Muscle System PP’s(4) A&P1
1/76
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
77 Terms
Types of Muscle Tissues
Cardiac (Heart)
Skeletal
(Muscles attached to bone)
Smooth
(Organs, lining of blood vessels)
Muscle contraction depends on?
Myofilaments (2)
Actin & Myosin
Sarcolemma
cell membrane of a muscle cell
Sarcoplasm
cytoplasm of a muscle cel!
Skeletal Muscle Characteristics
Long, thin, multinucleate fibers
Striations (sarcomeres)
Voluntary control
attach to and cover bony skeleton
Contracts rapidly & vigorously, tires
easily - May exert great force
Cardiac Muscle Characteristics
1 - 2 nuclei
Network of fibers - intercalated disks
Only in heart
Striations (sarcomeres)
Involuntary control
rhythmic, steady rate (autorhythmic)
Smooth Muscle Characteristics
Spindle-shaped, one centrally-located
nucleus (uninucleate)
No striations (sarcomeres)
Involuntary control
Walls of hollow organs & blood vessels
Slow & sustained contractions
Functions of Skeletal Muscle Tissue
Produce Skeletal Movement
(contractions pull on tendons)
Maintain Posture + Position (Tension)
Support Soft Tissues
(Abdominal & pelvic cavity visceral organs)
Guard Entrances and Exits (open digestive & urinary tract)
Maintain Body Temperature (Thermogenesis)
Store Nutrient Reserves
amino acids (Intense exercise, insufficient diet, stress) & Glucose storage
Functional Properties of Muscle
Tissue
Excitability
(receive and respond to stimuli)
Contractility
(shorten forcibly when stimulated)
Extensibility
(be stretched or extended)
Elasticity
(return to the original length)
Skeletal Muscle Anatomy CT components
Fascia (sheet of fibrous CT)
Superficial - separates muscle trom skin Deep - lines body wall and limbs; holds muscle with similar functions together
Tendon - dense regular connective tissue that attaches skeletal muscle to bone
Aponeurosis - a sheet of connective tissue
Skeletal Muscle Anatomy CT Wrappings
Three layers of CT are part of each skeletal muscle
Epimysium (outermost)
Perimysium
Endomysium (innermost)
Epimysium
Surrounds entire skeletal muscle
- Collagen fibers
- Separates muscles from tissues/organs
- Connected to deep fascia
Perimysium
Surrounds fascicles
(bundles of muscle fibers)
- Collagen and elastic
fibers
- Contains blood vessels and nerves to fascicles
Endomysium
Delicate, elastic CT
- Surrounds individual skeletal muscle cells (fibers)
- Contains: Capillary networks, Satellite cells, & Nerve fibers
Why is every muscle fiber (cell) supplied with an extensive supply of blood vessels and nerve fibers?
facilitate high-energy contraction and precise, voluntary control
blood vessels remove metabolic waste (like lactic acid) to sustain metabolism
Microscopic Anatomy of Skeletal Muscle Fibers
Multinucleate
T (transverse) tubules
Sarcoplasmic reticulum (SR)
Multinucleate
(fusion of myoblasts in embryo)
- Have lost ability to undergo mitosis
T (transverse) tubules
- membranous channels extend into sarcoplasm as invaginations continuous with sarcolemma
Filled with extracellular fluid and extend deep into cell
Sarcoplasmic reticulum (SR)
- Network of membranous channels that surround each myofibril and run parallel
- Same as endoplasmic reticulum in other cells
- Has a high concentration of calcium ions compared to sarcoplasm
- Membrane becomes more permeable to calcium ions when stimulated
Triads
Terminal cisternae - dilated ends of sarcoplasmic reticulum
- Terminal cisternae butt against T tubule on both sides of T tubule
Triad = TC - T - TC
Muscle Fibers
Each muscle fiber is one long, thin cell
• Myofibrils make up muscle fibers
• Myotilaments make up myofibrils
• Two types of myofilaments
- Thick filaments (myosin)
- Thin filaments (actin)
Skeletal muscle cells (fibers) are
multinucleate. How is this important to the
function of skeletal muscle cells?
to manage their extreme length (up to 30 cm) and high metabolic demands
Striations
The striped appearance (striations) of skeletal muscle due to the arrangements of thick & thin myofilaments within the myofibrils
- A band = Dark area overlap of thick and thin
- I band = Light area thin filaments alone
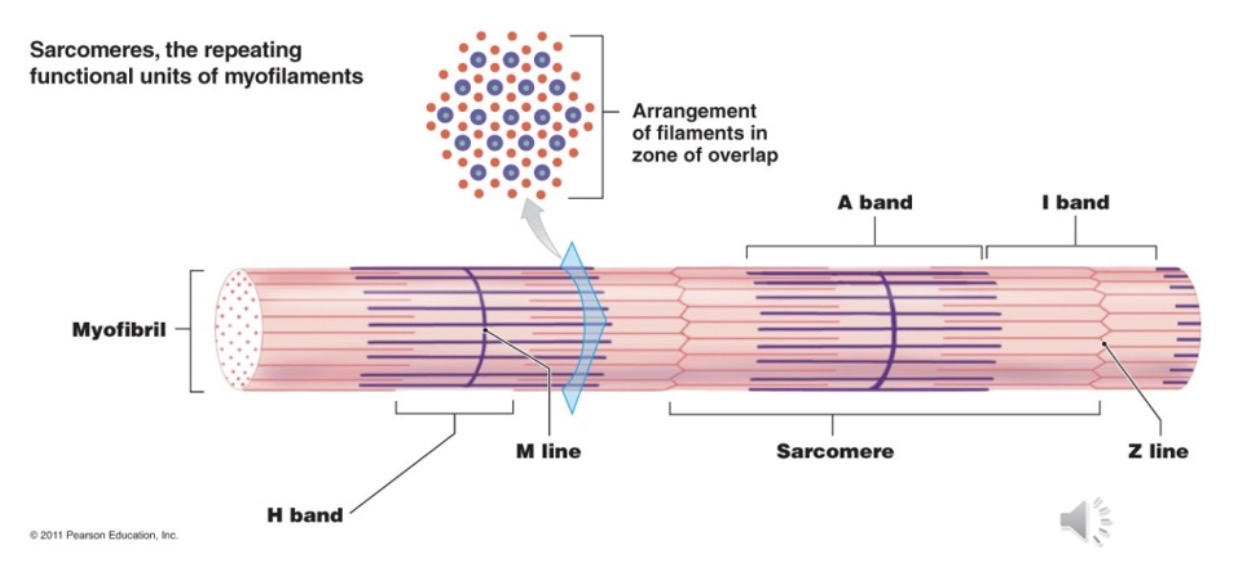
Sarcomeres
Length of myofibril divided into sarcomeres
- Sarcomere - functional unit of myofibril
- Z disc - separate one sarcomere from the
next sarcomere
- Z line - dense material between sarcomeres
- A band - dark band (length of thick)/ thick &
thin filaments
- I band - thin, but no thick mun
- H zone - center of A (heavy) -m
- M line - middle line or sarcomere; supporting proteins that hold thick filaments together; center of H zone
Levels of Functional Organization in a Skeletal Muscle
Skeletal Muscle (Surrounded by epimysium & Contains muscle fascicles)
Muscle Fascicle (Surrounded by perimysium & Contains muscle fibers)
Muscle Fiber (Surrounded by endomysium & Contains myofibrils)
Myofibril (Surrounded by sarcoplasmic reticulum & Consists of sarcomere)
Sarcomere (Contains thick (Myosin) &
thin (actin) filament)
Skeletal Muscle Proteins
Contractile Proteins
1. Myosin
2. Actin
Regulatory Proteins
1. Tropomyosin
2. Troponin
Structural proteins
1. Titin
2. Dystrophin
3. Myomesin
Contractile Proteins
Myosin (thick filaments) - Rod-like tail that ends in two globular heads (cross bridges)
- Cross bridges (head) interacts with active sites on thin filaments
Actin (thin filaments) - Coiled helical structure
- Myosin-binding site on each 'bead' of actin
Regulatory Proteins
Part of thin filament along with actin
Tropomyosin
- Rod-shaped protein
- Covers myosin-binding site on actin
Troponin
- Complex of 3 globular proteins
- One binds actin, one binds tropomyosin, one binds calcium
Structural Proteins
Titin - Holds the thick filaments in place; maintaining the organization of the A band
- Assists muscle cell back into shape after being stretched
- Helps muscle resist excessive stretching
Dystrophin - A cytoplasmic protein that links cytoskeleton to extracellular matrix; stabilizes the sarcolemma
Myomesin
- M line of the sarcomere; anchors myosin in A band
Skeletal Muscle Contraction
1. the H zones and I bands get smaller
2. The zones of overlap get larger
3. The Z lines move closer together
4. The width of the A band remains constant
Sliding filament theory
thin filaments sliding toward the center of each sarcomere, alongside the thick filaments (Hugh Huxley 1954)
- Muscle contraction involves the sliding movement of the thin filaments (actin) past the thick filaments (myosin)
- Sliding continues until the overlapping between the thin & thick filaments is complete
- (in a relaxed muscle cell, overlapping of thick & thin is only slight
Myofibrils shortening cause what?
The muscle fiber to shorten
Control of Skeletal Muscle Activity
Skeletal fibers contract only under control of nervous system
- Communication occurs at Neuromuscular Junction (NMJ)
- Each skeletal muscle fiber controlled by neuron at single NMJ
- Single axon braches within perimysium • End of branch = synaptic terminal (contains acetylcholine - ACh)
Synaptic cleft
- Motor end plate - region on sarcolemma that contains membrane receptors for ACh
- Junctional fold - increases surface area
Behavior of Skeletal Muscle Fibers (4)
Four major phases of contraction and relaxation
- Excitation (nerve action potentials lead to muscle action potentials)
- Excitation contraction coupling (event action potentials on sarcolemma to activation of myofilaments, preparing them to contract)
- Contraction (muscle fiber develops tension and may shorten)
- Relaxation (When stimulation ends, muscle fiber relaxes and returns to its resting length)
Contraction Process
ATP is already attached
• ATPase in myosin head hydrolyzes an ATP molecule
• Activates the head "cocking" it in an extended position - ADP + P; remain attached
• Head binds to actin active site forming a myosin-actin cross-bridge
Myosin releases ADP and Pi, and flexes pulling thin filament with it-power
stroke
• Upon binding more ATP, myosin releases actin & process can be repeated
- Recovery stroke recocks head
• Each head performs five power strokes per second
- Each stroke utilizes one molecule of ATP
Relaxation Process
Nerve stimulation and ACh release stop
• AChE breaks down ACh and fragments are reabsorbed into knob
• Stimulation by ACh stops
Ca+2 pumped back into SR by active transport
• Ca+2 binds to calsequestrin while in storage in SR
Ca+2 removed from troponin is pumped back into SR
•Tropomyosin reblocks the active sites of actin
Muscle fiber ceases to produce or maintain tension
Muscle fiber returns to its resting length - Due to recoil of elastic components and contraction of antagonistic muscles
Rigor Mortis
At death
- Circulation ceases
- No nutrients or oxygen to skeletal muscles
- Within hours skeletal muscles deprived of ATP
- SR unable to pump Ca++ out of SP
- Ca++ leaks into SP from ECF
- Triggers sustained contraction
- Without ATP, cross-bridges cannot detach
- Body becomes 'stiff as a board' - Rigor mortis lasts until lysosomal enzymes break down Z lines and titin
- Last about 15-25 hours
Botulism
Clostridium botulinum produces botulism toxin
• Botulism toxin is one of the deadliest
• Botulism toxin blocks exocytosis of synaptic vesicle at NMJ
• ACh is not released and the muscle contraction does not
occur
• Flaccid paralysis of skeletal muscle results
• Death usually results from paralysis of diaphragm and other respiratory muscles
Botox
Botox injections used cosmetically
• Medical use in treatment of
- Strabismus (crossed eyes)
- Blepharospasm (uncontrollable blinking)
- Chronic back spasms
Tetanus
Clostridium tetani
• Tetanus toxin blocks AChE
• Sustained powerful contractions
• Spastic paralysis
• 60% mortality rate
• 500,000 cases worldwide/year
• Only 100 cases/year in U.S
Tension Production
Tension is the force generated by the shortening of a sarcomere.
- Specific, quantifiable measure of the muscle's output
• Strength of the tension produced by muscle
fibers depends on:
- Number of pivoting cross bridges - Fiber's resting length at time of stimulation and
degree of overlap
- Frequency of stimulation
Length-Tension Relationship
Max. tension during contraction occurs when
resting sarcomere length is 2.0 - 2.4 um
• Too short: myosin crumples
• Overstretched: little to no crossbridges
• Resting muscle held to optimum length by: - Neural control & reflexes (e.g, stretch receptors)
- Joint positioning and bone structure
- Titin (elastic protein within sarcomeres)
Muscular Responses Recording a Muscle Contraction
Myogram - recording of a muscle contraction
• Twitch - a single contraction that lasts a fraction of a second (followed by relaxation) - Latent period - delay between
stimulation and contraction
- Contraction period
- Relaxation period
• Refractory period - time where muscle must return to its resting state (-90 mV) before it can be stimulated again
Contraction Strength of Twitches
Low frequency stimuli produce identical twitches
• Higher frequency stimuli (eg., 20 stimuli/s) produce temporal (wave) summation
- Each new twitch rides on the previous one generating higher tension
- Only partial relaxation between stimuli resulting in fluttering incomplete tetanus
• Unnaturally high stimulus frequencies (in lab experiments) cause a steady, contraction called complete (fused) tetanus
Muscular Responses
• Threshold Stimulus - The minimal strength of stimulation required to cause contraction
- A skeletal muscle fiber's resting membrane potential is~ -90 mV
- A skeletal muscle fiber must be depolarized from -90 mV to -55 mV before an impulse begins
- Therefore, the threshold stimulus is +35 mv
All-or-Nothing Response
If a muscle fiber is brought to threshold or above, it responds with a complete twitch
• If the stimulus is sub-threshold, the muscle fiber will not respond
Factors Affecting Tension at the Whole Muscle
Even if the same voltage is delivered, different stimuli cause twitches varying in tension, because:
- Fatigue - Muscles tire after continual use, reducing force output.
- Temperature - Warmer muscles' enzymes work more quickly, enhancing contraction speed
- Hydration - Affects cross-bridge formation and sarcomere function
Muscular Responses Motor Units
A motor unit is a motor neuron and the many skeletal muscle fibers it stimulates
• Because the motor neuron branches into several motor nerve endings, it can stimulate many skeletal muscle fibers simultaneously (causing simultaneous contraction)
• The number of muscle fibers in a motor unit varies from ~10 - over 1,000
Motor Unit Size
Small motor units-fine degree of control
- Three to six muscle tibers per neuron
- Eye and hand muscles
• Large motor units—more strength than control
- Powerful contractions supplied by large motor units with hundreds of fibers
- Gastrocnemius of calf has 1,000 muscle fibers per neuron
Muscular Responses Recruitment of Motor Units
Muscle is composed of many motor units, controlled by many different motor neurons, simultaneous contraction of all units does not necessarily occur
• As the intensity of stimulation increases, recruitment of motor units increases, until all contract simultaneously
• Muscles that produce precise movements are made up of small motor units
• Large motor units are active where greater contraction strength is needed, and precision is less important
Muscular Responses Muscle Tone
A certain amount of sustained contraction (tension) occurs in muscle fibers, even when a skeletal muscle is at rest
• Important in maintaining posture
• Small groups of motor units are alternately active and inactive
• Keeps skeletal muscles firm, but does not result in force strong enough to produce movement
Muscular Responses Types of Contractions - Isotonic
ISO = equal Ton = tension
• Muscle shortens and its
attachments move(s)
• Used for body movements and moving objects
- Concentric
- Eccentric
Concentric Isotonic Contraction
A muscle shortens and pulls on another structure (like a tendon) to produce movement and reduce the angle at joint
Eccentric Isotonic Contractions
The tension exerted by the myosin cross-bridges resists movement of a load and slows the lengthening process
Muscular Responses Types of Contraction - Isometric
Iso - equal/same
Metric - length
The muscle becomes taut, but the attachments) do not move (no contraction or extension)
Myosin crossbridges generate tension but the muscle does not shorten because the force of the load equals the muscle tensionPushing against a brick wall
Important for...
Posture
Joint stability
Energy Use and Muscular Activity
A single muscle fiber contains ~ 15 billion
thick filaments • When contracting, each thick filament
breaks down ~2500 ATP/second • Even small muscle contains thousands of muscle fibers
Muscle Metabolism Energy for Muscle Contraction
The energy used to power the interaction between actin and myosin comes from ATP
• ATP stored in skeletal muscles only lasts about six seconds
• АТР must be regenerated continuously if contraction is to continue
Production of ATP in Muscle Fibers
Three pathways in which ATP is
regenerated
1. Coupled reaction with Creatine Phosphate (CP)
2. Anaerobic cellular respiration
3. Aerobic cellular respiration
(ATP) Coupled Reaction with Creatine Phosphate (CP)
Relaxed muscles have excess ATP
• Use ATP to make CP
• ATP + C → ADP + CP
• CP stored in sarcoplasm
• Active muscle: CP gives P to ADP → ATP
• 15 sec burst of energy
• 100 m Dash
(ATP) Anaerobic Respiration
No O2 need for ATP synthesis
• Glycolysis: glucose
→ 2 pyruvic acid (PA) • If no O2 PA → lactic acid in cytosol
• Only 2 ATP/glucose
• Energy for 30 sec
• 400 m dash
(ATP) Aerobic Respiration
Muscle work > 30 sec requires O2
• If O2 PA to mitochondria
• Krebs cycle and Electron Transport
• 36 ATP/glucose • ~100 ATP/fatty acid
• O2 from blood and myoglobin
Glycogen
Glucose in active skeletal muscle obtained from glycogen
• Glycogen is polymer of glucose stored in
liver & skeletal muscles
• ~1.5% of total muscle weight is glycogen
• When muscle fiber begins to run short of ATP and CP, enzymes split glycogen into glucose subunits
• Glucose used to generate more ATP
Resting skeletal muscle Energy Use
- ATP Demand low
- Ample oxygen available
- Mitochondria produces surplus of ATF
- Extra ATP used to build up reserves of CP and glycogen
Moderate activity Energy Use
- Demand for ATP increases
- ATP production rises (oxygen
consumption increases)
- All ATP produced is used, no surplus available
Peak levels of activity Energy Use
- Enormous ATP demands; oxygen
limited
- Lactic acid formation (anaerobic)
Muscle Fatigue
A state of physiological inability to contract
• If no oxygen is available in muscle cells to complete aerobic respiration pyruvic acid (PA) is converted to lactic acid (LA) [lactate]
• Lactic acid causes muscle fatigue and soreness
Fatigue results from?
A relative deficit of ATP and/or accumulation of lactic acid (decreases pH; increases acidity)
What enables a skeletal muscle to continue contracting when there’s insufficient oxygen?
Glycolysis
What is more efficient than glycolysis?
Aerobic metabolism
Oxygen Debt (Postexercise)
• Elevated oxygen use after exercise
• Caused by change in muscle's chemistry during vigorous exercise
• Extra oxygen is used for restoring muscle processes
Use of extra oxygen (function)
• To convert lactic acid to glycogen (liver)
• to resynthesize creatine phosphate and ATP in muscle fibers
• To replace oxygen in myoglobin
Heat Production
Almost half of the energy released during muscle contraction is lost to heat, helps maintain body temperature at 37°C
• Excessive heat lost through negative feedback; sweating, dilation of superficial blood vessels, increased breathing rate and increased heart rate.
Graded Responses
• Muscle contractions are smooth and vary in strength based on demands
• Smoothness achieved by graded responses
• Variations in degrees of muscle contraction
• Changing the frequency of stimulation
• Changing the strength of the stimulus
Force of Contraction
• more motor units recruited = stronger contraction
• bulkier muscle = greater strength
(exercise causes hypertrophy)
Series-elastic elements are:
• Noncontractile structures of the body
• Tension must be exerted on tendons & coverings
Degree of muscle stretch = length-tension relationship
Velocity and Duration of Contraction
• Slow fibers
• Fast fibers
Major pathways for forming ATP
• Oxidative fibers - rely on aerobic pathways for ATP generation
• Glycolytic fibers - rely on anaerobic glycolysis
Muscle Fiber Characteristics
Color = Myoglobin content
• Red muscle fibers - high myoglobin content
• White muscle fibers - low myoglobin
• Fiber diameter varies
• Allocation of mitochondria varies
• Contraction velocity and resistance to fatigue differ between fibers
Slow Oxidative (SO) Muscle Fiber Type
Least powerful
• Fatigue resistant, red, myoglobin, many mitochondria, small fiber diameter
• Suited for endurance-type activity
• Marathon or triathalon