9531 Lecture 12- Spinal Cord Injury
1/52
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
53 Terms
What is the organization of the spinal column and spinal cord?
Segmentally organizes→ 31 segments and 31 cords exiting the spine
Cervical
7 vertebrae, but 8 nerve roots
Thoracic
Lumbar
Sacral
Coccygeal
What nerves exit above their corresponding vertebrae?
Cervical
What nerves exit below their corresponding vertebrae?
Thoracic, lumbar, sacral, coccygeal
Where is sensory information located?
dorsal horn
Where does motor information come from?
Ventral horn
UMN Basics/Review
Cell Body originates in the brain
The axons travel from the brain to the brain stem or the ventral (anterior) horn of the spinal cord
Here they synapse with LMN
90% will cross over to the contralateral side at the brainstem, 10% will cross in the spinal cord at the level that they’re exiting
LMN Basics/Review
The cell body od the LMN make up the ventral horn of the spinal cord
Travels from the spinal cord to the muscle they will effect (Efferent fibers)
Below L1, there are no UMN
UMN injuries or lesions react differently than LMN lesions
Where do UMN cross?
Cross over in the pyramidal tracts
Our lateral tract is where our muscle fibres will cross at the brainstem (90%)
Where do motor neurons cross?
The midline at the level of the brainstem or the level of where they exit
Lateral Spinothalamic Tract
Contains sensory neurons for pain and temperature
Will enter and synapse at the same side that they’re sensing
Will cross at the same level and the goes up to the brain where it’s interpreted
Dorsal Column
Fine touch and proprioception
Travels up on the same side as the stimulus before crossing at the brainstem
What is the general motor control by nerve segments?
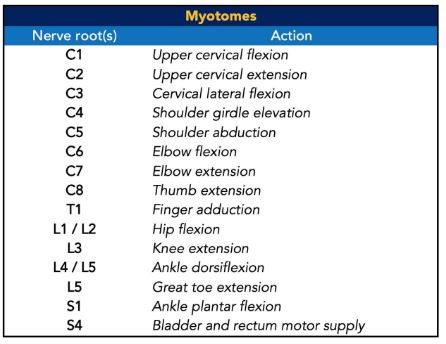
What is the general sensory area by nerve segments?
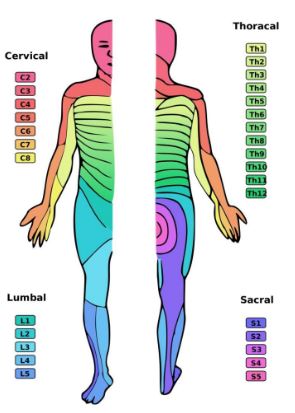
What is a complete SCI?
The absence of sensory and motor below the site of injury
What is an incomplete SCI?
Partial preservation of sensory and/or motor function below the site of injury
What is quadriplegia/tetraplegia?
Involves all four limbs and the trunk
What is paraplegia?
Affects the trunk and all or part of the legs
What is hemiplegia?
Affects one side of the body (left/Right)
What is a grade A SCI?
Complete- no sensory or motor function is preserved below the level of injury
What is a grade B SCI?
Sensory incomplete- Sensory but not motor function is preserved below the neurological level and no motor function is preserved more than three levels below the motor level on either side of the body
What is a grade C SCI?
Motor incomplete- motor function is preserved below the neurological level and more than half of key muscle functions below the neurological level of injury have a muscle grade less than 3
What is a grade D SCI?
Motor incomplete- motor function is preserved below the neurological level and at least half (half or more) of key muscle functions below the NLI have a muscle grade of equal or greater than 3
What is grade E SCI?
Normal- as per testing protocols
What are the grades of the MMT scale?
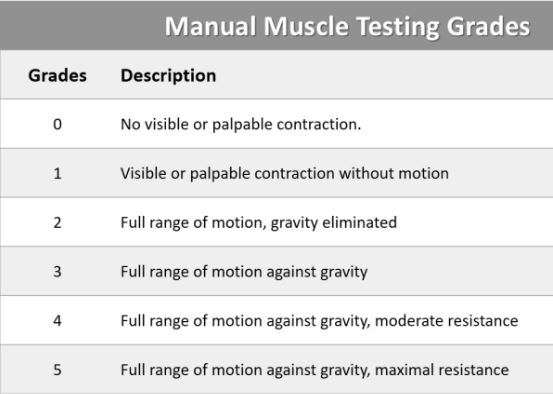
What do injuries above T12 present as?
UMN injuries (but not always)
What do injuries below the T12 tend to present as?
LMN injuries (but not always)
What are symptoms of an UMN vs LMN injury?
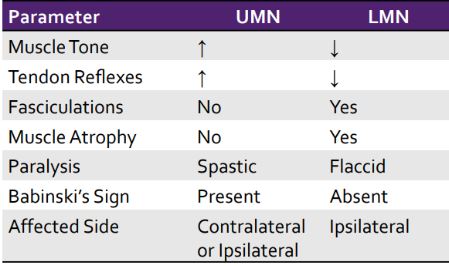
What are primary symptoms of an SCI?
Loss of motor control or coordination
Mobility issues extremely common
Approx. 70% require manual wheeled mobility
Approx. 30% require powered wheeled mobility
Loss of sensation
Depends on the level of the injury and which part of the spinal cord is injured
What are secondary complications of SCI?
Orthostasis (postural hypotension)
Autonomic dysreflexia
Bowel and Bladder dysfunction
Sexual dysfunction
Pressure Ulcers
DVT
Thermal Regulation
Pain
Spasticity & Heterotopic Ossification
Depression
What is orthostasis (postural hypotension)?
Sudden drop in BP when body position changes from lying to sitting or standing.
Additional signs and symptoms
Gray, nausea, dizziness, lightheaded, vision (tunnel/spots)
What are common injuries that occur that cause orthostasis?
More common with injuries above T6 and/or complete injuries
Not enough blood pressure that makes up the difference that occurs do to gravity
Don’t have enough musculature to compress to increase BP as artificial BP
Get someone horizontal to reestablish BP
What is autonomic dysreflexia?
Medical Emergency!
Sudden increase in BP (↑ 20 mmHg SBP )
T6 level or above
Noxious stimulus below level of injury causes massive imbalance in sympathetic discharge.
Presents as sudden onset of:
Throbbing Headache & feelings of anxiety
Profuse sweating, flushing, piloerection
Medical Emergency
Find and remove the cause
Use orthostasis to reduce BP, by sitting them up
Remove or reduce compression (socks, binders, etc.)
Can result in death if it keeps happening
Can be a full bladder, pebble in their shoe, pressure from a wheelchair
Decrease BP by getting someone more upright
Can remove artificial compression aids to decrease BP
What are risks and signs of a deep vein thrombosis (DVT)?
Risk due to:
Reduced circulation caused by lack of muscle contraction
Vascular damage due to low sensation, bumping into something while transferring for example
Prolonged bed rest
Can lead to a thrombotic stroke
Signs:
Swelling in the lower extremities
Localized redness
Low grade fever
What segments involve bowel and bladder injuries?
Sacral segments (S2-4)
What do UMN injuries result in, in terms of the bladder and bowel?
Injuries above T12 (UMN injuries) results in a reflexive (spastic) bowel and bladder
Urinary muscles may contract involuntarily causing “urge” incontinence
Reflexic bowel emptying
What do LMN injuries result in for bladder and bowel?
Flaccid bladder and bowel
Bladder doesn’t contract when full = difficulty annually emptying
Bowel has loss of anal sphincter tightness
A too full bladder will leak causing “overflow” incontinence
Decrease circulation
What is ranked as the top priority for those with paraplegia and #2 for those with quadriplegia?
Difficulty with erection (ED) and ejaculation
Difficulty with vaginal lubrication
Secondary posture and muscular function to engage in sexual intercourse
Can lead to impacts on mental health and self identity
What can spasticity lead to in those who suffer a SCI?
Common following SCI
Triggers can include touch, infection and rapid movements
Can lead to contractures & decreased functional independence
Can develop random unwanted movements
Can be used for purposeful functional movements→ ex. elicit movement from the stretch reflex
What are heterotopic ossifications?
15-20% of SCI cases
Calcification of connective tissue around joints (often shoulder/hip)
Occurs when calcium gets into a tendon
Results from immobility and decrease weight bearing, including passive
Warm swollen joint with limited ROM
What is the impact of thermal regulation on those with SCI?
Thermal regulation is another function ANS
Maintaining body temperature is often the problem for injuries above T6
Poikilothermia: The body will assume the temperature of the environment
Education on heat stroke or hypothermia
Where do pressure ulcers occur in SCI and how quick do they occur?
Most common over boney parts (heels, elbows, hips, base of spine)
90% of individuals, most or all are preventable
Develop gradually over hours or days
From laying down or sitting for a prolonged period of time
Can be from sitting in a wheelchair for a long period of time
What are symptoms of pressure ulcers?
Part of the skin becoming discoloured
Discoloured patches not turning white when pressed
A patch of skin that feels warm, spongy or hard
Pain or itchiness in the affected area
How do we monitor and prevent pressure sores from progressing?
Daily skin checks
Explore pressure relief methods
Changing positions frequently, micro = every 15-20 minutes, macro = every 2-3 hours
Pressure relieves cushions
Postures that reduce pressures in certain areas
What is the impact of pain following an SCI?
Pain is very common after a spinal cord injury
Reported by 75% - 85% of people with a spinal cord injury
Pain is an individual experience
Absence as a signal can be interrupted by pain
Areas of intact sensation
Some can experience phantom limb pain
Can feel muscle pull leading to pain
Can experience pain due to lack of sensation, at or below the level of injury
Burning sensation or painful numbness and tingling, electrical shock
Normal touch can be experienced as pain
What are 2 types of pain we can experience?
Nociceptive pain→ common pain that we experience in the body
Neuropathic → our organs, can experience referred pain
What are respiratory complications in SCI and where do the occur on the spinal cord?
Typically, no issues if the injury is below T12
Injuries above that level compromise the respiratory system to some degree
Diaphragm control → C4, technically C3-C5
Expansion and compression of the rib cage
Postural control for breathing
What difficulties with depression do some individuals experience?
Changes in sleep (too much or too little)
Feeling down or hopeless
Loss of interest or pleasure in activities
Changes in appetite
Diminished energy or activity
Difficulty concentrating or making decisions
Feelings of worthlessness or self-blame
Thoughts of death or suicide
What is anterior cord syndrome?
All motor neurons are travelling mostly anteriorly in our lateral corticospinal tract
Motor paralysis below the level of the lesion and the loss of pain, temperature and deep sensation below the level of the lesion
Likely to still have light touch and proprioception awareness
What is Brown Sequard Syndrome?
Damage to one half or one side of the spinal cord
Puncture wound
Ipsilateral or same side loss of motor function below the level of injury, reduction in deep touch and proprioception
Contralateral loss of pain, temperature and touch
Side with good or better motor control will have better sensation, and vice versa
What is posterior cord syndrome?
Around the dorsal part
Very rare, not many mechanisms that can result in this type of injury
Loss of fine touch and proprioception below the level of lesion
Motor control is likely relatively intact
What is central cord syndrome?
More common forms of incomplete spinal cord injury
From an extension injury of the cervical spine level
90% or more will be at the cervical level
Results in sensory loss below the site of the injury including bladder control
Tingling, burning or dull ache
Impairment in the arms, hands or lesser extent then in the legs
What is cauda equina syndrome?
No Damage to the cord itself, but to the nerves that extend below it from L1/L2
Generally incomplete injuries since it isn’t one cord that can be injured
Symptoms:
Loss of motor function and sensation below the level of injury
Absence of reflex arc
LMN type motor paralysis
Flaccid paralysis
Which complications of occur above neurological injury T6?
Orthostasis (Postural Hypotension)
Autonomic dysreflexia
Temperature dysregulation