FF - pediatrics
1/42
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
What are the APGAR categories?
appearance (color)
pulse
grimace (reflex irritability)
activity (mm tone)
respiration
What is the scoring for each APGAR category?
A: 0=blue, 1=blue extremities, 2=no blue
P: 0=absent, 1=<100 bpm, 2=100-140 bpm
G: 0=no response, 1=grimace, 2=cry or withdrawal
A: 0=flaccid, 1=some flexion, 2=active motion of extremities (kicking)
R: 0=absent, 1=weak cry, 2=strong cry
What is the normal range for APGAR?
8-10
How often is APGAR assessed?
at 1 min, 5 min, 10 min
What are the typical patterns of gross motor development?
primitive reflexes dominate movement before cortical control
general before localized responses
flexor tone before extensor tone
once antigravity/upright: extensor tone progresses before flexor tone
cephalic to caudal development
proximal to distal development
gross motor before fine motor control
What milestones do you see at month 3?
prone on elbows
can lift head in prone
belly crawl (3-9 months)
supine to sidelying (3-4 months)
What milestones do you see at months 5-6?
prone to supine
pull to sit w/o head lag
sitting w/ UE support
feet to mouth
propped or ring sitting w/ high guard
What milestones do you see at months 6-7?
supine to prone
quadruped
transfer objects b/w hands
trunk rotation in sitting
What milestones do you see at months 9-10?
quadruped creeping
cruises (walking on furniture) to sideways
plantigrade, pulls to stand
upright, unsupported sitting
improving grasping skills, 3 jaw chuck
What milestones do you see at months 10-15?
begins to walk unassisted
transitions in & out of squatting
controls grasp & release
stacks 2 cubes
What is the difference between the terms integrated and persistent?
integrated: primitive reflex disappears to allow for normal development
persistent: primitive reflex not integrated, indicating CNS dysfunction
What is the flexor withdrawal reflex?
When does this reflex become integrated?
painful stimulus to sole of foot → toes ext, foot DF, LE flex uncontrollably
1-2 months
What is the crossed extension reflex?
When does this reflex become integrated?
painful stimulus to ball of foot of extended LE → opposite LE flex, then ADD, then ext
1-2 months
When does the rooting reflex become integrated?
3 months
What is the traction reflex?
When does this reflex become integrated?
grasp forearm and pull up from supine into sitting → grasp & total flex of UE
2-5 months
When does ATNR become integrated?
4-6 months
What is the palmar grasp reflex?
When does this reflex become integrated?
maintained pressure to palm of hand → maintained finger flex (grasp)
4-6 months
What is the moro reflex?
When does this reflex become integrated?
drop pt backward from sitting position → UE ext & ABD, hand opening, crying, followed by UE flex & ADD
5-6 months
What is the STLR reflex?
When does this reflex become integrated?
prone → limb flex
supine → limb ext
6 months
What is the positive supporting reflex?
When does this reflex become integrated?
contact to the ball of the foot in standing position → rigid ext (co-contraction) of the LEs
6 months
What is the plantar grasp reflex?
When does this reflex become integrated?
maintained pressure to ball of foot → maintained toe flex
9 months
What is the STNR reflex?
When does this reflex become integrated?
head flex → UE flex, LE ext
head ext → UE ext, LE flex
8-12 months
What is the startle reflex?
When does this reflex become integrated?
sudden loud noise → sudden UE ext or ABD, crying
persists
Summarize the integration of primitive reflexes
1-2 months: flexor withdrawal, crossed extension
3 months: rooting
2-5 months: traction
6 months: palmar grasp, ATNR, moro, sucking, TLR, positive supporting (PAMS TP)
9 months: plantar grasp
8-12 months: Babinski, STNR
Describe plagiocephaly
results from prolonged asymmetrical pressure on the premature skull → creates parallelogram shape
ipsilateral occipito-parietal flattening, frontal bossing, anterior displacement of the ear
contralateral occipital bossing
How can you treat plagiocephaly & torticollis?
parent education
helmet
tummy time (head ext)
What are the classifications of cerebral palsy (CP)?
Describe each
spastic: high tone, synergy, crouched gait, toe walking
ataxic: low tone, tremor, wide BOS, nystagmus
dyskinetic: fluctuating tone, poor stability, hand tremor, athetosis
What are the levels of the Gross Motor Function Classification System of CP?
level 1: pt will walk w/o restrictions but will have limitations in more advanced gross motor skills
level 2: walk w/o AD but w/ limitations in walking outdoors & in the community
level 3: walk w/ AD and limitations in walking outdoors & in the community
level 4: self mobility will be very limited, children are transported or use power mobility outdoors & in the community
level 5: self mobility will be very limited even w/ AD, requires caregiver
How can you treat a pt w/ CP?
posterior walkers promote upright posture
address tone
standing frames should be used by age 2 to promote therapeutic benefits of standing
AFOs for PFor contractures
tendon lengthening procedures: WBAT & gentle PROM progressing slowly; avoid aggressive & end range & strengthening
What is the Pediatric Evaluation of Disability Index (PEDI)?
functional capability assessment for children 6 months to 7.5 years
3 domains: self care, mobility, social function
normal score = 50 ±10 points
What is the Functional Independence Measure for Children (WeeFIM)?
measures development & disability for children 6 months to 7 years as they go through preschool & elementary school
3 domains: self care, mobility, cognition
scoring: 1=total assistance, 7=IND
Describe Duchenne’s muscular dystrophy (DMD)
X-linked recessive, common in boys
dystrophin gene missing → mm cell destruction
causes pseudo-hypertrophy (collagen & fat replaces mms), commonly in the calves
(+) Gower sign
How can you treat pts w/ DMD?
maintain mobility & preserve strength
maintain joint ROM w/ active & passive
don’t over-fatigue
Describe Down syndrome (Trisomy 21)
results from presence of extra copy of the 21st chromosome
increased risk w/ increased age of the mother
hypotonia, ligamentous laxity
weak quads & hip ABD
How can you treat pts w/ Down syndrome?
encourage motor function
avoid forceful neck flex & rotation activities d/t laxity of odontoid ligament and potential for subluxation of AA joint
avoid hyperextension of elbows & knees during WB activities
Describe Scheuermann’s disease
Schmorl’s nodes & wedged thoracic spine
pain w/ long periods of standing/sitting or physical activity
pain w/ thoracic ext & rotation
increased thoracic kyphosis & lumbar lordosis
How can you treat pts w/ Scheuermann’s disease?
Schroth method
stretch pecs
strengthen thoracic extensors & scapular stabilizers
What nerves are damaged in Erb’s palsy?
What Sx’s do you see with this?
C5-6
loss of shoulder ABD/ER
waiter’s tip deformity
What nerves are damaged in Klumpke’s palsy?
What Sx’s do you see with this?
C8-T1
paralysis of hand intrinsics
claw hand
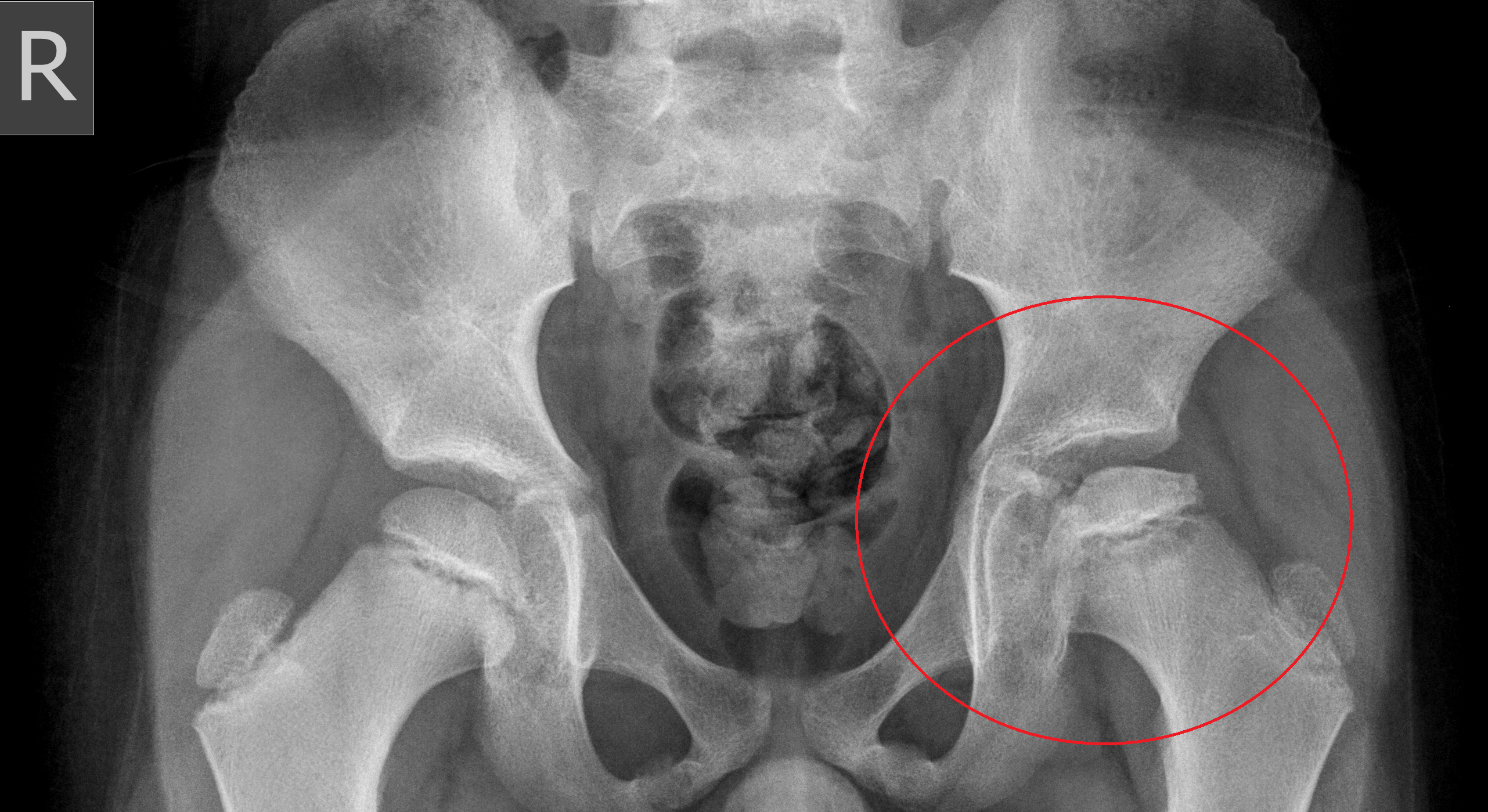
Describe Legg-Calve-Perthes disease
ages 2-13, males
short stature
deformity or flattening of femoral head d/t loss of blood supply → femoral head necrosis, fragments, ossification
pain worsens w/ activity
limping, stiffness
limited hip ext, ABD, IR (EABIR)
conservative Tx, bracing
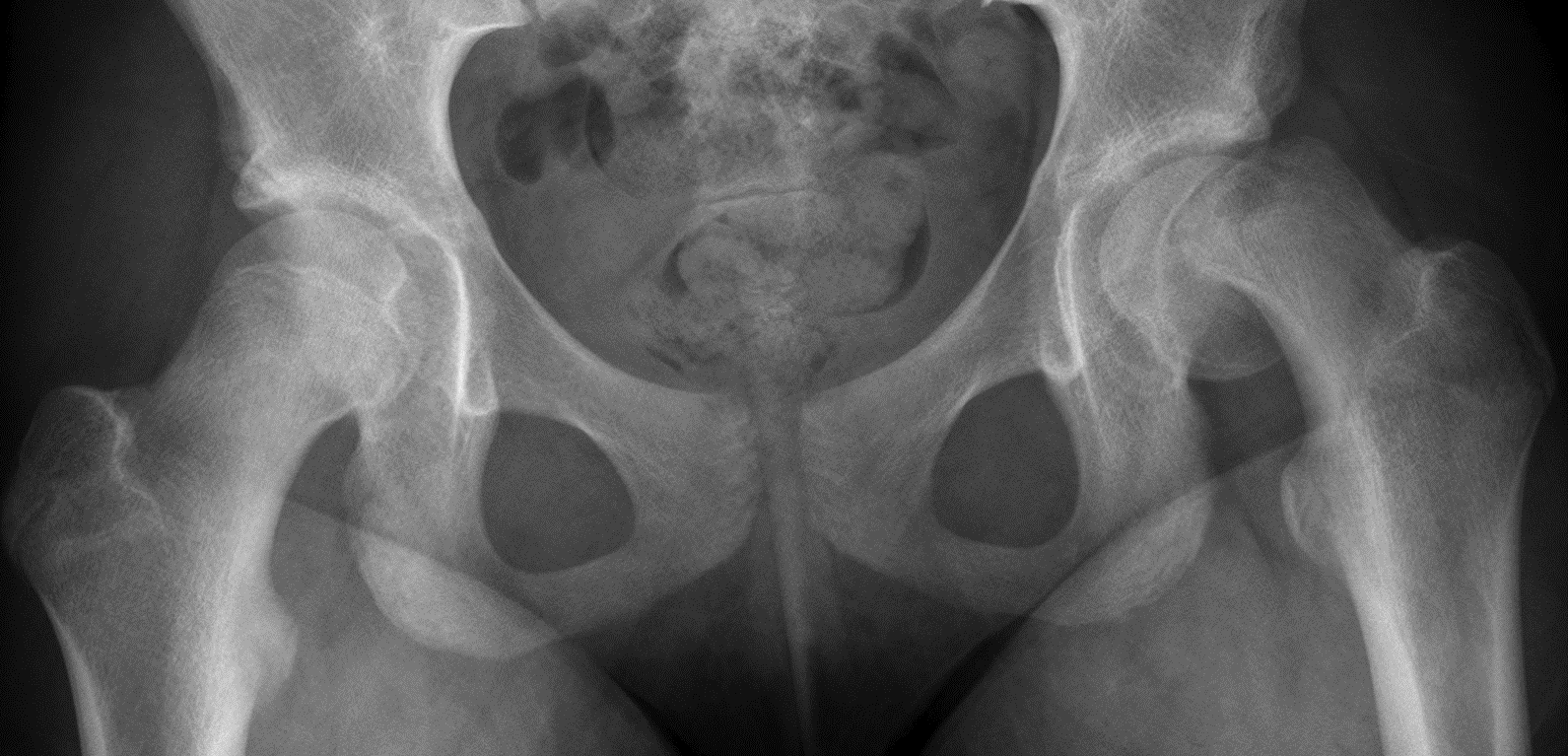
Describe slipped capital femoral epiphysis (SCFE)
ages 10-17
overweight
displacement of femoral head d/t slippage from the growth plate
pain worsens w/ activity
limping, stiffness
limited hip flex, ABD, IR (FABIR)
requires surgery to stabilize hip joint
What hip orthosis is used for Legg-Calve-Perthes disease?
Scottish rite brace
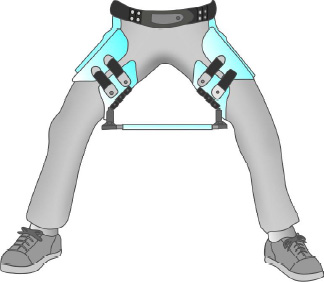
What hip orthoses are used for congenital hip dysplasia?
Pavlik harness
Frejka pillow