Comprehensive Guide to Sulfonamides and Beta-Lactam Antibiotics in Nursing
1/64
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
65 Terms
What are sulfonamides commonly known as?
Sulfa drugs
What is the mechanism of action for sulfonamides?
Bacteriostatic
What are the primary uses of sulfonamides?
Urinary tract infections, ulcerative colitis, otitis media, bacterial skin and eye infections, and treatment of infections with 2nd and 3rd degree burns.
What are some common adverse reactions to sulfonamides?
Nausea, vomiting, diarrhea, abdominal pain, stomatitis, photosensitivity, crystalluria, and sulfa allergy.
What serious condition can result from sulfonamide use?
Steven Johnson Syndrome
What are the contraindications for using sulfonamides?
Allergies to sulfa, use at the end of pregnancy, and breastfeeding.
In which patients should sulfonamides be used cautiously?
Patients with renal impairments, hepatic impairments, and bronchial asthma.
What should be monitored during treatment with sulfonamides?
All adverse reactions.
How should sulfonamides be administered in relation to meals?
On an empty stomach, 1 hour before or 2 hours after meals.
What is the recommended fluid intake while taking sulfonamides?
Increase fluid intake by 2,000 mL of water per day.
What color may urine and skin turn when taking sulfonamides?
Yellow-orange.
What is an important patient teaching point regarding sun exposure while on sulfonamides?
Avoid exposure to sun or UV light due to photosensitivity.
What should patients be informed about regarding the application of topical sulfonamides?
They may experience stinging or burning upon application.
What is the first step in burn treatment with topical sulfonamides?
Clean and remove debris before applying the ointment.
What should patients do if they experience adverse symptoms while taking sulfonamides?
Report the symptoms to their healthcare provider.
What is the expected outcome of using sulfonamides?
Effective treatment of the targeted infections.
What is the nursing process related to the administration of sulfonamides?
Administer on an empty stomach, push fluids, monitor for adverse reactions, and educate the patient.
What are the legal and ethical responsibilities of nurses regarding anti-infective drugs?
Ensure safe administration, monitor for adverse effects, and educate patients.
What should be done to prevent crystalluria when taking sulfonamides?
Increase fluid intake.
What is the significance of the synergistic agent in sulfamethoxazole/trimethoprim?
It enhances the antibacterial effect of sulfonamides.

What is the mechanism of action of beta-lactam antibiotics?
They break down the bacterial cell wall, causing bacteria to die.
Name two types of beta-lactam antibiotics.
Penicillins and Cephalosporins.
What are beta-lactams primarily used for?
Treating bacterial infections, including skin, lung, throat, and urinary tract infections.
What is a common side effect of beta-lactam antibiotics?
Allergic reactions, nausea, diarrhea, and abdominal pain.
What does prophylaxis mean in the context of penicillin use?
Preventive treatment to avoid infections.
What is the problem with natural penicillin?
Increased incidence of bacterial resistance and narrow spectrum of activity.
What causes resistance to penicillin?
Certain bacteria can produce penicillinase, an enzyme that inactivates penicillin.
What is the action of penicillin?
It stops bacteria from building their cell wall properly, leading to their death.
What should be monitored after administering penicillin?
Monitor for allergic reactions for 30 minutes post-administration.
What is anaphylactic shock?
A severe allergic reaction that can occur with penicillin administration.
What is the nursing process step related to assessing patients on antibiotics?
Assess allergy history, present symptoms, vital signs, and evaluate response to therapy.
What is the significance of C&S before starting antibiotics?
Culture and sensitivity tests help determine the appropriate antibiotic to use.
What are common adverse reactions to penicillin?
Nausea, vomiting, diarrhea, glossitis, stomatitis, and anaphylaxis.
What should patients be advised regarding penicillin and pregnancy?
Use barrier methods to avoid pregnancy while on oral antibiotics.
What is the effect of inadequate concentration of penicillin?
It may become bacteriostatic, retarding growth but not necessarily controlling infection.
What type of infections are penicillins used to treat?
UTIs, soft tissue infections, STIs, and for prophylaxis.
What is the role of respiratory support in nursing considerations for penicillin administration?
To protect the patient's airway in case of an allergic reaction.
What is the beta-lactam ring?
A structural component essential for the action of beta-lactam antibiotics.
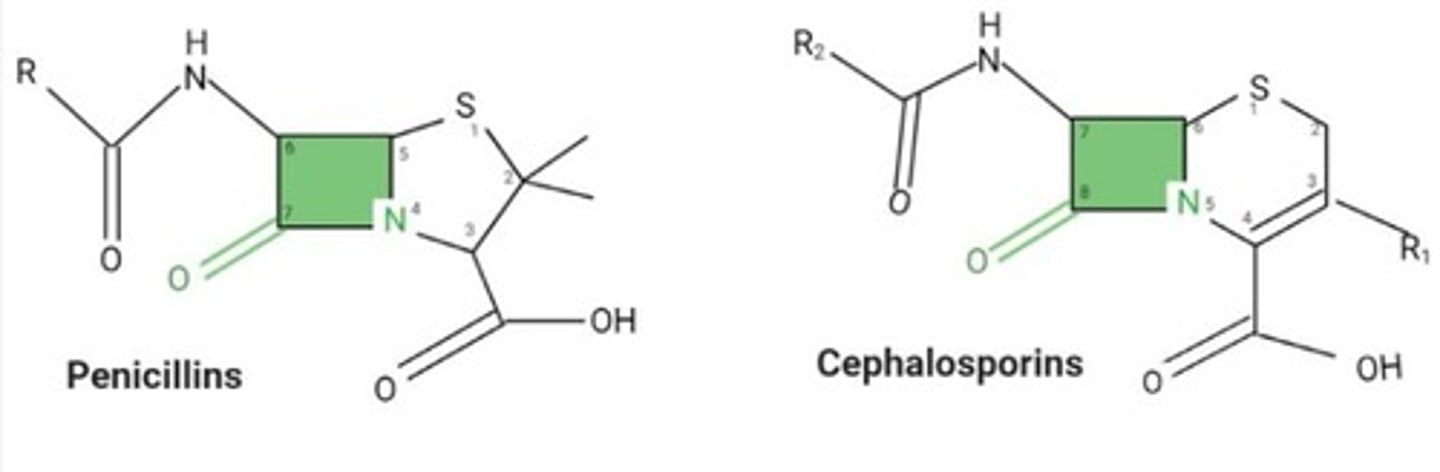
What types of infections can cephalosporins treat?
Skin infections and urinary tract infections (UTIs).
What should be done if a patient has a history of allergic reactions to antibiotics?
Monitor closely for signs of hypersensitivity and anaphylaxis.
What is the importance of taking penicillin on an empty stomach?
It enhances absorption and effectiveness of the medication.
What are the expected outcomes of anti-infective drugs?
Resolution of infection and improvement of symptoms.
What is the importance of adequate blood levels when administering penicillin?
Adequate blood levels are important for the effectiveness of the antibiotic.
When should oral penicillin be taken?
On an empty stomach.
What should patients be warned about when receiving IM penicillin?
It may sting.
What are potential superinfections associated with antibiotic use?
Oral, vaginal infections, and diarrhea.
What should patients be advised regarding the completion of antibiotic therapy?
Complete the full course of medication.
What can reduce the risk of superinfection when taking antibiotics?
Consuming yogurt or buttermilk.
What is a common adverse reaction to cephalosporins?
Nausea, vomiting, diarrhea.
What is a significant risk for patients allergic to penicillin when taking cephalosporins?
They may also be allergic to cephalosporins due to cross-sensitivity.
What is the primary use of vancomycin?
Treatment of serious gram-positive infections.
What serious adverse reactions can occur with vancomycin?
Nephrotoxicity and ototoxicity.
What should be monitored when administering vancomycin?
Renal function and signs of superinfection.
What is the recommended administration method for IV vancomycin to prevent adverse effects?
Administer slowly to prevent 'Red Man Syndrome'.
What should a nurse do if a client reports blood in their stools after antibiotic therapy?
Contact the primary health care provider immediately.
What is the priority nursing diagnosis for a client with a suspected fungal superinfection?
Altered Oral Mucous Membranes.
What should a nurse advise a client with skin irritation from penicillin therapy to avoid?
Harsh soaps, perfumed lotions, and rubbing the irritated area.
What instructions should be given to a client prescribed amoxicillin?
Take the drug on an empty stomach, an hour before or 2 hours after meals.
What should be done if a client misses a dose of amoxicillin?
Do not increase the next dosage; follow the prescribed schedule.
What is the significance of checking peak and trough levels for vancomycin?
To ensure therapeutic levels and prevent toxicity.
What precautions should be taken when administering vancomycin to patients with renal impairment?
Monitor closely for nephrotoxic effects.
What should be done if a client develops a mild skin irritation while on penicillin?
Advise them to avoid irritating products and actions.
What are the signs of a superinfection that should be monitored during antibiotic therapy?
Diarrhea, especially if it contains blood or mucus.
What should a nurse do before administering a cephalosporin to a client with a suspected urinary tract infection?
Collect urine for testing culture and sensitivity.
What is the recommended action if a client has a known allergy to penicillin?
Inform the primary health care provider before administering cephalosporins.