121 Sensorimotor
1/40
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
41 Terms
Character
Description of the sign/symptom. How it looks, feels, sounds, smells
Onset
Where did it start
Location
Where it occurs, and/or radiates to
Duration
Length of time it lasts and if it recurs
Severity
How bad it is
Pattern
What improves or or makes it worse
Associated factors
Other symptoms occurring or aggravating factors
Symptoms of neurologic problems
Numbness, tingling, memory loss tremors, pain/headaches, seizures, comprehension, coordination, incontinence
Symptoms of head and neck problems
Difficulty moving, dizziness, lightheaded, loss of consciousness, spinning sensation
Head and neck treatment
Muscle relaxants, anticonvulsants, analgesics, vertebral, laminectomy, hematoma evacuation, physical therapy
Lifestyle leading to head, neck, neurological problems
Poor diet, peripheral neuropathy, smoking, improper body mechanics, repetitive motions
Symptoms of eye problems
Recent vision changes, spots, floaters, blind spots, halos, rings, night blindness, diplopia, pain, redness, swelling, discharge
Symptoms of ear problems
Sudden hearing changes, presbycussis, ear drainage, ear pain, tinnitus, vertigo
Lifestyle causing health and ear problems
Environmental, exposures: sun, loud noise, water
Current symptoms of musculoskeletal problems
Difficulty chewing, pain, altered mobility
Lifestyle affecting musculoskeletal problems
Medications, substance use, high amounts of purine, misuse of assisted devices, poor posture, can cause isolation if chronic
Objective head and neck neurological data
Inspect and palpate, LOC, cognition, mini mental exam tests, thought process, facial expressions, speech, mood, perceptions, mobility
LOC assessment
Always start with least noxious stimuli (verbal, tactile, painful)
Alert
Eyes opened, oriented x3, needs no further stimulation to stay awake
Lethargic
Opens eyes, answers questions, returns to sleep
Obtunded
Opens eyes to loud voice, respond slow w confusion, unaware of environment
Stupor
Awakens to vigorous shake or painful stimuli, returns to unresponsive sleep
Comatose
unresponsive to all stimuli, eyes remain closed
Glasgow coma scale
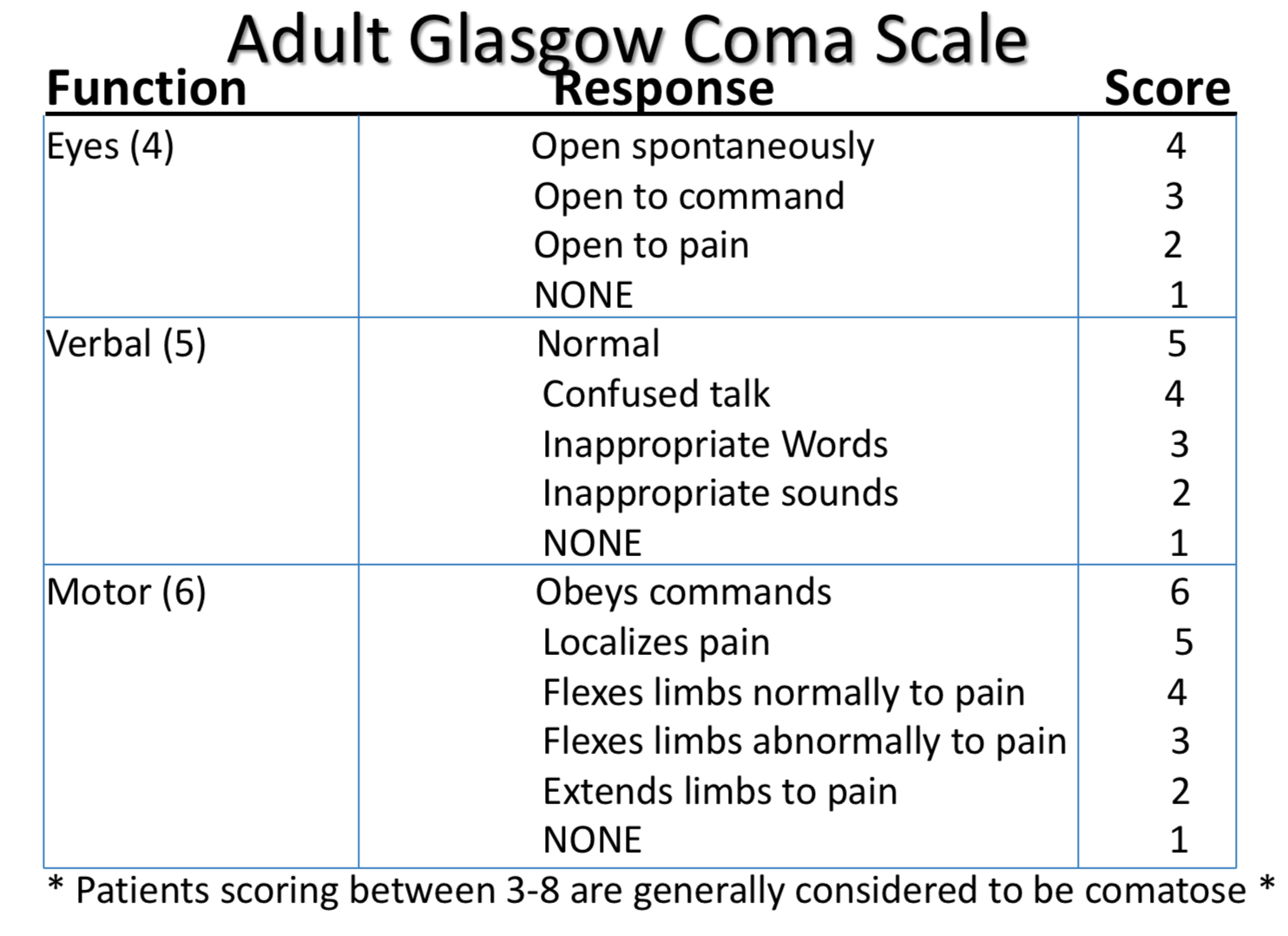
Objective neurological cranial and spinal nerves, inspect and palpate
12 cranial nerves, motor, sensory, cranial nerves can be motor, sensory, or both, mobility and balance, coordination, tactile, positions, reflexes
I olfactory
Function: smell, test: smell with eyes closed
II Optic
Function: visual acuity and field test: snellan chart, peripheral vision
III Oculomotor
Function: pupil reaction, test: pen light, perrla
IV Trochlear
Function: eye movement, test: following finger without moving head
V Trigeminal
Function: facial sensation, test:
VI abducens
Function: motor function, test: lateral eye function
VII Facial
Function: facial expressions, test: smile, wrinkle face, puff cheeks
VIII Acoustic
Function: hearing, balance, test: snap fingers, rhombergs test
IX Glossopharyngeal
Function: swallowing, voice, test: swallow, say “ahh”
X Vagus
Function: gag reflex, test: use tongue depressor
XI Spinal Accessory
Function: neck motion, test: shoulder shrugging
XII Hypoglossal
Function: tongue movement and strength, test: stick out tongue and apply resistance with tongue deep
Eye inspection
1. Assess eyelids and lashes for presence, width, redness, swelling, lesions, and discharge.
2. Note eyelid position relative to the eye.
3. Inspect conjunctiva and sclera with the client looking side to side, then up and down.
4. Conjunctiva: Should be clear, smooth, and moist (older adults may have yellow nodules).
5. Sclera: Should be white (may appear yellow in dark-skinned clients).
6. Assess palpebral conjunctiva by lowering it with thumbs; it should be clear.
Important to remember - ROM
Compare findings bilaterally, dominant side will be stronger, stop for pain, write the strength, do not force the body part beyond normal range
Tremors can be related to a
Neurological disorder
Enlarged head and facial bones can
Indicate presence of disease