Chapter 14 (Normal Human Microbiota)
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
Symbiosis
the relationship between normal microbiota and the host
Commensalism
one organism benefits and the other is unaffected
mutualism
both organisms benefit
Parasitism
One organism benefits and the other is harmed
microbiome
all of the microorganisms that live in a particular environment, such as a human body
virome
the entire population of viruses associated with the human body
transient microbiota
the microorganisms that are present in an animal for a short time without causing a disease
colonization
the ability of the microbe to stay attached to the body surface and replicate
adhesions
allow microbiota to attach to host cells
Gut-Brain Axis
brain activity alters gut function; gut microbiome can alter nervous system
food digestion, synthesizing vitamins, interfering with pathogen colonization (microbial antagonism), training and enhancing function of the immune system (produce immunomodulins), "Virtual organ system"
benefits of a microbiome:
immunomodulins
modify the secretion of cytokines; regulator
immunocompromised hosts
Individuals with weakened immune systems; susceptible to infection
opportunistic pathogens
cause disease when the host's defenses are compromised or when they grow in part of the body that is not natural to them
dysbiosis
microbial imbalance that causes adverse effects in humans
hygiene hypothesis
suggests that limiting exposure to pathogens may lower immune tolerance and the ability to cope with harmless antigens
Mouth, nose, lung, stomach, intestines, vagina, skin
Major the sites of colonization:
bioburden
number of microorganisms that typically inhabit an environment
The Skin
Acidic, high salt, low moisture, can contain lysozyme, mostly Gram + organisms
ex: Staph. epidermidis; Bacillus spp; yeasts
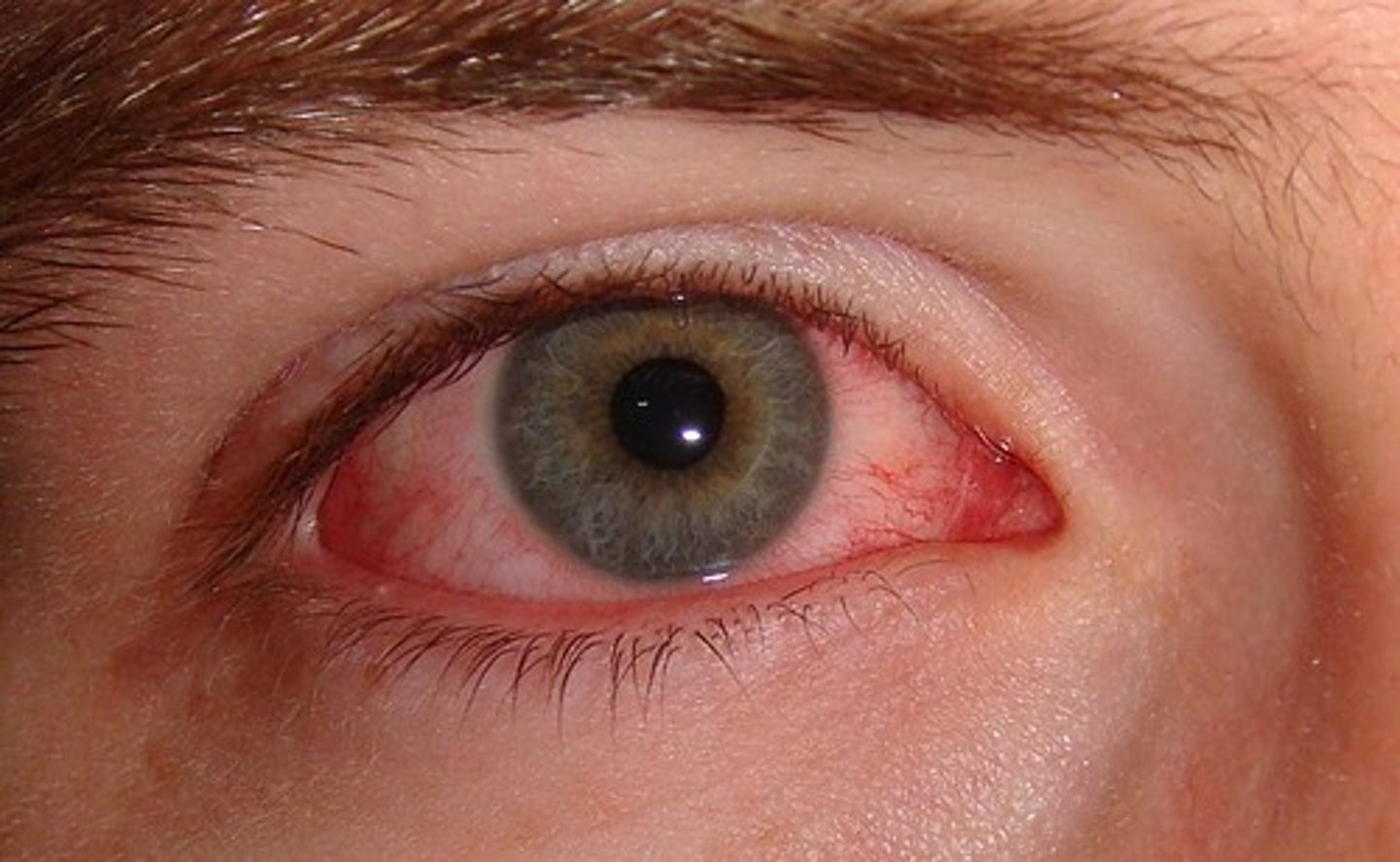
The Eye
Low bioburden, contains lysozyme, continual "washing" with tears, mostly transient bacteria
conjunctivitis
inflammation of the conjunctiva (outer eye)
The Nose (nasal cavity)
moist, mucous-lined, airflow constantly brings in microbes; transient microbes from environment
Pharynx
throat; from nasal cavity to trachea and esophagus
nasopharynx
part of the pharynx directly behind the nasal passages
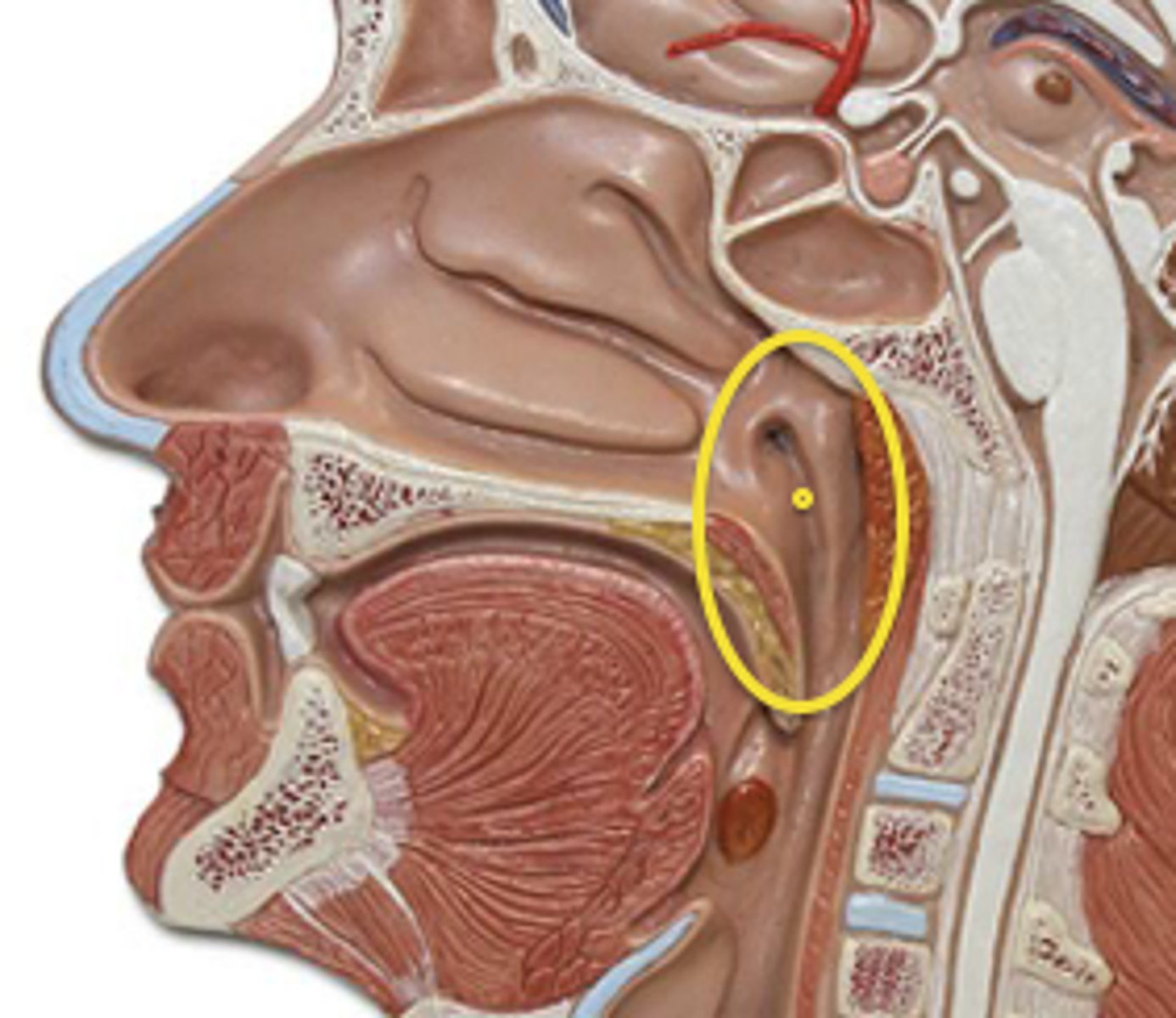
oropharynx
central portion of the pharynx between the roof of the mouth and the upper edge of the epiglottis
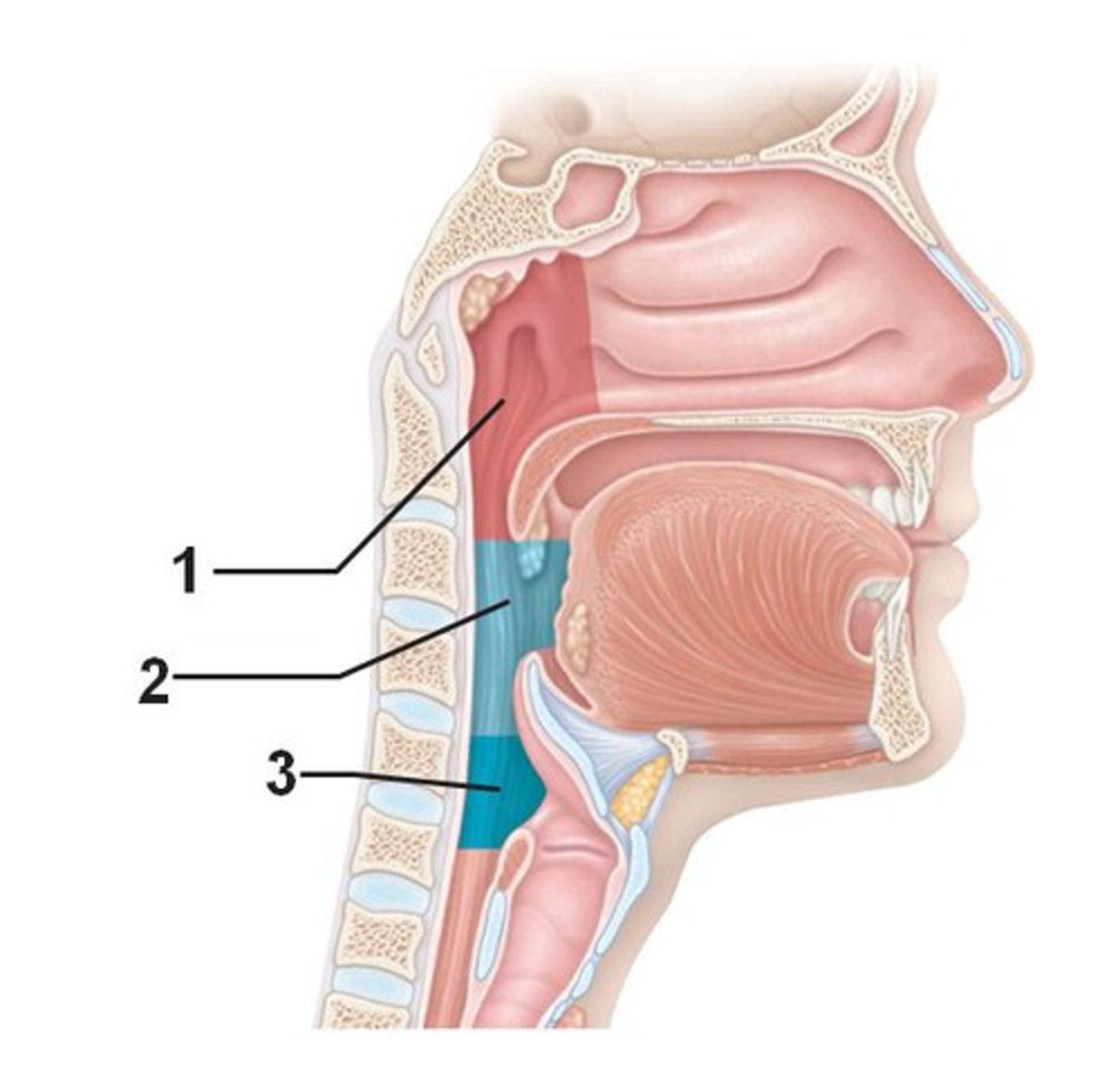
The Oral Cavity
defense with saliva (mechanically washes), contains lysozyme; microbes must adhere to survive here; dybiosis: bacteria fermenting = acid production, periodontal disease, bacteremia
oral cavity dysbiosis
bacteria fermenting causes acid production which breaks down tooth enamel, periodontal disease, bacteremia
Early oral cavity colonizers
Acquired within hours after birth from environment
- Steptococcus, Actinomyces, Lactobacillus, Some yeasts
After teeth emerge colonizers
Anaerobes colonize; Provotella, Fusobacterium
Biofilm formation in oral cavity
Steptococcus mutans and Streptococcus salivarius; produce a glycocalyx (helps stick to teeth and each other); forms dental plaque
Tooth surfaces: More aerobic
Below gums and tonsil crypts: Anaerobic
Oxygen dependance differences within the oral cavity:
teeth anaerobes
Fermentation causes acid production (dissolved tooth enamel), prevotella and fusobacterium; emergence of these begins colonization
upper respiratory system
nose, nasal cavity, paranasal sinuses, pharynx; highest bioburden of resp. tract; cilia keep microbes in nasopharynx or are funneled to stomach
lower respiratory system
trachea, bronchi, lungs
mucociliary escalator
cilia that transport mucus and foreign material out of the lower respiratory tract; sweeps foreign particles up and out of the lungs
The respiratory tract
similar to the nasal and oral cavities; streptococcus, prevotella, veillonella
respiratory tract dysbiosis
respiratory infections, chronic obstructive pulmonary disease (COPD), cystic fibrosis
The stomach
Acidic pH, lethal to most bacteria; low bioburden
ex: Streptococcus and Veillonella; H. pylori can grow in mucous lining of stomach
stomach dysbiosis
Malnourishment causes stomach pH to be higher (more microbes can survive); H pylori overgrowth can cause gastritis & gastric ulcers
The intestine
the digestive tube from stomach to anus; bacteroidetes and firmicutes phyla mainly; bile from pancreas is alkaline
dysbiosis = bloating, flatulence, deadly infection, inflammatory bowel disease
Intestine dysbiosis
bloating, flatulence; more deadly infections, inflammatory bowel disease
duodenum and jejunum
pH ~ 8; Limits growth; Mostly gram + (lactococci and enterococci and Actinobacteria)
ileum and colon
pH ~ 5-7; lower levels of bile salts; very diverse ecosystem; normal human intestine has 10^11 bacteria per gram of feces; anaerobes and facultative anaerobes
ferment unused energy substrates, train the immune system, prevent growth of pathogenic bacteria, regulate the development of the gut, produce vitamins for the host, produce hormones
Functions of Gastrointestinal tract microbiota:
genitourinary tract
urinary tract and reproductive organs
kidneys and ureters
which parts of the urinary tract should be microbe free?
urinary bladder
small number of microbes; mainly anaerobes
urethra
flow of urine out forces microbes out; mostly organisms on the outside; staphylococcus epidermidis
vagina
pH 4.5, acidic; lactobaccillus spp.
genitourinary tract dysbiosis
UTIs of the bladder or kidneys; yeast infections of vagina; correlation of microbiome and susceptibility to STDs
microbiome therapy
treats diseases by restoring a healthy balance to the body's microbial communities, commonly addressing gut dysbiosis to combat infections, inflammation, and metabolic disorders
prebiotics
nutrients that encourage the growth of beneficial microbes
probiotics
live microbes applied to or ingested into the body, intended to exert a beneficial effect
Fecal microbiota transplant
the process of transplantation of fecal bacteria from a healthy individual into a recipient
phage therapy
treatment of bacterial diseases using bacteriophages specific to a particular bacterium