IDST 124 Midterm
0.0(0)
Studied by 4 peopleCard Sorting
1/56
Earn XP
Description and Tags
Last updated 6:40 AM on 3/1/23
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
57 Terms
1
New cards
What are some of the tools that cultural anthropologists use in their work? Describe them.
1. ***cultural relativism*** (cultural anthropology’s starting point)
1. seek to understand others’ points of view by putting aside judgements and opening our minds to understand the unfamiliar
2. DISTINCT from moral relativism
2. ***research methods***
1. long-term, participant observation fieldwork in the local language
2. semi-structured interviews
3. developing relationships with key informants
2
New cards
anthropology’s goals in studying culture and global cultural diversity
HUMANISTIC goals
* to make sense of what we perceive as others’ groups confusing behaviors
* to humanize stigmatized and excluded communities
* to represent their voices for policymakers and the broader public
* to improve efforts at cross-cultural collaboration, including global health
* to make sense of what we perceive as others’ groups confusing behaviors
* to humanize stigmatized and excluded communities
* to represent their voices for policymakers and the broader public
* to improve efforts at cross-cultural collaboration, including global health
3
New cards
importance of cultural anthropology research findings
necessary for global health programs to develop mutual trust and respect with local communities
necessary to ensure that interventions are well-received and effective
necessary to ensure that interventions are well-received and effective
4
New cards
How can anthropology help global health experts understand the cultural implications of their efforts to prevent and provide treatment during epidemics? Give an example.
Anthropologists are studying & seeking to influence global health to promote culturally meaningful responses to global health crises - ex: global response to ebola
\
CASE STUDY of anthropological research: global conflicts over containing Ebola in West Africa:
* local govt and global responses to ebola outbreak (2013-2014):
* Guinean Village where infection first identified shunned, roads & bridges cut off
* Doctors without Borders worked with Guinean govt to establish an ebola treatment unit
* govt imposed restrictions on burial and funeral rites (bc ebola found to be MOST infectious AT death AND 2-3 days before/after → specialists informing govt focused on meeting UN WHO’s “safe burial” protocol)
* local reactions to burial and funeral restrictions:
* VIOLENT clashes erupted and ebola treatment workers attacked/prevented from entering villages (including 8 members of a delegation of doctors/politicians/journalists murdered in 2014, murders of Red Cross workers, pervasive violence against treatment centers and providers)
* ***anthropology’s question: what’s at stake for these communities*** → cultural relativism informs a response based on:
* not assuming these are “irrational” or “ignorant” reactions
* instead inquire and LISTEN to people’s concerns
* anthropologists learned from the Kissi people (of Guinea’s forest region):
* social organization of everyday life
* population of \~140K ppl in region across Liberia, Guinea, and Sierra Leone
* ppl live in small self-governing villages of abt 150 ppl tucked inside groves of mango or kola trees
* most ppl are farmers (rice, manioc, cotton)
* local craftsmanship including basket weaving, iron work, and music
* cultural worldview of the Kissi people
* prosperity requires virtuous behavior (THINK: karma) - **fulfilling obligations** of youth towards elders + of the living towards the dying/ancestors
* illness and death result from moral violations (THINK: karma) - not demonstrating ongoing care and commitment to the elders or ancestors results in violation of CULTURAL belief
* Kissi social organization as a reflectance of cultural worldview
* society is organized into lineages and male/female initiation societies
* these socialize the next generation + provide structure for the living throughout the life cycle who educate youth, establish and reaffirm social hierarchy, demarcate sacred space ***(including PROPER BURIAL space)***
* initiation societies’ power over natural and social worlds and life-cycle transitions
* birth of a child = reincarnation of the village dead
* birth of an adult = initiation: land spirit swallows adolescent children & expels them as social adults
* birth of an ancestor into the village of the dead
* importance of initiation societies’ burial and funeral rituals to ensure a dead person’s birth as ancestor
* ancestor is an elevated status that must be achieved through work of descendants to properly care for their dying and dead relative
* IF descendants fail to fulfill these obligations, the dead spirit is condemned to wander eternally , will angrily torment descendants & undermine their prosperity
* aspects of proper care for descendants
* descendants must care & wash a dying person throughout his/her last days
* hear their final wishes
* help them settle outstanding debts
* show appropriate forms of grief at death
* prepare the body by washing it
* burying the body in an appropriate sacred space
* make sacrifices to help the dead spirit attain peace
* ***HISTORICAL TRAUMA of colonialism shapes suspicions of outsiders***
* ppl in West Africa NOT ONLY fear their ancestors’ wrath but ALSO their collective memory of the slave trade, colonialism, and the initial culturally insensitive behvaior by Ebola treatment professionals all inform their sense that White & Muslim Outsiders are DANGERS
\
CASE STUDY of anthropological research: global conflicts over containing Ebola in West Africa:
* local govt and global responses to ebola outbreak (2013-2014):
* Guinean Village where infection first identified shunned, roads & bridges cut off
* Doctors without Borders worked with Guinean govt to establish an ebola treatment unit
* govt imposed restrictions on burial and funeral rites (bc ebola found to be MOST infectious AT death AND 2-3 days before/after → specialists informing govt focused on meeting UN WHO’s “safe burial” protocol)
* local reactions to burial and funeral restrictions:
* VIOLENT clashes erupted and ebola treatment workers attacked/prevented from entering villages (including 8 members of a delegation of doctors/politicians/journalists murdered in 2014, murders of Red Cross workers, pervasive violence against treatment centers and providers)
* ***anthropology’s question: what’s at stake for these communities*** → cultural relativism informs a response based on:
* not assuming these are “irrational” or “ignorant” reactions
* instead inquire and LISTEN to people’s concerns
* anthropologists learned from the Kissi people (of Guinea’s forest region):
* social organization of everyday life
* population of \~140K ppl in region across Liberia, Guinea, and Sierra Leone
* ppl live in small self-governing villages of abt 150 ppl tucked inside groves of mango or kola trees
* most ppl are farmers (rice, manioc, cotton)
* local craftsmanship including basket weaving, iron work, and music
* cultural worldview of the Kissi people
* prosperity requires virtuous behavior (THINK: karma) - **fulfilling obligations** of youth towards elders + of the living towards the dying/ancestors
* illness and death result from moral violations (THINK: karma) - not demonstrating ongoing care and commitment to the elders or ancestors results in violation of CULTURAL belief
* Kissi social organization as a reflectance of cultural worldview
* society is organized into lineages and male/female initiation societies
* these socialize the next generation + provide structure for the living throughout the life cycle who educate youth, establish and reaffirm social hierarchy, demarcate sacred space ***(including PROPER BURIAL space)***
* initiation societies’ power over natural and social worlds and life-cycle transitions
* birth of a child = reincarnation of the village dead
* birth of an adult = initiation: land spirit swallows adolescent children & expels them as social adults
* birth of an ancestor into the village of the dead
* importance of initiation societies’ burial and funeral rituals to ensure a dead person’s birth as ancestor
* ancestor is an elevated status that must be achieved through work of descendants to properly care for their dying and dead relative
* IF descendants fail to fulfill these obligations, the dead spirit is condemned to wander eternally , will angrily torment descendants & undermine their prosperity
* aspects of proper care for descendants
* descendants must care & wash a dying person throughout his/her last days
* hear their final wishes
* help them settle outstanding debts
* show appropriate forms of grief at death
* prepare the body by washing it
* burying the body in an appropriate sacred space
* make sacrifices to help the dead spirit attain peace
* ***HISTORICAL TRAUMA of colonialism shapes suspicions of outsiders***
* ppl in West Africa NOT ONLY fear their ancestors’ wrath but ALSO their collective memory of the slave trade, colonialism, and the initial culturally insensitive behvaior by Ebola treatment professionals all inform their sense that White & Muslim Outsiders are DANGERS
5
New cards
What is cultural relativism and how does it differ from moral relativism? How is cultural relativism important to anthropological understanding of health and illness?
* Moral = no distinct right or wrong – bc there are distinct views in this world, there is no unique right or wrong
* Difference = why does raising cultural relativism not also raise moral relativism?
* Cultural = anthropological approach to research in which you’re interested to learn about different views, trying to understand how do communities look at/understand different views cultural perspective says we need to understand the ritual/value/attitude within the larger cultural values/conditions of people’s lives
* To understand cultural differences/diversity, BEGIN with cultural relevance stance (to learn through the people’s perspective and the larger context of their society) (cultural asks us to put aside our own judgement to understand what’s going on) AND KNOW THAT bc of our different views on the world, we can’t make a definitive conclusion about what is “right” or “wrong” (moral = longer term stance that says I can’t judge; anthropologists are NOT doing this – anthropologists are saying here are the reasons for this thing, but we don’t think this is a moral stance)
* Use cultural to understand then make judgements/critiques with the most complete knowledge
* Know that cultural relativism does NOT mean that it is NOT possible to EVER make moral judgements – cultural relativism provides the CONTEXT for making a sound moral judgement
\
***CULTURAL relativism:***
Cultural relativism is the idea that beliefs, values, and practices are relative to the culture in which they occur. This means that cultural practices should be understood in the context of the culture that they are a part of, rather than being judged by standards of another culture. This concept emphasizes the importance of cultural diversity and highlights the fact that what may be considered normal or acceptable in one culture may not be in another.
\
***MORAL relativism:***
On the other hand, moral relativism is the idea that moral truths are relative to the individual or the culture in which they occur. This means that there are no objective moral truths that apply to all people and all cultures. Instead, moral truths are determined by the individual or the cultural context in which they occur.
\
***How is CULTURAL relativism important to anthropology in the context of health and illness?***
In anthropology, cultural relativism is an important concept in understanding health and illness. This is because different cultures have different beliefs and practices related to health and illness. For example, some cultures may believe that illness is caused by supernatural forces or spirits, while others may believe that it is caused by physical factors such as germs or environmental factors.
By understanding cultural relativism, __anthropologists are better able to understand and respect the beliefs and practices of the cultures they study__. This can help to __prevent misunderstandings and conflicts__ that may arise from a lack of cultural understanding. Additionally, by taking a cultural relativist approach, anthropologists can gain insights into the ways in which different cultures understand and respond to health and illness, which can inform the __development of more culturally sensitive health interventions__.
* Difference = why does raising cultural relativism not also raise moral relativism?
* Cultural = anthropological approach to research in which you’re interested to learn about different views, trying to understand how do communities look at/understand different views cultural perspective says we need to understand the ritual/value/attitude within the larger cultural values/conditions of people’s lives
* To understand cultural differences/diversity, BEGIN with cultural relevance stance (to learn through the people’s perspective and the larger context of their society) (cultural asks us to put aside our own judgement to understand what’s going on) AND KNOW THAT bc of our different views on the world, we can’t make a definitive conclusion about what is “right” or “wrong” (moral = longer term stance that says I can’t judge; anthropologists are NOT doing this – anthropologists are saying here are the reasons for this thing, but we don’t think this is a moral stance)
* Use cultural to understand then make judgements/critiques with the most complete knowledge
* Know that cultural relativism does NOT mean that it is NOT possible to EVER make moral judgements – cultural relativism provides the CONTEXT for making a sound moral judgement
\
***CULTURAL relativism:***
Cultural relativism is the idea that beliefs, values, and practices are relative to the culture in which they occur. This means that cultural practices should be understood in the context of the culture that they are a part of, rather than being judged by standards of another culture. This concept emphasizes the importance of cultural diversity and highlights the fact that what may be considered normal or acceptable in one culture may not be in another.
\
***MORAL relativism:***
On the other hand, moral relativism is the idea that moral truths are relative to the individual or the culture in which they occur. This means that there are no objective moral truths that apply to all people and all cultures. Instead, moral truths are determined by the individual or the cultural context in which they occur.
\
***How is CULTURAL relativism important to anthropology in the context of health and illness?***
In anthropology, cultural relativism is an important concept in understanding health and illness. This is because different cultures have different beliefs and practices related to health and illness. For example, some cultures may believe that illness is caused by supernatural forces or spirits, while others may believe that it is caused by physical factors such as germs or environmental factors.
By understanding cultural relativism, __anthropologists are better able to understand and respect the beliefs and practices of the cultures they study__. This can help to __prevent misunderstandings and conflicts__ that may arise from a lack of cultural understanding. Additionally, by taking a cultural relativist approach, anthropologists can gain insights into the ways in which different cultures understand and respond to health and illness, which can inform the __development of more culturally sensitive health interventions__.
6
New cards
What are some tools philosophers use in their work? Describe them.
* ***arguments:***
* establishing claims (conclusions) through a series of statements (premises)
* arguments can be generated, analyzed, reconstructed
* ***theories:***
* a systematic view that accounts for a particular area or set of problems in philosophy
* ***concepts:***
* basic ideas that can be employed in theories or arguments
* establishing claims (conclusions) through a series of statements (premises)
* arguments can be generated, analyzed, reconstructed
* ***theories:***
* a systematic view that accounts for a particular area or set of problems in philosophy
* ***concepts:***
* basic ideas that can be employed in theories or arguments
7
New cards
describe characteristics of arguments according to philosophy
arguments give ***logical structure*** to writing, thinking, and speaking
* initial assertions/statements of an argument are premises
* the claim that the argument tries to justify is the conclusion
\
***validity and soundness:***
* validity applies to an argument’s logical structure - if an argument is VALID, it is impossible for its premises to be true and its conclusion to be false. An argument can be valid but NOT sound bc the premises are clearly not true
* ex: all COVID vaccines insert microchips that track the vaccinated person’s whereabouts → I received a COVID vaccine → therefore, I received a microchip that tracks my whereabouts (VALID but NOT sound argument)
* sound arguments are logically valid AND have true or at least well-supported premises
* most of the writing in an essay will be spent supporting your premises.
* initial assertions/statements of an argument are premises
* the claim that the argument tries to justify is the conclusion
\
***validity and soundness:***
* validity applies to an argument’s logical structure - if an argument is VALID, it is impossible for its premises to be true and its conclusion to be false. An argument can be valid but NOT sound bc the premises are clearly not true
* ex: all COVID vaccines insert microchips that track the vaccinated person’s whereabouts → I received a COVID vaccine → therefore, I received a microchip that tracks my whereabouts (VALID but NOT sound argument)
* sound arguments are logically valid AND have true or at least well-supported premises
* most of the writing in an essay will be spent supporting your premises.
8
New cards
philosophical moral theories
1. ***utilitarian moral theories:*** morally good actions maximize welfare for all those affected
2. ***Kantian moral theory:*** our moral duty is to act in accordance with the moral law (which we give to ourselves in virtue of our rational nature)
3. ***virtue ethics:*** ethically good actions accord with the moral virtues (such as kindness, courage, and humility), which are excellent character traits (not one-off actions) learned through HABITUATION
9
New cards
bioethics theories and approaches
1. ***principles-based approach:***
1. respect for autonomy
2. justice
3. beneficence
4. non-maleficence
5. principles are ***specified in relevant bioethical context*** and balanced against each other where there is conflict in application
2. ***casuistry:***
1. novel or perplexing moral situations are compared to “settled” moral cases through a process of reasoning by analogy
3. ***narrative:***
1. attends to voice (who is narrating), and the trajectory of the story (past, present, future), among other narrative elements to help identify moral values and solutions to ethical problems
4. ***feminist:***
1. critical approach to traditional moral theory that situates people and groups in terms of social power and oppression and lived experience
10
New cards
what is autonomy and what is an autonomous choice?
2 ways autonomy might be understood:
1. as freedom (of action and from interference)
2. as a capacity (to self-govern or order one’s life according to what one values)
1. as freedom (of action and from interference)
2. as a capacity (to self-govern or order one’s life according to what one values)
11
New cards
What are some of the tools of literary studies? Describe them.
* writers use literary studies to organize our experience into meaningful form
* readers use literary studies to become perceptive of the narratives that surround us
* humans use literary studies to understand our surprising world and our (often weird) fellow travelers
* humanists use literary studies to exercise our curiosity and imagine alternatives to what is
* readers use literary studies to become perceptive of the narratives that surround us
* humans use literary studies to understand our surprising world and our (often weird) fellow travelers
* humanists use literary studies to exercise our curiosity and imagine alternatives to what is
12
New cards
What is involved in “close reading” a text?
need to think about:
1. What kind of narrative are you about to enter? → fiction or nonfiction; genre
2. Who is speaking? → narrator; narrative point of view; focalization
3. Where are we? → setting in space and time; realistic, symbolic
4. Who is involved? → characterization; types; historical figures; roles
5. How does the story unfold? → temporality; style of narration; structure
6. What special language, rhythms, vocabulary do you observe? → figurative language; diction; allusion; syntax
7. What larger patterns and ideas arise? → themes; philosophical insights; big questions; truths
1. What kind of narrative are you about to enter? → fiction or nonfiction; genre
2. Who is speaking? → narrator; narrative point of view; focalization
3. Where are we? → setting in space and time; realistic, symbolic
4. Who is involved? → characterization; types; historical figures; roles
5. How does the story unfold? → temporality; style of narration; structure
6. What special language, rhythms, vocabulary do you observe? → figurative language; diction; allusion; syntax
7. What larger patterns and ideas arise? → themes; philosophical insights; big questions; truths
13
New cards
What is stigma and how is it important for understanding the social dynamics of pandemics?
Stigma refers to a __*negative and discriminatory attitude*__ or perception towards a particular group or individual based on certain characteristics or traits that are considered different or deviant from the norm.
\
Can take many forms, including:
* social exclusion
* labeling
* stereotyping
* discrimination
Can have a significant impact on an individual's mental and physical well-being, as well as their social and economic opportunities
\
In PANDEMICS, stigma can play a crucial role in shaping the __*social dynamics and public response*__ to the outbreak.
* When a disease is stigmatized, individuals or groups who are perceived to be associated with the disease may face discrimination, social isolation, and even violence
* example: during the early days of the COVID-19 pandemic, AAPI faced a significant amount of racism and xenophobia, as the virus was initially believed to have originated in China. This stigma not only harms individuals and communities but can also hinder efforts to control the spread of the disease by discouraging people from seeking medical help or adhering to public health guidelines
Therefore, it is crucial to understand the role of stigma in shaping public attitudes and behavior during pandemics.
\
ALSO __*psychologically wanting to maintain a sense of normalcy is not necessarily part of stigma in pandemics, but it can contribute to the PERPETUATION of stigma*__ IF it leads to the denial or downplaying of the seriousness of the situation or the stigmatization of affected individuals or groups. During a pandemic, people may want to maintain a sense of normalcy to cope with the uncertainty and fear caused by the outbreak. This can manifest in behaviors such as downplaying the risk of infection, ignoring public health guidelines, or blaming others for the spread of the disease. These behaviors can contribute to the stigmatization of affected individuals or groups, such as people who have contracted the disease or belong to a certain ethnic or religious group.
\
Can take many forms, including:
* social exclusion
* labeling
* stereotyping
* discrimination
Can have a significant impact on an individual's mental and physical well-being, as well as their social and economic opportunities
\
In PANDEMICS, stigma can play a crucial role in shaping the __*social dynamics and public response*__ to the outbreak.
* When a disease is stigmatized, individuals or groups who are perceived to be associated with the disease may face discrimination, social isolation, and even violence
* example: during the early days of the COVID-19 pandemic, AAPI faced a significant amount of racism and xenophobia, as the virus was initially believed to have originated in China. This stigma not only harms individuals and communities but can also hinder efforts to control the spread of the disease by discouraging people from seeking medical help or adhering to public health guidelines
Therefore, it is crucial to understand the role of stigma in shaping public attitudes and behavior during pandemics.
\
ALSO __*psychologically wanting to maintain a sense of normalcy is not necessarily part of stigma in pandemics, but it can contribute to the PERPETUATION of stigma*__ IF it leads to the denial or downplaying of the seriousness of the situation or the stigmatization of affected individuals or groups. During a pandemic, people may want to maintain a sense of normalcy to cope with the uncertainty and fear caused by the outbreak. This can manifest in behaviors such as downplaying the risk of infection, ignoring public health guidelines, or blaming others for the spread of the disease. These behaviors can contribute to the stigmatization of affected individuals or groups, such as people who have contracted the disease or belong to a certain ethnic or religious group.
14
New cards
Who are the main characters of *The Plague*? Are there women characters? Explain.
Main characters of *The Plague*:
1. ==Dr. Bernard Rieux: physician, narrator==
2. ==Jean Tarrou: visitor to Oran, keeper of a diary==
3. ==Raymond Rambert: journalist==
4. ==Father Paneloux: Jesuit priest==
5. M. Othon: conservative magistrate (judge)
6. The Prefect: head medical administrator
7. Dr. Richard: chair of medical association
8. Joseph Grand: civil servant, statisticain, “novelist”
9. Dr. Castel: maker of the serum
10. Cottard: suicidal, criminal of some sort
11. Jacques Othon: son of M. Othon
12. Asthma patient
13. Madame Rieux: mother, wife to Dr. Rieux
\
women are the ones LOOKING AFTER the plague victims → this is why we have no documented SUFFERING of ppl bc the novel’s narrator says it will ONLY use documented understanding by Dr. RIEUX - Bernard Rieux offers *numbers/medical commission* → we as the readers see the problems with the health bureaucracy (they misinterpret the suffering and thus don’t act suddenly, causing shortage of the cream necessary for doctors to treat patients)
\
There are several women characters in the novel, although they are not as prominent as the male characters. They include:
1. Madame Rieux: the wife of Dr. Rieux, described as a supportive and caring spouse
2. Castel’s wife: the wife of another physician who is instrumental in developing a serum to treat the disease
3. the Spanish dancer: She is a woman who is infected with the disease and dies in the quarantine camp.
While the female characters in The Plague are not as prominent as the male characters, they still play important roles in the story. The novel portrays the outbreak of the disease as a crisis that affects all members of society, regardless of gender or social status.
1. ==Dr. Bernard Rieux: physician, narrator==
2. ==Jean Tarrou: visitor to Oran, keeper of a diary==
3. ==Raymond Rambert: journalist==
4. ==Father Paneloux: Jesuit priest==
5. M. Othon: conservative magistrate (judge)
6. The Prefect: head medical administrator
7. Dr. Richard: chair of medical association
8. Joseph Grand: civil servant, statisticain, “novelist”
9. Dr. Castel: maker of the serum
10. Cottard: suicidal, criminal of some sort
11. Jacques Othon: son of M. Othon
12. Asthma patient
13. Madame Rieux: mother, wife to Dr. Rieux
\
women are the ones LOOKING AFTER the plague victims → this is why we have no documented SUFFERING of ppl bc the novel’s narrator says it will ONLY use documented understanding by Dr. RIEUX - Bernard Rieux offers *numbers/medical commission* → we as the readers see the problems with the health bureaucracy (they misinterpret the suffering and thus don’t act suddenly, causing shortage of the cream necessary for doctors to treat patients)
\
There are several women characters in the novel, although they are not as prominent as the male characters. They include:
1. Madame Rieux: the wife of Dr. Rieux, described as a supportive and caring spouse
2. Castel’s wife: the wife of another physician who is instrumental in developing a serum to treat the disease
3. the Spanish dancer: She is a woman who is infected with the disease and dies in the quarantine camp.
While the female characters in The Plague are not as prominent as the male characters, they still play important roles in the story. The novel portrays the outbreak of the disease as a crisis that affects all members of society, regardless of gender or social status.

15
New cards
describe Dr. Bernard Rieux from *The Plague*
* narrator and protagonist of *The Plague*
* one of the first people in Oran to urge that stringent sanitation measures be taken to fight the rising epidemic
* staunch humanist and atheist → has little patience with the authorities' slow response to his call for action
* actions and personality imply that he believes in a personal as well as a social code of ethics
* when Oran is placed under quarantine, Dr. Rieux continues to fight the plague despite the signs that his efforts make little or no difference
* separated from his wife but does not allow his personal distress to distract him from his battle to relieve the collective social suffering wrought on the confused and terrified population of Oran
* one of the first people in Oran to urge that stringent sanitation measures be taken to fight the rising epidemic
* staunch humanist and atheist → has little patience with the authorities' slow response to his call for action
* actions and personality imply that he believes in a personal as well as a social code of ethics
* when Oran is placed under quarantine, Dr. Rieux continues to fight the plague despite the signs that his efforts make little or no difference
* separated from his wife but does not allow his personal distress to distract him from his battle to relieve the collective social suffering wrought on the confused and terrified population of Oran
16
New cards
describe Jean Tarrou from *The Plague*
* author of the account that Dr. Rieux uses to give greater texture to his chronicle of the plague
* vacationing in Oran when the epidemic requires a total quarantine of the city. As an outsider, his observations on Oran society are more objective than those of a citizen of the city
* beliefs about personal and social responsibility are remarkably similar to those of Dr. Rieux, but Tarrou is far more philosophical
* does not believe in God, so he does not believe in the illusion of an intrinsic rational and moral meaning in death, suffering, and human existence. For him, human existence gains meaning only when people choose freely to participate in the losing, but noble struggle against death and suffering
* contributes to the anti-plague effort in accordance with his code of ethics
* vacationing in Oran when the epidemic requires a total quarantine of the city. As an outsider, his observations on Oran society are more objective than those of a citizen of the city
* beliefs about personal and social responsibility are remarkably similar to those of Dr. Rieux, but Tarrou is far more philosophical
* does not believe in God, so he does not believe in the illusion of an intrinsic rational and moral meaning in death, suffering, and human existence. For him, human existence gains meaning only when people choose freely to participate in the losing, but noble struggle against death and suffering
* contributes to the anti-plague effort in accordance with his code of ethics
17
New cards
describe Joseph Grande from *The Plague*
* elderly civil servant in Oran.
* when he accepted his job as a young man, he was promised the opportunity for promotion, but, over the years, he never actively pursued it. Therefore, he remained in the same job for decades
* his marriage also settled into a daily humdrum. Eventually, Grand's wife Jeanne tired of the monotonous routine and left him.
* Over the years, Grand has tried to write her a letter, but he suffers from an intense anxiety over finding the "right words" to express himself. This anxiety also hinders his literary pursuit. Grand is trying to write a book, but he wants to create the perfect manuscript, so he has never gotten beyond the opening line
* when he accepted his job as a young man, he was promised the opportunity for promotion, but, over the years, he never actively pursued it. Therefore, he remained in the same job for decades
* his marriage also settled into a daily humdrum. Eventually, Grand's wife Jeanne tired of the monotonous routine and left him.
* Over the years, Grand has tried to write her a letter, but he suffers from an intense anxiety over finding the "right words" to express himself. This anxiety also hinders his literary pursuit. Grand is trying to write a book, but he wants to create the perfect manuscript, so he has never gotten beyond the opening line
18
New cards
describe Raymond Rambert from *The Plague*
* a journalist from Paris
* comes to Oran to research the sanitary conditions in the Arab population, but the sudden, unexpected total quarantine of Oran traps him in the city
* desperately struggles to find some method of escape from Oran to rejoin his wife in Paris
* comes to Oran to research the sanitary conditions in the Arab population, but the sudden, unexpected total quarantine of Oran traps him in the city
* desperately struggles to find some method of escape from Oran to rejoin his wife in Paris
19
New cards
describe Cottard from *The Plague*
* suspicious and paranoid
* in the past, he committed a crime that he does not name, so he constantly fears arrest and punishment
* when Oran falls under total quarantine, Cottard is happy because he no longer feels alone in his state of constant fear. Moreover, the plague occupies the authorities entirely, so he does not fear arrest
* he engages in the profitable smuggling trade during the epidemic and eschews all responsibility to help fight the disease
* in the past, he committed a crime that he does not name, so he constantly fears arrest and punishment
* when Oran falls under total quarantine, Cottard is happy because he no longer feels alone in his state of constant fear. Moreover, the plague occupies the authorities entirely, so he does not fear arrest
* he engages in the profitable smuggling trade during the epidemic and eschews all responsibility to help fight the disease
20
New cards
describe Father Paneloux from *The Plague*
* a Jesuit priest in Oran
* early during the epidemic, he delivers a sermon to his confused, frightened congregation declaring that the plague is a God-sent punishment for their sins. As the plague rages on, he modifies this stance, seeing the Plague as a supreme test of faith → __*shows that religion/faith is not a complete explanation for the absurd*__ (major theme of the novel)
* early during the epidemic, he delivers a sermon to his confused, frightened congregation declaring that the plague is a God-sent punishment for their sins. As the plague rages on, he modifies this stance, seeing the Plague as a supreme test of faith → __*shows that religion/faith is not a complete explanation for the absurd*__ (major theme of the novel)
21
New cards
What are two examples of insights anthropologists gain from studying the “everyday” lives of people in diverse cultures?
1. ***Understanding social norms and values:*** Anthropologists can gain insight into the social norms and values of a culture by studying the everyday behaviors and practices of its members. For instance, by observing how people interact with each other, what they eat, how they dress, and what they consider important in their daily lives, anthropologists can gain a deeper understanding of the values that shape that culture.
\
2. ***Examining power dynamics:*** Anthropologists can also gain insight into power dynamics by examining the everyday lives of people in diverse cultures. By studying how people negotiate relationships, how they resolve conflicts, and how they assert their individuality, anthropologists can gain a deeper understanding of how power operates in different contexts. For instance, by observing how gender roles are constructed and maintained in a particular culture, anthropologists can gain insights into the ways that power is distributed between men and women.
22
New cards
In *The Journal of the Plague Year*, there was uncertainty about how the disease spread. How did __stories__ about the plague spread? Name three different ways that people learned about the plague, according to Daniel Defoe.
5 kinds of stories are mentioned in Defoe:
1. ordinary discourse
2. printed newspapers
3. letteres
4. word of mouth
5. government’s “true account”
\
*How did these stories of the plague spread?*
1. ***Rumors and hearsay:*** According to Defoe, rumors and hearsay were a common way that people learned about the plague. People would pass on stories about the disease, often embellishing them in the process. These stories could be spread by word of mouth, or by letters sent from one city to another.
2. ***Official proclamations:*** Another way that people learned about the plague was through official proclamations from the government. The authorities would issue orders and regulations about how to deal with the disease, which would be posted in public places such as churches and marketplaces. These proclamations were often read out loud by town criers.
3. ***Personal experience:*** Finally, people learned about the plague through their own personal experience. Many people saw the symptoms of the disease firsthand, either in themselves or in their family members and neighbors. They might also witness the effects of the disease on the streets of their city, seeing the bodies of plague victims being carried away or buried in mass graves.
1. ordinary discourse
2. printed newspapers
3. letteres
4. word of mouth
5. government’s “true account”
\
*How did these stories of the plague spread?*
1. ***Rumors and hearsay:*** According to Defoe, rumors and hearsay were a common way that people learned about the plague. People would pass on stories about the disease, often embellishing them in the process. These stories could be spread by word of mouth, or by letters sent from one city to another.
2. ***Official proclamations:*** Another way that people learned about the plague was through official proclamations from the government. The authorities would issue orders and regulations about how to deal with the disease, which would be posted in public places such as churches and marketplaces. These proclamations were often read out loud by town criers.
3. ***Personal experience:*** Finally, people learned about the plague through their own personal experience. Many people saw the symptoms of the disease firsthand, either in themselves or in their family members and neighbors. They might also witness the effects of the disease on the streets of their city, seeing the bodies of plague victims being carried away or buried in mass graves.
23
New cards
how to represent a plague?
***tools to use/questions to think about:***
1. __*rumors*__: which rumor is true?
2. __*testimony*__: who do you believe?
3. __*symptoms/physicians*__: is this a singular/isolated event or something much larger?
4. __*books/wives tales*__: these spread terror/fear
5. __*government*__: are they concealing things?
6. __*HEALTH BUREAUCRACY*__*:* NEW mode of representation, thinking of ppl not as individuals but as a population (thinking of plague in terms of population, maps, and statistics)
\
***HOW?*** Take the numbers → create a map that is dependent NOT on anyone’s individual story but the story of a POPULATION → this becomes a story of PUBLIC health
* Maps as a form of representation are essential to POPULATION-level systems of connection
* A huge part of what is going on in Oran is *shipping* used to connect the disparate lands → Oran is a PORT city (in Algeria)
* Public health (use of stats + mapping) becomes a new way to tell a story
1. __*rumors*__: which rumor is true?
2. __*testimony*__: who do you believe?
3. __*symptoms/physicians*__: is this a singular/isolated event or something much larger?
4. __*books/wives tales*__: these spread terror/fear
5. __*government*__: are they concealing things?
6. __*HEALTH BUREAUCRACY*__*:* NEW mode of representation, thinking of ppl not as individuals but as a population (thinking of plague in terms of population, maps, and statistics)
\
***HOW?*** Take the numbers → create a map that is dependent NOT on anyone’s individual story but the story of a POPULATION → this becomes a story of PUBLIC health
* Maps as a form of representation are essential to POPULATION-level systems of connection
* A huge part of what is going on in Oran is *shipping* used to connect the disparate lands → Oran is a PORT city (in Algeria)
* Public health (use of stats + mapping) becomes a new way to tell a story
24
New cards
How does Camus’ description of everyday life in Oran in *The Plague* help us to understand some of the social effects of epidemics? Give two examples.
People lived selfishly in mundane ways and were relatively boring and monotonous and then compared it with the selfishness those people were feeling during the actual plague itself showed how people were not actually changing during the plague
\
*The Plague* provides a vivid description of everyday life in a city struck by an epidemic:
1. ***Loss of social connections:*** novel portrays how the spread of the disease disrupts the social fabric of the community.
1. the strict quarantine measures force people to isolate themselves from one another, and social gatherings and events are cancelled
2. in Oran, people are unable to visit friends and family members who are sick or attend funerals of those who have died
3. the disease creates a sense of isolation and loneliness, causing people to feel disconnected from their usual support networks
2. ***Heightened fear and suspicion:*** novel also highlights how epidemics can heighten feelings of fear and suspicion among people
1. as the disease spreads, fear and paranoia grow
2. people start to view each other with suspicion and distrust, and there is a breakdown in trust between neighbors and even family members.
3. this is reflected in the novel through the increasing reports of looting, hoarding, and other forms of anti-social behavior
\
*The Plague* provides a vivid description of everyday life in a city struck by an epidemic:
1. ***Loss of social connections:*** novel portrays how the spread of the disease disrupts the social fabric of the community.
1. the strict quarantine measures force people to isolate themselves from one another, and social gatherings and events are cancelled
2. in Oran, people are unable to visit friends and family members who are sick or attend funerals of those who have died
3. the disease creates a sense of isolation and loneliness, causing people to feel disconnected from their usual support networks
2. ***Heightened fear and suspicion:*** novel also highlights how epidemics can heighten feelings of fear and suspicion among people
1. as the disease spreads, fear and paranoia grow
2. people start to view each other with suspicion and distrust, and there is a breakdown in trust between neighbors and even family members.
3. this is reflected in the novel through the increasing reports of looting, hoarding, and other forms of anti-social behavior
25
New cards
In *The Plague*, why does Dr. Rieux tirelessly care for plague victims? Does Dr. Rieux spend a lot of time worried about being infected by caring for plague patients? Use evidence from your understanding of the novel.
Why does Rieux tirelessly care for plague victims?
* Utilitarian / virtue ethics - one physician in a city without many other physicians, feels obligated to help
* His wife was sick for most of the time and there was a very good chance that she wasn’t coming back - psychologically there’s not much left for Rieux if she doesn’t come back so might as well help
* Rieux felt that everyone had little-to-no choice but to concern themselves with fighting the plague
\
Rieux tirelessly cares for plague victims because he believes __*it is his duty as a doctor to do so*__. He understands that he has a responsibility to his patients and the community, and he does not want to abandon them during a crisis. He sees himself as a public servant and feels compelled to do everything in his power to fight the spread of the plague.
* "All I maintain is that on this earth there are pestilences and there are victims, and it's up to us, so far as possible, not to join forces with the pestilences" (102). This quote demonstrates his belief that he has a responsibility to fight against the plague, even though it is a difficult and dangerous task
\
Dr. Rieux DOES spend time worried about being infected by caring for plague patients, but he tries to put his fears aside in order to do his job. He takes precautions to protect himself, such as wearing a mask and gloves, but he does not let his fear prevent him from caring for his patients.
* "I have no idea what the future will hold, but I know that I'll do my duty, whatever happens" (123). This quote demonstrates Dr. Rieux's dedication to his patients, even in the face of uncertainty and danger
\
His tireless care for plague victims is __*motivated by his sense of duty and responsibility as a doctor*__. He is aware of the risks involved in caring for patients with a highly contagious disease, but he puts his fears aside and does his job to the best of his ability
* Utilitarian / virtue ethics - one physician in a city without many other physicians, feels obligated to help
* His wife was sick for most of the time and there was a very good chance that she wasn’t coming back - psychologically there’s not much left for Rieux if she doesn’t come back so might as well help
* Rieux felt that everyone had little-to-no choice but to concern themselves with fighting the plague
\
Rieux tirelessly cares for plague victims because he believes __*it is his duty as a doctor to do so*__. He understands that he has a responsibility to his patients and the community, and he does not want to abandon them during a crisis. He sees himself as a public servant and feels compelled to do everything in his power to fight the spread of the plague.
* "All I maintain is that on this earth there are pestilences and there are victims, and it's up to us, so far as possible, not to join forces with the pestilences" (102). This quote demonstrates his belief that he has a responsibility to fight against the plague, even though it is a difficult and dangerous task
\
Dr. Rieux DOES spend time worried about being infected by caring for plague patients, but he tries to put his fears aside in order to do his job. He takes precautions to protect himself, such as wearing a mask and gloves, but he does not let his fear prevent him from caring for his patients.
* "I have no idea what the future will hold, but I know that I'll do my duty, whatever happens" (123). This quote demonstrates Dr. Rieux's dedication to his patients, even in the face of uncertainty and danger
\
His tireless care for plague victims is __*motivated by his sense of duty and responsibility as a doctor*__. He is aware of the risks involved in caring for patients with a highly contagious disease, but he puts his fears aside and does his job to the best of his ability
26
New cards
How are the concepts of social transformation and continuity important to the study of pandemics and epidemics? Give an example.
The concepts of social transformation and continuity are crucial to the study of pandemics and epidemics because they help to understand how societies respond and adapt to these crises. __*Pandemics and epidemics can cause significant social changes, but they can also reveal pre-existing social structures and inequalities*__.
* Social transformation refers to significant changes in social norms, values, behaviors, and institutions. During pandemics and epidemics, social transformation can occur at different levels, such as individual, community, national, and global levels.
* ex: the COVID-19 pandemic has led to significant changes in social behavior, such as physical distancing, wearing masks, and working from home. These changes have transformed the way people interact and work, and they may have long-term effects on social norms and institutions.
* Continuity, on the other hand, refers to the persistence of social structures and practices over time. Pandemics and epidemics can reveal pre-existing social inequalities and vulnerabilities that may persist even after the crisis is over.
* ex: the COVID-19 pandemic has disproportionately affected vulnerable populations, such as low-income communities, racial and ethnic minorities, and older adults. These disparities reflect pre-existing social structures and inequalities, such as inadequate access to healthcare, housing, and employment opportunities.
THUS, studying social transformation and continuity during pandemics and epidemics can provide insights into the complex interactions between social structures and crises. __*By understanding how societies adapt and transform in response to these crises, researchers and policymakers can develop strategies to mitigate the negative effects of pandemics and epidemics and promote social resilience and equity*__.
* Social transformation refers to significant changes in social norms, values, behaviors, and institutions. During pandemics and epidemics, social transformation can occur at different levels, such as individual, community, national, and global levels.
* ex: the COVID-19 pandemic has led to significant changes in social behavior, such as physical distancing, wearing masks, and working from home. These changes have transformed the way people interact and work, and they may have long-term effects on social norms and institutions.
* Continuity, on the other hand, refers to the persistence of social structures and practices over time. Pandemics and epidemics can reveal pre-existing social inequalities and vulnerabilities that may persist even after the crisis is over.
* ex: the COVID-19 pandemic has disproportionately affected vulnerable populations, such as low-income communities, racial and ethnic minorities, and older adults. These disparities reflect pre-existing social structures and inequalities, such as inadequate access to healthcare, housing, and employment opportunities.
THUS, studying social transformation and continuity during pandemics and epidemics can provide insights into the complex interactions between social structures and crises. __*By understanding how societies adapt and transform in response to these crises, researchers and policymakers can develop strategies to mitigate the negative effects of pandemics and epidemics and promote social resilience and equity*__.
27
New cards
What is a common rationale given for why health care providers should care for patients even if doing so puts them at risk? What is a critique of this rationale? What other rationales are available for understanding why health care providers should undertake care of patients even when doing so puts them at risk?
***Tomlinson’s view:***
* A social contract requiring physicians care for patients when doing so poses risk is either between society and individual physicians or society and the profession.
* If it is between society and the profession, then only some physicians have a duty to such care.
* If it is between society and individuals, then every physician has a duty to such care.
* It is not plausible that every physician has agreed to care for patients when doing so poses risk.
* \[Physicians can only enter into social contracts by explicit agreement\]
* \[therefore, any social contract requiring physicians care for patients when doing so poses risk must be between society and the profession.\]Therefore, \[at most, IF there is such a social contract\] only some physicians have a duty to care for patients when doing so poses risk
\
***the language of “duty” in ethics:***
* What we are allowed to do, what we must do, and what we must not do
* Duty sets a minimal standard of conduct: what we must do
* Permissible acts: what we may do
* Prohibited acts: what we must not do
* Supererogatory acts: good acts above and beyond the call of duty (“virtuous”, but virtues of character are not determined by ‘one off’ actions, but are reliable modes of response from the practically wise person)
\
***the language of “virtue” in ethics:***
* Virtue-based ethics evaluates morality in terms of reliable traits of character and our shared human goals of living well
* Virtues: Excellence human traits of character (the practically wise acts for the right reasons, in the right way, toward the right end, and with respect to the right individuals)
* Vices: bad human traits – those who fail to both properly understand what is good and act against it. Typically each virtue has a vice at either extreme (i.e. courage is the virtue; the vices are cowardice and rashness).
* “Continent”: Acting as one should but not for the right reasons/motivation (duty would be consistent with continence)
* “Incontinent”: Knows what is right to do, but doesn’t do so
\
One common rationale given for why healthcare providers should care for patients even if doing so puts them at risk is the principle of beneficence, which is the __*ethical obligation to do good and promote the well-being of patients*__. Healthcare providers are trained to prioritize the needs of their patients and to act in their best interests, even if it means putting themselves at risk. In this view, the potential harm to the healthcare provider is outweighed by the benefit to the patient, and therefore it is their duty to provide care.
A critique of this rationale is that it __*may be too idealistic and unrealistic in practice, particularly during a pandemic or other public health crisis when healthcare providers may be overworked, under-resourced, and facing personal risks such as contracting a contagious disease*__. Some argue that the principle of beneficence should be balanced with the principle of non-maleficence, which is the ethical obligation to do no harm. This means that healthcare providers should not be asked to take on undue risks that may harm themselves or their loved ones, and that efforts should be made to minimize their exposure to infectious diseases.
Other rationales for understanding why healthcare providers should undertake care of patients even when doing so puts them at risk include the __*principle of justice, which is the ethical obligation to treat all patients fairly and equally*__. In this view, healthcare providers have a duty to provide care to those who need it regardless of their personal risks, because denying care to certain patients based on those risks would be unjust and discriminatory.
Another rationale is the __*social contract between healthcare providers and society*__, in which healthcare providers agree to provide care in exchange for certain benefits and protections from society. In this view, healthcare providers have a duty to fulfill their obligations to society even during times of crisis, because society provides them with the resources and support necessary to provide care.
Ultimately, the decision to provide care to patients even when doing so puts healthcare providers at risk is a complex and multifaceted issue that requires consideration of ethical principles, practical realities, and social obligations.
* A social contract requiring physicians care for patients when doing so poses risk is either between society and individual physicians or society and the profession.
* If it is between society and the profession, then only some physicians have a duty to such care.
* If it is between society and individuals, then every physician has a duty to such care.
* It is not plausible that every physician has agreed to care for patients when doing so poses risk.
* \[Physicians can only enter into social contracts by explicit agreement\]
* \[therefore, any social contract requiring physicians care for patients when doing so poses risk must be between society and the profession.\]Therefore, \[at most, IF there is such a social contract\] only some physicians have a duty to care for patients when doing so poses risk
\
***the language of “duty” in ethics:***
* What we are allowed to do, what we must do, and what we must not do
* Duty sets a minimal standard of conduct: what we must do
* Permissible acts: what we may do
* Prohibited acts: what we must not do
* Supererogatory acts: good acts above and beyond the call of duty (“virtuous”, but virtues of character are not determined by ‘one off’ actions, but are reliable modes of response from the practically wise person)
\
***the language of “virtue” in ethics:***
* Virtue-based ethics evaluates morality in terms of reliable traits of character and our shared human goals of living well
* Virtues: Excellence human traits of character (the practically wise acts for the right reasons, in the right way, toward the right end, and with respect to the right individuals)
* Vices: bad human traits – those who fail to both properly understand what is good and act against it. Typically each virtue has a vice at either extreme (i.e. courage is the virtue; the vices are cowardice and rashness).
* “Continent”: Acting as one should but not for the right reasons/motivation (duty would be consistent with continence)
* “Incontinent”: Knows what is right to do, but doesn’t do so
\
One common rationale given for why healthcare providers should care for patients even if doing so puts them at risk is the principle of beneficence, which is the __*ethical obligation to do good and promote the well-being of patients*__. Healthcare providers are trained to prioritize the needs of their patients and to act in their best interests, even if it means putting themselves at risk. In this view, the potential harm to the healthcare provider is outweighed by the benefit to the patient, and therefore it is their duty to provide care.
A critique of this rationale is that it __*may be too idealistic and unrealistic in practice, particularly during a pandemic or other public health crisis when healthcare providers may be overworked, under-resourced, and facing personal risks such as contracting a contagious disease*__. Some argue that the principle of beneficence should be balanced with the principle of non-maleficence, which is the ethical obligation to do no harm. This means that healthcare providers should not be asked to take on undue risks that may harm themselves or their loved ones, and that efforts should be made to minimize their exposure to infectious diseases.
Other rationales for understanding why healthcare providers should undertake care of patients even when doing so puts them at risk include the __*principle of justice, which is the ethical obligation to treat all patients fairly and equally*__. In this view, healthcare providers have a duty to provide care to those who need it regardless of their personal risks, because denying care to certain patients based on those risks would be unjust and discriminatory.
Another rationale is the __*social contract between healthcare providers and society*__, in which healthcare providers agree to provide care in exchange for certain benefits and protections from society. In this view, healthcare providers have a duty to fulfill their obligations to society even during times of crisis, because society provides them with the resources and support necessary to provide care.
Ultimately, the decision to provide care to patients even when doing so puts healthcare providers at risk is a complex and multifaceted issue that requires consideration of ethical principles, practical realities, and social obligations.
28
New cards
Should the Hippocratic Oath still guide medical practice? Give two reasons why or why not?
the Hippocratic Oath is a widely-known and ancient code of ethics for healthcare professionals, which originated in ancient Greece. It contains principles and values that guide the conduct of medical practitioners, including confidentiality, respect for life, and honesty. The question of whether the Hippocratic Oath should still guide medical practice is a complex one and has been debated for a long time.
\
__Reasons why the Hippocratic Oath SHOULD still guide medical practice:__
1. ***provides a moral compass:*** reminds healthcare professionals of their obligation to prioritize their patients' welfare and maintain ethical standards. It promotes compassion, integrity, and the idea that medical practitioners should do no harm. This ethical framework ensures that the doctor-patient relationship remains one of trust, respect, and mutual understanding.
2. ***relevant in contemporary medicine:*** while the Hippocratic Oath was written centuries ago, its principles and values remain relevant in modern healthcare. For instance, the obligation to maintain confidentiality is more important than ever in an era where data privacy is a significant concern. Similarly, the principle of informed consent is critical in today's patient-centered healthcare system.
\
__Reasons why the Hippocratic Oath should NOT guide medical practice:__
1. ***outdated:*** the Hippocratic Oath was written in a different era, and some of its provisions are no longer applicable to modern medicine. For example, the original oath forbids physicians from performing abortions or euthanasia, which are now legal in some countries. Some critics argue that the oath is not adaptable enough to the rapidly changing field of medicine.
2. ***it is not comprehensive enough:*** cannot address all the ethical issues that arise in modern healthcare. While it covers important principles such as confidentiality, respect for life, and honesty, it does not address issues such as resource allocation, conflicts of interest, and social justice. Critics argue that a more robust and comprehensive ethical framework is necessary to guide medical practice today.
\
THUS the Hippocratic Oath is still relevant in modern medicine, and its principles and values should continue to guide medical practice. However, it should be viewed as a starting point and not as the final word on medical ethics. As healthcare continues to evolve, healthcare professionals need to adapt and adopt a more comprehensive ethical framework that addresses the emerging ethical issues in healthcare.
\
__Reasons why the Hippocratic Oath SHOULD still guide medical practice:__
1. ***provides a moral compass:*** reminds healthcare professionals of their obligation to prioritize their patients' welfare and maintain ethical standards. It promotes compassion, integrity, and the idea that medical practitioners should do no harm. This ethical framework ensures that the doctor-patient relationship remains one of trust, respect, and mutual understanding.
2. ***relevant in contemporary medicine:*** while the Hippocratic Oath was written centuries ago, its principles and values remain relevant in modern healthcare. For instance, the obligation to maintain confidentiality is more important than ever in an era where data privacy is a significant concern. Similarly, the principle of informed consent is critical in today's patient-centered healthcare system.
\
__Reasons why the Hippocratic Oath should NOT guide medical practice:__
1. ***outdated:*** the Hippocratic Oath was written in a different era, and some of its provisions are no longer applicable to modern medicine. For example, the original oath forbids physicians from performing abortions or euthanasia, which are now legal in some countries. Some critics argue that the oath is not adaptable enough to the rapidly changing field of medicine.
2. ***it is not comprehensive enough:*** cannot address all the ethical issues that arise in modern healthcare. While it covers important principles such as confidentiality, respect for life, and honesty, it does not address issues such as resource allocation, conflicts of interest, and social justice. Critics argue that a more robust and comprehensive ethical framework is necessary to guide medical practice today.
\
THUS the Hippocratic Oath is still relevant in modern medicine, and its principles and values should continue to guide medical practice. However, it should be viewed as a starting point and not as the final word on medical ethics. As healthcare continues to evolve, healthcare professionals need to adapt and adopt a more comprehensive ethical framework that addresses the emerging ethical issues in healthcare.
29
New cards
What is the concept of moral status and why is it important for the one health movement?
“If an entity has moral status…we are morally obliged to give weight in our deliberations to its needs, interests, or well-being…not merely because protecting it may benefit ourselves or other persons, but because its needs have moral importance in their own right.”
\
The concept of moral status refers to the degree to which an individual or entity deserves moral consideration and respect. In other words, it's the degree to which something or someone has inherent value or worth that ought to be considered when making ethical decisions.
\
Moral status is important for the One Health movement because it __*involves the recognition of the intrinsic value of all living beings and ecosystems, and the interdependence of human, animal, and environmental health*__. One Health is a holistic approach that recognizes the interconnectedness of all living beings and their environments, and seeks to promote the health and wellbeing of all. In this context, moral status is important because it helps us to __*recognize and respect the intrinsic value and rights of animals and the environment, as well as the impact of our actions on their health and wellbeing*__. By recognizing the moral status of all living beings and ecosystems, we can make more informed and ethical decisions that promote the health and wellbeing of all, and create a more sustainable and just world for future generations.
\
The concept of moral status refers to the degree to which an individual or entity deserves moral consideration and respect. In other words, it's the degree to which something or someone has inherent value or worth that ought to be considered when making ethical decisions.
\
Moral status is important for the One Health movement because it __*involves the recognition of the intrinsic value of all living beings and ecosystems, and the interdependence of human, animal, and environmental health*__. One Health is a holistic approach that recognizes the interconnectedness of all living beings and their environments, and seeks to promote the health and wellbeing of all. In this context, moral status is important because it helps us to __*recognize and respect the intrinsic value and rights of animals and the environment, as well as the impact of our actions on their health and wellbeing*__. By recognizing the moral status of all living beings and ecosystems, we can make more informed and ethical decisions that promote the health and wellbeing of all, and create a more sustainable and just world for future generations.
30
New cards
Explain two different ways philosophers have tried to ground (or provide a basis for) attributing moral status.
* The capacity for rational autonomy (Kant)
* The ability to experience pleasures and pains (Peter Singer)
* Being a subject-of-a-life (Tom Regan)
* Being a living organism (Albert Schweitzer)
* Capacity for being in a caring relationship (Nel Noddings)
\
*There is no set of properties (of this sort) for moral status that captures all and only humans. If the “bar” for moral status is set high, many humans will fall below it, and if the “bar” is set low many nonhuman animals will rise above it.*
* The ability to experience pleasures and pains (Peter Singer)
* Being a subject-of-a-life (Tom Regan)
* Being a living organism (Albert Schweitzer)
* Capacity for being in a caring relationship (Nel Noddings)
\
*There is no set of properties (of this sort) for moral status that captures all and only humans. If the “bar” for moral status is set high, many humans will fall below it, and if the “bar” is set low many nonhuman animals will rise above it.*
31
New cards
What might be one problem with claiming that only human beings have moral status?
One problem with claiming that only human beings have moral status is that it is anthropocentric, meaning it __*prioritizes human interests and perspectives above all other forms of life on Earth*__. This view is often based on the assumption that humans are inherently more valuable than non-human animals or other forms of life, and therefore have greater moral standing.
\
However, this assumption has been __*challenged by many ethicists and environmentalists who argue that ALL forms of life have inherent value and deserve moral consideration*__. They point out that many non-human animals exhibit complex cognitive and emotional capacities, such as the ability to experience pain, pleasure, and suffering, as well as social and communicative behaviors that suggest a degree of self-awareness and moral agency.
\
Furthermore, many environmental problems, such as climate change and habitat destruction, are caused by human activities and have devastating consequences for non-human species and ecosystems. Therefore, it is important to consider the moral status of all forms of life and recognize our responsibility to protect and preserve the natural world for the benefit of all living beings.
\
However, this assumption has been __*challenged by many ethicists and environmentalists who argue that ALL forms of life have inherent value and deserve moral consideration*__. They point out that many non-human animals exhibit complex cognitive and emotional capacities, such as the ability to experience pain, pleasure, and suffering, as well as social and communicative behaviors that suggest a degree of self-awareness and moral agency.
\
Furthermore, many environmental problems, such as climate change and habitat destruction, are caused by human activities and have devastating consequences for non-human species and ecosystems. Therefore, it is important to consider the moral status of all forms of life and recognize our responsibility to protect and preserve the natural world for the benefit of all living beings.
32
New cards
Explain the questions and analytical framework of political ecology.
***defining political ecology:***
* the study of how political institutions and economic systems influence each other
* the roles of the state, classes, corporations in determining resource allocation, establishing & controlling profitability
\
political ecology has a critical focus on SYSTEMS that enable and expand inequality + exploitation
\
***analytical framework of political ecology:***
* examines relationships among politics, economics, and nature
* researchers advocate fundamental changes in the management of nature and the rights of people, directly or indirectly working with state and non-governmental organizations (NGOs) to challenge current conditions
* the study of how political institutions and economic systems influence each other
* the roles of the state, classes, corporations in determining resource allocation, establishing & controlling profitability
\
political ecology has a critical focus on SYSTEMS that enable and expand inequality + exploitation
\
***analytical framework of political ecology:***
* examines relationships among politics, economics, and nature
* researchers advocate fundamental changes in the management of nature and the rights of people, directly or indirectly working with state and non-governmental organizations (NGOs) to challenge current conditions
33
New cards
Explain the ways modernization theory and eco-scarcity perspectives get used to explain the relationship between humans and nature. Why are these approaches characterized as “apolitical” ecology perspectives? How should Shah’s *The Fever* be categorized and why?
*(modernization theory and ecoscarcity perspectives are part of APOLITICAL ecology paradigms)*
\
__**ECOSCARCITY:**__
* Thomas Malthus *Essay on the Principle of Population (1798)*
* As human populations grow out of proportion to the capacity of the environmental system to support them, there is a crisis both for humans and for nature
* ***limits to growth:***
* Paul Ehrlich (1968) *The Population Bomb* (a tremenous bestseller)
* Urged global population control
* some Americans responded by having fewer or no children
* legitimated the development of the Population Control Industry by USAID, Population Council, WWF, IMF, etc.
* ***critiques of ecoscarcity framework:***
* impacts of affluence and technology overwhelm the force of crude numbers. A very few members of the global village consume the majority of its resources
* assumption that the environment is comprised of a finite source of basic, unchanging, and essential elements, which set absolute limits for human action, is false
* scarcity and Higher Prices can Encourage Discovery and Use of Alternatives
\
__**MODERNIZATION:**__
* ecological problems - result from lack of modern economic techniques of management, exploitation, and conservation
* need economic efficiency
* ***critiques of modernization theory:***
* views environmental change and ecological conditions as the product of political decisions & specific economic interests
* demonstrates how costs and benefits of environmental change are largely distributed among social actors unequally . . . which reinforces OR reduces existing social and economic inequalities
\
Both modernization theory and eco-scarcity perspectives are often characterized as "apolitical" ecology perspectives because they do not explicitly address the social and political factors that contribute to environmental problems. These perspectives tend to focus on technical solutions to environmental problems rather than on the underlying social and political structures that create these problems.
\
Shah's *The Fever* should be categorized as a ***POLITICAL ecology perspective***. This perspective acknowledges the political and social factors that contribute to environmental problems and seeks to address these factors in order to achieve sustainable and equitable solutions. The book examines the political and economic systems that contribute to the spread of malaria and argues that addressing these underlying systems is necessary for effective malaria control. The book also highlights the importance of local knowledge and community participation in environmental decision-making.
\
__**ECOSCARCITY:**__
* Thomas Malthus *Essay on the Principle of Population (1798)*
* As human populations grow out of proportion to the capacity of the environmental system to support them, there is a crisis both for humans and for nature
* ***limits to growth:***
* Paul Ehrlich (1968) *The Population Bomb* (a tremenous bestseller)
* Urged global population control
* some Americans responded by having fewer or no children
* legitimated the development of the Population Control Industry by USAID, Population Council, WWF, IMF, etc.
* ***critiques of ecoscarcity framework:***
* impacts of affluence and technology overwhelm the force of crude numbers. A very few members of the global village consume the majority of its resources
* assumption that the environment is comprised of a finite source of basic, unchanging, and essential elements, which set absolute limits for human action, is false
* scarcity and Higher Prices can Encourage Discovery and Use of Alternatives
\
__**MODERNIZATION:**__
* ecological problems - result from lack of modern economic techniques of management, exploitation, and conservation
* need economic efficiency
* ***critiques of modernization theory:***
* views environmental change and ecological conditions as the product of political decisions & specific economic interests
* demonstrates how costs and benefits of environmental change are largely distributed among social actors unequally . . . which reinforces OR reduces existing social and economic inequalities
\
Both modernization theory and eco-scarcity perspectives are often characterized as "apolitical" ecology perspectives because they do not explicitly address the social and political factors that contribute to environmental problems. These perspectives tend to focus on technical solutions to environmental problems rather than on the underlying social and political structures that create these problems.
\
Shah's *The Fever* should be categorized as a ***POLITICAL ecology perspective***. This perspective acknowledges the political and social factors that contribute to environmental problems and seeks to address these factors in order to achieve sustainable and equitable solutions. The book examines the political and economic systems that contribute to the spread of malaria and argues that addressing these underlying systems is necessary for effective malaria control. The book also highlights the importance of local knowledge and community participation in environmental decision-making.
34
New cards
On what basis do anthropologists criticize scholars who describe cultural diversity by listing seemingly exotic rituals or scientifically false beliefs? What alternative do anthropologists approach to discussing cultural difference?
* “othering” cultures – cultural relativity
* Alternative = understanding cultures
* Alternative = understanding cultures
35
New cards
Explain the concept of ‘practical reason’ as it is used in anthropology. How have scholars used it to explain Ghanian people’s use of mosquito nets?
practical reason is the idea that people make decisions based on a practical assessment of what is reasonable or feasible in a given situation, rather than relying solely on abstract principles or beliefs. It involves the use of practical knowledge, skills, and experience to make decisions and take action.
\
in Ghana, people used bed nets to prevent nuisance mosquito bites, REGARDLESS of whether they knew that mosquito bites are the source of malaria transmission → used bed nets because it was more practical to stop mosquito bites IN GENERAL, NOT specifically to stop malaria-carrying mosquitoes from infecting them
\
in Ghana, people used bed nets to prevent nuisance mosquito bites, REGARDLESS of whether they knew that mosquito bites are the source of malaria transmission → used bed nets because it was more practical to stop mosquito bites IN GENERAL, NOT specifically to stop malaria-carrying mosquitoes from infecting them
36
New cards
Global health experts often expect that once people become educated about scientifically based approaches to preventing disease, they will use these approaches. How do anthropologists explain that this assumption is not always accurate? Give an example.
this assumption doesn’t recognize people’s many, everyday concerns:
* need to prioritize purchases when cash is limited
* the comfort and convenience of the specific remedy or prevention measure
* the availability of alternative, cheaper methods
* the prestige (or shame) associated with a particular health behavior
\
For example, in some cultures, traditional healers play a crucial role in providing health care. Even if people are educated about modern medical treatments, they may still prefer to seek out the services of traditional healers because of the trust and respect they have for them. Similarly, in some communities, certain health practices may be seen as socially acceptable or desirable, regardless of their scientific validity.
* need to prioritize purchases when cash is limited
* the comfort and convenience of the specific remedy or prevention measure
* the availability of alternative, cheaper methods
* the prestige (or shame) associated with a particular health behavior
\
For example, in some cultures, traditional healers play a crucial role in providing health care. Even if people are educated about modern medical treatments, they may still prefer to seek out the services of traditional healers because of the trust and respect they have for them. Similarly, in some communities, certain health practices may be seen as socially acceptable or desirable, regardless of their scientific validity.
37
New cards
How was the practice of slavery related to the spread of yellow fever in Philadelphia in 1793?
Yellow fever of 1793 was associated with the PORT bc the port was DIRTY/smelled bad ESP when a ship with enslaved ppl arrived + enslaved ppl kept in filthy ships + rich ppl of Philly were not hanging around port when enslaved ppl/food/shipped goods arrived → there was no account with why people would live in these conditions (bc ppl living here were impoverished)
* the living conditions for enslaved people were often cramped and unsanitary, which made them more vulnerable to diseases like yellow fever. Additionally, enslaved people were often forced to work in areas that were infested with mosquitoes, which increased their risk of contracting the disease
* As yellow fever began to spread in Philadelphia in the summer of 1793, many enslaved Africans became sick and died from the disease. As a result, many slave owners fled the city with their enslaved people, hoping to avoid the disease. However, this also contributed to the spread of the disease as infected mosquitoes traveled with them
* The practice of slavery was also related to the spread of yellow fever in other ways. Many enslaved Africans worked as porters, carters, and other laborers, and they frequently came into contact with goods and people from other parts of the world, including areas where yellow fever was prevalent. This increased the likelihood of the disease being introduced into Philadelphia.
* the living conditions for enslaved people were often cramped and unsanitary, which made them more vulnerable to diseases like yellow fever. Additionally, enslaved people were often forced to work in areas that were infested with mosquitoes, which increased their risk of contracting the disease
* As yellow fever began to spread in Philadelphia in the summer of 1793, many enslaved Africans became sick and died from the disease. As a result, many slave owners fled the city with their enslaved people, hoping to avoid the disease. However, this also contributed to the spread of the disease as infected mosquitoes traveled with them
* The practice of slavery was also related to the spread of yellow fever in other ways. Many enslaved Africans worked as porters, carters, and other laborers, and they frequently came into contact with goods and people from other parts of the world, including areas where yellow fever was prevalent. This increased the likelihood of the disease being introduced into Philadelphia.
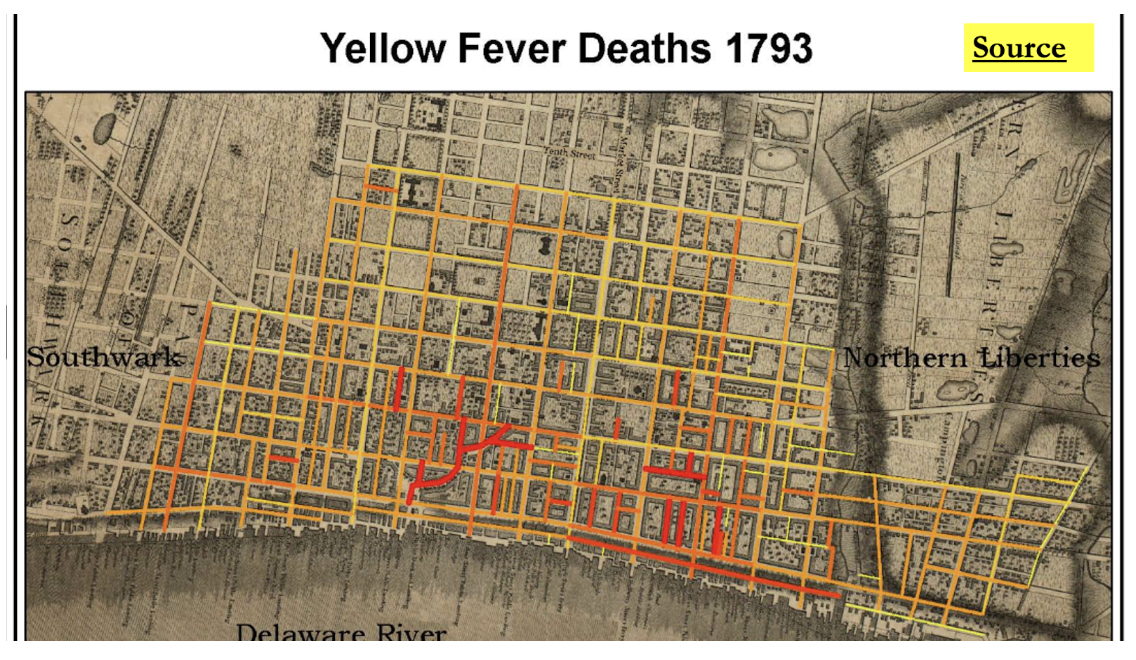
38
New cards
How did doctors differ in how they responded to the yellow fever epidemic in 1793? How did racialized myths of disease susceptibility impact care patterns in the outbreak?
Some doctors believed that the disease was caused by bad air (“miasma”), while others believed that it was caused by a contagious agent. These different beliefs led to different treatment strategies, with some doctors advocating for isolating patients and improving sanitation, while others focused on treating the symptoms of the disease.
\
Yellow fever is NOT person-to-person contagious BUT this was not known until the 1900s → ppl made sense of yellow fever with old understandings of disease (balanced organism - balance within organism and balance with respect to the world around you → weather could affect how you felt AND Dr. Benjamin Rush (“Anthony Fauci” of yellow fever) believed yellow fever was an imbalance that it caused too much heat in your body and associated BLOOD (blood = red, red also represented in fire and fever) with internal heat → *this is why Dr. Rush promoted blood-letting as a practice of getting rid of yellow fever*)
* Dr. Rush had a THEORY behind his blood-letting via leeches bc associated blood with fever and thought yellow fever brought about fever
* Dr. Rush also had theory that African Americans were IMMUNE to the disease - why? White people did not count African American lives → back to ethical question of whose lives are more important (at the time, it was WHITE lives that mattered so Black lives were seen as replaceable)
\
Racialized myths of disease susceptibility had a significant impact on care patterns during the outbreak. __*Some white doctors believed that Black people were IMMUNE to the disease or less likely to contract it*__. This belief was based on the observation that some Black people appeared to be less affected by the disease than their white counterparts. Result was that white doctors like Dr. Rush put Black community’s lives in danger bc asked Black community to provide NURSES (since believed to be immune to yellow fever). However, this myth of immunity was dangerous as it led to the neglect of Black patients, who were just as vulnerable to the disease as anyone else.
\
Yellow fever is NOT person-to-person contagious BUT this was not known until the 1900s → ppl made sense of yellow fever with old understandings of disease (balanced organism - balance within organism and balance with respect to the world around you → weather could affect how you felt AND Dr. Benjamin Rush (“Anthony Fauci” of yellow fever) believed yellow fever was an imbalance that it caused too much heat in your body and associated BLOOD (blood = red, red also represented in fire and fever) with internal heat → *this is why Dr. Rush promoted blood-letting as a practice of getting rid of yellow fever*)
* Dr. Rush had a THEORY behind his blood-letting via leeches bc associated blood with fever and thought yellow fever brought about fever
* Dr. Rush also had theory that African Americans were IMMUNE to the disease - why? White people did not count African American lives → back to ethical question of whose lives are more important (at the time, it was WHITE lives that mattered so Black lives were seen as replaceable)
\
Racialized myths of disease susceptibility had a significant impact on care patterns during the outbreak. __*Some white doctors believed that Black people were IMMUNE to the disease or less likely to contract it*__. This belief was based on the observation that some Black people appeared to be less affected by the disease than their white counterparts. Result was that white doctors like Dr. Rush put Black community’s lives in danger bc asked Black community to provide NURSES (since believed to be immune to yellow fever). However, this myth of immunity was dangerous as it led to the neglect of Black patients, who were just as vulnerable to the disease as anyone else.
39
New cards
What are some common metaphors that are important in pandemics? Explain how they work.
__**WEATHER:**__ used to say that plague is like a force of nature (a natural disaster beyond human ctrl)
* a sunny day = a good day BUT ALSO a sunny day can be ironic (how can the weather be so good but at the same time this HORROR is going on/happening to me)
* emotional mood/tone of narrator and citizens (dismal, stormy, monotonous, horrifically, uncomfortably-hot weather, etc)
* the weather holds BOTH a more religious interpretation but ALSO the *beginnings* of our public health understanding of disease
* can express God’s displeasure (provide RELIGIOUS understanding of the plague)
* can express the fact that this disease is contagious/miasmatic/atmospheric
* “The weather takes on heightened importance: “It seemed, from looking at them, that for the first time they were directly receiving an impression of what the weather was doing. Their faces rejoiced at the sight of a simple golden ray, while the days of rain would put a thick veil over their faces and their thoughts” (78)
* Why are they looking at the sky? Why else would they look up? (1) no where else to look bc locked up, (2) people look up to ask god why they would be suffering from this → sense of religion involved in looking up
\
__**WAR:**__ compares the fight against the disease to a military conflict, with healthcare workers and other essential personnel on the front lines battling against an invisible enemy. This metaphor helps to convey the seriousness and urgency of the situation, and the need for everyone to work together to overcome the pandemic
* “Scourges are actually a communal thing but it’s hard to believe in them when they’re right in front of you. Across the world, there have been so many plagues as wars. And yet plagues and wars leave people equally at a loss.”
* a sunny day = a good day BUT ALSO a sunny day can be ironic (how can the weather be so good but at the same time this HORROR is going on/happening to me)
* emotional mood/tone of narrator and citizens (dismal, stormy, monotonous, horrifically, uncomfortably-hot weather, etc)
* the weather holds BOTH a more religious interpretation but ALSO the *beginnings* of our public health understanding of disease
* can express God’s displeasure (provide RELIGIOUS understanding of the plague)
* can express the fact that this disease is contagious/miasmatic/atmospheric
* “The weather takes on heightened importance: “It seemed, from looking at them, that for the first time they were directly receiving an impression of what the weather was doing. Their faces rejoiced at the sight of a simple golden ray, while the days of rain would put a thick veil over their faces and their thoughts” (78)
* Why are they looking at the sky? Why else would they look up? (1) no where else to look bc locked up, (2) people look up to ask god why they would be suffering from this → sense of religion involved in looking up
\
__**WAR:**__ compares the fight against the disease to a military conflict, with healthcare workers and other essential personnel on the front lines battling against an invisible enemy. This metaphor helps to convey the seriousness and urgency of the situation, and the need for everyone to work together to overcome the pandemic
* “Scourges are actually a communal thing but it’s hard to believe in them when they’re right in front of you. Across the world, there have been so many plagues as wars. And yet plagues and wars leave people equally at a loss.”
40
New cards
What does “epistemology” mean and how is it relevant to virtue? To one’s world view?
Epistemology is the branch of philosophy that deals with knowledge and belief. It is concerned with the study of how we acquire knowledge, the limits of knowledge, and the reliability of different forms of knowledge. Epistemology explores questions such as: what is knowledge? How do we know what we claim to know? How certain can we be of our beliefs?
\
Epistemology is relevant to virtue because it helps us to understand how we come to form virtuous beliefs and actions. Virtue requires not only acting in accordance with certain values and principles, but also having the right beliefs and attitudes that support virtuous behavior. Epistemology can help us to evaluate the quality of our beliefs and ensure that they are grounded in reliable forms of knowledge.
\
Epistemology is also relevant to one's worldview because it underlies how we understand the world around us. Our beliefs about reality, morality, and meaning are based on the assumptions and presuppositions that we bring to our epistemological inquiry. By examining our epistemological assumptions, we can gain insight into the foundations of our worldview and how it shapes our understanding of the world.
\
Epistemology is relevant to virtue because it helps us to understand how we come to form virtuous beliefs and actions. Virtue requires not only acting in accordance with certain values and principles, but also having the right beliefs and attitudes that support virtuous behavior. Epistemology can help us to evaluate the quality of our beliefs and ensure that they are grounded in reliable forms of knowledge.
\
Epistemology is also relevant to one's worldview because it underlies how we understand the world around us. Our beliefs about reality, morality, and meaning are based on the assumptions and presuppositions that we bring to our epistemological inquiry. By examining our epistemological assumptions, we can gain insight into the foundations of our worldview and how it shapes our understanding of the world.
41
New cards
epistemological framework in Camus and Defoe
REMINDER: epistemology is all about *what does it mean?*
\
* Weather / atmospheric events - used to interpret what is happening in the human world (EPISTEMOLOGICAL framework)
* COMET appearing for several months before the plague (Defoe)
* Weather turning terrible as soon as Michel died (Camus)
* “Finger of God” - people explain the plague in both Camus and Defoe using religion
* religion explained the plague as God-punishing
\
* Weather / atmospheric events - used to interpret what is happening in the human world (EPISTEMOLOGICAL framework)
* COMET appearing for several months before the plague (Defoe)
* Weather turning terrible as soon as Michel died (Camus)
* “Finger of God” - people explain the plague in both Camus and Defoe using religion
* religion explained the plague as God-punishing
42
New cards
What is “poetic justice”? Give two examples of how it shows up in the course readings.
poetic justice is an outcome in which vice is punished and virtue rewarded usually in a manner peculiarly or ironically appropriate
\
* plague (esp yellow fever, more than any other disease) would seem conjured by God and divinely directed
* This is also message of Father Paneloux’s first sermon
* In *The American Plague*: When the slave trade first began, every European country that profited from the purchase and sale of Africans would soon see a yellow fever epidemic. (12)
* Also in *The American Plague*: the outbreak of yellow fever in America coincided with the arrival of slaves → as slavery diminished, so did the incidence of yellow fever; the ARGUMENT/PERSPECTIVE of the book was that the South DESERVED this plague (return of the repressed, the power of Africa reaching across the sea as punishment for white people enslaving people)
\
* plague (esp yellow fever, more than any other disease) would seem conjured by God and divinely directed
* This is also message of Father Paneloux’s first sermon
* In *The American Plague*: When the slave trade first began, every European country that profited from the purchase and sale of Africans would soon see a yellow fever epidemic. (12)
* Also in *The American Plague*: the outbreak of yellow fever in America coincided with the arrival of slaves → as slavery diminished, so did the incidence of yellow fever; the ARGUMENT/PERSPECTIVE of the book was that the South DESERVED this plague (return of the repressed, the power of Africa reaching across the sea as punishment for white people enslaving people)
43
New cards
We have discussed the metaphor of war, which is frequently used to discuss epidemic disease and its social effects. State __one__ positive outcome that can come from the use of this metaphor and __two__ problems with this metaphor.
One positive outcome of using the war metaphor for pandemics is that it can mobilize collective action and resources. Just as in a wartime scenario, the urgency and severity of the situation can prompt individuals and governments to take swift and coordinated action to contain and manage the outbreak.
\
However, there are also two major problems with this metaphor. Firstly, it can promote a sense of division and hostility, as it tends to frame the pandemic as an enemy to be fought and defeated. This can lead to stigmatization and discrimination against certain groups, such as those who are seen as responsible for spreading the disease.
\
Secondly, the war metaphor can lead to culturally-incompetent approaches to public health, such as mandatory lockdowns and heavy-handed enforcement measures that are put in effect by one group without looking at the culture of groups also subjected to these rules. This can undermine civil liberties and human rights, and may not always be the most effective or ethical way of managing a pandemic.
\
However, there are also two major problems with this metaphor. Firstly, it can promote a sense of division and hostility, as it tends to frame the pandemic as an enemy to be fought and defeated. This can lead to stigmatization and discrimination against certain groups, such as those who are seen as responsible for spreading the disease.
\
Secondly, the war metaphor can lead to culturally-incompetent approaches to public health, such as mandatory lockdowns and heavy-handed enforcement measures that are put in effect by one group without looking at the culture of groups also subjected to these rules. This can undermine civil liberties and human rights, and may not always be the most effective or ethical way of managing a pandemic.
44
New cards
*The American Plague* makes an analogy between the action of the yellow fever virus inside a person’s body and the narrative of the Trojan Horse. Explain how this analogy works.
“A virus in its own right is not actually alive—it only becomes alive by possessing something living. (8)
Once the \[virus and a healthy cell\] make contact in the bloodstream, a process with a technical name known as receptor-mediated endocytosis begins—a sort of molecular Trojan Horse. The healthy cell eventually enfolds the virus, taking it in and closing the door behind it.
Once inside, the virus hijacks the cell and its basic machinery, using the cell’s internal makeup to replicate the viral proteins and RNA, until the new particles burst through the cell.”
\
Extended metaphor: horse = well-protected disguise, walls of city = immune system → in Trojan horse story, the Greeks snuck in and took over the Trojans (the DEAD virus ENLIVENS itself by going into our bodies where it HIJACKS our powers of life and starts to REPLICATE itself)
Once the \[virus and a healthy cell\] make contact in the bloodstream, a process with a technical name known as receptor-mediated endocytosis begins—a sort of molecular Trojan Horse. The healthy cell eventually enfolds the virus, taking it in and closing the door behind it.
Once inside, the virus hijacks the cell and its basic machinery, using the cell’s internal makeup to replicate the viral proteins and RNA, until the new particles burst through the cell.”
\
Extended metaphor: horse = well-protected disguise, walls of city = immune system → in Trojan horse story, the Greeks snuck in and took over the Trojans (the DEAD virus ENLIVENS itself by going into our bodies where it HIJACKS our powers of life and starts to REPLICATE itself)
45
New cards
describe Absolom Jones and Richard Allen
*(historical figures, part of efforts to fight yellow fever outbreak of 1793)*
\
Absolom Jones (top left), Richard Allen (middle top) - leaders of the Black community of Philly, had recently organized a new African church (which right around the time a few years after became the AME (African Methodist Evangelical) church)
\
Absolom Jones (top left), Richard Allen (middle top) - leaders of the Black community of Philly, had recently organized a new African church (which right around the time a few years after became the AME (African Methodist Evangelical) church)

46
New cards
describe Benjamin Rush
*(historical figure, main doctor in effort to fight yellow fever outbreak of 1793)*
\
yellow fever is NOT person-to-person contagious BUT this was not known until the 1900s → ppl made sense of yellow fever with old understandings of disease (balanced organism - balance within organism and balance with respect to the world around you → weather could affect how you felt AND Dr. Benjamin Rush (“Anthony Fauci” of yellow fever) believed yellow fever was an imbalance that it caused too much heat in your body and associated BLOOD (blood = red, red also represented in fire and fever) with internal heat → *this is why Dr. Rush promoted blood-letting as a practice of getting rid of yellow fever*)
* Dr. Rush had a THEORY behind his blood-letting via leeches bc associated blood with fever and thought yellow fever brought about fever
* Also had theory that African Americans were IMMUNE to the disease - why? White people did not count African American lives → *back to ethical question of whose lives are more important* (at the time, it was WHITE lives that mattered so Black lives were seen as replaceable)
\
yellow fever is NOT person-to-person contagious BUT this was not known until the 1900s → ppl made sense of yellow fever with old understandings of disease (balanced organism - balance within organism and balance with respect to the world around you → weather could affect how you felt AND Dr. Benjamin Rush (“Anthony Fauci” of yellow fever) believed yellow fever was an imbalance that it caused too much heat in your body and associated BLOOD (blood = red, red also represented in fire and fever) with internal heat → *this is why Dr. Rush promoted blood-letting as a practice of getting rid of yellow fever*)
* Dr. Rush had a THEORY behind his blood-letting via leeches bc associated blood with fever and thought yellow fever brought about fever
* Also had theory that African Americans were IMMUNE to the disease - why? White people did not count African American lives → *back to ethical question of whose lives are more important* (at the time, it was WHITE lives that mattered so Black lives were seen as replaceable)
47
New cards
describe Leah Price
*(main character in* __*The Poisonwood Bible*__ *by Barbara Kingsolver)*
\
* eldest daughter of Nathan Price (a Baptist missionary who takes his family to the Belgian Congo in 1959 to convert the villagers)
* a bright, curious, and observant young woman who is fascinated by her surroundings in the Congo. She quickly learns the language and customs of the people and becomes friends with many of the villagers. Leah is also deeply committed to her father's mission, but as she grows older, she begins to question his methods and beliefs.
* Throughout the novel, Leah's character undergoes significant growth and transformation as she comes to understand the complexities of life in the Congo and begins to question her own beliefs and values. Overall, Leah is a complex and compelling character who represents the struggle to reconcile personal convictions with the realities of the world around us.
\
* eldest daughter of Nathan Price (a Baptist missionary who takes his family to the Belgian Congo in 1959 to convert the villagers)
* a bright, curious, and observant young woman who is fascinated by her surroundings in the Congo. She quickly learns the language and customs of the people and becomes friends with many of the villagers. Leah is also deeply committed to her father's mission, but as she grows older, she begins to question his methods and beliefs.
* Throughout the novel, Leah's character undergoes significant growth and transformation as she comes to understand the complexities of life in the Congo and begins to question her own beliefs and values. Overall, Leah is a complex and compelling character who represents the struggle to reconcile personal convictions with the realities of the world around us.
48
New cards
themes present in Leah’s narrative of *The Poisonwood Bible*
* Fearsome world of nature: snakes, killer ants, unseen parasites, lions
* “Poisonwood” Bible: white saviors can wreak havoc, “poison” a society
* Patronizing and deadly effects of colonization
* Blind faith can be a form of blindness, lead to terrible consequences
* Achieving independence from a brutal and powerful overseers
* “Poisonwood” Bible: white saviors can wreak havoc, “poison” a society
* Patronizing and deadly effects of colonization
* Blind faith can be a form of blindness, lead to terrible consequences
* Achieving independence from a brutal and powerful overseers
49
New cards
describe Tom Tomlinson
* philosopher and bioethicist who specializes in ethical issues related to healthcare and biomedical research
* proposed the idea of social contract as a reason for why health care providers should care for patients even if doing so puts them at risk
* research focuses on a wide range of topics related to bioethics, including informed consent, research ethics, end-of-life care, and the allocation of healthcare resources
* proposed the idea of social contract as a reason for why health care providers should care for patients even if doing so puts them at risk
* research focuses on a wide range of topics related to bioethics, including informed consent, research ethics, end-of-life care, and the allocation of healthcare resources
50
New cards
describe Immanuel Kant
* German philosopher (1724-1804) who is widely regarded as one of the most influential thinkers in the history of Western philosophy
* best known for his works on metaphysics, __***epistemology, ethics,***__ and political philosophy.
* Kant's philosophy is characterized by his emphasis on reason, autonomy, and the pursuit of universal principles.
* argued that knowledge is based on a priori concepts, which are innate to the mind and are necessary for understanding the world
* also believed that moral principles are based on the concept of the "categorical imperative," which states that actions should be based on principles that could be universally applied.
* best known for his works on metaphysics, __***epistemology, ethics,***__ and political philosophy.
* Kant's philosophy is characterized by his emphasis on reason, autonomy, and the pursuit of universal principles.
* argued that knowledge is based on a priori concepts, which are innate to the mind and are necessary for understanding the world
* also believed that moral principles are based on the concept of the "categorical imperative," which states that actions should be based on principles that could be universally applied.
51
New cards
describe Hippocrates
* renown Greek physician of the classical period, 460-\~370 BCE
* Large body of writings, but many probably in his tradition and not by him (including the __***Hippocratic Oath***__)
* Referred to in writings by philosophers Plato and Aristotle
* Typically, medical students take a “modern” version of the oath
* Large body of writings, but many probably in his tradition and not by him (including the __***Hippocratic Oath***__)
* Referred to in writings by philosophers Plato and Aristotle
* Typically, medical students take a “modern” version of the oath
52
New cards
describe Aristotle
* Greek philosopher and scientist who is widely regarded as one of the most important figures in the history of Western philosophy (384-322 BCE)
* philosophy covered a wide range of topics, including metaphysics, __***ethics,***__ politics, and biology. He believed that knowledge is acquired through observation and experience, and that the natural world can be understood through systematic investigation and analysis.
* ethical theory focused on the concept of happiness which he believed was the ultimate goal of human life. He argued that virtues such as courage, wisdom, and justice were essential to achieving this state, and that individuals should strive to live a life of balance and moderation
* Overall, Aristotle's philosophy has had a profound impact on Western thought and continues to be studied and debated by philosophers, scientists, and scholars today.
* philosophy covered a wide range of topics, including metaphysics, __***ethics,***__ politics, and biology. He believed that knowledge is acquired through observation and experience, and that the natural world can be understood through systematic investigation and analysis.
* ethical theory focused on the concept of happiness which he believed was the ultimate goal of human life. He argued that virtues such as courage, wisdom, and justice were essential to achieving this state, and that individuals should strive to live a life of balance and moderation
* Overall, Aristotle's philosophy has had a profound impact on Western thought and continues to be studied and debated by philosophers, scientists, and scholars today.
53
New cards
describe Walter Reed
* American physician (1851-1902) and army surgeon who is best known for his work on yellow fever and first implementing the idea of informed consent in research
* Reed and his team conducted a series of experiments and observations that ultimately led to the discovery that yellow fever was transmitted by mosquitoes. This breakthrough was a major milestone in the history of medicine, as it led to the development of effective measures to control and prevent the spread of the disease.
* set of experiments by the U.S. Army surgeon Walter Reed and colleagues (Yellow Fever Commission) in Cuba in 1900 showing that:
* the Aedes mosquito was the intermediate host for yellow fever
* other traditional routes of infection (dried blood, vomit, etc.) do not cause infection
* experiments are known for their use of informed consent and “heroism” and self-experimentation
* participants were 18 Americans (including 15 Army enlisted), and 15 Spanish immigrants to Cuba (who were less likely to have been exposed prior than local people)
* the U.S. Army was in Cuba at the time as part of a temporary occupying government after the Spanish-American war when Spain ceded control of Cuba
* Reed and his team conducted a series of experiments and observations that ultimately led to the discovery that yellow fever was transmitted by mosquitoes. This breakthrough was a major milestone in the history of medicine, as it led to the development of effective measures to control and prevent the spread of the disease.
* set of experiments by the U.S. Army surgeon Walter Reed and colleagues (Yellow Fever Commission) in Cuba in 1900 showing that:
* the Aedes mosquito was the intermediate host for yellow fever
* other traditional routes of infection (dried blood, vomit, etc.) do not cause infection
* experiments are known for their use of informed consent and “heroism” and self-experimentation
* participants were 18 Americans (including 15 Army enlisted), and 15 Spanish immigrants to Cuba (who were less likely to have been exposed prior than local people)
* the U.S. Army was in Cuba at the time as part of a temporary occupying government after the Spanish-American war when Spain ceded control of Cuba
54
New cards
Name three concerns about using gene-editing and gene-drives as a solution to intractable human diseases.
1. __***WORRY #1: Scientific Humility and Hubris: what’s the worry?***__
1. Hubris as a “dangerous overconfidence in one’s abilities” (Callies, 1093)
1. “extrinsic” worry: failure to account for important risks
2. “intrinsic” worry: “playing god” – not for us to mess with nature in this way
2. Humility as a moral character trait is a reliable tendency to have a modest opinion of one’s own accomplishments relative to others
3. The relevant vices are overweening pride (the excess); and self-diffidence (the deficiency)
4. *Epistemic* (to do with knowledge) humility is an intellectual trait to have a modest opinion of one’s intellectual achievements (relative to others and relative to knowledge)
5. The vices are epistemic arrogance (the excess) and paralyzing self-doubt (the deficiency)
\
2. __***WORRY #2: Sliding down the slippery slope***__
1. ”Slippery slope worries start with an empirical premise that says: If we do A, then it will lead to B. They then have a normative premise that says: We should avoid B.” (Callies 1095)
2. Better account: “The argument starts by considering an execution of a seemingly harmless action. The argument exhibits how the implementation of the action would inevitably lead to an undesired or detrimental consequence. Then, a conclusion is reached that aims to avoid the undesired consequence.” (Lillo-Unglaube et al., Frontiers in Psychology, 2014).
3. Core elements are:
1. An initial action/decision that seems benign or acceptable
2. A dangerous or to be avoided situation or case
3. A mechanism whereby 1 facilitates/causes 2
\
3. __***WORRY #3: The flip side: Actions and inactions***__
1. Slippery slopers and others worried about the possible detrimental effects (or hubris) of gene-editing and gene-drive draw attention to risks of the technology.
2. The other side draws attention to the harm of NOT acting
1. Kahn in the Ted Talk says, “it can be frightening to act, but sometimes not acting is worse” (1,000 people a day die of malaria, current use of insecticides, etc.)
2. “Recall that between 438,000 and 720,000 people die of malaria every year. So starting from the moment we have deployable gene drive technologies that could wipe out the disease, every day we wait kills between 1,200 and 2,000 people.” (Matthews, Vox 2018)
3. The __*ethical*__ question: Is there a moral difference between action and inaction such that we are less culpable for the harms of our inaction? Or are actions and inactions morally equivalent in terms of our responsibility?
\
4. __***WORRY #4: redirection of aid (and what we owe to future generations)***__
1. If aid is redirected to gene drive research, will it cut current efforts to use traditional means of combating malaria?
2. “would the “bad” of decreased funding for malaria… be more than compensated for by the “good” of eventual malaria eradication?” (Callies, p. 1095)
3. Raises the __*ethical*__ issue of what we owe future generations and how we compare trade-offs in welfare between current and future peoples.
4. What diminished welfare should we accept now to alleviate harms to future, not yet existing, people? (climate change!)
1. What do we owe to people who don’t yet, but will, exist?
2. How should we balance their (future) interests with our (current) ones?
\
==__***SUMMARY:***__ Using gene-drives and gene-editing to potentially eradicate malaria points to significant issues, many of which are independently important including:==
* The significance of intellectual humility in science
* The use of slippery slope arguments to warn of inevitable path to bad outcomes from a benign starting place
* The ethical question of whether there is a moral responsibility difference between action and inaction
* The ethical question of what we owe to future generations

55
New cards
What literary genre is *The Plague*? What literary genre is *The Fever*? Give two examples of how the difference in genre between these works is important for how they contribute to our understanding of pandemics.
* Genre of plague = fiction
* Genre of fever = nonfiction; long-form journalism
* Apolitical but biased POV – thought people/past decisions in general were failing; ex: cinchona bark thought that people had failed to prevent the spread/find the cure of malaria; critiqued human action but also doesn’t provide a better alternative
* Shah does NOT spend time IN the communities – she is drawing on OTHER people’s research these are not original arguments; her argument is a narrative based on other people’s arguments (thus NOT an ethnography bc ethnographies are based on author’s OWN research)
* Shah is giving us a narrative about what’s at stake but is IMPLYING political
\
The difference in genre between these two works is significant for how they contribute to our understanding of pandemics in two ways:
1. ***Perspective:*** "The Plague" provides a subjective and philosophical perspective on pandemics. It explores the human condition during a pandemic, the responses of different characters to the crisis, and the impact of the pandemic on their lives. It presents a deep reflection on the nature of existence, death, and human suffering. In contrast, "The Fever" provides an objective and scientific perspective on pandemics. It explores the biology of viruses, the history of pandemics, and the responses of governments, health organizations, and individuals to pandemics. It presents a detailed analysis of the scientific and social factors that shape the emergence and spread of pandemics.
2. ***Emphasis:*** "The Plague" emphasizes the emotional and psychological impact of pandemics on individuals and communities. It portrays the fear, isolation, and despair that people experience during a pandemic. It also shows the resilience, solidarity, and compassion that people display in times of crisis. In contrast, "The Fever" emphasizes the scientific and social dimensions of pandemics. It provides information on the origin, transmission, and prevention of pandemics. It also examines the social inequalities and political dynamics that influence the distribution of resources and the management of pandemics.
* Genre of fever = nonfiction; long-form journalism
* Apolitical but biased POV – thought people/past decisions in general were failing; ex: cinchona bark thought that people had failed to prevent the spread/find the cure of malaria; critiqued human action but also doesn’t provide a better alternative
* Shah does NOT spend time IN the communities – she is drawing on OTHER people’s research these are not original arguments; her argument is a narrative based on other people’s arguments (thus NOT an ethnography bc ethnographies are based on author’s OWN research)
* Shah is giving us a narrative about what’s at stake but is IMPLYING political
\
The difference in genre between these two works is significant for how they contribute to our understanding of pandemics in two ways:
1. ***Perspective:*** "The Plague" provides a subjective and philosophical perspective on pandemics. It explores the human condition during a pandemic, the responses of different characters to the crisis, and the impact of the pandemic on their lives. It presents a deep reflection on the nature of existence, death, and human suffering. In contrast, "The Fever" provides an objective and scientific perspective on pandemics. It explores the biology of viruses, the history of pandemics, and the responses of governments, health organizations, and individuals to pandemics. It presents a detailed analysis of the scientific and social factors that shape the emergence and spread of pandemics.
2. ***Emphasis:*** "The Plague" emphasizes the emotional and psychological impact of pandemics on individuals and communities. It portrays the fear, isolation, and despair that people experience during a pandemic. It also shows the resilience, solidarity, and compassion that people display in times of crisis. In contrast, "The Fever" emphasizes the scientific and social dimensions of pandemics. It provides information on the origin, transmission, and prevention of pandemics. It also examines the social inequalities and political dynamics that influence the distribution of resources and the management of pandemics.
56
New cards
How does the narrative of the divine show up in Defoe’s *A Journal of the Plague Year*? In Camus’ *The Plague*? In Crosby’s account of yellow fever?
When people start talking about how their faith in God began at the end, we got more of an insight into how the people and their stories developed as a result. They were praising god for saving them and allowing them to live and how he saved the area from dying so suddenly
57
New cards
What are 2 critiques of arguments in *The Fever* that are based on a political ecology perspective?
* Brazilian govt supported by world bank → encouraged development practices that increased environment → resulted in more water → resulted in more mosquitoes → more malaria
* Political: money/other interests (political, economic) drive development
* Apollitical: happens regardless of politics
* MODERNIZATION perspective: In the fever, shah tells us about new developments like housing (human actions) that promote malaria BUT the way that she analyzes this makes the spread of malaria seem almost natural (“inevitable under human progress” aka MODERNIZATION)
* Apolitical ecology says “this is the process of modernization” – does not say that human beings aren’t a part of the process but rather this (modernization) is inevitable
* POLITICAL ecology says there are certain people who made certain decisions deliberately via politics (says that DECISIONS are made that benefit some/serve some intersts but not other interests and we need to think about the poltical perspective)
* If you are a climate change activist and want to prevent climate change, you say that THESE are actions we can take TODAY – we can make certain decisions to change the behavior of how society is functioning WHILE APOLITICAL ecology says this is just what happens as a result of human nature
* Poltical ecology also holds people more accountable (asks questions about what are these changes and why have they happened) while apolitical does not hold people accountable
* ECOSCARCITY perspective: often ignores political decisions/role of political and economic interests in certain kinds of development
* Political: money/other interests (political, economic) drive development
* Apollitical: happens regardless of politics
* MODERNIZATION perspective: In the fever, shah tells us about new developments like housing (human actions) that promote malaria BUT the way that she analyzes this makes the spread of malaria seem almost natural (“inevitable under human progress” aka MODERNIZATION)
* Apolitical ecology says “this is the process of modernization” – does not say that human beings aren’t a part of the process but rather this (modernization) is inevitable
* POLITICAL ecology says there are certain people who made certain decisions deliberately via politics (says that DECISIONS are made that benefit some/serve some intersts but not other interests and we need to think about the poltical perspective)
* If you are a climate change activist and want to prevent climate change, you say that THESE are actions we can take TODAY – we can make certain decisions to change the behavior of how society is functioning WHILE APOLITICAL ecology says this is just what happens as a result of human nature
* Poltical ecology also holds people more accountable (asks questions about what are these changes and why have they happened) while apolitical does not hold people accountable
* ECOSCARCITY perspective: often ignores political decisions/role of political and economic interests in certain kinds of development