CPB Hardware
1/80
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
81 Terms
What is the effect of non-pulsatile flow?
Initiates intrinsic coagulation pathway through activation of factor XII (12)
What activates fibrinolytic system?
Kallikrein
What is the function of bradykinin?
Increased capillary permeability and development of tissue edema
What system does CPB activate?
Complement system which activates recruitment of leukocytes
What does the release of cytokines cause?
Myocardial dysfunction
What is ischemia reperfusion?
Tissue damage caused when blood supply returns after a period of ischemia, worsening the injury
What causes platelet dysfunctions in CPB?
Hypothermia
Hemodilution
Cardiotomy suction
Platelet aggregate formation
Formation of platelet leukocyte complexes
Platelet adhesion to artificial surfaces
What are the various emboly produced during CPB?
Fibrin
Platelet aggregates
Neutrophilic RBC debris
Gaseous
Spallated materials
How does optimal cardiac output decrease systemic inflammatory response to CPB?
Clears inflammatory mediators
What is the function of aprotinin-serine protease inhibitor?
Decrease systemic inflammatory response to CPB
WHat is the function of modified ultrafiltraion?
Decreases tissue edema and circulating inflammatory properties
What factors can help decrease systemic inflammatory response to CPB?
Leukocyte depletion filters
Pulsatile perfusion
Coating of membranes and tubings with heparin
What is the function of venous cannulation?
Allows deoxygenated blood to be drained from the patient into the extracorporeal circuit
What type of cannulation is typically used for a CABG?
Two-stage venous cannula because it does not involve opening the chambers of the heart
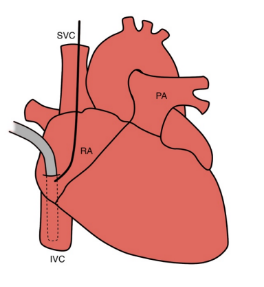
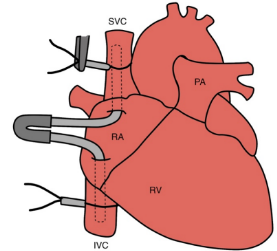
What is bicaval cannulation?
Two single-stage cannulae sit in the inferior and superior vena cavae and are connected using a Y-connected to the venous line
What can also be used as a cannulation site for more complex sugrery?
Femoral veins
What cannulation is used for femoral veins?
An elongated single-stage cannula passed up the femoral vein into the vena cava
How do they select the size of a venous cannula?
To allow one third of total flow drain through SVC cannula and two third of total flow drain through IVC
What is a double stage venous cannula?
IT has a wider portion with holes in the section designed to sit in the RA and a narrower tip designed to rest in the IVC
What can the tips of cannulas be made of?
Plastic or metal
What is the point of the internal diameter to outer diameter ratio?
It is used to determine flow efficiency, ratios below 1 indicates potential flow restriction
What do venous cannulas look like?
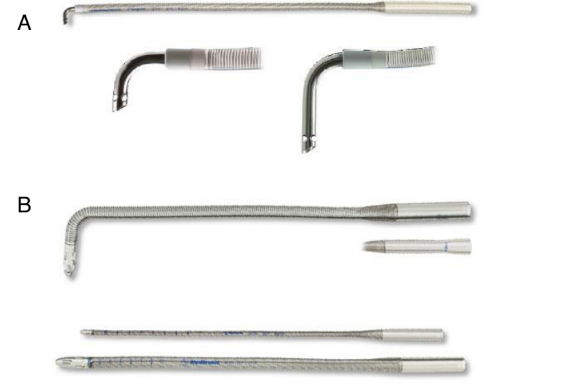
What is cavoatrial venous cannulation with two-stage canula typically used in?
Aortic valve procedures
Coronary bypass procedures
AVR+CABG procedures
Bentall procedure
What is the disadvantage of two stage venous cannula?
It rewarms the heart which causes less myocardial protection
What is venous drainage accompanied by?
Gravity siphonage
Where should the venous reservoir be?
Below the level of the patient
What are the determinants of venous drainage?
Height of the patient above venous reservoir
Patient’s blood volume
Resistance of tubing
Cannula dimensions
What are causes of low venous return?
Reduced venous pressure
Inadequate height of patient above venous reservoir
Malposition of venous cannula
Obstruction or excess resistance of lines and cannula
Kink/air lock
How to achieve augmented venous return?
Placing a roller pump in venous line
Centrifugal pump in venous line
Vacuum assisted venous drainage
How do you achieve adequate venous drainage?
Speeds of 1000-2000 RPM of kinetic pump or application of 20 mmHg vacuum to venous
What are potential problems of augmented venous returnt?
Hemolysis
Collapse of right atrium resulting in impaired venous drainage and chattering of venous line
Micro air aspiration
Where can peripheral cannulation be done?
Femoral veins
Iliac veins
Less common used sites, innominate vein and axillary vein
What are indications of peripheral cannulation?
Emergency closed cardiopulmonary assist
Support of ill patients before induction of anesthesia
Before sternotomy for reoperations
Minimal access surgery
Certain aortic and thoracic surgery
What is arterial cannulation?
Delivers oxygenated blood from the heart-lung machine directly into the patient’s arterial system
How do they determine the size of the arterial cannula?
The size of the vessel that is being cannulated and blood flow required
What is the most common site of arterial cannulation?
Ascending aorta
How are arterial cannulas sized?
Internal diameter
What are the advantages of metal tipped cannula?
Provides best internal diameter to outer diameter ratio
Easy to cannulate
What are the advantages of metal tipped cannula?
Jet effect → Hemolysis
No side holes to reduce sandblast effect
Traumatic → may damage posterior intima
What is the jet effect?
hemolysis caused by high-velocity jets of blood flowing through narrow openings, often after cardiac repairs
What type of arterial cannulas provide the best flow?
Thin-walled wire-wound cannulas and are very resistant to kinking
What is the ideal flow with aortic cannulation?
<100 mmHg pressure gradient
What happens if pressure gradient is >100 mmHg with aortic cannulation?
Hemolysis and protein denaturation
When should you suspect aortic dissection?
Increased CPB systemic line pressure
Sudden decrease in both venous return or arterial pressure
Decreased organ perfusion
Blue discoloration of aortic root
Bleeding from cannulation site
How do you manage aortic dissection?
Prompt cessation of CPB
Re-cannulation distal to dissection
Induction of deep hypothermia and a period of circulatory arrest while aorta is opened and repiared
What does sandblasting effect cause?
Perioperative stroke, aortic dissection, and postoperative renal dysfunction
What is epiaortic ultrasonic scanning?
Used to detect atherosclerotic plaque in the ascending aorta
What should mean pressure be during arterial cannulation?
70-80 mmHg
What are indications for femoral cannulation?
Aneurysm of ascending aorta or diffuse atherosclerosis of ascending aorta
In unstable patients before induction
Reoperations
When antegrade dissection complicates aortic cannulation
Minimally invasive cardiac surgery
How do you determine length of tubing?
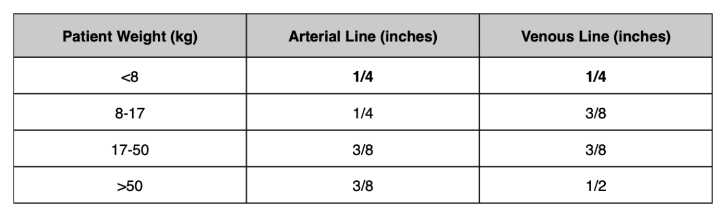
What is biomaterial tubing?
Binding heparin or other surface modifying agents into inner surface of the tubing may improve biocompatibility
What coats biomembrane mimicry?
Derivative of phosphorylcholine (memys,sorin)
What are the different heparin coated circuits?
Heprain bound to tubing is slowly released into circulation
Heparin is permanently bound covalently to biomaterial surface
Hybrid surface-combination of heparin releasing and heparin immobilized
What are surface modified additives for tubing?
Poly 2-methoxy-ethylacrylate which has hydrophobic properties and little tendency to react with blood products
What is the primary form of heat transfer?
Forced convection
When should you do cardiac venting?
Whenever the left ventricle is unable to handle the amount of blood that is returning to it
What is the purpose of cardiac venting?
Aid visualization and provide bloodless field
Avoid chamber distension
Reduce myocardial rewarming
Prevent cardiac ejection of air
What is cardiac venting?
A surgical technique used to remove blood and air from the heart chambers
What are potential sites of cardiac venting?
Pulmonary artery
Right superior pulmonary vein
Left atria
Left ventricle
Aortic root cardioplegia cannula
How do you monitor LV disension?
PA Catheter (measures real time cardiovascular pressures and oxygen saturation)
Left atrial monitoring line
Transesophageal echocardiogram
How do you prevent air embolism during cardiac venting?
Heart is allowed to fill before vent insertion
What is the function of arterial filters?
Remove air and particulate matter
What are limitations of arterial filters?
Relatively large volume required to prime the filters
Hemolysis, platelet loss, complement activation
Lack of proven benefit
Paradoxical risk of increased particulate embolism
What is the function of leukocyte depletion filters?
Non-woven polyester fibers that have been surface modified to remove leukocytes
Which immune cells are an important contributor to ischemia reperfusion injury?
Neutrophils
What is left heart bypass?
Blood is removed from the left heart and placed into left atrium and the lungs provide gas exchange
(no oxygenator)
What is the risk of left heart bypass?
Air embolism
When do you use left heart bypass?
Descending thoracic or large thoracoabdominal aortic aneurysms
What does left heart bypass consist of?
Tubing and centrifugal pump (no reservir, heat exchanger, or bubble)
What are minimal extracorporeal circuits composed of?
Single centrifugal pump
Membrane oxygenator
Surface modification
What is the priming volume for a minimal extracorporeal circuit?
500 mL
What are minimal extracorporeal circuits used for?
CABG, aortic, and mitral valve surgeries
What are the limitations of minimal extracorporeal circtuis?
Air embolization
Unable to handle excess venous return
Lack of heat exchanger
Need to use separate cell processing system
Increased cost
What is dialysis?
Blood is separated from crystalloid solution or dialysate by a semipermeable membrane
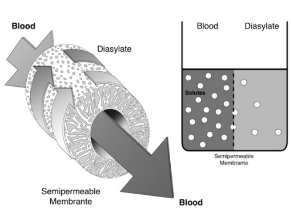
What is ultrafiltration?
Movement of water across a membrane due to transmembrane pressure gradient
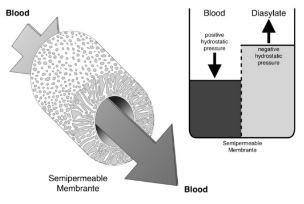
What is the function of ultrafiltration?
Removes excess fluid and results in increased hematocrit, decreased lung waters, and decreased tissue edema
What are the advantages of ultrafiltration?
Conserve platelets and coagulation factors → improve perioperative hemostasis
Conserve albumin → Reduce lung water and post operative ventilator support
What is conventional ultrafiltration?
Practice of withdrawing blood from the patient through venous reservoir during rewarming period and passing it through a hemoconcentrator and pumping it back into the patient through venous reservoir
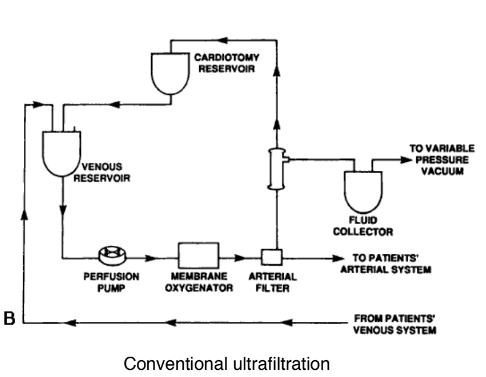
What is zero balanced ultrafiltration?
Volume of plasma water removed is replaced by a balanced electrolyte solution to remove inflammatory mediators
What is modified ultrafiltration?
Withdrawing blood from the patient through aortic cannula and passing it through hemoconcentrator and it goes back into the patient through venous cannula
What are the comparisons of the ultrafiltration methods?