Muscle Physiology, Cardiac Function, and Renal Processes: Key Concepts and Mechanisms
1/83
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
84 Terms
ATP splitting is much slower in smooth muscle, so cross-bridge activity and filament sliding occur about 10x more slowly in smooth muscle than in skeletal muscle.
true
Both the thin and thick filaments change length during muscle fiber shortening.
false
Ca2+ binding to tropomyosin causes myosin to change shape, physically moving it away from its blocking position.
False
Contractile activity in both skeletal muscle and multiunit smooth muscle is ____.
neurogenic
How long does a single action potential in a skeletal muscle fiber last?
1 to 2 milliseconds
How many additional pathways supply ATP as needed during muscle contraction?
3
If the muscle fiber is stimulated so rapidly that it does not have a chance to relax at all between stimuli, a smooth, sustained contraction of maximal strength known as ____________________ occurs.
tetanus
Muscles that produce precise, delicate movements have fewer muscle fibers in their motor units compared to muscles made for powerful movements.
true
Muscle tension is produced internally within the ____.
sarcomeres
One motor neuron, plus all the muscle fibers it innervates, is known as a(n):
motor unit
Cardiac contraction is graded by varying the strength of contraction of all the cardiac muscle cells by intrinsic and extrinsic control mechanisms.
true
__________ fibers are small terminal fibers that extend from the bundle of His and spread throughout the ventricular myocardium.
purkinje
In cardiac contractile cells, the L-type Ca2+ channels lie mostly in the:
transverse (T) tubules
Stroke volume is determined by:
the extent of venous return and by sympathetic activity
Sympathetic stimulation of the AV node reduces the AV nodal delay by increasing conduction velocity as a result of enhancing the inward current of what element?
calcium
The amount of blood pumped out of each ventricle with each contraction is called the __________.
stroke volume
Atrial excitation and contraction should be complete before the onset of ventricular contraction.
true
Atrial repolarization and ventricular depolarization occur __________.
simultaneously
Closure of the aortic valve produces a disturbance or notch on the aortic pressure curve, the dicrotic notch.
true
In a normal heart, what is the average amount of blood that's left in the ventricle at the end of systole when ejection is complete?
65 mL
Although ventricular pressure falls to 0 mm Hg during diastole, arterial pressure does not fall to 0 mm Hg because the next cardiac contraction refills the arteries before all the blood drains off.
true
Arteriolar smooth muscle normally displays a state of partial constriction known as __________, which establishes a baseline of arteriolar resistance.
vascular tone
At resting heart rate, about 80% of the cardiac cycle is spent in systole and 20% in diastole.
false
By the time the blood enters the venous system, blood pressure averages only:
17 mm Hg
Decreased blood flow in response to enhanced tissue activity is called active hyperemia.
false
During systole, no blood enters the arteries, while blood continues to leave, driven by elastic recoil.
false
Exchanges between blood and surrounding tissues across capillary walls are accomplished in two ways: passive __________ and __________ flow.
diffusion; bulk
Flow rate of blood through a vessel is inversely proportional to:
vascular resistance
Local arteriolar myogenic and chemical mechanisms that keep tissue blood flow fairly constant (despite rather wide deviations in mean arterial driving pressure) is termed:
autoregulation
Mean arterial pressure within the circulatory system is constantly monitored by:
baroreceptors
Although vasopressin promotes H2O conservation by the body, it cannot halt urine production.
true
A rise in plasma potassium concentration __________ stimulates aldosterone secretion by the __________ cortex.
directly; adrenal
Contraction of __________ cells closes off a portion of the filtering capillaries, reducing the surface area available for filtration within the glomerular tuft.
mesangial
During reabsorption, H2O passes primarily through __________ that are formed by specific plasma membrane proteins in the tubular cells.
aquaporins
Metabolic acidosis caused by the inability of the kidneys to adequately secrete:
hydrogen ions
One function of the kidney is to produce renin, an enzymatic hormone that triggers a chain reaction important in salt conservation by the kidneys.
true
Potassium secretion in the principal cells of the distal and collecting tubules is coupled to __________reabsorption by the energy-dependent basolateral __________pump.
Na; Na+-K+
Sodium is reabsorbed throughout the tubule with the exception of the:
descending limb of Henle's loop
Sodium reabsorption in the proximal tubule plays a pivotal role in reabsorbing glucose, amino acids, H2O, chloride ions and urea.
true
The __________ fluid that enters Henle's loop becomes progressively more concentrated (hypertonic) as it flows down the __________ limb.
isotonic; descending
what is the name of the functional unit of the kidney?
nephron
why can the juxtamedullary nephron concentrate urine more than cortical?
jux is deeper
would a kidney stone, which blocks the renal pelvis and causes a buildup of fluid/osmotic pressure in the bownmans capsule, increase or decrease net filtration pressure?
decrease
if afferent arteriolar resistance increases less blood blow into the glomerulus and the GFR
decreases
more sodium in the extracellular fluid equates to more water in the extracellular fluid
true
is the sodium glucose cotransporter a
symporter
the pressure exerted by a particular gas is directly proportional to the percentage of that gas in the total air mixture
true
each polypeptide chain contains how many iron containing nonprotein coding heme groups?
one
collectively the effect of CO2,acid, and other metabolic factors on the release of oxygen from the hemoglobin is referred to as what?
the Bohr effect
what enyme is found inside of erythrocytes that catalyzes the conversion of carbon dioxide to bicarbonate?
carbonic anhydrase
are the chemoreceptors activated by oxygen in anemic states?
yes
hypercapnia yields an increase in CO2 which increases the production of protons which increase the pH
false
how does resporiatory acitvity promote venous return?
as we breathe in more blood goes to the heart
at sea level atmosphoeric pressure is equal to how many mm Hg?
760 mm Hg
the sympathetic nervous system increases the caliber of the bronchioles
true
compliance is?
ability of vessel or airway to be stretched and how much effort is required to distend the vessel
during quiet breathing or passive respiration, the lungs are near maximal inflation
false
what is the purpose of carbonic anhydrase?
plays a role in CO2 transport cia the conversion of CO2 to bicarbonate HCO3 and vice versa
what is anemia?
below normal oxygen carrying capacity of the blood
leukocytes are able to exit the blood unlike erythrocytes
true
where does the common pathway start and what is the end product before the clot stabilization?
fXa and Fibrin/Fxllla
exchange of material is made directly between the blood and tissue cells
false
what specific factors influence venous return the most?
buffy coat and leukocytes
what is the name of the packed cell volume and what cell type is found here?
hematocrit and erythrocytes
what are the 2 ways you can modify cardiac output the most (ie what 2 variables can you change physiologically)?
stroke volume and heart rate
when resistance increases, the pressure gradient must increase in order to maintain the same flow rate
true
the major function of arterioles is to serve as a pressure reservoir
false
arteriolar walls contain little elastic connective tissue
true
the layer of smooth muscle in arterioles is innervated by which branch of the autonomic nervous system?
sympathetic
why is the wall of the left ventricle thicker than the wall of the right?
the left ventricle pumps blood into a higher-resistance, high pressure
what is the t wave?
ventricle repolarization
would blood going through an occluded vessel flow in
turbulent way
parasympathetic stimulation of the SA node causes the heart rate to decrease
true
what ion needs to be removed from the cytosol in order for smooth muscle to relax?
calcium
multi unit smooth muscle cells are all myogenic
false
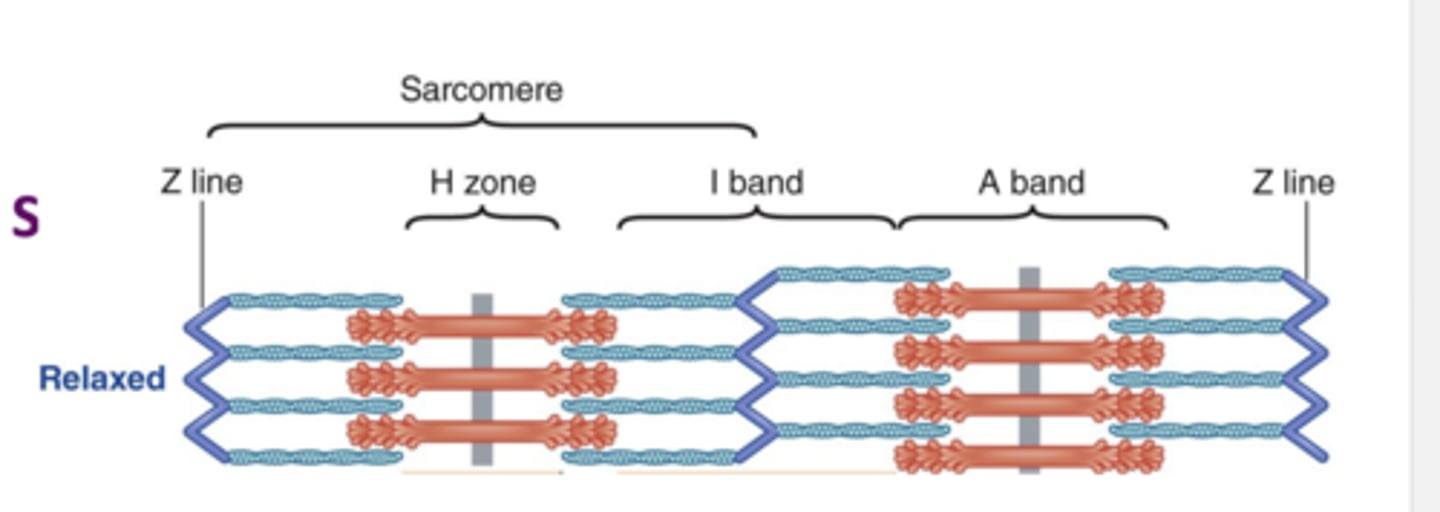
Does one sarcomere contain the entire
A band
what is the overall result of a power stroke?
actin is pulled away from the z line
what neurotransmitter is released at the
acetylcholine
what receptor superfamily do these receptors belong to?
chemically gated ion channels
what is the name of the pump that moves Ca_2 from the cytosol
SERCA pump
Voluntary movements are innervated by which
branch of the peripheral nervous system?
Somatic nervous system
What does Tropomyosin do At rest/relaxation?
At rest/relaxation: Tropomyosin blocks the binding site on
actin
What does C,T,I bind to ? individually
C binds Ca +2 , T Tropomyosin, I Actin. When Ca +2 binds to C, troponin I moves away from actin, allowing tropomyosin to move. Troponin T undergoes a conformational
change which moves tropomyosin away from
the myosin binding site on actin.Self Assessment:
What is the overall result of a power stroke?
What does this picture show?
Actin is pulled away from the Z line (center of
the sarcomere) and the sarcomere becomes
smaller