Pharmacology of Thyroid Drugs
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
28 Terms
Where is the Thyroid gland?
- Sits on the trachea, two lobes joined by isthmus
- Blood supply from superior and inferior thyroid arteries
- Arises from external caratoid artery, subclavian artery
- Blood flow is 4-6 ml/min/g tissue
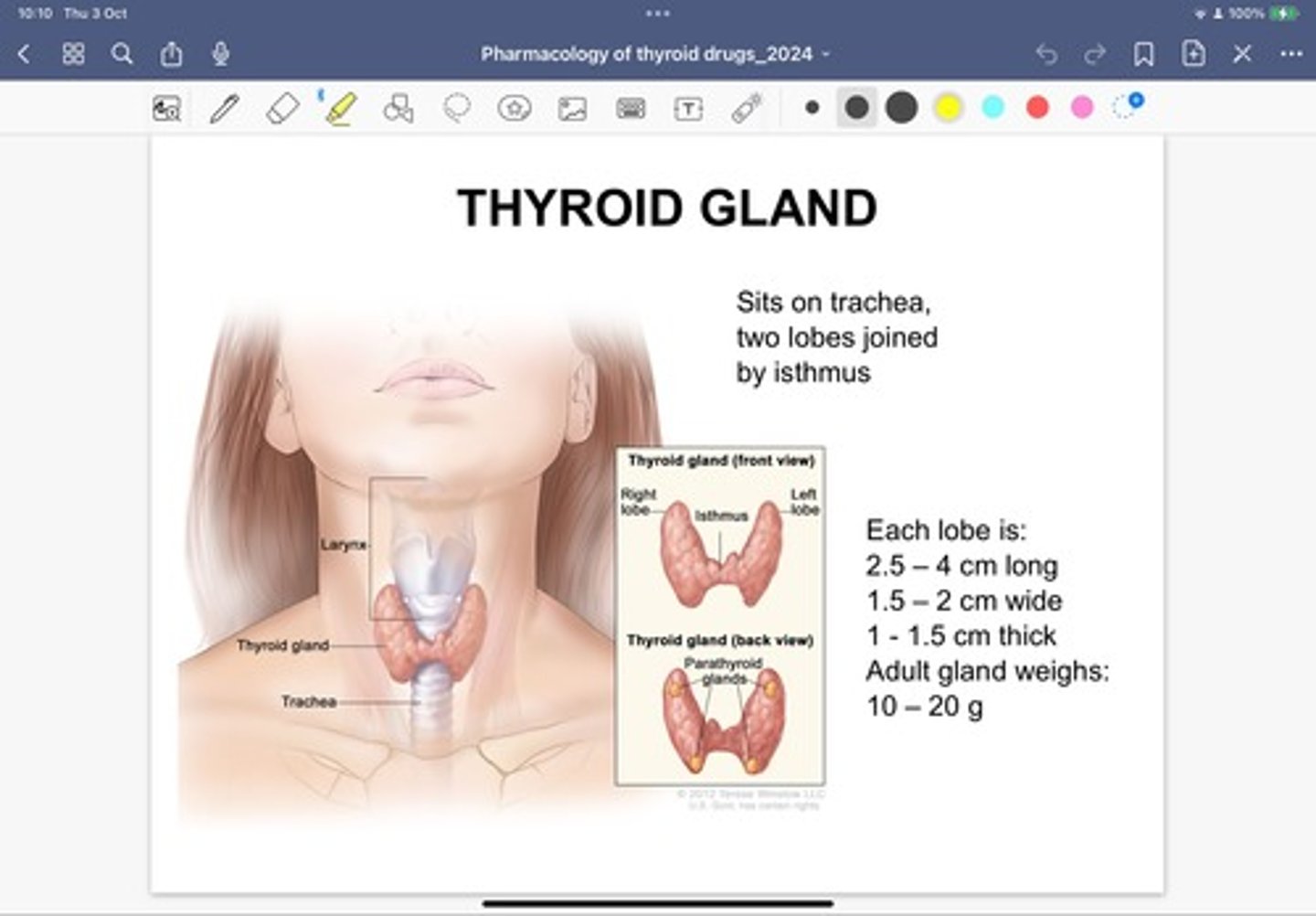
What are the components of the thyroid gland?
- The parathyroid makes PTH- involved in calcium metabolism
(increases blood calcium)
- The thyroid follicles are the structural and functional units of a
thyroid gland
- These follicles act as storage compartments filled with a
substance called the colloid which contains thyroglobulin
- The follicle wall is made up of a large number of cuboidal cells
called follicular cells
- Follicular cells secrete thyroid hormone
- In between thyroid follicles or within the wall we find C (or
parafollicular) cells– C cells secrete calcitonin which helps
deposit calcium in skeletal and and other tissues leading to hypocalcaemia
(opposite of PTH action)
What is thyroglobulin?
Thyroglobulin is a substrate for the synthesis of thyroxine (T4) and triiodothyronine (T3), which control metabolism and growth. It also stores the inactive forms of thyroid hormone and iodine
What is the action of the thyroid gland?
- 1) Concentrates iodine (from food) for incorporation into thyroid hormones
- 2) synthesis of thyroid hormones (for which it needs iodine)- T3/T4, Calcitonin
Functions of thyroid hormones?
- Neural development in foetus, growth in young child and controlling basal metabolic rate BMR
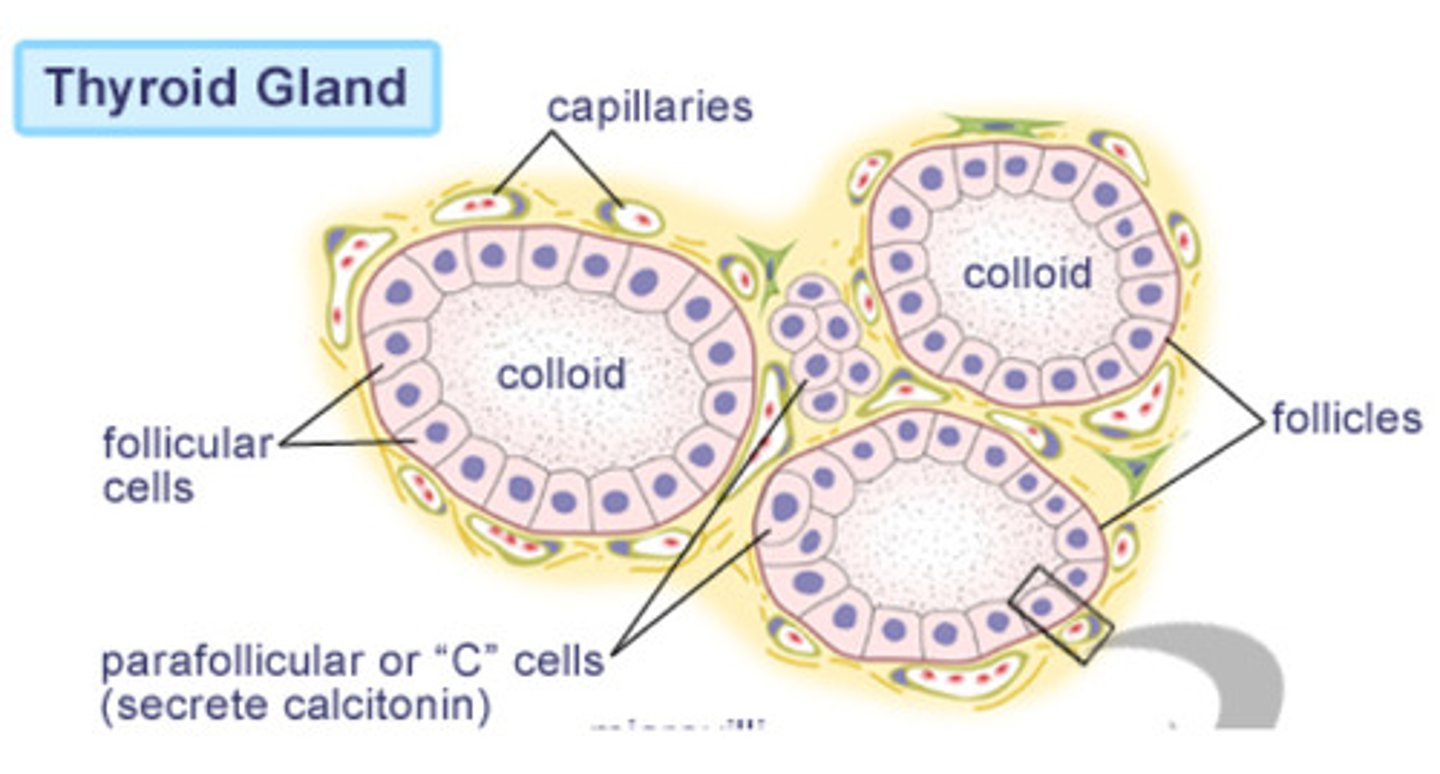
What is the structure of thyroid hormones?
- Tyrosine is basic amino acid building block
- Adding iodine to various positions on Tyrosine creates different thyroid hormones
What are thyrotrophs?
involved in regulating the hypothalamus-pituitary-thyroid (HPT) axis. They respond to thyrotropin-releasing hormone (TRH) from the hypothalamus by producing TSH.
TSH then stimulates thyroid follicular cells to release thyroxine (T4) and triiodothyronine (T3).
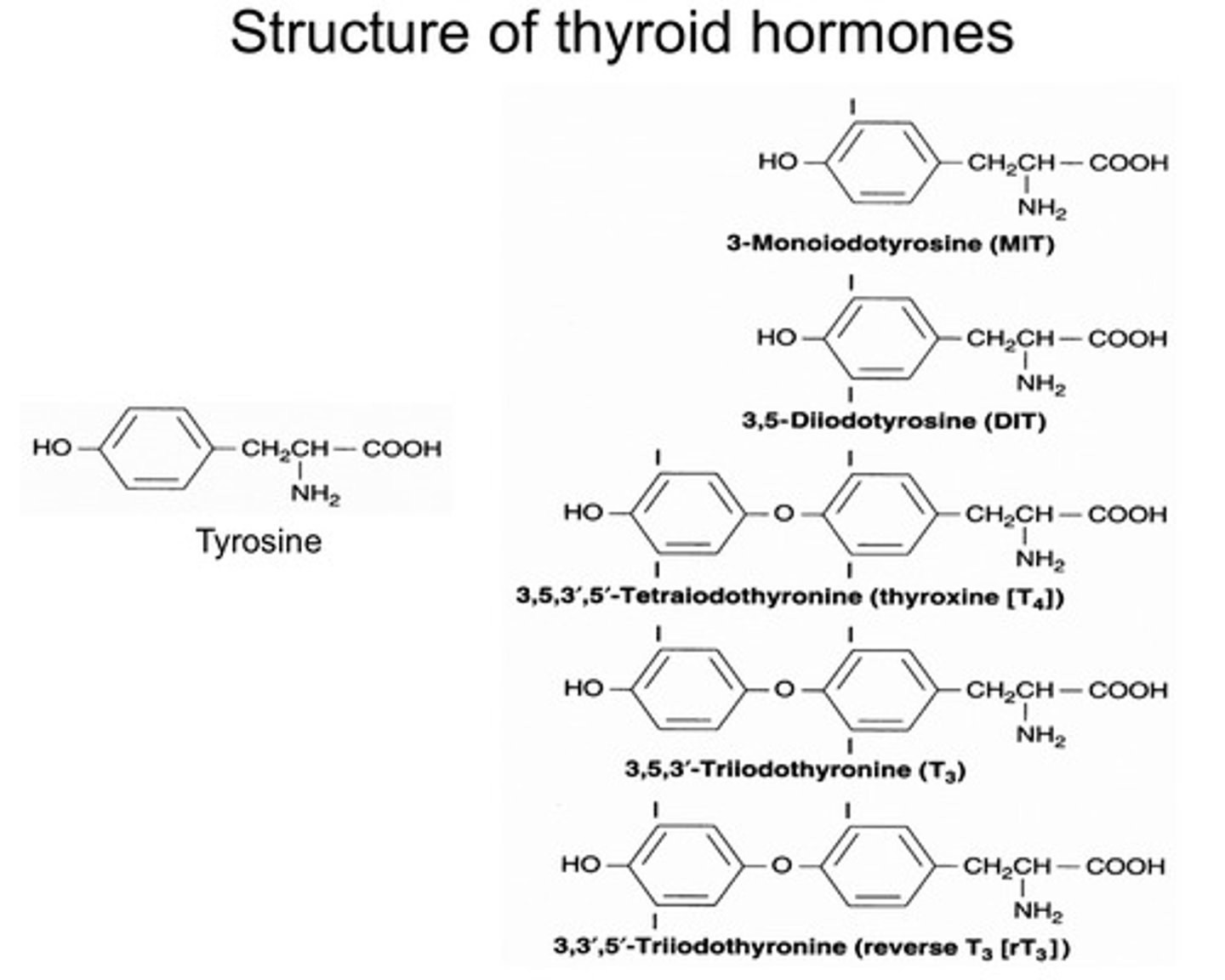
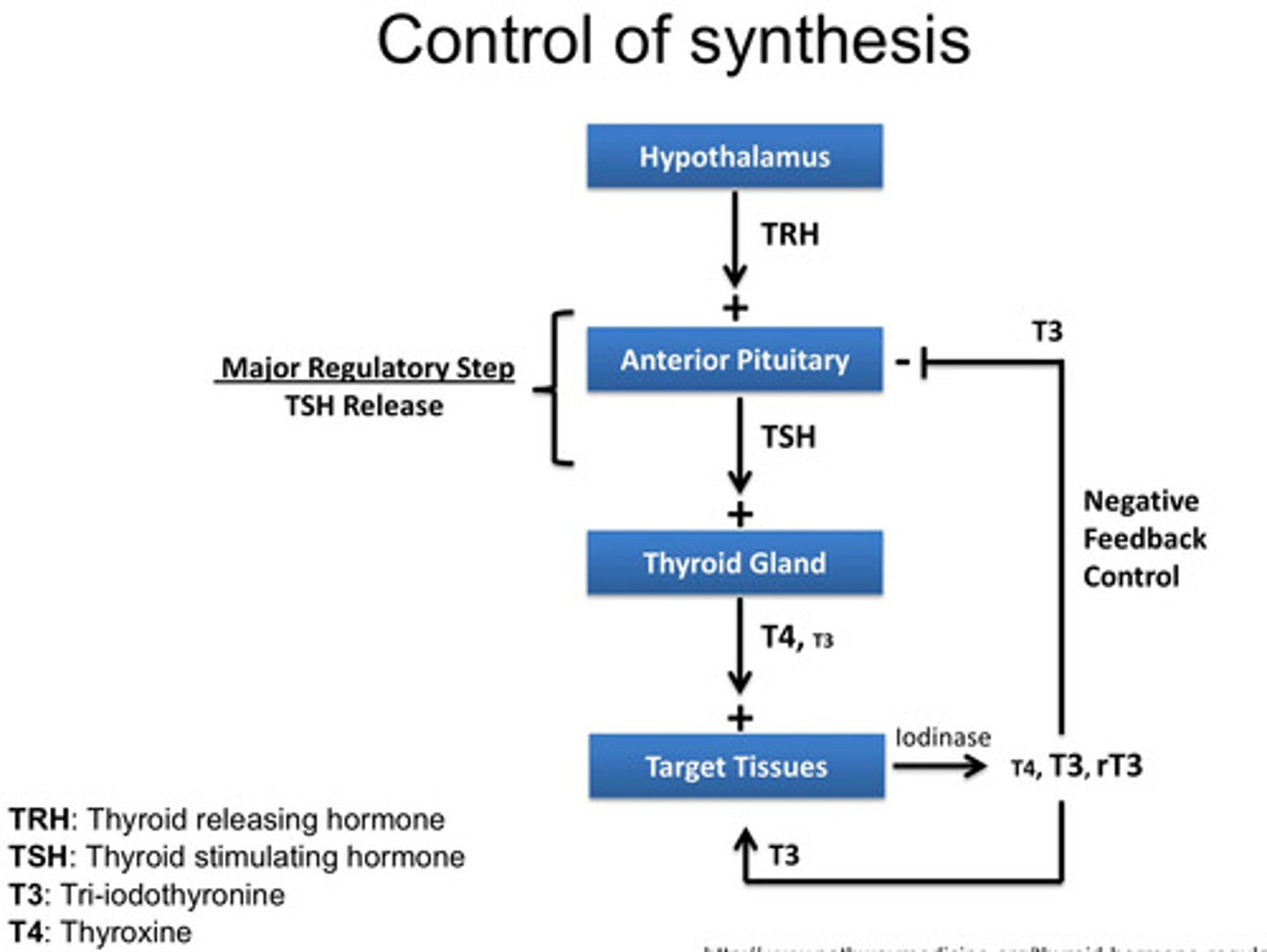
What is the control of synthesis of
thyroid hormones?
The synthesis of these hormones are controlled by the hypothalamic-pituitary-axis.
1) Neurones in the Hypothalamus release Thyroid Releasing Hormone TRH.
2)TRH travels to the anterior pituitary. This then stimulates the thyrotrophs (a different group of neurons at the anterior pituitary) that are responsible for making and secreting thyroid stimulating hormone (TSH)
3) Once TSH is made, it goes to the thyroid gland. Here TSH will stimulate the follicular cells, which then release thyroid hormones T3 and T4 which will then enter circulation and enter target tissues and elicit its biological effects.
- The main hormone released is
T4 which is converted to T3 in the periphery via the enzyme iodinase
- T3 is ~4x more potent at thyroid
receptors than T4
- T3 acts on the thyrotrophs at the anterior pituitary to
decrease release of TSH and to
decrease release of TRH from
hypothalamus (negative feedback system) - When we sufficient levels of T3
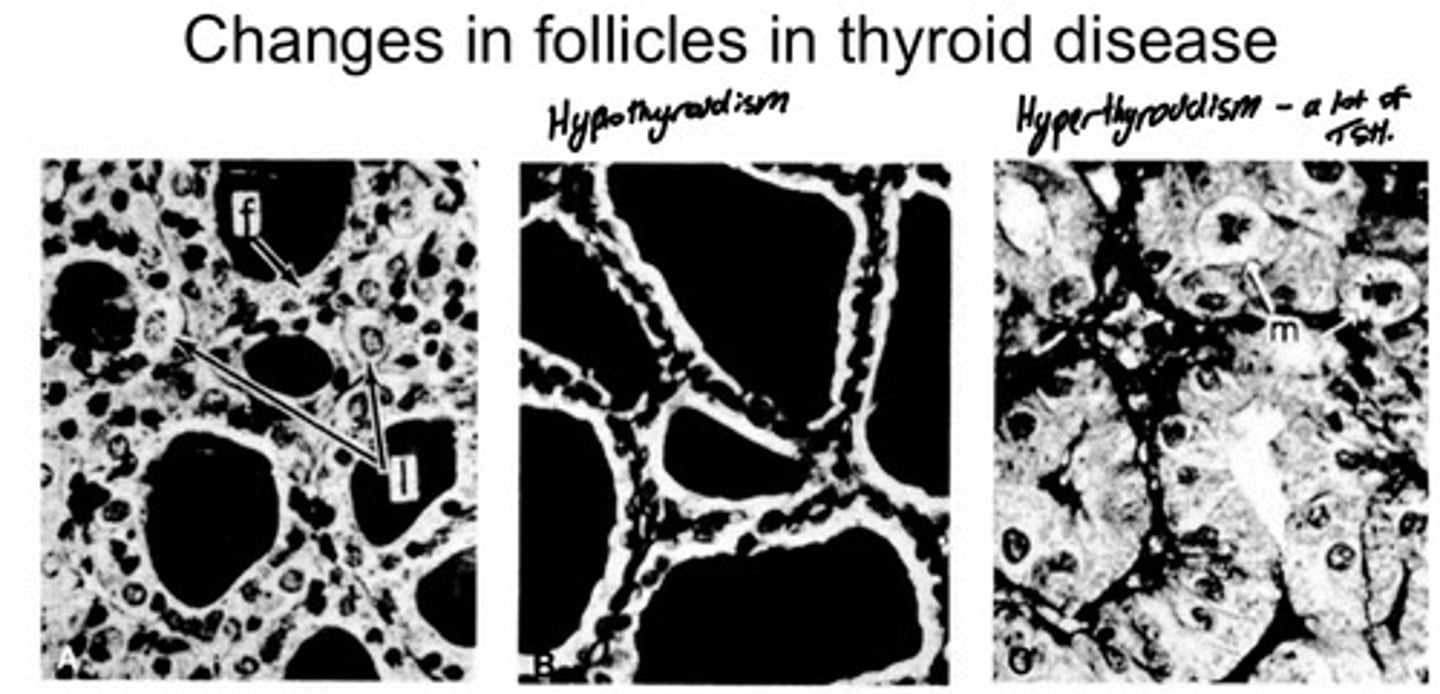
What changes in follicle in thyroid disease?
Hypothyroidism:
-Done in Rat studies using hypophysectomy, where you remove the thyroid
-Large Colloid - big lumen
-Collapsed follicular cells, flatter
Hyperthyroidism:
-Huge follicular cells
-Lumen (colloid) almost gone
-Stimulated rats with TSH and drug given, stimulates growth of follicular cells which normally would stimulate the production of thyroid hormones T3 and T4 but due to the negative feedback system you are also inhibitning the thyroid hormone synthesis , so you are ONLY stimulating TSH.
What are thyroglobulins?
a substrate for the synthesis of thyroxine (T4) and triiodothyronine (T3), which control metabolism and growth. It also stores the inactive forms of thyroid hormone and iodine
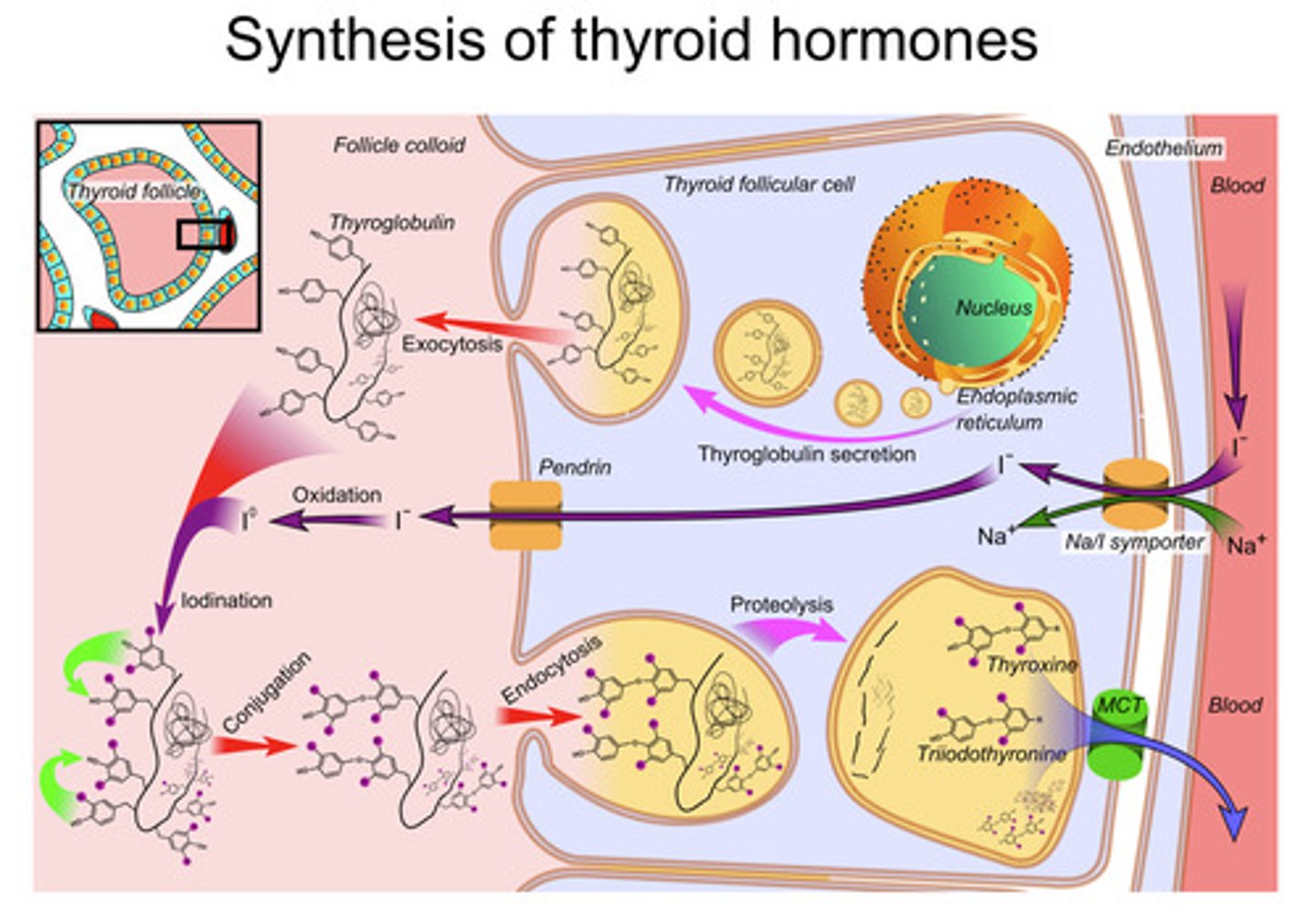
How are thyroid hormones synthesised?
-Whole process begins with iodide:
1- Iodide (I-) (ionised form of iodine), I- is trapped by follicular cells at the thyroid gland
2- Iodide diffuses into the apex of the follicular cells via Na/I symporter - one molecule of iodide in and 2 molecules of Na + in also
3- Iodide is transported into the colloid via Pendrin transporter
4- Inorganic iodide is oxidised (Oxidation step) via thyroid peroxidase (TPO) - an enzyme into iodine (Iodination step) and incorporated into thyroglobulin
tyrosines
5- Two DIT molecules combine to form T4 OR MIT combines with DIT to form T3 (Conjugation step)
6- The follicular cell takes up the T3 and T4 sitting on Thyroglobulin through endocytosis. These vesicles fuse with lysosomes where proteolysis occurs which leads to the release of T3, T4, DIT
and MIT
7- T4 and T3 is released into circulation through mainly the MCT 8 transporter
- DIT (Diiodotyrosine (DIT) is a precursor in the production of thyroid hormone) and MIT (Monoiodotyrosine (MIT) is a compound that is a precursor to active thyroid hormones) is deiodinised to yield tyrosine- T3 is also formed from
monodeiodination of T4 into the thyroid and peripheral tissues
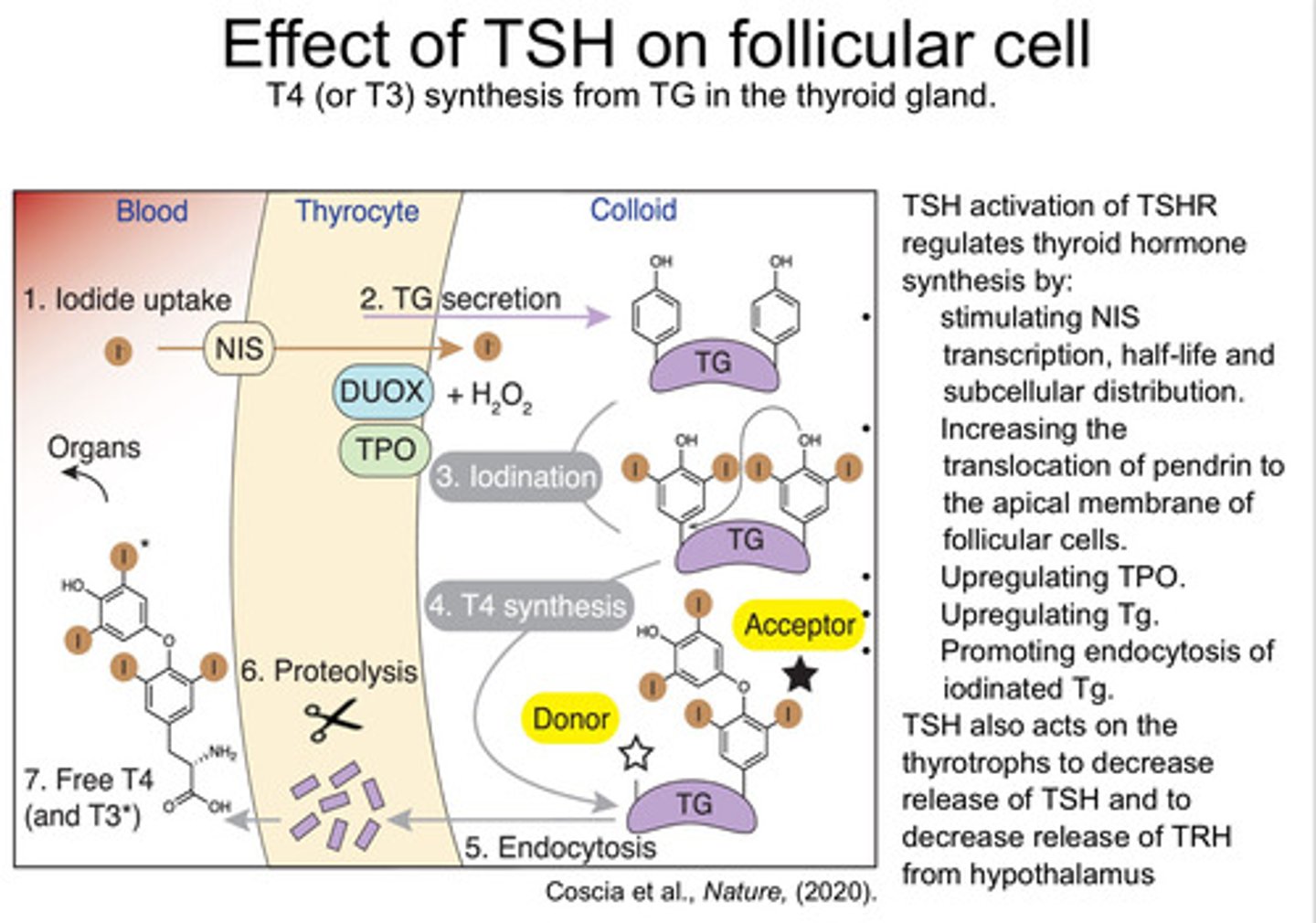
What is the effect of TSH on follicular cells?
- T4 or T3 synthesis from Thyroglobulin in
the thyroid gland
- TSH activation of TSHR regulates thyroid
hormone synthesis by:
- Stimulating NIS transcription, half-life and subcellular distribution.
- Upregulating TPO and Thyroglobulin
- Promoting endocytosis of iodinated
Thyroglobulin.
- Increasing the translocation of pendrin to the apical membrane of follicular
cells.
- TSH also acts on the thyrotrophs to decrease release of TSH and to decrease
How are the levels of Thyroid hormones are regulated in the body?
-Only free hormones not bound to thyroid hormone binding proteins can carry out its biological effect.
-Only 0.4% of T3 is active and only 0.04% of T4 is active
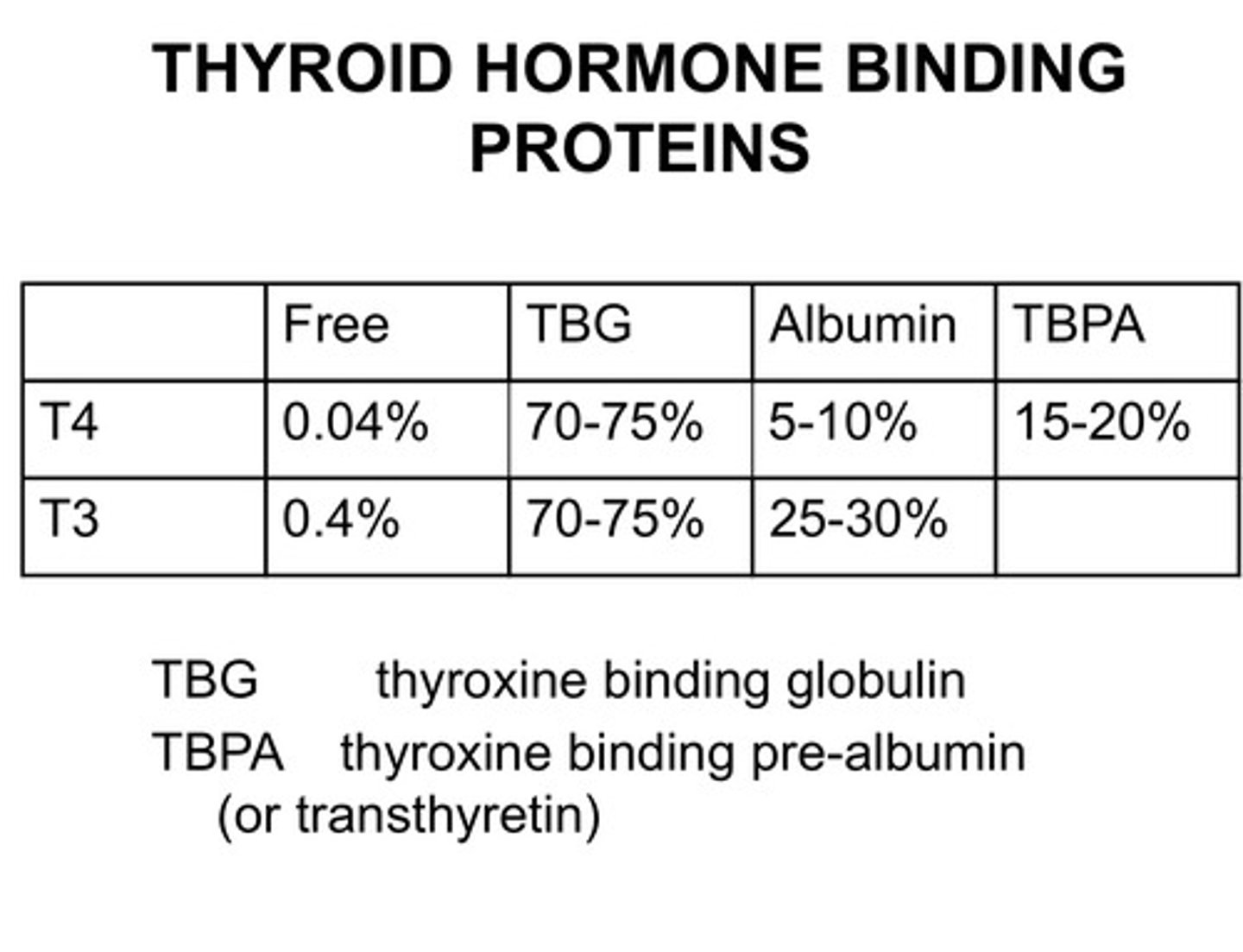
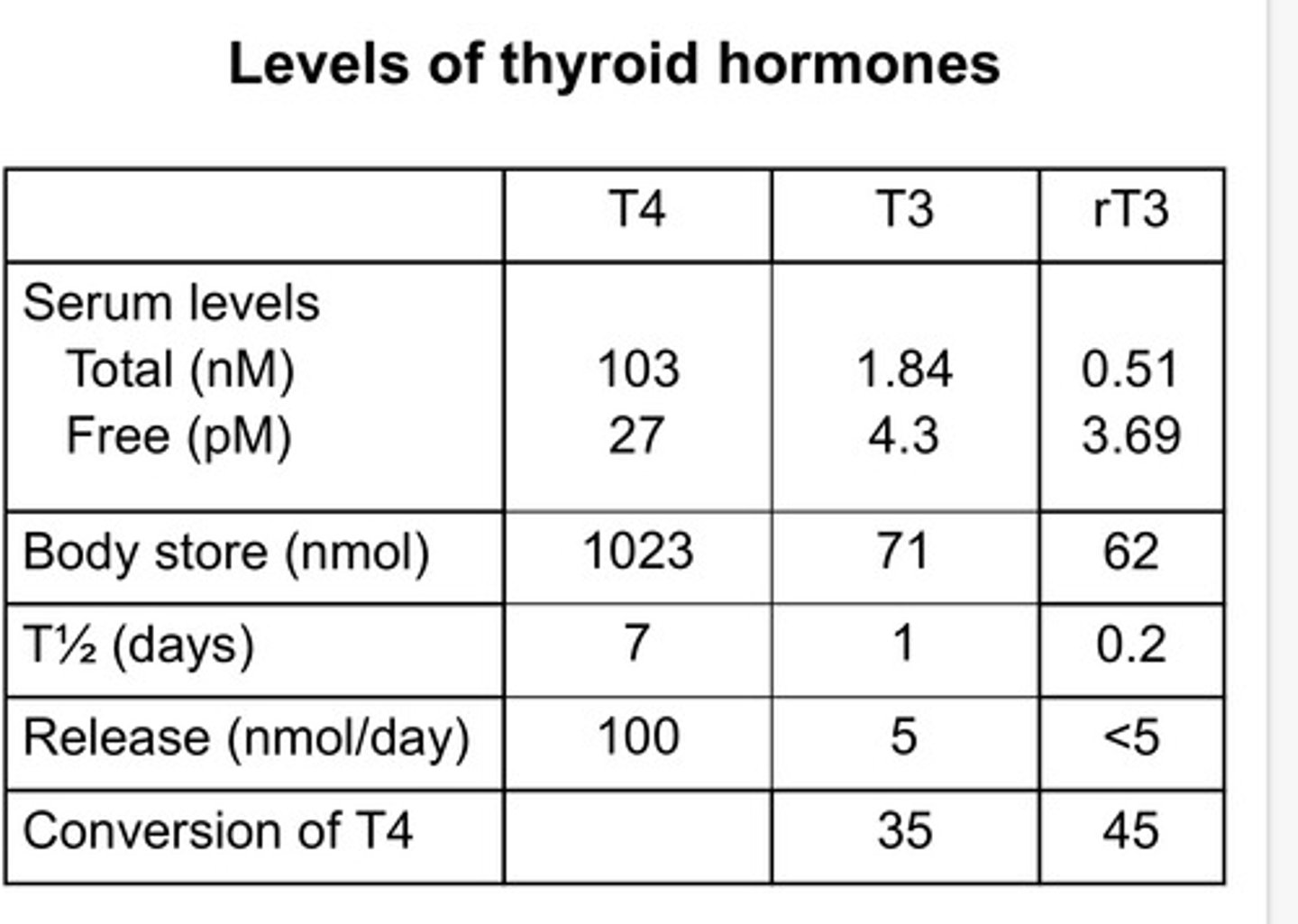
Levels of thyroid hormones averages
-the amount of free hormone is tiny compared to the amount thats binded to a protein
-All these factors effect levels of hormone:
-Only free hormones not bound to thyroid hormone binding proteins can carry out its biological effect.
-Half life
-Rate if Release
-Rate of conversion of T4 to T3
-How much of a hormone the body can store
How do Thyroid receptors work?
1- Thyroid hormones enter target cells by diffusion or by a specific carrier like MCT8
2- Thyroid hormones enter the nucleus to bind and activate THR, a nuclear receptor.
3- The Hormone-THR complex binds to thyroid hormone responsive
element (TRE) on DNA which results in - effects on a cellular level:
- Increased Na+/K+ ATPase levels
- Increased ATP production
- Increased O2 consumption
- Increased number of β-adrenergic receptors
What are the effects of thyroid hormones at a systemic level?
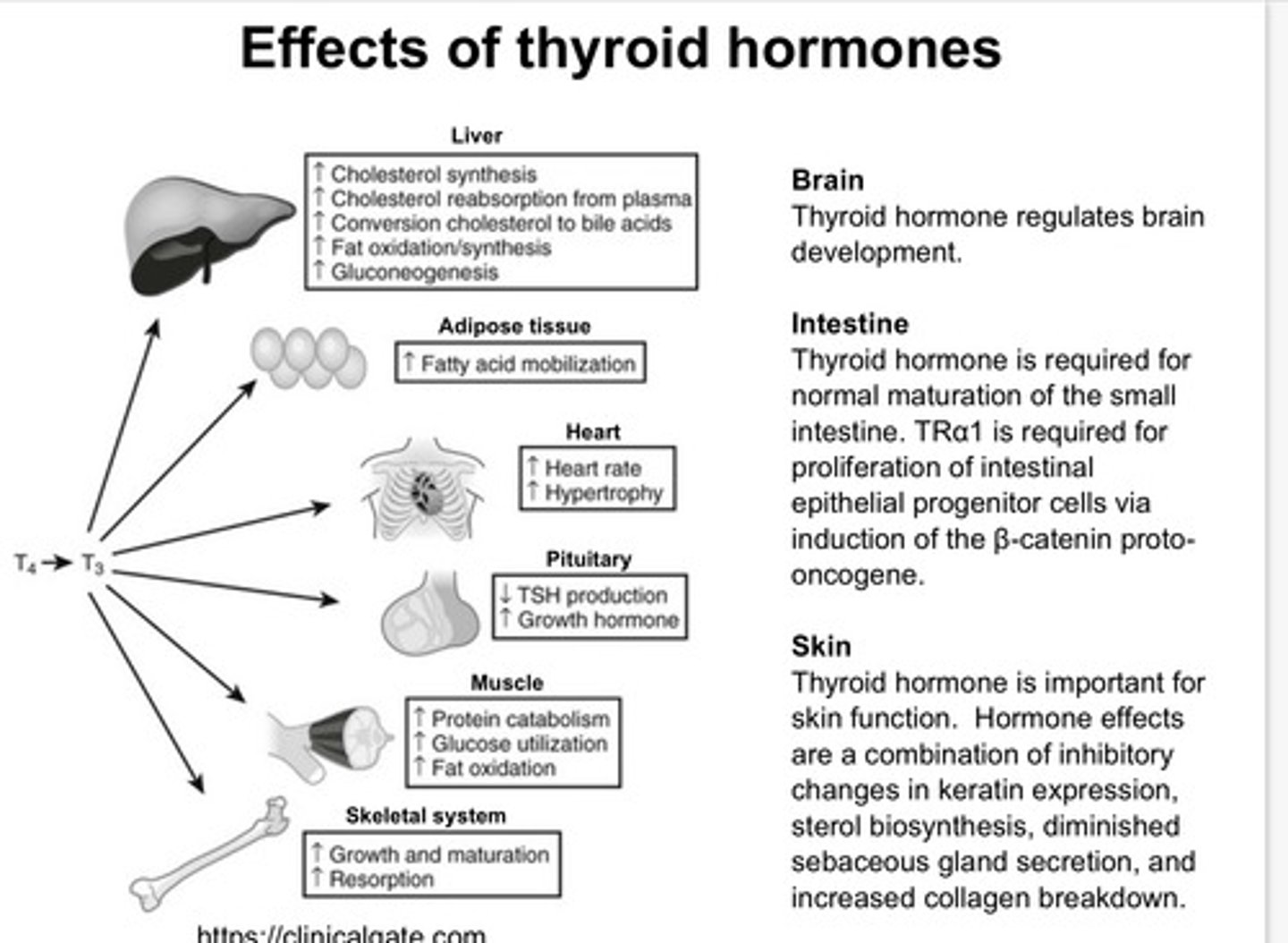
What are the types of thyroid disease?
- Primary (Thyroid)
- Secondary (Pituitary)
- Tertiary (Hypothalamic)
How do we test for primary thyroid disease?
- Hypothyroidism: low T3 and T4 with elevated TSH (due to the negative feedback mechansim)
-Hyperthyroidism:
High T3 and T4 with low TSH
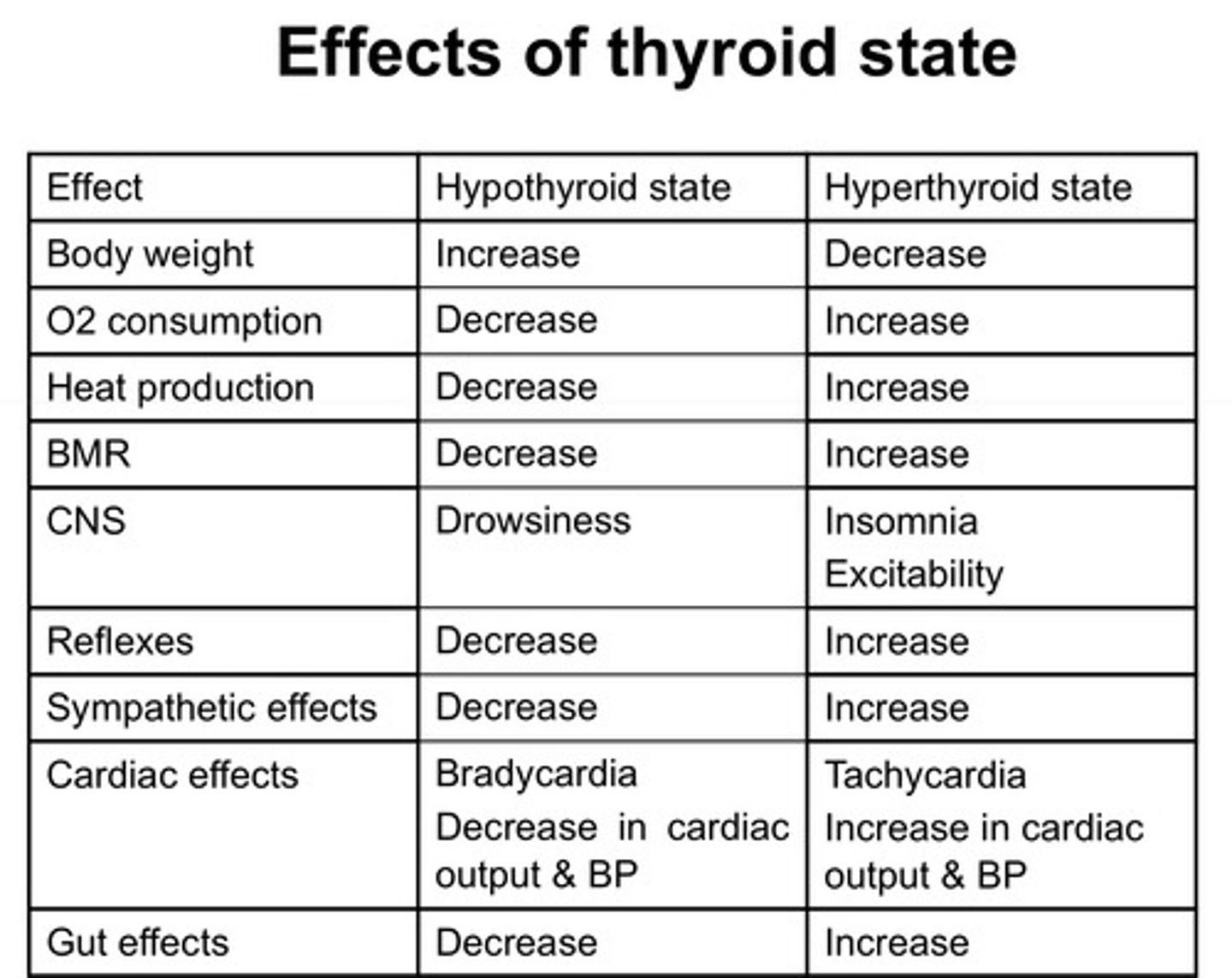
What are the effects of thyroid state on the body (Hypo or Hyper all opposite effects )?
Factors :
-Bodyweight - (hypo = increase in bodyweight as thyroid hormones play a role in Basal metabolic rate so a decreased BMR = food isnt metabolised as well = increased bodyweight
-O2 consumption
-Heat Production
-Basal Metabolic rate
-CNS
-Reflexes
-Sympathetic effects
-Cardiac effects
-Gut effects - decrease in gut motility
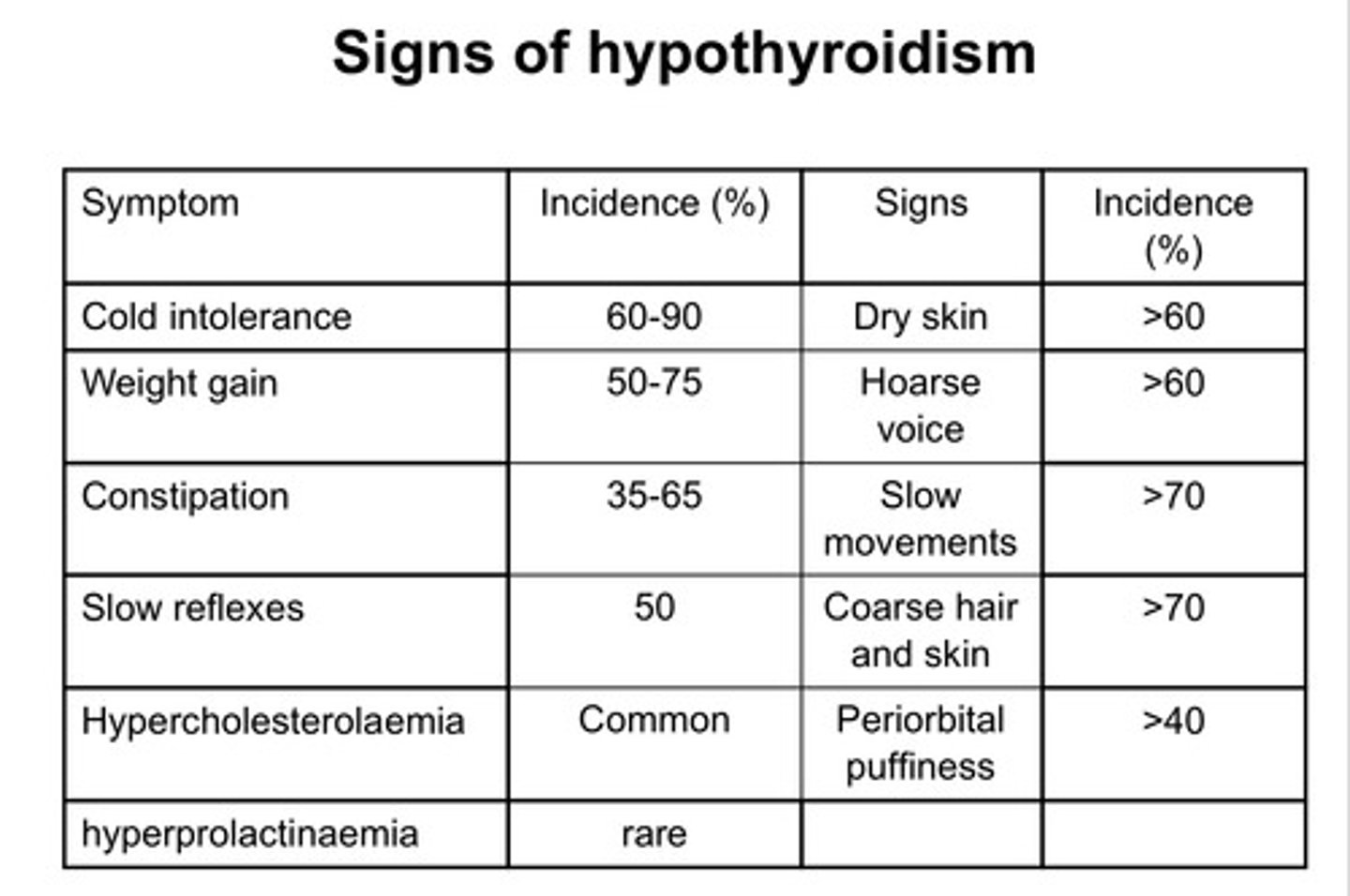
Signs of hypothyroidism
-Cold intolerance
-Weight gain
-Constipation
-Slow reflexes
-Hypocholesteraemia
-Hyperprolactinaemia
What are the causes of Hypothyroidism ?
Main ones:
1. Hashimoto's thyroditis - an autoimmune disease, where your body makes antibodies against thyroglobulin or thyroid perioxidase (TPO) (if you block TPO - follicular cells can't make T3 or T4)
2. Radiotherapy or surgery for hyperthyroidism
Other causes:
-Iodine Deficiency
-Goitrogen Consumption
Hyperthyroidism treatment
- Treatment: Thyroxine (T4)- half life is 6 days and the effects last for 14 days
- Monitor the effectiveness by getting TSH back within normal range and
measure ~3 months
- Liothyronine (sodium salt of T3)- half life is 2-4 days and effects last for 8 days
Other causes and treatments
- Myxoedema:
-When caused by iodine defiency: Dietary iodine requirement is 150 mcg/day so deficiency is classified as less
than 50 mcg/day
What is Goitrogen and how does it link to hypothyroidism and how is it treated?
- Suppresses hormone secretion- increases TSH secretion = goitre formation
(enlarged gland)
- Sources: kelp, cabbage, cassava, lithium, local drinking water (some),
cough mixtures
Treatment
- Decreased intake
Myxoedema
caused by extreme deficiency of thyroid secretion; also known as adult hypothyroidism
Signs of hyperthyroidism
-Nervousness/Anxiety
-Sweating
-Heat intolerance
-Palpitations
-Fatigue
-Weight loss
-Tremor
-Tachycardia
-Thyrotoxicosis (Too much TH in your body)
-Goitre - an enlarged thyroid
-Diarrhoea
-Exophthalmos (the protrusion of one or both eyes anteriorly out of the orbit due to an increase in orbital contents within the rigid bony orbit) and upper lid retraction
-Pretibial Myxoedema (scaly thickening and hardening of the skinn due to deposition of glycosaminoglycans)
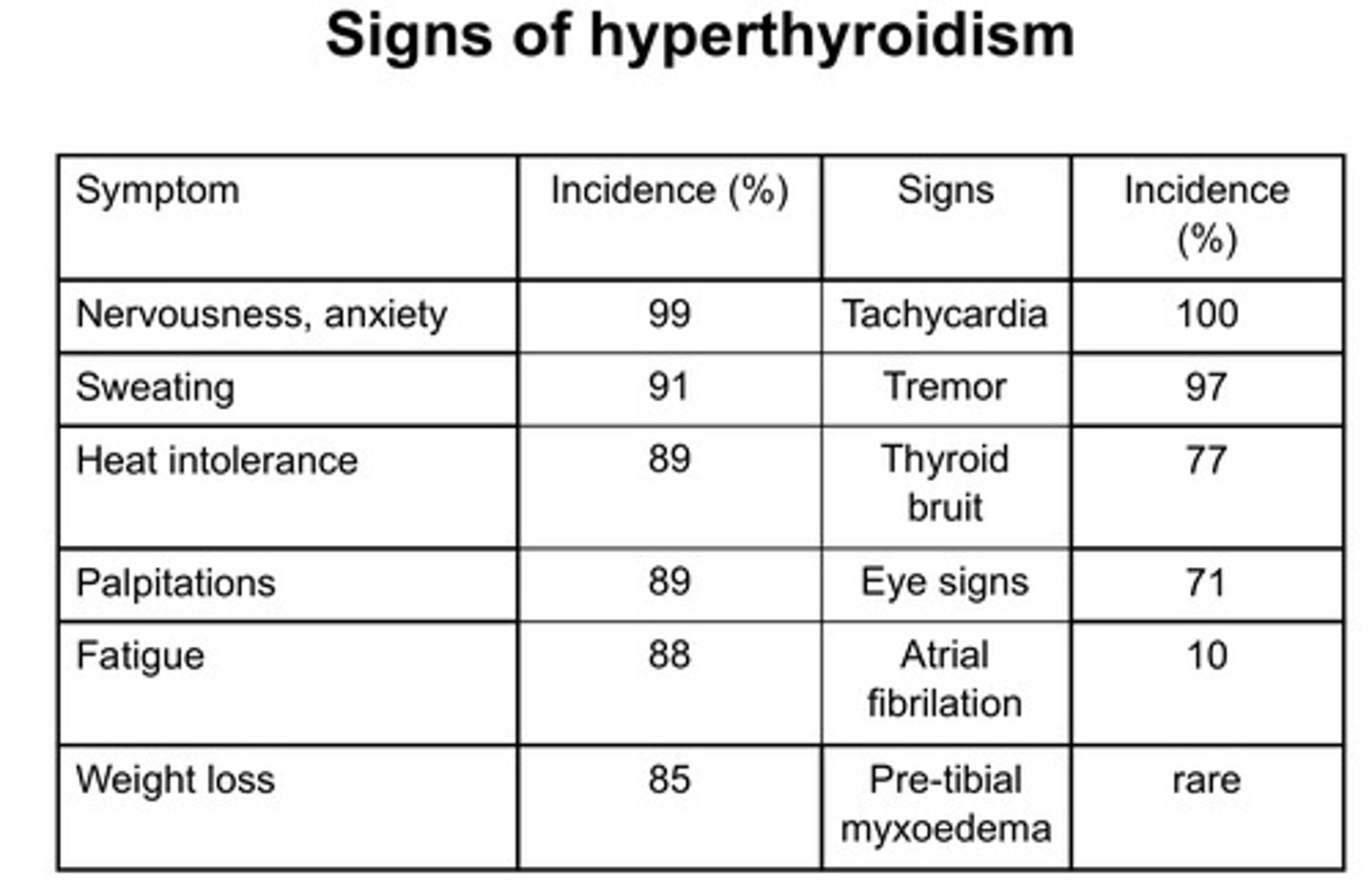
Causes of hyperthyroidism
- Grave’s disease: (aka diffuse toxic goitre - enlarged thyroid)- an autoimmune disease- TSAb (LATS)
produces prolonged stimulation of TSH receptors
- Caused by antibodies that stimulate the follicular cells that look like TSH. Thyrotrophs are being stimulated by this antibody rather than TSH so the negative feedback system doesn't work.
What is a life threatening complication for people with hyperthyroidism that is left untreated and is accompanied by a stressor e.g. an infection?
Treatment>
Thyroid Storm (Thyrotoxic Crisis)
-These patients can go into a coma
Features:
-Fever
-Tachycardia
-Agitation
-Nausea and vomiting
-Diarrhoea
-Jaundice
- Treatment: IV fluids - for hydration, propranolol, hydrocortisone - to stop allergic reactions, oral iodine solution and
propylthiouracil
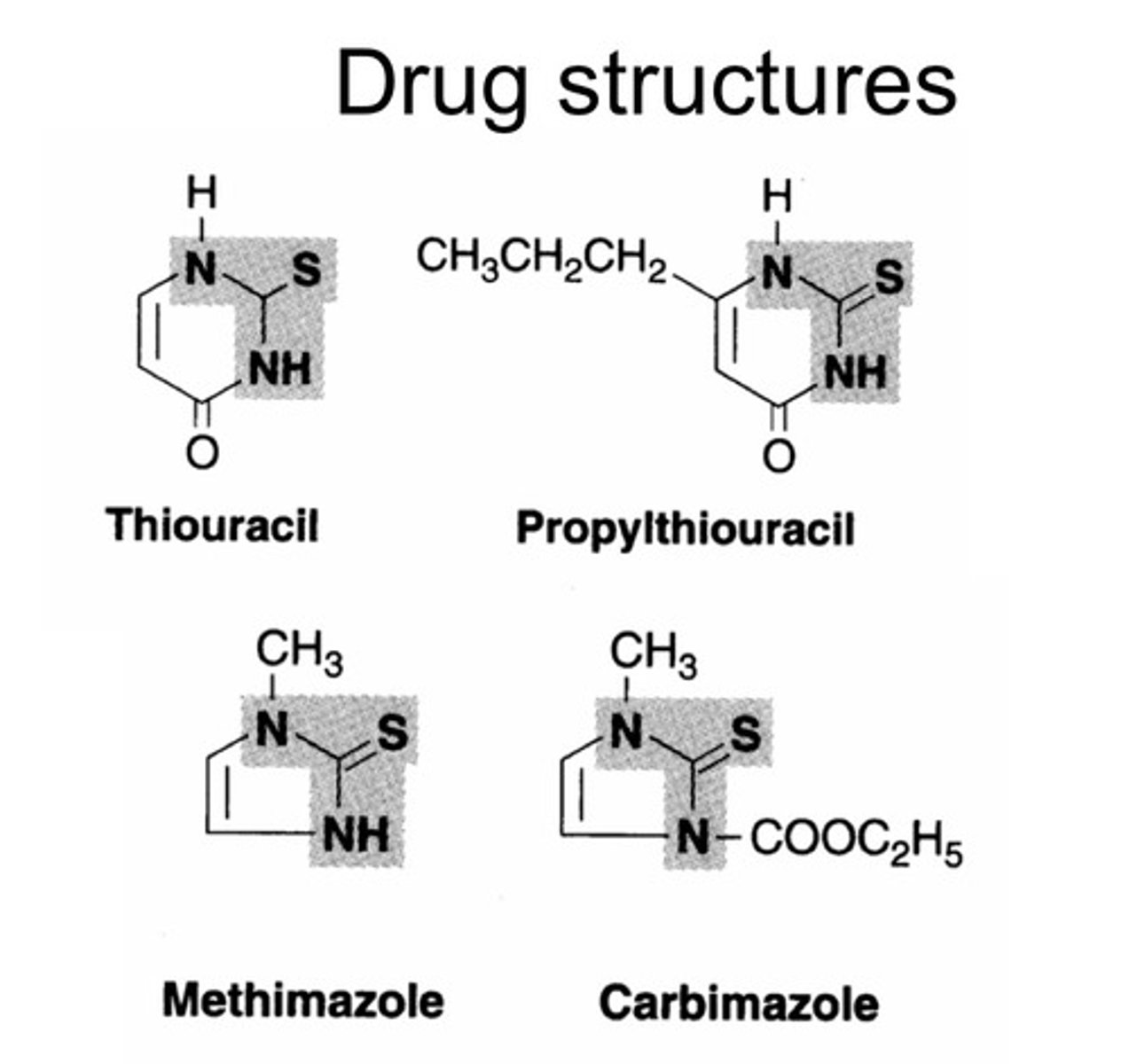
Hyperthyroidism treatments
- Antithyroid drugs, TPO inhibiting drugs called Thioamide like Carbimazole (converted to methimazole in body),
Propylthiouracil (inhibits thyroid peroxidase and also prevents peripheral
conversion of T4 to T3)
- Propylthiouracil: 4-8 weeks to become euthyroid because these drugs do not inhibit
TH release, reduce dose to maintenance
dose and monitor by measuring TSH and T4- treatment period is 12-18
months
- Side effects: Neutropenia and agranulocytosis, sore throat
-Radioiodine - Taken up into follicular cells and irradiates them. Beta and Gamma emitter. B particles kills cells and G cells pass through causing no damage. T1/2 8 days, 2 months completely decayed
- Surgery (partial thyroidectomy)
- Iodine in LUGOL’s solution- 5% I2 and 10% KI- this is used prior to surgery to
reduce vascularity of thyroid gland. Inhibits synthesis and release of T3/T4. Rapid onset (hence preferred for thyroid storms)
- Guanethidine (noradrenergic neurone blocker) and eye drops for exophthalamos
What is the role of Beta Blockers in hyperthyroidism treatment?
- Propranolol blocks sympathetic effects of thyroid hormones (e.g. tachycardia, sweating, anxiety, tremors)
-can also inhibit T4->T3 conversion