Section 11 - Renal System
1/89
Earn XP
Description and Tags
This chapter can be confusing. I recommend reading the book as the lecture notes are kind of jumbled.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
90 Terms
What are the two main functions of the urinary system?
Excretion of metabolic waste products
Regulation of extracellular fluid, both volume and concentration
Primarily extracellular water
Functionally, it is the ___ that controls the activities of the urinary system
Kidneys
Function of the Kidneys
Filtration of metabolite waste from the blood and water retention (which will then return to circulation later on)
What 3 shapes can the kidney take on? In what species is each shape found?
Bean-shaped
Most species, such as dogs, cats, goats, etc
Heart-shaped
The right kidney in horses
Lobulated
Cattle
Where does blood supply from the kindey come from?
Directly off of the descending aorta of the heart
How does filtered blood from the kidneys return to circulation?
Directly back to the vena cava via renal veins
The right kidney sits ___ on the aorta and has a slightly ____ blood pressure
Higher, higher
Which kidney is better at filtration? Left or right?
Right, due to its position on the aorta and its higher blood pressure
Kidney: Hilus
An indentation in the outer structure of the kidneys where blood vessels, nerves, and ureter enter or exit the kidney
Kidney: Cortex
Outer region of the kidney which houses the structures that filter metabolites out of the blood by allowing significant water to cross out of the blood
Kidney: Medulla
Inner region of the kidney (just below the cortex) where water is regulated.
Water is reabsored, concentrating metabolites prior to voiding.
Region of collection
Kidney: Renal Pelvis
An extension of the ureter into the kidney where urine is directly deposited by the medula for transport to the bladder
What is the filtered fluid that enters the renal pelvis called? Does it change any further?
Urine. Once the filtered fluid enters the renal pelvis, it remains unchanged
Exception is in horses, where it changes further in the bladder
Ureters
Highly muscular tubes that peristaltically pump urine unidirectionally away from the renal pelvis to the bladder.
How to the ureters enter the bladder? What does it form?
The ureters enter the bladder at an angle, forming a functional one-way valve that prevents backflow into the kidney. This is termed the ureterovesicular junction.
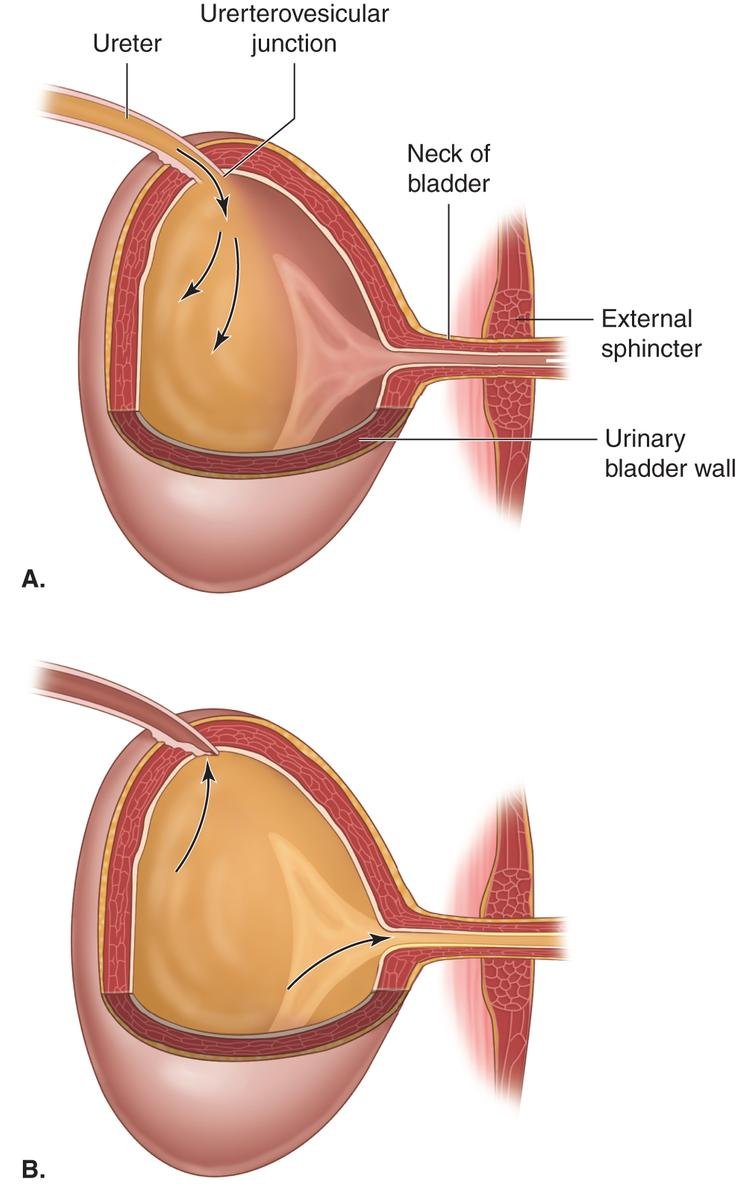
Bladder
A highly elastic, muscular storage vessel that can expand and fill with urine.
Epithelium can change configuration and allow for expansion
When the bladder is full, muscle contractions will lead to its emptying
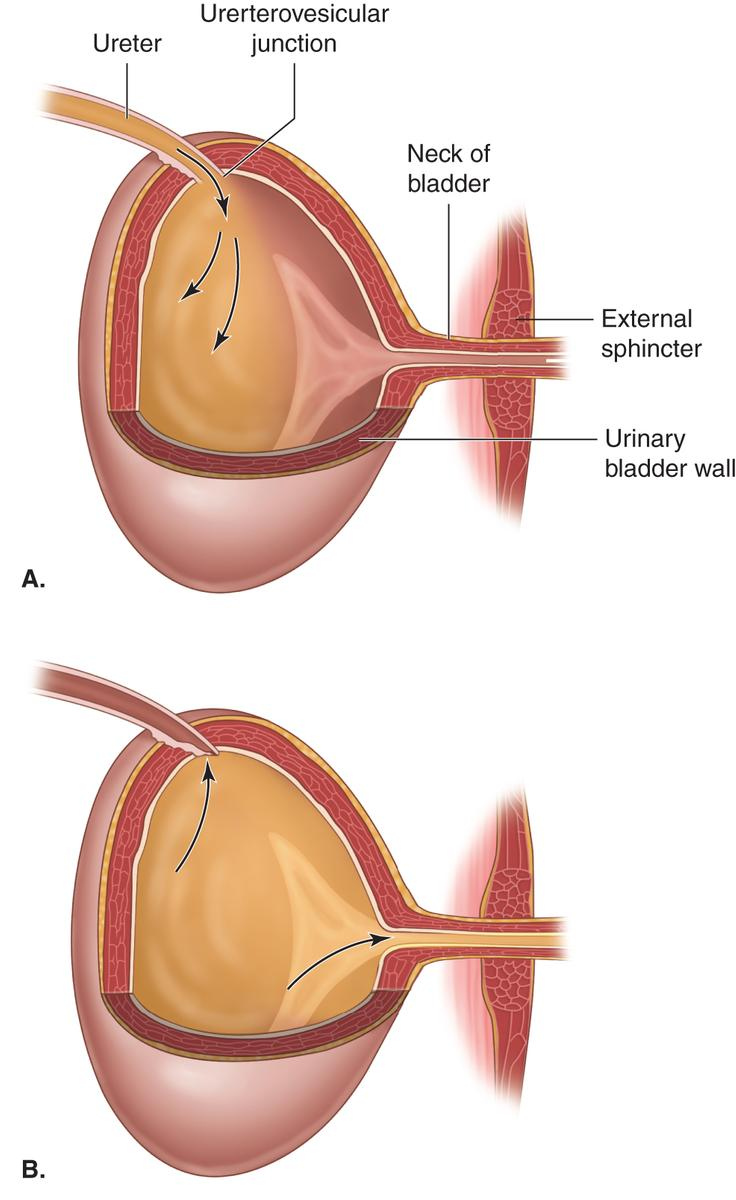
Neck of the Bladder
Highly elastic structure that forms an internal sphincter which is normally closed.
Opens during contraction to allow bladder to empty
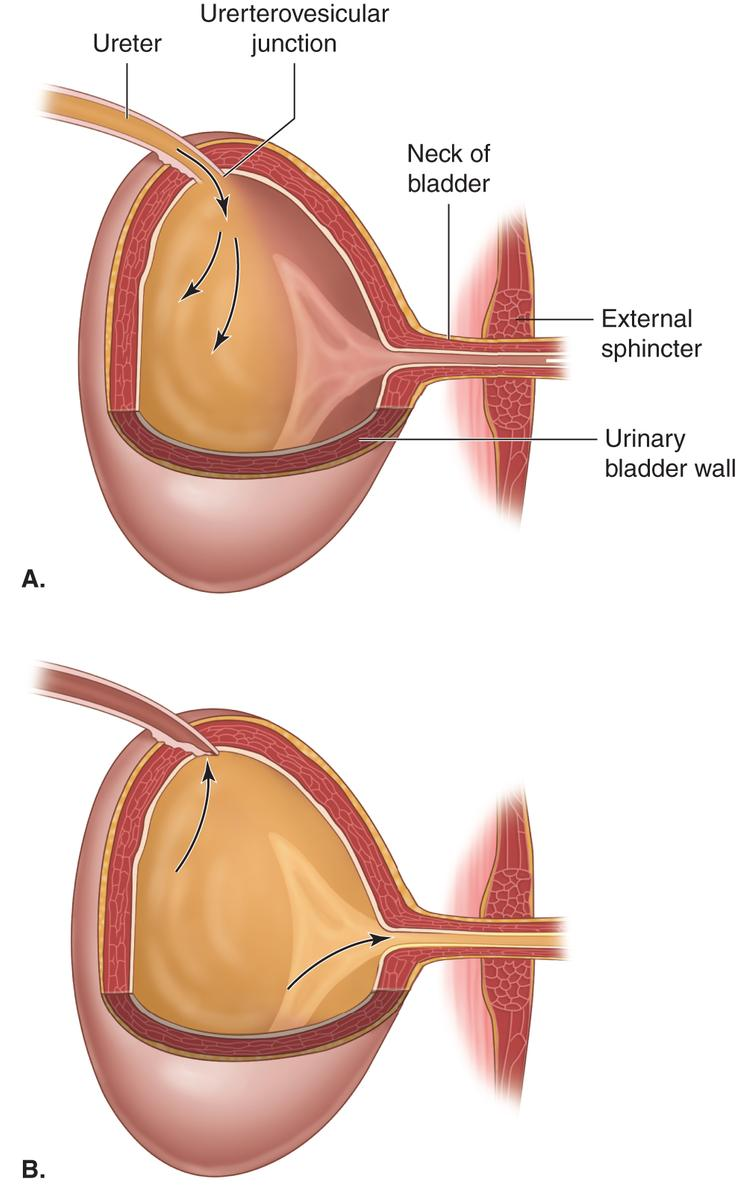
External sphincter
A skeletal sphincter muscle that makes up the junction between the bladder and the urethra. Prevents urine escape when its contracted.
Sacral spinal cord allows urine to escape through the neck and external sphincters
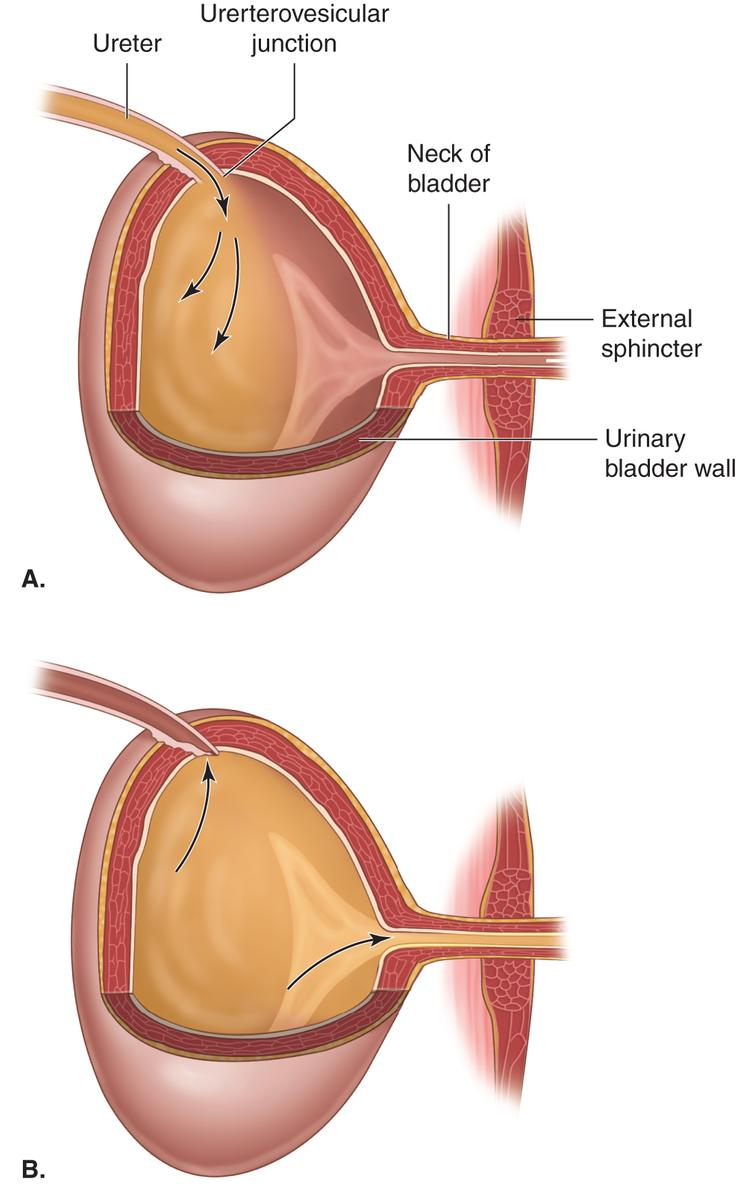
Urethra
A single muscular tube that peristaltically pumps urine outside of the body
What is urine expulsion a combination of?
Sphincter relaxation and muscles of the bladder contracting
Nephron
The functional unite of the kidney. Consists of a filtration zone and a water regulatory region.
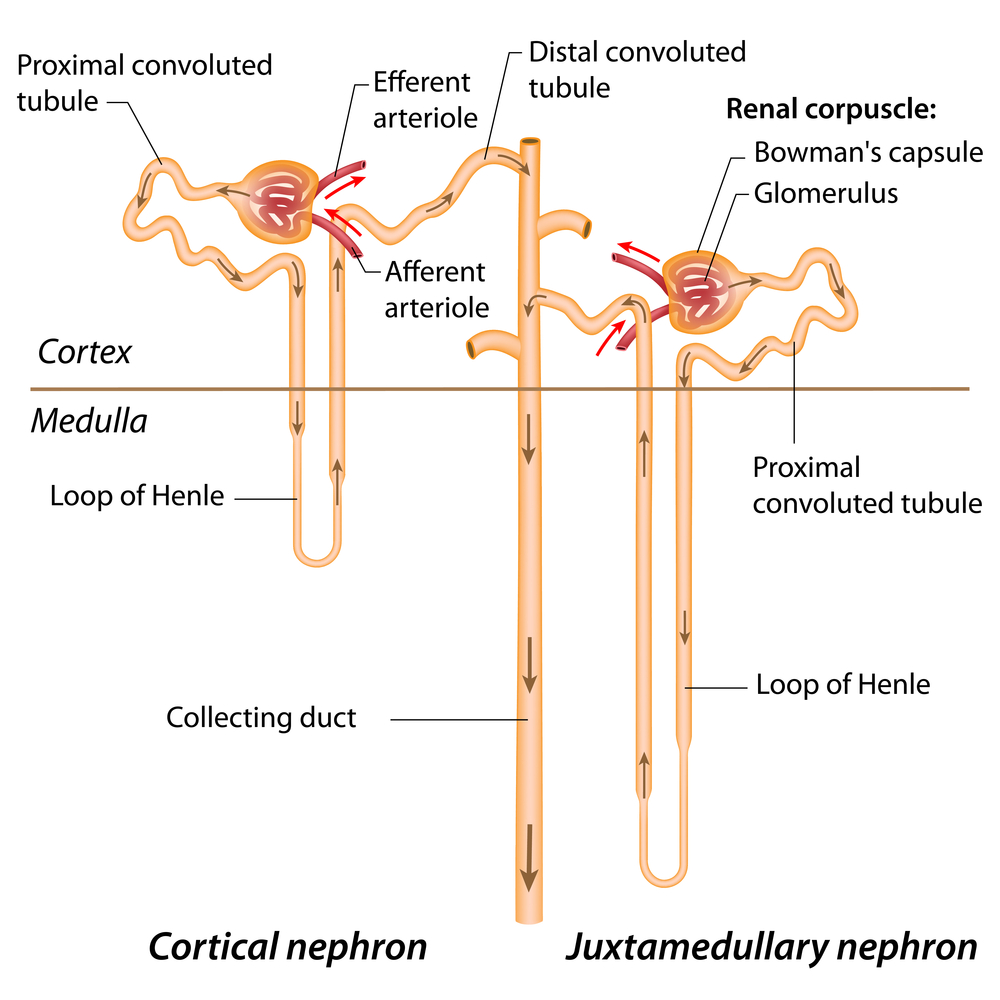
Glomerulus
Two specialized porous capillary beds located in the cortex of the kindey involved in blood filtration. High in pressure.
Akin to arterial end of capillary
Porous state allows larger molecules to cross the endothelium
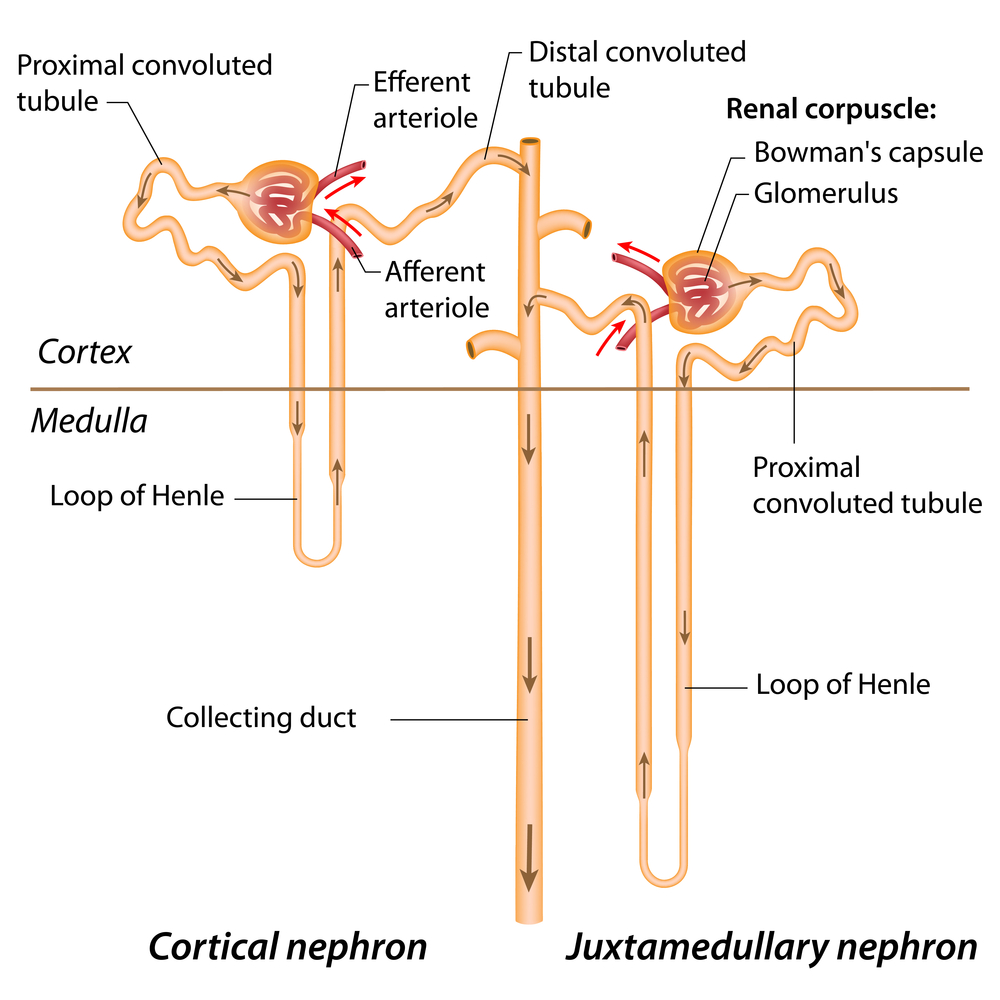
Peritubular capillary
Low pressure section of the glomeruli where blood perfuses (permeates) from the glomeruli
akin to venous end of capillary
Loop of Henle
The water regulating portion of the nephron
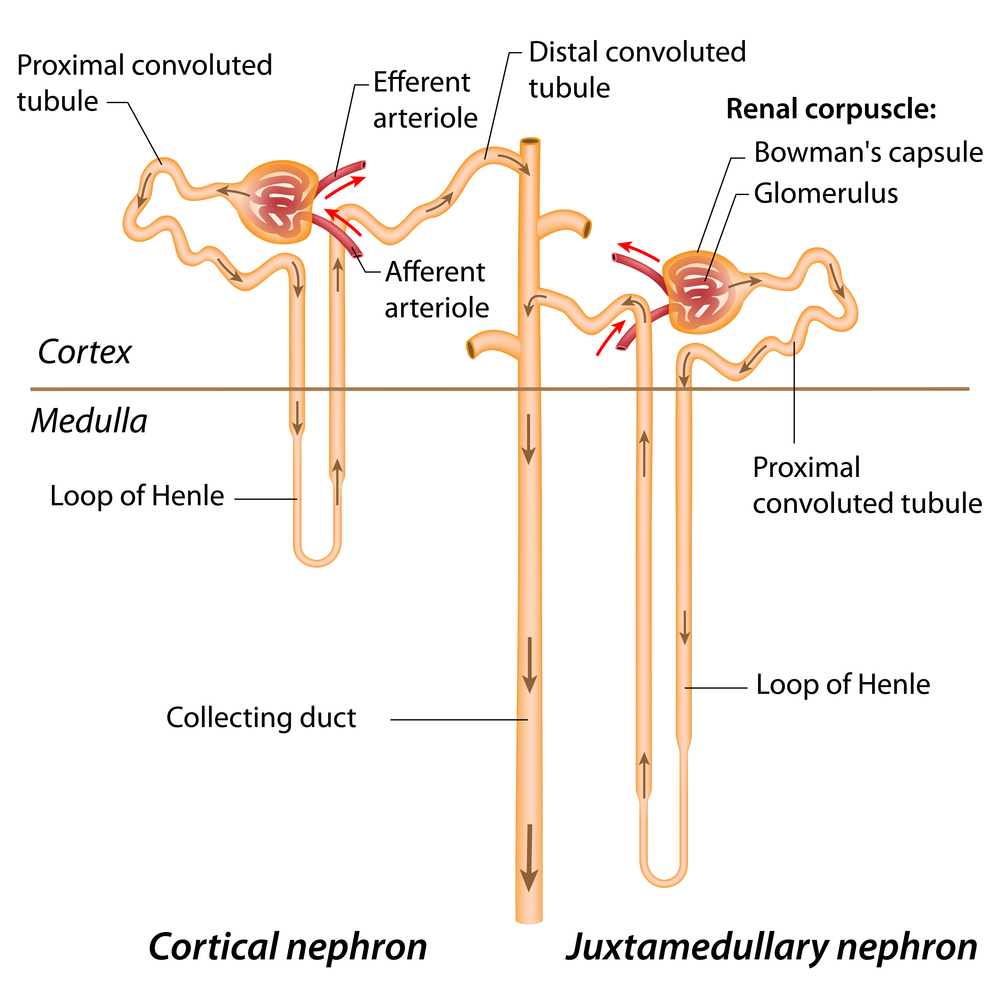
The ability of the nephron to reabsorb water is determined by what?
How far it extends into the medulla
Cortical Nephron
Type of nephron where the glomeruli are located high within the cortex and the loop of henle reaches only to the top of the medulla (left)
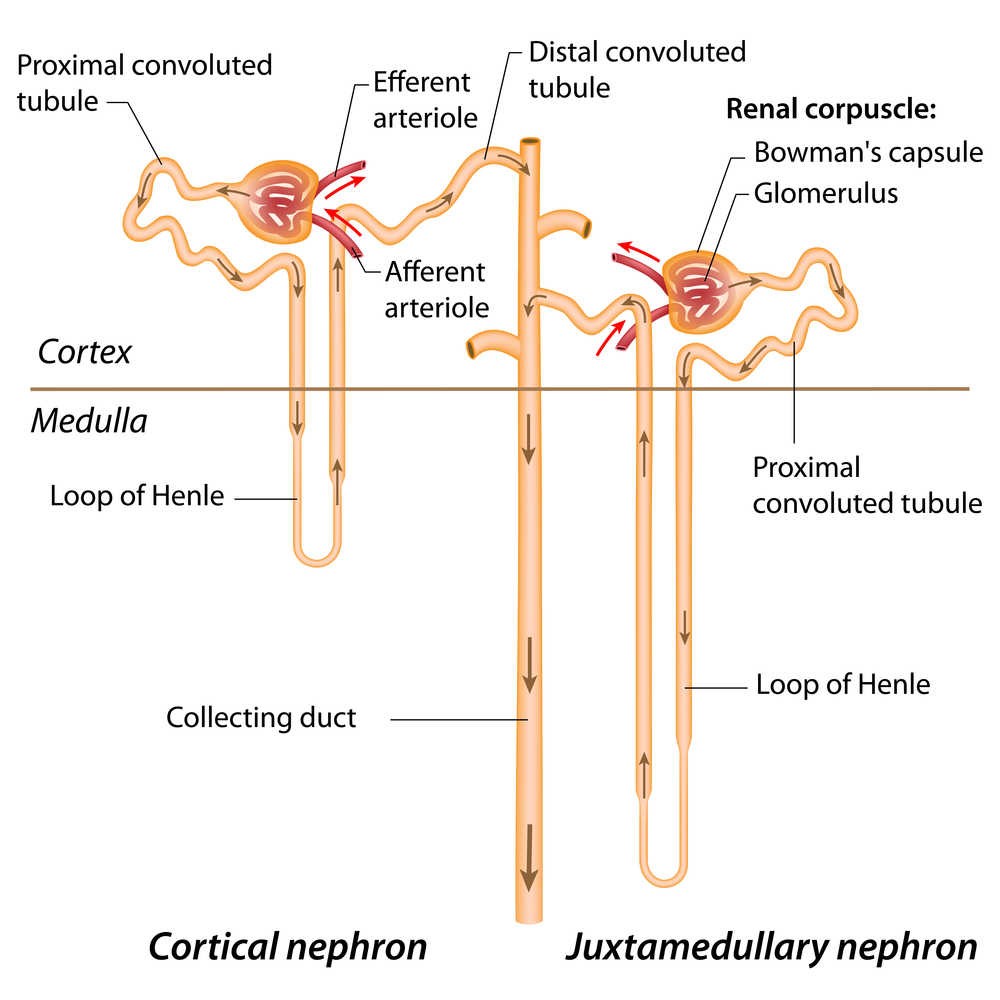
Juxtamedullary Nephron
Type of nephron where the glomeruli sit just above the cortical-medullary junction and the loop of henle plunges deep into the medulla (right)
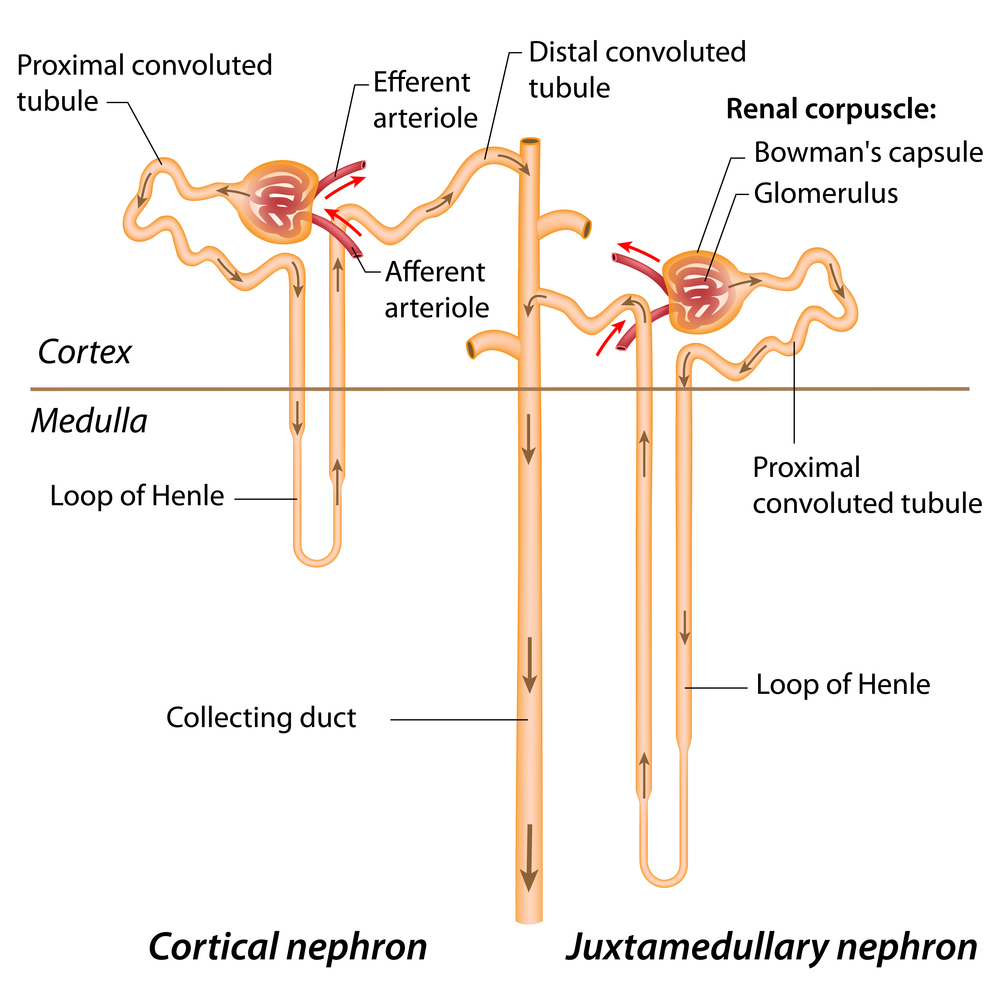
What do both the cortical and juztamedullary nephrons do?
Creates and maintains a significant osmotic pressure that moves water filtered by the glomerulus back into the body
Do the overall number and type of nephrons vary between species?
Yes.
Those that depend more on metabolic water would have more juxtamedullary nephrons
Bowmans capsule
A funnel-like structure that encapsulates the glomerulus and collects filtered materials from it. Connects directly to the proximal tubule.
How does pressure differentiate between the glomerulus and the bowmans capsule?
When pressure in the glomerulus is high, the pressure in the bowmals capsule is low.
How does the bowman’s capsule maintain its lower pressure?
via the loss of filtrate, both hydrostatic and osmotic
How is blood supplied to the glomerulus? How does it leave?
Supplied via the afferent arteriole and leaves via a veniole to the renal vein
How does the pressure difference between the glomerulus and the bowmans capsule allow the nephron to function?
Because liquid moves from areas of high to low pressure, the difference allows for the fluid within the glomerulus to pass through the clefts in the capillary bed to then be filtered into the bowmans capsule.
This process is primarily passive
What is the fluid thats filtered into the bowmans capsule called?
Glomerular filtrate (GF)
Proximal tubule
Transports materials from the bowmans capsule to the loop of henle
When GF (Glomerular filtrate) enters the proximal tubule, what is it then called?
Tubular fluid
What parts of the nephron are responsible for water regulation?
The proximal tube, loop of henle, and distal tubes.
The tubules
What percentage of of filtered water continues on as a component of urine?
1%
Loop of Henle
Contains descending tube, ascending tube, area of reabsorption, and connects to the distal tubule
Distal tubule
Transports materials from the loop of henle to the collecting ducts
Vasa Recta
Surrounds the loop of henle and regulates water and ion reabsorption
Juxtaglomerular apparatus
Specialized region where blood supply and the distal tubules are connected. This regulates kidney blood flow, rate of filtration, and the release of renin (an enzyme.
How is urine formed?
Glomerular filtration — filters materials passing through the glomerulus and into the bowmans capsule (GF) which then becomes tubular fluid upon entering the tubules
Tubular reabsorption — reabsorption of water and ions back into the blood supply as the fluid travels through the tubules
Finally ends when the fluid enters the renal pelvis, where it remains unchanged until expelled
Where does reabsorption take place in the nephron?
Entire length of the tubules
Where is true urine found?
Renal pelvis
Renal Blood Flow (RBF) and its importance
Rate of bloow flow to the kidneys, effectively equals the renal plasma flow
Important for the formation of glomerular filtrate
Glomerular filtration rate (GFR)
The portion of plasma filtered across the glomeruli
Filtration Fraction (FF)
Ratio of Glomerular filtration rate (GFR) to Renal blood flow (RBF)
GFR:RBF
Protein crossing the glomeruli and entering urine represents a what state?
Diseased
Dilation of the afferent arteriole leads to what?
Increased RBF, hydrostatic pressure, and potentially higher filtration
Constriction of the afferent arteriole leads to what?
Decreased RBF but higher hydrostatic pressure.
Constriction and Dilation of the afferent arteriole causes different things, but ultimately maintains what?
The filtration fraction (FF)
Tubular Reabsorption
Movement of substance in the FF back across the tubular epithelium into the interstitual fluid or capillary
Tubular Secretion
Movement of a substance not filtered at the glomerulus across the tubular epithelium into the tubular fluid
Why is Glucose unique in the urinary system?
Due to its size, it is easily filtered into the tubular fluid and reabsorped at 100% back into the body.
ADH
Antidiuretic hormone — controls the permeability of the epithelial cells to water
Without it, excessive water would leave as urine
What factors affect ADH release?
Decreased blood volume
Monitored by volume receptors (pressure) in the walls of major vessels. Stimulates ADH release to increase water retention
Cold environments
Inhibits ADH, causing increased urine production and thirst
Alcohol
Increases urination; water loss exceeds alcohol consumption
Angiotensin II
Controls GFR as well as maintains FF when RBF is decreased
Aldosterone
Regulates extracellular potassium (K) and requires reabsorption of sodium (Na)
Secretion is under the control of ADH
Parathyroid Hormone
Regulates calcium (Ca) reabsorption and the formation of the active form of vitamin D
Promotes Ca absorption in the gut via cacitriol
Micturition
Emptying of the bladder
Transfer of urine to the urinary bladder due to differences in hydrostatic pressure
The stretching of the bladder’s epithelium triggers what?
Pressure sensors that send signals to the control centers
Brain stem’s function in urination
Prevents contraction of the bladder and maintains contraction of the sphincter
When the bladder is full, what occurs?
Sensors in the bladder stimulate the cerebral cortex, allowing voluntary control of micturition.
Once mictruition starts, can it stop?
No. A second reflex is triggered that insures complete emptying of the bladder.
Bladder contractions continue until what?
No further flow is sensed through the urethra.
Why is urine formed?
Ultimately, to maintain balance of extracellular fluid by removing waste
General materials found in urine are present in extracellular fluid
If materials are in high concentration in the body, will they be excreted in urine? Low concentrations?
If the materials are in high concentration, they will be excreted. If in low concentration, they will be conserved.
What gives urine its yellowish color?
Bilirubin, which has been oxidized
In most animals, urine is watery. In what animal (that we learned of) is this not the case?
Horses, as their urine is syrupy
Urine has a nitrogenous component known as?
Urea (in most species)
Where is urea formed? What does it require? Toxicity?
Urea is formed from ammonia in the liver, of which is highly toxic. It requires a large amount of energy to be made. However, once transformed into urea, it is relatively non-toxic in comparison to ammonia.
Polyuria
Increase urine output
Oligouria
Decreased urine output
Anuria
No urine output
Dysuria
Painful urine output
Continence
Maintenance of urine in the bladder between urinations
Incontinence
Leaking of urine from bladder with sphincter closed
What factors lead to incontinence?
Age, injury (especially to spinal cord), and disease
Renal Clearance
Measurement of the ability of a kidney to remove compounds from plasma
Are most substances fully cleared upon each pass through the kidney?
No, only a few substances are. They must be freely filtered at the glomerulus and not reabsorbed
What is the normal pH of the body?
7.4
How does the kindey balance pH?
By filtering and secreting excess ions into tubular fluid and by creating buffers.
What are the 3 buffers that the kidney makes? What do these work together to form?
All 3 form the isohydric principle
Bicarbonate buffer — binds to hydrogen ions in the extracellular fluid, reacts with strong acids/bases
Biphosphate buffer — maintains intracellular pH (similar to bicarbonate)
Protein system buffers — Contain significant free anions which readily absorb and donate hydrogen
What do avians form instead of urea? Why?
Uric acid. Formed instead to maintain water, as creation of urea not only necessitates loss of water, but requires a large amount of energy
Important for animals that lay eggs.
In animals, of the 3, which would always indicate a diseased state?
Calcium, bilirubin, RBC
RBC will always indicate a diseased state
What is urine (utilize the term “blood plasma”) basically?
Urine is what is left of blood plasma after it has gone through filtration, reabsorption, and secretion.
What two hormones regulate water movement in the kidney?
ADH and Aldosterone
Does reabsorption of materials from the lumen of a nephron always require energy?
No. It can require energy (such as for glucose, ions, etc), but it can also be passive due to diffusion and osmosis (water, urea, some ions)