HBS Unit 3 Exam
1/97
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
98 Terms
what are the semilunar valves
the aortic and pulmonary valves
what are the atrioventricular valves
the tricuspid and mitral valves
critical structures located between the heart's upper (atria) and lower (ventricles) chambers.
papillary muscles
specialized, finger-like muscle projections located in the left and right ventricles of the heart that attach to mitral and tricuspid valve leaflets via chordae tendineae
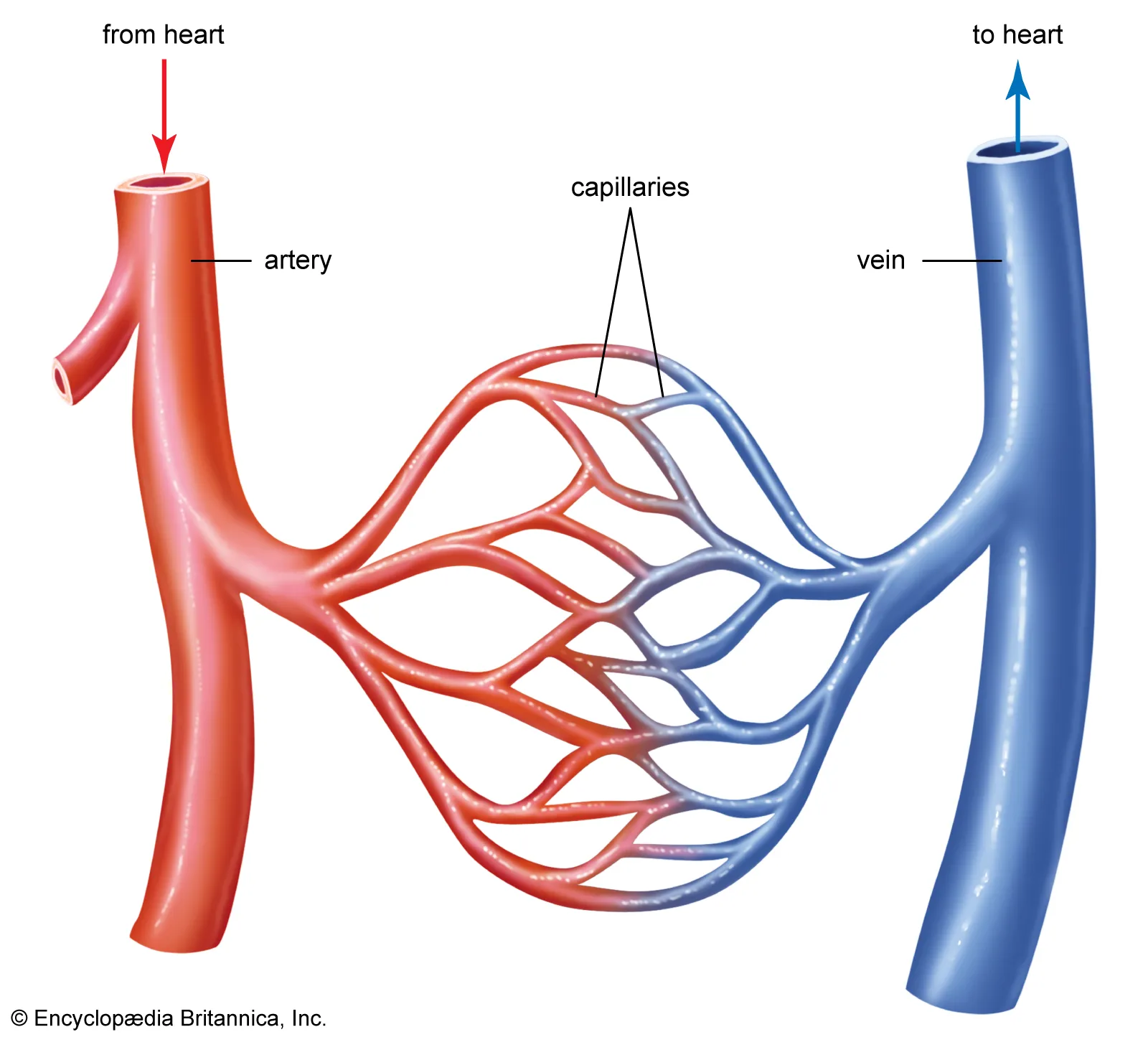
what is the anatomy of arteries, veins, and capillaries?
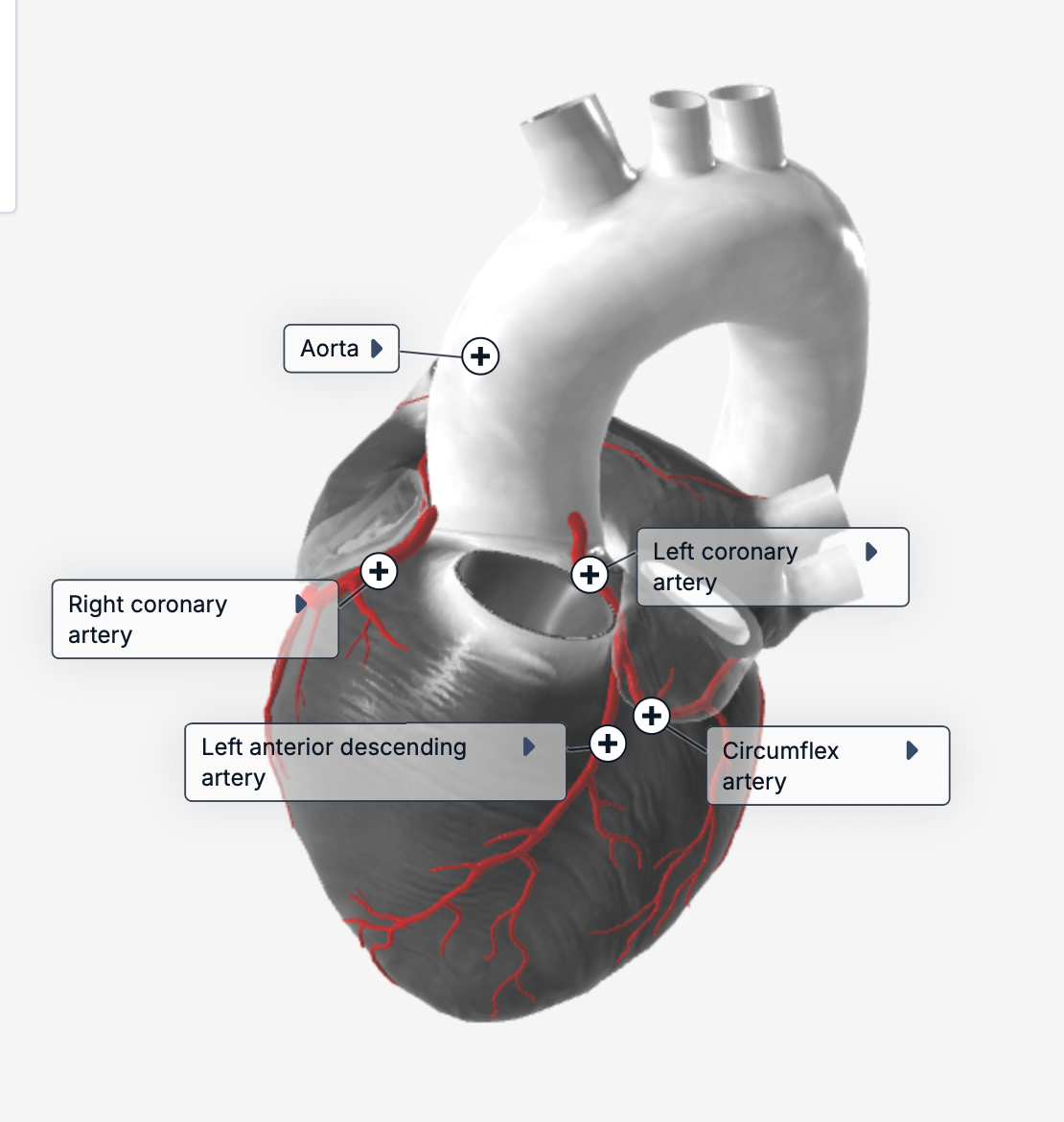
where is the right coronary artery on the heart?
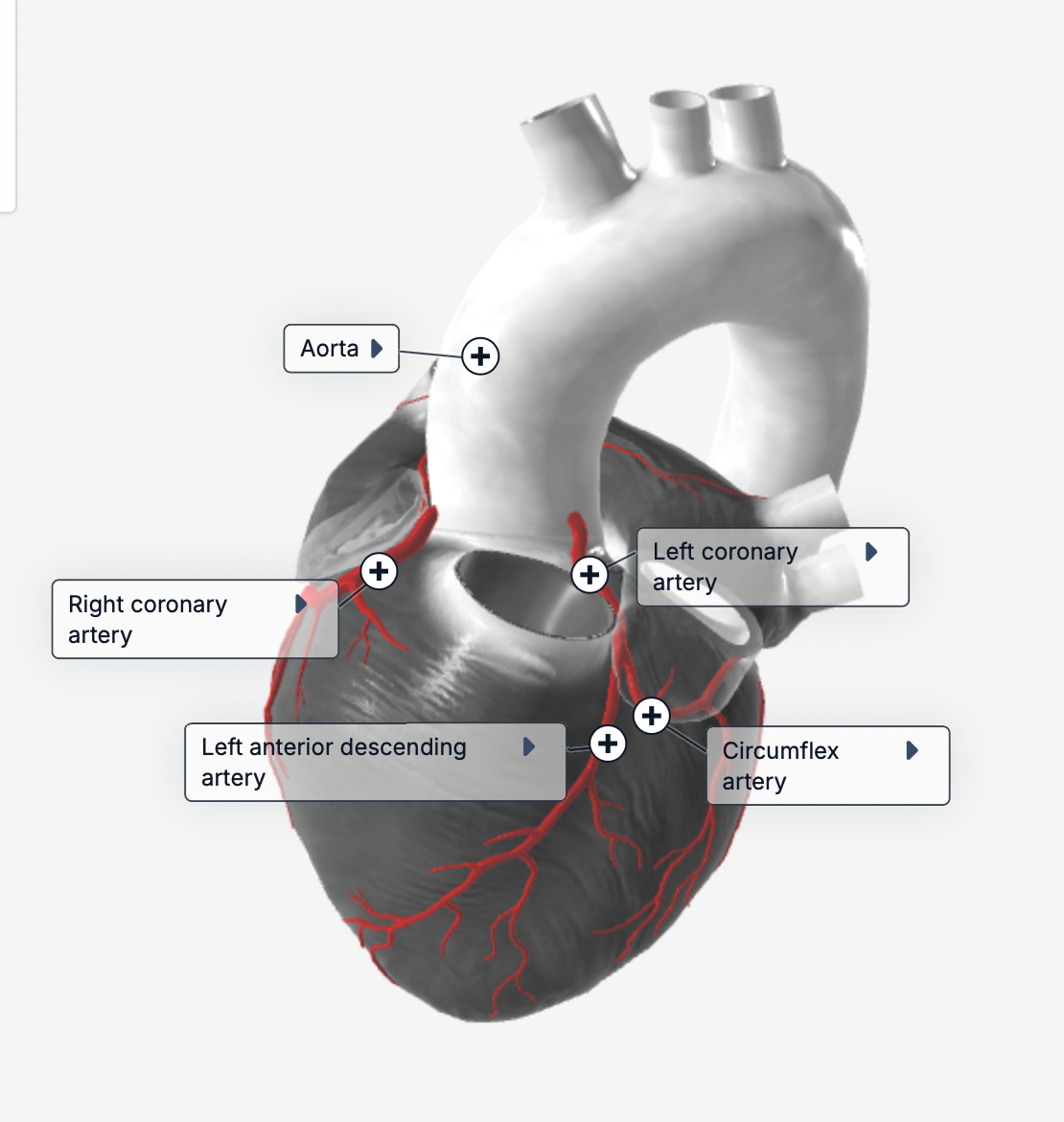
where is the left coronary artery?
where is the circumflex artery?
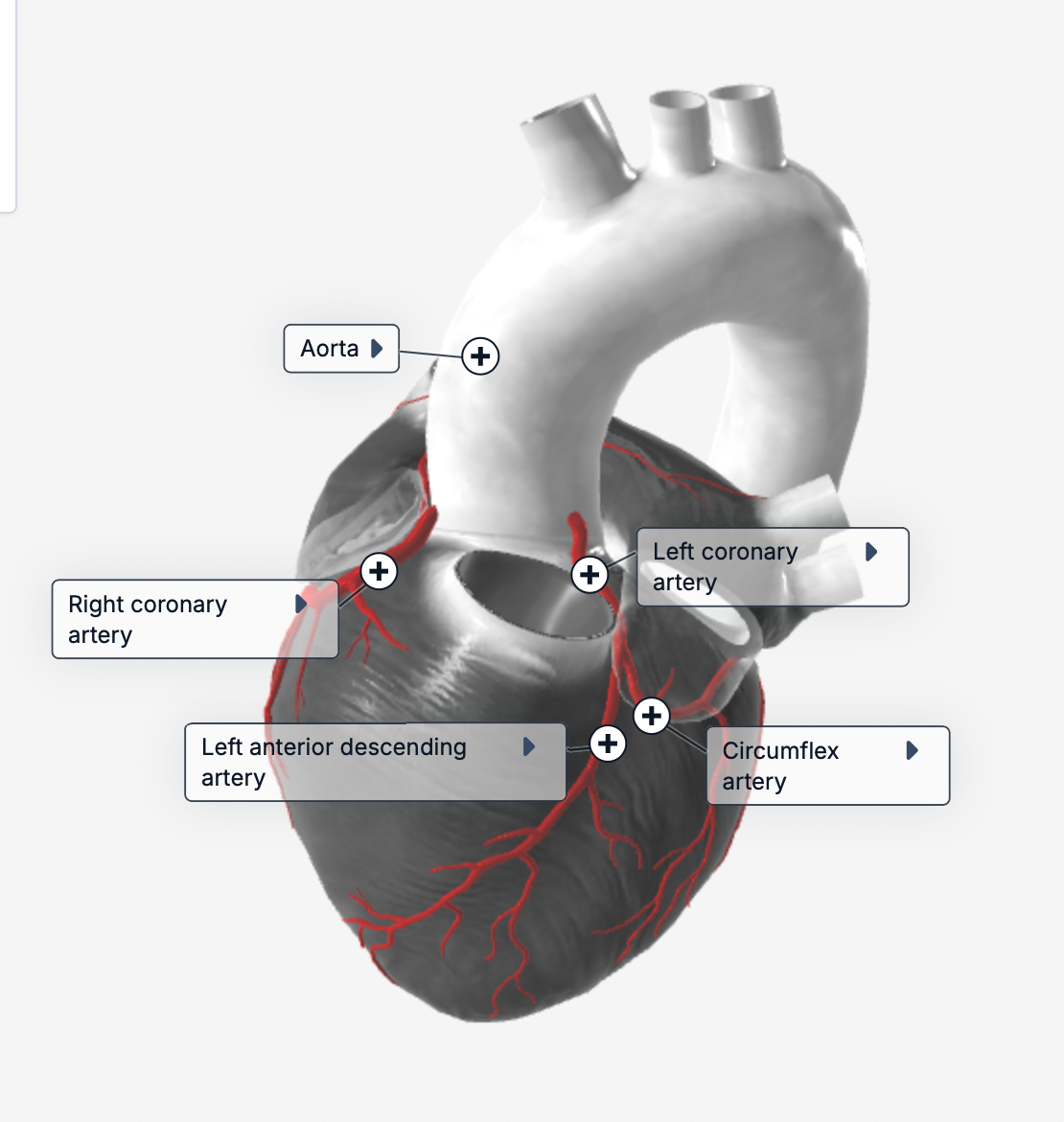
where is the left anterior descending artery?
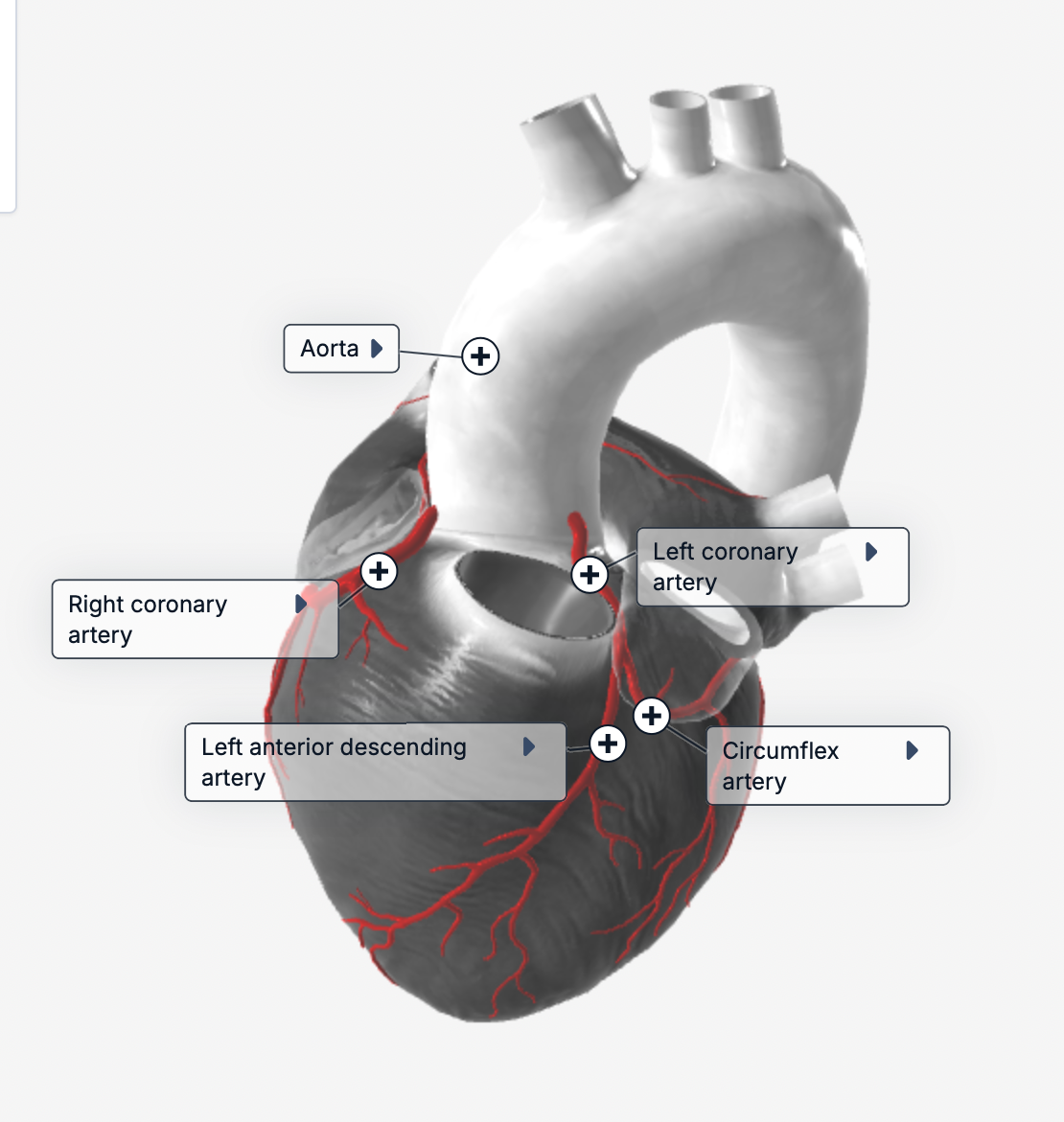
how to tell the difference between blood vessels?
Arteries have thick, muscular walls and a rounded shape, typically appearing pink/red.
Veins have thin, flimsy walls, often appear collapsed or flat, and are darker blue/purple.
Capillaries are microscopic and form thin, net-like structures.
carotid artery
The left and right common carotid arteries originate from different arteries but follow symmetrical paths up the neck where they branch to supply blood to the head, including the brain and face.
The right carotid originates from the brachiocephalic artery, and the left originates from the aortic arch.
jugular vein
Jugular veins take deoxygenated blood from the head back to the heart.
They travel down the neck where they meet the subclavian veins and drain into the brachiocephalic veins.
peripheral artery disease
a common circulatory problem caused by atherosclerosis (plaque buildup) narrowing arteries, usually in the legs, which reduces blood flow.
Common symptoms include leg pain, numbness, and cramping during activity (claudication).
Key risks include smoking, diabetes, high blood pressure, and age over 50
cardiac output
A measure of how much blood is pumped by both ventricles in one minute; quantified as mL per minute.
heart rate
A count of how many times the heart beats in a minute; quantified as beats per minute.
stroke volume
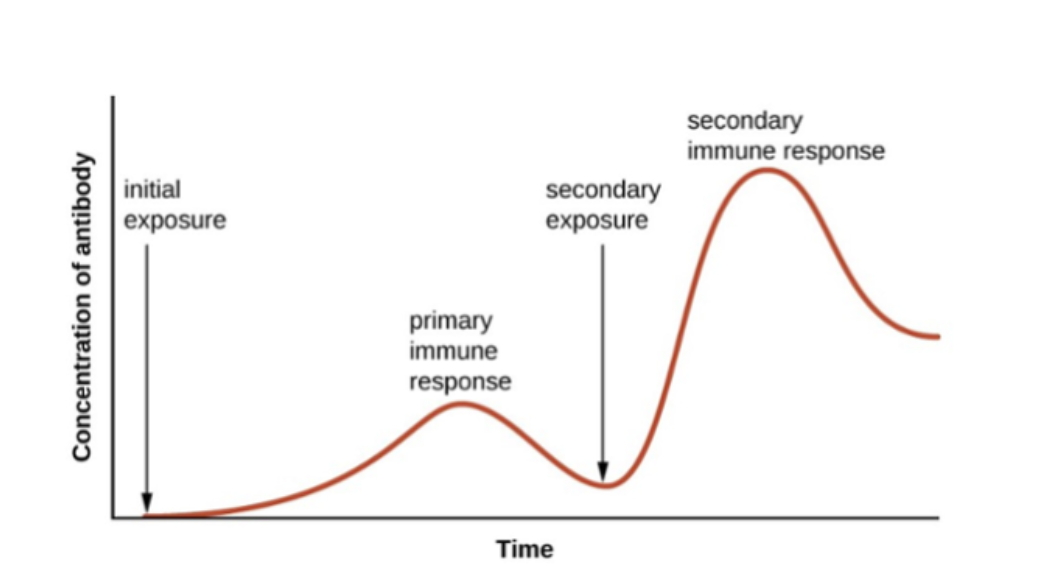
The amount of blood being pumped out of the heart with each heartbeat; quantified as mL per beat. On average, the stroke volume remains relatively stable at 75 mL/beat.
how to calculate cardiac output
cardiac output (mL/min) = heart rate (b/min) x stroke volume (mL/b)
Some of the more thrilling activities, like bungee jumping, can increase a person’s heart rate significantly. If a client’s heart rate jumps to 140 beats per minute, how would that affect their cardiac output?
increase their cardiac output
Dehydration decreases cardiac output.
true
What are some consequences of low cardiac output?
fatigue, Low levels of oxygen in the blood, Breathlessness or trouble breathing, and Hypotension. NOT HUNGER
hypertension
a chronic condition defined as consistently high blood pressure (typically ≥130/80 mmHg), where blood forces against artery walls too strongly. Known as a "silent killer," it usually shows no symptoms but causes severe damage to the heart, brain, and kidneys over time.
what are the risk factors for hypertension?
high salt intake, obesity, lack of physical activity, smoking, alcohol consumption, high stress, and insufficient sleep.
Non-modifiable factors include aging, family history, and race.
what does ABI stand for?
ankle-brachial index
how do you calculate ABI?
To calculate ABI, a medical professional uses the Doppler ultrasound device to listen to blood flow while also measuring and recording blood pressure in the arms and feet.
what is the process of the heart’s electrical system?
It starts at the SA node (pacemaker) in the right atrium, causing the atria to contract, then travels to the AV node, bundle of His, and Purkinje fibers, coordinating the contraction of the ventricles.
Initiation: The SA node fires an electrical signal.
Atrial Contraction: The signal travels through the atria, causing them to contract.
Delay: The AV node delays the signal, allowing the atria to fill the ventricles with blood.
Ventricular Contraction: The electrical signal travels through the bundle branches and Purkinje fibers, causing the ventricles to contract and pump blood to the body.
Sinoatrial (SA) node
The natural pacemaker in the right atrium, initiating impulses at 60–100 times per minute.
Atrioventricular (AV) node
Delays the impulse briefly to allow the ventricles to fill with blood from the atria.
Bundle of His / Bundle Branches
Transmit impulses from the AV node to the ventricles
Purkinje fibers
Distribute impulses rapidly throughout the ventricles, causing contraction.
arrythmia
an irregular heartbeat caused when the electrical signals that coordinate the heart’s beat misfire.
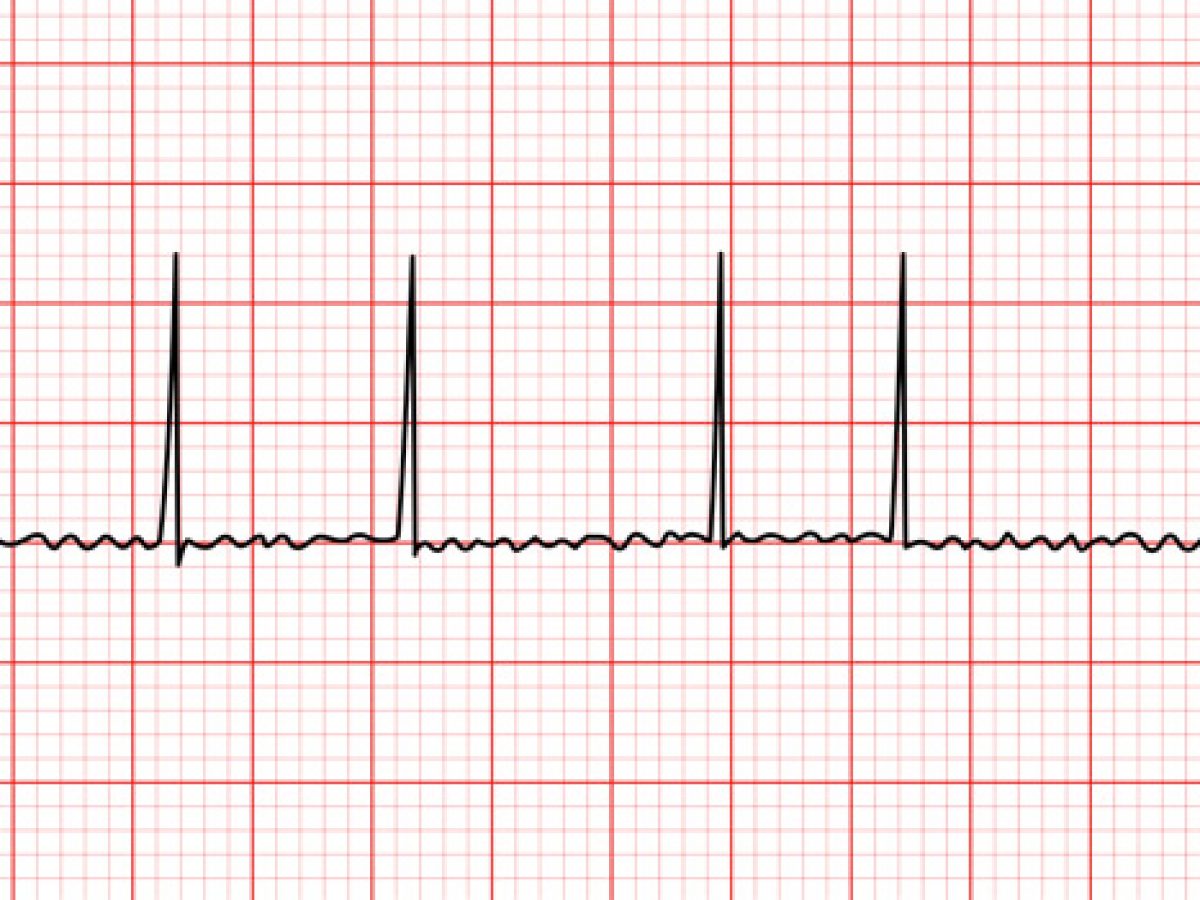
aFib
a common, often chronic, heart rhythm disorder where the upper chambers (atria) beat rapidly and irregularly. This quivering reduces pumping efficiency, increasing blood clot and stroke risk, and can cause palpitations, fatigue, and dizziness.
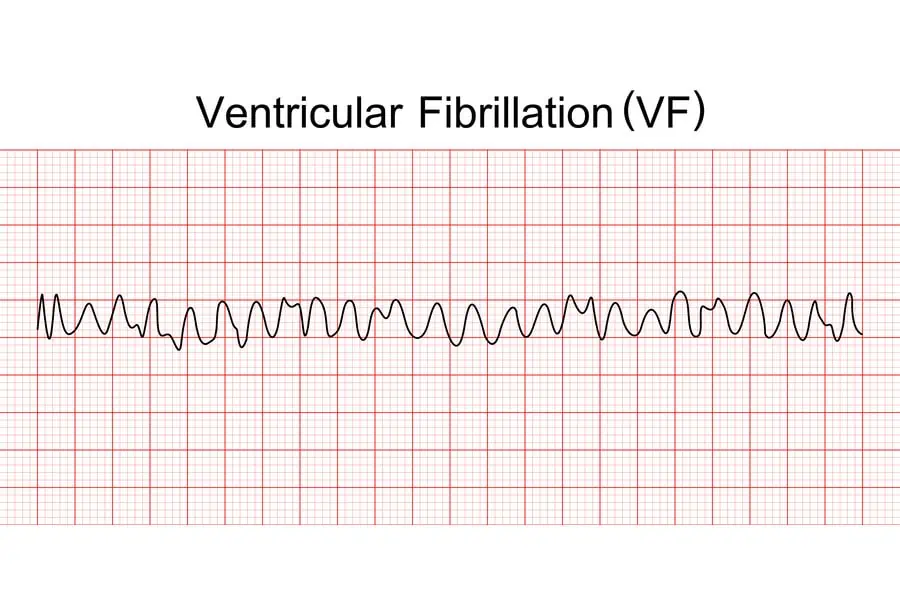
vFib
a life-threatening heart rhythm emergency where the heart's lower chambers quiver chaotically instead of pumping, causing immediate loss of consciousness and cardiac arrest.
It requires instant CPR and electrical defibrillation to prevent death.
It is often caused by heart attacks, heart disease, or severe electrolyte imbalances
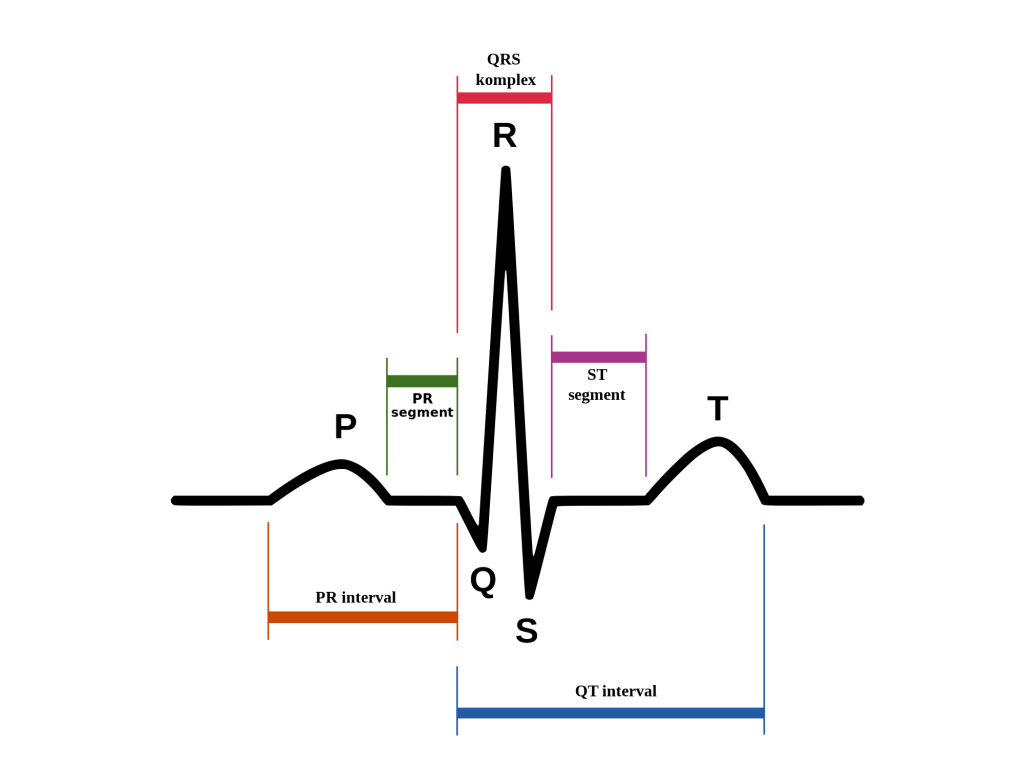
ekg + correspondence to the heart
P wave: Atrial depolarization (activation/contraction of the upper chambers).
PR Interval: Time for impulses to travel from the atria to the ventricles.
QRS Complex: Ventricular depolarization (contraction/pumping of the lower chambers).
ST Segment: Time between ventricular contraction and relaxation.
T wave: Ventricular repolarization (recovery/relaxation of the ventricles).
how do the lungs “work?”
The diaphragm contracts downward, and the intercostal muscles contract and open the ribcage to allow the lungs to expand
pulmonary edema
a serious, often life-threatening condition caused by excess fluid buildup in the lungs' alveoli, resulting in severe breathing difficulties.
Primarily triggered by heart issues (cardiogenic) or lung injuries (noncardiogenic), it leads to extreme shortness of breath, coughing, and low oxygen levels, requiring urgent medical attention.
risk factors for pulmonary edema
Cardiogenic (Heart-related): Most commonly caused by congestive heart failure, heart attack, or leaking/narrowed heart valves that prevent the heart from pumping effectively.
Noncardiogenic (Lung/Other-related): Kidney failure, severe infection (pneumonia), lung damage from toxin inhalation, pulmonary embolism, or sudden exposure to high altitudes.
Risk Factors: History of heart disease, hypertension, renal failure, smoking, or living at or visiting high altitudes
Pulmonary Fibrosis
a chronic, progressive lung disease where deep lung tissue becomes scarred, thickened, and stiff, hindering oxygen absorption.
It causes severe shortness of breath, a dry cough, and fatigue.
risk factors for Pulmonary Fibrosis
Age and Gender: Most commonly diagnosed in people in their 60s and 70s, with a higher prevalence in males.
Smoking: A significant risk factor that directly causes lung tissue damage and increases risk of developing disease
Occupational and Environmental Exposures: Long-term exposure to inhaled toxins is a leading cause. Things like Silica dust (sandblasting, stone cutting), Asbestos fibers, Hard metal dusts, Coal dust, and Organic dusts (mold, animal droppings, bird feathers).
Family History/Genetics: The risk is higher if a first-degree relative has the disease, with over 10 different gene mutations linked to increased risk.
Medical Conditions like Autoimmune Disorders (ex. Rheumatoid arthritis, scleroderma, and Sjogren’s syndrome), Chronic Viral Infections (ex. Epstein-Barr virus (EBV), hepatitis C, and herpes virus), and Gastroesophageal Reflux Disease (GERD)
anaphylaxis
A severe, potentially life-threatening allergic reaction that involves multiple body systems, prominently impacting the airway (causing swelling), gastrointestinal tract (leading to vomiting or diarrhea), cardiovascular system (triggering rapid heartbeat or hypotension), and skin (resulting in hives or itching).
Anaphylaxis can result from exposure to allergens such as certain foods, medications, or insect stings.
how is anaphyaxis treated?
epinephrine is the first-line and only effective treatment for anaphylactic shock
It is critical to administer it immediately via intramuscular injection into the thigh (often using an auto-injector) to reverse symptoms, such as closing airways and low blood pressures
spirometer
An instrument used to measure the volume of air inhaled and exhaled by the lungs, helping to assess lung function and diagnose respiratory conditions.
it measures lung volumes during normal breathing + with max effort.
MEASURES TOTAL LUNG CAPACITY
tidal volume
the vol. of air breathed in + out without concious effort
inspiratory reserve volume
the additional volume of air that can be inhaled with max effort after normal inspiration
expiratory reserve volume
the additional volume of air that can be forcibly exhaled after normal exhalation.
vital capacity
total volume of air exhaled after maximum exhalation
residual volume
volume of air in lungs after max
total lung capacity
total volume of the lungs: the sum of the vital capacity and the residual volume.
(TLC = VC + RV)
peak flow meter
a simple device to monitor how open your airways are. A patient blows into the device as hard as they can and the health care provider records the value shown on the indicator.
MEASURES FEV1
FEV1
forced expiratory volume
FEV1 is the maximum amount of air that can forcefully be exhaled in one second
____________
FEV1 greater than 80 percent of predicted value = Normal
FEV1 60 to 79 percent of predicted = Mild obstruction
FEV1 40 to 59 percent of predicted = Moderate obstruction
FEV1 less than 40 percent of predicted = Severe obstruction
Melissa Martin
the 11-year-old asthmatic
having trouble in gym and band class
Melissa’s FEV1 was measured as 79% once the doctor administered Melissa albuterol, a short-acting bronchodilator, her FEV1 was measured again as 93%. This response indicates that the impairment is reversible.
short-term meds for asthmatics
“rescue” medication
Melissa should use this when she experiences an episode of shortness of breath and wheezing
albuterol!
long-term meds for asthmatics
a long-term control medication that will hopefully cut down on the number of times she needs to use her rescue medication.
fluticasone!
what triggers asthma?
Allergens: Dust mites, pet dander, cockroaches, and mold.Irritants: Tobacco smoke (including second-hand), air pollution, strong odors/perfumes, and cleaning products.
Respiratory Infections: Colds, influenza, and viruses.
Weather & Environment: Cold air, high humidity, and changing weather conditions.
Physical Activity: Exercise-induced bronchoconstriction, often triggered by intense activity in dry/cold air.
Emotional Factors: Strong emotions like laughing, crying, or intense stress
Innate Immunity
(First Line)
General defenses present from birth, such as skin, mucus, stomach acid, and cells like phagocytes that destroy invaders immediately.
stomach acid, normal flora, phagocytes, tears, digestive enzymes, nasal mucosa, and cilia.
Adaptive Immunity
Second Line
Slower-acting, specific response that targets specific pathogens and creates "memory cells" to fight future infections faster.
plasma
A yellowish liquid that makes up about 55% of blood volume.
It is mostly water (about 90%) but also contains proteins (like fibrinogen and albumin), glucose, nutrients, and waste products.
the liquid base for whole blood
Red Blood Cells (Erythrocytes)
These make up about 45% of blood volume and are responsible for carrying oxygen from the lungs to the rest of the body.
They contain a protein called hemoglobin, which enables them to bind oxygen.
White Blood Cells (Leukocytes)
Part of the immune system, these cells protect the body against infections, viruses, and bacteria.
They are less numerous than red blood cells.
Platelets (Thrombocytes)
These are small cell fragments that play a critical role in blood clotting, helping to form a plug to stop bleeding when blood vessels are damaged.
how does the skin protect the body?
by acting as a multi-layered physical, chemical, and biological barrier against environmental threats, injury, and dehydration.
Physical Barrier: The outermost layer (epidermis) consists of tough, dead cells (keratin) that create a waterproof, durable shield against chemicals, pathogens, and physical trauma.
Immune Defense: Skin cells act as a first line of immune defense, using acidic secretions (sweat/oil) to kill harmful microbes.
Temperature Regulation: The skin controls heat loss by constricting blood vessels (keeping warmth in) or dilating them and producing sweat to cool the body down.
Protection from UV Radiation: Melanin, a pigment in the epidermis, absorbs and disperses harmful ultraviolet light to prevent DNA damage to skin cells.
Sensory Warning System: Nerve endings in the dermis detect heat, cold, pain, and pressure, allowing the body to react to danger.
Moisture Control: It prevents the body's internal fluids from evaporatin
prions
any of various infectious proteins that are abnormal forms of normal cellular proteins.
Prions proliferate by inducing normal proteins to convert to the abnormal form that causes diseases, such as mad cow disease, Creutzfeldt-Jakob disease, and kuru.
infectious, misfolded proteins that cause rare, fatal neurodegenerative diseases in humans and animals by inducing normal brain proteins to misfold into a diseased shape. Unlike viruses or bacteria, prions lack genetic material (DNA/RNA) and are highly resistant to standard sterilization methods
BRAIN
viruses
any of a large group of nonliving, submicroscopic infective agents that typically comprise an RNA or DNA core of genetic material surrounded by a protein coat.
Viruses are not cellular and require a host in which to replicate.
They cause various important diseases in all forms of life.
SINUSES
bacteria
tiny, single-celled organisms found everywhere on Earth, often existing as simple prokaryotic cells without a nucleus.
LUNGS
protists
microscopic, single-celled eukaryotic organisms that live parasitically, causing diseases in humans and mammals by multiplying within them. They are often transmitted via contaminated food/water (fecal-oral) or insect vectors.
LOWER GUT
fungi
microorganisms, including yeasts and molds, that cause diseases in humans, animals, or plants by breaking skin barriers or infecting tissues
FEET
helminths
parasitic worms
multicellular invertebrates ranging from microscopic to over a meter in length—that infect humans, primarily in the intestines, causing diseases like hookworm and ascariasis.
They are transmitted through contaminated soil, food, or water, impacting 1.5 billion people
INTESTINES
virus infection stages
Incubation Period (Entry & Replication): The virus enters the body and begins replicating in host tissues, often without symptoms. Although asymptomatic, the person can still be contagious.
Prodromal Period (Initial Symptoms): Early, non-specific symptoms appear, such as low-grade fever, malaise, and fatigue.
Period of Illness (Active/Acute Phase): The infection reaches its peak. Specific symptoms manifest, such as cough, body aches, and high fever. The immune system works heavily to combat the virus, which is now at its highest count.
Period of Decline: Symptoms begin to diminish as the immune system successfully lowers the number of virus particles.
Convalescence (Recovery): The body repairs damage and symptoms subside completely, leading to recovery
Sepsis stages
sepsis: The body’s immune system overreacts to an infection causing inflammation.
severe sepsis: Organs in the body begin to malfunction, blood pressure is low, and inflammation continues.
septic shock: Extremely low blood pressure that does not respond to IV fluids.
TIME for sepsis symptoms
T - Temperature: Body temperature that is higher or lower than normal.
I - Infection: Signs or symptoms of an infection, such as fever, cough, or a painful, red, or swollen wound.
M - Mental Decline: Confusion, sleepiness, or difficulty waking up.
E - Extremely ill: Severe pain, discomfort, or shortness of breath ("feeling like you might die")
what do pacemakers do?
they reset the SA node and stop it from misfiring
lymphatic system
consists of organs, ducts, and lymph nodes.
It transports a clear, watery fluid called lymph.
In addition to maintaining fluid levels in your body, the lymphatic system absorbs fats from the digestive tract, protects your body from pathogens, and transports and removes waste from the lymph fluid.
spleen
filters the blood of foreign cells + old RBCs in need of replacement
antigens
anything that stimulates an immune response + a foreign invader such as a pathogen
antibodies
Y-shaped proteins produced by B cells in the immune system to identify and neutralize foreign invaders like bacteria, viruses, and toxins.
They work by binding to specific antigens (harmful substances) to destroy them or mark them for removal.
proteins that work to neutralize pathogens.
B-Cells
a type of lymphocyte (white blood cell) that matures in bone marrow and produces antibodies
white blood cells, maturing in the bone marrow, that play a key role in adaptive immunity by producing highly specific antibodies.
They identify pathogens (bacteria/viruses) using surface receptors, activating to produce plasma cells (antibody factories) and memory cells for long-term immunity.
antivirals and vaccines
Vaccines: Prophylactic agents that stimulate the immune system to recognize and fight pathogens before infection occurs, offering lasting immunity.
Antivirals: Therapeutic agents used to treat, manage, and reduce the severity of existing infections by inhibiting viral replication, often acting by blocking cell entry or interfering with enzymes.
Specific Uses: Vaccines are crucial for controlling pandemics (e.g., COVID-19, smallpox). Antivirals are essential for chronic or acute infections where vaccines are less effective, such as HIV, Hepatitis C, and influenza.
function of immune system
Its primary functions include detecting foreign antigens, neutralizing invaders through specialized white blood cells and antibodies, and remembering pathogens for future protection
lymph
a clear-to-white, watery fluid circulating throughout the lymphatic system, acting as the body's drainage and immune defense system.
It consists of interstitial fluid, white blood cells (especially lymphocytes), proteins, and fats. Lymph collects waste, toxins, and pathogens from tissues, transporting them to lymph nodes to be filtered and destroyed.
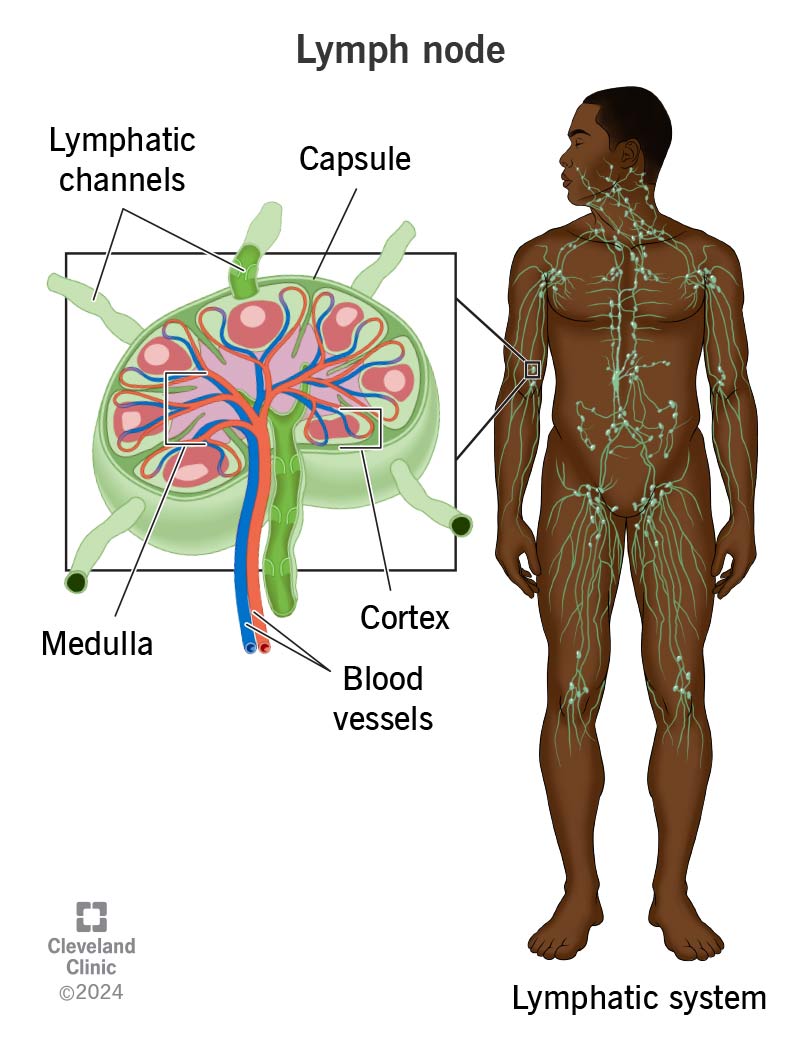
lymph node
Lymph nodes are small, bean-shaped organs that act as the body's immune system "checkpoints," filtering foreign substances like bacteria, viruses, and cancer cells from lymph fluid.
They contain high concentrations of white blood cells (lymphocytes) that fight infection and destroy these harmful agents.
They are found throughout the body, with clusters in the neck, armpits, and groin.
functions of the lymphatic system
The lymphatic system acts as a critical, multi-functional network for fluid balance, immunity, and nutrient absorption. It drains excess fluid (lymph) from tissues, filters pathogens and waste through lymph nodes, returns fluid to the bloodstream, and absorbs fats from the intestines, serving as a primary defense against infection.
skeletal muscle
Striations: Striated (striped appearance due to sarcomere alignment).
Voluntary: Yes, under conscious control.
Location: Attached to bones by tendons.
Functions: Produces body movement, maintains posture, and generates heat.
Role in Blood Movement: the "skeletal muscle pump" where contracting muscles compress nearby veins, forcing blood toward the heart
cardiac muscle
Striations: Striated (like skeletal muscle).
Voluntary: No, involuntary (autonomic control).
Location: Walls of the heart (myocardium).
Functions: Rhythmic contraction to pump blood throughout the body.
Role in Blood Movement: Acts as the primary pump, creating blood pressure to circulate blood through the entire cardiovascular system
smooth muscle
Striations: Non-striated (smooth appearance).
Voluntary: No, involuntary.
Location: Walls of hollow internal organs (stomach, bladder) and blood vessels.
Functions: Propels substances through organs (peristalsis) and regulates organ volume.
Role in Blood Movement: Constricts or dilates blood vessels (vasoconstriction/vasodilation) to regulate blood pressure and distribute blood flow throughout the body
Why do you think arteries, veins, and nerves are always oriented next to each other? Provide an example that illustrates your reasoning.
The proximity of components of the cardiovascular and nervous systems is efficient and assures organ placement is more compact.
Nervous and muscular tissues require a lot of energy and removal of wastes from their metabolic processes.
For example, the muscles of the forearm require input from the nervous system as well as a constant supply of blood, so by orienting together, the vessels and nerves can take the most efficient route to those muscles.
An abnormal swelling of a superficial vein of the legs is called a varicose vein. What do you think causes this condition, and why aren’t there varicose arteries?
Varicose veins develop when vein walls lose their normal strength and elasticity, causing them to become stretched out.
The weakened, damaged valves in varicose veins are unable to effectively pump blood up to the heart, and blood instead flows backward.
The backflow of blood causes pooling and swelling in the affected veins.
Arteries cannot be varicose because arterial walls contain a layer of thick muscle, and arteries do not have valves.
What are the potential consequences of untreated heart arrhythmia? How would that impact other body systems?
An arrhythmia can impact overall heart function, as well as the functioning of other body system.
While the heart is experiencing an abnormal rhythm, blood may not be circulated, starving the heart and other organs of needed oxygen.
How would an injury to the trachea impact function in the body?
The trachea is the main airway that leads from the larynx to the bronchi, supplying oxygen-rich air to the lungs and carrying carbon dioxide out of the lungs.
If a person’s trachea is injured, the person may have trouble breathing. Over time, a lack of oxygen could cause fatigue, shortness of breath, respiratory infections, and rapid heart rate.
Describe the interaction between the cardiovascular system and the respiratory system.
The respiratory and cardiovascular systems work as a team to oxygenate the cells and tissues of your body and remove carbon dioxide. The two systems interact through the pulmonary and systemic loops.
Emphysema is a condition that causes damage to the walls of the alveoli. How could you support a client with emphysema on your expedition? What recommendations do you have for them as they prepare for the trip?
A client with emphysema could be supported during an expedition by having them move slower and encouraging proper breathing.
If the individual has a fever, infection, nausea, or chest pain, I need to stop and evaluate them for other indicators of respiratory distress.
If allowed, I would suggest that the client prepare for the expedition by incorporating aerobic exercise such as walking, biking, and swimming, along with resistance training to improve their overall cardiovascular health.
Consider how the cardiovascular and respiratory systems interact. How might a problem with one system cause problems with the other? Explain an example for each.
A problem with the cardiovascular system might not move enough blood to the lungs to be oxygenated nor move enough oxygenated blood to the rest of the body.
A problem with the respiratory system might not allow adequate gas exchange in the alveoli of the lungs to allow the blood stream to acquire the needed oxygen for the body or to remove the waste carbon dioxide from the body.
A construction worker cuts their hand on a bacteria covered, rusted nail. How would the lymphatic, cardiovascular, and immune systems respond?
The immune system activates white blood cells, which are dispersed throughout the body through the bloodstream.
The cardiovascular system carries white blood cells and platelets to the injury to help fight infection and clot the blood to prevent loss.
The cardiovascular system also brings nutrients to help heal the wound and build new cells.
The lymphatic system drains and filters excess fluid that accumulates in the area.
What role do other human body systems, such as the digestive, integumentary, and respiratory systems play in protecting the body? Provide an example for each system that demonstrates how a feature, substance, or action of that system helps keep you well.
The digestive system enables you to take in nutrients such as vitamins as well as the energy your immune system needs to fight off disease.
The digestive system includes the liver, an organ that plays important roles in immune response, including detecting, capturing, and clearing out pathogens.
The integumentary system is the body’s first line of defense, preventing pathogens from entering the blood stream with its tough sheets of skin covered with oils and hairs.
The respiratory system includes mucus-lined membranes within the nose, throat, and lungs that trap pathogens and allow you to cough or sneeze them back out.
Explain how the immune system attempts to protect you from spreading disease.
With help from the innate immune system, the acquired immune system makes special proteins (called antibodies) to protect your body from disease spread through both direct and indirect contact.
After the body is exposed to an infectious agent, antibodies are produced by cells called B lymphocytes.
Describe two ways in which the cow eye and the human eye differ. How are these differences linked to function?
Human eyes do not have a tapetum that helps cows see in the dark.
Cow eyes have an oval-shaped pupil while human pupils are round, which affects the light let in and therefore the images or field of vision the animal or person sees.
conjunctivitis
pink eye
description: Also called pink eye, an infection of the conjunctiva that causes inflammation. Eyes are red and itchy, and may water or have a thick discharge.
cause: Most commonly caused by bacteria or viruses.
treatment: Stop wearing contact lenses until the infection clears. If caused by a bacterial infection, use the prescribed antibacterial eye drops and apply a cool or warm compress to the eye as needed to relieve symptoms.
loasis
description: Also called African eye worm, an infection that sometimes has no or symptoms that appear months after infection.
Symptoms can include the periodic appearance of itchy but not painful swellings, especially near joints, fatigue, muscle and joint pain, and a worm that crawls over the surface of the eye in the conjunctiva.
cause: Caused by a parasitic worm called the Loa loa and passed to humans through bites from deerflies (also known as mango or mangrove flies).
treatment: Eye worms require surgical removal + Diethylcarbamazine or DEC may be prescribed to kill the parasites in the body.
ONCHOCERCIASIS
Description: also called river blindness, a disease with symptoms including impaired vision or blindness caused by recurring conjunctivitis, and infection of the cornea and sclera, itching, rash, or bumps under the skin on the eyelid or around eyelashes.
cause: A parasitic worm called Onchocerca volvulus. The worms are transmitted through bites by blackflies of the genus Simulium, a fly that lives near fast-flowing streams and rivers.
treatment: Ivermectin is prescribed and administered orally to the infected person once or twice a year for 10–15 years.
trachoma
description - An infection that can cause vision impairment and blindness when the eyelid and eyelashes scratch and damage the cornea.
cause - Caused by Chlamydia trachomatis bacteria and spread through direct, personal contact. Primarily found in areas without clean, safe drinking water and sanitation.
treatment options - Surgery to treat the pain and damage of eyelashes scratching the corne, Antibiotics such as Zithromax™ (Z-Pak) to treat active infections, Facial cleanliness such as not touching the face and regularly washing hands and face, and Environmental improvements (ex. better sanitation, clean water supplies, and general good hygiene practices).
TRAUMATIC IRIDODIALYSIS
description - An eye injury where the iris detaches from the structure behind it (the ciliary body, which includes the ciliary muscle and processes). Signs and symptoms include an irregularly shaped pupil, eye pain, and blurry or impaired vision. Can result in glaucoma.
cause - Caused by blunt trauma such as impact from an object.
treatment - Surgical repair of the damage, and some patients may be prescribed eye drops to prevent glaucoma.