabilitation
______
Taking functional level, impairment level, and environment and applying it the the patient case

intervention: task-oriented balance rehabilitation - goals

intervention: motor system - treating underlying motor impairments

intervention - motor system - may be best to focus on ___

intervention - motor system - functional balance training: improving motor strategies: priorities

intervention: motor system: steady-state balance control goal

steady state balance control
These are great “low tech” examples of balance training methods.

steady state balance control: example

intervention - motor system: steady state balance control - research evidence showed significant improvements in ____; what reduce postural sway

effects of holding a cane on COP and BOS
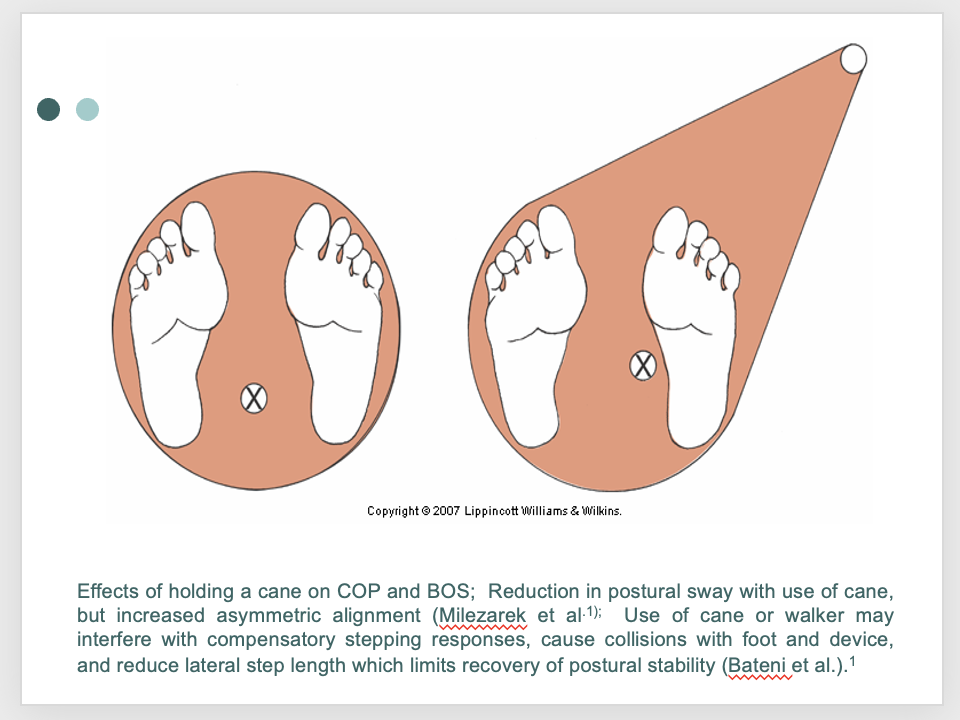
intervention: motor system - retraining reactive balance control - goal
______
The closest you can get to mimicking the reactive type they are stuggling with the better

intervention: motor system - retraining reactive balance control: expose patient to varying ____

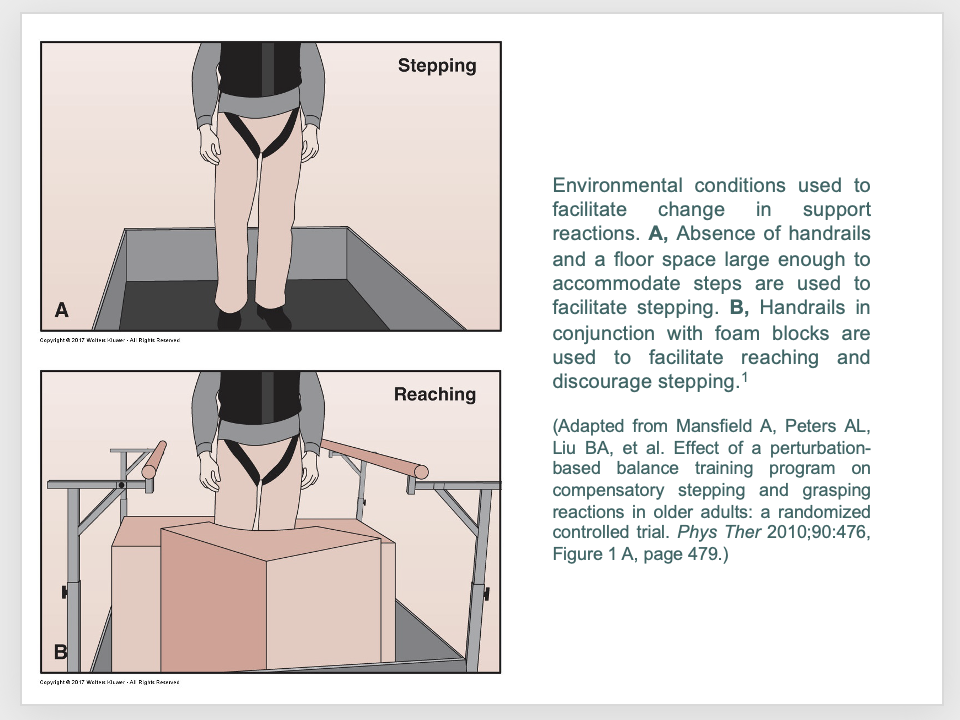
This is a safe way to practice (back into wedge of corner with chair in front
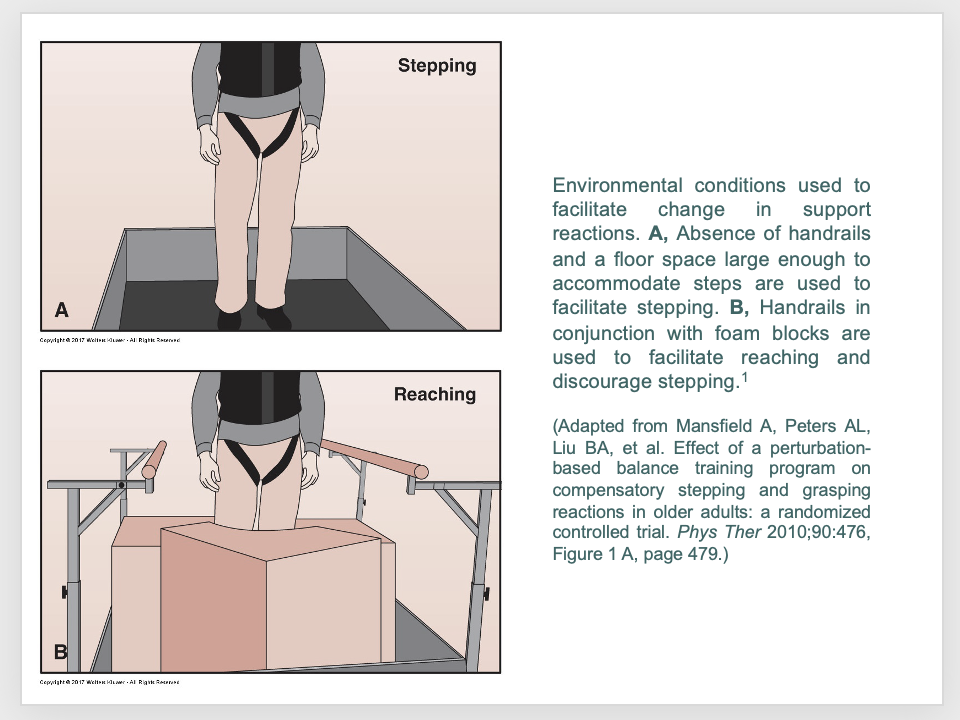
intervention: motor system - retraining reactive balance control: practice what?

intervention: motor system: retraining anticipatory balance control - goal

intervention: motor system: retraining anticipatory balance control - examples

intervention: motor system - training balance in sitting - goal

intervention: sensory systems - treating underlying sensory impairments: goal
intervention: sensory systems - functional balance training: improving sensory strategies goal

intervention: sensory systems - functional balance training: improving sensory strategies: to reduce visual dependence
__________
Idea with goggles: reduce vision but not eliminate it (easier then just closing eyes)
If someone is visual dependent – you have to reduce the thing they are dependent on
If the patient who has visual dependence and the sensory or vestibular are IMPAIRED do NOT do this – they need vision to be able to function

intervention: sensory systems - functional balance training: improving sensory strategies: to reduce somatosensory dependence
If they are relying on somatosensory all the time even when thy shouldn’t – reweight them ONLY IF they can use vestibular and visual systems

intervention: sensory systems - functional balance training: improving sensory strategies: to improve ability to use vestibular information
To use vestibular more – you have to mess with both vision and sensory systems

intervention: sensory systems - augmenting sensory inputs to improve balance control
Fingers give them proprioception

intervention: sensory systems - augmenting sensory inputs to improve balance control - Adding feedback as auditory, electrotactile

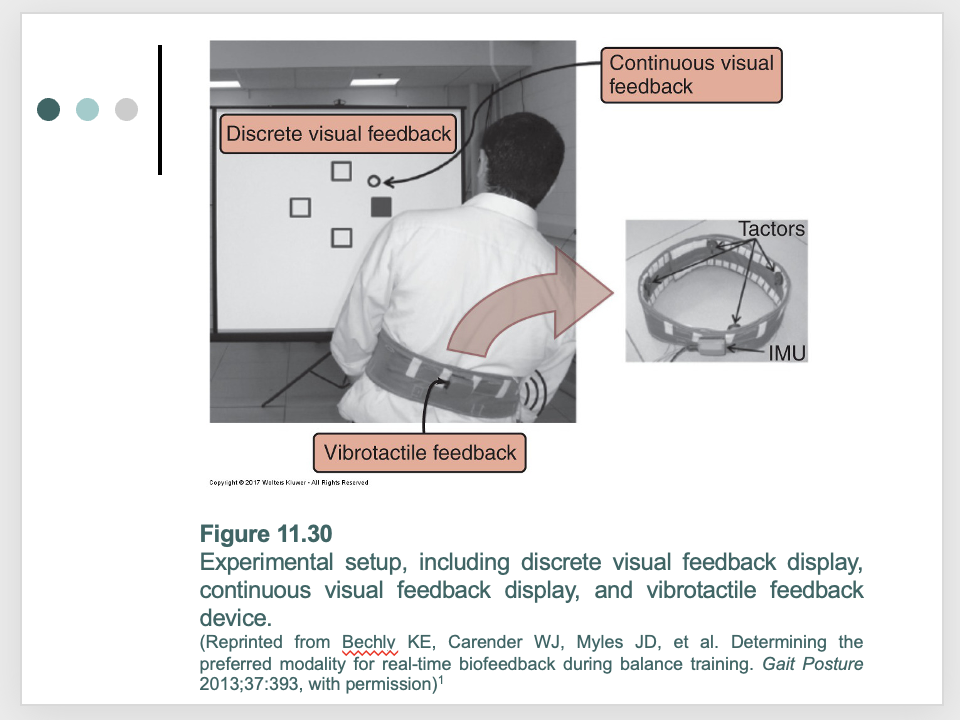
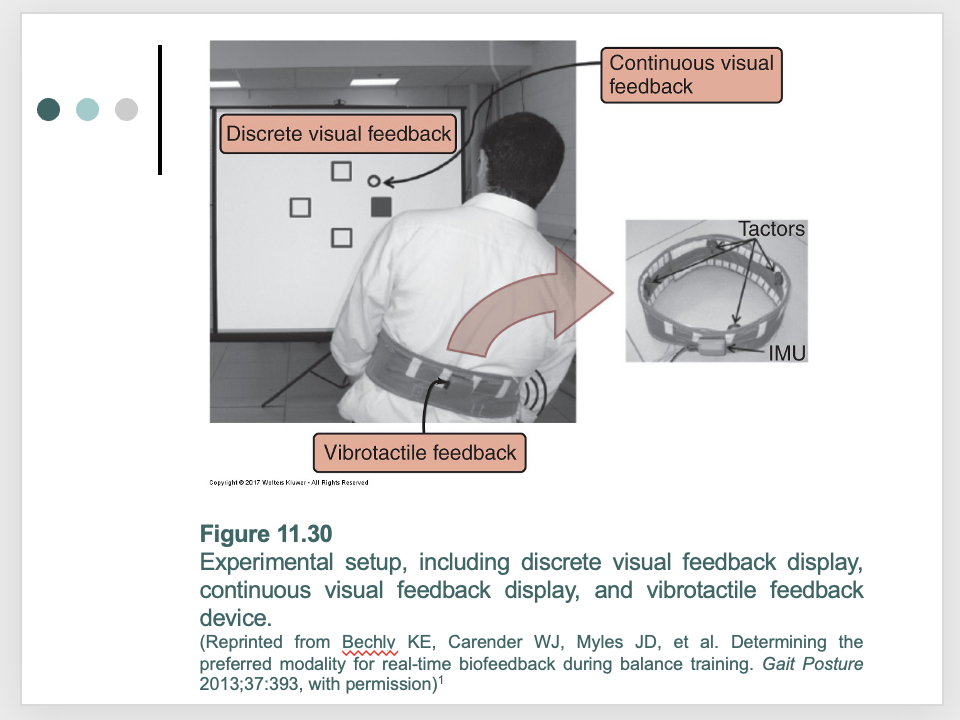
intervention - sensory systems: augmenting sensory inputs to improve balance control: use of vibratory shoe inserts

intervention - sensory systems: augmenting sensory inputs to improve balance control: Is one type of augmented feedback better than another?

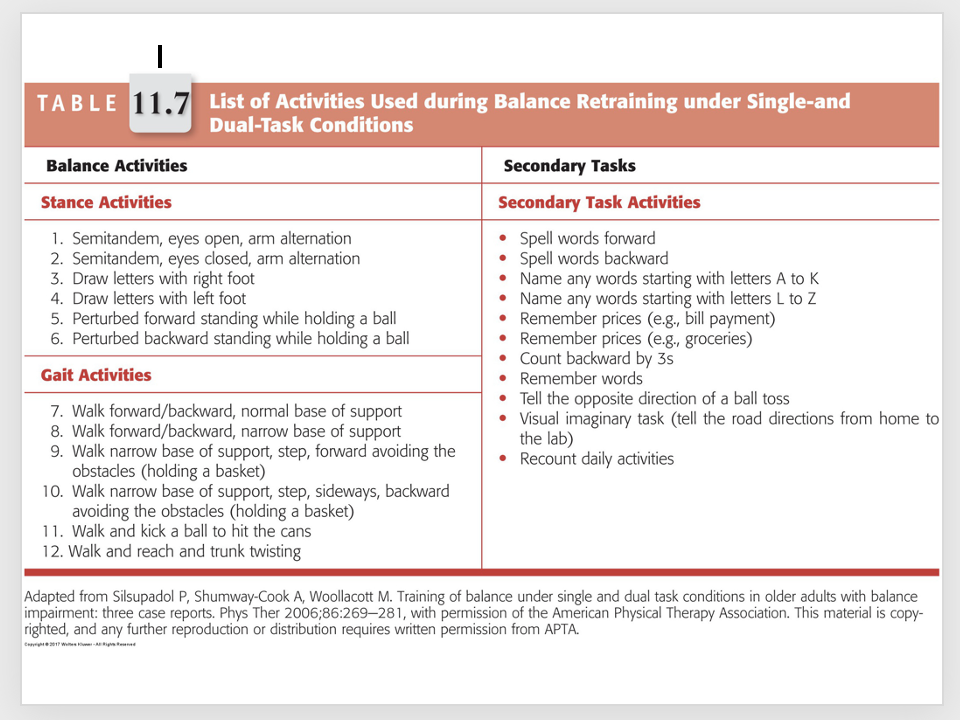
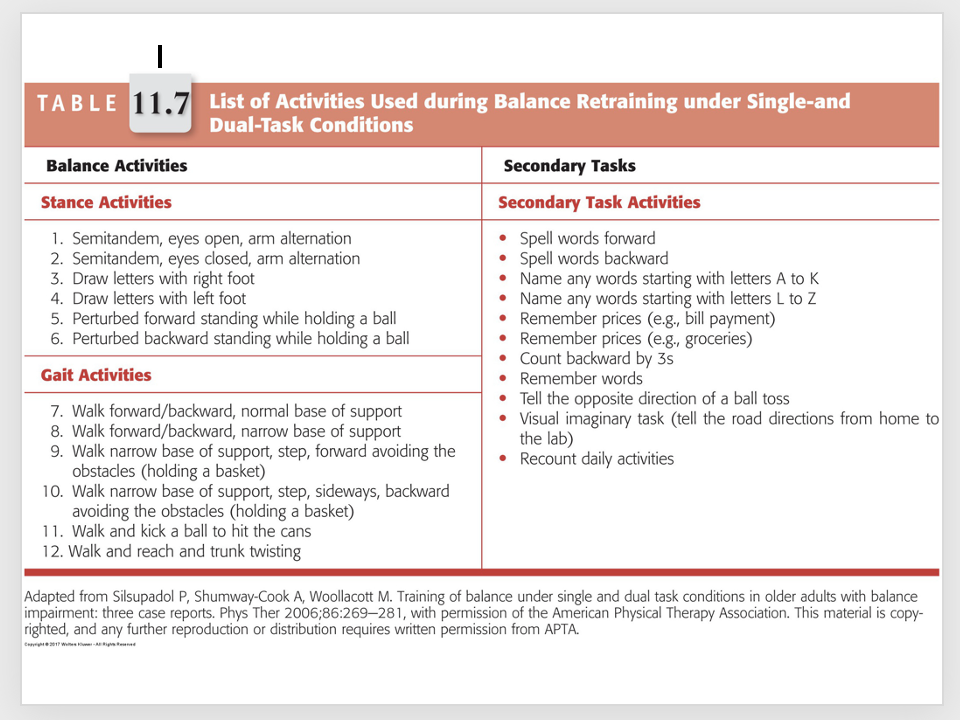
intervention: cognitive systems - training attention in isolation

intervention: cognitive systems - cognitive strategies to improve performance during dual-task conditions


#1: may hypothesize that impaired anticipatory aspects of postural control may be a contributing factor and choose a test or measure that specifically examines anticipatory aspects of postural control in standing (e.g., stool touch or lean over and pick up a slipper from the floor)
#2: suggests a hypothesis related to sensory components of balance control, specifically difficulty in maintaining balance when visual cues are removed and standing on a reduced slippery surface.
#3: This action typically involves several dynamic head movements with respect to a relatively stable standing position. These functional situations can then be tested specifically, for example, by observing whether the patient increases sway or requires assistance to prevent a fall
putting it all together: task specific approach

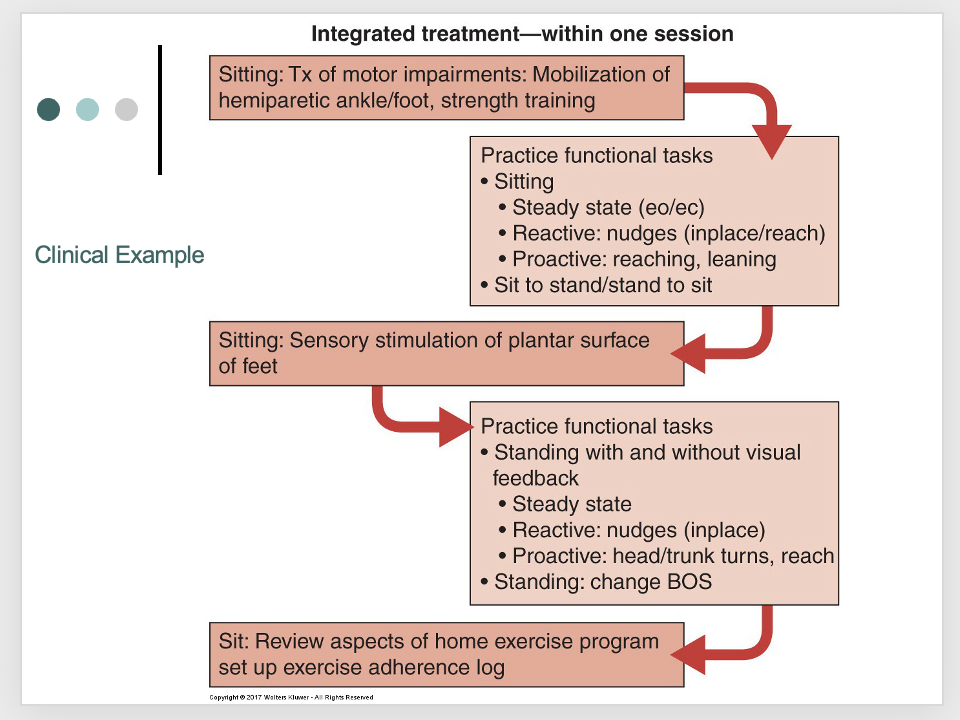
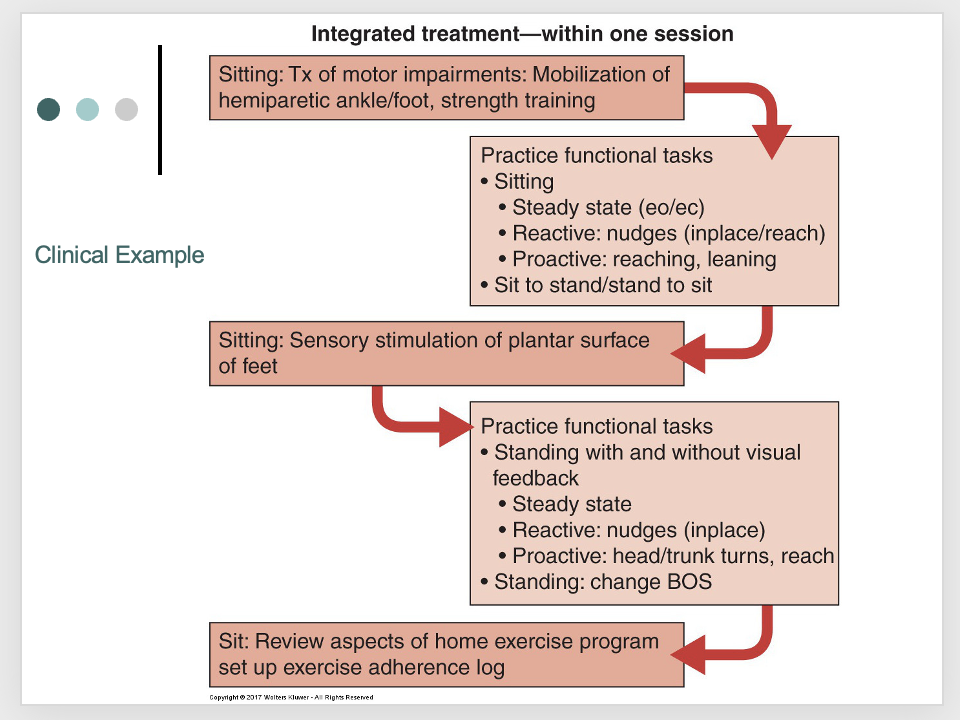
putting it all together: functional task level

provide appropriate feedback
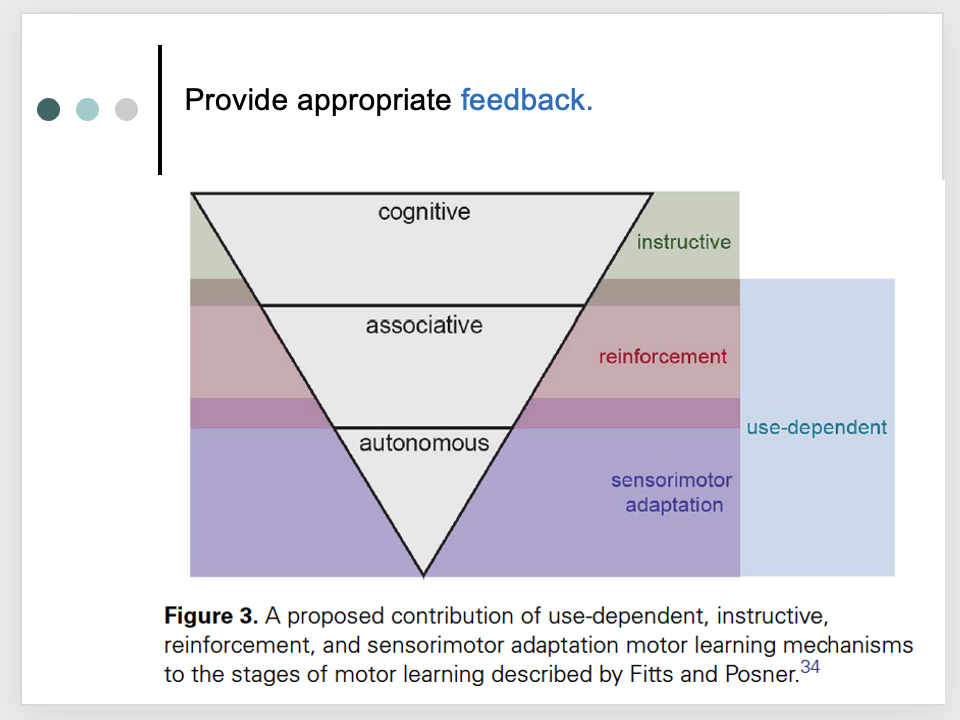
putting it all together: evidence-based fall prevention

promote ML with individualized training
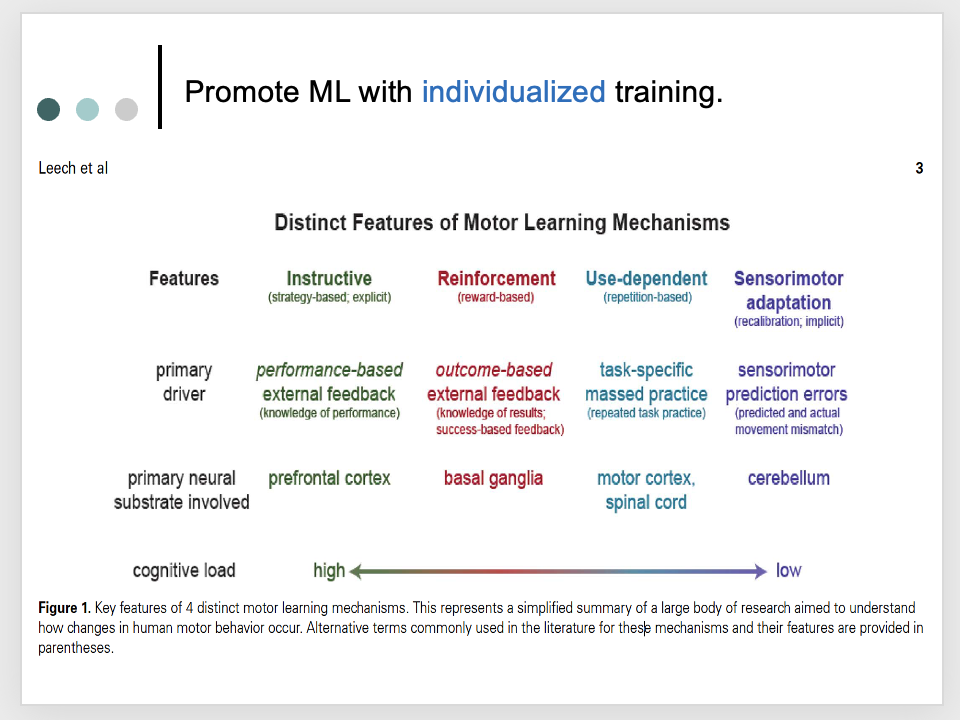
putting it all together: evidence-based fall prevention
