BIO 222 Lecture7.DigestiveSystemAnatomy.Pops - Part1 Review
1/130
Earn XP
Description and Tags
BIO 222 Anatomy & Physiology 2
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
131 Terms
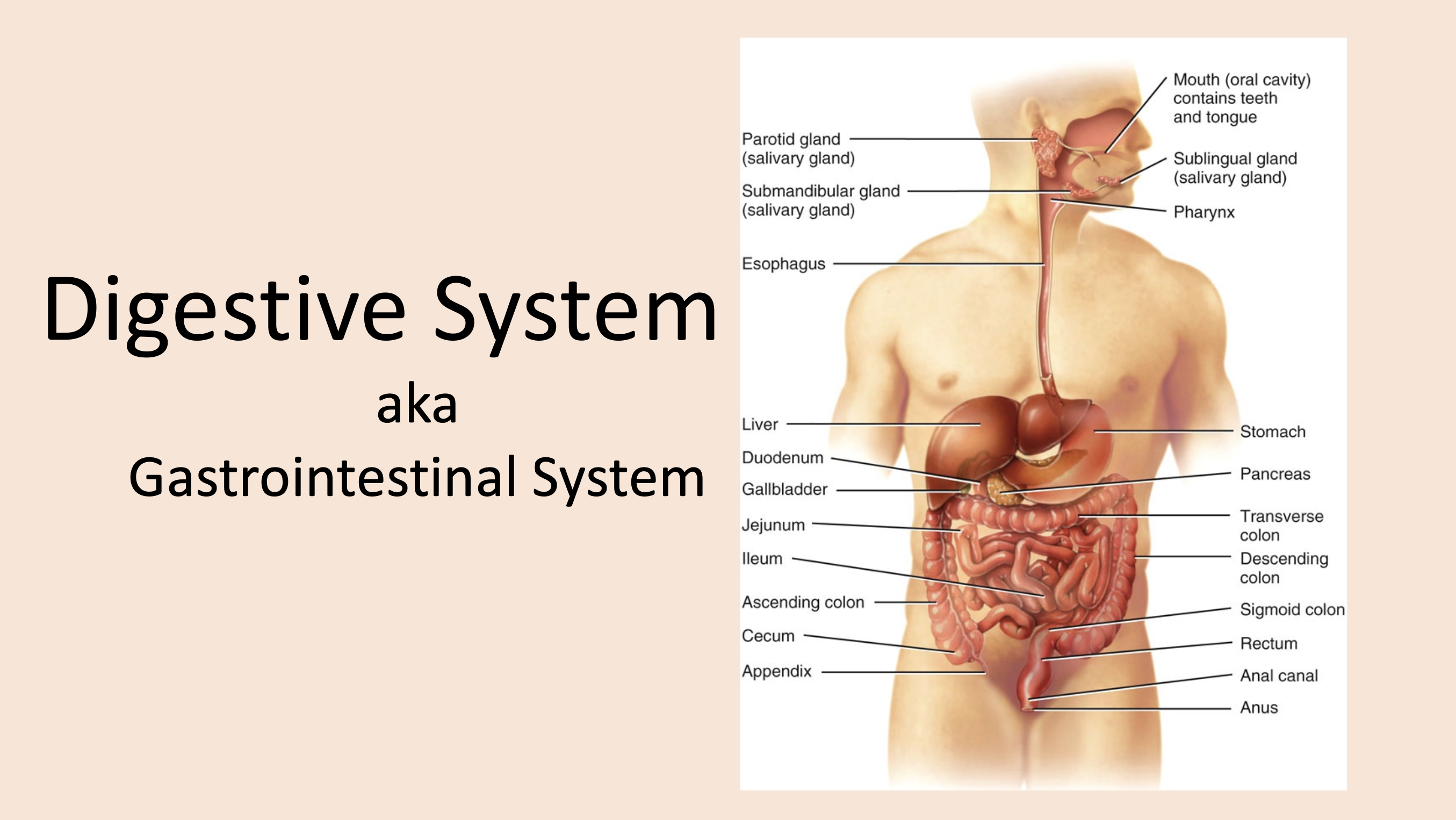
aka Gastrointestinal System
digestive system
aka alimentary canal
GI tract

Mouth → pharynx →esophagus →stomach →small intestine → large intestine.
~5-7 meters long.
Muscles in state of tonus.
GI tract

sustained contraction
tonus

Accessory organs/structures
teeth
tongue
salivary glands
liver
gall bladder
pancreas

Physical break down of food.
Assist in chewing/swallowing.
teeth
tongue

No contact with food.
Produce or store secretions that aid in the chemical breakdown of food.
salivary glands
liver
gall bladder
pancreas

Digestive System Process
ingestion
secretion
mixing and propulsion
digestion
absorption
defecation

Taking foods/liquids into mouth
ingestion

Release of H2O, acid, buffers, hormones, and enzymes into the lumen of the GI tract
secretion

Alternating contractions & relaxation of smooth muscle to churn food & move through GI tract.
peristalsis.
mixing and propulsion (motility)

Mechanical & chemical breakdown of food
digestion

Passage of digested products from GI tract into blood and lymph
absorption

Elimination of feces (stool)
defecation

Connecting Folds
peritoneum
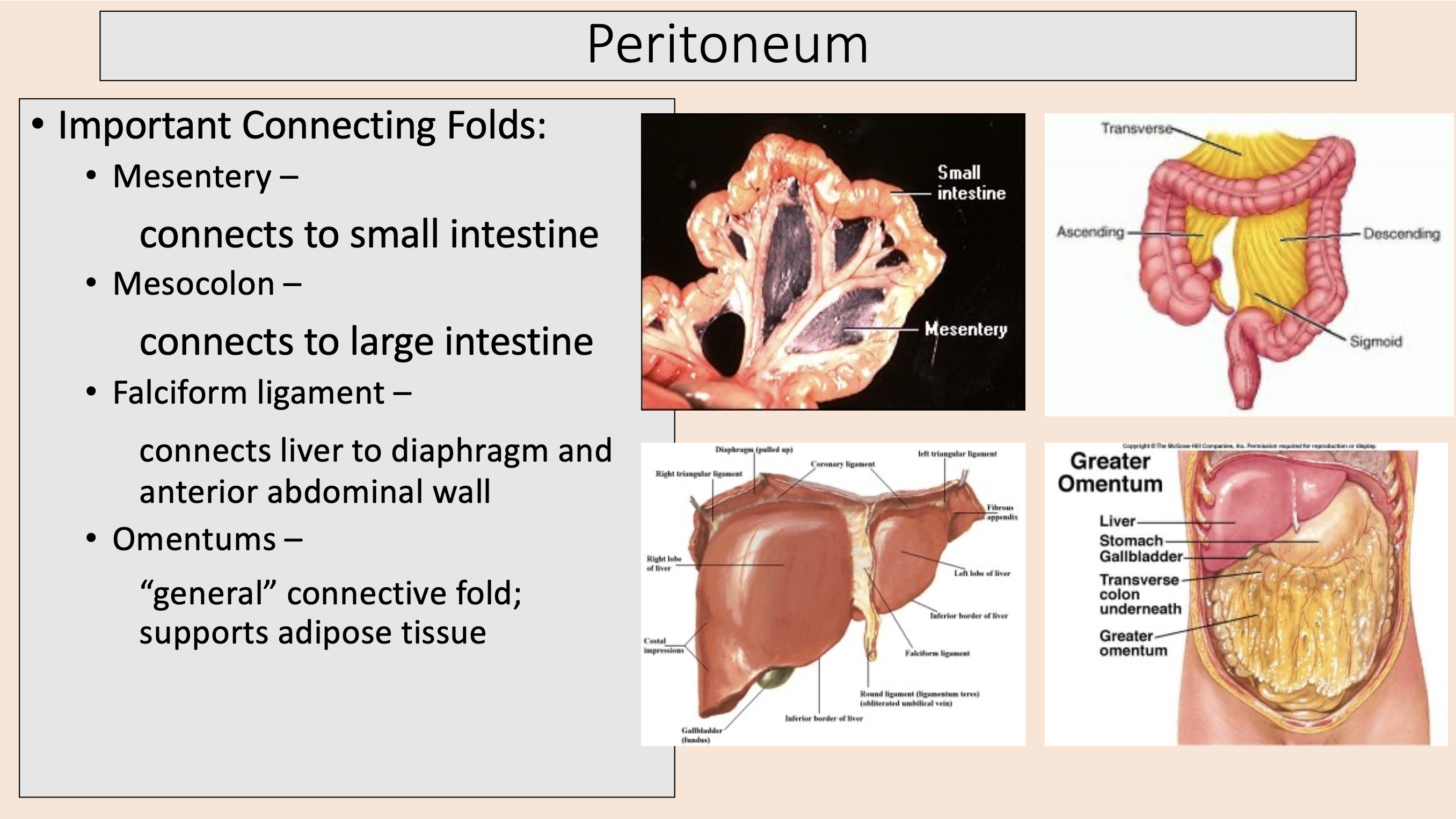
Important Connecting Folds:
mesentery
mesocolon
falciform ligament
omentums
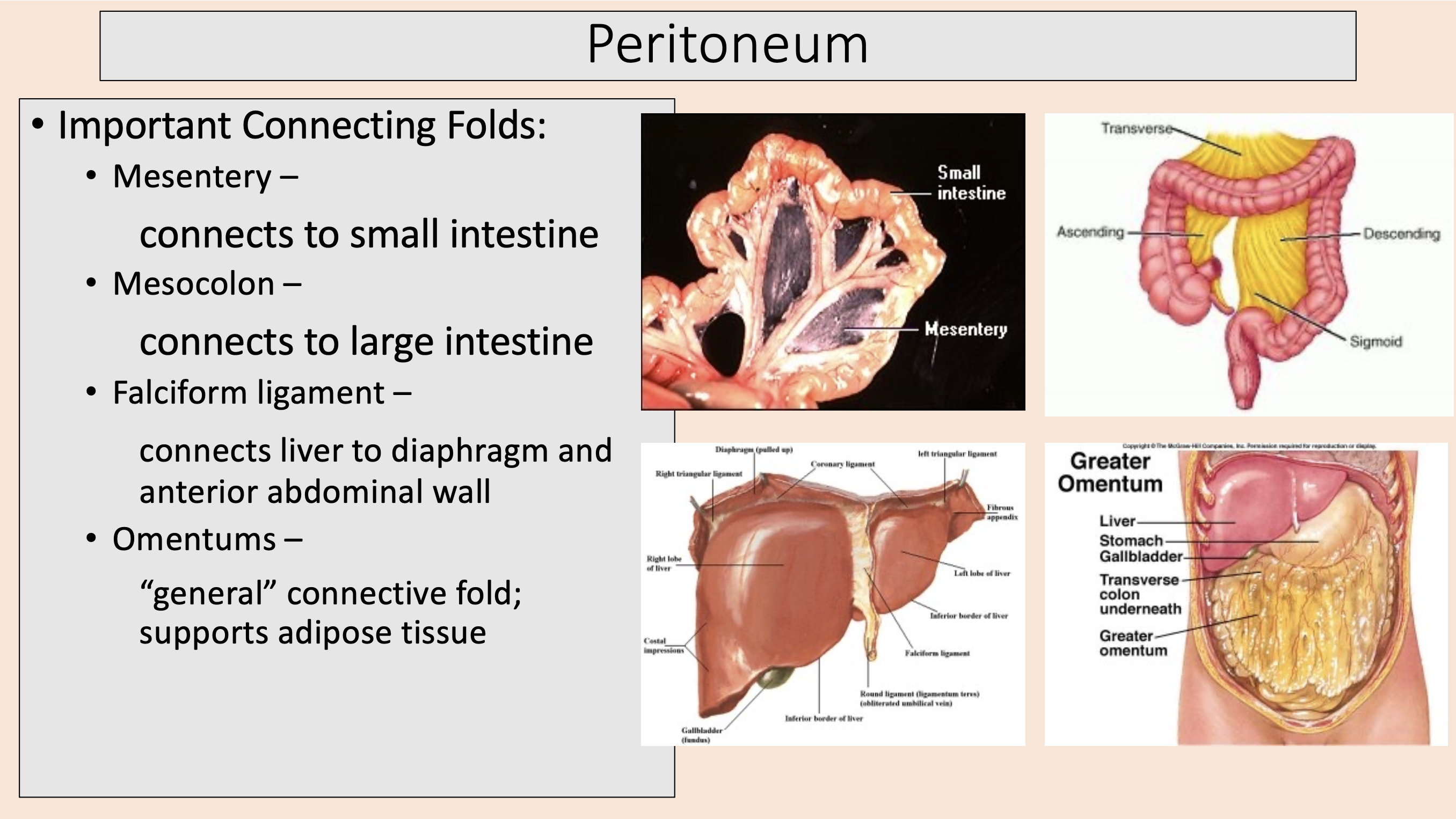
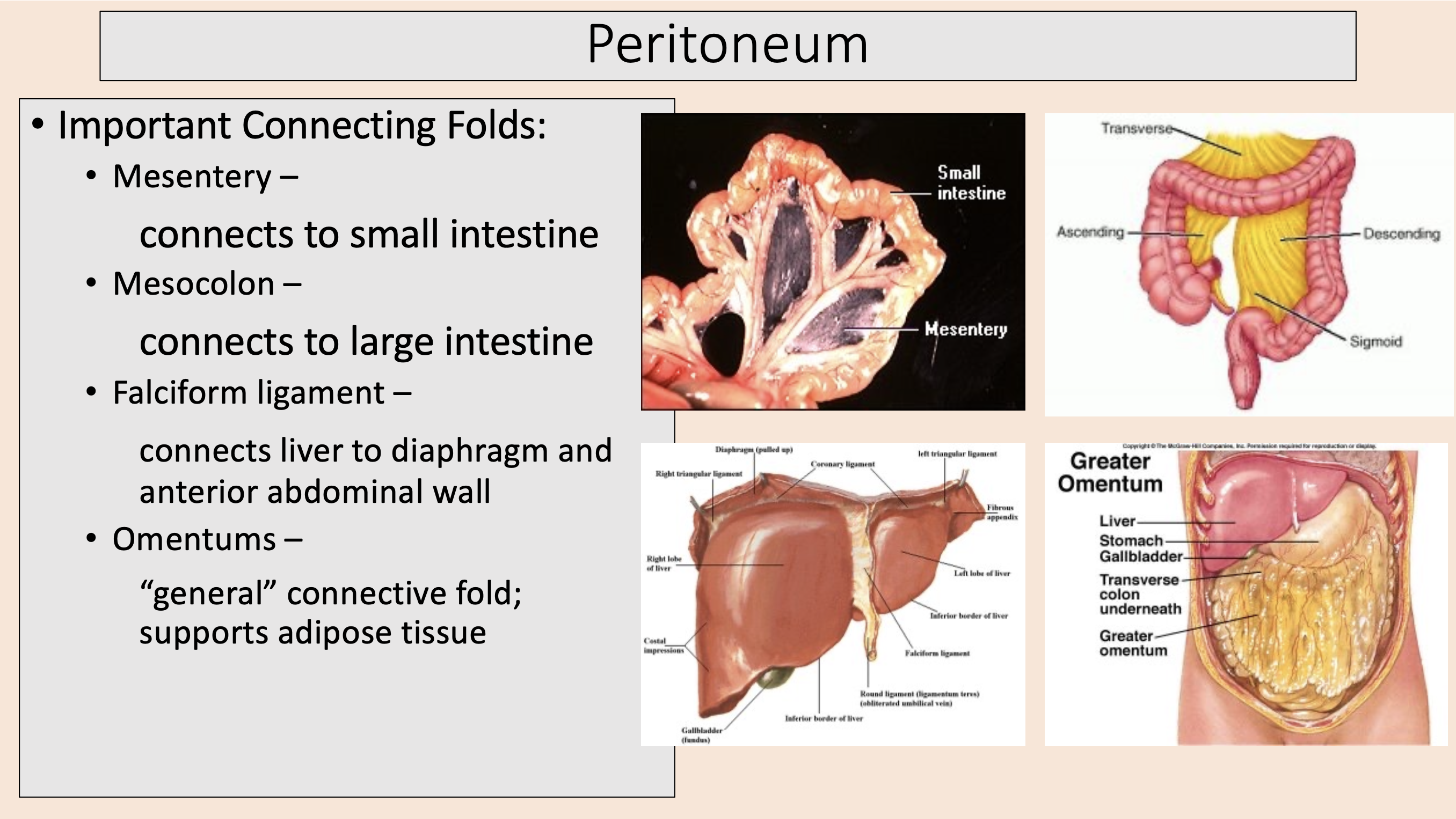
connects to small intestine
mesentery
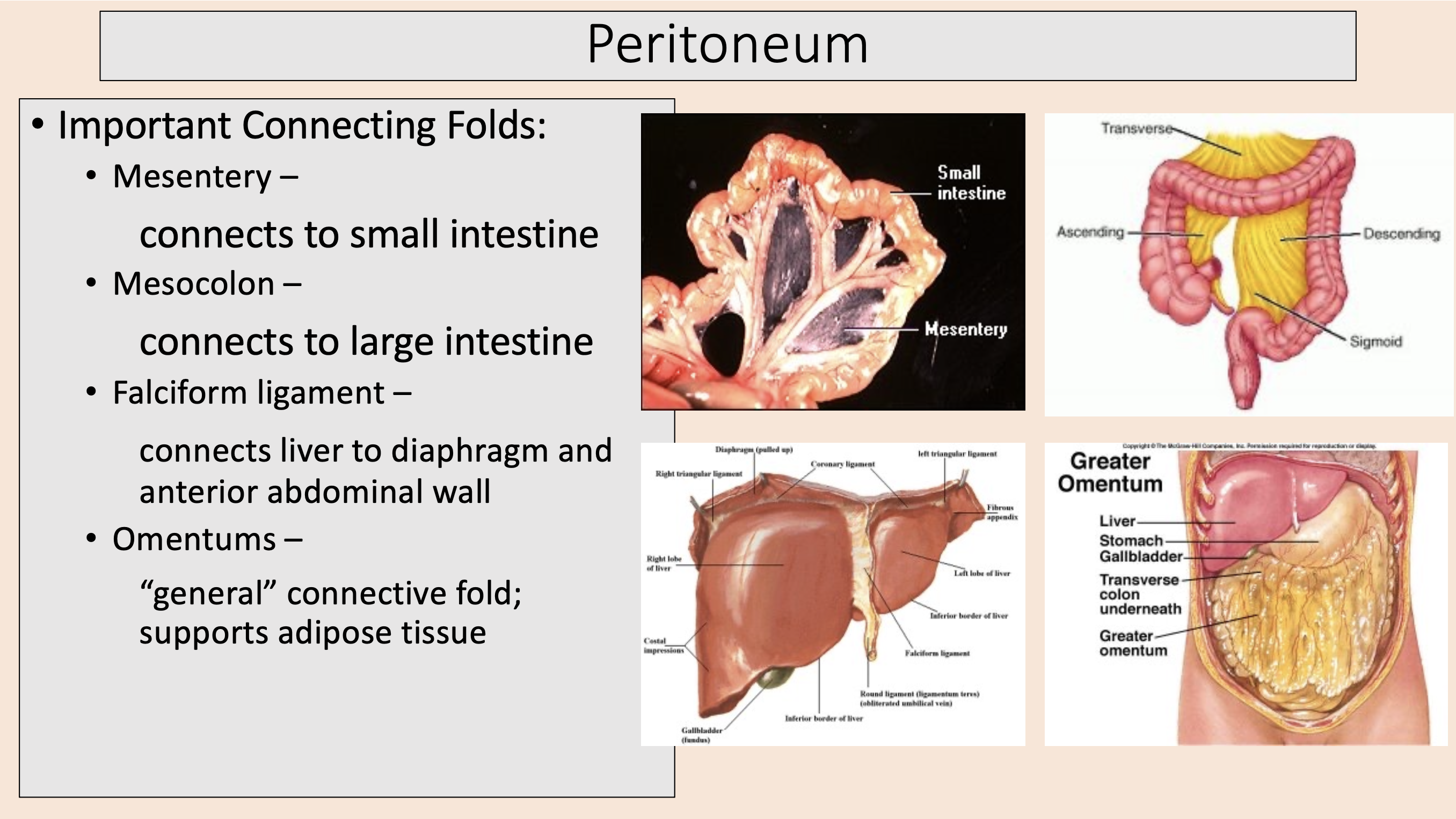
connects to large intestine
mesocolon
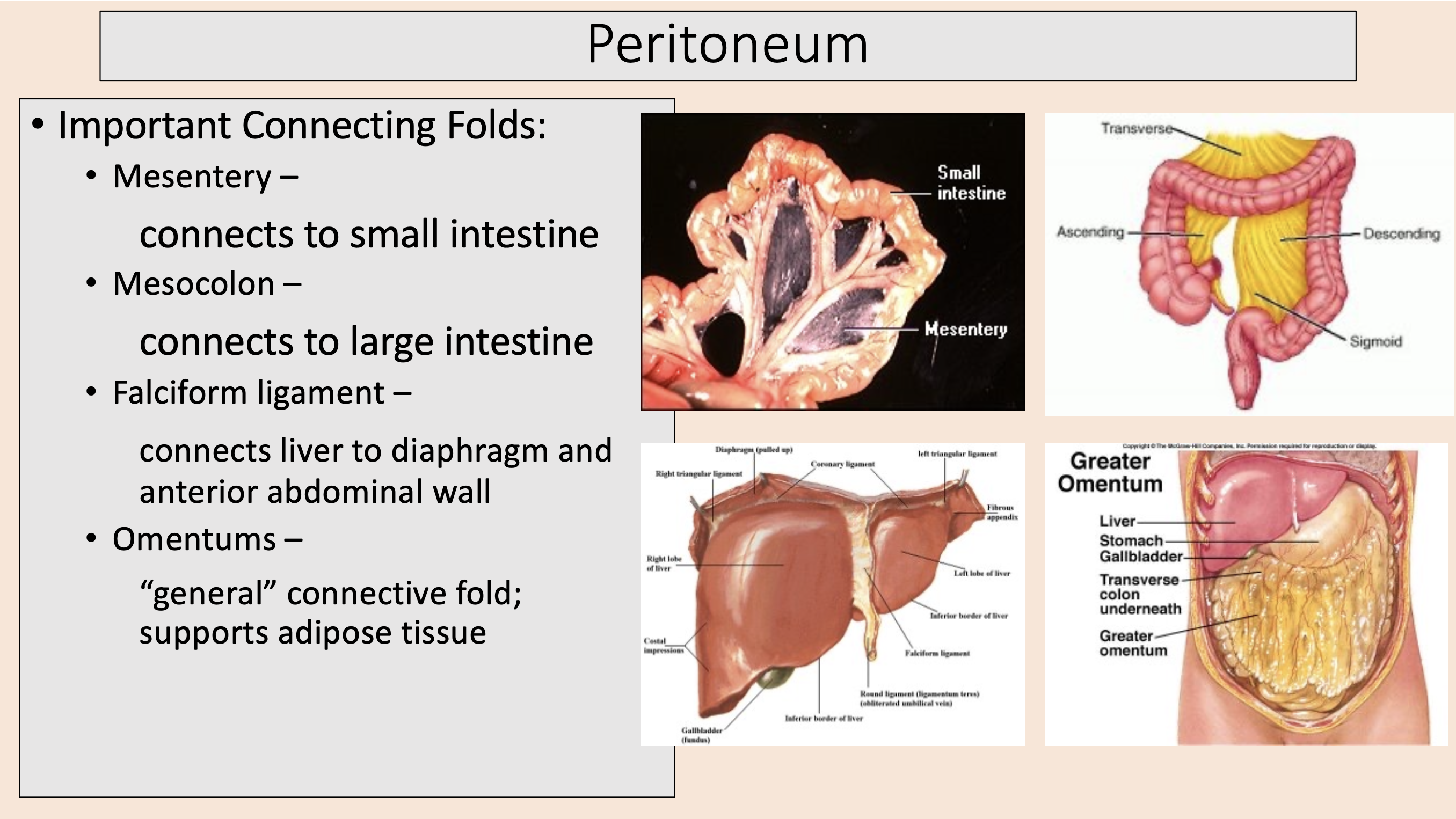
connects liver to diaphragm and anterior abdominal wall
falciform ligament
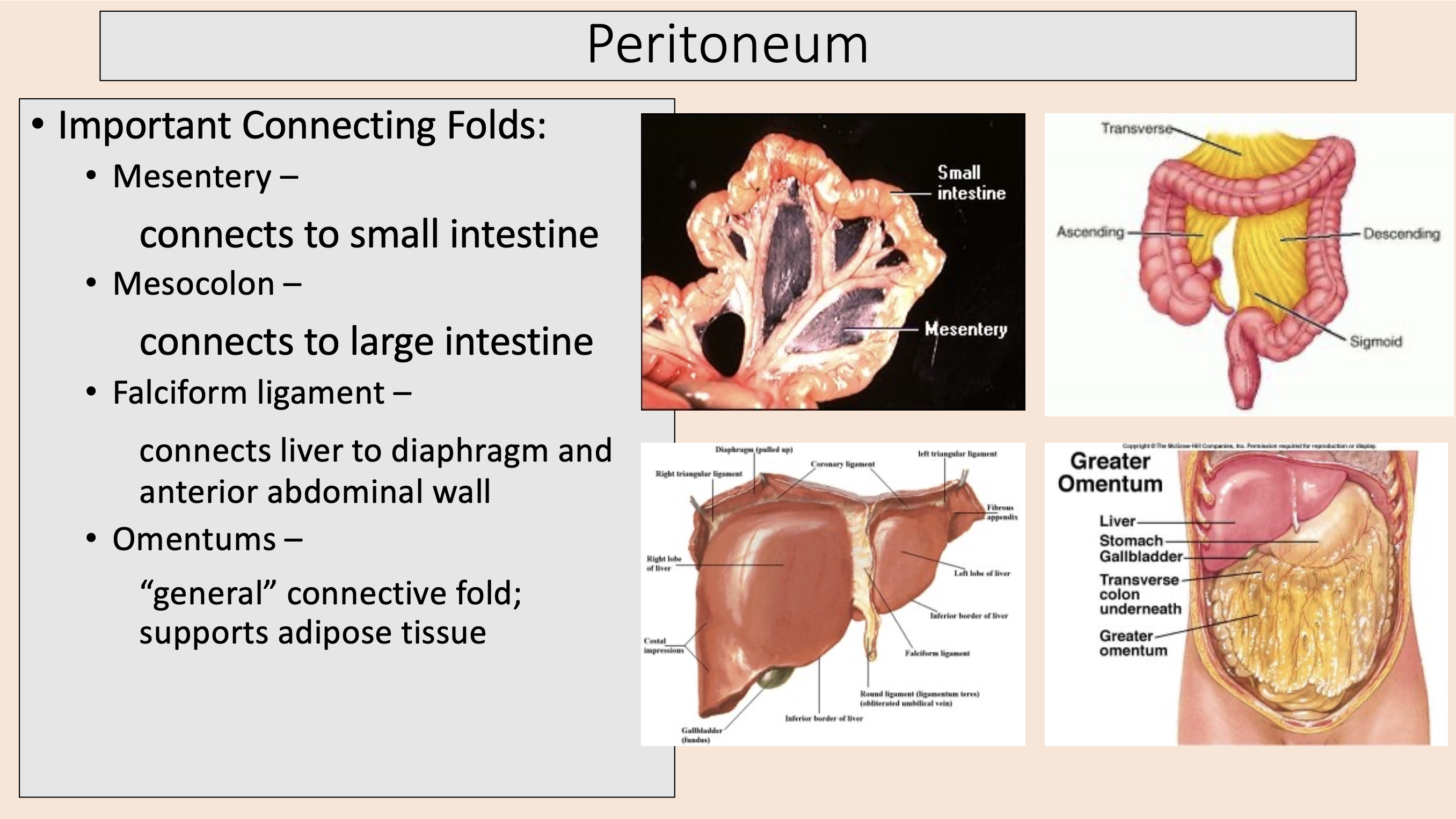
“general” connective fold; supports adipose tissue
omentums
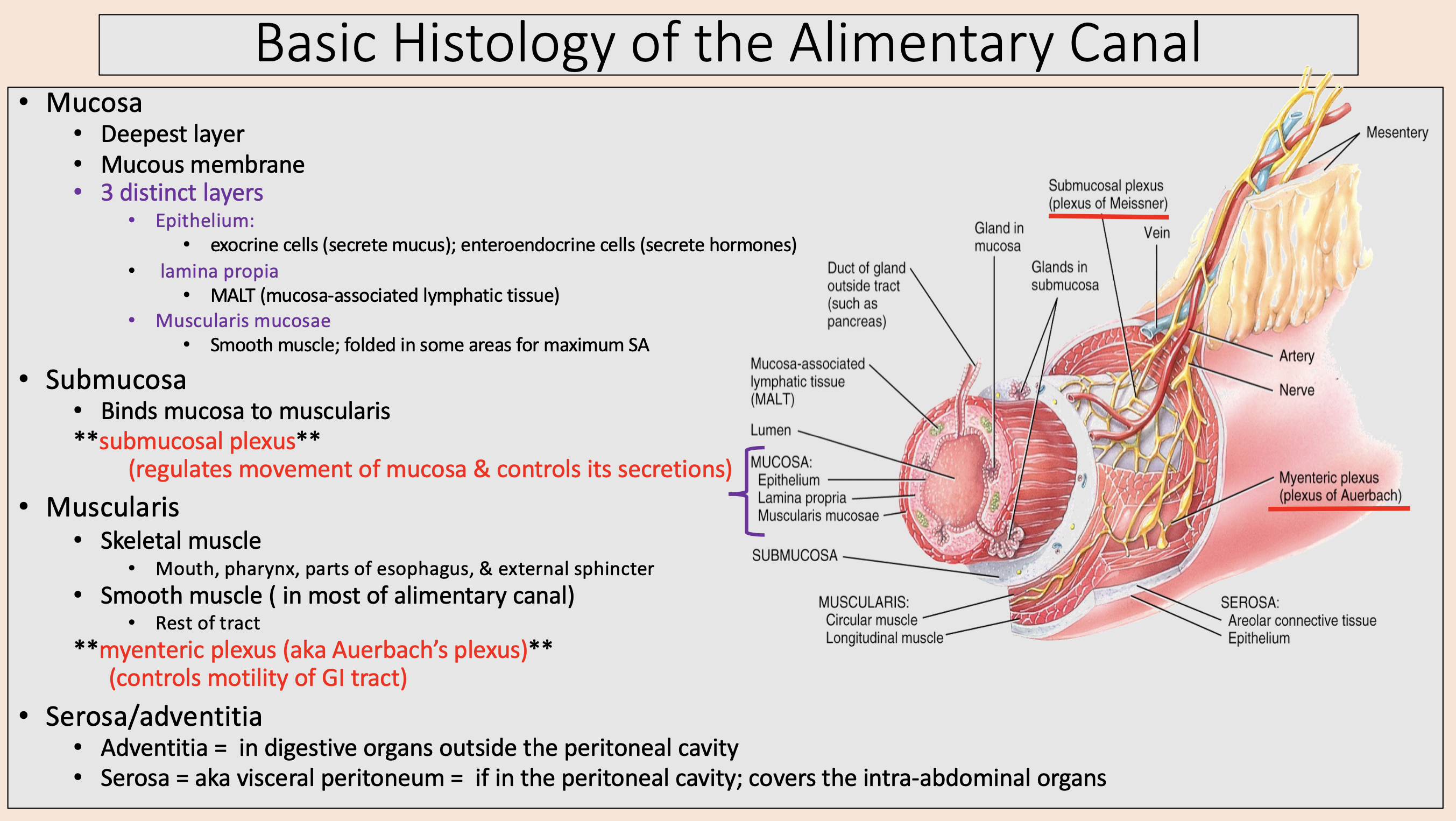
Deepest layer.
Mucous membrane.
mucosa
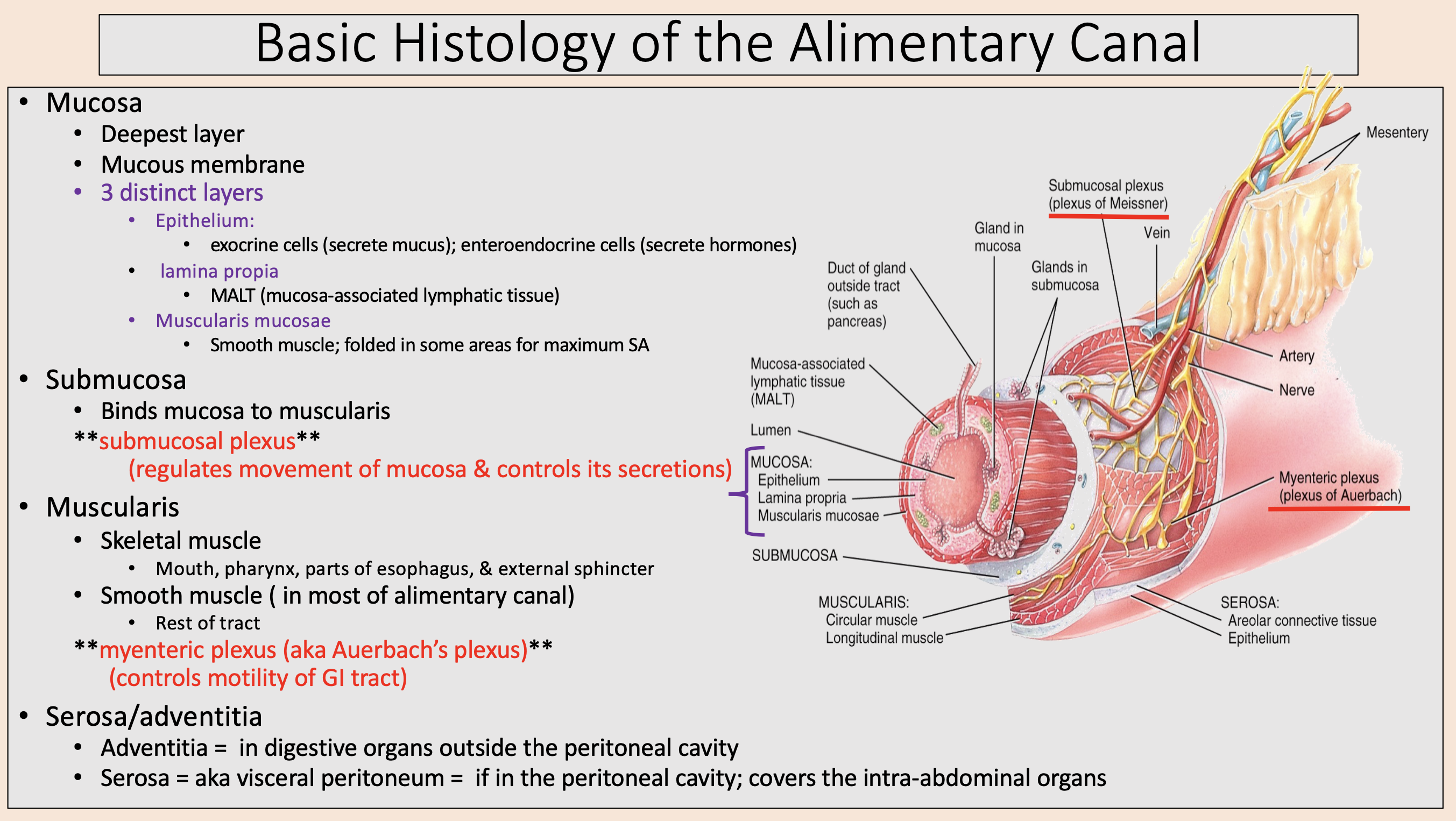
Mucosa 3 distinct layers:
epithelium
lamina propia
muscularis mucosae
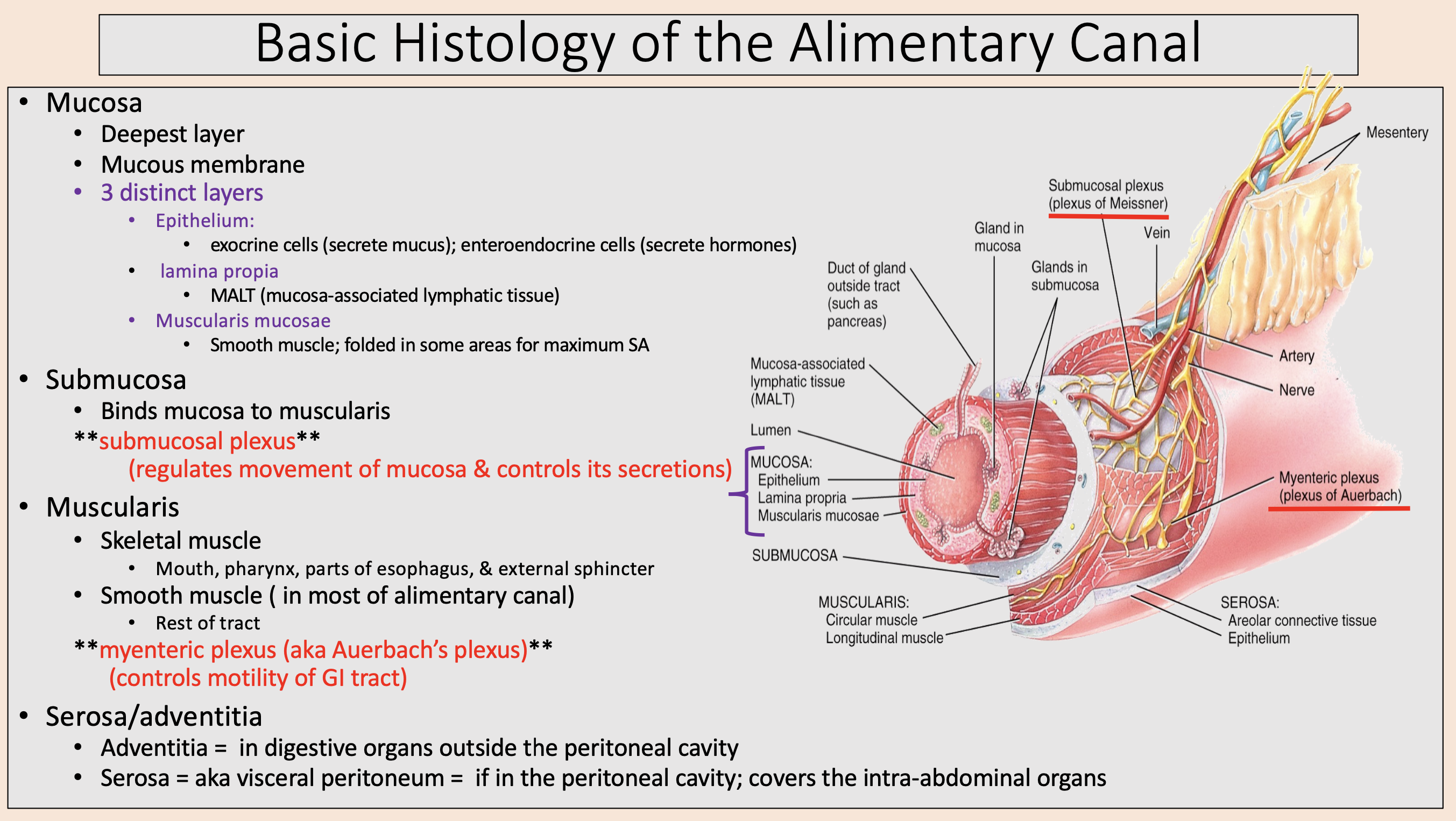
exocrine cells (secrete mucus); enteroendocrine cells (secrete hormones)
epithelium
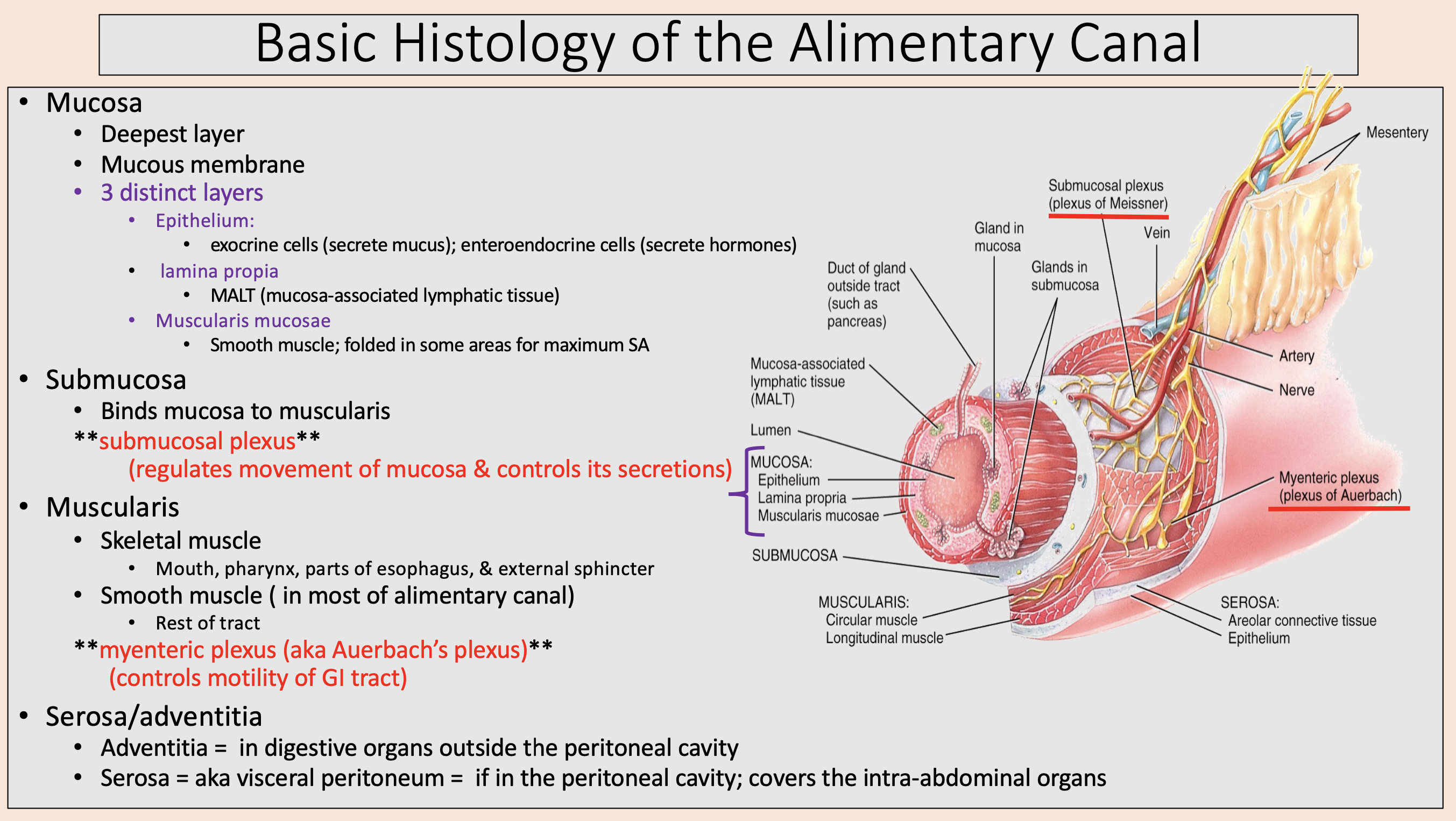
MALT (mucosa-associated lymphatic tissue)
lamina propia
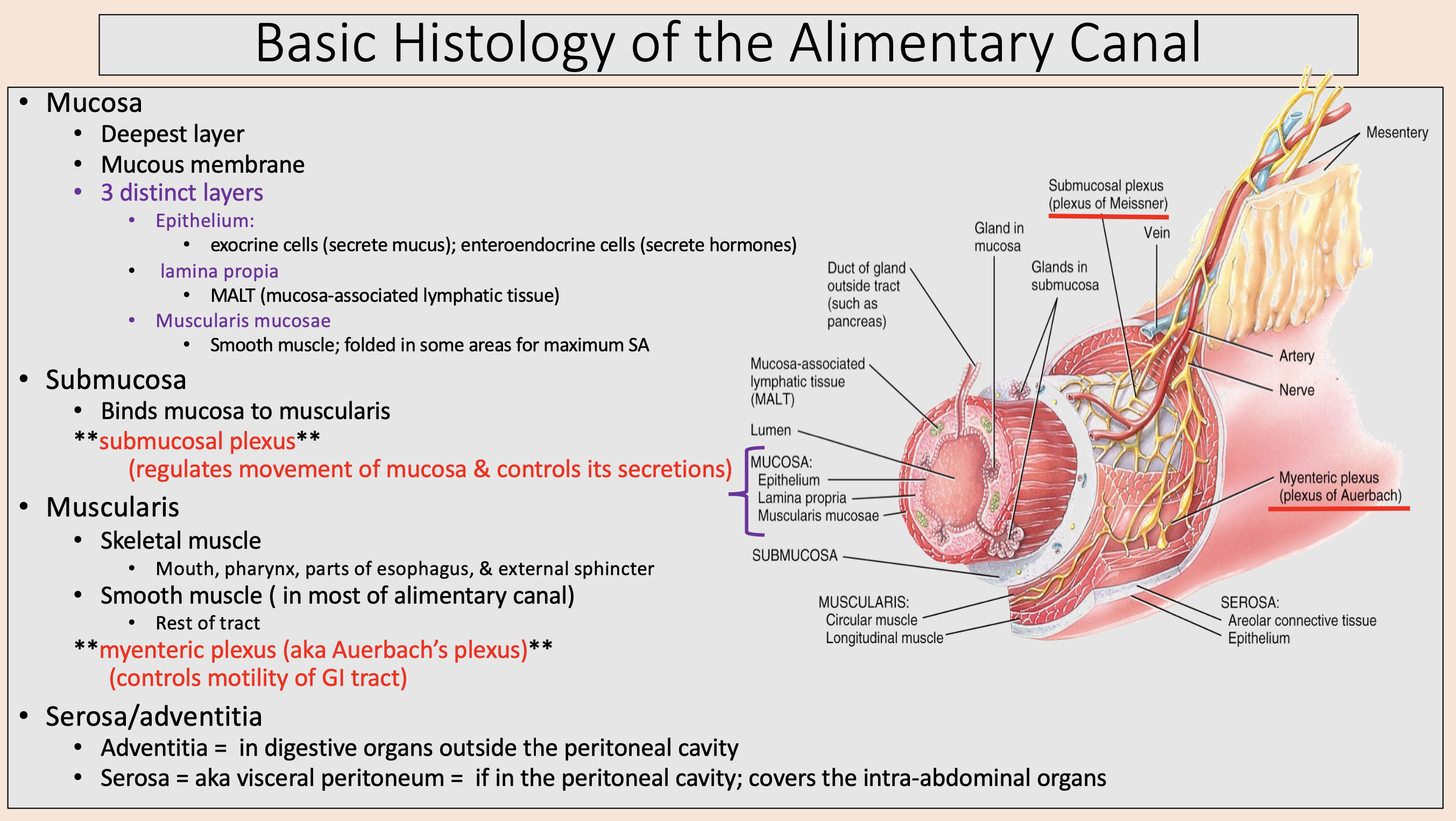
Smooth muscle; folded in some areas for maximum SA
muscularis mucosae
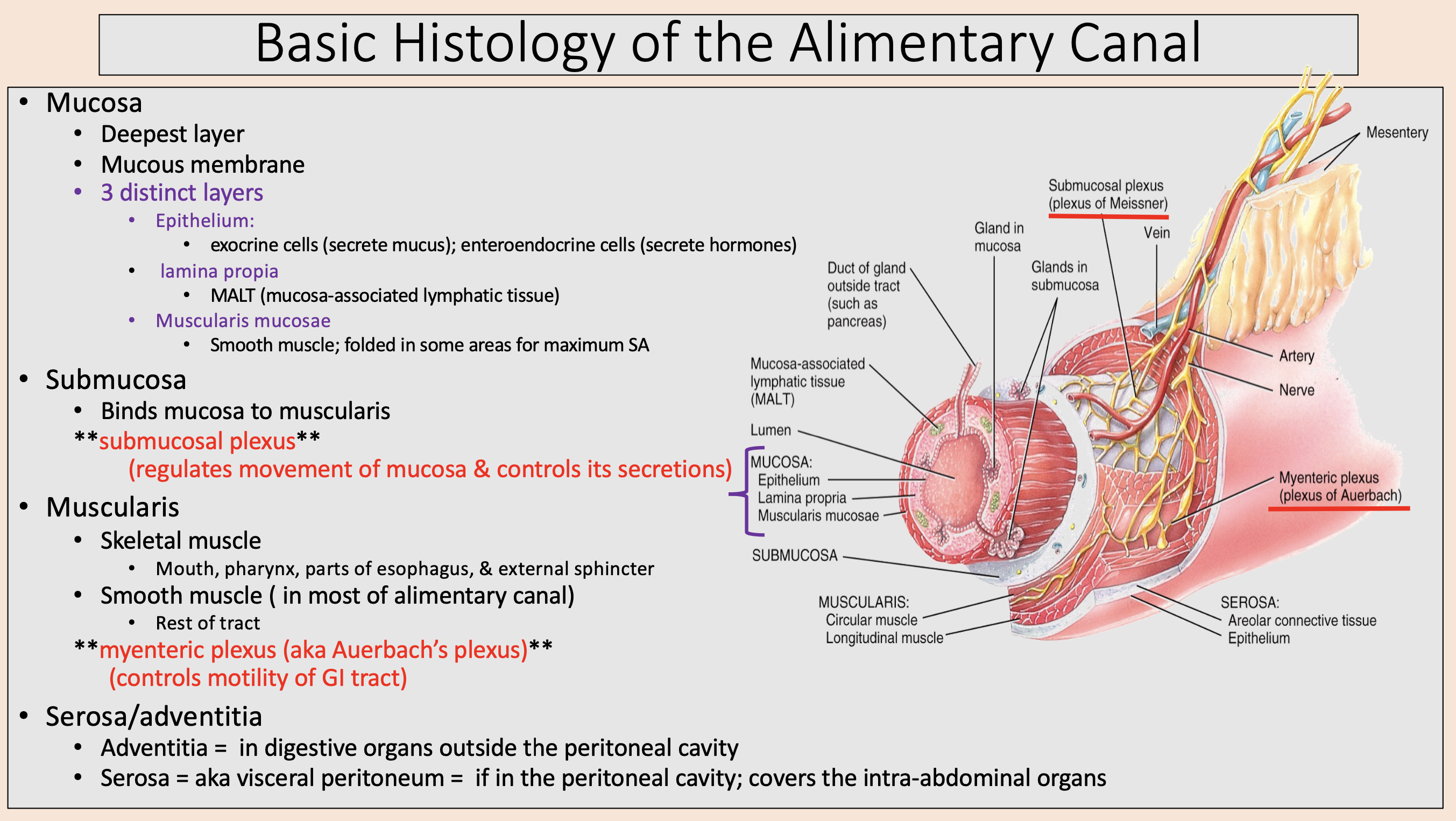
Binds mucosa to muscularis
submucosa
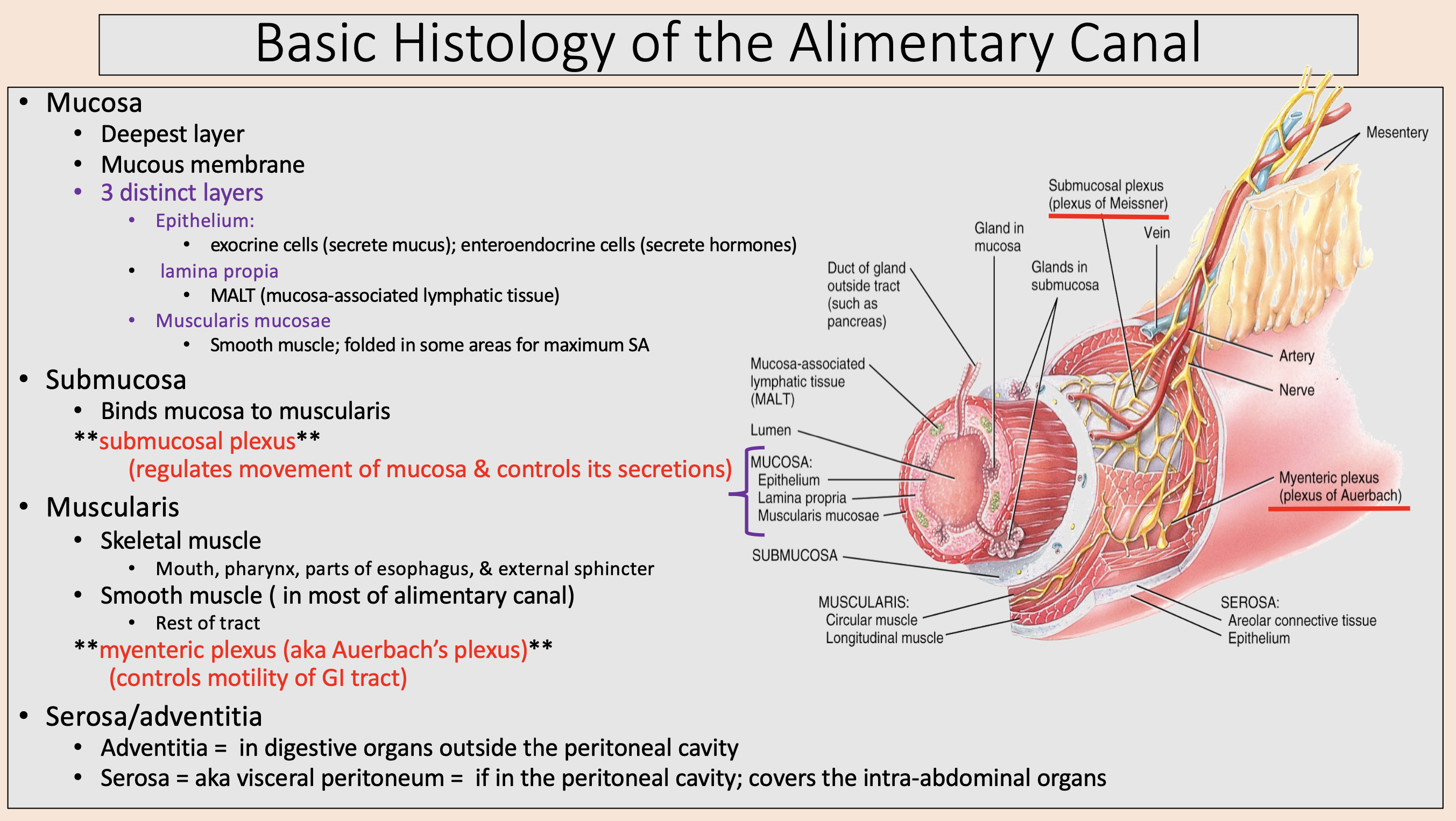
regulates movement of mucosa & controls its secretions
submucosal plexus
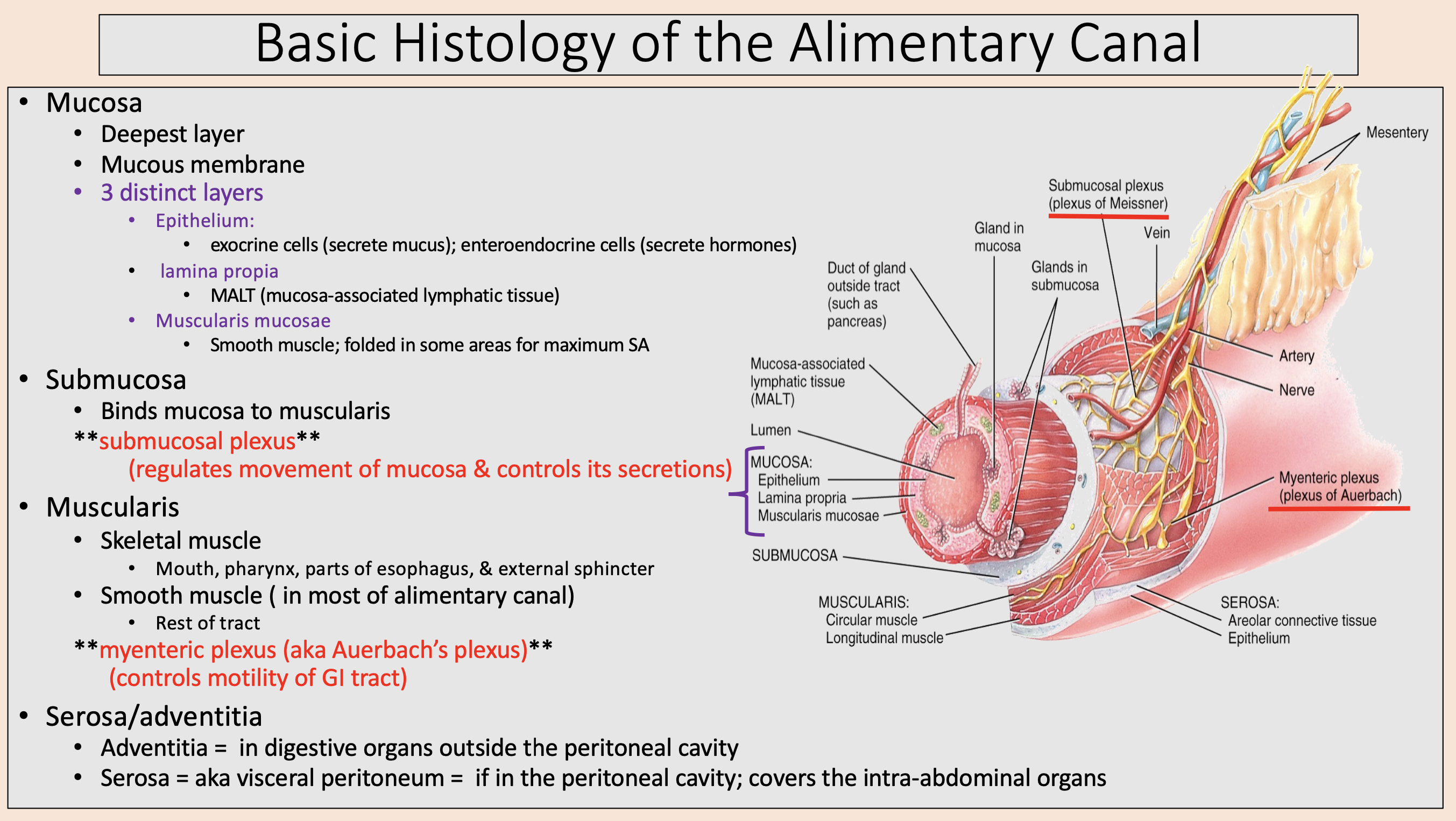
Skeletal muscle.
Smooth muscle ( in most of alimentary canal).
muscularis
Mouth, pharynx, parts of esophagus, & external sphincter
skeletal muscle
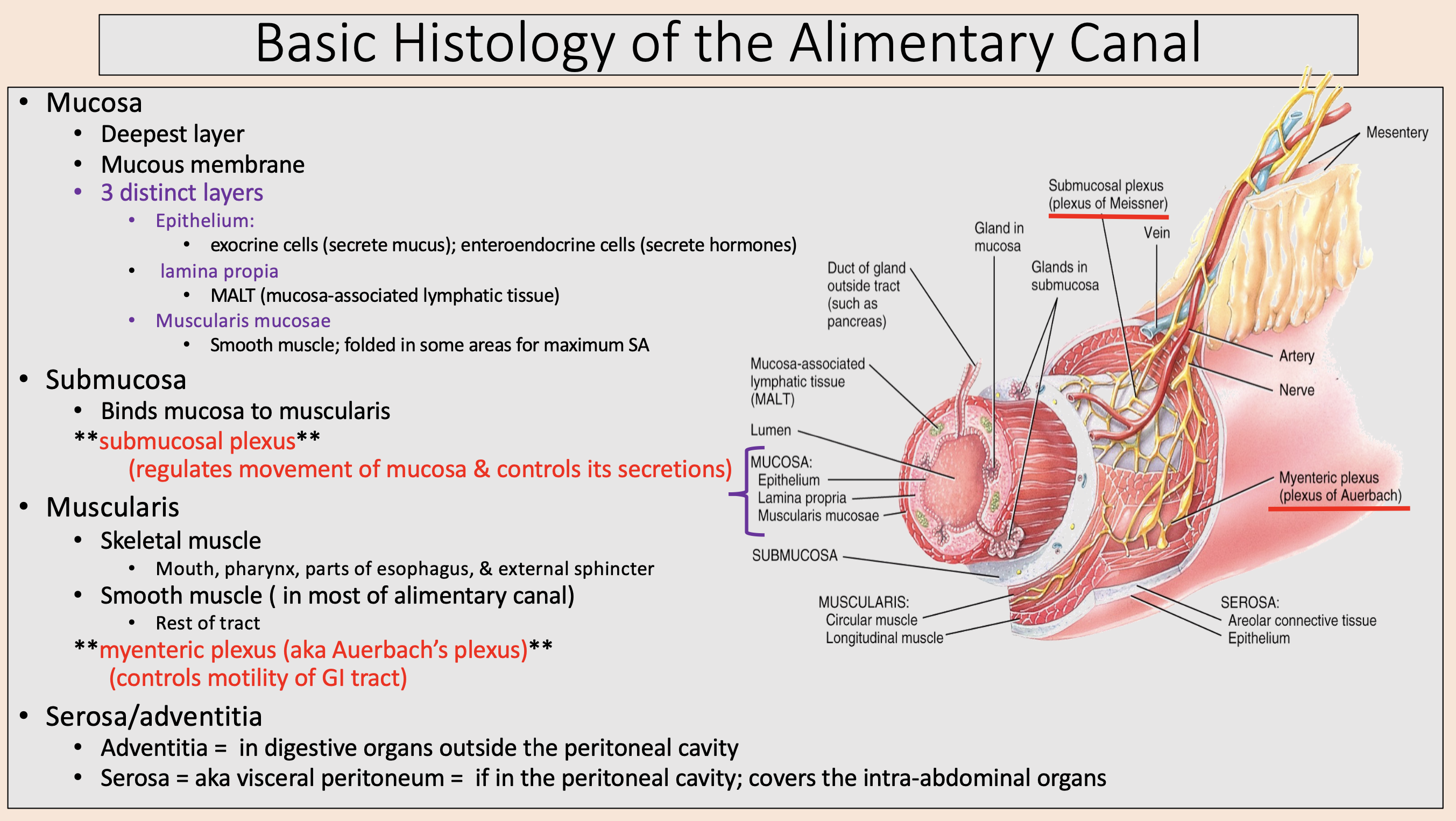
aka Auerbach’s plexus
myenteric plexus
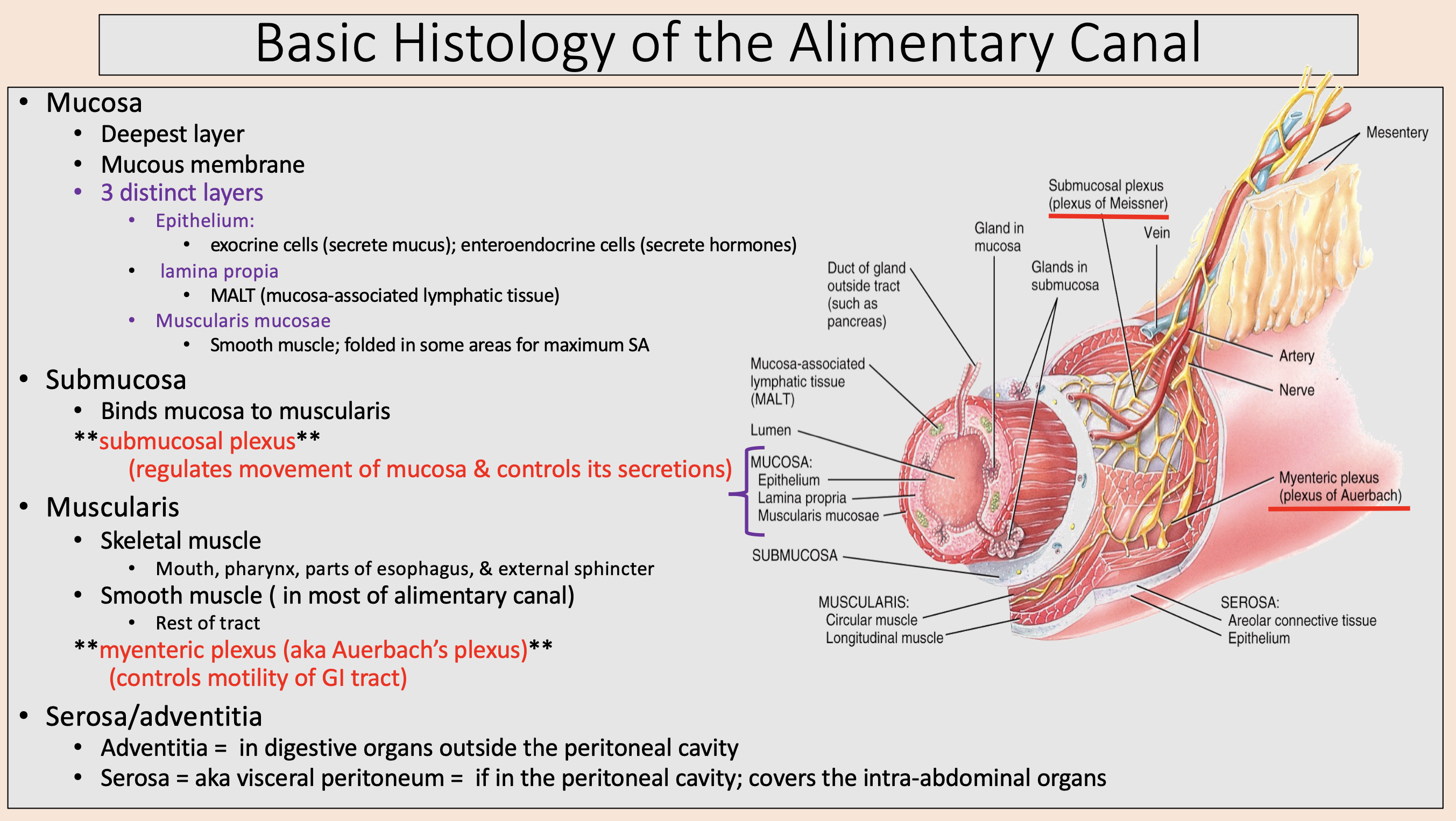
controls motility of GI tract
myenteric plexus
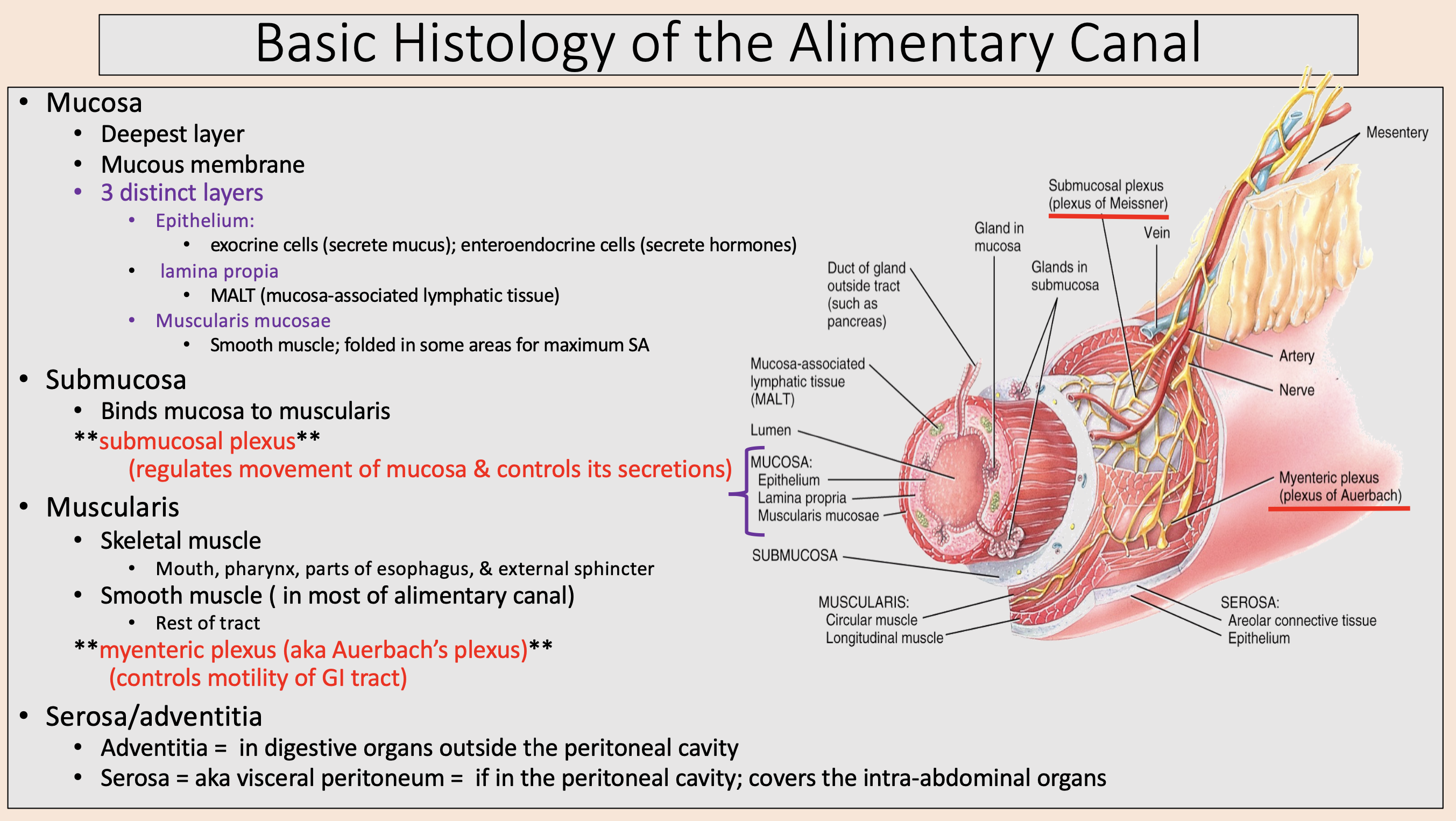
in digestive organs outside the peritoneal cavity
adventitia
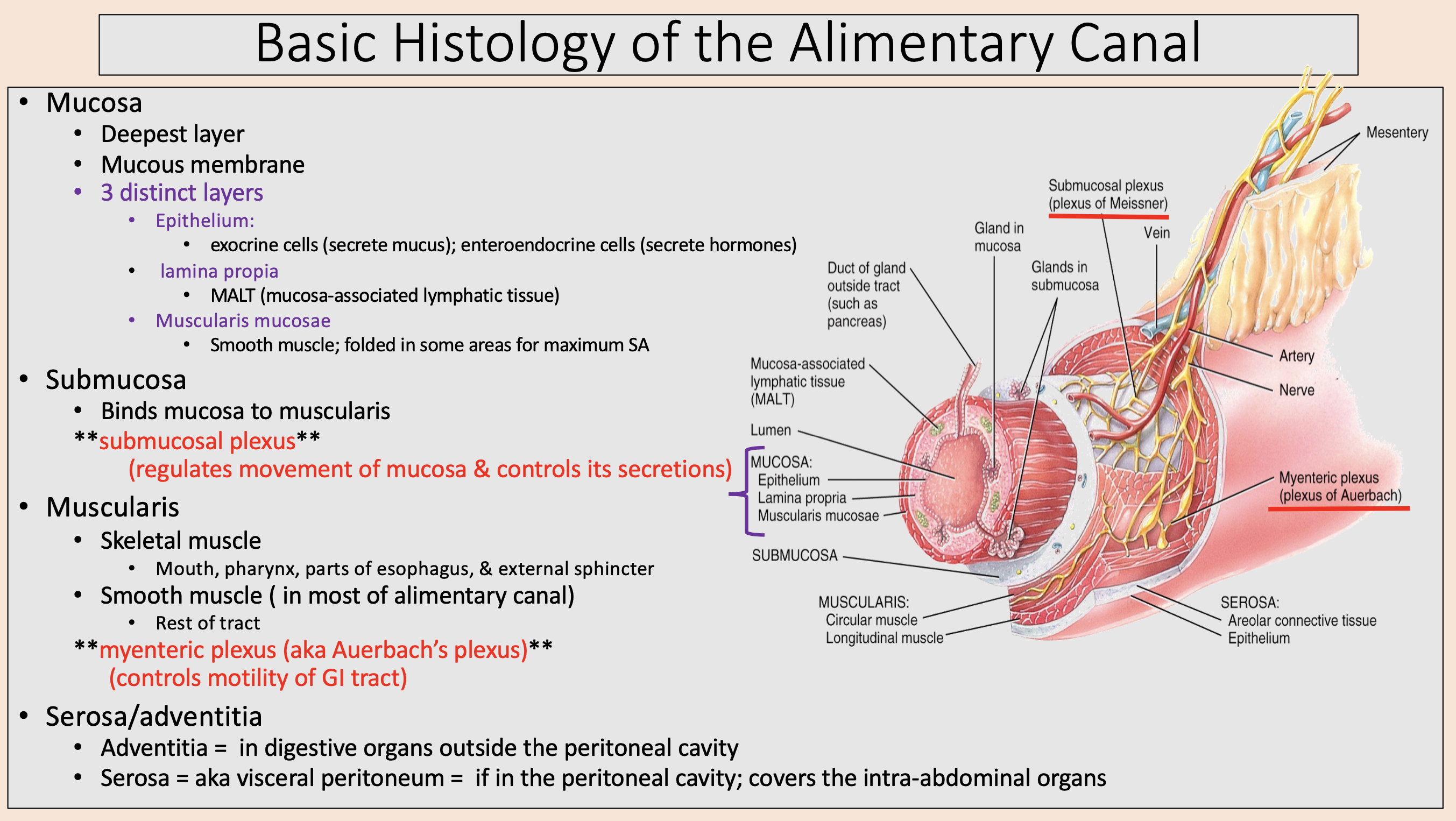
aka visceral peritoneum
serosa
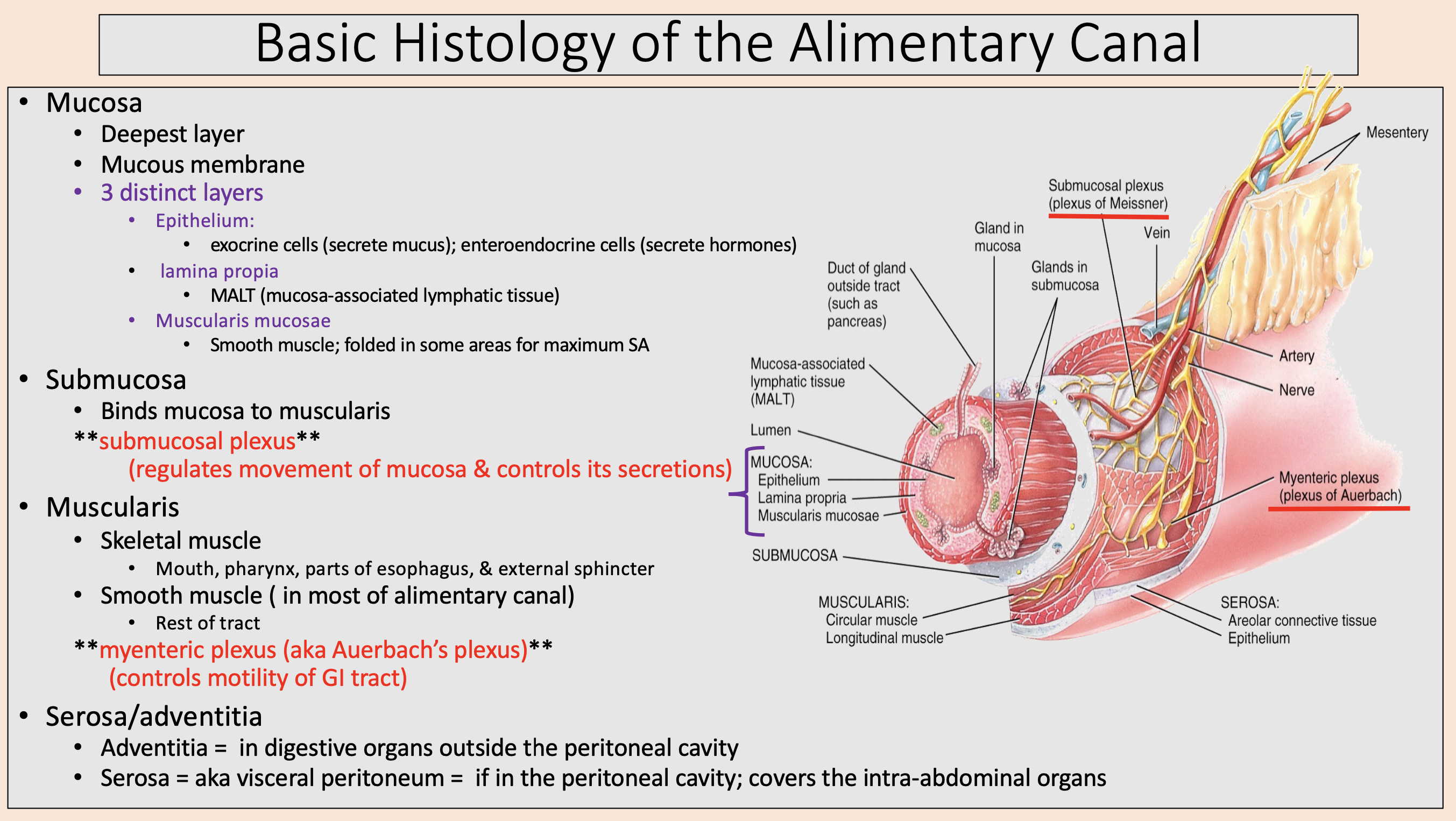
if in the peritoneal cavity; covers the intra-abdominal organs
serosa
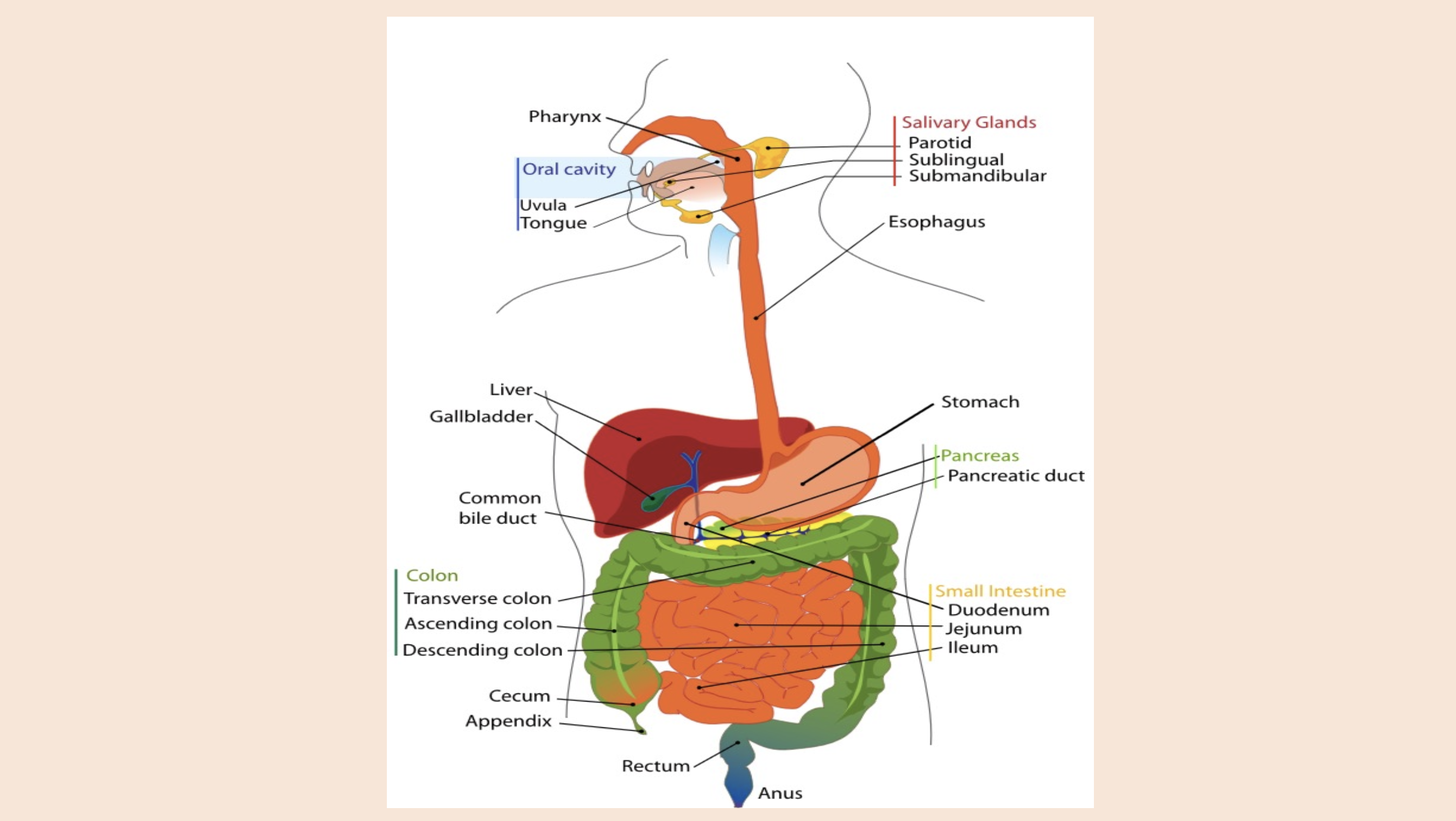
Oral cavity
uvula
tongue
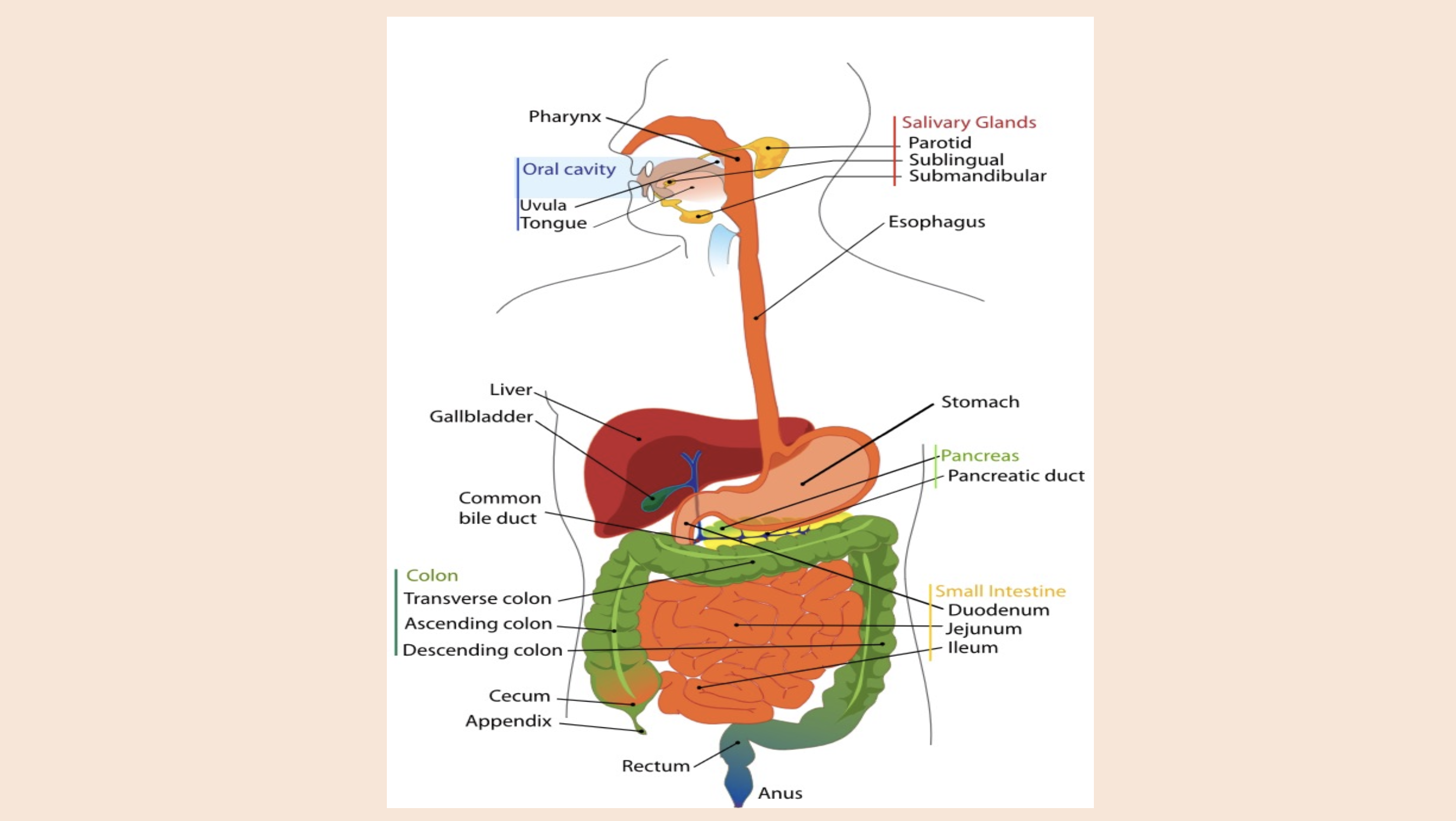
Salivary Glands
parotid
sublingual
submandibular
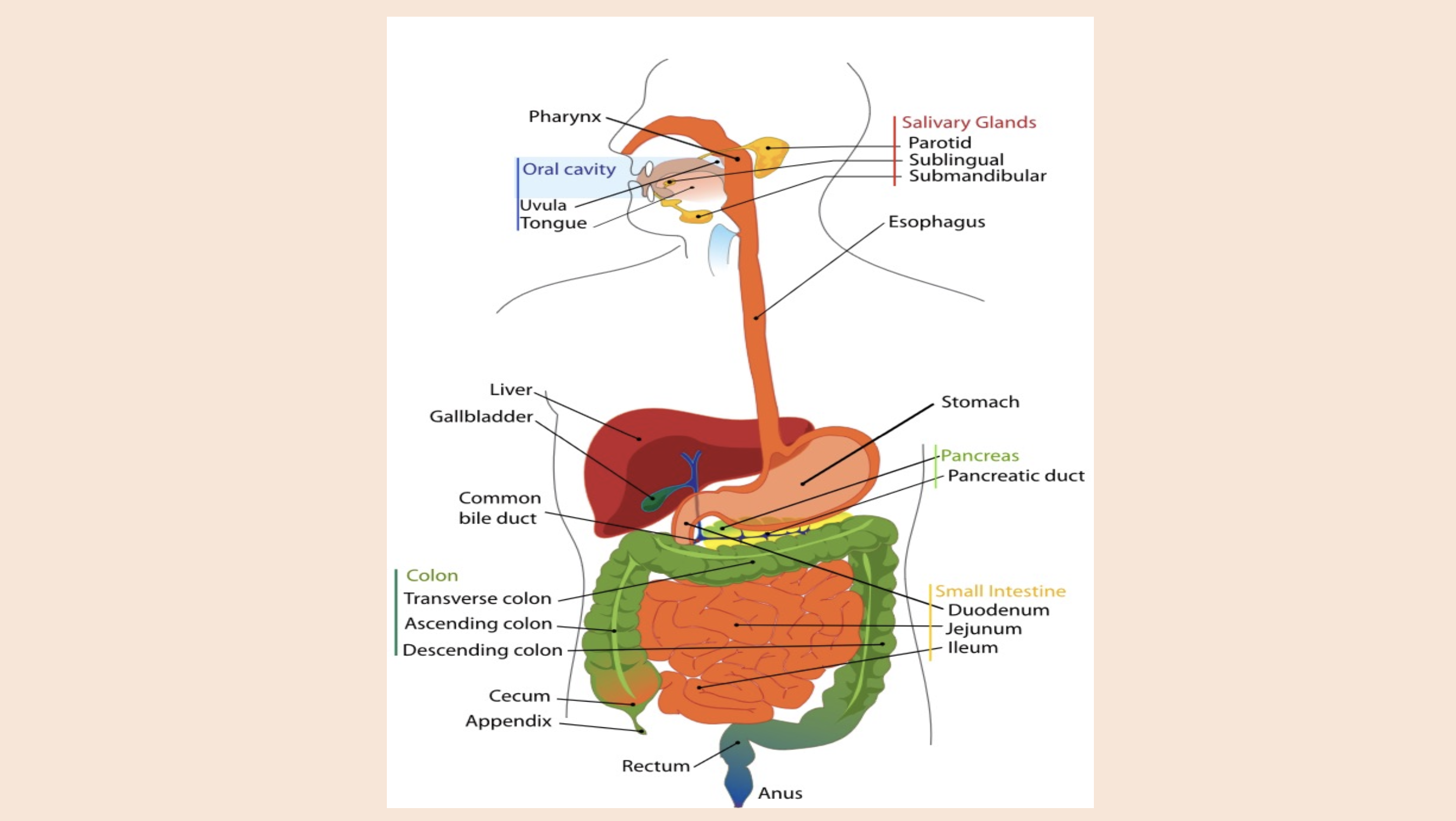
Pancreas
pancreatic duct
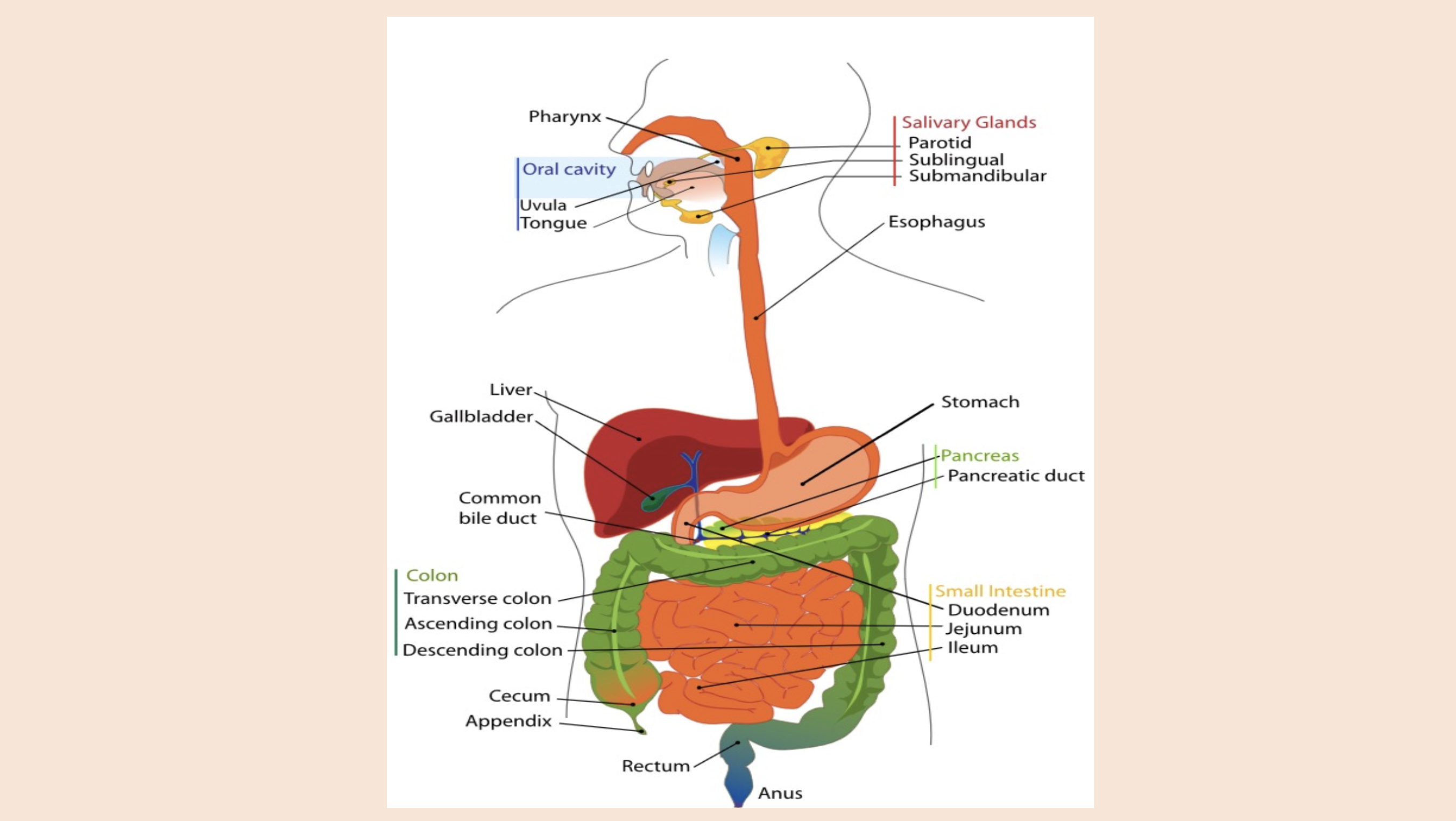
Colon
transverse colon
ascending colon
descending colon
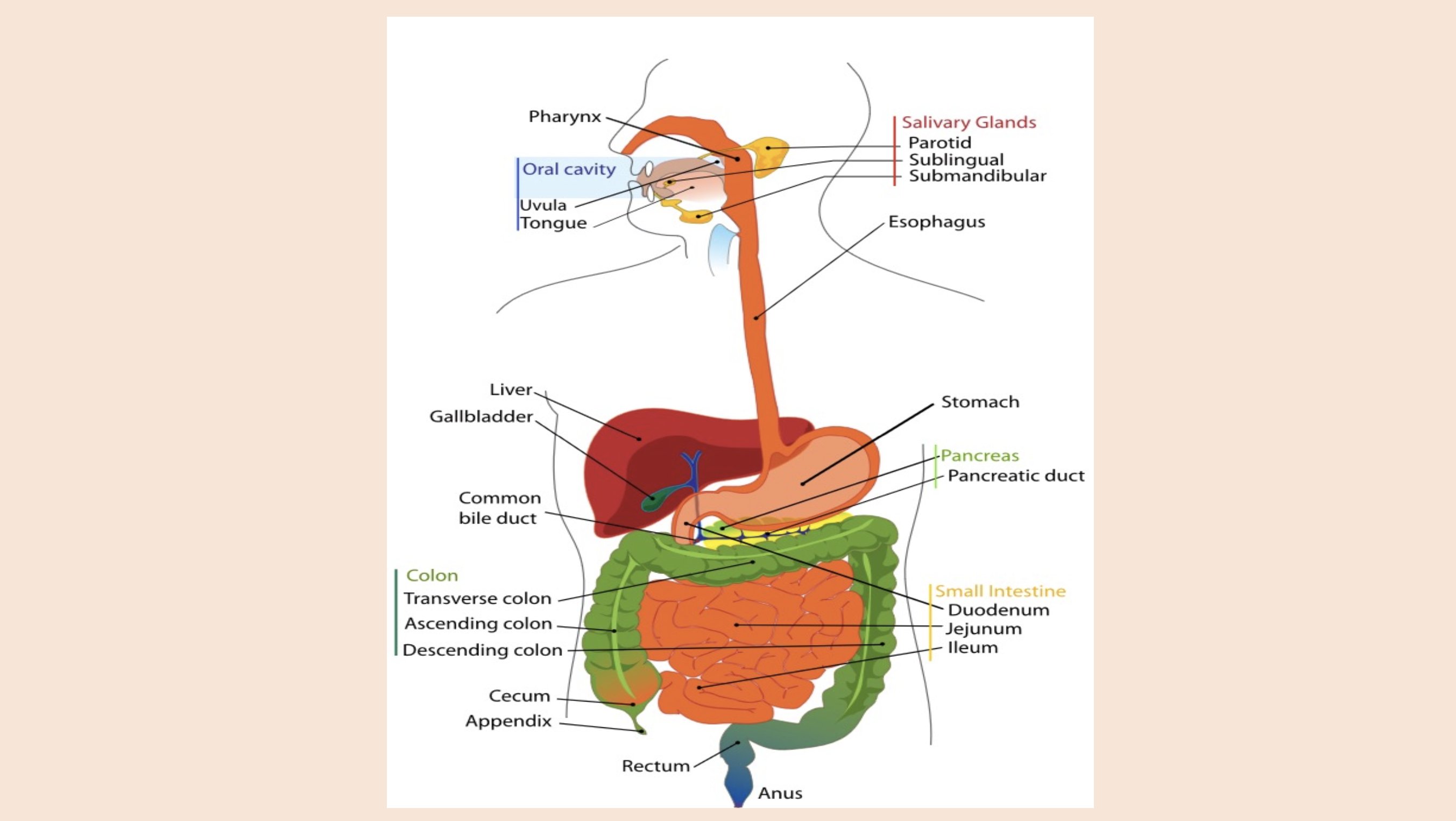
Small intestine
duodenum
jejunum
ileum
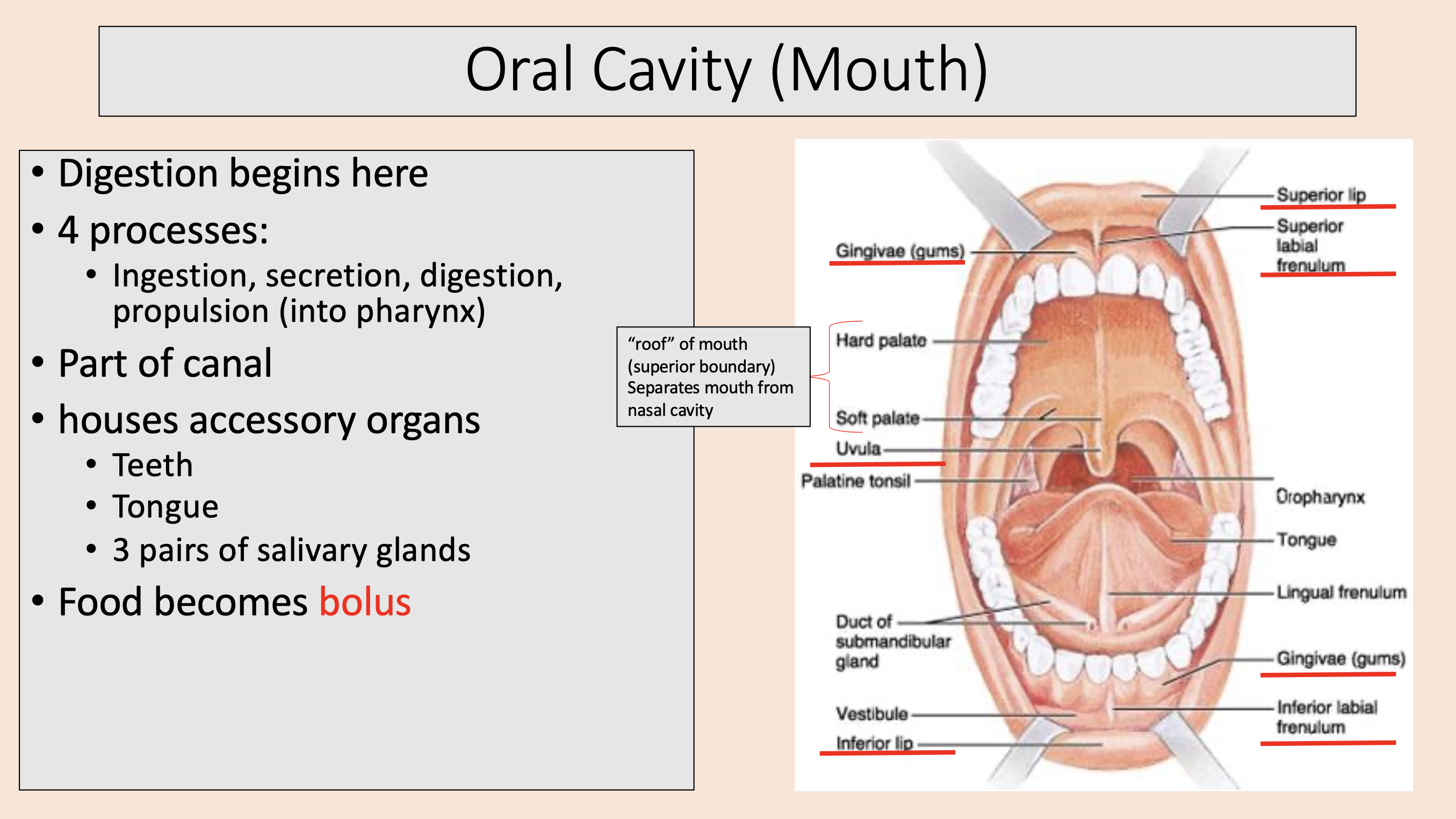
Digestion begins here.
Ingestion.
Secretion.
Digestion.
Propulsion (into pharynx).
Part of canal.
Houses teeth, tongue, 3 pairs of salivary glands.
Food becomes bolus.
oral cavity or mouth
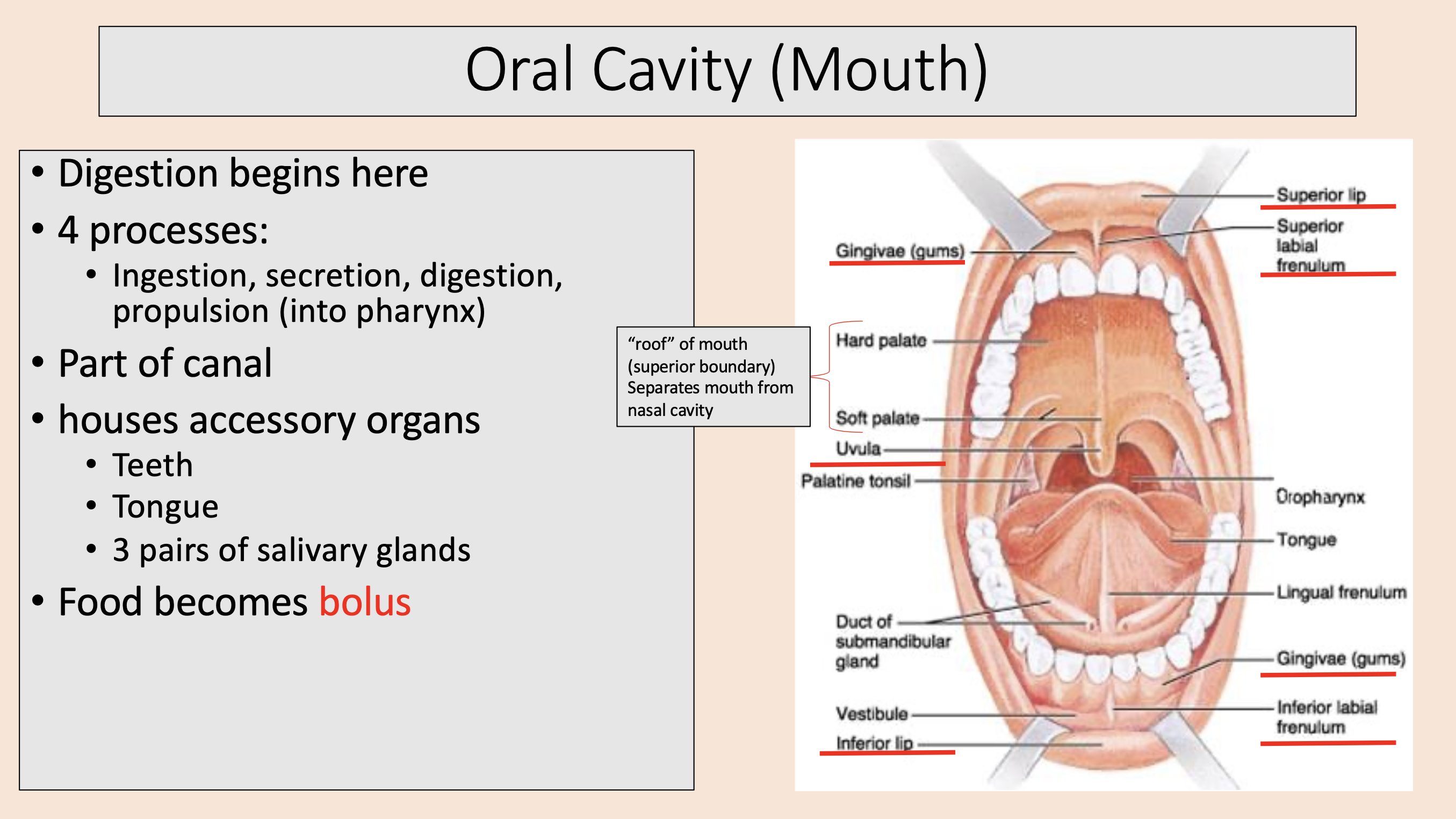
Food becomes
bolus
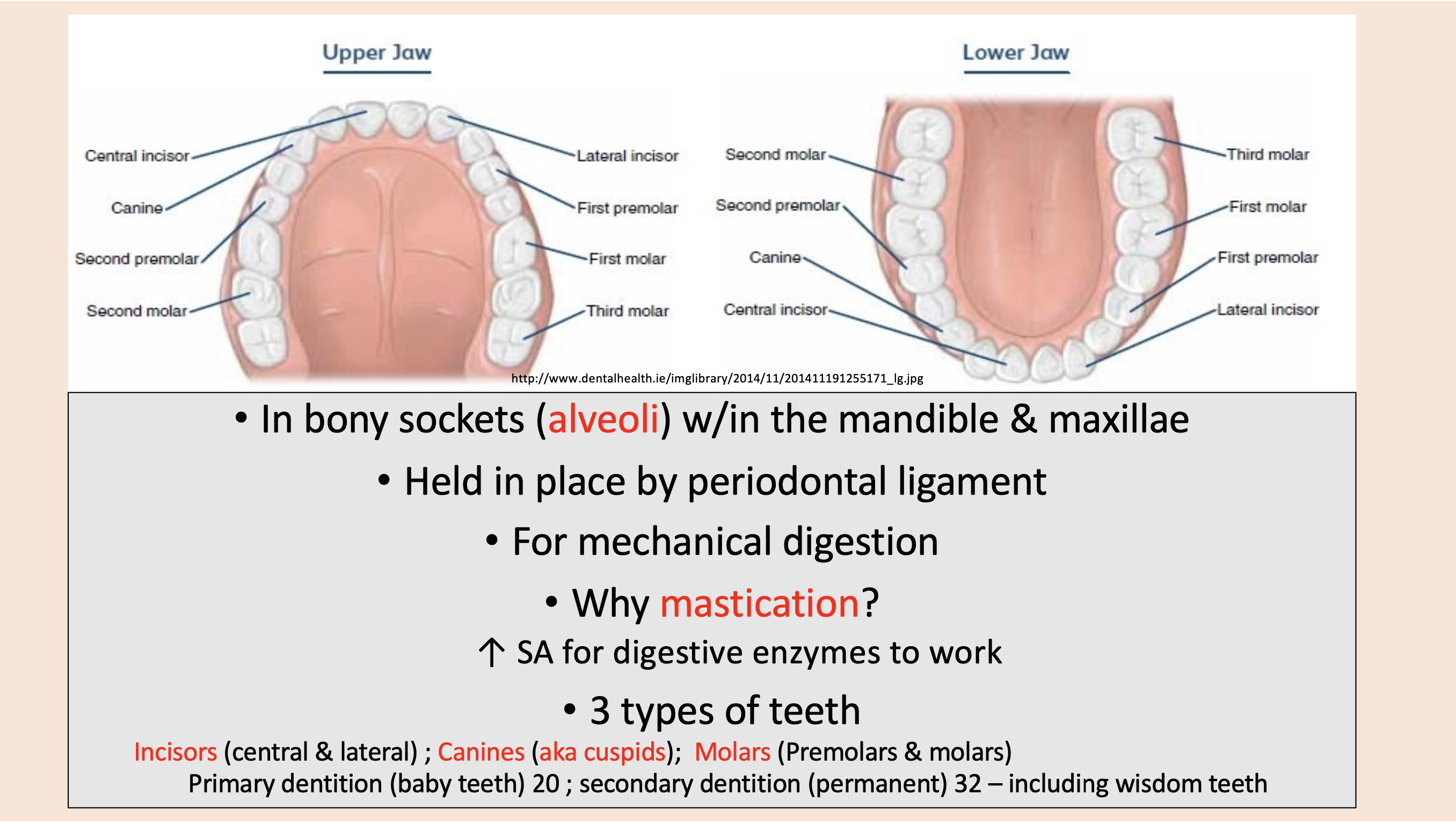
Central and lateral
incisors
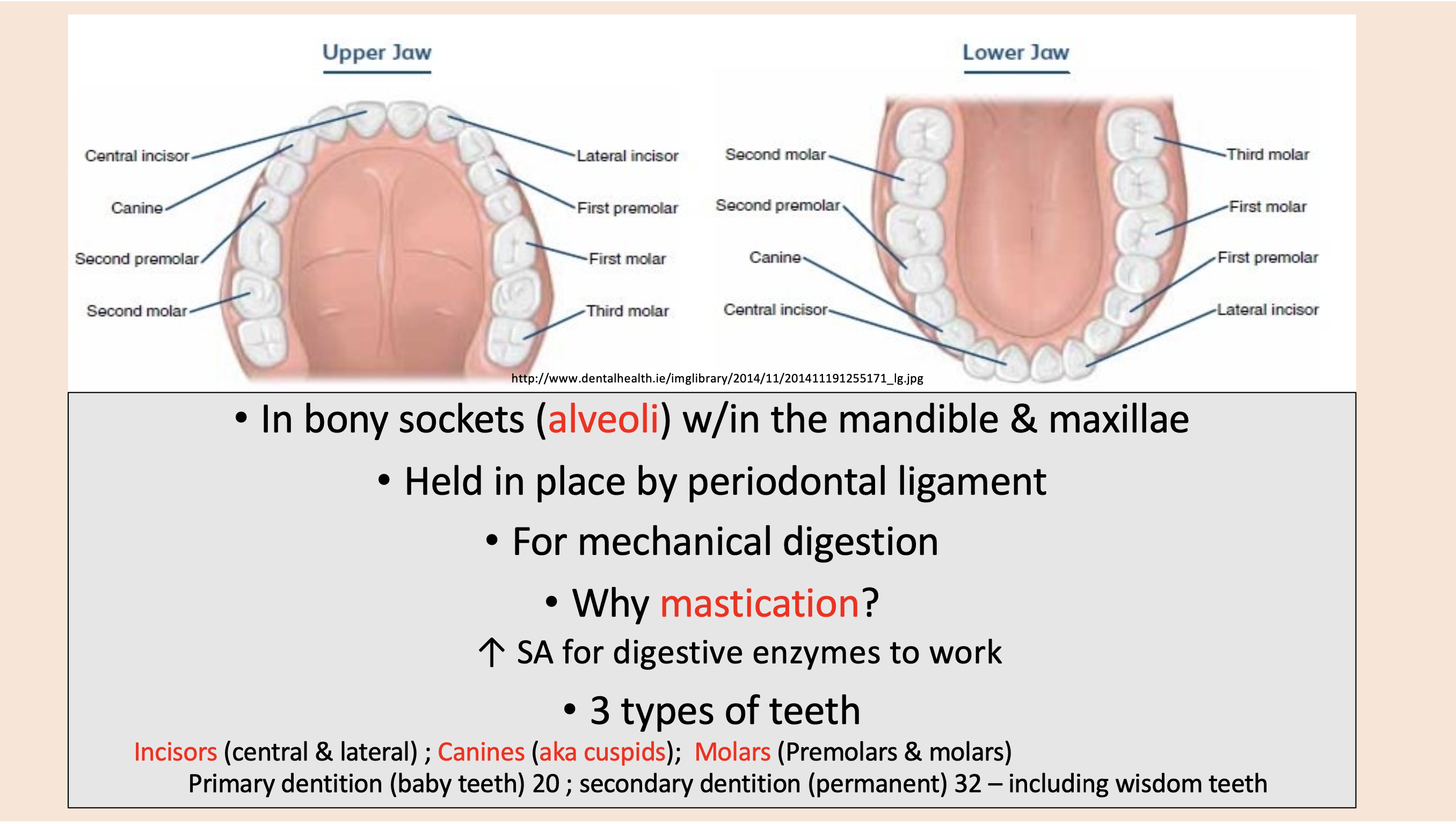
aka cuspids
canines
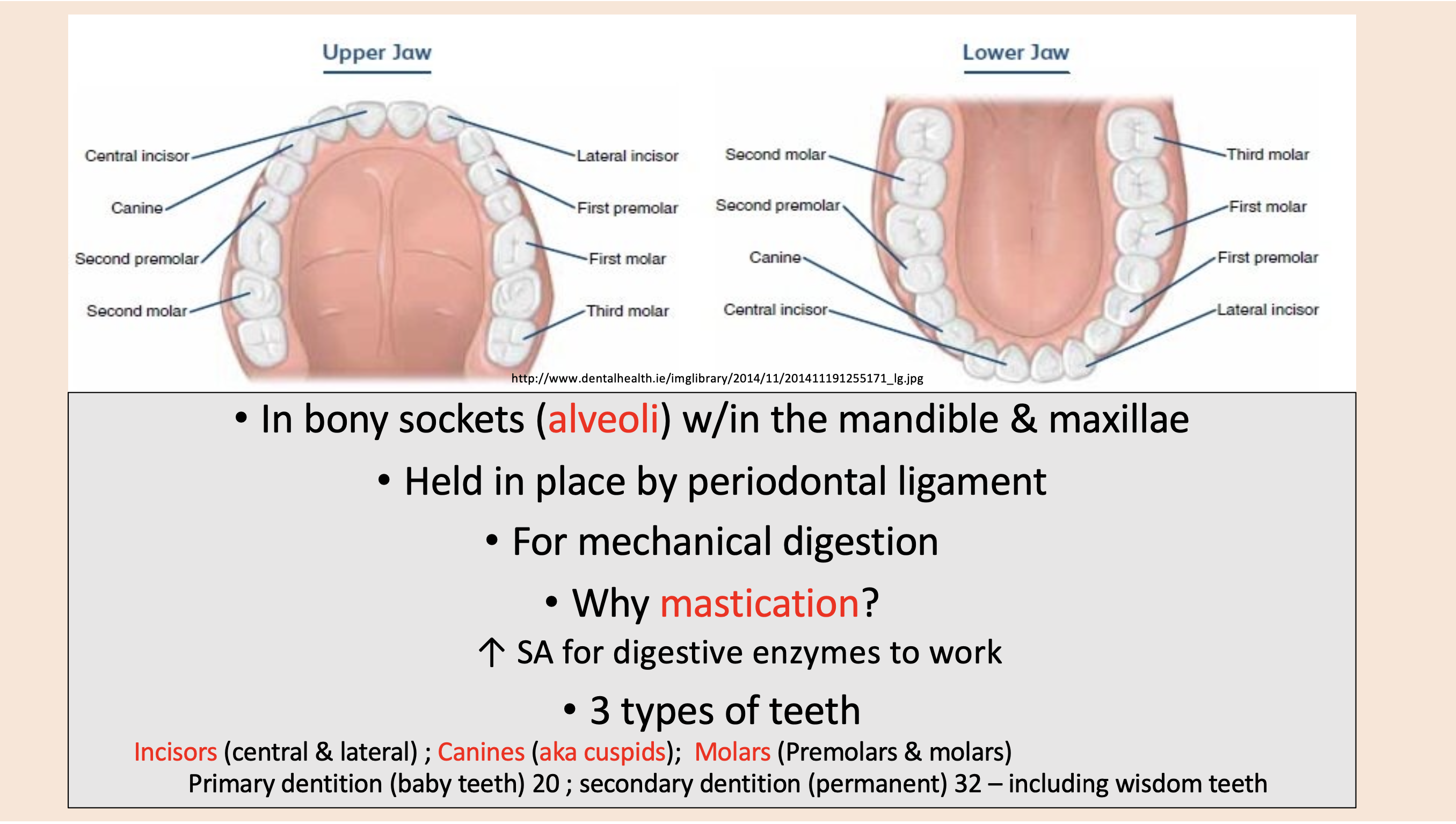
Premolars and molars
molars
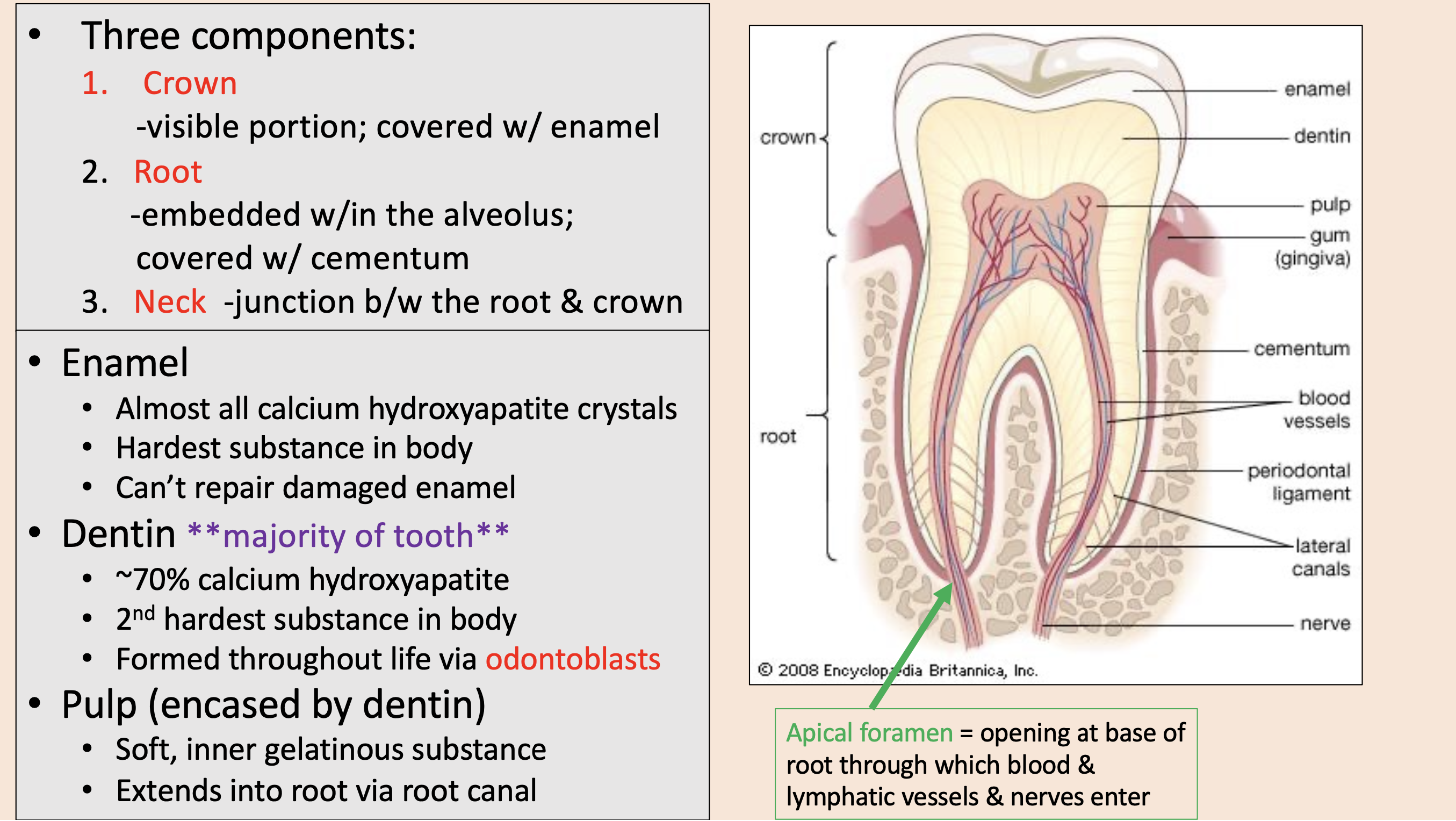
Three components of teeth:
crown
root
neck
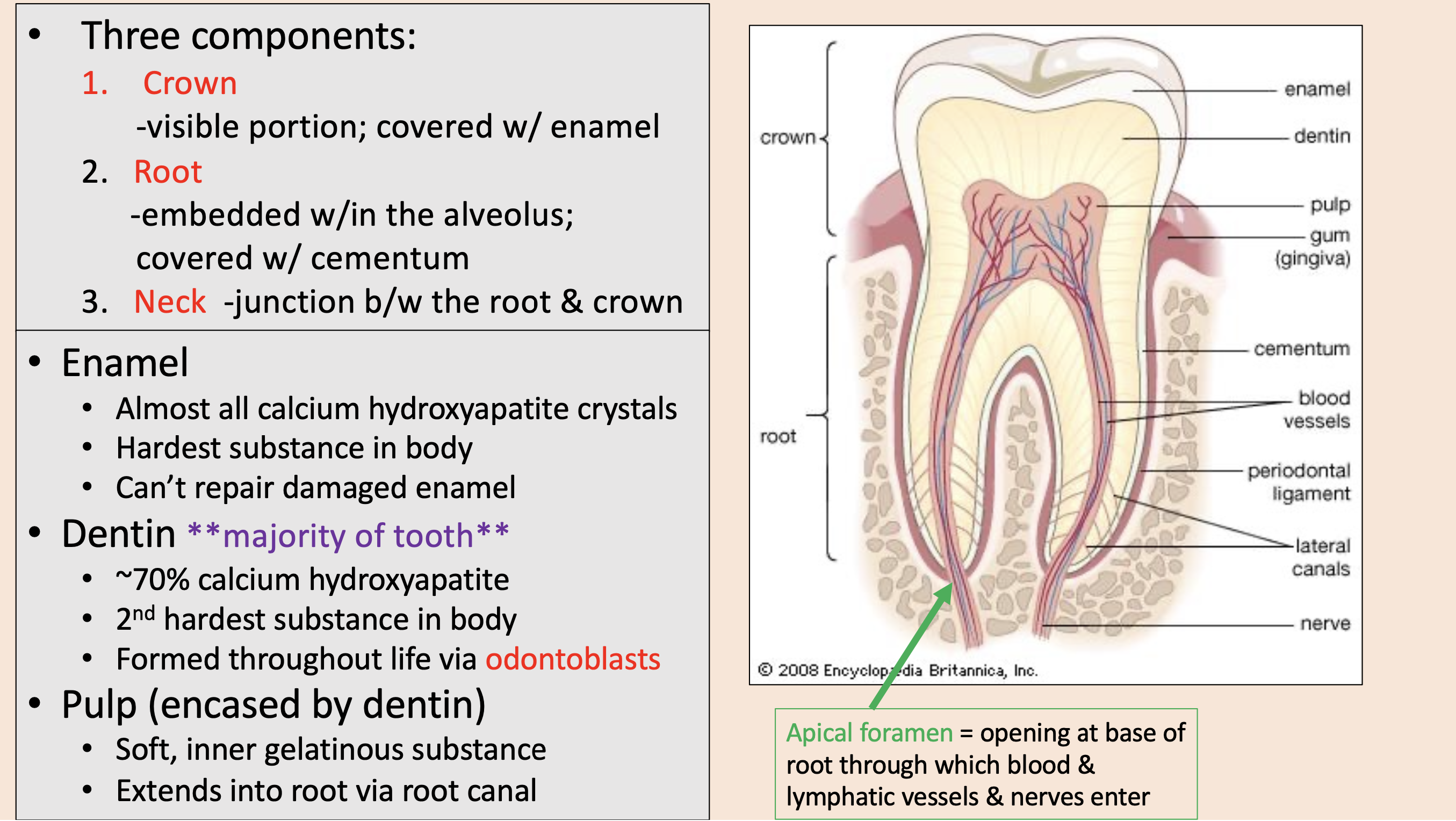
visible portion; covered with enamel
crown
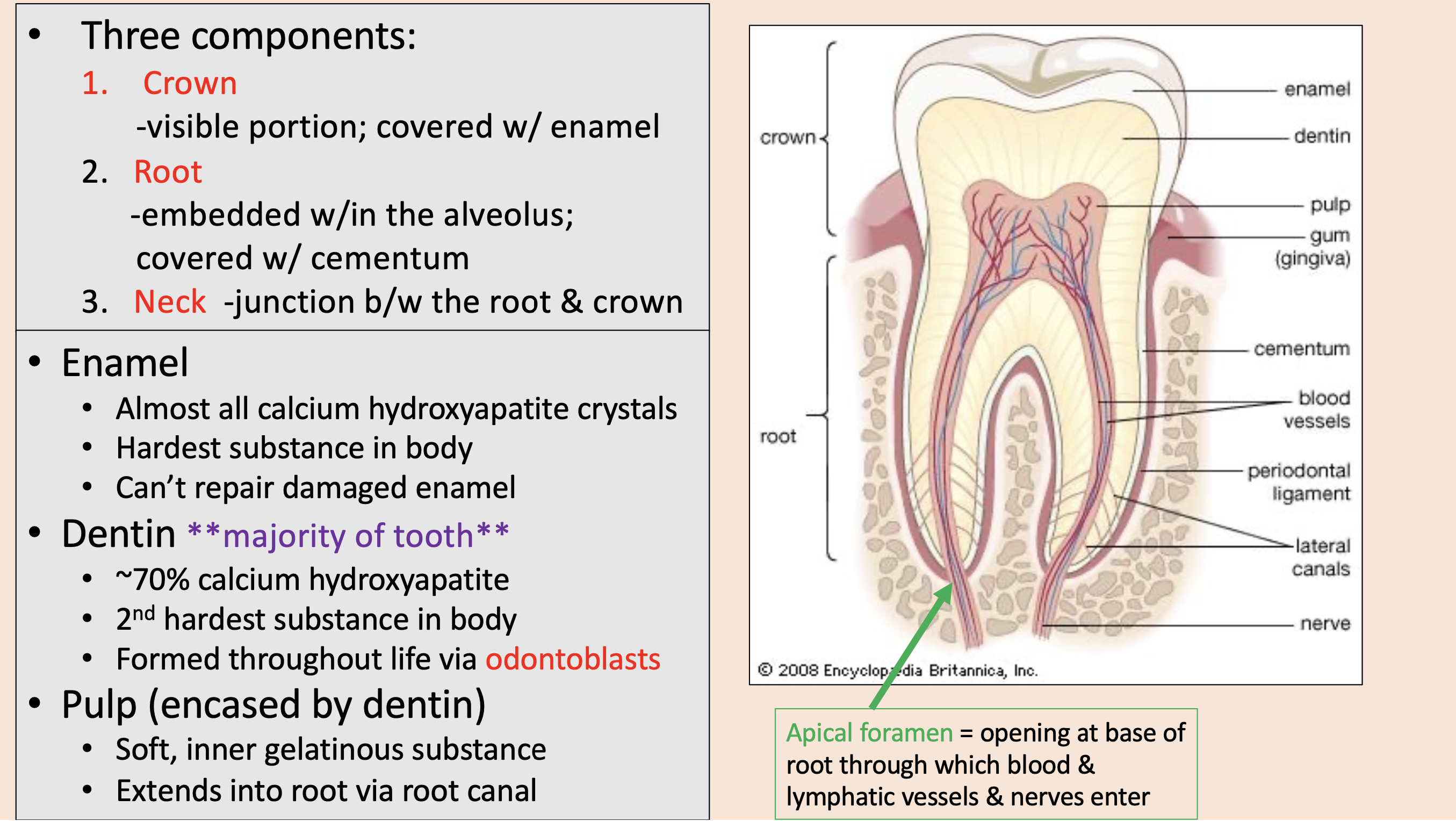
embedded w/in the alveolus; covered with cementum
root
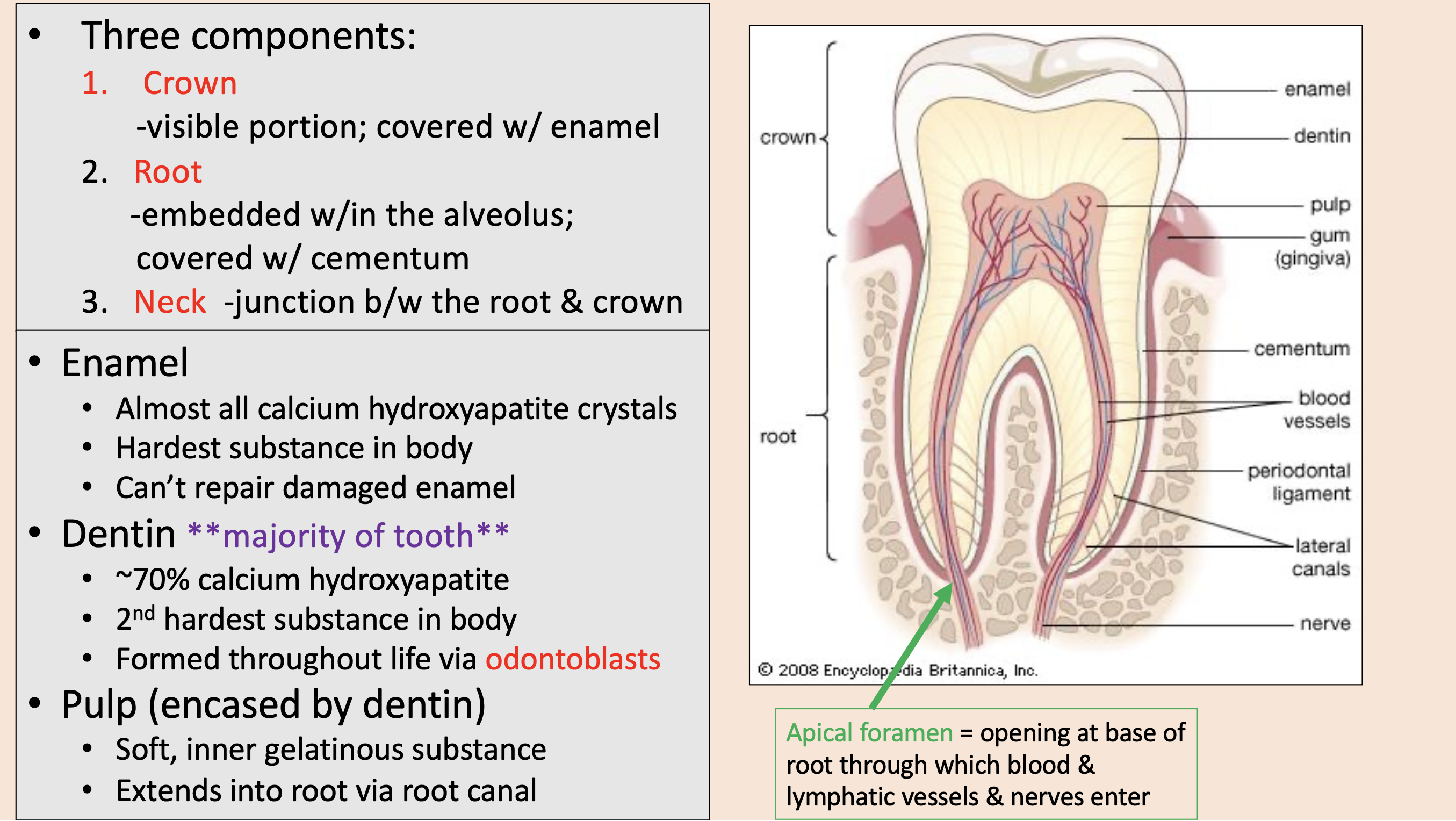
junction between the root & crown
neck
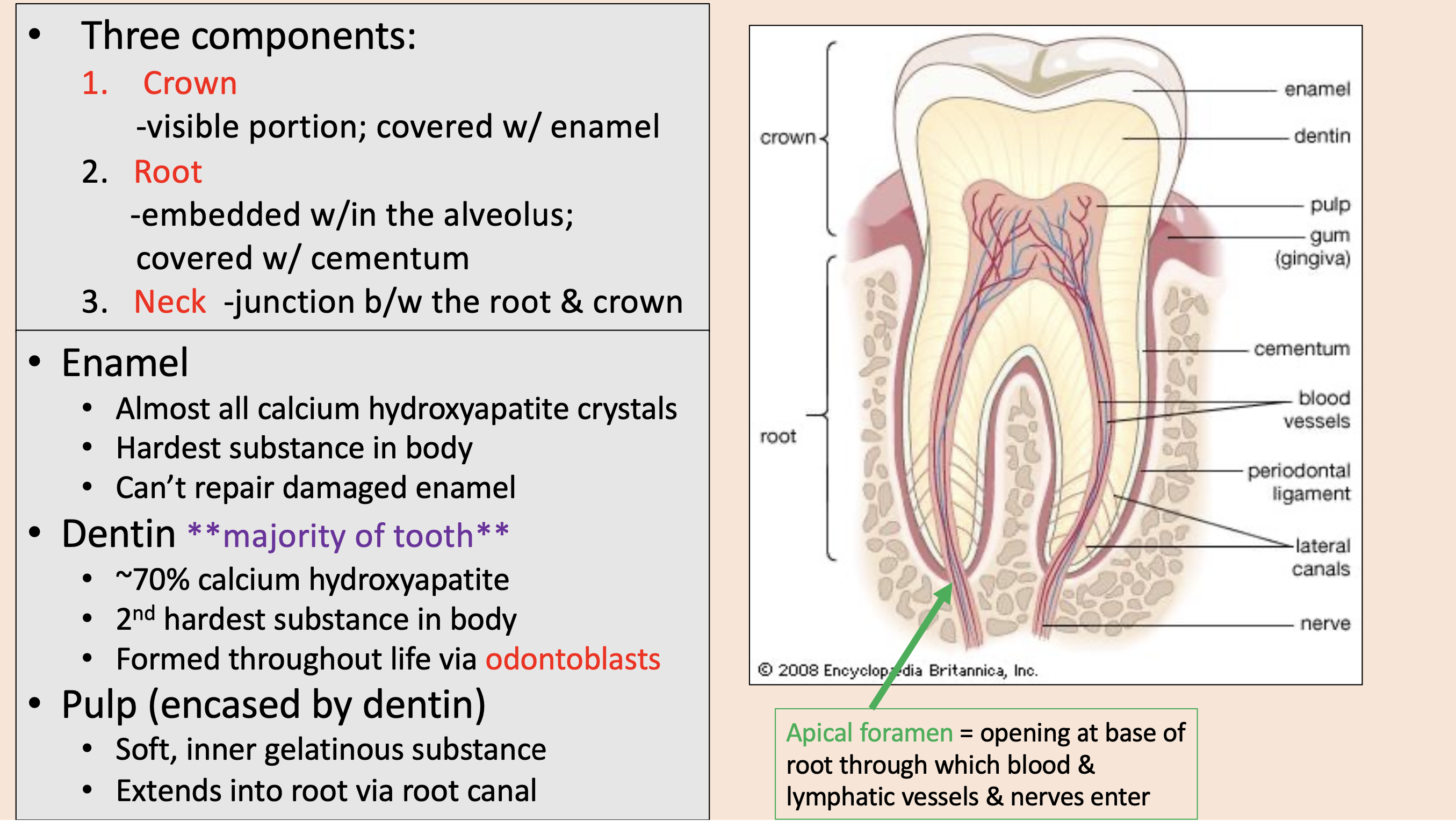
Almost all calcium hydroxyapatite crystals.
Hardest substance in body.
Can’t repair damaged enamel.
enamel
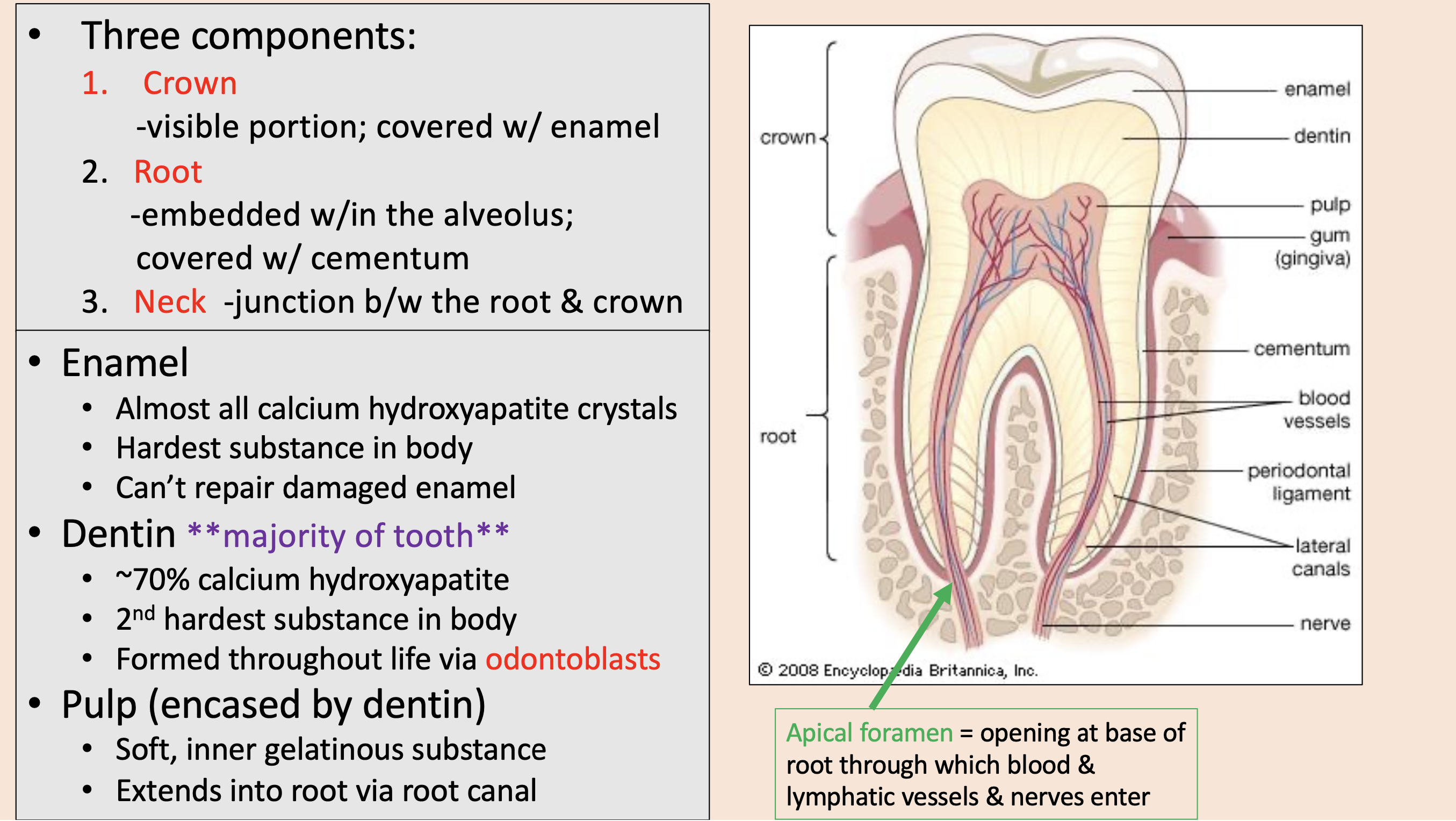
majority of tooth.
~70% calcium hydroxyapatite.
2nd hardest substance in body.
Formed throughout life via odontoblasts.
dentin
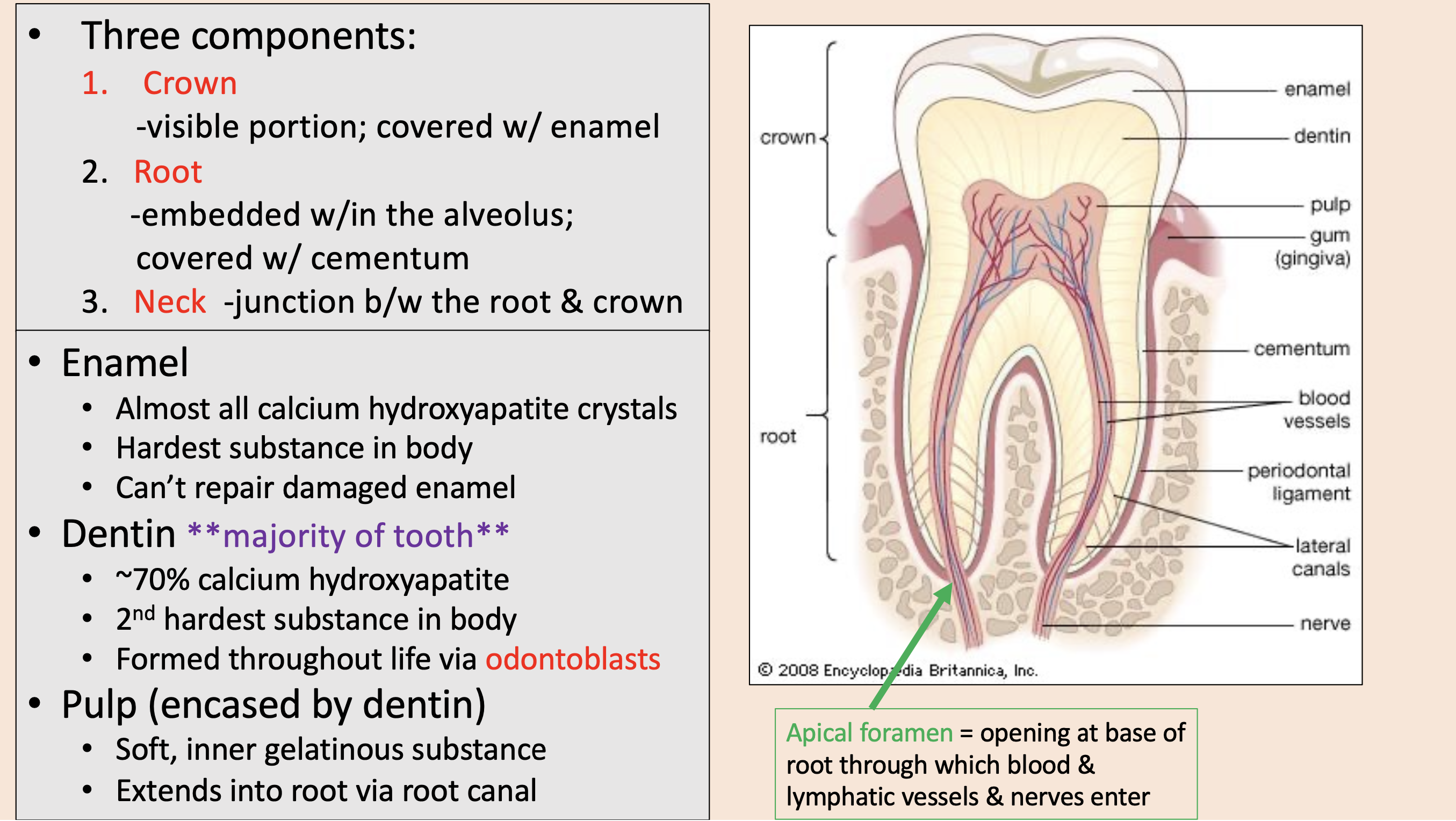
encased by dentin.
Soft, inner gelatinous substance.
Extends into root via root canal.
pulp
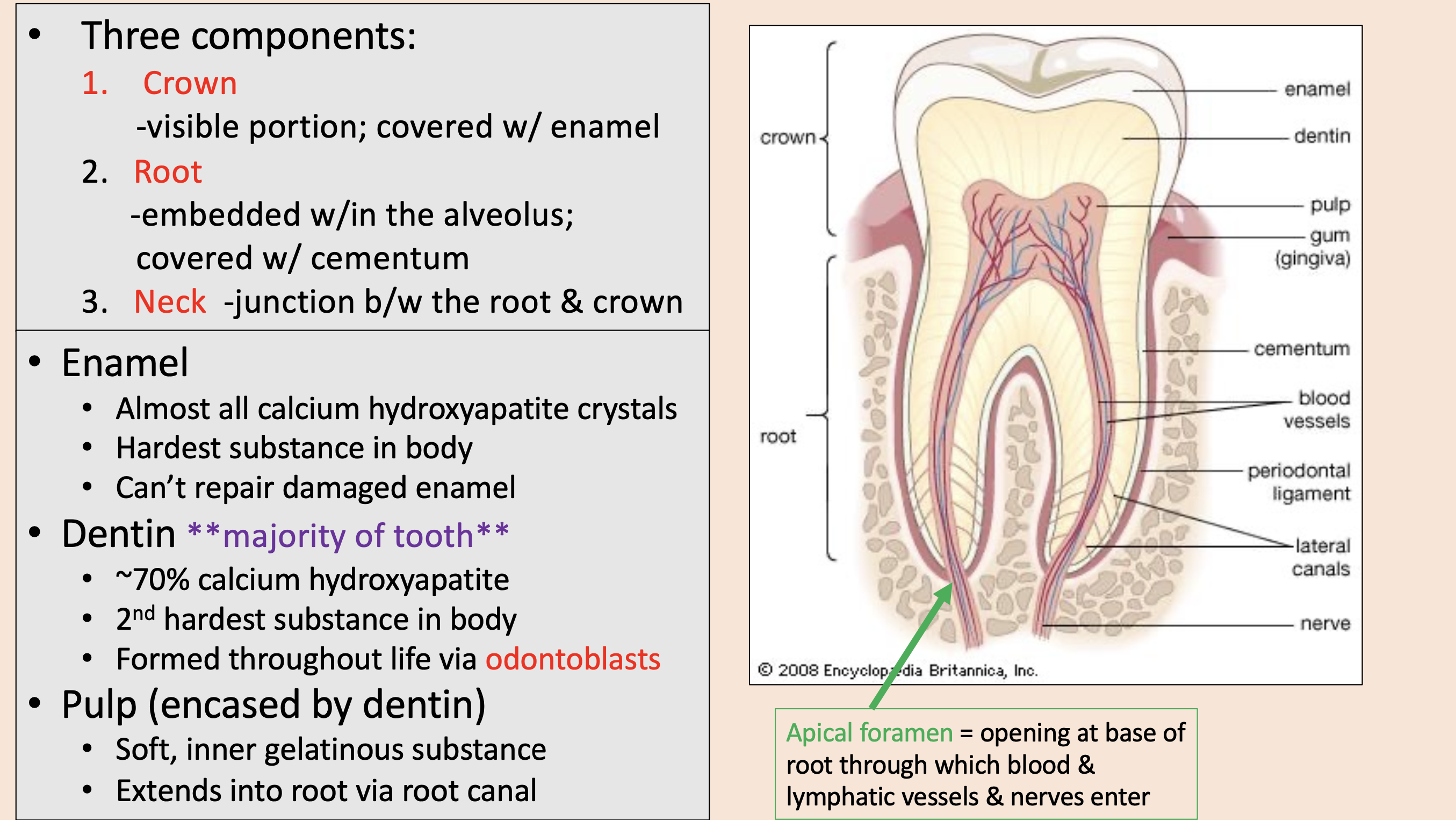
opening at base of root through which blood & lymphatic vessels & nerves enter
apical foramen
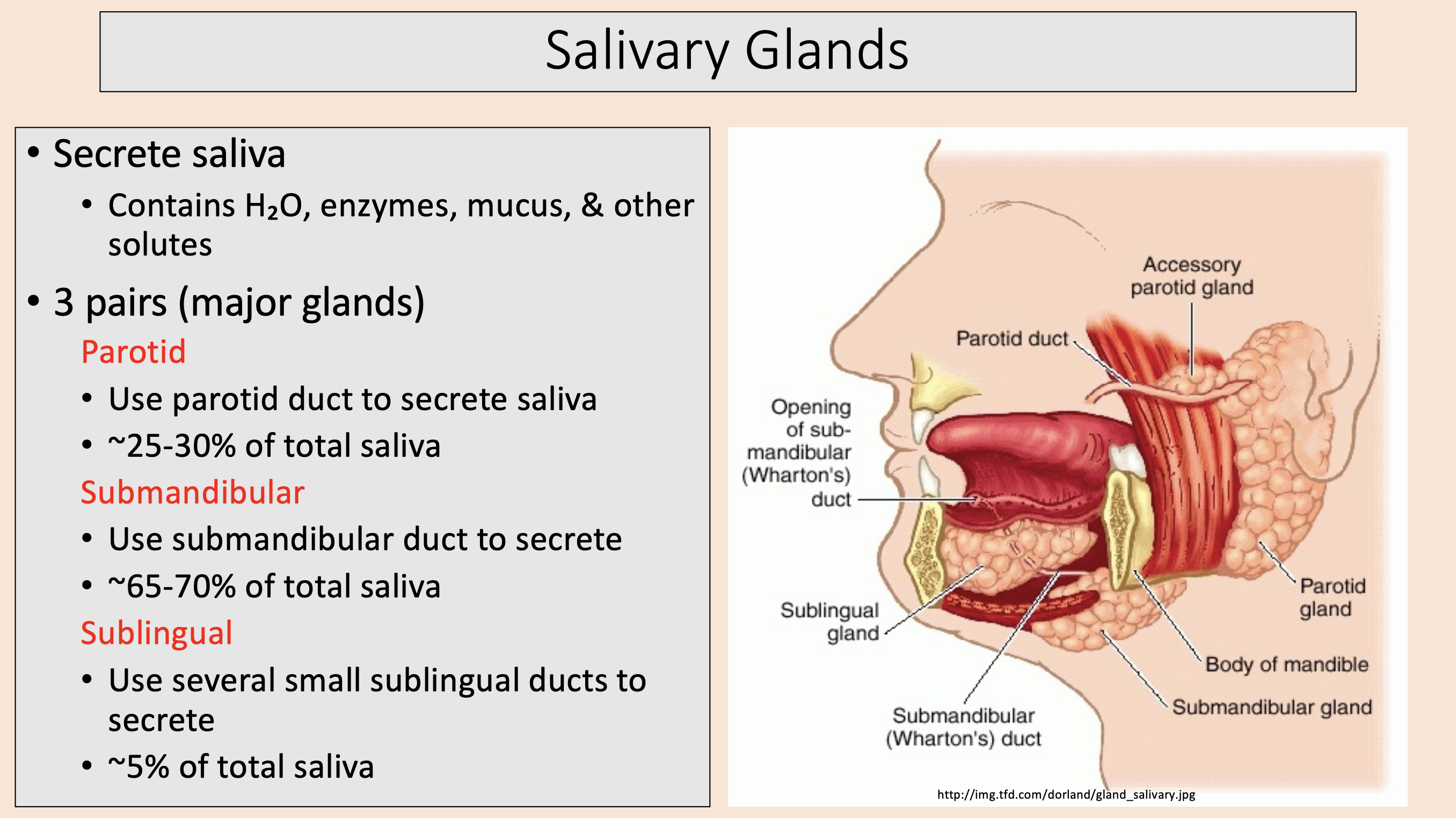
3 pairs (major glands)
parotid
submandibular
sublingual
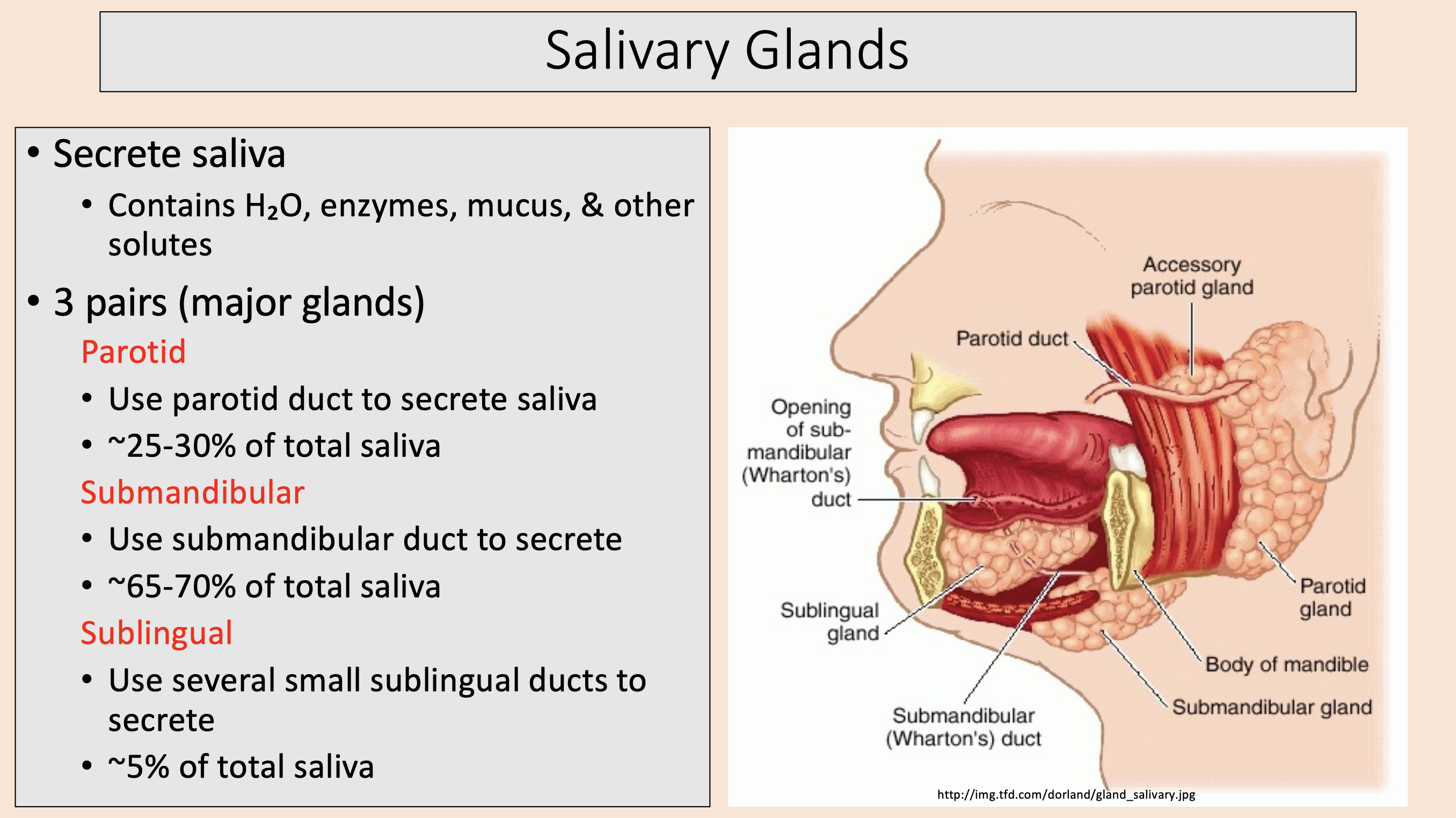
Use parotid duct to secrete saliva.
~25-30% of total saliva.
parotid
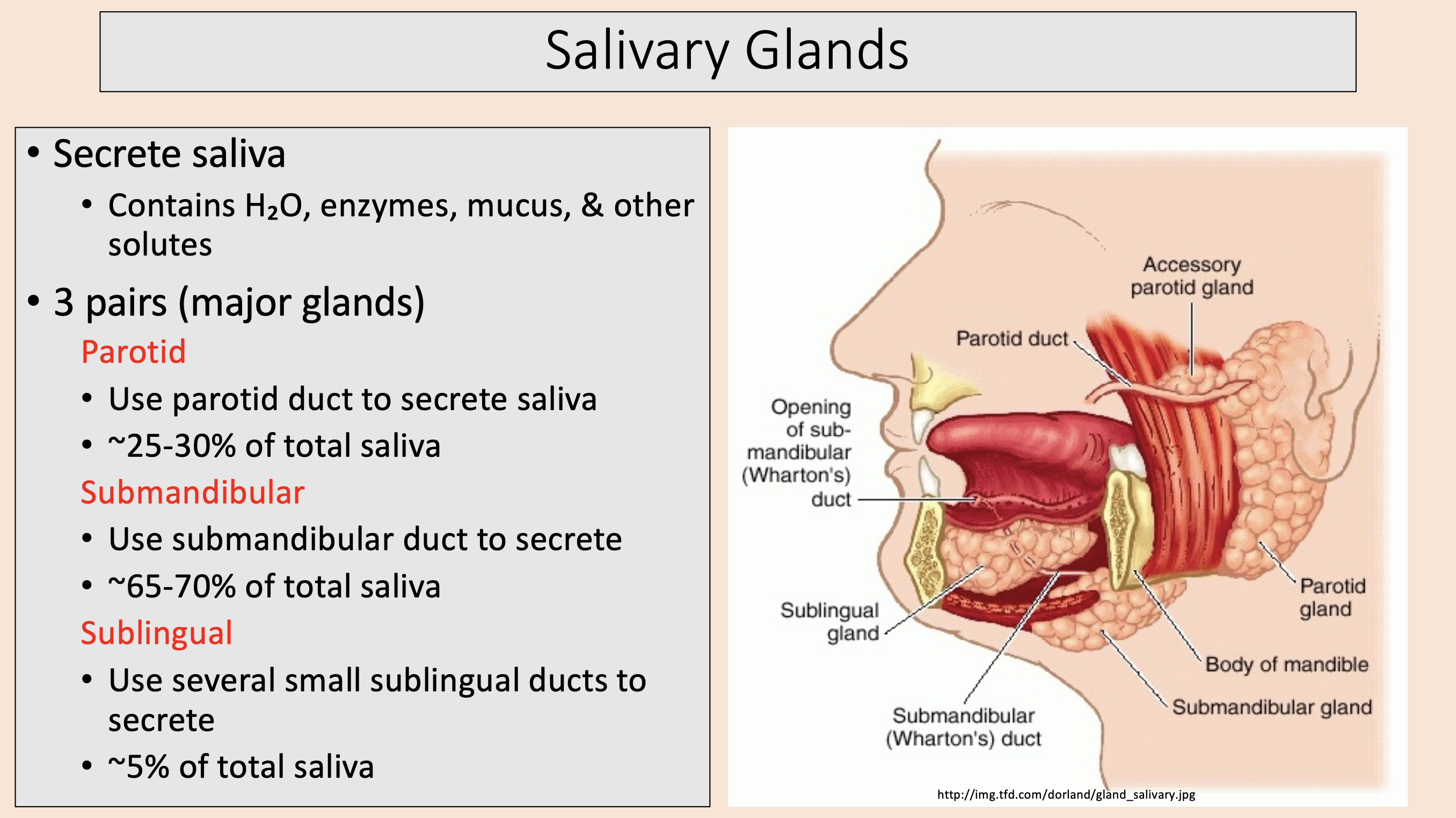
Use submandibular duct to secrete.
~65-70% of total saliva.
submandibular
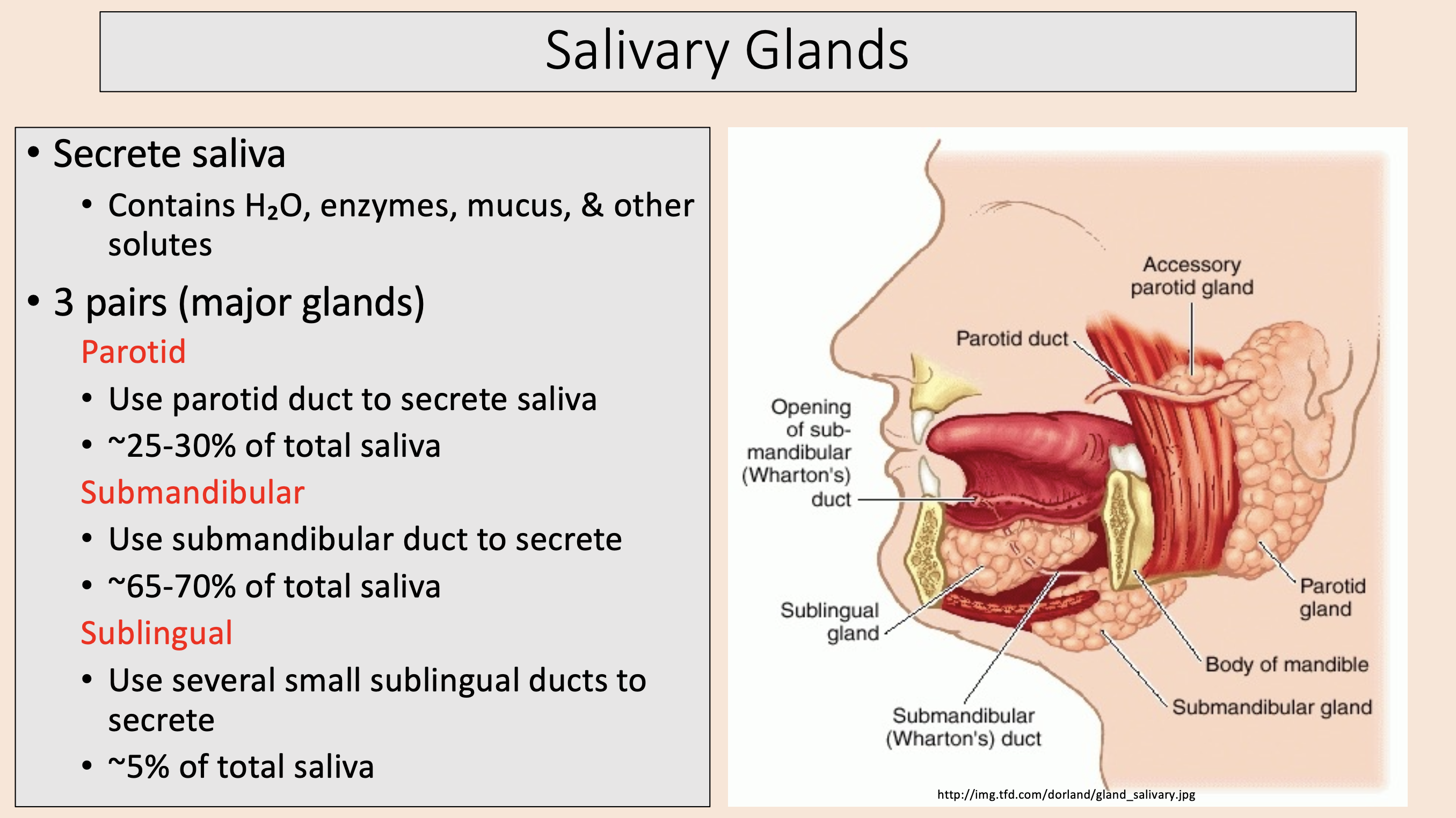
Use several small sublingual ducts to secrete.
~5% of total saliva.
sublingual
main component (99.5%)
water

Na+, Cl-, K+
electrolytes

saliva enzymes
salivary amylase
lingual lipase
lysozyme

First enzyme food encounters.
Catalyzes carbohydrate (starch) breakdown.
salivary amylase
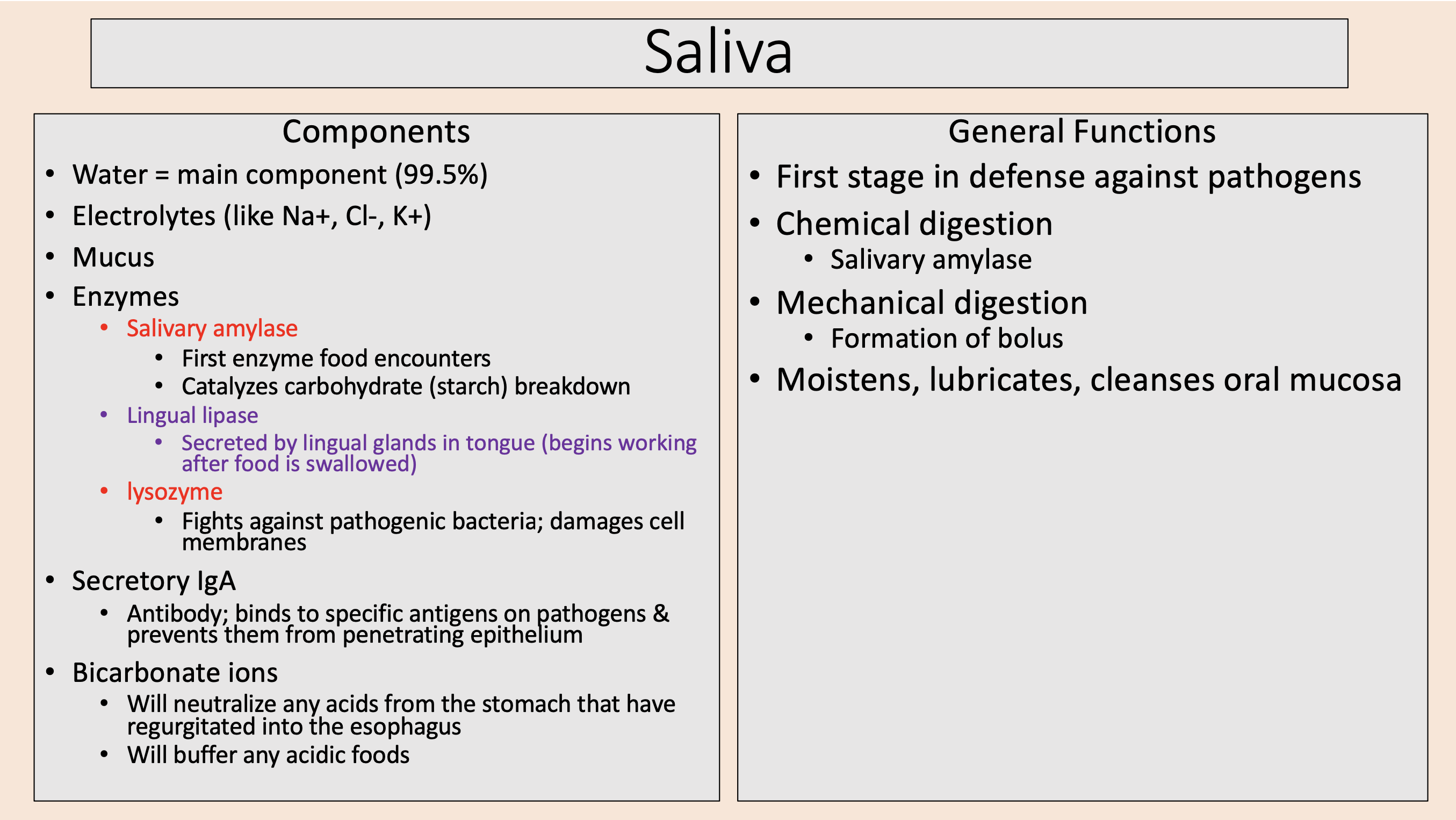

Secreted by lingual glands in tongue (begins working after food is swallowed)
lingual lipase
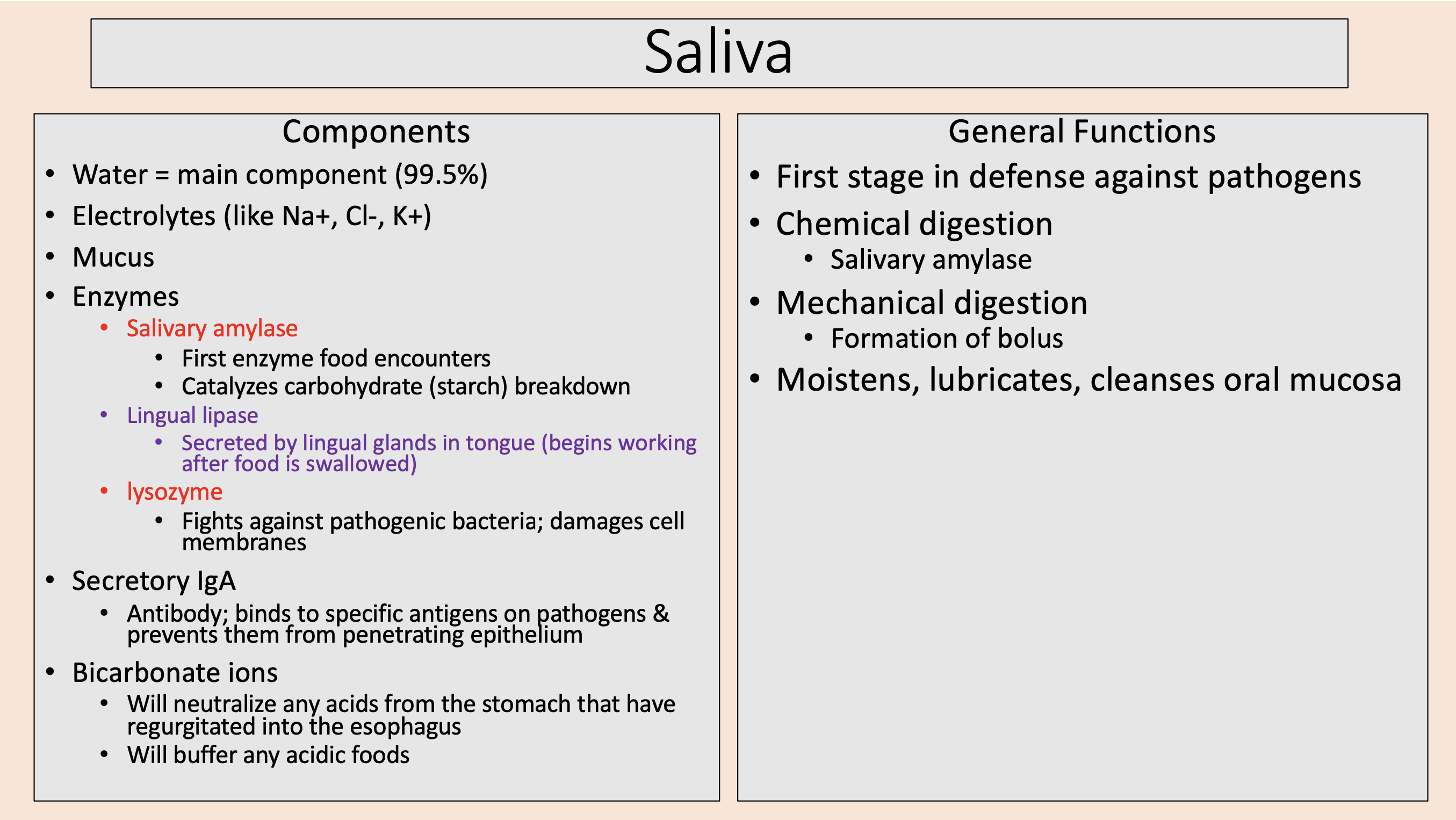

Fights against pathogenic bacteria; damages cell membranes
lysozyme
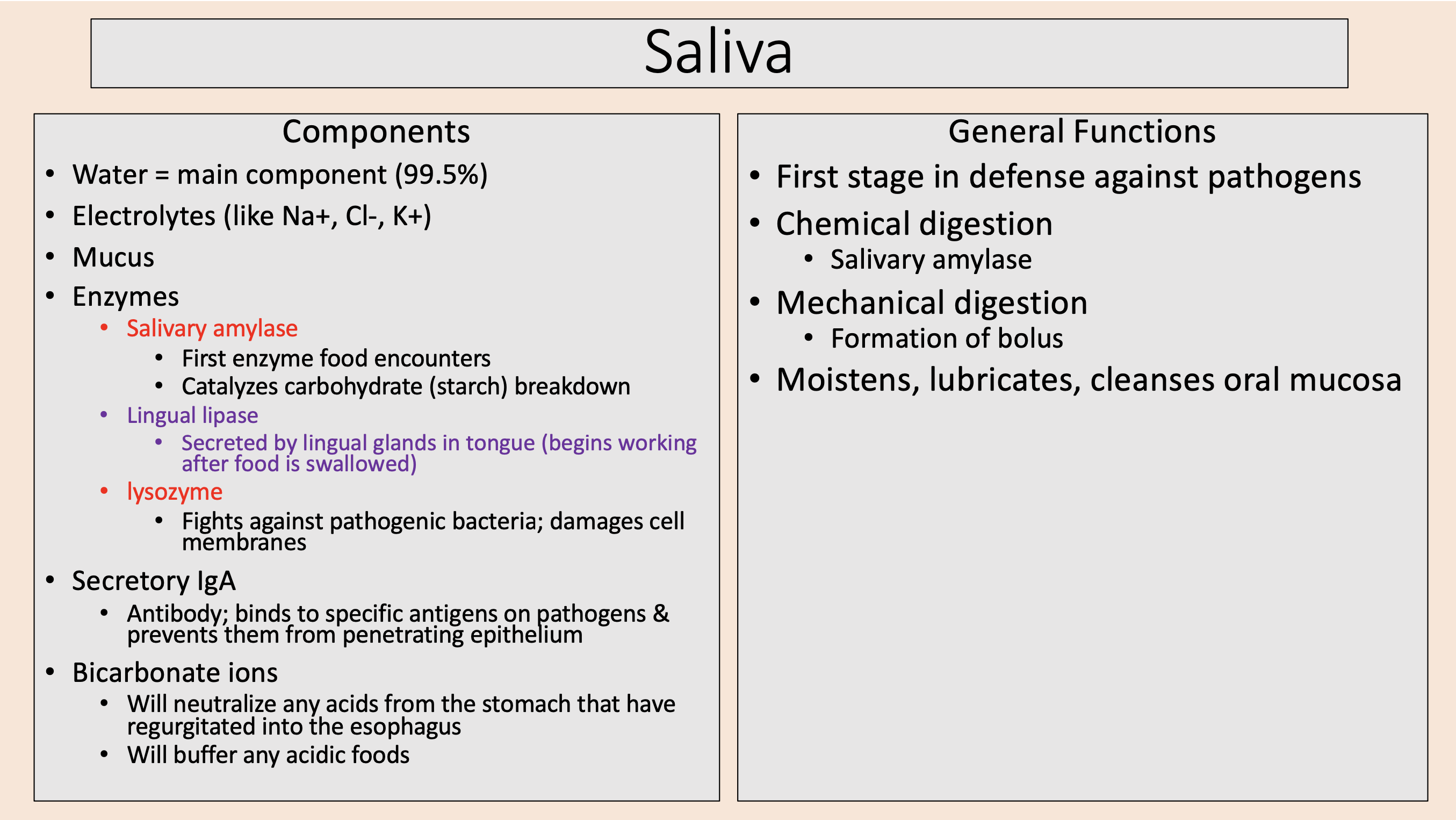

Antibody; binds to specific antigens on pathogens & prevents them from penetrating epithelium
secretory IgA
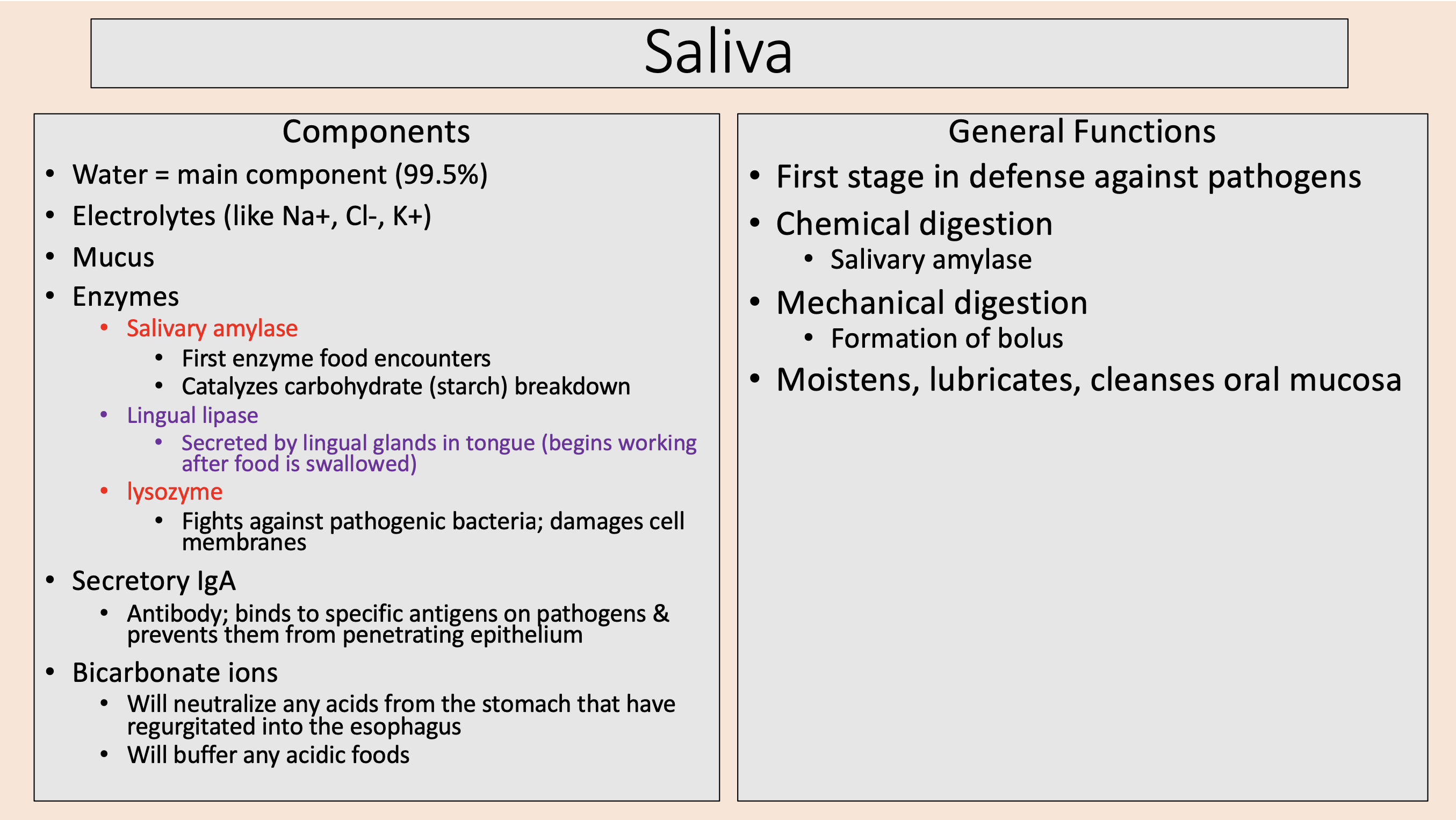

Will neutralize any acids from the stomach that have regurgitated into the esophagus.
Will buffer any acidic foods.
bicarbonate ions
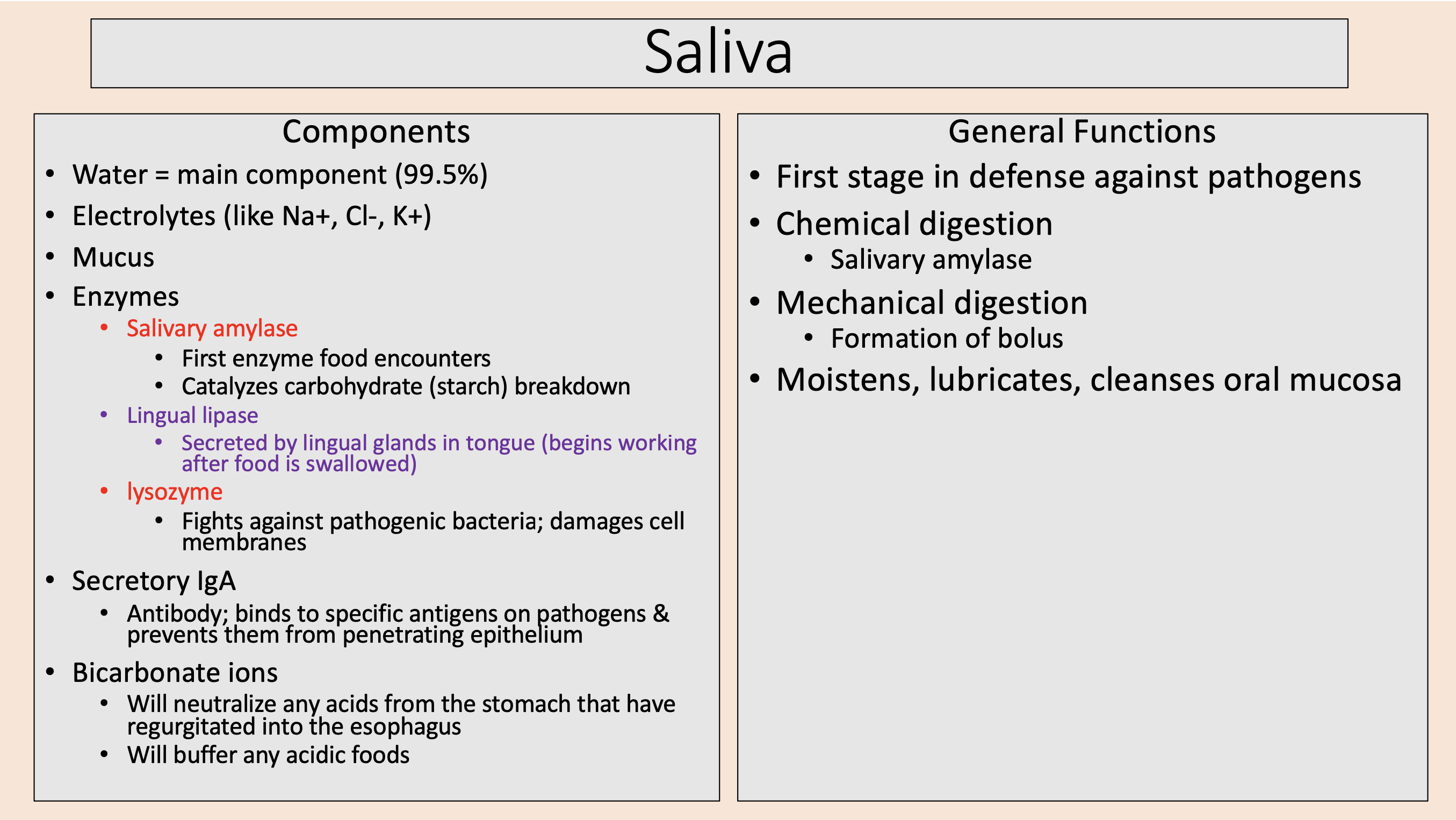

First stage in defense against pathogens.
Chemical digestion.
Mechanical digestion.
Moistens, lubricates, cleanses oral mucosa.
Saliva General Functions
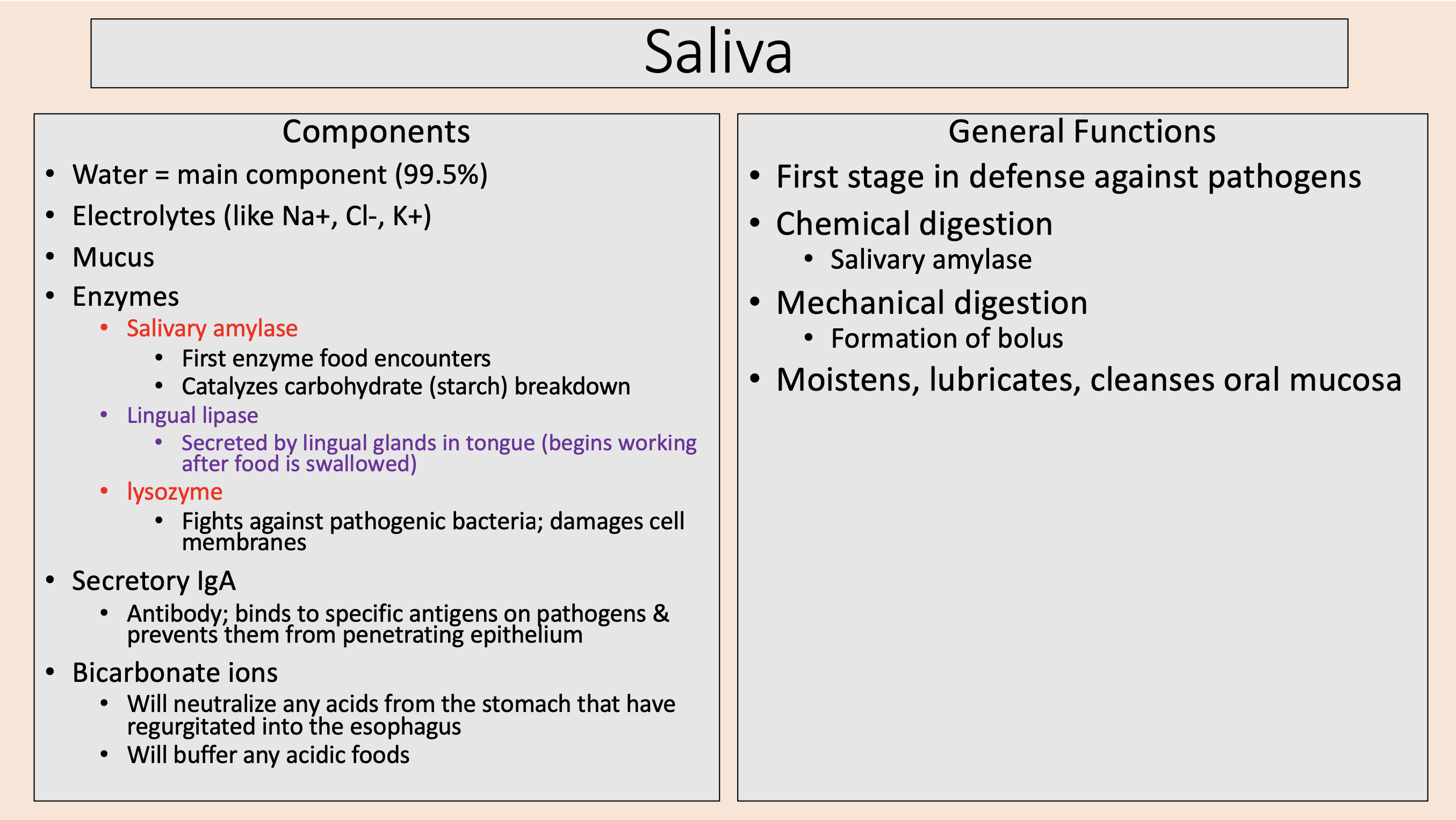

Salivary amylase
chemical digestion
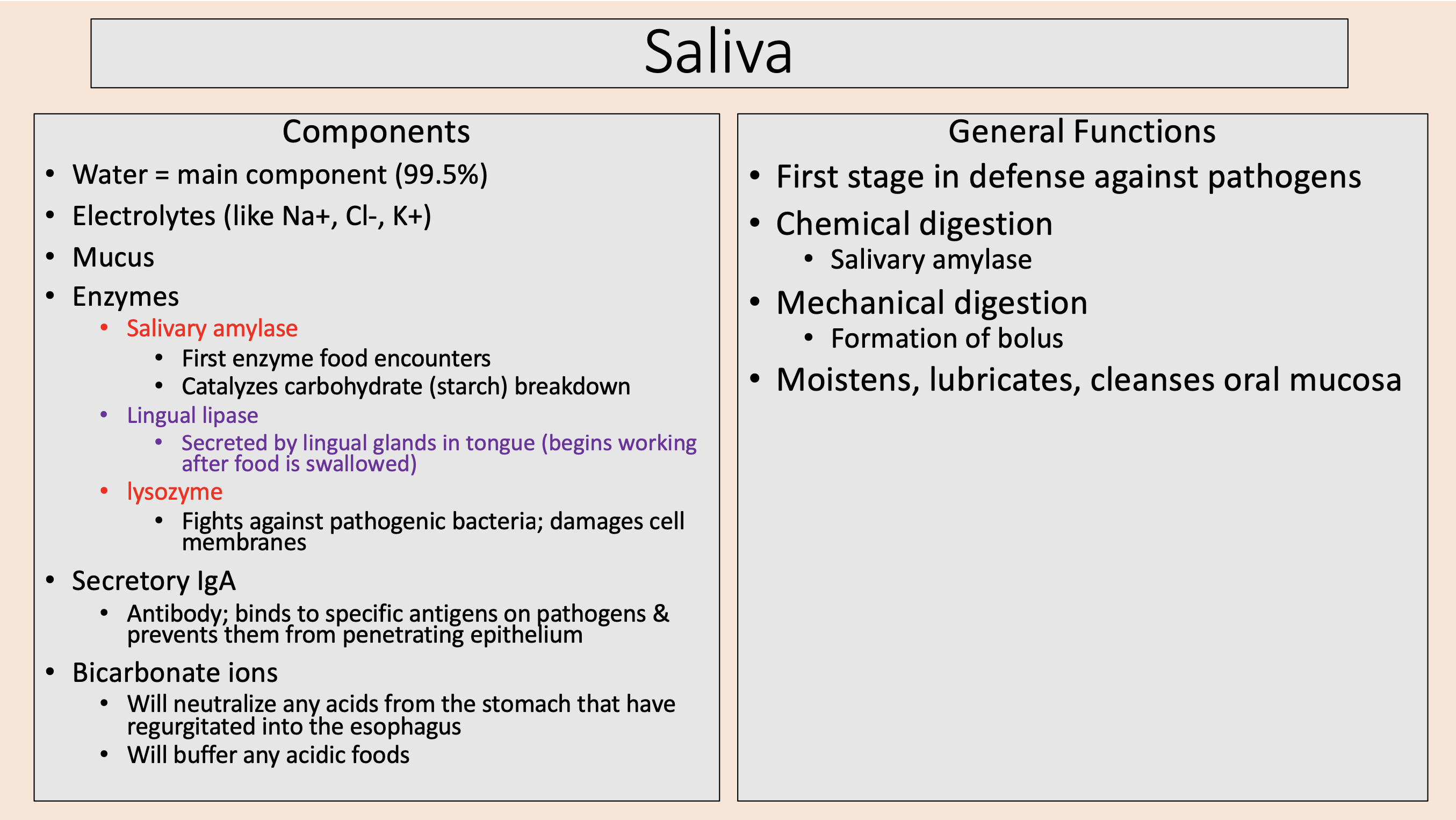

Formation of bolus
mechanical digestion
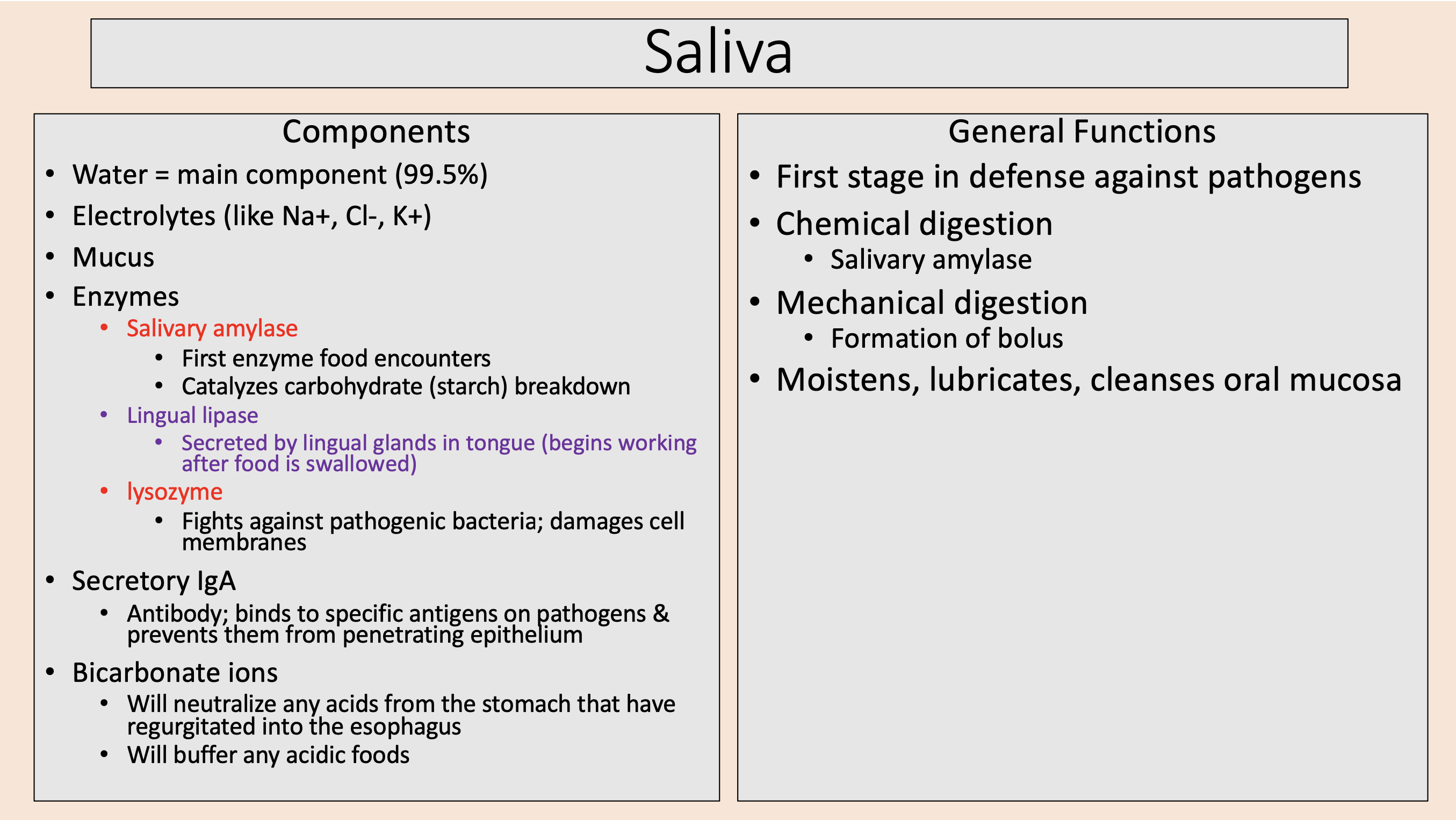

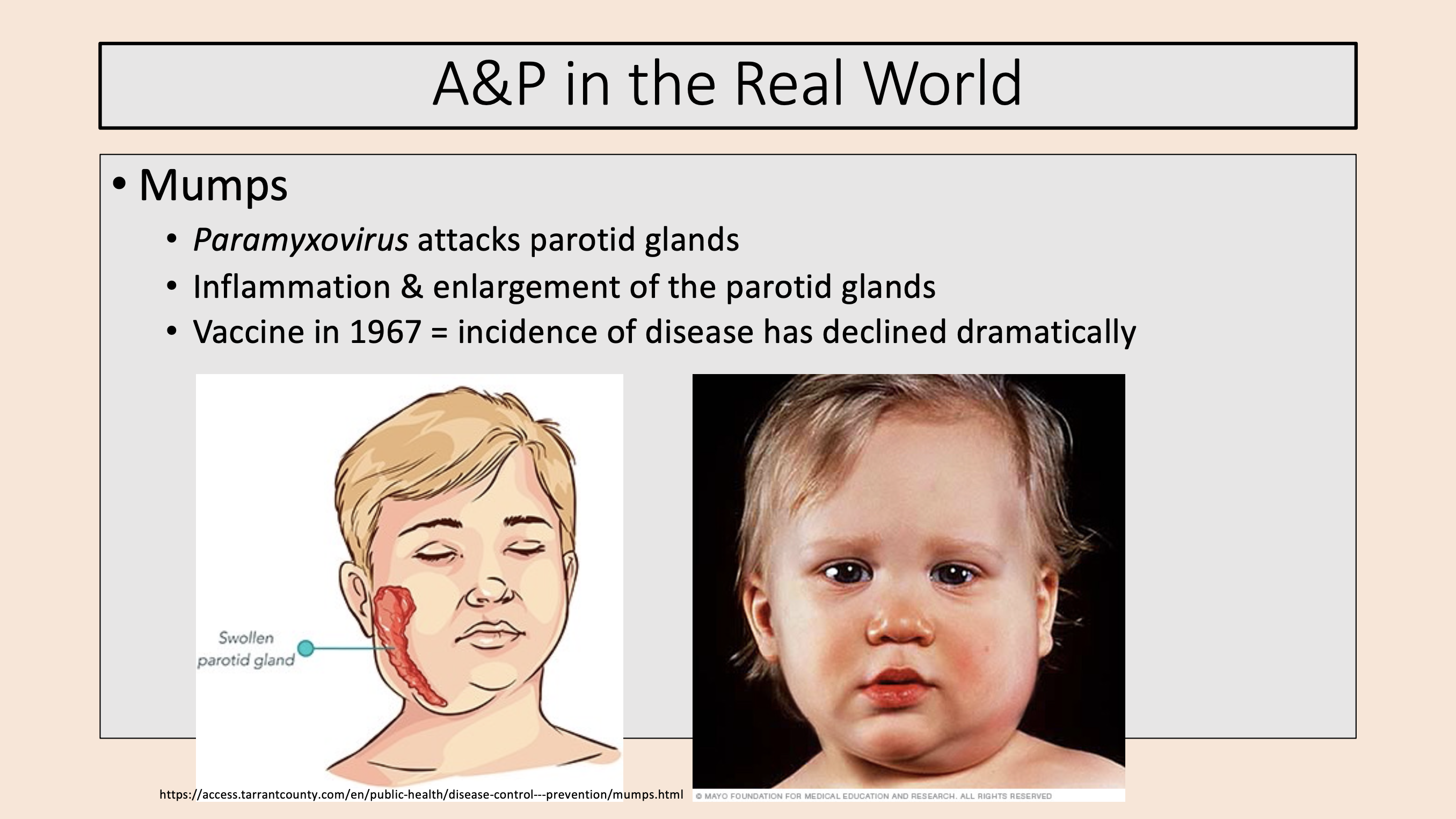
Paramyxovirus attacks parotid glands.
Inflammation & enlargement of the parotid glands.
Vaccine in 1967 = incidence of disease has declined dramatically.
mumps
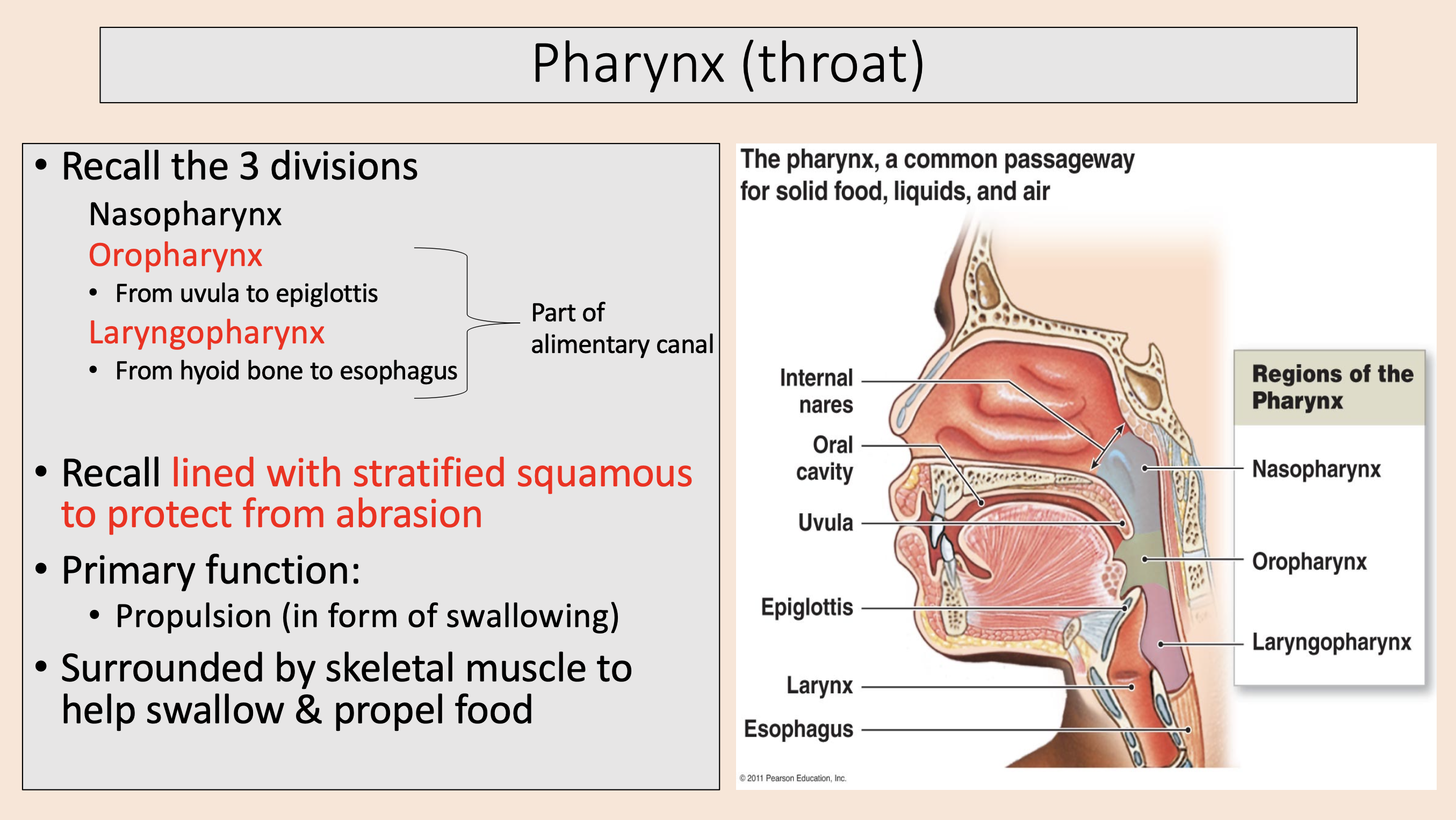
3 divisions of Pharynx (throat)
nasopharynx
oropharynx
laryngopharynx
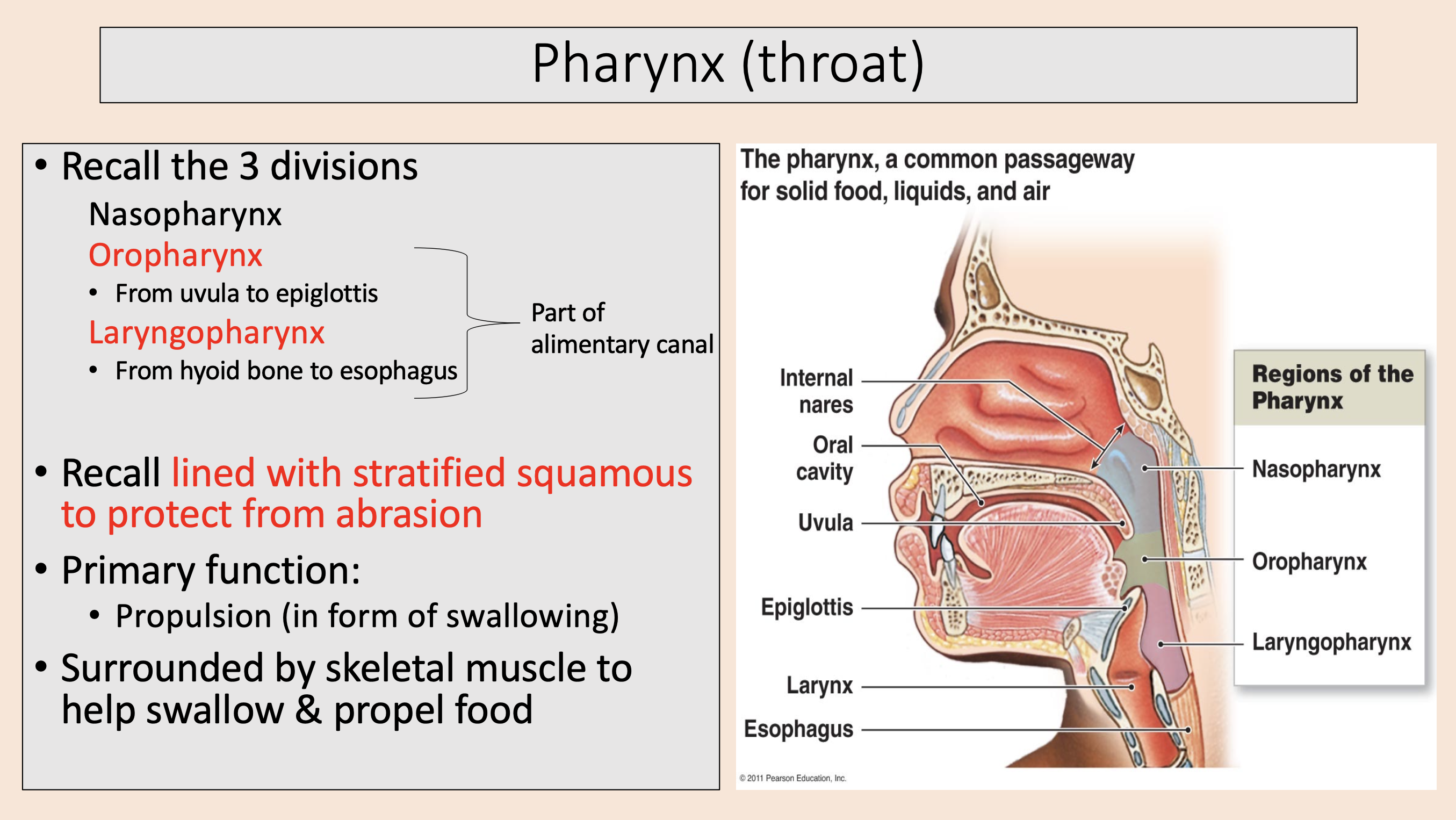
From uvula to epiglottis.
lined with stratified squamous to protect from abrasion.
oropharynx
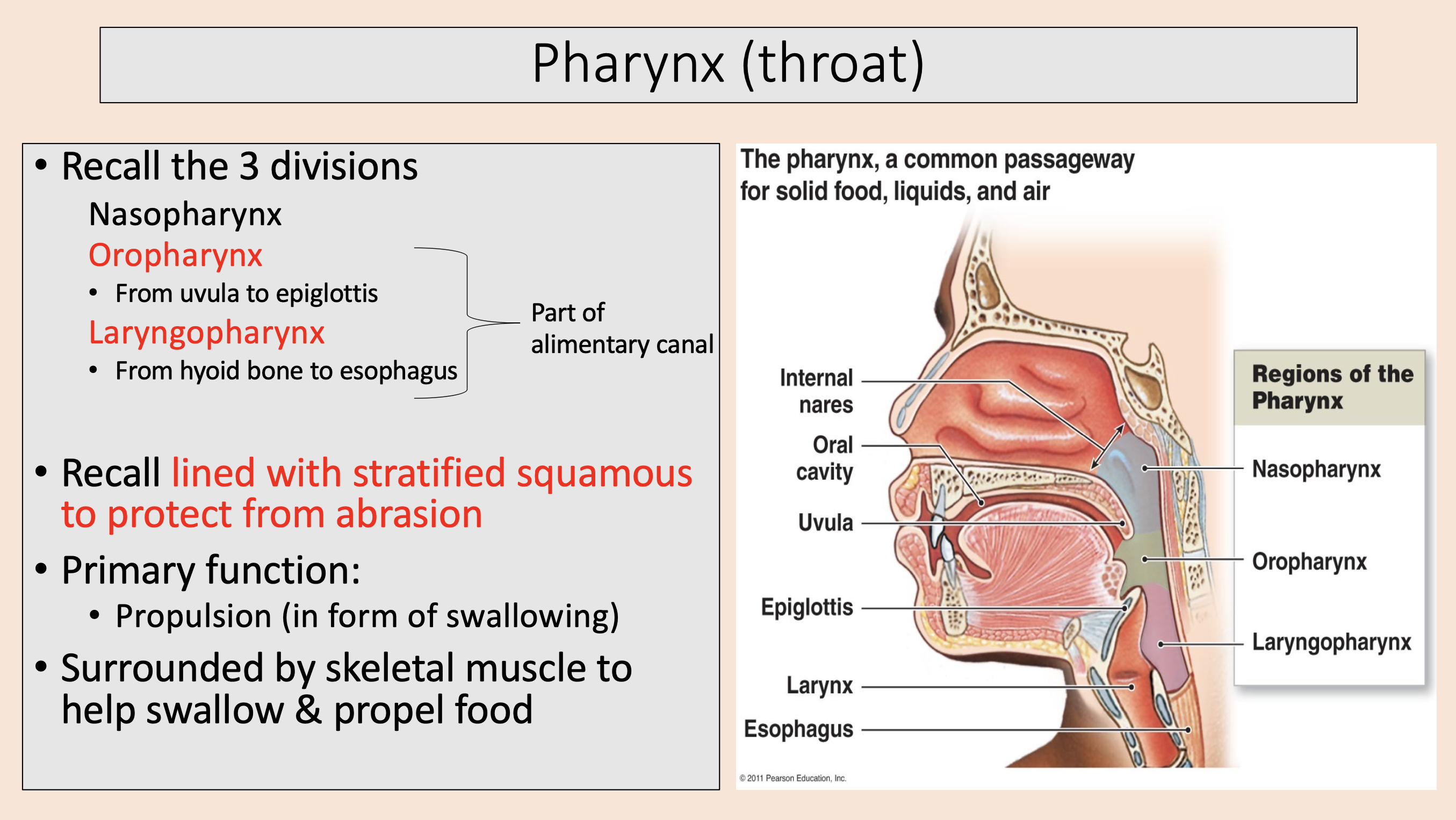
From hyoid bone to esophagus.
lined with stratified squamous to protect from abrasion.
laryngopharynx
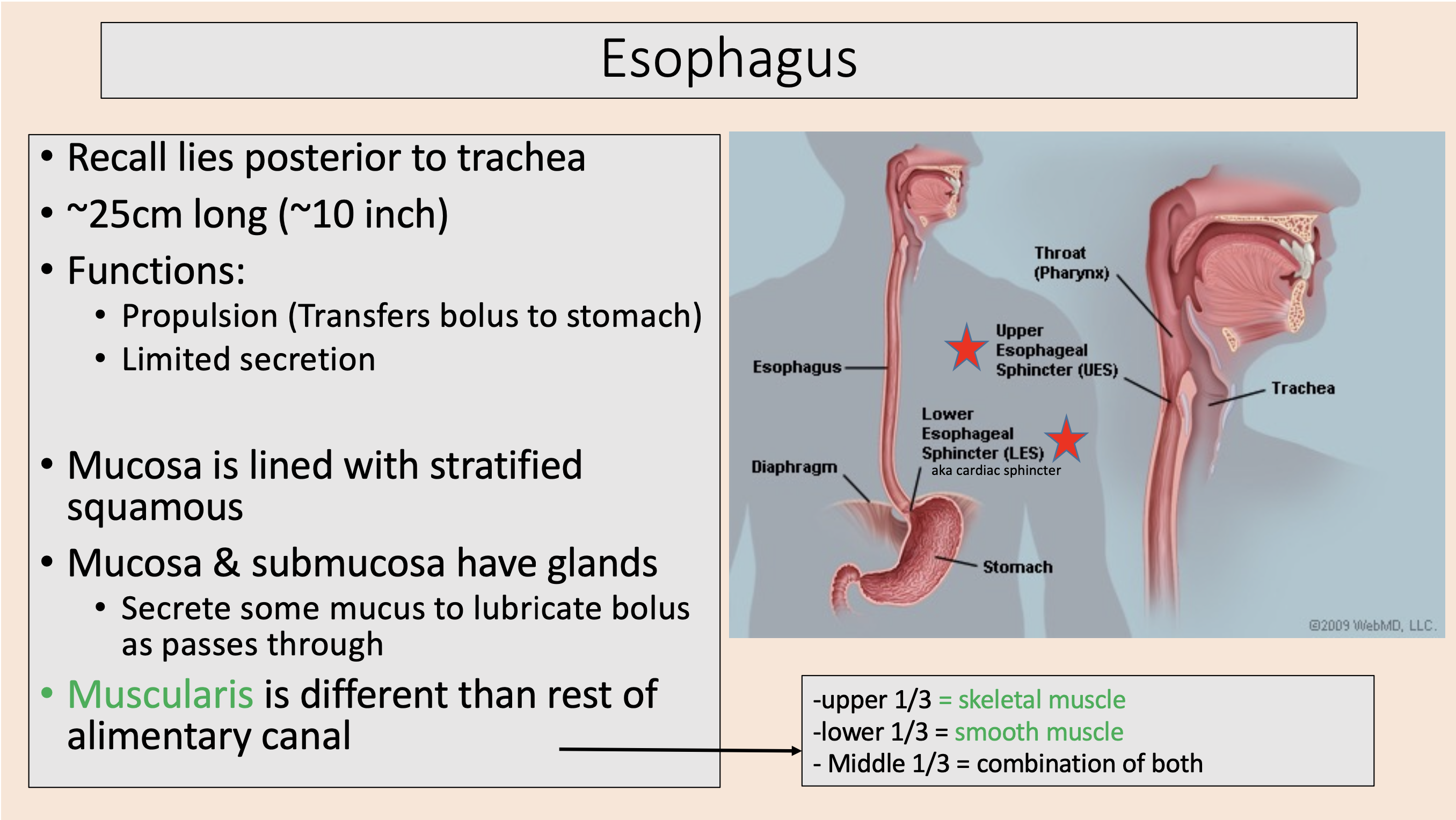
lies posterior to trachea.
~25cm long (~10 inch).
Propulsion (Transfers bolus to stomach).
Limited secretion.
Mucosa is lined with stratified squamous.
esophagus
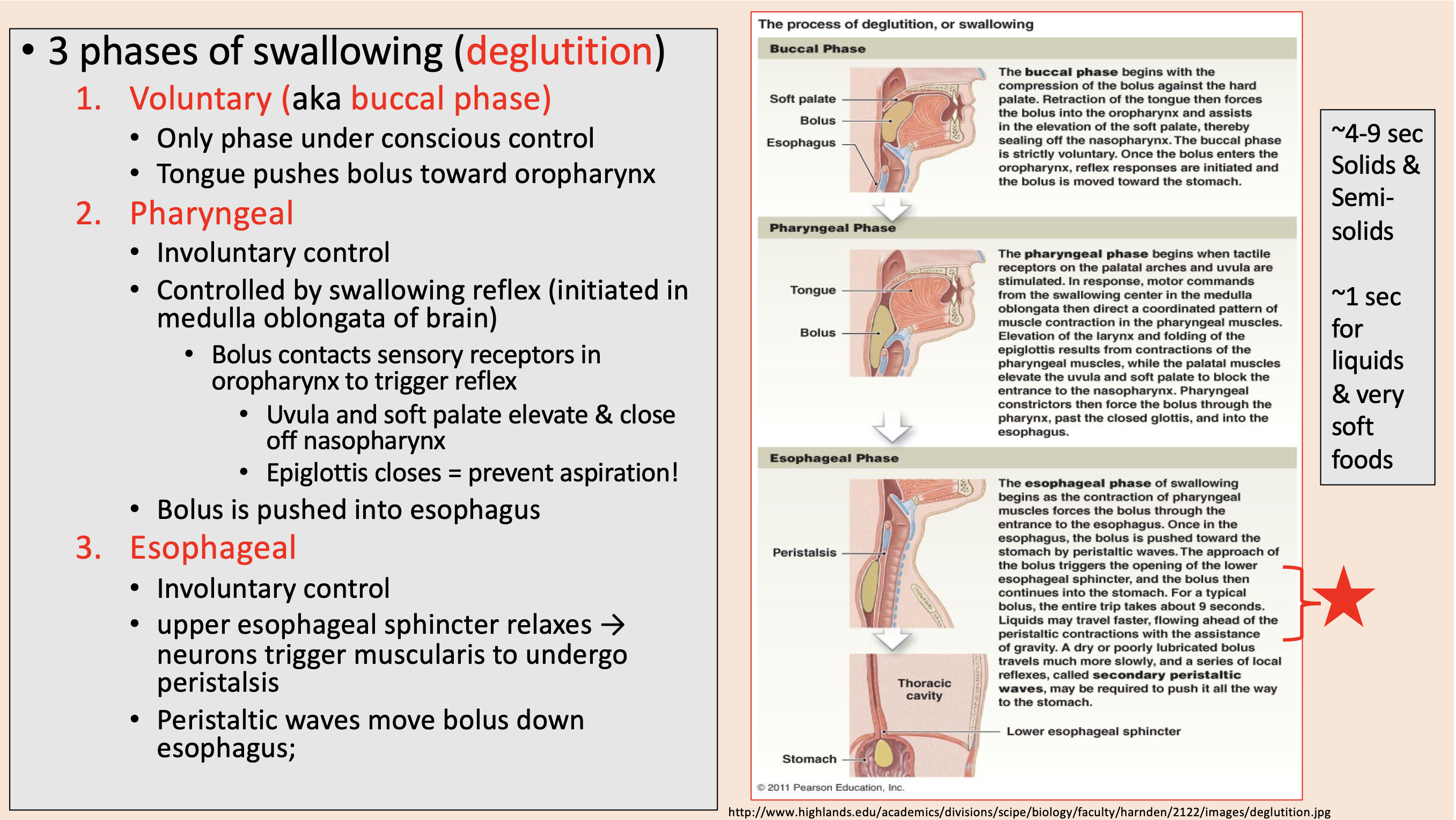
3 phases of swallowing (deglutition)
voluntary
pharyngeal
esophageal
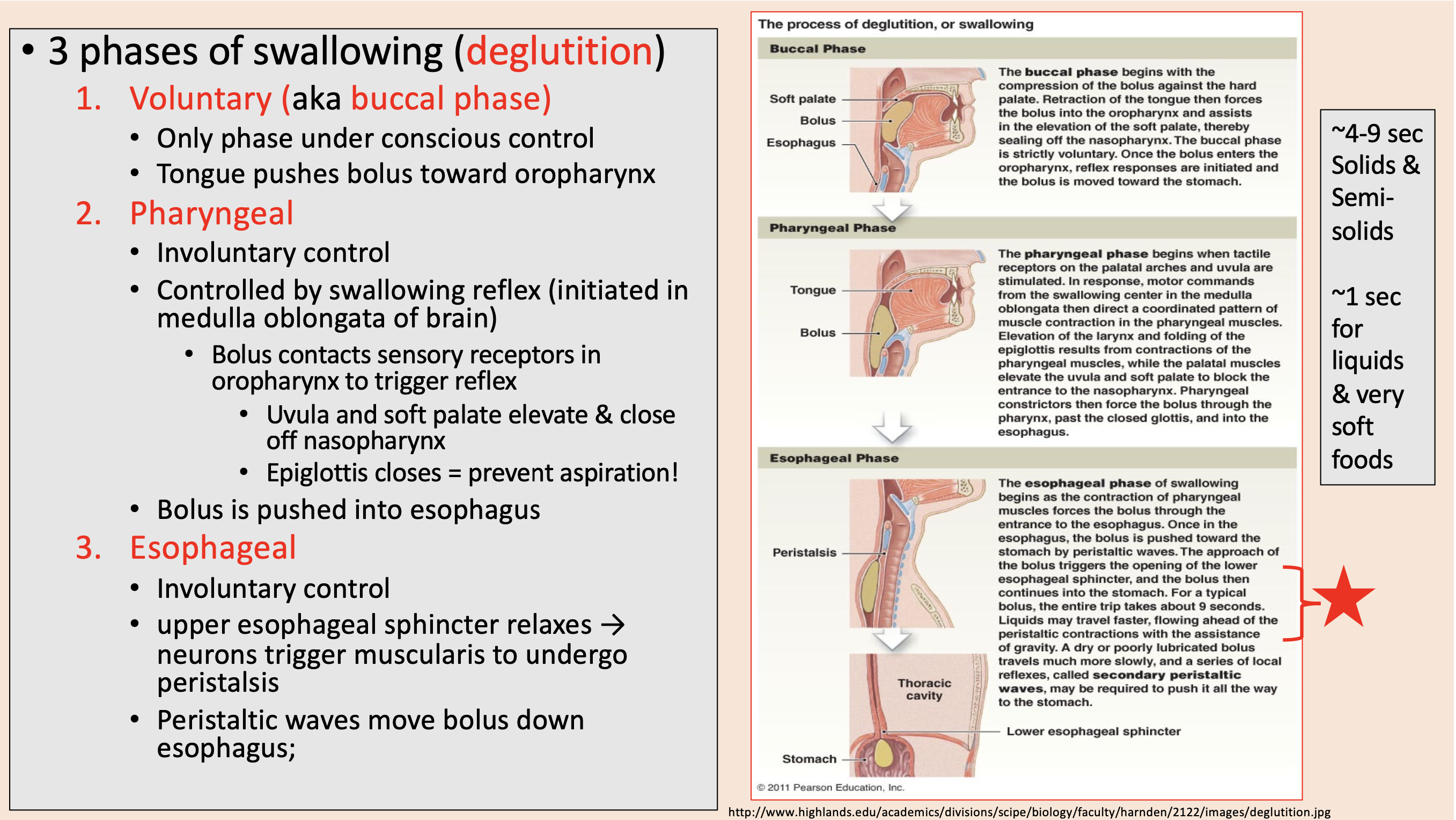
aka buccal phase
voluntary
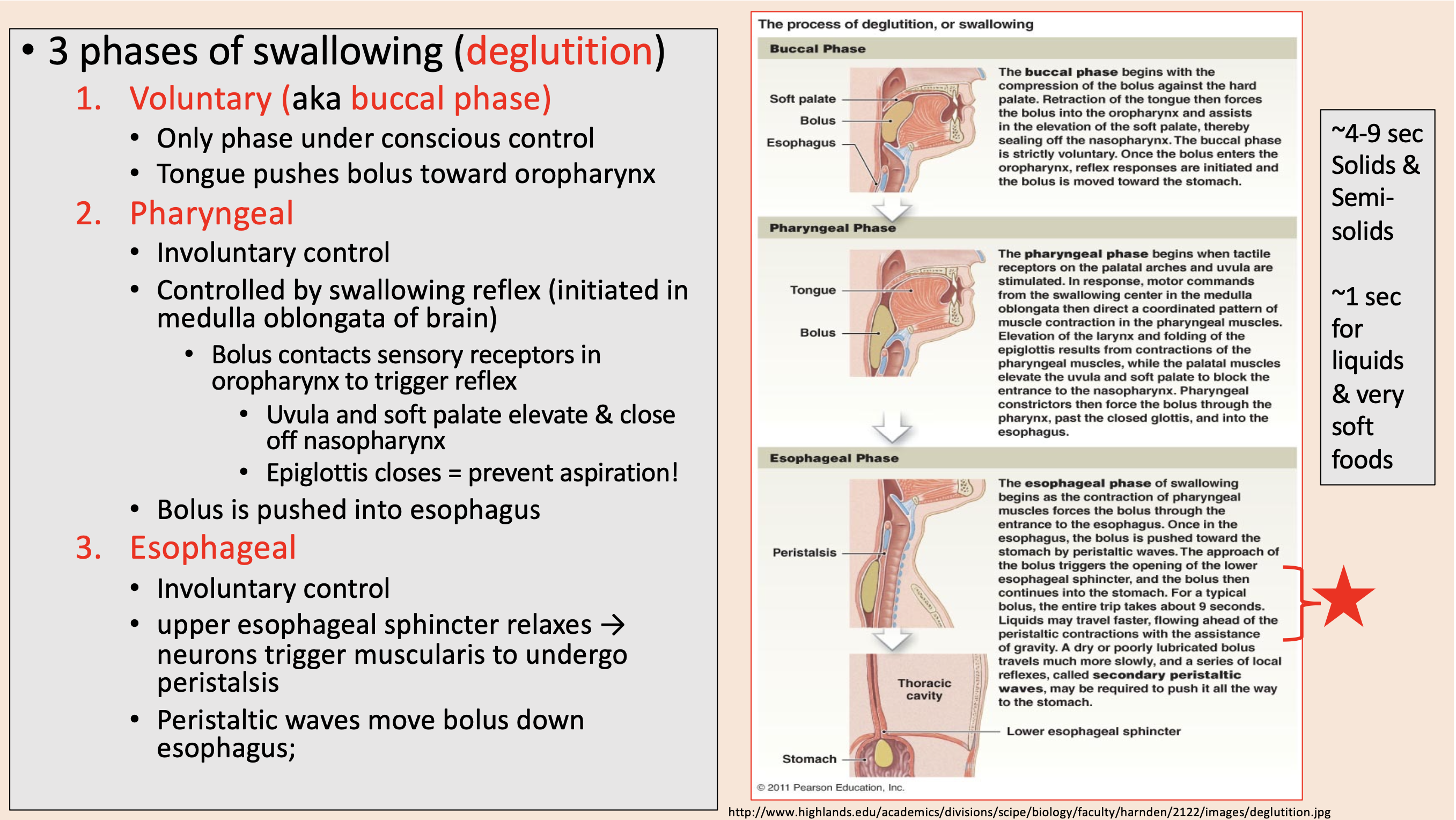
Only phase under conscious control.
Tongue pushes bolus toward oropharynx.
voluntary
Involuntary control.
Controlled by swallowing reflex (initiated in medulla oblongata of brain).
Bolus contacts sensory receptors in oropharynx to trigger reflex.
Uvula and soft palate elevate & close off nasopharynx.
pharyngeal
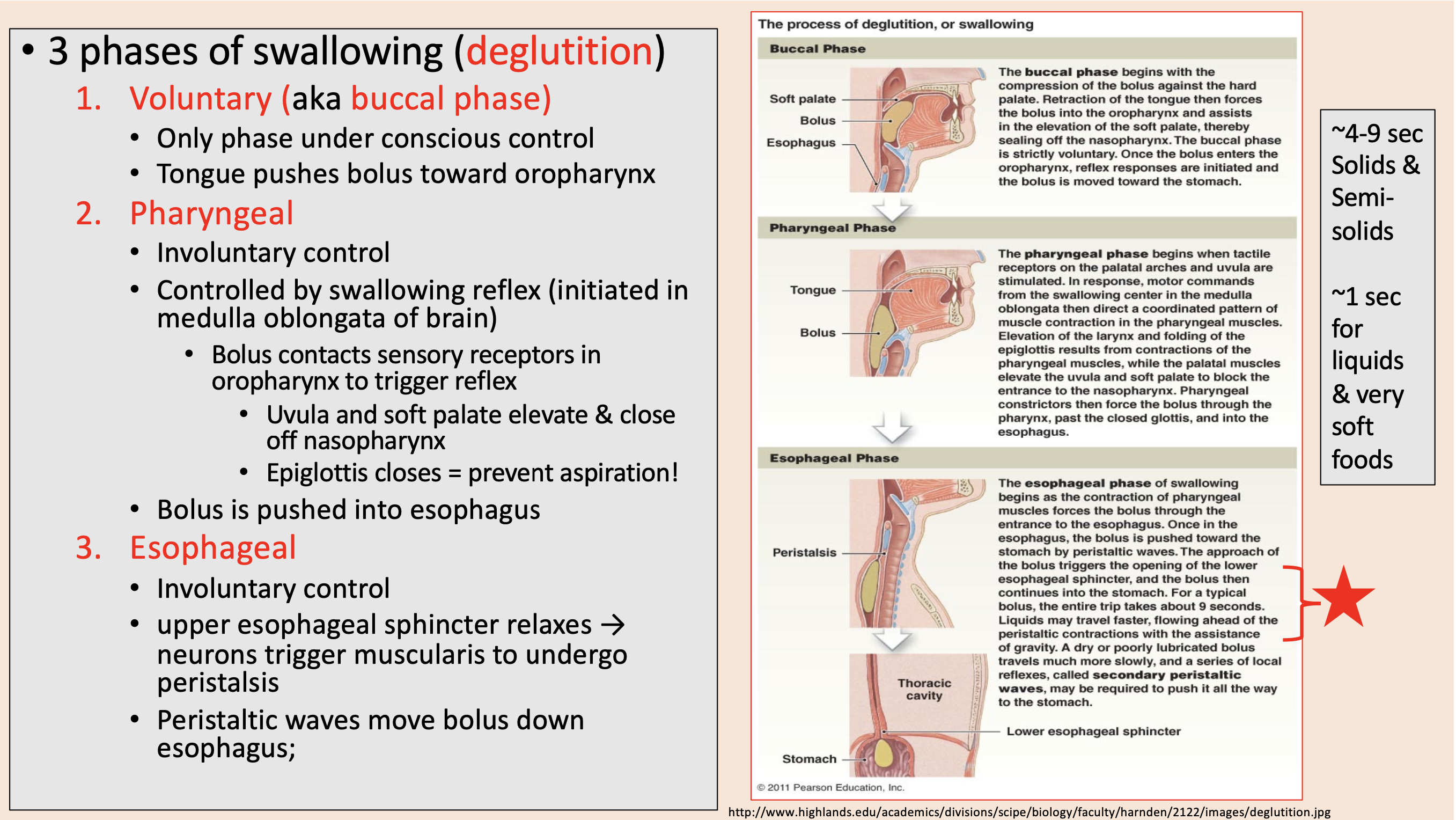
Epiglottis closes
prevent aspiration
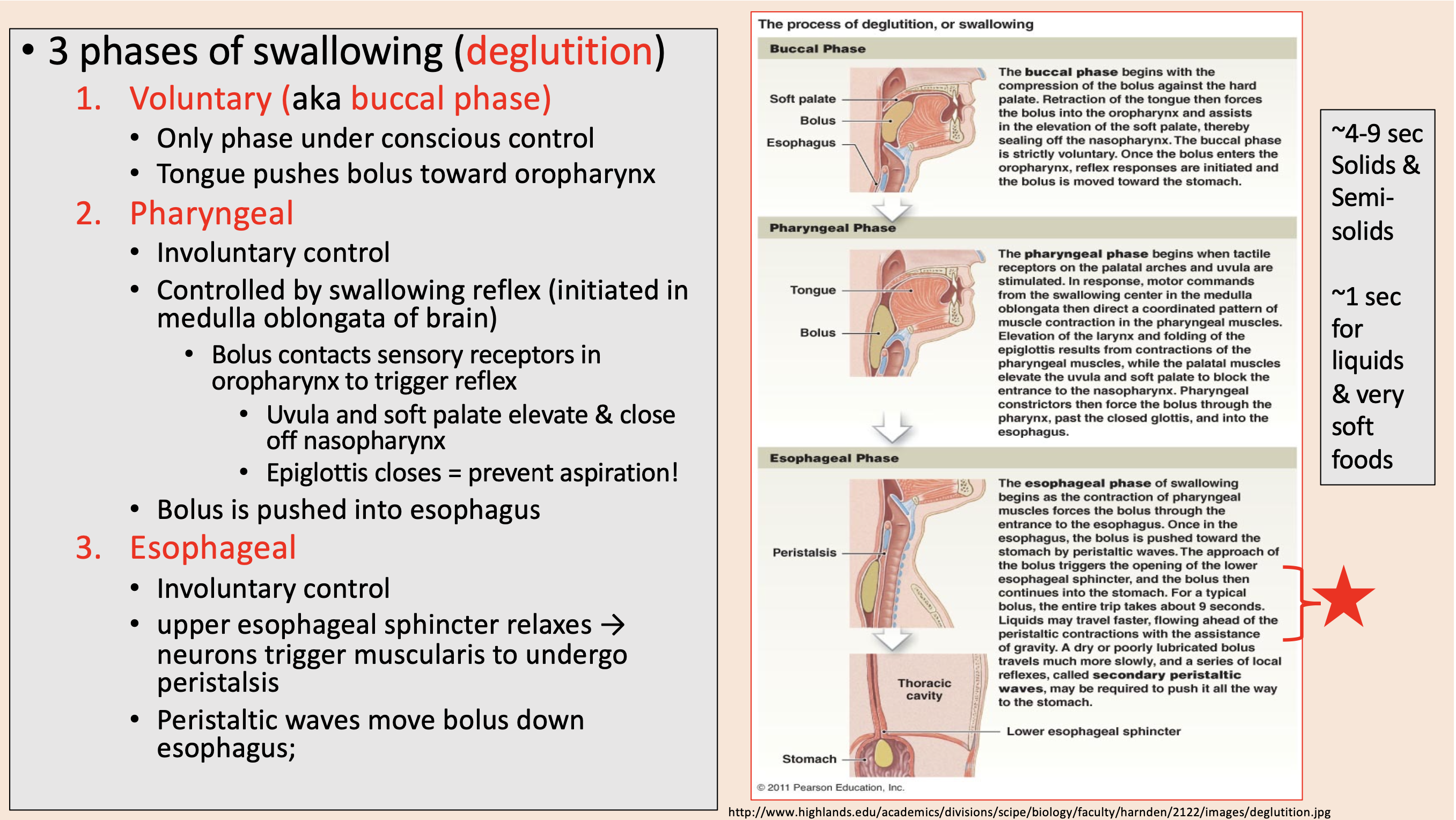
Involuntary control.
upper esophageal sphincter relaxes → neurons trigger muscularis to undergo peristalsis.
Peristaltic waves move bolus down esophagus.
esophageal
Lower esophageal sphincter fails to close adequately.
Stomach contents reflux – including the HCl.
The HCl irritates the lining of the esophageal wall = heart burn!
Gastroesophageal Reflux Disease (GERD)

5 anatomical regions of the stomach:
cardia
fundus
body
pyloricantrum
pylorus
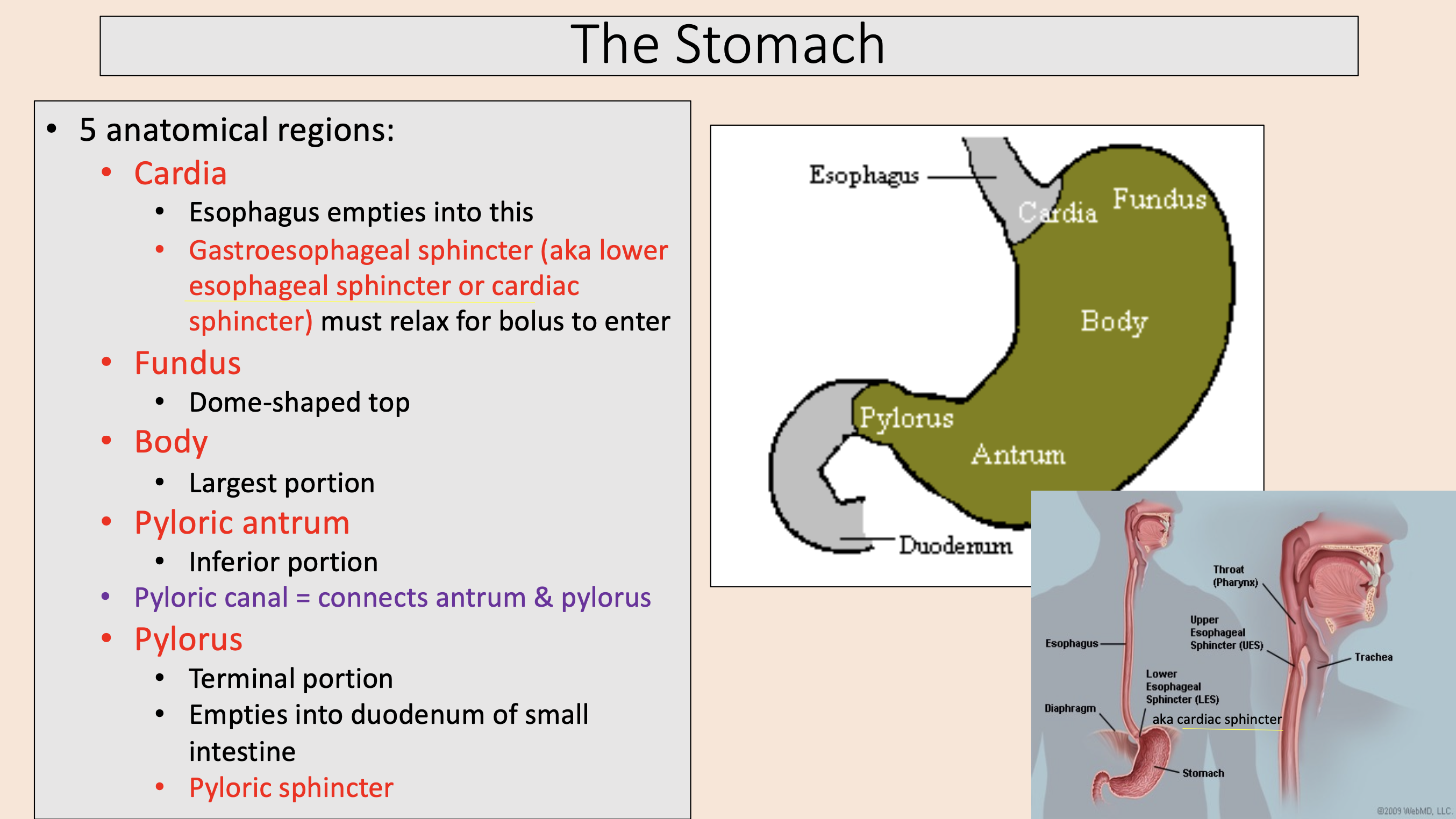
Esophagus empties into this.
Gastroesophageal sphincter (aka lower esophageal sphincter or cardiac sphincter) must relax for bolus to enter.
cardia
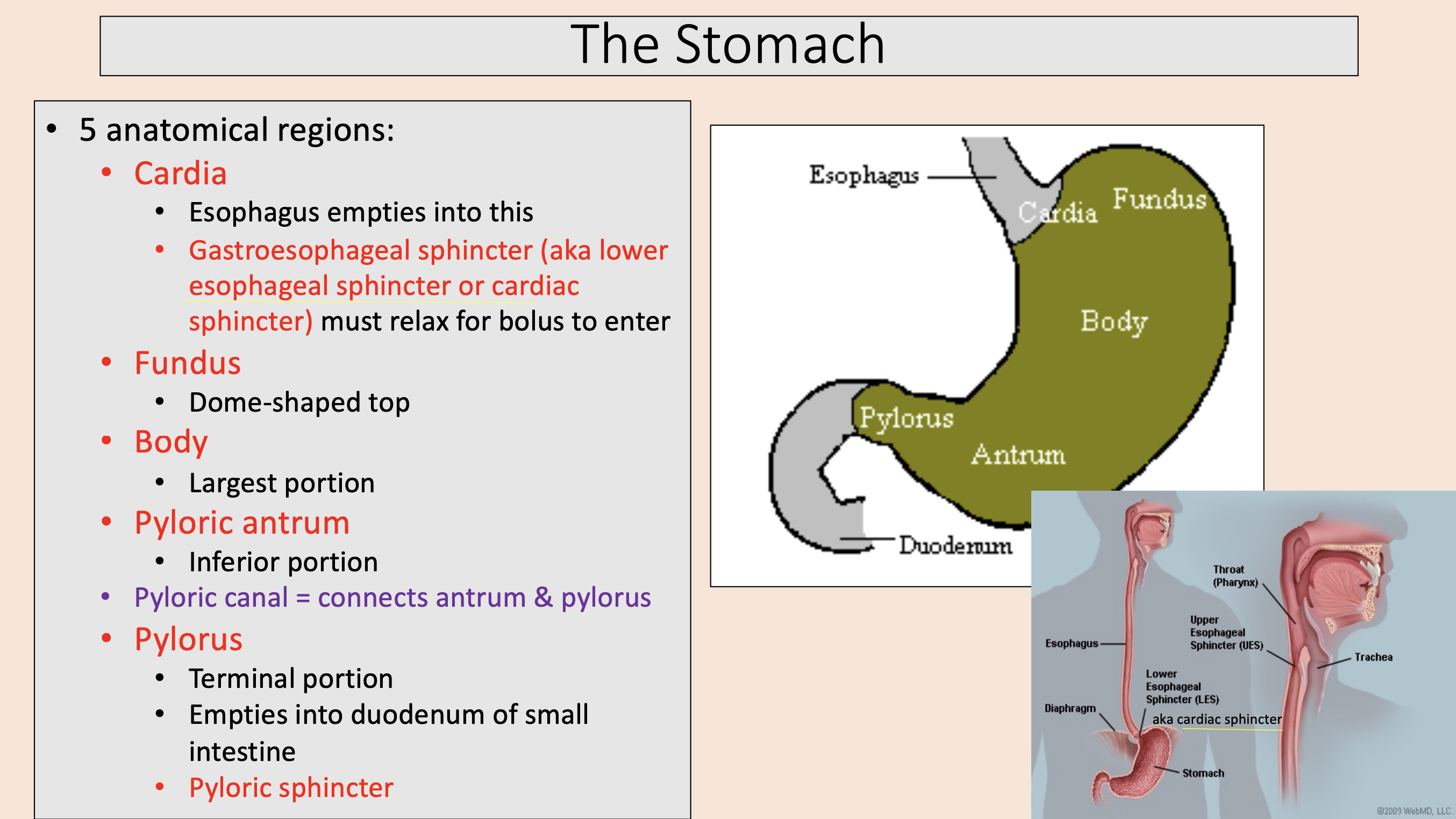
Dome-shaped top
fundus
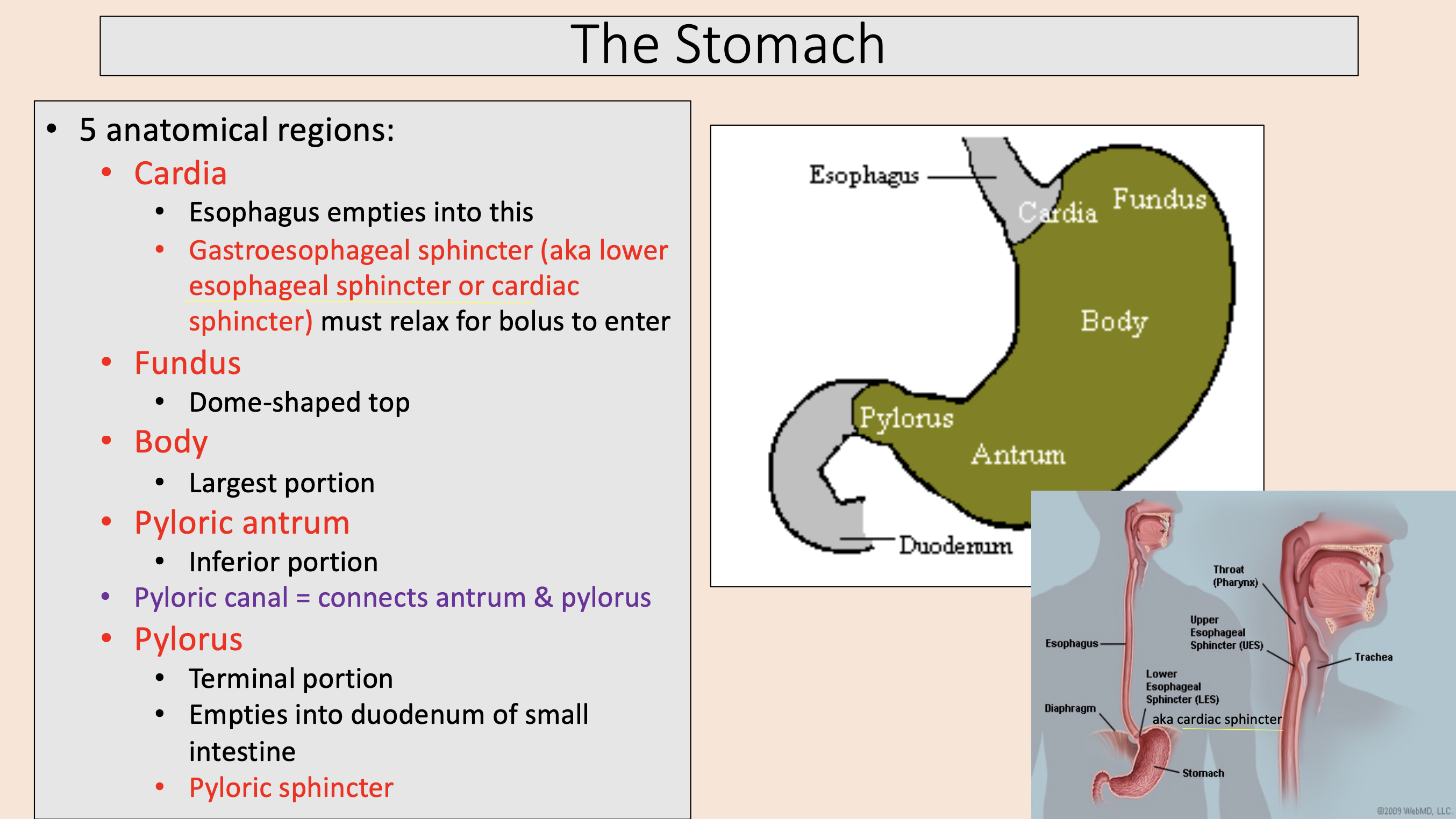
Largest portion
body
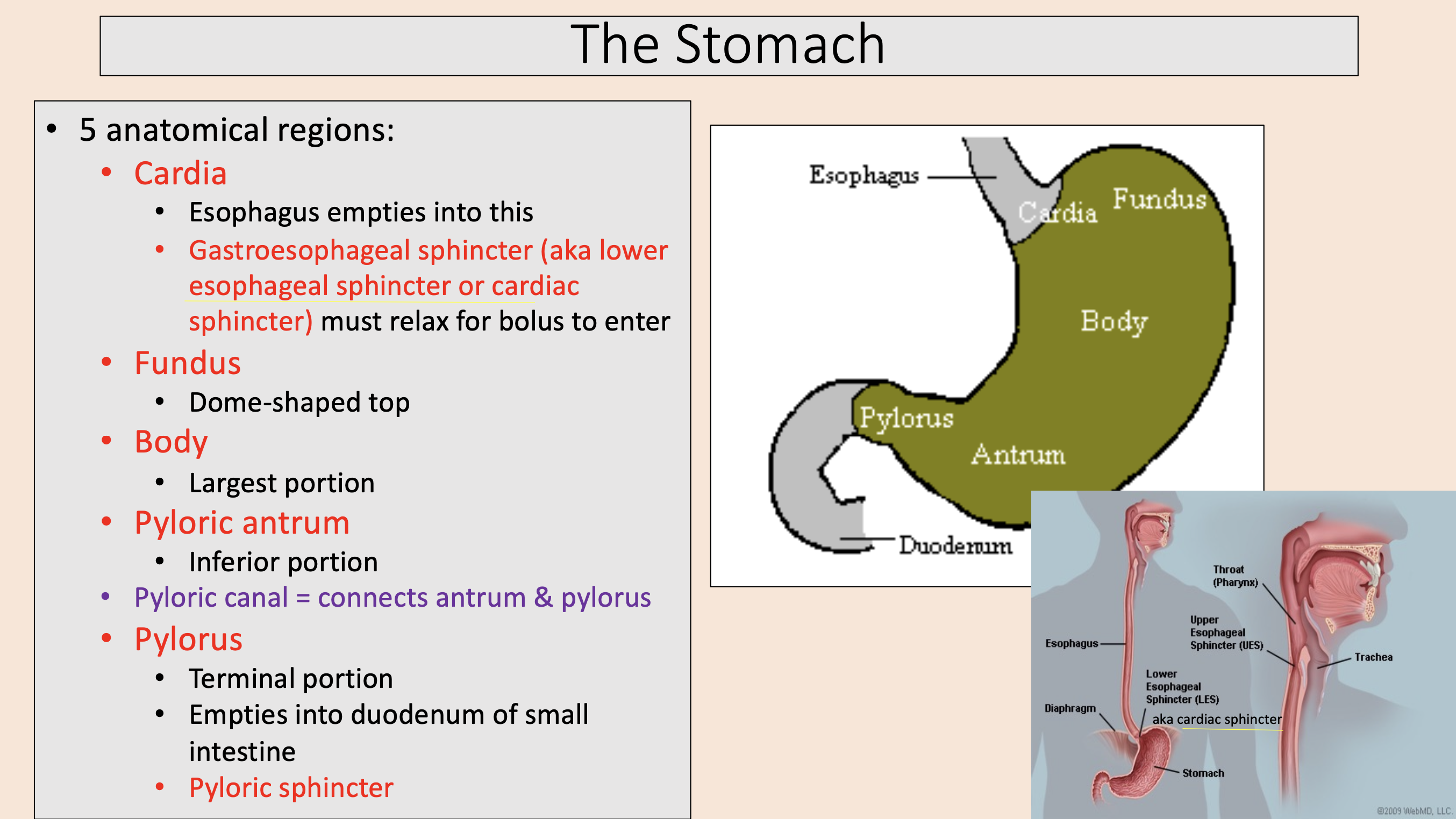
Inferior portion
pyloric antrum
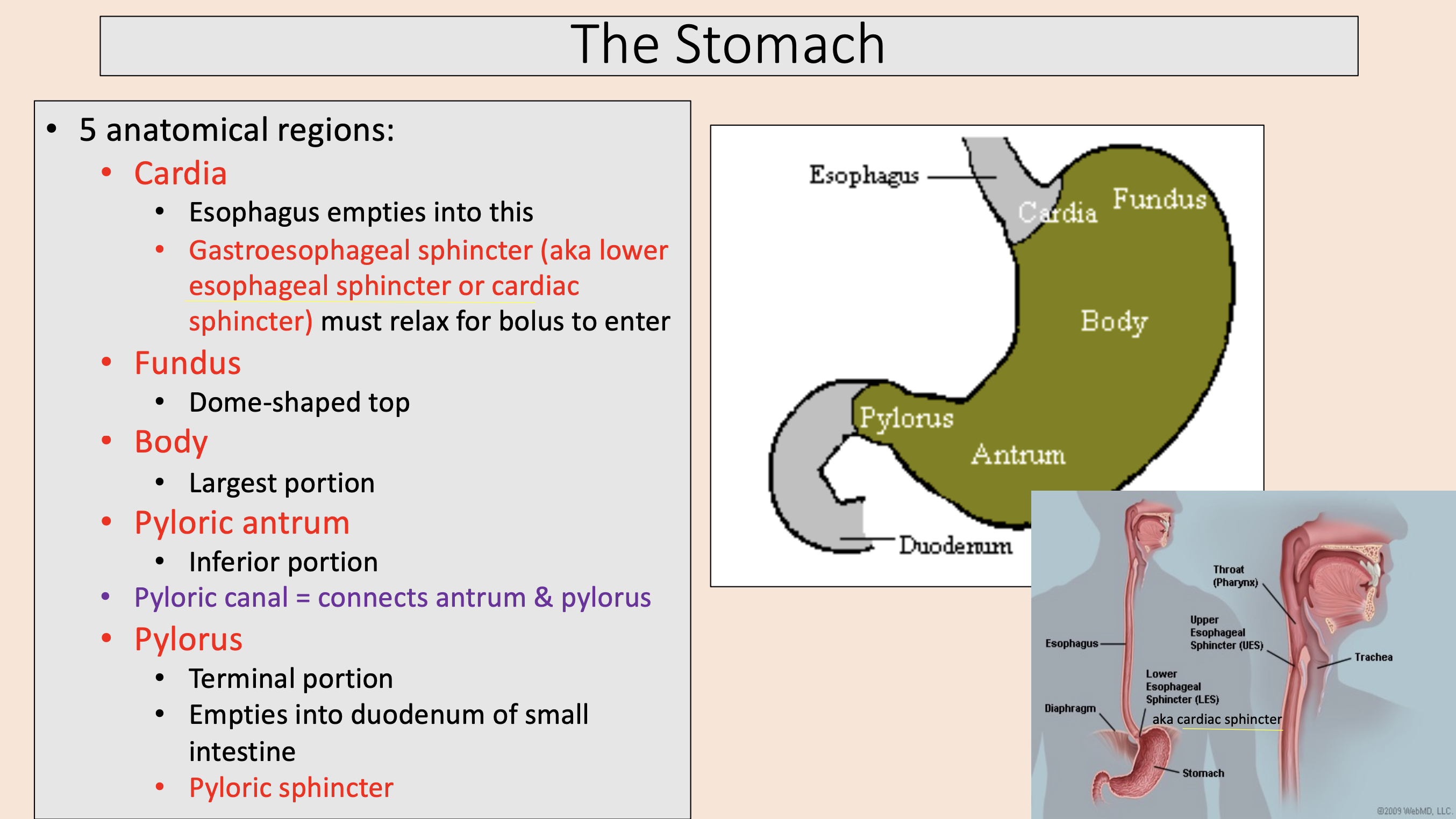
connects antrum & pylorus
pyloric canal
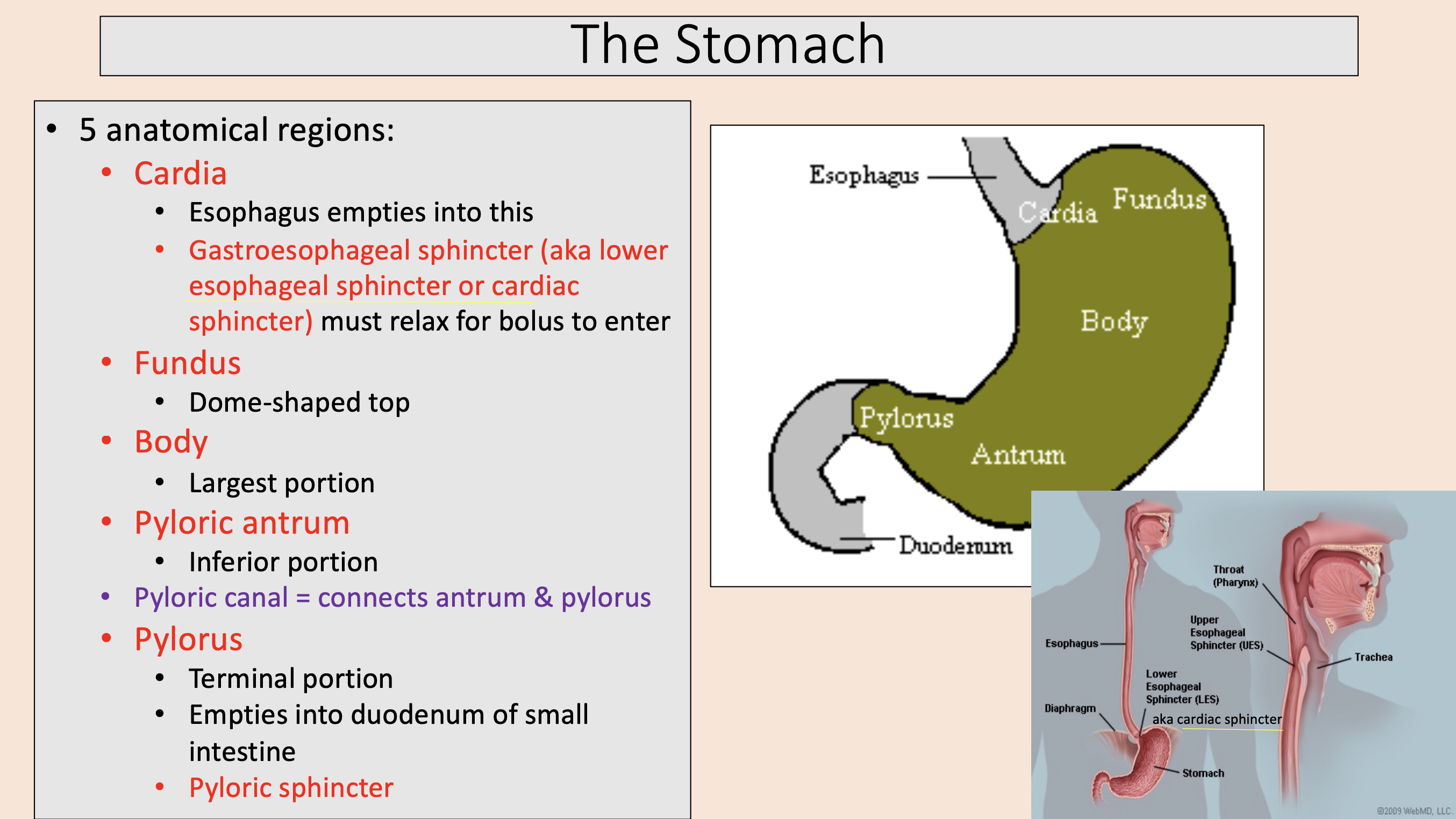
Terminal portion.
Empties into duodenum of small intestine.
Pyloric sphincter.
pylorus
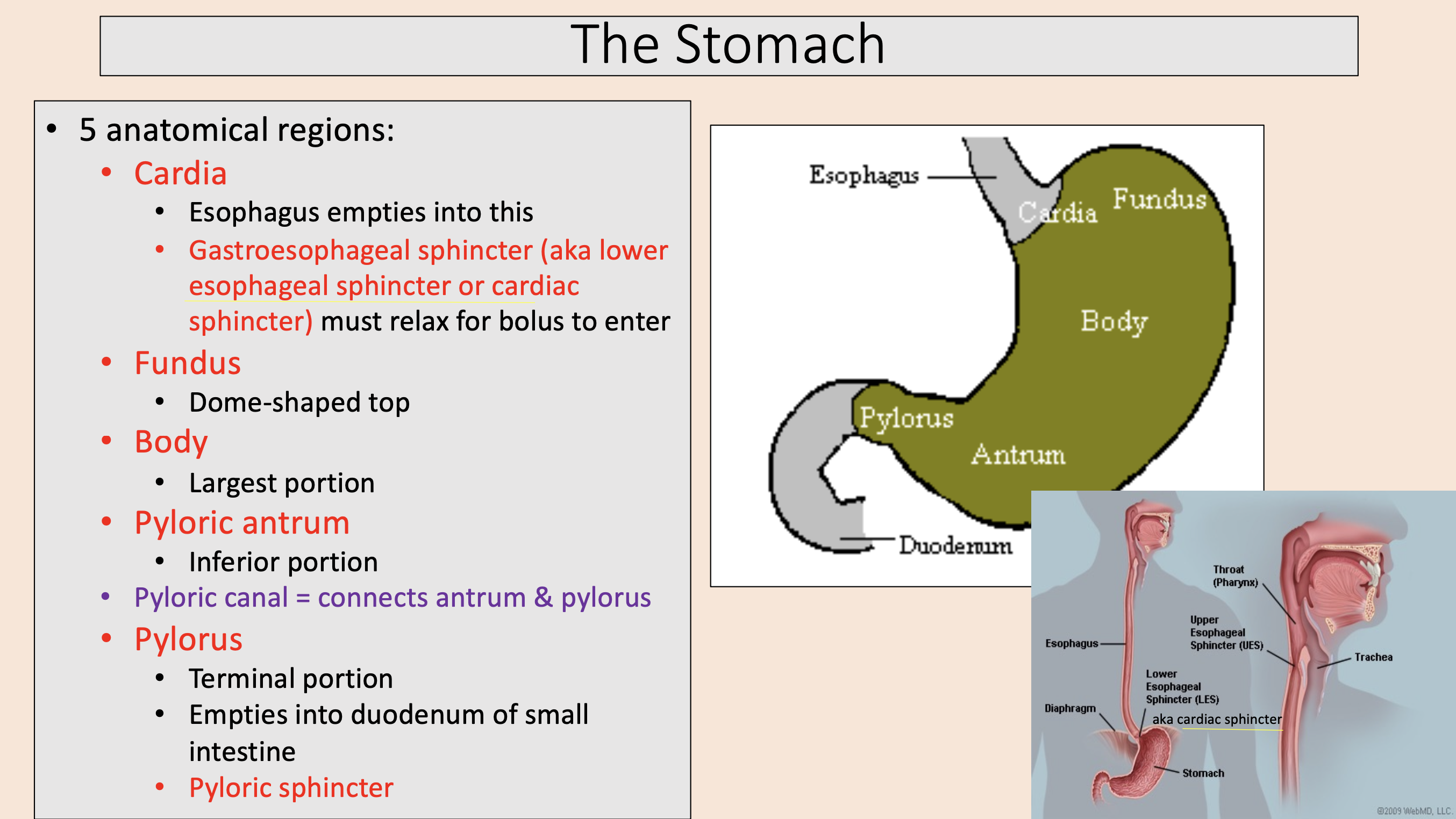
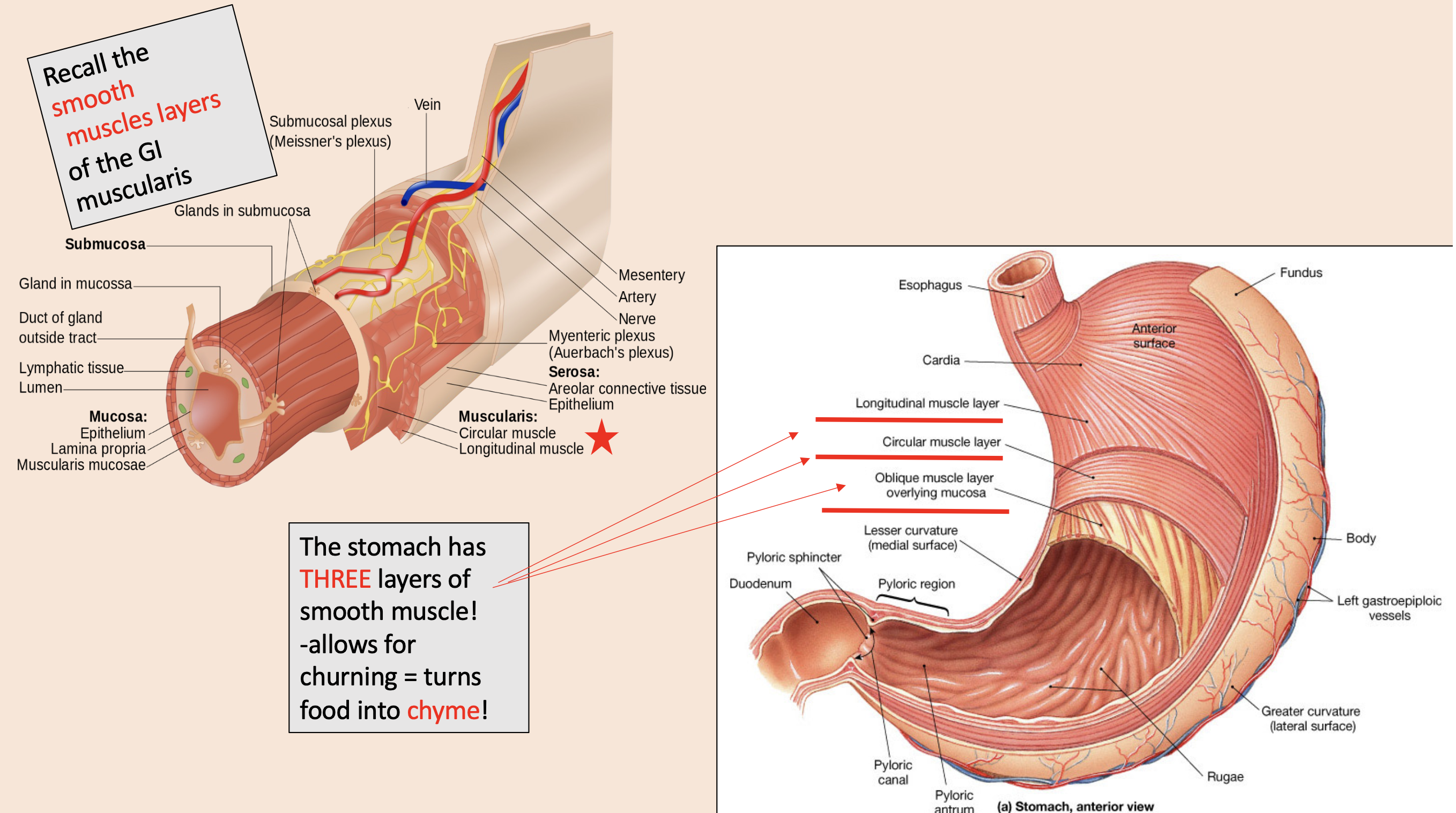
THREE layers of smooth muscle in the stomach
longitudinal muscle layer
circular muscle layer
oblique muscle layer overlying mucosa
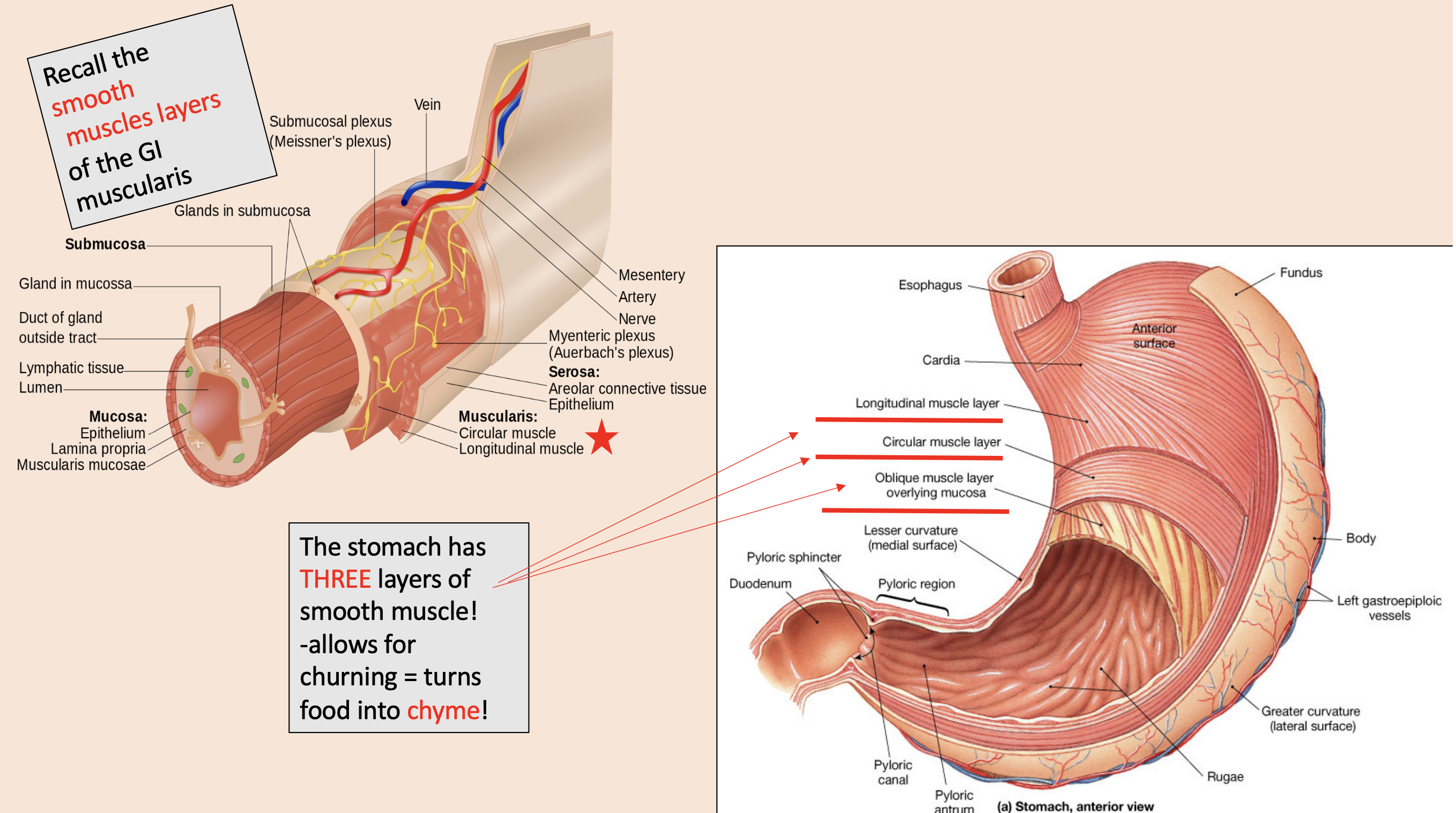
churning = turns food into
chyme
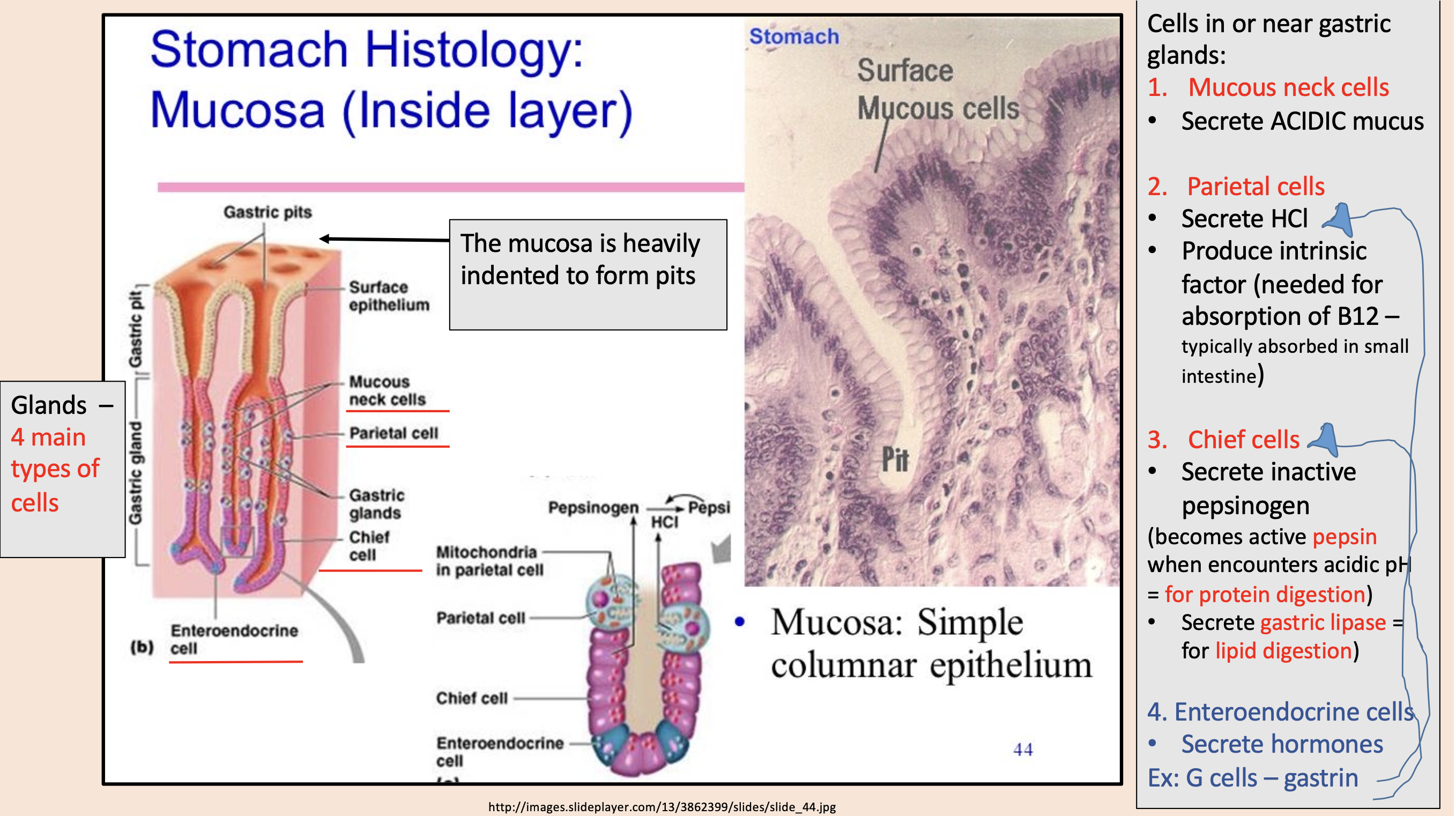
Secrete ACIDIC mucus
mucous neck cells
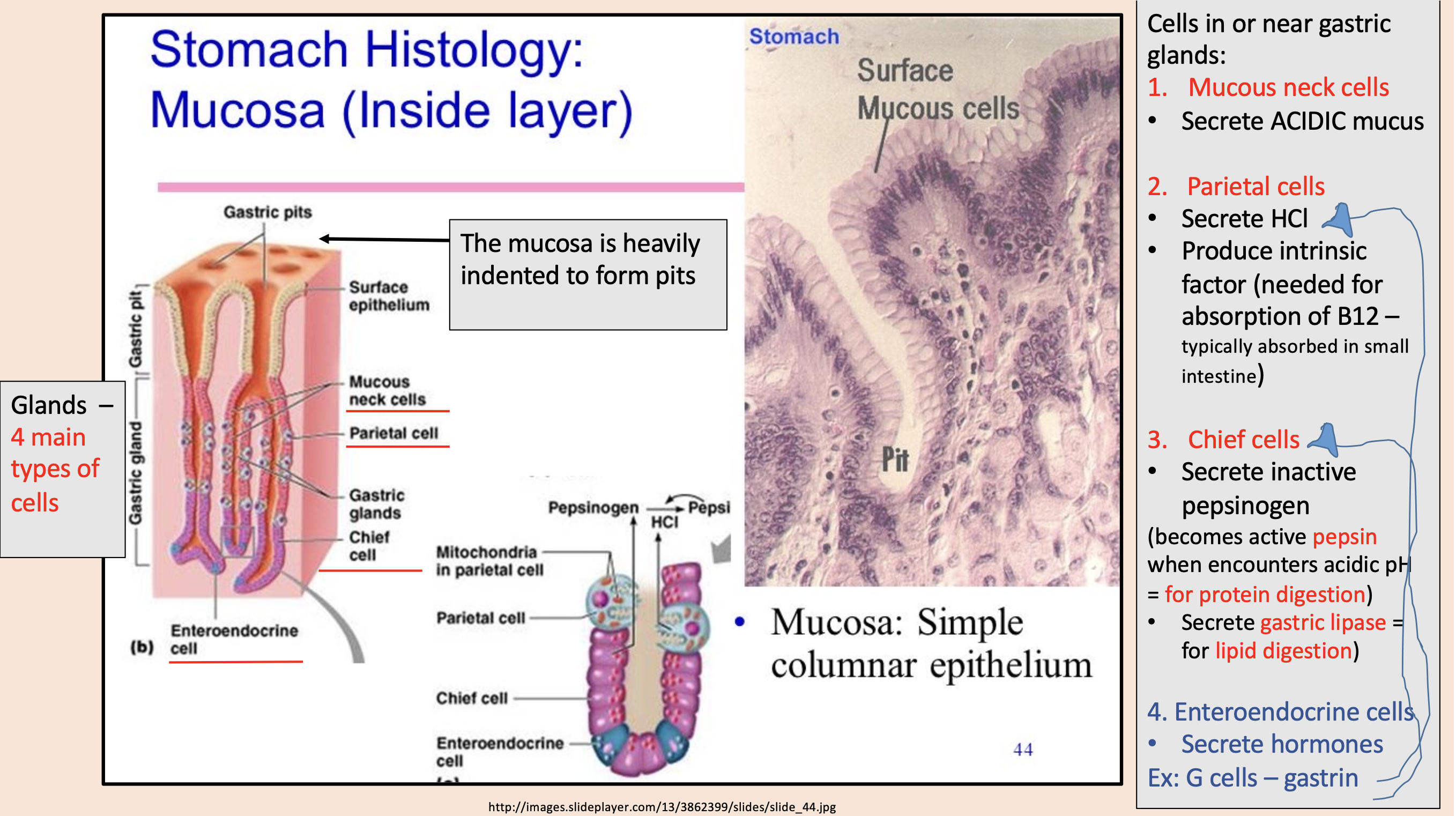
Secrete HCl.
Produce intrinsic factor (needed for absorption of B12 – typically absorbed in small intestine).
parietal cells
Secrete inactive pepsinogen (becomes active pepsin when encounters acidic pH = for protein digestion.
Secrete gastric lipase = for lipid digestion)
chief cells
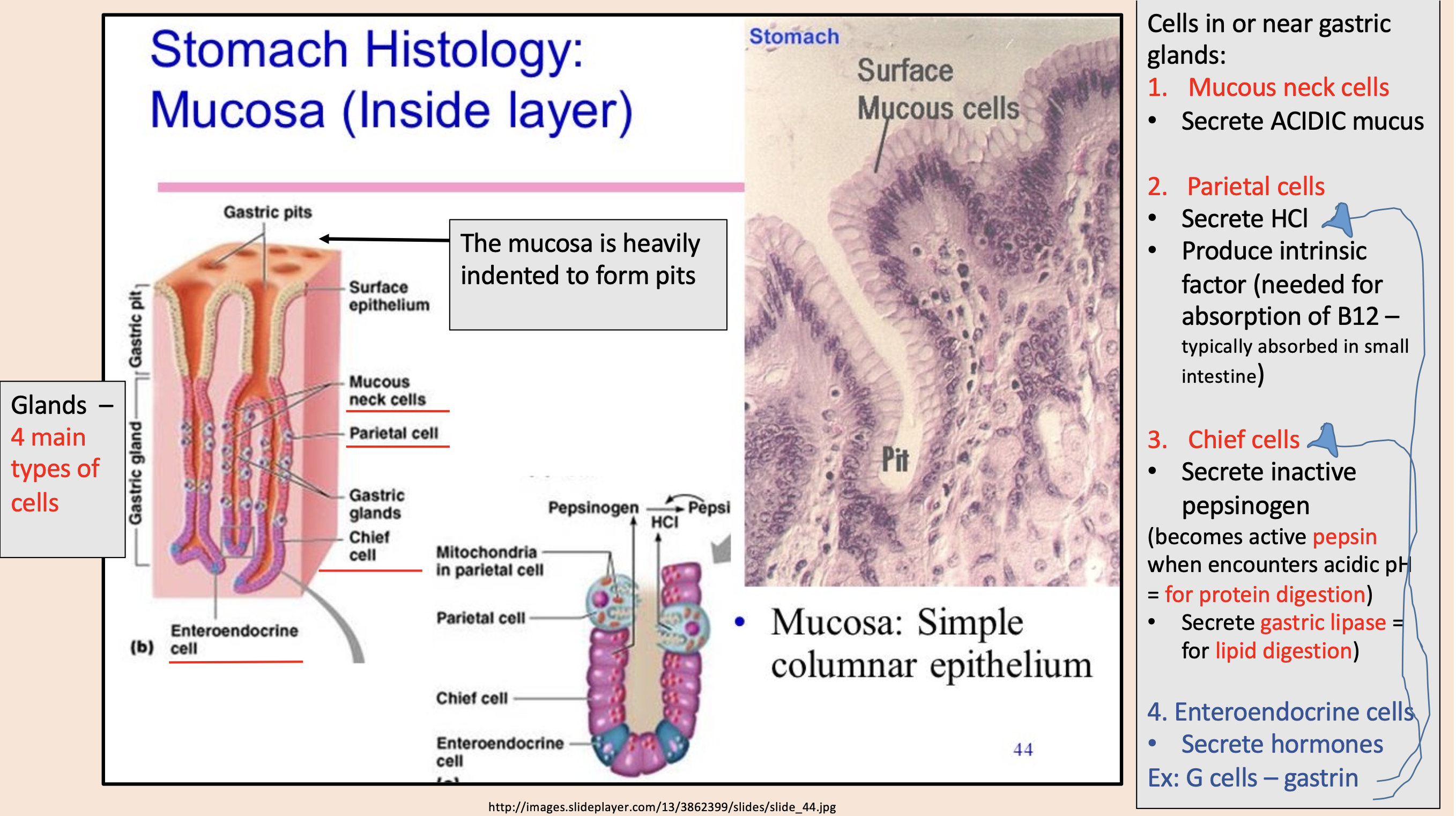
Secrete hormones
enteroendocrine cells
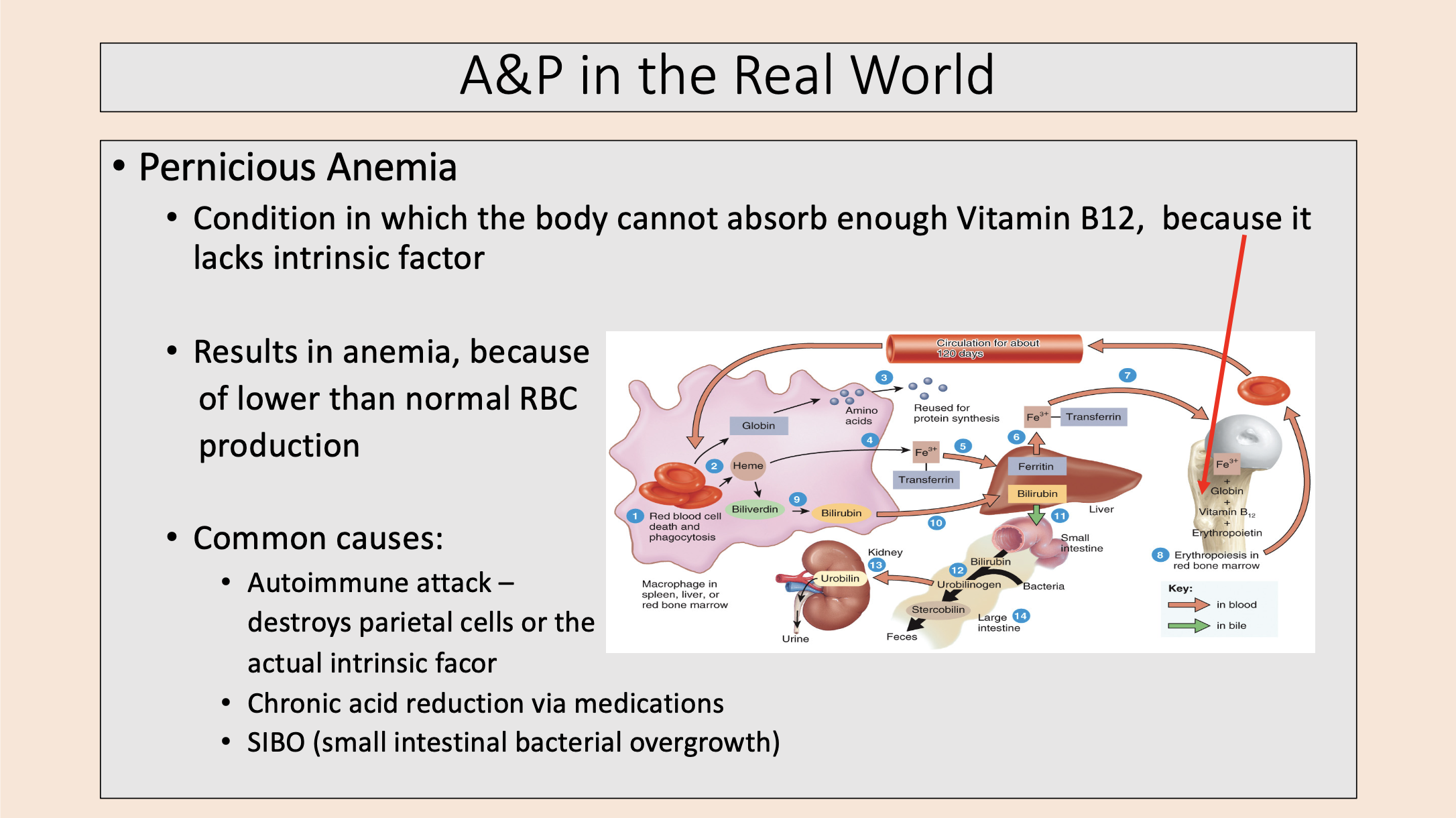
Condition in which the body cannot absorb enough Vitamin B12, because it lacks intrinsic factor.
pernicious anemia
3 divisions of the small intestine
duodenum
jejunum
ileum
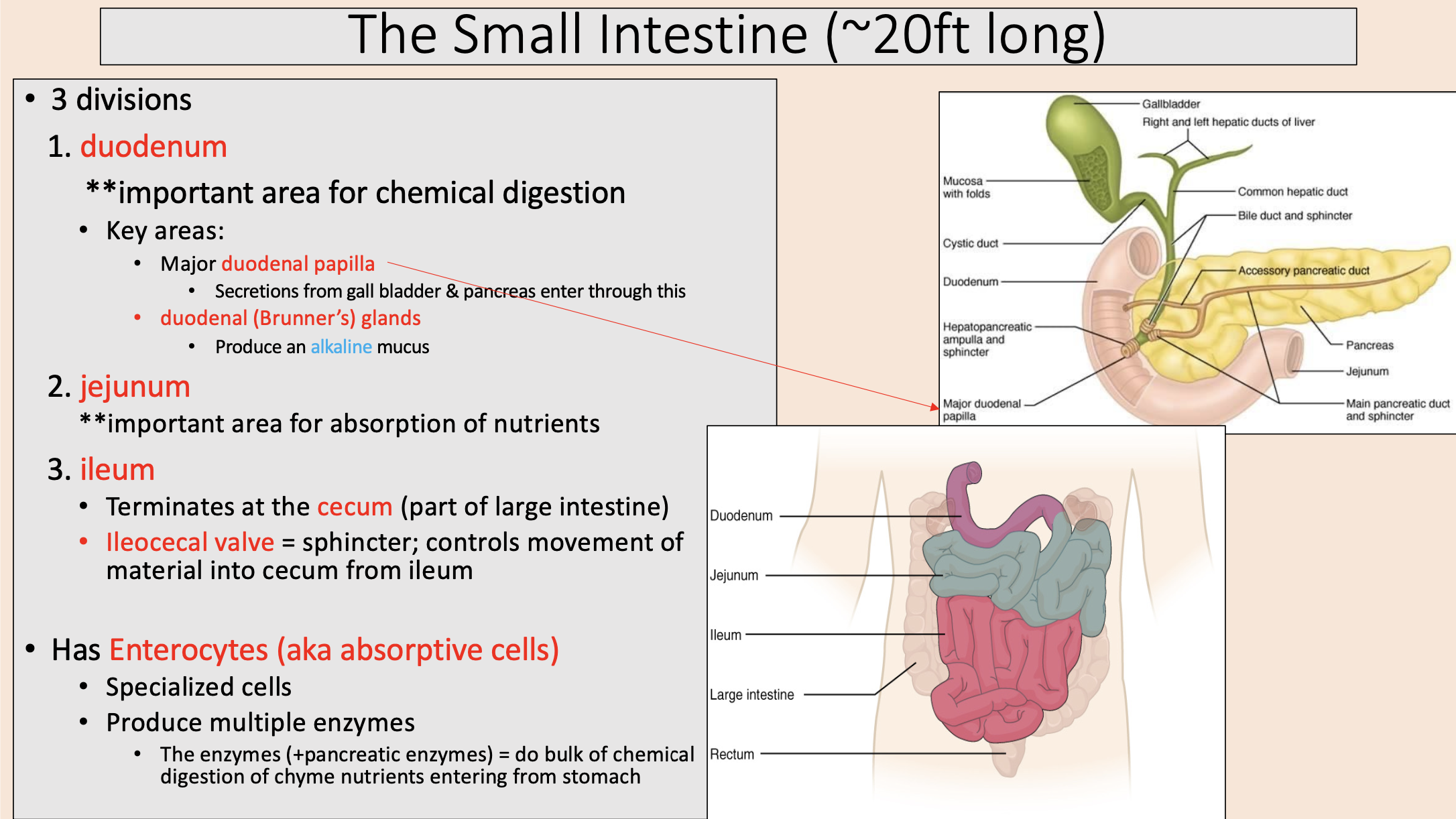
important area for chemical digestion
duodenum
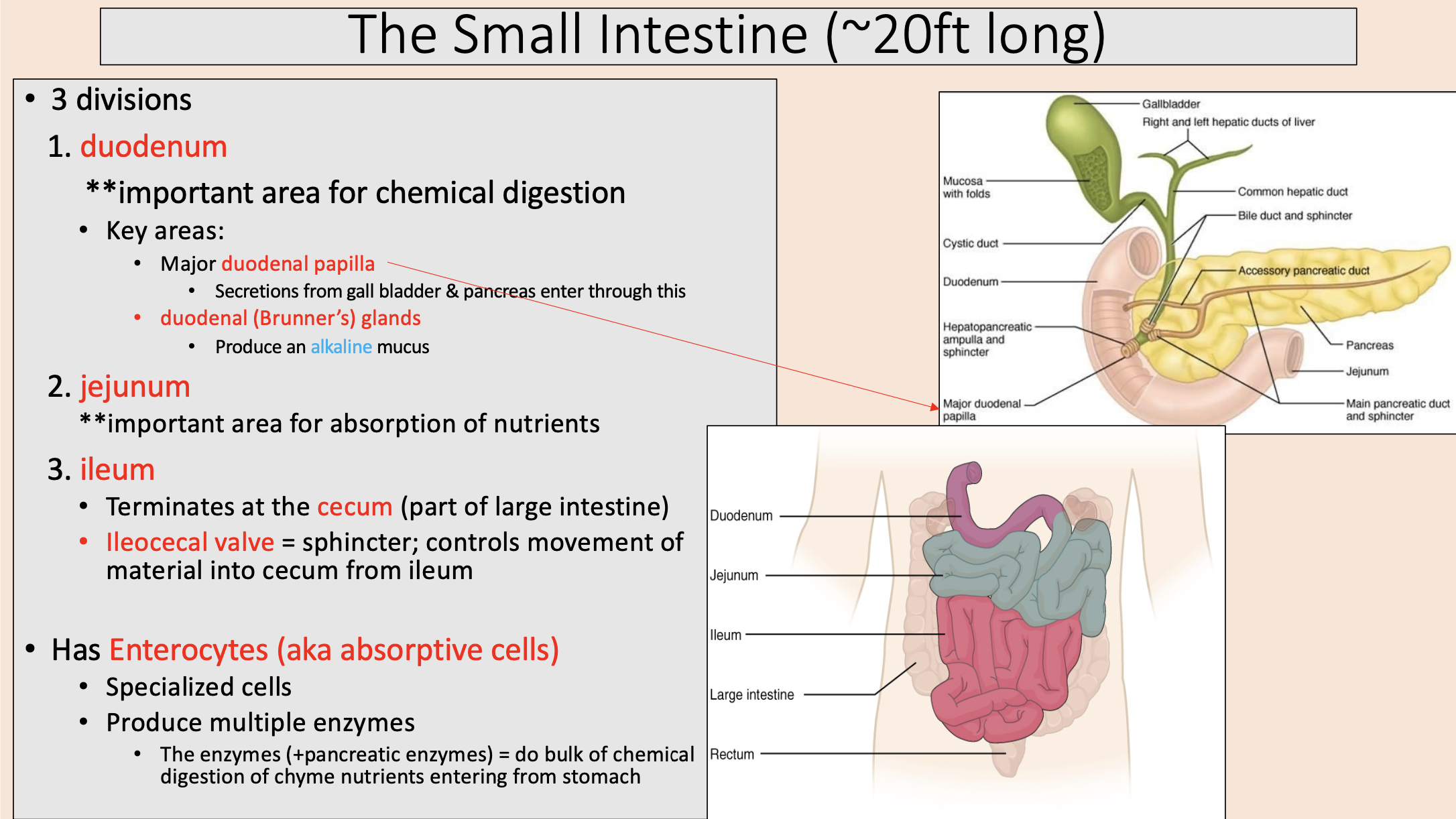
Secretions from gall bladder & pancreas enter through this
major duodenal papilla
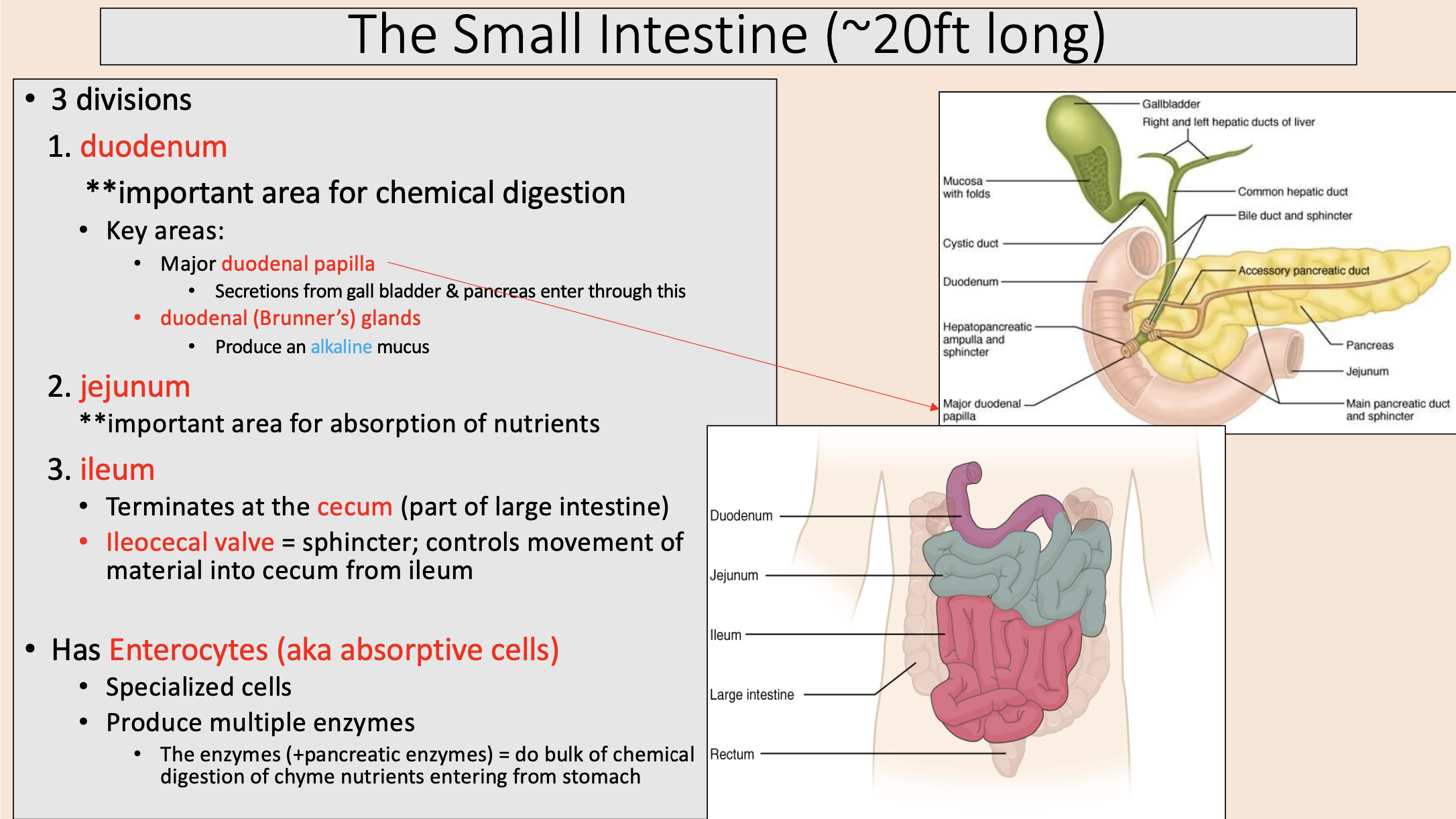
Produce an alkaline mucus
duodenal (Brunner’s) glands
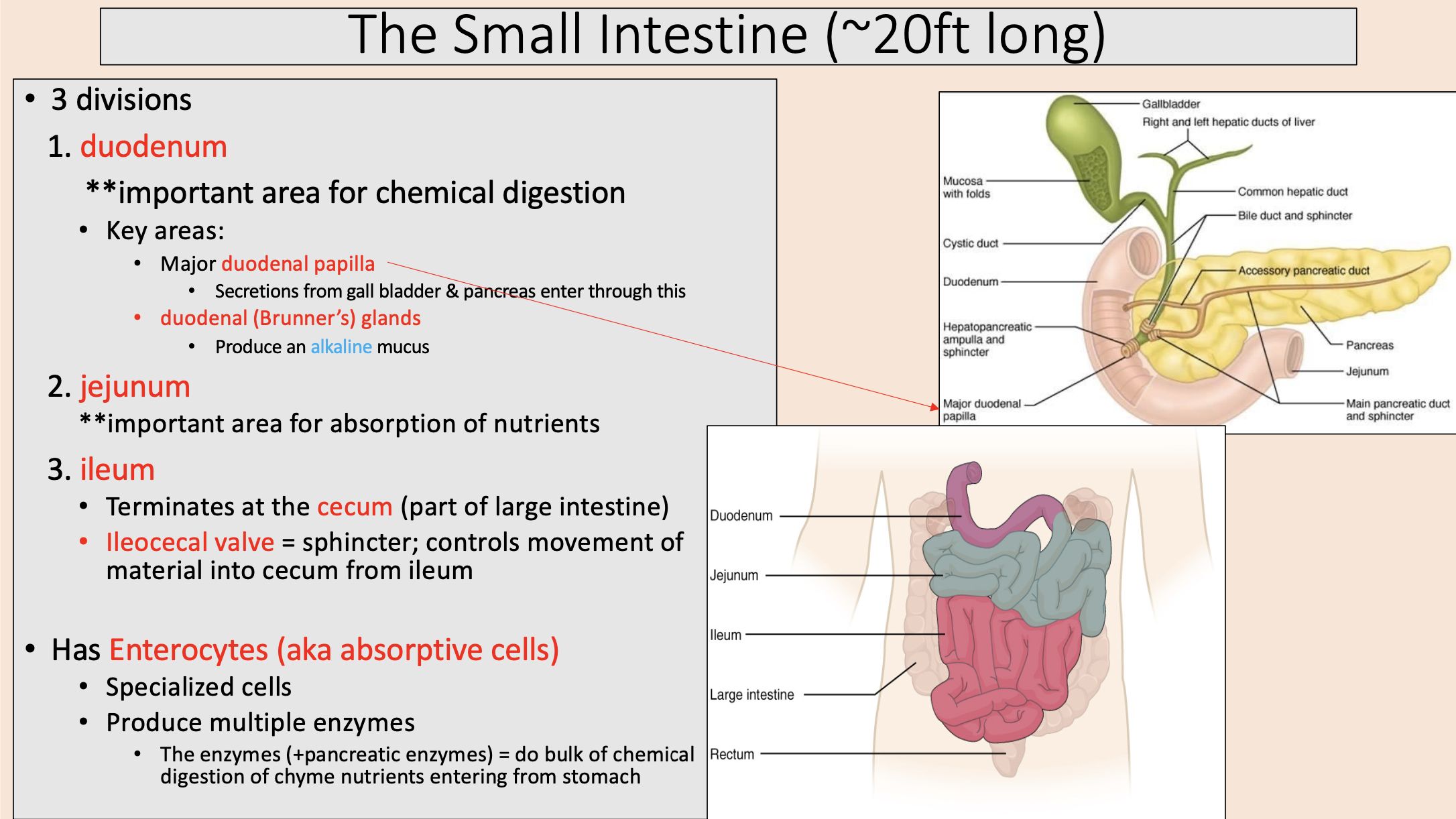
important area for absorption of nutrients
jejunum
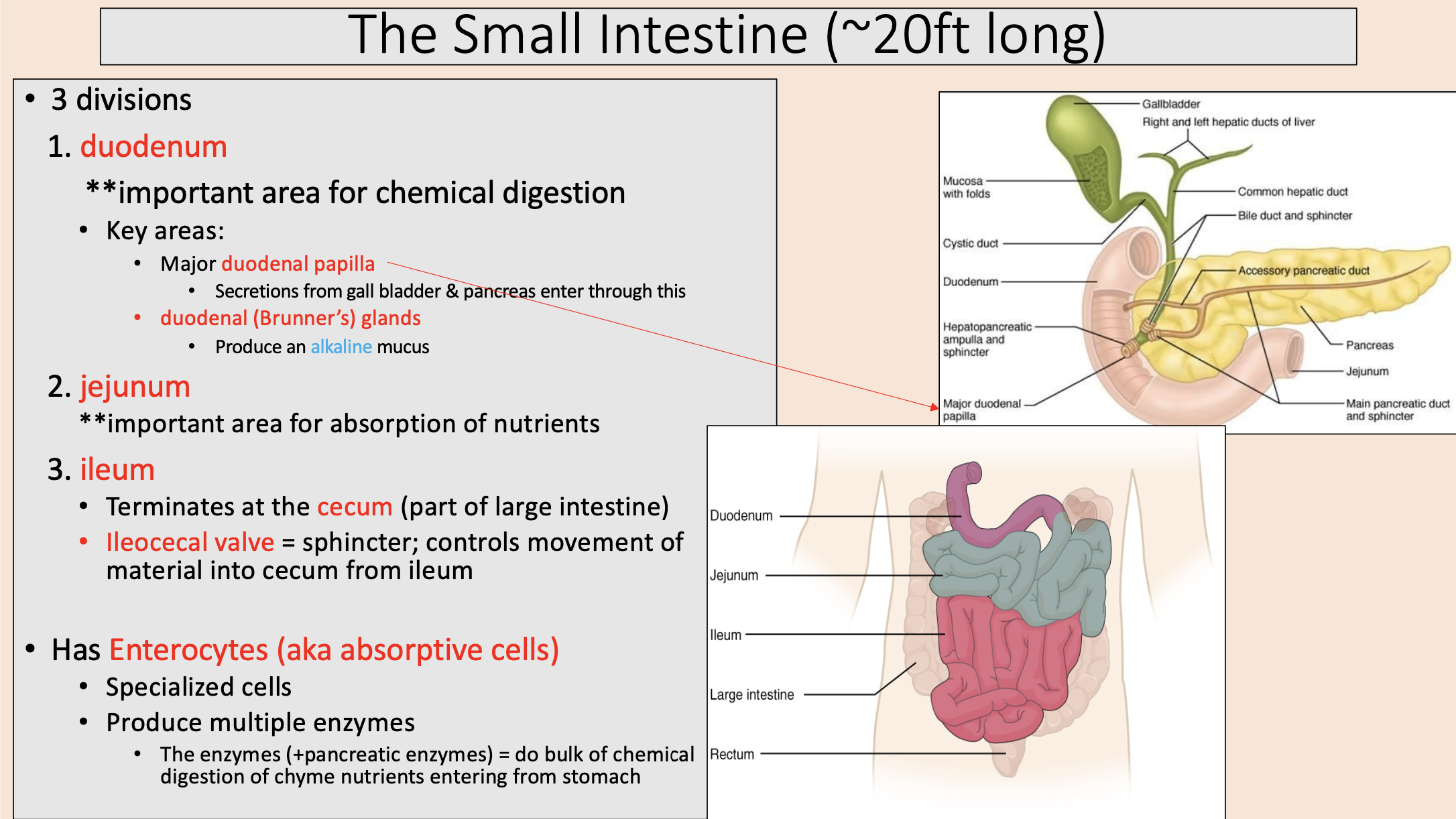
Terminates at the cecum (part of large intestine)
ileum
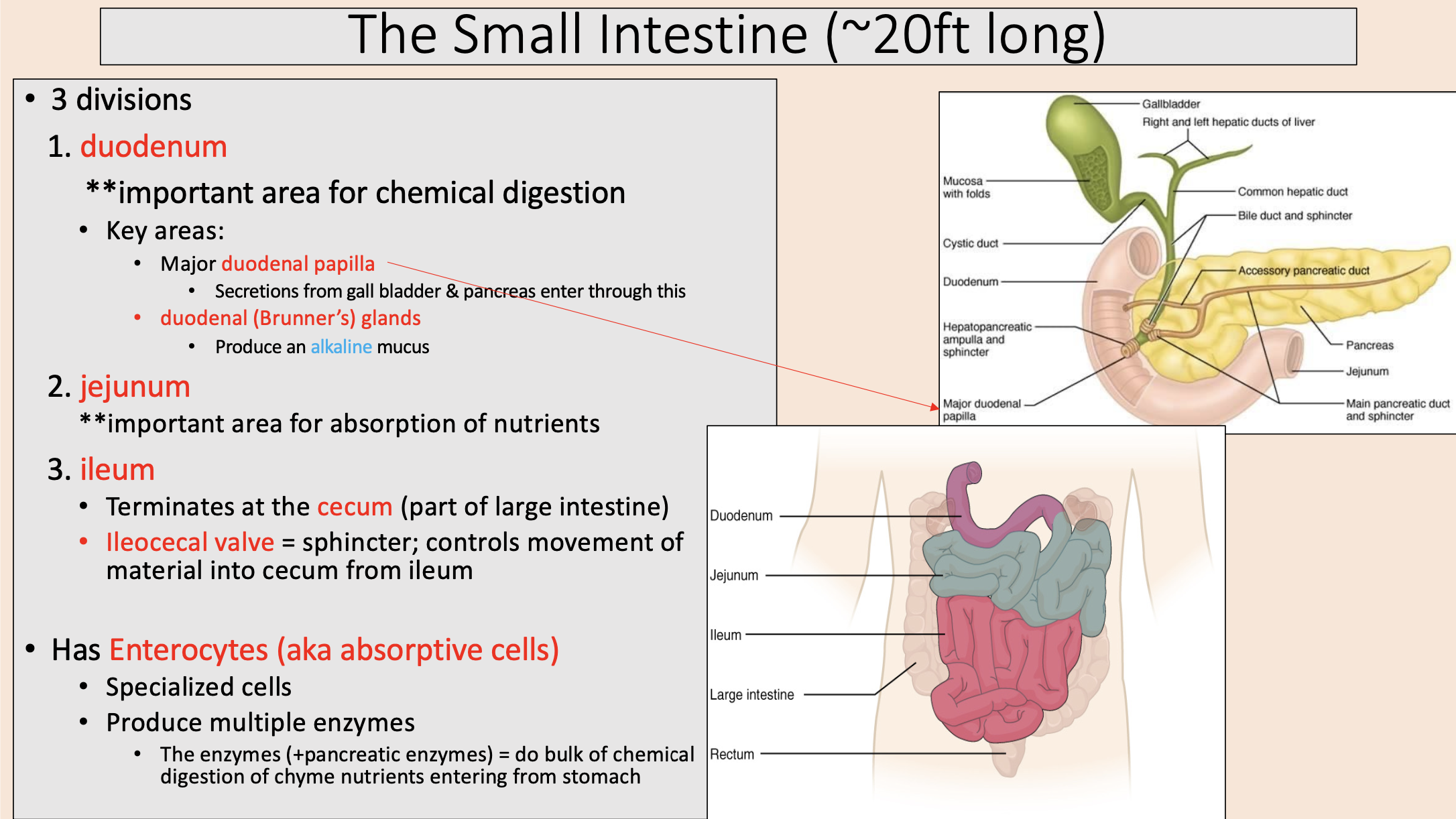
sphincter; controls movement of material into cecum from ileum
ileocecal valve