Bugs and Drugs of Importance
1/41
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
42 Terms
Classification of clinically important bacteria: Gram-positive cocci (STAPHS AND STREPS )
Staphylococcus aureus two types: MSSA (meticillin susceptible) and MRSA (meticillin resistant)
-Streptococcus pyogenes (sore throat causing)
-Streptococcus Pneumoniae (cause of pneumonia)
-Strep. epidermis (contaminant)
-Enterococci (in the gut)(class of bacteria)
Classification of clinically important bacteria :Gram-negative cocci
-Neisseria two types: Neisseria gonorrhoeae and N. meningitidis
-Moraxella (class of bacteria)
Classification of clinically important bacteria: Gram-positive rods
-Listeria (in soft cheeses) (class of bacteria)
-Corynebacteria (class of bacteria)
-Bacillus cereus
Clostridioides Difficile
-Clostridiodies botulinum
-Clostridium tetani
-Clostridium perfringens
Classification of clinically important bacteria: Gram-negative rods (everything else)
E.coli
H.pylori
P.aeruginosa
Klebsiella pneumoniae
Proteus mirabilis
Salmonella
How do we tell the difference between gram positive and negative in vitro?
gram staining
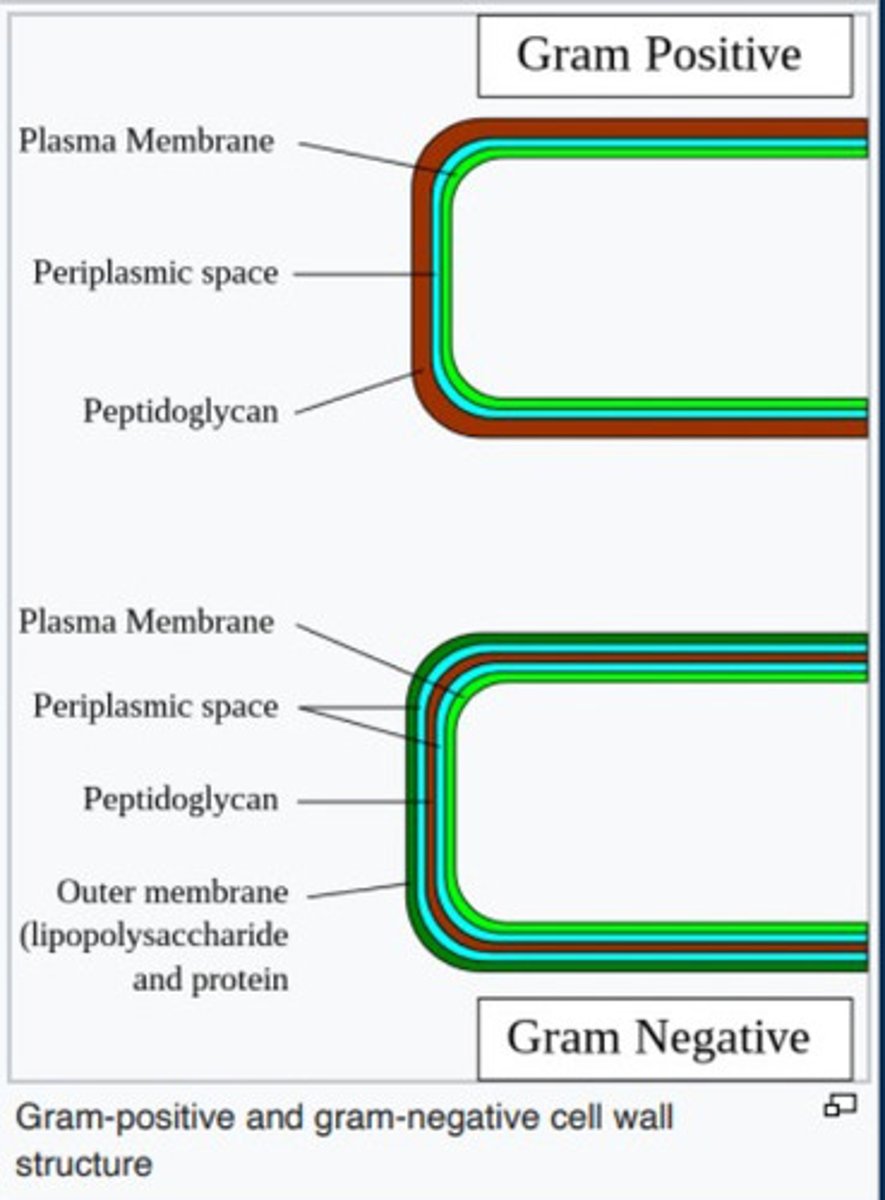
Why do gram negative not hold on to the stain
gram negative have the outer cell wall
Gram negative cell wall structure
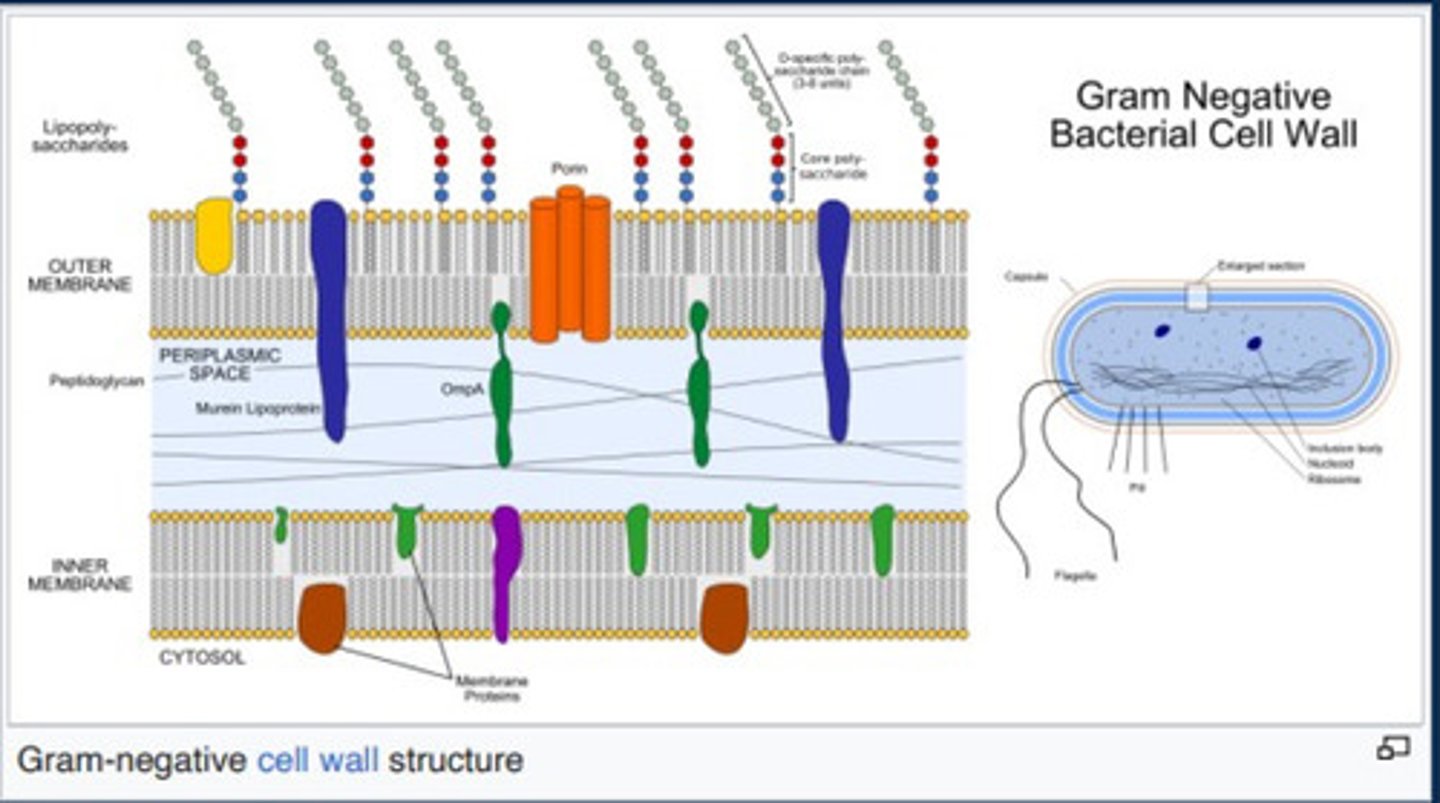
Why are gram negatives harder to treat
-Lipopolysaccharide chains on outside
-Outer and inner membrane = hard for antibiotics to penetrate
Whats the difference between aerobic vs anaerobic gram negative bacteria?
Aerobic:
-Require oxygen for growth (Obligate aerobes) OR can survive with & without oxygen (Facultative anaerobes)
-Use oxidative phosphorylation (aerobic respiration)
Anaerobic:
-Grow in low/no oxygen environments (Obligate anaerobes)
-Use fermentation or anaerobic respiration
what is the difference between rapid and fastidious aerobic gram negative bacteria?
-rapid grow quickly and easily - some of these ferment sugars
-Fastidious grow slower in special enriched conditions e.g. haemophilus
give an example of a non-fermenting gram-negative rapid bacteria?
Pseudomonas aeurinosa - hard to treat due to resistance mechanisms being developed
what are Pseudomonas' ( non-fermenting gram-negative rapid bacteria) resistance mechanisms?
-Produce enzymes that can activate beta lactams
-efflux pumps to pump drugs out
-Drug modifying enzymes within its cytoplasm
-often multi-drug resistant
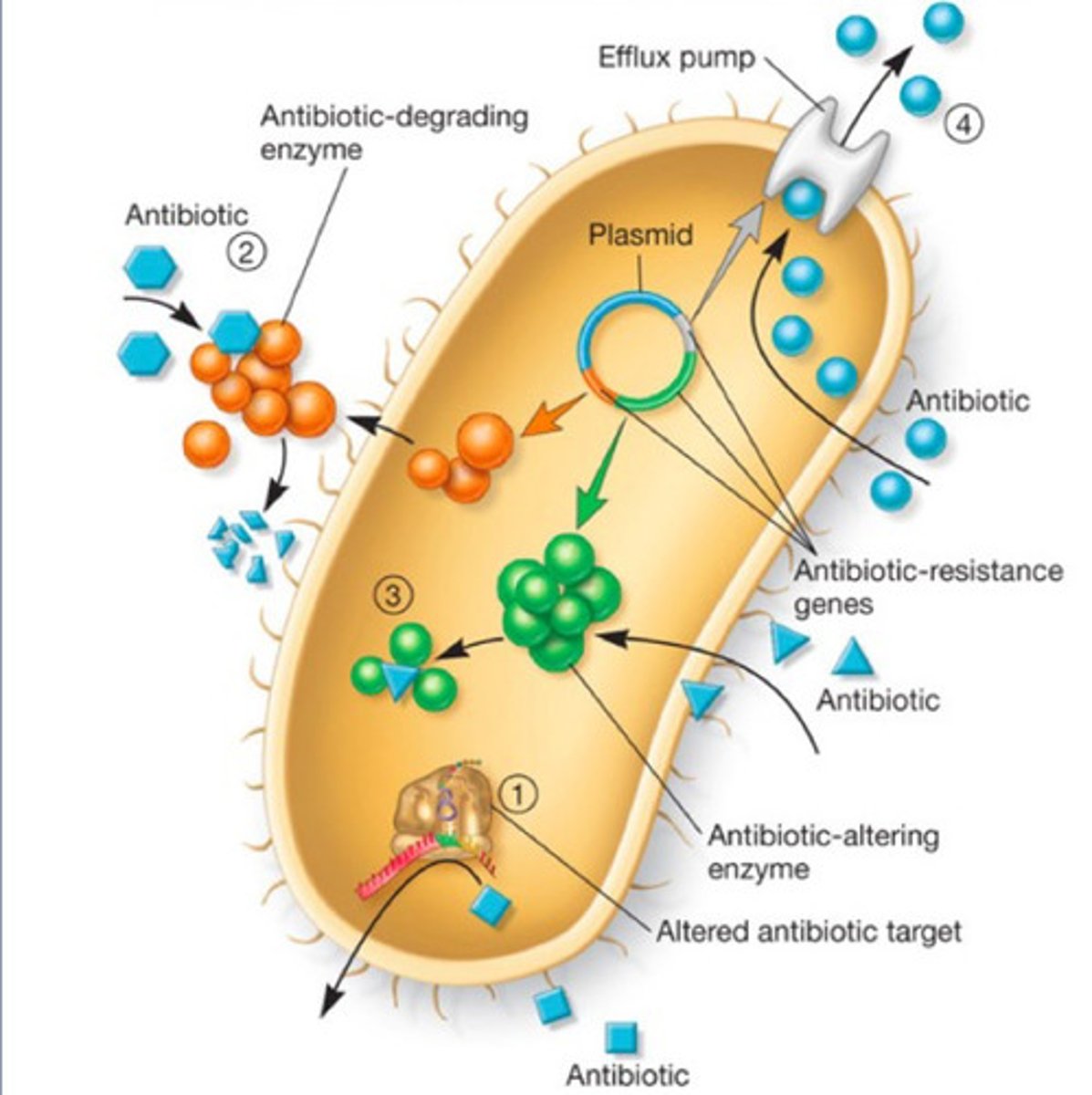
give an example of a fermenting gram negative rapid bacteria?
Enterobacteriaceae
What is the difference between colonisation, infection and contamination
-Colonisation: organism is part of our microbiome
-Contamination: microorganism present thats not supposed to be there
-Infection: microorganism is causing a clinical problem signs and symptoms
Give examples for non-fermenting gram negative rods?
-Haemophilus influenzae (food poisoning)
-Helicobacter pylori (gastric ulcers and cancer)
Other bacteria
M. tuberculosis
C. pneumoniae
M. pneumoniae
Classification of clinically important antibacterials: Beta-lactams
1) Penicillins e.g. amoxicillin
2) Cephalosporins e.g. cefalexin
3) Carbapenems d.g. meropenem
note: cause hypersensitivity reactions and don't work against MRSA
What are the main examples of penicillin to be aware of ?
not that important but good for your own info
Natural penicillins:
Benzylpenicillin
Phenoxymethylpenicillin
Aminopenicillins:
Amoxicillin
Ampicillin
Anti-staphylococcal penicillin's
flucloxacillin
Penicillins with beta-lactamase inhibitors:
Co-amoxiclav, piperacillin & tazobactam
Antipseudomonal penicillin :
Piperacillin
Penicillin / beta-lactamase inhibitor combinations (BLIs):
-Amoxicillin with clavulanic acid (co-amoxiclav)
• Piperacillin with tazobactam
Classification of clinically important antibacterials: Tetracyclines
Doxicycline
MOA: Bind to 30S subunit of bacterial ribosome, preventing protein chain elongation
example of clinically important antibacterials: aminoglycosides
-Gentamycin'
MOA: Bind to 30S bacterial ribosomal subunit - leads to incorrect protein formation & interruption of protein synthesis
example of clinically important antibacterials: Macrolides
-Clarithromycin
MOA: Bind to 50S ribosomal subunit - stops protein chain elongation
example of clinically important antibacterials: Fluoroquinolones
Ciprofloxacin
levofloxacin
Active against pseudomonas (one of the only ones)
MOA: Inhibit DNA gyrase enzyme involved in supercoiling of bacterial DNA – leads to bacterial cell death
Has many adverse effects (MHRA warning) e.g. cardiovascular - prolong QTc interval, Neurological – dizziness, confusion, hallucinations
example of clinically important antibacterials: Glycopeptides
Vancomycin
MOA: bind to terminal D-ala-D-ala chains on peptidoglycan in cell wall, preventing further elongation
example of clinically important antibacterials: Sulphonamides and related
Co-trimoxazole: sulfamethoxazole and trimethoprim
MOA:
Inhibit sequential steps in folate biosynthesis pathway - leads to inhibition of DNA synthesis
What are the different type of antibacterials modes of action?

What drugs are active vs MRSA?
• Vancomycin
• Teicoplanin
• Linezolid
• Co-trimoxazole
• Clindamycin
• Daptomycin
• Ceftaroline
• Tigecycline
• Delafloxacin
• Dalbavancin / oritavancin
What drugs are active vs Pseudomonas aeruginosa?
• Piperacillin & tazobactam
• Ceftazidime (& BLI - avibactam)
• Cefepime
• Ceftolozane & tazobactam
• Cefiderocol
• Meropenem (& BLI - vaborbactam)
• Imipenem & cilastatin (& BLI - relebactam)
• Aztreonam
• Gentamicin
• Amikacin
• Tobramycin
• Ciprofloxacin
• Levofloxacin
• Colistin
Can all antibacterials increase the risk of Clostridioides difficile infection (CDI)
yes
Which antibiotic classes are well-recognized for increasing CDI risk?
Fluoroquinolones
Clindamycin
Cephalosporins
Beta-lactam/beta-lactamase inhibitor combinations (e.g., co-amoxiclav, piperacillin & tazobactam)
Carbapenems
What is the 1st-line treatment for the first episode of CDI?
Oral vancomycin (IV vancomycin is not effective)
What is the 2nd-line treatment for a first episode of CDI if vancomycin is ineffective?
Fidaxomicin.
What is the 1st-line treatment for CDI relapse (within 12 weeks of the previous episode)?
Fidaxomicin
What are the treatment options for recurrent CDI after 12 weeks?
Vancomycin or fidaxomicin
When is metronidazole used in CDI treatment?
Only in combination with vancomycin for life-threatening CDI (given IV).
What does time-dependent killing mean?
The effectiveness of an antibiotic depends on the time its concentration stays above the Minimum Inhibitory Concentration (MIC).
Which antibiotic classes exhibit time-dependent killing?
Penicillins
Cephalosporins
Carbapenems
Monobactams
What does concentration-dependent killing mean?
The effectiveness of an antibiotic depends on its peak concentration (Cmax) relative to the MIC—higher doses lead to stronger killing effects.
Which antibiotics exhibit concentration-dependent killing?
Aminoglycosides
Fluoroquinolones
Metronidazole
What does exposure-dependent killing mean?
The effectiveness of an antibiotic depends on the total drug exposure over time (measured as Area Under the Curve (AUC) relative to MIC)
Which antibiotics exhibit exposure-dependent killing
Glycopeptides (e.g., vancomycin)
Macrolides (e.g., azithromycin, erythromycin)
Tetracyclines
Linezolid
Give examples of antibiotics with good bioavailability
• Amoxicillin • Cefalexin/Cefadroxil • Doxycycline • Fluoroquinolones • Co-trimoxazole • Trimethoprim • Clindamycin • Linezolid • Metronidazole
Give examples of antibiotics not abosrbed orally
• Benzylpenicillin • Piperacillin • Ceftriaxone/Cefotaxime/Ceftazidime • Meropenem/Ertapenem/Imipenem • Aztreonam • Aminoglycosides • Vancomycin/Teicoplanin • Daptomycin • Fidaxomicin