Exam 3 Pearson
1/102
Earn XP
Description and Tags
ch. 22 & 23
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
103 Terms
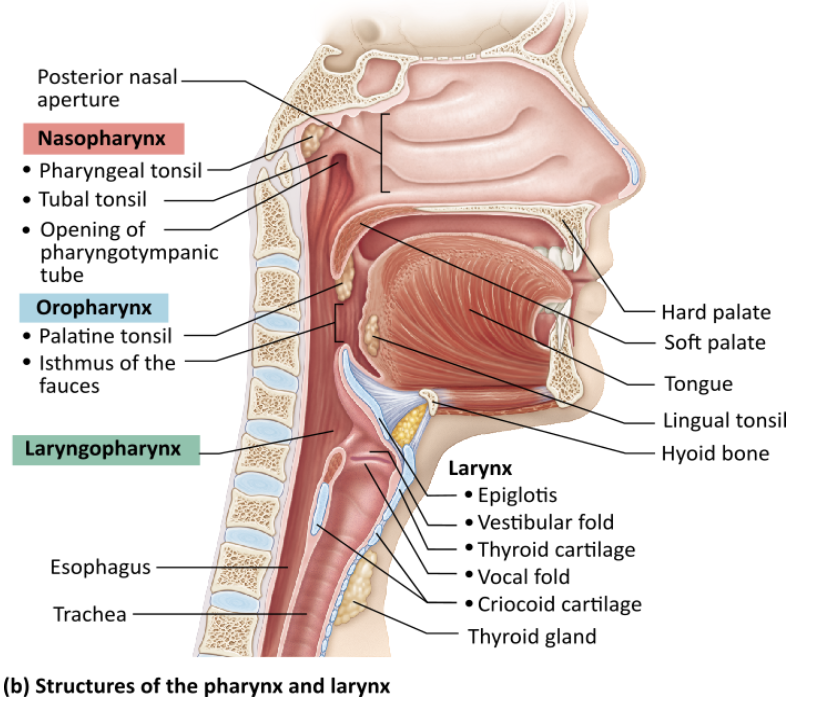
Which of the following is NOT a function of the nasal conchae?
filtering, heating, and moistening incoming air during inhalation |
increasing the mucosal surface area exposed to air |
reclaiming heat and moisture from expired air |
routing air and food into proper channels |
routing air and food into proper channels
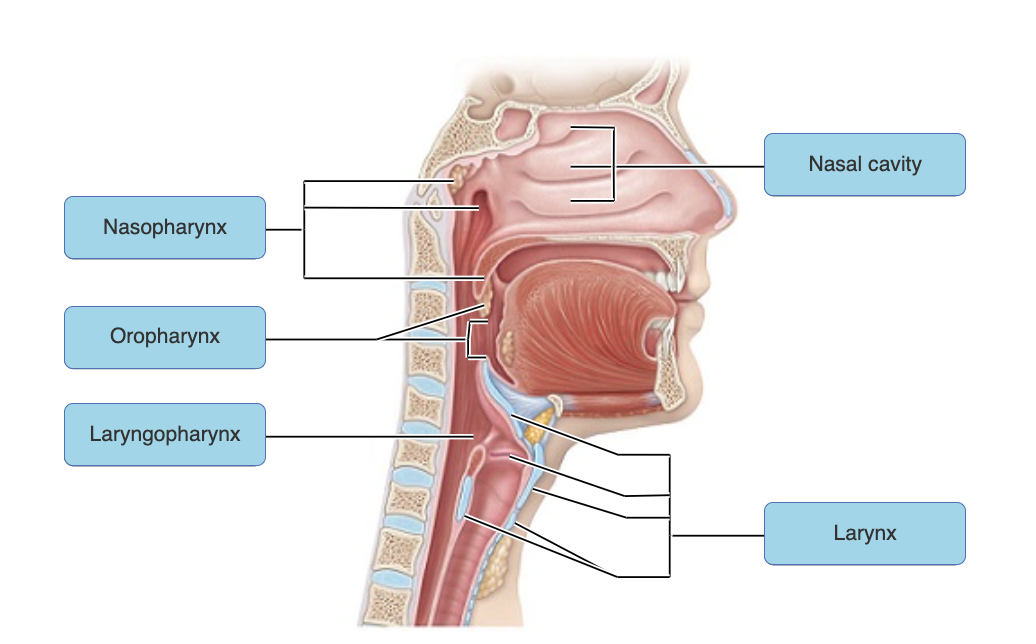
just know
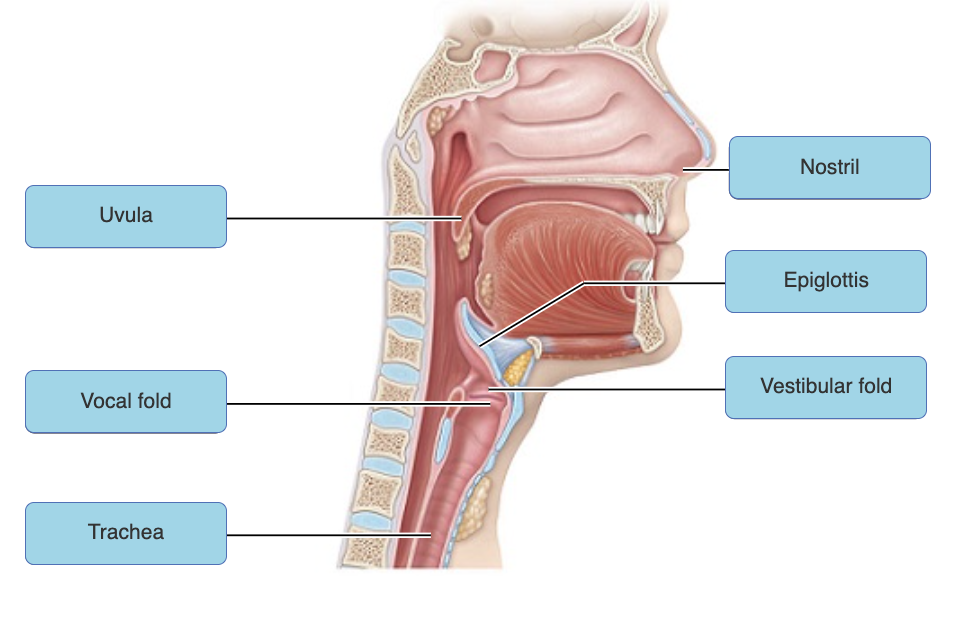
just know
Which of these structures is/are NOT properly matched with one of its/their functions?
pharyngeal tonsil: trap and destroy pathogens entering the nasopharynx in air |
nasal conchae: increase the mucosal surface area exposed to air |
nasopharynx: conduct air toward and from the larynx |
paranasal sinuses: house olfactory receptors |
paranasal sinuses: house olfactory receptors
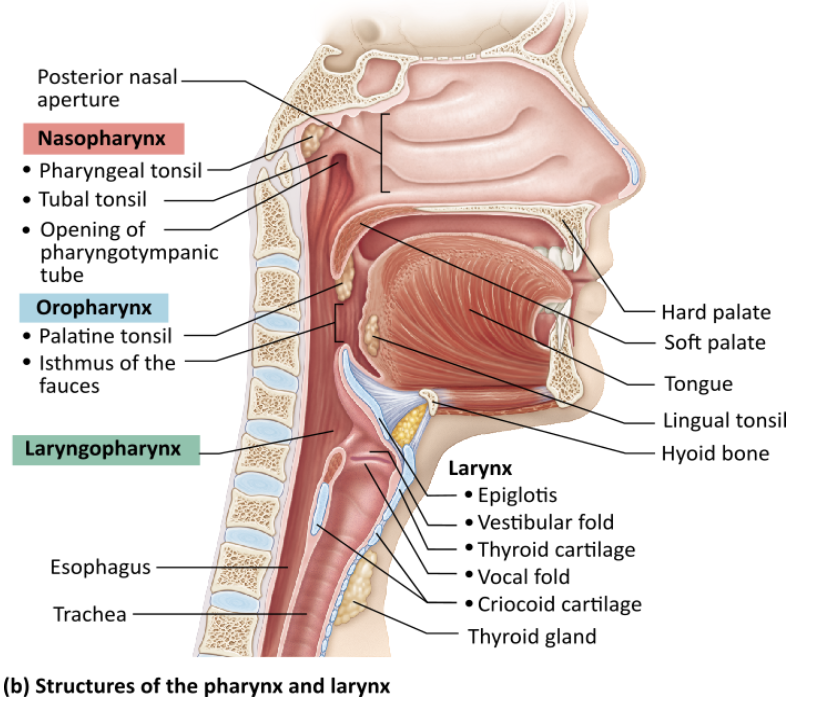
Which of the following regions contains the opening of a canal that equalizes pressure in the middle ear?
laryngopharynx |
nasopharynx |
larynx |
oropharynx |
nasopharynx |
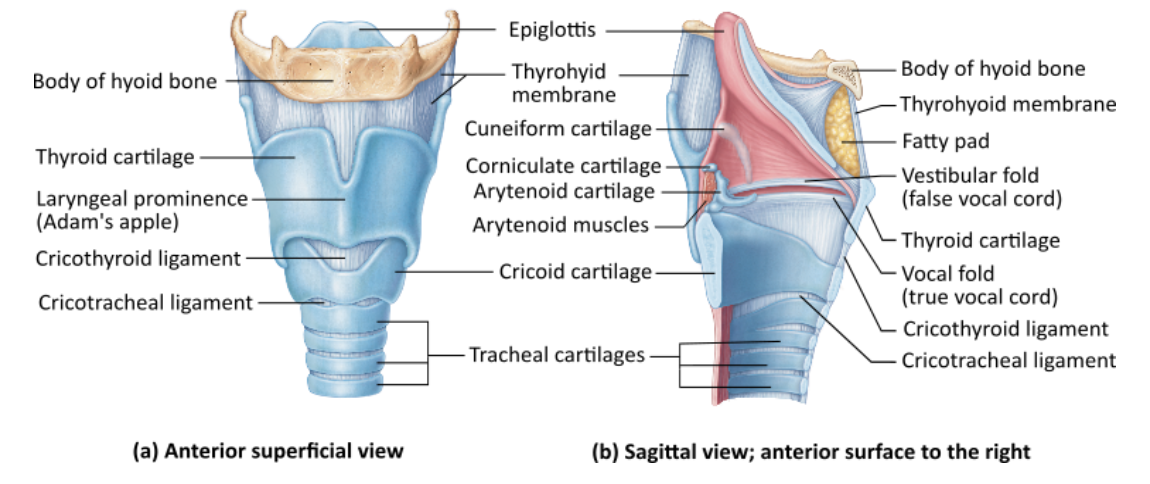
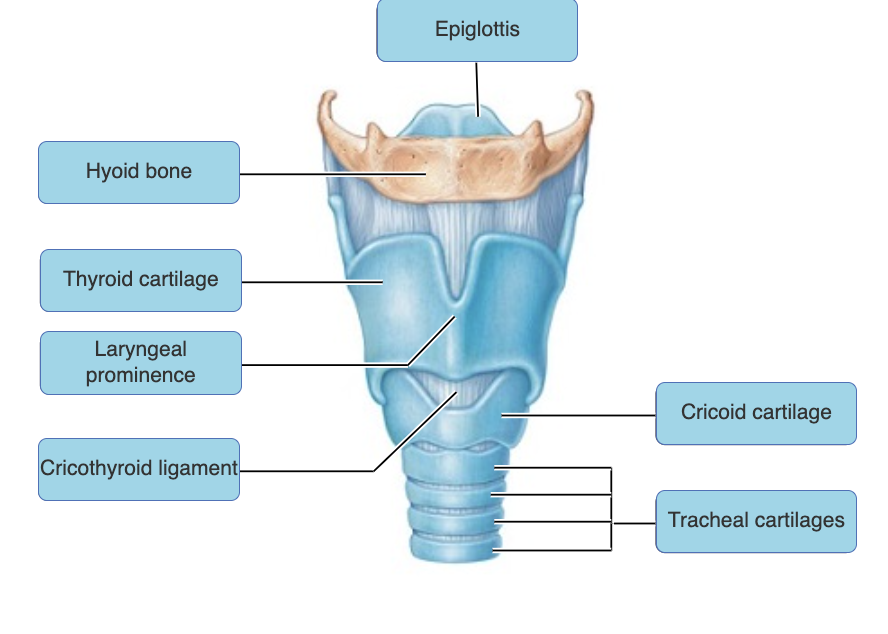
What part of the larynx covers the laryngeal inlet during swallowing to keep food out of the lower respiratory passages?
vocal folds |
thyroid cartilage |
epiglottis |
glottis |
glottis |
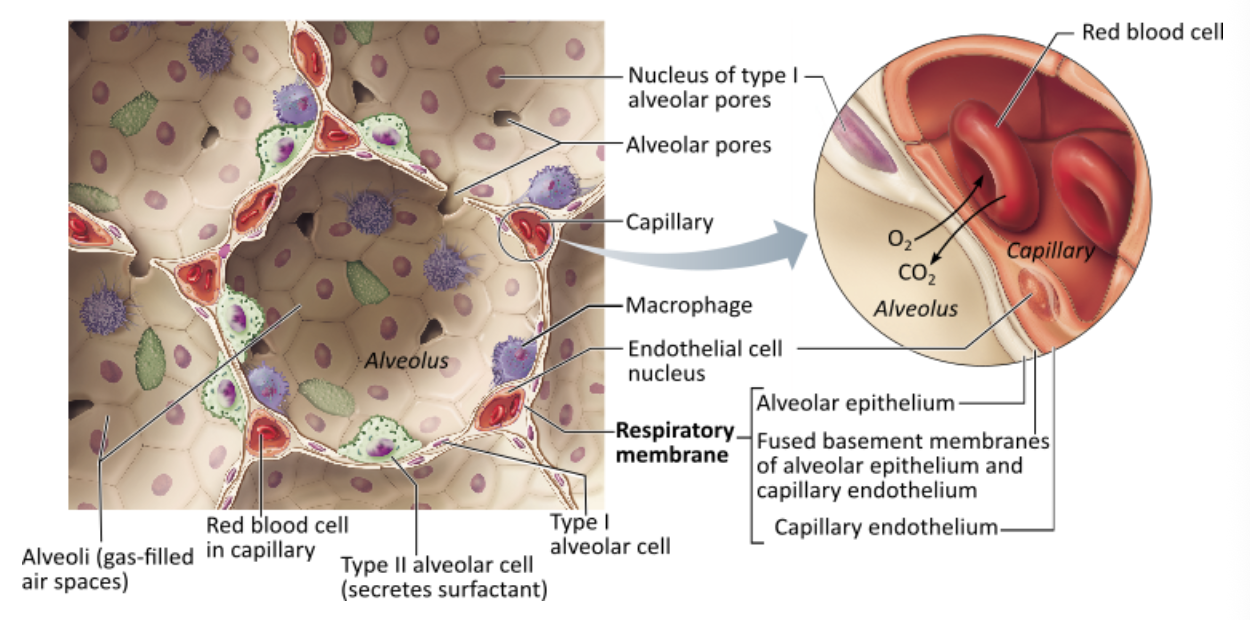
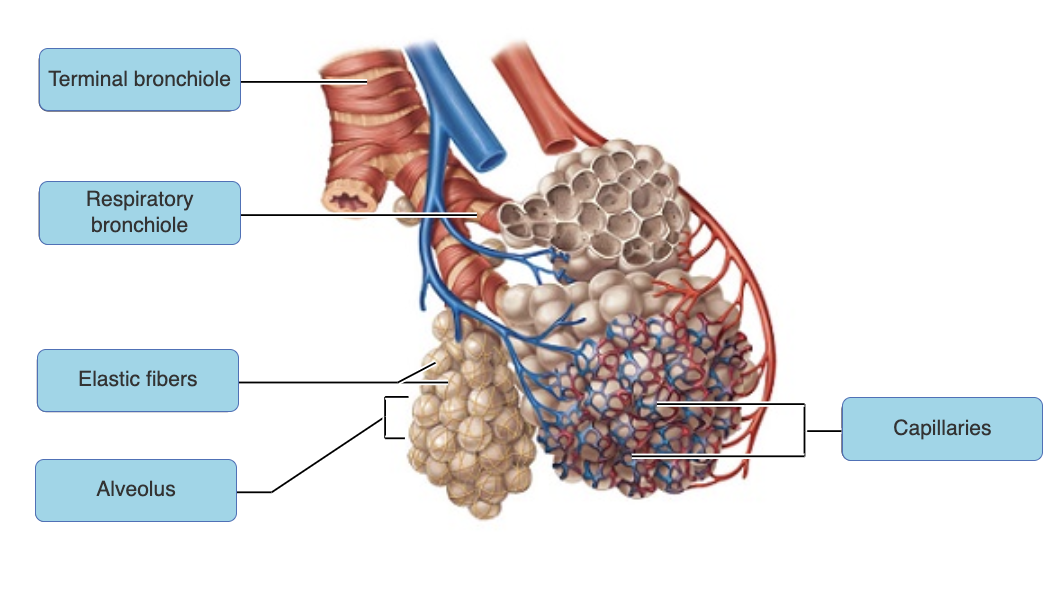
Which of these cells would be most effective in the disposal of inspired microorganisms that may enter the alveoli?
type II alveolar cells |
lymphocytes in blood circulating through the lungs |
alveolar macrophages |
type I alveolar cells |
alveolar macrophages
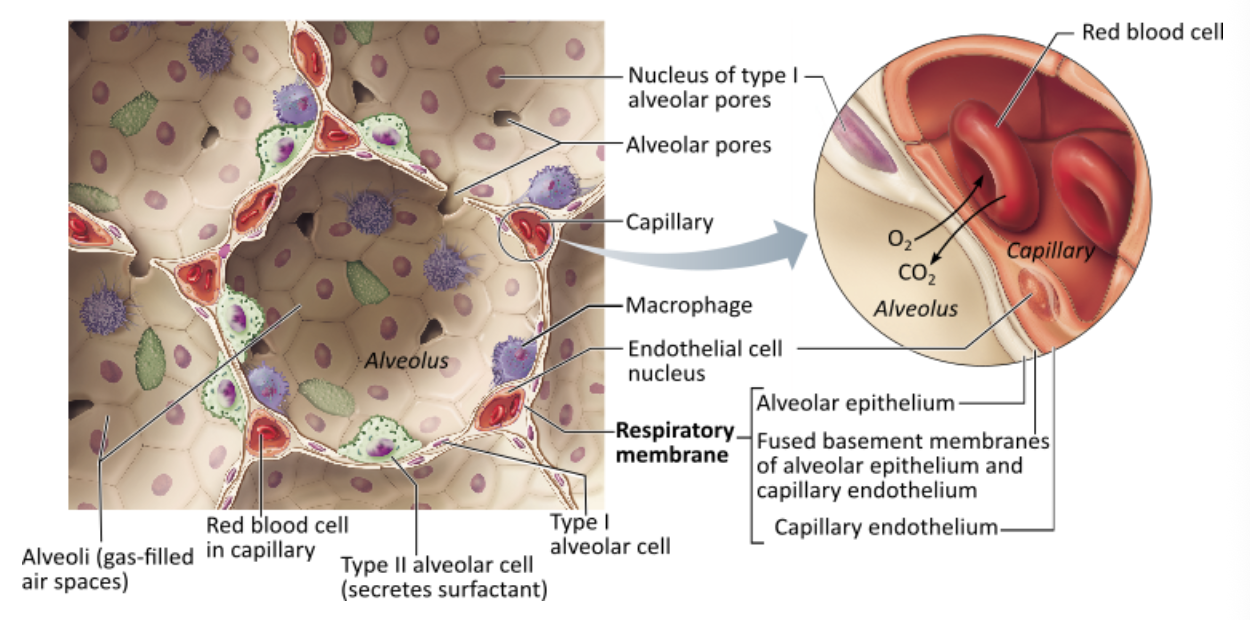
What type of epithelial tissue forms the walls of the alveoli?
simple squamous epithelium |
pseudostratified ciliated columnar epithelium |
stratified squamous epithelium |
simple cuboidal epithelium |
simple squamous epithelium |
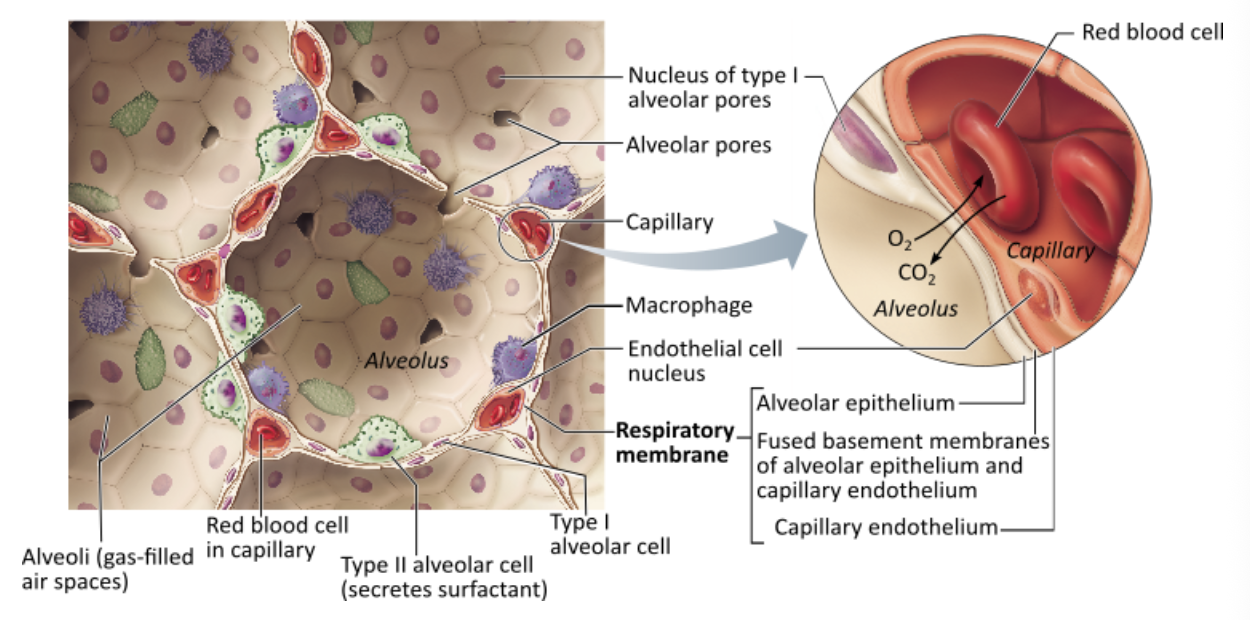
In children with infant respiratory distress syndrome (IRDS), the walls of the alveoli cling to each other and make them difficult to inflate. It is common in babies born prematurely. What cells in these infants are NOT fully developed and are NOT doing their job?
type II alveolar cells |
alveolar macrophages |
type I alveolar cells |
endothelial cells of alveolar capillaries |
type II alveolar cells |
just know
just know
just know
What structure prevents food and liquids from entering the trachea?
vestibular folds |
glottis |
epiglottis |
laryngeal prominence |
epiglottis |
Which of the following maintains the patency (openness) of the trachea?
surfactant production |
C-shaped cartilage rings |
surface tension of water |
pseudostratified ciliated epithelium |
C-shaped cartilage rings
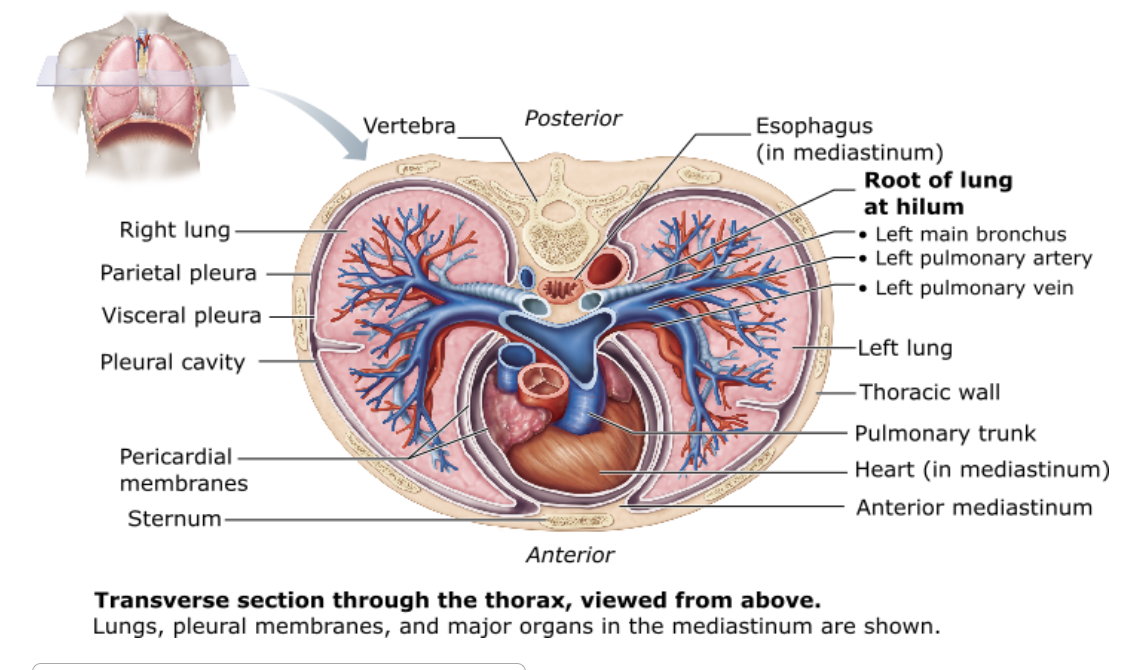
Which of the following cavities surround(s) the lungs alone?
mediastinum |
pericardial cavity |
pleural cavities |
thoracic cavity |
pleural cavities |
The lungs are perfused by two circulations: the pulmonary and the bronchial. The pulmonary circulation is for oxygenation of blood. The bronchial circulation supplies blood to the lung structures (tissue).
True |
False |
True |
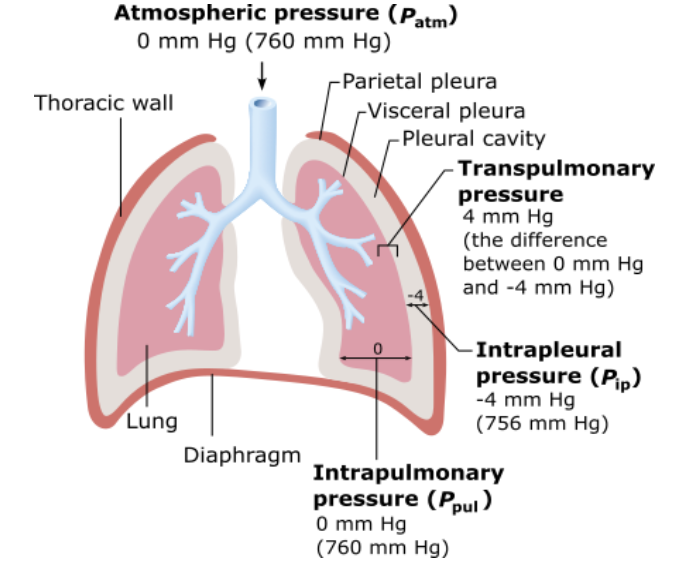
Which of the following pressures rises and falls with the phases of breathing but eventually equalizes with the pressure of the air in the environment?
intrapleural pressure |
atmospheric pressure |
intrapulmonary pressure |
transpulmonary pressure |
intrapulmonary pressure
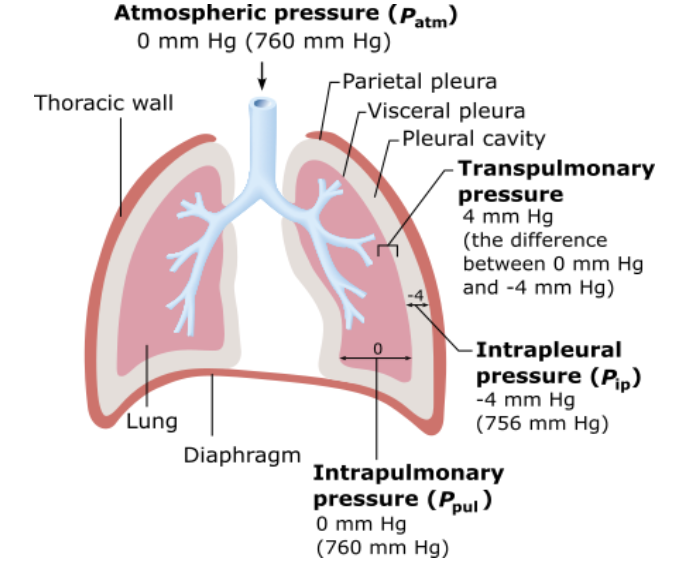
Which of the following pressures must remain negative to prevent lung collapse?
intrapleural pressure |
transpulmonary pressure |
intrapulmonary pressure |
atmospheric pressure |
intrapleural pressure |
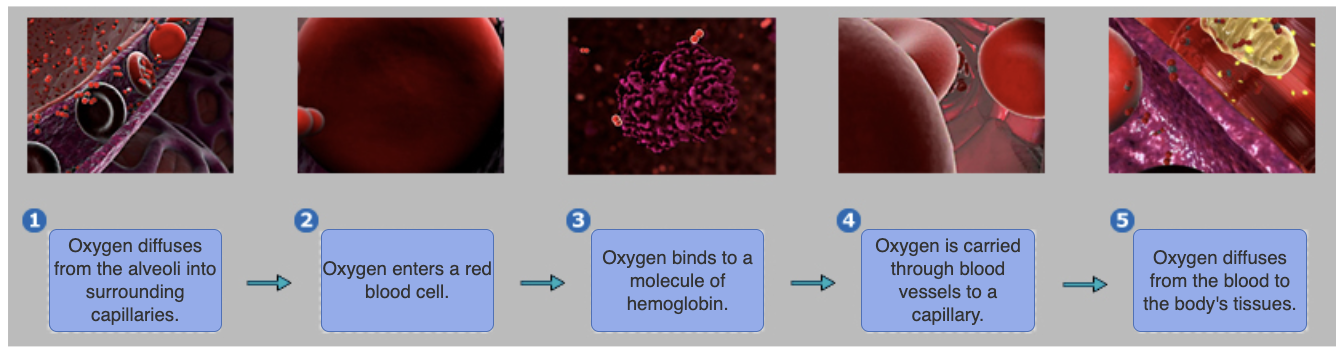
just know
Quiet inspiration is __________, and quiet expiration is __________.
an active process; a passive process |
an active process; also an active process |
a passive process; an active process |
a passive process; also a passive process |
an active process; a passive process |
Air moves out of the lungs when the pressure inside the lungs is ________.
greater than the intra-alveolar pressure |
less than the pressure in the atmosphere |
greater than the pressure in the atmosphere |
equal to the pressure in the atmosphere |
greater than the pressure in the atmosphere |
Surfactant helps to prevent the alveoli from collapsing by ________.
interfering with the cohesiveness of water molecules, thereby reducing the surface tension of alveolar fluid |
warming the air before it enters |
protecting the surface of alveoli from dehydration and other environmental variations |
humidifying the air before it enters |
interfering with the cohesiveness of water molecules, thereby reducing the surface tension of alveolar fluid |
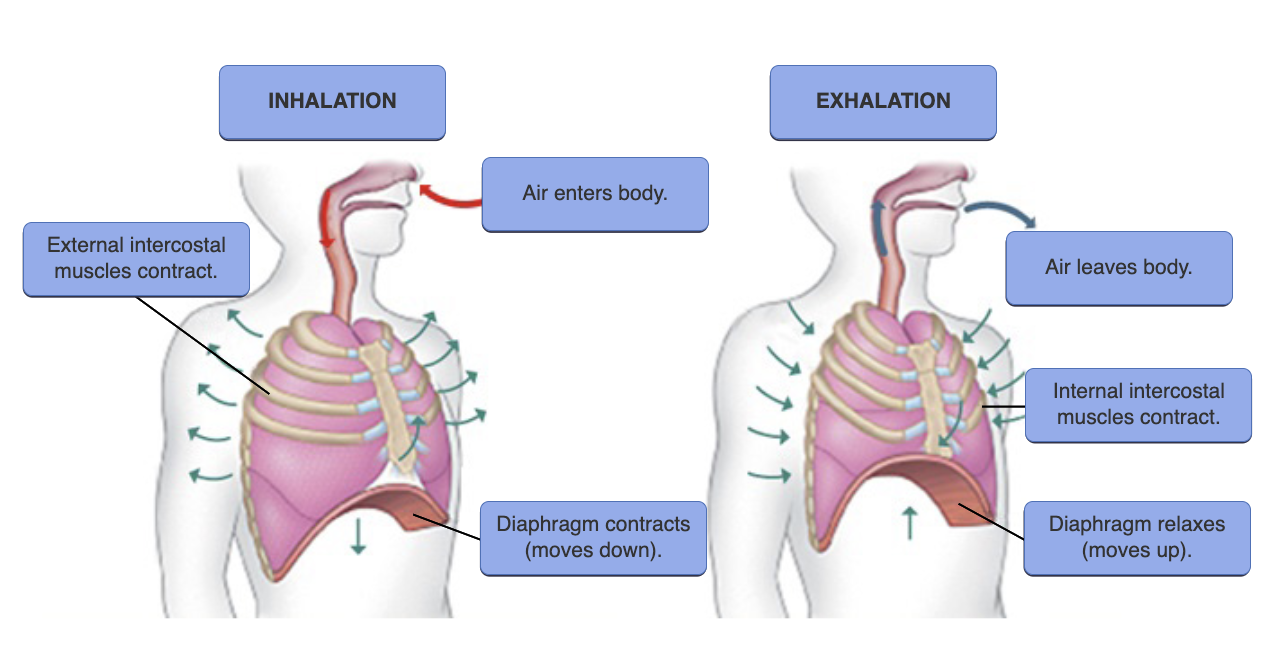
For inspiration of air, which of the following happens first?
diaphragm descends, thoracic volume begins to increase, and rib cage rises |
air (gases) flows into lungs |
thoracic cavity volume decreases |
intrapulmonary pressure drops |
diaphragm descends, thoracic volume begins to increase, and rib cage rises |
Which of the following descriptions accurately describes Boyle’s law?
The pressure of gas in your lungs is inversely proportional to the volume in your lungs. |
The partial pressure of a gas in the air you breathe in is equal to the total atmospheric pressure times the fractional concentration of the gas. |
How well a gas dissolves in a liquid such as blood depends on both its partial pressure and its solubility. |
The pressure of gas in your lungs is inversely proportional to the volume in your lungs.
Which muscles, when contracted, would increase the volume of air in the thoracic cavity?
diaphragm and external intercostals |
internal intercostals and external oblique |
diaphragm and internal intercostals |
diaphragm and external intercostals |
Which pressure is the result of the natural tendency of the lungs to decrease their size (because of elasticity) and the opposing tendency of the thoracic wall to pull outward and enlarge the lungs?
intrapulmonary pressure |
intrapleural pressure |
atmospheric pressure |
intrapleural pressure
During an allergic reaction, which of the following would aid respiration?
an increase in the parasympathetic nervous system |
acetylcholine (ACh) |
epinephrine |
histamine |
epinephrine |
If the transpulmonary pressure equals zero, what will happen to the lung?
lungs will collapse |
lung volume will stay the same |
lungs will inflate |
lungs will collapse |
The local matching of blood flow with ventilation is ________.
the Haldane effect |
chloride shifting |
ventilation-perfusion coupling |
the Bohr effect |
ventilation-perfusion coupling |
Which of the choices below determines the direction of respiratory gas movement?
the temperature |
molecular weight and size of the gas molecule |
solubility in water |
partial pressure gradient |
partial pressure gradient |
Ventilation perfusion coupling means that more blood flows past functional alveoli than past nonfunctional alveoli.
True |
False |
True
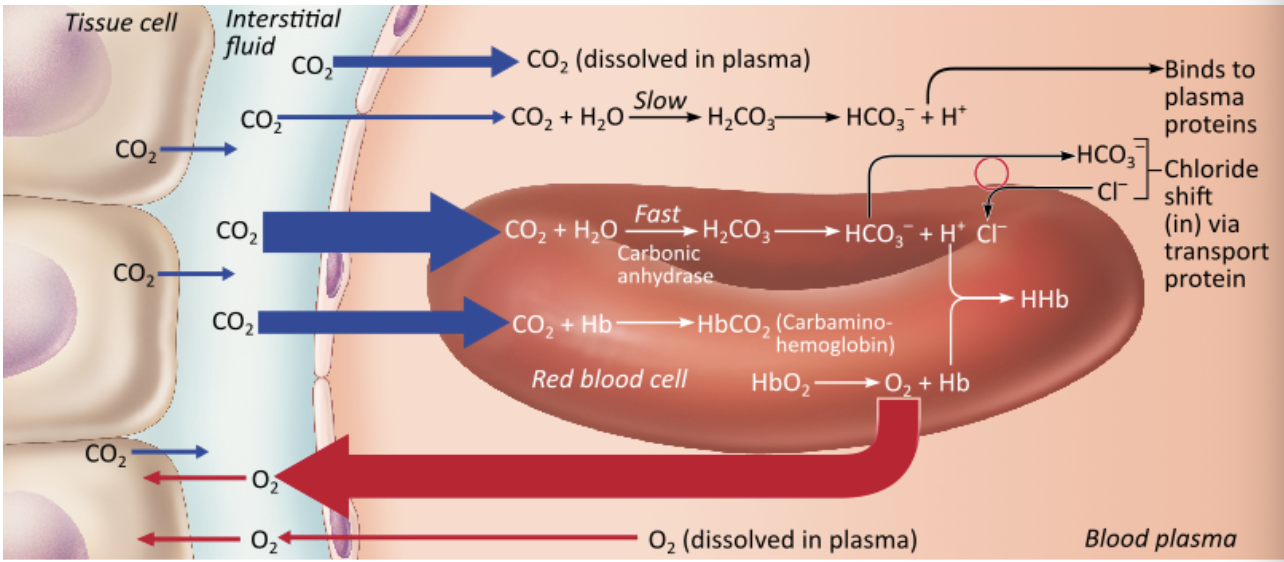
Which of the following would induce the loss of oxygen from the hemoglobin and the blood?
increase in hemoglobin that has oxygen bound to it already |
a decrease in blood temperature |
decreases in plasma carbon dioxide |
a drop in blood pH |
a drop in blood pH
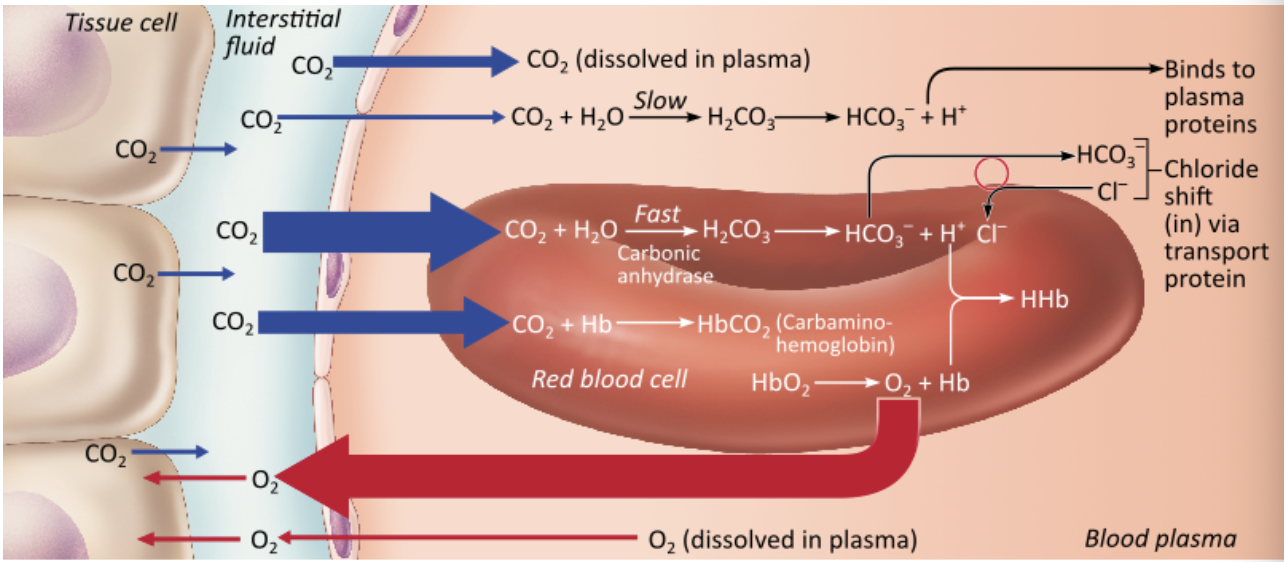
What is the most common method of carbon dioxide transport?
as bicarbonate ions in the plasma |
dissolved in the plasma |
chemically bound to hemoglobin as oxyhemoglobin |
chemically bound to hemoglobin as carbaminohemoglobin |
as bicarbonate ions in the plasma |
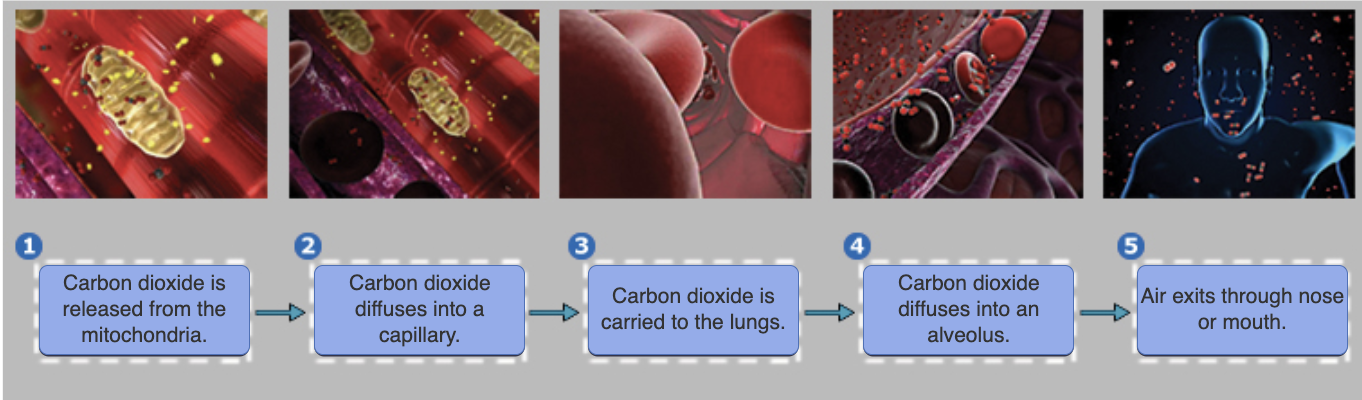
just know
If your core temperature becomes colder, it is more difficult for oxygen to dissociate from hemoglobin at any P02 .
True |
False |
True
In the plasma, the quantity of oxygen in solution is ________.
only about 1.5% of the oxygen carried in blood |
greater than the oxygen combined with hemoglobin |
about equal to the oxygen combined with hemoglobin |
not present except where it is combined with carrier molecules |
only about 1.5% of the oxygen carried in blood |
According to the oxygen-hemoglobin dissociation curve, PO2 in the lungs of 100 mm Hg results in Hb being 98% saturated. At high altitude, there is less O2. At a PO2 in the lungs of 80 mm Hg, Hb would be ________ saturated.
98% |
95% |
100% |
less than 50% |
95%
Increased temperature results in decreased O2 unloading from hemoglobin.
True |
False |
False |
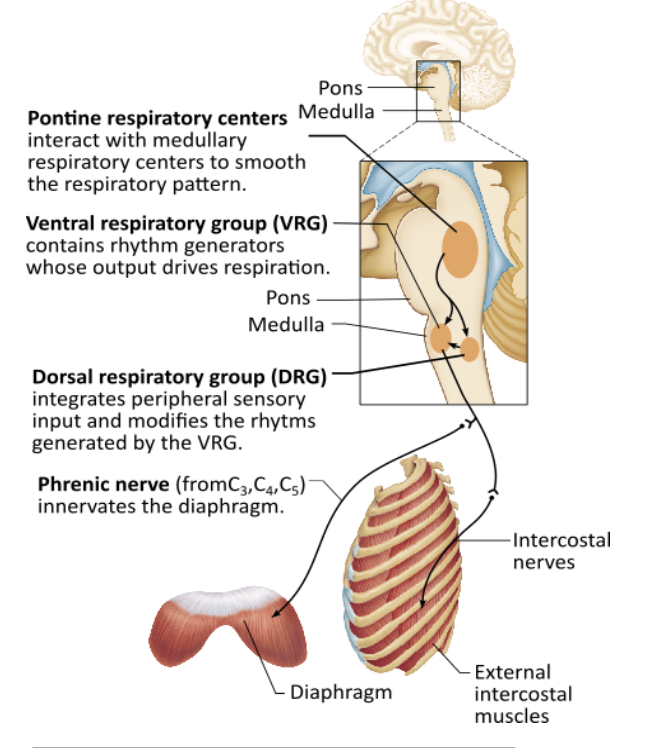
Which of the following modifies and smoothes the respiratory pattern?
dorsal respiratory group (DRG) |
pontine respiratory centers |
ventral respiratory group (VRG) |
diencephalon |
pontine respiratory centers |
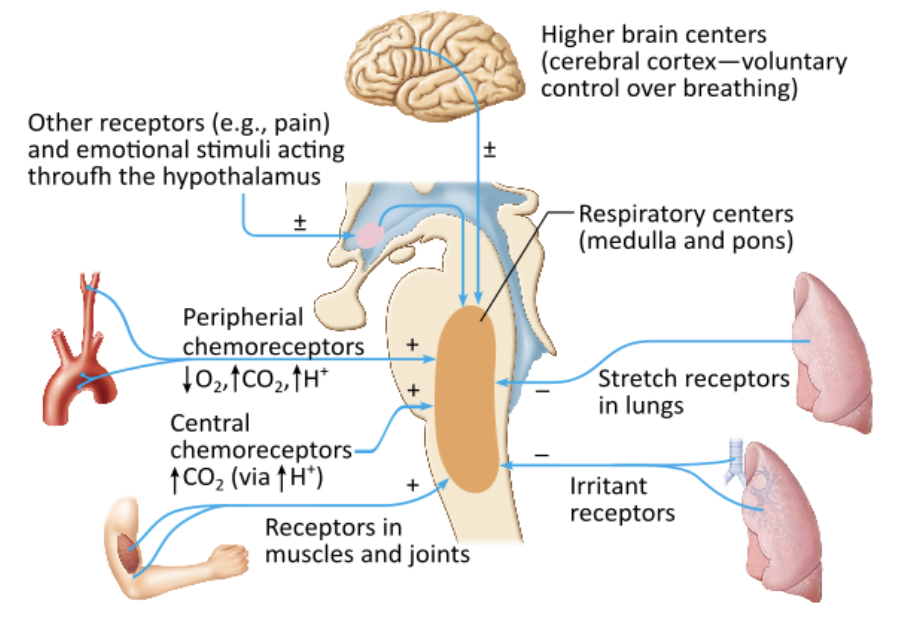
Which of the following stimuli is the most powerful respiratory stimulant to increase respiration?
an increase in blood pH |
rising carbon dioxide levels |
reduced oxygen levels |
arterial pH |
rising carbon dioxide levels
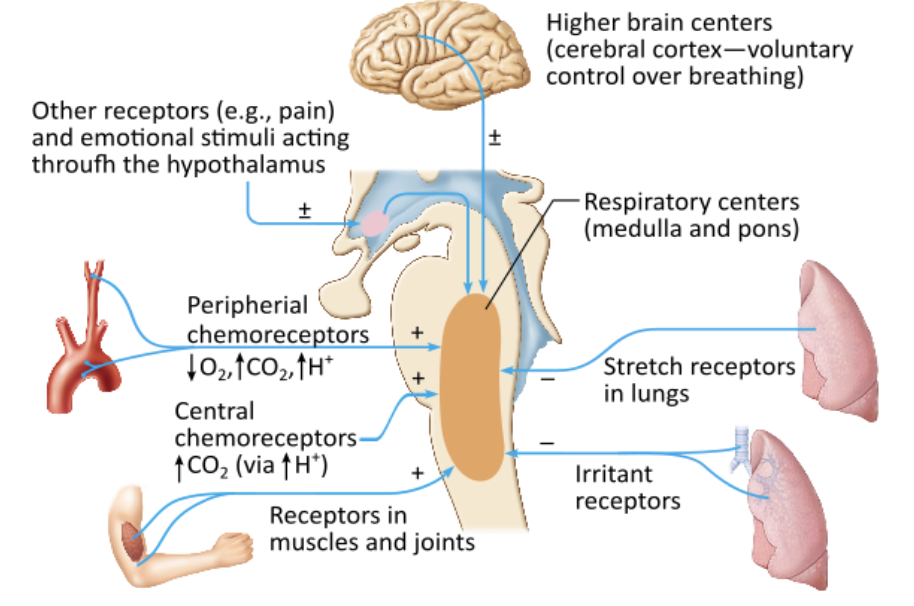
Which of the following inhibits/reduces the respiratory rate?
stimulation of stretch receptors in the lungs |
a rise in body temperature |
elevated carbon dioxide levels in the blood |
partial pressure of oxygen below 60 millimeters of mercury at chemoreceptors |
stimulation of stretch receptors in the lungs |
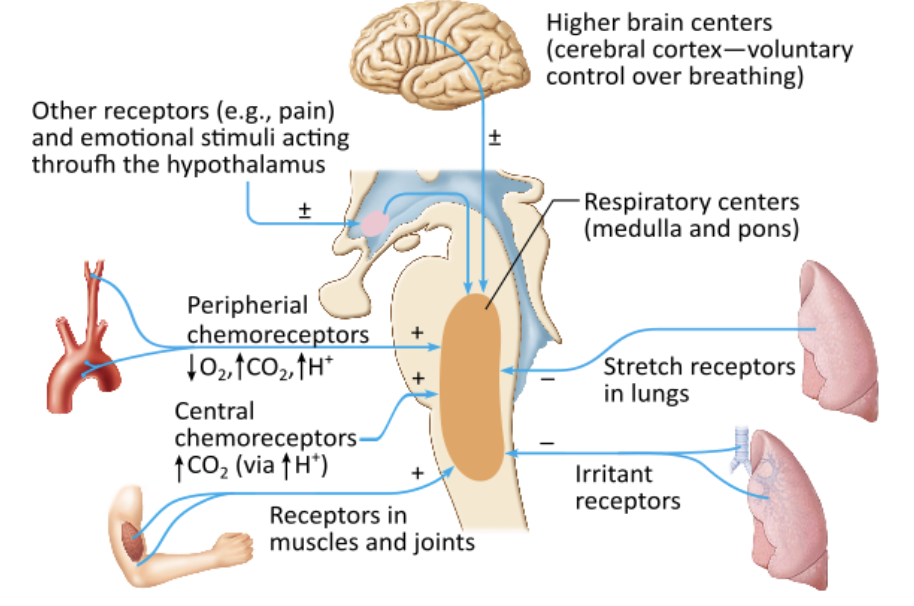
Which of the following conditions or scenarios increases the respiratory rate?
a drop in carbon dioxide levels in the blood |
acidosis |
alkalosis |
an increase in partial pressure of oxygen |
acidosis |
Respiratory control centers are located in the ________.
upper spinal cord and medulla |
pons and midbrain |
medulla and pons |
midbrain and medulla |
medulla and pons |
What area in the brain sets the respiratory rhythm?
hypothalamus |
dorsal respiratory group (DRG) |
ventral respiratory group (VRG) |
pontine respiratory group (PRG) |
ventral respiratory group (VRG) |
Inspiratory neurons send information to the diaphragm via what nerve?
phrenic nerve |
intercostal nerves |
glossopharyngeal nerve |
vagus nerve |
phrenic nerve |
What directly stimulates the central chemoreceptors, thus increasing respiration?
low O2 (oxygen) |
high pH |
H+ (hydrogen ions) |
high CO2 (carbon dioxide) |
H+ (hydrogen ions) |
As a result of hyperventilation, what will happen to the partial pressures of CO2 (pCO2) and pH?
decreased pCO2 and decreased pH |
increased pCO2 and decreased pH |
decreased pCO2 and increased pH |
increased pCO2 and increased pH |
decreased pCO2 and increased pH |
Which receptors inhibit inspiration during hyperinflation of the lungs?
pulmonary stretch receptors |
Hypothalamic receptors |
irritant receptors |
peripheral chemoreceptors |
pulmonary stretch receptors |
What stimulates increased respiration at the beginning of exercise?
increased plasma carbon dioxide levels |
increased hydrogen ion levels |
sensory input from receptors in joints, neural input from the motor cortex, and other factors |
decreased plasma oxygen levels |
sensory input from receptors in joints, neural input from the motor cortex, and other factors |
A homeostatic control mechanism controls respiration. What acts as the effector(s) in this system?
respiratory muscles |
peripheral chemoreceptors |
medulla oblongata |
central chemoreceptors |
respiratory muscles |
Which of the disorders below is characterized by destruction of the walls of the alveoli producing abnormally large air spaces that remain filled with air during exhalation?
emphysema |
coryza |
tuberculosis |
pneumonia |
emphysema
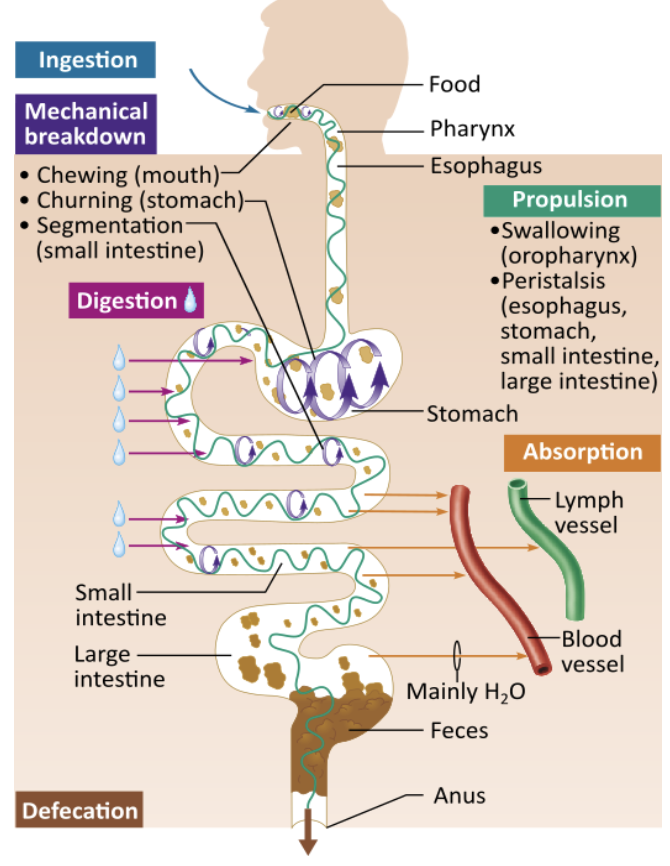
How would you classify chewing food?
mechanical breakdown |
propulsion |
digestion |
ingestion |
mechanical breakdown
Which of the following is NOT a means of mechanically breaking down food?
churning |
mastication |
segmentation |
peristalsis |
peristalsis |
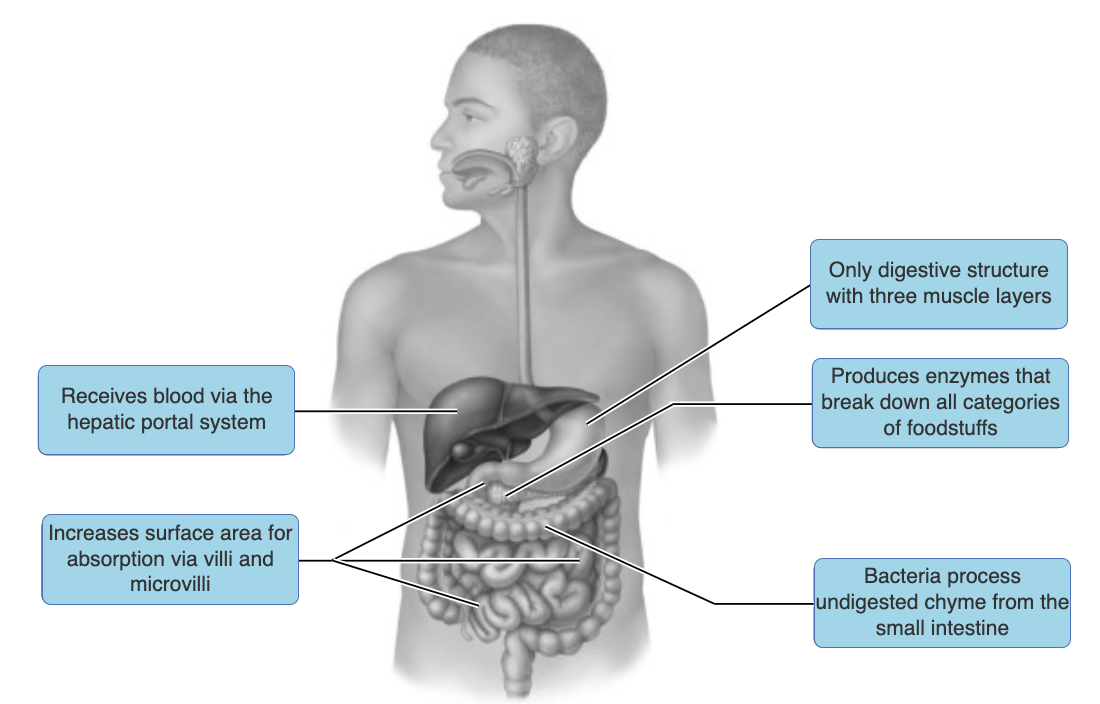
just know
When we ingest large molecules such as lipids, carbohydrates, and proteins, they must undergo catabolic reactions whereby enzymes split these molecules. This series of reactions is called ________.
secretion |
absorption |
mechanical breakdown |
digestion |
digestion
Digestion reduces large complex molecules to simpler compounds by the process of ________.
catabolism |
excretion |
mastication |
anabolism |
catabolism |
Peristaltic waves are ________.
churning movements of the gastrointestinal tract that aid in mechanical breakdown of chyme |
pendular movements of the gastrointestinal tract |
waves of muscular contractions that propel contents from one point to another |
segmental regions of the gastrointestinal tract |
waves of muscular contractions that propel contents from one point to another |
Which organ of the digestive tract is the body's major digestive organ?
stomach |
large intestine |
liver |
small intestine |
small intestine |
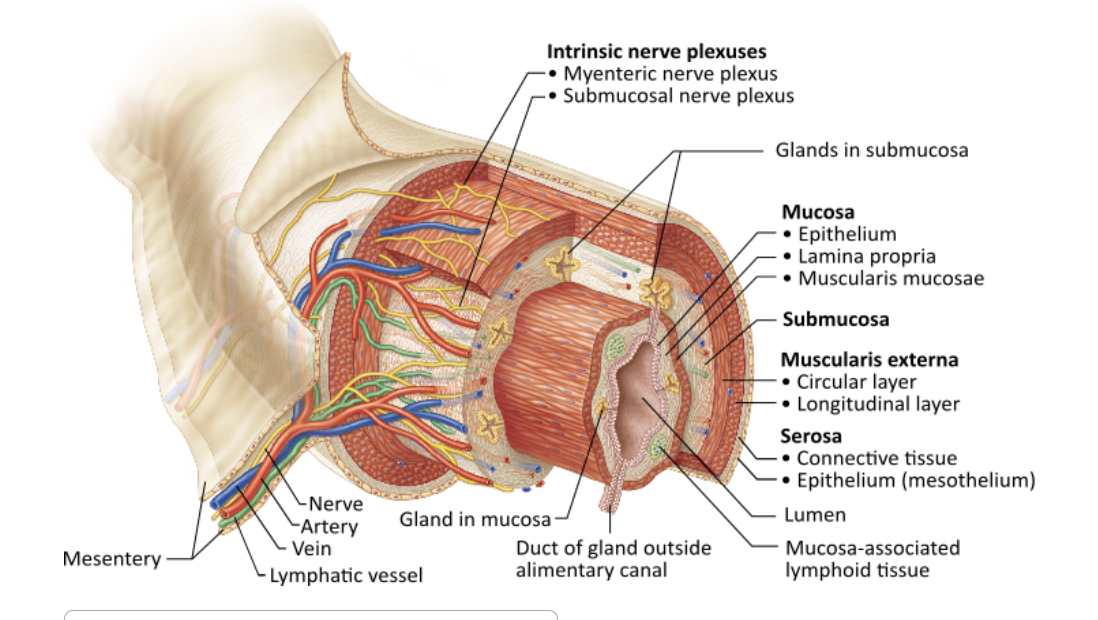
Which layer of the alimentary canal is constructed from either stratified squamous or simple columnar epithelium?
submucosa |
muscularis externa |
mucosa |
serosa |
mucosa
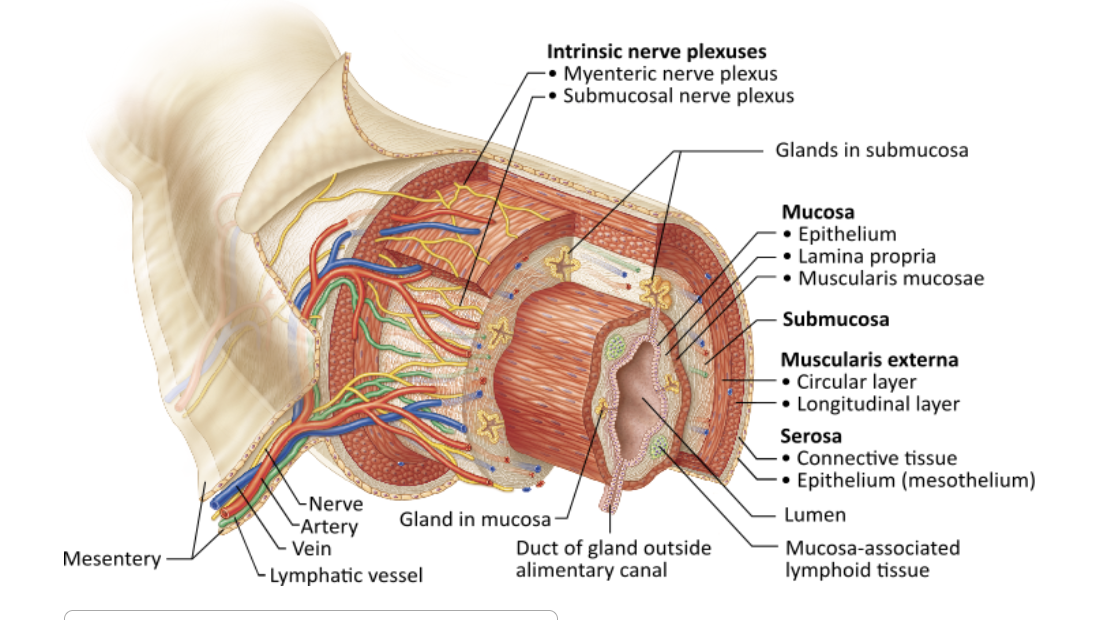
Which layer of the alimentary canal is responsible for segmentation and peristalsis?
mucosa |
muscularis externa |
serosa |
submucosa |
muscularis externa |
The __________ is the serous membrane that covers most digestive organs.
omenta |
parietal peritoneum |
mesentery |
visceral peritoneum |
visceral peritoneum |
The __________ circulation collects nutrient-rich venous blood draining from the digestive viscera.
pulmonary |
hepatic portal |
enterohepatic |
splanchnic |
hepatic portal |
Which of the following does NOT correctly describe basic regulation of digestive activity?
Short reflexes act locally in the GI tract. |
The enteric nervous system is under conscious control. |
pH, stretch, and osmolarity are some of the stimuli that can trigger digestive reflexes. |
Digestive system effectors are smooth muscle and glands. |
The enteric nervous system is under conscious control. |
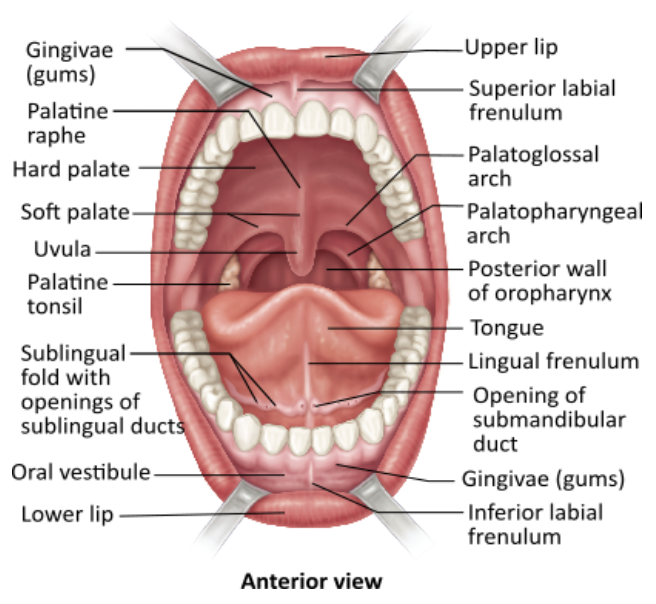
The uvula is an extension of the __________.
palatopharyngeal arch |
soft palate |
oral vestibule |
lingual frenulum |
soft palate
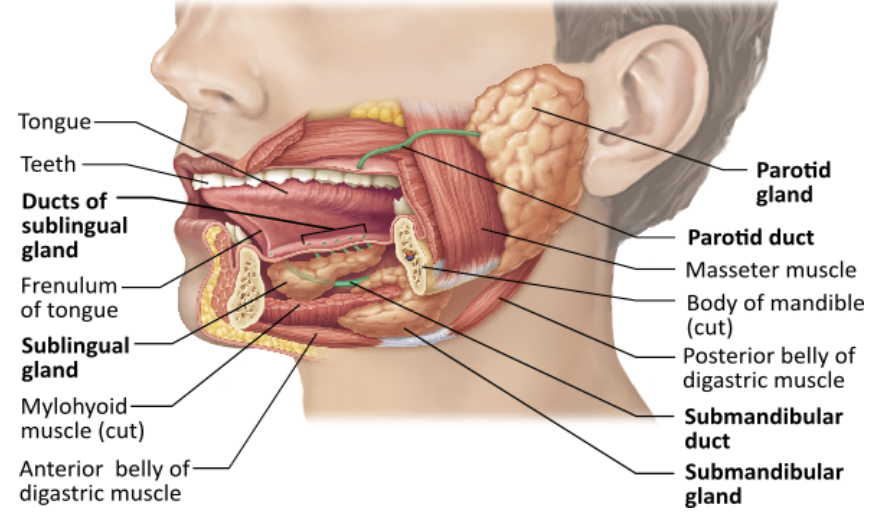
Which of the following is NOT a function of saliva?
Saliva contains enzymes that begin the chemical breakdown of proteins. |
Saliva dissolves food chemicals so that they can be tasted. |
Saliva cleanses the mouth. |
Saliva moistens food and helps compact it into a bolus. |
Saliva contains enzymes that begin the chemical breakdown of proteins. |
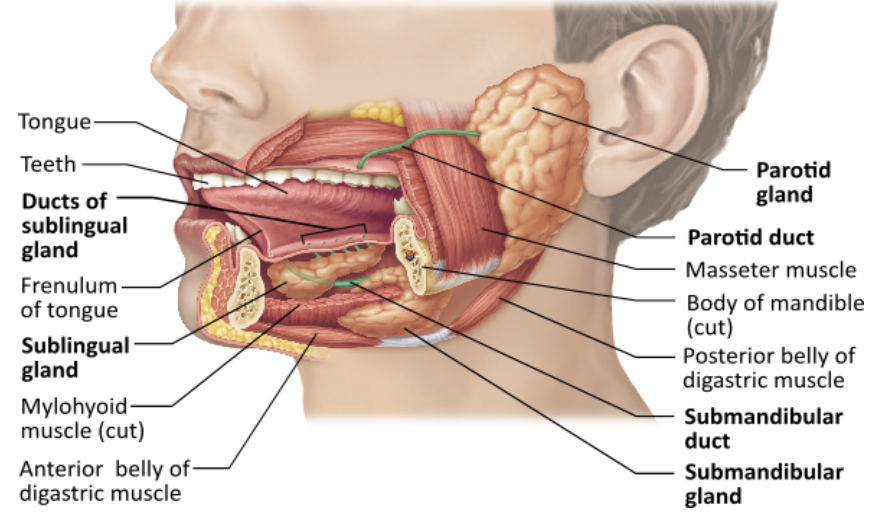
Which of the following inhibits salivation?
the sight or smell of food |
being stressed or frightened |
relaxing after a meal |
ingestion of spicy foods |
being stressed or frightened
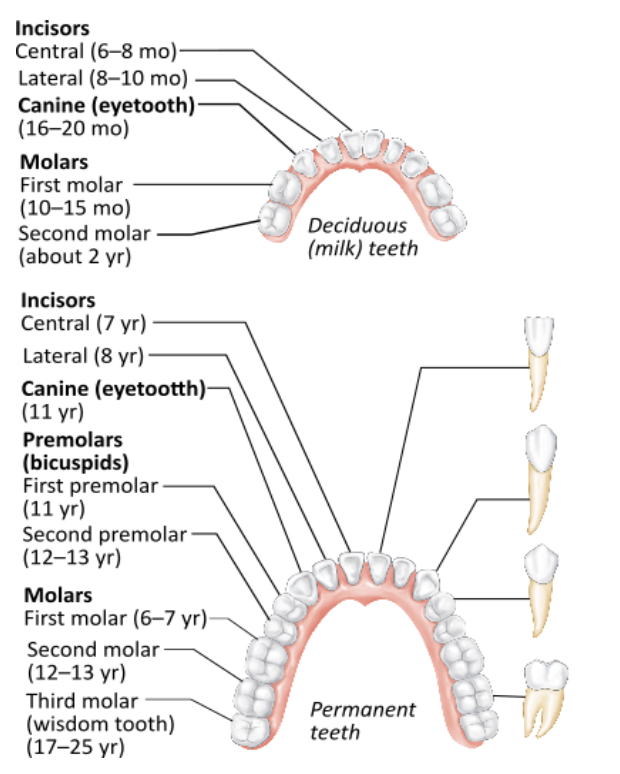
How many total permanent teeth should an adult have, assuming none have been lost or removed?
8 |
16 |
20 |
32 |
32 |
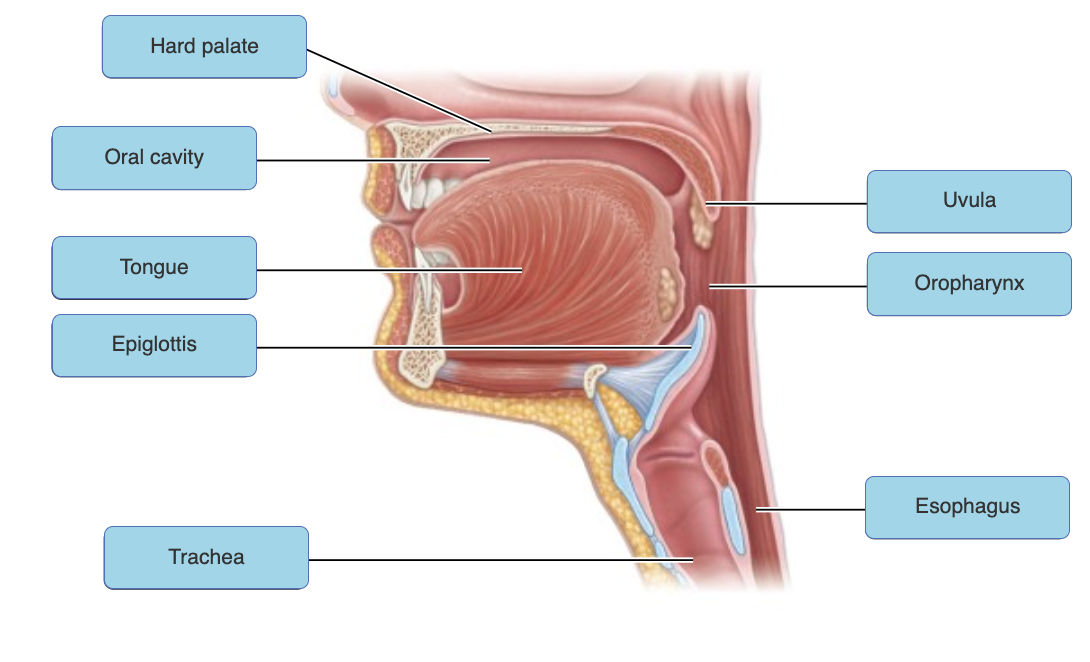
just know
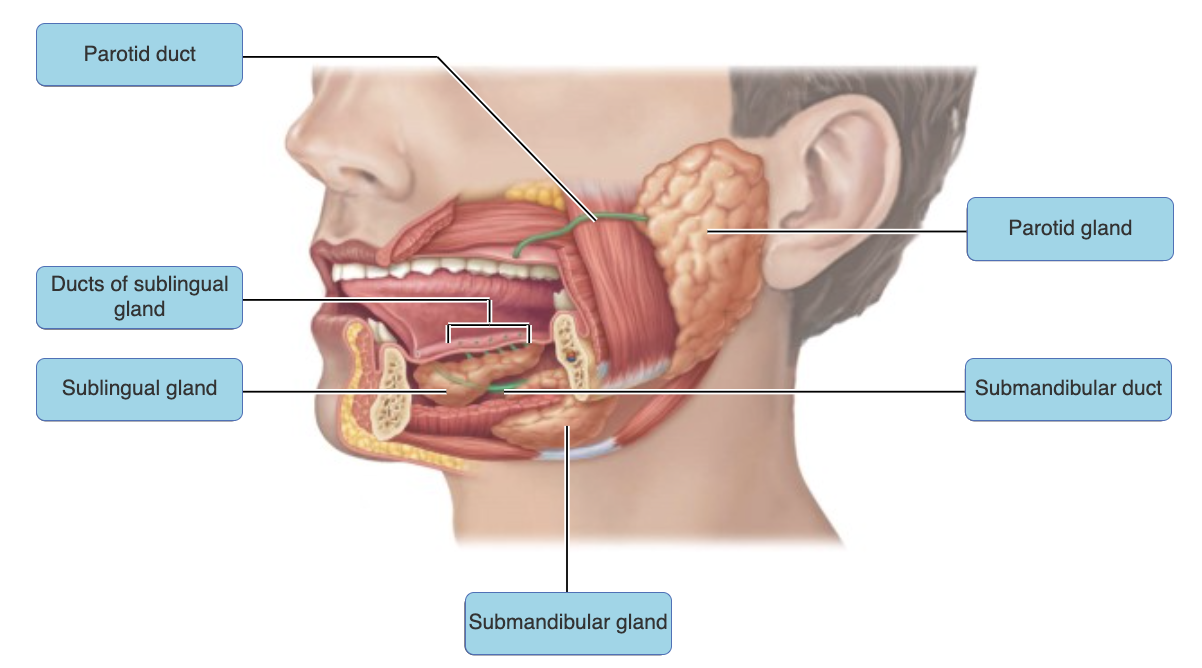
just know
The deciduous dentition consists of __________ teeth.
10 |
16 |
20 |
32 |
20
Which of the following are types of papillae on the tongue that contain taste buds?
vallate and filiform |
fungiform and vallate |
palatine and vallate |
fungiform, vallate, and filiform |
fungiform and vallate |
The digestive function of the liver is to produce digestive enzymes.
True |
False |
False |
All of the following are true of swallowing (deglutition) except one. Select the statement that is NOT true of swallowing.
The involuntary portion of swallowing takes place in the pharynx. |
The mouth, pharynx and esophagus all take part in swallowing. |
The epiglottis assists in propelling food into the trachea. |
The voluntary phase of swallowing takes place within the mouth. |
The epiglottis assists in propelling food into the trachea. |
Another term for swallowing is deglutition.
True |
False |
True
The soft palate reflexively opens the nasopharynx to allow the passage of food, which is now called a bolus.
True |
False |
False |
The __________ phase of gastric secretion begins as chyme enters the duodenum.
cephalic |
intestinal |
reflux |
gastric phase |
intestinal |
Gastric juice does not typically cause a burning sensation within the stomach. But reflux of gastric juice into the esophagus can cause a burning sensation. One reason for the burning sensation caused by the gastric reflux is that the esophagus ______.
secretes mucus that is not identical to stomach mucus |
is internally lined by epithelial cells that are in direct physical contact with the contents of the esophagus |
has enzymes that react with stomach acid to cause a burning sensation |
None of the listed responses is correct. |
secretes mucus that is not identical to stomach mucus |
Some antacid drugs block histamine receptors, resulting in reduction of the production and excretion of stomach acid. These drugs have the biggest effect on which of the following?
surface epithelial cells |
chief cells |
parietal cells |
mucous neck cells |
parietal cells |
Select the one response below that would NOT result from a drug that blocks histamine receptors in the cells lining the stomach.
It would cause the release of secretin and cholecystokinin. |
It would reduce the symptoms of heartburn. |
It would raise the pH of the stomach. |
It would lower the activity of parietal cells. |
It would cause the release of secretin and cholecystokinin. |
Pepsinogen, an inactive digestive enzyme, is secreted by the ________.
chief cells of the stomach |
parietal cells of the stomach |
Brunner's glands in the duodenum |
goblet cells of the small intestine |
chief cells of the stomach |
Which vitamin requires intrinsic factor in order to be absorbed?
C |
A |
K |
B12 |
B12 |
Which of the following produce intrinsic factor?
parietal cells |
enteroendocrine cells |
zymogenic cells |
mucous neck cells |
parietal cells |
The ingestion of a meal high in fat content would cause which of the following to occur?
Bile would be released from the gallbladder to emulsify the fat in the duodenum. |
This type of food would cause secretion of gastrin to cease, resulting in faster gastric emptying. |
The acid secretions from the stomach would be sufficient to digest this food but may cause heartburn. |
Increased production of trypsinogen. |
Bile would be released from the gallbladder to emulsify the fat in the duodenum.
Hormones or paracrines that inhibit gastric secretion include ________.
secretin |
histamine |
gastrin |
ACh |
secretin
Fats significantly delay the emptying of the stomach through hormonal and neuronal signals.
True |
False |
True
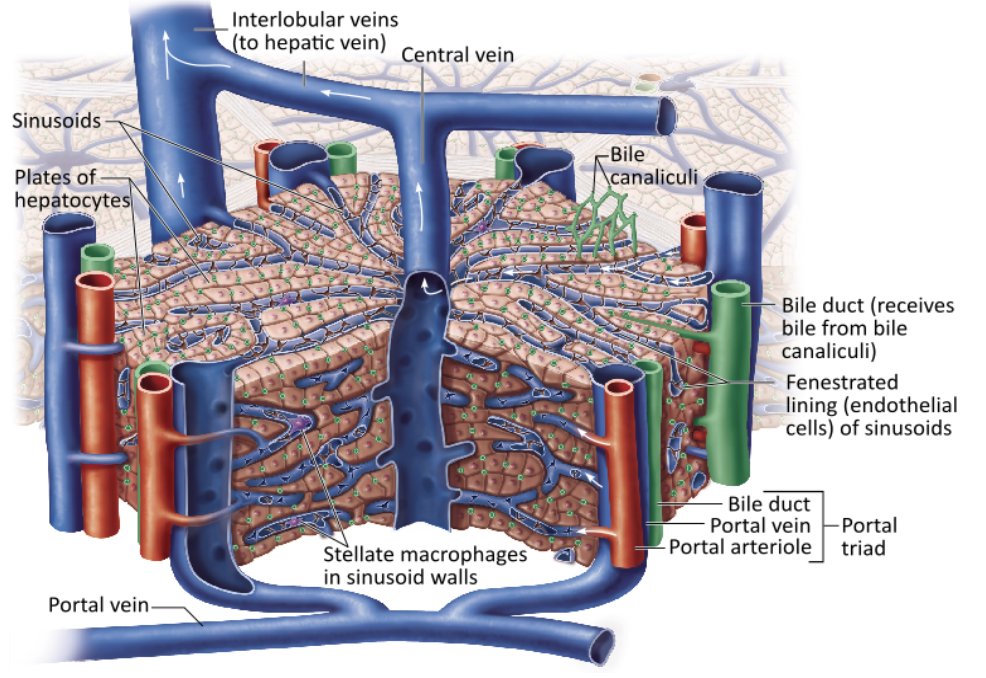
Which of the following constitute a portal triad?
the hepatic artery and two hepatic veins |
three lobules sharing a common central vein |
a bile duct along with a portal venule and arteriole |
the porta hepatis |
a bile duct along with a portal venule and arteriole |
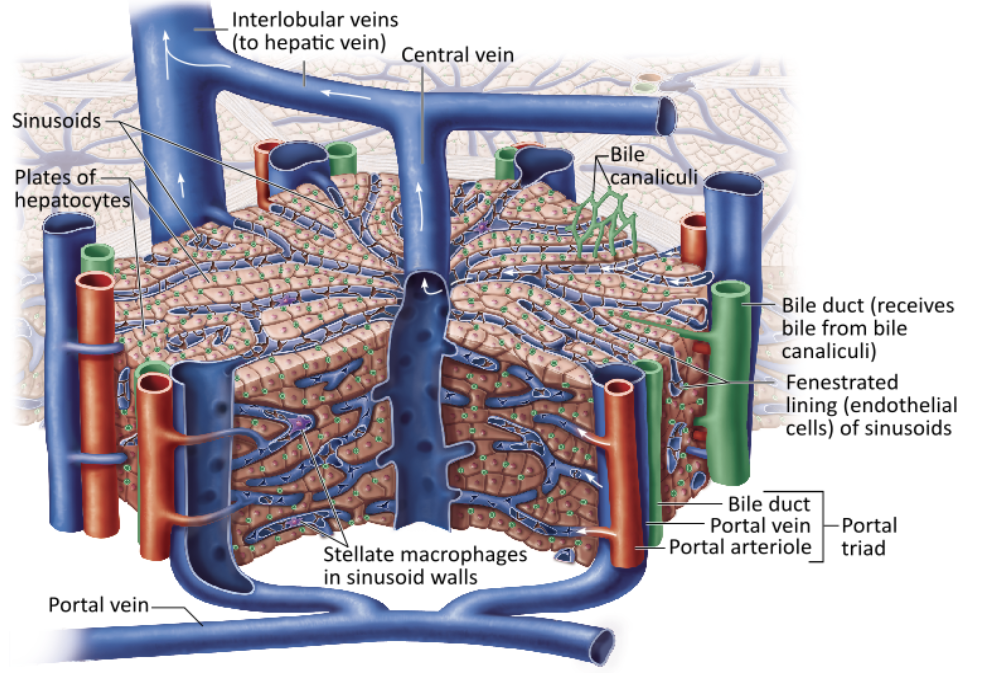
Which vessel delivers nutrient-rich blood to the liver from the digestive tract?
hepatic portal vein |
inferior vena cava |
central vein |
hepatic vein |
hepatic portal vein |
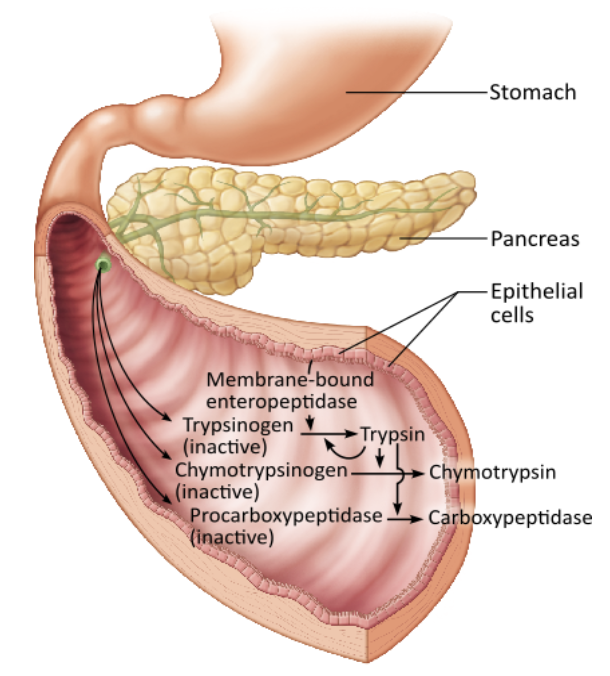
Which chemical activates the transformation of trypsinogen to trypsin?
amylase |
chymotrypsin |
enteropeptidase |
carboxypeptidase |
enteropeptidase
Bile is secreted by the __________ under hormonal influence of __________.
pancreas; secretin |
small intestine; CCK |
gallbladder; gastrin |
liver; secretin |
liver; secretin
Select the best explanation for why protease enzymes are secreted in inactive forms.
The immunoglobulins protecting the digestive tract would be digested without proper regulation of protein digesting enzymes. |
The enzymes would digest each other if they were not properly regulated. |
Inactive enzymes will simply be expelled with the feces if no protein is present in the digesting food; this will help to conserve energy. |
The cells producing inactive enzymes are themselves protected from the enzymes until they are safely within the lumen of the GI tract. |
The cells producing inactive enzymes are themselves protected from the enzymes until they are safely within the lumen of the GI tract. |
Hepatocytes do NOT ________.
detoxify toxic chemicals |
process nutrients |
produce digestive enzymes |
store fat-soluble vitamins |
produce digestive enzymes
Digestion and absorption of which of the following would be affected the most if the liver were severely damaged?
starches |
carbohydrates |
lipids |
proteins |
lipids |
The __________ is the first segment of the small intestine.
colon |
ileum |
duodenum |
jejunum |
duodenum |
Which of the following is NOT a structural modification of the small intestine that increases surface area?
rugae |
villi |
circular folds |
microvilli |
rugae |
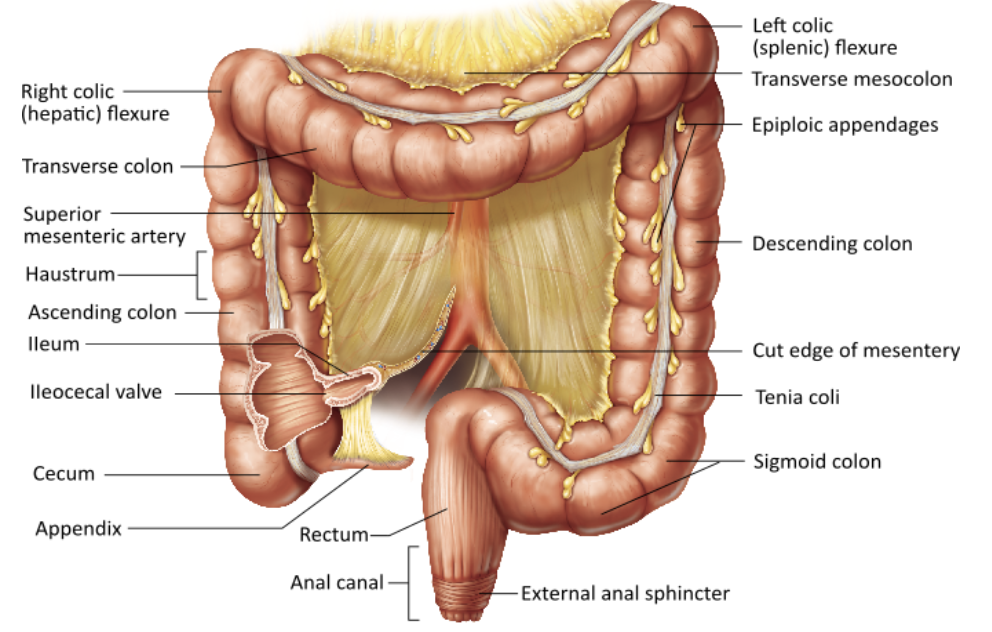
Which of the following propels food residue over large areas of the colon three to four times a day?
mass movement |
Valsalva's maneuver |
defecation reflex |
haustral contractions |
mass movement |
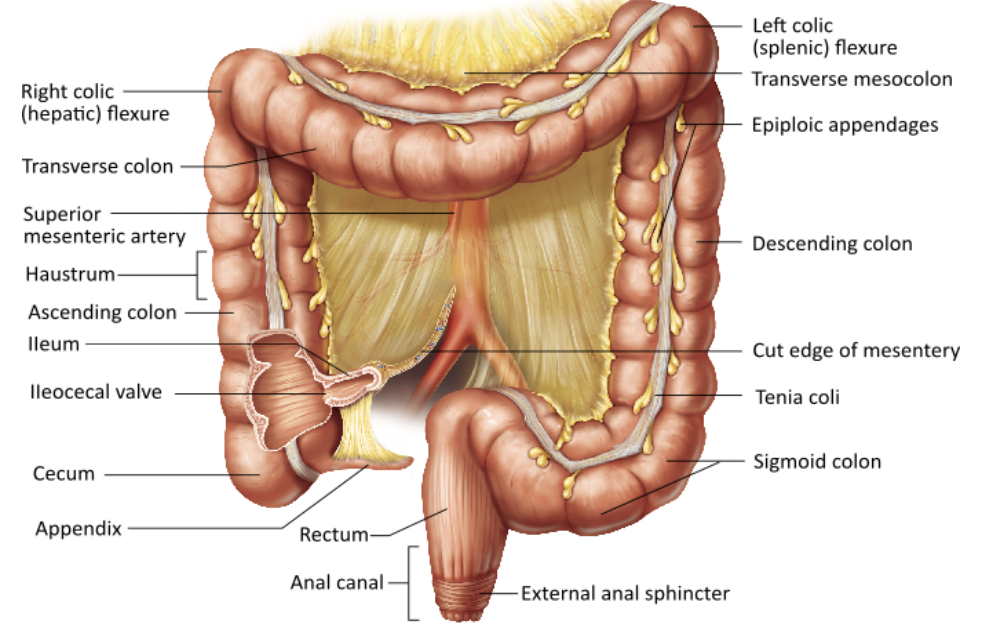
Which of the following is the primary physiological function of the large intestine?
primary digestion of food |
water absorption and feces elimination |
nutrient absorption |
mechanical breakdown of food |
water absorption and feces elimination |
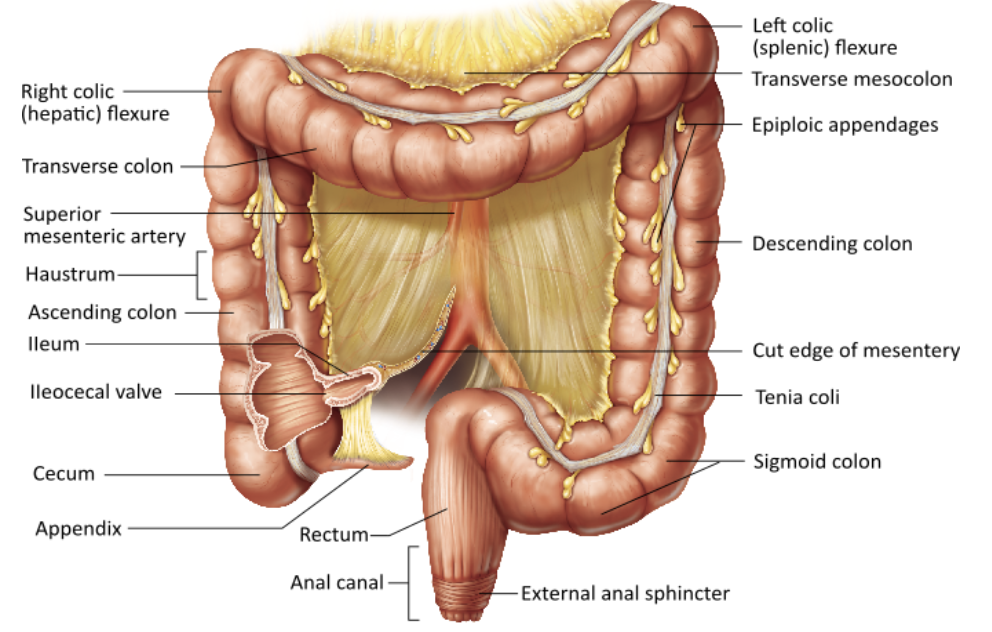
Which of the following is NOT a function of the large intestine?
absorption of water |
absorption of electrolytes |
synthesis of intrinsic factor |
synthesis of vitamins |
synthesis of intrinsic factor |
Which of the following is an essential role played by large intestine bacteria?
synthesis of vitamin K |
absorb bilirubin |
synthesize vitamins C and D |
produce gas |
synthesis of vitamin K |
Which of the following is NOT characteristic of the large intestine?
It has pocket-like sacs called haustra. |
It exhibits external muscular bands called teniae coli. |
It is longer than the small intestine. |
It does not contain villi. |
It is longer than the small intestine. |
Carbohydrates are digested into __________.
amino acids |
glycerol |
nucleotides |
monosaccharides |
monosaccharides |