Pediatrics Review - Emma Holliday Ramahi
1/277
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
278 Terms
General info about how the newborn tolerated labor (1min) and the newborn's response to resuscitation (5min)
What does the APGAR tell you?
What to do next (does not guide therapy)
How the baby will turn out (does NOT predict neurologic outcome)
What does the APGAR not tell you?
Erb-Duchenne C5-C6. (Klumpke is C7-C8 + T1) Refer if not better by 3- 6mo for neuroplasty
PE: When assessing Moro on an LGA newborn, the right arm remains extended and medially rotated.
Clavicular Fracture.
Will form a callus in 1wk. No tx needed. Can use figure of 8 splint.
PE: When palpating the clavicles on a LGA newborn, you feel crepitus and discontinuity on the left.
Caput succedaneum
"Edema. Crosses suture lines."
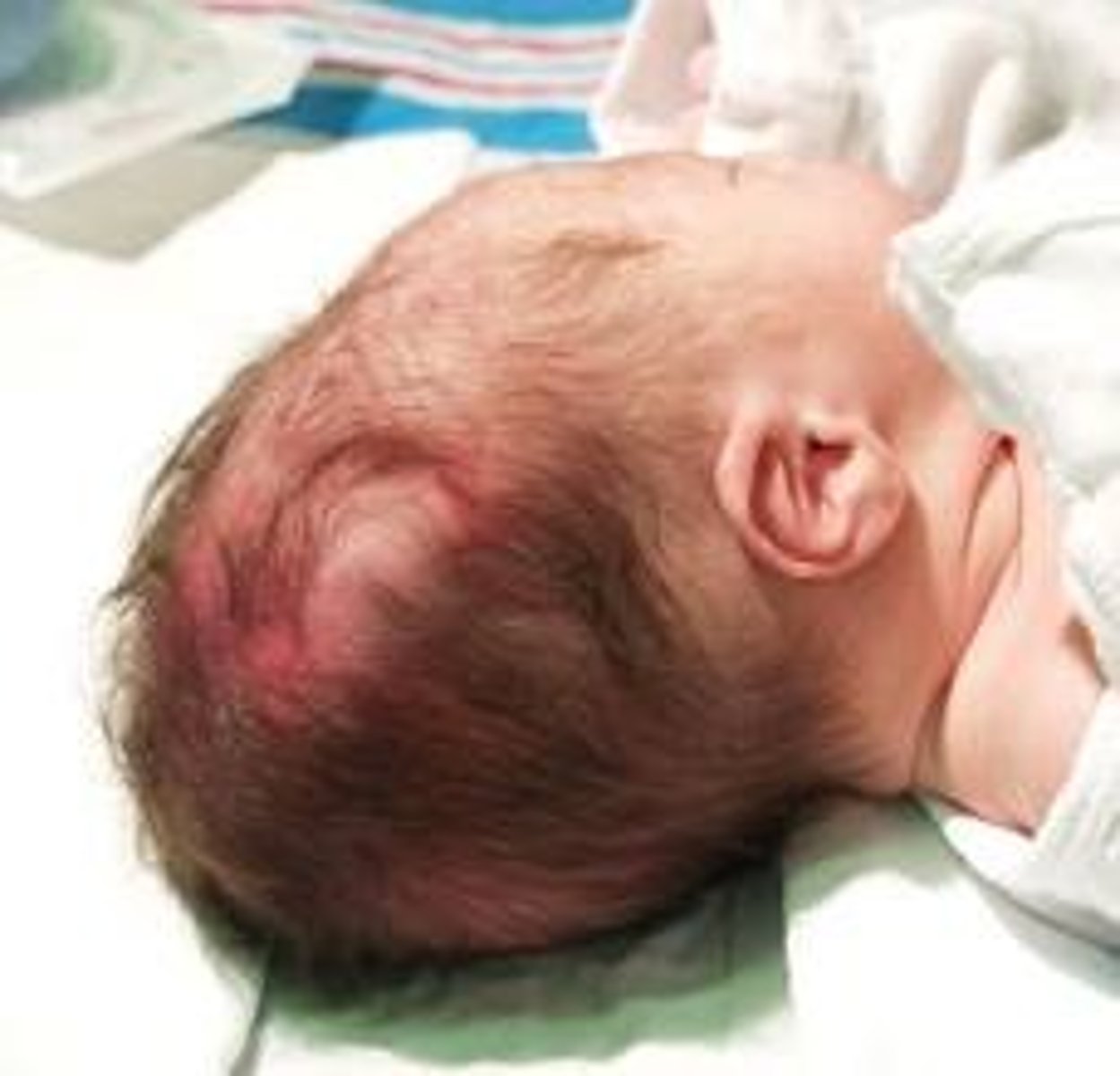
Cephalohematoma
"Fluctuance. Doesn't cross suture lines."
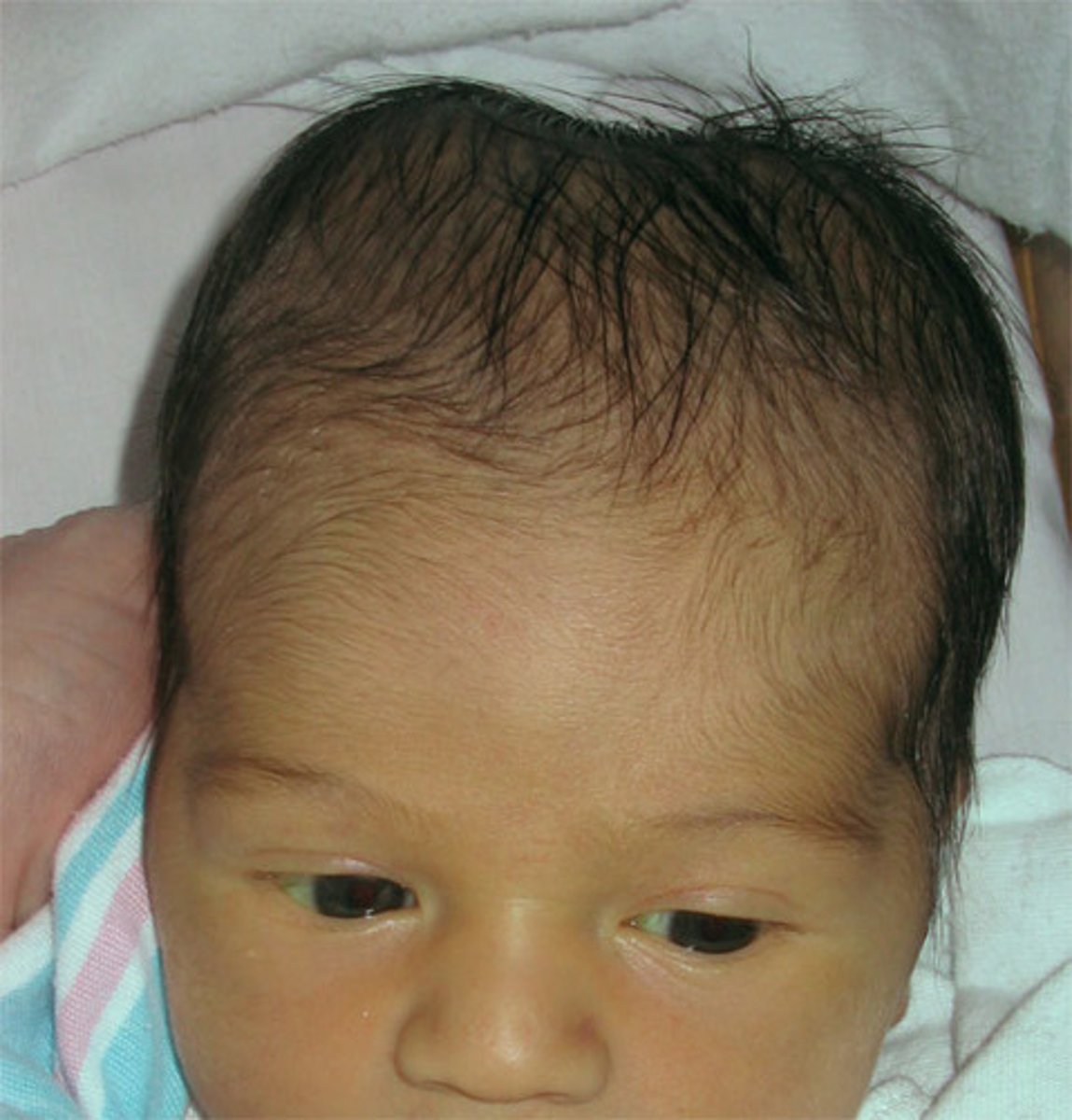
Mongolian Spots
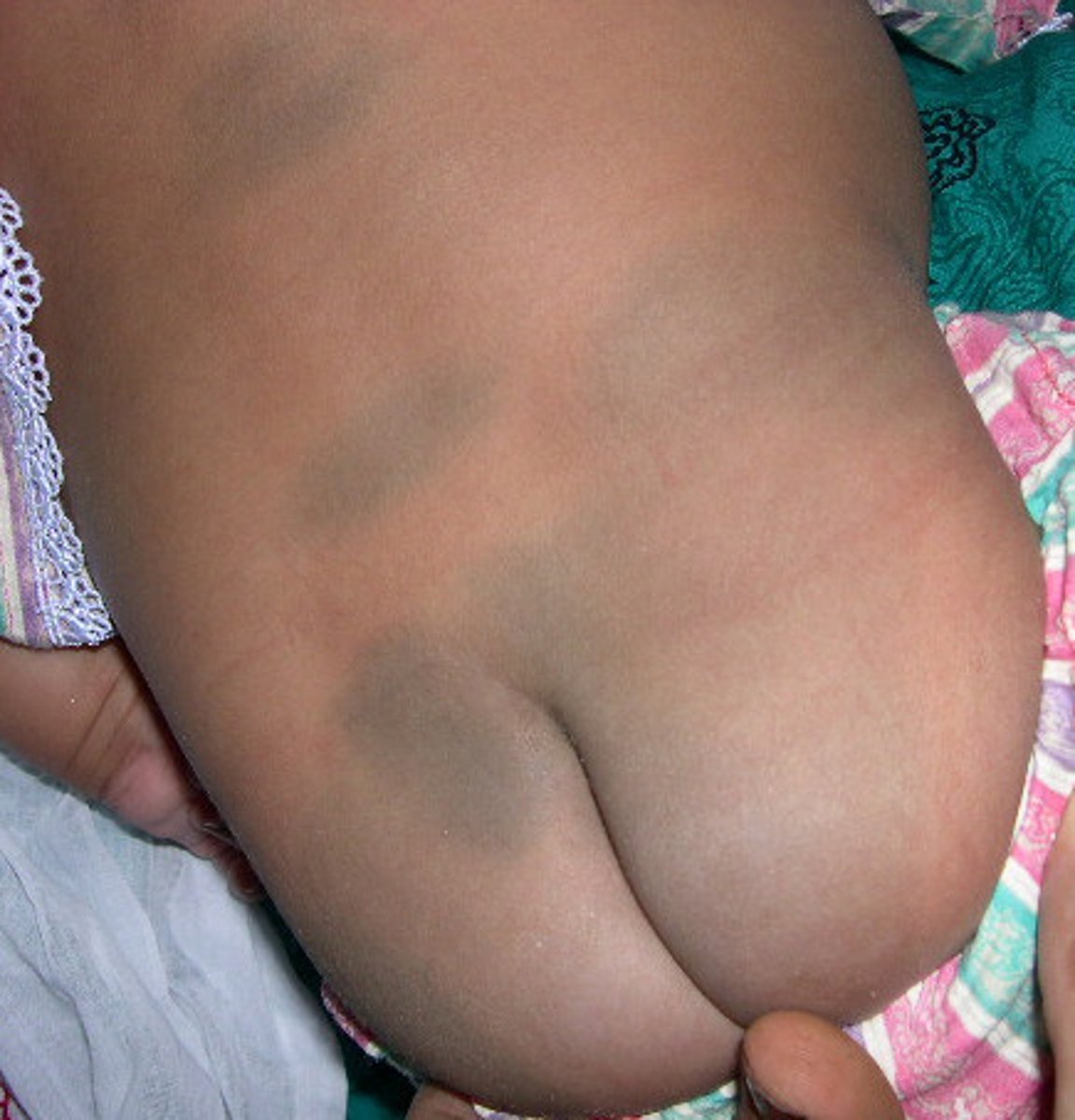
Nevus Simplex (Salmon Patch)
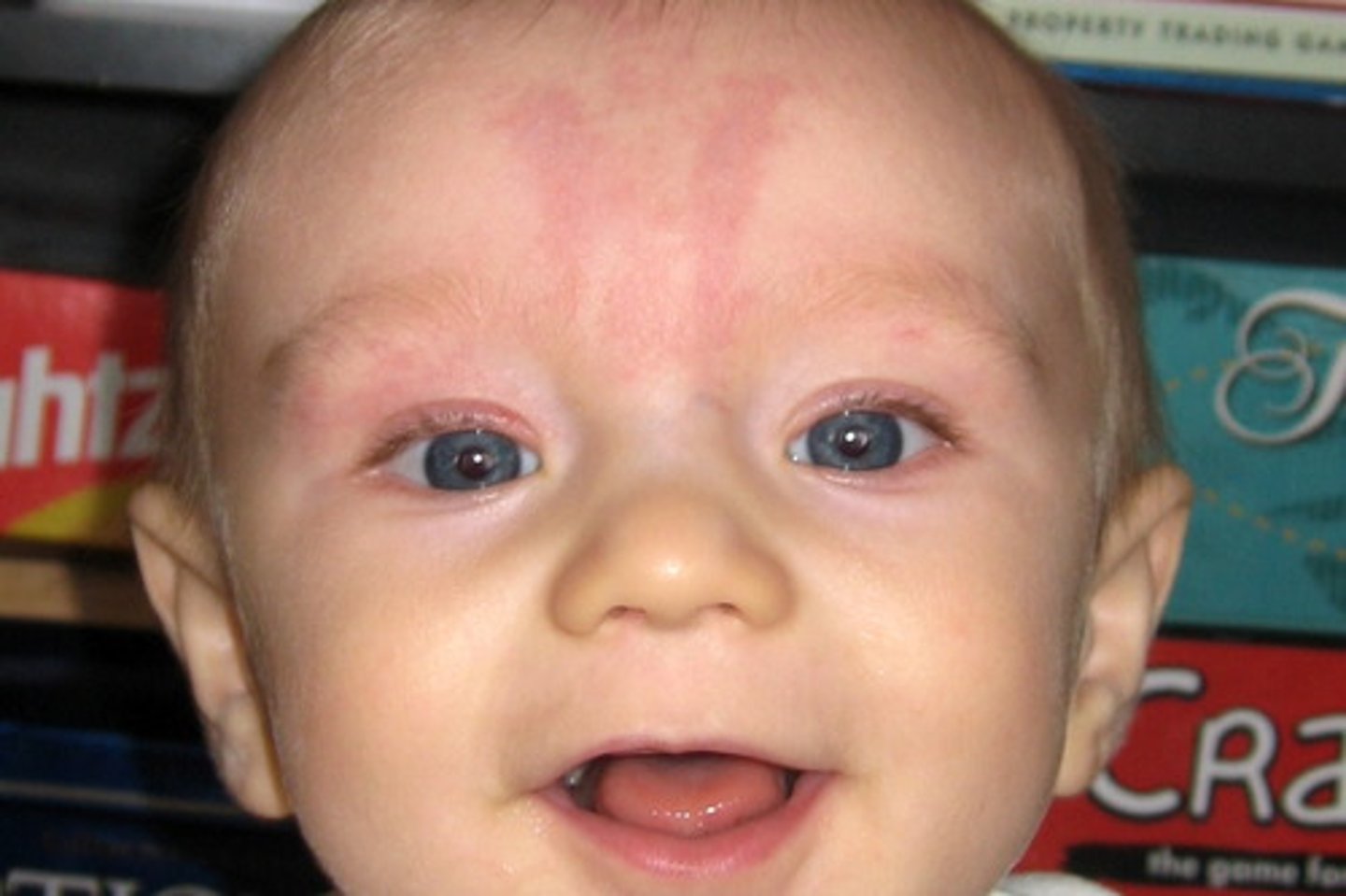
Milia
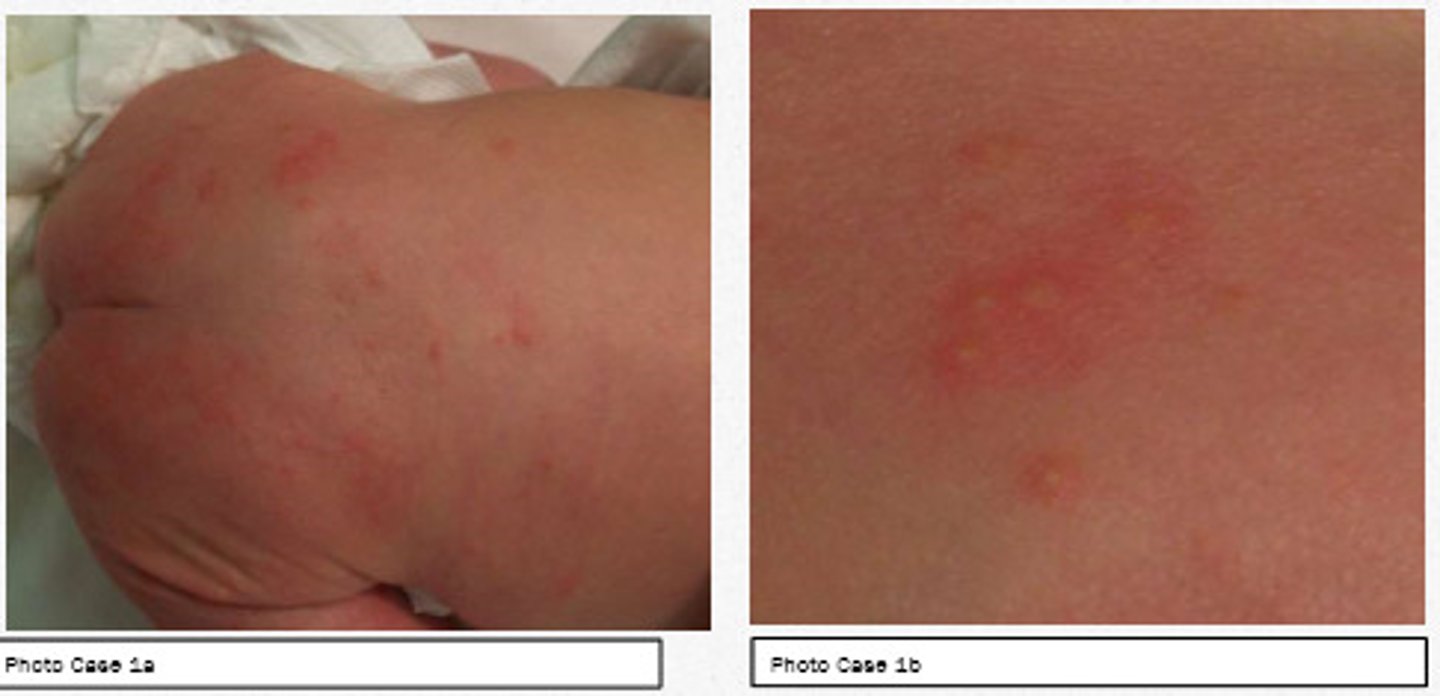
Erythema toxicum
Appears in up to half of newborns carried to term, usually between day 2-5 after birth. Resolves within first two weeks of life, and frequently individual lesions will appear and disappear within minutes or hours. It is a benign condition thought to cause no discomfort to the baby
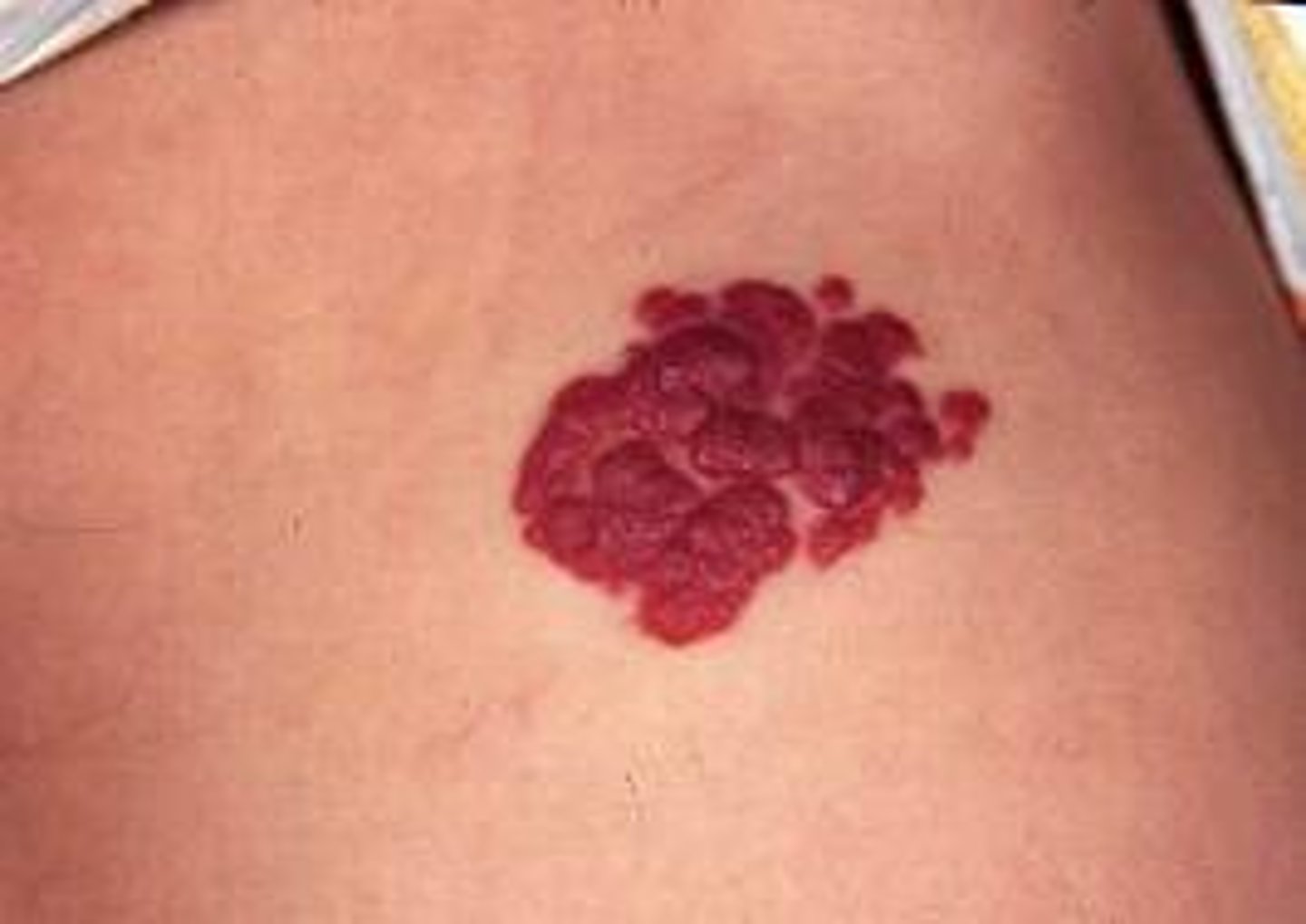
Strawberry Hemangioma
Neonatal Acne
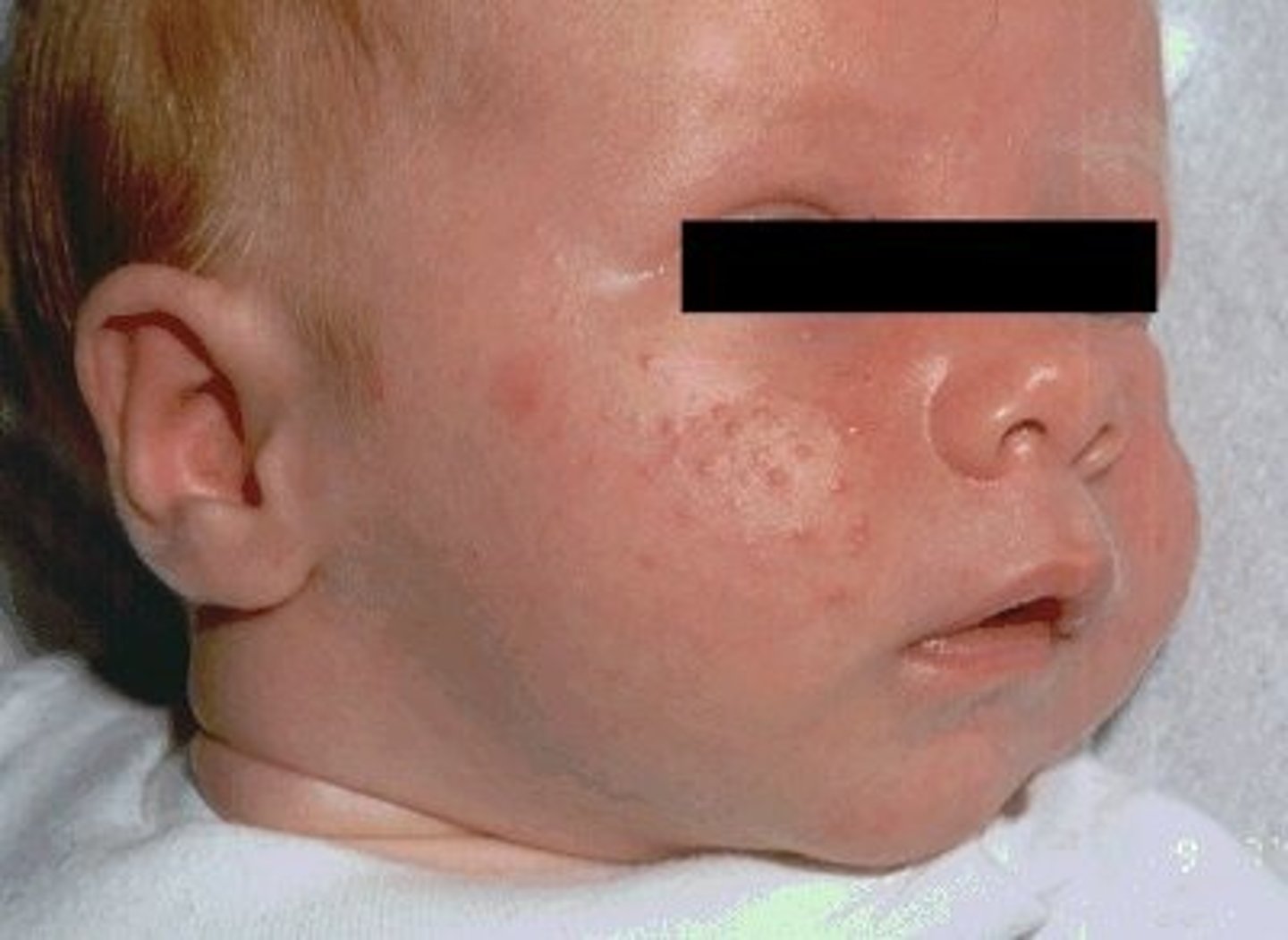
Nevus Sebaceous
"an area of alopecia with orange colored nodular skin"
Remove before adolescence b/c it can undergo malignant degeneration.
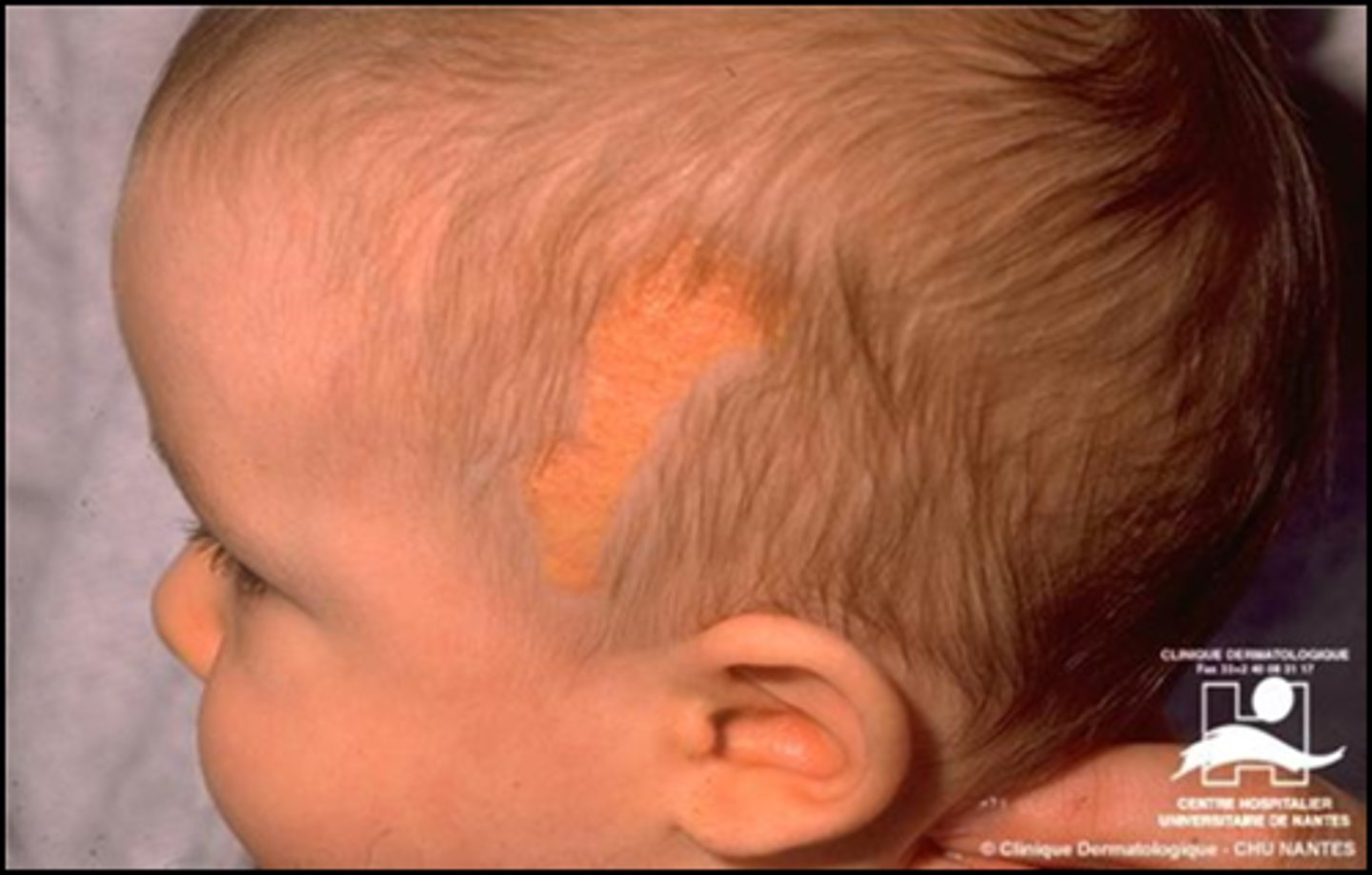
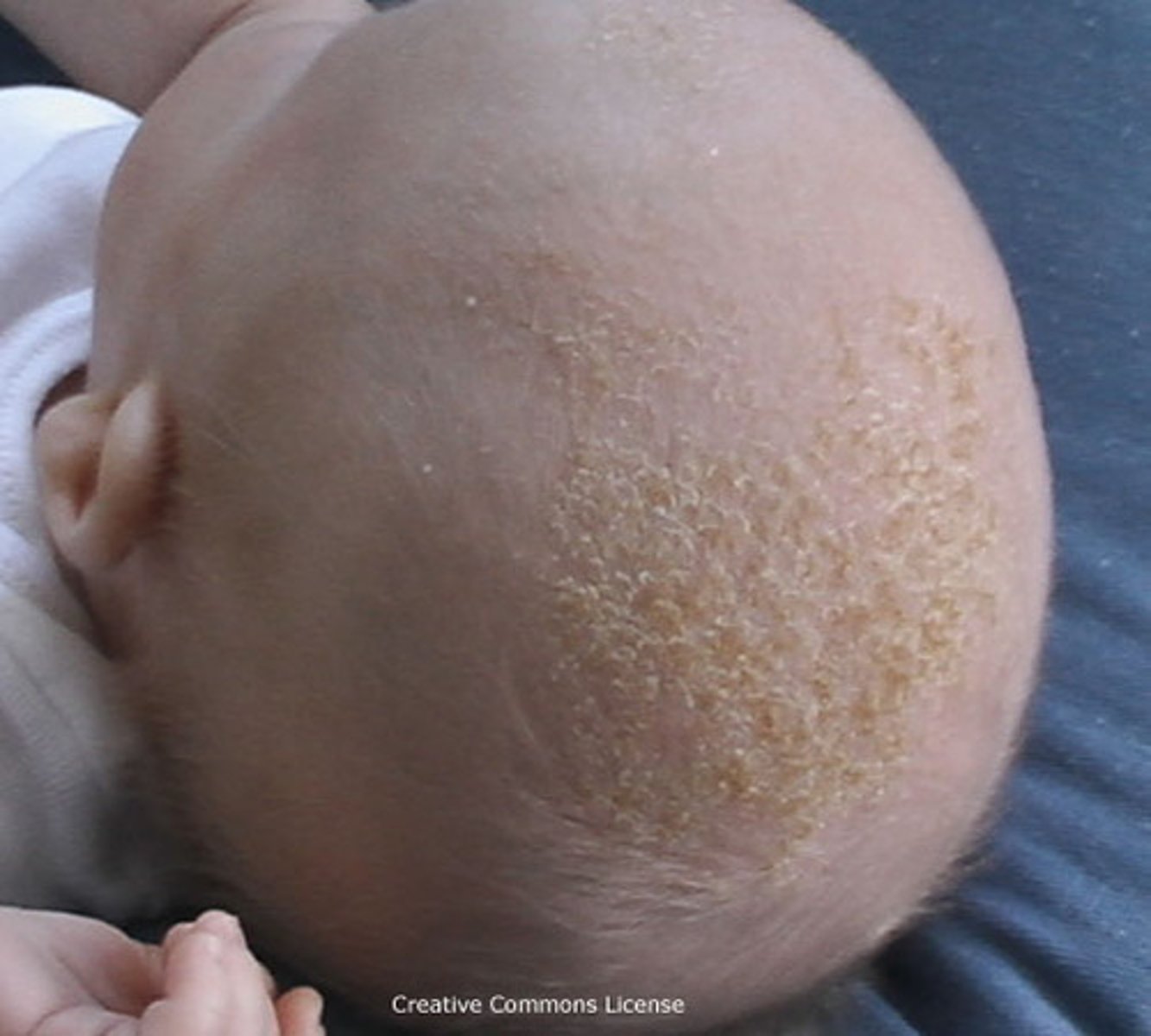
Seborrheic Dermatitis
"thick, yellow/white oily scale on an inflammatory base".
What to do? Gently clean w/ mild shampoo
Phenylketonuria and Galactosemia.
Two disorders screened for in every state because they are disastrous if not caught early (and happen to be a contraindication to breast feeding...)
Deficient G1p-uridyl- transferase. G1p accum to damage kidney, liver, brain.
• Sxs = MR direct hyperbili & jaundice, ↓glc, cataracts, seizures.
• Predisposed to E. coli sepsis.
• No lactose por vida.
Galactosemia.
• Deficient Phe hydrolxalase.
• Sxs = MR, vomiting, athetosis, seizures, developmental delay over 1st few mos
• Signs = fair hair, eyes, skin, musty smell.
• Low Phe diet.
Phenylketonuria.
Physiologic Jaundice. Gone by 5th DOL.
Liver conjugation not yet mature.
3 days old, bili @ 10, direct is 0.5. Eating & pooping well.
Breast feeding Jaundice. ↓feeding = dehydration = retain meconium & re- absorb deconjugated bili.
7 days old, bili @ 12, direct is 0.5. dry mucous membranes, not gaining weight.
Breast milk Jaundice. Breast milk has glucuronidase and de-conj bili.
14 days old, bili @ 12, direct is 0.5. Baby regained birth weight, otherwise healthy.
Pathologic Jaundice = on 1st DOL, bili >12, d-bili >2, rate of rise >5/day.
Test: Coombs
Positive: Rh or ABO incompatability
Negative: twin/twin or mom/fetus transfusion, IDM, spherocytosis, G6p-DH deficiency, etc.
1 day old, bili @ 14, direct is 0.5. Are you worried? Next best test? If positive? If negative?
Biliary atresia. Bile ducts cannot drain bile. Causes liver failure. Need surgery.
7 days old. Dark urine, pale stool. Bili @ 12, dbili is 8. LFTs also elevated.
Always r/o sepsis!
Galactosemia
Hypothyroid
Choledochal cyst
CF
Biliary atresia (<2mo)
Other causes of direct hyperbilirubinemia?
Gilbert - ↓glucoronyl transferase level
Crigler-Najjar (type1) - total deficiency
Random inherited causes of indirect hyperbili? (2)
Dubin-Johnson Sx - asx, black liver
Rotor Sx - NO black liver
Random inherited causes of direct hyperbili (2)
Indirect bili can cross BBB, deposit in basal ganglia and brainstem nuclei and cause kernicterus. (esp if bili is >20)
Why do we care about hyperbilirubinemia?
Phototherapy (Tbil>20)--> ionizes the uncoj bili so it can be excreted.
Double volume exchange transfusion (Tbil>25) if that doesn't work.
Treatment for hyperbilirubinemia
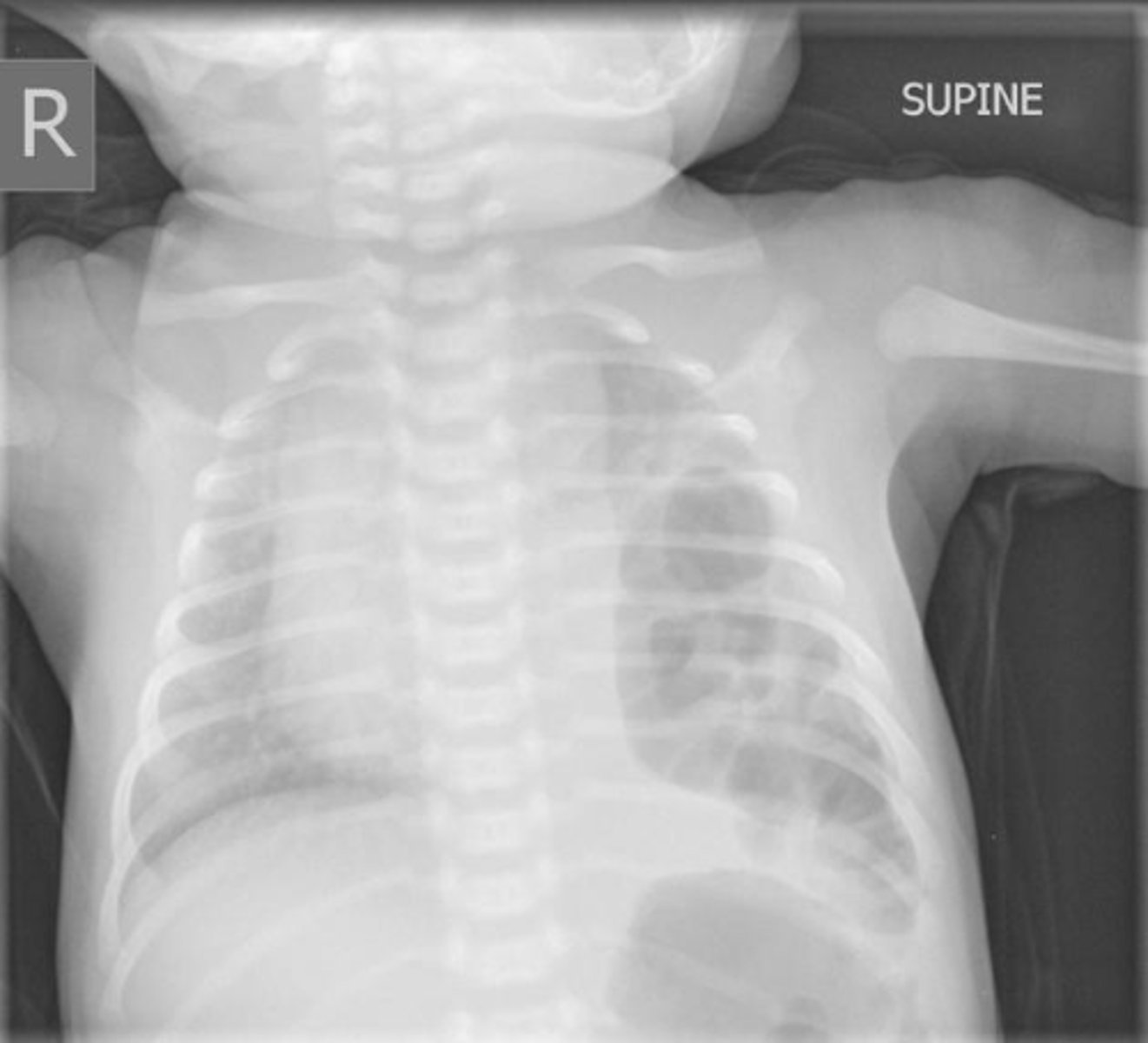
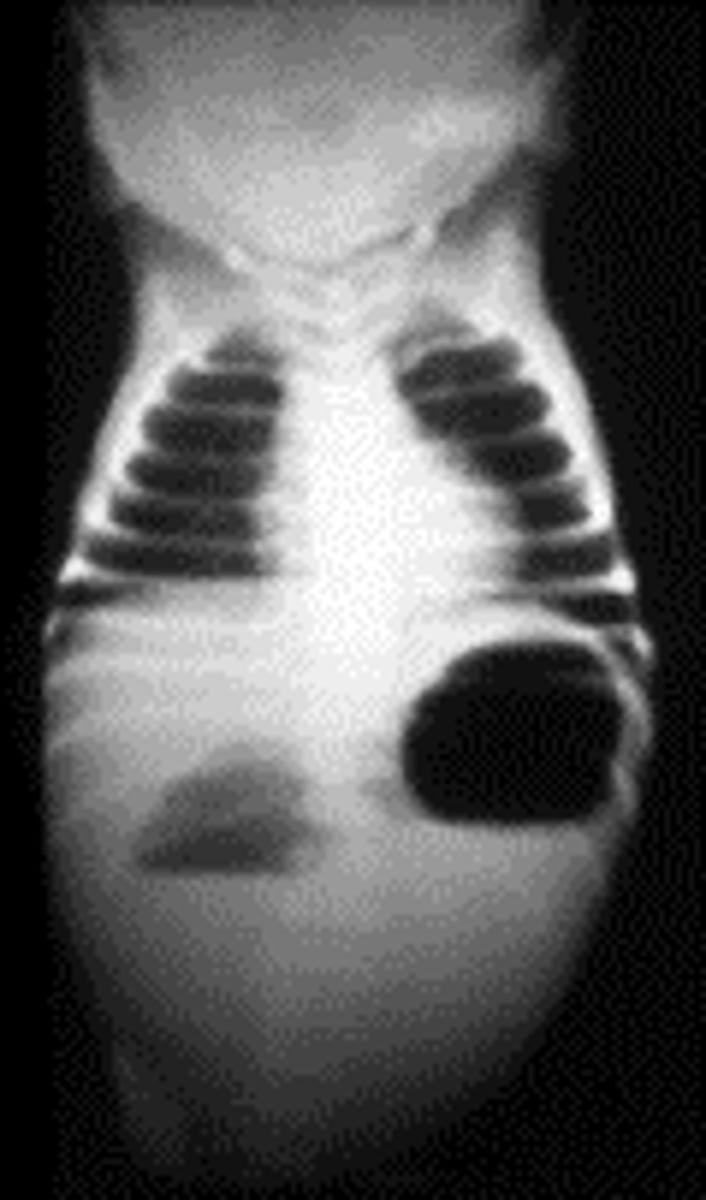
Diaphragmatic hernia
Concern: Pulmonary hypoplasia
Txt: If dx prenatally, plan delivery at @ place w/ ECMO. Let lungs mature 3-4 days then do surg
Baby is born w/ respiratory distress, scaphoid abdomen & this CXR.
• Biggest concern?
• Best treatment?
TE- Fistula
Dx: Place feeding tube, take xray, see it coiled in thorax
Also look for: VACTER associated anomalies- vertebral, anal
atresia, cardiac, radial and renal.
Baby is born w/ respiratory distress w/ excess drooling.
Best Dx test?
What else do you look for?
Choanal Atresia
Also look for: CHARGE associated anomalies- coloboma, heart defects, retarded growth, GU anomalies , Ear anomalies and deafness
1 week old baby becomes cyanotic when feeding but pinks up when crying.
• What else do you look for?
RDS
Prenatal Dx: L/S<2, give antenatal betamethasone
Pathophys: Surfactant def, can't keep alveoli open.
Txt: O2 therapy with nasal CPAP to keep alveoli open
32 wk premie has dyspnea, RR of 80 w/ nasal flaring.
- Prenatal Dx?
- Pathophys?
- Txt?
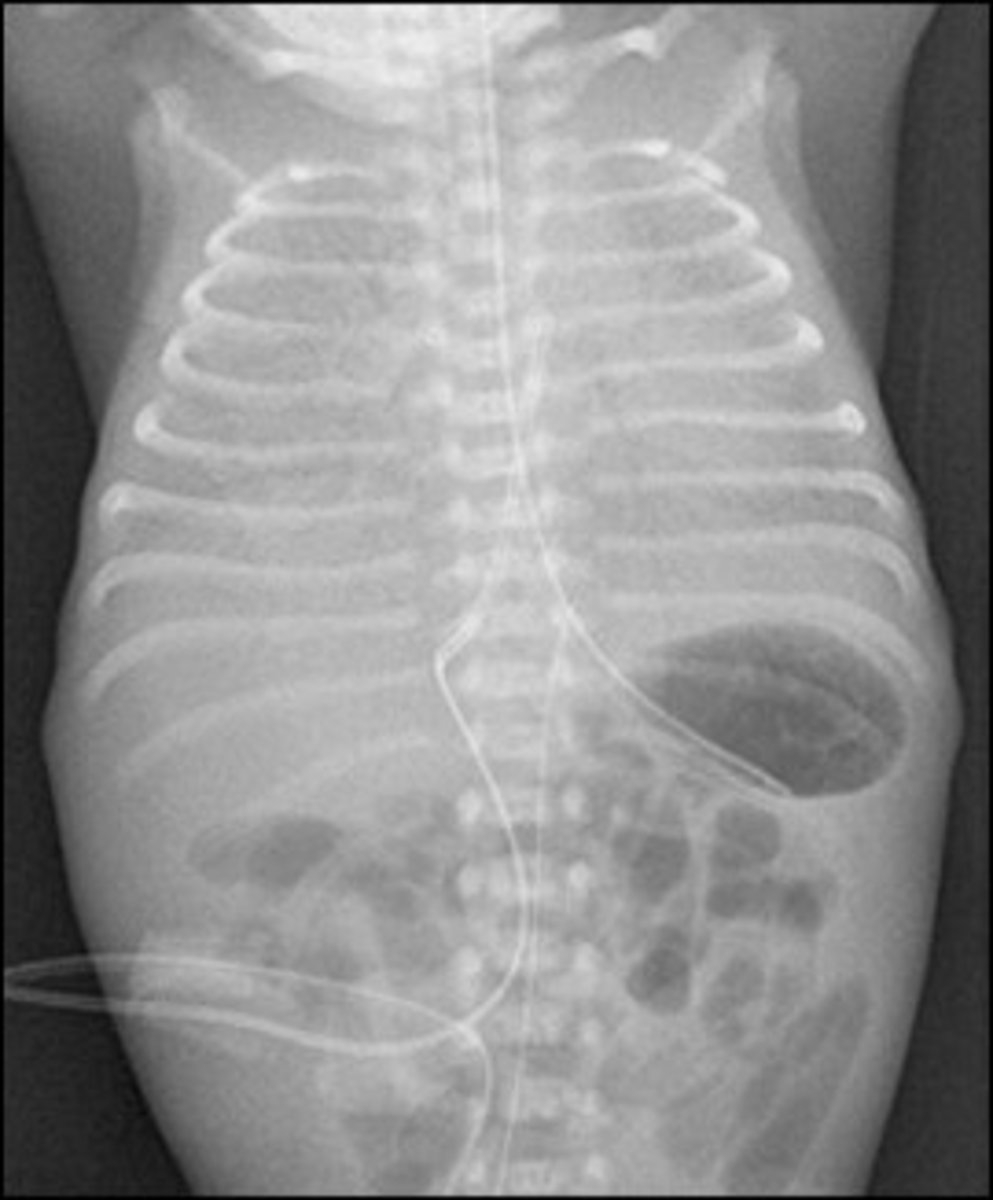
TTN
Pathophys: Lung fluid not squeezed out, retained
Prognosis: Usually minimal O2 needed. Self resolves in hrs to days
38 wk LGA infant born by C/S to an A2GDM has dyspnea/grunting
- Pathophys?
- Prognosis?
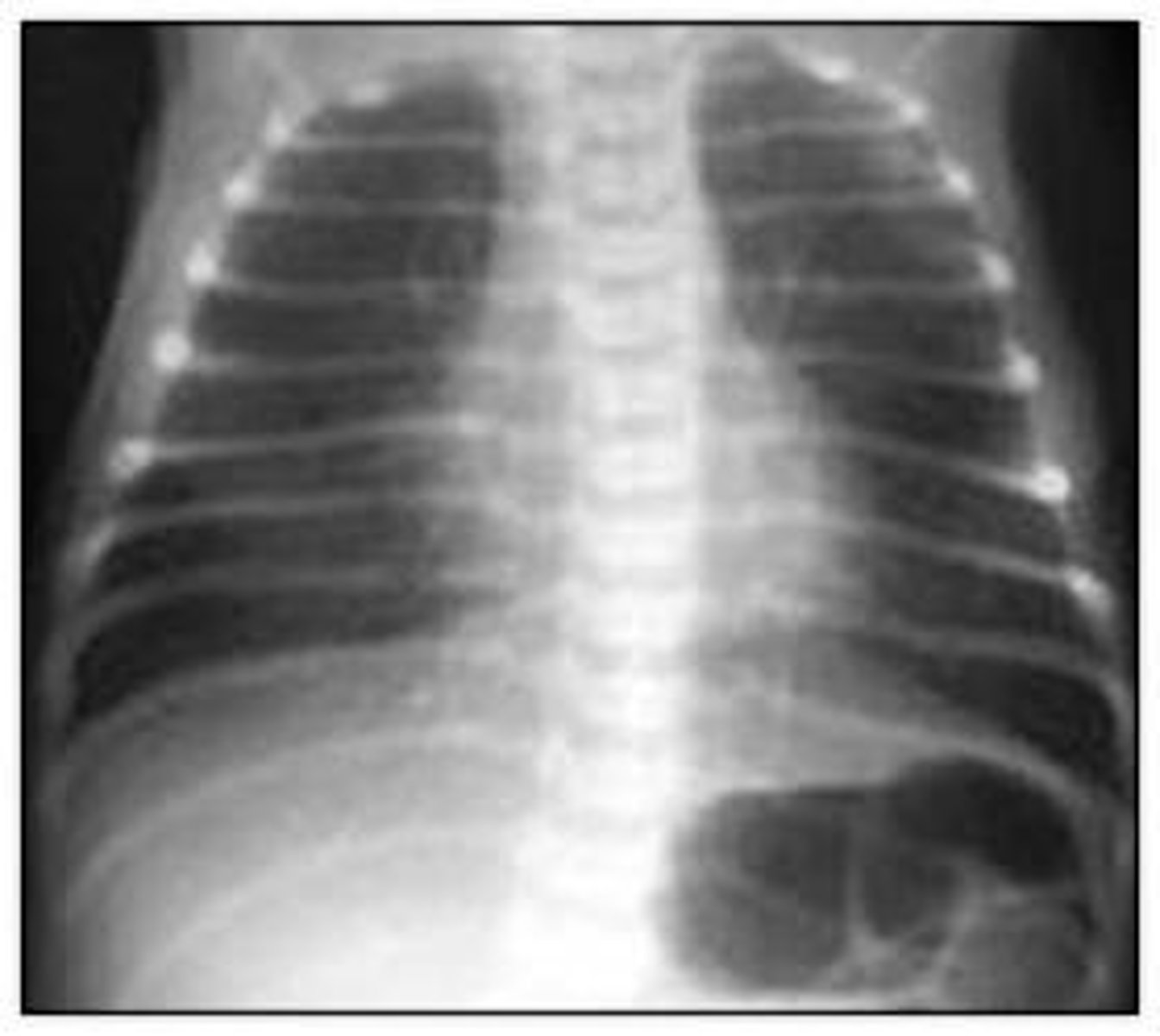
Meconium Aspiration Syndrome
Next: intubate and suction before stimulation
Complications: Pulmonary artery HTN, pneumonitis
41 wk AGA infant was born
after ROM yielded greenish-
brown fluid.
*Next best step?
*Complications?
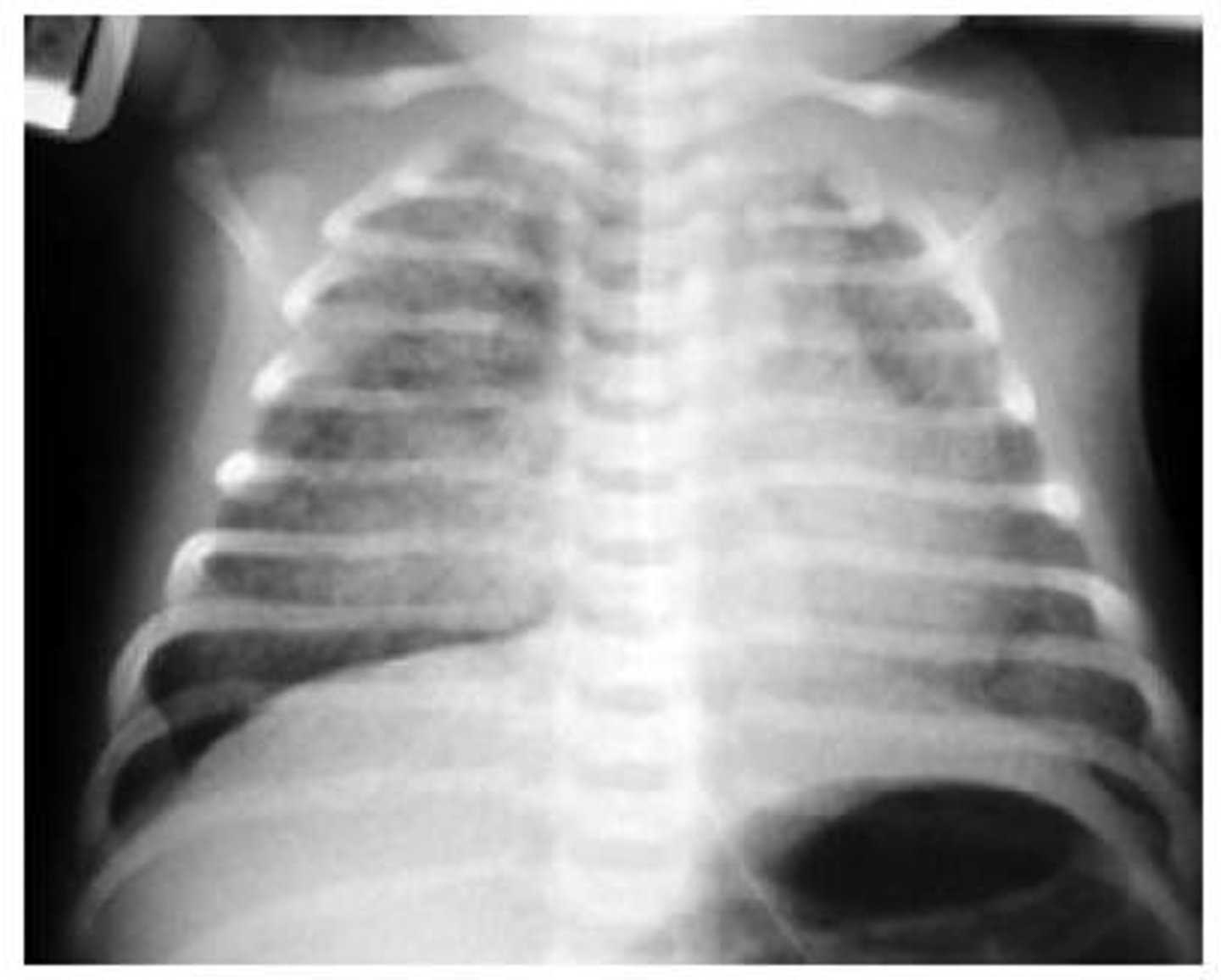
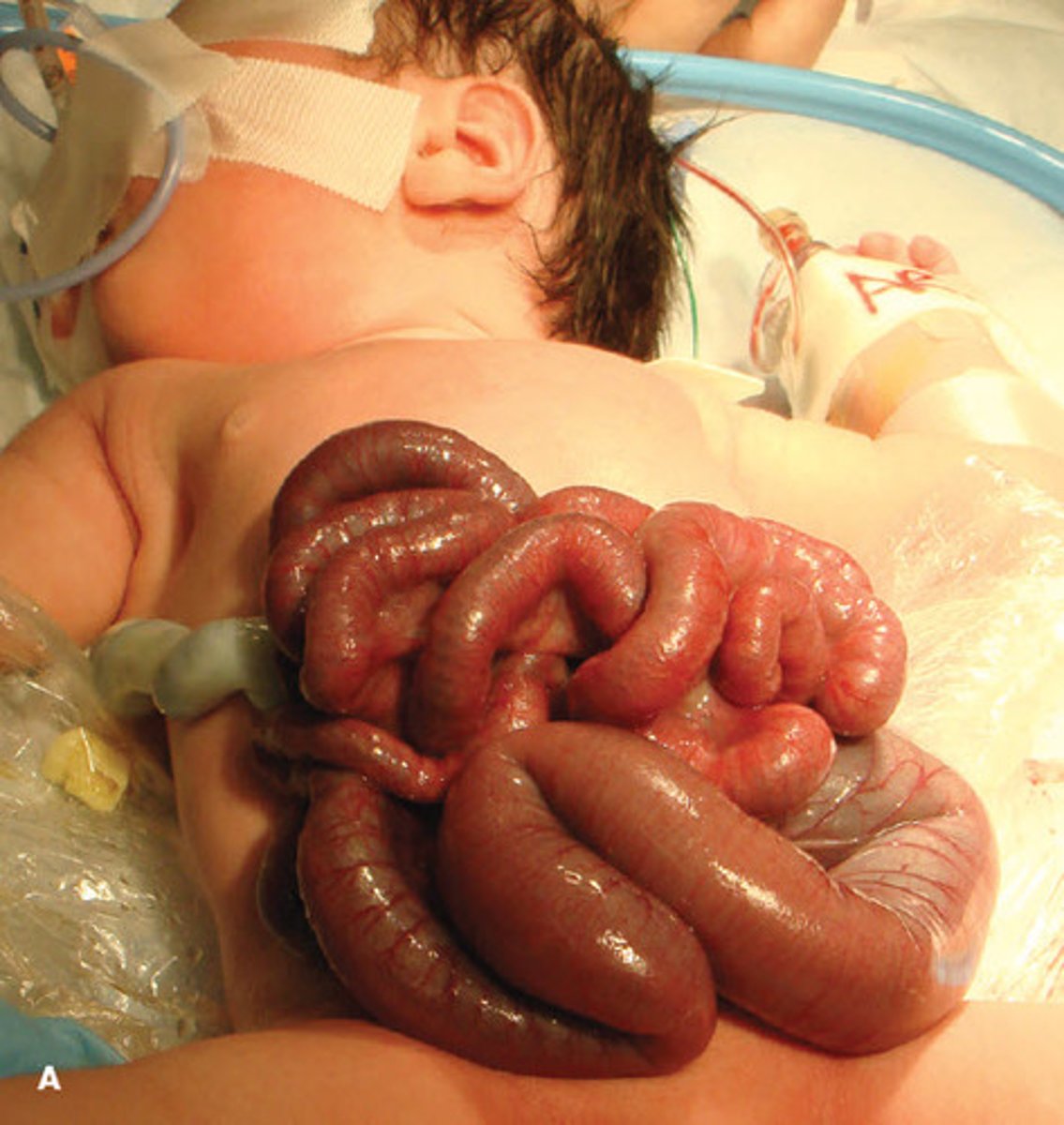
Gastroschisis
will see high maternal AFP
Not usually associated w/ other d/o
Complications: May be atretic or necrotic req removal. Short gut syndrome
Defect lateral (usually R) of midline, no sac
- Assoc w/ other d/o?
- Complications?
Omphalocele
Assoc w/ Edwards & Patau Trisomies, Beckwith Wiedemann Syndrome = big baby w/ big tongue, ↓glc, ear pits
Defect in the midline.
Covered by sac.
- Assoc w/ other disorders?
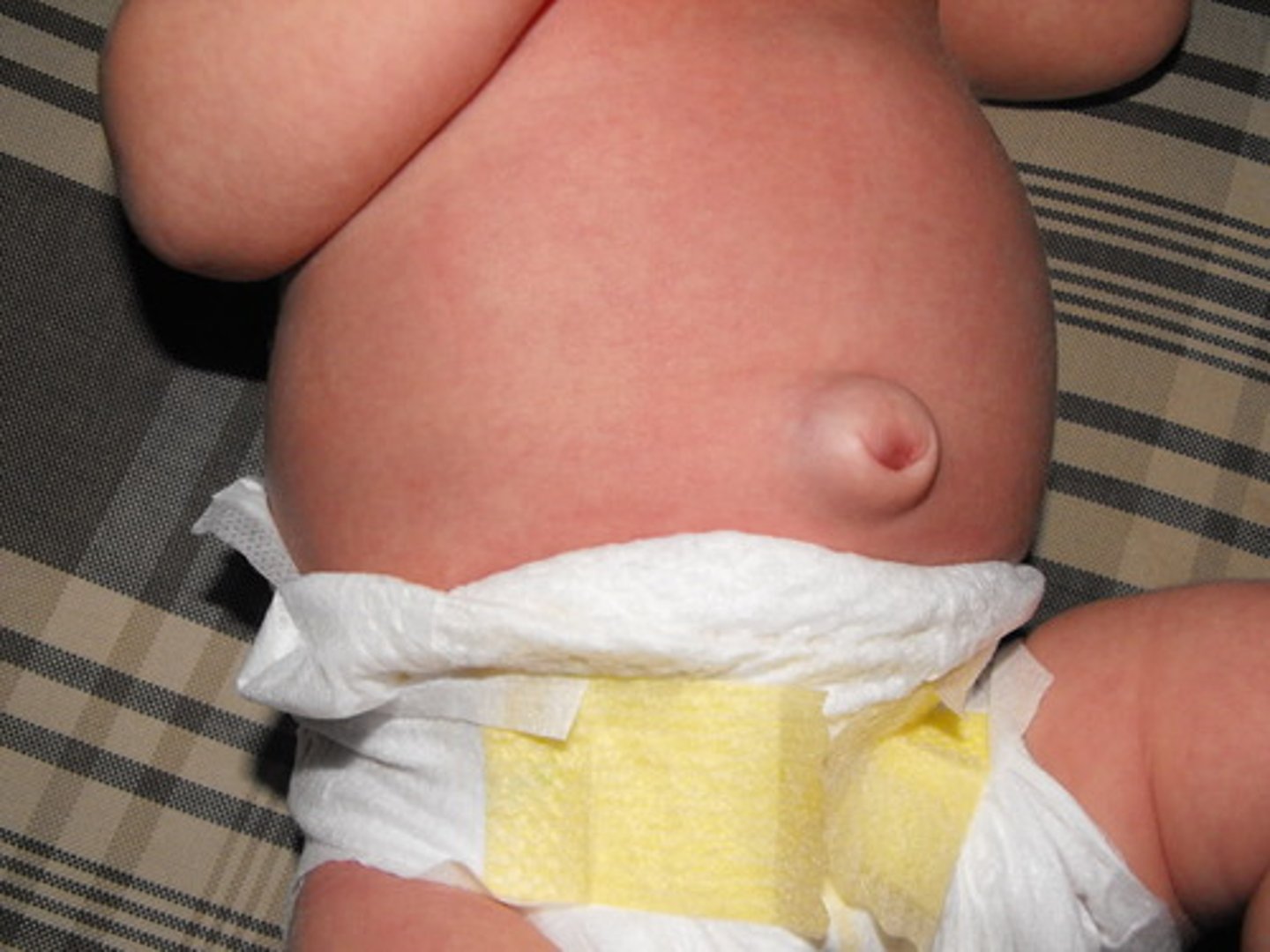
Umbilical hernia
Assoc w/ congenital hypothyroidism. (also big tongue)
Repair not needed unless persists past age 2 or 3yo
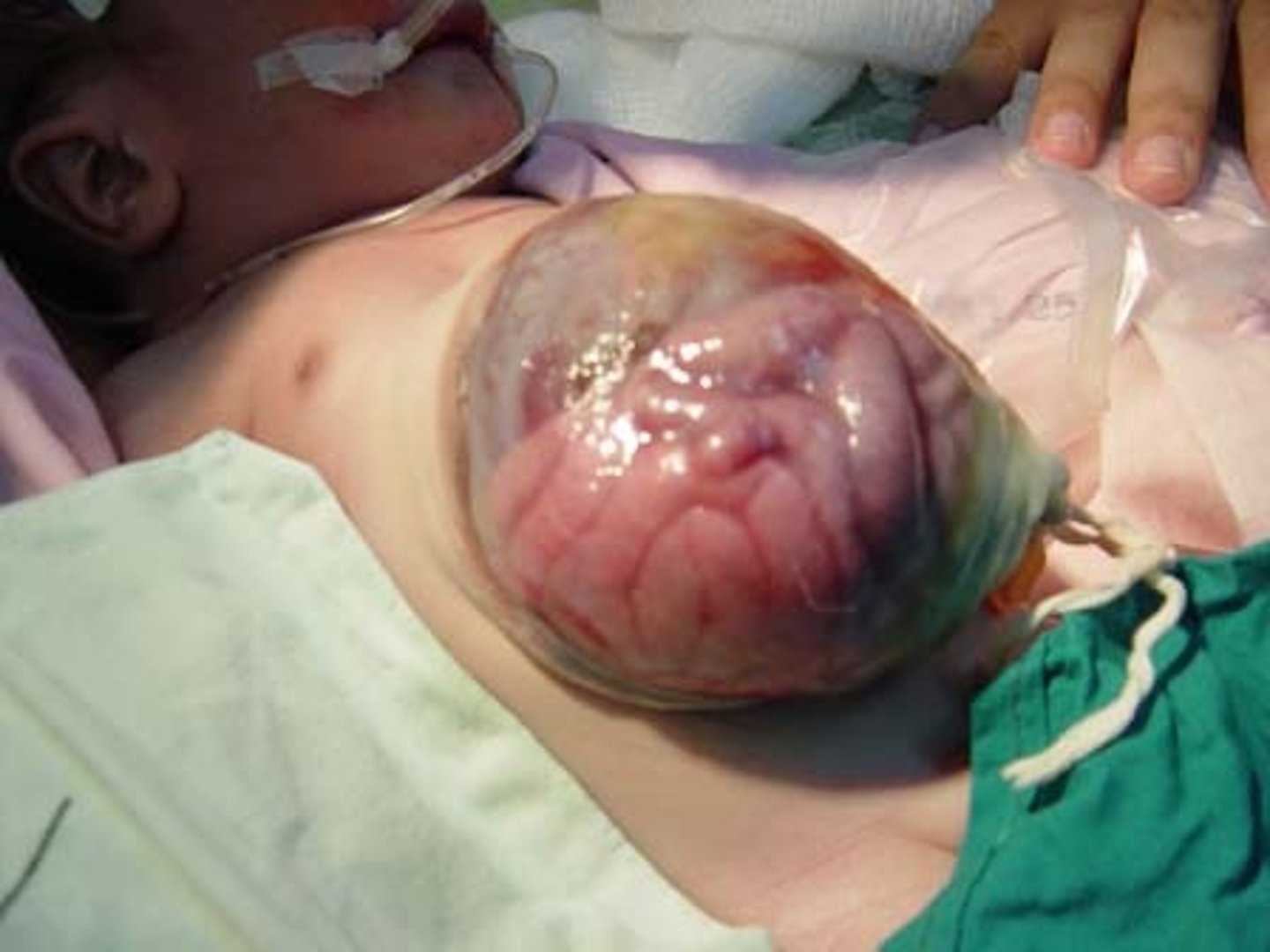
Defect in the midline. No bowel present.
- Assoc w/ other d/o?
- Txt?
Pyloric stenosis
Complications: hypochloremic metabolic alkalosis
Txt: immediate surgery referral for myotomy
4wk old infant w/ non- bileous vomiting and palpable "olive"
- Metabolic complications?
- Txt?
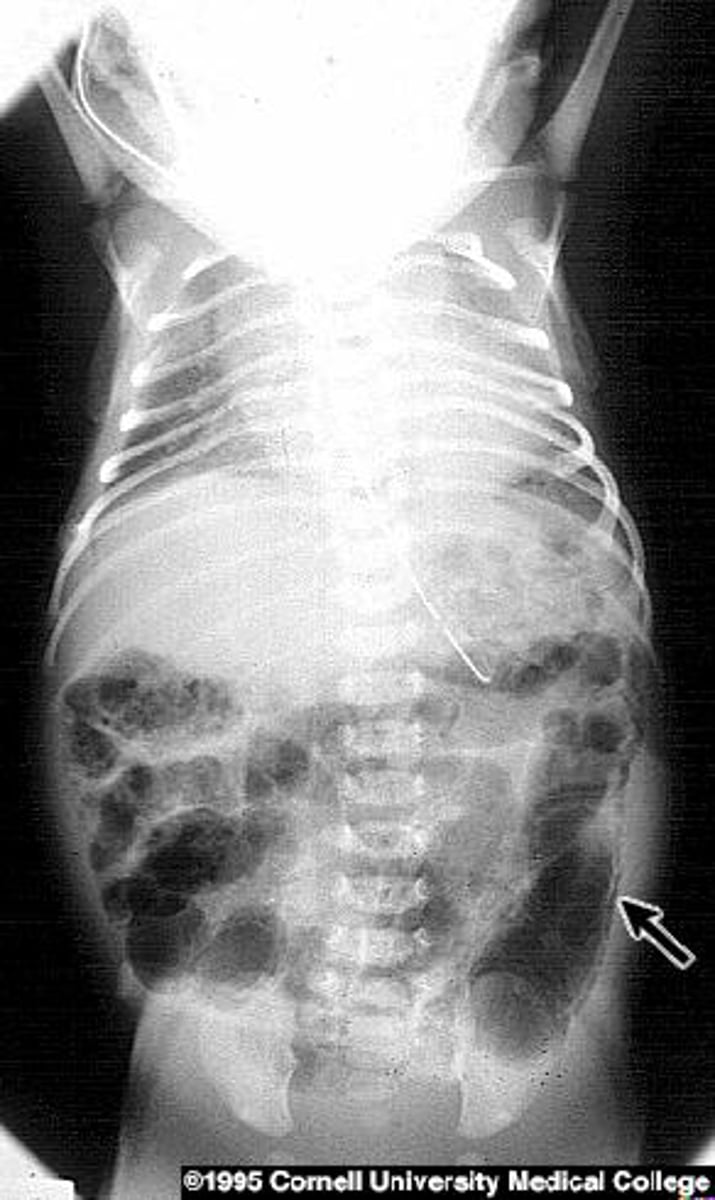
Intestinal Atresia
(Or Annular Pancreas)
Assoc w/ Down Syndrome (esp duodenal)
2wk old infant w/ bileous vomiting. The pregnancy was complicated by poly- hydramnios.
- Assoc w/?
Malrotation and volvulus
*Ladd's bands can kink the duodenum
Gut fails to rotate 270* counterclockwise around SMA
1 wk old baby w/ bileous vomiting, draws up his legs, has abd distension.
- Pathophys?
Meconium ileus- consider CF if +FH *gastrograffin enema is dx & tx
Hirschsprung's- DRE --> exposion of poo. bx showing no ganglia is gold standard
A 3 day old newborn has still not passed meconium.
- DDX? (name 2)
Necrotizing enterocolitis
- What do you see on X-ray? pneumocystis intestinal (air in bowel wall)
- Treatment? NPO, TPN (if nec), antibiotics and resection of necrotic bowel
- Risk factors? Premature gut, introduction of feeds, formula.
A 5 day old former 33 weeker develops bloody diarrhea
- What do you see on xray?
- Treatment?
- Risk factors?
Intussusception
*Barium enema is dx and tx
A 2mo old baby has colicky abd pain and current jelly stool w/ a sausage shapend mass in the RUQ.
Cryptorchidism
Assoc w/ prune belly syndrome
- Where are they usually? Inguinal canal
- Next best test? US if not palpable
- When to do surgery? If not descended by 1yr to avoid sterility/cancer
Newborn male with no palpable testes.
- Where are they usually?
- Next best test?
- When to do surgery?
Hypospadias
DON'T circumcise! Foreskin is used in eventual repair
Newborn male with urethral opening on the ventral surface.
- What do you NOT do?
Congenital Adrenal Hyperplasia
- Most common Cause? 21 Hydroxylase deficiency. (autosomal recessive)
- Definitive test? 17-OH progesterone before and after ACTH bolus
- Tx? Hydrocortisone and fludrocortisone (↑ doses in times of stress)
Newborn child with ambiguous genitalia. One month later has vomiting & ↓Na ↑K and acidosis.
- Most common Cause?
- Definitive test?
- Tx?
- Prenatal care? Control glc in the 1st trimester & take 4mg folate/day
- Risks to fetus? Placental insufficiency/IUGR, Congenital heart dz, NTD, Caudal regression syndrome, Small left colon syndrome
Mothers with pre-existing diabetes (esp type 1)
- Prenatal care?
- Risks to fetus?
- LGA. ↑risk of birth trauma (clavicle, Erbs), C/S & TTN
- Hypoglycemia. Why? Maternal hyperglycemia --> fetal hyperinsulinemia. Complications? Neonatal seizure (always check glc!). Treatment? Feed frequently if <40. IV dextrose if <20
- Hypocalcemia. Neonatal seizure (always check Ca!)
- Polycythemia. Why? Big baby needs more O2, hypoxia-->↑EPO. Complications? Renal or splenic vein thromboses
- Jaundice. More RBCs to bread down. Risk for kernicterus
- RDS. ↑insulin interferes w/ cortisol surge prior to birth that normally stimulates lung maturation. Check L/S ratio >2
Risks of infants born to mothers with gestational diabetes
Sepsis until proven otherwise
baby < 28 days old has a fever >100.4
CBC w/ diff, CXR, blood cultures, urine cultures (use catheter), LP
Sepsis workup in neonate
Prematurity, chorioamnionitis, intrapartum fever, maternal leukocytosis,
prolonged rupture of membranes (>18hrs), GBS+ mom.
Risk factors for neonatal sepsis?
Group B Strep
E. Coli
Lysteria monocytogenes
Most common neonatal sepsis bugs?
Ampicillin + Gentamicin until 48hr cx are negative
Cefotaxime + Ampicillin if meningitis suspected
Empiric txt for neonatal sepsis?
Syphilis
Tx w/ PCN
Maculopapular rash on palms and soles, snuffles, periostitis. Txt?
Toxoplasmosis
Tx w/ sulfadiazine + leucovorin.
Hydrocephalus, intracranial calcifications and chorioretinitis. Txt?
Rubella
No tx.
Cataracts, deafness and heart defects (esp PDA, VSD), extramedullary hematopoeisis. Txt?
CMV
Tx w/ ganciclovir, but won't prevent MR
Microcephaly, periventricular calcifications, deafness, thrombo- cytopenia and petechiae. Txt?
Congenital Varicella if mom infected 1st or 2nd trimester. If mom is exposed 5 days before - 2 days after delivery, baby gets VZIG.
Limb hypoplasia, cutaneous scars, cataracts, chorioretinits, cortical atrophy. Txt?
Chemical conjunctivitis caused by silver nitrate drops. Not common anymore b/c we use erythromycin.
Neonatal conjunctivitis: DOL 1-3, red conjunctiva and tearing.
Gonococcal conjunctivitis tx w/ topical erythromycin and IV 3rd gen ceph.
Neonatal conjunctivitis: DOL 3-5, bilateral purulent conjunctivitis can cause corneal ulceration.
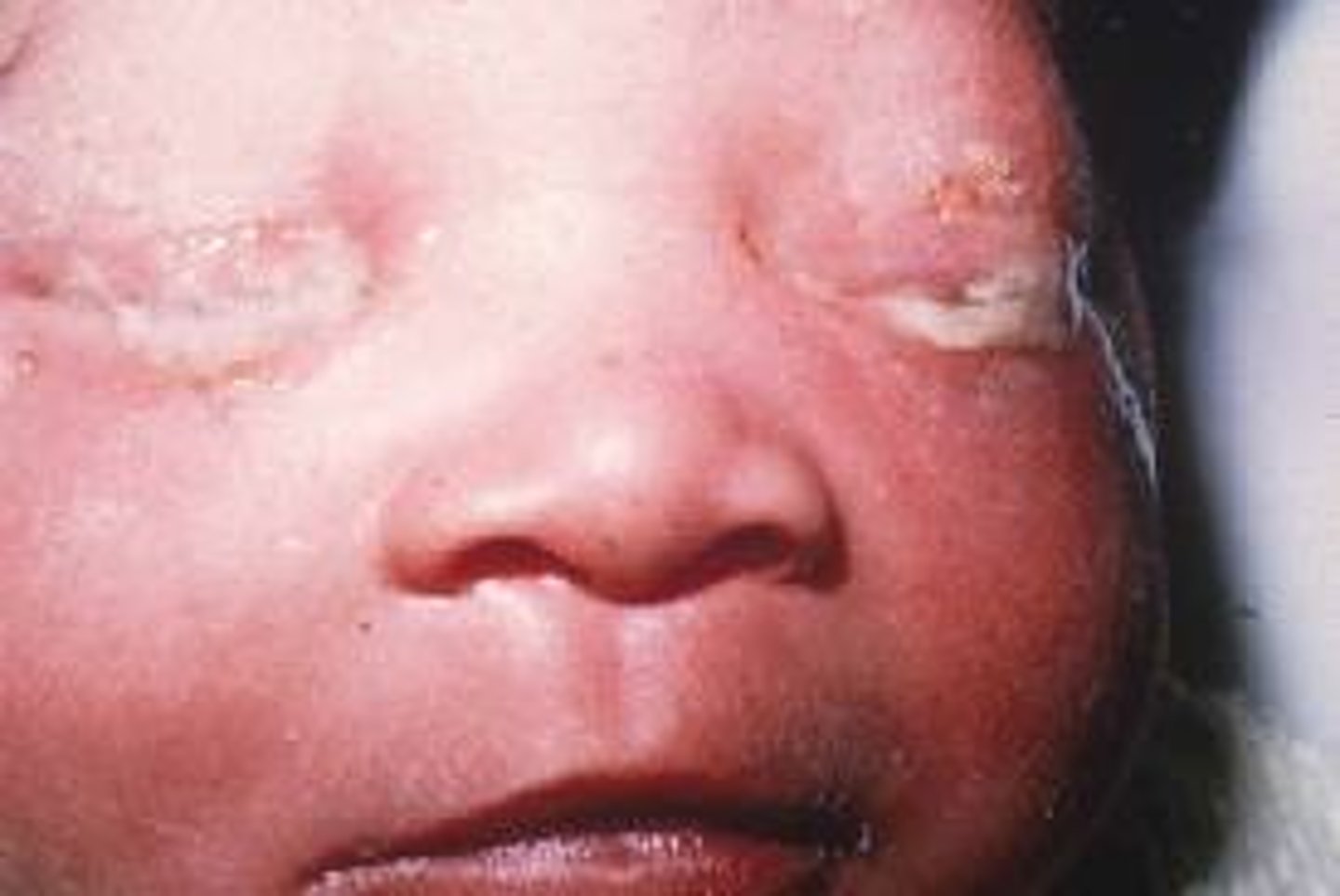
Chlamydia conjunctivitis tx w/ oral erythromycin. Complication is chlamydial pneumonia --> cough, nasal drainage, scattered crackles + bilat infiltrates on CXR
Neonatal conjunctivitis: DOL 7-14, red conjunctiva w/ mucoid discharge & lid swelling
Down's Syndrome
He will likely have moderate MR. Speech, gross and fine motor skill delay
A newborn baby has decreased tone, oblique palpebral fissures, a simian crease, big tongue, white spots on his iris
- What can you tell his mother about his expected IQ?
- Heart? VSD, endocardial cushion defects
- GI? Hirschsprung's, intestinal atresia, imperforate anus, annular pancreas
- Endocrine? Hypothyroidism
- Msk? Atlanto-axial instability
- Neuro? Increased risk of Alzheimer's by 30-35. (APP is on Chr21)
- Cancer? 10x increased risk of ALL
Common medical complications of Down's Syndrome?
Edward's syndrome (Trisomy 18)
Omphalocele, rocker-bottom feet/ hammer toe, microcephaly and clenched hand, multiple others.
Patau's syndrome (Trisomy 13)
Holoprosencephaly, severe mental retardation and microcephaly, cleft lip/palate, multiple others.
Turner's syndrome. XO.
Most common genotype of aborted fetuses
Txt? Estrogen replacement for secondary sex char, and avoid osteoporosis
14 year old girl with no breast development, short stature and high FSH.
Txt?
Horseshoe kidney, coarctation of aorta, bicuspid aortic valve
Anomalies assoc w/ Turner's syndrome?
Klinefelter's syndrome
*increased risk for gonadal malignancy
18 year old tall, lanky boy with mild MR has gynecomastia and hypogonadism.
Neurofibromatosis
Café-au-lait spots, seizures, large head. Autosomal dominant
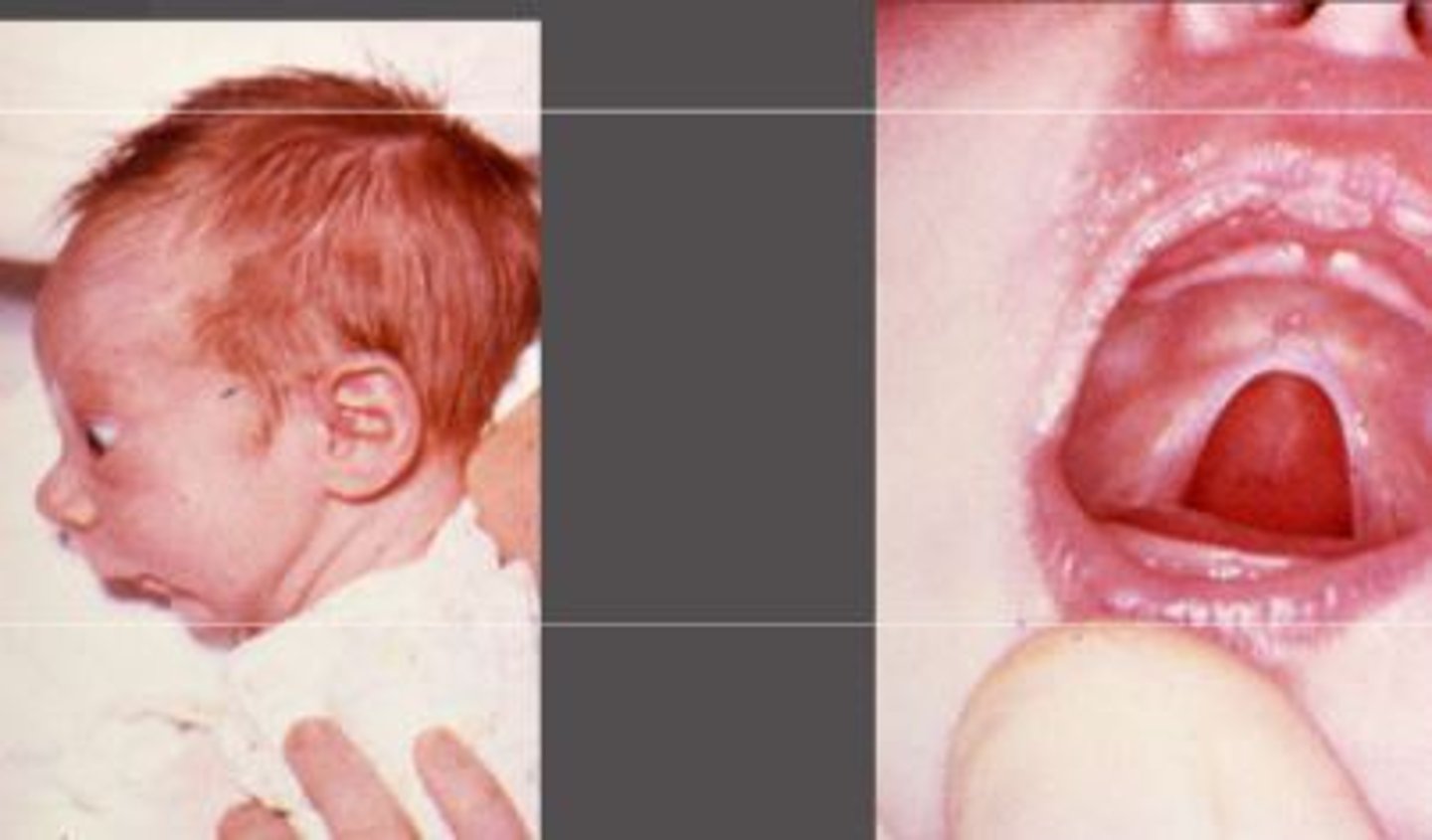
Pierre Robin Sequence
Mandibular hypoplasia, glossoptosis, cleft soft palate. W/ FAS or Edwards.
Smith Magenis Syndrome
Deletion on Chr17
Broad, square face, short stature, self-
injurious behavior.

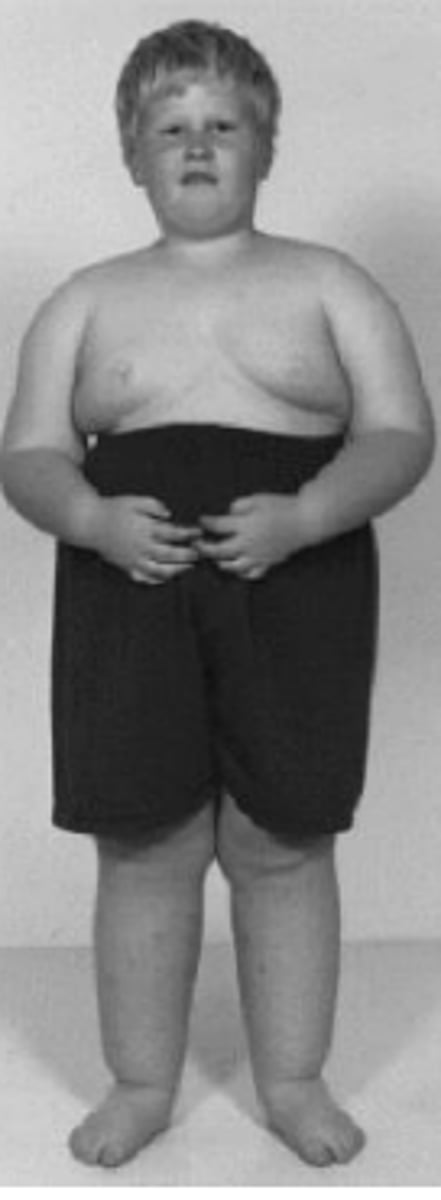
Prader-Willi Syndrome
Deletion on paternal Chr15
Hypotonia, hypogonadism, hyperphagia, skin picking, agression.
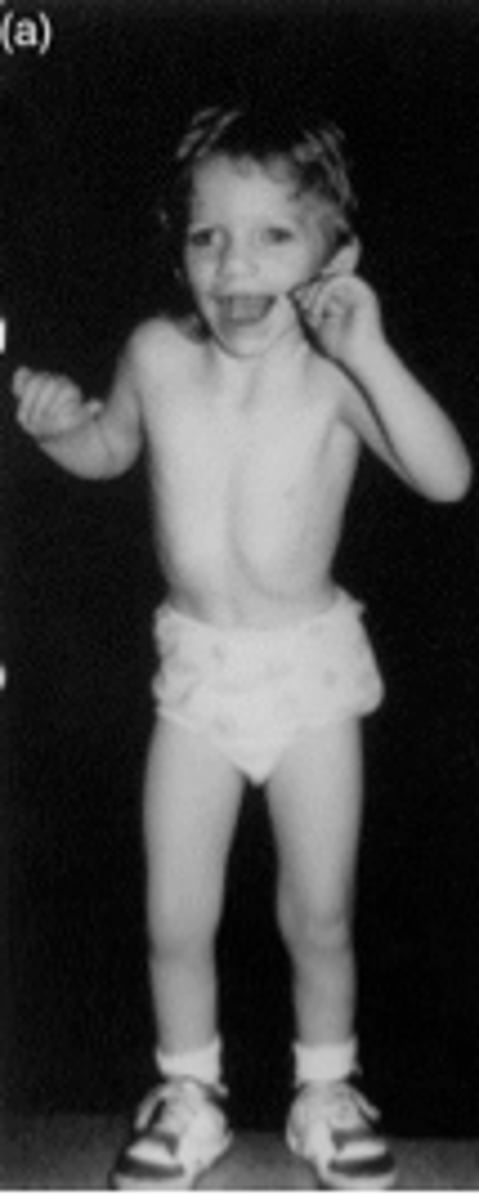
Angelman Syndrome
Deletion on maternal Chr15.
Seizures, strabismus, sociable w/ episodic laughter.
Williams Syndrome
Deletion on Chr7.
Elfin-appearance, friendly, increased empathy and verbal reasoning ability.

Cornelia de Lange
IUGR, hypertonia, distinctive facies, limb malformation, self-injurious behavior, hyperactive.

Fetal Alcohol Syndrome
Microcephaly, smooth philtrum, thin upper lip, ADHD-like behavior. Most common cause of mental retardation.
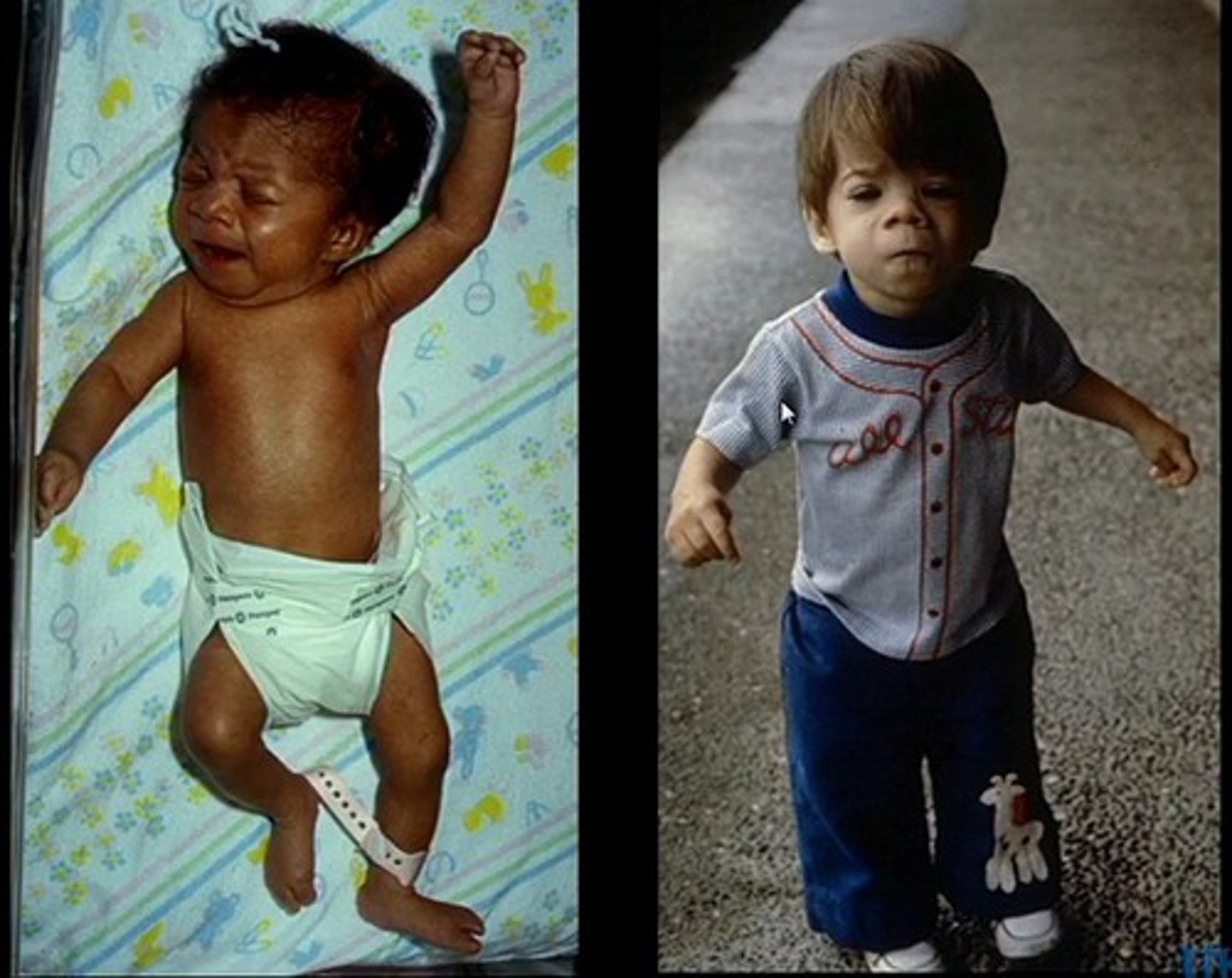
Fragile X Syndrome
CGG repeats on the X-chr w/ anticipation.
Most common type of MR in boys, Macrocephaly, macro- orchidism, large ears.
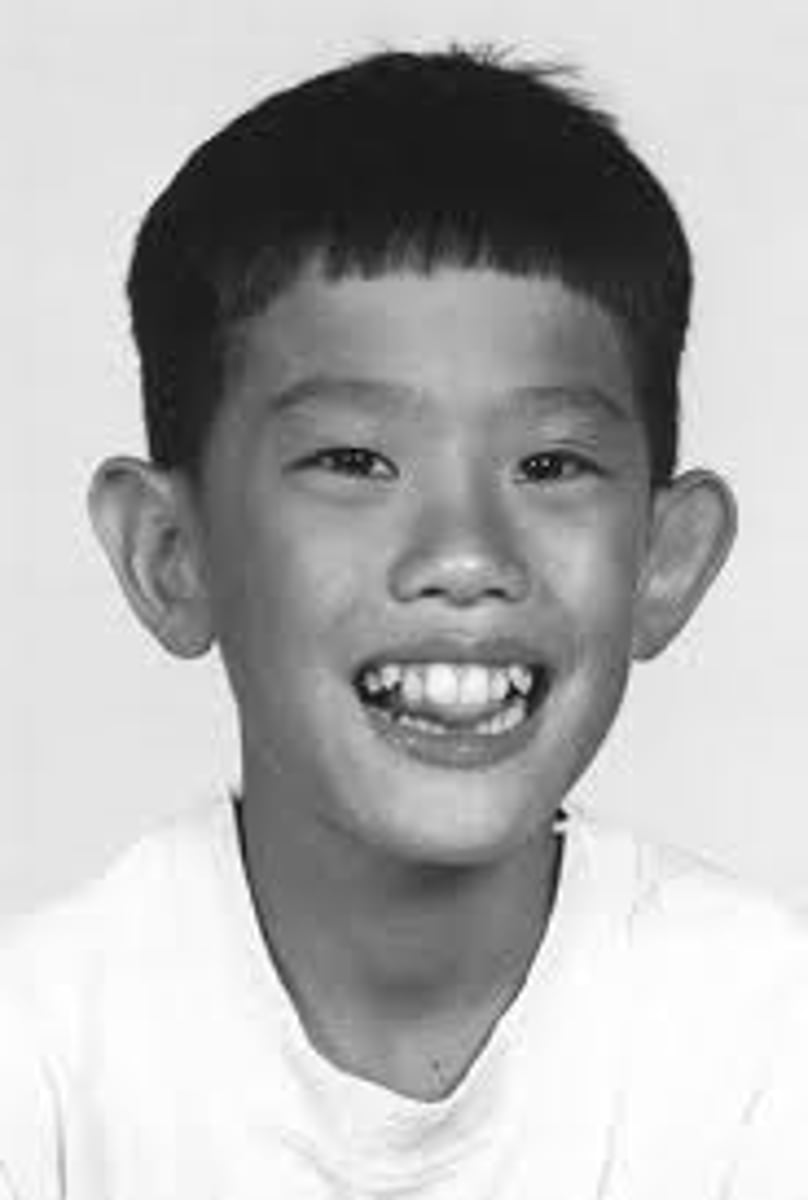
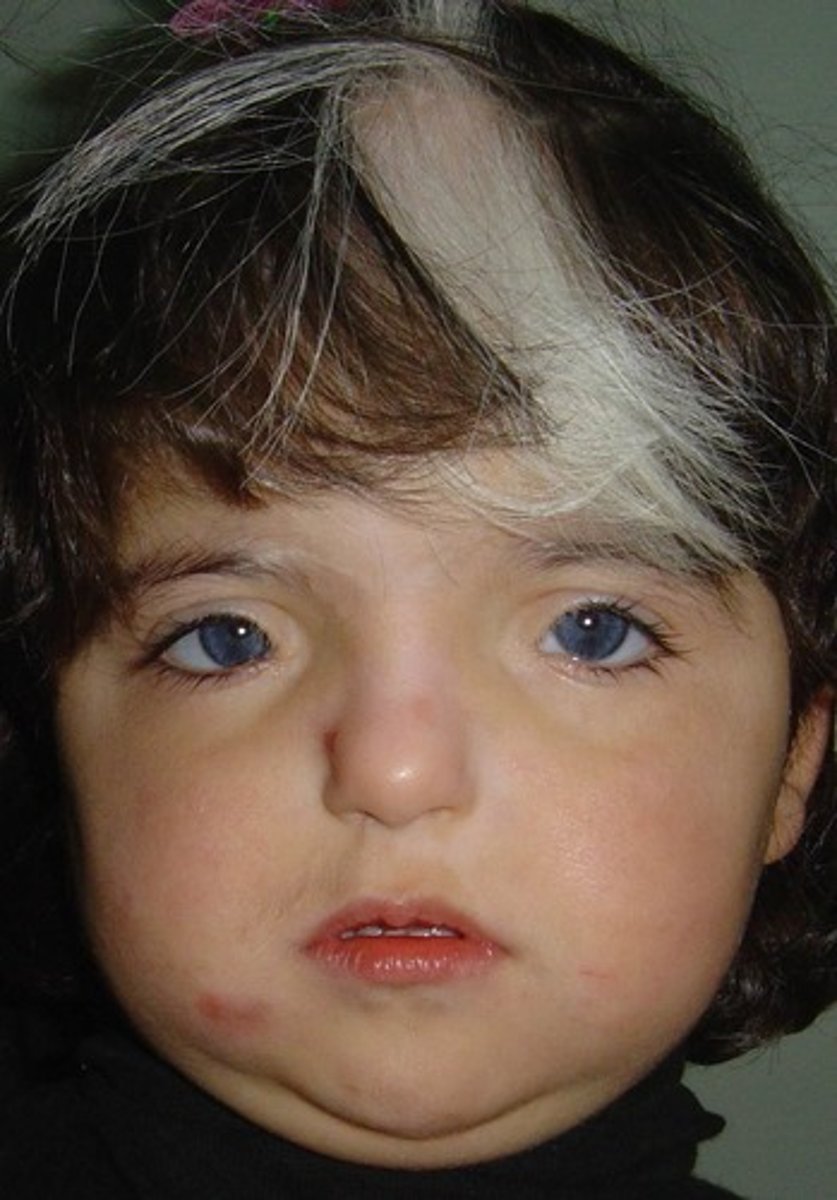
Waardenburg Syndrome
Autosomal dominant, or assoc w/ advanced paternal age. Short palpebral fissures, white forelock and deafness.
Bruton agammaglobulinemia
- x-linked
- infx start @ 6-9mo
- Absence of B cells on flow cytometry
- low levels of all Igs
2 y/o M w/ multiple ear infxns, diarrheal episodes & pneumonias. No tonsils seen on exam.
- Labs?
Combined variable immune deficiency. (acquired)
17 y/o F with decreased levels of IgG, IgM, IgE, and IgA but normal numbers of B cells.
Increased lymphoid tissue--> increased risk for lymphoma
Complication of Combined variable immune deficiency?
Selective IgA deficiency
Most common B-cell defect. Recurrent URIs, diarrhea.
Anaphylaxis reaction if given blood containing IgA
Complication of Selective IgA deficiency?
DiGeorge Syndrome
3wk old M with seizure, truncus arteriosus, micrognathia.
Microdeletion on Chr22
Genetic defect of DiGeorge Syndrome?
Candida
viruses
PCP pneumonia
Types of childhood infections in DiGeorge Sx?
SCID.
See infxns w/ bacterial, viral and opportunistic bugs.
Infant w/ severe infxns, no thymus or tonsils. Severe lymphopenia.
Most common inheritence is XLR. AR is ADA deficiency. Pediatric emergency! Need bone marrow transplant by age 1 or death.
SCID inheritance?
Txt?
Chronic granulomatous disease XLR. PMNs can ingest but not kill catalase + bugs.
3 y/o M child w/ recurrent swollen, infected lymph nodes in groin and staph aureus skin abscesses.
Nitrotetrazolium blue (yellow means they have the dz). New test is Flow cytometry w/ DHR-123
How to dx CGD?
Wisckott-Aldrich Syndrome.
Often present w/ prolonged bleeding after circumcision. Low IgM, high IgA and IgE, slightly low IgG.
18mo M baby w/ severe ezcema, petechiae, and recurrent ear infxns.
Diuresis of extravascular fluid
• Should regain birth weight by? 2wk
• Should double weight by? 6mo
• Should triple weight by? 1yr
Newborns lose 10% of birth weight in 1st week. Why?
Should regain BW by?
Should double weight by?
Should triple weight by?
increases 50% by 1 year
doubles by 5 years
Newborns increase 50% of length by?
Double length by?
Galactosemia, PKU, HIV, HSV on the breast, chemo, Li, Iodide, alcohol.
Contraindications to breastfeeding.
Breast milk is
- whey dominant
- more lactose
- more LCFA
- less Fe but its better absorbed
Nutritional characteristics of Breast milk vs. Formula
Constitutional Growth Delay
Child is likely to have normal final adult height.
14 y/o boy, always been below 5% in height. Parents are tall & were "late bloomers".
Bone age < Real age.
Familial Short Stature
14 y/o boy, always been below 5% in height. Father is 5'2" and mom is 4'10"
Bone age = Real age.
Obesity
Bone age > Real age.
14 y/o boy, 50% in height, 97% for weight.
Obesity
Precocious puberty
CAH
Hyperthyroidism
Bone age > Real age.
Pathologic Short Stature
Craniopharyngioma (vision problems, chect CT)
Hypothyroidism (check TFTs)
Hypopituitarism (check IgF1)
Turners (check karyotype).
14 y/o boy, starts out in 50% for height, in the past 2 years is now between the 5%-10%.
Other risks to consider?
Moro Reflex
From birth - 4/6mo
Primitive Reflex: When head is extended, arms and legs both flex.