RADSCI 313 Test 2
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
82 Terms
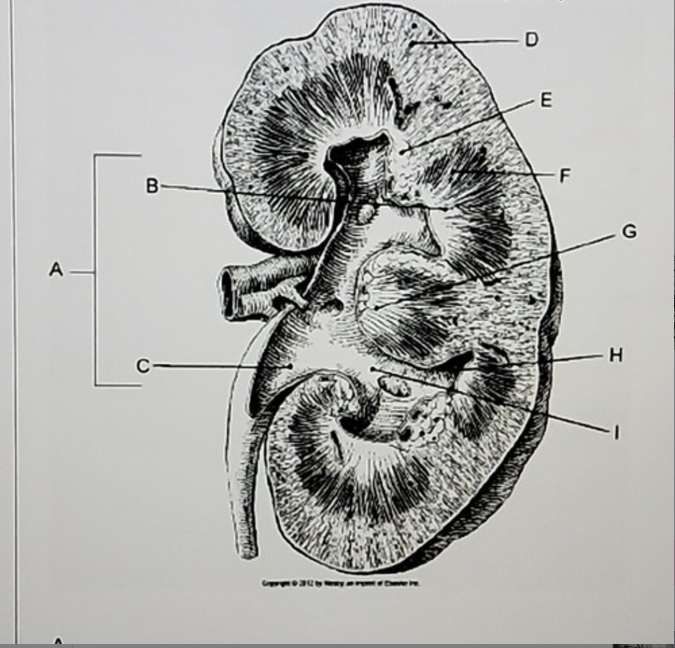
A. Hilum
B.
C. Renal pelvis
D. Renal cortex
E.
F. Renal medulla
G.
H. Minor calyx
I. Major calyx
Identify the structures
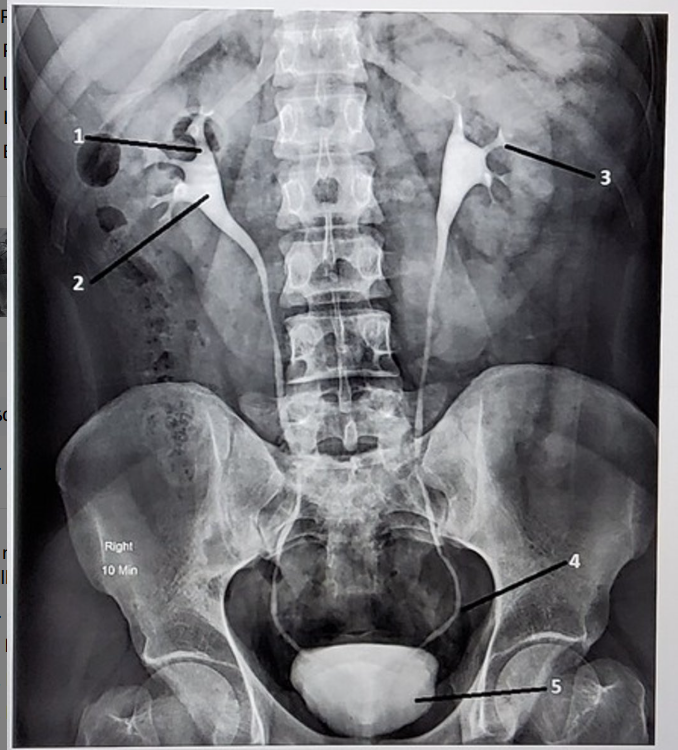
1. Right major calyx
2. Right renal pelvis
3. Left minor calyx
4. Left distal ureter
5. Bladder
Identify the anatomic structures labeled on this image. Your label should be descriptive (proximal/distal, which side of the body, etc)
A
A male patient comes to radiology for a voiding cystourethrogram. Which of the following projections and/or positions would be performed for this procedure?
A. 30° RPO
B. Recumbent lateral
C. Erect lateral
D. Erect PA
B
How do you get the patients salivary ducts to open when conducting a sialogram?
A. Think about food
B. Suck on a lemon wedge
C. IM injection of glucagon
D. Drink a large glass of water
C
One of the three constricted points along each ureter is the pelvic brim. The location of this constricted point is:
A. Where the distal ureters connect to the bladder
B. Where the bladder meets the symphysis pubic
C. Where the iliac blood vessels cross over the ureters
D. at the level of the ischial spines
D
The structural and functional unit of the kidney is:
A. the glomerulus
B. the calyx
C. Bowman capsule
D. the nephron
A
During an endoscopic retrograde cholangiopancreatogram, how does the contrast medium reach the biliary tree?
A. Direct instillation into the common bile duct
B. Orally, by swallowing the contrast
C. Injection into the cystic duct during surgery
D. IV injection
A
Saliva contains certain enzymes to begin the digestion of:
A. starch
B. lipids
C. proteins
D. minerals
1, 2, 3
During an operative cholangiogram, the surgeon injects the contrast medium directly into the biliary system. According to Bontrager's which of the following positions may the patient be placed into during the injection of the contrast media?
1. AP
2. AP oblique, RPO
3. AP oblique, LPO
1, 2, 5
The diaphragm has openings in it to allow certain anatomy to pass from the thoracic cavity into the abdominal cavity. Which of the following are diaphragmatic openings?
1. Esophageal hiatus
2. Aortic aperture
3. Cardiac hiatus
4. Fundal aperture
5. Caval hiatus
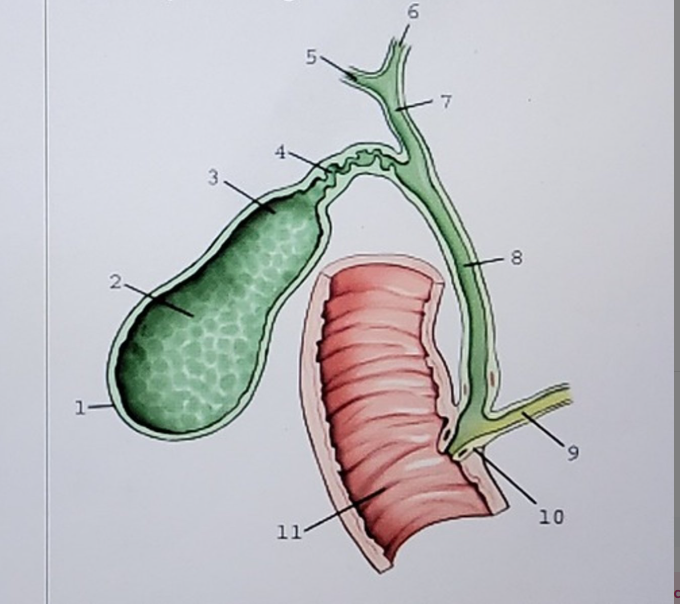
1. Fundus
2.
3.
4. Cystic duct
5.
6.
7.
8.
9.
10. Hepatopancreatic ampulla
11.
Label this picture
D
Which of the following structures is not one of the salivary glands?
A. Sublingual
B. Parotid
C. Submandibular
D. All of these are salivary glands
B
Diaphragm fluoroscopy is performed for which of the following reasons?
A. Investigate the reason for shortness of breath
B. Evaluate the patient for a paralyzed hemidiaphragm
C. Evaluate for abducens nerve palsy
D. It is part of the post-stroke evaluation
C
Radiographic examination of the salivary glands using contrast medium is called:
A. angiography
B. parotitis
C. sialography
D. sialostenosis
B
How is contrast media normally introduced during a retrograde cystogram?
A. With an injection through the urethra with a large syringe and catheter
B. Gravity flow through a catheter
C. Intravenously
D. With a cystoscope
A
What is the total capacity of the average adult bladder?
A. 350 to 500 mL
B. 100 to 250 mL
C. 500 to 750 mL
D. 1000 to 1200 mL
1 and 2
Functions of the kidney include:
1. Removal of waste products from the blood
2. Maintaining fluid and electrolyte balance
3. Recycling of red blood cells
A
Which of the following uses a fiber optic scope to diagnose and treat hepatobilliary disorders?
A. endoscopic retrograde cholangiopancreatiography (ERCP)
B. Percutaneous transhepatic cholangiography (PTC)
C. T-tube cholangriography
D. Operative cholangiography
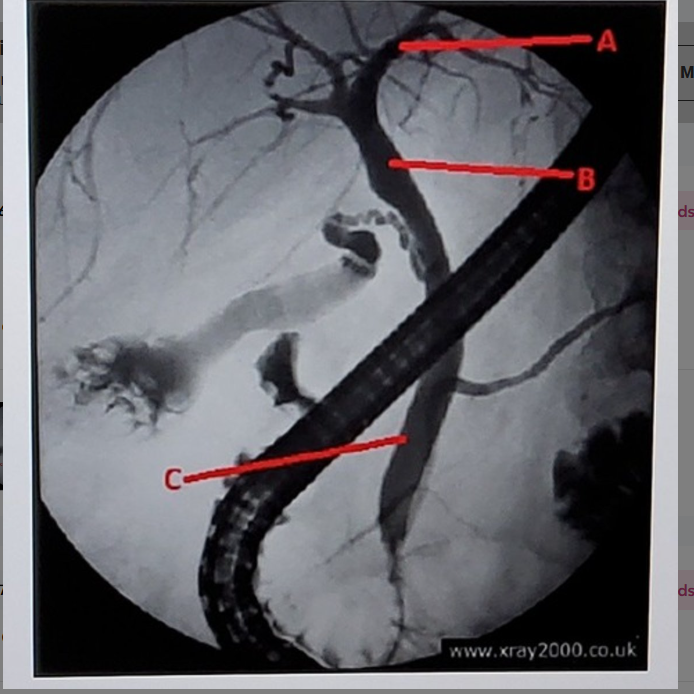
common bile duct
what is letter C
D
Radiographic examination of just the biliary ducts is termed:
A. Cholelithiasis
B. Cholecystography
C. Cholecystocholangiography
D. Cholangiography
D
The main function of bile is to:
A. break down cholesterol
B. begin the digestion of complex sugars
C. begin the digestion of proteins
D. emulsify fats
C
What is the primary function of cholecystokinin?
A. stimulates the production of bile
B. inhibits the formation of gallstones
C. stimulates the gallbladder to contract
D. serves as an enzyme to break down certain food nutrients
3, 4 and 5
As a member of the team performing a bronchoscopy, what is your roles as the radiologic technologist?
1. assist the pulmonologist by capturing and preserving tissue samples
2. monitor the patients vital signs
3. utilize the c-arm as directed by the pulmonologist, centering over the bronchoscope tip
4. ensure the entire team is wearing appropriate radiation protection apparel
5. perform a post-procedure mobile CXR if ordered
1 only
What type of contrast media is used for imaging the urinary and hepatobiliary systems?
1. water soluble nonionic contrast media
2. barium sulfate
3. oral, water soluble iodinated contrast media
4. oil-based iodinated contrast media
A
Which of these examinations is usually performed by a physician in an operating room?
A. retrograde urography
B. voiding cystourethrogram
C. IVU
D. Cystography
D
"chole-" is a prefix for terms pertaining to the:
A. Liver
B. ducts
C. gallbladder
D. bile
parotoid gland
what is letter E
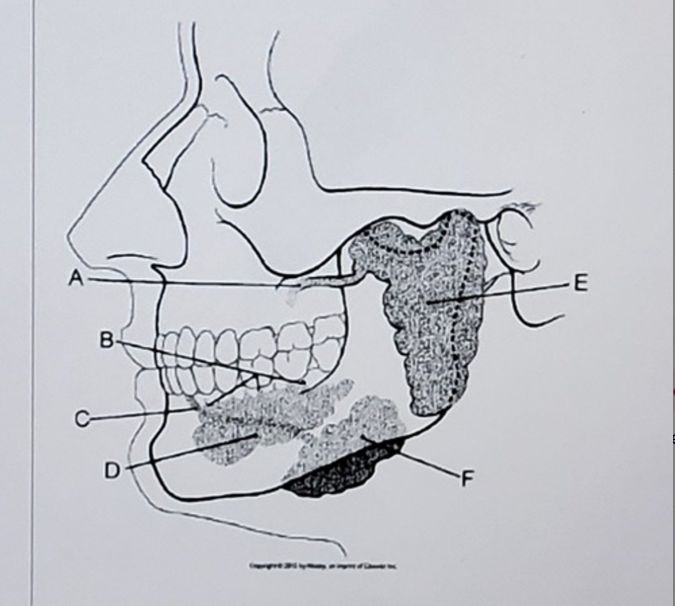
A
When preparing the contrast media for any cholangiography study, what precaution should always be followed?
A. ensure there are no air bubbles in the syringe, needle, or tubing as air bubbles mimic stones
B. have an extra supply of contrast media ready should the radiologist need to inject more than the usual amount
C. Always use the highest concentration of injectable contrast media your department has
D. Dilute the contrast media with 75% sterile saline to 25% contrast
B
How many degrees should the patient be rotated for AP oblique projections of the urinary bladder?
A. 16-30
B. 45-60
C. 10-15
D. 30-39
D
You have just injected 50cc of radiopaque. IV contrast into your patient for an intravenous urogram. You have paperwork to do and want to step out of the room to do it. Should you go? If not, how long do you stay with the patient to watch for an adverse reaction?
A. Stay with the patient for 25 minutes
B. Stay with the patient for 30 minutes
C. Stay with the patient for 5 minutes
D. Stay with the patient for 15 minutes
A
The respiration phase for exams pertaining to the urinary system is made on:
A. suspended on expiration
B. suspended on inspiration
C. shallow breathing
D. suspended respiration
D
Where is bile produced?
A. duodenal mucosa
B. gallbladder
C. pancreas
D. liver
1,2,3
During a diaphragm fluoroscopy exam, what activities does the radiologist ask the patient to perform?
1. Take short, quick breaths
2. Breath normally
3. take deep breaths
4. measure the distance the diaphragm moves between inspiration and expiration
D
Which position best demonstrates mobility of the kidneys?
A. Supine
B. lateral decubitus
C. RPO
D. upright
D
Which examination best demonstrates the functioning ability of the urinary system?
A. cystography
B. retrograde urography
C. voiding cystourethrography
D. intravenous urography
A
The central ray for AP and oblique projections of the urinary bladder when performed as part of a cystogram should be directed:
A. 2 inches above the symphysis pubis
B. to the iliac crests
C. to the symphysis pubic
D. to the ASIS
A
The central fay for scout radiographs of the urinary system is centered to the level of the:
A. iliac crest
B. ASIS
C. Xiphoid process
D. lower rib margin
C
When setting up for a aialogram, which type of contrast media will you obtain for the radiologist to use?
A. Gastrografin
B. Barium
C. Nonionic iodine-based contrast
D. Carbon dioxide crystals
B
The liver is divided into ______ major and minor lobes.
A. two
B. four
C. three
D. six
B
Which salivary gland has multiple small ducts which open into the floor of the mouth?
A. submandibular
B. sublingual
C. parotid
D. periramal
C
A radiograph of a right posterior oblique (RPO) position taken during an IVU reveals that the left kidney is foreshortened and superimposed over the spine. What must the technologist do to correct this error during the repeat exposure?
A. increase CR angulation
B. place the patient in the LPO position to better demonstrate the right kidney
C. decrease body rotation
D. increase body rotation
A
Radiography of the urethra is called _____________.
A. cystourethrography/retrograde urethrogram
B. cystography/cystogram
C. cystoureterography
D. retrograde urography
B
Which of the following is true regarding the kidneys?
A. the right kidney is longer and narrower than the left
B. the left kidney is longer and narrower than the right
C. the left kidney is lower than the right
D. both kidneys are the same width and length
1, 2, 3
Which of the following functions are performed by the gallbladder?
1. storage of bile
2. concentration of bile
3. contraction and release of bile
4. production of bile
A
Evaluation of the kidneys and ureters by direct catheterization of the ureter is called:
A. retrograde urography
B. IV urography
C. Nephrotomography
D. Infusion tomography
1,2,3
T-tube cholangriography is performed:
1. postoperatively
2. to visualize residual stones
3. on a patient who has had a cholecystectomy
C
To lace the left kidney parallel to the plane of the IR, it is necessary to rotate the patient:
A. 45° LPO
B. 45° RPO
C. 30° RPO
D. 30° LPO
A
The timing of imaging during an IVU begins when the:
A. injection is started
B. radiologist enters the room
C. the scout image is taken
D. injection is completed
all of the above
A bronchoscopy is performed for which of the following reasons?
1. investigate the reason for hemoptysis
2. treat certain lung conditions such as a mucous plug
3. obtain tissue samples for biopsy
4. remove a foreign body
D
Where is the IR centered for cystourethrography studies on men or women?
A. 2 inches below the symphysis pubis
B. 2 inches below the ASIS
C. ASIS
D. at the superior border of the symphysis pubis
1 and 3
which of the following types of contrast can be injected into a joint space for radiography of the menisci, cartilage, bursae, etc.?
1. Air
2. Barium
3. Iodinated contrast
1 and 2
These categories medications are commonly used in spinal pain management procedures:
1. corticosteroids
2. anesthetics
3. analgesics
D
Which of the three segments of the uterine tube communicates with the uterine cavity?
A. interstitial
B. Ampulla
C. Infundibulum
D. Isthmus
1, 2, 4, 5, 6
When performing an arthrogram or myelogram, which of the following are the usual duties of the radiologic technologist?
1. set up room and sterile tray
2. explain procedure to patient
3. sign the informed consent form as the primary person performing the exam
4. assist radiologist during exam
5. obtain any images requested by radiologist
6. obtain patient history
B
During a myelogram performed with the patient prone, why is a positioning block (bolster) placed under the abdomen for the lumbar puncture portion of the procedure?
A. For patient comfort
B. To widen the interspinous spaces
C. To prevent reflux of contrast media back into the syringe
D. To force the contrast media toward the head
D
A lumbar puncture most often occurs at what level in patients with no previous spine surgeries or injuries?
A: depends on where the pain is located
B: T-12 to L-1
C: L-4 to L-5
D: L2 to L3
C
How many pairs of spinal nerves arise from the spinal column?
A. 14
B. 29
C. 31
D. 24
C
Between which of the following is the subarachnoid space?
A. dura mater and arachnoid
B. pia mater and dura mater
C. arachnoid and pia mater
D. epidural and pia mater
B
Which two structures make up the central nervous system (CNS)?
A. brain and cerebellum
B. brain and spinal cord
C. cerebrum and spinal cord
D. cerebrum and cerebellum
A
The indications for this exam include headache, meningitis, CSF leak, intrathecal injection of chemotherapy medications.
A. lumbar puncture
B. epidural
C. lo-dose myelogram
D. discogram
C
The most common clinical indication for a myelogram is:
A. spinal cysts
B. bony injury to the spine
C. herniated nucleus pulposus (HNP)
D. benign tumors
C
What type of contrast is most frequently used to perform myelography today?
A. ionic, non-water soluble
B. non-ionic oil-based
C. non-ionic water soluble
D. ionic, water soluble
All of the above
Which of the following is a contraindication for myelography?
1. increased intracranial pressure
2. blood in the CSF
3. arachnoiditis
4. meningitis
B
Lo-dose myelograms are more common today than full-dose (high dose) myelograms. What is the major difference between lo-dose and full-dose myelography?
A. contrast media is the same concentration and immediate post injection images are taken in diagnostic before the patient goes to CT
B. contrast media is less concentrated and all imaging is done in CT
C. more contrast media is injected for the lo-dose exam
D. recovery time is longer for the full-dose exam
C
Which diagnostic imaging examination is used most often to initially diagnose vertebral compression fractures?
A. CT of the spine
B. Nuclear medicine bone scan
C. Lateral spine radiograph
D. MRI scan of the spine
B
___________ involves image-guided needle injection of contrast into the nucleus pulposus.
A. lumbar myelography
B. discography
C. arthrography
D. cervical myelography
C
What is the most common cause of vertebral compression fractures?
A. cancer
B. trauma
C. osteoporosis
D. infection
C
What is the purpose of tilting the table during Myelography?
A. to facilitate patient comfort
B. to attach the footboard
C. to move the contrast medium to the desired portion of the spinal column
D. to remove cerebrospinal fluid from the patient
B
Where is the contrast media instilled during a myelogram?
A. spinal cord
B. subarachnoid space
C. subdural space
D. epidural space
D
1. The ______ urethra is approximately 3.5 cm long.
a. membranous
b. anterior
c. external
d. prostatic
A
1. The ______ urethra extends from the penoscrotal junction to the external meatus.
a. penile
b. bulbar
c. membranous
d. prostatic
B
1. The innermost layer of the ureters is the:
a. adventitia.
b. mucosa.
c. muscularis.
d. submucosa.
A
1. The urine formation process begins with:
a. glomerular filtration.
b. tubular reabsorption.
c. tubular secretion.
d. water conservation.
false
true of false: Retrograde urethrograms (RUG) are most effective in evaluating the posterior urethra, whereas the voiding cystourethrogram (VCUG) provides optimal visualization of the anterior urethra
C
1. Indications for an RUG include:
a. recurrent urinary tract infections.
b. vesicoureteral reflux.
c. weak urinary stream.
d. urinary incontinence.
D
1. U.S. Food and Drug Administration regulations require all fluoroscopy units to be equipped with a cumulative timer device that typically alerts the operator every ______ minutes of the length of time the patient has been exposed.
a. 2
b. 3
c. 4
d. 5
C
1. During an RUG examination, the patient is positioned in a ______ º to ______ º right posterior oblique position.
a. 10; 20
b. 20; 30
c. 35; 45
d. 55; 65
D
1. RUG and VCUG complications include: 1. pain. 2. minor hematuria. 3. urinary tract infection.
a. 1 and 2
b. 1 and 3
c. 2 and 3
d. 1, 2, and 3
B
Signs and symptoms of urethral stricture include: 1. weak urinary stream. 2. frequent urination. 3. postvoid dribbling.
a. 1 and 2
b. 1 and 3
c. 2 and 3
d. 1, 2, and 3
A
___ is a chronic inflammatory disease that affects the genital skin and causes destructive scarring in the urethra.
a. Balanitis xerotica obliterans
b. Chondyloma acuminata
c. Urogenital tuberculosis
d. Infectious urethritis
A
Extravasation of contrast above the urogenital diaphragm only is consistent with a type ______ urethral injury.
a. II
b. III
c. IV
d. V
esophageal hiatus
the hole in the diaphragm that allows the esophagus to go through the abdominal cavity and attach to the stomach is called the __ __