Calcium homeostasis disorders
1/13
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
14 Terms
What is hyperparathyroidism?
Excessive secretion of parathyroid hormone (PTH) causing high calcium levels - hypercalcemia
What causes hyperparathyroidism?
typically caused by parathyroid adnoma - a bengign tumour on the parathyroid hormone or can be cause by hyperplasia of gland or carcinoma (rarely)
Secondary cause
compensatory PTH release due to chronic low levels of caclium and vitamin D
chronic kidney disease causes phosphate retention, low calcium and increase PTH
Vitamin D deficiency means calcium not absorbed - increase in PTH
What do we see in terms of blood in hyperparathyroidism?
parathyroid hormone secretion increases causes:
Increased bone reabsorption
increased renal calcium reabsorption
Increased activation of vitamin D
leads to hypercalcaemia
What are the consequences / symptoms of hyperparathyroidism?
bone fractures, bone pain from bone reabsorption - bone cysts or lesions may also occur as a result
lethargy, excessive thirst, anorexia, polyuria, heart block
Hypercalciuria leads to kidney stones
GI - nausea, constipation, peptic ulcers
fatifue and depression
How do we treat hyperparathyroidism?
1st line - surgery - surgical removal of overactive tissue
Cinacalcet - lowers parathyroid hormone if surgery cannot be performed
correct underlying causes of hyperparathyroid hormone e.g.
vitamin D analogues e.g. calcitriol, alfacalcidol
What is hypoparathyroidism?
Hypoparathyroidism is inadequate parathyroid hormone release which causes low calcium levels (hypocalcaemia) and high phosphate levels (hyperphosphatemia)
What causes hyperparathyroidism?
damage to thyroid hormone during surgery
autoimmune conditions
genetic
What do we see in terms of the pathophysiology of hypoparathyroidism?
Low parathyroid hormone results in:
low bone reabsorption → less calcium release
Low renal calcium reabsorption → more calcium excreted
Low activation of vitamin D → Low GI calcium absorption
Result - hypocalcemia, hyperphosphatemia
What symptoms do we see in hypoparathyroidism?
symptoms due to low calcium levels
Hyperexcitability of nerves - pins and needles, muscle spasms, and cramps, seizures and convulsions
chvostek sign - twitching of facial muscles
dental abnormalities
dry scaly skin
brittle hair and nails
cataracts
How do we treat hypoparathyroidism?
vitamin D supplements to enhance Ca2+ reabsorption and utilisation
oral calcium supplements
What is pagets disease?
Excessive osteoclastic activity which increase bone breakdown, followed by disorganised osteoblastic repair - bone is dense but structurally weak leading to enlarged, deformed bones prone to fracture
Commonly affects the skull, pelvis, spine, femur and tibia
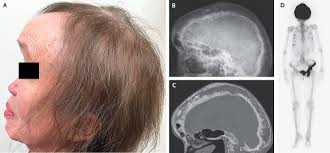
How do we treat pagents disease?
Bisphosphonates e.g. zoledronic acid IV given to reduce osteoclast activity
vitamin D and calcium - support bone health (as patients prone to fractures)
pain management
What is rickets?
Caused by vitamin D deficiency - vitamin D deficiency in children causes rickets but in adults causes osteomalacia
Rickets causes bowed legs due to inadequate vitamin D, meaning hypocalcaemia as calcium requires vitamin D for absorption
How do we treat rickets?
dietary prevention
calcium and vitamin D supplementation
e.g. calcichew D3 tablets
colecalciferol - vitamin d3
Note vitamin D also called calcitriol of cholecalciferol