Why do multicellular and unicellular organisms need nutrients and oxygen?

To sustain life by providing energy, growth, and eliminating waste.
What are the benefits of multicellularity?
More protection, resource sharing, and specialization/compartmentalization
What are the downsides of multicellularity?
Competition with neighboring cells for resources and more waste products requiring efficient cell cleaning to prevent toxicity.
How does the circulatory system address the needs of multicellular organisms?
By distributing nutrients, transporting gases, removing waste, transporting hormones, maintaining homeostasis, and preventing excessive bleeding.
How are nutrients distributed in the body?
Nutrients are distributed from the digestive tract, liver, and adipose tissue to ensure cells receive nutrients for energy and growth.
How are gases transported in the body?
Oxygen is transported from the lungs to body tissues, and carbon dioxide is transported from tissues to the lungs
How is waste removed from body tissues?
Waste is transported from tissues to the excretory system (kidneys) for elimination.
What role does the circulatory system play in hormone transport?
It transports hormones to target organs to regulate and balance body functions.
What is perfusion?
The flow of blood through tissue, essential for the delivery of oxygen and nutrients and the removal of waste products.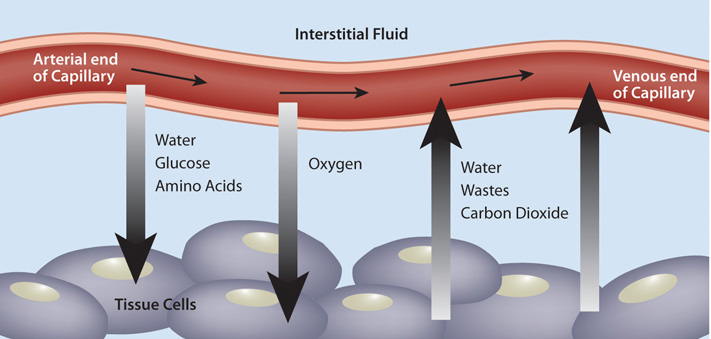
What is ischemia?
Inadequate blood flow to tissue, leading to tissue damage and a buildup of metabolic waste.
What is hypoxia?
Adequate blood flow but a reduction of oxygen in the tissue.
What is the key difference between hypoxia and ischemia?
Hypoxia has enough blood flow but not enough oxygen, while ischemia has reduced or blocked blood flow even if there is enough oxygen.
How does the circulatory system help maintain homeostasis?
By regulating body temperature and preventing excessive bleeding.
What is the correct order of blood flow through the heart starting from the venae cavae?
Venae cavae → Right atrium → Tricuspid valve → Right ventricle → Pulmonary valve → Pulmonary artery → Lungs → Pulmonary veins → Left atrium → Mitral valve → Left ventricle → Aortic valve → Aorta → Body tissues (capillaries) → Systemic veins.
What is the function of the atria in the heart?
Atria act as reservoirs where blood collects from veins before being pumped into the ventricles. They are thin-walled structures that receive blood.
What is the function of the ventricles in the heart?
Ventricles are muscular chambers that pump blood out of the heart at high pressure to the arteries. They are thick and muscular for powerful contractions.
Describe pulmonary circulation.
The right side of the heart pumps blood to the lungs and back.
Describe systemic circulation.
The left side of the heart pumps blood to the rest of the body and back.

What is the coronary sinus?
It is the largest vein that drains deoxygenated blood from the heart muscle to the right atrium.
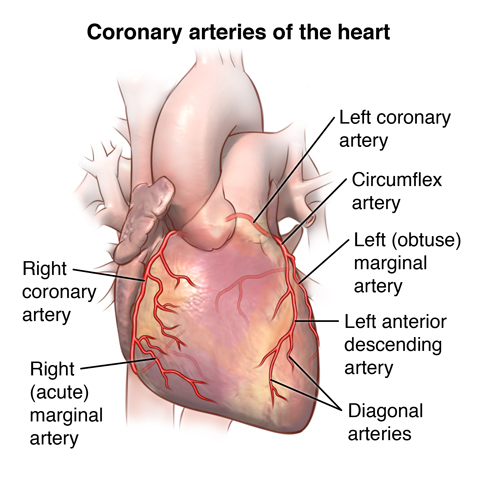
What is the role of the coronary artery?
It supplies oxygenated blood to the heart muscle (myocardium).
What is the function of the atrioventricular (AV) valves?
They prevent backflow of blood from the ventricles to the atria during contraction.
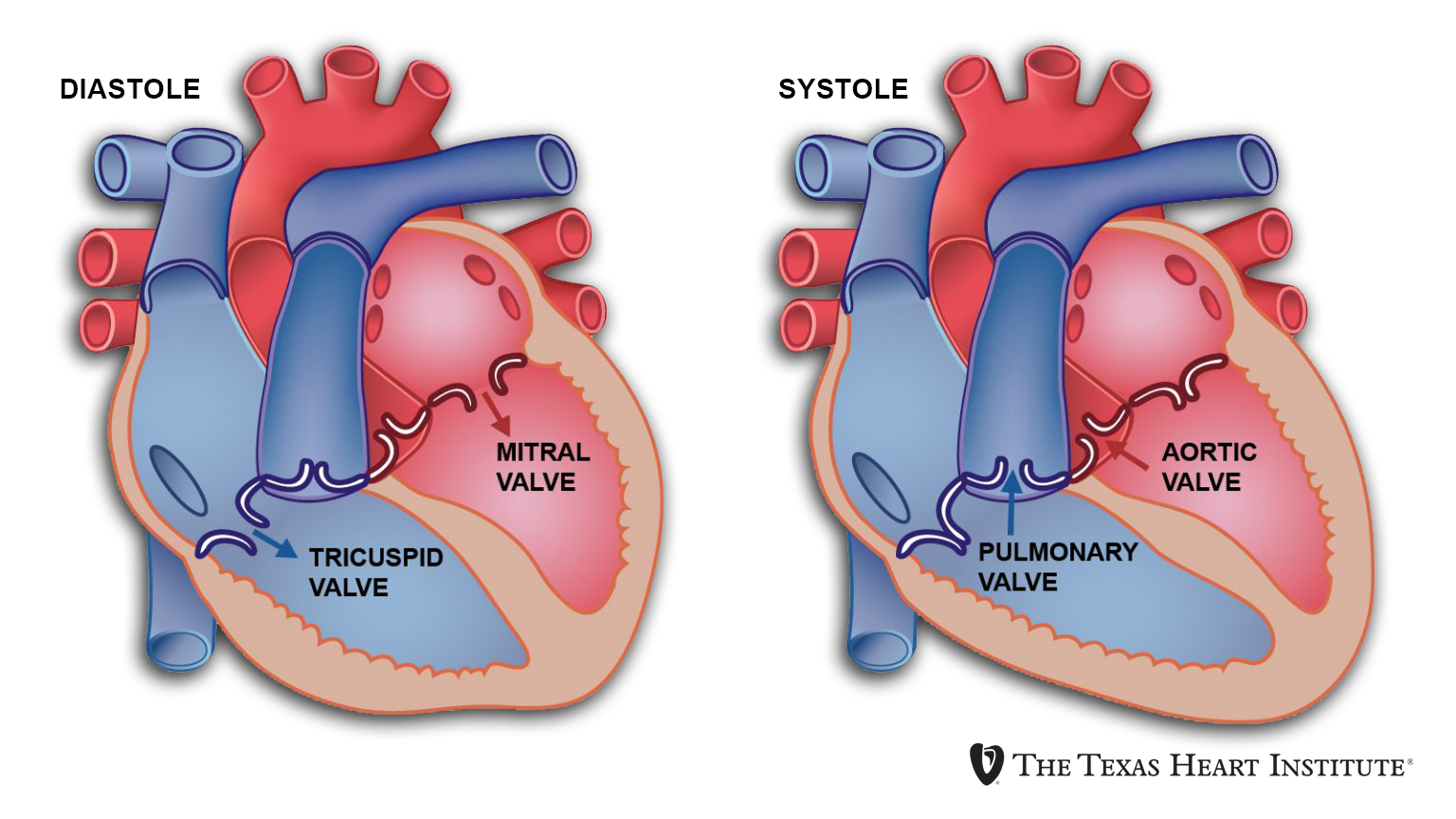
Where is the mitral (bicuspid) valve located?
Between the left atrium and the left ventricle.

Where is the tricuspid valve located?
Between the right atrium and the right ventricle.

What is the function of the semilunar valves?
They prevent backflow of blood from the arteries to the ventricles.

Where is the pulmonary valve located?
Between the right ventricle and the pulmonary artery.

Where is the aortic valve located?
Between the left ventricle and the aorta.

What happens during diastole?
Heart chambers relax and fill with blood, atrial contraction aids in filling ventricles, and pressure decreases.
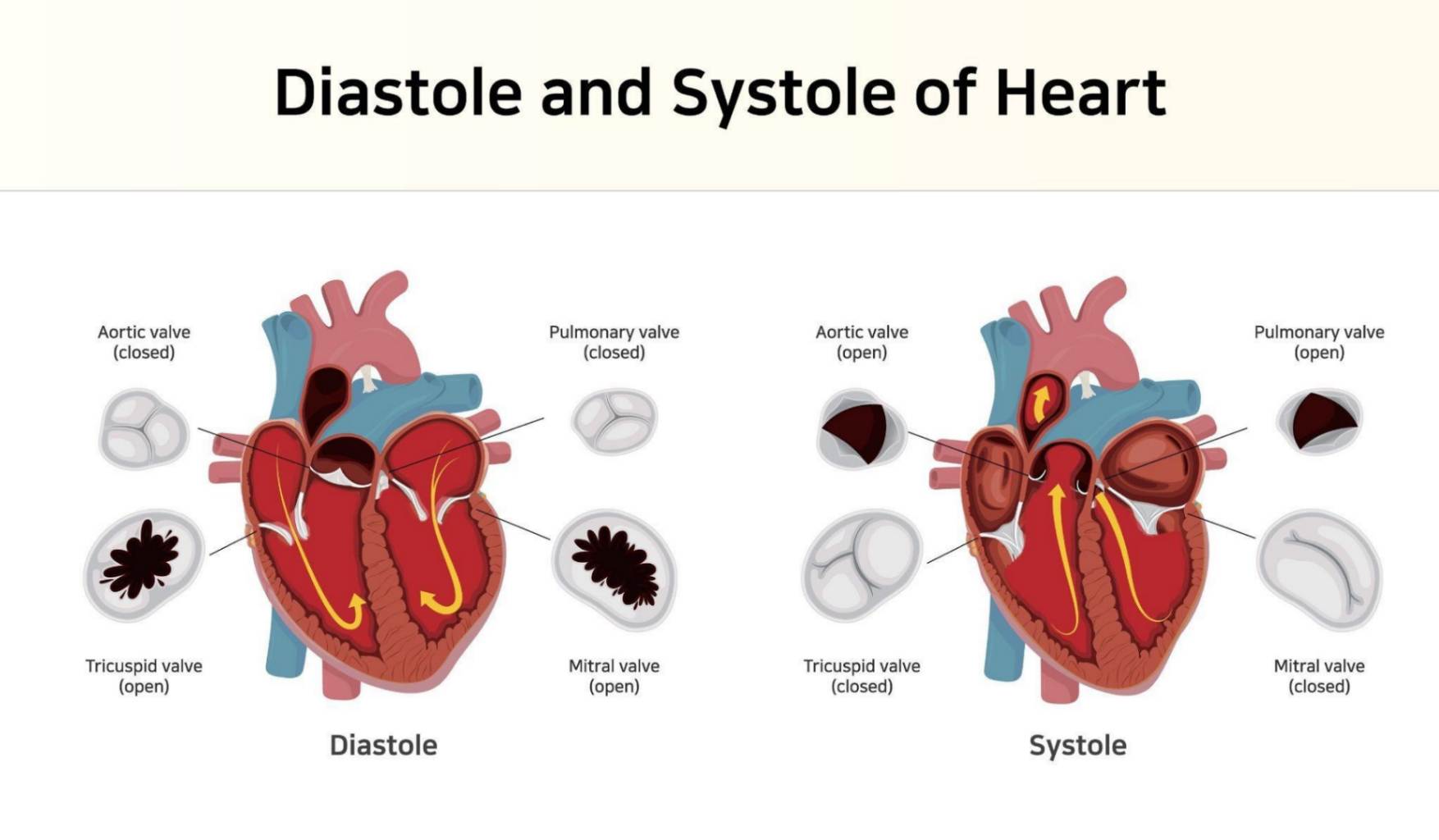
What happens during systole?
It is the contraction phase where blood is pumped out of the ventricles into the pulmonary artery and aorta, AV valves close, pressure increases, and semilunar valves open to allow blood flow.

What are the venae cavae and their functions?
The venae cavae are two large veins that return deoxygenated blood from the body back to the heart.
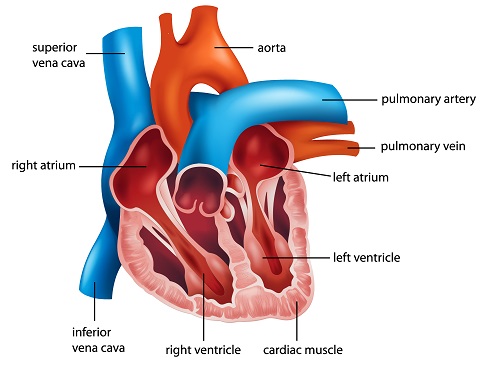
What is the function of the Superior Vena Cava (SVC)?
It carries deoxygenated blood from the upper half of the body (head, neck, arms, and upper torso) back to the right atrium of the heart

What is the function of the Inferior Vena Cava (IVC)?
It carries deoxygenated blood from the lower half of the body (abdomen, pelvis, and legs) back to the right atrium of the heart.

What components make up the electrical conduction pathway of the heart?
The pathway consists of the sinoatrial (SA) node, atrioventricular (AV) node, bundle of His, and Purkinje fibers.
Where does the electrical impulse in the heart begin, and how many signals per minute does it generate?
The impulse begins at the SA node, generating 60-100 signals per minute without neurological input.
What is the location and function of the SA node?
The SA node is located in the right atrium and initiates the depolarization wave that causes the atrias to contract.
What happens during atrial systole and what is the atrial kick?
During atrial systole, the atria contract, pushing additional blood into the ventricles. This extra push is known as the atrial kick.
Where is the AV node located and what is its function?
The AV node is located at the junction of the atria and ventricles. It delays the electrical impulse to allow the ventricles to fill completely before contracting.
What is the pathway of the electrical impulse after the AV node?
The impulse travels down the bundle of His, which branches inside the interventricular septum, and then goes to the Purkinje fibers.
What is the role of the Purkinje fibers in heart conduction?
The Purkinje fibers distribute the electrical signals throughout the ventricular muscle to ensure coordinated contraction.
How are cardiac muscle cells connected, and what is the significance of these connections?
Cardiac muscle cells are connected by intercalated discs, which contain many gap junctions. These connections allow the cytoplasm of adjacent cells to connect, facilitating coordinated ventricular contraction.

What is the role of gap junctions in cardiac muscle cells?

allow for coordinated contraction of the heart muscle.
What ensures that the ventricles contract in a coordinated manner?
The coordinated contraction of the ventricles is ensured by the electrical signals distributed by the Purkinje fibers and the connectivity provided by intercalated discs with gap junctions.
Why can the heart generate electrical impulses even if all innervation is cut?
The SA node can generate electrical impulses autonomously at a rate of 60-100 signals per minute without neurological input.
Where is the interventricular septum?
a muscular wall that divides the heart's ventricles, or lower chambers, into left and right halves
What is the primary pacemaker of the heart?
The SA (sinoatrial) node.
Why is the delay at the AV node important?
It allows the ventricles time to fill completely with blood before they contract.
What would happen if the AV node did not delay the electrical signal?
The ventricles might not fill completely, leading to less efficient blood circulation.
What would be the consequence of damaged Purkinje fibers?
Disrupted or uncoordinated ventricular contractions, leading to inefficient blood pumping.
What are gap junctions and where are they found?
Gap junctions are specialized connections in intercalated discs that allow ions and electrical impulses to pass directly between cardiac cells.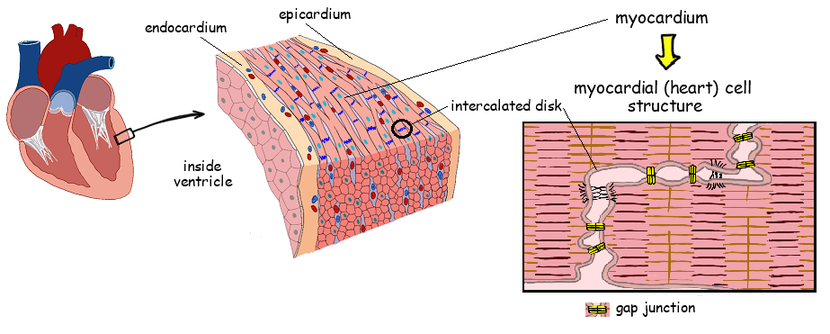
What is the sequence of electrical conduction through the heart?
SA node → Atria → AV node → Bundle of His → Right and Left Bundle Branches → Purkinje fibers → Ventricles.
What condition can result from an SA node that does not function properly?
Arrhythmias, such as bradycardia (slow heart rate) or tachycardia (fast heart rate).
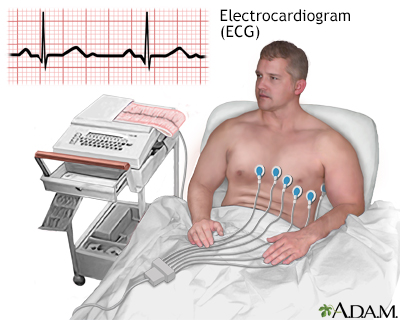
What is an Electrocardiogram (ECG/EKG)?
A test that detects the heart's electrical impulses on the body's surface using electrodes placed on the skin.
What does the P wave represent on an ECG?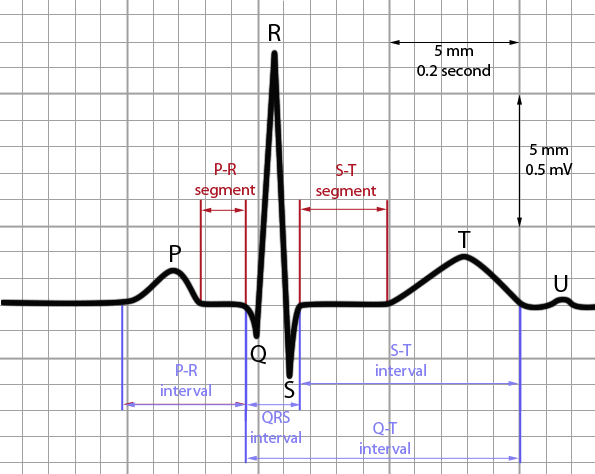
Atrial depolarization, which corresponds to the contraction of the atria.
What is indicated by the PR segment on an ECG?

The time it takes for the electrical impulse to travel from the atria to the ventricles through the AV node.
What does the QRS complex represent on an ECG?

The contraction of the ventricles.
What does the ST segment represent on an ECG?

The period at the end of ventricular contraction and the start of ventricular relaxation.
What is the significance of the T wave on an ECG?

It represents the electrical activity of the ventricles resetting (relaxing) for the next heartbeat.
What does the QT interval measure on an ECG?

The total time for the ventricles to contract and then reset.
How is the circulatory system controlled?
It is under autonomic control, regulated by the parasympathetic and sympathetic nervous systems.
What effect does the parasympathetic nervous system have on the heart?
It slows down the heart rate, often referred to as the "rest and digest" response.
Which nerve is responsible for slowing down the heart rate?
The vagus nerve.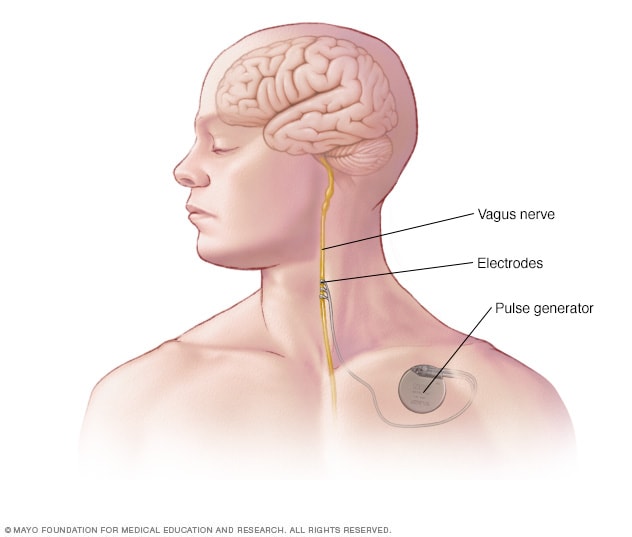
What effect does the sympathetic nervous system have on the heart?
It speeds up the heart rate and increases the contractility of the cardiac muscle, often referred to as the "fight or flight" response.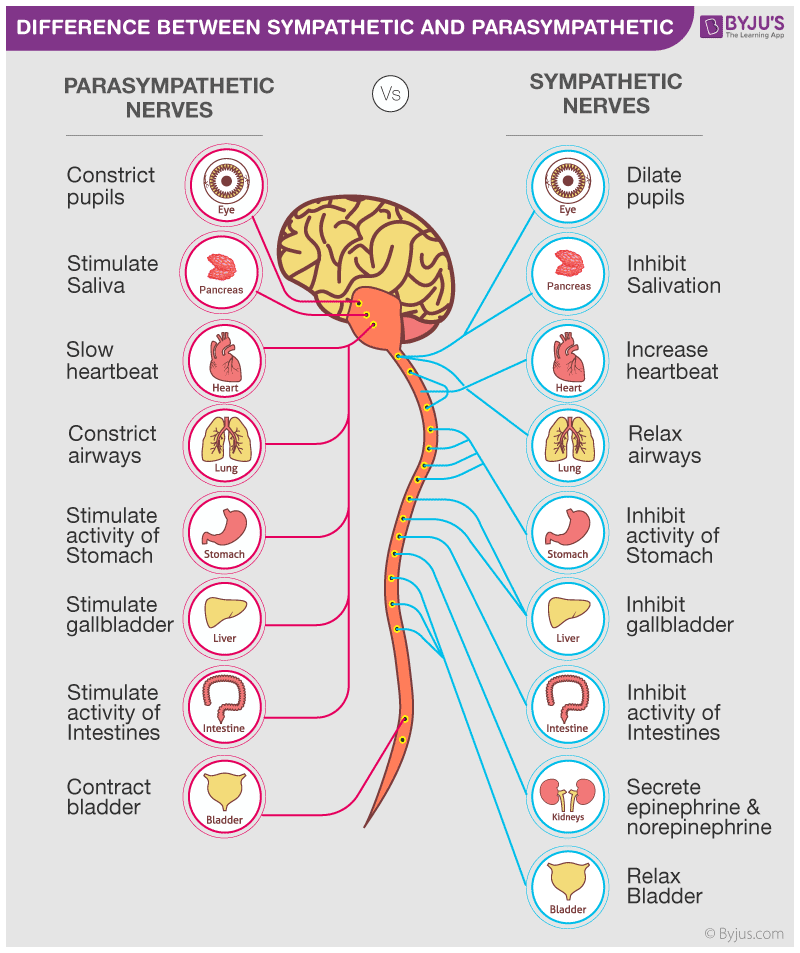
How are electrodes positioned for an ECG?
They are placed on the skin on opposite sides of the heart to detect electrical impulses.
What physiological event occurs during the PR segment?

The electrical impulse travels from the atria to the ventricles through the AV node.
During which part of the ECG does ventricular depolarization occur?
During the QRS complex.

How does the autonomic nervous system influence heart rate and cardiac output?
By using the parasympathetic system to slow the heart rate and the sympathetic system to increase heart rate and contractility.

What could cause changes in the ST segment on an ECG?
Conditions such as myocardial infarction (heart attack) or ischemia can cause changes in the ST segment.
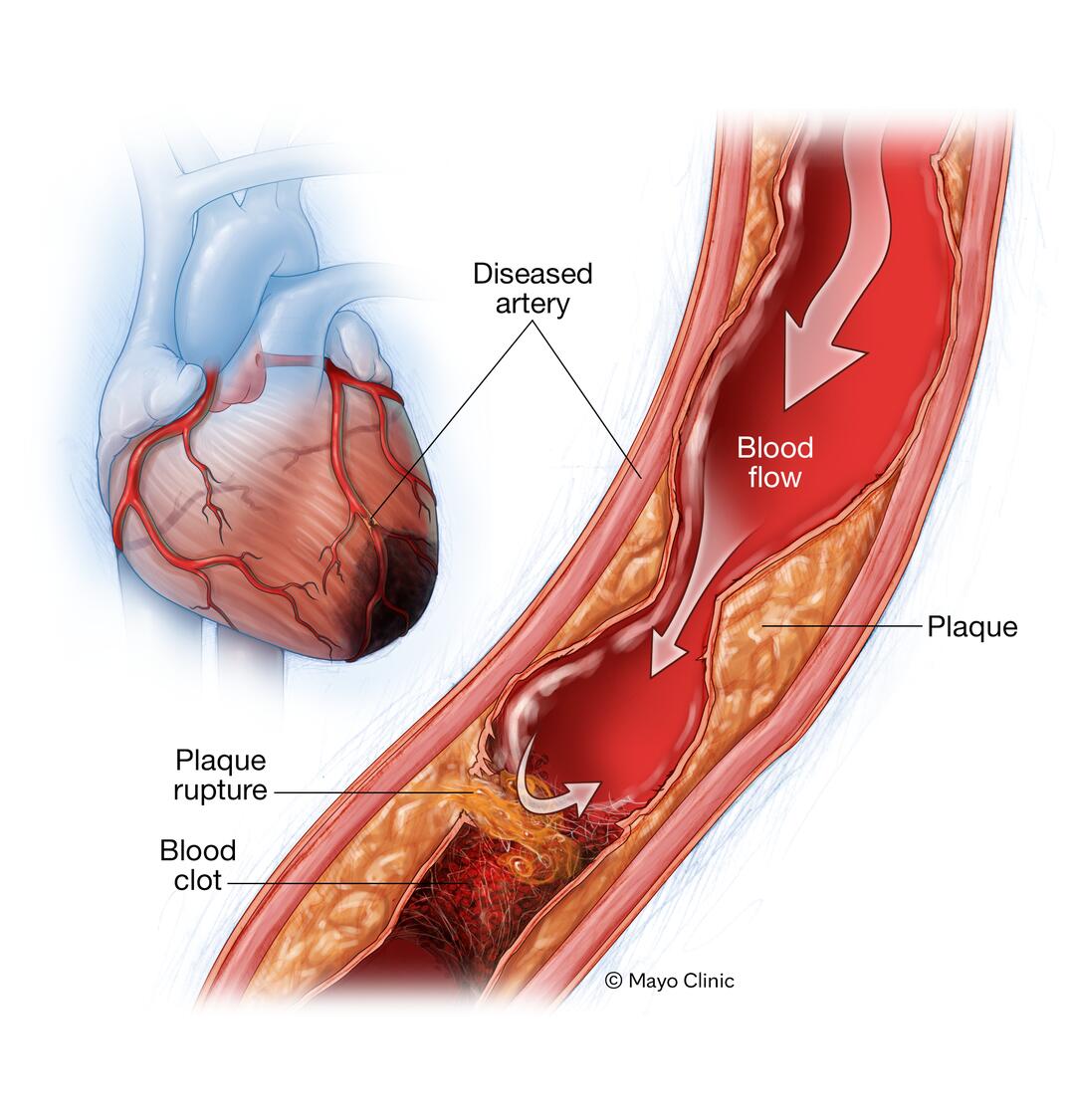
What is the role of the vagus nerve in heart function?

It regulates the slowing down of the heart rate through parasympathetic activity.
Why is the delay at the AV node reflected in the PR segment important?

It ensures that the ventricles have enough time to fill with blood before they contract, optimizing cardiac efficiency.
How does the sympathetic nervous system increase heart rate and contractility? What does it release?
By releasing adrenaline (epinephrine) and norepinephrine, which act on the heart to increase the rate and force of contractions.
Why is the QRS complex typically larger than the P wave on an ECG?

Because it represents the larger muscle mass of the ventricles contracting compared to the atria.
How can the vagus nerve be stimulated to affect heart rate?
Techniques like deep breathing, cold water immersion, or the Valsalva maneuver can stimulate the vagus nerve, slowing the heart rate.
What causes the "Lub" sound in the heart?
The closure of the AV (atrioventricular) valves at the beginning of systole to prevent backflow of blood.
What causes the "Dup" sound in the heart?
The closure of the semilunar valves at the end of systole to prevent backflow of blood.
Why is diastole longer than systole?
Because the heart spends more time relaxing and filling with blood than contracting.
Give an example of heart rate variation in different populations.
45 bpm in athletes to 80+ bpm in children and elderly.
What is stroke volume (SV)?
The amount of blood pumped by the heart with each beat.
How is cardiac output calculated?
Cardiac output (CO) = Stroke Volume (SV) * Heart Rate (HR).
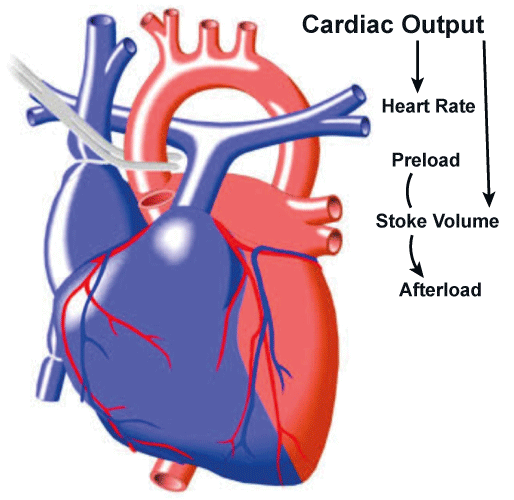
What is the Frank-Starling Mechanism?
The heart's ability to adjust its strength of contraction based on how much blood fills it.
How does increased venous return affect the heart?
It causes the heart chambers, especially the ventricles, to fill more, leading to stronger contractions and increased stroke volume.
What is venous return?
The flow of blood back to the heart from the body through the vena cava.
How do heart muscle fibers respond to increased stretch from more blood return?
They contract more forcefully, similar to a stretched rubber band snapping back.
How can the body increase venous return?
By increasing total blood volume (e.g., reducing urine output) and contracting large veins to push more blood toward the heart.
What role do venous valves play in blood circulation?
They ensure that blood moves in the right direction and does not flow backward when veins contract.
What is ventricular tachycardia (V-Tach)?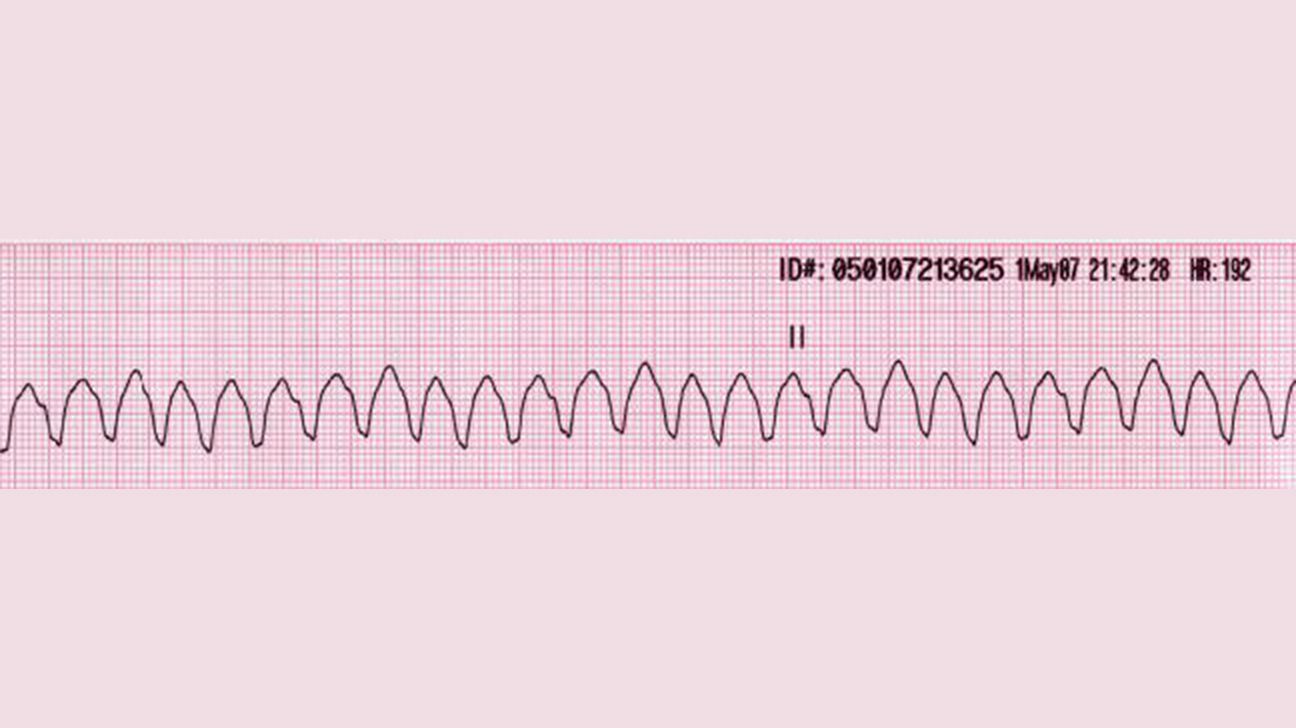
A rapid rate of ventricular contraction where the heart cannot fill properly with blood, potentially stopping blood pumping.
Why is V-Tach life-threatening if not corrected?

Because the heart may stop pumping blood despite its fast rate, leading to death if not forced out of the abnormal rhythm.
What happens during systole?
The heart contracts to pump blood out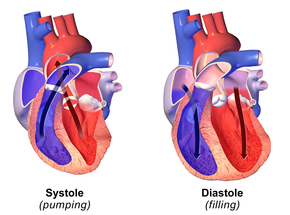
What happens during diastole?
The heart relaxes and fills with blood

What is the significance of the AV valves during the cardiac cycle?
They prevent backflow of blood into the atria during ventricular contraction (systole)

What is the significance of the semilunar valves during the cardiac cycle?
They prevent backflow of blood into the ventricles after ventricular contraction.

What might cause a reduction in stroke volume?
Conditions like V-Tach where the heart doesn't fill properly with blood or heart failure.
How does the body respond to low blood volume to increase venous return?
By reducing urine output to retain more water and increasing blood volume.
What ensures the forward movement of blood in veins?
Venous valves that prevent backflow and ensure unidirectional flow toward the heart.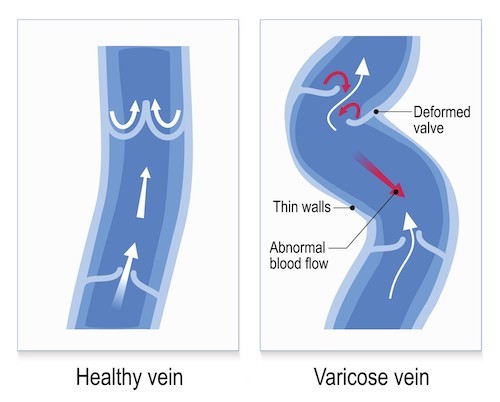
What is the function of the heart in the circulatory system?
The heart is a muscular pump that drives blood through the blood vessels.
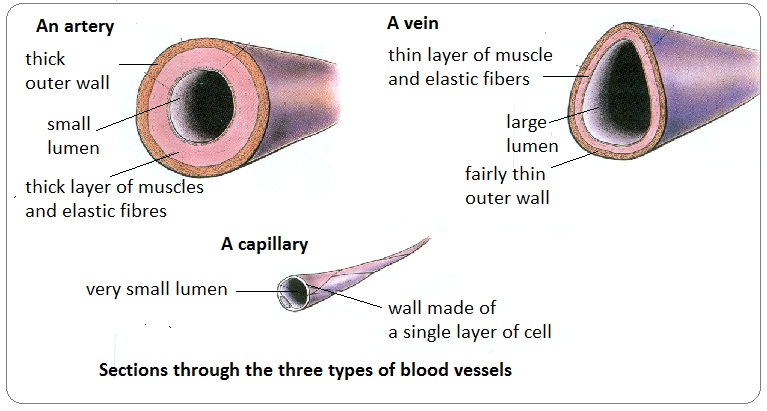
What is the function of arteries in the circulatory system?
Arteries carry blood away from the heart at high pressure.
Which artery is the largest in the body?
The aorta.
What types of arteries branch off from the aorta?
Carotid, subclavian, and renal arteries, which supply blood to peripheral tissues.

Why do arteries have thick muscular walls?
To handle the high pressure of blood pumped from the heart and to regulate blood flow into capillaries
Which arteries carry deoxygenated blood?
The pulmonary artery and umbilical arteries.
How do capillaries facilitate material exchange?
They have thin walls that allow for diffusion of gases, nutrients, and wastes between blood and tissues.

What happens to blood in the interstitial space when it leaves capillaries?
It can cause bruising if there is leakage from blood vessels.